Abstract
Purpose of the Review
Cancer therapy-related cardiac dysfunction (CTRCD) has been identified as a threat to overall and cancer-related survival. Although aerobic exercise training (AET) has been shown to improve cardiorespiratory fitness (CRF), the relationship between specific exercise regimens and cancer survival, heart failure development, and reduction of CTRCD is unclear. In this review, we discuss the impact of AET on molecular pathways and the current literature of sports in the field of cardio-oncology.
Recent Findings
Cardio-oncological exercise trials have focused on variations of AET intensity by using moderate continuous and high intensity interval training, which are applicable, safe, and effective approaches to improve CRF.
Summary
AET increases CRF, reduces cardiovascular morbidity and heart failure hospitalization and should thus be implemented as an adjunct to standard cancer therapy, although its long-term effect on CTRCD remains unknown. Despite modulating diverse molecular pathways, it remains unknown which exercise regimen, including variations of AET duration and frequency, is most suited to facilitate peripheral and central adaptations to exercise and improve survival in cancer patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cancer poses a major health and economic burden worldwide and warrants further improvement of diagnostic and treatment measures [1, 2]. Prognosis of cancer patients depends not only on adequate and timely diagnostics and treatment of cancer but also on handling of cardiovascular co-morbidities [3, 4]. Improvement or stabilizing of cardiorespiratory fitness (CRF), which is an independent predictor of cardiovascular events and mortality [5], has attracted much attention in recent years as a potential tool to interfere with cancer survival, cancer recurrence, as well as prevention and treatment of cardiovascular diseases associated with cancer and cancer therapy [6, 7]. A growing number of home-based and supervised exercise interventions, ranging from resistance training (RT) to aerobic exercise training (AET) in the form of either moderate continuous (MCT) or high intensity interval training (HIIT), have become available in clinical medicine and cardio-oncology. In this review we discuss the current literature on sports in cardio-oncology and the impact of AET on cardiovascular morbidity, heart failure hospitalization, and cancer therapy-related cardiac dysfunction (CTRCD). We further discuss molecular mechanisms associated with exercise-induced modification of cellular pathways. We comment on potential adaptations of training regimens to improve central and peripheral adaptations of exercise in cancer patients.
Definition of Cancer Therapy-Related Cardiac Dysfunction
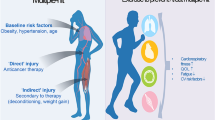
CTRCD is a descriptive term incorporating potential presentations of cancer patients including cardiac injury, heart failure, immune checkpoint inhibitor-related myocarditis, or cardiomyopathy [8]. CTRCD can be either asymptomatic or display symptoms of different severity (mild to very severe) [8]. Symptomatic CTRCD contains heart failure (HF) as a clinical syndrome consisting of cardinal clinical symptoms (e.g., breathlessness or fatigue) that may be accompanied by clinical signs of HF (e.g., peripheral oedema) and is divided into categories based on the measurement of left ventricular ejection fraction, LVEF (heart failure with reduced ejection fraction, HFrEF, LVEF ≤ 40%; heart failure with mildly reduced ejection fraction, HFmrEF, LVEF 41–49%; heart failure with preserved ejection fraction, HFpEF, LVEF ≥ 50%) [8,9,10]. Asymptomatic CTRCD requires an LVEF ≥ 50% and a new relative decline in global longitudinal strain (GLS) by > 15% from baseline and/or a new rise in cardiac biomarkers (defined as cardiac Troponin I or T above the 99th percentile, a BNP ≥ 35 pg/mL, an NT-proBNP ≥ 125 pg/mL, or a new significant rise from baseline beyond the biological and analytical variation of the assay used) [8]. Moderate, asymptomatic CTRCD refers to a new LVEF reduction by ≥ 10 percentage points to an LVEF of 40–49%, or a new LVEF reduction by < 10 percentage points to an LVEF of 40– 49% and either a new relative decline in GLS by > 15% from baseline, or a new rise in cardiac biomarkers, as defined above. Severe asymptomatic CTRCD is diagnosed if a new LVEF reduction to < 40% is observed [8].
Patients undergoing anthracycline-based (AC-based) chemotherapy and showing elevated cardiac troponin levels are more prone to developing CTRCD [11]. Likewise, a study on HER-2 positive breast cancer patients receiving trastuzumab demonstrated that 19% of patients who developed CTRCD during treatment displayed positive troponin levels at baseline, and troponin was a predictor of a lack of recovery despite optimized heart failure treatment [12]. Repetitive measurements of troponin during trastuzumab therapy revealed that increased baseline troponin was associated with a fourfold risk of left ventricular dysfunction [13]. However, it needs to be considered that baseline troponin in these studies represents pre-trastuzumab and post-AC therapy states. Thus, the impact of elevated baseline troponin levels in therapy-naïve breast cancer patients (before initiation of AC-based therapy) on the development of left ventricular dysfunction needs to be studied more deeply.
Cardiovascular Morbidity and Heart Failure in Cancer
A diagnosis of cancer has been independently associated with an enhanced risk of cardiovascular mortality, stroke, HF, and pulmonary embolism [14•, 15,16,17,18]. After a follow-up of more than 25 years breast cancer survivors of the CLUE II cohort displayed a significantly higher risk of death from cardiovascular disease compared to a cancer-free control group (HR = 1.65, CI = 1.00 to 2.73) [19]. On top of chemotherapy-induced cardiotoxicity, radiation therapy also predisposes to a higher prevalence of cardiovascular events [20].
Decline of LVEF often occurs within the first year of cancer treatment and has been acknowledged as a threat to long-term morbidity in patients undergoing cardiotoxic (e.g., AC-based) chemotherapy with or without overt signs of HF [8, 21,22,23]. This has led to early screening and surveillance protocols (for instance using the HFA-ICOS risk assessment tool) to identify high-risk patients [22, 24]. These protocols, derived from the definition of CTRCD, implement echocardiographic variables, such as GLS [25] and LVEF, as well as biomarkers, such as NTproBNP and troponin [8, 26,27,28]. Higher troponin levels have been associated with a fourfold risk of developing left ventricular (LV) dysfunction in breast cancer (BC) patients following AC-therapy [13]. There is conflicting data on the role of baseline troponin and NTproBNP on all-cause mortality across tumor entities [29, 30]. Variables of resting echocardiography have also demonstrated prognostic value in cancer patients. Increased baseline indexed left ventricular end-diastolic volume was shown to be a predictor of major cardiovascular events, defined as symptomatic HF or cardiac death, during AC-based chemotherapy in patients with preserved LVEF [31]. Baseline GLS can predict left ventricular dysfunction in patients receiving AC and/or trastuzumab [32, 33].
In breast cancer survivors (CS) the clinical incidence of HF has been estimated to be around 2%, while a subclinicial cardiac dysfunction following AC-based treatment was observed in 10% [34]. Extensive reviews demonstrated an incidence of HF of 5% if AC therapy was applied > 400 mg/m2 [35]. Early introduction of HF medication and meticulous follow-up in patients showing cardiotoxicity has shown potential to improve LVEF [23, 36, 37], although decreased LVEF, pulmonary hypertension, enlarged left ventricular size, and anemia were shown to be negative long-term prognosticators [38]. If untreated, early-onset, progressive AC-based cardiotoxicity was shown to have comparable cardiovascular mortality to idiopathic dilated cardiomyopathy (IDCM) with an LVEF < 50% (overall survival rates at 5 and 10 years: cancer patients 86% and 61% and IDCM 88% and 75%; p = 0.61) [39] and was demonstrated to be dose-dependent [40].
Impact of Cardiorespiratory Fitness on Cancer
Higher cardiorespiratory fitness (CRF), which is usually expressed through peak oxygen consumption (VO2peak), has been associated with lower cancer incidence [41] and better survival in large cohorts of cancer patients [6, 42]. The risk of cardiovascular disease-related mortality in CS is reduced by 14% per 1 metabolic equivalent (3.5 ml O2/kg/min) increase in CRF [43•]. In a single-center study of adult-onset cancer patients with a median follow-up of almost five years, higher CRF was an independent predictor of overall, cancer-related, and cardiovascular mortality [43•]. Higher (self-reported) CRF prior to cancer diagnosis was associated with a graded reduction on cardiovascular events in a large prospective study with long-term breast CS [44]. Late cardiac effects of AC-based therapy were prospectively investigated in female breast cancer patients without cardiovascular risk factors: Physically active individuals reported less symptoms of HF compared to sedentary controls after 5 years [45].
The ability of exercise intervention to prevent CTRCD, as it is defined currently, is less clear. In a meta-analysis, eight studies were analyzed in which LVEF and GLS were measured prior and after chemotherapy in BC patients [46]. GLS and LVEF did not differ between groups with or without exercise. CTRCD incidence was only reported in two out of eight trials [47, 48], with two cumulative patients in the UC groups diagnosed with CTRCD. It has been suggested that the reason for the lack of CTRCD prevention through exercise are short follow-ups, the heterogeneity of applied exercise protocols, some of which were not based on cardiopulmonary exercise testing (CPET), and the failure to adequately phenotype patients [49, 50•]. Exercise prescriptions were largely generic and based on predicted maximal heart rate, which may be insufficient to characterize adequate training corridors in patients on [51] and off [52] drug therapy.
Exercise Interventions in Cancer Patients
The gold standard to determine training corridors for structured, individualized exercise training in healthy individuals is CPET [53,54,55]. In oncology, CPET has primarily been used to conduct pre-operative risk stratification in colon [56], rectal [57], and lung cancer [58], but not as a standard to design training intensity for exercise trials. Recommendations for exercise prescriptions in cancer patients have already been published using the subjective BORG scale [59], percentage of VO2peak, percentage of peak heart rate, or blood lactate levels as approaches to determine training corridors for exercise intensity [49, 60, 61]. Although formulae to predict peak heart rate [62] and VO2peak [63] have been suggested, individual exercise testing prior to training is the most accurate approach and mandatory to improve (the lack of) comparability of trials in sports cardio-oncology. Apart from VO2peak, which is exertion-dependent, application of submaximal CPET variables, such as the oxygen equivalent at the first ventilatory threshold (VT1), or percentage of VO2peak at VT1, may bear the potential to prescribe exercise intensities without the need for maximal exertion and may reduce adverse events during strenuous exercise [55, 64, 65•]. This, however, needs to be further studied in a cancer population.
The methodological heterogeneity of exercise trials in sports cardio-oncology is demonstrated by one of the first retrospective, exploratory trials (a sub-analysis of the HF-ACTION trial with LVEF ≤ 35%) to investigate AET (three supervised sessions/week, 60–70% of heart rate reserve, HRR, for 20–45 min) in cancer, which found cardiovascular mortality or HF hospitalization to be higher in AET after a median follow-up of 35 months (41 vs 67%, adjusted HR 1.94, CI 1.12–3.16, p = 0.017) [66], while VO2peak did not differ compared to usual care (UC, p = 0.710). This intention-to-treat analysis was not powered for the primary endpoint and information on anticancer therapy, cancer stage, and type were not collected. These (hypothesis-generating) results were refuted by several trials showing a beneficial effect of physical activity (PA = unstructured activity vs. structured AET) on mortality: A meta-analysis of 16 exercise trials on breast and colon cancer survivors demonstrated a reduced mortality rate if patients increased their PA from pre-to post-diagnosis (RR = 0.61; CI = 0.46–0.80).
There is a large body of data supporting an increase of CRF through AET in randomized controlled trials in cancer patients after chemotherapy [67, 68], while mitigation of chemotherapy-induced reduction of VO2peak has been demonstrated in high-volume AET as opposed to UC (2.5 ml/kg/min vs. 3.4 ml/kg/min) without significant side effects [69], and may even lead to an increase of VO2peak during chemotherapy in patients with subclinical signs of cardiotoxicity [70]. Another study in breast cancer patients demonstrated a significant benefit of CRF and quality of life after a 16-week high intensity exercise intervention (AET or RT) during chemotherapy compared to UC [71]. These results were confirmed in a multi-center trial in early-stage BC patients on AC-based chemotherapy showing an increase of the secondary endpoint VO2peak at the end of chemotherapy (+ 1.6 ml/kg/min, p = 0.041) and after 3 months (+ 3.1 ml/kg/min, p < 0.001) with combined AET and RT compared to UC [50•]. However, there was no difference for the primary endpoint change in LVEF at the end of chemotherapy (0.7%, p = 0.349) and 3-month follow-up (1.1, p = 0.196), or the secondary endpoint GLS (− 0.3, p = 0.500 and − 1.0, p = 095), which may either suggest that follow-up was too short, or that functional rather than echocardiographic variables may better represent early onset cardiotoxicity; this clearly needs further investigations.
The Brexit trial, the cancer exercise study with the longest follow-up period so far, demonstrated a lower percentage of “functional disability,” defined as VO2peak ≤ 18 ml/kg/min (12 vs. 36%) after a 12 months follow-up in an exercise training group consisting of combined supervised and home-based AET (including MCT and HIIT elements) and RT, compared to UC. The training group displayed a 9% improvement of VO2peak compared to a 7% decline in UC [65•]. Exercise did not influence resting LVEF, but improved left and right ventricular ejection fraction reserve and stroke volume and led to a lower increase of post-chemo troponin compared to UC. A tremendous and clinically relevant net increase of 3.5 ml/kg/min of VO2peak in the AET group raises the question whether current definitions of CTRCD, which are based on resting and laboratory markers, should be enriched by functional exercise variables to better risk stratify cancer patients. This trial also suggests a combination of MCT and HIIT in a non-linear training model combining effects on VO2peak; clearly, this needs further investigation in a long-term follow-up.
Apart from improvement of CRF (VO2peak), AET was shown to mitigate cardiovascular risk factors, such as sarcopenic obesity [72] and inflammatory markers [73] in breast CS, cholesterol profile in prostate cancer [74, 75] and survivors of childhood cancer [76], as well as endothelial function in breast and prostate cancer survivors [77, 78]. Structured pre-operative AET also seems to reduce post-operative complications and length of hospital stay [79] and facilitates efficacy of cancer therapy [80].
Recurrence and mortality of cancer were reduced following a 6-month exercise trial after colon cancer surgery [81]. Although heterogeneity of study designs were reported, similar results were gained in a meta-analysis of eight randomized controlled exercise trials in cancer patients showing a reduced risk of cancer recurrence in exercising individuals and a lower risk of mortality [82].
In breast cancer patients exercise training has shown positive effects on CRF and reduction of cancer-related symptoms in patients before initiation of chemotherapy [45]. Likewise, exercise can modulate angiogenic factors and tumor biology during neoadjuvant therapy, which may have positive effects on treatment response [83]. Exercise training is safe during chemotherapy [48, 69] and can even improve CRF during this period [50•]. Several studies demonstrated positive effects of exercise on CRF, cardiovascular events, and survival after adjuvant chemotherapy [65•, 68, 84, 85]. Exercise training also demonstrated reduction of arthralgia induced by aromatase inhibitors during maintenance therapy [86]. Professional support in cancer rehabilitation is of pivotal importance as structured and personalized exercise rehabilitation training in breast cancer survivors reduces fatigue and fatigue-related biomarkers [87], and can also improve social and physical function [88]. Taken together, evidence for the beneficial effects of exercise on patients’ well-being and CRF have been demonstrated across the whole temporal continuum of cancer treatment and should induce integration of exercise as a main pillar of standard-cancer therapy [89]. Future trials will also provide more insights on the effects of structured, individualized exercise to improve quality of life and fatigue in more advanced cancer stages, such as metastatic breast cancer [90].
Muscle wasting and sarcopenia is a major problem in cancer patients and contributes to a reduction of CRF and survival [91,92,93]. Resistance training (RT), as a measure to reduce or even reverse muscle wasting, is recommended in addition to endurance training to improve CRF by current guidelines of sports cardiology and cardio-oncology [8, 94] as it improves skeletal muscle and mitochondrial respiration [95]. Assessment of muscle strength in cancer patients is usually performed by measuring handgrip strength [96], and RT intensity to establish training prescriptions should be identified by the one repetition maximum (1 RPM) [89, 94]. A meta-analysis of randomized trials of RT during and after chemotherapy in cancer survivors demonstrated the most effective increase of muscle strength at intensities below 75% of 1 RPM [97] and provides evidence for a safe integration of RT into training of cancer patients.
Recent trials used combined AET and RT to demonstrate improvement of CRF in patients during and after chemotherapy [50•, 65•, 98], but did not include frail and sarcopenic patients [96, 99]. Future exercise studies in cancer patients need to take this into account and should also enroll sarcopenic cancer patients who should be trained with combined RT and AET and additional structured nutritional advice. Trials are warranted to gain data on which RT intensity before, during, and after chemotherapy is most suitable to improve muscular strength and antagonize sarcopenia and muscle wasting. Following principles of exercise sciences, variations of exercise intensity, duration, and frequency should be applied in cancer patients. Repetitive re-assessments of training corridors throughout the treatment periods should be implemented for both AET and RT (a prospective design for exercise intervention has been suggested by our group, [89]). As exercise interventions in trials of sports cardio-oncology are heterogeneous, exercise prescriptions should be based on objective measures gained by repetitive cardiopulmonary exercise testing and handgrip strength assessment. Repetitive testing is of pivotal importance, since drug therapy may change throughout the treatment cycles, which may affect cardiopulmonary response to exercise and alter pre-defined training corridors (e.g., the implementation of beta-blockers to treat left ventricular dysfunction and heart failure). Analogous to cardiac sports groups, cancer patients should primarily receive supervised training in the form of “cancer sports groups,” which should be enacted by trained personnel. These training sessions may be performed in specialized facilities, or even within hospitals, depending on the patients` health status and extent of functional disability. Prescriptions of exercise should be done by professional exercise scientists in close cooperation with the treating physicians. Supervised training should be preferred as it may be more effective and safer compared to home-based training. However, in less compromised patients, the advent of telemonitoring and app-based solutions may bear the potential to improve home-based training with maintenance of adequate exercise monitoring. Future trials of sports cardio-oncology should make use of this digital progress [89].
Variation of Exercise Intensity: HIIT Vs. MCT
Variations of exercise intensity are established approaches to increase exercise performance, but data on the net benefit of MCT versus HIIT is conflicting. In healthy individuals a meta-analysis of 28 trials demonstrated a greater improvement of VO2peak in HIIT compared to MCT [100]. HIIT was introduced in the form of the “Norwegian model” into cardiological trials by comparing post-infarct HFrEF patients under optimal medical therapy into an MCT (70% of peak heart rate), HIIT (95% of peak heart rate, 4 × 4 min, 3x/week for 12 weeks), or UC group [101]. HIIT outperformed MCT in changes of VO2peak, LV diameters, LVEF, NTproBNP, and surrogate markers for mitochondrial and endothelial function [101]. These results were not confirmed in a larger randomized trial of patients with LVEF ≤ 35%, in which almost half of the patients did not adhere to the recommended training corridors [102]. Although a cohort of patients with HF and HFpEF displayed no differences in VO2peak improvement between MCT and HIIT [103], a meta-analysis of three RCT HFpEF trials recently demonstrated a benefit for HIIT [104]. When comparing isocaloric HFrEF studies, MCT and HIIT did not differ in VO2peak [105] or LVEF improvement at rest [106].
A meta-analysis of 12 studies with cancer patients and survivors compared CPET data after exercise intervention and found no differences of VO2peak between MCT and HIIT, both being superior to UC [107]. However, heterogeneity of included trials and lack of objective pre-intervention CPET data limit this study`s generalizability. Compared to UC, HIIT proved to be superior to improve VO2peak and cardiovascular risk factors, such as LDL-cholesterol or arterial stiffness, in different types of cancer [108, 109]. HIIT was also shown to modulate sympathetic tone [110], which may be a driving mechanism to develop HF in cancer. Apart from VO2peak improvement, positive effects of HIIT on quality of life have been described in cancer patients and CS [71, 111], but more data needs to be acquired on long-term safety and whether HIIT, as a time-sparing alternative or complementary approach, is better suited than MCT to facilitate chemotherapeutic response through decrease of tissue hypoxia [112].
Although pre-clinical and clinical trials on exercise have been published to mitigate cardiotoxic effects of cancer therapy, improve CRF, and reduce overall mortality [113], the protective molecular mechanisms of exercise leading to peripheral and central adaptations have not been entirely elucidated. Extracardiac contributions to the increase of VO2peak depending on specific exercise regimens have not been sufficiently elucidated in exercise trials of cancer patients. Deeper knowledge of molecular processes of different exercise regimens in cancer patients would facilitate designing more targeted training strategies.
Molecular Biology of Exercise Regimens
Exercise has been suggested as cardiovascular therapy more than 2 decades ago [114] and knowledge on macroscopic and microscopic adaptations to training has increased since then, with beneficial effects on organ, vascular, and cellular structures and processes (for an overview see Fig. 1).
Impact of exercise training on macroscopic and microscopic structures and processes. Oxygen, which is transported along the upper and lower respiratory tract, diffuses into the vascular system and is delivered to the peripheral working musculature, where it is extracted from cells. Determinants of cardiac output, the driver of circulation, are stroke volume and heart rate increase during exercise. The amount of intracelluar oxygen uptake depends on arterial oxygen content, which is a function of partial pressure of oxygen (paO2), oxygen saturation and hemoglobin levels, as well as endothelial function, which is, among others, regulated by endothelial nitric oxide-synthase (eNOS) and crosstalk with microRNA. Paracrine mediators between muscle cells (myo- and mitokines) and nerval modulation at the neuromuscular junction modulate intracellular downstream signaling. A balance between reactive oxygen species (ROS), programmed cell death and protein degradation (ubiquitination) as well as hypertrophy mediated through the phosphoinositid-3-kinase/Akt cascade (PI3K/Akt) is achieved through structured exercise training leading to physiological myocardial remodeling in the form of the athletic heart. Modulation of calcium sensitivity through regulation of membrane-bound Na+/Ca2+-exchanger, sarcoplasmic/endoplasmic reticulum Ca2+- ATPase (SERCA) and phospholamban is another mechanism to optimize myocardial actin-myosin interaction. Upregulation of mitochondrial and respiratory chain enzymes lead to more effective aerobic energy disposal. Partial renewal of myocardial cells via stem cell proliferation can also be triggered through increased workload. Created with Biorender.com
A major problem of cancer is cardiac and muscle wasting [115]. Balance between cell growth (also as a driver of cancerogenesis) and atrophy is maintained through the ubiquitin–proteasome system (UPS) [116] and myostatin-signaling [117], as well as auto- and mitophagy [118,119,120]. MCT has been shown to counteract muscle wasting in a heart failure animal model [121] and in humans [122] by reducing muscle ring finger 1 (Mu-RF1) expression, which is involved in skeletal muscle wasting. After 12 weeks of MCT, a significant reduction in myostatin expression in 24 HF patients was observed compared to UC [123]. MCT has also been shown to stimulate IGF-1, which triggers phosphoinositid-3-kinase (PI3K) and Akt expression leading to (physiological) myocardial hypertrophy [124], while this pathway may be inhibited through exercise in certain cancer cells [125, 126].
Reactive oxygen species (ROS), which can be triggered by increased expression of NADPH and xanthine oxidase leading to myofibrillar damage [127], is another mechanism to drive exercise intolerance: MCT proved to decrease the amount of nitrotyrosine and carbonylated proteins, thus reducing ROS load on muscular cells [128]. MCT can also induce modification of microRNA, which is involved in cellular morphogenesis, antifibrotic metabolism, inflammation, and cell death, which has been identified to preserve cell integrity [129]. Facilitation of paracrine signaling [130], NO-synthase [131], and neuromuscular transmission [132], as well as an increase of mitochondrial density [133], can be achieved through MCT. AET (MCT and HIIT) also leads to increased activity of mitochondrial and respiratory chain enzymes through activation of peroxisome proliferator-activated receptor-gamma coactivator-1 protein-alpha (PGC-1α) and may be downregulated by cancer cells [80, 115, 118, 134,135,136,137]. There is conflicting data whether facilitation of endothelial NO synthase (eNOS), as a surrogate to increase endothelial function, is best achieved through HIIT or MCT [101, 138].
HF leads to reduced Ca2+- uptake into the sarcoplasmatic reticulum due to diminished activity of sarco/endoplasmatic reticulum Ca2+ -ATPase (SERCA) [139], which may also be one mechanism of cancer-related exercise intolerance [118]. HIIT has been shown to increase expression of Na/Ca2+ exchanger [140] and triggers hyperphosphorylation of phospholamban [141] leading to improved contractility of cardiomyocytes. Formation of new, functional cells through exercise may also be a mechanism, which could enhance exercise tolerance in cancer patients: Wistar rats exercising with MCT (55–60% of VO2peak) and HIIT (85–90% of VO2peak) for 30 min/day, 4 days/week, and for 4 weeks both displayed significantly increased newly formed cardiomyocytes compared to sedentary controls, with the highest number gained in HIIT [142].
In summary, both HIIT and MCT interact with multiple pathways leading to improved central and peripheral adaptations to exercise. Taking advantage of such exercise-induced effects without fostering cancer growth will be one major task of future trials of sports cardio-oncology.
Exercise Volume as a Function of Intensity, Frequency, and Duration: Significance for Planning Future Exercise Trials in the Cancer Population
Like in healthy individuals, a minimal amount of exercise volume must be applied in cancer patients to improve CRF [8, 94, 143]. Current clinical exercise trials have focused on examining variations of exercise intensity (HIIT vs. MCT) with relatively constant exercise duration (30–45 min) and frequency (3 × /week) [144, 145]; the impact of the latter two on exercise volume, which is the product of intensity, duration, and frequency, remains to be determined. Scarce data in humans is available for mitochondrial adaptations to exercise by increasing frequency and duration [144]. The most appropriate exercise regimen to improve capillary density (and reduce potential tumor-associated hypoxia in cancer patients) in skeletal muscles of humans has not been determined [144].
An exercise regimen, which has not been investigated in the cancer population, is low-volume sprint interval training (SIT), which requires less total work to complete relative to MCT and HIIT and is performed at intensities close to VO2peak [146]. Similar to HIIT, SIT is better able to upregulate mitochondrial density (mediated through AMPK and p38 MAPK phosphorylation and PGC-1α increase) [147] and content (measured by activity of citrate synthase) [148] after each training session relative to MCT.
Current evidence in healthy subjects suggests that improvement of VO2peak is rather gained through preservation of intensity (with preferably longer bouts) than duration or frequency [149], but data is lacking in cancer patients. In healthy subjects, increase of VO2peak has been primarily attributed to increases of stroke volume after up to 6 weeks of training rather than by enhancing arteriovenous O2 difference [150]. There is an urgent need to investigate additional mechanisms of central and peripheral adaptations in exercising cancer patients with overt or occult cardiotoxicity and co-existing HF medication to treat CTRCD. For clinical practice, the benefits and exercise-limitations of drugs limiting cardiac output (such as beta-blockers) have to be weighed carefully in cancer patients in the absence of clear indications, such as reduced LVEF, or a history of myocardial infarction. This should be regarded similarly to treating “normal” HFpEF patients, for whom beta-blockers have been shown to display severe exercise limitations [10, 151, 152].
In summary, an array of molecular adaptations have been demonstrated in different exercise regimens in healthy, cancer, and HF patients [145, 153], some of which are antagonized by cancer cells [83]. The diverse molecular response to exercise regimens suggests that AET (MCT, HIIT, and low-volume SIT) exerts its effects on multiple complementary pathways, which differ from established single-pathway inhibition of standard cancer therapy and may qualify exercise as a “pleiotropic drug” in cardio-oncological therapy. However, finding the most appropriate training regimen to reduce the risk for cardiotoxicity and CTRCD and eventually prognosis of cancer patients will require both further clinical and molecular studies in exercise sciences. It should also be critically discussed whether the definition of CTRCD, which entirely depends on resting measurements, should be enriched by functional (at best CPET) data to better risk stratify cancer patients. Studies should not only be performed to investigate hard clinical endpoints but also should be designed to include analysis of exercise-induced molecular changes on and off chemotherapy as well as during different cycles of exercise training to better understand the pathophysiology of CTRCD and beneficial effects of exercise. As cancer and HF-induced catabolism is a major concern, training should always integrate RT and nutritional protocols to foster protein synthesis accordingly. Importantly, exercise interventions, including MCT, HIIT, and SIT must follow principles of exercise sciences using CPET as a gold standard for testing, instead of estimating exercise intensity from predicted peak heart rate. By doing this, heterogeneity of trials in sports cardio-oncology will be reduced.
Conclusion
Physical inactivity is not only a risk factor to develop cancer but is also a predictor for HF and cardiovascular death [154]. Exercise interventions, both AET (MCT and HIIT) and RT, during chemotherapy have been shown to be safe and applicable [155, 156] and have the potential to improve CRF and prevent development of long-term HF [97, 157, 158] by affecting multiple molecular pathways. This should trigger the implementation of exercise training as an adjunct to standard cancer-related therapy in the form of cardio-oncological rehabilitation, which is not generally available despite “guideline recommendations” [8, 159,160,161,162]. More exercise trials are needed to elucidate the most appropriate training regimen to prevent and antagonize CTRCD, whose definition may require revision in the future to incorporate additional functional variables.
Data Availability
We did not perform analysis of original data. All information is included in this manuscript.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance
Siegel RL, Miller KD, Fuchs HE, Jemal A. Cancer statistics, 2022. CA Cancer J Clin. 2022;72(1):7–33. https://doi.org/10.3322/caac.21708.
WHO: Cancer Key Facts. https://www.who.int/news-room/fact-sheets/detail/cancer (2022). Accessed 29 Mar 2024.
Finke D, Heckmann MB, Wilhelm S, Entenmann L, Hund H, Bougatf N, et al. Coronary artery disease, left ventricular function and cardiac biomarkers determine all-cause mortality in cancer patients-a large monocenter cohort study. Clin Res Cardiol. 2023;112(2):203–14. https://doi.org/10.1007/s00392-022-02001-6.
Hurria A, Jones L, Muss HB. Cancer treatment as an accelerated aging process: assessment, biomarkers, and interventions. Am Soc Clin Oncol Educ Book. 2016;35:e516–22. https://doi.org/10.1200/edbk_156160.
Kodama S, Saito K, Tanaka S, Maki M, Yachi Y, Asumi M, et al. Cardiorespiratory fitness as a quantitative predictor of all-cause mortality and cardiovascular events in healthy men and women: a meta-analysis. JAMA. 2009;301(19):2024–35. https://doi.org/10.1001/jama.2009.681.
Lahart IM, Metsios GS, Nevill AM, Carmichael AR. Physical activity, risk of death and recurrence in breast cancer survivors: a systematic review and meta-analysis of epidemiological studies. Acta Oncol. 2015;54(5):635–54. https://doi.org/10.3109/0284186x.2014.998275.
Zheng C, Beresford SA, Van Horn L, Tinker LF, Thomson CA, Neuhouser ML, et al. Simultaneous association of total energy consumption and activity-related energy expenditure with risks of cardiovascular disease, cancer, and diabetes among postmenopausal women. Am J Epidemiol. 2014;180(5):526–35. https://doi.org/10.1093/aje/kwu152.
Lyon AR, López-Fernández T, Couch LS, Asteggiano R, Aznar MC, Bergler-Klein J, et al. 2022 ESC Guidelines on cardio-oncology developed in collaboration with the European Hematology Association (EHA), the European Society for Therapeutic Radiology and Oncology (ESTRO) and the International Cardio-Oncology Society (IC-OS). Eur Heart J. 2022;43(41):4229–361. https://doi.org/10.1093/eurheartj/ehac244.
McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, Böhm M, et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J. 2021;42(36):3599–726. https://doi.org/10.1093/eurheartj/ehab368.
McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, Böhm M, et al. 2023 Focused Update of the 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J. 2023;44(37):3627–39. https://doi.org/10.1093/eurheartj/ehad195.
Xue K, Gu JJ, Zhang Q, Liu X, Wang J, Li XQ, et al. Cardiotoxicity as indicated by LVEF and troponin T sensitivity following two anthracycline-based regimens in lymphoma: Results from a randomized prospective clinical trial. Oncotarget. 2016;7(22):32519–31. https://doi.org/10.18632/oncotarget.8685.
Cardinale D, Colombo A, Torrisi R, Sandri MT, Civelli M, Salvatici M, et al. Trastuzumab-induced cardiotoxicity: clinical and prognostic implications of troponin I evaluation. J Clin Oncol. 2010;28(25):3910–6. https://doi.org/10.1200/jco.2009.27.3615.
Zardavas D, Suter TM, Van Veldhuisen DJ, Steinseifer J, Noe J, Lauer S, et al. Role of troponins I and T and N-terminal prohormone of brain natriuretic peptide in monitoring cardiac safety of patients with early-stage human epidermal growth factor receptor 2-positive breast cancer receiving trastuzumab: a herceptin adjuvant study cardiac marker substudy. J Clin Oncol. 2017;35(8):878–84. https://doi.org/10.1200/jco.2015.65.7916.
Paterson DI, Wiebe N, Cheung WY, Mackey JR, Pituskin E, Reiman A, et al. Incident cardiovascular disease among adults with cancer: a population-based cohort study. JACC CardioOncol. 2022;4(1):85–94. https://doi.org/10.1016/j.jaccao.2022.01.100. This large study illustrates that a diagnosis of cancer is independently associated with increased risk for cardiovascular death.
Totzeck M, Mincu RI, Heusch G, Rassaf T. Heart failure from cancer therapy: can we prevent it? ESC Heart Fail. 2019;6(4):856–62. https://doi.org/10.1002/ehf2.12493.
Totzeck M, Mincu RI, Mrotzek S, Schadendorf D, Rassaf T. Cardiovascular diseases in patients receiving small molecules with anti-vascular endothelial growth factor activity: a meta-analysis of approximately 29,000 cancer patients. Eur J Prev Cardiol. 2018;25(5):482–94. https://doi.org/10.1177/2047487318755193.
Totzeck M, Mincu RI, Rassaf T. Cardiovascular adverse events in patients with cancer treated with bevacizumab: a meta-analysis of more than 20 000 patients. J Am Heart Assoc. 2017;6(8). https://doi.org/10.1161/jaha.117.006278.
Totzeck M, Schuler M, Stuschke M, Heusch G, Rassaf T. Cardio-oncology - strategies for management of cancer-therapy related cardiovascular disease. Int J Cardiol. 2019;280:163–75. https://doi.org/10.1016/j.ijcard.2019.01.038.
Ramin C, Schaeffer ML, Zheng Z, Connor AE, Hoffman-Bolton J, Lau B, et al. All-cause and cardiovascular disease mortality among breast cancer survivors in CLUE II, a long-standing community-based cohort. J Natl Cancer Inst. 2021;113(2):137–45. https://doi.org/10.1093/jnci/djaa096.
Santoro F, Tarantino N, Pellegrino PL, Caivano M, Lopizzo A, Di Biase M, et al. Cardiovascular sequelae of radiation therapy. Clin Res Cardiol. 2014;103(12):955–67. https://doi.org/10.1007/s00392-014-0718-y.
Armenian SH, Lacchetti C, Barac A, Carver J, Constine LS, Denduluri N, et al. Prevention and monitoring of cardiac dysfunction in survivors of adult cancers: American Society of Clinical Oncology Clinical Practice Guideline. J Clin Oncol. 2017;35(8):893–911. https://doi.org/10.1200/jco.2016.70.5400.
Bloom MW, Hamo CE, Cardinale D, Ky B, Nohria A, Baer L, et al. Cancer therapy-related cardiac dysfunction and heart failure: Part 1: definitions, pathophysiology, risk factors, and imaging. Circ Heart Fail. 2016;9(1):e002661. https://doi.org/10.1161/circheartfailure.115.002661.
Cardinale D, Colombo A, Bacchiani G, Tedeschi I, Meroni CA, Veglia F, et al. Early detection of anthracycline cardiotoxicity and improvement with heart failure therapy. Circulation. 2015;131(22):1981–8. https://doi.org/10.1161/circulationaha.114.013777.
Zamorano JL, Lancellotti P, Rodriguez Muñoz D, Aboyans V, Asteggiano R, Galderisi M, et al. 2016 ESC Position Paper on cancer treatments and cardiovascular toxicity developed under the auspices of the ESC Committee for Practice Guidelines: The Task Force for cancer treatments and cardiovascular toxicity of the European Society of Cardiology (ESC). Eur Heart J. 2016;37(36):2768–801. https://doi.org/10.1093/eurheartj/ehw211.
Laufer-Perl M, Arnold JH, Mor L, Amrami N, Derakhshesh M, Moshkovits Y, et al. The association of reduced global longitudinal strain with cancer therapy-related cardiac dysfunction among patients receiving cancer therapy. Clin Res Cardiol. 2020;109(2):255–62. https://doi.org/10.1007/s00392-019-01508-9.
Michel L, Mincu RI, Mahabadi AA, Settelmeier S, Al-Rashid F, Rassaf T, et al. Troponins and brain natriuretic peptides for the prediction of cardiotoxicity in cancer patients: a meta-analysis. Eur J Heart Fail. 2020;22(2):350–61. https://doi.org/10.1002/ejhf.1631.
Michel L, Mincu RI, Mrotzek SM, Korste S, Neudorf U, Rassaf T, et al. Cardiac biomarkers for the detection of cardiotoxicity in childhood cancer-a meta-analysis. ESC Heart Fail. 2020;7(2):423–33. https://doi.org/10.1002/ehf2.12589.
Michel L, Rassaf T, Totzeck M. Biomarkers for the detection of apparent and subclinical cancer therapy-related cardiotoxicity. J Thorac Dis. 2018;10(Suppl 35):S4282-s95. https://doi.org/10.21037/jtd.2018.08.15.
Pavo N, Raderer M, Hülsmann M, Neuhold S, Adlbrecht C, Strunk G, et al. Cardiovascular biomarkers in patients with cancer and their association with all-cause mortality. Heart. 2015;101(23):1874–80. https://doi.org/10.1136/heartjnl-2015-307848.
López-Sendón J, Álvarez-Ortega C, Zamora Auñon P, Buño Soto A, Lyon AR, Farmakis D, et al. Classification, prevalence, and outcomes of anticancer therapy-induced cardiotoxicity: the CARDIOTOX registry. Eur Heart J. 2020;41(18):1720–9. https://doi.org/10.1093/eurheartj/ehaa006.
Mousavi N, Tan TC, Ali M, Halpern EF, Wang L, Scherrer-Crosbie M. Echocardiographic parameters of left ventricular size and function as predictors of symptomatic heart failure in patients with a left ventricular ejection fraction of 50–59% treated with anthracyclines. Eur Heart J Cardiovasc Imaging. 2015;16(9):977–84. https://doi.org/10.1093/ehjci/jev113.
Thavendiranathan P, Negishi T, Coté MA, Penicka M, Massey R, Cho GY, et al. Single versus standard multiview assessment of global longitudinal strain for the diagnosis of cardiotoxicity during cancer therapy. JACC Cardiovasc Imaging. 2018;11(8):1109–18. https://doi.org/10.1016/j.jcmg.2018.03.003.
Oikonomou EK, Kokkinidis DG, Kampaktsis PN, Amir EA, Marwick TH, Gupta D, et al. Assessment of prognostic value of left ventricular global longitudinal strain for early prediction of chemotherapy-induced cardiotoxicity: a systematic review and meta-analysis. JAMA Cardiol. 2019;4(10):1007–18. https://doi.org/10.1001/jamacardio.2019.2952.
Sae Jang KJR, Charles L. Loprinzi, Saro Armenian, Daniel John Lenihan, Joerg Herrmann. Systematic review and meta-analysis of definitions and reported incidences of anthracycline cardiotoxicity. 2019 ASCO Annual Meeting: J Clin Oncol 2019; e:23081. https://doi.org/10.1200/JCO.2019.37.15_suppl.e23081.
Herrmann J, Lerman A, Sandhu NP, Villarraga HR, Mulvagh SL, Kohli M. Evaluation and management of patients with heart disease and cancer: cardio-oncology. Mayo Clin Proc. 2014;89(9):1287–306. https://doi.org/10.1016/j.mayocp.2014.05.013.
Ohtani K, Fujino T, Ide T, Funakoshi K, Sakamoto I, Hiasa KI, et al. Recovery from left ventricular dysfunction was associated with the early introduction of heart failure medical treatment in cancer patients with anthracycline-induced cardiotoxicity. Clin Res Cardiol. 2019;108(6):600–11. https://doi.org/10.1007/s00392-018-1386-0.
Ohtani K, Ide T, Hiasa KI, Sakamoto I, Yamashita N, Kubo M, et al. Cardioprotective effect of renin-angiotensin inhibitors and β-blockers in trastuzumab-related cardiotoxicity. Clin Res Cardiol. 2019;108(10):1128–39. https://doi.org/10.1007/s00392-019-01448-4.
Yoon HJ, Kim KH, Kim HY, Park H, Cho JY, Hong YJ, et al. Impacts of non-recovery of trastuzumab-induced cardiomyopathy on clinical outcomes in patients with breast cancer. Clin Res Cardiol. 2019;108(8):892–900. https://doi.org/10.1007/s00392-019-01417-x.
Fornaro A, Olivotto I, Rigacci L, Ciaccheri M, Tomberli B, Ferrantini C, et al. Comparison of long-term outcome in anthracycline-related versus idiopathic dilated cardiomyopathy: a single centre experience. Eur J Heart Fail. 2018;20(5):898–906. https://doi.org/10.1002/ejhf.1049.
Swain SM, Whaley FS, Ewer MS. Congestive heart failure in patients treated with doxorubicin: a retrospective analysis of three trials. Cancer. 2003;97(11):2869–79. https://doi.org/10.1002/cncr.11407.
Squires RW, Shultz AM, Herrmann J. Exercise training and cardiovascular health in cancer patients. Curr Oncol Rep. 2018;20(3):27. https://doi.org/10.1007/s11912-018-0681-2.
Fardman A, Banschick GD, Rabia R, Percik R, Fourey D, Segev S, et al. Cardiorespiratory fitness and survival following cancer diagnosis. Eur J Prev Cardiol. 2021;28(11):1242–9. https://doi.org/10.1177/2047487320930873.
Groarke JD, Payne DL, Claggett B, Mehra MR, Gong J, Caron J, et al. Association of post-diagnosis cardiorespiratory fitness with cause-specific mortality in cancer. Eur Heart J Qual Care Clin Outcomes. 2020;6(4):315–22. https://doi.org/10.1093/ehjqcco/qcaa015. This work clearly illustrates the inverse association of cardiopulmonary fitness and all-cause mortality in cancer patients.
Okwuosa TM, Ray RM, Palomo A, Foraker RE, Johnson L, Paskett ED, et al. Pre-diagnosis exercise and cardiovascular events in primary breast cancer: women’s health initiative. JACC CardioOncol. 2019;1(1):41–50. https://doi.org/10.1016/j.jaccao.2019.08.014.
Nagy AC, GulAcsi BP, CserEp Z, Hangody L, Forster T. Late cardiac effect of anthracycline therapy in physically active breast cancer survivors - a prospective study. Neoplasma. 2017;64(1):92–100. https://doi.org/10.4149/neo_2017_111.
Murray J, Bennett H, Bezak E, Perry R. The role of exercise in the prevention of cancer therapy-related cardiac dysfunction in breast cancer patients undergoing chemotherapy: systematic review. Eur J Prev Cardiol. 2022;29(3):463–72. https://doi.org/10.1093/eurjpc/zwab006.
Foulkes SJ, Howden EJ, Bigaran A, Janssens K, Antill Y, Loi S, et al. Persistent impairment in cardiopulmonary fitness after breast cancer chemotherapy. Med Sci Sports Exerc. 2019;51(8):1573–81. https://doi.org/10.1249/mss.0000000000001970.
Howden EJ, Bigaran A, Beaudry R, Fraser S, Selig S, Foulkes S, et al. Exercise as a diagnostic and therapeutic tool for the prevention of cardiovascular dysfunction in breast cancer patients. Eur J Prev Cardiol. 2019;26(3):305–15. https://doi.org/10.1177/2047487318811181.
Scott JM, Nilsen TS, Gupta D, Jones LW. Exercise therapy and cardiovascular toxicity in cancer. Circulation. 2018;137(11):1176–91. https://doi.org/10.1161/circulationaha.117.024671.
Antunes P, Joaquim A, Sampaio F, Nunes C, Ascensão A, Vilela E, et al. Effects of exercise training on cardiac toxicity markers in women with breast cancer undergoing chemotherapy with anthracyclines: a randomized controlled trial. Eur J Prev Cardiol. 2023;30(9):844–55. https://doi.org/10.1093/eurjpc/zwad063. Compared to usual care, exercise training increased peak oxygen consumption during and after chemotherapy, but established markers of cardiotoxicity did not change in this short-term follow-up.
Wonisch M, Hofmann P, Fruhwald FM, Kraxner W, Hödl R, Pokan R, et al. Influence of beta-blocker use on percentage of target heart rate exercise prescription. Eur J Cardiovasc Prev Rehabil. 2003;10(4):296–301. https://doi.org/10.1097/00149831-200308000-00013.
Hofmann P, Von Duvillard SP, Seibert FJ, Pokan R, Wonisch M, Lemura LM, et al. %HRmax target heart rate is dependent on heart rate performance curve deflection. Med Sci Sports Exerc. 2001;33(10):1726–31. https://doi.org/10.1097/00005768-200110000-00017.
Guazzi M, Arena R, Halle M, Piepoli MF, Myers J, Lavie CJ. 2016 focused update: clinical recommendations for cardiopulmonary exercise testing data assessment in specific patient populations. Eur Heart J. 2018;39(14):1144–61. https://doi.org/10.1093/eurheartj/ehw180.
Guazzi M, Wilhelm M, Halle M, Van Craenenbroeck E, Kemps H, de Boer RA, et al. Exercise testing in heart failure with preserved ejection fraction: an appraisal through diagnosis, pathophysiology and therapy - a clinical consensus statement of the Heart Failure Association and European Association of Preventive Cardiology of the European Society of Cardiology. Eur J Heart Fail. 2022;24(8):1327–45. https://doi.org/10.1002/ejhf.2601.
Malhotra R, Bakken K, D’Elia E, Lewis GD. Cardiopulmonary exercise testing in heart failure. JACC Heart Fail. 2016;4(8):607–16. https://doi.org/10.1016/j.jchf.2016.03.022.
West MA, Lythgoe D, Barben CP, Noble L, Kemp GJ, Jack S, et al. Cardiopulmonary exercise variables are associated with postoperative morbidity after major colonic surgery: a prospective blinded observational study. Br J Anaesth. 2014;112(4):665–71. https://doi.org/10.1093/bja/aet408.
West MA, Parry MG, Lythgoe D, Barben CP, Kemp GJ, Grocott MP, et al. Cardiopulmonary exercise testing for the prediction of morbidity risk after rectal cancer surgery. Br J Surg. 2014;101(9):1166–72. https://doi.org/10.1002/bjs.9551.
Ha D, Mazzone PJ, Ries AL, Malhotra A, Fuster M. The utility of exercise testing in patients with lung cancer. J Thorac Oncol. 2016;11(9):1397–410. https://doi.org/10.1016/j.jtho.2016.04.021.
Borg GA. Psychophysical bases of perceived exertion. Med Sci Sports Exerc. 1982;14(5):377–81.
D’Ascenzi F, Anselmi F, Fiorentini C, Mannucci R, Bonifazi M, Mondillo S. The benefits of exercise in cancer patients and the criteria for exercise prescription in cardio-oncology. Eur J Prev Cardiol. 2021;28(7):725–35. https://doi.org/10.1177/2047487319874900.
Sasso JP, Eves ND, Christensen JF, Koelwyn GJ, Scott J, Jones LW. A framework for prescription in exercise-oncology research. J Cachexia Sarcopenia Muscle. 2015;6(2):115–24. https://doi.org/10.1002/jcsm.12042.
Karvonen J, Vuorimaa T. Heart rate and exercise intensity during sports activities. Practical application Sports Med. 1988;5(5):303–11. https://doi.org/10.2165/00007256-198805050-00002.
Michalski M, Rowed K, Lavery JA, Moskowitz CS, Capaci C, Stene G, et al. Validity of estimated cardiorespiratory fitness in patients with primary breast cancer. JACC CardioOncol. 2022;4(2):210–9. https://doi.org/10.1016/j.jaccao.2022.05.003.
Wernhart S, Mincu R, Balcer B, Rammos C, Muentjes C, Rassaf T. The cardiorespiratory optimal point as a discriminator of lesion severity in adults with congenital heart disease. J Sports Med Phys Fitness. 2023;63(8):941–8. https://doi.org/10.23736/s0022-4707.23.14835-3.
Foulkes SJ, Howden EJ, Haykowsky MJ, Antill Y, Salim A, Nightingale SS, et al. Exercise for the prevention of anthracycline-induced functional disability and cardiac dysfunction: the BREXIT study. Circulation. 2023;147(7):532–45. https://doi.org/10.1161/circulationaha.122.062814. Exercise performance and cardiac reserve improved in early stage breast cancer patients compared to usual care after 12 months of training.
Jones LW, Douglas PS, Khouri MG, Mackey JR, Wojdyla D, Kraus WE, et al. Safety and efficacy of aerobic training in patients with cancer who have heart failure: an analysis of the HF-ACTION randomized trial. J Clin Oncol. 2014;32(23):2496–502. https://doi.org/10.1200/jco.2013.53.5724.
Scott JM, Zabor EC, Schwitzer E, Koelwyn GJ, Adams SC, Nilsen TS, et al. Efficacy of exercise therapy on cardiorespiratory fitness in patients with cancer: a systematic review and meta-analysis. J Clin Oncol. 2018;36(22):2297–305. https://doi.org/10.1200/jco.2017.77.5809.
Lee K, Tripathy D, Demark-Wahnefried W, Courneya KS, Sami N, Bernstein L, et al. Effect of aerobic and resistance exercise intervention on cardiovascular disease risk in women with early-stage breast cancer: a randomized clinical trial. JAMA Oncol. 2019;5(5):710–4. https://doi.org/10.1001/jamaoncol.2019.0038.
Courneya KS, McKenzie DC, Mackey JR, Gelmon K, Friedenreich CM, Yasui Y, et al. Effects of exercise dose and type during breast cancer chemotherapy: multicenter randomized trial. J Natl Cancer Inst. 2013;105(23):1821–32. https://doi.org/10.1093/jnci/djt297.
Kerrigan DJ, Reddy M, Walker EM, Cook B, McCord J, Loutfi R, et al. Cardiac rehabilitation improves fitness in patients with subclinical markers of cardiotoxicity while receiving chemotherapy: a randomized controlled study. J Cardiopulm Rehabil Prev. 2023;43(2):129–34. https://doi.org/10.1097/hcr.0000000000000719.
Mijwel S, Jervaeus A, Bolam KA, Norrbom J, Bergh J, Rundqvist H, et al. High-intensity exercise during chemotherapy induces beneficial effects 12 months into breast cancer survivorship. J Cancer Surviv. 2019;13(2):244–56. https://doi.org/10.1007/s11764-019-00747-z.
Dieli-Conwright CM, Courneya KS, Demark-Wahnefried W, Sami N, Lee K, Buchanan TA, et al. Effects of aerobic and resistance exercise on metabolic syndrome, sarcopenic obesity, and circulating biomarkers in overweight or obese survivors of breast cancer: a randomized controlled trial. J Clin Oncol. 2018;36(9):875–83. https://doi.org/10.1200/jco.2017.75.7526.
Sturgeon KM, Brown JC, Sears DD, Sarwer DB, Schmitz KH. WISER survivor trial: combined effect of exercise and weight loss interventions on inflammation in breast cancer survivors. Med Sci Sports Exerc. 2023;55(2):209–15. https://doi.org/10.1249/mss.0000000000003050.
Ndjavera W, Orange ST, O’Doherty AF, Leicht AS, Rochester M, Mills R, et al. Exercise-induced attenuation of treatment side-effects in patients with newly diagnosed prostate cancer beginning androgen-deprivation therapy: a randomised controlled trial. BJU Int. 2020;125(1):28–37. https://doi.org/10.1111/bju.14922.
Wall BA, GalvãO DA, Fatehee N, Taaffe DR, Spry N, Joseph D, et al. Exercise improves V˙O2max and body composition in androgen deprivation therapy-treated prostate cancer patients. Med Sci Sports Exerc. 2017;49(8):1503–10. https://doi.org/10.1249/mss.0000000000001277.
Rueegg CS, Zürcher SJ, Schindera C, Jung R, Deng WH, Bänteli I, et al. Effect of a 1-year physical activity intervention on cardiovascular health in long-term childhood cancer survivors-a randomised controlled trial (SURfit). Br J Cancer. 2023;129(8):1284–97. https://doi.org/10.1038/s41416-023-02410-y.
Gilbert SE, Tew GA, Fairhurst C, Bourke L, Saxton JM, Winter EM, et al. Effects of a lifestyle intervention on endothelial function in men on long-term androgen deprivation therapy for prostate cancer. Br J Cancer. 2016;114(4):401–8. https://doi.org/10.1038/bjc.2015.479.
Lee K, Kang I, Mack WJ, Mortimer J, Sattler F, Salem G, et al. Effects of high-intensity interval training on vascular endothelial function and vascular wall thickness in breast cancer patients receiving anthracycline-based chemotherapy: a randomized pilot study. Breast Cancer Res Treat. 2019;177(2):477–85. https://doi.org/10.1007/s10549-019-05332-7.
Sebio Garcia R, Yáñez Brage MI, Giménez Moolhuyzen E, Granger CL, Denehy L. Functional and postoperative outcomes after preoperative exercise training in patients with lung cancer: a systematic review and meta-analysis. Interact Cardiovasc Thorac Surg. 2016;23(3):486–97. https://doi.org/10.1093/icvts/ivw152.
Yang L, Morielli AR, Heer E, Kirkham AA, Cheung WY, Usmani N, et al. Effects of exercise on cancer treatment efficacy: a systematic review of preclinical and clinical studies. Cancer Res. 2021;81(19):4889–95. https://doi.org/10.1158/0008-5472.Can-21-1258.
Meyerhardt JA, Heseltine D, Niedzwiecki D, Hollis D, Saltz LB, Mayer RJ, et al. Impact of physical activity on cancer recurrence and survival in patients with stage III colon cancer: findings from CALGB 89803. J Clin Oncol. 2006;24(22):3535–41. https://doi.org/10.1200/jco.2006.06.0863.
Morishita S, Hamaue Y, Fukushima T, Tanaka T, Fu JB, Nakano J. Effect of exercise on mortality and recurrence in patients with cancer: a systematic review and meta-analysis. Integr Cancer Ther. 2020;19:1534735420917462. https://doi.org/10.1177/1534735420917462.
Jones LW, Fels DR, West M, Allen JD, Broadwater G, Barry WT, et al. Modulation of circulating angiogenic factors and tumor biology by aerobic training in breast cancer patients receiving neoadjuvant chemotherapy. Cancer Prev Res (Phila). 2013;6(9):925–37. https://doi.org/10.1158/1940-6207.Capr-12-0416.
Hayes SCSM, Spence R, Pyke C, Saunders C, Bashford J, Eakin E. Can exercise influence survival following breast cancer: results from a randomised, controlled trial. J Clin Oncol. 2017;35:S10067-S. https://doi.org/10.1200/JCO.2017.35.15_suppl.10067.
Jones LW, Habel LA, Weltzien E, Castillo A, Gupta D, Kroenke CH, et al. Exercise and risk of cardiovascular events in women with nonmetastatic breast cancer. J Clin Oncol. 2016;34(23):2743–9. https://doi.org/10.1200/jco.2015.65.6603.
Irwin ML, Cartmel B, Gross CP, Ercolano E, Li F, Yao X, et al. Randomized exercise trial of aromatase inhibitor-induced arthralgia in breast cancer survivors. J Clin Oncol. 2015;33(10):1104–11. https://doi.org/10.1200/jco.2014.57.1547.
Zimmer P, Baumann FT, Oberste M, Schmitt J, Joisten N, Hartig P, et al. Influence of personalized exercise recommendations during rehabilitation on the sustainability of objectively measured physical activity levels, fatigue, and fatigue-related biomarkers in patients with breast cancer. Integr Cancer Ther. 2018;17(2):306–11. https://doi.org/10.1177/1534735417713301.
Schultz EB, Zubac D, Bloch W, Baurecht H, Rickert J, Baumann FT. Moderate intensity exercise reduces side effects of cancer therapy and maintains cardiorespiratory fitness in male breast cancer patients: findings from the BRECA male crossover study. Breast Care (Basel). 2023;18(6):483–92. https://doi.org/10.1159/000534090.
Wernhart S, Rassaf T. Exercise, cancer, and the cardiovascular system: clinical effects and mechanistic insights. Basic Res Cardiol. 2024. https://doi.org/10.1007/s00395-024-01034-4.
Hiensch AE, Monninkhof EM, Schmidt ME, Zopf EM, Bolam KA, Aaronson NK, et al. Design of a multinational randomized controlled trial to assess the effects of structured and individualized exercise in patients with metastatic breast cancer on fatigue and quality of life: the EFFECT study. Trials. 2022;23(1):610. https://doi.org/10.1186/s13063-022-06556-7.
Bauer J, Morley JE, Schols A, Ferrucci L, Cruz-Jentoft AJ, Dent E, et al. Sarcopenia: a time for action An SCWD Position Paper. J Cachexia Sarcopenia Muscle. 2019;10(5):956–61. https://doi.org/10.1002/jcsm.12483.
Anker MS, Lena A, Roeland EJ, Porthun J, Schmitz S, Hadzibegovic S, et al. Patient-reported ability to walk 4 m and to wash: new clinical endpoints and predictors of survival in patients with pre-terminal cancer. J Cachexia Sarcopenia Muscle. 2023;14(4):1670–81. https://doi.org/10.1002/jcsm.13247.
Hadzibegovic S, Porthun J, Lena A, Weinländer P, Lück LC, Potthoff SK, et al. Hand grip strength in patients with advanced cancer: a prospective study. J Cachexia Sarcopenia Muscle. 2023;14(4):1682–94. https://doi.org/10.1002/jcsm.13248.
Pelliccia A, Sharma S, Gati S, Bäck M, Börjesson M, Caselli S, et al. 2020 ESC Guidelines on sports cardiology and exercise in patients with cardiovascular disease. Eur Heart J. 2021;42(1):17–96. https://doi.org/10.1093/eurheartj/ehaa605.
Porter C, Reidy PT, Bhattarai N, Sidossis LS, Rasmussen BB. Resistance exercise training alters mitochondrial function in human skeletal muscle. Med Sci Sports Exerc. 2015;47(9):1922–31. https://doi.org/10.1249/mss.0000000000000605.
McDonald J, Sayers J, Anker SD, Arends J, Balstad TR, Baracos V, et al. Physical function endpoints in cancer cachexia clinical trials: systematic review 1 of the cachexia endpoints series. J Cachexia Sarcopenia Muscle. 2023;14(5):1932–48. https://doi.org/10.1002/jcsm.13321.
Strasser B, Steindorf K, Wiskemann J, Ulrich CM. Impact of resistance training in cancer survivors: a meta-analysis. Med Sci Sports Exerc. 2013;45(11):2080–90. https://doi.org/10.1249/MSS.0b013e31829a3b63.
Antunes JMM, Ferreira RMP, Moreira-Gonçalves D. Exercise training as therapy for cancer-induced cardiac cachexia. Trends Mol Med. 2018;24(8):709–27. https://doi.org/10.1016/j.molmed.2018.06.002.
Foulkes SJ, Haykowsky MJ, Li T, Wang J, Kennedy M, Kirkham AA, et al. Determinants of impaired peak oxygen uptake in breast cancer survivors: JACC: CardioOncology Primer. JACC CardioOncol. 2024;6(1):33–7. https://doi.org/10.1016/j.jaccao.2023.11.005.
Milanović Z, Sporiš G, Weston M. Effectiveness of high-intensity interval training (HIT) and continuous endurance training for VO2max improvements: a systematic review and meta-analysis of controlled trials. Sports Med. 2015;45(10):1469–81. https://doi.org/10.1007/s40279-015-0365-0.
Wisløff U, Støylen A, Loennechen JP, Bruvold M, Rognmo Ø, Haram PM, et al. Superior cardiovascular effect of aerobic interval training versus moderate continuous training in heart failure patients: a randomized study. Circulation. 2007;115(24):3086–94. https://doi.org/10.1161/circulationaha.106.675041.
Ellingsen Ø, Halle M, Conraads V, Støylen A, Dalen H, Delagardelle C, et al. High-intensity interval training in patients with heart failure with reduced ejection fraction. Circulation. 2017;135(9):839–49. https://doi.org/10.1161/circulationaha.116.022924.
Mueller S, Winzer EB, Duvinage A, Gevaert AB, Edelmann F, Haller B, et al. Effect of high-intensity interval training, moderate continuous training, or guideline-based physical activity advice on peak oxygen consumption in patients with heart failure with preserved ejection fraction: a randomized clinical trial. JAMA. 2021;325(6):542–51. https://doi.org/10.1001/jama.2020.26812.
Siddiqi TJ, Rashid AM, Javaid SS, Siddiqi AK, Usman MS, Hervir O, et al. High-intensity interval training versus moderate continuous training in patients with heart failure with preserved ejection fraction: a systematic review and meta-analysis. Curr Probl Cardiol. 2023;48(8):101720. https://doi.org/10.1016/j.cpcardiol.2023.101720.
Gomes Neto M, Durães AR, Conceição LSR, Saquetto MB, Ellingsen Ø, Carvalho VO. High intensity interval training versus moderate intensity continuous training on exercise capacity and quality of life in patients with heart failure with reduced ejection fraction: a systematic review and meta-analysis. Int J Cardiol. 2018;261:134–41. https://doi.org/10.1016/j.ijcard.2018.02.076.
Haykowsky MJ, Timmons MP, Kruger C, McNeely M, Taylor DA, Clark AM. Meta-analysis of aerobic interval training on exercise capacity and systolic function in patients with heart failure and reduced ejection fractions. Am J Cardiol. 2013;111(10):1466–9. https://doi.org/10.1016/j.amjcard.2013.01.303.
Wallen MP, Hennessy D, Brown S, Evans L, Rawstorn JC, Wong Shee A, et al. High-intensity interval training improves cardiorespiratory fitness in cancer patients and survivors: a meta-analysis. Eur J Cancer Care (Engl). 2020;29(4):e13267. https://doi.org/10.1111/ecc.13267.
Adams SC, DeLorey DS, Davenport MH, Stickland MK, Fairey AS, North S, et al. Effects of high-intensity aerobic interval training on cardiovascular disease risk in testicular cancer survivors: a phase 2 randomized controlled trial. Cancer. 2017;123(20):4057–65. https://doi.org/10.1002/cncr.30859.
Isanejad A, Nazari S, Gharib B, Motlagh AG. Comparison of the effects of high-intensity interval and moderate-intensity continuous training on inflammatory markers, cardiorespiratory fitness, and quality of life in breast cancer patients. J Sport Health Sci. 2023;12(6):674–89. https://doi.org/10.1016/j.jshs.2023.07.001.
Toohey K, Pumpa K, McKune A, Cooke J, Welvaert M, Northey J, et al. The impact of high-intensity interval training exercise on breast cancer survivors: a pilot study to explore fitness, cardiac regulation and biomarkers of the stress systems. BMC Cancer. 2020;20(1):787. https://doi.org/10.1186/s12885-020-07295-1.
Adams SC, DeLorey DS, Davenport MH, Fairey AS, North S, Courneya KS. Effects of high-intensity interval training on fatigue and quality of life in testicular cancer survivors. Br J Cancer. 2018;118(10):1313–21. https://doi.org/10.1038/s41416-018-0044-7.
Herranz-Gómez A, Cuenca-Martínez F, Suso-Martí L, Varangot-Reille C, Calatayud J, Blanco-Díaz M, et al. Effectiveness of HIIT in patients with cancer or cancer survivors: an umbrella and mapping review with meta-meta-analysis. Scand J Med Sci Sports. 2022;32(11):1522–49. https://doi.org/10.1111/sms.14223.
Kang DW, Wilson RL, Christopher CN, Normann AJ, Barnes O, Lesansee JD, et al. Exercise cardio-oncology: exercise as a potential therapeutic modality in the management of anthracycline-induced cardiotoxicity. Front Cardiovasc Med. 2021;8:805735. https://doi.org/10.3389/fcvm.2021.805735.
Shephard RJ, Balady GJ. Exercise as cardiovascular therapy. Circulation. 1999;99(7):963–72. https://doi.org/10.1161/01.cir.99.7.963.
Zu XL, Guppy M. Cancer metabolism: facts, fantasy, and fiction. Biochem Biophys Res Commun. 2004;313(3):459–65. https://doi.org/10.1016/j.bbrc.2003.11.136.
Attaix D, Ventadour S, Codran A, Béchet D, Taillandier D, Combaret L. The ubiquitin-proteasome system and skeletal muscle wasting. Essays Biochem. 2005;41:173–86. https://doi.org/10.1042/eb0410173.
Rodriguez J, Vernus B, Chelh I, Cassar-Malek I, Gabillard JC, Hadj Sassi A, et al. Myostatin and the skeletal muscle atrophy and hypertrophy signaling pathways. Cell Mol Life Sci. 2014;71(22):4361–71. https://doi.org/10.1007/s00018-014-1689-x.
Zong WX, Rabinowitz JD, White E. Mitochondria and cancer. Mol Cell. 2016;61(5):667–76. https://doi.org/10.1016/j.molcel.2016.02.011.
Laker RC, Drake JC, Wilson RJ, Lira VA, Lewellen BM, Ryall KA, et al. Ampk phosphorylation of Ulk1 is required for targeting of mitochondria to lysosomes in exercise-induced mitophagy. Nat Commun. 2017;8(1):548. https://doi.org/10.1038/s41467-017-00520-9.
White E, Mehnert JM, Chan CS. Autophagy, metabolism, and cancer. Clin Cancer Res. 2015;21(22):5037–46. https://doi.org/10.1158/1078-0432.Ccr-15-0490.
Cunha TF, Bacurau AV, Moreira JB, Paixão NA, Campos JC, Ferreira JC, et al. Exercise training prevents oxidative stress and ubiquitin-proteasome system overactivity and reverse skeletal muscle atrophy in heart failure. PLoS ONE. 2012;7(8):e41701. https://doi.org/10.1371/journal.pone.0041701.
Gielen S, Sandri M, Kozarez I, Kratzsch J, Teupser D, Thiery J, et al. Exercise training attenuates MuRF-1 expression in the skeletal muscle of patients with chronic heart failure independent of age: the randomized Leipzig Exercise Intervention in Chronic Heart Failure and Aging catabolism study. Circulation. 2012;125(22):2716–27. https://doi.org/10.1161/circulationaha.111.047381.
Lenk K, Erbs S, Höllriegel R, Beck E, Linke A, Gielen S, et al. Exercise training leads to a reduction of elevated myostatin levels in patients with chronic heart failure. Eur J Prev Cardiol. 2012;19(3):404–11. https://doi.org/10.1177/1741826711402735.
Wei X, Liu X, Rosenzweig A. What do we know about the cardiac benefits of exercise? Trends Cardiovasc Med. 2015;25(6):529–36. https://doi.org/10.1016/j.tcm.2014.12.014.
Agostini D, Natalucci V, Baldelli G, De Santi M, Donati Zeppa S, Vallorani L, et al. New insights into the role of exercise in inhibiting mTOR signaling in triple-negative breast cancer. Oxid Med Cell Longev. 2018;2018:5896786. https://doi.org/10.1155/2018/5896786.
Leung PS, Aronson WJ, Ngo TH, Golding LA, Barnard RJ. Exercise alters the IGF axis in vivo and increases p53 protein in prostate tumor cells in vitro. J Appl Physiol (1985). 2004;96(2):450–4. https://doi.org/10.1152/japplphysiol.00871.2003.
Vega RB, Konhilas JP, Kelly DP, Leinwand LA. Molecular mechanisms underlying cardiac adaptation to exercise. Cell Metab. 2017;25(5):1012–26. https://doi.org/10.1016/j.cmet.2017.04.025.
Linke A, Adams V, Schulze PC, Erbs S, Gielen S, Fiehn E, et al. Antioxidative effects of exercise training in patients with chronic heart failure: increase in radical scavenger enzyme activity in skeletal muscle. Circulation. 2005;111(14):1763–70. https://doi.org/10.1161/01.Cir.0000165503.08661.E5.
Souza RW, Fernandez GJ, Cunha JP, Piedade WP, Soares LC, Souza PA, et al. Regulation of cardiac microRNAs induced by aerobic exercise training during heart failure. Am J Physiol Heart Circ Physiol. 2015;309(10):H1629–41. https://doi.org/10.1152/ajpheart.00941.2014.
Landers-Ramos RQ, Sapp RM, Jenkins NT, Murphy AE, Cancre L, Chin ER, et al. Chronic endurance exercise affects paracrine action of CD31+ and CD34+ cells on endothelial tube formation. Am J Physiol Heart Circ Physiol. 2015;309(3):H407–20. https://doi.org/10.1152/ajpheart.00123.2015.
Scarpulla RC. Transcriptional paradigms in mammalian mitochondrial biogenesis and function. Physiol Rev. 2008;88(2):611–38. https://doi.org/10.1152/physrev.00025.2007.
de Souza PA, de Souza RW, Soares LC, Piedade WP, Campos DH, Carvalho RF, et al. Aerobic training attenuates nicotinic acethylcholine receptor changes in the diaphragm muscle during heart failure. Histol Histopathol. 2015;30(7):801–11. https://doi.org/10.14670/hh-11-581.
Hambrecht R, Fiehn E, Yu J, Niebauer J, Weigl C, Hilbrich L, et al. Effects of endurance training on mitochondrial ultrastructure and fiber type distribution in skeletal muscle of patients with stable chronic heart failure. J Am Coll Cardiol. 1997;29(5):1067–73. https://doi.org/10.1016/s0735-1097(97)00015-6.
Irrcher I, Ljubicic V, Hood DA. Interactions between ROS and AMP kinase activity in the regulation of PGC-1alpha transcription in skeletal muscle cells. Am J Physiol Cell Physiol. 2009;296(1):C116–23. https://doi.org/10.1152/ajpcell.00267.2007.
Gaude E, Frezza C. Defects in mitochondrial metabolism and cancer. Cancer Metab. 2014;2:10. https://doi.org/10.1186/2049-3002-2-10.
Kim Y, Triolo M, Erlich AT, Hood DA. Regulation of autophagic and mitophagic flux during chronic contractile activity-induced muscle adaptations. Pflugers Arch. 2019;471(3):431–40. https://doi.org/10.1007/s00424-018-2225-x.
Liu Y, Sun Y, Guo Y, Shi X, Chen X, Feng W, et al. An overview: the diversified role of mitochondria in cancer metabolism. Int J Biol Sci. 2023;19(3):897–915. https://doi.org/10.7150/ijbs.81609.
Van Craenenbroeck EM, Frederix G, Pattyn N, Beckers P, Van Craenenbroeck AH, Gevaert A, et al. Effects of aerobic interval training and continuous training on cellular markers of endothelial integrity in coronary artery disease: a SAINTEX-CAD substudy. Am J Physiol Heart Circ Physiol. 2015;309(11):H1876–82. https://doi.org/10.1152/ajpheart.00341.2015.
Hasenfuss G, Reinecke H, Studer R, Meyer M, Pieske B, Holtz J, et al. Relation between myocardial function and expression of sarcoplasmic reticulum Ca(2+)-ATPase in failing and nonfailing human myocardium. Circ Res. 1994;75(3):434–42. https://doi.org/10.1161/01.res.75.3.434.
Wisløff U, Loennechen JP, Falck G, Beisvag V, Currie S, Smith G, et al. Increased contractility and calcium sensitivity in cardiac myocytes isolated from endurance trained rats. Cardiovasc Res. 2001;50(3):495–508. https://doi.org/10.1016/s0008-6363(01)00210-3.
Kemi OJ, Ellingsen O, Ceci M, Grimaldi S, Smith GL, Condorelli G, et al. Aerobic interval training enhances cardiomyocyte contractility and Ca2+ cycling by phosphorylation of CaMKII and Thr-17 of phospholamban. J Mol Cell Cardiol. 2007;43(3):354–61. https://doi.org/10.1016/j.yjmcc.2007.06.013.
Waring CD, Vicinanza C, Papalamprou A, Smith AJ, Purushothaman S, Goldspink DF, et al. The adult heart responds to increased workload with physiologic hypertrophy, cardiac stem cell activation, and new myocyte formation. Eur Heart J. 2014;35(39):2722–31. https://doi.org/10.1093/eurheartj/ehs338.
Uth J, Fristrup B, Sørensen V, Helge EW, Christensen MK, Kjærgaard JB, et al. Exercise intensity and cardiovascular health outcomes after 12 months of football fitness training in women treated for stage I-III breast cancer: results from the football fitness After Breast Cancer (ABC) randomized controlled trial. Prog Cardiovasc Dis. 2020;63(6):792–9. https://doi.org/10.1016/j.pcad.2020.08.002.
MacInnis MJ, Gibala MJ. Physiological adaptations to interval training and the role of exercise intensity. J Physiol. 2017;595(9):2915–30. https://doi.org/10.1113/jp273196.
Zucker IH, Musch TI. Benefits of exercise training on cardiovascular dysfunction: molecular and integrative. Am J Physiol Heart Circ Physiol. 2018;315(4):H1027–31. https://doi.org/10.1152/ajpheart.00516.2018.
Burgomaster KA, Howarth KR, Phillips SM, Rakobowchuk M, Macdonald MJ, McGee SL, et al. Similar metabolic adaptations during exercise after low volume sprint interval and traditional endurance training in humans. J Physiol. 2008;586(1):151–60. https://doi.org/10.1113/jphysiol.2007.142109.
Coffey VG, Hawley JA. The molecular bases of training adaptation. Sports Med. 2007;37(9):737–63. https://doi.org/10.2165/00007256-200737090-00001.
Little JP, Safdar A, Bishop D, Tarnopolsky MA, Gibala MJ. An acute bout of high-intensity interval training increases the nuclear abundance of PGC-1α and activates mitochondrial biogenesis in human skeletal muscle. Am J Physiol Regul Integr Comp Physiol. 2011;300(6):R1303–10. https://doi.org/10.1152/ajpregu.00538.2010.
Tjønna AE, Leinan IM, Bartnes AT, Jenssen BM, Gibala MJ, Winett RA, et al. Low- and high-volume of intensive endurance training significantly improves maximal oxygen uptake after 10-weeks of training in healthy men. PLoS ONE. 2013;8(5):e65382. https://doi.org/10.1371/journal.pone.0065382.
Montero D, Diaz-Cañestro C, Lundby C. Endurance training and V˙O2max: role of maximal cardiac output and oxygen extraction. Med Sci Sports Exerc. 2015;47(10):2024–33. https://doi.org/10.1249/mss.0000000000000640.
Wernhart S, Papathanasiou M, Mahabadi AA, Rassaf T, Luedike P. Betablockers reduce oxygen pulse increase and performance in heart failure patients with preserved ejection fraction. Int J Cardiol. 2023;370:309–18. https://doi.org/10.1016/j.ijcard.2022.10.009.
Wernhart S, Papathanasiou M, Rassaf T, Luedike P. The controversial role of beta-blockers in heart failure with preserved ejection fraction. Pharmacol Ther. 2023;243:108356. https://doi.org/10.1016/j.pharmthera.2023.108356.
Adams V, Reich B, Uhlemann M, Niebauer J. Molecular effects of exercise training in patients with cardiovascular disease: focus on skeletal muscle, endothelium, and myocardium. Am J Physiol Heart Circ Physiol. 2017;313(1):H72-h88. https://doi.org/10.1152/ajpheart.00470.2016.
La Gerche A, Howden EJ, Haykowsky MJ, Lewis GD, Levine BD, Kovacic JC. Heart failure with preserved ejection fraction as an exercise deficiency syndrome: JACC Focus Seminar 2/4. J Am Coll Cardiol. 2022;80(12):1177–91. https://doi.org/10.1016/j.jacc.2022.07.011.
Tsai E, Mouhayar E, Lenihan D, Song J, Durand JB, Fadol A, et al. Feasibility and outcomes of an exercise intervention for chemotherapy-induced heart failure. J Cardiopulm Rehabil Prev. 2019;39(3):199–203. https://doi.org/10.1097/hcr.0000000000000388.
Viamonte SG, Joaquim A, Alves A, Vilela E, Capela A, Ferreira C, et al. Adherence, safety, and satisfaction of a cardio-oncology rehabilitation program framework versus community exercise training for cancer survivors: findings from the CORE trial. Support Care Cancer. 2023;31(3):173. https://doi.org/10.1007/s00520-023-07638-1.
Pandey A, Parashar A, Kumbhani D, Agarwal S, Garg J, Kitzman D, et al. Exercise training in patients with heart failure and preserved ejection fraction: meta-analysis of randomized control trials. Circ Heart Fail. 2015;8(1):33–40. https://doi.org/10.1161/circheartfailure.114.001615.
Pandey A, Garg S, Khunger M, Darden D, Ayers C, Kumbhani DJ, et al. Dose-response relationship between physical activity and risk of heart failure: a meta-analysis. Circulation. 2015;132(19):1786–94. https://doi.org/10.1161/circulationaha.115.015853.
Gilchrist SC, Barac A, Ades PA, Alfano CM, Franklin BA, Jones LW, et al. Cardio-oncology rehabilitation to manage cardiovascular outcomes in cancer patients and survivors: a scientific statement from the American Heart Association. Circulation. 2019;139(21):e997–1012. https://doi.org/10.1161/cir.0000000000000679.
Lakoski SG, Eves ND, Douglas PS, Jones LW. Exercise rehabilitation in patients with cancer. Nat Rev Clin Oncol. 2012;9(5):288–96. https://doi.org/10.1038/nrclinonc.2012.27.
Pituskin E, Cox-Kennett N, Foulkes S, Driga A, Dimitry R, Thompson RB, et al. Cardio-oncology and cancer rehabilitation: is an integrated approach possible? Can J Cardiol. 2023. https://doi.org/10.1016/j.cjca.2023.09.024.
Rassaf T, Totzeck M, Backs J, Bokemeyer C, Hallek M, Hilfiker-Kleiner D, et al. Onco-cardiology: consensus paper of the German Cardiac Society, the German Society for Pediatric Cardiology and Congenital Heart Defects and the German Society for Hematology and Medical Oncology. Clin Res Cardiol. 2020;109(10):1197–222. https://doi.org/10.1007/s00392-020-01636-7.
Acknowledgements
The editors would like to thank Drs. Wilhelm Bloch and Arjang Ruhpawar for handling the review of this manuscript.
Funding
Open Access funding enabled and organized by Projekt DEAL.
Author information
Authors and Affiliations
Contributions
Both authors contributed to the study conception and design. Material preparation was performed by Simon Wernhart and Tienush Rassaf. The first draft of the manuscript was written by Simon Wernhart and both authors commented on previous versions of the manuscript. Both authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethical Approval
Ethical approval was not necesssary as no data analysis was performed for this review.
The images of Fig. 1 were created with Biorender.com.
Consent to Participate
Not applicable.
Competing Interests
TR is co-founder of Mycor, a start-up focussing on the development of algorithms to detect amyloidosis. None of these is related to the submitted manuscript. TR is section editor for Cardio-oncology for Current Heart Failure Reports. All other authors declare no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wernhart, S., Rassaf, T. Relevance of Cardiovascular Exercise in Cancer and Cancer Therapy-Related Cardiac Dysfunction. Curr Heart Fail Rep 21, 238–251 (2024). https://doi.org/10.1007/s11897-024-00662-0
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11897-024-00662-0