Abstract
This study assessed the influence of different physical and psychological illnesses on life satisfaction in individuals. A nationally representative sample (N = 2,966) of non-institutionalized Spanish adults between the ages of 18 and 65 years completed a self-report measure on treated physical and psychological problems as well as a measure of overall life satisfaction. The results showed that although physical and psychological problems both had an impact on life satisfaction, greater effect sizes were generally found for psychological rather than for physical illness. Regression analysis, which controlled for the effects of comorbidity and sociodemographic variables (e.g. age, gender, marital status, employment status, and education level), revealed a significant impact on life satisfaction in cancer and migraine (in the domain of physical problems), and in depression, lack of concentration, insomnia, and stress/anxiety (in the domain of psychological problems). Further multivariate analyses were conducted to estimate decreases in the Satisfaction With Life Scale for each of the conditions assessed. A lack of significant interactions revealed that the effect of comorbid physical and/or psychological problems could be additive. The present results show that people who are afflicted with psychological problems exhibit a marked decrease in life satisfaction. As a whole, this negative impact is significantly greater than the decrease associated with physical problems.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
The importance of measuring constructs of psychological well-being as a criterion variable has been stressed in the field of economics (Layard 2010). Traditionally, the impact of health problems on the performance of the healthcare system has been analyzed in terms of their economic cost in an attempt to guide public health policies (Blanchflower and Oswald 2004; Ferrer-i-Carbonell et al. 2002). Yet, in relation to the physical or psychological health of the general population, a benefit-cost system based on units of subjective well-being can provide better measures of policy effectiveness (Forward Scotland and Scottish Council Foundation 2008; Layard 2010; Veenhoven 2008). Consequently, examining the specific impact of different diseases on well-being becomes essential. The present study aims to explore an array of self-reported physical and psychological problems in a nationally representative sample and their consequences in terms of decreases in life satisfaction.
It is now a well-established fact that many different psychological and physical problems can affect individuals’ functioning (Ganev 2000; Murray and Lopez 1996; Ustun et al. 1999). The personal and social costs of these conditions can be assessed by measuring their impact on life expectancy and their quality of life (QoL) (Funk et al. 2010; Lopez et al. 2006; Mathers and Loncar 2006; Williams 1999). One of the first major sources of data on the impact of diseases was the World Health Organization (WHO) Global Burden of Disease Study (GBDS) (Murray and Lopez 1996). The GBDS uses a measure of disability-adjusted life years (DALYs), which includes years of life lost due to premature mortality and years lived with disability, adjusted for the severity of each disease. Based on these metrics, the GBDS has shown that the burden of diseases can vary greatly.
One of the novel findings of the GBDS was that mental illnesses have a significant impact on individuals’ functionality in addition to physical illnesses. In fact, four psychiatric disorders appeared among the 10 leading causes of disability: unipolar depressive disorders, schizophrenia, alcohol abuse disorder, and bipolar disorder (Ustun et al. 2004). Moreover, recent analyses, comparing results for 1990 and 2010, show the total burden of mental and substance use disorders increased by 37.6 % in that period, and, specifically, the burden of these disorders as a proportion of all-cause DALYs increased from 5.4 % in 1990 to 7.4 % in 2010 (Whiteford et al. 2013). Thus, while traditionally not regarded as a major public health concern, disability due to psychological or behavioral problems has a significant impact on populations. Poor mental health status also has additional costs that go beyond the impact of the mental disorder itself, for example, by increasing susceptibility to physical illness (Prince et al. 2007).
The impact of physical and psychological problems has been supported by empirical studies of QoL. These studies have clearly demonstrated that psychological and physical problems affect daily functioning (Graham et al. 2011; Pirkola et al. 2009). However, apart from a few exceptions (Bruffaerts et al. 2012; Merikangas et al. 2007; Pinto-Meza et al. 2009), studies have not attempted to compare the impact of both physical and psychological illnesses on QoL and functionality. This poses a significant limitation since the relationship between a specific condition (e.g. cancer) and life satisfaction could be due to the presence of a comorbidity (e.g. depression). Hence, it is only by studying the impact of physical and psychological diseases simultaneously that potential confounders can be removed to reach solid conclusions.
In general, previous research that has explored the impact of health problems on QoL face several limitations. For example, most evidence on the relationship between QoL and health is derived from studies with nonrepresentative samples (Diener and Chan 2011) or from those focused on specific disorders such as hypertension (Bardage and Isacson 2001), obesity (Jian and Lubetkin 2005), or depression (Saarni et al. 2007). Further, although items related to psychological well-being are commonly included in QoL measures (Lehman 1988), scores on these items are rarely reported in detail. Moreover, many studies have utilized single items of limited reliability (Bergsma et al. 2010; Oswald and Powdthavee 2007) or have relied on scales measuring subjective overall health status rather than specific illnesses (Graham et al. 2011).
To our knowledge, there are no national studies that have directly addressed the relationship between life satisfaction and physical and psychological problems simultaneously in the same study. The present study aims to fill this gap by exploring an array of representative self-reported physical and psychological problems in a nationally representative sample. To assess the impact of these disorders on well-being, we selected the Satisfaction With Life Scale (SWLS), as it has been shown to be sensitive in detecting the impact of different living conditions on psychological well-being (Diener et al. 2012).
2 Methods
2.1 Participants
This is a population-based study of the non-institutionalized adult population of Spain aged 18–65 years which is estimated at 29.3 million (Instituto Nacional de Estadística 2010). Individuals gave informed consent to participate. A stratified, multi-stage, clustered design was used, based on the political regions in Spain, to obtain a nationally representative sample. A probability proportion to size design was used to select clusters. The sample included quotas for gender, age, and socioeconomic status within these regions according to data from the 2006 national census (INE 2010). A survey firm (Millward Brown) carried out the fieldwork from May to July of 2007. After the deletion of cases with incomplete data (1.1 %), the sample included in the analysis consisted of 2,966 participants. The demographic characteristics of the sample are reported in Table 1.
2.2 Procedure
Participants were individually contacted at their place of residence by one of 121 trained interviewers. In the first interview, participants were asked sociodemographic questions about socioeconomic status and education level. After this initial contact, a booklet containing several self-report measures, including the SWLS, and a series of questions related to perceived physical and psychological health were given to participants. Interviewers returned to participants’ homes within 2 weeks to collect the questionnaires. At this time, participants were compensated for their involvement in the study.
2.3 Instruments
2.3.1 Satisfaction with Life
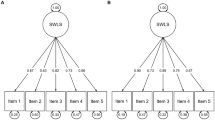
The five-item SWLS (Pavot and Diener 1993) was used to assess general life satisfaction. Individuals were asked to rate their degree of agreement with each item on a 7-point Likert scale, from “absolutely disagree” to “absolutely agree”. Scores on this scale range from 5 to 35 points. Higher scores indicate higher levels of life satisfaction. Previous research has shown that Cronbach’s alphas range from .79 to .89 (Pavot and Diener 2008). We used the Spanish version of the scale which has shown very good reliability and validity (Vázquez et al. 2013). The scale showed high reliability (α = .88) in the present study.
2.3.2 Physical and Psychological Health
To assess physical and psychological health, participants responded to items covering twelve physical and nine psychological problems. This was similar to the self-report procedure used in the European Study of the Epidemiology of Mental Disorders (ESEMeD) (Pirkola et al. 2009). Participants used a yes/no format to indicate whether they were currently suffering from each problem and, if so, whether they were receiving treatment for it. Physical problems included in the questionnaire were diabetes, cardiovascular events, obesity, respiratory problems, cancer, stomachache, backache, rheumatism, osteoporosis, migraine/headaches, motor disability, and sensory disability. Psychological difficulties included in the questionnaire were anorexia, bulimia, concentration problems, insomnia, stress/anxiety, depression, neuropsychiatric problems, sexual dysfunction, and addictions.
2.3.3 Data Analysis
Data were weighted to account for the sampling design and to generalize the results obtained in the study sample to the Spanish population. All statistical analyses were conducted incorporating the sample weights using Stata version 11 (StataCorp 2010) and the Stata’s survey command (svy), which fits statistical models for complex survey data. Confidence intervals (CI) were constructed at the 95 % CI. The results section is divided into two sub-sections, with each one containing different analyses according to the questions addressed.
In the first subsection, the mean SWLS score of the healthy group (i.e. participants who did not report any physical or psychological condition, N = 1,411) was compared with with the mean SWLS score of people who suffered from a physical or psychological problem. Comparisons between the healthy control group and each subgroup of people with a given problem were conducted using unpaired t-tests for weighted data. Cohen’s d was reported as effect size measure. Cohen’s guidelines (Cohen 1988) were employed as standard to evaluate the magnitude of the effect size: Cohen’s d values of .20, .50, and .80 constitute small, medium, and large effect sizes, respectively.
In the second subsection, a hierarchical regression analysis was conducted to assess the relationships between each physical or mental disorder assessed in the survey with total SWLS scores, controlling for sociodemographic characteristics: age group (0 = 18–25; 1 = 26–35; 2 = 36–45; 3 = 46–55; and 4 = 56+ years, considering 18–25 years as the reference category), gender (0 = male, 1 = female), marital status (0 = married or in partnership, 1 = no), current employment status (0 = yes, 1 = no), and education level (0 = baccalaureate or higher education, 1 = rest of the categories).
The dependent variable was SWLS score. The first block was composed by sociodemographic characteristics, while the second one was composed by physical and mental disorders. The increase in the proportion of variance explained (increase in the adjusted R 2) was tested when the second block was added, by means of the difference in the likelihood ratio Chi square for each model, which tested the null hypothesis that the second block of predictors contributed nothing beyond the set of sociodemographic variables entered in the model at the first step. The ordinary least squares (OLS) estimation was employed; the use of OLS trades robustness for some improvement in efficiency (Buntin and Zaslavsky 2004) and has been shown to yield the best fit of data (Alonso et al. 2011). Heteroskedasticity was assessed using White’s General Test for Heteroskedasticity in the error distribution (White 1980), which regressed the squared residuals on all distinct regressors, cross-products, and squares of regressors. The presence of multicollinearity in the multiple regression model was assessed by means of the variance inflation factor (VIF). Values below 10 (and in some cases, 5) have traditionally been considered adequate in the literature.
For descriptive purposes, an index for the estimated individual-level effect of each disorder on the SWLS score was obtained employing the methodology proposed by Alonso et al. (2011), which takes into account the possible combinations of comorbid disorders. This statistical control is important as population-based studies have found that physical problems (e.g. arthritis, back pain, and migraine) are associated with psychological problems (mostly depression and anxiety) (Scott et al. 2007; Pinto-Meza et al. 2009; El-Gabalawy et al. 2011). Given that the number of possible combinations of comorbid disorders in the data (221 − 22 = 2,097,130) far exceeds the number of respondents, it was necessary to impose some structure on the terms used to capture the effects of comorbidity. For this purpose, two-way interaction terms corresponding to the total number of comorbid disorders, as well as each of them individually, were included in the model. As the prediction equation includes interaction terms, the predictive effect of each disorder is distributed across a number of different coefficients. To summarize all of the component effects into a single term, the percentage of variation of mean SWLS score for each disorder was obtained. This was achieved by estimating the predictive value of the outcome for each respondent using the coefficients in the final model and then repeating this exercise in a modified form at 21 different times, with each instance assuming that one of the 21 disorders no longer existed. The percentage of variation of mean SWLS scores was calculated as the difference between the predictions of the basal and simulated models in each of the 21 cases. This percentage can be interpreted as the variation in SWLS scores attributable to each disorder. A positive percentage indicates that the mean SWLS score is higher in the simulated model, and thus, the disorder has a negative effect over the SWLS score.
Final analyses were carried out considering the two-way interaction terms that corresponded to the variables found to be significant in the previous regression model, excluding disorders with small number of cases. Pairwise interaction terms between the disorders with a significant main effect in the regression model were included as a third block in the hierarchical regression model, keeping the sociodemographic variables in the first block, and the physical and mental disorders in the second one.
3 Results
3.1 Effect of Physical and Psychological Problems on SWLS Scores
Mean estimate SWLS scores of participants who reported each one of the physical or psychological problems were compared with the mean estimate SWLS score of the healthy control group [Mean estimate score = 25.08, 95 % CI = (24.81, 25.35)]. Significant differences in SWLS scores were found between the healthy control group and participants reporting physical problems (Table 2), as well as between the healthy control group and participants reporting psychological problems (Table 3). Anorexia and bulimia were excluded from analyses because the number of incidences of these conditions was very low.
As shown in Tables 2 and 3, most physical and psychological problems were associated with lower mean estimated SWLS scores than those observed in the healthy control group. In general, Cohen’s effect sizes were higher for psychological than for physical problems; mean Cohen’s d was .76 (SD = .34) for mental disorders and .52 (SD = .23) for physical disorders.
3.2 Multiple Regression Analyses. Comparison Between Simulated and Basal Models
The final hierarchical regression model, which took all participants into consideration, showed an adequate fit [F(27, 2938) = 12.96, p < .001; RMSE = 5.40]. The adjusted R 2 value was .12. The result of White’s General Test for Heteroskedasticity [χ2 (341) = 371.34; p = .12] suggested that the error term could be homoskedastic as it remained constant across observations. All of the variables considered in the model had an associated VIF value lower than 2 and a mean VIF of 1.25.
In Table 4, the results corresponding to the second block of the hierarchical regression model are shown. The analysis was controlled for sociodemographics, which were included in the first block of the model. Being married or in a partnership (|β| = .18; p < .001), and being of a higher educational level (|β| = .09; p < .001) were associated with a higher SWLS score in the model. In contrast, depression, concentration problems, stress/anxiety, insomnia, and migraine/headaches were significantly related to lower levels of satisfaction with life; moreover, the effect of cancer was marginally significant, while the effect of rheumatism in the SWLS score was found significant although positive. A significant increase in the percentage of variance was observed when the physical and mental conditions were added to the model [ΔR 2 = .08; F(19, 2,938) = 14.11, p < .001].
In regards to significant predictors in the previous model, Table 4 also shows that cancer, depression, concentration problems, and insomnia had a greater attributable effect on the variation in SWLS score. Age, gender, marital status, employment status, and education level were controlled for in these analyses. The variation in mean SWLS scores represents the percentage of variation in mean scores between the simulated and the final model. A positive percentage indicates that the mean SWLS score in subjects with each disease is higher in the simulated model, implying that the disease has a negative effect on the SWLS score.
3.3 Multiple Regression Analyses. Testing for Interactions
Two-way interaction terms which included pairwise variables with a significant main effect (rheumatism, migraine/headaches, concentration problems, insomnia, stress/anxiety, and depression) were introduced as a third block in the hierarchical regression model. The increase in the percentage of variance explained was not significant when this third block was added [ΔR 2 = .01; F(15, 2,923) = 1.17, p = .29]. Cancer (β = − .04, p = .028), migraine/headaches (β = − .05, p = .024), concentration problems (β = − .09, p = .009), insomnia (β = − .11, p = .002), stress/anxiety (β = − .07, p = .007), and depression (β = − .10, p = .005), had a significant and negative impact on SWLS scores at a 95 % confidence level. The paradoxical effect of rheumatism increasing the SWLS score, as shown in Table 4, was not already significant in this analysis (β = .04; p = .10). However, more importantly, none of the 15 interaction terms in this model were found to be significant; only a marginally significant effect for the interaction between migraine/headaches and insomnia was found (p = .07). These results are available upon request.
4 Discussion
In the present study, we analyzed the influence of physical and psychological problems on life satisfaction. The results suggested that both physical and psychological problems have a significant impact on life satisfaction as measured by the SWLS, which is a widely used and psychometrically sound measure. With regards to psychological problems, depression, difficulties with concentration, anxiety/stress, and insomnia independently predicted unique variance in life satisfaction. These findings are in line with those of previous studies that have shown that symptoms of depression and anxiety are associated with decreased subjective QoL (Bow-Thomas et al. 1999; Graham et al. 2011; Ho et al. 1998; Lam and Rosenheck 2000; Narvaez et al. 2008; Ruggeri et al. 2001) and quality-adjusted life-years (Saarni et al. 2007) in both clinical and general populations. Our findings also support those of a study conducted in a Dutch national representative sample by Bergsma et al. (2010). The authors found that individuals with mental disorders (namely mood/anxiety and alcohol/drug abuse or dependency) have significantly lower levels of happiness and satisfaction with their life (in this case, measured with a single item) versus their healthy counterparts.
With regards to physical problems, cancer and migraine/headache independently accounted for reductions in levels of life satisfaction. However, diabetes, respiratory problems, stomachache, and osteoporosis did not appear to be predictive of life satisfaction when regression analyses were conducted. Our results are also consistent with research that has shown that patients with mental disorders, such as depression or schizophrenia, may generally experience a lower QoL than those with chronic physical diseases (Bonicatto et al. 2001; Tsuang and Winokur 1975). However, it is important to note that cancer showed the highest impact out of all the problems we assessed for in our study. One strength of our study was the use of the well-established SWLS to reliably capture and measure the construct of life satisfaction (Diener et al. 2012). Other well-known studies that have been conducted in the general population have typically used a single item to assess life satisfaction (Deaton 2008; Oswald and Wu 2010; Strine et al. 2008). Another strength of this study was its use of a nationally representative sample. We drew on such a sample in order to examine the overall effects of a wide array of psychological and physical problems on individuals’ life satisfaction. The advanced method we used allowed us to derive an objective index of the reduction in life satisfaction that was specifically attributable to each problem after controlling for the effects of comorbidities and sociodemographic variables. These indexes could be useful for weighing the direct impact of different problems on life satisfaction in future studies, as this has not yet been assessed. Since no significant interactions were found we can conclude that the effect of comorbid physical and/or psychological problems on life satisfaction is additive. Thus, when estimating the magnitude of the drop in SWLS score as an effect of a combination of two problems, the estimated decreases in SWLS score for each of the two problems should be added. A similar lack of interaction between physical and mental conditions has also been reported in Pinto-Meza et al. (2009) study using a large sample of primary care patients. In that study, the authors found that, with the exception of an interaction between chronic pain and mood disorders, the effects of physical or psychological problems on QoL were independent from each other.
Despite its strengths, the study has several limitations. First, it could be argued that the selection of disorders covered in our study could have been wider. Nevertheless, it is important to note that the spectrum of physical and psychological problems included in our study was similar to those examined in other national and international representative studies (e.g. Alonso et al. 2004; Merikangas et al. 2007). Secondly, as this is a cross-sectional study, it does not adequately address causal pathways between self-reported health status and life satisfaction. Although our results are consistent with findings that health problems have a direct impact on satisfaction with life, the relationship may also work in reverse (Chida and Steptoe 2008; Pressman and Cohen 2005; Veenhoven 2008). In fact, a recent meta-analysis showed that psychological well-being, including happiness, life satisfaction, and positive affect, may have a causal effect on several objective parameters of health (Howell et al. 2007). This bidirectionality is important since positive moods (e.g. happiness, contentment), positive traits (e.g. optimism, extraversion), and life satisfaction have been associated with decreased mortality risk and improved health (Friedman et al. 1993; Hampson et al. 2006; Howell et al. 2007; Lyubomirsky et al. 2005; Pressman and Cohen 2005; Ryff and Singer 1998). Thirdly, the model we tested failed to include other theoretically relevant predictors of SWLS, such as neuroticism and extraversion, which may have altered the estimated effects of health variables on life satisfaction. Another limitation is that, due to the the analytic method employed in our study (see Alonso et al. 2011), the percentage of variation in the SWLS can be influenced, at the same time, by the main effect of the disorder and the term of interaction between the total number of chronic conditions (in which the disorder is also included). Finally, all our data were based on self-reported information and we did not use physiological measures or objective physical outcomes to assess for medical problems. It is possible that self-reports may have been confounded by a third variable, such as neuroticism. However, it should be noted that self-reports on health status are the most common source of information in large samples and are considered to be a valid assessment tool (Gravelle and Sutton 2006; Lubeck and Hubert 2005; Moriarty et al. 2003; Ritter et al. 2001).
It is now widely accepted that health-related problems pose an enormous economic and personal burden on the general population (Bruffaerts et al. 2012; Mathers and Loncar 2006; WHO 2009; Graham et al. 2011). Our findings show that they also bear a toll on life satisfaction. This is timely in light of a global trend to supplement traditional economic indicators with measures of well-being, not only to address health issues (Oswald and Powdthavee 2007), but to also assess a society’s development and to guide policymaking (Bok 2010; Diener et al. 2009; Dolan and White 2007; Forward Scotland and Scottish Council Foundation 2008; Grossi et al. 2012; Heliwell et al. 2012; Stiglitz et al. 2009). Therefore, studies of well-being could contribute to more efficaceous distributions of resources devoted to healthcare in our societies. Funding for mental health prevention and treatment should especially be emphasized, given that cost-effective interventions already exist (Chisholm et al. 2007).
Regardless of the causal direction between psychological and behavioral problems and life satisfaction, the present results clearly show that people who are afflicted with psychological problems exhibit a marked decrease in life satisfaction. As a whole, this negative impact is significantly greater than the decrease associated with physical problems and should be taken into account by healthcare institutions and reflected in policies. Generally, our results may be helpful in the process of implementing a cost-benefit system based on well-validated units of subjective well-being (Diener et al. 2012) in the domain of healthcare policymaking (Forward Scotland and Scottish Council Foundation 2008; Layard 2010).
References
Alonso, J., Ferrer, M., Gandek, B., Ware, J. E., Aaronson, N. K., Mosconi, P., et al. (2004). Health-related quality of life associated with chronic conditions in eight countries: Results from the International Quality of Life Assessment (IQOLA Project). Quality of Life Research, 13, 283–298.
Alonso, J., Petukhova, M., Vilagut, G., Chatterji, S., Heeringa, S., Üstün, T. B., et al. (2011). Days out of role due to common physical and mental conditions: Results from the WHO World Mental Health surveys. Molecular Psychiatry, 16, 1234–1246.
Bardage, C., & Isacson, D. (2001). Hypertension and health-related quality of life: An epidemiological study in Sweden. Journal of Clinical Epidemiology, 54, 172–181.
Bergsma, A., Veenhoven, R., Have, M., & Graaf, R. (2010). Do they know how happy they are? On the value of self-rated happiness of people with a mental disorder. Journal of Happiness Studies, 12, 793–806.
Blanchflower, D. G., & Oswald, A. J. (2004). Well-being over time in Britain and the USA. Journal of Public Economics, 88, 1359–1386.
Bok, D. (2010). The politics of happiness. What government can learn from the new research on well-being. Princeton: Princeton University Press.
Bonicatto, S. C., Dew, M. A., Zaratiegui, R., Lorenzo, L., & Pecina, P. (2001). Adult outpatients with depression: Worse quality of life than in other chronic medical diseases in Argentina. Social Science and Medicine, 52, 911–919.
Bow-Thomas, C. C., Velligan, D. I., Miller, A. L., & Olsen, J. (1999). Predicting quality of life from symptomatology in schizophrenia at exacerbation and stabilization. Psychiatry Research, 86, 131–142.
Bruffaerts, R., Vilagut, G., Demyttenaere, K., Alonso, J., Alhamzawi, A., Andrade, L. H., et al. (2012). Role of common mental and physical disorders in partial disability around the world. The British Journal of Psychiatry, 200(6), 454–461.
Buntin, M. B., & Zaslavsky, A. M. (2004). Too much ado about two-part models and transformation? Comparing methods of modeling Medicare expenditures. Journal of Health Economics, 23, 525–542.
Chida, Y., & Steptoe, A. (2008). Positive psychological well-being and mortality: A quantitative review of prospective observational studies. Psychosomatic Medicine, 70, 741–756.
Chisholm, D., Lund, C., & Saxena, S. (2007). Cost of scaling up mental healthcare in low- and middle-income countries. British Journal of Psychiatry, 191, 528–535.
Cohen, J. (1988). Statistical power analysis for the behavioral sciences. New York: Academic Press.
Deaton, A. (2008). Income, health, and well-being around the world: Evidence from the Gallup World Poll. Journal of Economic Perspectives, 22, 53–72.
Diener, E., & Chan, M. Y. (2011). Happy people live longer: Subjective well-being contributes to health and longevity. Applied Psychology: Health and Well-Being., 3(1), 1–43.
Diener, E., Inglehart, R., & Tay, L. (2012). Theory and validity of life satisfaction scales. Social Indicators Research. doi: 10.1007/s11205-012-0076-y.
Diener, E., Lucas, R., Schimmack, U., & Heliwell, J. (2009). Well-being for public policy. Oxford: Oxford University Press.
Dolan, P., & White, M. P. (2007). How can measures of subjective well-being be used to inform public policy? Perspectives on Psychological Science, 2, 71–85.
El-Gabalawy, R., Mackenzie, C. S., Shooshtari, S., & Sareen, J. (2011). Comorbid physical health conditions and anxiety disorders: A population-based exploration of prevalence and health outcomes among older adults. General Hospital Psychiatry, 33, 556–564.
Ferrer-i-Carbonell, A., Bernard, M. S., & van Praag, B. M. S. (2002). The subjective costs of health losses due to chronic diseases. An alternative model for monetary appraisal. Health Economics, 11, 709–722.
Forward Scotland and Scottish Council Foundation. (2008). A wellbeing framework for Scotland: A better way for measuring society’s progress in the 21st century. http//www.forward-scotland.org.uk/Publications/Wellbeing-Better-Measure-Society-s-Progress.html.
Friedman, H. S., Tucker, J. S., Tomlinson-Keasey, C., Schwartz, J. E., Wingard, D. L., & Criqui, M. H. (1993). Does childhood personality predict longevity? Journal of Personality and Social Psychology, 65, 176–185.
Funk, M., Drew, N., Freeman, M., & Faydi, E. (2010). Mental health and development: Targeting people with mental health conditions as a vulnerable group. Geneva: World Health Organization. http://whqlibdoc.who.int/publications/2010/9789241563949_eng.pdf.
Ganev, K. (2000). Long-term trends of symptoms and disability in schizophrenia and related disorders. Social Psychiatry and Psychiatric Epidemiology, 35, 389–395.
Graham, C., Higuera, L., & Lora, E. (2011). Which health conditions cause the most unhappiness? Health Economics, 20(12), 1431–1447.
Gravelle, H., & Sutton, M. (2006). Income, relative income, and self-reported health in Britain 1979–2000. Centre of Health Economics, University of York. http://www.york.ac.uk/media/economics/documents/discussionpapers/2006/0606.pdf.
Grossi, E., Blessi, G. T., Sacco, P. L., & Buscema, M. (2012). The interaction between culture, health and psychological well-being: Data mining from the Italian culture and well-being project. Journal of Happiness Studies, 13, 129–148.
Hampson, S. E., Goldberg, L. R., Vogt, T. M., & Dubanoski, J. P. (2006). Forty years on: Teachers’ assessments of children’s personality traits predict self-reported health behaviors and outcomes at midlife. Health Psychology Review, 25, 57–64.
Heliwell, J., Layard, R., & Sachs, J. (2012). (Eds.) World happiness report. New York: The Earth Institute (Columbia University). http://www.earth.columbia.edu/sitefiles/file/Sachs%20Writing/2012/World%20Happiness%20Report.pdf.
Ho, B. C., Nopoulos, P., Flaum, M., Arndt, S., & Andreasen, N. C. (1998). Two-year outcome in first-episode schizophrenia: Predictive value of symptoms for quality of life. American Journal of Psychiatry, 155, 1196–1201.
Howell, R. T., Kern, M. L., & Lyubomirsky, S. (2007). Health benefits: Meta-analytically determining the impact of well-being on objective health outcomes. Health Psychology Review, 1, 83–136.
INE, Instituto Nacional de Estadística (2010). Estimacion de población, 2002–2010. Madrid: Instituto Nacional de Estadística. http://www.ine.es/jaxiBD/menu.do?L=0&divi=EPOB&his=0&type=db.
Jian, H., & Lubetkin, E. (2005). The impact of obesity on health-related quality-of-life in the general adult US population. Journal of Public Health, 7, 156–164.
Lam, J. A., & Rosenheck, R. A. (2000). Correlates of improvement in quality of life among homeless persons with serious mental illness. Psychiatric Services, 51, 116–118.
Layard, R. (2010). Measuring subjective well-being. Science, 327, 534–535.
Lehman, A. F. (1988). Quality of life interview for chronically mentally ill. Evaluation and Program Planning, 11, 51–62.
Lopez, A. D., Mathers, C. D., Ezzati, M., Jamison, D. T., & Murray, C. J. (2006). Global and regional burden of disease and risk factors, 2001: Systematic analysis of population health data. The Lancet, 367, 1747–1757.
Lubeck, D. P., & Hubert, H. B. (2005). Self-report was a viable method for obtaining health care utilization data in community dwelling seniors. Journal of Clinical Epidemiology, 58, 286–290.
Lyubomirsky, S., King, L., & Diener, E. (2005). The benefits of frequent positive affect: Does happiness lead to success? Psychological Bulletin, 131, 803–855.
Mathers, C. D., & Loncar, D. (2006). Projections of global mortality and burden of disease from 2002 to 2030. PLoS Medicine, 3(11), e442. doi:10.1371/journal.pmed.0030442.
Merikangas, K. R., Ames, M., Cui, L., Stang, P. E., Ustun, T. B., Von Korff, M., et al. (2007). The impact of comorbidity of mental and physical conditions on role disability in the US adult household population. Archives of General Psychiatry, 64, 1180–1188.
Moriarty, D. G., Zack, M. M., & Kobau, R. (2003). The Centers for Disease Control and Prevention’s healthy days measures—Population tracking of perceived physical and mental health over time. Health and Quality of Life Outcomes, 1, 1–8.
Murray, C.J.L., & Lopez, A.D. (1996). The global burden of disease and injury series (volume 1): A comprehensive assessment of mortality and disability from diseases, injuries, and risk factors in 1990 and projected to 2020. Cambridge, MA: Harvard School of Public Health on behalf of the World Health Organization and the World Bank, Harvard University Press.
Narvaez, J. M., Twamley, E. W., McKibbin, C. L., Heaton, R. K., & Patterson, T. L. (2008). Subjective and objective quality of life in schizophrenia. Schizophrenia Research, 98, 201–208.
Oswald, A. J., & Powdthavee, N. (2007). Obesity, unhappiness, and the challenge of affluence: Theory and evidence. Economic Journal, 1, 441–454.
Oswald, A. J., & Wu, S. (2010). Objective confirmation of subjective measures of human well-being: Evidence from the USA. Science, 327, 576–579.
Pavot, W., & Diener, E. (1993). Review of the Satisfaction With Life Scale. Psychological Assessment, 5, 164–172.
Pavot, W., & Diener, E. (2008). The Satisfaction With Life Scale and the emerging construct of life satisfaction. The Journal of Positive Psychology, 3, 137–152.
Pinto-Meza, A., Fernández, A., Fullana, M. A., Haro, J. M., Palao, D., Luciano, J. V., et al. (2009). Impact of mental disorders and chronic physical conditions in health-related quality of life among primary care patients: Results from an epidemiological study. Quality of Life Research, 18, 1011–1018.
Pirkola, S., Suvisaari, J., Elovainio, M., Partonen, T., Aalto, A., Honkonen, T., et al. (2009). General health and quality-of-life measures in active, recent, and comorbid mental disorders: A population-based health 2000 study. Comprehensive Psychiatry, 50, 108–114.
Pressman, S. D., & Cohen, S. (2005). Does positive affect influence health? Psychological Bulletin, 131, 925–971.
Prince, M., Patel, V., Saxena, S., Maj, M., Maselko, J., Phillips, M., et al. (2007). No health without mental health. The Lancet, 370, 859–877.
Ritter, P. L., Steward, A. L., Kaymaz, H., Sobel, D. S., Block, D. A., & Lorig, K. R. (2001). Self-reports of health care utilization compared to provider records. Journal of Clinical Epidemiology, 54, 136–141.
Ruggeri, M., Bisoffi, G., Fontecedro, L., & Warner, R. (2001). Subjective and objective dimensions of quality of life in psychiatric patients: A factor analytical approach. The South Verona Outcome Project 4. British Journal of Psychiatry, 178, 268–275.
Ryff, C. D., & Singer, B. (1998). The contours of positive human health. Psychological Inquiry, 9, 1–28.
Saarni, S. I., Suvisaari, J., Sintonen, H., Pirkola, S., Koskinen, S., Aromaa, A., et al. (2007). Impact of psychiatric disorders on health-related quality of life: General population survey. British Journal of Psychiatry, 190, 326–332.
Scott, K., Bruffarts, R., Tsang, A., et al. (2007). Depression-anxiety relationships with chronic physical conditions: Results from the World Mental Health Surveys. Journal of Affective Disorders, 103, 113–120.
StataCorp (2010). Stata statistical software. Release 11. College Station, TX: Stata Corporation.
Stiglitz, J.E., Sen, A., & Fitoussi, J.P. (2009). Commission on the measurement of economic performance and social progress. http://www.stiglitz-sen-fitoussi.fr.
Strine, T. W., Mokdad, A. H., Balluz, L. S., Gonzalez, O., Crider, R., Berry, J. T., et al. (2008). Depression and anxiety in the United States: Findings from the 2006 behavioral risk factor surveillance system. Psychiatric Services, 59, 1383–1390.
Tsuang, M. T., & Winokur, G. (1975). The Iowa 500: Field work in 35-year follow-up of depression, mania, and schizophrenia. Canadian Psychiatric Association Journal, 5, 359–365.
Ustun, T., Ayuso-Mateos, J. L., Chatterji, S., Mathers, C., & Murray, C. J. (2004). Global burden of depressive disorders in the year 2000. The British Journal of Psychiatry, 184, 386–392.
Ustun, T. B., Rehm, J., Chatterji, S., Saxena, S., Trotter, R., Room, R., et al. (1999). Multiple-informant ranking of the disabling effects of different health conditions in 14 countries. WHO/NIH Joint Project CAR Study Group. Lancet, 354, 111–115.
Vázquez, C., Duque, A., & Hervás, G. (2013). Satisfaction With Life Scale in a representative sample of Spanish adults: Validation and normative data. Spanish Journal of Psychology, 16, E82. doi:10.1017/sjp.2013.82.
Veenhoven, R. (2008). Healthy happiness: Effects of happiness on physical health and the consequences for preventive health care. Journal of Happiness Studies, 9, 449–469.
White, H. (1980). A heteroskedasticity-consistent covariance matrix and a direct test for heteroskedasticity. Econometrica, 48, 817–838.
Whiteford, H. A., Degenhardt, L., Rehm, J., Baxter, A. J., Ferrari, A. J., Erskine, H. E., et al. (2013). Global burden of disease attributable to mental and substance use disorders: Findings from the Global Burden of Disease Study 2010. Lancet, 6736, 1–12.
WHO (2009). Disease and injury regional estimates for 2004. Geneva: World Health Organization. http://www.who.int/healthinfo/global_burden_disease/estimates_regional/en/index.html.
Williams, A. (1999). Calculating the global burden of disease: Time for a strategic reappraisal? Journal of Health Economics, 8, 1–8.
Acknowledgments
We thank Margarita Alvarez, Jesús Gallardo, and Isabel de Julian (Coca-Cola Institute of Happiness) for their assistance in all stages of this research and anonymous reviewers for their comments on previous versions of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vázquez, C., Rahona, J.J., Gómez, D. et al. A National Representative Study of the Relative Impact of Physical and Psychological Problems on Life Satisfaction. J Happiness Stud 16, 135–148 (2015). https://doi.org/10.1007/s10902-014-9501-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10902-014-9501-z