Abstract
The present research assessed the effects of lettuce glycoside B (LGB), a compound separated and purified from Pterocypsela laciniata, on irradiation-induced pulmonary fibrosis and explored the mechanism involved. Animal model of irradiation exposure inducing pulmonary fibrosis was established by Co irradiator. Rats were intraperitoneally treated with LGB (100, 200 and 400 mg/kg) once per day for a month. Lung index data were analyzed. The levels of fibrosis were assessed by hydroxyproline (Hyp) of pulmonary and lung tissue sections after irradiation exposure. Alveolitis and fibrosis levels were calculated from semi-quantitative analysis of hematoxylin and eosin and Masson’s trichrome lung section staining. The serum levels of transforming growth factor β1 (TGF-β1), interleukin (IL)-6, and tumor necrosis factor-α (TNF-α) were also evaluated. Antioxidant enzymes of superoxide dismutase (SOD) were measured in serum. Moreover, we also measured serum malondialdehyde (MDA) levels, a marker of oxidative stress. Treatment with LGB significantly reduced mortality rates and lung index scores and MDA content, enhanced SOD and other antioxidant enzymes activity, and regulated serum levels of TGF-β1, IL-6, and TNF-α. These results demonstrated that LGB significantly inhibited irradiation-induced pulmonary fibrosis. Furthermore, the results suggested promising clinical effect of LGB therapies for treating irradiation-induced pulmonary fibrosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pulmonary fibrosis induced by irradiation is a common complication related to full body irradiation induced by hematopoietic stem cell transplantation, nuclear accidents, and thoracic radiotherapy for cancers like lung carcinoma, breast carcinoma, thymoma, and lymphoma [1, 2]. These complications develop for about half a year at least to several years after radiation damage in humans and about 3 months after irradiation exposure in mice [1, 3]. Recently, clinical research statistics have indicated that the irradiation associated pulmonary fibrosis rate among people with carcinoma that accept irradiation exposure is getting significantly higher [1, 3]. The convention therapy for pulmonary fibrosis mainly includes chemical agents like steroid agents, NSAID, and immunosuppressive drugs [1, 4, 5]. These kinds of agents could effectively ameliorate pneumonitis in acute phase after irradiation for about 3 months [1, 4, 5]. However, they cannot successfully ameliorate fibrosis symptoms [1]. Moreover, immunosuppressive drugs could lead to various adversary side effects that may even cause death among patients [1, 4, 5]. When people are exposed to radiation, oxidative stress happens immediately, and it endures throughout the whole process of this radiation damage [1–3, 6]. It is indicated that radiation could activate the oxidant generating associated enzymes, mitochondrial leakage. Moreover, it could activate the respiratory burst in the phagocytic cells, and eventually lead to the infiltration of damaged tissue [1–3, 6]. So it is suggested that antioxidant therapy tactics were the most promising treatment methods to antagonize the irradiation-induced pulmonary fibrosis [1–3, 6].
Lettuce glycoside B (LGB) is a compound grown in Henan Province of China, and later separated and purified by scientists from Pterocypsela laciniata [7]. It is a kind of sesquiterpene glycoside and is completely soluble in water [7]. Pterocypsela laciniata belongs to Pterocypsela plant of Asteraceae [7]. As a very popular traditional Chinese herbal medicine, it has various effects, such as repulsion of heat (in Chinese medicine term) and acceleration of blood circulation in human body [7]. However, various pharmacological effects of LGB and the related mechanism so far are rarely explored. It should be noted that LGB was reported to have effects toward cerebral ischemia reperfusion injury induced by middle cerebral artery occlusion [7]. Scientists measured brain histopathology and brain infarct rate to evaluate the effects of LGB on brain ischemia injury and found that it was very effective agent to cure that injury [7]. Besides, the expressions of nerve growth factor (NGF) and neurotrophin-3 (NT-3) were also significantly upregulated by LGB [7]. However, no studies have been conducted to clarify the pharmacological effects in pulmonary fibrosis models treated with LGB.
For antagonizing oxidative stress induced by reactive oxygen species (ROS), lung cells activate a wide range of endogenous antioxidant enzymes including glutathione peroxidase (GSHPx), superoxide dismutase (SOD) and catalase (CAT) [1, 3, 4, 6]. The transcription of the antioxidant enzymes is regulated by nuclear transcription factor NF-E2-related factor 2 (Nrf2), and it plays important roles in the modulation of oxidative stress environment [1, 3, 4, 6]. In normal homeostatic environment, Nrf2 transcription is suppressed by negative regulator Kelch-like ECH-associated protein 1 (Keap1) [1, 3]. But after exposure to ROS, Nrf2 separates from cytosolic Keap1 and translocates to nucleus, in which it combines with the antioxidant response element (ARE) in the promoter regions of various genes that are responsible for the expression of antioxidant enzymes and activate the their transcription [1, 3].
In the current research, we speculated that the LGB treatment could effectively antagonize irradiation exposure-induced pulmonary fibrosis. Firstly, we assessed the activities of LGB to inhibit irradiation-induced pulmonary fibrosis and then evaluated whether LGB therapy affected the expression of endogenous antioxidant enzymes including SOD in animal models. As far as we know, this study is the first to explore the treatment efficacy of LGB in irradiation-induced pulmonary fibrosis in vivo.
Materials and Methods
Animals
Male Sprague-Dawley (SD) rats weighing 180–220 g were used in our current research (purchased from Experimental Animal Center, Shanghai, China). They were housed in an SPF-graded animal care facility according to the guidelines of the Care and Use of Laboratory Animals of our hospital. The Committee on the Ethics of Animal Experiments of our hospital approved all the experiment procedure. All interceptive treatment was processed under fluothane anesthesia. During the experiments, all the efforts were made to minimize the suffering of the animals. The rats were allowed free access to food and water. All rats were caged in a well-controlled SPF environment with a 12/12-h light/dark cycle, and observed once per day for 4 months after irradiation exposure. The natural death of the animals was recorded. And during the experiments, we have paid special attention to abnormalities in breathing, fur ruffling, hunched posture, and breathing rate decline.
Irradiation Exposure and Drug Treatment
A 60Co irradiator was used to generate gamma-ray radiation [1]. The rats were irradiated to 22 Gy at a dose rate of 290 cGy/min, and the radiation beam was restricted to the entire thorax [1]. The irradiated rat models were intraperitoneally injected with LGB (100, 200 and 400 mg/kg, Aladdin, China) once per day for a month. Another group of irradiated rats received radiation without any treatment. The control group rats were serviced by normal food, and they were not exposed in irradiation.
Histopathology Process
After body weight assessment, all rats were sacrificed at 4 month after the first irradiation. Both lungs were weighed and evaluated. The left lungs were frozen with liquid nitrogen and kept at −70 °C for further experiments. The right lungs were fixed with 4 % paraformaldehyde for histological assessment and immunohistochemical evaluation. Rat blood samples were collected from the heart and let to clot for 1 h at room temperature. Serum samples were collected by centrifugation at 4,500 rpm for 5 min at 4 °C. Then they were stored at −70 °C for further experiments.
Lung Index Measurement
The ratio of the wet lung weight to body weight was applied as the lung index calculation formula [1].
Collagen Content Assessment
Lung collagen content was evaluated by the hydroxyproline (Hyp) assessment kit according to the manufacturer’s protocol (Boster, China). Briefly, 100 mg of lung tissue was hydrolyzed in 1 ml of lysis buffer solution at 100 °C for about 20 min, and the final absorbance was then measured at 550 nm.
MDA Content and SOD Activity Measurements
Serum samples were evaluated for MDA content and SOD activity by commercially available kits following by the manufacturer’s protocol instructions (Boster, China). MDA is an end product of ROS-induced peroxidation of cell membrane lipids [1]. It is a stable and reliable marker of oxidative stress damage [1]. MDA content was quantified by chromogen generation assessment of the chemical reaction between MDA and 2-thiobarbituric acid [1]. SOD activity was assessed by observing the sample’s ability to inhibit the reduction of ferricytochrome c via xanthine/xanthine oxidase [1]. Overall, this method is dependent on the inhibition of nitroblue tetrazolium (NBT) reduction via the xanthine/xanthine oxidase system [1].
Cytokine Levels Assessment
Serum levels of TGF-β1, IL-6, and TNF-α were determined using the commercially available TGF-β1, IL-6, and TNF-α ELISA kit according to the manufacturer’s protocol instructions (Beyotime, China). The OD value was determined at 450 nm using an ELISA reader and calculated at the linear portion of the curve.
Statistical Analysis
All experiments were performed at least in triplicates. Each group consisted of at least 10 rats. One-way analysis of variance (ANOVA) was performed and Tukey post hoc test was applied for multiple group comparison. Statistical analyses were performed using the SPSS 13.0 program. The results are expressed as mean ± SEM. Differences of p < 0.05 were considered statistically significant.
Results
LGB Reduced Mortality and Inhibited Fibrous Nodules
Irradiated rats with LGB treatment had a lower mortality rate compared with those without any treatment (data not shown). All control rats survived until the end of 4 months. Signs of congested edema were significantly ameliorated in LGB-treated pulmonary tissues compared with those in the groups without treatment. Four months post-irradiation exposure, the lungs of LGB-treated rats showed signs of edema and uneven surfaces as well as scattered punctuate bleeding points same as the model group, but the severity is significantly decreased than that of the untreated rats (data not shown).
LGB Reduced the Lung Index Score
We then tried to find out whether LGB treatments affected the lung index, which refers to the ratio of lung wet weight to body weight. The lung index was significantly lower (p < 0.05) in LGB-treated animals relative to model group at 120 days post-irradiation (Fig. 1). These results indicated that LGB could significantly attenuate congested edema in pulmonary tissues post-irradiation.
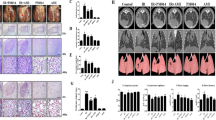
Effects of LGB on a lung index score, b combined alveolitis score, c combined fibrosis score, and d hydroxyproline (Hyp) content. Values are the mean ± SEM. Statistical significance for the difference between the data of the control group versus model group: *p < 0.05. Statistical significance for the difference between the data of untreated model group versus LGB-treated model groups: # p < 0.05
LGB Improves Histological Changes and Reduces Collagen Deposition in Pulmonary Tissues
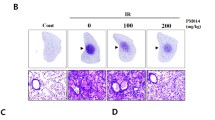
H&E staining of the lung sections indicated that treatment with LGB significantly improved irradiation-induced pathological changes, and the regional fibrotic foci, collagen depositions were greatly reduced after LGB treatment (Figure not shown). The alveolitis and fibrosis scores of LGB-treated animals were significantly lower (p < 0.05) than those of the untreated rats at 120 days post-irradiation. We also examined the degree to which LGB treatment decreased Hyp, which is the major constituent of collagen. Similarly, we found that the content of Hyp was significantly lower (p < 0.05) in LGB-treated animals than that of the untreated ones at 120 days post-irradiation (Fig. 1).
LGB Regulated the Serum Redox
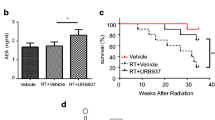
We then evaluated whether LGB treatment regulated the redox balance post-irradiation. Serum MDA content and SOD activity were measured to assess the oxidative and antioxidant status. The serum MDA concentration was significantly lower (p < 0.05) in LGB-treated animals than that of the untreated ones at 120 days post-irradiation exposure. Serum SOD activity was significantly higher (p < 0.05) in LGB-treated animals compared with that of the untreated ones (Fig. 2).
Effects of LGB on serum MDA content (a) and SOD activity (b). Values are the mean ± SEM. Statistical significance for the difference between the data of the control group versus model group: *p < 0.05. Statistical significance for the difference between the data of untreated model group versus LGB-treated model groups: # p < 0.05 (Color figure online)
LGB Modulated Cytokine Levels
We then evaluated whether LGB treatment regulated the disruptive expression of cytokines in serum following irradiation exposure. We found that the serum level of TGF-β1 was significantly lower (p < 0.05) in the LGB-treated rats compared with the untreated rats (Fig. 3). Similarly, the serum levels of IL-6 and TNF-α were significantly lower (p < 0.05) in the LGB-treated rats than the untreated rats at the end of 4 month (Fig. 3).
Effects of LGB on TGF-β1 (a), IL-6 (b), and TNF-α (c). Values are the mean ± SEM. Statistical significance for the difference between the data of the control group versus model group: *p < 0.05. Statistical significance for the difference between the data of untreated model group versus LGB-treated model groups: # p < 0.05 (Color figure online)
Discussion
Results of the present study have demonstrated that irradiation-induced pulmonary fibrosis in rats was significantly ameliorated by LGB treatment. LGB treatment reduced the mortality rate and lung index score, ameliorate lung histological damage, reduced collagen deposition, modulated the redox state of serum, and modulate the serum levels of TGF-β1, IL-6, and TNF-α. Given the current results, we suggested that LGB treatment significantly ameliorates irradiation-induced pulmonary fibrosis. Our data indicated that LGB has the potential for treating irradiation-induced pulmonary fibrosis.
Increasing evidence suggests that oxidative stress could lead to irradiation-induced pulmonary fibrosis [1, 8–12]. The ROS-induced activation of inflammatory cells can lead a positive feedback loop [1, 8, 13–23]. And elevated expression of large amount intracellular oxidative enzymes and large amounts of ROS and reactive nitrogen species are formed [1, 13]. As the balance between oxidant and antioxidant are destroyed, tissue damage then is getting more and more serious [1, 13]. It could be imagined that therapeutic intervention that defends against or ameliorate oxidant attack could be useful for irradiation-induced pulmonary fibrosis treatment [1, 13].
MDA serum levels and the SOD activity are crucial indicators of oxidative stress and the body’s respond to various oxidative stresses [1, 13]. MDA levels mainly reflect the degree of lipid peroxidation, and SOD plays an important role in balancing between oxidatant and antioxidant with capacities to neutralize free radical forms of oxygen and thus protects cells from oxidative attack [1, 13]. Our present results indicated that LGB had a potent anti-oxidative ability.
The development of irradiation-induced pulmonary fibrosis also associated with inflammatory cytokines that is of vital importance in forming a positive feedback loop to enhance the chemotoxis and oxidative stress [1, 24–28]. To investigate the effects of LGB treatment on inflammation status, we measured the serum levels of key inflammatory cytokines. The cytokines were significantly reduced in the LGB-treated rats compared with the untreated model rats. And the lower alveolitis score of the LGB-treated rats implied that LGB reduced the infiltration of inflammatory immune cells.
Overall, the present results of our research demonstrated that LGB treatment provided potent and enduring antioxidant and anti-inflammatory activities against irradiation-induced pulmonary fibrosis in experiment animals. The findings indicated the function might be mediated by suppressing the expression of pro-inflammatory factors and oxidative stress suppression.
References
You, H., Wei, L., Sun, W. L., et al. (2014). The green tea extract epigallocatechin-3-gallate inhibits irradiation-induced pulmonary fibrosis in adult rats. International Journal of Molecular Medicine, 34, 92–102.
Rhieu, B. H., Epperly, M. W., Cao, S., et al. (2014). Improved longevity of hematopoiesis in long-term bone marrow cultures and reduced irradiation-induced pulmonary fibrosis in Toll-like receptor-4 deletion recombinant-negative mice. In Vivo, 28, 441–448.
Wu, Z., Wang, X., Yang, R., et al. (2013). Effects of carbon ion beam irradiation on lung injury and pulmonary fibrosis in mice. Experimental and Therapeutic Medicine, 5, 771–776.
Kalash, R., Berhane, H., Goff, J., et al. (2013). Effects of thoracic irradiation on pulmonary endothelial compared to alveolar type-II cells in fibrosis-prone C57BL/6NTac mice. In Vivo, 27, 291–297.
Gao, F., Fish, B. L., Moulder, J. E., et al. (2013). Enalapril mitigates radiation-induced pneumonitis and pulmonary fibrosis if started 35 days after whole-thorax irradiation. Radiation Research, 180, 546–552.
Rhieu, B. H., Epperly, M. W., Cao, S., et al. (2014). Increased hematopoiesis in long-term bone marrow cultures and reduced irradiation-induced pulmonary fibrosis in von willebrand factor homologous deletion recombinant mice. In Vivo, 28, 449–456.
Zhan, H., Li, S., Sun, J., et al. (2014). Lettuce glycoside B ameliorates cerebral ischemia reperfusion injury by increasing nerve growth factor and neurotrophin-3 expression of cerebral cortex in rats. Indian Journal of Pharmacology, 46, 63–68.
Ali, E. N., & Mansour, S. Z. (2011). Boswellic acids extract attenuates pulmonary fibrosis induced by bleomycin and oxidative stress from gamma irradiation in rats. Chinese Medicine, 6, 36.
Wang, L., Feng, Y., Fu, X. L., et al. (2006). Effects of gene therapy with replication-defective adenovirus ericlosing Egr-1 promoter and Smad7 cDNA on irradiation-induced pulmonary fibrosis: experiment with mice. Zhonghua Yi Xue Za Zhi, 86, 2847–2852.
Epperly, M. W., Franicola, D., Zhang, X., et al. (2006). Reduced irradiation pulmonary fibrosis and stromal cell migration in Smad3-/- marrow chimeric mice. In Vivo, 20, 573–582.
Epperly, M. W., Guo, H., Shields, D., et al. (2004). Correlation of ionizing irradiation-induced late pulmonary fibrosis with long-term bone marrow culture fibroblast progenitor cell biology in mice homozygous deletion recombinant negative for endothelial cell adhesion molecules. In Vivo, 18, 1–14.
Epperly, M. W., Guo, H., Gretton, J. E., et al. (2003). Bone marrow origin of myofibroblasts in irradiation pulmonary fibrosis. American Journal of Respiratory Cell and Molecular Biology, 29, 213–224.
Cheresh, P., Kim, S. J., Tulasiram, S., et al. (2013). Oxidative stress and pulmonary fibrosis. Biochimica et Biophysica Acta, 1832, 1028–1040.
Brass, D. M., Spencer, J. C., Li, Z., et al. (2012). Innate immune activation by inhaled lipopolysaccharide, independent of oxidative stress, exacerbates silica-induced pulmonary fibrosis in mice. PloS One, 7, e40789.
Inghilleri, S., Morbini, P., Campo, I., et al. (2011). Erratum to “factors influencing oxidative imbalance in pulmonary fibrosis: an immunohistochemical study”. Pulmonary Medicine, 2011, 515608.
Inghilleri, S., Morbini, P., Campo, I., et al. (2011). Factors influencing oxidative imbalance in pulmonary fibrosis: an immunohistochemical study. Pulmonary Medicine, 2011, 421409.
Cui, Y., Robertson, J., Maharaj, S., et al. (2011). Oxidative stress contributes to the induction and persistence of TGF-beta1 induced pulmonary fibrosis. International Journal of Biochemistry & Cell Biology, 43, 1122–1133.
Mazur, W., Lindholm, P., Vuorinen, K., et al. (2010). Cell-specific elevation of NRF2 and sulfiredoxin-1 as markers of oxidative stress in the lungs of idiopathic pulmonary fibrosis and non-specific interstitial pneumonia. APMIS, 118, 703–712.
Kliment, C. R., & Oury, T. D. (2010). Oxidative stress, extracellular matrix targets, and idiopathic pulmonary fibrosis. Free Radical Biology and Medicine, 49, 707–717.
Kliment, C. R., Englert, J. M., Gochuico, B. R., et al. (2009). Oxidative stress alters syndecan-1 distribution in lungs with pulmonary fibrosis. Journal of Biological Chemistry, 284, 3537–3545.
Vuorinen, K., Ohlmeier, S., Lepparanta, O., et al. (2008). Peroxiredoxin II expression and its association with oxidative stress and cell proliferation in human idiopathic pulmonary fibrosis. Journal of Histochemistry and Cytochemistry, 56, 951–959.
Helal, G. K., & Helal, O. K. (2009). Metallothionein attenuates carmustine-induced oxidative stress and protects against pulmonary fibrosis in rats. Archives of Toxicology, 83, 87–94.
Walters, D. M., Cho, H. Y., & Kleeberger, S. R. (2008). Oxidative stress and antioxidants in the pathogenesis of pulmonary fibrosis: a potential role for Nrf2. Antioxidants & Redox Signaling, 10, 321–332.
Xie, H., Wang, R., Tang, X., et al. (2012). Paraquat-induced pulmonary fibrosis starts at an early stage of inflammation in rats. Immunotherapy, 4, 1809–1815.
Zhao, Y., Cui, A., Wang, F., et al. (2012). Characteristics of pulmonary inflammation in combined pulmonary fibrosis and emphysema. Chinese Medical Journal, 125, 3015–3021.
Bui, S., Boisserie-Lacroix, V., Ceccato, F., et al. (2012). Pulmonary inflammation in cystic fibrosis. Archives de Pediatrie, 19(Suppl 1), S8–12.
Becker, K. A., Henry, B., Ziobro, R., et al. (2012). Role of CD95 in pulmonary inflammation and infection in cystic fibrosis. Journal Of Molecular Medicine, 90, 1011–1023.
Yang, H. Z., Wang, J. P., Mi, S., et al. (2012). TLR4 activity is required in the resolution of pulmonary inflammation and fibrosis after acute and chronic lung injury. American Journal of Pathology, 180, 275–292.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhou, Y., Gao, Y., Chen, Y. et al. Effects of Lettuce Glycoside B in Ameliorating Pulmonary Fibrosis Induced by Irradiation Exposure and its Anti-Oxidative Stress Mechanism. Cell Biochem Biophys 71, 971–976 (2015). https://doi.org/10.1007/s12013-014-0295-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-014-0295-8