Abstract
Purpose of Review
Sleep disturbances are amongst most frequent non-motor symptoms of Parkinson’s Disease (PD), and they are similarly frequently reported in other alpha-syncleinopathies, such as Dementia with Lewy Bodies (DLB) and Multiple System Atrophy (MSA). More recently, the orexin system has been implicated in control of arousal based on salient environmental set points, and its dysregulation in sleep issues in alpha-synucleinopathies suggested by the findings from the translational animal models. However, its role in the patients with alpha-synucleinopathies remains unclear. We thus set to systematically review, and to critically assess, contemporary evidence on the association of the orexinergic system and sleep disturbances in alpha-synucleinopathies. In this systematic review, studies investigating orexin and sleep in alpha-synucleinopathies (Rapid Eye Movement (REM) Behaviour Disorder (RBD), Parkinson's Disease (PD), Dementia with Lewy Bodies (DLB), Multiple System Atrophy (MSA)) were identified using electronic database searches of PubMed, Web of Science and PsychINFO using MeSH terms, keywords, and title words such as “Alpha-synucleinopathies” AND “Orexin” AND “Sleep Disturbances”.
Recent findings
17 studies were included in this systemic review, of which 2 studies on RBD, 10 on PD, 4 on DLB, and 1 on MSA patients. Taken together, RBD and PD studies suggest a potential adaptive increase in orexin levels in early stages of the neurodegenerative process, with reduced levels more often reported for later, more advanced stages of illness. To date, no differences in orexin levels were demonstrated between MSA patients and healthy controls.
Summary
There is a dearth of studies on the role of orexin levels in alpha-synucleinopathies. Moreover, significant methodologic limitations in the current body of work, including use of non-standardised research protocols and lack of prospective, multi-centre studies, disallow for any finite conclusion in regards to underlying pathomechanisms. Nonetheless, a picture of a complex, multifaceted relationship between the dysregulation of the orexinergic pathway and sleep disturbances in alpha-synucleinopathies is emerging. Hence, future studies disentangling orexinergic pathomechanisms of alpha-syncleinopathies are urgently needed to obtain a more comprehensive account of the role of orexinergic pathway in alpha-synucleinopathies. Pharmacological manipulations of orexins may have multiple therapeutic applications in treatment strategies, disease diagnosis, and might be effective for treating both motor and non-motor symptoms.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It has been argued that alpha-synucleinopathies, and in particular Parkinson disease (PD), are amongst the fastest growing neurological disorder worldwide [1]; they are a group of neurodegenerative disorders characterised by pathological hallmarks such as abnormal accumulation of alpha-synuclein positive inclusions in the neurons and/or glial cells that trigger progressive neuronal death through a series of cascading cellular pathways (i.e., mitochondrial impairment, lysosomal dysfunction) [2, 3]. Neurodegenerative diseases that are classified as alpha-synucleinopathies include Parkinson’s Disease (PD), Multiple System Atrophy (MSA), and Dementia with Lewy Bodies (DLB) [2]. All alpha-synucleinopathies appear to exhibit similar clinical, neurochemical, and morphological features and disease pathomechanisms including neuroinflammation [2]. Despite that, variation in clinical phenotypes between and within alphasynucleinopathies has been widely reported, depending on the cellular location and pattern of accumulation [4, 5]. For example, neuronal inclusions, Lewy bodies and Lewy neurites are distinct characteristics for PD and DLB, whilst alpha-synuclein positive glial cytoplasmic inclusions in oligodendrocytes are hallmarks in MSA [2,3,4, 6].
Patients with alpha-synucleinopathies commonly suffer from significant and debilitating sleep disturbances that include nocturnal and diurnal manifestations such as insomnia, excessive daytime sleepiness, periodic limb movements [7], circadian rhythm abnormalities, poor sleep quality and rapid eye movement sleep behaviour disorders (RBD) (please refer to some relevant studies and disorders listed in Table 1) [15]. For instance, nocturnal sleep disturbances affect 60% to 98% of people with PD [24,25,26], whilst excessive daytime sleepiness, and other sleep disturbances occur in approximately 80% of DLB patients [13, 15, 27]. Although the underlying pathomechanism of these sleep disturbances remains elusive, numerous preclinical and clinical studies have argued the association of orexin and sleep disturbances in alpha-synucleinopathies [28,29,30,31].
Orexin, also known as hypocretin, is a neuropeptide that is predominantly released from orexinergic neurons in the lateral hypothalamus and the perifornical area; it exist in two orexin isoforms, orexin-A and orexin-B [28, 32,33,34]. Orexin-A acts predominantly on orexin-1 (OX1R) and orexin-2 receptors (OX2R) whilst Orexin-B on the OX2R [28]. There is a widespread and complimentary expression of OXRs receptors in most brain areas, although OX1R are principally expressed in amygdala and locus coeruleus, and OX2R is predominantly expressed in the hypothalamus [28, 35]. Orexin-A and -B are also known to be involved in a number of other functions, including stress-adaptive responses [36], feeding behaviour [37], reward-seeking, drug addiction [38] and even in pathological conditions such as migraines and headaches [39,40,41]. Importantly, orexin neurons play a central role in promoting wakefulness and stabilising sleep by modulating cholinergic and monoaminergic neurons via strong projections to brain regions involved in the sleep-wake circuitry, such as the locus coeruleus, dorsal raphe nucleus and tuberomammillary nucleus [42], whilst GABAergic neurons regulate orexinergic neurons to sustain vigilance [28, 35, 43, 44]. As such, the orexin may signal an overall arousal need, defined as a need to counteract actual or potential hazards [45]. In pathologic situations of its reduction, arousal is no longer appropriately coupled to internal and external environment, and sleep-wake instability ensues [45].
Thus, increasingly, the orexinergic system has also been implicated as a key pathophysiological centre for sleep disturbances, pertaining to disorders of hypersomnolence (i.e., narcolepsy type 1, narcolepsy type 2, hypersomnia) [46]. In both animal and human studies, downregulation of the OXR receptors, disrupted OXR signalling, and orexin knockout mice were reported to exhibit narcolepsy, excessive daytime sleepiness, and cataplexy [28, 32, 42, 43, 47,48,49,50].
Interestingly, further investigation into orexin receptor polymorphisms have found significant association to specific sleep disturbances in alpha-synucleinopathies [51]. For instance, Rissling and colleagues (2005) conducted an association study analysing the distribution of preprohypocretin polymorphisms in patients with PD with and without sudden onset of sleep [51]. They found significant differences in genotype and allele distribution between patients with PD with, and without, sudden onset of sleep [51]. Particularly, the variant allele T of the preprohypocretin polymorphism was more commonly found in patients with PD with sudden onset of sleep [51]. This suggests a role that genetic factors might play in the pathogenesis of sleep disturbances in alpha-synucleinopathies.
Other clinical studies have also investigated orexin levels using either plasma, spinal CSF or ventricular CSF in alpha-synucleinopathies such as PD [29, 30], MSA [52, 53], and DLB [31, 54], and even in the prodromal stage of alpha-synucleinopathies such as RBD [55, 56]. However, the findings remain inconsistent, with some studies indicating that orexin levels might be lower, elevated, or unaffected in alpha-synucleinopathies [29,30,31, 54, 57, 58].
To date, available treatments for sleep disorders in alpha-synucleinopathies are only partially effective, partly due to the limited mechanistic insight into their oetiology and hence, we set to systemically review and to obtain a more comprehensive and critical overview of the role of orexin in sleep in patients with alpha-synucleinopathies.
Methods
Search Strategies
This systematic review was conducted following the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines [59] (Fig. 1.). Relevant studies were identified by two reviewers using the electronic databases of PubMed, PsychINFO (EBSCOhost) and Web of Science. The following keywords were used: (Alpha-synucleinopathies OR REM Behaviour Disorder OR Parkinson’s Disease OR Dementia with Lewy Bodies OR Multiple System Atrophy) AND (Orexin) AND (Sleep OR Sleep Disorders OR Sleep Disturbances) (Table 2). Eligible papers were extracted from 2002 until August 2023. The references of the selected articles were also examined to retrieve documents missed by the literature search.
Inclusion and Exclusion Criteria
Each article was first considered by title and abstract. This systematic review included: 1) original research articles; 2) only papers written in English; 3) observational, descriptive, longitudinal, retrospective, cross-sectional, or cohort studies; 4) studies that investigated orexin, sleep and alpha-synucleinopathies and 5) human studies. Assigned reviewers independently screened each eligible study, and disagreements were resolved through discussion after retrieving full text to determine whether inclusion and exclusion criteria were met (Tables 3 and 4).
Data Extraction
For each article, two reviewers (KR and SQ) independently extracted the following data: study name and year, the country, type of study, study aim, the subtype of alpha-synucleinopathy, sample size and age of patients, the methods used, main findings and critical evaluation of the study. Subsequently, articles were classified and grouped according to the subtype of alpha-synucleinopathy (i.e., RBD, PD, MSA or DLB).
Quality Assessment
The quality of studies was evaluated using the Quality Assessment Tool for Quantitative Studies, developed by the Effective Public Health Practice Project (EPHPP; www.ephpp.ca/tool.html) for observational, descriptive, longitudinal, cross-sectional, or cohort studies original research articles [60]. Any disagreements were resolved by discussion with the panel of reviewers, or by consulting with a senior reviewer. For the EPHPP scale, the following criteria were rated for each study on a scale of strong, moderate, or weak: selection bias, study design, blinding, data collection methods, confounders, and withdrawals/attrition (if any). Subsequently, these ratings were compiled to form a global rating: studies were rated as strong if they had no weak ratings, moderate if they had one weak rating, and weak if they received two or more weak ratings.
Results
Methodological Quality Assessment Results
Comprehensive tables of the methodological quality assessment of studies using the EPHPP Quality Assessment Tool for Quantitative Studies [60] are displayed in the supplementary section. Quality assessment of studies using the Quality Assessment Tool for Quantitative Studies by EPHPP are presented in Supplementary Table 1. Selection bias was generally rated as moderate as participants in most studies were selected from clinics or hospital settings. Study design was generally rated as moderate as they were observational studies. Studies were rated as weak or strong for confounders. Those rated as weak were because they did not account for potential confounding variables, such as age, disease duration, etc. All studies used valid and reliable measures for sleep (Epworth Sleepiness Scale, Pittsburgh Sleep Quality Index, Multiple Sleep Latency Test etc) and orexin level (radioimmunoassay, ELISA etc). No withdrawals were reported in any of the included studies. No observable association was found between global rating scores and the outcome of the findings.
Studies characteristics
Our systematic analysis identified 17 studies investigating the association of the orexin pathway and sleep in alpha-synucleinopathies that fulfilled our criteria. These studies were published between the year 2002 and 2022. Among the 17 identified studies, 2 studies included patients with RBD [55, 56], 10 studies with patients with PD [29, 30, 57, 61,62,63,64,65,66,67], 4 studies with patients with DLB [31, 54, 58, 68] and 2 studies with patients with MSA [52, 53] (Table 7). It is also worth noting that level of orexin was measured differently in these studies: 12 studies measured orexin levels in spinal CSF [29, 31, 53,54,55,56,57, 61, 63,64,65, 68], 2 studies used ventricular CSF [62, 66], 2 studies were done on plasma orexin levels only [30, 67] and one study included autopsy findings [58] (Table 5).
Rapid eye movement behaviour disorder (RBD)
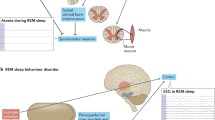
Rapid Eye Movement (REM) behaviour disorder (RBD) is a parasomnia characterized by abnormal, violent dream-enacting behaviour, accompanied by an excess of muscle tone (muscle atonia) and/or phasic muscle twitching during REM sleep [69,70,71,72]. Most motor events during RBD episodes typically range from simple elementary movements such as laughing, gesturing, or singing to complex, violent behaviours such as punching, kicking, or biting [72,73,74]. RBD can be categorized into idiopathic RBD (iRBD) when presented with symptoms not ascribable to any other neurological disorders or secondary RBD (sRBD) when associated with other neurological conditions such as narcolepsy type 1 [72, 73, 75]. Importantly, iRBD is increasingly recognised to present an early stage of alpha-synucleinopathy process, such as occur in PD, MSA and DLB [76,77,78,79].
In a recent cross-sectional study in China, Yuan and colleagues collected spinal CSF and serum samples from three groups of patients; iRBD, PD with RBD, and PD without RBD, in order to investigate the association between orexin and tumour necrosis factor alpha (TNF-alpha) levels with motor, sleep, and cognitive symptoms [56]. Interestingly, despite abnormal CSF orexin levels (<200 pg/ml) in all the three groups (PD with RBD: 177.69 ± 46.04 pg/ml; PD without RBD: 177.31 ± 29.4 pg/ml and iRBD: 166.23 ± 40.62 pg/ml), orexin levels in the three groups were not reported significantly lower than in the control group [56]. Moreover, no significant difference in CSF orexin levels between the three groups was demonstrated, despite Unified Parkinson's Disease Rating Scale (UPDRS-III) scores being significantly higher in the PD with RBD and PD without RBD groups and REM sleep behavior disorder questionnaire (RBDQ-HK) scores significantly higher in RBD, perhaps suggesting that orexin levels may not be a sensitive marker for motor severity and sleep behaviours [56].
However, these findings are somewhat inconsistent with an earlier study that measured CSF orexin levels in five iRBD patients and control group (consisting of narcolepsy and multiple sclerosis patients) and reported slightly higher orexin levels between 250 and 454 pg/ml (mean 369.2 ± 43.91 pg/ml) in iRBD group [55]. In this study, the Epworth Sleepiness Score (ESS) was reported normal at 5.3 (scored out of 24 points) in iRBD patients, which may suggest an underlying compensatory mechanism at play [55]. Several methodological factors could explain these contrasting findings. Firstly, the small sample sizes of both studies increase likelihood of speculative findings [55]. Secondly, in study by Yuan and colleagues, it is not clear whether RBD appeared before or after motor symptoms, and thus, set of different neuropathologic trajectories may be at play here [56]. Additionally, neither study made attempt at classification according to patients’ respective medication status, and as such it may not be reflective of the observable symptomatic behaviours (i.e., any sleep disturbances). Consequently, results of sleep scales such as ESS and RBDQ may be insufficiently sensitive to reflect the actual clinical status. Finally, perhaps unsurprisingly, neither study demonstrated an association between sleep, or disease severity measures, and orexin levels.
Parkinson’s Disease
Parkinson’s disease (PD) is the second most common neurodegenerative disorder associated with the presence of intraneuronal Lewy bodies and Lewy neurites, loss of dopaminergic neurons in the substantia nigra, aberrant intracellular alpha-synuclein protein aggregations and neuroinflammation [80, 81]. Consequently, patients with PD exhibit a diverse range of motor and non-motor symptoms including resting tremor, bradykinesia, autonomic dysfunction, cognitive deficits, depression, and postural instability [82, 83]. Of non-motor symptoms, they also frequently display a range of general and more distinct sleep disturbances, including insomnia, sleep attacks (not unlike those in narcolepsy) [27], excessive daytime sleepiness, as well as parasomnias, such as REM Behaviour Disorder [84,85,86,87,88,89,90,91,92,93,94].
As a result of the high prevalence of sleep disturbances in patients with PD, there is a growing interest in orexin as fluctuations in CSF orexin and degeneration of orexinergic neurons have been associated with the development of sleep disorders that mimic early stages of alpha-synucleinopathy in other groups of patients (e.g. secondary RBD in narcolepsy) [29, 30, 57, 61,62,63,64,65, 95].
Several studies failed to demonstrate significant changes in orexin levels in PD patients [63, 64]. For example, Asai and colleagues measured CSF orexin levels in three groups of patient with PD; those without sleep disturbances, those with excessive daytime somnolence, and patients with sleep attacks and found no significant differences in orexin levels between the three groups, although orexin levels negatively correlated with disease duration [63]. Additionally, Compta and colleagues also measured CSF orexin-A levels in patient with PD with dementia, and without dementia [64]. Interestingly, despite higher ESS scores in both groups than in controls, there was no difference in CSF orexin-A levels between the three groups [64].
Orexin has been argued to play a neuroprotective and immune-regulatory role in the central nervous system, which may be affected in later stages of alpha-synucleinopathy process, when alpha-synuclein may act to promote the degradation of OX1R through lysosomal and proteasomal pathways [30, 96]. In that light, another study that reported reduced orexin levels in hyper-somnolent PD patients, as compared to controls, is of interest [57]. Here, glial fibrillary acidic protein (GFAP) levels, suggestive of neuroinflammation, were reported as significantly higher in patients with hypersomnolence and narcolepsy, but not in patient with PD without hypersomnolence [57].
In past, several studies also reported lower orexin CSF levels in patients with PD. For instance, in a retrospective study conducted in China that investigated association between CSF orexin levels, sleep, and clinical characteristics the significantly lower levels of CSF orexin in patients with PD (median = 272 pg/mL), as compared to controls (median = 352.2 pg/mL), were demonstrated [29]. In keeping, in another retrospective, case-control, post-mortem study of patients with PD, a reduced number of orexinergic neurons, and lower CSF and prefrontal orexin levels were similarly reported [95]. Moreover, lower CSF orexin levels, correlated with PD disease severity, were also reported [66]. Notably, Wienecke and colleagues [61] measured repeated CSF orexin levels in two patients with PD and reported a marked decrease of orexin concentrations over time, suggesting a progressive loss of orexin as disease advances [61].
Notwithstanding this, an uneven polymorphic picture emerges from studies where the association of orexin levels to specific sleep characteristics was investigated. For example, Ogawa and colleagues report no significant correlation between CSF orexin levels and PD clinical characteristics, including excessive daytime somnolence scores, presence of RBD, or use of dopamine agonists [29]. Moreover, this lack of association remained for the duration of a follow up [29]. In striking contrast, Wienecke and colleagues have demonstrated a strong link between CSF orexin levels and the mean sleep latencies on MSLT [61].
In regards to links between orexin and sleep macrostructure, Bridoux and colleagues have reported a significant positive correlation between orexin-A levels and the percentage of REM epochs without atonia, but they failed to demonstrate any correlation with total sleep time, REM duration or REM latency [62]. Strikingly, however, in this study, patients with loss of REM atonia had higher median orexin levels than the four patients with REM sleep atonia (235 pg/mL versus 94 pg/mL) [62].
Whilst the pathomechanisms behind these diverse findings remain unclear, a potential insight could be gleamed from the prospective study by Huang and colleagues [30]. They report an initial increase in orexin-A levels in early-stage and medium-stage PD, with decreased levels then demonstrated in advanced stage of PD [30]. These findings suggests that orexin levels may reflect the dynamic changes occurring in disease severity and disease duration.
Other methodological and physiological factors could also potentially account for these polymorphic findings (see Table 6). Firstly, sampling of orexin from different areas and times may explain differences in orexin level; e.g. orexin levels fluctuate over the day due to circadian rhythmicity [97]. Also, orexin level in spinal CSF is reportedly reduced in acute neurological disorders, whilst ventricular CSF orexin correlated with prefrontal cortex orexin concentration [65]. Secondly, in a similar vein, reduction in CSF orexin level depends heavily on the level and progression of degeneration of orexin neurons in the lateral hypothalamus [98]. For instance, in a study investigating the relationship between CSF orexin levels and orexin neuronal loss, Gerashchenko and colleagues reported that maximal reduction of CSF orexin level was only observed on day 60 without further decline or recovery, following a neurotoxin-induced lateral hypothalamic injury [98]. This suggests CSF orexin level may not be a very sensitive indicator of loss of orexinergic neurons in the early stage of PD as remaining orexinergic neurons engage in a compensatory mechanism to counteract and increase CSF orexin levels.
Thirdly, it is worth highlighting that these studies have adopted different methodological approaches in terms of including the subtypes of sleep disturbances (i.e., nocturnal versus diurnal; sleep attacks, hypersomnolence, RBD), subtypes of PD (i.e., with or without dementia) and the choice of controls used or other pathological conditions [30, 62, 64, 65, 67]. On a similar note, pathological relevance of CSF orexin levels in alpha-synucleinopathies also needs to be accounted for. For instance, the benchmark for abnormal CSF orexin levels is predominantly based on diagnosis of narcolepsy (i.e., normal: >200 pg/mL, intermediate: 110 to 200 pg/mL, and abnormal: <110 pg/mL) [99]. Lastly, in most of these studies, there is also the lack of consideration of other interplaying factors that may affect the availability of orexin levels and clinical symptomology. For example, in a preclinical study, Zhan and colleagues reported that higher expression of TNF-a in neuroinflammation-induced PD mice model, is associated with the degradation of orexinergic neurons, which led to development of other non-motor symptoms and sleep disturbances [100] . Future human studies should consider utilizing a translational approach to investigate modulation of the orexinergic pathway at cellular, subcellular, and molecular level.
In summary, in keeping to those in iRBD, studies of patient with PD report diverse findings, with some stating higher, other lower than normal range, and some found normal levels of orexin in patients with PD [29, 30, 57, 61,62,63,64,65,66,67, 95]. Thus, to date, the reliability of orexin levels as a predictive biomarker of sleep disturbances remains unclear [29, 30, 62]. It has been similarly argued that besides potential methodological and physiological factors, these contrasting findings may reflect a complex, multifaceted pathomechanisms of the orexinergic pathway in alpha-synucleinopathies.
Dementia with Lewy Bodies
Dementia with Lewy Bodies (DLB) is characterised by the accumulation of aggregated alpha-synuclein protein in Lewy bodies and Lewy neurites [101]). Core clinical features of DLB include neuropsychiatric symptoms, progressive cognitive decline, and parkinsonism [102]. Alpha-synuclein aggregation in orexin-containing neurons in the hypothalamus has been demonstrated [103], and various studies further reported its interference with multiple cellular functions [58, 104], potentially contributing to progressive loss of orexin-containing neurons loss in DLB. Moreover, abnormal sleep-wake rhythms, excessive daytime sleepiness, insomnia and RBD have all similarly been reported to occur in DLB [105].
Several studies have investigated orexin levels in patients with DLB [31, 54, 58, 68]. In a cross-sectional study, Trotti and colleagues examined the association of orexin, dementia biomarkers and sleep disturbances in four clinical populations: Alzheimer’s Disease (AD), frontotemporal dementia (FTD), DLB and healthy controls [54]. Here, orexin levels were predominantly associated to the type of sleep disturbances. More specifically, lower orexin-A levels were related to frequency of nightmares (patients with nightmares: 203.9 ± 29.8 pg/mL, patients without nightmares: 240.4 ± 46.1 pg/mL) and vivid dreams (209.1 ± 28.3 versus 239.5 ± 47.8 pg/mL) [54]. These findings are consistent with an earlier study by Lessig and colleagues [58] who reported reduced neocortical orexin immunoreactivity in DLB, as compared to AD patients and controls [58]. In this study, orexin levels were significantly linked with severity of hypersomnolence and alpha-synuclein levels [58], perhaps similarly suggesting that dysregulation of orexin regulating sleep-wake stability may be a more sensitive biomarker of distinct sleep phenotypes.
Conversely, other studies failed to report significant reductions in orexin levels in DLB [31, 68]. For instance, Inagawa and colleagues did not demonstrate significant differences in CSF orexin A levels between patients with DLB (271.6 ± 114.5 pg/mL) and controls (301.0 ± 64.0 pg/mL) [31]. Similarly, Baumann and colleagues showed normal levels of orexin levels in DLB (mean 521 pg/mL), as compared to controls (497 pg/mL) and AD patients (474 pg/mL) [68].
A lack of standardisation of protocols for orexin sampling, small samples sizes, different circadian rhythms, and inconsistent reporting on other potential confounding factors, such are medications and disease severity likely underlie at least some of the reported differential findings [31, 54, 58, 68].
Multiple System Atrophy
Multiple system atrophy (MSA) is clinically characterised by varying combination of parkinsonism, pyramidal signs, and progressive autonomic failure, and/or cerebellar ataxia; it is also pathologically characterised by the abnormal accumulation of alpha-synuclein in oligodendrocytes [106, 107]. As with other alpha-synucleinopathies, sleep disturbances such as RBD, fragmented sleep, excessive daytime somnolence and nocturnal stridor are frequently reported in MSA [52, 53, 108].
Perhaps unsurprisingly given its prevalence, there are only a few studies that investigated links between orexin levels and disease severity, mostly with negative findings [52, 53]. In a small retrospective study conducted in the Netherlands, Abdo and colleagues reported that CSF orexin levels did not differ between MSA patient group (mean = 343 pg/mL) and controls (mean = 339 pg/mL) [52], although no sleep measurements were included. In keeping, Martinez-Rodriguez and colleagues reported normal CSF orexin level (>200 pg/mL) in MSA patients with significant sleep issues, suggesting that orexin levels may not be a sensitive biomarker for detecting sleep disorders in MSA [53].
The lack of clear findings is somewhat surprising given that loss of approximately 70% of orexin-producing neurons in the posterior hypothalamic regions has been reported [109]. Again, methodologic differences, small sample sizes and lack of standardisation of CSF sampling protocols (ventricular vs spinal) have been argued to underlie some of these findings, or lack of them [95].
Discussion
We have critically reviewed the contemporary literature that investigates the orexinergic system and sleep disturbances in alpha-synucleinopathies. Our findings overwhelmingly highlight scarcity of studies that investigated the association of orexin and sleep in alpha-synucleinopathies, and further emphasise the lack of systematic and standardised methodological research protocols. Nonetheless, for iRBD and PD patients certain pattern appears to be emerging, that of an initial (compensatory) adaptive increase in orexin production, with subsequent reduction in CSF orexin levels, linked to later stages, or to more severe PD. Given that distinct alpha-synucleinopathies differ in their spatio-temporal evolution and cellular localisation, this may explain why to date, no such pattern has been reported for MSA patients [52, 53].
In striking opposition to human data, the potential role for orexin as a therapeutical intervention in alleviating sleep disturbances and other symptoms of alpha-synucleinopathies has been supported by many preclinical studies. For instance, the neuroprotective role of orexin-A on dopaminergic neurons and BDNF levels in the substantia nigra has been reported [110,111,112,113,114,115]. Nonetheless, its translational and clinical role in alpha-synucleinopathy patients is yet to be fully understood.
Also, numerous studies have reported sex-specific differences in demographics, biomarkers, and clinical features in alpha-synucleinopathies [116,117,118]. Coincidentally, orexin has multiple endocrine effects, including its role in the regulation of central and peripheral signals for metabolic homeostasis [32]. More specifically, orexin have been reported to inhibit the release of prolactin and growth hormone with a modulatory effect on the release of luteinizing hormone [28, 32]. Orexin also controls the hypothalamic-pituitary axis (HPA) through OX2R receptor through stimulating adrenocorticotropin (ACTH) and corticosteroid secretions via activation of cortico-trophin-releasing hormones and vasopressin [32, 119]. Notwithstanding these findings, none of the reviewed studies accounted for possible sex differences and thus, its possible theoretical interplay in alpha-synucleinopathy presentations and illness trajectories similarly remains unclear [28, 32].
Moreover, several limitations across the 17 studies that were critically assessed affected our ability to draw definitive conclusions. These limitations included small sample sizes, methodological inconsistencies, and potential biases in data collection and reporting. For instance, the variability in study designs and the lack of rigorous phenotyping in regards to a specific subtype, disease severity, possible role of medications, sleep issues/disorders and cognitive symptoms, in some cases further compromised the reliability and generalizability of the findings. Consequently, while the assessed studies provide valuable insights, their limitations necessitate cautious interpretation of the results. Hence, to obtain a more integrative and coherent framework of the role of orexinergic pathway in sleep disturbances in alpha-synucleinopathies, future studies should systematically account for (1) a specific subtype of alpha-synucleinopathies (i.e., PD with or without dementia), (2) specific sleep phenotype (i.e., sleep attacks, hypersomnolence), (3) disease progression, rate, and severity (i.e., early versus late onset), (4) the standardised collection protocol for orexin measurements, (5) circadian effect, e.g. consistency in the time of orexin measurement, (6) consideration of medications (i.e., dopaminergic treatments) and finally (7) direct quantification of sex hormones and their relation to orexin and sleep disturbances severity.
Conclusions
Taken together, the body of work to date suggests an important, if complex and multidimensional, relationship between the dysregulation of the orexinergic pathway and the emergence of sleep disturbances in alpha-synucleinopathies. Moreover, it is possible that this interplay differentially impacts different alpha-synucleinopathies and their phenotypes, with no clear relationship so far being shown for the MSA.
Scarcity of studies and significant methodologic limitations in the current body of work disallow meaningful conclusion regarding the underlying pathomechanisms. Thus, we propose, sufficiently powered, large, longitudinal multi-centre studies of carefully phenotyped cohorts should be undertaken to obtain a more comprehensive account of the role of orexinergic pathway in sleep and other non-motor symptoms of alpha-synucleinopathies. With the new agonist and orexin receptor antagonists emerging [120], this is the perfect timing to explore therapeutic applications in treatment strategies that might be effective for treating both motor and non-motor symptoms in alpha-synucleinopathies.
Key References
• P. Tall, M.A. Qamar, I. Rosenzweig, V. Raeder, A. Sauerbier, Z. Heidemarie, C. Falup- Pecurariu, and K.R. Chaudhuri, The Park Sleep subtype in Parkinson's disease: from concept to clinic. Expert Opin Pharmacother 24 (2023) 1725-1736.
- An updated outline of treatment strategies for improvement of disorders of sleep and wakefulness in PD patients.
• M. Alrouji, H.M. Al-Kuraishy, A.I. Al-Gareeb, D. Zaafar, and G.E.-S. Batiha, Orexin pathway in Parkinson’s disease: a review. Molecular Biology Reports (2023) 1-14.
- A comprehensive review of implicated orexinergic pathways in Parkinson's Disease.
• T. Ogawa, Y. Kajiyama, H. Ishido, S. Chiba, G.S. Revankar, T. Nakano, S. Taniguchi, T. Kanbayashi, K. Ikenaka, and H. Mochizuki, Decreased cerebrospinal fluid orexin levels not associated with clinical sleep disturbance in Parkinson’s disease: A retrospective study. Plos one 17 (2022) e0279747.
- A retrospective study that demonstrated decreased CSF orexin levels in patients with PD, but without correlation to clinical characteristics.
• H. Asai, M. Hirano, Y. Furiya, F. Udaka, M. Morikawa, T. Kanbayashi, T. Shimizu, and S. Ueno, Cerebrospinal fluid-orexin levels and sleep attacks in four patients with Parkinson's disease. Clinical Neurology and Neurosurgery 111 (2009) 341-344.
- A small study that was amongst first to suggest that orexin transmission is likely involved in sleep attacks in PD.
References
Dorsey ER, Sherer T, Okun MS, Bloem BR. The emerging evidence of the Parkinson pandemic. J Parkinsons Dis. 2018;8:S3–8.
Calabresi P, Mechelli A, Natale G, Volpicelli-Daley L, Di Lazzaro G, Ghiglieri V. Alpha-synuclein in Parkinson’s disease and other synucleinopathies: from overt neurodegeneration back to early synaptic dysfunction. Cell Death Dis. 2023;14:176.
Spillantini MG, Schmidt ML, Lee VM-Y, Trojanowski JQ, Jakes R, Goedert M. α-Synuclein in Lewy bodies. Nature. 1997;388:839–40.
McCann H, Stevens CH, Cartwright H, Halliday GM. α-Synucleinopathy phenotypes. Parkinsonism Relat Disord. 2014;20:S62–7.
Malfertheiner K, Stefanova N, Heras-Garvin A. The concept of α-Synuclein strains and how different conformations may explain distinct neurodegenerative disorders. Front Neurol. 2021;12:737195.
Beyer K, Ariza A. Protein aggregation mechanisms in synucleinopathies: commonalities and differences. J Neuropathol Exp Neurol. 2007;66:965–74.
Drakatos P, Olaithe M, Verma D, Ilic K, Cash D, Fatima Y, Higgins S, Young AH, Chaudhuri KR, Steier J, Skinner T, Bucks R, Rosenzweig I. Periodic limb movements during sleep: a narrative review. J Thorac Dis. 2021;13:6476–94.
Zhang X, Sun X, Wang J, Tang L, Xie A. Prevalence of rapid eye movement sleep behavior disorder (RBD) in Parkinson’s disease: a meta and meta-regression analysis. Neurol Sci. 2017;38:163–70.
Melka D, Tafesse A, Bower JH, Assefa D. Prevalence of sleep disorders in Parkinson’s disease patients in two neurology referral hospitals in Ethiopia. BMC Neurol. 2019;19:1–6.
Kumar S, Bhatia M, Behari M. Sleep disorders in Parkinson's disease. Mov Disord. 2002;17:775–81.
Ylikoski A, Martikainen K, Partinen M. Parkinson's disease and restless legs syndrome. Eur Neurol. 2015;73:212–9.
Baumann-Vogel H, Hor H, Poryazova R, Valko P, Werth E, Baumann CR. REM sleep behavior in Parkinson disease: frequent, particularly with higher age. PLoS One. 2020;15:e0243454.
Ferman TJ, Boeve BF. Sleep in Parkinson’s disease and dementia with Lewy bodies. Psychiatry of Parkinson's Disease: Karger Publishers; 2012. p. 61–70.
Pistacchi M, Gioulis M, Contin F, Sanson F, Marsala SZ. Sleep disturbance and cognitive disorder: epidemiological analysis in a cohort of 263 patients. Neurol Sci. 2014;35:1955–62.
Elder GJ, Lazar AS, Alfonso-Miller P, Taylor JP. Sleep disturbances in Lewy body dementia: a systematic review. Int J Geriatr Psychiatry. 2022;37.
Plazzi G, Corsini R, Provini F, Pierangeli G, Martinelli P, Montagna P, Lugaresi E, Cortelli P. REM sleep behavior disorders in multiple system atrophy. Neurology. 1997;48:1094–6.
Lin J-Y, Zhang L-Y, Cao B, Wei Q-Q, Ou R-W, Hou Y-B, Liu K-C, Xu X-R, Jiang Z, Gu X-J. Sleep-related symptoms in multiple system atrophy: determinants and impact on disease severity. Chin Med J. 2021;134:690–8.
Palma J-A, Fernandez-Cordon C, Coon EA, Low PA, Miglis MG, Jaradeh S, Bhaumik AK, Dayalu P, Urrestarazu E, Iriarte J. Prevalence of REM sleep behavior disorder in multiple system atrophy: a multicenter study and meta-analysis. Clin Auton Res. 2015;25:69–75.
Ghorayeb I, Yekhlef F, Chrysostome V, Balestre E, Bioulac B, Tison F. Sleep disorders and their determinants in multiple system atrophy. J Neurol Neurosurg Psychiatry. 2002;72:798–800.
Vetrugno R, Provini F, Cortelli P, Plazzi G, Lotti EM, Pierangeli G, Canali C, Montagna P. Sleep disorders in multiple system atrophy: a correlative video-polysomnographic study. Sleep Med. 2004;5:21–30.
Moreno-López C, Santamaría J, Salamero M, Del Sorbo F, Albanese A, Pellecchia MT, Barone P, Overeem S, Bloem B, Aarden W. Excessive daytime sleepiness in multiple system atrophy (SLEEMSA study). Arch Neurol. 2011;68:223–30.
Ghorayeb I, Dupouy S, Tison F, Meissner WG. Restless legs syndrome in multiple system atrophy. J Neural Transm. 2014;121:1523–7.
Stefanova N, Bücke P, Duerr S, Wenning GK. Multiple system atrophy: an update. Lancet Neurol. 2009;8:1172–8.
Barone P, Antonini A, Colosimo C, Marconi R, Morgante L, Avarello TP, Bottacchi E, Cannas A, Ceravolo G, Ceravolo R. The PRIAMO study: a multicenter assessment of nonmotor symptoms and their impact on quality of life in Parkinson's disease. Movement disorders: official journal of the Movement Disorder Society. 2009;24:1641–9.
Maggi G, Trojano L, Barone P, Santangelo G. Sleep disorders and cognitive dysfunctions in Parkinson’s disease: a meta-analytic study. Neuropsychol Rev. 2021:1–40.
Biabani N, Birdseye A, Higgins S, Delogu A, Rosenzweig J, Cvetkovic Z, Nesbitt A, Drakatos P, Steier J, Kumari V, O'Regan D, Rosenzweig I. The neurophysiologic landscape of the sleep onset: a systematic review. J Thorac Dis. 2023;15:4530–43.
Tall P, Qamar MA, Rosenzweig I, Raeder V, Sauerbier A, Heidemarie Z, Falup-Pecurariu C, Chaudhuri KR. The park sleep subtype in Parkinson's disease: from concept to clinic. Expert Opin Pharmacother. 2023;24:1725–36. An updated outline of treatment strategies for improvement of disorders of sleep and wakefulness in PD patients.
Alrouji M, Al-Kuraishy HM, Al-Gareeb AI, Zaafar D, Batiha GE-S. Orexin pathway in Parkinson’s disease: a review. Mol Biol Rep. 2023;1–14. A comprehensive review of implicated orexinergic pathways in Parkinson's disease.
Ogawa T, Kajiyama Y, Ishido H, Chiba S, Revankar GS, Nakano T, Taniguchi S, Kanbayashi T, Ikenaka K, Mochizuki H. Decreased cerebrospinal fluid orexin levels not associated with clinical sleep disturbance in Parkinson’s disease: a retrospective study. PLoS One. 2022;17:e0279747. A retrospective study that demonstrated decreased CSF orexin levels in patients with PD, but without correlation to clinical characteristics.
Huang S, Zhao Z, Ma J, Hu S, Li L, Wang Z, Sun W, Shi X, Li M, Zheng J. Increased plasma orexin-a concentrations are associated with the non-motor symptoms in Parkinson’s disease patients. Neurosci Lett. 2021;741:135480.
Inagawa Y, Shimizu S, Takenoshita N, Tsugawa A, Hirose D, Kanbayashi T, Imanishi A, Sakurai H, Hanyu H, Kanetaka H. Association between cerebrospinal fluid orexin a level and severity of rapid eye movement sleep behaviour disorder in dementia with Lewy bodies. Psychogeriatrics: the official journal of the Japanese Psychogeriatric Society. 2021;21:128–30.
Al-Kuraishy HM, Abdulhadi MH, Hussien NR, Al-Niemi MS, Rasheed HA, Al-Gareeb AI. Involvement of orexinergic system in psychiatric and neurodegenerative disorders: a scoping review. Brain Circ. 2020;6:70.
De Lecea L, Sutcliffe J. The hypocretins/orexins: novel hypothalamic neuropeptides involved in different physiological systems. Cellular and Molecular Life Sciences CMLS. 1999;56:473–80.
Sakurai T, Amemiya A, Ishii M, Matsuzaki I, Chemelli RM, Tanaka H, Williams SC, Richardson JA, Kozlowski GP, Wilson S. Orexins and orexin receptors: a family of hypothalamic neuropeptides and G protein-coupled receptors that regulate feeding behavior. Cell. 1998;92:573–85.
Jin J, Chen Q, Qiao Q, Yang L, Xiong J, Xia J, Hu Z, Chen F. Orexin neurons in the lateral hypothalamus project to the medial prefrontal cortex with a rostro-caudal gradient. Neurosci Lett. 2016;621:9–14.
Xiao F, Jiang M, Du D, Xia C, Wang J, Cao Y, Shen L, Zhu D. Orexin a regulates cardiovascular responses in stress-induced hypertensive rats. Neuropharmacology. 2013;67:16–24.
Yamanaka A, Sakurai T, Katsumoto T, Yanagisawa M, Goto K. Chronic intracerebroventricular administration of orexin-a to rats increases food intake in daytime, but has no effect on body weight. Brain Res. 1999;849:248–52.
Aston-Jones G, Smith RJ, Sartor GC, Moorman DE, Massi L, Tahsili-Fahadan P, Richardson KA. Lateral hypothalamic orexin/hypocretin neurons: a role in reward-seeking and addiction. Brain Res. 2010;1314:74–90.
Holland PR. The orexins and their involvement in the modulation of trigeminovascular nociceptive transmission. University College London (United Kingdom): University of London; 2006.
Holland PR, Goadsby PJ. Cluster headache, hypothalamus, and orexin. Curr Pain Headache Rep. 2009;13:147–54.
Holland PR. Biology of neuropeptides: Orexinergic involvement in primary headache disorders. Headache: the Journal of Head and Face Pain. 2017;57:76–88.
Maski K, Mignot E, Plazzi G, Dauvilliers Y. Disrupted nighttime sleep and sleep instability in narcolepsy. J Clin Sleep Med. 2022;18:289–304.
Saper CB, Cano G, Scammell TE. Homeostatic, circadian, and emotional regulation of sleep. J Comp Neurol. 2005;493:92–8.
Li T-L, Lee Y-H, Wu F-H, Hwang L-L. Orexin-a directly depolarizes dorsomedial hypothalamic neurons, including those innervating the rostral ventrolateral medulla. Eur J Pharmacol. 2021;899:174033.
Schone C, Burdakov D. Orexin/Hypocretin and organizing principles for a diversity of wake-promoting neurons in the brain. Curr Top Behav Neurosci. 2017;33:51–74.
Pizza F, Barateau L, Dauvilliers Y, Plazzi G. The orexin story, sleep and sleep disturbances. J Sleep Res. 2022;31:e13665.
Diniz Behn CG, Klerman EB, Mochizuki T, Shih-Chieh L, Scammell TE. Abnormal sleep/wake dynamics in orexin knockout mice. Sleep. 2010;33:297–306.
Chemelli RM, Willie JT, Sinton CM, Elmquist JK, Scammell T, Lee C, Richardson JA, Williams SC, Xiong Y, Kisanuki Y. Narcolepsy in orexin knockout mice: molecular genetics of sleep regulation. Cell. 1999;98:437–51.
Broughton R, Valley V, Aguirre M, Roberts J, Suwalski W, Dunham W. Excessive daytime sleepiness and the pathophysiology of narcolepsy-cataplexy: a laboratory perspective. Sleep. 1986;9:205–15.
Barateau L, Lopez R, Chenini S, Rassu A-L, Scholz S, Lotierzo M, Cristol J-P, Jaussent I, Dauvilliers Y. Association of CSF orexin-a levels and nocturnal sleep stability in patients with hypersomnolence. Neurology. 2020;95:e2900–11.
Rissling I, Körner Y, Geller F, Stiasny-Kolster K, Oertel WH, Möller JC. Preprohypocretin polymorphisms in Parkinson disease patients reporting “sleep attacks”. Sleep. 2005;28:871–5.
Abdo W, Bloem B, Kremer H, Lammers G, Verbeek M, Overeem S. CSF hypocretin-1 levels are normal in multiple-system atrophy. Parkinsonism Relat Disord. 2008;14:342–4.
Martinez-Rodriguez JE, Seppi K, Cardozo A, Iranzo A, Stampfer-Kountchev M, Wenning G, Tolosa E, Högl B, Santamaria J, Poewe W. Cerebrospinal fluid hypocretin-1 levels in multiple system atrophy. Movement disorders: official journal of the Movement Disorder Society. 2007;22:1822–4.
Trotti LM, Bliwise DL, Keating GL, Rye DB, Hu WT. Cerebrospinal fluid hypocretin and nightmares in dementia syndromes. Dement Geriatr Cogn Disord Extra. 2021;11:19–25.
Anderson K, Vincent A, Smith I, Shneerson J. Cerebrospinal fluid hypocretin levels are normal in idiopathic REM sleep behaviour disorder. Eur J Neurol. 2010;17:1105–7.
Yuan Y, Zhang Y, Cheng Y, Hou Y, Huang Z, Ma J, Li N, Zhan S. Cerebrospinal fluid TNF-α and orexin in patients with Parkinson's disease and rapid eye movement sleep behavior disorder. Front Neurol. 2022;13:826013.
Takahashi Y, Kanbayashi T, Hoshikawa M, Imanishi A, Sagawa Y, Tsutsui K, Takeda Y, Kusanagi H, Nishino S, Shimizu T. Relationship of orexin (hypocretin) system and astrocyte activation in Parkinson’s disease with hypersomnolence. Sleep Biol Rhythms. 2015;13:252–60.
Lessig S, Ubhi K, Galasko D, Adame A, Pham E, Remidios K, Chang M, Hansen LA, Masliah E. Reduced hypocretin (orexin) levels in dementia with Lewy bodies. Neuroreport. 2010;21:756.
Moher D, Liberati A, Tetzlaff J, Altman DG, P. Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151:264–9.
Thomas B, Ciliska D, Dobbins M, Micucci S. A process for systematically reviewing the literature: providing the research evidence for public health nursing interventions. Worldviews Evid-Based Nurs. 2004;1:176–84.
Wienecke M, Werth E, Poryazova R, Baumann-Vogel H, Bassetti CL, Weller M, Waldvogel D, Storch A, Baumann CR. Progressive dopamine and hypocretin deficiencies in Parkinson’s disease: is there an impact on sleep and wakefulness? J Sleep Res. 2012;21:710–7.
Bridoux A, Moutereau S, Covali-Noroc A, Margarit L, Palfi S, Nguyen J-P, Lefaucheur J-P, Césaro P, d’Ortho M-P, Drouot X. Ventricular orexin-a (hypocretin-1) levels correlate with rapid-eye-movement sleep without atonia in Parkinson’s disease. Nat Sci Sleep. 2013:87–91.
Asai H, Hirano M, Furiya Y, Udaka F, Morikawa M, Kanbayashi T, Shimizu T, Ueno S. Cerebrospinal fluid-orexin levels and sleep attacks in four patients with Parkinson's disease. Clin Neurol Neurosurg 2009;111:341–4. A small study that was amongst first to suggest that orexin transmission is likely involved in sleep attacks in PD.
Compta Y, Santamaria J, Ratti L, Tolosa E, Iranzo A, Munoz E, Valldeoriola F, Casamitjana R, Ríos J, Marti MJ. Cerebrospinal hypocretin, daytime sleepiness and sleep architecture in Parkinson's disease dementia. Brain. 2009;132:3308–17.
Yasui K, Inoue Y, Kanbayashi T, Nomura T, Kusumi M, Nakashima K. CSF orexin levels of Parkinson's disease, dementia with Lewy bodies, progressive supranuclear palsy and corticobasal degeneration. J Neurol Sci. 2006;250:120–3.
Drouot X, Moutereau S, Nguyen J, Lefaucheur J, Creange A, Remy P, Goldenberg F, d’Ortho M. Low levels of ventricular CSF orexin/hypocretin in advanced PD. Neurology. 2003;61:540–3.
Afdal A, Indra S, Permana H. The relationship between plasma hypocretin levels and sleep disorders in patients with Parkinson's disease. Biosci Med: J Biomed Transl Res. 2021;5:856–61.
Baumann CR, Dauvilliers Y, Mignot E, Bassetti CL. Normal CSF hypocretin-1 (orexin A) levels in dementia with Lewy bodies associated with excessive daytime sleepiness. Eur Neurol. 2004;52:73–6.
A.A.o.S. Medicine. The international classification of sleep disorders:(ICSD-3). American Academy of Sleep Medicine; 2014.
Wasserman D, Bindman D, Nesbitt AD, Cash D, Milosevic M, Francis PT, Chaudhuri KR, Leschziner GD, Ferini-Strambi L, Ballard C. Striatal dopaminergic deficit and sleep in idiopathic rapid eye movement behaviour disorder: an explorative study. Nat Sci Sleep. 2021;1–9.
Wasserman D, Gullone S, Duncan I, Veronese M, Gnoni V, Higgins S, Birdseye A, Gelegen EC, Goadsby PJ, Ashkan K. Restricted truncal sagittal movements of rapid eye movement behaviour disorder. NPJ Parkinson's Disease. 2022;8:26.
Dauvilliers Y, Schenck CH, Postuma RB, Iranzo A, Luppi P-H, Plazzi G, Montplaisir J, Boeve B. REM sleep behaviour disorder. Nat Rev Dis Prim. 2018;4:19.
Boeve BF. REM sleep behavior disorder: updated review of the core features, the RBD-neurodegenerative disease association, evolving concepts, controversies, and future directions. Ann N Y Acad Sci. 2010;1184:15.
Fernández-Arcos A, Iranzo A, Serradell M, Gaig C, Santamaria J. The clinical phenotype of idiopathic rapid eye movement sleep behavior disorder at presentation: a study in 203 consecutive patients. Sleep. 2016;39:121–32.
Högl B, Stefani A, Videnovic A. Idiopathic REM sleep behaviour disorder and neurodegeneration—an update. Nat Rev Neurol. 2018;14:40–55.
Galbiati A, Verga L, Giora E, Zucconi M, Ferini-Strambi L. The risk of neurodegeneration in REM sleep behavior disorder: a systematic review and meta-analysis of longitudinal studies. Sleep Med Rev. 2019;43:37–46. A comprehensive review of
Boeve BF. Idiopathic REM sleep behaviour disorder in the development of Parkinson's disease. Lancet Neurol. 2013;12:469–82.
Chan P-C, Lee H-H, Hong C-T, Hu C-J, Wu D. REM sleep behavior disorder (RBD) in dementia with Lewy bodies (DLB). Behav Neurol. 2018;2018
Mahowald MW, Schenck CH. REM sleep behaviour disorder: a marker of synucleinopathy. Lancet Neurol. 2013;12:417–9.
Bloem BR, Okun MS, Klein C. Parkinson's disease. Lancet. 2021;397:2284–303.
Trist BG, Hare DJ, Double KL. Oxidative stress in the aging substantia nigra and the etiology of Parkinson's disease. Aging Cell. 2019;18:e13031.
Sveinbjornsdottir S. The clinical symptoms of Parkinson's disease. J Neurochem. 2016;139:318–24.
Gyorfi O, Nagy H, Bokor M, Moustafa AA, Rosenzweig I, Kelemen O, Keri S. Reduced CA2-CA3 hippocampal subfield volume is related to depression and normalized by l-DOPA in newly diagnosed Parkinson's disease. Front Neurol. 2017;8:84.
Amara AW, Chahine LM, Videnovic A. Treatment of sleep dysfunction in Parkinson’s disease. Curr Treat Options Neurol. 2017;19:1–16.
Videnovic A, Noble C, Reid KJ, Peng J, Turek FW, Marconi A, Rademaker AW, Simuni T, Zadikoff C, Zee PC. Circadian melatonin rhythm and excessive daytime sleepiness in Parkinson disease. JAMA Neurol. 2014;71:463–9.
Stevens S, Comella CL, Stepanski EJ. Daytime sleepiness and alertness in patients with Parkinson disease. Sleep. 2004;27:967–72.
Mantovani S, Smith SS, Gordon R, O'Sullivan JD. An overview of sleep and circadian dysfunction in Parkinson's disease. J Sleep Res. 2018;27:e12673.
Wasserman D, Gullone S, Duncan I, Veronese M, Gnoni V, Higgins S, Birdseye A, Gelegen EC, Goadsby PJ, Ashkan K, Ray Chaudhuri K, Tononi G, Drakatos P, Rosenzweig I. Restricted truncal sagittal movements of rapid eye movement behaviour disorder. NPJ Parkinsons Dis. 2022;8:26.
Schapira AH, Chaudhuri KR, Jenner P. Non-motor features of Parkinson disease. Nat Rev Neurosci. 2017;18:435–50.
Ray Chaudhuri K, Leta V, Bannister K, Brooks DJ, Svenningsson P. The noradrenergic subtype of Parkinson disease: from animal models to clinical practice. Nat Rev Neurol. 2023;1–13.
N. Non-tremor dominant Parkinson’s, the different syndromes in Parkinson’s disease: an overview. In: Genetics, neurology, behavior, and diet in Parkinson's disease: the neuroscience of Parkinson’s disease, vol. 2; 2020. p. 235.
Ballesio A, Zagaria A, Curti DG, Moran R, Goadsby PJ, Rosenzweig I, Lombardo C. Peripheral brain-derived neurotrophic factor (BDNF) in insomnia: a systematic review and meta-analysis. Sleep Med Rev. 2023;67:101738.
Ferini-Strambi L, Liguori C, Lucey BP, Mander BA, Spira AP, Videnovic A, Baumann C, Franco O, Fernandes M, Gnarra O, Krack P, Manconi M, Noain D, Saxena S, Kallweit U, Randerath W, Trenkwalder C, Rosenzweig I, Iranzo A, et al. Role of sleep in neurodegeneration: the consensus report of the 5th think tank world sleep forum. Neurol Sci. 2024;45:749–67.
Gelegen C, Cash D, Ilic K, Sander M, Kim E, Simmons C, Bernanos M, Lama J, Randall K, Brown JT, Kalanj-Bognar S, Cooke S, Ray Chaudhuri K, Ballard C, Francis P, Rosenzweig I. Relevance of sleep and associated structural changes in GBA1 mouse to human rapid eye movement behavior disorder. Sci Rep. 2022;12:7973.
Fronczek R, Overeem S, Lee SY, Hegeman IM, van Pelt J, van Duinen SG, Lammers GJ, Swaab DF. Hypocretin (orexin) loss in Parkinson's disease. Brain. 2007;130:1577–85.
Fan JK, Wang MC, Yang HM, Zhang JN, Gu L, Zhang H. α-Synuclein induced the occurrence of RBD via interaction with OX1R and modulated its degradation. NeuroMolecular Med. 2023:1–15.
Kok S, Meinders A, Overeem S, Lammers G, Roelfsema F, Frolich M, Pijl H. Reduction of plasma leptin levels and loss of its circadian rhythmicity in hypocretin (orexin)-deficient narcoleptic humans. J Clin Endocrinol Metab. 2002;87:805–9.
Gerashchenko D, Murillo-Rodriguez E, Lin L, Xu M, Hallett L, Nishino S, Mignot E, Shiromani PJ. Relationship between CSF hypocretin levels and hypocretin neuronal loss. Exp Neurol. 2003;184:1010–6.
Mignot E, Lammers GJ, Ripley B, Okun M, Nevsimalova S, Overeem S, Vankova J, Black J, Harsh J, Bassetti C. The role of cerebrospinal fluid hypocretin measurement in the diagnosis of narcolepsy and other hypersomnias. Arch Neurol. 2002;59:1553–62.
Zhan S, Che P, Zhao X k, Li N, Ding Y, Liu J, Li S, Ding K, Han L, Huang Z. Molecular mechanism of tumour necrosis factor alpha regulates hypocretin (orexin) expression, sleep and behaviour. J Cell Mol Med. 2019;23:6822–34.
Zupancic M, Mahajan A, Handa K. Dementia with Lewy bodies: diagnosis and management for primary care providers. Prim Care Companion CNS Disord. 2011;13:26212.
McKeith IG, Dickson DW, Lowe J, Emre M, O'brien J, Feldman H, Cummings J, Duda J, Lippa C, Perry E. Diagnosis and management of dementia with Lewy bodies: third report of the DLB consortium. Neurology. 2005;65:1863–72.
Thannickal TC, Lai Y-Y, Siegel JM. Hypocretin (orexin) cell loss in Parkinson's disease. Brain. 2007;130:1586–95.
Roy S, Lee V, Trojanowski J. Axonal transport and neurodegenerative diseases. Encyclopedia of Neuroscience. 2009;1:1199–203.
McKeith I, Perry E, Perry R. Report of the second dementia with Lewy body international workshop: diagnosis and treatment. Neurology. 1999;53:902–2.
Ahmed Z, Asi Y, Sailer A, Lees A, Houlden H, Revesz T, Holton J. The neuropathology, pathophysiology and genetics of multiple system atrophy. Neuropathol Appl Neurobiol. 2012;38:4–24.
Fanciulli A, Wenning GK. Multiple-system atrophy. N Engl J Med. 2015;372:249–63.
Ferini-Strambi L, Marelli S. Sleep dysfunction in multiple system atrophy. Curr Treat Options Neurol. 2012;14:464–73.
Benarroch EE, Schmeichel AM, Sandroni P, Low PA, Parisi JE. Involvement of hypocretin neurons in multiple system atrophy. Acta Neuropathol. 2007;113:75–80.
Liu M-F, Xue Y, Liu C, Liu Y-H, Diao H-L, Wang Y, Pan Y-P, Chen L. Orexin-a exerts neuroprotective effects via OX1R in Parkinson’s disease. Front Neurosci. 2018;12:835.
Liu C, Xue Y, Liu MF, Wang Y, Liu ZR, Diao HL, Chen L. Orexins increase the firing activity of nigral dopaminergic neurons and participate in motor control in rats. J Neurochem. 2018;147:380–94.
Feng Y, Liu T, Li X-Q, Liu Y, Zhu X-Y, Jankovic J, Pan T-H, Wu Y-C. Neuroprotection by orexin-a via HIF-1α induction in a cellular model of Parkinson's disease. Neurosci Lett. 2014;579:35–40.
Pasban-Aliabadi H, Esmaeili-Mahani S, Abbasnejad M. Orexin-a protects human neuroblastoma SH-SY5Y cells against 6-hydroxydopamine-induced neurotoxicity: involvement of PKC and PI3K signaling pathways. Rejuvenation Res. 2017;20:125–33.
Sheng Q, Xue Y, Wang Y, Chen A-Q, Liu C, Liu Y-H, Chu H-Y, Chen L. The subthalamic neurons are activated by both orexin-a and orexin-B. Neuroscience. 2018;369:97–108.
Bubser M, Fadel JR, Jackson LL, Meador-Woodruff JH, Jing D, Deutch AY. Dopaminergic regulation of orexin neurons. Eur J Neurosci. 2005;21:2993–3001.
Raheel K, Deegan G, Di Giulio I, Cash D, Ilic K, Gnoni V, Chaudhuri KR, Drakatos P, Moran R, Rosenzweig I. Sex differences in alpha-synucleinopathies: a systematic review. Front Neurol. 2023;14
Russillo MC, Andreozzi V, Erro R, Picillo M, Amboni M, Cuoco S, Barone P, Pellecchia MT. Sex differences in Parkinson’s disease: from bench to bedside. Brain Sci. 2022;12:917.
Jurado-Coronel JC, Cabezas R, Rodríguez MFÁ, Echeverria V, García-Segura LM, Barreto GE. Sex differences in Parkinson’s disease: features on clinical symptoms, treatment outcome, sexual hormones and genetics. Front Neuroendocrinol. 2018;50:18–30.
Czerwinska J, Chojnowska K, Kaminski T, Bogacka I, Smolinska N, Kaminska B. Orexin receptor expression in the hypothalamic–pituitary–adrenal and hypothalamic–pituitary–gonadal axes of free-living European beavers (Castor fiber L.) in different periods of the reproductive cycle. Gen Comp Endocrinol. 2017;240:103–13.
Saitoh T, Sakurai T. The present and future of synthetic orexin receptor agonists. Peptides. 2023;167:171051.
Author information
Authors and Affiliations
Contributions
KR and SQ selected, reviewed, and OI, BF, MLS and VM assessed all the eligible studies. All authors were involved in reviewing and drafting of the manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare the following competing financial interest(s): grants from Celgene and Kallyope, Massachusetts Medical Society, Oxford University Press, UptoDate and Wolters Kluwer (P.J.G); consulting fees from Aeon Biopharma, Abbvie, Amgen, CoolTech LLC, Epalex, Eli Lilly, Sanofi, Gerson Lehrman Group, Guidepoint, Linpharma, Lundbeck, Novartis, Pfizer, Vector Metric, SAI Med Partners, Satsuma, Shiratronics and Teva Pharmaceuticals (P.J.G). Grants from the Medical Research Council (MRC) (MR/P006264/1 and MR/N013700/1, PhD studentship for E.C.S and grant from Eli Lilly and Company (Eli Lilly Research Award Program (LRAP)) (P.H.). The advisory board for AbbVie, UCB, GKC, Bial Cynapsus, Lobsor, Stada, Zambon, Profile Pharma, Synovion, Roche, Therevance, Scion, Britannia, Acadia, 4D Pharma, receives grants from Bial, Britannia Pharmaceuticals, AbbVie, UCB, GKC, EU Horizon 2020, Parkinson's UK, NIHR, Parkinson’s Foundation, Wellcome Trust, Kirby Laing Foundation, MRC, MDS (MDS NMS Project), royalties or licenses from Oxford (book), Cambridge publishers (book), MAPI institute (KPPS, PDSS 2) and expert testimony from GMC, NICE, NIHR (K.R.C). Authors K.R., S.Q.R, V.M., B.F., O.I., M.L.S., C.M., A.D., S.L.N., L.P., I.R. have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Kausar Raheel, See Qi Rui, Veronica Munday, K Ray Chaudhuri, Ivana Rosenzweig as joint authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Raheel, K., See, Q.R., Munday, V. et al. Orexin and Sleep Disturbances in Alpha-Synucleinopathies: a Systematic Review. Curr Neurol Neurosci Rep 24, 389–412 (2024). https://doi.org/10.1007/s11910-024-01359-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11910-024-01359-6