Abstract
Anesthetics such as propofol can provide neuroprotective effects against cerebral ischemia. However, the underlying mechanism of this beneficial effect is not clear. Therefore, we subjected male Sprague–Dawley rats to 2 h of middle cerebral artery occlusion and investigated how post-ischemic administration of propofol affected neurologic outcome and the expression of basic fibroblast growth factor (bFGF). After 2 h of ischemia, just before reperfusion, the animals were randomly assigned to receive either propofol (20 mg kg−1 h−1) or vehicle (10 % intralipid, 2 ml kg−1 h−1) intravenously for 4 h. Neurologic scores, infarct volume, and brain water content were measured at different time points after reperfusion. mRNA level of bFGF was measured by real-time PCR, and the protein expression level of bFGF was analyzed by immunohistochemistry and Western blot. At 6, 24, 72 h, and 7 days of reperfusion, infarct volume was significantly reduced in the propofol-treated group compared to that in the vehicle-treated group (all P < 0.05). Propofol post-treatment also attenuated brain water content at 24 and 72 h and reduced neurologic deficit score at 72 h and 7 days of reperfusion (all P < 0.05). Additionally, in the peri-infarct area, bFGF mRNA and protein expression were elevated at 6, 24, and 72 h of reperfusion compared to that in the vehicle-treated group (all P < 0.05). These results show that post-ischemic administration of propofol provides neural protection from cerebral ischemia–reperfusion injury. This protection may be related to an early increase in the expression of bFGF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
As the population ages, patients with a history of stroke will increasingly require surgery or sedation. It is important to be able to provide safe anesthesia with neuroprotective potential in such cases. Many intravenous anesthetics and sedatives, including propofol, benzodiapepines and barbiturates, have shown to provide neuroprotective effects in animal models of cerebral ischemia [1–4]. In particular, propofol post-conditioning has been reported to provide protection against hypoxic injury and paraquat toxicity under in vitro and in vivo conditions [5, 6]. Studies have indicated that neuroprotective effects of such anesthetics may stem from their ability to suppress cerebral metabolic rate, antagonize glutamate-mediated excitotoxicity, and enhance inhibitory synaptic transmission [7–10]. However, the mechanism(s) by which intravenous anesthetics such as propofol provide neuroprotection is unclear.
Neurotrophic factors are known to have neuroprotective effects in cerebral ischemia. For example, basic fibroblast growth factor (bFGF) has been shown to promote survival and proliferation of neurons, suppress apoptosis, and ameliorate ischemic injury [11–13]. Propofol has been shown to enhance neurogenesis in a bilateral carotid artery occlusion model in rats [14]; however, its effect on growth factors is unknown. In the current study, we investigated whether administration of propofol to rats after transient focal cerebral ischemia provides neuroprotection and whether this protection is related to expression of bFGF.
Materials and Methods
Animal Preparation and Experimental Groups
The study was approved by the Animal Research Committee of China Medical University. Male Sprague–Dawley rats (Center for Experimental Animals, China Medical University; 270-300 g) were anesthetized with chloral hydrate (i.p., 350 mg kg−1). Chloral hydrate was chosen to be the anesthetic for the surgical procedure in this study because it provides prompt induction of anesthesia and its less effect on the cardiovascular and central nervous system than does isoflurane and other anesthetics [15, 16]. The animals were surgically prepared for middle cerebral artery occlusion (MCAO) according to the technique by Longa and colleagues [17]. Ropivacaine (Naropin, AstraZeneca) was infiltrated at the surgical site 10 min before the operation. The left common carotid artery was exposed via a midline pretracheal incision. The external carotid artery and the common carotid artery were ligated. Through a small arteriotomy, a 4-0 surgical nylon monofilament with a silicone-coated tip was inserted into the common carotid artery just below the carotid bifurcation and was advanced into the internal carotid artery to a distance of 18–20 mm from the carotid artery bifurcation until slight resistance was felt. The monofilament was removed from the common carotid artery at the end of the 2-h ischemic interval. Cerebral blood flow was monitored by laser-Doppler flow (LDF) on the ischemic side of the skull. Successful MCAO was defined as ≥80 % decrease in cerebral blood flow and was confirmed by laser-Doppler flowmetry. Rats in which the cerebral blood flow did not decrease by more than 80 % were excluded from the study. Sham-operated rats were subjected to the same surgical procedure except that the nylon monofilament was not inserted. Rectal temperature was maintained at 37 ± 0.5 °C with a heating lamp. Catheters were inserted into the right femoral artery and vein for blood pressure monitoring, analysis of blood gases including pH, hematocrit, PaO2, and PaCO2 and for intravenous infusion.
The rats (n = 311) were allocated into three groups: sham group (n = 8), 2 h MCAO without reperfusion group (n = 8), and 2 h MCAO with reperfusion group (n = 295). Rats subjected to 2 h MCAO and reperfusion were randomly assigned to receive propofol (Diprivan, AstraZeneca) (n = 147) or vehicle (n = 148), and these rats were then divided into four subgroups per group: 6-h reperfusion, 24-h reperfusion, 72-h reperfusion, and 7-day reperfusion (n = 56, 109, 74 and 56 respectively). Propofol (20 mg kg−1 h−1) or the same volume of vehicle (10 % intralipid) was administered intravenously for 4 h beginning at 2 h of ischemia, just before reperfusion. The dosing regimen was based on a previous study that used a rat focal ischemia model [18]. At intervals of 6 h, 24 h, 72 h, and 7 days after reperfusion, the rats underwent the following assessments.
Neurologic Function Assessment
Neurologic deficit scores were assessed by an investigator blinded to the animal grouping on days 1, 3, and 7 after ischemia. All rats were evaluated by the modified neurological severity score (mNSS) [19, 20]. Briefly, the mNSS is a composite of sensory, motor, reflex, and balance tests. Neurologic function was graded on a scale of 0–18. For the injury scores, 1 point was awarded for the inability to perform a test or for the lack of a tested reflex. Thus, higher scores indicate more severe injuries.
Infarct Volume Measurement
At 6 h, 24 h, 72 h, or 7 days after reperfusion, the rats were reanesthetized (chloral hydrate i.p., 350 mg kg−1) and decapitated. Their brains were removed, frozen at −20 °C and sectioned into six coronal slices (2-mm thick) that were immediately immersed in 2 % 2,3,5-triphenyltetrazolium chloride (TTC) (Sigma, St. Louis, MO)saline solution at 37 °C for 30 min before being transferred to 4 % paraformaldehyde for fixation. The fixed brain slices were photographed and quantified for ischemic damage with an image analysis system (Motic Images Advanced 3.2) by an investigator blinded to treatment group. The degree of brain damage was corrected for the contribution made by brain edema/swelling as described by Shimakura and colleagues [21]. The total infarct area was determined by summing the damaged area from six slices; it is presented as a percentage of the contralateral hemisphere.
Brain Water Content
Eight rats each from the propofol- and vehicle-treated groups were euthanized after the neurologic examination on days 1 and 3 post-ischemia. The brain water content in the ipsilateral and contralateral hemispheres was determined by the wet/dry weight ratio method as described previously [22, 23] and expressed as follows: (wet weight−dry weight)/wet weight of brain tissue × 100 %.
Real-Time PCR Assessment of bFGF mRNA Expression
Sham-operated rats and rats that underwent MCAO with or without reperfusion were euthanized for the measurement of bFGF mRNA expression. We extracted total RNA from fresh brain tissue collected from the peri-infarct area using RNeasy columns (Qiagen, Valencia, CA). RNA concentrations were measured spectrophotometrically in a Gen-Quant RNA/DNA calculator (Pharmacia Biotech, UK). One microgram of total RNA from the sample preparation was reverse transcribed with an Omniscriptase Reverse Transcriptase kit (Qiagen) and 5 μM random primers (Sigma, St. Louis, MO) according to the manufacturer’s instructions. The rat-specific primers for the genes of bFGF and glyceraldehyde 3-phosphate dehydrogenase (GAPDH) were designed by using Primer Premier 5 (Premier Biosoft, Palo Alto, CA, USA). The primer sequences for bFGF were (forward) 5′-TGGCTATGAAGGAAGATGG-3′ and (reverse) 3′-CGTTTCAGTGCCACATACC-5′. Real-time PCR was carried out on a 7500 Fast Real-Time PCR System (Applied Biosystems, Irvine, CA) with Power SYBR Green (Applied Biosystems). GAPDH was used as an endogenous control to normalize gene expression. In brief, the PCR mixtures were preheated at 50 °C for 2 min and then at 95 °C for 10 min to activate the AmpliTaq Gold DNA polymerase; then samples underwent 40 cycles of amplification (95 °C for 15 s; 60 °C for 30 s; 68 °C for 40 s). A final extension step was performed at 60 °C for 10 min. Each reaction was carried out in triplicate. Graphs were plotted, and analysis was performed with the ΔΔCt method.
Immunohistochemical Assessment of bFGF
The rats were killed by transcardiac perfusion with 200 ml of saline followed by 200 ml of phosphate-buffered paraformaldehyde. The brains were removed carefully, immersed in fixative, and refrigerated at 4 °C for 24–48 h. The brains were immersed in 30 % sucrose solution in phosphate buffered saline (PBS) for 24 h, then immediately frozen in liquid nitrogen and stored at −80 °C until use. Coronal sections were cut at −20 °C to a thickness of 15 μm. The sections were mounted onto slides and processed for histology and immunohistochemistry. Staining with hematoxylin and eosin was used to confirm neuronal damage after ischemic insults. For immunohistochemical analysis, endogenous peroxidase activity was quenched with 2 % hydrogen peroxide for 5 min at room temperature. Bovine serum albumin (5 %) was used to block nonspecific protein binding. Sections were incubated with rabbit polyclonal anti-bFGF antibody (diluted 1:200, Abcam, Cambridge, MA, USA). Negative control sections were incubated without the primary antibody. Sections were rinsed with PBS and incubated with biotinylated goat anti-rabbit secondary antibody. The sections were then incubated with streptavidin horseradish peroxidase, and diaminobenzidine (DAB) substrate was used for visualization of the catalyzed peroxidase reaction product. For semiquantitative measurements of bFGF density, stained sections were examined under a microscope (Leica Germany). For each rat, we selected three sections (Bregma −0.8 mm, −1.2 mm, −2.8 mm) and photographed immunoreactive cells from 12 locations in the peri-infarct area in a microscopic field at 40× magnification (4 fields per section × 3 sections per rat). Sections (n = 6 rats per group) were analyzed by an investigator blinded to the experimental cohort using Image J software (version 1.42q; NIH, Bethesda, MD).
Western Blot Assessment of bFGF
The rats were decapitated, and the brain tissues surrounding the infarct area were sampled and normalized for protein. Briefly, protein was separated on 12 % polyacrylamide gels with a 4 % stacking gel (SDS-PAGE), transferred to nitrocellulose membrane, and stained with rabbit polyclonal anti-bFGF antibody (diluted 1:300, Abcam). The secondary antibody was a goat anti-rabbit antibody conjugated with horseradish peroxidase (diluted 1:5,000, Santa Cruz Biotechnology, Santa Cruz, CA, USA). Proteins were detected by chemiluminescence with the ECL kit (Invitrogen, Carlsbad, CA, USA). The grayscales are directly proportional to the concentration of the conjugated peroxidase and, therefore, to the protein concentration in the Western blot membrane of each band. A polyclonal antibody to β-actin (diluted 1:300, Sigma) was applied as an internal control. The bFGF protein bands were scanned, and the relative densities were analyzed with Image J software and normalized to that of β-actin.
Statistical Analysis
Data are presented as mean ± standard deviation (SD). One-way analysis of variance (ANOVA) was used to compare group differences, and Student-Newman-Kuels post hoc test was applied to compare groups of the same duration of reperfusion if ANOVA revealed a significant difference. Differences between two groups were analyzed with Student’s t test. P < 0.05 was considered to be statistically significant.
Results
During the surgical procedure, physiological variables such as mean arterial blood pressure, pH, hematocrit, PaO2, and PaCO2 were within the normal range and did not differ significantly between the propofol-treated (20 mg kg−1 h−1) and vehicle-treated rats (data not shown, all P > 0.05). Mortality usually occurs within 24 h after transient cerebral ischemia. Propofol post-treatment did not affect the overall mortality rate, which was 13.5 % (20 of 148) in vehicle-treated rats and 12.9 % (19 of 147) in propofol-treated rats (P > 0.05) within 7 days after reperfusion.
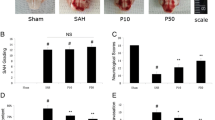
TTC staining revealed that MCAO caused infarct damage to the frontoparietal cortex, temporal cortex, and lateral portion of the neostriatum in the left hemisphere (Fig. 1A). Infarct volume (as a percent of the contralateral hemisphere) was greater at 24 h, 72 h, and 7 days of reperfusion than at 6 h of reperfusion in both treatment groups (n = 6/group, P < 0.05). Infarct volume reached a peak at 24 h of perfusion with no obvious changes observed during the remainder of the study time course. However, at 24 h, 72 h, and 7 days, the infarct volume in the striatum, cortex, and entire hemisphere was smaller in the propofol-treated rats than in the vehicle-treated rats (Fig. 1B–D; n = 6/group, P < 0.05).
Propofol post-treatment (20 mg kg−1 h−1, intravenous administration) protects rats from transient cerebral ischemia. A Representative coronal rat brain slices stained with TTC at 6 h (1, 2) and 24 h (3, 4) of reperfusion after 2-h middle cerebral artery occlusion. Slices 1 and 3 are from rats that received vehicle; slices 2 and 4 are from rats that received propofol. B–D Percent infarct volume in the cortex (B), striatum (C), and entire hemisphere (D). Data are presented as mean ± SD. n = 6 rats/group; *P < 0.05 versus the vehicle-treated group at 6 h of reperfusion (ANOVA with post hoc Student-Newman-Kuels test F = 21.6, 18.2, 20.6 respectively, P < 0.01); # P < 0.05 versus the vehicle-treated group at the same time point (Student’s t test)
Brain water content in the ipsilateral hemisphere was significantly lower in the propofol-treated group than in the vehicle-treated group at 24 h and 72 h of reperfusion (24 h: propofol, 81.2 ± 0.56 % vs. vehicle, 82.5 ± 0.61 %; P < 0.05; 72 h: propofol, 80.4 ± 0.52 % vs. vehicle, 81.9 ± 0.58 %, P < 0.01; n = 8/group, Fig. 2). Brain water content in the contralateral hemisphere was not significantly affected by MCAO and did not differ between propofol- and vehicle-treated groups (n = 8/group, P > 0.05).
MCAO produced substantial neurologic deficit by 24 h post-infarct in vehicle- and propofol-treated rats (Fig. 3). With increased duration of reperfusion, the neurologic deficit scores in both groups decreased. However at 72 h and 7 days of reperfusion, deficit scores were significantly lower in the propofol-treated rats than in the vehicle-treated rats (72 h: propofol, 6.2 ± 1.5 vs. vehicle, 8.5 ± 1.8, P < 0.05; 7 days: propofol, 3.8 ± 1.5 vs. vehicle, 7.2 ± 1.8, P < 0.01; n = 12/group, Fig. 3).
Propofol post-treatment (20 mg kg−1 h−1, intravenous administration) ameliorates neurologic deficits in rats after transient cerebral ischemia at 72 h and 7 days of reperfusion. Data are presented as mean ± SD. n = 12 rats/group; *P < 0.05, **P < 0.01 versus vehicle-treated group. mNSS, modified neurological severity score (Student’s t test)
Real-time PCR showed that, compared with baseline in the sham group, bFGF mRNA expression levels were unchanged in rats subjected to 2 h MCAO without reperfusion (data not shown) and in vehicle-treated rats at 6 h of reperfusion (Fig. 4; both P > 0.05); however, at 6 h of reperfusion, bFGF mRNA in the propofol-treated group was significantly greater than the baseline level. At 24 h of reperfusion, bFGF mRNA expression peaked in both the vehicle- and propofol-treated groups (Fig. 4). Levels were significantly greater in the propofol-treated rats than in the vehicle-treated rats at 6, 24, and 72 h of reperfusion (n = 8/group; Fig. 4). Expression in both groups returned to baseline by 7 days and was no longer significantly different (P > 0.05).
Propofol post-treatment (20 mg kg−1 h−1, intravenous administration) increases bFGF mRNA expression after transient cerebral ischemia. Data are presented as mean ± SD. n = 8 rats/group; **P < 0.01 versus the vehicle-treated group at the 6-h time point (ANOVA with post hoc Student-Newman-Kuels test, F = 165.5,P < 0.01); # P < 0.05, ## P < 0.01 versus the vehicle-treated group at the same time point (Student’s t test)
Immunohistochemistry revealed bFGF-positive cells in the ipsilateral peri-infarct areas. Most bFGF immunoreactivity appeared in plasma and nuclei of neuron-like and glia-like cells. The expression of bFGF was slight in the vehicle-treated group [mean optical density (OD) = 0.116 ± 0.008] at 6 h of reperfusion but strong in the propofol-treated group (OD = 0.145 ± 0.011, n = 6/group, P < 0.01). After 24 and 72 h reperfusion, the expression of bFGF increased significantly in both vehicle- and propofol-treated groups compared to that at 6 h. At those time points, mean OD was significantly greater in the propofol group (24 h: 0.208 ± 0.013; 72 h: 0.198 ± 0.013) than in the vehicle group (24 h: 0.165 ± 0.09; 72 h: 0.162 ± 0.011; n = 6/group, both P < 0.05). At 7 days of reperfusion, bFGF expression in neither group was significantly different from that at 6 h (both P > 0.05) (Fig. 5).
Propofol post-treatment (20 mg kg−1 h−1, intravenous administration) increases bFGF protein expression after transient cerebral ischemia. Rats were subjected to 2 h of middle cerebral artery occlusion followed by treatment with vehicle (A–D) or propofol (E–H). Representative photomicrographs (original magnification × 200) of bFGF-immunostained sections from the peri-infarct area of the ipsilateral hemisphere of rats at 6 h (A, E), 24 h (B, F), 72 h (C, G), and 7 days (D, H) of reperfusion. Scale bar = 20 μm. (I) Mean optical density value of bFGF evaluated by immunohistochemical analysis. Data are presented as mean ± SD. n = 6 rats/group; *P < 0.05 versus the vehicle-treated group at 6 h of reperfusion (ANOVA with post hoc Student-Newman-Kuels test, F = 57.6, P < 0.01); # P < 0.05 versus the vehicle-treated group at the same time point (Student’s t test)
Results from Western blot analysis were similar to those from immunohistochemistry. After 6, 24, and 72 h of reperfusion, the integrated density value ratio of bFGF to β-actin was significantly greater in the propofol-treated group than in the vehicle-treated group (n = 8/group, P < 0.05; Fig. 6) for the same period of reperfusion.
Propofol post-treatment (20 mg kg−1 h−1, intravenous administration) increases bFGF protein expression after transient cerebral ischemia. A Representative Western blot of bFGF in the peri-infarct area of the ipsilateral hemisphere of rats at 6 h, 24 h, 72 h, and 7 days after reperfusion from 2-h middle cerebral artery occlusion. B Optical density (OD) value of bFGF evaluated by Western blot analysis. Data are presented as mean ± SD. n = 8 rats/group; * P < 0.05 versus the vehicle-treated group at 6 h of reperfusion (ANOVA with post hoc Student-Newman-Kuels test, F = 15.1,P < 0.01); # P < 0.05 versus the vehicle-treated group at the same time point (Student’s t test)
Discussion
In this study we showed that propofol administered after transient cerebral ischemia reduced infarction volume and brain edema and improved neurologic function. These effects were shown for the first time to be associated with early expression of bFGF in the peri-infarct regions. Our findings may be applicable in the immediate aftermath of stroke as well as to patients with a stroke history undergoing surgery, patients in the intensive care unit under sedation, and patients undergoing neurosurgery, who may benefit from the neuroprotective effects of intravenous anesthetics. Our results provide additional understanding of the protective mechanism of anesthetics.
Researchers have proposed that propofol might provide neuroprotection to the ischemic brain by reducing cerebral blood flow [8, 24], intracranial pressure [25], and cerebral metabolic rate [8, 26]. Others have attributed its protection to antioxidant properties [27], potentiation of GABAA receptor-mediated inhibition of synaptic transmission [28], or inhibition of glutamate release [29]. Additionally, propofol was shown to favorably modulate apoptosis-regulating proteins, suppress apoptosis, and promote the survival of neurons in the areas that surround infarction [30]. Studies by Harman et al. [2] indicated that propofol can protect fetal brain against ischemia–reperfusion injury. Additionally, they reported that propofol provided a strong neuroprotective effect at the ultrastructural and mitochondrial levels [2]. Propofol post-conditioning induces long-term neuroprotection and can reduce internalization of AMPAR GluR2 subunit in the long term [18]. In this study, we confirmed that protection afforded by post-ischemic administration of propofol is still present at 7 days of reperfusion.
bFGF is an 18-kDa polypeptide shown to downregulate expression of NMDA receptors, antagonize excitotoxicity and excess intracellular calcium and free radicals, improve regional cerebral blood flow, enhance the survival of neurons, and increase axonal sprouting during neuronal injury [13, 31–33]. Consistent with our current findings, it has been reported that in normal brain tissue, bFGF is expressed at low levels, but that several hours after focal cerebral ischemia, bFGF protein levels increase in the peri-infarct brain regions. These levels increase even further by 24 h and return to normal after 7–14 days [34–36]. In mice with a null mutation of bFGF gene, both infarct volume and mortality rates were markedly increased after cerebral ischemia, indicating that endogenous bFGF contributes to protection against ischemic brain damage [12]. Exogenous bFGF administered before cerebral ischemia or several hours after ischemia was shown to reduce the infarction size and improve neurologic function [11, 37]. However, little research has been carried out to determine the effect of anesthetics on neurotrophic factor expression. In a bilateral carotid artery occlusion model in rats, propofol was shown to enhance neurogenesis after 28 days [14]. In our study, we found that propofol post-treatment was associated with an early increase in bFGF mRNA and protein expression, which likely contributed to the observed functional recovery.
In conclusion, we have shown that administration of propofol before reperfusion reduces cerebral infarct volume and brain edema and attenuates neurologic deficits associated with transient focal cerebral ischemia. These protective effects were associated with an increase in the expression of bFGF mRNA and protein in the regions surrounding the brain infarction. Our results suggest propofol as an anesthetic choice for neurosurgery and sedation in the ICU and indicate that it has potential for use in the treatment of cerebral ischemia.
References
Kawaguchi M, Furuya H, Patel PM (2005) Neuroprotective effects of anesthetic agents. J Anesth 19:150–156
Harman F, Hasturk AE, Yaman M, Arca T, Kilinc K, Sargon MF, Kaptanoglu E (2012) Neuroprotective effects of propofol, thiopental, etomidate, and midazolam in fetal rat brain in ischemia-reperfusion model. Childs Nerv Syst 28:1055–1062
Schwartz-Bloom RD, Miller KA, Evenson DA, Crain BJ, Nadler JV (2000) Benzodiazepines protect hippocampal neurons from degeneration after transient cerebral ischemia: an ultrastructural study. Neuroscience 98:471–484
Cole DJ, Cross LM, Drummond JC, Patel PM, Jacobsen WK (2001) Thiopentone and methohexital, but not pentobarbitone, reduce early focal cerebral ischemic injury in rats. Can J Anaesth 48:807–814
Li H, Tan J, Zou Z, Huang CG, Shi XY (2011) Propofol post-conditioning protects against cardiomyocyte apoptosis in hypoxia/reoxygenation injury by suppressing nuclear factor-kappa B translocation via extracellular signal-regulated kinase mitogen-activated protein kinase pathway. Eur J Anaesthesiol 28:525–534
Ariyama J, Shimada H, Aono M, Tsuchida H, Hirai KI (2000) Propofol improves recovery from paraquat acute toxicity in vitro and in vivo. Intensive Care Med 26:981–987
Hans P, Bonhomme V, Collette J, Albert A, Moonen G (1994) Propofol protects cultured rat hippocampal neurons against N-methyl-D-aspartate receptor-mediated glutamate toxicity. J Neurosurg Anesthesiol 6:249–253
Schlunzen L, Juul N, Hansen KV, Cold GE (2012) Regional cerebral blood flow and glucose metabolism during propofol anaesthesia in healthy subjects studied with positron emission tomography. Acta Anaesthesiol Scand 56:248–255
Jin YH, Zhang Z, Mendelowitz D, Andresen MC (2009) Presynaptic actions of propofol enhance inhibitory synaptic transmission in isolated solitary tract nucleus neurons. Brain Res 1286:75–83
Herring BE, McMillan K, Pike CM, Marks J, Fox AP, Xie Z (2011) Etomidate and propofol inhibit the neurotransmitter release machinery at different sites. J Physiol 589:1103–1115
Watanabe T, Okuda Y, Nonoguchi N et al (2004) Postischemic intraventricular administration of FGF-2 expressing adenoviral vectors improves neurologic outcome and reduces infarct volume after transient focal cerebral ischemia in rats. J Cereb Blood Flow Metab 24:1205–1213
Kiprianova I, Schindowski K, von Bohlen und Halbach O, Krause S, Dono R, Schwaninger M, Unsicker K (2004) Enlarged infarct volume and loss of BDNF mRNA induction following brain ischemia in mice lacking FGF-2. Exp Neurol 189:252–260
Chen J, Li Y, Katakowski M, Chen X, Wang L, Lu D, Lu M, Gautam SC, Chopp M (2003) Intravenous bone marrow stromal cell therapy reduces apoptosis and promotes endogenous cell proliferation after stroke in female rat. J Neurosci Res 73:778–786
Lasarzik I, Winkelheide U, Stallmann S, Orth C, Schneider A, Tresch A, Werner C, Engelhard K (2009) Assessment of postischemic neurogenesis in rats with cerebral ischemia and propofol anesthesia. Anesthesiology 110:529–537
Jiang X, Gao L, Zhang Y, Wang G, Liu Y, Yan C, Sun H (2011) A comparison of the effects of ketamine, chloral hydrate and pentobarbital sodium anesthesia on isolated rat hearts and cardiomyocytes. J Cardiovasc Med (Hagerstown) 12:732–735
Li W, Zheng B, Xu H, Deng Y, Wang S, Wang X, Su D (2012) Isoflurane prevents neurocognitive dysfunction after cardiopulmonary bypass in rats. J Cardiothorac Vasc Anesth. doi:10.1053/j.jvca.2012.09.005..
Longa EZ, Weinstein PR, Carlson S, Cummins R (1989) Reversible middle cerebral artery occlusion without craniectomy in rats. Stroke J Cerebral circul 20:84–91
Wang H, Luo M, Li C, Wang G (2011) Propofol post-conditioning induced long-term neuroprotection and reduced internalization of AMPAR GluR2 subunit in a rat model of focal cerebral ischemia/reperfusion. J Neurochem 119:210–219
Chen J, Sanberg PR, Li Y, Wang L, Lu M, Willing AE, Sanchez-Ramos J, Chopp M (2001) Intravenous administration of human umbilical cord blood reduces behavioral deficits after stroke in rats. Stroke J Cerebral Circul 32:2682–2688
Chen J, Li Y, Wang L, Zhang Z, Lu D, Lu M, Chopp M (2001) Therapeutic benefit of intravenous administration of bone marrow stromal cells after cerebral ischemia in rats. Stroke 32:1005–1011
Shimakura A, Kamanaka Y, Ikeda Y, Kondo K, Suzuki Y, Umemura K (2000) Neutrophil elastase inhibition reduces cerebral ischemic damage in the middle cerebral artery occlusion. Brain Res 858:55–60
Ping A, Chun ZX, Xue XY (2005) Bradykinin preconditioning induces protective effects against focal cerebral ischemia in rats. Brain Res 1059:105–112
Wang J, Tsirka SE (2005) Neuroprotection by inhibition of matrix metalloproteinases in a mouse model of intracerebral haemorrhage. Brain 128:1622–1633
Van Hemelrijck J, Fitch W, Mattheussen M, Van Aken H, Plets C, Lauwers T (1990) Effect of propofol on cerebral circulation and autoregulation in the baboon. Anesth Analg 71:49–54
Watts AD, Eliasziw M, Gelb AW (1998) Propofol and hyperventilation for the treatment of increased intracranial pressure in rabbits. Anesth Analg 87:564–568
Dam M, Ori C, Pizzolato G, Ricchieri GL, Pellegrini A, Giron GP, Battistin L (1990) The effects of propofol anesthesia on local cerebral glucose utilization in the rat. Anesthesiology 73:499–505
Wilson JX, Gelb AW (2002) Free radicals, antioxidants, and neurologic injury: possible relationship to cerebral protection by anesthetics. J Neurosurg Anesthesiol 14:66–79
Ito H, Watanabe Y, Isshiki A, Uchino H (1999) Neuroprotective properties of propofol and midazolam, but not pentobarbital, on neuronal damage induced by forebrain ischemia, based on the GABAA receptors. Acta Anaesthesiol Scand 43:153–162
Engelhard K, Werner C, Hoffman WE, Matthes B, Blobner M, Kochs E (2003) The effect of sevoflurane and propofol on cerebral neurotransmitter concentrations during cerebral ischemia in rats. Anesth Analg 97:1155–1161 table of contents
Engelhard K, Werner C, Eberspacher E, Pape M, Blobner M, Hutzler P, Kochs E (2004) Sevoflurane and propofol influence the expression of apoptosis-regulating proteins after cerebral ischaemia and reperfusion in rats. Eur J Anaesthesiol 21:530–537
Jin-qiao S, Bin S, Wen-hao Z, Yi Y (2009) Basic fibroblast growth factor stimulates the proliferation and differentiation of neural stem cells in neonatal rats after ischemic brain injury. Brain Dev 31:331–340
Lenhard T, Schober A, Suter-Crazzolara C, Unsicker K (2002) Fibroblast growth factor-2 requires glial-cell-line-derived neurotrophic factor for exerting its neuroprotective actions on glutamate-lesioned hippocampal neurons. Mol Cell Neurosci 20:181–197
Tanaka R, Miyasaka Y, Yada K, Ohwada T, Kameya T (1995) Basic fibroblast growth factor increases regional cerebral blood flow and reduces infarct size after experimental ischemia in a rat model. Stroke 26:2154–2158 discussion 2158–2159
Speliotes EK, Caday CG, Do T, Weise J, Kowall NW, Finklestein SP (1996) Increased expression of basic fibroblast growth factor (bFGF) following focal cerebral infarction in the rat. Brain Res Mol Brain Res 39:31–42
Lin TN, Te J, Lee M, Sun GY, Hsu CY (1997) Induction of basic fibroblast growth factor (bFGF) expression following focal cerebral ischemia. Brain Res Mol Brain Res 49:255–265
Wei OY, Huang YL, Da CD, Cheng JS (2000) Alteration of basic fibroblast growth factor expression in rat during cerebral ischemia. Acta Pharmacol Sin 21:296–300
Fujiwara K, Date I, Shingo T, Yoshida H, Kobayashi K, Takeuchi A, Yano A, Tamiya T, Ohmoto T (2003) Reduction of infarct volume and apoptosis by grafting of encapsulated basic fibroblast growth factor-secreting cells in a model of middle cerebral artery occlusion in rats. J Neurosurg 99:1053–1062
Acknowledgments
This work was supported by NSFC (81000824, 81101402, 81171782), and NIH (K01AG031926, R01AT007317, R01NS078026). We thank Claire Levine for assistance with this manuscript.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Zhao, XC., Zhang, LM., Tong, DY. et al. Propofol Increases Expression of Basic Fibroblast Growth Factor After Transient Cerebral Ischemia in Rats. Neurochem Res 38, 530–537 (2013). https://doi.org/10.1007/s11064-012-0945-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-012-0945-4