Abstract
Arthritis is characterized by irreversible joint destruction and presents a global health burden. Natural alternatives to synthetic drugs have been gaining popularity for their safety and effectiveness. Juglanin has demonstrated a range of anti-inflammatory effects in various tissues and cell types. However, the pharmacological function of Juglanin in arthritis and chondrocytes has been little studied. ATDC5 cells were treated with 1 μg/mL lipopolysaccharide (LPS) in the presence or absence of juglanin (2.5, 5 μM) for 24 h. The effects of juglanin on cellular nucleotide-binding domain leucin-rich repeat receptor 3 (NLRP3) inflammasome complex and endproduct interleukin 1β (IL-1β) and interleukin (IL-18) were assessed by reverse transcription-polymerase chain reaction (RT-PCR), enzyme-linked immunosorbent assay (ELISA), and Western blot experiments. The oxidative stress was measured by super oxide dismutase (SOD) activity and NADPH oxidase 4 (NOX4) expression. The dependent effect of juglanin on silent information regulator 2 homolog 1 (SIRT1) was evaluated by siRNA knockdown approach. Juglanin significantly reduced cellular oxidative stress by downregulating NOX4 expression production and rescuing the decreased activity of total SOD induced by LPS. Juglanin inhibited the activation of the TxNIP/NLRP3/ASC/caspase-1 axis, and decreased production of IL-1β and IL-18. Moreover, juglanin rescued the LPS-induced decrease in SIRT1 expression. SIRT1 silencing abolished the anti-NLRP3 inflammasome effect of juglanin, indicating that the effects of juglanin are dependent on its amelioration on SIRT1 expression. Juglanin possesses an anti-inflammatory and anti-ROS capacity in chondrocytes, and this study provides available evidence that juglanin may be of use in the treatment of arthritis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
As a chronic inflammatory disease, arthritis involves a wide range of inflammatory mechanisms. Arthritis is the most common arthritic disease worldwide, but due to its complicated etiology, a safe and reliable treatment to halt or prevent arthritis has not yet been developed [1]. Chondrocytes are the most abundant cell type found in articular cartilage, and therefore, chondrocyte dysfunction is a major factor in the pathogenesis of this painful degenerative joint disease. In normal joints, chondrocytes are quiescent, fully differentiated cells, which function to regulate anabolism/catabolism of the cartilage matrix and maintain joint homeostasis and cell survival [2]. However, in arthritis, exposure to proinflammatory cytokines and oxidative stress induces chondrocytes to perpetuate the inflammatory response and assume a hypertrophic proliferative state [3, 4]. Lipopolysaccharides (LPS) are a proinflammatory byproduct of Gram-negative bacteria that are recognized to contribute to arthritis by activating the NLRP3 inflammasome, immune cells, and chondrocytes, inducing cartilage matrix destruction, and eliciting a pain response [5, 6]. The stimulation of chondrocytes with LPS is a common experimental method to simulate arthritis in vitro [7].
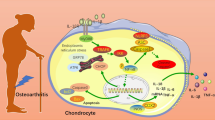
The assembly and activation of the NLRP3 inflammasome complex is a significant event in the pathogenesis of arthritis. The NLRP3 Nod-like receptor protein can be activated by a wide range of ligands, including signaling molecules; bacteria and viruses; cell debris; and byproducts of microbial metabolism, such as LPS, among other things. Upon activation of NLRP3, this receptor binds to ASC, which mediates the cleavage of caspase 1 to form the NLRP3 inflammasome complex. Caspase 1 then cleaves pro-interleukin (IL)-1β and pro-IL-18, thereby triggering the inflammatory response mediated by the secretion of these mature cytokines [8, 9]. Oxidative stress is another major factor in the development and progression of arthritis. Increased production of reactive oxygen species (ROS) and decreased super oxide dismutase (SOD) activity leads to an imbalance in the oxidant/antioxidant ratio, which has been shown to be involved in the pathogenesis of arthritis [10]. NADPH oxidase 4 (NOX4) has been shown to enhance ROS production in arthritis, and its activation and expression are increased by LPS [11, 12]. The increased expression of the pro-oxidant enzymes including SOD and NLRP3 inflammasome has been connected to the pathogenesis of arthritis. LPS treatment triggers extracellular matrix-aggrecan degradation [13] and pro-oxidant gene expression [12]. Furthermore, increased production of ROS causes thioredoxin-interacting protein (TxNIP) to dissociate from thioredoxin and bind to NLRP3, thereby activating the inflammasome and contributing to IL-1β maturation in arthritis [14]. The sirtuin 1 (SIRT1) transcriptional pathway is known for its protective role in various cells and tissues, and the expression of SIRT1 is reduced by LPS [15]. Rescuing the reduction in SIRT1 activity is an attractive treatment target for mitigating inflammation and oxidative stress in arthritis [16,17,18]. Additionally, research has shown that SIRT1 can inhibit the activation of the NLRP3 inflammasome [19]. Importantly, the potential role of NLRP3 inflammasome in chondrocytes has been reported in recent studies. The expressions of caspase 1, ASC, and NLRP3 proteins in lysates of primary chondrocytes from OA knee joint explants is needed for the maturation of IL-1β and IL-18 [20]. Exposure to proinflammatory cytokines such as TNF-α induced chondrocyte damage due to NLRP3 inflammasome activation [21].
Juglanin is a naturally occurring flavonoid compound isolated from Polygonum aviculare, a type of knotgrass, which has been shown to exert anti-inflammatory, antioxidative stress, and anti-cancer effects. Molecular structure of juglanin is shown in Fig. 1. Recent research has shown that juglanin can also inhibit LPS-induced neuroinflammation and lung injury by suppressing the expression of proinflammatory cytokines, including tumor necrosis factor-α (TNF-α), IL-1β, and IL-6, and inhibiting the activation of the nuclear factor-κB (NF-κB) inflammatory signaling pathway [22]. Interestingly, a contemporary study found that juglanin might ameliorate arthritis by inhibiting the IL-1β-induced expression of cytokines, including cyclooxygenase 2 (COX2) and prostaglandin E2 (PGE2); oxidative stress; the expression of degradative enzymes, including matrix metalloproteinases (MMPs) and a disintegrin and metalloprotease thrombospondin (ADAMTS); and activation of the NF-κB pathway [23]. These findings present an excellent basis for further research regarding the role of juglanin in arthritis. In the present study, we investigated the effects of juglanin on some other aspects of oxidative stress and inflammation, including ROS, SOD, and NOX4 production, TxNIP-mediated NLRP3 inflammasome activation, and the involvement of the SIRT1 pathway. Our findings show that juglanin exerts a potent anti-inflammatory effect in LPS-induced chondrocytes.
MATERIALS AND METHODS
Cell Culture and Treatment
Prior to the experiments, the chondrogenic ATDC5 cells (Bang-yi Biotechnology, China) were differentiated for 1 week by culturing in the T75 cell culture flask with a differentiation medium (DMEM/F-12 (1:1) containing GlutaMAX I and supplemented with 5% fetal serum, 1% sodium pyruvate, and 0.5% gentamicin). The cell cultures were maintained in a humidified atmosphere (5% CO2) at 37 °C, and the culture media was replaced with fresh media every second or third day. For LPS stimulation, ATDC5 cells were plated in T25 cell culture flasks and grown to 80–90% confluence. The cells were then treated with 1 μg/mL LPS [5, 6, 18] (Sigma-Aldrich, USA) in the presence or absence of juglanin (> 98% Purity) (2.5, 5 μM) (Yuanye Biotech, China) [20,21,22,23] for 24 h. The juglanin powder was firstly dissolved in DMSO and stored in −20 °C freezer and diluted in PBS for cell culture.
Real-Time PCR
For real-time polymerase chain reaction (PCR) analysis, total RNA was extracted from the cells using TRIZOL reagent (Life Science Inc., USA) in accordance with the manufacturer’s protocol. Then, 1–2 μg of total RNA was used to perform reverse transcription PCR using a One-Step First cDNA Synthesis Kit (Life Science Inc., USA). Real-time PCR was performed using the SYBR Green method on an HT-7500 Real-time PCR system (ABI System Inc., USA). Briefly, the cells were pre-incubated for 5 min at 95 °C followed by 40 cycles at 95 °C for 30 s, and 60 °C for 30 s. The resulting data are presented as relative fold changes, which were obtained by normalizing to GAPDH. Quantification of the target genes was performed using the 2−ΔΔCt method. The following primers were used in this study: NOX4 (forward: 5′-TGCCTGCTCATTTGGCTGT-3′, reverse: 5′-CCGGCACATAGGTAAAAGGATG-3′); TxNIP (forward: 5′-GGCTAAAGTGCTTTGGATGC-3′, reverse: 5′-AGGTCTCATGATCACCATCTCA-3′); SIRT1 (forward: 5′-CAGCAAGGCGAGCATAAA-3′; reverse: 5′-TTCAGAACCACCAAAGCG-3′); GAPDH (forward: 5′-ACCCCTTCATTGACCTCAAC-3′, reverse: 5′-CTTGACGGTGCCATGGAATT-3′).
Western Blot Analysis
After the indicated treatment, the cells were washed with ice-cold PBS buffer (pH 7.4) and lysed using RIPA buffer (0.5% Triton X-100, 0.5% sodium deoxycholate salt, 150 mM NaCl, 20 mM Tris (pH 7.4), 10 mM EDTA, containing protease/inhibitor cocktail (Roche, Switzerland). A Bradford Assay (BioRad, USA) was used to determine the concentration and quality of the lysed samples. Equal amounts of samples (20 μg) were loaded onto 10% SDS-PAGE gels, and the proteins of interest were separated according to size. The protein mixture was then transferred onto PVDF membranes (Millipore, USA) and blocked with 5% non-fat milk for 1 h. The blots were incubated with following primary antibody: NOX4 (1:1000, Cat#14347–1-AP, Proteintech, USA), TXNIP (1:2000, Cat#14715, Cell Signaling Technology, USA), NLRP3 (1:1000, cat#19771–1-AP, Proteintech, USA), ASC (1:1000, Cat#sc-22,514-R, Santa Cruz Biotechnology, USA), caspase-1 p10 (1:500, Cat#sc-514, Santa Cruz Biotechnology, USA), SIRT1 (1:1000, Cat#13161–1-AP, Proteintech, USA), and β-actin (1:1000, sc-130,656, Santa Cruz Biotechnology, USA) separately overnight at 4 °C, and then incubated with corresponding chemiluminescence-labeled secondary antibodies for 1 h at room temperature (Cell Signaling Technology, USA). An automatic C-DiGit™ Blot Scanner (LI-COR Biosciences, USA) was used to visualize the reacted blots. The densitometry of the blots was analyzed using the ImageJ software. Firstly, the Western blot bands were scanned, and the background was subtracted. The target bands were then selected, and the signal intensities were quantified. Data were exported for statistical analysis.
Elisa
After the indicated treatment, the cell culture media was collected and centrifuged at 1000 rpm for 10 min to remove any cell debris. The supernatant was then used to perform enzyme-linked immunosorbent assay (ELISA) using commercial kits for IL-1β and IL-18 in accordance with the manufacturer’s instructions (R&D Systems, USA, Cat# MLB00C, #DY122–05). Ninety-six-plate reader spectrometry was used to collect the resulting data. A standardized 4-PL curve was used to obtain absolute values. The relative levels of IL-1β and IL-18 were normalized to the total protein level. The results are expressed as fold changes.
Determination of ROS and Total SOD
To measure the cellular ROS, the living cells were stained with dihydroethidium dye (DHE) (Sigma-Aldrich, USA). The cells were washed 3 times and loaded with 5 μM fluorescent DHE probe for 30 min at 37 °C in darkness. The fluorescent signals were detected at an excitation wavelength of 518 nm using a fluorescent microscope. The results of ROS staining were analyzed using the ImageJ software. The regions of interest (ROIs) were defined and the number of cells in the ROIs were counted. Then, the integrated density value (IDV) of fluorescence in the ROIs was analyzed. Average levels of ROS = IDV/the average number of cells.
For total SOD determination, the cells were suspended in 130 mM KCl plus 50 mM PBS supplemented with 0.1 ml of 0.1 M dithiothreitol. The cells were centrifuged at 10,000 rpm for 15 min at 4 °C, and the supernatant was collected for biochemical evaluation. To determine total SOD activity, a previously described method based on the inhibition of the formation of the NADH–PMS–NBT complex was used [24].
SIRT1 Knockdown
For our SIRT1 knockdown experiment, the SIRT1-specific DNA sequence was targeted using a SIRT1 siRNA-based approach. We transfected ATDC5 chondrocytes with SIRT1 siRNA (siSIRT1: 5′-CCACCUGAGUUGGAUGAUA-3′) using Lipofectamine RNAi Max reagent (Thermo Fisher Scientific, USA) in accordance with the manufacturer’s instructions. The transfected cells were grown in a 5% O2/ 95% CO2 incubator at 37 °C for 48–72 to silence SIRT1 expression. To verify successful knockdown, Western blot analysis was performed by blotting SIRT1 protein against its specific antibody.
Statistical Analysis
All experiments were repeated in triplicate, and the experimental data are presented as means ± standard deviation (S.D.). Comparisons between groups were performed using the ANOVA method followed by Boneferri’s post hoc test (SPSS, version 22.0). An indexed value of P < 0.05 was deemed statistically significant.
RESULTS
Juglanin Prevents LPS-Induced Oxidative Stress in ATDC5 Chondrocytes
Firstly, we assessed the effects of juglanin on LPS-induced oxidative stress by measuring the ROS, SOD, and NOX4. Our results show that LPS induced a 3.8-fold increase in ROS, which was reduced to 2.4- and 1.5-fold by 2.5 and 5 μM juglanin (Fig. 2a). Meanwhile, LPS induced a decrease in total SOD activity of 58%, which was rescued to decreases of only 29% and 12% by the two respective doses of juglanin (Fig. 2b). In the presence of LPS alone, the gene and protein expression of NOX4 was increased to 3.7- and 3.3-fold, while the two doses of juglanin dose-responsively reduced the gene expression of NOX4 to 2.6- and 1.8-fold, and the protein expression to 2.4- and 1.6-fold (Fig. 3a, b). Thus, juglanin treatment can reduce LPS-induced oxidative stress by downregulating NOX4-mediated ROS production and preserving the level of the antioxidant SOD.
Juglanin prevented LPS-induced oxidative stress in ATDC5 chondrocytes. Cells were treated with 1 μg/mL LPS in the presence or absence of juglanin (2.5, 5 μM) for 24 h. a intracellular ROS was measured by dihydroethidium (DHE) staining. Scale bar, 100 μm. B Total SOD activity (n = 4, ****P < 0.0001 vs. vehicle group; ##P < 0.01 vs. LPS group; ^^P < 0.01 vs. LPS + 2.5 μM juglanin).
Juglanin prevented LPS-induced expression of NADPH oxidase 4 (NOX4) in ATDC5 chondrocytes. Cells were treated with 1 μg/mL LPS in the presence or absence of juglanin (2.5, 5 μM) for 24 h. a gene expression of NOX4 as measured by real-time PCR. B protein of NOX4 as measured by Western blot analysis (n = 4, ****P < 0.0001 vs. vehicle group; ##P < 0.01 vs. LPS group; ^^P < 0.01 vs. LPS + 2.5 μM juglanin).
Juglanin Inhibits the Activation of the NLRP3 Inflammasome via TxNIP
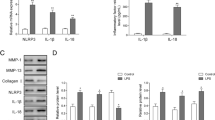
Next, we determined the effects of juglanin treatment on the activation of the NLRP3 inflammasome in chondrocytes induced by LPS. TxNIP binds to the NLRP3 receptor and acts as a key activator of the NLRP3 inflammasome complex. As shown in Fig. 4a, b, LPS induced a 3.5- and 3.1-fold increase in the gene and protein expression of TxNIP, respectively. Meanwhile, the addition of the two doses of juglanin dose-responsively reduced the expression of TxNIP to only 2.4- and 1.8-fold at the gene level, and 2.3- and 1.6-fold at the protein level. We confirmed whether this inhibition of TxNIP suppressed the assembly and activation of the NLRP3 inflammasome by measuring the expression of NLRP3, ASC, and cleaved caspase 1 (p10). As shown in Fig. 5, LPS increased the expression of these three respective molecules by 3.2-, 2.8-, and 3.6-fold. However, upon the addition of 2.5 and 5 μM juglanin, the expression of NLRP3 was reduced to 2.2- and 1.5-fold, ASC was reduced to 2.1- and 1.7-fold, and p10 was reduced to 2.5- and 1.8-fold, showing a noticeable dose-dependent inhibitory effect on NLRP3 inflammasome assembly.
Juglanin prevented LPS-induced expression of TxNIP in ATDC5 chondrocytes. Cells were treated with 1 μg/mL LPS in the presence or absence of juglanin (2.5, 5 μM) for 24 h. a gene expression of TxNIP. B protein of TxNIP as measured (n = 4, ****P < 0.0001 vs. vehicle group; ##P < 0.01 vs. LPS group; ^^P < 0.01 vs. LPS + 2.5 μM juglanin).
Juglanin ameliorated LPS-induced activation of NLRP3 inflammasome in ATDC5 chondrocytes. Cells were treated with 1 μg/mL LPS in the presence or absence of juglanin (2.5, 5 μM) for 24 h. expression of NLRP3, ASC, and cleaved caspase-1 (p10) were measured by Western analysis (n = 4, **P < 0.01 vs. vehicle group; ##P < 0.01 vs. LPS group; ^^P < 0.01 vs. LPS + 2.5 μM juglanin).
Juglanin Inhibits the Production of IL-1β and IL-18
To confirm the inhibition of NLRP3 inflammasome activation, we measured the expression levels of two important proinflammatory cytokines produced by the NLRP3 inflammasome, IL-1β and IL-18. The importance of these two cytokines in arthritis has been well-documented [22, 23]. The results of ELISA in Fig. 6a, b show that the protein secretion of IL-1β and IL-18 were significantly increased upon exposure to LPS, but juglanin dose-dependently reduced this increase in their expression by more than half. Thus, juglanin successfully prevented the production of IL-1β and IL-18 by inhibiting the assembly and activation of the NLRP3 inflammasome.
Juglanin ameliorated LPS-induced secretions of IL-1β and IL-18 in ATDC5 chondrocytes. Cells were treated with 1 μg/mL LPS in the presence or absence of juglanin (2.5, 5 μM) for 24 h. a secretions of IL-1β. b. Secretions of IL-18 (n = 5, ****P < 0.0001 vs. vehicle group; ##P < 0.01 vs. LPS group; ^^P < 0.01 vs. LPS + 2.5 μM juglanin).
The Effects of Juglanin Are Mediated through SIRT1
We determined whether the SIRT1 protective pathway was involved in mediating the effects of juglanin described above. SIRT1 has been shown to suppress NLRP3 activation in various cell types, but the exact involvement of the SIRT1/NLRP3 pathway in chondrocytes remains unclear [25]. As shown in Fig. 7a, b, LPS reduced the expression of SIRT1 by about half at both the gene and protein levels, while remarkably, juglanin dose-responsively restored SIRT1 expression to only 7% and 4% below baseline at the respective gene and protein levels. Finally, we performed a SIRT1 siRNA knockdown experiment to assess whether SIRT1 signaling is required for the effects of juglanin. The successful knockdown of SIRT1 is shown in Fig. 8a. The results in Fig. 8b, c show that knockdown of SIRT1 almost completely abolished the ameliorative effect of on LPS-induced increased NLRP3 inflammasome activation and secretion of IL-18. Thus, the ability of juglanin to reduce NLRP3 inflammasome activation and cytokine production is dependent on the SIRT1 pathway.
Juglanin preserved LPS-induced reduction of SIRT1 in ATDC5 chondrocytes. Cells were treated with 1 μg/mL LPS in the presence or absence of juglanin (2.5, 5 μM) for 24 h. a gene expression of SIRT1. B protein of SIRT1 (n = 4, ****P < 0.0001 vs. vehicle group; ##P < 0.01 vs. LPS group; ^^P < 0.01 vs. LPS + 2.5 μM juglanin).
Silencing of SIRT1 abolished the protective effects of juglanin against LPS-induced activation of NLRP3 inflammasome in ATDC5 chondrocytes. Cells were transfected with SIRT1 siRNA, followed by treatment with 1 μg/mL LPS in the presence or absence of juglanin (5 μM) for 24 h. a successful knockdown of SIRT1 (1, 0.46) is shown in Fig. 7a. B knockdown of SIRT1 abolished the inhibitory effects of Juglanin in NLRP3 expression. C secretions of IL-18 (n = 5, ****P < 0.0001 vs. vehicle group; ##P < 0.01 vs. LPS group; ^^P < 0.01 vs. LPS + 2.5 μM juglanin).
DISCUSSION
The inflammatory processes and overproduction of ROS products involved in the development and progression of arthritis are diverse and complex. To test the anti-ROS activity of juglanin, we assessed three different types of redox indicators. Firstly, we measured its effect on DHE oxidation. DHE is oxidized by the superoxide (O2−) and forms hydrogen peroxide (H2O2) by SOD family protein or forms the peroxynitrite, and DHE oxidation reflects ROS reaction from superoxide. Secondly, we surveyed cellular SOD activity which represents the antioxidant capacity to superoxide. Thirdly, we assessed NOX4 expression in cytoplasm, which has been shown to be involved in arthritis development [11, 12]. NOX4 is one of NADPH oxidase complexes, and only releases hydrogen peroxide, so NOX4-derived ROS is a part of the redox reaction in cytoplasm. Our data shows that juglanin significantly reduced cellular oxidative stress by downregulating NOX4 overproduction and ameliorating SOD activity by LPS.
Numerous studies have explored the potential of flavonoids to reduce oxidative stress and chronic inflammation in diseases including arthritis. Flavonoids such as juglanin have been shown to exert a wide range of antioxidant effects [26,27,28]. For example, juglanin has been shown to reduce the production of ROS and cellular senescence in dermal fibroblasts [29]. Additionally, it has been demonstrated that juglanin can induce breast cancer cell apoptosis and autophagy through ROS/JNK signaling [30]. Other flavonoids have been demonstrated to reduce NOX4 signaling [31], but the effects of juglanin on NOX4 have not been thoroughly assessed. Here, we found that, concordant with previous research, treatment with juglanin could significantly reduce the production of ROS, while ameliorating the LPS-induced decrease in total SOD activity. The inhibitory effect of juglanin on ROS production is likely the result of its inhibitory effect on NOX4 expression demonstrated in our study. These findings suggest a significant antioxidant effect of juglanin in the arthritis microenvironment.
The NLRP3 inflammasome has been receiving increasing attention for its potential as a treatment target against arthritis. Flavonoids have been demonstrated to inhibit the activation of NLRP3 in an array of tissues, cell types, and diseases, including kidney, colon, and ischemia/reperfusion injury, and gout arthritis [32]. The citrus flavonoid rutin has been found to inhibit NOX4 expression as well as activation of the TxNIP/NLRP3/caspase-1/IL-1β axis in vivo [33]. Another study found that the flavonoid morin could inhibit inflammation in an IL-1β-stimulated arthritis chondrocyte cell model [34]. Interestingly, a recent study found that the flavonoid curcumin could protect against arthritis by inhibiting the release of TNF-α, IL-1β, and cleaved caspase 1, and suppressing the activation of the NLRP3 inflammasome [35]. Honokiol, another flavonoid, has been shown to alleviate intravertebral disc degradation by preventing the activation of the inflammatory TxNIP/NLRP3/caspase-1/IL-1β axis [36]. In the present study, we show that juglanin can suppress the activation of the TxNIP/NLRP3/ASC/caspase-1 axis and the subsequent assembly and activation of the NLRP3 inflammasome. Additionally, we confirmed this inhibition by demonstrating a corresponding decrease in the production of IL-1β and IL-18, the two products of the NLRP3 inflammasome.
The SIRT1 signaling pathway is regarded as a key protective mechanism in arthritis. Studies have shown that flavonoids can modulate the expression of SIRT1, which may be useful in the treatment of a wide range of diseases, including cancers, diabetes, aging, and arthritis [37]. In healthy cartilage, SIRT1 is expressed to maintain cartilage homeostasis, but upon short-term exposure of chondrocytes to inflammatory cytokines, SIRT1 takes on a protective role by promoting cell survival and preventing degradation of the cartilage ECM. In severe arthritis, however, when chondrocytes have suffered long-term exposure to cytokines, SIRT1 expression is barely detectable and cartilage undergoes excessive degradation [38]. Previous research has demonstrated the inhibitory effect of SIRT1 on NLRP3 inflammasome activation by downregulating the expression of NLRP3, ASC, and caspase-1, which is consistent with our findings [39]. Here, we found that the inhibitory effects of juglanin on NLRP3 inflammasome activation were abolished in SIRT1-silent chondrocytes, thereby demonstrating the reliance of juglanin on SIRT1 to mediate its anti-inflammatory effects. A representative schematic of the molecular mechanisms is shown in Fig. 9.
There are several limitations to the current study. We only investigated the beneficial effects of Juglanin against LPS-induced activation of NLRP3 inflammasome in ATDC5 chondrocytes. It has to be realized that the pathophysiology of arthritis is complex. A variety of risk factors have been associated with the initiation and progression of arthritis, including genetics, aging, and joint injuries. Further in vivo experiments using animal models and clinical trials should be performed to further explore the pharmacological function of Juglanin in arthritis.
In summary, our findings demonstrate a distinct ability of juglanin to mitigate LPS-induced inflammation in chondrocytes by improving the oxidant/antioxidant ratio and inhibiting the activation of the NLRP3 inflammasome through modulating SIRT1 expression. While these results show a promising multi-functional anti-inflammatory capacity of juglanin, further research is required to determine whether these same results are achievable in vivo.
Data Availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Khan, N.M., A. Haseeb, M.Y. Ansari, P. Devarapalli, S. Haynie, and T.M. Haqqi. 2017. Wogonin, a plant derived small molecule, exerts potent anti-inflammatory and chondroprotective effects through the activation of ROS/ERK/Nrf2 signaling pathways in human osteoarthritis chondrocytes. Free Radical Biology and Medicine. 106: 288–301.
Singh, P., K.B. Marcu, M.B. Goldring, and M. Otero. 2019. Phenotypic instability of chondrocytes in osteoarthritis: On a path to hypertrophy. Annals of the New York Academy of Sciences. 1442 (1): 17–34.
Zhuang, Z., G. Ye, and B. Huang. 2017. Kaempferol alleviates the interleukin-1β-induced inflammation in rat osteoarthritis chondrocytes via suppression of NF-κB. Medical Science Monitor: International Medical Journal of Experimental and Clinical Research. 23: 3925–3931.
Dreier, R. 2010. Hypertrophic differentiation of chondrocytes in osteoarthritis: The developmental aspect of degenerative joint disorders. Arthritis research & therapy. 12 (5): 216.
Bauernfeind, F.G., G. Horvath, A. Stutz, E.S. Alnemri, K. MacDonald, D. Speert, Z. Huang, T. Stabler, F. Pei, and V. Kraus. 2016. Both systemic and local lipopolysaccharide (LPS) burden is associated with knee osteoarthritis (OA). Osteoarthritis and Cartilage. 24: S329–S330.
Coant, N., M. Simon-Rudler, T. Gustot, M. Fasseu, S. Gandoura, K. Ragot, W. Abdel-Razek, D. Thabut, P. Lettéron, E. Ogier-Denis, and R. Ouziel. 2011. Glycogen synthase kinase 3 involvement in the excessive proinflammatory response to LPS in patients with decompensated cirrhosis. Journal of hepatology. 55 (4): 784–793.
Luo, X., J. Wang, X. Wei, S. Wang, and A. Wang. 2019. Knockdown of lncRNA MFI2-AS1 inhibits lipopolysaccharide-induced osteoarthritis progression by miR-130a-3p/TCF4. Life sciences. 117019.
Fernandes-Alnemri, T., J. Wu, B.G. Monks, K.A. Fitzgerald, and V. Hornung. 2009. Cutting edge: NF-κB activating pattern recognition and cytokine receptors license NLRP3 inflammasome activation by regulating NLRP3 expression. The Journal of Immunology. 183 (2): 787–791.
X. Yu, P. Lan, X. Hou, Q. Han, N. Lu, T. Li, C. Jiao, J. Zhang, C. Zhang, Z. Tian HBV inhibits LPS-induced NLRP3 inflammasome activation and IL-1β production via suppressing the NF-κB pathway and ROS production. Journal of hepatology. 2017;66(4):693–702.
Lepetsos, P., and A.G. Papavassiliou. 2016. ROS/oxidative stress signaling in osteoarthritis. Biochimica et Biophysica Acta 1862 (4): 576–591.
Drevet, S., G. Gavazzi, L. Grange, C. Dupuy, and B. Lardy. 2018. Reactive oxygen species and NADPH oxidase 4 involvement in osteoarthritis. Experimental gerontology. 111: 107–117.
Clavijo-Cornejo, D., K. Martínez-Flores, K. Silva-Luna, G.A. Martínez-Nava, J. Fernández-Torres, Y. Zamudio-Cuevas, M. Guadalupe Santamaría-Olmedo, J. Granados-Montiel, C. Pineda, and A. López-Reyes. 2016. The overexpression of NALP3 inflammasome in knee osteoarthritis is associated with synovial membrane prolidase and NADPH oxidase 2. Oxidative Medicine and Cellular Longevity 2016: 1472567.
Tiku, M.L., S. Gupta, and D.R. Deshmukh. 1999. Aggrecan degradation in chondrocytes is mediated by reactive oxygen species and protected by antioxidants. Free Radical Research 30 (5): 395–405.
Mitroulis, I., P. Skendros, and K. Ritis. 2010. Targeting IL-1β in disease; the expanding role of NLRP3 inflammasome. European journal of internal medicine. 21 (3): 157–163.
Jiao, P., W. Li, L. Shen, Y. Li, L. Yu, and Z. Liu. 2020. The protective effect of doxofylline against lipopolysaccharides (LPS)-induced activation of NLRP3 inflammasome is mediated by SIRT1 in human pulmonary bronchial epithelial cells. Artif Cells Nanomed Biotechnol. 48 (1): 687–694.
Chen, H., J. Qi, Q. Bi, and S. Zhang. 2017. Suppression of miR-301a alleviates LPS-induced inflammatory injury in ATDC5 chondrogenic cells by targeting Sirt1. International Journal of Clinical and Experimental Pathology 10: 8991–9000.
Zheng, W., Z. Feng, S. You, H. Zhang, Z. Tao, Q. Wang, H. Chen, and Y. Wu. 2017. Fisetin inhibits IL-1β-induced inflammatory response in human osteoarthritis chondrocytes through activating SIRT1 and attenuates the progression of osteoarthritis in mice. International Immunopharmacology 45: 135–147.
Jamali-Raeufy, N., S. Kardgar, T. Baluchnejadmojarad, M. Roghani, and M. Goudarzi. 2019. Troxerutin exerts neuroprotection against lipopolysaccharide (LPS) induced oxidative stress and neuroinflammation through targeting SIRT1/SIRT3 signaling pathway. Metabolic brain disease. 34 (5): 1505–1513.
Li, Y., X. Yang, Y. He, W. Wang, J. Zhang, W. Zhang, T. Jing, B. Wang, and R. Lin. 2017. Negative regulation of NLRP3 inflammasome by SIRT1 in vascular endothelial cells. Immunobiology. 222 (3): 552–561.
Bougault, C., M. Gosset, X. Houard, C. Salvat, L. Godmann, T. Pap, C. Jacques, and F. Berenbaum. 2012. Stress-induced cartilage degradation does not depend on the NLRP3 inflammasome in human osteoarthritis and mouse models. Arthritis and Rheumatism 64 (12): 3972–3981.
Wang, C., Y. Gao, Z. Zhang, C. Chen, Q. Chi, K. Xu, and L. Yang. 2020. Ursolic acid protects chondrocytes, exhibits anti-inflammatory properties via regulation of the NF-κB/NLRP3 inflammasome pathway and ameliorates osteoarthritis. Biomedicine & Pharmacotherapy 130: 110568.
Zhou, G.Y., Y.X. Yi, L.X. Jin, W. Lin, P.P. Fang, X.Z. Lin, Y. Zheng, and C.W. Pan. 2016. The protective effect of juglanin on fructose-induced hepatitis by inhibiting inflammation and apoptosis through TLR4 and JAK2/STAT3 signaling pathways in fructose-fed rats. Biomedicine & Pharmacotherapy 81: 318–328.
Chen, X., C. Zhang, X. Wang, and S. Huo. 2019. Juglanin inhibits IL-1β-induced inflammation in human chondrocytes. Artificial cells, nanomedicine, and biotechnology. 47 (1): 3614–3620.
Kakkar, Z.Y.P., B. Das, and P.N. Viswanathan. 1984. A modified spectrophotometeric assay of superoxide dismutase (SOD). Ind. J. Biochem. Biophys 21: 130–132.
Li, Y., P. Wang, X. Yang, W. Wang, J. Zhang, Y. He, W. Zhang, T. Jing, B. Wang, and R. Lin. 2016. SIRT1 inhibits inflammatory response partly through regulation of NLRP3 inflammasome in vascular endothelial cells. Molecular immunology. 77: 148–156.
Van Kiem, P., N.T. Mai, C. Van Minh, N.H. Khoi, N.H. Dang, N.P. Thao, N.X. Cuong, N.H. Nam, N.X. Nhiem, Y. Vander Heyden, and J. Quetin-Leclercq. 2010. Two new C-glucosyl benzoic acids and flavonoids from Mallotus nanus and their antioxidant activity. Archives of pharmacal research. 33 (2): 203–208.
Torel, J., J. Cillard, and P. Cillard. 1986. Antioxidant activity of flavonoids and reactivity with peroxy radical. Phytochemistry. 25 (2): 383–385.
Burda, S., and W. Oleszek. 2001. Antioxidant and antiradical activities of flavonoids. Journal of agricultural and food chemistry. 49 (6): 2774–2779.
Yang, H.H., K. Hwangbo, M.S. Zheng, J.K. Son, H.Y. Kim, S.H. Baek, H.C. Choi, S.Y. Park, and J.R. Kim. 2014. Inhibitory effects of juglanin on cellular senescence in human dermal fibroblasts. Journal of natural medicines. 68 (3): 473–480.
Sun, Z.L., J.L. Dong, and J. Wu. 2017. Juglanin induces apoptosis and autophagy in human breast cancer progression via ROS/JNK promotion. Biomedicine & Pharmacotherapy. 85: 303–312.
Ugusman, A., Z. Zakaria, C.K. Hui, N.A. Nordin, and Z.A. Mahdy. 2012. Flavonoids of Piper sarmentosum and its cytoprotective effects against oxidative stress. EXCLI journal. 11: 705.
Lim, H., M.Y. Heo, and H.P. Kim. 2019. Flavonoids: Broad spectrum agents on chronic inflammation. Biomolecules & Therapeutics 27 (3): 241.
Wang, W., Q.H. Wu, Y. Sui, Y. Wang, and X. Qiu. 2017. Rutin protects endothelial dysfunction by disturbing Nox4 and ROS-sensitive NLRP3 inflammasome. Biomedicine & Pharmacotherapy. 86: 32–40.
Qu, Y., C. Wang, N. Liu, C. Gao, and F. Liu. 2018. Morin exhibits anti-inflammatory effects on IL-1β-stimulated human osteoarthritis chondrocytes by activating the Nrf2 signaling pathway. Cellular Physiology and Biochemistry. 51 (4): 1830–1838.
Sun, Y., W. Liu, H. Zhang, H. Li, J. Liu, F. Zhang, T. Jiang, and S. Jiang. 2017. Curcumin prevents osteoarthritis by inhibiting the activation of inflammasome NLRP3. Journal of Interferon & Cytokine Research. 37 (10): 449–455.
Tang, P., J.M. Gu, Z.A. Xie, Y. Gu, Z.W. Jie, K.M. Huang, J.Y. Wang, S.W. Fan, X.S. Jiang, and Z.J. Hu. 2018. Honokiol alleviates the degeneration of intervertebral disc via suppressing the activation of TXNIP-NLRP3 inflammasome signal pathway. Free Radical Biology and Medicine. 120: 368–379.
Ayissi, V.B., A. Ebrahimi, and H. Schluesenner. 2014. Epigenetic effects of natural polyphenols: A focus on SIRT1-mediated mechanisms. Molecular nutrition & food research. 58 (1): 22–32.
Dvir-Ginzberg, M., and J. Steinmeyer. 2013. Towards elucidating the role of SirT1 in osteoarthritis. Frontiers in bioscience (Landmark edition) 18: 343–355.
Zhang, S., L. Jiang, F. Che, Y. Lu, Z. Xie, and H. Wang. 2017. Arctigenin attenuates ischemic stroke via SIRT1-dependent inhibition of NLRP3 inflammasome. Biochemical and biophysical research communications. 493 (1): 821–826.
Author information
Authors and Affiliations
Contributions
Tingting Wang and Yishuo Li contributed to the study conception, experimental design, and data analysis; Tingting Wang, Jiakai Wang, and Tao Sun contributed to investigation and data collection; Yishuo Li contributed to the draft writing.
Corresponding author
Ethics declarations
Competing Interests
The authors declare that they have no conflict of interest.
Consent for Publication
All authors read and approved the final manuscript.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wang, T., Wang, J., Sun, T. et al. Amelioration of Juglanin against LPS-Induced Activation of NLRP3 Inflammasome in Chondrocytes Mediated by SIRT1. Inflammation 44, 1119–1129 (2021). https://doi.org/10.1007/s10753-020-01407-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-020-01407-6