Abstract
Bisphenol A (BPA) is a major environmental pollutant and food contaminant with endocrine-disrupting effects on human and animal health. Perinatal and developmental exposure to BPA has been known to cause hepatotoxicity in adulthood. However, its intergenerational effects in a metabolically challenged population have been scarcely investigated. Our study was designed to assess the intergenerational effect of an environmentally relevant dose of BPA and diet-induced parental obesity on the hepatic health outcome of F1 offspring. Wistar rats were given a high-fat diet to induce obesity, followed by chronic low dosages of BPA (10 ppm × 180 days) in drinking water. Post-treatment, rats were crossed within groups to obtain the F1 generation. Weanling pups were observed for weight gain, levels of hepatic antioxidants, liver function enzymes, cholesterol, C-reactive protein, and triglyceride in the serum. Histological changes in the liver tissue were also investigated. mRNA expression of energy homeostasis genes (FTO and MCR-4) in the liver was analyzed alongside blood biomarkers. We observed higher birth weight and rapid weight gain in the test group in comparison with controls, which was consistent with the changes in mRNA and protein expression of FTO and MCR-4. BPA caused a significant, treatment-related change in the inflammatory marker C-reactive protein, lipid peroxidation, antioxidants, and lipid profile. These findings were accompanied by histological changes in the liver tissue characteristic of hepatic steatosis indicating the onset of the non-alcoholic fatty liver disease (NAFLD). Our study offers a link between exposure to BPA in parents and onset of NAFLD in their offspring.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Bisphenol A (BPA) is a polymeric, organic, endocrine-disrupting chemical (EDC) used globally at an industrial scale to produce plastics, liners of epoxy resin aluminum cans, thermal receipts, stabilizers, pesticides, paints, and dental sealants (Hashimoto and Nakamura 2000; Raisuddin and Sharma 2018). It has been detected in food products and various environmental media including air, soil, and water (Hashimoto and Nakamura 2000; Geens et al. 2012; Cwiek-Ludwicka and Ludwicki 2014). It is well known that BPA is absorbed into the blood through the gastrointestinal tract and transported to other tissues (Pottenger et al. 2000). As a result of its biological affinity, BPA has been detected in urine, amniotic fluid, neonatal blood, placenta, cord blood, and breast milk at levels that are identified to be of genetic relevance (Ikezuki et al. 2002; Vandenberg et al. 2010; Shafei et al. 2018; Deceuninck et al. 2015).
Early developmental exposure to BPA is reported to prompt obesity that emerges later in life (Angle et al. 2013; Manikkam et al. 2013; Hoepner 2019). BPA-induced obesity, however, includes other disease phenotypes that incorporate insulin resistance, glucose intolerance, and reproductive health issues such as primordial follicle loss and polycystic ovaries in females, and testis and prostate deformities in males (Alonso-Magdalena et al. 2010; Manikkam et al. 2012; Ma et al. 2019).
Obesity itself is among the greatest public health epidemics of the twenty-first century, with about currently one-third of adults globally classified as being overweight or obese, and the situation is set to worsen by 2030 (Kelly et al. 2008; Stevens et al. 2012; Ng et al. 2014). It has been linked to numerous and diverse health consequences including cardiovascular disease, hepato-biliary disorders, type 2 diabetes mellitus, malignancies, and changes in the expression of genes that regulate the energy homeostasis and adipogenesis (Bell et al. 2010; Acevedo et al. 2013; Fuster et al. 2016; Krashes et al. 2016; Shafei et al. 2018; Malone and Hansen 2019). Children of obese parents are at risk of being obese and developing an array of metabolic disorders later in life (Whitaker et al. 1997; Wang et al. 2017).
Non-alcoholic fatty liver disease (NAFLD) is the most common chronic liver disease prevailing in approximately 20–30% of the adult population across the world (Vernon et al. 2011). Obesity has been directly correlated with NFALD, which is characterized by the accumulation of lipids in the liver and includes a spectrum of histopathological changes such as simple fatty liver, non-alcoholic steatohepatitis (NASH), fibrosis, and ultimately cirrhosis, which may progress to hepatocellular carcinoma (Weinhouse et al. 2014; Hercog et al. 2019). The pathogenesis of NAFLD is closely related to metabolic syndrome and insulin resistance. NAFLD is thought to be the hepatic manifestation of metabolic disorders like obesity, diabetes, and dyslipidemia (El-Serag et al. 2004; Yki-Järvinen 2010; Kumar et al. 2020). Reports also indicate an association of NAFLD with low-grade inflammation in the liver (Rodriguez-Hernandez et al. 2013; Kumar et al. 2020).
Research indicates that prenatal exposure to BPA is also a potential contributor to the onset of metabolic disorders including obesity and type 2 diabetes (Provvisiero et al. 2016; Dunder et al. 2018; Tudurí et al. 2018). Intrauterine exposure to plastics with BPA increases the incidence of male and female reproductive anomalies and obesity (Salian et al. 2009; Manikkam et al. 2012; Manikkam et al. 2013). It has been demonstrated that BPA has a confounding role in obesity of offspring when the parents were exposed to it (Dabeer et al. 2020). Susiarjo et al. (2013) showed the transgenerationally disruptive effect of BPA on the genomic imprinting in the placenta and embryonic tissue of the offspring. Balci et al. (2020) showed that fetal and neonatal exposure to BPA in combination with another EDC di(2-ethylhexyl) phthalate (DEHP) lead to significant testicular histopathological alterations accompanied by increase in apoptosis markers and autophagic proteins in the testicular tissue. Similarity, Manikkam et al. (2013) investigated effects of a mixture of plastic-derived endocrine disruptors such as BPA, and dibutyl phthalate (DBP) on the epigenetic transgenerational inheritance of adult onset disease and associated DNA methylation epimutations in sperms. It was observed the selected EDCs have potential to promote epigenetic transgenerational inheritance of adult onset disease. The interplay of BPA as a known obesogenic EDC and obesity in forthcoming generations is interesting to contemplate. A systemic review with meta-analysis by Wu et al. (2020) concluded that there was a positive correlation between the level of BPA and obesity risk and the dose-response analysis showed that with an increase of 1ng/ml BPA the risk of obesity increased by 11%. Furthermore, a significant interaction of peroxisome proliferator-activated receptor-γ (PPAR-γ) with BPA was reported by Sharma et al. (2018, 2019). Induction of PPAR-γ has been shown to promote obesity in exposed individuals (Shao et al. 2016). Our study aims to evaluate the intergenerational, toxic effect of BPA on weanling F1 offspring of obese parents and its possible role in the early onset of NAFLD.
Materials and methods
Chemicals
BPA, epinephrine, hematoxylin, Ponceau S, sulfosalicylic acid, Trizol reagent, RIPA lysis buffer (#R0278), 1× protease inhibitor cocktail (#I3786), thiobarbituric acid, and Triton X-100 were purchased from Sigma-Aldrich Co. (St. Louis, MO, USA). 1-Chloro-2,4-dinitrobenzene, 5,5′-dithiobis-2-nitrobenzoic acid, acrylamide, bisacrylamide, butylated hydroxytoluene, ethylene-diaminetetraacetic acid (EDTA), eosin, β-mercaptoethanol (BME), nicotinamide adenine dinucleotide phosphate (NADP), oxidized glutathione (GSSG), reduced glutathione (GSH), and tris-hydroxymethyl aminomethane were procured from Sisco Research Laboratories Pvt. Ltd. (Mumbai, India). Orthophosphoric acid (OPA) was purchased from SD Fine Chemicals Ltd. (Ambala, India). FTO and MCR-4 primary antibodies were purchased from Biorbyt (Cambridgeshire, UK). Broad-range, pre-stained protein ladder Page Ruler (#26616), insulin Rat ELISA Kit (# ERINS), Maxima SYBR Green/Fluorscein qPCR Master Mix (2×) (K0241), and Verso cDNA Synthesis kit (AB1453A) were procured from Thermo Scientific (Waltham, MA, USA). Polyvinylidene difluoride (PVDF) membrane was obtained from MDI Membrane Technologies (Ambala, India). Quanti Chrom™ Alkaline Phosphatase Assay Kit, EnzyChrom™ Aspartate Transaminase Assay Kit, and Enzy Chrom™ Alanine Transaminase Assay Kit were procured from BioAssay Systems (San Francisco, USA). The rat C-Reactive Protein/CRP ELISA Kit (RK00195) was manufactured by ABclonal Technology (Woburn, USA). All other chemicals and reagents were of high purity grade and obtained locally from accredited vendors.
Animals
Wistar rats of either sex (weighing 40–60 g) (3–4 weeks age) were obtained from the Central Animal House Facility of the university. The animals were kept under a controlled temperature of 24 ± 3 °C, light-dark cycle of 12–12 h, and had access to food and drinking water ad libitum. Humidity was maintained at 50 ± 3%. All experimental protocols were approved by the Institutional Animal Ethics Committee (Project #1330).
Treatment
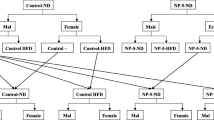
Animals were randomly divided into four groups comprising of six males and six females (n = 12). The experimental design is elaborated on in Fig. 1. Males and females of each group were housed in separate cages and marked duly. Control group (I) was given a standard diet, and those of group II were given a high-fat diet with 40–45% fat added to the standard diet as described by Marques et al. (2015). A detailed composition of each diet is given in Supplementary Material Table 1. Animals of group III were given a standard diet. Animals of group IV were given a high-fat diet to induce obesity. All animals had free access to drinking water (ad libitum). Obesity was induced in 4–5 weeks and was checked using parameters described by Novelli et al. (2007). Thereafter, animals of groups III and IV were given 10 ppm BPA suspended in drinking water to maintain uniformity in terms of age of animals. BPA dosage was decided according to a previous report of Rashid et al. (2009). After 180 days of BPA exposure, one male from each group was randomly assigned to one female from within its group for mating. Post visualization of vaginal plug, females were housed separately for parturition. The pups stayed with their respective mothers until weaning. Six F1 offspring of either sex (n=12) were marked from each group, making sure they were not siblings (to minimize any genetic predisposition to disease). Physical measures were taken at various time intervals. Finally, six pups of either sex (n=12) from each group were sacrificed at postnatal day 21 (PND21) to obtain biological samples. Serum samples and liver tissues were collected for enzyme activity measurement, histological staining, antioxidant analysis, lipid profile analysis, and gene expression analysis.
Necropsy
Necropsy of F1 generation animals was carried out at PND21. All animals were fasted overnight and euthanized under mild anesthesia.
Birth weight and progressive weight gain
F1 offspring were marked duly and weighed weekly. Birth weight (in grams) was taken at PND1 (to minimize maternal rejection) and then weights were measured weekly at PND8, PND15, and PND21.
Tissue and blood sample collection
Blood collected in clot-activator containing tubes was allowed to clot at room temperature for 10 min. Tubes were centrifuged at 1000 × g for 10 min, and serum was aliquoted and stored at −80 °C until further analysis. The liver was excised, washed, and placed in an ice-cold saline solution. A small portion of excised liver was stored in a 10% formalin solution for histopathological studies, and the rest of the sample was flash frozen in liquid nitrogen for biochemical and expression studies.
Biomarker analysis
Assessment of lipid profile was performed by testing the serum samples for concentration of triglycerides (TG), total cholesterol (TC), high-density lipoprotein (HDL), and low-density lipoprotein (LDL). The serum was diluted with a 1× 0.1 M phosphate buffer. HDL analysis was conducted using the Mg2+ precipitation method with phosphotungstic acid as the precipitant. Cholesterol esters in the sample were hydrolyzed to cholesterol and fatty acids. Cholesterol and NAD+ generate cholestenone and NADH in the presence of cholesterol dehydrogenase. WST8 is reduced to formazan dye by diaphorase and NADH through oxidation/reduction reaction. The color intensity of formazan thus formed was measured at 460 nm to calculate cholesterol, HDL, and LDL concentrations. TGs in the sample were hydrolyzed to glycerol and fatty acids by lipoprotein lipase. Glycerol and NAD+ generate dihydroxyacetone and NADH in the presence of glycerol dehydrogenase. WST8 was reduced to formazan dye by diaphorase and NADH through oxidation/reduction reaction. The color intensity of the formazan is proportional to TG concentration and was calculated by measuring it at a wavelength of 460 nm (Manual of Laboratory Operations 1974).
Liver function was assessed by analyzing activities of aspartate aminotransferase (AST), alanine aminotransferase (ALT), and alkaline phosphatase (ALP). AST activity was calculated kinetically in serum samples based on the quantification of oxaloacetate produced by AST. For this assay, oxaloacetate and NADH were converted to malate and NAD by the enzyme malate dehydrogenase. The decrease in NADH absorbance at 340 nm was considered proportionate to AST activity. ALT activity was measured by quantification of pyruvate produced by ALT using serum as substrate. In turn, pyruvate and NADH were converted to lactate and NAD by the enzyme lactate dehydrogenase (LDH). The decrease in NADH absorbance was measured kinetically at 340 nm. ALP activity measured was measured kinetically using p-nitrophenyl phosphate as the substrate. The formation of the resultant yellow product was measured at maximal absorbance of 405nm. The rate of the reaction is directly proportional to the enzyme activity. CRP was measured using a rat-specific enzyme-linked immunosorbent assay (ELISA) as per the manufacturers’ instructions.
Calculation of homeostatic model assessment for insulin resistance (HOMA-IR)
HOMA-IR is a mathematical model for assessment of insulin resistance, calculated using the fasting blood glucose and serum insulin levels. Blood glucose was measured after overnight fasting using a hand-held glucometer at PND21. Serum insulin was measured based on the principle given by Hales and Randle (1963). Sample (25 μl) was added to 100 μl of the enzyme conjugate in each well of a microtiter plate. The solution was incubated at room temperature for 60 min on a horizontal shaker. The samples were discarded, and the wells were washed five times. The plate was dried after the last wash. A TMB solution (200 μl) was added to each well, covered properly, and incubated at room temperature for 15 min. Subsequently, 50 μl of stopping solution was added to each well, and the plate was read at 450 nm immediately.
HOMA-IR was calculated by using the formula given below:
where FG stands for fasting blood glucose and FI stands for fasting serum insulin.
Assessment of oxidative stress
Flash-frozen portions of the liver from various groups were homogenized separately using 1× phosphate buffer (0.1 M, pH 7.4) at 4 °C to make 10% w/v homogenate. A portion of it was aliquoted for assessment of lipid peroxidation (LPO), and the rest was further centrifuged at 4 °C for 30 min at 12,000 × g to obtain post mitochondrial supernatant (PMS) for various biochemical measurements.
LPO
Thiobarbituric acid reactive substances (TBARS) were measured spectrophotometrically by the method of Mihara and Uchiyama (1978), with modification. Briefly, tissue homogenate was mixed with 10 mmol butylated hydroxytoluene (BHT), 0.67% thiobarbituric acid (TBA), and 1% chilled OPA. The mixture was incubated at 90 °C for 45 min. After cooling, the precipitate was removed by centrifugation at 1000 × g for 10 min at room temperature. The absorbance of the supernatant was recorded at 532 nm spectrophotometrically against blanks containing reagents but no sample. The level of LPO was determined using an extinction coefficient of 1.56 × 105, and results expressed as mmol of TBARS formed h-1g-1 tissue.
GSH
GSH, a major free nonenzymatic antioxidant, ubiquitously distributed in cells, was measured using the method of Jollow et al. (1974). Briefly, PMS was mixed with 4% sulfosalicylic acid (SSA) (1:1). The samples were then kept at 4 °C for 1 h and subsequently centrifuged at 4000 ×g for 15 min. Thereafter, 2.2 ml phosphate buffer, 0.4 ml of the supernatant, and 0.4 ml of 10 mM 5,5′-dithiobis (2-nitrobenzoic acid) (DTNB) were mixed, and absorbance was measured at 412 nm. GSH concentration was expressed in μmol of GSH g-1 tissue.
Superoxide dismutase (SOD) activity
SOD activity was measured according to the method of Misra and Fridovich (1972). The method is based on the ability of SOD to inhibit the auto-oxidation of epinephrine at alkaline pH. PMS (0.2 ml) was treated with 0.8 ml of 50 mmol glycine buffer (pH 10.4) and 20 μl epinephrine. SOD activity was measured kinetically at 480 nm. The activity was measured indirectly by the oxidized product of epinephrine, i.e., adrenochrome. SOD activity was expressed as nmoles of (-) epinephrine protected from oxidation min-1mg-1 protein using a molar extinction coefficient of 4020 M-1 cm-1.
Catalase (CAT) activity
CAT activity was measured kinetically on a spectrophotometer by the method of Claiborne (1985). PMS was diluted with 0.1 M 1× phosphate buffer (1:40), and the enzymatic activity was measured kinetically in presence of 1 ml of 0.05 mmol H2O2. The enzymatic activity was expressed as μmol of H2O2 consumed min-1mg-1 tissue using the molar extinction coefficient 39.6 M-1 cm-1 at 240nm.
Glutathione S-transferase (GST) activity
GST activity was measured spectrophotometrically in the PMS of liver tissue by the method of Habig et al. (1974). The reaction mixture consisted of 1.575 ml of 0.1 M sodium phosphate buffer (pH 7.4), 0.2 ml GSH (10 mmol), 0.025 ml (10 mmol) CDNB, and 0.2 ml 10% PMS. The enzyme activity was calculated as nmol of CDNB conjugates formed min-1mg-1 protein using a molar extinction coefficient of 9.6× 103 M-1 cm-1 at 340 nm.
Glutathione reductase (GR) activity
GR activity was assayed by the method of Carlberg and Mannervik (1975), as modified by Mohandas et al. (1984). The reaction mixture consisted of 0.1 M 1× phosphate buffer (pH 7.4), 0.5 mmol EDTA, 1 mmol GSSG, 0.1 mmol NADPH, and 10% PMS in a total volume of 2.0 ml. The enzyme activity was quantitated at 25 °C by measuring the disappearance of NADPH at 340 nm and expressed as nmole NADPH oxidized min-1mg-1 protein using a molar extinction coefficient of 6.22×103 M-1 cm-1.
mRNA expression
Total RNA was isolated from cells using Trizol. Flash-frozen liver samples (50 mg) were homogenized in 1 ml Trizol reagent at 4 °C. A chloroform extraction was performed according to the manufacturers’ instructions. Equal amounts of DNase I treated RNA samples (100 ng) were used to prepare the cDNA library using a Verso cDNA Synthesis Kit (AB1453A) as per the manufacturers’ instructions. Forward and reverse primers for MCR-4 and FTO were used to perform quantitative real-time PCR on the Roche platform using Maxima Sybr Green dye (K0241) as per the manufacturers’ guidelines (Supplementary Table 2). The mRNA level and fold change for each gene compared to control were calculated using the cycle threshold (Ct) and value of the housekeeping gene (β actin) for normalization (Burd 2010). All samples were assayed in duplicate.
Immunoblot analysis of proteins
The flash-frozen liver tissue was homogenized in 1× RIPA lysis buffer with 1× protease inhibitor cocktail in a Potter-Elvehjem homogenizer on ice. The homogenized samples were centrifuged at 10,000 × g for 15 min at 4 °C. Supernatant was preserved for the protein analysis and stored at −80 °C. Protein was quantified by the Bradford method (McCarthy and Nations 1979) at absorbance of 595 nm in a TECAN Infinite M-200 Plate Reader (TECAN Group Ltd., Männedorf, Switzerland) with compatible software (Magellan™ data analysis software version 6.6.0.1; TECAN Group Ltd.). Equal amounts of protein (30–40 μg) with 6× Laemmle loading buffer were electrophoresed using 10% sodium dodecyl sulfate polyacrylamide gel electrophoresis (SDS-PAGE) with SDS running buffer and with reference bands of broad-range, pre-stained protein ladder (Page Ruler, Thermo Scientific). Mini-PROTEAN® Tetra Cell SDS-PAGE gel running unit (Bio-Rad, CA, USA) was used for electrophoresis. Electrophoresed protein was transferred from gel to PVDF membrane in 1× transfer buffer. Membranes carrying the proteins were blocked using 3% (w/v) BSA dissolved in 1× TBST for 1 h to reduce non-specific binding. Later, they were incubated with primary and HRP-conjugated IgG secondary antibodies dissolved in 3% BSA-TBST solution. Proteins were detected with Clarity Western ECL substrate purchased from Bio-Rad in LAS-4000 from Fujifilm (Tokyo, Japan). The density of the protein bands was analyzed by Multi Gauge Image Reader software from Fujifilm.
Histological analysis
Freshly excised liver tissue fixed in 10% neutral formalin was embedded in paraffin to form a block. Sections of 5 μm thickness were cut using a microtome. The paraffin-embedded tissues were de-paraffinized using xylene and ethanol. Slides were washed using 0.1 M PBS and permeabilized with 0.1 M citrate + 0.1% Triton X-100 solution. The de-paraffinized sections were stained with hematoxylin and eosin (HE). Slides were observed at 40 × magnification using a light microscope. To avoid bias, slides were coded and examined by a histopathologist in a blinded manner.
Statistical analysis
Data were expressed as the means ± standard error (SE) and analyzed using analysis of variance (ANOVA) followed by Tukey’s test. P < 0.05 was considered as significant. Statistical analysis was performed using GraphPad Prism 5 software (GraphPad Software Inc., San Diego, CA, USA).
Results
Effect on body weight of F1 offspring
Male offspring of group IV (77.19±2.6 grams) animals showed higher weight gain in comparison with progeny of control I (60.82 ± 1.9 grams; p = 0.0002), group II (62.52 ± 1.9 grams; p = 0.0006), and group III (66.49 ±1.9 grams; p = 0.01) animals (Fig 2a). The average weight gain was highest in female offspring of group IV (71.60 ± 2.0 grams) when compared with the female offspring of groups III (64.39 ± 2.0 grams; p = 0.257), I (52.86 ± 3.5 grams; p = 0.0004) and II (52.25 ± 2.3 grams; p = 0.0003) (Fig 2b). However, no difference was observed in the litter size and sex ratio at birth. Additionally, no pregnancy loss was seen in any of the groups.
Birth weight and progressive weight gain of F1 generation animals. a Male offspring of BPA-exposed obese animals (IV) (77.19 ± 2.6) exhibited higher birth weight and the overall progressive weight gain was significantly higher than offspring of only obese factor (II) (62.52 ± 1.9; ***p = 0.006), only BPA-exposed (III) (66.49 ± 1.9; *p = 0.01), and control (I) (60.82 ± 1.9; ***p = 0.0002) animals. Weight gain trend changes were not significant among males of groups I and II (p = 0.943), I and III (p = 0.276) and groups II and III (p = 0.572). b Female offspring of BPA-exposed obese (IV) (71.60 ± 2.0) (***p = 0.0004; &&&p = 0.003) and only BPA-exposed (III) (64.39 ± 2.4 grams) (*p = 0.0295; &p = 0.209) animals exhibited significantly higher progressive weight gain through PND1-21 when compared with the female offspring of sham control (I) (52.86 ± 3.5) and obese (II) animals (52.25 ± 2.3). No significant difference was found among groups I and II (p = 0.995) and III and IV (p = 0.257). Data are shown as means ± SE (n = 6 of either sex). Weights are expressed in grams; PND, postnatal day; SE, standard error
Disturbance in liver function
Male offspring of only group IV (128.1 ± 5.4 U/l) showed a statistically significant increase in AST activities when compared with male offspring of control group I (82.22 ± 0.5 U/l; p = 0.001) (Fig 3a). Offspring of group II (102.8 ± 11.93 U/l; p = 0.862) and III (101.6 ± 5.3 U/l; p = 0.678) parents did not show any significant differences in AST activity levels when similarly compared. Female offspring of groups III (103.5 ± 4.0 U/l; p = 0.046) and IV (136.7 ± 5.7 U/l; p = 0.001) but not group II (99.9 ± 5.5 U/l; p = 0.102) showed significant increase in AST activities when compared with control I (80.13 ± 3.5 U/l) animals (Fig 3b). The levels of ALT were not significantly differed among both male (I: 47.75 ± 3.1 U/l, II: 59.98 ± 3.3 U/l, III: 53.87 ± 4.5 U/l, and IV: 60.22 ± 5.9 U/l) and female (I: 44.61 ± 2.5 U/l, II: 52.02 ± 2.6 U/l, 57.5 ± 2.4 U/l, and IV: 57.68 ± 2.6 U/l) (p > 0.05) offspring (Fig 3c and d).
Assessment of liver function enzymes aspartate aminotransferase (AST) and alanine aminotransferase (ALT) in weanling F1 generation animals. a Male offspring of BPA-exposed obese animals (IV) (128.1 ± 5.4; ***p = 0.001) exhibited a significant increase in serum AST when compared with the offspring of sham control (I) (82.22±0.5) animals at PND21. The male offspring of obese (II) (102.8 ± 11.9; p = 0.022) and BPA-exposed (III) (101.6 ± 5.3; p = 0.246) groups did not show any statistically significant change in AST when compared with sham control (I) and among each other (p = 0.993) at PND21. b Female offspring of only obese (II) (99.9 ± 5.5; *p=0.012), only BPA-exposed (III) (103.5 ± 4.0; *p = 0.046), and BPA-exposed obese (IV) (136.7 ± 5.7; ***p = 0.001) parents showed statistically significant increase in serum AST when compared with female offspring of sham control (I) (80.13 ± 3.5) animals. c ALT levels in the samples of male offspring of control group (I) (47.75 ± 3.1), obese (II) (59.98 ± 3.3), BPA-exposed (III) (53.87 ± 4.5), and BPA-exposed obese (IV) (60.22 ± 5.9) animals did not show statistically significant variation when compared among groups (p > 0.05) at PND21. d ALT in the samples of female offspring of sham control (I) (44.61 ± 2.5), obese (II) (52.02 ± 2.6), BPA-exposed (III) (57.50 ± 2.4), and BPA-exposed obese (IV) (57.6 ± 2.6) animals did not show any statistically significant change when compared among groups (p > 0.05) at PND21. Data are shown as means ± SE (n = 6 of either sex). AST and ALT levels are expressed in units per liter; PND, postnatal day; SE, standard error; AST, aspartate aminotransferase; ALT, alanine aminotransferase.
Serum ALP activity levels in samples obtained from male offspring of group IV (231.2 ± 14.1 U/l; p = 0.001) were increased significantly when compared with group I (153.8 ± 13.5 U/l). However, this was not the case with animals of groups II (182.0 ± 8.2 U/l; p = 0.413) and III (180.9 ± 14.2 U/l; p = 0.447). Similar findings were observed in female offspring, when groups I (205.9 ± 5.2 U/l; p = 0.001), II (221.9 ± 8.9 U/l; p = 0.001), and III (235.8 ± 12.96 U/l; p = 0.025) were compared with animals of group IV (265.4±12.53 U/l) (Fig 4a and b). The pro-inflammatory cytokine CRP levels in male offspring of group IV (430.4 ± 18.2 μg/l) were significantly higher than males of groups III (306.6 ± 3.3 μg/l; p < 0.0001), II (335.4 ± 8.3 μg/l; p < 0.0001), and I (258.9 ± 2.1 μg/l; p < 0.0001). CRP levels were similarly increased in females of groups IV (335.6 ±6.9 μg/l; p < 0.0001), III (298.2 ± 9.2 μg/l; p < 0.0001), and II (306.5 ± 4.5 μg/l; p < 0.0001) when compared with female offspring of control group I (239.2 ± 4.0 μg/l) (Fig 4 and b).
Effect on alkaline phosphatase (ALP) and pro-inflammatory cytokine C-reactive protein (CRP) in F1 generation animals at PND21. a Male offspring of BPA-exposed obese (IV) (231.2 ± 14.1) animals showed significant increase in serum ALP when compared with sham control (I) (153.8 ± 13.05; **p = 0.001) and only BPA-exposed (III) (180.9 ± 14.1; *p = 0.0482) male offspring at PND21. However, no statistically significant variations in serum ALP were observed among other groups (p > 0.05) PND21. b ALP levels in samples of female offspring of BPA-exposed obese (IV) (265.4 ± 12.53) showed a statistically significant increase when compared with samples of control (I) (205.9 ± 5.2; **p = 0.001), obese (II) (204.9 ± 6.0; **p = 0.001), and only BPA exposed (III) (222.7 ± 12.31; *p = 0.025). However, no significant variation in ALP levels was seen among only groups I, II, and III that were at PND21. c Male offspring of sham control (I) (258.9 ± 2.1) animals showed significantly lower CRP levels when compared with offspring of obese (335.4 ± 8.3; **p = 0.0002), BPA-exposed (III) (306.6 ± 3.3; *p = 0.017), and BPA-exposed obese (IV) (430.4 ± 18.2; ***p < 0.0001) animals at PND21. CRP levels in animals of group (IV) (***p < 0.0001) were significantly higher than those of groups II and III on PND21. d Female offspring of sham control (I) (239.2 ± 4.0; ***p < 0.0001) animals showed significantly lower CRP levels when compared with offspring of obese (306.5 ± 4.5), BPA-exposed (III) (298.2 ± 9.2), and BPA-exposed obese (IV) (335.6 ± 6.9) animals at PND21. CRP levels in females of group (IV) were significantly higher than those of groups II (&p = 0.002) and III (&&p = 0.0002) on PND21. Data are shown as means ± SE (n = 6 of either sex). ALP levels are expressed in units per liter; CRP levels are expressed in micrograms per liter. ALP, alkaline phosphatase; CRP, C-reactive protein; PND, postnatal day; SE, standard error.
Development of insulin resistance
At PND21, both male and female (p < 0.001) offspring of group II (M: 0.536 ± 0.02; F: 0.514 ± 0.02), III (M: 0.300 ± 0.0; F: 0.240 ± 0.0), and IV (M: 0.467 ± 0.0; F: 0.877 ± 0.0) animals showed an increase in the HOMA-IR index when compared with their respective control (I) (M: 0.293 ± 0.01; F: 0.283 ± 0.0) animals (Fig 5a and b).
Homeostatic model assessment for insulin resistance at PND21. a Male offspring of obese (II) (0.536 ± 0.02), BPA-exposed (III) (0.300 ± 0.01), and BPA-exposed obese (IV) (0.467 ± 0.01) animals exhibited increased levels of HOMA-IR when compared with control (I) (0.29 ± 0.007) (***p < 0.0001) animals. HOMA-IR levels showed significant variations when compared among groups II, III, and IV (***p < 0.0001). b Female offspring of obese (II) (0.514 ± 0.02), BPA-exposed (III) (0.240 ± 0.01), and BPA-exposed obese (IV) (0.877 ± 0.03) animals exhibited increased levels of HOMA-IR when compared with control (I) (0.28 ± 0.007) (***p < 0.0001) animals. HOMA-IR levels showed significant variations when compared among groups II, III, and IV (***p < 0.0001). Data are shown as means ± SE (n = 6 of either sex). HOMA-IR, homeostatic model assessment for insulin resistance; PND, postnatal day; SE, standard error
Disruption of lipid homeostasis
Serum cholesterol levels in male and female offspring of BPA-exposed obese (IV) animals (M: 221.3 ± 5.4; F: 138.2 ± 5.7 mg/dl) were significantly higher when compared to the respective control (I) group (M:73.6 ± 1.6; F: 81.8 ± 5.2 mg/dl; p<0.0001). However, increase in cholesterol levels of males of groups II (171.8 ± 7.0 mg/dl; p<0.0001) and III (111.0 ± 1.8 mg/dl; p=0.0002) was statistically more pronounced than respective females (II: 108.6 ± 5.1mg/dl; p=0.036) (III: 97.4 ± 1.4 mg/dl; p=0.13) when compared with their controls (I) (Fig 6a and b). Serum TG levels of group IV animals (M: 117.8 ± 3.1; F: 138.2 ± 5.7) were significantly increased when compared with animals of group III (M: 103.40±2.8 mg/dl; p=0.02) (F: 97.40±1.4 mg/dl; p<0.0001) and respective control (I) animals (M: 91.60 ± 2.6 mg/dl; F: 69.80 ± 0.8 mg/dl) (p<0.0001). However, only female offspring of group II (M: 116.60 ± 3.5; F: 108.6 ± 5.1 mg/dl) had significantly lower levels of TG when compared to group IV (Fig 6c and d). Serum HDL levels of group IV animals (M:15.8±1.6 mg/dl; F:15.4±1.7 mg/dl) and II (M:21.4±1.2 mg/dl; F:21.2±0.9 mg/dl) were significantly lower than their respective controls (M:28.2±1.2 mg/dl; F:25.6±1.2 mg/dl) and group III counterparts (M:23.2±1.7 mg/dl; F:20.6±1.6 mg/dl) (Fig. 7a and b). Serum LDL levels of group IV animals (M: 54.6±2.1 mg/dl; F:52.2±7) were significantly higher when compared with their respective controls (M:34.62±1.8 mg/dl; F:34.6±1.5 mg/dl). However, only males of group IV showed significant increase in LDL levels over their group II (46.2±2.6 mg/dl) and III (39.0±1.3 mg/dl) (Fig. 7c and d).
Changes in serum cholesterol and triglycerides (TG) of weanling F1 generation animals. a Male offspring of only obese (II) (171.8 ± 7.0; ***p = 0.001), only BPA-exposed (III) (111.0 ± 1.8; **p = 0.002), and BPA-exposed obese (IV) (221.3 ± 5.4; ***p < 0.0001) animals exhibited significant increase in cholesterol levels when compared with sham control (I) (73.60 ± 1.6). However, group II and III animals had significantly lower cholesterol levels when compared with group IV (&&&p < 0.0001). b Female offspring if obese (II) (108.6 ± 5.1; *p = 0.036) and BPA-exposed obese (IV) (138.2 ± 5.1; **p = 0.005) animals exhibited significant increase in cholesterol levels. Significant variation was also seen in females of group III (97.40±1.4; &p=0.02) and group IV. c Male offspring of control (I) (91.60 ± 2.6; ***p < 0.0001) and BPA-exposed (III) (103.40 ± 2.8; &p = 0.0205) animals had significantly lower levels of serum TG when compared with male offspring of BPA-exposed obese (IV) (117.8 ± 3.1) animals. Significant decrease was also observed in serum TG levels among group I (**p = 0.002) when compared with group II (116.6 ± 3.5). d Female offspring if obese (II) (108.6 ± 5.1; *p = 0.02) and BPA-exposed obese (IV) (138.2 ± 5.7; p < 0.0001) animals exhibited significant increase in serum TG levels when compared with control (I) (69.80 ± 0.8). Serum TG levels in group IV animals were also significantly higher than group III (###p < 0.0001) and group II (&&p = 0.002). Data are shown as means ± SE (n = 6 of either sex). Cholesterol and TG levels are expressed in milligrams per deciliter; TG, triglycerides; PND, postnatal day; SE, standard error
Alterations in high-density lipoprotein (HDL) and low-density lipoprotein (LDL) of F1 generation at PND21. a Male offspring of only obese (II) (21.4 ± 1.2; *p = 0.026) and BPA-exposed obese (IV) (15.8 ± 1.6; **p = 0.01) animals exhibited significant increase in HDL levels when compared with sham control (I) (28.20±1.2). Group IV animals also had significantly lower serum HDL levels when compared to only BPA exposed (III) (23.20 ± 1.7; &p = 0.014). b Female offspring of obese (II) (21.20 ± 0.9; *p = 0.049), only BPA-exposed (III) (20.60 ± 1.6; *p = 0.0431), and BPA-exposed obese (IV) (15.40 ± 1.7; ***p = 0.0005) animals exhibited significant decrease in serum HDL levels when compared with control (I) (25.6 ± 1.2). c Male offspring of only obese (II) (46.20 ± 2.6; **p = 0.005) and BPA-exposed obese (IV) (54.60 ± 2.1; ***p < 0.0001) animals exhibited significant increase in LDL levels when compared with control (I) (34.60 ± 1.8) animals. Serum LDL in group IV animals was also significantly higher than group II (p = 0.047) and group III animals (p= 0.0003). d Female offspring of BPA-exposed obese (IV) (52.20 ± 2.7) animals only showed significantly increased serum LDL levels when compared with control (I) (34.60±1.8; ***p = 0.0003). No significant variations were observed among group II (45.40 ± 2.8) and III (45.80 ± 1.8) animals. Data are shown as means ± SE (n = 6 of either sex). HDL and LDL are expressed in milligrams per deciliter. HDL, high-density lipoprotein; LDL, low-density lipoprotein; PND, postnatal day; SE, standard error
Lipid peroxidation and alteration in antioxidant profile
We checked non-enzymatic and enzymatic antioxidants in the tissue samples of all groups. Mean levels of non-enzymatic antioxidant assays and antioxidant enzymes in male offspring are given in Table 1, and female offspring are shown in Table 2. All values are expressed in mean and standard error mean. Overall, male and female offspring of groups IV had significantly decreased antioxidant enzymatic activity levels when compared with respective control (I) animals. Although the hepatic GSH content was decreased in all groups, the effect was most pronounced in male and female animals of group IV (p < 0.0001). Hepatic lipid peroxidation was most pronounced in males of group IV followed by females of group IV when compared with animals of other groups (Tables 1 and 2).
Change in mRNA expression
Quantitative RT-PCR analysis showed a significant decrease in fold change of MCR-4 mRNA expression in male offspring of only group IV (0.278 ± 0.03; p = 0.013) but not groups II (0.568 ± 0.06; p= 0.13) and III (0.837 ± 0.2; p = 0.788) (Fig 8a). Additionally, female offspring of all groups, i.e., II (0.313 ± 0.01; p < 0.001), III (0.637 ± 0.09; p = 0.003), and IV (0.0634 ± 0.01; p < 0.001), showed statistically significant decrease in fold change of MCR-4 mRNA expression (Fig 8b) when compared with sham control (I) animals. Numerically, the fold change decrease was most prominent in the samples of group IV. Fold change in FTO mRNA expression in samples of male offspring of group II (2.810 ± 0.15; p = 0.0006) and IV (4.17 ± 0.3; p < 0.001) was significantly increased when compared with offspring of the control (I) group (Fig 8c). However, this increase was also seen in the F1 females of groups II (2.806 ± 0.2; p = 0.009) and IV (3.793 ± 0.3; p = 0.006) (Fig 8d).
Changes in mRNA expression of MCR-4 and FTO gene of weanling F1 generation progeny. a Twenty-one-day-old male offspring of BPA-exposed obese (IV) (0.27 ± 0.03; *p = 0.013) showed a statistically significant decrease in mRNA expression of MCR-4 gene when compared with control (I). However, no significant change in mRNA expression of MCR-4 gene was seen in F1 generation of only obese (II) (0.56 ± 0.06) and only BPA-exposed (III) (0.83 ± 0.2) animals at PND21. b Female offspring of only obese (II) (0.31 ± 0.01; ***p < 0.0001), only BPA-exposed (III) (0.063 ± 0.09; ***p = 0.003), and BPA-exposed obese (IV) (0.063 ± 0.01; ***p < 0.001) animals exhibited statistically significant decrease in fold change of MCR-4 mRNA expression at PND21. c Male F1 progeny of BPA-exposed obese (IV) (4.18 ± 0.3) animals exhibited a statistically significant increase in fold change of FTO gene mRNA expression when compared with offspring of control (I) (***p < 0.0001), obese (II) (2081 ± 0.1; **p = 0.003), and BPA-exposed (III) (1.3 ± 0.01; ***p < 0.0001). Males of group II also had significantly higher mRNA expression of FTO gene when compared with groups (I) (&&&p = 0.0006) and (III) (##p = 0.002). d Female F1 progeny of BPA-exposed obese (IV) (3.79 ± 0.3) animals exhibited a statistically significant increase in fold change of FTO gene mRNA expression when compared with control (I) (**p = 0.009) and BPA-exposed (III) (1.63 ± 0.3; **p = 0.003). Data are shown as means ± SE (n = 6 of either sex). MCR-4, melanocortin receptor 4; FTO, fat mass obesity-related gene; mRNA, messenger ribonucleic acid; PND, postnatal day; SE, standard error
Changes in protein expression
Densitometric analysis of MCR-4 and FTO proteins in western blot analysis revealed similar results in both male and female progenies. Offspring of all groups expressed statistically significant changes over the control (I) group. Numerically, the decrease in the protein density of MCR-4 in offspring of group IV animals was most pronounced. A significant increase in FTO protein concentration was found in offspring of groups II and IV when compared with sham control (I) progenies (Fig 9).
Densitometric analysis to assess the effect on protein expression of MCR-4 and FTO. a Male F1 offspring of only obese (II) (***p < 0.001), only BPA-exposed (III) (***p < 0.001), and BPA-exposed obese (IV) (***p < 0.001) animals exhibited statistically significant decrease in MCR-4 protein expression when compared with control (I) group at PND21. b Female F1 offspring of only obese (II) (***p < 0.001), only BPA-exposed (III) (***p < 0.001), and BPA-exposed obese (IV) (***p < 0.001) animals exhibited statistically significant decrease in MCR-4 protein expression when compared with control (I) group at PND21. c Male F1 offspring of only obese (II) (***p < 0.001), only BPA-exposed (III) (**p < 0.01), and BPA-exposed obese (IV) (***p < 0.001) animals exhibited statistically significant increase in FTO protein expression when compared with control (I) group at PND21. d Female F1 offspring of only obese (II) (**p < 0.01), only BPA-exposed (III) (**p < 0.01), and BPA-exposed obese (IV) (***p < 0.001) animals exhibited statistically significant increase in FTO protein expression when compared with control (I) group at PND21. e Western blots expressing β actin, MCR-4, and FTO protein in male and female weanling F1 generation animals of control (I), only obese (II), only BPA-exposed (III), and BPA-exposed obese (IV) animals. Data are shown as means ± SE (n = 6 of either sex). MCR-4, melanocortin receptor 4; FTO, fat mass obesity-related gene; mRNA, messenger ribonucleic acid; PND, postnatal day; SE, standard error
Manifestations of fatty liver hallmarks in liver histology
The liver tissue samples obtained from offspring of obese (II) animals showed mild central vein, mononuclear infiltration of portal vein, and sinusoidal congestion. Offspring of BPA exposed (III) exhibited mild hepatic sinusoidal congestion but normal hepatocellular parenchyma. However, offspring of BPA-exposed obese (IV) animals exhibited most signs of hepatotoxicity including periportal congestion, fatty degeneration of hepatocytes, lipid vacuolation, and portal vein hyperplasia (Figs. 10 and 11).
Histological changes in liver tissue of male F1 generation animals at PND21. I) Normal hepatocellular parenchyma with normal sinusoidal spaces; II) mild central vein congestion, mild sinusoidal congestion; III) mild sinusoidal congestion, normal hepatocellular parenchyma; IV) periportal congestion, hepatocytes showing fatty degeneration, portal vein hyperplasia. PV, portal vein; CV, central vein; A, vein congestion; B, sinusoidal congestion; C, hepatocyte degeneration; D, fatty degeneration of hepatocytes (lipid deposition); E, mononuclear infiltration. All images were taken at 40× magnification.
Histological changes in liver tissue of female F1 generation animals at PND21. I) Normal hepatocellular parenchyma with normal sinusoidal spaces and central vein; II) portal vein congestion, sinusoidal congestion, mononuclear cell infiltration; III) mild hepatocellular degeneration with normal central vein; IV) fatty degeneration of hepatocytes (hepatocyte showing micro vacuolation), narrowing of sinusoidal lumen, sinusoidal congestion, periportal congestion. PV, portal vein; CV, central vein; A, vein congestion; B, sinusoidal congestion; C, hepatocyte degeneration; D, fatty degeneration of hepatocytes (lipid deposition); E, mononuclear infiltration. All images were taken at 40× magnification.
Discussion
BPA exposure in humans has increased down the generations due to its excessive production and use in various activities. Exposure to BPA in humans and animals is caused by its leaching in ground water, food supplies, and medical devices (Hashimoto and Nakamura 2000; Geens et al. 2012; Cwiek-Ludwicka and Ludwicki 2014). Studies have unanimously concluded a potential role for long-term exposure to BPA in liver disorders, diabetes, cancer, and cardiometabolic disorders (Nakagawa and Tayama 2000; Yang et al. 2009; Alonso-Magdalena et al. 2010; Shafei et al. 2018; Shu et al. 2019). We found that the body weight of offspring with parental obesity and low-dose BPA exposure was significantly higher than their respective counterparts. BPA has shown opposing effects on birth weight with various levels of exposure. High-dose BPA exerts weight-reducing effects (Kim et al. 2001). However, low-dose exposure leads to weight gain (Vandenberg et al. 2012; Angle et al. 2013; Kobroob et al. 2018; Dabeer et al. 2020). Results of the present study succeed as a step further by providing a strong connection of perinatal BPA exposure with liver disease in F1 generations. NAFLD is histologically defined by the presence of steatosis in hepatocytes, regardless of whether it is macro-vesicular, mixed, or micro-vesicular (Kleiner et al. 2005). In previous studies, high-fat diet (HFD) was used to induce fatty liver changes, metabolic syndrome, dyslipidemia, obesity, and insulin resistance (Fellmann et al. 2013; Takahashi et al. 2012). However, our approach was more environmentally relevant as combined effect of parental exposure to low-dose parental BPA exposure in conjunction with HFD was investigated. The offspring of all groups were without BPA exposure and fed a normal diet; hence, any toxicity could directly be ascribed to intra-/transgenerational effects of parental BPA exposure scenario. We investigated, step by step, the previously established hallmarks of hepatotoxicity to understand and analyze the extent of intergenerational effects of parental obesity and BPA exposure in F1 offspring.
Birth weight and progressive weight gain in neonates are the primary indicators of neonatal health. Children of obese parents are at a higher risk of developing metabolic disorders later in life (Whitaker et al. 1997; Wang et al. 2017). The F1 offspring of test group (IV) and obese parent group (II) had significantly higher body weight at birth. However, progressive weight gain from PND1-21 was highest in test group pups, which indicates higher predisposition to development of metabolic disorders including obesity and diabetes.
The liver is the primary organ for glucose metabolism and maintenance of glucose and lipid homeostasis. A disrupted lipid homeostasis may lead to adipogenesis due to disorderly energy homeostasis (Bell et al. 2010; Acevedo et al. 2013; Fuster et al. 2016; Malone and Hansen 2019; Krashes et al. 2016). Evaluation of liver-specific biochemical markers revealed an imbalance in liver-specific enzyme levels among group IV offspring. Increased AST levels accompanied by high ALP and pro-inflammatory cytokine CRP clearly indicate liver damage and inflammation. Our findings support the results of previous studies showing compromised status of antioxidants leading to liver tissue damage (Li et al. 2015; Li et al. 2016; Liu et al. 2016). Studies have reported on the intra-/transgenerational effects of parental obesity and chronic parental BPA exposure on cardiovascular health via disruption of fatty acid and glucose metabolism (Dunder et al. 2018; Shu et al. 2019).
Blood glucose and serum insulin are strong indicators of hepatic health as well. A disruption in ratio of glucose and insulin can result in development of metabolic disorders such as diabetes and insulin resistance. We calculated insulin resistance by the mathematical model HOMA-IR. Female offspring exhibited a higher level of insulin resistance than their male counterparts. This result is also in line with the previous findings showing that glucose metabolism is different in females and males (Dabeer et al. 2020). Scientists have established that insulin is the primary stimulator of hepatic lipogenesis acting through activation of the sterol regulatory element-binding protein-1c (SREBP-1c) transcription factor (Ferré and Foufelle 2007). Insulin resistance is found in most patients with primary NAFLD and is more severe in NASH (Valenti et al. 2002). It is evident from the findings of this study that perinatal exposure to low-dose BPA is associated with increased insulin resistance accompanied by hepatic steatosis.
An analysis of antioxidants in the liver tissue revealed decreased antioxidant enzyme activity in F1 offspring of BPA-exposed obese parents, clearly indicating oxidative, stress-induced hepatotoxicity. Previously, Kumar et al. (2020) have reported a strong association between CRP level and NAFLD. Data from our study are in conformity with those findings. Offering a conclusive role for disruption of antioxidants not only in BAP-induced hepatotoxicity but in other toxicities such as neurotoxicity and endocrine toxicity, there are reports on a protective effect of compounds and herbal extract with proven antioxidant properties (Khan et al. 2018; Mohammed et al. 2020).
Development of sophisticated techniques has facilitated our understanding of the melanocortinergic network and identified its role in regulation of feeding behavior, energy expenditure, glucose homeostasis, and autonomic outflow (Krashes et al. 2016). We specifically inspected the expression of the MCR-4 receptor as it is a critical coordinator in mammalian energy homeostasis and regulation of body weight, and its down-regulation has been shown to cause an increase in body weight, leading to obesity (Huszar et al. 1997; Krashes et al. 2016). Offspring of BPA-exposed obese animals exhibited a 2-fold or more decrease in MCR-4 expression depicting a down-regulation of the gene. Additionally, female offspring exhibited greater decrease when compared with their male counterparts in treatment groups. These results similarly translated to the protein expression of MCR-4. The other gene we inspected was FTO gene. It is an example of a regulatory “master switch” gene that influences control over several key regulatory pathways in weight gain and obesity regulation. It has also been correlated with metabolic syndrome and diabetes risk (Bell et al. 2010; Merkestein and Sellayah 2015). The offspring of group IV animals showed 4-fold increase in mRNA expression of FTO. The protein level of FTO was also similarly increased. These results were complementary to the analysis of lipid parameters and body weight gain in F1 generation.
All these results together combined indicate an early onset of NAFLD, which could only be confirmed by histological analysis. Liver tissue of test F1 offspring showed high lipid vacuolation, loss of hepatocytes, inflammation, and apoptosis accompanied with peribiliary infiltration and hemorrhage. These are the histological hallmarks of NAFLD. Taken together, our results demonstrate that parental diet and BPA exposure offset a cascade of processes in the F1 generation, which results in the onset of NAFLD. Parental obesity and BPA exposure contribute towards increased birth weight and progressive weight gain, which predisposes the offspring to higher circulating cholesterol and lipids. It also affects the expression of energy homeostasis genes. The combined effect of these transgenerational results in adipogenesis, oxidative stress, and insulin resistance, leading to fat accumulation in liver cells and onset of NAFLD. Our results demonstrate that a high-fat parental diet and chronic BPA exposure have wide-ranging effects on the metabolism of offspring in rodents and even low dose of BPA accompanied by parental obesity can have deleterious effects on the liver.
Conclusions
In this study, we evaluated the intergenerational effects of perinatal exposure to BPA on the liver of F1 generation offspring with obese parentage. Looking at the big picture after combining results from a wide array of experiments, we conclude that the prenatal exposure to BPA could induce oxidative damage and disrupt normal metabolic profiles in the liver of F1 generation of obese parents leading to compromise of glucose and lipid homeostasis. Changes in the levels of expression of obesity-related genes in offspring led to an accumulation of lipid in liver tissue, and the combined effect led to onset of NAFLD. Our study offers a link between parental exposures and onset of NAFLD in F1 generation in a murine model.
Availability of data and materials
Additional data are provided in Supplementary Material files 1 to 3.
References
Acevedo N, Davis B, Schaeberle CM, Sonnenschein C, Soto AM (2013) Perinatally administered bisphenol A as a potential mammary gland carcinogen in rats. Environ Health Perspect 121(9):1040–1046. https://doi.org/10.1289/ehp.1306734
Alonso-Magdalena P, Vieira E, Soriano S, Menes L, Burks D, Quesada I, Nadal A (2010) Bisphenol A exposure during pregnancy disrupts glucose homeostasis in mothers and adult male offspring. Environ Health Perspect 118(9):1243–1250. https://doi.org/10.1289/ehp.1001993
Angle BM, Do RP, Ponzi D, Stahlhut RW, Drury BE, Nagel SC, Welshons WV, Besch-Williford CL, Palanza P, Parmigiani S, vom Saal FS, Taylor JA (2013) Metabolic disruption in male mice due to fetal exposure to low but not high doses of bisphenol A (BPA): evidence for effects on body weight, food intake, adipocytes, leptin, adiponectin, insulin and glucose regulation. Reprod Toxicol (Elmsford, NY) 42:256–268. https://doi.org/10.1016/j.reprotox.2013.07.017
Balci A, Ozkemahli G, Erkekoglu P, Zeybek ND, Yersal N, Kocer-Gumusel B (2020) Histopathologic, apoptotic and autophagic, effects of prenatal bisphenol A and/or di(2-ethylhexyl) phthalate exposure on prepubertal rat testis. Environ Sci Pollut Res 27(16):20104–20116. https://doi.org/10.1007/s11356-020-08274-6
Bell CG, Finer S, Lindgren CM, Wilson GA, Rakyan VK, Teschendorff AE, Akan P, Stupka E, Down TA, Prokopenko I, Morison IM, Mill J, Pidsley R, International Type 2 Diabetes 1q Consortium et al (2010) Integrated genetic and epigenetic analysis identifies haplotype-specific methylation in the FTO type 2 diabetes and obesity susceptibility locus. PloSone 5(11):e14040. https://doi.org/10.1371/journal.pone.0014040
Burd EM (2010) Validation of laboratory-developed molecular assays for infectious diseases. Clin Microbiol Rev 23(3):550–576. https://doi.org/10.1128/CMR.00074-09
Carlberg I, Mannervik B (1975) Purification and characterization of the flavoenzyme glutathione reductase from rat liver. J Biol Chem 250(14):5475–5480
Claiborne A (1985) Catalase activity. In: Greenwald RA (ed) CRC handbook of methods in oxygen radical research. CRC Press, Boca Raton, pp 283–284
Cwiek-Ludwicka K, Ludwicki JK (2014) Endocrine disruptors in food contact materials; is there a health threat? Rocz Panstw Zakl Hig 65(3):169–177
Dabeer S, Afjal MA, Ahmad S, Fatima M, Habib H, Parvez S, Raisuddin S (2020) Transgenerational effect of parental obesity and chronic parental bisphenol A exposure on hormonal profile and reproductive organs of preadolescent Wistar rats of F1 generation: a one-generation study. Hum Exp Toxicol 39(1):59–76. https://doi.org/10.1177/0960327119873017
Deceuninck Y, Bichon E, Marchand P, Boquien CY, Legrand A, Boscher C, Antignac JP, Le Bizec B (2015) Determination of bisphenol A and related substitutes/analogues in human breast milk using gas chromatography-tandem mass spectrometry. Anal Bioanal Chem 407(9):2485–2497. https://doi.org/10.1007/s00216-015-8469-9
Dunder L, HalinLejonklou M, Lind L, Risérus U, Lind PM (2018) Low-dose developmental bisphenol A exposure alters fatty acid metabolism in Fischer 344 rat offspring. Environ Res 166:117–129. https://doi.org/10.1016/j.envres.2018.05.023
El-Serag HB, Tran T, Everhart JE (2004) Diabetes increases the risk of chronic liver disease and hepatocellular carcinoma. Gastroenterology 126(2):460–468. https://doi.org/10.1053/j.gastro.2003.10.065
Fellmann L, Nascimento AR, Tibiriça E, Bousquet P (2013) Murine models for pharmacological studies of the metabolic syndrome. Pharmacol Ther 137(3):331–340. https://doi.org/10.1016/j.pharmthera.2012.11.004
Ferré P, Foufelle F (2007) SREBP-1c transcription factor and lipid homeostasis: clinical perspective. Horm Res 68(2):72–82. https://doi.org/10.1159/000100426
Fuster JJ, Ouchi N, Gokce N, Walsh K (2016) Obesity-induced changes in adipose tissue microenvironment and their impact on cardiovascular disease. Circ Res 118(11):1786–1807. https://doi.org/10.1161/CIRCRESAHA.115.306885
Geens T, Aerts D, Berthot C, Bourguignon JP, Goeyens L, Lecomte P, Maghuin-Rogister G, Pironnet AM, Pussemier L, Scippo ML, Van Loco J, Covaci A (2012) A review of dietary and non-dietary exposure to bisphenol-A. Food Chem Toxicol: Int J Publ Br Ind Biol Res Assoc 50(10):3725–3740. https://doi.org/10.1016/j.fct.2012.07.059
Habig WH, Pabst MJ, Jakoby WB (1974) Glutathione S-transferases. The first enzymatic step in mercapturic acid formation. J Biol Chem 249(22):7130–7139
Hales CN, Randle PJ (1963) Immunoassay of insulin with insulin-antibody precipitate. Biochem J 88(1):137–146. https://doi.org/10.1042/bj0880137
Hashimoto Y, Nakamura M (2000) Estrogenic activity of dental materials and bisphenol-A related chemicals in vitro. Dent Mater J 19(3):245–262. https://doi.org/10.4012/dmj.19.245
Hercog K, Maisanaba S, Filipič M, Sollner-Dolenc M, Kač L, Žegura B (2019) Genotoxic activity of bisphenol A and its analogues bisphenol S, bisphenol F and bisphenol AF and their mixtures in human hepatocellular carcinoma (HepG2) cells. Sci Total Environ 687:267–276. https://doi.org/10.1016/j.scitotenv.2019.05.486
Hoepner LA (2019) Bisphenol A: a narrative review of prenatal exposure effects on adipogenesis and childhood obesity via peroxisome proliferator-activated receptor gamma. Environ Res 173:54–68. https://doi.org/10.1016/j.envres.2019.03.012
Huszar D, Lynch CA, Fairchild-Huntress V, Dunmore JH, Fang Q, Berkemeier LR, Gu W, Kesterson RA, Boston BA, Cone RD, Smith FJ, Campfield LA, Burn P, Lee F (1997) Targeted disruption of the melanocortin-4 receptor results in obesity in mice. Cell 88(1):131–141. https://doi.org/10.1016/s0092-8674(00)81865-6
Ikezuki Y, Tsutsumi O, Takai Y, Kamei Y, Taketani Y (2002) Determination of bisphenol A concentrations in human biological fluids reveals significant early prenatal exposure. Human Reprod (Oxford, England) 17(11):2839–2841. https://doi.org/10.1093/humrep/17.11.2839
Jollow DJ, Mitchell JR, Zampaglione N, Gillette JR (1974) Bromobenzene-induced liver necrosis. Protective role of glutathione and evidence for 3,4-bromobenzene oxide as the hepatotoxic metabolite. Pharmacology 11(3):151–169. https://doi.org/10.1159/000136485
Kelly T, Yang W, Chen CS, Reynolds K, He J (2008) Global burden of obesity in 2005 and projections to 2030. Int J Obes (2005) 32(9):1431–1437. https://doi.org/10.1038/ijo.2008.102
Khan J, Salhotra S, Ahmad S, Sharma S, Abdi S, Banerjee BD, Parvez S, Gupta S, Raisuddin S (2018) The protective effect of α-lipoic acid against bisphenol A-induced neurobehavioral toxicity. Neurochem Int 118:166–175. https://doi.org/10.1016/j.neuint.2018.06.0
Kim JC, Shin HC, Cha SW, Koh WS, Chung MK, Han SS (2001) Evaluation of developmental toxicity in rats exposed to the environmental estrogen bisphenol A during pregnancy. Life Sci 69(22):2611–2625. https://doi.org/10.1016/s0024-3205(01)01341-8
Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, Ferrell LD, Liu YC, Torbenson MS, Unalp-Arida A, Yeh M, McCullough AJ, Sanyal AJ, Nonalcoholic Steatohepatitis Clinical Research Network (2005) Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology (Baltimore, Md) 41(6):1313–1321. https://doi.org/10.1002/hep.20701
Kobroob A, Peerapanyasut W, Chattipakorn N, Wongmekiat O (2018) Damaging effects of bisphenol A on the kidney and the protection by melatonin: emerging evidences from in vivo and in vitro studies. Oxidative Med Cell Longev 2018:3082438. https://doi.org/10.1155/2018/3082438
Krashes MJ, Lowell BB, Garfield AS (2016) Melanocortin-4 receptor-regulated energy homeostasis. Nat Neurosci 19(2):206–219. https://doi.org/10.1038/nn.4202
Kumar R, Porwal YC, Dev N, Kumar P, Chakravarthy S, Kumawat A (2020) Association of high-sensitivity C-reactive protein (hs-CRP) with non-alcoholic fatty liver disease (NAFLD) in Asian Indians: a cross-sectional study. J Fam Med Prim Care 9(1):390–394. https://doi.org/10.4103/jfmpc.jfmpc_887_19
Li S, Tan HY, Wang N, Zhang ZJ, Lao L, Wong CW, Feng Y (2015) The role of oxidative stress and antioxidants in liver diseases. Int J Mol Sci 16(11):26087–26124. https://doi.org/10.3390/ijms161125942
Li S, Hong M, Tan HY, Wang N, Feng Y (2016) Insights into the role and interdependence of oxidative stress and inflammation in liver diseases. Oxidative Med Cell Longev 2016:4234061. https://doi.org/10.1155/2016/4234061
Liu X, Zheng L, Zhang R, Liu G, Xiao S, Qiao X, Wu Y, Gong Z (2016) Toxicological evaluation of advanced glycation end product Nε-(carboxymethyl)lysine: acute and subacute oral toxicity studies. Regul Toxicol Pharmacol : RTP 77:65–74. https://doi.org/10.1016/j.yrtph.2016.02.013
Ma Y, Liu H, Wu J, Yuan L, Wang Y, Du X, Wang R, Marwa PW, Petlulu P, Chen X, Zhang H (2019) The adverse health effects of bisphenol A and related toxicity mechanisms. Environ Res 176:108575. https://doi.org/10.1016/j.envres.2019.108575
Malone JI, Hansen BC (2019) Does obesity cause type 2 diabetes mellitus (T2DM)? Or is it the opposite? Pediatr Diabetes 20(1):5–9. https://doi.org/10.1111/pedi.12787
Manikkam M, Guerrero-Bosagna C, Tracey R, Haque MM, Skinner MK (2012) Transgenerational actions of environmental compounds on reproductive disease and identification of epigenetic biomarkers of ancestral exposures. PLoS One 7(2):e31901. https://doi.org/10.1371/journal.pone.0031901
Manikkam M, Tracey R, Guerrero-Bosagna C, Skinner MK (2013) Plastics derived endocrine disruptors (BPA, DEHP and DBP) induce epigenetic transgenerational inheritance of obesity, reproductive disease and sperm epimutations. PLoS One 8(1):e55387. https://doi.org/10.1371/journal.pone.0055387
Manual of Laboratory Operations (1974) Lipid research clinics program, volume 1. Lipid and lipoprotein analysis. National Heart and Lung Institute, National Institutes of Health. DHEW Publication No. INIHI, Bethesda, pp 75–628
Marques C, Meireles M, Norberto S, Leite J, Freitas J, Pestana D, Faria A, Calhau C (2015) High-fat diet-induced obesity rat model: a comparison between Wistar and Sprague-Dawley rat. Adipocyte 5(1):11–21. https://doi.org/10.1080/21623945.2015.1061723
McCarthy JL, Nations C (1979) Activity of some dehydrogenase enzymes in mitochondria from Physarum polycephalum. Comp Biochem Physiol B, Comp Biochem 63(4):495–499. https://doi.org/10.1016/0305-0491(79)90052-x
Merkestein M, Sellayah D (2015) Role of FTO in adipocyte development and function: recent insights. Int J Endocrinol 2015:521381. https://doi.org/10.1155/2015/521381
Mihara M, Uchiyama M (1978) Determination of malonaldehyde precursor in tissues by thiobarbituric acid test. Anal Biochem 86(1):271–278. https://doi.org/10.1016/0003-2697(78)90342-1
Misra HP, Fridovich I (1972) The role of superoxide anion in the autoxidation of epinephrine and a simple assay for superoxide dismutase. J Biol Chem 247(10):3170–3175
Mohammed ET, Hashem KS, Ahmed AE, Aly MT, Aleya L, Abdel-Daim MM (2020) Ginger extract ameliorates bisphenol A (BPA)-induced disruption in thyroid hormones synthesis and metabolism: involvement of Nrf-2/HO-1 pathway. Sci Total Environ 703:134664. https://doi.org/10.1016/j.scitotenv.2019.134664
Mohandas J, Marshall JJ, Duggin GG, Horvath JS, Tiller DJ (1984) Low activities of glutathione-related enzymes as factors in the genesis of urinary bladder cancer. Cancer Res 44(11):5086–5091
Nakagawa Y, Tayama S (2000) Metabolism and cytotoxicity of bisphenol A and other bisphenols in isolated rat hepatocytes. Arch Toxicol 74(2):99–105. https://doi.org/10.1007/s002040050659
Ng M, Fleming TD, Robinson M, Thomson B, Graetz N, Margono C, Mullany EC et al (2014) Global, regional, and national prevalence of overweight and obesity in children and adults during 1980–2013: a systematic analysis for the Global Burden of Disease Study 2013. Lancet (London, England) 384(9945):766–781. https://doi.org/10.1016/S0140-6736(14)60460-8
Novelli EL, Diniz YS, Galhardi CM, Ebaid GM, Rodrigues HG, Mani F, Fernandes AA, Cicogna AC, Novelli Filho JL (2007) Anthropometrical parameters and markers of obesity in rats. Lab Anim 41(1):111–119. https://doi.org/10.1258/002367707779399518
Pottenger LH, Domoradzki JY, Markham DA, Hansen SC, Cagen SZ, Waechter JM Jr (2000) The relative bioavailability and metabolism of bisphenol A in rats is dependent upon the route of administration. Toxicol Sci: An Off J Soc Toxicol 54(1):3–18. https://doi.org/10.1093/toxsci/54.1.3
Provvisiero DP, Pivonello C, Muscogiuri G, Negri M, de Angelis C, Simeoli C, Pivonello R, Colao A (2016) Influence of bisphenol A on type 2 diabetes mellitus. Int J Environ Res Public Health 13(10):989. https://doi.org/10.3390/ijerph13100989
Raisuddin S, Sharma S (2018) Endocrine-disrupting chemicals in food and their toxicological implications. In: Sachan A, Hendrich S (eds) Food toxicology: current advances and future challenges. Apple Academic Press, Oakville, pp 199–250
Rashid H, Ahmad F, Rahman S, Ansari RA, Bhatia K, Kaur M, Islam F, Raisuddin S (2009) Iron deficiency augments bisphenol A-induced oxidative stress in rats. Toxicology 256(1-2):7–12. https://doi.org/10.1016/j.tox.2008.10.022
Salian S, Doshi T, Vanage G (2009) Perinatal exposure of rats to bisphenol A affects the fertility of male offspring. Life Sci 85(21-22):742–752. https://doi.org/10.1016/j.lfs.2009.10.004
Shafei A, Ramzy MM, Hegazy AI, Husseny AK, El-Hadary UG, Taha MM, Mosa AA (2018) The molecular mechanisms of action of the endocrine disrupting chemical bisphenol A in the development of cancer. Gene 647:235–243. https://doi.org/10.1016/j.gene.2018.01.016
Shao X, Wang M, Wei X, Deng S, Fu N, Peng Q, Jiang Y, Ye L, Xie J, Lin Y (2016) Peroxisome proliferator-activated receptor-γ: master regulator of adipogenesis and obesity. Curr Stem Cell Res Ther 11(3):282–289. https://doi.org/10.2174/1574888x10666150528144905
Sharma S, Ahmad S, Khan MF, Parvez S, Raisuddin S (2018) In silico molecular interaction of bisphenol analogues with human nuclear receptors reveals their stronger affinity vs. classical bisphenol A. Toxicol Mech Methods 28(9):660–669. https://doi.org/10.1080/15376516.2018.1491663
Sharma S, Ahmad S, Afjal MA, Habib H, Parvez S, Raisuddin S (2019) Dichotomy of bisphenol A-induced expression of peroxisome proliferator-activated receptors in hepatic and testicular tissues in mice. Chemosphere 236:124264. https://doi.org/10.1016/j.chemosphere.2019.06.234
Shu L, Meng Q, Diamante G, Tsai B, Chen YW, Mikhail A, Luk H, Ritz B, Allard P, Yang X (2019) Prenatal bisphenol A exposure in mice induces multitissue multiomics disruptions linking to cardiometabolic disorders. Endocrinology 160(2):409–429. https://doi.org/10.1210/en.2018-00817
Stevens GA, Singh GM, Lu Y, Danaei G, Lin JK, Finucane MM, Bahalim AN, McIntire RK, Gutierrez HR, Cowan M, Paciorek CJ, Farzadfar F, Riley L, Ezzati M, Global Burden of Metabolic Risk Factors of Chronic Diseases Collaborating Group (Body Mass Index) (2012) National, regional, and global trends in adult overweight and obesity prevalences. Popul Health Metrics 10(1):22. https://doi.org/10.1186/1478-7954-10-22
Susiarjo M, Sasson I, Mesaros C, Bartolomei MS (2013) Bisphenol A exposure disrupts genomic imprinting in the mouse. PLoS Genet 9(4):e1003401. https://doi.org/10.1371/journal.pgen.1003401
Takahashi Y, Soejima Y, Fukusato T (2012) Animal models of nonalcoholic fatty liver disease/nonalcoholic steatohepatitis. World J Gastroenterol 18(19):2300–2308. https://doi.org/10.3748/wjg.v18.i19.2300
Tudurí E, Marroqui L, Dos Santos RS, Quesada I, Fuentes E, Alonso-Magdalena P (2018) Timing of exposure and bisphenol-A: implications for diabetes development. Front Endocrinol 9:648. https://doi.org/10.3389/fendo.2018.00648
Valenti L, Fracanzani AL, Dongiovanni P, Santorelli G, Branchi A, Taioli E, Fiorelli G, Fargion S (2002) Tumor necrosis factor alpha promoter polymorphisms and insulin resistance in nonalcoholic fatty liver disease. Gastroenterology 122(2):274–280. https://doi.org/10.1053/gast.2002.31065
Vandenberg LN, Chahoud I, Heindel JJ, Padmanabhan V, Paumgartten FJ, Schoenfelder G (2010) Urinary, circulating, and tissue biomonitoring studies indicate widespread exposure to bisphenol A. Environ Health Perspect 118(8):1055–1070. https://doi.org/10.1289/ehp.0901716
Vandenberg LN, Colborn T, Hayes TB, Heindel JJ, Jacobs DR Jr, Lee DH, Shioda T, Soto AM, vom Saal FS, Welshons WV, Zoeller RT, Myers JP (2012) Hormones and endocrine-disrupting chemicals: low-dose effects and nonmonotonic dose responses. Endocr Rev 33(3):378–455. https://doi.org/10.1210/er.2011-1050
Vernon G, Baranova A, Younossi ZM (2011) Systematic review: the epidemiology and natural history of non-alcoholic fatty liver disease and non-alcoholic steatohepatitis in adults. Aliment Pharmacol Ther 34(3):274–285. https://doi.org/10.1111/j.1365-2036.2011.04724.x
Wang Y, Min J, Khuri J, Li M (2017) A systematic examination of the association between parental and child obesity across countries. Adv Nutr (Bethesda, Md) 8(3):436–448. https://doi.org/10.3945/an.116.013235
Weinhouse C, Anderson OS, Bergin IL, Vandenbergh DJ, Gyekis JP, Dingman MA, Yang J, Dolinoy DC (2014) Dose-dependent incidence of hepatic tumors in adult mice following perinatal exposure to bisphenol A. Environ Health Perspect 122(5):485–491. https://doi.org/10.1289/ehp.1307449
Whitaker RC, Wright JA, Pepe MS, Seidel KD, Dietz WH (1997) Predicting obesity in young adulthood from childhood and parental obesity. N Engl J Med 337(13):869–873. https://doi.org/10.1056/NEJM199709253371301
Wu W, Li M, Liu A, Wu C, Li D, Deng Q, Zhang B, Du J, Gao X, Hong Y (2020) Bisphenol A and the risk of obesity a systematic review with meta-analysis of the epidemiological evidence. Dose-Response : a publication of International Hormesis Society 18(2):1559325820916949. https://doi.org/10.1177/1559325820916949
Yang M, Ryu JH, Jeon R, Kang D, Yoo KY (2009) Effects of bisphenol A on breast cancer and its risk factors. Arch Toxicol 83(3):281–285. https://doi.org/10.1007/s00204-008-0364-0
Yki-Järvinen H (2010) Nutritional modulation of nonalcoholic fatty liver disease and insulin resistance: human data. Curr Opin Clin Nutr Metab Care 13(6):709–714. https://doi.org/10.1097/MCO.0b013e32833f4b34
Acknowledgements
Dr. S.D. Sharma of the Central Instrumentation Facility, School of Chemical and Life Sciences, Jamia Hamdard, New Delhi, India, facilitated the use and troubleshooting of instruments. Dr. Wara Prasad, Veterinary Pathologist, facilitated the histopathological analysis of slides.
Funding
The student fellowship and project grant was funded by University Grants Commission-Maulana Azad National Foundation (UGC-MANF- Grant #201516-MANF-2015-17-UTT-59439).
Author information
Authors and Affiliations
Contributions
S. Dabeer: conceptualization, methodology, investigation, writing — original draft, formal analysis, data curation; S. Raisuddin: conceptualization, supervision, funding acquisition, resources, data curation, project administration, writing — original draft and editing, formal analysis, data curation.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The manuscript does not contain clinical studies, patient data, or any studies with human participants performed by any of the authors. All applicable international, national, and/or institutional guidelines for the care and use of animals were followed. All procedures performed in studies involving animals were in accordance with the ethical standards of the institution at which the studies were conducted, as detailed in “Materials and methods.” The project was approved by the Institutional Animal Ethics Committee of the university (Project #1330).
Consent for publication
Not applicable. No human subjects involved. All included authors have given consent for publication of data and manuscript.
Competing interests
The authors declare no competing interests.
Approval of authors
All the authors made contributions to this manuscript and have approved the submission version of the manuscript.
Additional information
Responsible Editor: Mohamed M. Abdel-Daim
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dabeer, S., Raisuddin, S. Perinatal exposure to environmental endocrine disruptor bisphenol A aggravates the onset of non-alcoholic fatty liver disease (NAFLD) in weanling F1 offspring of obese rats. Environ Sci Pollut Res 30, 3146–3165 (2023). https://doi.org/10.1007/s11356-022-22246-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-022-22246-y