Abstract
Purpose
Although barbiturates are considered to be cerebral protectants, little is known regarding the relative efficacy of different barbiturates to reduce ischemie brain injury. In a model of middle cerebral artery occlusion (MCAo), we compared the relative effects of 1.0 and 0.4 burst-suppression doses of thiopentone, methohexital, and pentobarbitone on cerebral infarct.
Methods
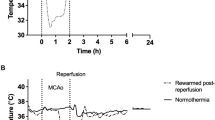
During isoflurane anesthesia, MCAo was achieved via a temporal craniotomy. Thirty minutes before MCAo the rats were randomized to receive one of the following which was maintained throughout the study. Halothane (n = 20)−1.2 MAC halothane, thiopentone (n = 20), methohexital (n = 20), or pentobarbitone (n = 20). The first ten animals in each barbiturate group received the respective barbiturate in a dose sufficient to maintain burst-suppression of the electroencephalogram (3–5 bursts·min−1). The subsequent ten animals in each barbiturate group received 40% of the burst-suppression dose. After 180 min of MCAo and 120 min of reperfusion, cerebral injury was assessed.
Results
For the burst-suppression animals, injury volume (mm3, mean ± SD) was less in the thiopentone group (88 ± 14) than the halothane (133 ± 17), methohexital (126 ± 19), or pentobarbitone ( 130 ± 17) groups (P < 0.05). For 0.4 burst-suppression animals, injury volume was less for the methohexital group (70 ± 22) than the halothane (124 ± 24), thiopentone (118 ± 15), or pentobarbitone (121 ± 20) groups (P < 0.05).
Conclusions
These data are inconsistent with the longstanding assumption that electrophysiologically comparable doses of the various classes of barbiturates have equivalent protective efficacy. They in turn suggest that mechanisms other than, or at least in addition to, metabolic suppression may contribute to the protective effect of barbiturates.
Résumé
Objectif
Bien que les barbituriques soient considérés comme des protecteurs cérébraux, on en sait peu sur leur efficacité relative à réduire la lésion cérébrale ischémique. Nous avons comparé, chez un modèle d’occlusion de l’artère cérébrale moyenne (OACM), les effets relatifs de doses de thiopental, méthohexital et pentobarbital, capables de suppression totale et à 40 % (1,0 et 0,4) des bouffées du tracé électroencéphalographique (EEG), sur l’infarctus cérébral.
Méthode
Pendant l’anesthésie à l’isoflurane, l’OACM a été provoquée au moyen d’une craniotomie temporale. Trente minutes avant l’occlusion, les rats ont été randomisés et ont reçu un des médicaments suivants, thérapie maintenue tout au long de l’étude : 1,2 CAM d’halothane (n = 20), du thiopental (n = 20), du méthohexital (n = 20) ou du pentobarbital (n = 20). Les dix premiers animaux de chaque groupe barbiturique ont reçu une dose du médicament suffisante pour maintenir la suppression des bouffées du tracé EEG (3–5·min−1). Les dix animaux suivants de chaque groupe barbiturique ont reçu 40 % de la dose causant la suppression des bouffées. On a évalué la lésion cérébrale après 180 min d’OACM suivie de 120 min de reperfusion.
Résultats
Pour les animaux chez qui il y a eu suppression des bouffées du tracé EEG, le volume lésionnel (mm3, moyenne ± écart type) a été plus bas avec le thiopental (88 ± 14) qu’avec l’halothane (133 ± 17), le méthohexital (126 ± 19) ou le pentobarbital (130 ± 17) (P < 0,05). Pour une suppression à 40 %, le volume lésionnel a été moindre avec le méthohexital (70 ± 22) qu’avec l’halothane (124 ± 24), le thiopental (118 ± 15) ou le pentobarbital (121 ± 20) (P < 0,05).
Conclusion
Ces données contredisent l’hypothèse de longue date voulant que des doses comparables, au plan électrophysiologique, de diverses classes de barbituriques présentent une efficacité protectrice équivalente. Elles évoquent, par ailleurs, que des mécanismes de suppression métabolique différents, ou tout au moins additionnels, peuvent contribuer à l’effet protecteur des barbituriques.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Nehls DG, Todd MM, Spetzler RF, Drummond JC, Thompson RA, Johnson PC. A comparison of the cerebral protective effects of isoflurane and barbiturates during temporary focal ischemia in primates. Anesthesiology 1987; 66: 453–64.
Warner DS, Zhou J, Ramani R, Todd MM. Reversible focal ischemia in the rat: effects of halothane, isoflurane, and methohexital anesthesia. J Cereb Blood Flow Metab 1991; 11: 794–802.
Drummond JC, Cole DJ, Patel PM, Reynolds LW. Focal cerebral ischemia during anesthesia with etomidate, isoflurane, or thiopental: a comparison of the extent of cerebral injury. Neurosurgery 1995; 37: 742–9.
Michenfelder JD, Theye RA. Cerebral protection by thiopental during hypoxia. Anesthesiology 1973; 39: 510–7.
Michenfelder JD. The interdependency of cerebral functional and metabolic effects following massive doses of thiopental in the dog. Anesthesiology 1974; 41: 231–6.
Todd MM, Warner DS. A comfortable hypothesis reevaluated. Cerebral metabolic depression and brain protection during ischemia (Editorial). Anesthesiology 1992; 76: 161–4.
Warner DS, Takaoka S, Wu B, et al. Electroencephalographic burst suppression is not required to elicit maximal neuroprotection from pentobarbital in a rat model of focal cerebral ischemia. Anesthesiology 1996; 84: 1475–84.
Cole DJ, Kalichman MW, Shapiro HM, Drummond JC. The non-linear potency of sub-MAC concentrations of nitrous oxide in decreasing the anesthetic requirement of enflurane, halothane, and isoflurane in rats. Anesthesiology 1990; 73: 93–9.
Cole DJ, Drummond JC, Osborne TN, Matsumura J. Hypertension and hemodilution during cerebral ischemia reduce brain injury and edema. Am J Physiol 1990; 259: H211–7.
Cole DJ, Schell RM, Przybelski RJ, Drummond JC, Bradley K. Focal cerebral ischemia in rats: effect of hemodilution with — cross-linked hemoglobin on CBF. J Cereb Blood Flow Metab 1992; 12: 971–6.
Swanson RA, Morton MT, Tsao-Wu G, Savalos RA, Davidson C, Sharp FR. A semiautomated method for measuring brain infarct volume. J Cereb Blood Flow Metab 1990; 10: 290–3.
Sano T, Patel PM, Drummond JC, Cole DJ. A comparison of the cerebral protective effects of etomidate, thiopental and isoflurane in a model of forebrain ischemia in the rat. Anesth Analg 1993; 76: 990–7.
Schmid-Elsaesser R, Schröder M, Zausinger S, Hungerhuber E, Baethmann A, Reulen H-J. EEG burst suppression is not necessary for maximum barbiturate protection in transient focal cerebral ischemia in the rat. J Neurol Sci 1999; 162: 14–9.
Hoff JT, Smith AL, Hankinson HL, Nielsen SL. Barbiturate protection from cerebral infarction in primates. Stroke 1975; 6: 28–33.
Corkill G, Sivalingam S, Reitan JA, Gilroy BA, Helphrey MG. Dose dependency of the post-insult protective effect of pentobarbital in the canine experimental stroke model. Stroke 1978; 9: 10–2.
Wang T, Raley-Susman KM, Wang J, Chambers G, Cottrell JE, Kass IS. Thiopental attenuates hypoxic changes of electrophysiology, biochemistry, and morphology in rat hippocampal slice CA1 pyramidal cells. Stroke 1999; 30: 2400–7.
Zhu H, Cottrell JE, Kass IS. The effect of thiopental and propofol on NMDA- and AMPA-mediated glutamate excitotoxicity. Anesthesiology 1997; 87: 944–51.
Bickler PE, Buck LT, Feiner JR. Volatile and intravenous anesthetics decrease glutamate release from cortical brain slices during anoxia. Anesthesiology 1995; 83: 1233–40.
Almaas R, Saugstad OD, Pleasure D, Rootwelt T. Effect of barbiturates on hydroxyl radicals, lipid peroxidation, and hypoxic cell death in human NT2-N neurons. Anesthesiology 2000; 92: 764–74.
Miao N, Nagao K, Lynch IIIC. Thiopental and methohexital depress Ca2+ entry into and glutamate release from cultured neurons. Anesthesiology 1998; 88: 1643–53.
Kimbro JR, Kelly PJ, Drummond JC, Cole DJ, Patel PM. Isoflurane and pentobarbital reduce AMPA toxicity in vivo in the rat cerebral cortex. Anesthesiology 2000; 92: 806–12.
Weiss M, Buhl R, Birkhahn A, Mirow N, Schneider M, Wernet P. Do barbiturates and their solutions suppress FMLP-induced neutrophil chemiluminescence? Eur J Anaesthesiol 1994; 11: 371–9.
Smith DS, Rehncrona S, Siesjö BK. Inhibitory effects of different barbiturates on lipid peroxidation in brain tissue in vitro: comparison with the effects of promethazine and chlorpromazine. Anesthesiology 1980; 53: 186–94.
Ashwal S, Cole DJ, Osborne TN, Pearce WJ. Dual effects of L-NAME during transient focal cerebral ischemia in spontaneously hypertensive rats. Am J Physiol 1994; 267: H276–84.
Samdani AF, Dawson TM, Dawson VL. Nitric oxide synthase in models of focal ischemia. Stroke 1997; 28: 1283–8.
Clower BR, Yamamoto Y, Cain L, Haines DE, Smith RR. Endothelial injury following experimental subarachnoid hemorrhage in rats: effects on brain blood flow. Anat Rec 1994; 240: 104–14.
Iadecola C, Zhang F, Xu S, Casey R, Ross ME. Inducible nitric oxide synthase gene expression in brain following cerebral ischemia. J Cereb Blood Flow Metab 1995; 15: 378–84.
Dawson DA. Nitric oxide and focal cerebral ischemia: multiplicity of actions and diverse outcome. Cerebrovasc Brain Metab Rev 1994; 6: 299–324.
Shibuta S, Kosaka J, Mashimo T, Fukuda Y, Yoshiya I. Nitric oxide-induced cytotoxicity attenuation by thiopentone sodium but not pentobarbitone sodium in primary brain cultures. Br J Pharmacol 1998; 124: 804–10.
Hatano Y, Nakamura K, Moriyama S, Mori K, Toda N. The contractile responses of isolated dog cerebral and extracerebral arteries to oxybarbiturates and thiobarbiturates. Anesthesiology 1989; 71: 80–6.
Yakushiji T, Nakamura K, Hatano Y, Mori K. Comparison of the vasodilator effects of thiopentone and pentobarbitone. Can J Anaesth 1992; 39: 604–9.
Heyer EJ, Macdonald RL. Barbiturate reduction of calcium-dependent action potentials: correlation with anesthetic action. Brain Res 1982; 236: 157–71.
Gundersen CB, Umbach JA, Swartz BE. Barbiturates depress currents through human brain calcium channels studied in Xenopus oocytes. J Pharmacol Exp Ther 1988; 247: 824–9.
Zhan R-Z, Fujiwara N, Yamakura T, Taga K, Fukuda S, Shimoji K. Differential inhibitory effects of thiopental, thiamylal and phenobarbital on both voltage-gated calcium channels and NMDA receptors in rat hippocampal slices. Br J Anaesth 1998; 81: 932–9.
Giffard RG, Weiss JH, Swanson RA, Choi DW. Secobarbital attenuates excitotoxicity but potentiates oxygen-glucose deprivation neuronal injury in cortical cell culture. J Cereb Blood Flow Metab 1993; 13: 803–10.
Buchan AM, Xue D, Huang Z-G, Smith KH, Lesiuk H. Delayed AMPA receptor blockade reduces cerebral infarction induced by focal ischemia. Neuroreport 1991; 2: 473–6.
Cai Z, McCaslin PP. Acute, chronic and differential effects of several anesthetic barbiturates on glutamate receptor activation in neuronal culture. Brain Res 1993; 611: 181–6.
Zeman S, Lodge D. Pharmacological characterization of non-NMDA subtypes of glutamate receptor in the neonatal rat hemisected spinal cord in vitro. Br J Pharmacol 1992; 106: 367–72.
Swanson RA, Seid LL. Barbiturates impair astrocyte glutamate uptake. Glia 1998; 24: 365–71.
Miyazaki H, Nakamura Y, Arai T, Kataoka K. Increase of glutamate uptake in astrocytes. A possible mechanism of action of volatile anesthetics. Anesthesiology 1997; 86: 1359–66.
Qu H, Faerø E, Jørgensen P, et al. Decreased glutamate metabolism in cultured astrocytes in the presence of thiopental. Biochem Pharmacol 1999; 58: 1075–80.
Patel PM, Goskowicz RL, Drummond JC, Cole DJ. Etomidate reduces ischemia-induced glutamate release in the hippocampus in rats subjected to incomplete forebrain ischemia. Anesth Analg 1995; 80: 933–9.
Hatfield RH, Mendelow AD, Perry RH, Alvarez LM, Modha P. Triphenyltetrazolium chloride (TTC) as a marker for ischaemic changes in rat brain following permanent middle cerebral artery occlusion. Neuropathol Appl Neurobiol 1991; 17: 61–7.
Isayama K, Pitts LH, Nishimura MC. Evaluation of 2,3,5-triphenyltetrazolium chloride staining to delineate rat brain infarcts. Stroke 1991; 22: 1394–8.
Du C, Hu R, Csernansky CA, Hsu CY, Choi DW. Very delayed infarction after mild focal cerebral ischemia: a role for apoptosis? J Cereb Blood Flow Metab 1996; 16: 195–201.
Kawaguchi M, Kimbro JR, Drummond JC, Cole DJ, Kelly PJ, Patel PM. Isoflurane delays but does not prevent cerebral infarction in rats subjected to focal ischemia. Anesthesiology 2000; 92: 1335–42.
Author information
Authors and Affiliations
Corresponding author
Additional information
Support for this study was provided by the Department of Anesthesiology, Loma Linda University-School of Medicine.
Rights and permissions
About this article
Cite this article
Cole, D.J., Cross, L.M., Drummond, J.C. et al. Thiopentone and methohexital, but not pentobarbitone, reduce early focal cerebral ischemic injury in rats. Can J Anesth 48, 807–814 (2001). https://doi.org/10.1007/BF03016699
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03016699