Abstract
Post-transplant diabetes mellitus (PTDM) worsens outcomes after kidney transplantation, and immunosuppression agents contribute to PTDM. We have previously shown that tacrolimus (TAC) and sirolimus (SIR) cause hyperglycemia in normal rats. While there is little data on the mechanism for immunosuppressant-induced hyperglycemia, we hypothesized that the TAC and SIR-induced changes are reversible. To study this possibility, we compared normal rats treated for 2 weeks with either TAC, SIR, or a combination of TAC and SIR prior to evaluating their response to glucose challenge, with parallel groups also treated for 2 weeks after which treatment was stopped for 4 weeks, prior to studying their response to glucose challenge. Mean daily glucose and growth velocity was decreased in SIR, and TAC+SIR-treated animals compared to controls (P < 0.05). TAC, SIR, and TAC+SIR treatment also resulted in increased glucose response to glucose challenge, compared to controls (P < 0.05). SIR-treated animals also had elevated insulin concentrations in response to glucose challenge, compared to controls (P < 0.05). Insulin content was decreased in TAC and TAC+SIR, and islet apoptosis was also increased after TAC+SIR treatment (P < 0.05). Four weeks after treatments were stopped, all differences resolved between groups. In conclusion, TAC, SIR, and the combination of TAC+SIR-induced changes in glucose and insulin responses to glucose challenge that were accompanied by changes in islet apoptosis and insulin content. These changes were no longer present 4 weeks after cessation of therapy suggesting immunosuppressant-induced changes in glucose metabolism are likely reversible.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Post-transplant diabetes mellitus (PTDM) increases allograft dysfunction and cardiovascular morbidity and mortality after kidney transplant [1, 2]. Tacrolimus (TAC) and sirolimus (SIR) are among the most commonly used immunosuppression drugs for kidney transplantation, and have been strongly implicated in the etiology of PTDM [3]. We have previously shown that both TAC and SIR, individually and in combination, cause hyperglycemia and hyperinsulinemia in normal male Sprague–Dawley rats after short-term treatment [4]. There is some clinical evidence that pancreatic pathology observed with toxic levels of tacrolimus improve once the dose is decreased, and changing immunosuppressant regimen from tacrolimus to other drugs can result in improvements in glucose management [5, 6]. With this background, we have hypothesized that immunosuppressant-induced hyperglycemia is reversible. To evaluate this further, we have compared groups of rats treated for 2 weeks with TAC, SIR or a combination of TAC+SIR with rats treated with the same doses and duration of immunosuppressants, who then had no treatment for 4 weeks.
Results
Daily glucose and weight were monitored during treatment with TAC, SIR, or TAC+SIR. As observed previously, TAC, SIR, and TAC+SIR-treated animals had less weight gain compared to controls (Fig. 1; P < 0.01). Mean daily glucose was elevated overall in SIR or TAC+SIR-treated animals, compared to controls, but not enough to explain the lack of weight gain (Fig. 2; P < 0.05). After 2 weeks treatment, an oral glucose challenge was performed after an overnight fast. Fasting glucose was higher in TAC-treated animals as compared to controls (Fig. 3a; P < 0.05). Fasting insulin was lower in TAC-treated animals (compared to SIR-treated animals) and TAC+SIR-treated animals (compared to SIR-treated animals and controls) (Fig. 3b; P < 0.05). Insulin resistance was assessed by calculating homeostasis model assessment of insulin resistance (HOMA-IR). HOMA-IR was significantly lower in TAC+SIR-treated animals compared to the other groups (Fig. 3c; P < 0.05).
Fasting glucose, insulin, and HOMA-IR after 2 weeks treatment. a Fasting glucose was higher in TAC-treated animals as compared to controls (* P < 0.05), b Fasting insulin was lower in TAC-treated animals (compared to SIR-treated animals) and TAC+SIR-treated animals (compared to SIR-treated animals and controls) (* P < 0.05), c HOMA-IR was significantly lower in TAC+SIR-treated animals compared to the other groups (* P < 0.05)
The glucose response to glucose challenge was greater in animals treated with TAC, SIR or TAC+SIR compared to controls (Fig. 4a; P < 0.05). The SIR-treated animals, but not TAC or TAC+SIR, also had a significantly increased insulin response to oral glucose challenge, as well (Fig. 4b; P < 0.05 compared to control and TAC+SIR). Animals were then killed and the pancreata were evaluated for islet area, number, apoptosis, and insulin content. Islet area and number were not different between groups, but insulin immunofluorescence staining was reduced in rats treated with TAC+SIR and TAC, compared to those treated with control or SIR (Fig. 5a). Glucagon content was not different (data not shown). Islet apoptosis was also significantly higher in TAC+SIR-treated animals compared to TAC, SIR, or controls (Fig. 9).
Immunosuppressant concentrations were measured after 2 weeks of treatment. SIR concentration was 24 ± 5 ng/ml and TAC concentration was 14 ± 4 ng/ml in the SIR and TAC groups, respectively, and SIR and TAC concentrations were 19 ± 3 ng/ml and 15 ± 5 ng/ml, in the TAC+SIR group.
These results were compared to groups of rats who were treated at the same time with the same immunosuppressant medications and doses for 2 weeks, prior to stopping treatment for 4 weeks. Random blood glucose in all treatment groups returned to those of the controls by 3 weeks after treatment was stopped (Fig. 6). Weight also increased similar to controls in all groups once treatment was stopped (data not shown). Fasting glucose on the day of the oral glucose challenge was the same as controls, or lower in SIR-treated animals (Fig. 7a; P < 0.05). Fasting insulin was no longer different between groups (data not shown), and HOMA-IR was significantly lower in SIR-treated animals after 6 weeks compared to 2 weeks, suggesting improved sensitivity (Fig. 7b; P < 0.05). Glucose response to glucose challenge was no longer increased compared to controls in all groups (Fig. 8a). Insulin response to oral glucose challenge was now decreased in all treatment groups compared to controls even though glucose response was normal (Fig. 8b; P < 0.05) suggesting increased sensitivity, as also suggested by the HOMA-IR results, especially in SIR-treated animals (Fig. 7b).
Random blood glucose before and after immunosuppressant treatment. Mean glucose concentration is shown for each group. Treatment was given days 0–14. The last day of treatment is shown by a vertical line. Injections were then stopped, with results shown after treatment cessation. *** P < 0.05 compared to control
Fasting glucose and HOMA-IR. a Fasting glucose normalized in all groups after 4 weeks of cessation of therapy, but was significantly lower in SIR-treated animals, compared to controls (* P < 0.05). b HOMA-IR was significantly higher in SIR-treated rats after 2 weeks compared to the group treated for 2 weeks, followed by 4 weeks of no treatment. * P < 0.05 versus rats treated for 2 weeks with SIR
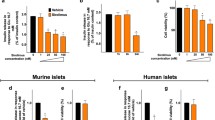
Glucose and insulin responses to oral glucose challenge 4 weeks after cessation of treatment. a Mean glucose concentration is shown. There were no significant differences between groups. b Insulin AUCs, expressed in arbitrary units, for the four treatment groups are shown (mean ± SEM). Insulin concentrations were significantly lower in all treatment groups as compared to controls. ** P < 0.005 compared to controls, * P < 0.05 compared to controls
Changes in the pancreas were also resolved 4 weeks after cessation of therapy. Islet number and area and insulin staining (Fig. 5b) were not different between groups 4 weeks after cessation of therapy, and islet apoptosis significantly decreased in the TAC+SIR-treated animals (Fig. 9). As expected, no animal had measurable levels of immunosuppressant drugs after the 4 week hiatus in immunosuppressant treatment.
Discussion
New onset diabetes after transplantation or PTDM has been recognized as a potential consequence of organ transplantation in many recipients. PTDM is associated with increased risk of graft failure, and fatal and nonfatal cardiovascular disease in kidney transplant recipients [1, 2]. While in the past, various definitions have been used, the 2003 International Consensus Guidelines developed criteria for PTDM that were based on the American Diabetes Association criteria for diagnosis of diabetes in non-transplant patients [2]. While the incidence of PTDM is still argued and may depend on specific immunosuppressant protocols and pre-existing risk for type 2 diabetes, a recent retrospective analysis of consecutive non-diabetic patients who received kidney transplantation found the incidence of PTDM to be as high as 74% using the new consensus criteria [3].
The etiology of PTDM is multifactorial, but one clear contributing factor is the use of immunosuppressant medications. In fact, immunosuppressant medication was the strongest risk factor for development of PTDM in one retrospective study [3]. Tacrolimus and cyclosporine have been clearly associated with increased risk; in fact, many studies have demonstrated the diabetogenicity of calcineurin inhibitors, tacrolimus and cyclosporine [2, 3, 7–9]. Generally, randomized trials have shown that TAC has a stronger association with onset of PTDM than cyclosporine [10]. Data from United States renal database in 2002 showed the 2 year incidence of PTDM after KTX was approximately 8% in the cyclosporine group compared to 18% in the TAC group [11]. A recent study showed that 33% of KTX recipients had prediabetes as suggested by impaired glucose tolerance and 20% had PTDM by 1 year of transplant using TAC-based therapy [12].
While past studies have been inconsistent, recent studies have also implicated sirolimus in PTDM, as well [3]. For example, retrospective studies of kidney transplant recipients did not show an association between SIR and increased risk of PTDM [13, 14]. However, using data from the United States renal database, SIR was independently associated with increased onset of PTDM in patients with KTX [15]. SIR has been linked to a defect in insulin secretion as well as insulin resistance, and exerts antiproliferative effects on multiple cell types including pancreatic ductal cells and endothelial cells in vitro [16]. SIR not only impairs in vivo proliferation of islet beta cells in a pregnant murine model but high doses of SIR can also cause apoptosis in rat and human islets [17, 18].
We have previously shown that both TAC, and particularly SIR, can increase both glucose and insulin, in a dose-dependent manner, suggesting insulin resistance [4]. Clinically, insulin resistance has been reported to be more prevalent in patients with TAC-based than cyclosporine-based immunosuppression [19]. In these studies, we observed greater hyperinsulinemia with SIR than with TAC. In fact, SIR is well known to cause hypertriglyceridemia in clinical settings, as expected with insulin resistance [20]. SIR also worsened hyperglycemia and hyperinsulinemia in diabetic P obesus rats which further supports an effect of sirolimus on insulin action [21].
In the present studies, we confirmed that both TAC and SIR caused hyperglycemia, accompanied by significant elevations in insulin concentration with SIR treatment. Immunosuppressant treatment resulted in less weight gain, as has been described in other studies, most likely due to their direct effects on cell growth and anabolism than uncontrolled glucose concentration as the glucose elevations, while significant, were generally mild [22].
The short-term effects of these medications on insulin resistance, insulin secretion, and pancreatic insulin content were reversed within 4 weeks. Random glucose significantly improved within 3 weeks of stopping therapy. After 4 weeks, an oral glucose challenge no longer showed an exaggerated glucose response compared to controls. Hyperinsulinemia in SIR-treated animals also resolved after treatment cessation, although insulin still increased appropriately to a glucose load. This data, including a decrease in HOMA-IR in 6 weeks compared to 2 week animals, suggests improved insulin sensitivity after treatment was stopped. Weight increased toward control values as soon as immunosuppressant treatment was stopped. These results altogether suggest the toxic effects of these drugs are reversible, just as cytoplasmic swelling and vacuolization, observed with tacrolimus and cyclosporine were reversible with lowered drug dose, and hyperglycemia appeared to resolve with changing tacrolimus to other medications in retrospective studies [5, 6, 23].
Calcineurin inhibitor-associated PTDM has been suggested to impair insulin secretion [24]. Animal models of calcineurin inhibitor treatment showed decreased glucokinase activity and reduced insulin gene expression, with resultant decrease in insulin secretion [25–27]. One potential mechanism for tacrolimus inhibition of insulin secretion is through inhibition of PKC-mediated (Ca2+-dependent and independent) and Ca2+-independent GTP signaling pathways [28]. Tacrolimus may also have direct toxic effects on islets as suggested in pancreas transplant recipients [23].The mechanism for sirolimus effects is less clear, but sirolimus has antiproliferative effects on multiple cell types, including pancreatic ductal cells and endothelial cells in vitro [16]. In our studies, the combination of TAC and SIR, in particular, significantly increased islet apoptosis. After immunosuppression was stopped, all effects resolved, including hyperglycemia, decreased pancreatic insulin content, and apoptosis, and insulin sensitivity was even greater than controls. These results strongly suggest that the effects of short-term TAC and SIR treatment are reversible.
In conclusion, we have confirmed that tacrolimus, and sirolimus, alone and in combination, cause hyperglycemia in previously normal adult rats. The mechanism involved insulin resistance in SIR-treated animals, as it was accompanied by hyperinsulinemia and increased HOMA-IR, and decreased insulin secretion with tacrolimus treatment, and accelerated islet apoptosis after combination therapy. However, 4 weeks after treatment was stopped, all effects, including changes observed in the islets themselves, were reversed. Whether longer term treatment could lead to changes that are no longer reversible is as yet unknown.
Materials and methods
Animal care
The protocol was approved by the Research and Development Committee of the Omaha Veterans Affairs Medical Center. Adult, male Sprague–Dawley rats (150–200 g) were kept under 12 h dark and light periods and fed standard lab chow except prior to fasting samples (2 and 6 weeks) when food but not water was removed for 12 h.
Experimental design
Two groups of animals (n = 5/group) were each given one of four daily treatment regimens for a total of eight groups. Two groups received daily tacrolimus and diluent (4 mg/kg/day; LC Laboratories, Woburn, MA) subcutaneously for 2 weeks. Two groups received daily sirolimus and diluent (2 mg/kg/day; LC Laboratories, Woburn, MA) subcutaneously for 2 weeks. Two groups received a daily subcutaneous injection of tacrolimus (1 mg/kg/day) and sirolimus (0.08 mg/kg/day) for 2 weeks. Finally, two groups received two injections of diluent daily (10% ethanol/sunflower oil) and served as the control (C) group. These drug doses were chosen based on our previously published studies as sub-maximal doses for causing hyperglycemia [4]. While all animals received treatment for 2 weeks, half of the groups were studied immediately after the 2 weeks treatment while the other half were kept for four more weeks, without further injections before being studied. Daily weights and random blood glucoses were measured by glucometer (Ultra®).
After 2 weeks of treatment, an oral glucose challenge was performed on one group from each treatment regimen (1 g/kg by gavage) prior to kill. Twelve hours before the glucose challenge, food but not water was removed from the animals so they would be fasting. Glucose and insulin were measured from blood taken by tail vein prior to administration of the glucose load. Blood was removed from the tail vein for glucose and insulin measurements 15, 30, 60, and 120 min after glucose load. These groups were then killed and pancreata harvested for further analysis.
The remaining groups received no further treatment for four more weeks. Daily weights and random glucoses were measured. After 4 weeks, animals were studied with an oral glucose challenge prior to kill. Subsequently pancreata were harvested for further analysis.
Insulin and immunosuppressant concentrations
Plasma insulin concentration was measured by radioimmunoassay (Linco Research: St. Charles, MO) with sensitivity of 0.1 ng/ml, and no cross reactivity with proinsulin. Tacrolimus and sirolimus concentrations were performed on whole blood samples by liquid chromatography–tandem mass spectrometry 24 h after last injection in lysed specimens by the Clinical Laboratory of The Nebraska Medical Center [29]. Intra-assay variations were 3.5 and 3.9%, and interassay variations were 2.7 and 5.0%, for tacrolimus and sirolimus, respectively. Insulin resistance was evaluated with the homeostasis model assessment of insulin resistance (HOMA-IR; fasting glucose (mmol/l) × fasting insulin (μu/l)/22.5) [30].
Pancreas histology, apoptosis and hormone content
Pancreata were harvested after killing, placed in formalin, fixed, and set in paraffin blocks. Sections were cut and then processed in one of three ways. Some were stained with hematoxylin and eosin (H&E) for light microscopy. All islets in each pancreatic section were photographed at 2× magnification and analyzed at 20× magnification. Image J software was used to calculate islet area (NIH, Bethesda, MD). Area values were calculated in square pixels and converted to square micrometers.
The remainder were processed to assess apoptosis, and to assess insulin and glucagon content by immunofluorescence. Apoptosis was assessed by the terminal deoxynucleotidyl transferase-mediated dUTP-biotin nick end of DNA fragments (TUNEL) method (DeadEnd Colorimetric TUNEL System, Promega, Madison, WI). Mean number of apoptotic cells/islet was compared between groups.
Immunofluorescence was performed by subjecting pancreatic sections to antigen retrieval by first autoclaving for 15 min in Antigen Unmasking Solution (Vector Labs, Burlingame, CA), blocking in 5% goat serum for 30 min, then incubating them with specific anti-insulin (Dako Cytomation, Carpinteria, CA) or anti-glucagon antibodies (Cell Signaling Technology, Danvers, MA) prior to incubation with the designated fluorescence-linked second antibody, prior to visualization by fluorescence microscopy, compared between groups.
Number of islets, mean islet area, and number of islets exhibiting apoptosis were measured or calculated by a blinded reviewer in each pancreatic slide section. All calculations were made by a blinded reviewer.
Statistical analysis
Change in weight between groups over time was compared by two-way analysis of variance (ANOVA). Bonferroni test was used for post-test analysis. Differences between groups in fasting glucose, insulin, HOMA-IR, islet area, and apoptotic cells/islet were compared by one-way ANOVA with Tukey’s multiple comparison tests for post-hoc differences. Differences between groups over time in HOMA-IR and apoptotic cells/islet were compared by two-way ANOVA, with Bonferroni test for post-test analysis. Glucose and insulin concentration responses to oral glucose load were calculated as area under the curve, and compared by one-way ANOVA with Tukey’s multiple comparison tests for post-hoc differences. A P value < 0.05 was considered significant. All data represented by mean ± SEM, unless otherwise specified.
References
J. Hjelmesaeth, A. Hartmann, T. Leivestad, H. Holdaas, S. Sagedal, M. Olstad et al., The impact of early-diagnosed new-onset post-transplantation diabetes mellitus on survival and major cardiac events. Kidney Int. 69(3), 588–595 (2006)
J. Davidson, A. Wilkinson, J. Dantal, F. Dotta, H. Haller, D. Hernandez et al. New-onset diabetes after transplantation: 2003 International consensus guidelines. in Proceedings of an International Expert Panel Meeting, Barcelona, Spain, 19 February 2003. Transplantation 75(10 Suppl), SS3–24 (2003)
E. Sulanc, J.T. Lane, S.E. Puumala, G.C. Groggel, L.E. Wrenshall, R.B. Stevens, New-onset diabetes after kidney transplantation: an application of 2003 international guidelines. Transplantation 80(7), 945–952 (2005)
J.L. Larsen, R.G. Bennett, T. Burkman, A.L. Ramirez, S. Yamamoto, J. Gulizia et al., Tacrolimus and sirolimus cause insulin resistance in normal sprague dawley rats. Transplantation 82(4), 466–470 (2006)
L. Ghisdal, N.B. Bouchta, N. Broeders, L. Crenier, A.D. Hoang, D. Abramowicz et al., Conversion from tacrolimus to cyclosporine A for new-onset diabetes after transplantation: a single-centre experience in renal transplanted patients and review of the literature. Transpl. Int. 21(2), 146–151 (2008)
M. Ramos-Cebrian, J.V. Torregrosa, A. Gutierrez-Dalmau, F. Oppenheimer, J.M. Campistol, Conversion from tacrolimus to cyclosporine could improve control of posttransplant diabetes mellitus after renal transplantation. Transplant. Proc. 39(7), 2251–2253 (2007)
Randomised trial comparing tacrolimus (FK506) and cyclosporin in prevention of liver allograft rejection. European FK506 Multicentre Liver Study Group. Lancet 344(8920), 423–428 (1994)
J.D. Pirsch, J. Miller, M.H. Deierhoi, F. Vincenti, R.S. Filo, A comparison of tacrolimus (FK506) and cyclosporine for immunosuppression after cadaveric renal transplantation. FK506 Kidney Transplant Study Group. Transplantation 63(7), 977–983 (1997)
F.G. Cosio, T.E. Pesavento, K. Osei, M.L. Henry, R.M. Ferguson, Post-transplant diabetes mellitus: increasing incidence in renal allograft recipients transplanted in recent years. Kidney Int. 59(2), 732–737 (2001)
F. Vincenti, S. Friman, E. Scheuermann, L. Rostaing, T. Jenssen, J.M. Campistol et al., Results of an international, randomized trial comparing glucose metabolism disorders and outcome with cyclosporine versus tacrolimus. Am. J. Transplant. 7(6), 1506–1514 (2007)
R.S. Woodward, M.A. Schnitzler, J. Baty, J.A. Lowell, L. Lopez-Rocafort, S. Haider et al., Incidence and cost of new onset diabetes mellitus among U.S. wait-listed and transplanted renal allograft recipients. Am. J. Transplant. 3(5), 590–598 (2003)
E. Porrini, J.M. Moreno, A. Osuna, R. Benitez, I. Lampreabe, J.M. Diaz et al., Prediabetes in patients receiving tacrolimus in the first year after kidney transplantation: a prospective and multicenter study. Transplantation 85(8), 1133–1138 (2008)
Y.S. Chien, Y.T. Chen, C.H. Chuang, Y.T. Cheng, F.R. Chuang, H. Hsieh, Incidence and risk factors of new-onset diabetes mellitus after renal transplantation. Transplant. Proc. 40(7), 2409–2411 (2008)
M. Veroux, D. Corona, G. Giuffrida, M. Gagliano, M. Sorbello, C. Virgilio et al., New-onset diabetes mellitus after kidney transplantation: the role of immunosuppression. Transplant. Proc. 40(6), 1885–1887 (2008)
O. Johnston, C.L. Rose, A.C. Webster, J.S. Gill, Sirolimus is associated with new-onset diabetes in kidney transplant recipients. J. Am. Soc. Nephrol. 19(7), 1411–1418 (2008)
C.T. Bussiere, J.R. Lakey, A.M. Shapiro, G.S. Korbutt, The impact of the mTOR inhibitor sirolimus on the proliferation and function of pancreatic islets and ductal cells. Diabetologia 49(10), 2341–2349 (2006)
E. Bell, X. Cao, J.A. Moibi, S.R. Greene, R. Young, M. Trucco et al., Rapamycin has a deleterious effect on MIN-6 cells and rat and human islets. Diabetes 52(11), 2731–2739 (2003)
E. Zahr, R.D. Molano, A. Pileggi, H. Ichii, S.S. Jose, N. Bocca et al., Rapamycin impairs in vivo proliferation of islet beta-cells. Transplantation 84(12), 1576–1583 (2007)
W. Sui, H. Zou, G. Zou, Q. Yan, H. Chen, W. Che et al., Clinical study of the risk factors of insulin resistance and metabolic syndrome after kidney transplantation. Transpl. Immunol. 20(1–2), 95–98 (2008)
H.A. Hakeam, A.H. Al-Jedai, S.M. Raza, K. Hamawi, Sirolimus induced dyslipidemia in tacrolimus based vs. tacrolimus free immunosuppressive regimens in renal transplant recipients. Ann. Transplant. 13(2), 46–53 (2008)
M. Fraenkel, M. Ketzinel-Gilad, Y. Ariav, O. Pappo, M. Karaca, J. Castel et al., mTOR inhibition by rapamycin prevents beta-cell adaptation to hyperglycemia and exacerbates the metabolic state in type 2 diabetes. Diabetes 57(4), 945–957 (2008)
J.J. Gibbons, R.T. Abraham, K. Yu, Mammalian target of rapamycin: discovery of rapamycin reveals a signaling pathway important for normal and cancer cell growth. Semin. Oncol. 36(Suppl 3), S3–S17 (2009)
C.B. Drachenberg, D.K. Klassen, M.R. Weir, A. Wiland, J.C. Fink, S.T. Bartlett et al., Islet cell damage associated with tacrolimus and cyclosporine: morphological features in pancreas allograft biopsies and clinical correlation. Transplantation 68(3), 396–402 (1999)
M.F. Crutchlow, R.D. Bloom, Transplant-associated hyperglycemia: a new look at an old problem. Clin. J. Am. Soc. Nephrol. 2(2), 343–355 (2007)
E. Oetjen, D. Baun, S. Beimesche, D. Krause, I. Cierny, R. Blume et al., Inhibition of human insulin gene transcription by the immunosuppressive drugs cyclosporin A and tacrolimus in primary, mature islets of transgenic mice. Mol. Pharmacol. 63(6), 1289–1295 (2003)
R.G. Radu, S. Fujimoto, E. Mukai, M. Takehiro, D. Shimono, K. Nabe et al., Tacrolimus suppresses glucose-induced insulin release from pancreatic islets by reducing glucokinase activity. Am. J. Physiol. Endocrinol. Metab. 288(2), E365–E371 (2005)
J.B. Redmon, L.K. Olson, M.B. Armstrong, M.J. Greene, R.P. Robertson, Effects of tacrolimus (FK506) on human insulin gene expression, insulin mRNA levels, and insulin secretion in HIT-T15 cells. J. Clin. Invest. 98(12), 2786–2793 (1996)
Y. Uchizono, M. Iwase, U. Nakamura, N. Sasaki, D. Goto, M. Iida, Tacrolimus impairment of insulin secretion in isolated rat islets occurs at multiple distal sites in stimulus-secretion coupling. Endocrinology 145(5), 2264–2272 (2004)
A. Volosov, K.L. Napoli, S.J. Soldin, Simultaneous simple and fast quantification of three major immunosuppressants by liquid chromatography–tandem mass-spectrometry. Clin. Biochem. 34(4), 285–290 (2001)
R. Muniyappa, H. Chen, R. Muzumdar, F.H. Einstein, X. Yan, L.Q. Yue et al., Comparison between surrogate indexes of insulin sensitivity/resistance and hyperinsulinemic euglycemic clamp estimates in rats. Am. J. Physiol. Endocrinol. Metab. 297, E1023–E1029 (2009)
Acknowledgment
We deeply appreciate the secretarial assistance of Pamela Welch and Mary Monaghan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Shivaswamy, V., McClure, M., Passer, J. et al. Hyperglycemia induced by tacrolimus and sirolimus is reversible in normal sprague–dawley rats. Endocr 37, 489–496 (2010). https://doi.org/10.1007/s12020-010-9332-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-010-9332-6