ABSTRACT
Purpose
To study the effects of N-acetylcysteine (NAC, C5H9NO3S) on diet-induced obesity and obesity-related metabolic disorders.
Methods
Six-week-old male C57BL/6 mice fed a chow or high-fat diet (HFD) were treated with NAC (2 g/L) in drinking water for 11 weeks. Its influences on body weight and food intake were manually measured, and influence on body composition were analyzed by magnetic residence imaging. Glucose meter and ELISA were used to determine serum glucose and insulin levels, as well as lipid content in the liver. The effects of NAC treatment on mRNA levels of genes involved in inflammation, thermogenesis, and lipid metabolism in various tissues were determined by real time PCR.
Results
NAC supplementation inhibited the increase of fat mass and the development of obesity when mice were fed an HFD. NAC treatment significantly lowered HFD-induced macrophage infiltration, and enhanced adiponectin gene expression, resulting in reduced hyperglycemia and hyperinsulinemia, and improvement of insulin resistance. NAC oral administration suppressed hepatic lipid accumulation, as evidenced by lower levels of triglyceride and cholesterol in the liver. The beneficial effects are associated with a decrease of hepatic Pparγ and its target gene expression, and an increase in the expression of genes responsible for lipid oxidation and activation of farnesoid X receptor. Furthermore, NAC treatment also stimulates expression of thermogenic genes.
Conclusion
These results provide direct proof of the protective potential of NAC against HFD-induced obesity and obesity-associated metabolic disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
N-acetylcysteine (NAC, C5H9NO3S) is a thiol compound that stimulates glutathione-S-transferase activity and promotes detoxification by providing sulfhydryl groups and acting as a scavenger of free radicals through direct interaction with reactive oxygen species (1,2). It is a precursor of L-cysteine and reduced glutathione (GSH), and acts as an antioxidant by restoring the pool of intracellular reduced GSH. NAC has been commonly used to treat paracetamol (acetaminophen) intoxication and cystic fibrosis (3,4). The mucolytic agent of NAC has been used for several decades to treat chronic obstructive pulmonary disease.
In addition to its antioxidant and anti-inflammation properties, there is a growing interest in the beneficial effects of NAC for treating metabolic disorders. NAC is capable of protecting pancreatic β cells and preserving insulin levels by enhancing pancreatic-duodenal homeobox-1 (PDX-1) expression, a major regulator of beta cell identity and function (5,6). NAC supplementation suppresses fructose and high sucrose diet-induced hyperglycemia and hyperinsulinemia, and improves peripheral insulin sensitivity (7–9). The beneficial effects of NAC on glucose metabolism were also reported in alloxan-induced diabetes in CD-1 mice and diabetic db/db mice (10,11). Administered in drinking water, NAC lowered plasma and liver triglyceride levels in Balb/c mice fed a saturated fat-enriched diet and significantly affected lipid metabolism (12). Yang et al. (13) reported that NAC administration partially reduces plasma triglycerides, total cholesterol, and LDL levels while increasing the HDL level in rats fed a high fat diet (HFD) for 4 weeks. Similar results were obtained in mice subjected to a high cholesterol diet and supplemented with NAC and sesame oil (14). Short-term NAC administration in drinking water prevented high-sucrose induced weight gain and dyslipidemia (15). Collectively, these studies show that NAC is capable of restoring dys-regulated glucose and lipid metabolism, suggesting its potential application in diet-induced obesity, which is closely associated with oxidative stress, inflammation, and metabolic disturbance (16).
By employing HFD-induced obesity as a model, we systemically examined the beneficial effects of NAC administration on preventing HFD-induced obesity and obesity-associated metabolic disorders including hypertrophy of adipocytes, fatty liver, and insulin resistance. Mechanistically, the beneficial effects observed are accompanied by suppression of HFD-induced inflammation, modulation of nuclear receptor-mediated lipid metabolism, and regulation of thermogenic gene expression. Our results provide new and critical evidence in support of the application of NAC in the management of metabolic disorders.
MATERIALS AND METHODS
Materials
N-acetylcysteine (NAC, C5H9NO3S) was purchased from Sigma (St. Louis, MO). RNeasy Tissue kit was from Qiagen (Valencia, CA). First-strand cDNA synthesis system was obtained from OriGene (Rockville, MD). PerfeCTa® SYBR® Green FastMix was acquired from Quanta BioSciences (Gaithersburg, MD). Mercodia Insulin ELISA kit was from Mercodia Developing Diagnostics (Winston Salem, NC). A TUREtrack glucose meter was purchased from Nipro Diagnostics Inc. (Fort Lauderdale, FL). Oil Red O solution was obtained from Electron Microscopy Science (Hatfield, PA). Cholesterol and triglyceride commercial kits were purchased from Thermo Fisher Scientific Inc. (Waltham, MA). High-fat diet (60% kJ/fat) was purchased from Bio-serv (Frenchtown, NJ, catalog number S3282). C57BL/6 mice were purchased from the Charles River Laboratories (Wilmington, MA).
Animals and Treatment
All procedures performed on mice were approved by the Institutional Animal Care and Use Committee at the University of Georgia, Athens, Georgia. Six-week-old male C57BL/6 mice were housed under standard conditions with a 12 h light–dark cycle in 4 groups (Chow, Chow-NAC, HFD, HFD-NAC, 5 mice/per group). Mice fed an HFD or a regular chow had free access to the drinking water with/without NAC (2 g/L) for 11 weeks. Food consumption was determined by measuring the difference between the amount of food provided to each cage and the amount left at the end of the week throughout the experiment. Food intake per mouse was calculated based on the amount of food consumed divided by time and the number of mice per cage. Animals were weighed weekly and their body composition was determined using EchoMRI-100TM from Echo Medical Systems (Houston, TX).
Glucose Tolerance Test (GTT) and Insulin Tolerance Test (ITT)
Glucose and insulin tolerance tests were performed during weeks 10–11. For GTT, mice were injected intraperitoneally with glucose at 1.5 g/kg body weight after 6 h fasting. Blood samples were taken at designated time points (0, 30, 60, 90, 120 min), and the glucose concentrations were measured using a glucometer. For ITT, mice fasted for 4 h and blood glucose levels were measured after an intraperitoneal injection of insulin (Humulin, from Eli Lilly) at 0.75 U/kg. Blood samples were collected from fasted mice and insulin level was measured using commercial assay kits according to the manufacturer’s instruction. The same groups of animals were used for GTT and ITT with a time interval of 1 week.
Histochemical and Oil Red O Analysis
Mouse liver, epididymal, and subcutaneous white adipose as well as brown adipose tissues were collected at the end of the study, fixed in 10% formalin, and embedded in paraffin. H&E staining was performed with tissue sections at a thickness of 6 μm. Frozen hepatic sections (9 μm) were used for Oil Red O staining. Microscopic examination was performed and photographs were taken under a regular light microscope.
Hepatic Lipid Analysis
Hepatic lipid analysis was performed following the established procedure (17,18). Briefly, liver samples (100–200 mg) were freshly collected and homogenized in phosphate buffered saline (1 ml), mixed with 5 ml of an organic solvent (chloroform: methanol = 2:1, vol/vol) and incubated overnight at 4°C. The mixture was centrifuged and the organic phase collected. The collected fraction was dried and lipids were re-dissolved in 1% Triton X-100. The amounts of cholesterol and triglyceride were determined using a commercial kit following the manufacturers’ instructions.
Gene Expression Analysis by Real Time PCR (RT-PCR)
Total RNA was isolated from the mouse liver, and white and brown adipose tissues using RNeasy kit or TRIZOL reagent. Two μg of total RNA were used for the first strand cDNA synthesis as recommended by the manufacturer. RT-PCR was performed using SYBR Green as an indicator on the ABI StepOne Plus Real-Time PCR system according to the recommend protocol. The PCR was carried out for 40 cycles at 95°C for 15 s and 60°C for 1 min. Fluorescence was read during the reaction, allowing a continuous monitoring of the amount of PCR product. The data were normalized to internal control Gapdh mRNA and analyzed using the ΔΔCt method. The primer sequences employed are summarized in Supplemental Table S1.
Statistical Analysis
Statistical analysis was done by two-way ANOVA. All data are reported as mean ± standard deviation (SD) with statistical significance set at P < 0.05.
RESULTS
NAC Administration Suppresses HFD-Induced Gain of Body Weight and Fat Mass
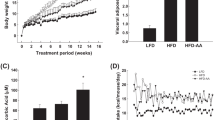
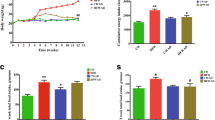
To evaluate the effect of NAC provided in drinking water on HFD-induced weight gain, we fed C57BL/6 mice chow or an HFD (60% kJ/fat), simultaneously providing drinking water with/without 2 g/L NAC for a total of 11 weeks. As expected, mice on an HFD rapidly gained weight, reaching 48 g at the end of 11 weeks compared to 30 g for animals fed regular chow (Fig. 1a). However, access to NAC containing water did not affect the growth rate of mice on regular chow, whereas the NAC treatment dramatically inhibited HFD-induced weight gain, exhibiting 15 g less than that of obese mice and a weight close to that of the control mice with a regular chow at the end of 11 weeks. The difference in body weight is recognized by animal appearance (Fig. 1b).
NAC treatment protects mice from HFD-induced obesity. Eight-week-old C57BL/6 male mice were fed a chow or HFD with free access to drinking water with or without 2 g/L NAC for 11 weeks. (a) Time and body weight curve; (b) Photographs of control and treated mice at the end of experiment; (c) Fat mass and lean mass of different groups of animals at the end of 11-week feeding; (d) Average calories intake per mouse of different groups was calculated based on daily food (food-energy conversion: HFD, 1 g = 5.49 kcal; regular diet, 1 g = 3.46 kcal). Each data point represents the average ± SD of 5 animals. #P < 0.05, ##P < 0.01 compared to chow fed animals; *P < 0.05, **P < 0.01 compared to HFD fed animals.
Body composition analysis revealed that the NAC treatment largely suppressed the gain of fat mass, with an approximately 55% reduction in fat mass compared to that of control animals, irrespective of mice with regular chow or HFD feeding (Fig. 1c). Moreover, difference in body weight is not correlated with calorie intake (Fig. 1d). Body fat reduction was further determined by weighing fat pads. The results in Fig. 2a show that the NAC treatment significantly blocked the increase of fat pads, including epididymal (EWAT) and subcutaneous (SubWAT) adipose tissues in HFD-fed mice by ~1.1 g and ~1.4 g, respectively. Accordingly, H&E staining of adipocytes demonstrate that NAC reduced the size of adipocytes in EWAT and SubWAT in mice fed an HFD; this was further confirmed by quantitative analysis using an imaging system (Fig. 2b-d). These results demonstrate that administration of NAC through drinking water blocks lipid accumulation in adipose tissue.
NAC treatment reduces fat mass and average size of adipocytes. Mice were sacrificed at the end of 11-week treatment and the epididymal and subcutaneous adipose pads were collected. Adipose tissues were fixed in 10% neutrally buffered formalin and H&E staining was performed to show the morphology of adipose tissues. (a) Weight of epididymal (EWAT) and subcutaneous (SubWAT) adipose tissues; (b) Average size of adipocytes calculated from 200 adipocytes from 5 separate slides; (c) and (d) Representative images of H&E staining of EWAT and SubWAT (100×). #P < 0.05, ##P < 0.01 compared to chow fed animals; *P < 0.05, **P < 0.01 compared to HFD fed animals (n = 5).
Supplementation of NAC in Drinking Water Inhibits HFD-induced Chronic Inflammation in Adipose Tissue
Macrophage infiltration in WAT is a major characteristic in HFD-induced obesity (19). We therefore performed real-time PCR analysis to determine the levels of adipose macrophages and inflammation. Results in Fig. 3a-c show that HFD-induced macrophage infiltration, as evidenced by increased mRNA levels of macrophage specific marker genes Cd68, F4/80, and Cd11c, by ~ 33.2-, 22.3-, and 40.6-fold, respectively, over that of control animals fed regular chow. HFD also enhanced the Mcp1 gene expression (Fig. 3d), which encodes the macrophage chemotactic factor. In contrast, induced expression of these genes is markedly suppressed by NAC treatment, suggesting the anti-inflammation effect of NAC on diet-induced obesity. In addition, NAC also inhibited HFD-induced expression of gp91 (phox), a subunit of NADPH oxidase involving in oxidative stress (Fig. 3e). Adiponectin mRNA level was significantly lower in HFD fed obese mice, whereas NAC evidently promoted adiponectin gene expression (Fig. 3f). To extend the investigation of the inhibitory role of NAC on inflammation, we exposed in vitro the RAW264.7 macrophage cell line to LPS in the presence of different amounts of NAC. As predicted, LPS dramatically induced expression of inflammatory factor genes including iNos, Cox2, Mcp1, and Tnfα, whereas NAC markedly inhibited LPS-induced gene expression in a dose-dependent manner (Supplemental Fig. 1). These data show that NAC is capable of suppressing macrophage activation and macrophage-mediated inflammation.
NAC treatment inhibits inflammation and oxidative stress, and enhances adiponectin gene expression in EWAT. Total RNA was extracted from EWAT and relative mRNA levels of selected genes were determined by RT-PCR. Inflammation is monitored by the mRNA levels of marker genes of macrophages: (a) Cd68; (b) F4/80; (c) Cd11c; (d) chemotactic factor gene Mcp1; (e) Oxidative gene marker of NADPH oxidase subunit, gp91 (phox); and (f) Adiponectin gene. Each data point represents the mean ± SD, (n = 5). #P < 0.05, ##P < 0.01 compared to chow animals; *P < 0.05, **P < 0.01 compared to HFD fed animals (n = 4).
NAC Treatment Improved Obesity-associated Insulin Resistance
Adiposity and chronic inflammation are the major contributors to obesity-associated insulin resistance. To determine whether NAC treatment improves insulin sensitivity, we fasted mice for 6 h and performed intraperitoneal glucose tolerance tests. The results in Fig. 4a show that HFD feeding induced higher fasting glucose levels compared to that of animals fed a regular chow, and exhibited a much slower clearance rate of injected glucose. NCA-treated mice exhibited a much higher clearance rate, which was better represented using the calculated area under the curve (AUC, Fig. 4b). NAC-treated mice also showed a rapid response to insulin administration (Fig. 4c). Accordingly, obesity-associated hyperinsulinemia was strikingly ameliorated by NAC treatment (8.3 μg/l vs. 1.1 μg/l) (Fig. 4d). It is noteworthy that NAC treatment also enhanced insulin sensitivity in chow-fed mice (Fig. 4a-c). These results validate our prediction that NAC protects animals against obesity-associated insulin resistance.
NAC treatment improves hyperinsulinemia and hyperglycemia of animals fed an HFD. (a) Glucose tolerance test. Animals were fasted for 6 h and injected (i.p.) with glucose (1.5 g/kg) and blood glucose levels were determined. (b) Area under the curve from (a). (c) Insulin tolerance test. Animals were fasted for 4 h followed by injection (i.p.) of insulin (0.75U/kg) and blood glucose levels were determined. (d) Serum insulin levels at the end of the 11-week feeding with or without NAC treatment. Each data point represents the mean ± SD (n = 5). *P < 0.05, **P < 0.01 compared to HFD-fed animals.
NAC Administration Blocks Lipid Accumulation in the Liver by Modulating Nuclear Receptor-mediated Lipid Metabolism
Consumption of an HFD leads to fatty liver disease. Results in Fig. 5a show that liver weight in HFD-fed mice was 1.7-fold higher than that of animals fed a chow food. NAC treatment reduced liver weight in mice fed either a chow or an HFD. H&E-stained liver sections showed normal liver structure of mice on chow with or without NAC treatment. However, there was extensive hepatocyte vacuolation in animals fed an HFD (Fig. 5c), reflecting intrahepatic fat accumulation. In contrast, NAC treatment efficiently blocked lipid accumulation in hepatocytes, which was evidenced by Oil Red O staining of liver sections (Fig. 5d). Blockage of hepatic lipid accumulation by NAC was further confirmed by measurements of hepatic triglyceride and cholesterol levels (Fig. 5b). Taken together, these results demonstrate that NAC treatment is capable of blocking hepatic lipid accumulation.
NAC treatment inhibits lipid accumulation in the liver. At the end of the 11-week feeding, mice were sacrificed and liver samples were collected. (a) Liver weight of animals with or without NAC treatment; (b) Hepatic total triglyceride and cholesterol levels; (c) Photographs of liver sections with H&E staining (200×); (d) Lipid distribution in the liver revealed by Oil Red O staining (200×). #P < 0.05, ##P < 0.01 compared to chow fed animals; *P < 0.05, **P < 0.01 compared to HFD fed animals (n = 5).
To further understand how NAC treatment affects hepatic lipid metabolism, we performed RT-PCR to evaluate the effect of NAC treatment on mRNA levels of genes responsible for lipid homeostasis. The PPARγ-mediated pathway is responsible for lipid storage (20). As shown in Fig. 6a-d, HFD significantly enhanced mRNA levels of hepatic Pparγ1 and Pparγ2 by 2.7- and 4.8-fold, respectively, compared to that of chow-fed animals. In contrast, NAC treatment significantly inhibited Pparγ expression, suppressing the induction of its target genes, including Cd36 (84%) and monoacylglycerol O-acyltransferase 1 (Mgat1, 98%). Moreover, NAC treatment also reduced Cyp7a1 gene expression but enhanced Shp expression. Both Cyp7a1 and Shp are target genes of the farnesoid X receptor (FXR). NAC treatment also increased mRNA levels of genes involved in fatty acid metabolism including carnitine palmitoyltransferase I (Cpt1a, Cpt1b).
Effect of NAC treatment on expression of genes involved in regulation of hepatic lipid storage and metabolism. Mice were sacrificed at the end of NAC treatment and liver samples were harvested, and total RNA was extracted. RT- PCR analysis was performed to evaluate relative mRNA levels of selected genes. (a) Pparγ1; (b) Pparγ2 and its target genes; (c) Cd36; (d) Mgat1; (e) Cyp7a1; (f) Shp; (g) Cpt1a; and (h) Cpt1b. Each data point represents the mean ± SD, (n = 4). #P < 0.05, ##P < 0.01compared to chow fed animals; *P < 0.05, **P < 0.01 compared to HFD fed animals.
NAC Treatment Increases Expression of the Genes Involved in Energy Expenditure in HFD-fed Mice
H&E-stained brown adipose tissue (BAT) show that HFD feeding increased fat deposition in brown adipocytes, resulting in BAT whitening. NAC treatment, however, dramatically inhibited adipocyte expansion in both chow- and HFD-fed mice (Fig. 7a). Since BAT plays an important role in thermogenesis, we examined the changes of thermogenic gene expression in BAT to assess the potential effect of NAC treatment on BAT activity. NAC treatment significantly enhanced the transcriptional levels of the genes that are critical for cellular thermogenesis, including Dio2, Pgc-1α, Pgc-1β, Cidea, and Ucp3. (Fig. 7b), suggesting that NAC treatment influences energy expenditure in BAT.
Effect of NAC treatment on thermogenesis. Animals were sacrificed at the end of 11-week treatment and BAT was collected and total RNA extracted. (a) Photographs of BAT section with H&E staining (200×); Relative mRNA levels of (b) Ucp1; (c) Ucp3; (d) Pgc1α, and (e) Dio2. Each data point represents the mean ± SD, (n = 4). #P < 0.05, ##P < 0.01 compared to chow fed animals; *P < 0.05, **P < 0.01 compared to HFD fed animals.
DISCUSSION
In this study we demonstrate that NAC supplementation greatly inhibited HFD-induced gain of body weight and fat mass (Figs. 1 and 2). NAC treatment significantly curbed HFD-induced macrophage infiltration and enhanced the adiponectin gene expression, resulting in improvement of hyperglycemia, hyperinsulinemia, and insulin resistance (Figs. 3 and 4). NAC treatment almost entirely blocked lipid accumulation in the liver, which was evidenced by lower levels of triglyceride and cholesterol in the liver (Fig. 5). The beneficial effects are associated with expression suppression of hepatic Pparγ and its target genes, and an increase in mRNA levels of genes responsible for lipid oxidation and FXR activation (Fig. 6). Furthermore, NAC treatment stimulates thermogenic gene expression (Fig. 7). These results provide direct evidence to support the use of NAC supplementation as an effective means of blocking HFD-induced metabolic disorders.
Previous studies have shown that HFD feeding elevates production of reactive oxygen species in adipose tissue and boosts macrophage infiltration and inflammation (19,21,22), while chronic inflammation is closely associated with metabolic disorders (23). We have shown that macrophage elimination by clodronate liposomes (24) or overexpression of superoxide dismutase 3 gene (25) is capable of maintaining redox homeostasis and blocking HFD-induced obesity. Herein, consistent with its antioxidant and anti-inflammation properties, NAC treatment notably inhibited HFD-induced oxidative stress and chronic inflammation in adipose tissue, which was evidenced by suppression of NADPH oxidase subunit Gp91 phox, macrophage chemokine Mcp1, and macrophage marker gene expression. In addition, we demonstrate that NAC treatment significantly reduced LPS-induced expression of inflammatory factor genes, including iNos, Cox2, Tnfα in RAW264.7 macrophage cells in vitro. In line with our results, Calzadilla et al. also demonstrated that NAC inhibited ROS levels and reduced adipocyte differentiation by inhibition of C/EBPβ and Pparγ gene expression and fat accumulation using 3 T3-L1 pre-adipocytes (26). Mechanically, NAC suppressed the proteasome activity (27) of NFκB kinases (28), thereby inhibiting activation of NF-κB, a master regulator for inflammation.
The beneficial effects of NAC in modulating glucose homeostasis are primarily achieved by its activity in suppressing inflammation. Growing evidence demonstrates that HFD-induced lipid overload in adipose tissue, liver, and muscle leads to an increased stress response, stimulating recruitment of immune cells and activation of inflammatory pathways. Consequently, chronic inflammation blunts insulin action in stressed tissues by inhibiting insulin signal transduction and causing cellular insulin resistance (29,30). NAC directly or indirectly removes diet-induced ROS production, alleviating the inflammatory reaction, thus resulting in improved insulin sensitivity. In addition, our data also shows that NAC elevates adiponectin expression. Adiponection is an adipocytokine secreted from adipocytes (31). Previous studies show that adiponectin expression and its plasma concentration were inversely related to the development of obesity (32). Adiponectin-deficient mice developed diet-induced glucose intolerance and insulin resistance (33,34). In contrast, overexpression of adiponectin in mice leads to improved insulin sensitivity and glucose tolerance (35). These studies demonstrate the important role of adiponectin in maintaining glucose homeostasis. In line with these reports, results in Fig. 3f show a significant reduction of adiponectin expression in obese mice, concordant with insulin resistance in these mice. NAC treatment elevated adiponectin gene expression, suggesting its contribution to the improved insulin sensitivity.
Results in Fig. 5 show that NAC treatment inhibited diet-induced lipid accumulation in the liver, evidenced by H&E and Oil Red O staining of liver sections. The effect is in part related to the suppression of hepatic PPARγ-mediated fat storage. HFD stimulated both Pparγ1 and Pparγ2 gene expression in the liver, concordant with HFD-induced hepatic lipid accumulation (Fig. 6a-b). Blockage of HFD-induced expression of Pparγ and its target genes reduces lipid storage. Moreover, NAC treatment also reduced Cyp7a1 gene expression but increased Shp transcript level. Both are the target genes of FXR, indicating that the potential effect of NAC is related to activation of the nuclear receptor FXR, which is an endogenous sensor for bile acids, and plays an important role in cholesterol and lipid metabolism. Our previous study demonstrated that activation of FXR by GW4064 significantly curbed HFD-induced hepatic steatosis by markedly reducing expression of lipid transporter Cd36 gene (17). Therefore, induction of expression of FXR target genes facilitates the suppression of hepatic steatosis. In addition, previous studies also show that oxidative stress can lead to triglyceride accumulation in hepatocytes through up-regulation of lipogenic transcription factors and enzymes involved in fatty acid synthesis (36). Therefore, effective prevention of diet-induced hepatic oxidative stress by NAC may also reduce de novo lipid synthesis.
Furthermore, we observed that NAC treatment markedly inhibited lipid accumulation in BAT, even in chow-fed mice, according to the average size and the density of vacuole type structures in the H&E-stained BAT sections. BAT is known for its role in thermogenesis (37). Bartelt et al. (38) reported that increased BAT activity enhanced triglyceride-rich lipoprotein metabolism in mice, suggesting its beneficial role in mobilizing lipids utilization. Our real-time PCR analysis shows NAC treatment enhanced thermogenic gene expression, including Ucp3, Pgc1α, and Dio2, suggesting that NAC treatment may enhance energy expenditure. Concordant with our results, Novelli et al. (15) showed that NAC is able to inhibit carbohydrate oxidation and enhance fat oxidation in rats fed a high-sucrose diet, boosting whole body energy expenditure.
Taken together, our current study demonstrates that supplement of NAC in drinking water is capable of suppressing inflammation, modulating glucose and lipid metabolism, and stimulating thermogenic gene expression in HFD-fed mice, consequently preventing mice from diet-induced obesity and obesity-associated liver steatosis and insulin resistance. These results provide direct evidence to support that NAC supplementation can be considered as an effective means in blocking diet-induced obesity and associated complications.
Abbreviations
- ANOVA:
-
Analysis of variance
- BAT:
-
Brown adipose tissue
- CD68:
-
Cluster of differentiation 68
- Cox2:
-
Cyclooxygenase 2
- Cpt1:
-
Carnitine palmitoyltransferase 1
- Cyp7a1:
-
Cholesterol 7 alpha-hydroxylase
- Dio2:
-
Type II iodothyronine deiodinase
- FXR:
-
Farnesoid X receptor
- Gapdh:
-
Glyceraldehyde-3-Phosphate Dehydrogenase
- GTT:
-
Glucose tolerance test
- H&E:
-
Haematoxylin and eosin stain
- HDL:
-
High-density lipoprotein
- HFD:
-
High fat diet
- Inos:
-
Inducible nitric oxide synthase
- ITT:
-
Insulin tolerance test
- LDL:
-
Low-density lipoprotein
- LPS:
-
Lipopolysaccharide
- Mcp1:
-
Monocyte chemotactic protein 1
- Mgat1:
-
Monoacylglycerol O-acyltransferase 1
- NADPH:
-
Nicotinamide adenine dinucleotide phosphate
- Pgc1α:
-
Peroxisome proliferator-activated receptor gamma coactivator 1-alpha
- Ppar:
-
Peroxisome proliferator-activated receptor
- RT-PCR:
-
Real time PCR
- SD:
-
Standard deviation
- Shp:
-
Small heterodimer partner
- Tnfα:
-
Tumor necrosis factor alpha
- Ucp:
-
Uncoupling Protein
- WAT:
-
White adipose tissue
REFERENCES
Millea PJ. N-acetylcysteine: multiple clinical applications. Am Fam Physician. 2009;80(3):265–9.
Kelly GS. Clinical applications of N-acetylcysteine. Altern Med Rev. 1998;3(2):114–27.
Atkuri KR, Mantovani JJ, Herzenberg LA, Herzenberg LA. N-Acetylcysteine--a safe antidote for cysteine/glutathione deficiency. Curr Opin Pharmacol. 2007;7(4):355–9.
Tirouvanziam R, Conrad CK, Bottiglieri T, Herzenberg LA, Moss RB, Herzenberg LA. High-dose oral N-acetylcysteine, a glutathione prodrug, modulates inflammation in cystic fibrosis. Proc Natl Acad Sci U S A. 2006;103(12):4628–33.
Tanaka Y, Gleason CE, Tran PO, Harmon JS, Robertson RP. Prevention of glucose toxicity in HIT-T15 cells and Zucker diabetic fatty rats by antioxidants. Proc Natl Acad Sci U S A. 1999;96(19):10857–62.
McKinnon CM, Docherty K. Pancreatic duodenal homeobox-1, PDX-1, a major regulator of beta cell identity and function. Diabetologia. 2001;44(10):1203–14.
Song D, Hutchings S, Pang CC. Chronic N-acetylcysteine prevents fructose-induced insulin resistance and hypertension in rats. Eur J Pharmacol. 2005;508(1–3):205–10.
Diniz YS, Rocha KK, Souza GA, Galhardi CM, Ebaid GM, Rodrigues HG. Effects of N-acetylcysteine on sucrose-rich diet-induced hyperglycaemia, dyslipidemia and oxidative stress in rats. Eur J Pharmacol. 2006;543(1–3):151–7.
Blouet C, Mariotti F, Azzout-Marniche D, Mathe V, Mikogami T, Tome D, et al. Dietary cysteine alleviates sucrose-induced oxidative stress and insulin resistance. Free Radic Biol Med. 2007;42(7):1089–97.
Ho E, Chen G, Bray TM. Supplementation of N-acetylcysteine inhibits NFkappaB activation and protects against alloxan-induced diabetes in CD-1 mice. FASEB J. 1999;13(13):1845–54.
Kaneto H, Kajimoto Y, Miyagawa J, Matsuoka T, Fujitani Y, Umayahara Y, et al. Beneficial effects of antioxidants in diabetes: possible protection of pancreatic beta-cells against glucose toxicity. Diabetes. 1999;48(12):2398–406.
Lin CC, Yin MC, Hsu CC, Lin MP. Effect of five cysteine-containing compounds on three lipogenic enzymes in Balb/cA mice consuming a high saturated fat diet. Lipids. 2004;39(9):843–8.
Yang R, Le G, Li A, Zheng J, Shi Y. Effect of antioxidant capacity on blood lipid metabolism and lipoprotein lipase activity of rats fed a high-fat diet. Nutrition. 2006;22(11–12):1185–91.
Korou LM, Agrogiannis G, Pantopoulou A, Vlachos IS, Iliopoulos D, Karatzas T, et al. Comparative antilipidemic effect of N-acetylcysteine and sesame oil administration in diet-induced hypercholesterolemic mice. Lipids Health Dis. 2010;9:23.
Novelli EL, Santos PP, Assalin HB, Souza G, Rocha K, Ebaid GX, et al. N-acetylcysteine in high-sucrose diet-induced obesity: energy expenditure and metabolic shifting for cardiac health. Pharm Res. 2009;59(1):74–9.
Fernandez-Sanchez A, Madrigal-Santillan E, Bautista M, Esquivel-Soto J, Morales-Gonzalez A, Esquivel-Chirino C, et al. Inflammation, oxidative stress, and obesity. Int J Mol Sci. 2011;12(5):3117–32.
Ma Y, Huang Y, Yan L, Gao M, Liu D. Synthetic FXR agonist GW4064 prevents diet-induced hepatic steatosis and insulin resistance. Pharm Res. 2013;30(5):1447–57.
Ma Y, Gao M, Liu D. Chlorogenic acid improves high Fat diet-induced hepatic steatosis and insulin resistance in mice. Pharm Res. 2015;32(4):1200–9.
Weisberg SP, McCann D, Desai M, Rosenbaum M, Leibel RL, Ferrante Jr AW. Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest. 2003;112(12):1796–808.
Gavrilova O, Haluzik M, Matsusue K, Cutson JJ, Johnson L, Dietz KR, et al. Liver peroxisome proliferator-activated receptor gamma contributes to hepatic steatosis, triglyceride clearance, and regulation of body fat mass. J Biol Chem. 2003;278(36):34268–76.
Furukawa S, Fujita T, Shimabukuro M, Iwaki M, Yamada Y, Nakajima Y, et al. Increased oxidative stress in obesity and its impact on metabolic syndrome. J Clin Invest. 2004;114(12):1752–61.
Oliver E, McGillicuddy F, Phillips C, Toomey S, Roche HM. The role of inflammation and macrophage accumulation in the development of obesity-induced type 2 diabetes mellitus and the possible therapeutic effects of long-chain n-3 PUFA. Proc Nutr Soc. 2010;69(2):232–43.
Wellen KE, Hotamisligil GS. Obesity-induced inflammatory changes in adipose tissue. J Clin Invest. 2003;112(12):1785–8.
Bu L, Gao M, Qu S, Liu D. Intraperitoneal injection of clodronate liposomes eliminates visceral adipose macrophages and blocks high-fat diet-induced weight gain and development of insulin resistance. AAPS J. 2013;15(4):1001–11.
Cui R, Gao M, Qu S, Liu D. Overexpression of superoxide dismutase 3 gene blocks high-fat diet-induced obesity, fatty liver and insulin resistance. Gene Ther. 2014;21(9):840–8.
Calzadilla P, Sapochnik D, Cosentino S, Diz V, Dicelio L, Calvo JC, et al. N-acetylcysteine reduces markers of differentiation in 3 T3-L1 adipocytes. Int J Mol Sci. 2011;12(10):6936–51.
Pajonk F, Riess K, Sommer A, McBride WH. N-acetyl-L-cysteine inhibits 26S proteasome function: implications for effects on NF-kappaB activation. Free Radic Biol Med. 2002;32(6):536–43.
Oka S, Kamata H, Kamata K, Yagisawa H, Hirata H. N-acetylcysteine suppresses TNF-induced NF-kappaB activation through inhibition of IkappaB kinases. FEBS Lett. 2000;472(2–3):196–202.
Glass CK, Olefsky JM. Inflammation and lipid signaling in the etiology of insulin resistance. Cell Metab. 2012;15(5):635–45.
Lee BC, Lee J. Cellular and molecular players in adipose tissue inflammation in the development of obesity-induced insulin resistance. Biochim Biophys Acta. 2014;1842(3):446–62.
Scherer PE, Williams S, Fogliano M, Baldini G, Lodish HF. A novel serum protein similar to C1q, produced exclusively in adipocytes. J Biol Chem. 1995;270(45):26746–9.
Diez JJ, Iglesias P. The role of the novel adipocyte-derived hormone adiponectin in human disease. Eur J Endocrinol. 2003;148(3):293–300.
Kubota N, Terauchi Y, Yamauchi T, Kubota T, Moroi M, Matsui J, et al. Disruption of adiponectin causes insulin resistance and neointimal formation. J Biol Chem. 2002;277(29):25863–6.
Maeda N, Shimomura I, Kishida K, Nishizawa H, Matsuda M, Nagaretani H, et al. Diet-induced insulin resistance in mice lacking adiponectin/ACRP30. Nat Med. 2002;8(7):731–7.
Ma Y, Liu D. Hydrodynamic delivery of adiponectin and adiponectin receptor 2 gene blocks high-fat diet-induced obesity and insulin resistance. Gene Ther. 2013;20(8):846–52.
Sekiya M, Hiraishi A, Touyama M, Sakamoto K. Oxidative stress induced lipid accumulation via SREBP1c activation in HepG2 cells. Biochem Biophys Res Commun. 2008;375(4):602–7.
Cannon B, Nedergaard J. Brown adipose tissue: function and physiological significance. Physiol Rev. 2004;84(1):277–359.
Bartelt A, Bruns OT, Reimer R, Hohenberg H, Ittrich H, Peldschus K, et al. Brown adipose tissue activity controls triglyceride clearance. Nat Med. 2011;17(2):200–5.
Acknowledgments and Disclosures
We thank Mrs. Francisca Burnley for proofreading and English editing. This work was supported in part by the National Institute of Health [RO1 HL098295].
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 23 kb)
Fig. S1
NAC treatment represses LPS-induced expression of inflammation response genes in macrophages. RAW264.7 cells were treated with LPS (100 ng/ml) in the presence of various doses of NAC for 24 h. Cells were harvested and total RNA was extracted for RT-PCR analysis. Relative mRNA levels of (a) Inos; (b) Cox2; (c) Mcp1; and (d) Tnfα. **P < 0.01 compared to LPS treatment without NAC (n = 3). (GIF 50 kb)
Rights and permissions
About this article
Cite this article
Ma, Y., Gao, M. & Liu, D. N-acetylcysteine Protects Mice from High Fat Diet-induced Metabolic Disorders. Pharm Res 33, 2033–2042 (2016). https://doi.org/10.1007/s11095-016-1941-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-016-1941-1