Abstract
Chronic neuropathic pain can significantly reduce quality of life and place an economic burden on individuals and society. Spinal cord stimulation (SCS) is an alternative approach to the treatment of neuropathic pain when standard pharmacological agents have failed. However, an improved understanding of the mechanisms by which SCS inhibits pain is needed to enhance its clinical utility. This review summarizes important findings from recent studies of SCS in animal models of neuropathic pain, highlights current understanding of the spinal neurophysiological and neurochemical mechanisms by which SCS produces an analgesic effect, and discusses the potential clinical applicability of these findings and future directions for research.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pharmacological therapy for neuropathic pain remains inadequate, with most drugs being effective in less than 50 % of patients [1]. An alternative treatment strategy, spinal cord stimulation (SCS), has been clinically proven to be effective for treating a variety of chronic pain conditions that are refractory to current pharmacotherapies [2, 3]. It is especially useful for neurogenic pain. Clinically, SCS is achieved by an electrode that is placed in the epidural space over the dorsal column structure a few levels above the affected spinal segments. Mild to moderate electrical pulses at various frequencies (eg, 50–60 Hz) are delivered to the spinal cord to elicit paresthesia in the painful region. Although the clinical benefit of SCS is substantial, detailed knowledge of how SCS inhibits pain is lacking. A better understanding of its precise mechanisms of action may help physicians better select appropriate patients and optimize stimulation parameters to improve SCS efficacy and achieve long-term pain relief.
Nociceptive afferent neurons of the dorsal root ganglia and trigeminal ganglia transmit noxious information to the spinal cord, principally to superficial (I/II) and deep (V) laminae [4]. Nociceptive information can be integrated and modified at the terminals of primary afferent fibers and at the synaptic junctions of projection neurons in the dorsal horn before their dispatch to higher supraspinal centers (Fig. 1). Thus, the dorsal horn serves as both a relay station for ascending pain signaling and an important site for integration and modulation of pain. Importantly, spinal neuronal circuits show dynamic change in response to differential environmental cues. Nerve injury and intense erratic noxious inputs induce a dysfunction of spinal segmental pain inhibition and a prolonged state of dorsal horn neuronal hyperexcitability, which amplifies ascending pain signaling and results in unremitting pain [5–7]. Increasing evidence suggests that SCS-induced analgesia is intricately linked with spinal segmental mechanisms. From a mechanistic point of view, studies of SCS in experimental pain conditions may correlate with clinical SCS analgesia better than studies performed in uninjured animals [8]. This review summarizes major findings from recent experimental work, updates current understanding of the spinal physiological and neurochemical basis for SCS analgesia, and discusses future directions for improving the use of SCS in pain management.
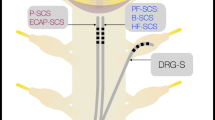
Schematic diagram illustrating potential spinal segmental mechanisms underlying spinal cord stimulation (SCS)-induced pain inhibition. The intensities of dorsal column and dorsal roots stimulations can be calibrated by recording the antidromic compound action potentials at the sciatic nerve. SCS-induced inhibition can be examined by means of in vivo extracellular recording of dorsal horn neuronal activity. Antidromic (eg, dorsal column stimulation) or orthodromic (eg, peripheral nerve stimulation or dorsal root stimulation) activation of Aα/β-afferents may activate spinal inhibitory interneurons (I) via collateral branches. The inhibitory interneurons include GABAergic neurons located in superficial laminae dorsal horn. Roles of glycinergic inhibitory interneuron in SCS analgesia remain unclear. Activity of inhibitory interneurons attenuates ascending pain signaling by inhibiting (Ө, black) local excitatory interneurons (E) and transmission cells (T) that mediate nociceptive inputs in the same segment. Transmission cells are most likely to be wide-dynamic-range (WDR) neurons that receive both A- and C- afferent inputs. It is unclear if the inhibitory interneuron directly attenuates activity of nociceptive-specific projection neurons (N) in the superficial dorsal horn. In addition to γ-aminobutyric acid (GABA), spinal neurotransmitters that contribute to intrinsic inhibition by SCS also include acetylcholine. SCS may evoke releasing of serotonin and norepinephrine into dorsal horn from descending fibers (indicated by dashed line) originating in supraspinal pain modulatory structures, which in turn decrease pain transmission through pre- and postsynaptic inhibitory mechanisms (Ө, black)
Spinal Neurophysiological Mechanisms
Lesion studies have shown that a large portion of the analgesic effect produced by SCS is mediated through the dorsal column. Therefore, the primary goal of SCS is to activate the dorsal column, which contains axons that originate in the large-diameter afferent sensory neurons (eg, Aβ afferent fiber). According to the gate-control theory, some of these sensory neurons send collateral branches to the affected spinal segments, where C-fiber inputs from the peripheral painful area and activity of nociceptive projection neurons are inhibited. As the fundamental biological basis for SCS-induced analgesia, the gate-control theory postulates that activity in large-diameter Aβ afferent fibers attenuates spinal ascending pain transmission by activating inhibitory interneurons in the dorsal horn of the spinal cord [9, 10]. However, the precise location and identity of these “gate-keepers” were not very clear until recently. Using homozygotic transgenic mice that express enhanced green fluorescent protein under control of the gad1 gene promoter to identify glutamic acid decarboxylase 67–expressing neurons, Daniele et al. [11•] provide complementary morphological and functional evidence that a significant group of inhibitory interneurons expressing γ-aminobutyric acid (GABA) in laminae II dorsal horn can be activated by convergent Aβ-fiber inputs. These GABAergic neurons represent important inhibitory gates in dorsal horn (Fig. 1). They may not only suppress nociceptive inputs mediated by thinly myelinated Aδ- or unmyelinated C- fibers, but may also attenuate low-threshold activation of nociceptive projection neurons that may occur after nerve injury due to the loss of tonic inhibition [6, 12]. Accordingly, SCS should attenuate pathological pain (eg, allodynia and hyperalgesia) as well as nociceptive pain. This prediction was supported by clinical findings that SCS inhibited the nociceptive withdrawal flexion reflexes and attenuated C-fiber–mediated heat response in humans [13, 14]. Similarly, our recent electrophysiological study showed that stimulation of dorsal column, the primary target of SCS, inhibited the C-fiber–mediated response of dorsal horn wide-dynamic-range (WDR) neurons in both nerve-injured and sham-operated rats [15••].
Transcutaneous spinal cord direct current stimulation at an intensity below the sensory threshold also has been shown to inhibit spinal pain transmission and the lower limb nociceptive flexion reflex in healthy human patients [16]. The nociceptive flexion reflex may have a linear relationship with subjective pain intensity/threshold and is mediated by a complex neuronal network in the spinal cord, including WDR neurons. Regardless, SCS preferentially attenuates exaggerated pain sensitivity under pathological conditions [17], and dorsal column stimulation does not inhibit the C-fiber component of the flexor reflex in rats [18]. The reason for these conflicting results remains unclear, but it may be partially due to use of different stimulation parameters (eg, intensity). According to the gate-control theory, activation of more Aβ-fibers may lead to stronger pain suppression than stimulation at the lower intensities. SCS often has been tested at an intensity slightly below the motor threshold, which is considered to be the tolerance threshold in animal behavioral studies [2, 19•]. Motor threshold represents a reflex response to stimulation of dorsal column fibers [20], but it was previously unclear how motor threshold correlates with Aα/β-fiber activation. By examining the antidromic compound action potential that results from graded stimulation applied through the SCS lead, we found that SCS at the motor threshold may activate only a small fraction of the afferent Aβ-fiber population in nerve-injured rats [21]. These findings support the predictions from a computer model for SCS [22, 23]. In addition, the size of the compound action potential waveform was larger in animals that responded to SCS analgesia than in animals that did not, indicating a more efficient activation of the dorsal column structure in responders [21].
In addition to nociceptive projection neurons in the superficial dorsal horn, WDR neurons located in the deeper lamina are also important to pain processing and are candidates for the “transmission” cells in the gate-control theory [24–26]. WDR neurons are readily sensitized by intense noxious inputs and develop hyperexcitability after nerve injury. Stimulating the dorsal column at clinical SCS parameters was shown to suppress the enhanced responsiveness of WDR cells in neuropathic rats [15••, 27]. Our in vivo electrophysiology study revealed some important features of dorsal column stimulation–induced neuronal inhibition that mimic features of SCS analgesia [15••]. For example, ongoing pain and tactile allodynia are two characteristic features of neuropathic pain that are often attenuated by SCS [3, 28–30]. Similarly, dorsal column stimulation inhibited spontaneous discharges, which may contribute to ongoing pain [31, 32], and attenuated the evoked mechanical responses of WDR neurons in nerve-injured rats [15••]. During SCS in patients, an antidromic sciatic compound action potential can be recorded in lower limbs [33]. Therefore, we used the antidromic sciatic compound action potential in our animal studies to ensure that the intensity of stimulation did not activate Aδ-fibers (Fig. 1), which would produce painful paresthesia in humans. The SCS-induced neuronal inhibition is reversible and repeatable, and hence, may provide a biological basis for designing closed-loop biofeedback systems that communicate and record neural responses after SCS.
Although the gate-control theory is fundamental to our understanding of SCS-induced pain inhibition, details of spinal neuronal circuitries involved in gate control and other potential segmental mechanisms involved in SCS analgesia warrant further study. Dorsal horn neurons can be inhibited through both GABAergic and glycinergic mechanisms. However, the role of glycinergic interneurons in SCS analgesia is unclear. It is also intriguing that most superficial inhibitory interneurons not only receive excitatory Aβ-fiber inputs, but also receive excitatory drive from high-threshold Aδ- and C-fibers [12, 34], a fact that contradicts the predictions of gate-control theory (eg, high-threshold inputs inhibit the activity of inhibitory interneurons). Thus, it remains to be examined whether the effects of SCS on different dysfunctional sensory modalities (eg, heat, cold, and mechanical hypersensitivities) and under different pathological pain conditions (eg, inflammatory and neuropathic pain) stem from distinct mechanistic pathways. In addition to activating the gating mechanism, synchronized antidromic dorsal column volley may directly induce inhibitory postsynaptic potentials in dorsal horn neurons [35] and facilitate primary afferent depolarization, which elicits presynaptic inhibition of incoming afferent inputs [36]. SCS-induced peripheral vasodilation was shown to require multisegmental spinal integration [37]. It is unclear if synaptic integration from adjacent spinal segments is also required for SCS analgesia.
Spinal Neurochemical Mechanisms
GABA
The synchronous A-fiber inputs may induce dynamic segmental neurochemical changes. In particular, the GABAergic inhibitory interneurons in superficial laminae dorsal horn can be activated by convergent Aβ-fiber inputs and release GABA [11•, 38], an important inhibitory neurotransmitter in the gate-control mechanism (Fig. 1). In neuropathic pain models, SCS increased spinal GABA release in animals that responded well to SCS analgesia and caused an associated decrease in release of glutamate and aspartate [28, 39, 40]. The inhibition of animal pain behavior and WDR neuronal hyperexcitability was closely associated with the time course of elevated GABA levels in the dorsal horn after SCS. The investigators suggested that GABAb receptor may play a more important role than GABAa receptor in mediating the inhibitory effect [40, 41]. In line with these findings, intrathecal administration of subeffective doses of baclofen enhanced SCS analgesia in both animal models and patients [42–44]. Interestingly, the duration of time that extracellular GABA level remained elevated significantly exceeded the duration of SCS [40]. This finding may indicate a dysfunctional GABAergic reuptake mechanism after nerve injury. Intracellular GABA content of dorsal horn neurons decreased during the early phase of neuropathic pain but increased in the later phase [45]. Thus, the involvement of the GABAergic mechanism in SCS analgesia may change during the progress of neuropathic pain. In addition to intrinsic dorsal horn neurons, other sources and mechanisms involved in the release of GABA by SCS under neuropathic pain conditions warrant further study.
Serotonin (5-HT)
A host of data suggests that SCS analgesia also involves modulation of other neurotransmitter systems in spinal cord [28, 40, 46, 47]. Linderoth et al. [48] showed that SCS induced serotonin release in the spinal dorsal horn of cats. They further demonstrated that the increase in endogenous serotonin content after SCS may involve local GABAergic circuitry [19•]. Nerve injury changes the expression and function of various serotonin receptor subtypes (5-HT 1–7) that exert diverse effects on spinal pain processing [49–51]. Recently, Song et al. [52••] enhanced our understanding of the respective roles of different spinal 5-HT receptors in SCS analgesia under neuropathic pain conditions. They suggested that activation of 5-HT2A, 5-HT3, and 5-HT4 receptors in the dorsal horn may contribute to the SCS-induced decreases in neuronal excitability and spinal pain transmission. Intriguingly, the 5-HT3 receptor is known as a nonselective cationic channel that mediates fast excitatory responses and plays a role in pain facilitation [53–55]. It is rather surprising that activation of the 5-HT3 receptor also contributes to SCS analgesia, but it is possible that nerve injury changes 5-HT3 activity or that SCS analgesia is partially mediated through activation of spinal GABAergic interneurons that express 5-HT3 receptors [52••]. In addition to activating 5-HT receptors, increased release of serotonin also may increase the expression and synthesis of dynorphin, enkephalin, and GABA within the spinal cord [56], providing a mechanism for the delayed and prolonged analgesic action of SCS.
Muscarinic and Adrenergic Mechanisms
Cholinergic and adrenergic neurotransmissions are two other important mechanisms of SCS analgesia. In vivo microdialysis studies suggested that SCS induces release of both acetylcholine and noradrenaline in the spinal cord [46, 57, 58]. Similar to GABA, dorsal horn acetylcholine content was significantly elevated only in neuropathic rats that responded to SCS analgesia, whereas the release was unaffected in the nonresponsive animals [46, 58]. Importantly, SCS-induced pain inhibition was completely blocked by intrathecally administered atropine and a muscarinic M4 receptor antagonist and partially attenuated by M1 and M2 antagonists. Thus, the inhibition of neuropathic mechanical hypersensitivity by SCS is associated at least partially with an increased release of acetylcholine that activates spinal muscarinic receptors [46]. In line with this finding, transcutaneous electric nerve stimulation (TENS), another therapeutic modality based on the gate-control theory, also activates spinal cholinergic mechanisms to achieve pain inhibition [59]. Interestingly, the activation of cholinergic interneurons, which in turn release acetylcholine in the spinal dorsal horn, may also partially contribute to the enhancement of SCS analgesia by intrathecal clonidine in nerve-injured rats [60]. Because muscarinic receptors and α1 adrenoceptors are also located on GABAergic interneurons in the dorsal horn [61, 62], acetylcholine and noradrenaline may excite spinal GABAergic interneurons by binding to the respective receptors to produce analgesia after SCS [58, 63]. Thus, SCS may initiate a feed-forward activation of various spinal segmental inhibitory mechanisms, though some may be compromised by nerve injury [6, 7, 64]. Studies by Linderoth and coworkers [42, 44, 65] not only added to our understanding of the neurochemical basis for SCS analgesia, but also provided important rationales for developing a mechanism-based treatment strategy for improving SCS analgesia. For example, intrathecal administration of a subeffective dose of baclofen or a muscarinic receptor agonist transformed nerve-injured rats that had not responded to SCS into responders. A combination of SCS and intrathecal amitriptyline (a tricyclic antidepressant) or fluoxetine (a selective serotonin/noradrenaline reuptake inhibitor) also enhanced SCS-induced inhibition of mechanical hypersensitivity in nerve-injured rats [66].
Influence of Stimulation Parameters
The frequency of electrical stimulation significantly affects neurotransmitter release and neural modulation. The most effective parameters for SCS have not been systematically investigated, and there is no consensus regarding whether the most commonly used frequency (50–60 Hz) is optimal for relief of neuropathic pain. SCS at 300 Hz was shown to restore locomotion in animal models of Parkinson’s disease [67]. An even higher frequency, 500 Hz, was shown to improve peripheral blood flow more effectively than lower-frequency SCS by activating transient receptor potential vanilloid type 1 (TRPV1)-containing fibers and causing release of calcitonin gene–related peptide (CGRP) [68]. In contrast, Maeda et al. [29••] reported that lower frequencies of SCS (4 Hz and 60 Hz) inhibited mechanical hypersensitivity in neuropathic rats to a greater degree than did higher frequencies (100 Hz and 250 Hz). Using c-fos staining as a marker of neuronal activation, their subsequent study suggested that SCS at the lower frequencies activated both supraspinal and spinal mechanisms, whereas the higher frequency (100 Hz) mainly activated spinal mechanisms [69]. Ultra high–frequency SCS (kHz range) was applied at the cervical level to reduce torticollis spasmodicus [70], but it is unclear such high frequencies provide better pain relief than conventional SCS or achieve adequate pain relief without producing uncomfortable paresthesia. SCS analgesia may involve distinct mechanisms of action at different stimulation frequencies. Thus, it will be meaningful to identify the SCS frequencies that optimally modulate the release of different neurotransmitters under neuropathic pain conditions. Because serotonin-containing terminals and GABAergic, enkephalinergic, and dynorphinergic neurons have similar distributions in the dorsal horn, future studies may also examine whether different neurotransmitter systems interact synergistically during SCS analgesia.
Spinal Neuronal Plasticity and the Prolongation of SCS Analgesia
In experimental animals, the duration of neuronal inhibition and pain relief by SCS often exceeds the stimulation period [15••, 29••]. These findings are consistent with clinical observations that analgesia not only occurs during the SCS, but also often outlasts the period of SCS [3, 71]. The extended pain relief suggests that SCS analgesia may have two components: an immediate action and a carryover effect. Importantly, some patients may obtain prolonged pain inhibition after several SCS sessions [17, 71]. Although the classical interpretation of gate-control mechanism and the release of inhibitory neurotransmitters may explain the immediate and short-term action of SCS, they do not readily explain the prolonged pain inhibition. Rather, repetitive SCS may lead to prolonged pain inhibition through a progressive resolution of the underlying pathophysiologic mechanism of neuropathic pain, in particular, the reversal of central sensitization.
Our recent study suggested that when parameters were modeled after those of clinical SCS, stimulation of the dorsal column not only inhibited the established WDR neuronal hyperexcitability in neuropathic rats, but also blocked wind-up [15••]. The wind-up of WDR neuronal response to repetitive noxious inputs reflects a short-term increase in spinal neuronal excitability and is a potential forerunner of the longer-lasting central sensitization [15••, 72]. Importantly, SCS also normalized the long-term potentiation in WDR neurons [73], a phenomenon that may share mechanisms with hyperalgesia [74, 75]. These findings suggest that synchronized Aα/β-fiber firing is capable of blocking, as well as reversing, spinal neuronal sensitization induced by intense noxious inputs. In particular, prevention of wind-up development suggests that early intervention of the neuronal sensitization process with SCS may benefit pain treatment. In support of this notion, a recent animal study showed that when SCS was applied early after nerve injury (1 day), more rats exhibited a reduction in mechanical allodynia and the reduction persisted longer than when SCS was given at a later time point (16 days) [76]. Therefore, the innate plasticity of spinal pain processing neurons is preserved after nerve injury. From this perspective, the development of central sensitization and its reversal by SCS may be two directions of the same plastic pathway. This notion may have important implications for clinical use of SCS. For example, psychophysiological studies may help to identify responders and predict the long-term outcome of SCS analgesia by examining whether trial SCS can inhibit the temporal summation of pain (eg, wind-up) in patients. If SCS antagonizes the development of central sensitization, applying SCS during surgical procedures, soon after injury, or at the early stage of neuropathic pain may help to prevent the later development of pain hypersensitivity or limit its severity and duration. Repetitive treatments and combining SCS with pharmacotherapy, such as an N-methyl-D-aspartate (NMDA) receptor blocker, may help to terminate the process of central sensitization. A recent finding by Truin et al. [77] supports this possibility. The investigators observed that intrathecal administration of a subeffective dose of ketamine, an NMDA antagonist, converted neuropathic rats from SCS nonresponders to SCS responders. It also prolonged the pain relief in SCS responders. Additional work is required to fully understand the spinal mechanisms and cellular circuits that underlie the carryover effect of SCS and are not explained by gate-control theory.
Understanding the SCS-induced intracellular events (eg, receptor trafficking, signaling cascade, and transcriptional modulation) that occur within dorsal horn neurons is still in its infancy. Information is limited in regard to whether the reversal of central sensitization and the build-up of long-lasting pain relief after SCS may involve transcriptional and post-translational changes. Intriguingly, studies of SCS-induced vasodilation have suggested that SCS may activate extracellular signal–regulated kinase (ERK) and protein kinase B (AKT) pathways [78, 79]. Recently, two separate studies showed that SCS activated the immediate early gene c-fos, mostly in the superficial dorsal horn, in nerve-injured rats [69, 80]. It is known that c-fos activation produces a signal transduction cascade that could lead to long-term changes in cell properties and excitability via actions such as gene expression regulation. Although ERK and c-fos activation may be induced by various types of stimuli, their expression is not normally elicited by light touch. However, ERK and c-fos can be induced by repetitive light touch in animals after nerve injury. They contribute to the neuronal sensitization process after nerve injury and are often markers of neuronal excitation to noxious stimuli [81, 82]. Therefore, the physiological implications of ERK and c-fos activation in SCS analgesia remain to be clarified. If ERK and c-fos are expressed in GABAergic or glycinergic interneurons, it would suggest a prolonged modulation of GABAergic inhibition. The expression of multiple genes may be regulated by c-fos. If de novo protein synthesis does play a role in sustaining the long-term beneficial effect of SCS, some interesting questions can be raised. Of particular interest would be the identification of specific downstream signaling events and specific proteins that are synthesized after c-fos activation in response to SCS. In addition, how these molecular changes are involved in inverting the process of central sensitization and in the proposed mechanism of SCS-induced analgesia under neuropathic pain conditions should be examined.
Supraspinal Mechanisms for SCS Analgesia
Because this review focuses on experimental evidence pertaining to the spinal mechanisms of SCS in the treatment of neuropathic pain, the supraspinal biological basis, which is also important for SCS analgesia, is only briefly discussed here. Over two decades ago, Rees and Roberts [83] suggested that the long-lasting inhibition of dorsal horn neurons by dorsal column stimulation involves activation of the anterior pretectal nucleus; its output in turn activates the descending pain inhibitory pathway. Importantly, the activation of neurons in the anterior pretectal nucleus outlasts the period of stimulation by an amount proportional to the duration of pain relief, suggesting that a remote nervous system action also may contribute to the long-lasting carryover effect of SCS. A comprehensive set of studies conducted by the Saade group [13, 84, 85] also demonstrated activation of a spinal-brainstem-spinal loop by SCS. Thus, SCS may induce ascending inhibition relayed by thalamocortical systems (eg, inhibits cortical pain processing), as well as trigger the descending pain inhibition mediated by the brainstem system [84, 86, 87]. Descending modulatory pathways are important to the development and maintenance of neuropathic pain [88]. The plastic changes occur at supraspinal pain-processing structures after nerve injury and enhance descending pain facilitation [88–91]. Future studies may examine which supraspinal structures and pathways are essential to SCS analgesia under neuropathic pain condition and whether SCS reduces descending pain facilitation and/or restores descending pain inhibition.
Recently, Linderoth and colleagues [19•, 44, 52••] suggested that an important component of SCS analgesia may be activation of both the descending serotonergic and noradrenergic systems (Fig. 1). Intriguingly, SCS induces an increase in c-fos expression in brainstem pain modulatory circuitry [69]. Thus, it is important to examine if the carryover effect of SCS involves long-term plastic changes and remodeling in supraspinal structures and if activation of supraspinal pain modulatory systems work in concert with spinal segmental mechanisms (eg, a site-to-site synergy) to inhibit neuropathic pain. Chronic neuropathic pain has been linked with a host of negative emotional, psychological, and cognitive outcomes [92–94]. Therefore, the treatment also should be multidimensional. Because SCS exerts a profound effect on neuronal activity across various levels of the neuronal axis, it would be important to examine if SCS alleviate both the sensory descriptive component (eg, intensity, modality) and the affective component of pathological pain [84, 87, 95]. To date, these issues have received little attention. Future studies may identify the important supraspinal mechanisms that contribute to the immediate analgesic action, the carryover effect, and the alleviation of negative emotional component of chronic pain from SCS.
Conclusions
Here, we review recent studies of spinal neurophysiological and neurochemical mechanisms of SCS-induced analgesia (Fig. 1). These studies help assemble a coherent picture of the behavioral, cellular, and molecular processes that allow SCS to moderate neuropathic pain in future. The lack of systemic side effects or potential for addiction, the general satisfactory treatment efficacy, and the potential of achieving prolonged pain relief in some patients represent important rationales for raising SCS in the continuum of pain treatment options. Future mechanistic studies of SCS will help to improve and broaden the use of SCS as a treatment option for many patients in pain.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Baron R. Mechanisms of disease: neuropathic pain–a clinical perspective. Nat Clin Pract Neurol. 2006;2:95–106.
Meyerson BA, Linderoth B. Mode of action of spinal cord stimulation in neuropathic pain. J Pain Symptom Manage. 2006;31:S6–12.
Kumar K, Taylor RS, Jacques L, Eldabe S, Meglio M, Molet J, Thomson S, O’Callaghan J, Eisenberg E, Milbouw G, Buchser E, Fortini G, Richardson J, North RB. Spinal cord stimulation versus conventional medical management for neuropathic pain: a multicentre randomised controlled trial in patients with failed back surgery syndrome. Pain. 2007;132:179–88.
Cavanaugh DJ, Lee H, Lo L, Shields SD, Zylka MJ, Basbaum AI, Anderson DJ. Distinct subsets of unmyelinated primary sensory fibers mediate behavioral responses to noxious thermal and mechanical stimuli. Proc Natl Acad Sci U S A. 2009;106:9075–80.
Yan LH, Hou JF, Liu MG, Li MM, Cui XY, Lu ZM, Zhang FK, An YY, Shi L, Chen J. Imbalance between excitatory and inhibitory amino acids at spinal level is associated with maintenance of persistent pain-related behaviors. Pharmacol Res. 2009;59:290–9.
Torsney C, MacDermott AB. Disinhibition opens the gate to pathological pain signaling in superficial neurokinin 1 receptor-expressing neurons in rat spinal cord. J Neurosci. 2006;26:1833–43.
Moore KA, Kohno T, Karchewski LA, Scholz J, Baba H, Woolf CJ. Partial peripheral nerve injury promotes a selective loss of GABAergic inhibition in the superficial dorsal horn of the spinal cord. J Neurosci. 2002;22:6724–31.
Linderoth B, Meyerson BA. Spinal cord stimulation: exploration of the physiological basis of a widely used therapy. Anesthesiology. 2010;113:1265–7.
Melzack R, Wall PD. Pain mechanisms: a new theory. Science. 1965;150:971–9.
Costigan M, Woolf CJ. No DREAM, No pain. Closing the spinal gate. Cell. 2002;108:297–300.
• Daniele CA, MacDermott AB: Low-threshold primary afferent drive onto GABAergic interneurons in the superficial dorsal horn of the mouse. J.Neurosci. 2009, 29:686–695. This article provides complementary morphological and functional evidence that GABAergic inhibitory interneurons in superficial dorsal horn can be activated by convergent Aβ-fiber inputs, thus an important pain inhibitory mechanism supporting the gate-control theory.
Takazawa T, MacDermott AB. Synaptic pathways and inhibitory gates in the spinal cord dorsal horn. Ann N Y Acad Sci. 2010;1198:153–8.
Saade N, Atweh AF, Tabet MS, Jabbur SJ. Inhibition of nociceptive withdrawal flexion reflexes through a dorsal column-brainstem-spinal loop. Brain Res. 1985;335:306–8.
Marchand S, Bushnell MC, Molina-Negro P, Martinez SN, Duncan GH. The effects of dorsal column stimulation on measures of clinical and experimental pain in man. Pain. 1991;45:249–57.
•• Guan Y, Wacnik PW, Yang F, Carteret AF, Chung CY, Meyer RA, Raja SN: Spinal cord stimulation-induced analgesia: electrical stimulation of dorsal column and dorsal roots attenuates dorsal horn neuronal excitability in neuropathic rats. Anesthesiology 2010, 113:1392–1405. This electrophysiological study demonstrates that SCS attenuates dorsal horn neuronal excitability in nerve-injured rats. It provides an important cellular mechanism underlying SCS analgesia and an in vivo model allows the neurophysiologic basis for the actions of SCS to be studied.
Cogiamanian F, Vergari M, Schiaffi E, Marceglia S, Ardolino G, Barbieri S, Priori A. Transcutaneous spinal cord direct current stimulation inhibits the lower limb nociceptive flexion reflex in human beings. Pain. 2011;152:370–5.
Gybels J, Kupers R. Central and peripheral electrical stimulation of the nervous system in the treatment of chronic pain. Acta Neurochir Suppl (Wien). 1987;38:64–75.
Meyerson BA, Ren B, Herregodts P, Linderoth B. Spinal cord stimulation in animal models of mononeuropathy: effects on the withdrawal response and the flexor reflex. Pain. 1995;61:229–43.
• Song Z, Ultenius C, Meyerson BA, Linderoth B: Pain relief by spinal cord stimulation involves serotonergic mechanisms: an experimental study in a rat model of mononeuropathy. Pain 2009, 147:241–248. This study provides important evidence that spinal 5-HT system contributes to SCS analgesia, and that activation of descending serotonergic pathways by SCS may attenuate spinal pain transmission by activation of local GABAergic circuitry.
Gerasimenko YP, Lavrov IA, Courtine G, Ichiyama RM, Dy CJ, Zhong H, Roy RR, Edgerton VR. Spinal cord reflexes induced by epidural spinal cord stimulation in normal awake rats. J Neurosci Methods. 2006;157:253–63.
Yang F, Carteret AF, Wacnik PW, Chung CY, Xing L, Dong X, Meyer RA, Raja SN, Guan Y: Bipolar spinal cord stimulation attenuates mechanical hypersensitivity at an intensity that activates a small portion of A-fiber afferents in spinal nerve-injured rats. Neuroscience 2011.
Feirabend HK, Choufoer H, Ploeger S, Holsheimer J, van Gool JD. Morphometry of human superficial dorsal and dorsolateral column fibres: significance to spinal cord stimulation. Brain. 2002;125:1137–49.
Holsheimer J. Computer modelling of spinal cord stimulation and its contribution to therapeutic efficacy. Spinal Cord. 1998;36:531–40.
Woolf CJ. Central sensitization: uncovering the relation between pain and plasticity. Anesthesiology. 2007;106:864–7.
Latremoliere A, Woolf CJ. Central sensitization: a generator of pain hypersensitivity by central neural plasticity. J Pain. 2009;10:895–926.
Guan Y, Borzan J, Meyer RA, Raja SN. Windup in dorsal horn neurons is modulated by endogenous spinal mu-opioid mechanisms. J Neurosci. 2006;26:4298–307.
Yakhnitsa V, Linderoth B, Meyerson BA. Spinal cord stimulation attenuates dorsal horn neuronal hyperexcitability in a rat model of mononeuropathy. Pain. 1999;79:223–33.
Stiller CO, Cui JG, O’Connor WT, Brodin E, Meyerson BA, Linderoth B. Release of gamma-aminobutyric acid in the dorsal horn and suppression of tactile allodynia by spinal cord stimulation in mononeuropathic rats. Neurosurgery. 1996;39:367–74.
•• Maeda Y, Wacnik PW, Sluka KA: Low frequencies, but not high frequencies of bi-polar spinal cord stimulation reduce cutaneous and muscle hyperalgesia induced by nerve injury. Pain 2008, 138:143–152. This animal behavioral study uses a miniature quadripolar electrode to mimic the actions of SCS in clinical situations. It demonstrates that stimulation frequency is important to the effectiveness of SCS and that repeated SCS results in a cumulative pain relief in nerve-injured rats.
Smits H, Ultenius C, Deumens R, Koopmans GC, Honig WM, van Kleef M, Linderoth B, Joosten EA. Effect of spinal cord stimulation in an animal model of neuropathic pain relates to degree of tactile “allodynia”. Neuroscience. 2006;143:541–6.
Campbell JN, Meyer RA. Mechanisms of neuropathic pain. Neuron. 2006;52:77–92.
Djouhri L, Koutsikou S, Fang X, McMullan S, Lawson SN. Spontaneous pain, both neuropathic and inflammatory, is related to frequency of spontaneous firing in intact C-fiber nociceptors. J Neurosci. 2006;26:1281–92.
Buonocore M, Bonezzi C, Barolat G. Neurophysiological evidence of antidromic activation of large myelinated fibres in lower limbs during spinal cord stimulation. Spine. 2008;33:E90–3. Phila Pa 1976.
Takazawa T, MacDermott AB. Glycinergic and GABAergic tonic inhibition fine tune inhibitory control in regionally distinct subpopulations of dorsal horn neurons. J Physiol. 2010;588:2571–87.
Narikawa K, Furue H, Kumamoto E, Yoshimura M. In vivo patch-clamp analysis of IPSCs evoked in rat substantia gelatinosa neurons by cutaneous mechanical stimulation. J Neurophysiol. 2000;84:2171–4.
Shimoji K, Shimizu H, Maruyama Y, Matsuki M, Kuribayashi H, Fujioka H. Dorsal column stimulation in man: facilitation of primary afferent depolarization. Anesth Analg. 1982;61:410–3.
Barron KW, Croom JE, Ray CA, Chandler MJ, Foreman RD. Spinal integration of antidromic mediated cutaneous vasodilation during dorsal spinal cord stimulation in the rat. Neurosci Lett. 1999;260:173–6.
Schoffnegger D, Heinke B, Sommer C, Sandkuhler J. Physiological properties of spinal lamina II GABAergic neurons in mice following peripheral nerve injury. J Physiol. 2006;577:869–78.
Baba H, Yoshimura M, Nishi S, Shimoji K. Synaptic responses of substantia gelatinosa neurones to dorsal column stimulation in rat spinal cord in vitro. J Physiol. 1994;478(Pt 1):87–99.
Cui JG, O’Connor WT, Ungerstedt U, Linderoth B, Meyerson BA. Spinal cord stimulation attenuates augmented dorsal horn release of excitatory amino acids in mononeuropathy via a GABAergic mechanism. Pain. 1997;73:87–95.
Cui JG, Meyerson BA, Sollevi A, Linderoth B. Effect of spinal cord stimulation on tactile hypersensitivity in mononeuropathic rats is potentiated by simultaneous GABA(B) and adenosine receptor activation. Neurosci Lett. 1998;247:183–6.
Lind G, Schechtmann G, Winter J, Meyerson BA, Linderoth B. Baclofen-enhanced spinal cord stimulation and intrathecal baclofen alone for neuropathic pain: Long-term outcome of a pilot study. Eur J Pain. 2008;12:132–6.
Lind G, Meyerson BA, Winter J, Linderoth B. Intrathecal baclofen as adjuvant therapy to enhance the effect of spinal cord stimulation in neuropathic pain: a pilot study. Eur J Pain. 2004;8:377–83.
Schechtmann G, Lind G, Winter J, Meyerson BA, Linderoth B. Intrathecal clonidine and baclofen enhance the pain-relieving effect of spinal cord stimulation: a comparative placebo-controlled, randomized trial. Neurosurgery. 2010;67:173–81.
Janssen SP, Truin M, van Kleff M, Joosten EA. Differential GABAergic disinhibition during the development of painful peripheral neuropathy. Neuroscience. 2011;184:183–94.
Schechtmann G, Song Z, Ultenius C, Meyerson BA, Linderoth B. Cholinergic mechanisms involved in the pain relieving effect of spinal cord stimulation in a model of neuropathy. Pain. 2008;139:136–45.
Cui JG, Linderoth B, Meyerson BA. Effects of spinal cord stimulation on touch-evoked allodynia involve GABAergic mechanisms. An experimental study in the mononeuropathic rat. Pain. 1996;66:287–95.
Linderoth B, Gazelius B, Franck J, Brodin E. Dorsal column stimulation induces release of serotonin and substance P in the cat dorsal horn. Neurosurgery. 1992;31:289–96.
Liu FY, Qu XX, Ding X, Cai J, Jiang H, Wan Y, Han JS, Xing GG. Decrease in the descending inhibitory 5-HT system in rats with spinal nerve ligation. Brain Res. 2010;1330:45–60.
Liu FY, Xing GG, Qu XX, Xu IS, Han JS, Wan Y. Roles of 5-hydroxytryptamine (5-HT) receptor subtypes in the inhibitory effects of 5-HT on C-fiber responses of spinal wide dynamic range neurons in rats. J Pharmacol Exp Ther. 2007;321:1046–53.
Suzuki R, Rahman W, Rygh LJ, Webber M, Hunt SP, Dickenson AH. Spinal-supraspinal serotonergic circuits regulating neuropathic pain and its treatment with gabapentin. Pain. 2005;117:292–303.
•• Song Z, Meyerson BA, Linderoth B: Spinal 5-HT receptors that contribute to the pain-relieving effects of spinal cord stimulation in a rat model of neuropathy. Pain 2011, 152:1666–1673. This extensive in vivo pharmacological study offers critical information about the respective roles of different spinal 5-HT receptor subtypes in SCS analgesia under neuropathic pain condition. It suggests that activation of 5-HT2A,3,4 receptors is important to SCS analgesia, partly via GABAergic interneurons.
Wei F, Dubner R, Zou S, Ren K, Bai G, Wei D, Guo W. Molecular depletion of descending serotonin unmasks its novel facilitatory role in the development of persistent pain. J Neurosci. 2010;30:8624–36.
Asante CO, Dickenson AH. Descending serotonergic facilitation mediated by spinal 5-HT3 receptors engages spinal rapamycin-sensitive pathways in the rat. Neurosci Lett. 2010;484:108–12.
Fukushima T, Ohtsubo T, Tsuda M, Yanagawa Y, Hori Y. Facilitatory actions of serotonin type 3 receptors on GABAergic inhibitory synaptic transmission in the spinal superficial dorsal horn. J Neurophysiol. 2009;102:1459–71.
Wang YY, Wu SX, Liu XY, Wang W, Li YQ. Effects of c-fos antisense oligodeoxynucleotide on 5-HT-induced upregulation of preprodynorphin, preproenkephalin, and glutamic acid decarboxylase mRNA expression in cultured rat spinal dorsal horn neurons. Biochem Biophys Res Commun. 2003;309:631–6.
Levin BE, Hubschmann OR. Dorsal column stimulation: Effect on human cerebrospinal fluid and plasma catecholamines. Neurology. 1980;30:65–71.
Song Z, Meyerson BA, Linderoth B. Muscarinic receptor activation potentiates the effect of spinal cord stimulation on pain-related behavior in rats with mononeuropathy. Neurosci Lett. 2008;436:7–12.
Radhakrishnan R, Sluka KA. Spinal muscarinic receptors are activated during low or high frequency TENS-induced antihyperalgesia in rats. Neuropharmacology. 2003;45:1111–9.
Schechtmann G, Wallin J, Meyerson BA, Linderoth B. Intrathecal clonidine potentiates suppression of tactile hypersensitivity by spinal cord stimulation in a model of neuropathy. Anesth Analg. 2004;99:135–9.
Zhang HM, Chen SR, Cai YQ, Richardson TE, Driver LC, Lopez-Berestein G, Pan HL. Signaling mechanisms mediating muscarinic enhancement of GABAergic synaptic transmission in the spinal cord. Neuroscience. 2009;158:1577–88.
Chen SR, Pan HL. Spinal GABAB receptors mediate antinociceptive actions of cholinergic agents in normal and diabetic rats. Brain Res. 2003;965:67–74.
Gassner M, Ruscheweyh R, Sandkuhler J. Direct excitation of spinal GABAergic interneurons by noradrenaline. Pain. 2009;145:204–10.
Miraucourt LS, Moisset X, Dallel R, Voisin DL. Glycine inhibitory dysfunction induces a selectively dynamic, morphine-resistant, and neurokinin 1 receptor- independent mechanical allodynia. J Neurosci. 2009;29:2519–27.
Lind G, Schechtmann G, Winter J, Linderoth B. Drug-enhanced spinal stimulation for pain: a new strategy. Acta Neurochir Suppl. 2007;97:57–63.
Song Z, Meyerson BA, Linderoth B: The interaction between antidepressant drugs and the pain-relieving effect of spinal cord stimulation in a rat model of neuropathy. Anesth Analg 2011.
Fuentes R, Petersson P, Siesser WB, Caron MG, Nicolelis MA. Spinal cord stimulation restores locomotion in animal models of Parkinson’s disease. Science. 2009;323:1578–82.
Gao J, Wu M, Li L, Qin C, Farber JP, Linderoth B, Foreman RD. Effects of spinal cord stimulation with “standard clinical” and higher frequencies on peripheral blood flow in rats. Brain Res. 2010;1313:53–61.
Maeda Y, Ikeuchi M, Wacnik P, Sluka KA. Increased c-fos immunoreactivity in the spinal cord and brain following spinal cord stimulation is frequency-dependent. Brain Res. 2009;1259:40–50.
Waltz JM. Spinal cord stimulation: a quarter century of development and investigation. A review of its development and effectiveness in 1,336 cases. Stereotact Funct Neurosurg. 1997;69:288–99.
Kumar K, Taylor RS, Jacques L, Eldabe S, Meglio M, Molet J, Thomson S, O’Callaghan J, Eisenberg E, Milbouw G, Buchser E, Fortini G, Richardson J, North RB. The effects of spinal cord stimulation in neuropathic pain are sustained: a 24-month follow-up of the prospective randomized controlled multicenter trial of the effectiveness of spinal cord stimulation. Neurosurgery. 2008;63:762–70.
Li J, Simone DA, Larson AA. Windup leads to characteristics of central sensitization. Pain. 1999;79:75–82.
Wallin J, Fiska A, Tjolsen A, Linderoth B, Hole K. Spinal cord stimulation inhibits long-term potentiation of spinal wide dynamic range neurons. Brain Res. 2003;973:39–43.
Ji RR, Kohno T, Moore KA, Woolf CJ. Central sensitization and LTP: do pain and memory share similar mechanisms? Trends Neurosci. 2003;26:696–705.
Ikeda H, Stark J, Fischer H, Wagner M, Drdla R, Jager T, Sandkuhler J. Synaptic amplifier of inflammatory pain in the spinal dorsal horn. Science. 2006;312:1659–62.
Truin M, van Kleef M, Linderoth B, Smits H, Janssen SP, Joosten EA. Increased efficacy of early spinal cord stimulation in an animal model of neuropathic pain. Eur J Pain. 2011;15:111–7.
Truin M, Janssen SP, van Kleef M, Joosten EA. Successful pain relief in non-responders to spinal cord stimulation: The combined use of ketamine and spinal cord stimulation. Eur J Pain. 2011;15:1049.
Wu M, Linderoth B, Foreman RD. Putative mechanisms behind effects of spinal cord stimulation on vascular diseases: a review of experimental studies. Auton Neurosci. 2008;138:9–23.
Wu M, Komori N, Qin C, Farber JP, Linderoth B, Foreman RD. Extracellular signal-regulated kinase (ERK) and protein kinase B (AKT) pathways involved in spinal cord stimulation (SCS)-induced vasodilation. Brain Res. 2008;1207:73–83.
Smits H, Kleef MV, Honig W, Gerver J, Gobrecht P, Joosten EA. Spinal cord stimulation induces c-Fos expression in the dorsal horn in rats with neuropathic pain after partial sciatic nerve injury. Neurosci Lett. 2009;450:70–3.
Ji RR, Baba H, Brenner GJ, Woolf CJ. Nociceptive-specific activation of ERK in spinal neurons contributes to pain hypersensitivity. Nat Neurosci. 1999;2:1114–9.
Suzuki R, Morcuende S, Webber M, Hunt SP, Dickenson AH. Superficial NK1-expressing neurons control spinal excitability through activation of descending pathways. Nat Neurosci. 2002;5:1319–26.
Rees H, Roberts MH. Activation of cells in the anterior pretectal nucleus by dorsal column stimulation in the rat. J Physiol. 1989;417:361–73.
El-Khoury C, Hawwa N, Baliki M, Atweh SF, Jabbur SJ, Saade NE. Attenuation of neuropathic pain by segmental and supraspinal activation of the dorsal column system in awake rats. Neuroscience. 2002;112:541–53.
Saade NE, Tabet MS, Soueidan SA, Bitar M, Atweh SF, Jabbur SJ. Supraspinal modulation of nociception in awake rats by stimulation of the dorsal column nuclei. Brain Res. 1986;369:307–10.
Salibi NA, Saade NE, Banna NR, Jabbur SJ. Dorsal column input into the reticular formation. Nature. 1980;288:481–3.
Ren B, Linderoth B, Meyerson BA. Effects of spinal cord stimulation on the flexor reflex and involvement of supraspinal mechanisms: an experimental study in mononeuropathic rats. J Neurosurg. 1996;84:244–9.
Ossipov MH, Lai J, Malan Jr TP, Porreca F. Spinal and supraspinal mechanisms of neuropathic pain. Ann N Y Acad Sci. 2000;909:12–24.
Vera-Portocarrero LP, Zhang ET, Ossipov MH, Xie JY, King T, Lai J, Porreca F. Descending facilitation from the rostral ventromedial medulla maintains nerve injury-induced central sensitization. Neuroscience. 2006;140:1311–20.
Gardell LR, Vanderah TW, Gardell SE, Wang R, Ossipov MH, Lai J, Porreca F. Enhanced evoked excitatory transmitter release in experimental neuropathy requires descending facilitation. J Neurosci. 2003;23:8370–9.
Suzuki R, Dickenson A. Spinal and supraspinal contributions to central sensitization in peripheral neuropathy. Neurosignals. 2005;14:175–81.
King T, Vera-Portocarrero L, Gutierrez T, Vanderah TW, Dussor G, Lai J, Fields HL, Porreca F. Unmasking the tonic-aversive state in neuropathic pain. Nat Neurosci. 2009;12:1364–6.
Qu C, King T, Okun A, Lai J, Fields HL, Porreca F. Lesion of the rostral anterior cingulate cortex eliminates the aversiveness of spontaneous neuropathic pain following partial or complete axotomy. Pain. 2011;152:1641–8.
Pedersen LH, Blackburn-Munro G. Pharmacological characterisation of place escape/avoidance behaviour in the rat chronic constriction injury model of neuropathic pain. Psychopharmacology (Berl). 2006;185:208–17.
Stiller CO, Linderoth B, O’Connor WT, Franck J, Falkenberg T, Ungerstedt U, Brodin E. Repeated spinal cord stimulation decreases the extracellular level of gamma-aminobutyric acid in the periaqueductal gray matter of freely moving rats. Brain Res. 1995;699:231–41.
Acknowledgment
Dr. Yun Guan thanks Claire F. Levine, MS (Scientific Editor, Department of Anesthesiology and Critical Care Medicine, Johns Hopkins University) for editing the manuscript.
Disclosure
Dr. Yun Guan has received a research grant from Medtronic.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Guan, Y. Spinal Cord Stimulation: Neurophysiological and Neurochemical Mechanisms of Action. Curr Pain Headache Rep 16, 217–225 (2012). https://doi.org/10.1007/s11916-012-0260-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11916-012-0260-4