Abstract
Oxidized low-density lipoprotein (oxLDL) plays a central role in the pathogenesis of atherosclerosis, in part via an effect to promote endothelial dysfunction. In the present study, we evaluated the expression profiles of long non-coding RNAs (lncRNAs) and protein-coding mRNAs in endothelial cells following oxLDL stimulation. LncRNAs and mRNAs from human umbilical vein endothelial cells (HUVECs) were profiled with the Arraystar Human lncRNA Expression Microarray V3.0 following 24 h of oxLDL treatment (100 µg/mL). Of the 30,584 lncRNAs screened, 923 were significantly up-regulated and 975 significantly down-regulated (P < 0.05) in response to oxLDL exposure. In the same HUVEC samples, 518 of the 26,106 mRNAs screened were up-regulated and 572 were down-regulated. Of these differentially expressed lncRNAs, CLDN10-AS1 and CTC-459I6.1 were the most up-regulated (~87-fold) and down-regulated (~28-fold), respectively. Bioinformatic assignment of the differentially regulated genes into functional groups indicated that many are involved in signaling pathways among which are the cytokine receptor, chemokine, TNF, MAPK and Ras signaling pathways, olfactory transduction, and vascular smooth muscle cell function. This is the first report profiling oxLDL-mediated changes in lncRNA and mRNA expression in human endothelial cells. The novel targets revealed substantially extend the list of potential candidate genes involved in atherogenesis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Atherosclerosis is a progressive inflammatory vascular disease that leads to atheromatous plaque development within the intima of the arteries [1–4]. Endothelial dysfunction plays a central role in the development and natural course of atherosclerosis [5–8]. Oxidized low-density lipoprotein cholesterol (oxLDL) is a well-established risk factor for atherothrombosis and exerts a plethora of effects to promote endothelial dysfunction, plaque progression, and inflammatory interactions between monocytes and the underlying vessel wall [9–11]. Understanding the molecular pinnings of how oxLDL incites endothelial activation may uncover novel approaches to limit atherosclerosis.
Non-coding RNAs (ncRNAs) form a high percentage of the mammalian genome. Two major subgroups of ncRNAs that have been identified are the long ncRNAs (lncRNAs) and the microRNAs (miRNAs) [12, 13]. LncRNAs are generally described as sequences that are longer than 200 nucleotides. Due to the absence of open reading frames, lncRNAs do not possess any translational ability but they are however able to alter gene expressions and signaling pathways [14]. Although lncRNAs do not appear to be as evolutionarily conserved as protein-coding genes, the available evidence strongly indicate that lncRNAs are intimately involved in the regulation of tissue homeostasis as well as a wide variety of cellular functions that include proliferation, migration, invasion, angiogenesis, differentiation, and survival [14].
In recent years, lncRNAs have not only been implicated as novel regulators of multiple physiological and pathological conditions but also as potential therapeutic targets due to their ability to function as a molecular signal to regulate gene transcription and epigenetic modifications [15]. Indeed there is a growing appreciation of the role of lncRNAs in the regulation of cardiovascular diseases (CVDs) [16]. For example, the lncRNA Novlnc6 was recently found to be associated with acute myocardial infarction and another Mhrt has been linked with heart failure along with other lncRNAs that are involved in controlling hypertrophy, mitochondrial function, and cardiomyocyte death [16–19].
The endothelial-expressed lncRNAs MALAT1 and Tie-1-AS have been reported to control endothelial function in the vascular system [20, 21], and ANRIL has been demonstrated to regulate cell proliferation, cell adhesion, and apoptosis—cellular activities crucial for atherosclerosis [22]. Furthermore, a recent report noted the negative transcriptional regulatory role of lncRNA NAT APOA1-AS for APOA1, which is the main protein constituent of high-density lipoprotein (HDL), an important lipoprotein that is associated with reduced atherosclerosis [23].
Overall, these studies project lncRNAs as evolving regulators in CVDs and atherosclerosis. That said, our understanding of the underlying influence and function of lncRNAs in endothelial dysfunction and atherosclerosis remains still quite limited [24, 25]. In the present study, we performed the first transcriptome profiling of lncRNA expression upon oxLDL treatment in endothelial cells.
Materials and methods
Cell culture
Human umbilical vein endothelial cells (HUVECs, Lonza) and Human coronary artery endothelial cells (HCAECs, Lonza) were cultured in endothelial cell growth medium-2 (EGMTM-2 Bulletkit™; Lonza) supplemented with growth factors, serum, and antibiotics at 37 °C in humidified 5% CO2 incubator. Confluent HUVECs were maintained in 6-well plates for 24 h with or without the presence of oxLDL (100 µg/mL; Alfa Aesar). Cells were serum-starved overnight before they were treated with either oxLDL or the vehicle.
RNA preparation
Total RNA, isolated from HUVECs using the TRIzol™ (Invitrogen) reagent and according to the manufacturer’s instructions, was quantified with the NanoDrop ND-1000 spectrophotometer. RNA integrity was confirmed by standard denaturing agarose gel electrophoresis.
Microarray profiling
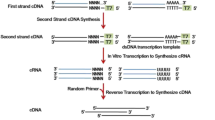
The expression profile of 30,584 human lncRNAs and 26,106 protein-coding transcripts was conducted with the Arraystar Human LncRNA Microarray V3.0. Sample labeling and array hybridization were performed on the Agilent Array platform. In brief, total RNA from each sample was amplified and transcribed into fluorescent cRNA (Arraystar Flash RNA Labeling Kit, Arraystar) before 1 µg of each labeled cRNA was hybridized onto the microarray slide. The hybridized arrays were subsequently washed, fixed, and scanned using the Agilent DNA Microarray Scanner (Product#G2505C). Array images so collected were studied with the Agilent Feature Extraction software (version 11.0.1.1). We utilized the GeneSpring GX v11.5.1 software package (Agilent Technologies) to conduct quantile normalization and process the data. Statistical significance for differentially expressed (DE) genes was evaluated with the Student’s t-test and adjusted for multiple testing by the Benjamini–Hochberg method to minimize the false discovery rate. Volcano plot filtering, set at a threshold of ≥ 2.0 folds, was used to screen for lncRNAs and mRNAs that exhibited significantly different (P < 0.05; unpaired t-test) expression levels in the two study groups. Pathway analysis was based on the current Kyoto Encyclopedia of Genes and Genomes (KEGG) database. Gene Ontology (GO) analysis was performed with the topGO package of bioconductor system.
Validation qPCR
Confluent HUVECs and HCAECs were starved overnight and then maintained for 24 h with either the diluent or oxLDL (100 µg/mL). Total RNA was isolated and qPCR for lncRNAs was performed using standard protocols. The sequences for primers used to perform validation qPCR are described in Supplementary Table 1.
Results
Quality Assessment of lncRNAs and mRNAs data
RNA integrity and genomic DNA contamination of the six samples evaluated were measured by denaturing agarose gel electrophoresis. The intensity of the upper 28S ribosomal RNA band in all of the samples was about twice that of the lower 18S band, thereby confirming RNA integrity. The absence of smears above the 28S band attested to the purity of the RNA samples (Supplementary Fig. 1A). RNA quantity and purity were also confirmed with the NanoDrop ND-1000. All samples had an A260 /A280 ratio that was close to 2.0 and an A260/A230 ratio that exceeded 1.8 (Supplementary Fig. 1A). Box plots that included the 10th and 90th percentile values revealed comparable expression values after normalization (Supplementary Fig. 1B).
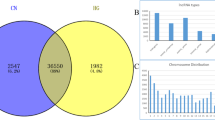
Scatter plots were generated to provide a profile of HUVEC lncRNAs (Fig. 1a) and mRNAs (Fig. 1b) that were up-regulated, down-regulated, or unaffected by oxLDL treatment. Overall, the average fold-changes for DE lncRNAs and mRNAs under the two study conditions were similar (Fig. 1c). Volcano plot filtering uncovered 923 significantly up-regulated and 975 significantly down-regulated lncRNAs in HUVECs treated with oxLDL in comparison to vehicle-treated control samples (Fig. 1d, P < 0.05). LncRNAs that demonstrated the greatest differences in expression ranged from 895 to 3307 bp. Specifically, CLDN10-AS1 (RNA length: 895 bp, chromosome 13) was the most up-regulated lncRNA (~87 fold) and CTC-459I6.1 (RNA length: 535 bp, chromosome 5) the most down-regulated (28 fold) in HUVECs subjected to oxLDL treatment. Table 1 lists the 10 most up-/down-regulated lncRNAs in response to oxLDL treatment. OxLDL also produced changes at the transcript level; specifically the levels of 1090 mRNAs were altered following oxLDL exposure with 518 up-regulated and 572 down-regulated (Fig. 1e, P < 0.05). Proinflammatory macrophage marker HLA-DPB1 (Major Histocompatibility Complex, Class II, DP Beta-1) was the most up-regulated (~241 fold) mRNA transcript after oxLDL stimulation in endothelial cells. Validation qPCR performed for 7 up-regulated and 5 down-regulated lncRNA showed similar trend for HUVECs and HCAECs after oxLDL treatment (Table 2).
LncRNA and mRNA expression profiles in HUVECs treated with oxLDL (100 µg/mL) vs. control. a, b Scatter plots comparing the variation in lncRNA and mRNA expression. The values plotted are the averaged normalized signal values (log2 scaled) for the control (x axis) and the oxLDL treatment (y axis) groups. The green lines indicate fold-change. LncRNAs and mRNAs above the top green line and below the bottom green line exhibit at least a 2.0-fold difference between the two study groups. c Box-and-Whisker plots (10th, 90th percentile) showing average fold-change of lncRNAs and mRNAs. Median intensity is denoted with a “−” sign and mean intensity denoted with a “+” sign. d, e Volcano plots detailing magnitude of expression difference. The vertical green lines correspond to 2.0-fold up-regulation and 2.0-fold down-regulation of expression. The horizontal green line indicates a p value of ≤ 0.05. Red points represent lncRNAs and mRNAs with statistically significant differential expression (fold-change ≥ 2.0, P ≤ 0.05)
LncRNA chromosomal distribution and subtype analysis
Supplementary Fig. 2 shows the dendrograms generated for hierarchical analysis of clustered DE lncRNAs and mRNAs in the two study groups. Although lncRNAs modulated by oxLDL treatment were abundant and present on every chromosome, they were most commonly found on chromosomes 1, 2, and 5 (Fig. 2a). Further probing revealed that while these DE lncRNAs were generally expressed along the entire length of the chromosomes, there was notable clustering (Fig. 2b). LncRNA subgroup analysis, which helps identify the functional relationship between lncRNAs and their associated protein-coding genes, demonstrated that the majority (~50%) of the DE lncRNAs were intergenic in origin followed by intron and natural antisense lncRNAs (Fig. 2c).
Distribution, location, and classification of differentially expressed lncRNAs in HUVECs treated with oxLDL (100 µg/mL) versus control. Demonstration of a numbers and b chromosomal location of DE lncRNAs on different chromosomes. c Bar graph representing types of differently expressed lncRNAs, depending upon their genomic location
LncRNAs and associated protein-coding transcripts
We conducted additional investigations to gather further insights into the DE lncRNAs and their associated protein-coding transcripts. The 10 most up- and down-regulated lncRNAs with their known associated protein-coding genes are summarized in Fig. 3. Interestingly, all 20 lncRNAs demonstrated a direct correlation in fold-change with its associated mRNA (Fig. 3).
Network co-expression and bioinformatics analyses of samples from HUVECs treated with oxLDL (100 µg/mL) vs. control. Representation of DE lncRNAs and associated genes with respect to fold-change. Ten significantly up-regulated and 10 down-regulated lncRNAs with known target genes were selected for presentation in the figure
Bioinformatics analyses
Pathway analysis with the current KEGG database yielded several pertinent findings (Tables 3, 4). Briefly, lncRNAs up-regulated in response to oxLDL treatment are most commonly associated with the cytokine–cytokine receptor interface, chemokine signaling pathway, TNF signaling pathway, and estrogen signaling pathway (Table 3). The most down-regulated lncRNAs are notably involved in olfactory transduction, MAPK signaling pathway, Ras signaling pathway, cytoskeletal actin regulation, and vascular smooth muscle contraction (Table 4).
Table 5 details the results of the GO analysis that grouped the DE mRNAs under the following three categories: Biological Processes, Cellular Component, and Molecular Function. GO terms most broadly associated with up-regulated mRNAs were regulation of biological processes, extracellular space, and binding (Table 5). GO terms associated with down-regulated mRNA were mainly enriched in single-organism process, membrane components, and carbohydrate derivative binding (Table 5).
Discussion
We have come a long way since the initial description of how modified LDL is involved in the transformation of macrophages to foam cells in the atherosclerotic process [26, 27]. It is now well established that foam cells release proinflammatory cytokines, reactive oxygen species (ROS), and matrix degrading proteolytic enzymes, which together promote plaque formation and destabilization [4]. These observations provided the impetus behind the notion that oxidative modification of LDL alters its biological signature such that it acquires the ability to nurture the atherosclerotic process via multiple avenues [9, 28]. Specifically, oxLDL is capable of inciting endothelial cell dysfunction, proliferation, apoptosis, and necrosis, all of which are critical components of the atherosclerotic state [29, 30]. Under physiological conditions, endothelial cells release nitric oxide (NO), which serves to maintain vascular tone [31]. In the presence of oxLDL, however, NO release is inhibited and the NO that is generated is quickly inactivated by the enhanced production of ROS [31–33]. OxLDL-associated endothelial cell loss—either via necrosis or apoptosis—not only augments vascular permeability and promotes smooth muscle cell (SMC) proliferation but also amplifies coagulation which together aid in the process of atherogenesis [34, 35].
In addition to its role in atherogenesis, oxLDL has been highlighted as a biomarker for CVD in recent years [36, 37]. Mechanisms of oxLDL-mediated endothelial dysfunction have been well studied [38, 39]. Although the molecular mechanisms have been studied for many years, the detailed epigenetic alterations with a special emphasis on the crosstalk between oxLDL and lncRNAs have remained unknown.
Although several thousands of lncRNAs have been recognized in mammals, our understanding of regulation and function of lncRNAs is still limited. However, due to recent rapid advancements in the molecular biology field, immense attention has been reaped by lncRNAs and their roles. The lncRNAs have already been reported in a broad range of physiological and pathological conditions but their function in the development of CVDs and especially in atherosclerosis is inadequately understood. MIAT and ANRIL were the earliest lncRNAs identified as a risk factor for CVDs [40–42]. ANRIL regulates genes involved in cell proliferation, cell adhesion, and apoptosis, and also correlates with the gravity of atherosclerosis in humans [22, 41]. Although these observations imply that lncRNAs can modulate numerous processes linked to CVDs including cell proliferation, endothelial function, lipid metabolism, and inflammation, comprehensive information on endothelial lncRNAs regulated by oxLDL was missing.
Therefore, for investigating the outcome of oxLDL treatment on endothelial cell transcriptome, we performed lncRNA and mRNA microarray analysis on total RNA isolated from oxLDL-stimulated HUVECs. We identified novel lncRNAs and target genes providing insights into the differential regulation of lncRNAs and mRNAs by oxLDL in endothelial cells. A total of 30,584 lncRNAs were screened, where 923 were notably up-regulated and 975 were appreciably down-regulated (P < 0.05) in response to oxLDL in HUVECs. In a total of 26,106 mRNAs screened, 518 were significantly up-regulated and 572 significantly down-regulated. The validation qPCR performed for 10 most up- and down-regulated lncRNAs showed similar trend for 7/10 up-regulated and 5/10 down-regulated lncRNAs (Table 2). The DE lncRNAs were dispersed over all the chromosomes, with maximum number identified for chromosome 1 (Fig. 2a, b). Majority of DE lncRNAs were intergenic in nature (Fig. 2c). Our data show that the first 20 lncRNAs with known target mRNA demonstrated a direct correlation in fold-change with its associated mRNA (Fig. 3). For most functional groups, it is challenging to predict the overall effects of oxLDL treatment on HUVECs, since a variety of genes with diverse functional roles were differentially regulated simultaneously. However, pathway analysis revealed that DE mRNAs up-regulated in response to oxLDL treatment are primarily involved in cytokine–cytokine receptor interface and pathways such as chemokine signaling, TNF signaling, and estrogen signaling (Table 3). The most down-regulated DE mRNAs are notably involved in olfactory transduction, MAPK signaling, Ras signaling, cytoskeletal actin regulation, and vascular smooth muscle contraction (Table 4). Interestingly, profile of the DE genes assessed in this study showed some similarities to other reports by Deng et al. and Minta et al. on DE genes in oxLDL-treated SMCs [43, 44]. Among the top 15 up-regulated genes, HMOX1 was up-regulated in both studies conducted in SMCs along with our study in HUVECs [43, 44]. In another study, oxLDL treatment in human coronary artery SMCs induced a gene regulation profile similar to the gene appearance pattern observed in the aortas of apoE−/− mice [45]. In accordance with Reeve et al. and Minta et al., our data also documented that oxLDL induces expression of NQO1 [NAD(P)H dehydrogenase quinone 1] not only in SMCs but also in endothelial cells [43, 45]. This understanding further backs the proposition that the effect of oxLDL on endothelial cell assumes great significance for the development of atherosclerosis. Results of bioinformatics GO analysis, as described in Table 5, grouped the DE mRNAs under the following three categories: Biological Processes, Cellular Component, and Molecular Function. GO terms most broadly associated with up-regulated DE mRNAs were in regulation of biological, extracellular space, and binding (Table 5). GO terms associated with down-regulated DE mRNA were mainly enriched in single-organism process, membrane, and carbohydrate derivative process (Table 5). This is the first lncRNA and mRNA transcriptome profile of oxLDL-mediated changes in human endothelial cells. To confirm that our data are not HUVEC-specific, we also treated HCAECs with oxLDL and performed qPCR for 10 most up- and down-regulated lncRNAs, which showed similar trend (Table 2).
Although interest in the contribution of lncRNAs to human health and disease is booming, the mechanism of action has only been pinpointed for a limited number of lncRNAs. Collaborative initiatives, such as the Encyclopedia of DNA Elements (ENCODE) project, aiming to recognize every functional element in the human genome are required [46]. However, the lack of defined functional motifs and regulatory regions and low expression levels of some lncRNAs are the major challenges. Majority of the lncRNAs are expressed as countless transcript alternates and the fact that they are poorly conserved challenges defining their specific biological roles and mechanisms of activity. Budding genomic, epigenomic, and bioinformatics approaches will be central in characterizing the lncRNAs. In order to avoid confusion and to facilitate the use and reproduction of the data, we have provided more detailed information (e.g., size, chromosomal localization, etc.) of oxLDL-associated DE lncRNAs in HUVECs. In our study, several lncRNAs were observed to be differentially regulated, which has not been stated before. Additional studies on novel genes reported in our study will offer first-hand cues regarding the mechanisms of CVD development by oxLDL. We conceive that our recent investigation further adds to the current understanding of the molecular mechanism of oxLDL-mediated endothelial cell dysfunction and apoptosis, and may provide targets for future therapeutic interventions against different CVDs including atherosclerosis.
Abbreviations
- ANRIL:
-
Antisense non-coding RNA in the INK4
- CVD:
-
Cardiovascular disease
- DE:
-
Differentially expressed
- ENCODE:
-
Encyclopedia of DNA Elements
- GO:
-
Gene ontology
- HDL:
-
High-density lipoprotein
- HLA-DPB1:
-
Major Histocompatibility Complex, Class II, DP Beta-1
- HUVECs:
-
Human umbilical vein endothelial cells
- KEGG:
-
Kyoto Encyclopedia of Genes and Genomes
- lncRNA:
-
Long non-coding RNAs
- MIAT:
-
Myocardial infarction-associated transcript
- miRNA:
-
MicroRNA
- ncRNA:
-
Non-coding RNAs
- NO:
-
Nitric oxide
- NQO1:
-
NAD(P)H dehydrogenase quinone 1
- O2 − :
-
Oxygen radical
- oxLDL:
-
Oxidized low-density lipoprotein
- piRNAs:
-
PIWI-interacting RNAs
- ROS:
-
Reactive oxygen species
- SMC:
-
Smooth muscle cell
- snoRNAs:
-
Small nucleolar RNAs
- t-UCRs:
-
Transcribed ultra-conserved regions
References
Hein TW, Singh U, Vasquez-Vivar J, Devaraj S, Kuo L, Jialal I (2009) Human C-reactive protein induces endothelial dysfunction and uncoupling of eNOS in vivo. Atherosclerosis 206:61–68. doi:10.1016/j.atherosclerosis.2009.02.002
Verma S, Wang CH, Li SH, Dumont AS, Fedak PW, Badiwala MV, Dhillon B, Weisel RD, Li RK, Mickle DA, Stewart DJ (2002) A self-fulfilling prophecy: C-reactive protein attenuates nitric oxide production and inhibits angiogenesis. Circulation 106:913–919
Jialal I, Verma S, Devaraj S (2009) Inhibition of endothelial nitric oxide synthase by C-reactive protein: clinical relevance. Clin Chem 55:206–208. doi:10.1373/clinchem.2008.119206
Hansson GK, Robertson AK, Soderberg-Naucler C (2006) Inflammation and atherosclerosis. Annu Rev Pathol 1:297–329. doi:10.1146/annurev.pathol.1.110304.100100
Szmitko PE, Wang CH, Weisel RD, Jeffries GA, Anderson TJ, Verma S (2003) Biomarkers of vascular disease linking inflammation to endothelial activation: Part II. Circulation 108:2041–2048. doi:10.1161/01.CIR.0000089093.75585.98
Szmitko PE, Wang CH, Weisel RD, de Almeida JR, Anderson TJ, Verma S (2003) New markers of inflammation and endothelial cell activation: Part I. Circulation 108:1917–1923. doi:10.1161/01.CIR.0000089190.95415.9F
Verma S, Anderson TJ (2002) Fundamentals of endothelial function for the clinical cardiologist. Circulation 105:546–549
Verma S, Buchanan MR, Anderson TJ (2003) Endothelial function testing as a biomarker of vascular disease. Circulation 108:2054–2059. doi:10.1161/01.CIR.0000089191.72957.ED
Steinberg D, Witztum JL (2010) Oxidized low-density lipoprotein and atherosclerosis. Arterioscler Thromb Vasc Biol 30:2311–2316. doi:10.1161/ATVBAHA.108.179697
Valente AJ, Irimpen AM, Siebenlist U, Chandrasekar B (2014) OxLDL induces endothelial dysfunction and death via TRAF3IP2: inhibition by HDL3 and AMPK activators. Free Radic Biol Med 70:117–128. doi:10.1016/j.freeradbiomed.2014.02.014
Davignon J and Ganz P (2004) Role of endothelial dysfunction in atherosclerosis. Circulation 109:III27-32. doi:10.1161/01.CIR.0000131515.03336.f8
Djebali S, Davis CA, Merkel A, Dobin A, Lassmann T, Mortazavi A, Tanzer A, Lagarde J, Lin W, Schlesinger F, Xue C, Marinov GK, Khatun J, Williams BA, Zaleski C, Rozowsky J, Roder M, Kokocinski F, Abdelhamid RF, Alioto T, Antoshechkin I, Baer MT, Bar NS, Batut P, Bell K, Bell I, Chakrabortty S, Chen X, Chrast J, Curado J, Derrien T, Drenkow J, Dumais E, Dumais J, Duttagupta R, Falconnet E, Fastuca M, Fejes-Toth K, Ferreira P, Foissac S, Fullwood MJ, Gao H, Gonzalez D, Gordon A, Gunawardena H, Howald C, Jha S, Johnson R, Kapranov P, King B, Kingswood C, Luo OJ, Park E, Persaud K, Preall JB, Ribeca P, Risk B, Robyr D, Sammeth M, Schaffer L, See LH, Shahab A, Skancke J, Suzuki AM, Takahashi H, Tilgner H, Trout D, Walters N, Wang H, Wrobel J, Yu Y, Ruan X, Hayashizaki Y, Harrow J, Gerstein M, Hubbard T, Reymond A, Antonarakis SE, Hannon G, Giddings MC, Ruan Y, Wold B, Carninci P, Guigo R, Gingeras TR (2012) Landscape of transcription in human cells. Nature 489:101–108. doi:10.1038/nature11233
Ulitsky I, Bartel DP (2013) lincRNAs: genomics, evolution, and mechanisms. Cell 154:26–46. doi:10.1016/j.cell.2013.06.020
Wang S, Tran EJ (2013) Unexpected functions of lncRNAs in gene regulation. Commun Integr Biol 6:e27610. doi:10.4161/cib.27610
Wapinski O, Chang HY (2011) Long noncoding RNAs and human disease. Trends Cell Biol 21:354–361. doi:10.1016/j.tcb.2011.04.001
Uchida S, Dimmeler S (2015) Long noncoding RNAs in cardiovascular diseases. Circ Res 116:737–750. doi:10.1161/CIRCRESAHA.116.302521
Wu CL, Wang Y, Jin B, Chen H, Xie BS, Mao ZB (2015) Senescence-associated Long Non-coding RNA (SALNR) Delays Oncogene-induced Senescence through NF90 Regulation. J Biol Chem 290:30175–30192. doi:10.1074/jbc.M115.661785
Han P, Li W, Lin CH, Yang J, Shang C, Nurnberg ST, Jin KK, Xu W, Lin CY, Lin CJ, Xiong Y, Chien HC, Zhou B, Ashley E, Bernstein D, Chen PS, Chen HS, Quertermous T, Chang CP (2014) A long noncoding RNA protects the heart from pathological hypertrophy. Nature 514:102–106. doi:10.1038/nature13596
Vausort M, Wagner DR, Devaux Y (2014) Long noncoding RNAs in patients with acute myocardial infarction. Circ Res 115:668–677. doi:10.1161/CIRCRESAHA.115.303836
Vilsboll T, Rosenstock J, Yki-Jarvinen H, Cefalu WT, Chen Y, Luo E, Musser B, Andryuk PJ, Ling Y, Kaufman KD, Amatruda JM, Engel SS, Katz L (2010) Efficacy and safety of sitagliptin when added to insulin therapy in patients with type 2 diabetes. Diabetes Obes Metab 12:167–177. doi:10.1111/j.1463-1326.2009.01173.x
Michalik KM, You X, Manavski Y, Doddaballapur A, Zornig M, Braun T, John D, Ponomareva Y, Chen W, Uchida S, Boon RA, Dimmeler S (2014) Long noncoding RNA MALAT1 regulates endothelial cell function and vessel growth. Circ Res 114:1389–1397. doi:10.1161/CIRCRESAHA.114.303265
Holdt LM, Hoffmann S, Sass K, Langenberger D, Scholz M, Krohn K, Finstermeier K, Stahringer A, Wilfert W, Beutner F, Gielen S, Schuler G, Gabel G, Bergert H, Bechmann I, Stadler PF, Thiery J, Teupser D (2013) Alu elements in ANRIL non-coding RNA at chromosome 9p21 modulate atherogenic cell functions through trans-regulation of gene networks. PLoS Genet 9:e1003588. doi:10.1371/journal.pgen.1003588
Lund-Katz S, Phillips MC (2010) High density lipoprotein structure-function and role in reverse cholesterol transport. Subcell Biochem 51:183–227. doi:10.1007/978-90-481-8622-8_7
Singh KK, Matkar PN, Quan A, Mantella L-E, Teoh H, Al-Omran M, Verma S (2016) Investigation of TGFbeta1-induced long noncoding RNAs in endothelial cells. Int J Vasc Med 2016:2459687. doi:10.1155/2016/2459687
Singh KK, Mantella L-E, Pan Y, Quan A, Sabonguia S, Sandhu P, Teoh H, Al-Omran M, verma S (2016) A global profile of glucose-sensitive endothelial-expressed long non-coding RNAs. Can J Physiol Pharmacol 94:1007–1014
Toshima S, Hasegawa A, Kurabayashi M, Itabe H, Takano T, Sugano J, Shimamura K, Kimura J, Michishita I, Suzuki T, Nagai R (2000) Circulating oxidized low density lipoprotein levels. A biochemical risk marker for coronary heart disease. Arterioscler Thromb Vasc Biol 20:2243–2247
Goldstein JL, Brown MS, Krieger M, Anderson RG, Mintz B (1979) Demonstration of low density lipoprotein receptors in mouse teratocarcinoma stem cells and description of a method for producing receptor-deficient mutant mice. Proc Natl Acad Sci U S A 76:2843–2847
Penn MS and Chisolm GM (1994) Oxidized lipoproteins, altered cell function and atherosclerosis. Atherosclerosis 108 :S21–S29
Chisolm GM, Ma G, Irwin KC, Martin LL, Gunderson KG, Linberg LF, Morel DW, DiCorleto PE (1994) 7 beta-hydroperoxycholest-5-en-3 beta-ol, a component of human atherosclerotic lesions, is the primary cytotoxin of oxidized human low density lipoprotein. Proc Natl Acad Sci U S A 91:11452–11456
Morel DW, Hessler JR, Chisolm GM (1983) Low density lipoprotein cytotoxicity induced by free radical peroxidation of lipid. J Lipid Res 24:1070–1076
Blair A, Shaul PW, Yuhanna IS, Conrad PA, Smart EJ (1999) Oxidized low density lipoprotein displaces endothelial nitric-oxide synthase (eNOS) from plasmalemmal caveolae and impairs eNOS activation. J Biol Chem 274:32512–32519
Singh KK, Shukla PC, Quan A, Al-Omran M, Lovren F, Pan Y, Brezden-Masley C, Ingram AJ, Stanford WL, Teoh H, Verma S (2013) BRCA1 is a novel target to improve endothelial dysfunction and retard atherosclerosis. J Thorac Cardiovasc Surg 146(949–960):e4. doi:10.1016/j.jtcvs.2012.12.064
Cominacini L, Rigoni A, Pasini AF, Garbin U, Davoli A, Campagnola M, Pastorino AM, Lo Cascio V, Sawamura T (2001) The binding of oxidized low density lipoprotein (ox-LDL) to ox-LDL receptor-1 reduces the intracellular concentration of nitric oxide in endothelial cells through an increased production of superoxide. J Biol Chem 276:13750–13755. doi:10.1074/jbc.M010612200
Li D, Mehta JL (2000) Upregulation of endothelial receptor for oxidized LDL (LOX-1) by oxidized LDL and implications in apoptosis of human coronary artery endothelial cells: evidence from use of antisense LOX-1 mRNA and chemical inhibitors. Arterioscler Thromb Vasc Biol 20:1116–1122
Salvayre R, Auge N, Benoist H, Negre-Salvayre A (2002) Oxidized low-density lipoprotein-induced apoptosis. Biochim Biophys Acta 1585:213–221
Trpkovic A, Resanovic I, Stanimirovic J, Radak D, Mousa SA, Cenic-Milosevic D, Jevremovic D, Isenovic ER (2015) Oxidized low-density lipoprotein as a biomarker of cardiovascular diseases. Crit Rev Clin Lab Sci 52:70–85. doi:10.3109/10408363.2014.992063
Bjorkbacka H, Fredrikson GN, Nilsson J (2013) Emerging biomarkers and intervention targets for immune-modulation of atherosclerosis—a review of the experimental evidence. Atherosclerosis 227:9–17. doi:10.1016/j.atherosclerosis.2012.10.074
Galle J, Hansen-Hagge T, Wanner C, Seibold S (2006) Impact of oxidized low density lipoprotein on vascular cells. Atherosclerosis 185:219–226. doi:10.1016/j.atherosclerosis.2005.10.005
Di Pietro N, Formoso G, Pandolfi A (2016) Physiology and pathophysiology of oxLDL uptake by vascular wall cells in atherosclerosis. Vascul Pharmacol. doi:10.1016/j.vph.2016.05.013
Kotake Y, Nakagawa T, Kitagawa K, Suzuki S, Liu N, Kitagawa M, Xiong Y (2011) Long non-coding RNA ANRIL is required for the PRC2 recruitment to and silencing of p15(INK4B) tumor suppressor gene. Oncogene 30:1956–1962. doi:10.1038/onc.2010.568
McPherson R, Pertsemlidis A, Kavaslar N, Stewart A, Roberts R, Cox DR, Hinds DA, Pennacchio LA, Tybjaerg-Hansen A, Folsom AR, Boerwinkle E, Hobbs HH, Cohen JC (2007) A common allele on chromosome 9 associated with coronary heart disease. Science 316:1488–1491. doi:10.1126/science.1142447
Ishii N, Ozaki K, Sato H, Mizuno H, Saito S, Takahashi A, Miyamoto Y, Ikegawa S, Kamatani N, Hori M, Saito S, Nakamura Y, Tanaka T (2006) Identification of a novel non-coding RNA, MIAT, that confers risk of myocardial infarction. J Hum Genet 51:1087–1099. doi:10.1007/s10038-006-0070-9
Minta J, Jungwon Yun J, St Bernard R (2010) Microarray analysis of ox-LDL (oxidized low-density lipoprotein)-regulated genes in human coronary artery smooth muscle cells. Cell Biol Int Rep 17:e00007. doi:10.1042/CBR20100006
Deng DX, Spin JM, Tsalenko A, Vailaya A, Ben-Dor A, Yakhini Z, Tsao P, Bruhn L, Quertermous T (2006) Molecular signatures determining coronary artery and saphenous vein smooth muscle cell phenotypes: distinct responses to stimuli. Arterioscler Thromb Vasc Biol 26:1058–1065. doi:10.1161/01.ATV.0000208185.16371.97
Reeve JL, Stenson-Cox C, O’Doherty A, Porn-Ares I, Ares M, O’Brien T, Samali A (2007) OxLDL-induced gene expression patterns in CASMC are mimicked in apoE-/- mice aortas. Biochem Biophys Res Commun 356:681–686. doi:10.1016/j.bbrc.2007.03.027
Encode Project Consortium, Birney E, Stamatoyannopoulos JA, Dutta A, Guigo R, Gingeras TR, Margulies EH, Weng Z, Snyder M, Dermitzakis ET, Thurman RE, Kuehn MS, Taylor CM, Neph S, Koch CM, Asthana S, Malhotra A, Adzhubei I, Greenbaum JA, Andrews RM, Flicek P, Boyle PJ, Cao H, Carter NP, Clelland GK, Davis S, Day N, Dhami P, Dillon SC, Dorschner MO, Fiegler H, Giresi PG, Goldy J, Hawrylycz M, Haydock A, Humbert R, James KD, Johnson BE, Johnson EM, Frum TT, Rosenzweig ER, Karnani N, Lee K, Lefebvre GC, Navas PA, Neri F, Parker SC, Sabo PJ, Sandstrom R, Shafer A, Vetrie D, Weaver M, Wilcox S, Yu M, Collins FS, Dekker J, Lieb JD, Tullius TD, Crawford GE, Sunyaev S, Noble WS, Dunham I, Denoeud F, Reymond A, Kapranov P, Rozowsky J, Zheng D, Castelo R, Frankish A, Harrow J, Ghosh S, Sandelin A, Hofacker IL, Baertsch R, Keefe D, Dike S, Cheng J, Hirsch HA, Sekinger EA, Lagarde J, Abril JF, Shahab A, Flamm C, Fried C, Hackermuller J, Hertel J, Lindemeyer M, Missal K, Tanzer A, Washietl S, Korbel J, Emanuelsson O, Pedersen JS, Holroyd N, Taylor R, Swarbreck D, Matthews N, Dickson MC, Thomas DJ, Weirauch MT, Gilbert J, Drenkow J, Bell I, Zhao X, Srinivasan KG, Sung WK, Ooi HS, Chiu KP, Foissac S, Alioto T, Brent M, Pachter L, Tress ML, Valencia A, Choo SW, Choo CY, Ucla C, Manzano C, Wyss C, Cheung E, Clark TG, Brown JB, Ganesh M, Patel S, Tammana H, Chrast J, Henrichsen CN, Kai C, Kawai J, Nagalakshmi U, Wu J, Lian Z, Lian J, Newburger P, Zhang X, Bickel P, Mattick JS, Carninci P, Hayashizaki Y, Weissman S, Hubbard T, Myers RM, Rogers J, Stadler PF, Lowe TM, Wei CL, Ruan Y, Struhl K, Gerstein M, Antonarakis SE, Fu Y, Green ED, Karaoz U, Siepel A, Taylor J, Liefer LA, Wetterstrand KA, Good PJ, Feingold EA, Guyer MS, Cooper GM, Asimenos G, Dewey CN, Hou M, Nikolaev S, Montoya-Burgos JI, Loytynoja A, Whelan S, Pardi F, Massingham T, Huang H, Zhang NR, Holmes I, Mullikin JC, Ureta-Vidal A, Paten B, Seringhaus M, Church D, Rosenbloom K, Kent WJ, Stone EA, Program NCS, Baylor College of Medicine Human Genome Sequencing C, Washington University Genome Sequencing C, Broad I, Children’s Hospital Oakland Research I, Batzoglou S, Goldman N, Hardison RC, Haussler D, Miller W, Sidow A, Trinklein ND, Zhang ZD, Barrera L, Stuart R, King DC, Ameur A, Enroth S, Bieda MC, Kim J, Bhinge AA, Jiang N, Liu J, Yao F, Vega VB, Lee CW, Ng P, Shahab A, Yang A, Moqtaderi Z, Zhu Z, Xu X, Squazzo S, Oberley MJ, Inman D, Singer MA, Richmond TA, Munn KJ, Rada-Iglesias A, Wallerman O, Komorowski J, Fowler JC, Couttet P, Bruce AW, Dovey OM, Ellis PD, Langford CF, Nix DA, Euskirchen G, Hartman S, Urban AE, Kraus P, Van Calcar S, Heintzman N, Kim TH, Wang K, Qu C, Hon G, Luna R, Glass CK, Rosenfeld MG, Aldred SF, Cooper SJ, Halees A, Lin JM, Shulha HP, Zhang X, Xu M, Haidar JN, Yu Y, Ruan Y, Iyer VR, Green RD, Wadelius C, Farnham PJ, Ren B, Harte RA, Hinrichs AS, Trumbower H, Clawson H, Hillman-Jackson J, Zweig AS, Smith K, Thakkapallayil A, Barber G, Kuhn RM, Karolchik D, Armengol L, Bird CP, de Bakker PI, Kern AD, Lopez-Bigas N, Martin JD, Stranger BE, Woodroffe A, Davydov E, Dimas A, Eyras E, Hallgrimsdottir IB, Huppert J, Zody MC, Abecasis GR, Estivill X, Bouffard GG, Guan X, Hansen NF, Idol JR, Maduro VV, Maskeri B, McDowell JC, Park M, Thomas PJ, Young AC, Blakesley RW, Muzny DM, Sodergren E, Wheeler DA, Worley KC, Jiang H, Weinstock GM, Gibbs RA, Graves T, Fulton R, Mardis ER, Wilson RK, Clamp M, Cuff J, Gnerre S, Jaffe DB, Chang JL, Lindblad-Toh K, Lander ES, Koriabine M, Nefedov M, Osoegawa K, Yoshinaga Y, Zhu B, de Jong PJ (2007) Identification and analysis of functional elements in 1% of the human genome by the ENCODE pilot project. Nature 447:799–816. doi:10.1038/nature05874
Acknowledgements
This work was supported by in part by grants from the Canadian Institutes of Health Research and Heart and Stroke Foundation of Canada to S. Verma. S. Verma is the Canada Research Chair in Atherosclerosis at the University of Toronto.
Authors’ contributions
KKS and SV designed the studies and the experiments. KKS, PNM, YP, AQ, and VG conducted the experiments. KKS drafted the manuscript. KKS, AQ, HT, MAO, and SV interpreted the data and critically edited the manuscript. All authors read and approved the final manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Singh, K.K., Matkar, P.N., Pan, Y. et al. Endothelial long non-coding RNAs regulated by oxidized LDL. Mol Cell Biochem 431, 139–149 (2017). https://doi.org/10.1007/s11010-017-2984-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-017-2984-2