Abstract
Background
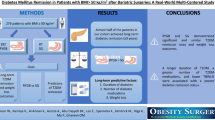
Laparoscopic sleeve gastrectomy (LSG) and laparoscopic Roux-en-Y gastric bypass (LRYGB) achieve similar type 2 diabetes mellitus (T2DM) remission rates. Since a great variability exists in defining T2DM remission, an expert panel proposed partial and complete remission criteria that include the maintenance of fasting plasma glucose (FPG) and glycosylated hemoglobin (A1c) objectives for at least 1 year. The 2-year T2DM remission rate and time needed to reach it after LSG or LRYGB were compared using different remission criteria.
Methods
This was a prospective cohort study of 55 T2DM subjects operated on with LSG (n = 21) or LRYGB (n = 34). Four models for defining remission were used: Buchwald criteria (FPG <100 mg/dl or A1c <6 %), American Diabetes Association (ADA) complete (FPG <100 mg/dl plus A1c <6 % maintained for at least 1 year), ADA partial (FPG <125 mg/dl with A1c <6.5 % maintained for at least 1 year), and ADA complete without time requirement.
Results
Both groups were comparable, except for higher A1c levels in the LSG group. The remission rate ranged from 43.6 % using ADA complete remission to 92.7 % with Buchwald criteria, with no differences between surgical procedures. Differences were found in the time to achieve remission only when ADA complete remission criteria (5.1 ± 2.9 months LRYGB and 9.0 ± 3.8 months LSG, p = 0.014) and ADA without time requirement criteria (4.9 ± 2.7 months LRYGB and 8.4 ± 3.9 months LSG, p = 0.005) were used.
Conclusions
T2DM remission rate varies widely depending on the criteria used for its definition. Remission occurred sooner after LRYGB when the strictest criteria to define remission were used.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The worldwide prevalence of type 2 diabetes mellitus (T2DM) continues to rise in parallel with growing obesity rates [1]. In this regard, more than 60 % of T2DM patients are obese, and this combination now constitutes a public health problem [2]. Recent large-scale trials evaluating medical therapy for obesity and diabetes have yielded disappointing results, and they suggest that substantial resources are required to achieve modest weight loss and diabetes control [3, 4], with a neutral effect on cardiovascular outcomes [5]. Bariatric surgery is recommended for adults with a body mass index (BMI) above 35 Kg/m2 and T2DM, mainly when the latter or associated comorbidities are difficult to control with lifestyle and pharmacologic therapy [6]. The most commonly performed laparoscopic bariatric procedures are laparoscopic Roux-en-Y gastric bypass (LRYGB) and laparoscopic sleeve gastrectomy (LSG) [7]. LRYGB, a hybrid technique, achieves a greater improvement in glucose metabolism than purely restrictive techniques [8]. On the other hand, among restrictive techniques, LSG has yielded the best results in terms of T2DM remission, similar to those of LRYGB [9].
Great heterogeneity exists in defining remission criteria for T2DM. In this respect, some authors only consider diabetes medication withdrawal while others suggest different cutoffs for fasting plasma glucose (FPG) and glycosylated hemoglobin (A1c) or a combination of both. Since the publication of a meta-analysis on bariatric surgery and diabetes remission by Buchwald et al. in 2004, the remission criteria used by the authors (FPG <100 mg/dl or A1c <6 %) have been widely accepted [8]. However, in 2009, an expert panel of endocrinologists of the American Diabetes Association (ADA) proposed new criteria for partial, complete, and prolonged remission. Complete T2DM remission was defined as glycemia below diabetic range in the absence of pharmacologic therapy for at least 1 year [10]. These ADA criteria are stricter than those previously described, and few authors have considered them when defining diabetes remission, and they have not fully evaluated the time criterion [11–13].
The aim of the present study was to compare T2DM remission rates 2 years after LSG and LRYGB using the new ADA criteria [10] and those proposed in previous studies [8, 14]. The time needed to reach therapeutic goals of A1c, FPG, and medication withdrawal for each laparoscopic bariatric procedure was also assessed.
Material and Methods
This was an observational study on a prospective cohort of severely obese patients undergoing bariatric surgery at the Hospital del Mar, Barcelona. Patients were between 18 and 55 years of age and met the 1991 bariatric surgery criteria of the National Institutes of Health [15]. Indication for the type of surgical procedure (LSG or LRYGB) was based on clinical criteria and the consensus of the Bariatric Surgery Unit. Inclusion criteria were patients with T2DM and at least 2 years of follow-up. In accordance with the study protocol approved by the hospital Ethics Committee, all patients were evaluated preoperatively; at 3, 6, 12, and 18 months post-surgery; and annually from years 2 to 4. Diabetes therapy was supervised by the endocrinologist of the Bariatric Surgery Unit during the preoperative, in-hospital, and follow-up periods. Protocol visits included measurements of weight, waist circumference, blood pressure, and laboratory parameters including glucose and A1c levels. All patients signed their informed consent for the procedure.
Two hundred and sixty-three patients underwent surgery between January 2006 and May 2011. Of these, 56 patients had T2DM, and one was lost to follow-up; therefore, the final analysis included 55 patients, 34 underwent LRYGB and 21 LSG.
Anthropometric and Biochemical Measurements
Glucose was determined by the oxidase method. A1c was quantified by chromatography (Biosystems, Barcelona, Spain). BMI was calculated as weight in kilograms divided by the square of height in meters. The percentage of excess weight loss (% EWL) was calculated based on the excess weight above the ideal weight (weight corresponding to BMI of 25 Kg/m2). T2DM diagnosis was defined as two fasting plasma glucose concentrations above 125 mg/dl or A1c ≥6.5 % or treatment with oral hypoglycemic agents or insulin [16]. Hypertension was defined as systolic blood pressure >140 mmHg and/or diastolic blood pressure >90 mmHg or current treatment with antihypertensive agents [17]. Dyslipidemia was considered when total cholesterol was >240 mg/dl or low-density lipoprotein (LDL) cholesterol >160 mg/dl or use of lipid-lowering medication. The T2DM remission rate was evaluated using four different criteria: the criteria reported in the meta-analysis of Buchwald et al. [8] (Buchwald criteria), those for complete and partial remission defined by the expert panel (ADA complete and ADA partial criteria) [10], and an approach that uses the same cutoffs for complete remission of the ADA without applying the time criterion (ADA complete without time criteria). The cutoff levels of A1c and FPG for each criterion are shown in Table 1. The time elapsed from surgery until patients met the A1c and FPG targets for remission according to each definition was assessed.
Surgical Techniques
The LRYGB technique involved a 150-cm antecolic Roux limb with a 25-mm circular pouch-jejunostomy and exclusion of 50 cm of the proximal jejunum. In LSG, the longitudinal resection of the stomach from the angle of His to approximately 5-cm proximal to the pylorus was performed using a 35 French bougie inserted along the lesser curvature. All operations were performed by the same team of surgeons.
Statistical Analysis
Data are expressed as mean ± standard deviation for continuous variables and as percentages and frequencies for categorical variables. Student’s t test was performed to assess differences between two means. Either chi-square test or Fisher’s exact test was used to test the degree of association of categorical variables. A p value <0.05 was considered statistically significant. Statistical analysis was made with SPSS (version 14.0 for Windows; SPSS, Chicago, IL).
Results
All 55 diabetic patients were Caucasian, with a mean age of 49.0 ± 4.9 years and a baseline BMI of 45.4 ± 4.9 Kg/m2; 80 % were women. Baseline characteristics of LRYGB and LSG patients are listed in Table 2. Both groups were comparable, except for higher A1c levels in the LSG group.
Progressive weight loss was observed during the 2-year follow-up, reaching a maximum % EWL at 18 months for LRYGB (78.7 ± 18.3 %) and at 12 months for LSG (78.1 ± 16.9 %). No differences in % EWL between groups were found during follow-up (Fig. 1). Mean A1c and FPG levels decreased rapidly after 3 months, remaining within normal values during the 2-year-follow-up (Figs. 2 and 3) with no differences between groups.
As shown in Table 1, remission rates using ADA complete remission criteria were the lowest and those observed using the Buchwald criteria were the highest. No differences between bariatric surgery procedures were observed in terms of remission rates, regardless of the remission criteria used (Fig. 4).
The time elapsed from surgery until achievement of the metabolic goals for each remission criterion is presented in Table 3. No differences between groups were found using the Buchwald and ADA partial remission criteria. Using ADA complete remission with or without time criteria, remission was achieved earlier in the LRYGB than in the LSG group.
Discussion
Two-year remission rates varied widely depending on the criteria used for its definition, from 43.6 % with the ADA complete remission criteria to 92.7 % using the Buchwald criteria. In this observational study, no differences were found between LSG and LRYGB in terms of T2DM remission during the 2-year follow-up, regardless of the remission criteria applied. However, remission was achieved earlier with LRYGB using ADA complete remission criteria.
As described previously, a slight variation in definition can yield significant differences in remission rates, although the differences reported in previous studies were less prominent than those found in the present study. On one hand, Pournaras et al. [12], in a cohort of 209 patients undergoing LRYGB with a minimum 1-year follow-up, reported a 17-% difference when comparing ADA complete remission with Buchwald criteria (40.6 and 57.5 %, respectively). On the other hand, Blackstone et al. [11] reported a T2DM remission rate at 14 months after LRYGB ranging from 43.2 % with combined criteria of A1c <5.7 % plus FPG <100 mg/dl in the absence of hypoglycemic medication to 59.4 % with criteria that only included FPG <100 mg/dl in the absence of hypoglycemic medication.
The present study is the first to highlight the impact of the new ADA complete remission criteria including the time requirement. Its application resulted in a 20-% difference (from 58.1 to 43.6 %) in the T2DM remission rate observed. To achieve ADA complete remission at 2 years, it is mandatory that metabolic control goals be present for at least 12 months. Some studies used the cutoffs for A1C and FPG proposed by the ADA, but they did not include the time criterion, while others did not use it strictly [3, 11–13, 18]. First, Pournaras et al. [12] and Ramos-Levi et al. [18] reported a 1-year follow-up, and thus, the time criterion could not be assessed unless patients were off medication before surgery. Mingrone et al. [3] conducted a 2-year-follow-up study, but the only criterion for remission was withdrawal of hypoglycemic medication for at least 1 year.
There is a growing appreciation for the role of bariatric surgery as a tool in diabetes management. If we are to be able to develop evidence to support recommendations for this procedure in diabetes, we must be able to compare results across studies. In this respect, the findings of the present study highlight the need to define uniform criteria of remission. In our opinion, the ADA criteria offer several advantages over the other definitions. First, the inclusion of a time factor may be critical since T2DM is a chronic disease in which duration is closely related to the onset of complications [19–21]. Second, to define complete and partial remission, it uses the same A1C and FPG cutoff values that are associated with the risk of developing microvascular complications and diabetes [19–23]. Nevertheless, the 5.7-% A1c cutoff value proposed by other authors to define complete remission [11] might be more accurate since previous studies demonstrate a higher risk of T2DM [24] above this value.
It should be remarked that all diabetes remission definitions are focussed on glucose levels, although there is an increasing body of evidence that hyperglycemia is not the only problem and that other factors might be implicated in the development of chronic complications. In this respect, a recent study showed that the isolated mild hyperglycemia seen in maturity-onset diabetes of the young (MODY) type 2 patients, in the absence of other comorbidities, was associated with a low prevalence of chronic complications, suggesting that other factors, besides hyperglycemia, may be implicated in the micro- and macrovascular damage [25].
Besides differences in definition, other factors could also contribute to the different remission rates reported by previous studies. Predictors of T2DM remission after bariatric surgery are known to be those associated with the degree of beta cell dysfunction such as diabetes duration or need for insulin treatment [26–28]. Patients in the present study probably had less severe diabetes than those of the Pournaras study since very few required insulin treatment (2.9 vs 31.9 %), and they had better metabolic control (A1c 6.5 ± 0.7 vs 8.1 ± 1.9 %). These differences in diabetes severity may account for the significant differences in remission rates found in these two studies even when the same criteria were applied (91.2 vs 57.5 % with Buchwald criteria).
As seen from the main studies in bariatric surgery such as the Buchwald meta-analysis [8], the T2DM remission rate currently accepted is around 70 % and thus above the 43.6 % obtained in the present study with the ADA complete remission criteria. Furthermore, it should be taken into account that patients in the present report had shorter disease evolution and better metabolic control compared with most studies. Thus, with the widespread use of this criterion, the accepted remission rate of T2DM will presumably be below 40 %.
Another interesting finding in the present study is that patients undergoing LRYGB achieved diabetes remission earlier after surgery than patients in the LSG group when ADA complete remission criteria was used. These results differ from those described in previous literature where no differences between surgical techniques were detected [9, 29–33]. Although it should be noted that these studies used A1C and FPG cutoff levels similar to ADA partial remission or Buchwald criteria, with which we also found no differences.
From a physiopathological point of view, surgical techniques with a malabsorptive component like LRYGB produce a greater T2DM remission than that obtained after restrictive techniques, such as vertical banded gastroplasty [8, 9]. Furthermore, glucose metabolism improvement occurs soon after the procedure, when significant weight loss has not yet been achieved [29–32]. These findings could be explained by changes in gut hormonal mechanisms, such as increased secretion of incretins that enhance insulin sensitivity [33–35]. On the other hand, in the case of LSG, different hormonal mechanisms have been proposed that could account for the marked improvement in glucose metabolism associated with this technique, similar to that achieved with malabsorptive techniques. LSG includes gastric fundus resection, unlike other restrictive techniques, which causes a decrease in ghrelin concentration, a hormone that produces insulin resistance [33–36]. These different hormonal mechanisms could account for the differences detected between surgical techniques, although further research in this field is needed.
The present study was not without limitations. First, patients were not randomly assigned to the surgical procedure. Second, patients were only followed for 2 years. A longer-term follow-up would allow evaluation of prolonged remission. And finally, patients included in the present study had a short duration of diabetes as reflected in the small number requiring insulin treatment and the fair metabolic control; therefore, the results found cannot be extrapolated to the whole diabetic population.
Conclusions
Use of various definitions can yield significant differences in T2DM remission rates after bariatric surgery. If we are to be able to develop evidence to support recommendations for this procedure in diabetes, we must be able to compare results across studies, and use of universal criteria is mandatory. No differences were observed between LRYGB and LSG in the T2DM remission rate with different criteria, although, using ADA complete remission criteria, remission was obtained earlier after LRYGB.
References
Whiting DR, Guariguata L, Weil C, et al. IDF diabetes atlas: global estimates of the prevalence of diabetes for 2011 and 2030. Diabetes Res ClinPract. 2011;94(3):311–21.
Dixon JB, le Roux CW, Rubino F, et al. Bariatric surgery for type 2 diabetes. Lancet. 2012;379(9833):2300–11.
Mingrone G, Panunzi S, De Gaetano A, et al. Bariatric surgery versus conventional medical therapy for type 2 diabetes. N Engl J Med. 2012;366(17):1577–85.
Schauer PR, Kashyap SR, Wolski K, et al. Bariatric surgery versus intensive medical therapy in obese patients with diabetes. N Engl J Med. 2012;366(17):1567–76.
Look AHEAD Research Group, Wing RR, Bolin P, et al. Cardiovascular effects of intensive lifestyle intervention in type 2 diabetes. N Engl J Med. 2013;369(2):145–54.
American Diabetes Association. Standards of medical care in diabetes. Diabetes Care. 2012;35 Suppl 1:S11–63.
Buchwald H, Oien DM. Metabolic/bariatric surgery worldwide 2011. Obes Surg. 2013;23(4):427–36.
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292(14):1724–37.
Abbatini F, Rizzello M, Casella G, et al. Long-term effects of laparoscopic sleeve gastrectomy, gastric bypass, and adjustable gastric banding on type 2 diabetes. Surg Endosc. 2010;24(5):1005–10.
Buse JB, Caprio S, Cefalu WT, et al. How do we define cure of diabetes? Diabetes Care. 2009;32(11):2133–5.
Blackstone R, Bunt JC, Cortés MC, et al. Type 2 diabetes after gastric bypass: remission in five models using HbA1c, fasting blood glucose, and medication status. Surg Obes Relat Dis. 2012;8(5):548–55.
Pournaras DJ, Aasheim ET, Søvik TT, et al. Effect of the definition of type II diabetes remission in the evaluation of bariatric surgery for metabolic disorders. Br J Surg. 2012;99(1):100–3.
Ramos-Levi AM, Cabrerizo L, Matía P, et al. Which criteria should be used to define type 2 diabetes remission after bariatric surgery? BMC Surg. 2013;13:8.
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122(3):248–56.
Hubbard VS, Hall WH. National Institutes of Health Consensus Development Conference draft statement on gastrointestinal surgery for severe obesity. Obes Surg. 1991;1(3):257–65.
Genuth S, Alberti KG, Bennett P, et al. Follow-up report on the diagnosis of diabetes mellitus. Diabetes Care. 2003;26(11):3160–7.
Chobanian AV, Bakris GL, Black HR, et al. The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA. 2003;289(19):2560–72.
Ramos-Levi AM, Sanchez-Pernaute A, Cabrerizo L, et al. Remission of type 2 diabetes mellitus should not be foremost goal after bariatric surgery. Obes Surg. 2013;23(12):2020–5.
Patel A, MacMahon S, Chalmers J, et al. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med. 2008;358(24):2560–72.
The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993;329(14):977–86.
Stratton IM, Adler AI, Neil HA, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ. 2000;321(7258):405–12.
Zhang X, Gregg EW, Williamson DF, et al. A1C level and future risk of diabetes: a systematic review. Diabetes Care. 2010;33(7):1665–73.
Selvin E, Steffes MW, Zhu H, et al. Glycated hemoglobin, diabetes, and cardiovascular risk in nondiabetic adults. N Engl J Med. 2010;362(9):800–11.
Ackermann RT, Cheng YJ, Williamson DF, et al. Identifying adults at high risk for diabetes and cardiovascular disease using hemoglobin A1c National Health and Nutrition Examination Survey 2005–2006. Am J Prev Med. 2011;40(1):11–7.
Steele AM, Shields BM, Wensley KJ, et al. Prevalence of vascular complications among patients with glucokinase mutations and prolonged, mild hyperglycemia. JAMA. 2014;311(3):279–86.
Dixon JB, Chuang LM, Chong K, et al. Predicting the glycemic response to gastric bypass surgery in patients with type 2 diabetes. Diabetes Care. 2013;36(1):20–6.
Hamza N, Abbas MH, Darwish A, et al. Predictors of remission of type 2 diabetes mellitus after laparoscopic gastric banding and bypass. Surg Obes Relat Dis. 2011;7(6):691–6.
Lee WJ, Chong K, Chen JC, et al. Predictors of diabetes remission after bariatric surgery in Asia. Asian J Surg. 2012;35(2):67–73.
Jiménez A, Casamitjana R, Flores L, et al. Long-term effects of sleeve gastrectomy and Roux-en-Y gastric bypass surgery on type 2 diabetes mellitus in morbidly obese subjects. Ann Surg. 2012;256:1023–9.
Vidal P, Ramón JM, Goday A, et al. Laparoscopic gastric bypass versus laparoscopic sleeve gastrectomy as a definitive surgical procedure for morbid obesity. Mid-term results. Obes Surg. 2012;23:292–9.
Kehagias I, Karamanakos SN, Argentou M, et al. Randomized clinical trial of laparoscopic Roux-en-Y gastric bypass versus laparoscopic sleeve gastrectomy for the management of patients with BMI < 50 kg/m2. Obes Surg. 2011;21:1650–6.
Yang X, Yang G, Wang W, et al. A meta-analysis: to compare the clinical results between gastric bypass and sleeve gastrectomy for the obese patients. Obes Surg. 2013;23:1001–10.
Peterli R, Wölnerhanssen B, Peters T, et al. Improvement in glucose metabolism after bariatric surgery: comparison of laparoscopic Roux-en-Y gastric bypass and laparoscopic sleeve gastrectomy: a prospective randomized trial. Ann Surg. 2009;250(2):234–41.
Karamanakos SN, Vagenas K, Kalfarentzos F, et al. Weight loss, appetite suppression, and changes in fasting and postprandial ghrelin and peptide YY levels after Roux-en-Y gastric bypass and sleeve gastrectomy: a prospective, double blind study. Ann Surg. 2008;247(3):401–7.
Ramón JM, Salvans S, Crous X, et al. Effect of Roux-en-Y gastric bypass vs sleeve gastrectomy on glucose and gut hormones: a prospective randomised trial. J Gastrointest Surg. 2012;16(6):1116–22.
Tschöp M, Smiley DL, Heiman ML. Ghrelin induces adiposity in rodents. Nature. 2000;407(6806):908–13.
Conflict of Interest
The authors have no conflict of interest to declare.
Author information
Authors and Affiliations
Consortia
Corresponding author
Rights and permissions
About this article
Cite this article
Mas-Lorenzo, A., Benaiges, D., Flores-Le-Roux, J.A. et al. Impact of Different Criteria on Type 2 Diabetes Remission Rate After Bariatric Surgery. OBES SURG 24, 1881–1887 (2014). https://doi.org/10.1007/s11695-014-1282-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-014-1282-2