Abstract
Introduction
Snoring sounds are discussed to contain acoustic information about their geneses. Nocturnal snoring can easily be recorded acoustically but it is difficult to visually verify its genesis. Contrary, snoring patterns induced by drug-induced sleep endoscopy (DISE) can be visually differentiated. The aim of the study was to classify patterns of obstructions and vibration during DISE and to evaluate acoustic characteristics between these different patterns of snoring.
Methods
DISE was performed in 41 male patients with sleep-disordered breathing. The recorded video sequences (n = 108) were classified visually at a mute mode in different patterns of snoring (velar, velar obstructive, tonsillar, post-apnoeic). The sound tracks of these subgroups were analysed and compared with regard to the parameters sound pressure level, loudness, sharpness, roughness, fluctuations strength and centre frequency.
Results
Obstructive snoring patterns revealed a higher loudness than non-obstructive patterns (>25 sone). Velar snoring showed more roughness (>150 cAsper) than tonsillar and post-apnoeic snoring and revealed the lowest centre frequency (<3000 Hz) of all patterns. Tonsillar snoring presented the highest sharpness (>1.6 acum) whereas post-apnoeic snoring revealed the largest fluctuation strength (>50 cVacil).
Conclusion
Different snoring patterns induced by DISE can be classified visually, and an approach to differentiate them acoustically by means of psychoacoustic analyses is demonstrated. On the basis of these results, nocturnal snoring might also be differentiated by psychoacoustic algorithms which could be implemented in acoustic polygraphic screening devices in the future.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Snoring is reported to occur either as a symptom of obstructive sleep apnoea or as sound phenomenon occurring independent of obstructive apnoeas. Depending on the site and mechanism of obstructions and vibrations, snoring sounds have specific acoustic characteristics. Whilst palatinal snoring is reported to have a main frequency below 500 Hz, the one found for tongue base snoring is above 500 Hz. Snoring episodes terminating obstructive apnoeas can exceed frequency maxima up to 4000 Hz [1–8]. Nevertheless, the data vary extremely depending on the method of recording and the parameters analysed. Most data deal with nocturnal snoring sounds, leading to the methodical problem that the analysed snoring sounds are not classified visually. The classification of a certain type of obstruction or vibration is performed by indirect classification on base of poly(somno)graphic information.
A potential visualisation can be obtained by flexible nasal endoscopy during simulated snoring under wake conditions [9]. Nevertheless, simulated snoring sounds have been shown to differ from real nocturnal snoring [10].
Drug-induced sleep endoscopy (DISE) is commonly used for evaluation of the upper airway in patients with sleep-disordered breathing [11–16]. During the procedure, the site of vibration and obstruction can be detected visually. Besides that, the different types of obstruction- and vibration-induced snoring sounds can be recorded.
The aim of the study was to evaluate the specific characteristics of different types of snoring sounds, which are induced by DISE in order to create algorithms for acoustic analyses of snoring sounds in the future.
Methods
General procedure
The study was performed in male patients (n = 41) with suspected sleep-disordered breathing after written consent of the patients at a tertiary referral centre. The study was approved by the local ethic committee (2011–55). A polygraphic or polysomnographic recording to verify the sleep-disordered breathing by apnoea-hypopnea-index (AHI) was performed prior to DISE. Age and the body mass index (BMI) were documented.
Drug-induced sleep endoscopy
Drug-induced sleep endoscopy (DISE) was performed in an operation room, and patients were monitored with oxygen saturation, non-invasive blood pressure and ECG by an anaesthesiologist. DISE was performed by bolus-wise application of 10–20 mg Disoprivan 1 % (Propofol-Lipuro 10 mg/ml; B. Braun Melsungen AG, Bonn, Germany). Depth of sedation was monitored by detection of the BiSpectral Index ® (BIS). A BIS value of 40 was aimed at to simulate slow wave sleep (S3 sleep) [17–19]. During DISE, a continuous video documentation of the upper airway was achieved by flexible nasal endoscopy. Parallel to the visual recording, an external condenser microphone with a flat frequency response curve from 20 to 20,000 Hz (RODE NT3, Silverwater, Australia) was placed in front of the patients’ mouth in a distance of 30 cm. The microphone was linked to the video recording system (AIDA, Storz, Tuttlingen, Germany).
Visual evaluation
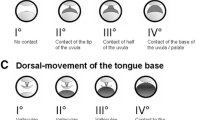
The video sequences were analysed with respect to the pattern of collapse and vibration. One hundred and eight snoring episodes were included in the study. Between one and three episodes were chosen from each patient. The depth of sedation measured by BIS at which the snoring samples were chosen ranged between 70 and 40. The video samples of each snoring episode were classified on the basis of the visual appearance at a mute mode by the first author. Obstruction and vibration patterns were classified as follows:
-
1.
Snoring terminating an obstructive apnoea (the first snoring episode after an apnoeic event independent from the pattern of vibration n = 22)
-
2.
Tonsillar snoring (oropharynx; lateral, n = 21)
-
3.
Velar snoring (velum; anterior–posterior, n = 50)
-
4.
Obstructive velar snoring (velum; anterior–posterior and lateral or circular, n = 15)
One episode of snoring of each type is shown in Fig. 1a–d
a Series of consecutive images of one snoring episode terminating an obstructive apnoea. A complete lateral collapse is visible at the first image. The deep oropharynx expands within the following three images (arrows indicating the direction of movement). The fifth image shows an open airway with a view to the epiglottis. b Series of consecutive images of one snoring episode with a lateral collapse of the tonsils. Hyperplastic tonsils (arrows indicating the direction of movement) are visible in the first two pictures leaving a narrow airway with view to the edge of the epiglottis. During the snoring episode, a complete lateral obstruction occurs leading to vibrations at the level of the tonsils. c Series of consecutive images of one snoring episode with an anterior–posterior vibration of the soft palate. The uvula (asterisk) vibrates at an anterior–posterior direction. No obstruction is detectable. d Series of consecutive images of one snoring episode with an anterior–posterior vibration and a circular collapse at the velum level. Additional to the anterior–posterior vibration, a circular collapse (bent arrows) can be detected at the velum level leading to an obstructive component
The distributions of the depth of sedation and different snoring types were as follows:
BIS 70: n = 20 (tonsillar snoring n = 3, velar snoring n = 17)
BIS 60: n = 39 (post-apnoeic snoring n = 1, tonsillar snoring n = 10, velar snoring n = 22, obstructive velar snoring n = 6)
BIS 50: n = 37 (post-apnoeic snoring n = 11, tonsillar snoring n = 6, velar snoring n = 11, obstructive velar snoring n = 9)
BIS 40: n = 12 (post-apnoeic snoring n = 10, tonsillar snoring n = 2)
Acoustic evaluation
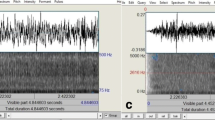
After visual classification, the sound tracks of each snoring sample were transformed into a WAV format (16,000 Hz, 16-Bit, mono signal; Adobe Audition 1.5, Adobe Systems, München, Germany). The sound pressure level was by an external sound level metre (sound level metre 322 Datalog, Voltcraft, Conrad Electronic, Hirschau, Germany). The samples were analysed by psychoacoustic software (dbSONIC, Metravib, Limonest, France) as previously published [20] with regard to the following parameters: sound pressure level ([dB], A-weighted), loudness (sone), sharpness (acum), roughness (cAsper), fluctuation strength (cVacil) and centre frequency (Hz) (mean values for each parameter). The psychoacoustic parameters loudness, sharpness, roughness and fluctuation strength were described by Fastl and Zwicker [21].
Statistic evaluation
The psychoacoustic parameters were analyses by mixed model analyses providing the regression coefficient beta, standard errors, 95 % confidence intervals (95 % CI), p values and estimate mean values. Calculations were controlled for random effects for patients and depth of sedation. Analyses were performed with SAS 9.3 (SAS Institute, Cary, NC, USA).
Results
Patients’ baseline data
The mean age of the patients was 53.4 years (standard deviation (SD) 7.2). The mean BMI was 28.7 (SD 6.3). The mean AHI was 12.4 (SD 8.1; min 1.2; max 30.9).
Level
The mean sound pressure level ([dB], A-weighted) was highest for obstructive velar snoring (mean 79.45; 95 % CI 78.27; 80.64). Post-apnoeic (estimated difference −6.63; 95 % CI −10.81; −2.46), velar (estimated difference −10.29; 95 % CI −13.99; −6.59) and tonsillar snoring (estimated difference −7.40; 95 % CI −11.44; −3.36) did not differ from each other and showed significant lower levels than obstructive velar snoring (Fig. 2a, Tables 1 and 2).
a–f Analyses of the parameters sound pressure level (a), loudness (b), sharpness (c), roughness (d), fluctuation strength (e) and centre frequency (f). Data are given as raw mean values (δ), median and percentile 25/75 % (box), whisker 5/95, 1 and 99 % (x), and minimum and maximum value (−). Obstructive velar snoring showed a higher sound pressure level than the other snoring patterns (a). Obstructive snoring patterns (post-apnoeic, tonsillar, velar obstructive) reveal a higher loudness than non-obstructive velar snoring (b). The sharpness is elevated as soon as lateral tonsillar obstructions occur (c). An enhanced roughness is present in velar snoring patterns regardless of an obstructive component (d). Post-apnoeic snoring episodes reveal a high level of fluctuation strength than non-apnoeic sounds (e). Velar non-obstructive snoring presented the lowest centre frequency of the different snoring patterns (f)
Loudness
Velar snoring with vibrations with an anterior–posterior pattern revealed a lower loudness (sone) (mean 18.99; 95 % CI 17.88; 20.09, estimated difference to obstructive velar snoring −11.05; 95 % CI −16.30; −5.81) than all other types of snoring. As soon as obstructive patterns are classified (post-apnoeic (estimated difference to obstructive velar snoring − 0.30; 95 % CI −6.12; 5.52), tonsillar (estimated difference to obstructive velar snoring −0.37; 95 % CI −6.20; 5.46), velar obstructive), the loudness raises (Fig. 2b, Tables 1 and 2).
Sharpness
The acoustic characteristics of obstructions and vibrations at tonsillar level revealed a higher sharpness (acum) (mean 1.65; 95 % CI 1.61; 1.69; estimated difference to obstructive velar snoring 0.24; 95 % CI 0.12; 0.36) compared to the other types of snoring sounds (Fig. 2c, Tables 1 and 2).
Roughness
Velar snoring (mean 216.71; 95 % CI 184.77; 248.65; estimated difference to obstructive velar snoring 28.05; 95 % CI −48.45; 104.56) as well as obstructive velar snoring (mean 184.41; 95 % CI 147.61; 221.22) revealed a higher roughness (cAsper) compared to tonsillar and post-apnoeic snoring (Fig. 2d, Tables 1 and 2).
Fluctuation strength
Post-apnoeic snoring showed higher fluctuation strength (cVacil) (mean 71.51; 95 % CI 56.92; 86.11; estimated difference to obstructive velar snoring 38.76; 95 % CI 18.78; 58.74) than the other snoring types (Fig. 2e, Tables 1 and 2).
Centre frequency
Velar snoring revealed a lower centre frequency (Hz) (mean 2673.40; 95 % CI 1957.42; 3389.39; estimated difference to obstructive velar snoring 3592.98; 95 % CI −6461.34; −724.63) than other types of snoring episodes. No differences with respect to the centre frequency were detected between post-apnoeic, tonsillar and obstructive velar snoring (Fig. 2f, Tables 1 and 2).
Control for random effects for patients and depth of sedation
Vibrations of the velum (velar snoring) without obstructive patterns were more frequent at less deeper levels of sedation (BIS 70 and 60). The deeper the sedation was performed (BIS 50 and 40), the more obstructive patterns were detected (post-apnoeic snoring). A potential influence of the individual patient (n = 41) and the depth of sedation (BIS 70–40) were controlled for random effects. The controlled estimate means are given in Table 2. Velar obstructive snoring was taken as reference to which the other snoring patterns were compared. The difference between the estimate means are given as parameter estimate as an estimated difference to the respective parameter of obstructive velar snoring with standard error, p value and 95 % CI (Table 2).
Discussion
Although snoring is a main symptom in obstructive sleep apnoea, the acoustic characteristics of snoring sounds remain unanalysed by routine poly(somno)graphy. In recent years, various publications differentiate specific snoring types and anatomic structures that may create specific snoring sounds. Tongue base snoring is reported to have predominant frequency patterns above 500 Hz and palatinal snoring below 500 Hz [3, 4, 1, 2, 5–8]. Most data are based on the visualisation of vibrating structures during sleep endoscopy. Thereby, a possible differentiation between palatal and non-palatal snoring is frequently reported. Contrary to that, other sites of obstruction can hardly be detected by acoustic analyses [4, 1, 7, 22–25].
As recent publications report multi-level obstruction patterns during sleep and even a change of obstructions levels depending on the depth of sedation during sleep endoscopy [26, 27, 13, 16], other structures apart from the velum and tongue base need to get into focus of acoustic investigations. To the opinion of the authors, focusing on only one pattern of vibration (e.g. just palatinal vs. non-palatinal) seems to be too idealised. Therefore, the presented study evaluates several subtypes of vibration and collapse patterns (velar, velar obstructive, tonsillar, post-apnoeic) in order to achieve a more practical view on the different types of snoring.
Moreover, mostly, a single method of acoustic analysis (e.g. centre or peak frequency) is performed depending on the available equipment of software. This results in the inability to distinguish other sites of obstruction or vibration apart from palatal or non-palatal. The acoustic information of a snoring noise cannot be evaluated by simple frequency analyses alone.
A more complex approach of analysis seems to be necessary. The present study provides a standardised procedure of analysis by psychoacoustic parameters as previously described [20, 28, 29, 21]. A review of Pevernagie et al. lists several methods of acoustic evaluation of snoring sounds [8]. These approaches are mostly a single method approach resulting in a limited informative value. In our opinion, multiple parameters provide a wider range for classifying specific subgroups of snoring. Therefore, the use of several psychoacoustic parameters is intended in the presented study. An “acoustic fingerprint” of different subtypes of snoring can be obtained.
The present data enable a differentiation between obstructive and non-obstructive snoring sounds, which might be of clinical relevance. Non-obstructive snoring as it can be observed at the velum caused by an anterior–posterior vibration reveals less loudness and a lower level than snoring with obstructive components. In addition, the velum can be determined as site of vibration or obstruction by an enhanced roughness compared to tonsillar or post-apnoeic snoring episodes.
Contrary to that, an increased sharpness gives evidence for snoring sounds, which are caused by a lateral collapse of the oropharynx at the tonsil level.
Despite the fact that the patterns of vibration in post-apnoeic snoring are not as homogeneous as in the other three types, it can be demonstrated that the fluctuation strength of snoring sounds terminating an apnoeic event is higher than in any other snoring type.
By taking all measured psychoacoustic parameters into account, different types of snoring and patterns of vibration or obstruction can be differentiated. As demonstrated in Table 3, different patterns of distribution of psychoacoustic parameters can be detected. The characterisation of a specific pattern of vibration or obstruction can only be achieved by merging different psychoacoustic parameters. To our knowledge, the present study for the first time provides an acoustic classification in a large number of visually classified patterns of obstruction.
Snoring sounds and patterns of obstruction induced by DISE may vary from natural nocturnal snoring [30, 1]. This fact has to be taken into account when interpreting data of DISE. Up to now, no better method of getting obstructions and vibrations visualised than DISE is available, and nocturnal sleep endoscopy (during natural sleep) remains a goal, which seems hardly achievable in the near future on a routine basis.
DISE remains a valuable procedure for the detection of the site of obstruction. Often, a potential surgical therapy is based on the results of DISE [31, 32]. It needs to be discussed, whether the obtained data of obstruction site and acoustic characteristics of snoring resemble the nocturnal situation. Induced sleep does not resemble natural sleep in terms of brain activity, which is altered by drug application. It has been demonstrated, however, that respiratory parameters are not altered by drug-induced sleep [33]. The principle of DISE is based on this assumption. If the visualised patterns of obstructions and vibrations do not only exist in induced sleep but also in natural sleep, it can be assumed that the corresponding acoustic characteristics exist in both states as well. Apart from that, the present study does not aim to compare snoring sounds during natural and induced sleep. The main goal was to introduce an alternative way of acoustic analysis apart from simple frequency analyses in order to distinguish between different subgroups of acoustic characteristics.
Further research is needed to establish cut-off values for the different types of snoring. A simple algorithm to characterise different snoring samples taking all psychoacoustic parameters into account is suggested in Table 3. On the basis of these findings, a potential classification of vibration and obstruction patterns might lead to a more focused surgical approach in the treatment of snoring and obstructive sleep apnoea. Further research needs to evaluate the therapeutic outcome of specific surgical techniques in specific patterns of obstruction (e.g. surgery of the soft palate in a palatal collapse anterior–posterior vs. lateral or circular).
Conclusion
Different patterns of obstruction and vibration during DISE create specific psychoacoustic parameters. Psychoacoustic parameters enable a differentiation between visually classified patterns of vibration and obstruction in snoring episodes obtained during DISE. The “acoustic fingerprint” obtained might be a step towards an evaluation of nocturnal snoring sounds which can be performed during poly(somno)graphy on a routine basis in the future. The aim should be an algorithm for acoustic analysis which enables the differentiation between different sites of obstruction and vibration as well as apnoeic and non-apnoeic snoring which might contribute to a more individualised treatment of snoring.
References
Agrawal S, Stone P, McGuinness K, Morris J, Camilleri AE (2002) Sound frequency analysis and the site of snoring in natural and induced sleep. Clin Otolaryngol Allied Sci 27(3):162–166
Fiz JA, Abad J, Jane R, Riera M, Mananas MA, Caminal P, Rodenstein D, Morera J (1996) Acoustic analysis of snoring sound in patients with simple snoring and obstructive sleep apnoea. Eur Respir J 9(11):2365–2370
Herzog M, Schmidt A, Bremert T, Herzog B, Hosemann W, Kaftan H (2008) Analysed snoring sounds correlate to obstructive sleep disordered breathing. Eur Arch Otorhinolaryngol 265(1):105–113
Hill PD, Lee BW, Osborne JE, Osman EZ (1999) Palatal snoring identified by acoustic crest factor analysis. Physiol Meas 20(2):167–174
Miyazaki S, Itasaka Y, Ishikawa K, Togawa K (1998) Acoustic analysis of snoring and the site of airway obstruction in sleep related respiratory disorders. Acta Otolaryngol 537:47–51
Osborne JE, Osman EZ, Hill PD, Lee BV, Sparkes C (1999) A new acoustic method of differentiating palatal from non-palatal snoring. Clin Otolaryngol Allied Sci 24(2):130–133
Saunders NC, Tassone P, Wood G, Norris A, Harries M, Kotecha B (2004) Is acoustic analysis of snoring an alternative to sleep nasendoscopy? Clin Otolaryngol Allied Sci 29(3):242–246
Pevernagie D, Aarts RM, De Meyer M (2010) The acoustics of snoring. Sleep Med Rev 14(2):131–144. doi:10.1016/j.smrv.2009.06.002
Herzog M, Metz T, Schmidt A, Bremert T, Venohr B, Hosemann W, Kaftan H (2006) The prognostic value of simulated snoring in awake patients with suspected sleep-disordered breathing: introduction of a new technique of examination. Sleep 29(11):1456–1462
Herzog M, Schieb E, Bremert T, Herzog B, Hosemann W, Kaftan H, Kuhnel T (2008) Frequency analysis of snoring sounds during simulated and nocturnal snoring. Eur Arch Otorhinolaryngol 265(12):1553–1562. doi:10.1007/s00405-008-0700-2
Pringle MB, Croft CB (1993) A grading system for patients with obstructive sleep apnoea—based on sleep nasendoscopy. Clin Otolaryngol Allied Sci 18(6):480–484
Kezirian EJ, Hohenhorst W, de Vries N (2011) Drug-induced sleep endoscopy: the VOTE classification. Eur Arch Otorhinolaryngol 268(8):1233–1236. doi:10.1007/s00405-011-1633-8
Koo SK, Choi JW, Myung NS, Lee HJ, Kim YJ (2013) Analysis of obstruction site in obstructive sleep apnea syndrome patients by drug induced sleep endoscopy. Am J Otolaryngol 34(6):626–630. doi:10.1016/j.amjoto.2013.07.013
Ravesloot MJ, de Vries N (2011) One hundred consecutive patients undergoing drug-induced sleep endoscopy: results and evaluation. Laryngoscope 121(12):2710–2716. doi:10.1002/lary.22369
Steinhart H, Kuhn-Lohmann J, Gewalt K, Constantinidis J, Mertzlufft F, Iro H (2000) Upper airway collapsibility in habitual snorers and sleep apneics: evaluation with drug-induced sleep endoscopy. Acta Otolaryngol 120(8):990–994
Vroegop AV, Vanderveken OM, Boudewyns AN, Scholman J, Saldien V, Wouters K, Braem MJ, Van de Heyning PH, Hamans E (2013) Drug-induced sleep endoscopy in sleep-disordered breathing: report on 1249 cases. Laryngoscope. doi:10.1002/lary.24479
Dahaba AA, Xue JX, Xu GX, Liu QH, Metzler H (2011) Bilateral Bispectral Index (BIS)-Vista as a measure of physiologic sleep in sleep-deprived anesthesiologists. Minerva Anestesiol 77(4):388–393
Nieuwenhuijs D, Coleman EL, Douglas NJ, Drummond GB, Dahan A (2002) Bispectral index values and spectral edge frequency at different stages of physiologic sleep. Anesth Analg 94(1):125–129, table of contents
Sleigh JW, Andrzejowski J, Steyn-Ross A, Steyn-Ross M (1999) The bispectral index: a measure of depth of sleep? Anesth Analg 88(3):659–661
Herzog M, Bremert T, Herzog B, Hosemann W, Kaftan H, Muller A (2011) Analysis of snoring sound by psychoacoustic parameters. Eur Arch Otorhinolaryngol 268(3):463–470. doi:10.1007/s00405-010-1386-9
Fastl H, Zwicker, E. (2007) Springer series in information sciences, vol 22. 22 psychoacoustics facts and models, vol 35, Thrid edn. Springer, Berlin, Heidelberg, New York
Quinn SJ, Huang L, Ellis PD, Williams JE (1996) The differentiation of snoring mechanisms using sound analysis. Clin Otolaryngol Allied Sci 21(2):119–123
Beeton RJ, Wells I, Ebden P, Whittet HB, Clarke J (2007) Snore site discrimination using statistical moments of free field snoring sounds recorded during sleep nasendoscopy. Physiol Meas 28(10):1225–1236. doi:10.1088/0967-3334/28/10/008
Jones TM, Walker P, Ho MS, Earis JE, Swift AC, Charters P (2006) Acoustic parameters of snoring sound to assess the effectiveness of sleep nasendoscopy in predicting surgical outcome. Otolaryngol Head Neck Surg 135(2):269–275. doi:10.1016/j.otohns.2005.11.051
Won TB, Kim SY, Lee WH, Han DH, Kim DY, Kim JW, Rhee CS, Lee CH (2012) Acoustic characteristics of snoring according to obstruction site determined by sleep videofluoroscopy. Acta Otolaryngol 132(Suppl 1):S13–S20. doi:10.3109/00016489.2012.660733
Borek RC, Thaler ER, Kim C, Jackson N, Mandel JE, Schwab RJ (2012) Quantitative airway analysis during drug-induced sleep endoscopy for evaluation of sleep apnea. Laryngoscope 122(11):2592–2599. doi:10.1002/lary.23553
Hong SD, Dhong HJ, Kim HY, Sohn JH, Jung YG, Chung SK, Park JY, Kim JK (2013) Change of obstruction level during drug-induced sleep endoscopy according to sedation depth in obstructive sleep apnea. Laryngoscope 123(11):2896–2899. doi:10.1002/lary.24045
Rohrmeier C, Herzog M, Ettl T, Kuehnel TS (2013) Distinguishing snoring sounds from breath sounds: a straightforward matter? Sleep Breath. doi:10.1007/s11325-013-0866-8
Rohrmeier C, Herzog M, Haubner F, Kuehnel TS (2012) The annoyance of snoring and psychoacoustic parameters: a step towards an objective measurement. Eur Arch Otorhinolaryngol 269(5):1537–1543. doi:10.1007/s00405-011-1878-2
Jones TM, Ho MS, Earis JE, Swift AC, Charters P (2006) Acoustic parameters of snoring sound to compare natural snores with snores during ‘steady-state’ propofol sedation. Clin Otolaryngol 31(1):46–52
Eichler C, Sommer JU, Stuck BA, Hormann K, Maurer JT (2012) Does drug-induced sleep endoscopy change the treatment concept of patients with snoring and obstructive sleep apnea? Sleep Breath Schlaf Atmung. doi:10.1007/s11325-012-0647-9
Pilaete K, De Medts J, Delsupehe KG (2013) Drug-induced sleep endoscopy changes snoring management plan very significantly compared to standard clinical evaluation. Eur Arch Otorhinolaryngol. doi:10.1007/s00405-013-2795-3
Rabelo FA, Braga A, Kupper DS, De Oliveira JA, Lopes FM, de Lima Mattos PL, Barreto SG, Sander HH, Fernandes RM, Valera FC (2010) Propofol-induced sleep: polysomnographic evaluation of patients with obstructive sleep apnea and controls. Otolaryngol Head Neck Surg 142(2):218–224. doi:10.1016/j.otohns.2009.11.002
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Herzog, M., Plößl, S., Glien, A. et al. Evaluation of acoustic characteristics of snoring sounds obtained during drug-induced sleep endoscopy. Sleep Breath 19, 1011–1019 (2015). https://doi.org/10.1007/s11325-014-1085-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-014-1085-7