Abstract
Purpose
This study aimed to investigate the level of fertility related quality of life (FertiQoL) in women with recurrent pregnancy loss (RPL), and to further examine moderated mediation effects of dispositional mindfulness and negative emotions on the relationship between perceived stress and FertiQoL.
Methods
A cross-sectional study was conducted with 262 participants recruited from the infertility outpatient clinics. A self-administered, structured questionnaire including the Simplified Chinese version of FertiQoL tool, the Perceived Stress Scale-10 (PSS-10), the Chinese Version of the Hospital Anxiety and Depression Scale (HADS), and the Mindfulness Attention Awareness Scale (MAAS) was used to collect information in this research. The mediation model and moderated mediation model were conducted using the PROCESS macro for SPSS.
Results
The mean score of Core FertiQoL was 64.59 (SD = 14.76) among women with RPL. Mediation analysis revealed that the association between perceived stress and FertiQoL was partially mediated by negative emotions (indirect effect = − 0.194 for anxiety, and − 0.151 for depression, all P < 0.001). Moderated mediation analysis indicated that the indirect effects of perceived stress on FertiQoL through negative emotions were significantly moderated by dispositional mindfulness. Specifically, the indirect effects of perceived stress on FertiQoL through negative emotions decreased were significant as dispositional mindfulness levels increased.
Conclusion
Overall, women with RPL experienced poor FertiQoL. The Moderated mediation model provides a better understanding of how perceived stress, negative emotions and dispositional mindfulness work together to affect FertiQoL. Interventions aiming to improve FertiQoL in women with RPL should consider targeting these aspects.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Recurrent pregnancy loss (RPL) is defined as two or more failed clinical pregnancies prior to 24 weeks of gestation [1, 2]. It has been estimated to affect approximately 5% of women trying to conceive [3]. RPL is a traumatic life event [4] and could have harmful effects on the women’s psychological adjustment and health-related quality of life (QoL) [5, 6]. Previous literature reviews on psychological adjustment to RPL suggested that most of women with a history of pregnancy loss experience difficulty in psychological adjustment leading to depression and/or anxiety that last for several months [7, 8]. Furthermore, various quantitative studies have revealed that women with recurrent miscarriage reported extensive functional disability and lower level of QoL compared with that of women without recurrent miscarriage [5, 9]. However, little is known of the related factors and underlying mechanisms of impact on QoL by RPL-factors that are very important for the promotion of optimal health for women with history of RPL.
Psychological stress, one of the common conditions among women who have experienced RPL [10], is considered as an important contributor to reduced QoL in general [11, 12]. The effect of perceived stress on QoL has been reported in previous studies [11,12,13], which found that perceived stress could not only directly predict lower QoL, but also influence QoL through negative emotions [11, 13] such as anxiety and/or depression. A cross-sectional study has shown that psychological stress was a significant predictor of low infertility-related QoL experienced by women who underwent fertility treatment in Taiwan [14]. In addition, studies confirmed the predictive effects of infertility-related stress on negative emotions [15, 16], which in turn led to diminished QoL in women with infertility [17, 18]. Accordingly, negative emotions could mediate the effect of perceived stress on QoL, but their specific influence in women with RPL is not well described. Moreover, in view of the higher prevalence of self-reported stress and negative emotions among RPL patients [6, 19], the underlying pathways of negative emotions require further exploration.
Mindfulness is defined as the awareness that emerges through purposefully paying attention, in the present moment and nonjudgmentally, to the unfolding of experiences moment by moment [20]. Dispositional mindfulness has been considered to be an inherent, yet modifiable, trait, where all people have varying capacities to attend and to be aware of what is occurring in the present moment [21]. Many studies of dispositional mindfulness to date have theoretically and empirically reported positive correlations with psychological well-being [22, 23]. Dispositional mindfulness encourages individuals to view thoughts and feelings as temporary mental events rather than facts [24], facilitates disengagement of attention in the face of unpleasant stimuli [25, 26], and enhances brain functioning associated with a positive mood [27, 28]. According to the stress-buffering role of mindfulness [29], psychological stress interacting with dispositional mindfulness could buffer against the negative impact of psychological stress. Studies have shown that mindful individuals may have greater abilities to handle a set of stressors by greater awareness of symptoms of stress at low levels and greater tendency to receptively observe stressors with acceptance and equanimity [29,30,31], which could help alleviate the negative effects of psychological stress on mental health outcomes and psychological well-being. Such moderating effect of dispositional mindfulness has been reported for groups of undergraduate students [29, 32], community adults [33, 34], and clinical populations [35, 36]. Besides, specific studies have referred to dispositional mindfulness for having moderated the association of negative emotions and physiological stress reactivity [30, 37, 38]. However, whether dispositional mindfulness produces a directly or indirectly protective effect for the negative impact of psychological stress on QoL in women with RPL is unknown.
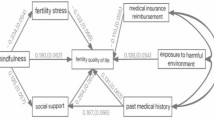
Given the high rate of poor QoL in women with RPL found in previous studies combined with the lack of information focused on both the negative and positive indicators of psychological adjustment outcomes, this study pursued three specific goals: first, to test how perceived stress, negative emotions (anxiety and depression), dispositional mindfulness, and QoL are interrelated in women with RPL; second, to examine whether anxiety and depression mediate the relationship between perceived stress and QoL; and third, to detect whether moderating effect of dispositional mindfulness exists in the relationship between perceived stress and QoL, and test whether dispositional mindfulness serves as a buffering mechanism in the “perceived stress—negative emotions—QoL” mediation pathway (see Fig. 1).
Materials and methods
Participants
A cross-sectional survey was conducted from the infertility outpatient clinics at the Reproductive Medical Center of Shandong University between September 2017 and October 2018. The study was approved by the Institutional Review Board of Reproductive Medical Center of Shandong University (project number 2017-51). Informed consent was obtained from all individual participants included in the study. All patients attending the infertility outpatient clinic were consecutively recruited by a trained nurse. The inclusion criteria were as follows: (i) age more than 18, (ii) a history of two or more miscarriages or stillbirths before 24 weeks of gestation, and (iii) ability to understand and answer the questionnaires. The exclusion criterion was having a history of mental illness or a severe medical condition that could interfere with the baseline measurements. The estimated sample size was 189, based on a moderate f2 effect size of 0.15, α of 0.05, power of 0.95, and total number of predictors of 13 using G*Power [39]. Of 280 women who met the inclusion criteria and were invited to participate in this study, 276 consented and completed the questionnaires. After eliminating incomplete questionnaires, 262 women with RPL remained for analysis. A comparison of the 14 excluded women with the 262 included participants found no significant differences in the demographic or clinical-related variables.
Measures
The data were collected using a self-administered, structured questionnaire, which included a study-specific questionnaire on sociodemographic variables and clinically relevant information. To assess psychological adjustment related to RPL, scales measuring perceived stress, dispositional mindfulness, negative emotion, and fertility relevant QoL were administered.
The demographic and clinical questionnaire was designed by the authors and included participant’s age, marriage duration, education, monthly incomes, employment status, number of live born children, number of abortions, history of assisted reproductive technology (ART) use, and duration of infertility.
The Perceived Stress Scale-10 (PSS-10) was used to assess the degree to which the participants appraised events as stressful during the past month [40]. It consists of 10 items that rate on a 5-points Likert scale ranging from 0 (never) to 4 (very often). The total score of the PSS-10 ranges from 0 to 40, with higher scores indicating more stress. This scale has been verified with good reliability and validity in China [41, 42]. The Cronbach’s alpha in this study was 0.837.
The Mindfulness Attention Awareness Scale (MAAS) is the most widely used trait mindfulness scale to measure how frequently individuals are in mindful states over time [21]. It has 15 items using a 6-point Likert scale ranging from 1 (almost always) to 6 (almost never). High scores reflect high levels of trait mindfulness. The Chinese version of the MAAS is regarded as a good measurement of dispositional mindfulness with good reliability and validity [43, 44]. In the current study, the Cronbach’s alpha was 0.862.
The Chinese Version of the Hospital Anxiety and Depression Scale (HADS) is a commonly used self-report scale to assess the levels of anxiety and depression among patients in nonpsychiatric hospital clinics [45]. It consists of a seven-item anxiety subscale (HADS-A) and a seven-item depression subscale (HADS-D). Item responses are graded on a four-point Likert-type scale (0–3). The scores in each subscale are computed by summing the corresponding items, with higher scores indicating higher anxiety and depression. In the current study, the Cronbach’s alphas of two subscales were 0.862 and 0.816, respectively.
The Simplified Chinese version of the Fertility Quality of Life (FertiQoL) tool is a disease-specific instrument and designed for all people experiencing fertility problems to assess their QoL, including the Core FertiQoL module and the optional treatment module [46]. The 24 items from the Core FertiQoL are categorized into four domains, including emotional, mind–body, relational, and social domains. The 10 items from optional treatment module are conceptualized as treatment environment and treatment tolerability, which assess current thoughts and feelings directly related to fertility treatment. Items from these domains are presented in the questionnaire randomly and rated on a scale of 0–4. The FertiQoL yields six subscale and three total scores with a range of 0 to 100. The FertiQoL tool has been translated into 20 different languages and is available on the FertiQoL website (www.fertiqol.org/). In this study, We just analyzed for the Core FertiQoL module since the treatment module was unsuitable to some participants who were enrolled in the diagnostic phase without any infertility treatment. The score of the Core FertiQoL is the average scores of all four subscales, ranging from 0 to 100. Higher scores mean higher Core FertiQoL. The Cronbach’s alpha for the Core FertiQoL module was 0.813 and ranged between 0.779 and 0.847 for the subscales.
Statistical analysis
Data analysis were conducted by SPSS version 22.0 (IBM Corp. 2013). Mean ± Standard Deviations (after confirmation of normal distribution using the Kolmogorov–Smirnov test), frequency, and percentages were used to describe the characteristics of the patients. Independent t test and analysis of variance analysis (ANOVA) were used to examine the differences in Core FertiQoL by sample characteristics. Pearson’s correlations were used to examine the associations among perceived stress, dispositional mindfulness, anxiety and depression, and Core FertiQoL.
Figure 1 shows a theoretical model to assess the role of dispositional mindfulness, anxiety, and depression in the relationship between perceived stress and Core FertiQoL, the mediation and moderated mediation model were conducted using the SPSS PROCESS V3.2 macro developed by Hayes [47]. First, anxiety and depression were set separately as mediator in the relationship between perceived stress and Core FertiQoL using Model 4 [48]. Bootstrapping procedures were set to 5000 samples and were used to test the estimated indirect effects. If the 95% CI of indirect effect did not contain 0, it indicated that the mediating effect was significant. Next, Model 59 [48] was used to examine the moderated mediation effect that was whether dispositional mindfulness moderated the direct and indirect effects (through anxiety or depression) of perceived stress on Core FertiQoL. A conceptual framework of the Model 4 and Model 59 is presented in Figs. 1 and 2, respectively. The simple slope test by both pick-a-point method and the Johnson–Neyman method using the PROCESS macro were performed to test the significance of the moderation effect. The procedure of pick-a-point method involves selecting a value or values of the moderator, calculating the conditional effect of X on Y at that value or values, and generating a confidence interval [49]. The Johnson–Neyman method is essentially the pick-a-point approach conducted in reverse [49]. All mediation and moderated mediation models had adjusted for covariates that were significantly associated with Core FertiQoL in the univariate analyses. To avoid multi-collinearity effects, four main variables (perceived stress, dispositional mindfulness, anxiety and depression) were standardized in all models. P values reported were two tailed, and p value < 0.05 was considered significant.
Anxiety and depression mediate the relationship between perceived stress and Core FertiQoL. Path coefficients to the left of the “/” were for analysis using anxiety as mediator. Path coefficients to the right of the “/” were for analysis using depression as mediator. Educational, Monthly incomes, ART history, and Infertility duration were entered as covariates in all analyses. FertiQoL fertility quality of life, ART assisted reproduction technique. *P < 0.05, **P < 0.01, ***P < 0.001
Results
Sociodemographic characteristics and core FertiQoL
The participants’ demographic characteristics are listed in Table 1. Of the 262 participants, with a mean age of 32.32 (SD = 5.45), 43.9% had completed at least a college education; 55.1% were predominantly manual workers; 29.4% had a low average monthly household income (< ¥3000); 59.6% were employed; and 71.0% had at least one live birth child. The mean number of pregnancy losses was 3.18 (SD = 1.23), and 66.4% had a history of three or more pregnancy losses; 86.6% had never received ART. The mean score of Core FertiQoL was 64.59 (SD = 14.76). The independent t test and ANOVA results showed that the Core FertiQoL scores were significantly different based on the level of education (F = 3.468, P = 0.033), monthly incomes (F = 9.475, P < 0.001), and ART history (t = 2.555, P = 0.011). In addition, Pearson correlation analysis showed that there was significant correlation between infertility duration and Core FertiQoL scores (r = − 0.172, P = 0.007), and the Core FertiQoL scores were not significantly different with other sociodemographic data (Table 2).
Correlational analyses
Results from Pearson correlation analyses revealed that Core FertiQoL was negatively associated with perceived stress (r = − 0.530, P < 0.001) and the two negative emotions (r = − 0.561, P < 0.001 for anxiety; r = − 0.502, P < 0.001 for depression), and positively associated with dispositional mindfulness (r = 0.448, P < 0.001). Besides, the four subscale scores of Core FertiQoL, including emotional, mind–body, relational and social, were all significantly negatively associated with perceived stress (all P < 0.001) and the two negative emotions (all P < 0.001 for anxiety and depression), and positively associated with dispositional mindfulness (all P < 0.01). Moreover, perceived stress was positively associated with both anxiety (r = 0.577, P < 0.001) and depression (r = 0.653, P < 0.001), and negatively associated with dispositional mindfulness (r = − 0.469, P < 0.001). Dispositional mindfulness was negatively associated with the two negative emotions (r = − 0.568, P < 0.001 for anxiety; r = − 0.445, P < 0.001 for depression).
Mediation analysis
Results presented in Fig. 2 indicated significant indirect effects of anxiety and depression in mediating the association between perceived stress and Core FertiQoL (− 0.194 for anxiety, P < 0.001; and -0.151 for depression, P < 0.001). The bootstrapped 95% CI did not include 0 for the indirect effect of perceived stress on the Core FertiQoL scores through two negative emotions (− 0.269 to − 0.125 for anxiety, P < 0.001; and − 0.235 to − 0.080 for depression, P < 0.001), confirming the significant indirect effect. The direct effect of perceived stress on Core FertiQoL was significant after analyzing for mediation (− 0.287, P < 0.001 for anxiety; and − 0.330, P < 0.001 for depression), indicating a partial mediation of negative emotions. The mediation effect ratios of anxiety and depression were 30.3% (− 0.194/− 0.287–0.194 × 100%) and 31.4% (− 0.151/− 0.330–0.151 × 100%), respectively.
Moderated mediation analyses
Moderated mediation analysis established whether dispositional mindfulness moderated the direct and indirect effect (through anxiety) of perceived stress on Core FertiQoL. Figure 3 shows the results of moderated mediation model. The results revealed that dispositional mindfulness (β = − 0.086, P = 0.041) only moderated the relationships between perceived stress and anxiety. The results of the Johnson-Neyman method demonstrated that the effects of perceived stress on anxiety were significant across the levels of dispositional mindfulness. The pick-a-point method (Table 3) indicated that the positive effects of perceived stress on anxiety decreased as dispositional mindfulness increased under three different levels (low, one standard deviation below mean; medium, mean; high, one standard deviation above mean). Figure 4 illustrates the different slopes associated with different dispositional mindfulness levels. In addition, the conditional indirect effects of perceived stress on core FertiQoL through anxiety at various levels of dispositional mindfulness were examined and listed in Table 4. The results showed that the conditional indirect effect decreased were significant as dispositional mindfulness levels increased. The bootstrapped 95% CI did not include 0 for the pairwise contrasts between conditional indirect effects, which further confirmed that the mediation effect was moderated by dispositional mindfulness.
Moderation effect of dispositional mindfulness on the link between perceived stress and Core FertiQoL through anxiety. Educational, Monthly incomes, ART history, and Infertility duration were entered as covariates in all analyses. FertiQoL fertility quality of life, ART assisted reproduction technique. *P < 0.05, **P < 0.01, ***P < 0.001
Similarly, moderated mediation analysis established whether dispositional mindfulness moderated the direct and indirect effect (through depression) of perceived stress on Core FertiQoL. Figure 5 shows the results of moderated mediation model. The results revealed that dispositional mindfulness (β = 0.188, P = 0.003) only moderated the relationships between depression and Core FertiQoL. The results of the Johnson–Neyman method demonstrated that the effects of depression on Core FertiQoL were significant when the standard scores of dispositional mindfulness were lower than 0.45. The pick-a-point method (Table 5) indicated that the negative effects of depression on Core FertiQoL decreased as dispositional mindfulness increased under three different levels (low, one standard deviation below mean; medium, mean; high, one standard deviation above mean). Figure 6 illustrates the different slopes associated with different dispositional mindfulness levels. In addition, the conditional indirect effects of perceived stress on core FertiQoL through depression at various levels of dispositional mindfulness were examined and listed in Table 6. The results showed that the conditional indirect effect decreased were significant as dispositional mindfulness levels increased. The bootstrapped 95% CI did not include 0 for the pairwise contrasts between conditional indirect effects, which further confirmed that the mediation effect was moderated by dispositional mindfulness.
Moderation effect of dispositional mindfulness on the link between perceived stress and Core FertiQoL through depression. Educational, Monthly incomes, ART history, and Infertility duration were entered as covariates in all analyses. FertiQoL fertility quality of life, ART assisted reproduction technique. *P < 0.05, **P < 0.01, ***P < 0.001
Discussion
This study investigated the FertiQoL in women with RPL and examined the relationships between perceived stress, negative emotions, dispositional mindfulness, and FertiQoL. The findings showed that participants experienced comparable poor FertiQoL than that found in infertile women in Aarts’s studies [50] (e.g., N = 473, Means = 70.8, SD = 13.9, which is significantly higher than this study at P < 0.05), which was consistent with previous studies [9]. The results of univariate analyses showed that core FertiQoL in women with RPL was significantly different depending on education, monthly income, history of ART, and duration of infertility. Participants who had lower education level, lower monthly income, and longer duration of infertility experienced poor core FertiQoL, which confirmed results from previous studies [51,52,53]. The analysis of the history of having used ART related to QoL was a topic of interest in previous studies. Chachamovich and colleagues reported that previous in vitro fertilization (IVF) was associated with lower vitality and poor psychological health scores [54]. However, Nilay et al. [55] demonstrated better FertiQoL results regarding the orientation to the treatment environment in the couples with a previous IVF failure compared to couples without history of IVF failure. The present study revealed that RPL women who had a history of having used ART had lower FertiQoL. It is conceivable that the uncertainty of treatment outcomes combined with financial impact of ART may have exacerbated psychological stress in women who had a history of ART [10].
As expected, the results showed that perceived stress, anxiety, and depression were significantly associated with the FertiQoL. The two negative emotions of anxiety and depression partially mediated the relationship between perceived stress and FertiQoL. That was, perceived stress directly predicted not only decreased FertiQoL, but also increased anxiety and depression, which in turn was related to decreased FertiQoL. This finding in keeping with those of previous studies among women in late pregnancy and infertile women where perceived stress may increase negative emotions, and subsequently, have a negative impact on health-related QoL [13, 56]. The potential mechanism for this may be that women after a miscarriage would suffer from a grief reaction and have doubts about procreative competence, contributing to increasing anxiety and depressive [4, 8]. Women with elevated levels of negative emotions would be at higher risk of miscarriage by dysregulation of the activation of the hypothalamic–pituitary–adrenal axis [57, 58] contributing to a deteriorating FertiQoL. Moreover, there were indeed significant negative correlations between negative emotions and the emotional subscale of the FertiQoL. Given that emotions are an important domain of the core FertiQoL, it is expected that there would be a reciprocal relationship between negative emotions (anxiety and depression) and deteriorating FertiQoL.
Additionally, the moderated mediation analysis revealed that dispositional mindfulness moderated the relationship between perceived stress and FertiQoL through negative emotions. More specifically, the indirect effects of perceived stress on FertiQoL through negative emotions were attenuated in the women with higher dispositional mindfulness, and reinforced in those with lower dispositional mindfulness. As predicted by stress-buffering role of mindfulness, dispositional mindfulness buffered the negative influence of perceived stress and negative emotions. These findings were consistent with the results of several other studies. By studying 292 patients with digestive tract cancer, Zhong et al. found that dispositional mindfulness buffered the negative impact of perceived stress on psychological symptoms [36]. In a number of studies in adults, previous researches suggested that dispositional mindfulness buffered the impact of negative emotions on physiological arousal [30, 38]. Within the context of this study, dispositional mindfulness might facilitate better self-regulation of emotional and cognitive activities and reduce reactions to potentially emotional and stressful stimuli. With such response styles, it is plausible that mindful women with RPL would be better able to regulate their emotional responses to miscarriage and let go of negative emotions. Women with higher levels of mindfulness would be mindfully aware of and accommodate miscarriage related negative thoughts and emotions, which may facilitate a transition from grief and passiveness to senses of perceived control and self-efficacy to deal with miscarriage. These improvements in appraising and reacting to psychological stress resulted from miscarriage help women with RPL avoid negative emotions and achieve better FertiQoL. Therefore, this evidence of the protective role of dispositional mindfulness in buffering the negative effect of perceived stress highlights that interventions to improve the FertiQoL among women with RPL should integrate components that enhance dispositional mindfulness. In fact, trait mindfulness as an essential psychological intervention target could be addressed by the Mindfulness Based Program for Infertility, which has been applied and has shown consistent effectiveness in infertile women in term of mindfulness, experiential avoidance, and depression and anxiety symptoms [59]. However, it should to be emphasized that the moderating effect of dispositional mindfulness was not significant on the directly effect of perceived stress on FertiQoL, which was inconsistent with a previous study [60]. One explanation for this might be the difference of samples (population-based sample vs. women with RPL) and stressors (general stressors vs. miscarriage). Moreover, perhaps when dealing with deterioration in QoL resulted from a traumatic life stressor such as a miscarriage, high trait mindfulness is not enough, and actual mindfulness-based stress reduction practice may be necessary [61].
Strengths and limitations
This study advances the current state of knowledge by explaining the relationships among perceived stress, anxiety, depression, dispositional mindfulness, and FertiQoL in women with RPL. Specifically, the present study contributes to literature by investigating possible psychological mechanisms that may underlie the relationship between psychological stress and FertiQoL-increased negative emotions. Moreover, the results verify that dispositional mindfulness was a protective factor for alleviating or eliminating the indirect effects of perceived stress on FertiQoL through negative emotions. Based on these findings, interventions designed to encourage adaptive stress management, improve mindfulness levels, and provide the necessary skills to deal with stressful situations are likely to reduce or eliminate psychological stress and negative emotions and improve the FertiQoL in women with RPL.
Despite these findings, several limitations should be mentioned. First, many confounding factors that might influence the results were not collected, such as data on some important reproductive information including gestational age at miscarriage, and reason for miscarriage. For future studies, a better study design and a thorough collection of data are recommended. Second, the findings were not adjusted for multiple comparisons, which might lead to increase the likelihood of obtaining at least one false-positive result. So the conclusions regarding the results of multiple comparisons should be interpreted with caution. In fact, most of the comparisons showed differences at a P-value < 0.01 in this study, which could be interpreted as trend values. Additionally, considering that the purpose of multiple comparisons was just to fully identify potential confounding factors related to the FertiQoL, the adjusted p-values might result in increasing the number of instances that the significant factors were rejected when in fact it should not have been. so we did not adjust for p-values in this study. Third, due to study’s cross-sectional design and small sample recruited from only one center in Shandong Province, the causal inference among study variables and generalizability of the results are limited. Longitudinal research with a larger multicenter sample size is required for further verification. In addition, the assessments were based on participants’ self-reporting, which might be subject to information bias.
Conclusion
This is the first investigation of a relationship between perceived stress and FertiQoL in women with RPL using a moderated mediation model. The poor FertiQoL were experienced in women with RPL, especially who were in lower education level, lower monthly income, and had longer duration of infertility and historically used ART. Anxiety and depression could mediate the association of perceived stress and FertiQoL. Moreover, dispositional mindfulness played a moderating role in indirect effects of perceived stress on FertiQoL through negative emotions, in which indirect effects were attenuated with the dispositional mindfulness increasing. As a result, future interventions seeking to improve FertiQoL in women with RPL should include alleviating negative emotions (anxiety and depression) and increasing dispositional mindfulness as primary intervention targets.
References
Practice Committee of the American Society for Reproductive Medicine. (2013). Definitions of infertility and recurrent pregnancy loss: a committee opinion. Fertility and Sterility,99(1), 63. https://doi.org/10.1016/j.fertnstert.2012.09.023.
Bender Atik, R., Christiansen, O. B., Elson, J., Kolte, A. M., Lewis, S., Middeldorp, S., et al. (2018). ESHRE guideline: recurrent pregnancy loss. Human Reproductive Open. https://doi.org/10.1093/hropen/hoy004.
Rai, R., & Regan, L. (2006). Recurrent miscarriage. The Lancet,368(9535), 601–611.
Bellhouse, C., Temple-Smith, M., Watson, S., & Bilardi, J. (2019). "The loss was traumatic.. some healthcare providers added to that": Women's experiences of miscarriage. Women Birth,32(2), 137–146. https://doi.org/10.1016/j.wombi.2018.06.006.
Abbaspoor, Z., Razmju, P. S., & Hekmat, K. (2016). Relation between quality of life and mental health in pregnant women with prior pregnancy loss. Journal of Obstetrics and Gynaecology Research,42(10), 1290–1296. https://doi.org/10.1111/jog.13061.
He, L., Wang, T., Xu, H., Chen, C., Liu, Z., Kang, X., et al. (2019). Prevalence of depression and anxiety in women with recurrent pregnancy loss and the associated risk factors. Archives of Gynecology and Obstetrics,300(4), 1061–1066. https://doi.org/10.1007/s00404-019-05264-z.
Lok, I. H., & Neugebauer, R. (2007). Psychological morbidity following miscarriage. Best Practice & Research Clinical Obstetrics & Gynaecology,21(2), 229–247.
Farren, J., Mitchell-Jones, N., Verbakel, J. Y., Timmerman, D., Jalmbrant, M., & Bourne, T. (2018). The psychological impact of early pregnancy loss. Human Reproductive Update,24(6), 731–749. https://doi.org/10.1093/humupd/dmy025.
Tavoli, Z., Mohammadi, M., Tavoli, A., Moini, A., Effatpanah, M., Khedmat, L., et al. (2018). Quality of life and psychological distress in women with recurrent miscarriage: a comparative study. Health and Quality of Life Outcomes,16(1), 150.
Coughlan, C., Walters, S., Ledger, W., & Li, T. C. (2014). A comparison of psychological stress among women with and without reproductive failure. International Journal of Gynecology & Obstetrics,124(2), 143–147.
Seo, E. J., Ahn, J. A., Hayman, L. L., & Kim, C. J. (2018). The association between perceived stress and quality of life in university students: The parallel mediating role of depressive symptoms and health-promoting behaviors. Asian Nursing Research,12(3), 190–196. https://doi.org/10.1016/j.anr.2018.08.001.
Yang, J., Guo, J., Tang, Y., Huang, L., Wiley, J., Zhou, Z., et al. (2019). The mediating effect of coping styles and self-efficacy between perceived stress and satisfaction with QOL in Chinese adolescents with type 1 diabetes. Journal of Advanced Nursing,75(7), 1439–1449. https://doi.org/10.1111/jan.13933.
Zhang, H., Zhang, Q., Gao, T., Kong, Y., Qin, Z., Hu, Y., et al. (2019). Relations between stress and quality of life among women in late pregnancy: The parallel mediating role of depressive symptoms and sleep quality. Psychiatry Investigation,16(5), 363–369. https://doi.org/10.30773/pi.2019.02.14.
Cheng, C. Y., Stevenson, E. L., Yang, C. T., & Liou, S. R. (2018). Stress and quality of life for Taiwanese women who underwent infertility treatment. Journal of Obstetric, Gynecologic, and Neonatal Nursing,47(4), 498–508. https://doi.org/10.1016/j.jogn.2018.03.005.
Gana, K., & Jakubowska, S. (2016). Relationship between infertility-related stress and emotional distress and marital satisfaction. Journal of Health Psychology,21(6), 1043–1054. https://doi.org/10.1177/1359105314544990.
Kim, J. H., Shin, H. S., & Yun, E. K. (2018). A dyadic approach to infertility stress, marital adjustment, and depression on quality of life in infertile couples. Journal of Holistic Nursing,36(1), 6–14. https://doi.org/10.1177/0898010116675987.
Shahraki, Z., Ghajarzadeh, M., & Ganjali, M. (2019). Depression, anxiety, quality of life and sexual dysfunction in Zabol women with infertility. Maedica (Buchar),14(2), 131–134. https://doi.org/10.26574/maedica.2019.14.2.131.
Shahraki, Z., Tanha, F. D., & Ghajarzadeh, M. (2018). Depression, sexual dysfunction and sexual quality of life in women with infertility. BMC Womens Health,18(1), 92. https://doi.org/10.1186/s12905-018-0584-2.
Kolte, A. M., Olsen, L. R., Christiansen, O. B., Schmidt, L., & Nielsen, H. S. (2019). Pregnancy outcomes after recurrent pregnancy loss: A longitudinal cohort study on stress and depression. Reprod Biomed Online,38(4), 599–605. https://doi.org/10.1016/j.rbmo.2018.12.006.
Kabat-Zinn, J. (2003). Mindfulness-based interventions in context: Past, present, and future. Clinical Psychology: Science and Practice,10(2), 144–156. https://doi.org/10.1093/clipsy.bpg016.
Brown, K. W., & Ryan, R. M. (2003). The benefits of being present: mindfulness and its role in psychological well-being. Journal of Personality and Social Psychology,84(4), 822–848. https://doi.org/10.1037/0022-3514.84.4.822.
Hicks, A., Phillips, K., Siwik, C., Salmon, P., Litvan, I., Jablonski, M. E., et al. (2019). The role of dispositional mindfulness in a stress-health pathway among Parkinson's disease patients and caregiving partners. Quality of Life Research,28(10), 2705–2716. https://doi.org/10.1007/s11136-019-02217-6.
Sala, M., Rochefort, C., Lui, P. P., & Baldwin, A. S. (2019). Trait mindfulness and health behaviours: A meta-analysis. Health Psychology Review. https://doi.org/10.1080/17437199.2019.1650290.
Chiesa, A., Serretti, A., & Jakobsen, J. C. (2013). Mindfulness: top-down or bottom-up emotion regulation strategy? Clinical Psychology Review,33(1), 82–96. https://doi.org/10.1016/j.cpr.2012.10.006.
Britton, W. B., Shahar, B., Szepsenwol, O., & Jacobs, W. J. (2012). Mindfulness-based cognitive therapy improves emotional reactivity to social stress: results from a randomized controlled trial. Behavior Therapy,43(2), 365–380. https://doi.org/10.1016/j.beth.2011.08.006.
Feldman, G., Lavalle, J., Gildawie, K., & Greeson, J. M. (2016). Dispositional mindfulness uncouples physiological and emotional reactivity to a laboratory stressor and emotional reactivity to executive functioning lapses in daily life. Mindfulness (N Y),7(2), 527–541. https://doi.org/10.1007/s12671-015-0487-3.
Mascaro, J. S., Rilling, J. K., Negi, L. T., & Raison, C. L. (2013). Pre-existing brain function predicts subsequent practice of mindfulness and compassion meditation. Neuroimage,69, 35–42. https://doi.org/10.1016/j.neuroimage.2012.12.021.
Way, B. M., Creswell, J. D., Eisenberger, N. I., & Lieberman, M. D. (2010). Dispositional mindfulness and depressive symptomatology: Correlations with limbic and self-referential neural activity during rest. Emotion,10(1), 12–24.
Bergin, A. J., & Pakenham, K. I. (2016). The stress-buffering role of mindfulness in the relationship between perceived stress and psychological adjustment. Mindfulness,7(4), 928–939.
Daubenmier, J., Hayden, D., Chang, V., & Epel, E. (2014). It's not what you think, it's how you relate to it: Dispositional mindfulness moderates the relationship between psychological distress and the cortisol awakening response. Psychoneuroendocrinology,48, 11–18. https://doi.org/10.1016/j.psyneuen.2014.05.012.
Lucas-Thompson, R. G., Miller, R. L., Seiter, N. S., & Prince, M. A. (2019). Dispositional mindfulness predicts cortisol, cardiovascular, and psychological stress responses in adolescence. Psychoneuroendocrinology,110, 104405. https://doi.org/10.1016/j.psyneuen.2019.104405.
Bravo, A. J., Pearson, M. R., Stevens, L. E., & Henson, J. M. (2016). Depressive symptoms and alcohol-related problems among college students: A moderated-mediated model of mindfulness and drinking to Cope. Journal of Studies on Alcohol and Drugs,77(4), 661–666. https://doi.org/10.15288/jsad.2016.77.661.
Su, M. R., & Shum, K. K. (2019). The moderating effect of mindfulness on the mediated relation between critical thinking and psychological distress via cognitive distortions among adolescents. Frontiers in Psychology,10, 1455. https://doi.org/10.3389/fpsyg.2019.01455.
Sugiura, Y., & Sugiura, T. (2018). Mindfulness as a moderator in the relation between income and psychological well-being. Frontiers in Psychology,9, 1477. https://doi.org/10.3389/fpsyg.2018.01477.
Rudaz, M., Ledermann, T., & Grzywacz, J. G. (2018). Spiritual coping, perceived growth, and the moderating role of spiritual mindfulness in cancer survivors. Journal of Psychosocial Oncology,36(5), 609–623. https://doi.org/10.1080/07347332.2018.1464091.
Zhong, M., Goh, P. H., Li, D., Bao, J., & Xu, W. (2017). Dispositional mindfulness as a moderator between perceived stress and psychological symptoms in Chinese digestive tract cancer patients. Journal of Health Psychology. https://doi.org/10.1177/1359105317736576.
Skoranski, A., Kelly, N. R., Radin, R. M., Thompson, K. A., Galescu, O., Demidowich, A. P., et al. (2018). Relationship of mindfulness to distress and cortisol response in adolescent girls at-risk for type 2 diabetes. Journal of Child and Family Studies,27(7), 2254–2264. https://doi.org/10.1007/s10826-018-1065-9.
Brown, K. W., Weinstein, N., & Creswell, J. D. (2012). Trait mindfulness modulates neuroendocrine and affective responses to social evaluative threat. Psychoneuroendocrinology,37(12), 2037–2041. https://doi.org/10.1016/j.psyneuen.2012.04.003.
Faul, F., Erdfelder, E., Buchner, A., & Lang, A. G. (2009). Statistical power analyses using G*Power 3.1: Tests for correlation and regression analyses. Behavior Research Methods,41(4), 1149–1160. https://doi.org/10.3758/brm.41.4.1149.
Cohen, S., Kamarck, T., & Mermelstein, R. (1983). A global measure of perceived stress. Journal of Health and Social Behavior,24(4), 385–396.
Leung, D. Y., Lam, T. H., & Chan, S. S. (2010). Three versions of Perceived Stress Scale: Validation in a sample of Chinese cardiac patients who smoke. BMC Public Health,10, 513. https://doi.org/10.1186/1471-2458-10-513.
Lu, W., Bian, Q., Wang, W., Wu, X., Wang, Z., & Zhao, M. (2017). Chinese version of the Perceived Stress Scale-10: A psychometric study in Chinese university students. PLoS ONE,12(12), e0189543. https://doi.org/10.1371/journal.pone.0189543.
Deng, Y.-Q., Li, S., Tang, Y.-Y., Zhu, L.-H., Ryan, R., & Brown, K. (2012). Psychometric properties of the Chinese translation of the mindful attention awareness scale (MAAS). Mindfulness (N Y),3(1), 10–14.
Lianchao, A., & Tingting, M. (2020). Mindfulness, rumination and post-traumatic growth in a Chinese cancer sample. Psychol Health Med,25(1), 37–44. https://doi.org/10.1080/13548506.2019.1612079.
Chan, Y.-F., Leung, D. Y. P., Fong, D. Y. T., Leung, C.-M., & Lee, A. M. (2010). Psychometric evaluation of the Hospital Anxiety and Depression Scale in a large community sample of adolescents in Hong Kong. Quality of Life Research,19(6), 865–873. https://doi.org/10.1007/s11136-010-9645-1.
Boivin, J., Takefman, J., & Braverman, A. (2011). The Fertility Quality of Life (FertiQoL) tool: Development and general psychometric properties. Fertility & Sterility,96(2), 409–415.e403.
Hayes, A. F., & Rockwood, N. J. (2017). Regression-based statistical mediation and moderation analysis in clinical research: Observations, recommendations, and implementation. Behaviour Research and Therapy,98, 39–57. https://doi.org/10.1016/j.brat.2016.11.001.
Hayes, A. F. (2018). Introduction to mediation, moderation, and conditional process analysis second edition: A regression-based approach. New York, NY: Guilford Press.
Hayes, A. F., & Matthes, J. (2009). Computational procedures for probing interactions in OLS and logistic regression: SPSS and SAS implementations. Behavior Research Methods,41(3), 924–936. https://doi.org/10.3758/brm.41.3.924.
Aarts, J. W., van Empel, I. W., Boivin, J., Nelen, W. L., Kremer, J. A., & Verhaak, C. M. (2011). Relationship between quality of life and distress in infertility: A validation study of the Dutch FertiQoL. Human Reproduction,26(5), 1112–1118. https://doi.org/10.1093/humrep/der051.
Hasson, J., Tulandi, T., Shavit, T., Shaulov, T., Seccareccia, E., & Takefman, J. (2017). Quality of life of immigrant and non-immigrant infertile patients in a publicly funded in vitro fertilisation program: A cross-sectional study. BJOG,124(12), 1841–1847. https://doi.org/10.1111/1471-0528.14709.
Goker, A., Yanikkerem, E., Birge, O., & Kuscu, N. K. (2018). Quality of life in Turkish infertile couples and related factors. Human Fertility (Cambridge),21(3), 195–203. https://doi.org/10.1080/14647273.2017.1322223.
ZurloCattaneo DellaVoltaVallone, M. C. M. F. F. (2018). Predictors of quality of life and psychological health in infertile couples: The moderating role of duration of infertility. Quality of Life Research,27(4), 945–954. https://doi.org/10.1007/s11136-017-1781-4.
Chachamovich, J. R., Chachamovich, E., Zachia, S., Knauth, D., & Passos, E. P. (2007). What variables predict generic and health-related quality of life in a sample of Brazilian women experiencing infertility? Human Reproduction,22(7), 1946–1952. https://doi.org/10.1093/humrep/dem080.
Karaca, N., Karabulut, A., Ozkan, S., Aktun, H., Orengul, F., Yilmaz, R., et al. (2016). Effect of IVF failure on quality of life and emotional status in infertile couples. European Journal of Obstetrics, Gynecology, and Reproductive Biology,206, 158–163. https://doi.org/10.1016/j.ejogrb.2016.09.017.
Kim, J. H., & Shin, H. S. (2013). A structural model for quality of life of infertile women. Journal of Korean Academy of Nursing,43(3), 312–320. https://doi.org/10.4040/jkan.2013.43.3.312.
Qu, F., Wu, Y., Zhu, Y. H., Barry, J., Ding, T., Baio, G., et al. (2017). The association between psychological stress and miscarriage: A systematic review and meta-analysis. Scientific Reports,7(1), 1731. https://doi.org/10.1038/s41598-017-01792-3.
Li, W., Newell-Price, J., Jones, G. L., Ledger, W. L., & Li, T. C. (2012). Relationship between psychological stress and recurrent miscarriage. Reproductive Biomedicine Online,25(2), 180–189. https://doi.org/10.1016/j.rbmo.2012.03.012.
Galhardo, A., Cunha, M., & Pinto-Gouveia, J. (2019). A 7-year follow-up study of the Mindfulness-Based Program for Infertility: Are there long-term effects? Clinical Psychology & Psychotherapy. https://doi.org/10.1002/cpp.2362.
Branstrom, R., Duncan, L. G., & Moskowitz, J. T. (2011). The association between dispositional mindfulness, psychological well-being, and perceived health in a Swedish population-based sample. The British Journal of Health Psychology,16(Pt 2), 300–316. https://doi.org/10.1348/135910710x501683.
Schell, L. K., Monsef, I., Wockel, A., & Skoetz, N. (2019). Mindfulness-based stress reduction for women diagnosed with breast cancer. Cochrane Database of Systematic Review. https://doi.org/10.1002/14651858.CD011518.pub2.
Acknowledgements
This work was supported by grants from the Shandong medical and health science and technology development plan (2017WS301). We are thankful for the generous contributions of the research participants and the staffs who assisted with data collection during the study.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. GL and ZJ analyzed and interpreted data and drafted the article; GL contributed to data interpretation and critical review; XH, ZJ and XS were responsible for the collection of data and literature review; WT and XK were in charge for literature review; FM was in charge for study design and essential help.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, G., Jiang, Z., Han, X. et al. A moderated mediation model of perceived stress, negative emotions and mindfulness on fertility quality of life in women with recurrent pregnancy loss. Qual Life Res 29, 1775–1787 (2020). https://doi.org/10.1007/s11136-020-02460-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-020-02460-2