Abstract
Purpose
To estimate the comorbidity of mental disorders with chronic physical conditions and to assess their independent and combined effects on health-related quality of life (HRQOL).
Methods
Face-to-face cross-sectional survey of adult attendants to public primary care (PC) centres from Catalonia (Spain). A total of 3,815 out of 5,402 selected patients provided data for this study. We report frequency of chronic physical conditions among participants with mental disorders and the contribution of each mental disorder and chronic physical condition to HRQOL.
Results
Chronic pain is the most frequent condition among those with mental disorders (74.54%). The effect of chronic physical conditions on HRQOL is rather minor when compared to the effect of mental disorders (especially mood disorders). However, chronic pain plays an important role in HRQOL loss.
Conclusions
Mood disorders and chronic pain negatively affect HRQOL of PC patients. Especial efforts should be made to detect and treat mental disorders and chronic pain at this level.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The co-occurrence of mental disorders with chronic physical conditions is common both in general population samples [1–3] and in primary care (PC) samples [4]. Several studies have found poorer physical health status among people with mental disorders relative to those without mental disorders [5–7]. Higher rates of mental disorders, especially depression and anxiety, have been reported in people with medical diseases compared with those without them [1, 7, 8]. While physical [9, 10] and mental disorders [4, 11–13] have negative effects in disability, it is suggested that physical–mental comorbidity is even more disabling with regard to functioning [14–16].
Health-related quality of life (HRQOL), a subjective outcome measure commonly used to evaluate the impact of mental disorders and physical conditions, provides a multidimensional perspective encompassing patient’s emotional, physical, and social functioning. An inverse relationship between multimorbidity and HRQOL has been recently found [17, 18]. However, comparisons among aforementioned studies are difficult given the absence of a uniform way of defining and measuring multimorbidity, failure to systematically consider psychiatric comorbidity, and the effects of potential confounding variables that could have an impact on HRQOL such as age, gender, educational level, and perceived social support.
Considering aforementioned studies, we hypothesize that PC patients with comorbid mental disorders and chronic physical conditions will present the worst HRQOL.
The aims of this study are (1) to estimate the comorbidity of mental disorders with chronic physical conditions and (2) to assess the independent and combined effects of mental disorders and chronic physical conditions on HRQOL. The present study is part of a larger project aimed to estimate the prevalence of mental disorders in the PC of Catalonia [19].
Methods
Participants
The study was a face-to-face cross-sectional survey of a representative sample of adult attendants (18 years or older) to primary health care centres from Catalonia (Spain). Catalonia is one of the 17 autonomous regions that conform Spain, with a population of 7,134,697 inhabitants according to the 2006 census. In 1981, Spain began a process of decentralization of health services management being them now managed by each autonomous region.
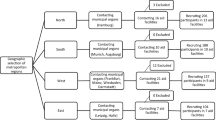
A stratified multistage probability sample without replacement was drawn. Replacement was prohibited to ensure that every individual had a known probability of selection. The sampling frame was all health regions of Catalonia (a total of seven). The first stage consisted of the selection of the PC centres within each health region. The number of PC centres to be selected in each region was proportional to the population of the region. However, in order to have a minimum set of interviews even in the smaller regions, at least six PC centres were chosen per region. The probability of selection of each PC centre was related to the population of the catchment area covered by the centre. All PC physicians of the health centres were invited to participate. A total of 618 PC physicians participated in the study (representing the 69% of all contacted PC physicians). The third stage consisted in the random selection of patients. Patients were selected with a systematic sampling strategy from the daily list of all patients with an appointment with each of the participating PC physicians.
A total of 5,402 patients were selected. Among them, 654 (12.1%) did not attend to the visit with the respective family physician, 764 (16.1%) did not accept to participate, and 164 (3.5%) were excluded because they showed cognitive impairment severe enough to preclude an adequate interview. Weighted response rate was 80.5%, leaving a study sample of 3,820 participants from 78 PC centres. However, one of the PC centres was excluded because of data loss. Therefore, the sample considered in the present study comprised 3,815 patients.
Materials
Mental disorders were assessed with the Spanish versions of the Structured Clinical Interview for DSM-IV Axis I Disorders SCID-I (major depressive episode, dysthymic disorder, and anxiety disorder modules, excluding obsessive–compulsive disorder) [20] and the Mini Neuropsychiatric Diagnostic Interview MINI (manic/hypomanic episodes, obsessive–compulsive disorder, substance and alcohol use disorders, anorexia nervosa, and bulimia nervosa) [21, 22]. Both instruments allow diagnoses according to DSM-IV [23] criteria.
Health-related quality of life was assessed with the Spanish version 2.0 of the 12-item Short-Form Health Survey SF-12 [24–26]. The SF-12 is a valid and reliable widely used instrument for the assessment of HRQOL. Two measures were derived from the SF-12: a physical component summary scale (PCS-12), indicating physical quality of life, and a mental component summary scale (MCS-12), indicating mental quality of life. Each scale uses all 12 items but with different weights. PCS-12 and MCS-12 scales were scored using norm-based methods.
Chronic physical conditions were assessed using a checklist that included questions about a wide range of chronic physical conditions including allergies, arthritis or rheumatism, asthma, back pain, bronchitis, cataracts, constipation, diabetes, hearing impairment, heart disease, heart attack, high blood pressure, migraines or frequent headaches, neck pain, prostate-related conditions, stroke, ulcer, vision impairment. Similar conditions, or conditions having similar risk factors, were grouped together. Only the more frequent conditions were considered in the analyses (i.e. chronic pain including: arthritis or rheumatism, chronic back pain, chronic neck pain, and migraines or frequent headaches; cardiovascular disease including: stroke, hearth attack, and hearth disease; respiratory conditions including asthma and bronchitis; high blood pressure; and diabetes).
Respondents were asked whether they had ever experienced each of the symptom-based conditions in the checklist. In case of conditions typically identified by medical diagnosis, respondents were asked whether a doctor or other health professional ever told them they had the condition.
Perceived social support was assessed by means of one item of the Spanish version [27] of the Sheehan Disability Scales [28]. The Sheehan Disability Scales measure the severity of disability in three inter-related domains and include two optional ratings of perceived stress and perceived social support. We used one of these optional items (the one evaluating perceived social support that asks the following: “During the last week, how much support have you received from your friends, family, work mates, etc. considering the support you have needed?”). Participants could answer using a scale ranging from 0 to 100%.
Procedure
Data were collected between October 2005 and March 2006 using a paper-and-pencil personal interview. After a visit with a PC physician, individuals were offered to participate in the study. They were evaluated in their PC centres after acceptance (signing an informed consent form). During an approximately 45 min clinical interview, the instruments were administered. After data collection, responses were processed using response automatic capture software TeleForm©.
A group of 20 trained clinical psychologists evaluated participants. All interviewers were trained by one of the study investigators (AS, DP, JMH, or AP) during a 2-day course. Ethics approval was obtained from Sant Joan de Déu Foundation Ethics Board.
Statistical analyses
We report frequency of chronic physical conditions as well as PCS-SF12 and MCS-SF12 means among participants with and without 12-month mental disorders based on weighted data, along with their confidence intervals.
After testing normality of PCS-SF12 and MCS-SF12 variables, we found that both showed slightly right-skewed distributions. In light of this, one possible alternative was to transform data. However, we decided to fit linear regression models following suggestions by Lumley et al. [29] who argued that normality is not required to fit a linear regression when sample size is large enough, since the Central Limit Theorem guarantees that coefficient estimates will be normally distributed.
Thus, the effect of chronic physical conditions and mental disorders on HRQOL was assessed using linear regression models. We report estimated parameters (β) for the contribution of each chronic physical condition to HRQOL adjusting for sociodemographic variables (gender, age, and educational level), perceived social support, and comorbid mental disorders categories (mood and anxiety disorders) and chronic physical conditions. We also report the estimated parameters for the contribution of each mental disorder category to HRQOL, adjusting for sociodemographic variables, perceived social support, and comorbid chronic physical conditions and mental disorders categories. Interactions between each mental disorder category and each chronic physical condition were tested for both the PCS-SF12 and MCS-SF12.
The results of the analysis have been weighted to account for the different probability of selection given the stratified sampling. All analyses were carried out with the STATA 9 for PC [30] using methods especially designed for analysing complex sample surveys and weighted data. All significance tests were made using two-sided tests evaluated at the 0.05 level of significance.
Results
Among 3,815 patients evaluated, 62.94% were women. Mean age was 54.36 years (95% CI = 53.45–55.26) and educational level distribution was as follows: primary studies 48.22%, secondary 26.08%, university degree 13.31%, and no studies 12.39%.
Chronic pain was by far the most frequent chronic physical condition among those with and without mental disorders (74.54 and 63.06%, respectively). By mental disorder category, chronic pain was the most frequent among those with mood disorders (82.62%) and anxiety disorders (77.28%). High blood pressure, cardiovascular diseases, and diabetes were slightly more frequent among those without mental disorders (Table 1).
Among participants with mental disorders, those with comorbid cardiovascular diseases had the poorest physical HRQOL (PCS-SF12 = 38.65) and those with comorbid respiratory conditions the poorest mental HRQOL (MCS-SF12 = 37.65) (Table 1). By mental disorder categories, participants with mood disorders and comorbid chronic physical conditions showed worse HRQOL (both PCS-SF12 and MCS-SF12) than participants with anxiety disorders and comorbid chronic physical conditions.
Health-related quality of life was substantially decreased in its physical component by the comorbidity between diabetes and mood disorders (PCS-SF12 = 36.63) and in its mental component by the comorbidity between mood disorders and chronic pain (Table 1).
Overall chronic physical conditions had less impact on HRQOL than mental disorders (Tables 2, 3). While chronic pain and cardiovascular diseases significantly reduced physical HRQOL, after adjusting by sociodemographics, perceived social support, other comorbid chronic physical conditions, and comorbid mental disorders, a reduction between 5.72 and 4.67 points in the PCS-SF12 was observed (less than one SD). On the contrary, after adjusting by sociodemographics, perceived social support, other comorbid mental disorders, and comorbid chronic physical conditions, mood disorders and, to a lesser extent, anxiety disorders had a substantial impact on HRQOL. Mood disorders alone explained a reduction of 19.97 points in the MCS-SF12 (almost two SD).
After testing, possible interactions between each mental disorder category and each chronic physical condition for the PCS-SF12 and MCS-SF12, we found that the interaction between mood disorders and chronic pain negatively affected the PCS-SF12 [β for chronic pain was −4.92 (−5.67, −4.17); β for mood disorders was 0.02 (−2.80, 2.85); and β for their interaction was −4.60 (−7.26, −1.95)].
Discussion
Our results need to be interpreted within the context of the study limitations. First, the cross-sectional nature of the study does not allow us to assume that the reduction in HRQOL is in fact a consequence of either mental disorders or chronic physical conditions. Second, chronic physical conditions were ascertained using a checklist rather than physician’s examination. However, checklist have been found to provide useful information about both treated and currently untreated chronic conditions [31], and they can predict outpatient health care use, hospitalisations and mortality [32]. Additionally, methods research has shown that self-report of chronic physical conditions shows moderate to high agreement with medical records data [33]. Third, the chronic pain category grouped four conditions (arthritis or rheumatism, chronic back pain, chronic neck pain, and migraines or frequent headaches). This fact could have overestimated its frequency since if it was more questioned, it could have been more frequently answered.
The present findings show a relative specificity between kind of disorder and the area of HRQOL affected. While chronic physical conditions mostly affected the physical component of the measure used, mental disorders affected both of them, especially the mental component. Our findings are consistent with prior literature in suggesting that mental disorders are often more disabling than chronic physical conditions [34–37] and that mood disorders are especially disabling [37, 38]. However, we could not be sure if mood disorders truly affected HRQOL or if they affected participants’ self-perceptions about their HRQOL. Would this be true, this would not only affect our results, but a large number of studies on HRQOL, since the instrument we used is among the most used in assessing this construct. In any case, according to our findings, mental disorders (particularly mood disorders) could be considered as important determinants of how patients’ feel about themselves and their lives. If an objective is to improve patients’ HRQOL, especial efforts should be made to detect and treat mental disorders at the PC level.
The presence of chronic pain was quite common among those with and without mental disorders, and was especially frequent among those with mood and anxiety disorders. In fact, several chronic painful physical conditions have been associated to major depression [39, 40]. General population-based studies suggest that depressive disorders could be risk factors for incident back pain [41] and future chronic back pain [42]. Additionally, in a recent 13-years follow-up study, chronic back pain emerged as one of the strongest predictors of major depression and the combination of both conditions was associated with greater disability [43]. According to our data and consistent with data from general population-based studies assessing chronic painful conditions such as back or neck pain [40], the comorbidity of chronic pain and mood disorders is high in PC patients and among those with the most negative impact on HRQOL. Moreover, the only significant interaction found affecting HRQOL was mood disorders/chronic pain, having it a negative effect on the physical component of the measure used. However, when looking data in detail, we observed that chronic pain was substantially more impairing than mood disorders. In the linear regression fitted with the interaction mood disorders/chronic pain, we found that mood disorders alone were not statistically significant while chronic pain alone and the interaction were. That is, it seems that most of the HRQOL loss in the physical component of the measure used is explained by the presence of chronic pain and that mood disorders add more impairment in those suffering from chronic pain. Unfortunately, the causal mechanism linking these conditions could not be derived from our data and seems to be a controversial topic [39]. In any case, and consistent with previous findings from a different kind of sample (general population) [40], chronic pain seems to be a kind of condition that commonly appears to be comorbid with some others (e.g. mood disorders or other chronic physical conditions).
In light of this, we could suggest that PC patients seeking consultation for chronic pain should be systematically evaluated for depression. Common misdiagnosis of mental disorders in patients with chronic pain could be related to the idea that it may be natural to be depressed if you suffer from pain and that no especial intervention is needed. When comorbidity between chronic pain and mood disorders occur, HRQOL is affected in all dimensions. Thus, there is a need of a through detection of mental disorders (mainly mood disorders) in all patients with chronic pain. Additionally, policy efforts aiming to improve patients HRQOL should be devoted to evaluate and treat the common comorbid physical and mental disorders that could be found at the PC level.
To conclude, mental disorders (particularly mood disorders) are especially disabling at PC. Additionally, chronic pain is an important source of HRQOL loss that commonly courses in comorbidity. PC physicians are at a privileged position for improving patients’ HRQOL.
References
Buist-Bouwman, M. A., de Graaf, R., Volleberg, W. A. M., & Ormel, J. (2005). Comorbidity of physical and mental disorders and the effect on work-loss days. Acta Psychiatrica Scandinavica, 111, 436–443.
Kessler, R. C., Ormel, J., Demler, O., & Stang, P. E. (2003). Comorbid mental disorders account for the role impairment of commonly occurring chronic physical disorders: Results from the national comorbidity survey. Journal of Occupational and Environmental Medicine, 45, 1257–1266.
Neeleman, J., Ormel, J., & Bijl, R. V. (2001). The distribution of psychiatric and somatic ill-health: association with personality and socioeconomic status. Psychosomatic Medicine, 63, 239–247.
Berardi, D., Berti Ceroni, G., Leggieri, G., Rucci, P., Ustün, B., & Ferrari, G. (1999). Mental, physical and functional status in primary care attenders. International Journal of Psychiatry in Medicine, 29, 133–148.
Harter, M. C., Conway, K. P., & Merikangas, K. R. (2003). Associations between anxiety disorders and physical illness. European Archives of Psychiatry and Clinical Neuroscience, 253, 313–320.
Kendrick, T. (1996). Cardiovascular and respiratory risk factors and symptoms among general practice patients with long-term mental illness. British Journal of Psychiatry, 169, 733–739.
Scott, K. M., Browne, O., McGee, M. A., & Wells, J. E. (2006). New Zealand Mental Health Survey Research Team. Mental–physical comorbidity in Te Rau Hinegaro: The New Zealand Mental Health Survey. Australian and New Zealand Journal of Psychiatry, 40, 882–888.
Katon, W. J., & Ciechanowski, P. S. (2002). Impact of major depression on chronic medical illness. Journal of Psychosomatic Research, 53, 859–863.
Sprangers, M. A. G., de Regt, E. B., Andries, F., van Agt, H. M., Bijl, R. V., de Boer, J. B., et al. (2000). Which chronic conditions are associated with better or poorer quality of life? Journal of Clinical Epidemiology, 53, 895–907.
Stewart, A., Greenfield, S., Hays, R. D., Wells, K., Rogers, W. H., Berry, S. D., et al. (1989). Functional status and well-being of patients with chronic conditions: results from the medical outcomes study. JAMA, 262, 907–913.
Beekman, A. T. F., Penninx, B. W. J. H., Deeg, D., de Beurs, E., Geerling, S. W., & van Tilburg, W. (2002). The impact of depression on the well-being, disability and use of services in older adults: a longitudinal perspective. Acta Psychiatrica Scandinavica, 105, 20–27.
Bijl, R. V., & Ravelli, A. (2000). Current and residual functional disability associated with psychopathology: findings from The Netherlands Mental Health Survey and Incidence Study (NEMESIS). Psychological Medicine, 30, 657–668.
Ormel, J., Von Korff, M., Ustun, T. B., Pini, S., Korten, A., & Oldehinkel, T. (1994). Common mental disorders and disability across cultures. Results from the WHO collaborative study on psychological problems in general health care. JAMA, 272, 1741–1748.
Arnow, B. A., Hunkeler, E. M., Blasey, C. M., Lee, J., Constantino, M. J., Fireman, B., et al. (2006). Comorbid depression, chronic pain, and disability in primary care. Psychosomatic Medicine, 68, 262–268.
Stang, P. E., Brandenburg, N. A., Lane, M. C., Merikangas, K. R., Von Korff, M. R., & Kessler, R. C. (2006). Mental and physical comorbid conditions and days in role among persons with arthritis. Psychosomatic Medicine, 68, 152–158.
Sullivan, M. D., LaCroix, A. Z., Russo, J. E., & Walker, E. A. (2001). Depression and self-reported physical health in patients with coronary disease: mediating and moderating factors. Psychosomatic Medicine, 63, 248–256.
Fortin, M., Lapointe, L., Hudon, C., Vanasse, A., Ntetu, A. L., & Maltais, D. (2004). Multimorbidity and quality of life in primary care: a systematic review. Health and Quality of Life Outcomes, 2, 51.
Fortin, M., Bravo, G., Hudon, C., Lapointe, L., Almirall, J., Dubois, M. F., et al. (2006). Relationship between multimorbidity and health-related quality of life of patients in primary care. Quality of Life Research, 15, 83–91.
Serrano-Blanco, A., Palao, D., Luciano, J. V., Pinto-Meza, A., Luján, L., Fernández, A., Roura, P., Bertsch, J., Mercader, M., Haro, J. M. (2009). Prevalence of mental disorders in primary care: results from the diagnosis and treatment of mental disorders in primary care study (DASMAP). Social Psychiatry and Psychiatric Epidemiology (in press).
First, M. B., Gibbon, M., Spitzer, R. L., Williams, J. B. W. (1996). User’s Guide for the Structured Clinical Interview for DSM-IV Axis I Disorders. Research Version. New York, NY: Biometrics Research.
Sheehan, D. V., Lecrubier, Y., Sheehan, H., Amorim, P., Janavs, J., Weiller, E., et al. (1998). The Mini-International Neuropsychiatric Interview (M.I.N.I): The development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. Journal of Clinical Psychiatry, 59(Suppl 20), 22–33.
Ferrando, L., Bobes, J., Gibert, J. (2000). MINI International neuropsychiatric Interview. Versión en Español 5.0. Accessed September 2005, from http://entomologia.rediris.es/pub/bscw.cgi/d602335/MINI%20Entrevista%20Neuropsiquiatrica%20Internacional.pdf.
American Psychiatric Association. (1994). Diagnostic and statistical manual of mental disorders (4th ed.). Washington, DC: American Psychiatric Association.
Gandek, B., Ware, J. E., Aaronson, N. K., Apolone, G., Bjorner, J. B., Brazier, J. E., et al. (1998). Cross-validation of item selection and scoring for the SF-12 Health Survey in nine countries: results from the IQOLA Project. International Quality of Life Assessment. Journal of Clinical Epidemiology, 51, 1171–1178.
Vilagut, G., Ferrer, M., Rajmil, L., Rebollo, P., Permanyer-Miralda, G., Quintana, J. M., et al. (2005). The Spanish version of the Short Form 36 Health Survey: a decade of experience and new developments. Gaceta Sanitaria, 19, 135–150.
Ware, J. E., Jr, Kosinki, M., & Keller, S. D. (1996). A 12-Item Short Form Health Survey: construction of scales and preliminary tests of reliability and validity. Medical Care, 34, 220–233.
Bobes, J., Badia, X., Luque, A., Garcia, M., González, M. P., Dal-Ré, R., et al. (1999). Validation of the Spanish versions of the Liebowitz Social Anxiety Scale, Social Anxiety and Distress Scale and the Sheehan Disability Inventory for the evaluation of social phobia. Medicina Clinica, 112, 530–538.
Sheehan, D. V., Harnett-Sheehan, K., & Raj, B. A. (1996). The measurement of disability. International Clinical Psychopharmacology, 11(Suppl 3), 89–95.
Lumley, T., Diehr, P., Emerson, S., & Chen, L. (2002). The importance of the normality assumption in large public health data sets. Annual Review of Public Health, 23, 151–169.
StataCorp. (2005). STATA Statistical Software: Release 9. StataCorp LP.
Knight, M., Stewart-Brown, S., & Fletcher, L. (2001). Estimating health needs: the impact of a checklist of conditions and quality of life measurements on health information derived from community surveys. Journal of Public Health Medicine, 23, 179–186.
Fan, V. S., Au, D., Heagerthy, P., Deyo, R. A., McDonell, M. B., & Fihn, S. D. (2002). Validation of case-mix measures derived from self-reports of diagnoses and health. Journal of Clinical Epidemiology, 55, 371–380.
Evaluation of National Health Interview Survey diagnostic reporting. (1994). Vital and health statistics. Series 2, 120, pp 1–116.
Armenian, H. K., Pratt, L. K., Gallo, J., & Eaton, W. W. (1998). Psychopathology as a predictor of disability: a population-based follow-up study in Baltimore, Maryland. American Journal of Epidemiology, 148, 269–275.
Hays, R. D., Wells, K. B., Sherbourne, C. D., Rogers, W., & Spritzer, K. (1995). Functioning and well-being outcomes of patients with depression compared with chronic general medical illnesses. Archives of General Psychiatry, 52, 11–19.
Ormel, J., Kempen, G. I., Deeg, D. J., Brilman, E. I., van Sonderen, E., & Relyveld, J. (1998). Functioning, well being, and health perception in late middle-aged and older people: comparing the effects of depressive symptoms and chronic medical conditions. Journal of the American Geriatrics Society, 46, 39–48.
Pinto-Meza, A., Haro, J. M., Palacin, C., Torres, J. V., Ochoa, S., Vilagut, G. Rt al. (2007). Impacto de los trastornos del ánimo, de ansiedad y de las enfermedades físicas crónicas en la calidad de vida de la población general de España. Resultados del estudio ESEMeD-España. Actas Españolas de Psiquiatría, 35 (Suppl 2), 12–20.
Spitzer, R. L., Kroenke, K., Linzer, M., Hahn, S. R., Williams, J. B., deGruy, F. V., I. I. I., et al. (1995). Health-related quality of life in primary care patients with mental disorders. Results from the PRIME-MD 1000 Study. JAMA, 274, 1511–1517.
Ohayon, M. M., & Schatzberg, A. F. (2003). Using chronic pain to predict depressive morbidity in the general population. Archives of General Psychiatry, 60, 39–47.
Pinto-Meza, A., Serrano-Blanco, A., Codony, M., Reneses, B., von Korff, M., Haro, J. M., et al. (2006). Prevalencia y comorbilidad física y mental del dolor dorsal y del dolor cervical crónicos en España: resultados del estudio ESEMED. Medicina Clínica, 127, 325–330.
Larson, S. L., Clark, M. R., & Eaton, W. W. (2004). Depressive disorder as a long-term antecedent risk factor for incident back pain: a 13-year follow-up study from the Baltimore Epidemiological Catchment Area Sample. Psychological Medicine, 34, 211–219.
Currie, S. R., & Wang, J. (2005). More data on major depression as an antecedent risk factor for first onset of chronic back pain. Psychological Medicine, 35, 1275–1282.
Currie, S. R., & Wang, J. (2004). Chronic back pain and major depression in the general Canadian population. Pain, 107, 54–60.
Acknowledgments
This study was funded by the “Direcció General de Planificació i Avaluació Sanitària, Departament de Salut, Generalitat de Catalunya” (Barcelona, Spain). AF and JVL are grateful to the “Ministerio de Sanidad y Consumo, Instituto de Salud Carlos III” (Red RD06/0018/0017) for a predoctoral and a postdoctoral contract, respectively.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pinto-Meza, A., Fernández, A., Fullana, M.A. et al. Impact of mental disorders and chronic physical conditions in health-related quality of life among primary care patients: results from an epidemiological study. Qual Life Res 18, 1011–1018 (2009). https://doi.org/10.1007/s11136-009-9522-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-009-9522-y