Abstract
Systemic lupus erythematosus (SLE) is a multisystem disease affecting many organs, and the most severe complication is lupus nephritis. Podocyte injury and loss play vital roles in the pathogenesis of lupus nephritis. Studies have shown that ubiquitin carboxyl-terminal hydrolase L1 (UCH-L1) is involved in the pathogenesis and progression of many diseases, such as neurodegenerative disorders, cancers, and diabetes. Recently, numerous studies have indicated that UCH-L1 was upregulated in the podocytes in immune complex-mediated glomerulonephritis. This increase was correlated with disease aggravation. In this review, we discuss the role and mechanism of UCH-L1 in the pathogenesis of many diseases and, particularly, in lupus nephritis. Hence, we highlight the role of UCH-L1 in lupus nephritis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Systemic lupus erythematosus (SLE) is a chronic autoimmune disease characterized by loss of tolerance against self-antigens, lymphoproliferation, polyclonal autoantibody production, and immune complex deposition, leading to multi-organ injuries [1]. Lupus nephritis is the most severe complication of SLE [2]. Proteinuria is an important risk factor for the progression of renal diseases in patients with lupus nephritis [3]. Podocytes and their slit-diaphragms are vital for the integrity of the renal basement membrane, which acts as a barrier to urinary protein loss. At the early stage of lupus nephritis, podocytes were affected and correlated with the disease histological changes [4]. The loss of podocytes in the urine (also termed podocyturia) has been detected in patients with lupus nephritis, which could be useful in monitoring the disease activity [5, 6]. Recently, studies have shown that ubiquitin C-terminal hydrolase-L1 (UCH-L1) is not expressed in glomerular podocytes of the normal kidney, but de novo expressed and correlated with podocyte injury in lupus nephritis [7–9]. Considering the expression of UCH-L1 in injured glomerular podocytes and the vital role of podocytes in lupus nephritis, we hypothesize that UCH-L1 may be a target for the treatment of this disease. In this review, we discussed recent development of UCH-L1 in the pathogenesis of many diseases and in particular lupus nephritis, with a view of providing insights into the pathogenesis and treatment of lupus nephritis.
LUPUS NEPHRITIS
Studies have revealed that up to 2/3 of SLE patients develop glomerular injury, which is denoted as lupus nephritis, due to immune complex deposition [10]. Approximately 60% of those patients develop a proliferative form of lupus nephritis (termed class III or IV), while 20–40% develop membranous lupus nephritis (class V) [10, 11]. The ISN classification of lupus nephritis was reviewed in ref. [12]. Clinically, proteinuria and hematuria are two characteristic features in patients with lupus nephritis. The pathogenesis of lupus nephritis is a complex process (Table 1). Both the adaptive and innate immune systems contribute to the development of lupus nephritis. In the adaptive immune system, B lymphocytes (B cells) and T lymphocytes (T cells) are essential for the development of lupus nephritis [13, 14]. Activation of B cells and their maturation to plasma cells promote the production of autoantibodies (like anti-DNA antibodies and anti-nucleosome antibodies) and proinflammatory cytokines [15]. T cells provide help for B cell production of nephritogenic autoantibodies, regulate B cell responses, and modulate T helper and effector functions and expansion. T cells infiltrate the kidney to injure parenchymal cells directly via cytotoxicity or indirectly through activation and recruitment of macrophages and natural killer (NK) cells [16, 17]. The innate immune system contributes to the pathogenesis of lupus nephritis in multiple ways. In the early stages of the disease, dendritic and other myeloid cells activate T cells, and produce key mediators including B cell-activating factor, which results in the activation of the adaptive immune system [18, 19]. The complement system, a key component of the innate immune system, is thought to play an important role in the pathogenesis of lupus nephritis [20], and the exact mechanism was shown in refs. [20] and [21]. Autophagy, which is involved in autoimmunity, plays a vital role in maintaining the homeostasis of T cell and B cell [22]. Genome-wide association studies reveal that autophagy-relative genes such as apolipoprotein L1 (APOL1) and myotubularin-related phosphatase 3 (MTMR3) are associated with lupus nephritis, which highlighted the vital role of autophagy in the pathogenesis of lupus nephritis [23–26]. Cell death can result in the release of chromatin or nucleosomes. These not only activate the immune system but also act as the driving antigens in the induction of anti-double-stranded (ds) DNA autoantibodies, which is a hallmark of SLE. Subsequently, the formed immune complex is deposited within the basement membranes and the mesangial matrix of glomeruli. This indicates that cell death may be an initiating event in lupus nephritis [27]. Currently, the pathogenesis of lupus nephritis has not been fully understood, here we provided the newly identified theory in this process.
PODOCYTE INJURY
Podocytes, also called visceral glomerular epithelial cells, are highly differentiated cells that line the outside of the glomerular capillary. They comprise a cell body with extending major processes that further branch into foot processes separated by a slit-diaphragm, which is an electron-dense membrane that spans the 30-nm space between their interdigitating foot processes [28]. The podocyte architecture is predominantly maintained by a contractile apparatus composed of microfilaments including actin, myosins, α-actinin, talin, vinculin, paxillin, and palladin [29–31]. Previously, it was thought that podocytes are static cells; time-lapse imaging showed the dynamics of podocyte movement, shedding, and replacement [32]. Podocytes are a part of the glomerular filtration barrier together with capillary endothelial cells and the glomerular basement membrane (GBM), which ensures the selective permeability of the glomerular capillary wall [28]. Besides the filtration barrier to protein, podocytes also possess other critical roles like a charge barrier to protein, maintaining the capillary loop shape, synthesizing and maintaining the GBM, counteracting the intraglomerular pressure, and producing and secreting vascular endothelial growth factor required for glomerular endothelial cell integrity [33].
Proteinuria, a common manifestation in lupus nephritis, reflects podocyte injury. Injury to the podocyte leads to a loss of interdigitating foot processes with detachment from the GBM and disruption of the glomerular sieve and charge-selective barrier resulting in massive proteinuria [34]. The proteins expressed by podocytes are vital for the integrity of the filtration barrier in lupus nephritis (Table 2) [35, 36]. Synaptopodin is a proline-rich actin-associated protein. It mainly distributes the cytoplasm of glomerular podocytes and plays a role in the regulation of the actin-based shape and motility of the podocyte foot processes [37]. Glomerular epithelial protein 1 (GLEPP1) is a membrane protein tyrosine phosphatase. It acts as a cellular receptor, which is involved in regulatory mechanisms related to the foot process structure and/or function [38]. Podocalyxin, a CD34-related sialomucin, is normally located at the apical part of the foot process. The absence or the change of spatial organization both has a detrimental effect on the glomerular filtration function [39, 40]. Nephrin and podocin are the main protein components of the slit-diaphragm in podocytes. They are significantly reduced in the earlier stages of lupus nephritis and their expression correlates with disease histology [4]. Wilms tumor protein 1 (WT1), a nuclear zinc finger transcription factor, is implicated in cell cycle regulation and cell proliferation [41].
Recently, podocyturia has been found to be involved in the progression of lupus nephritis [42, 43]. Nakamura et al. [43] showed that podocytes were present in the urine of active lupus nephritis but not in SLE patients with stable renal function or healthy controls. The number of urinary podocytes was correlated with the proteinuria and hematuria excretion scores. Also, Mansur and co-workers reported that the levels of podocyturia were higher in patients with lupus nephritis particularly in class IV than in the controls [6]. Treatment with corticosteroids, cyclophosphamide, or azathioprine significantly diminished the podocyturia in patients with lupus nephritis [44]. Renal biopsy remains the gold standard for the diagnosis and prognosis of lupus nephritis; however, it is an invasive method. Perez-Hernandez and colleagues discovered that urinary dedifferentiated podocytes were found in active lupus nephritis, and the levels of podocyte-specific protein podocalyxin, synapotopodin, podocin, nephrin, and WT-1 were significantly increased and correlated with proteinuria and histological features in lupus nephritis patients [45]. These results suggest that podocyturia could be a potentially useful non-invasive marker for evaluating the progression of glomerular disease including lupus nephritis [45].
Currently, the potential mechanisms of podocyte injury in lupus nephritis remain not fully understood. Here, we summarized the recent papers relevant to podocyte injury in lupus nephritis. Smad7, an inhibitory SMAD, is activated in injured podocytes in vitro and in human lupus nephritis. It participates in negative control of transforming growth factor -β/Smad signaling besides its pro-apoptotic activity [46]. Notch activation stimulates human renal progenitors’ entry into the S-phase of the cell cycle and cell division, whereas its downregulation is required for differentiation toward the podocyte lineage. A persistent activation of the Notch pathway would induce podocytes to cross the G2/M checkpoint, resulting in cytoskeleton disruption and cell death. In the glomeruli of healthy adult kidneys, Notch expression was almost absent, however remarkably upregulated in podocytes in patients with glomerular disorders [47]. Neonatal Fc receptor, a newly recognized molecular present on human renal podocytes, acts as an immune sensor that evokes an inflammatory response, which may lead to functional and morphological changes in podocytes in glomerulonephritides [48]. Several Toll-like receptors have been found correlated with podocyte injury [49, 50]. miR-26a could regulate podocyte differentiation and cytoskeletal integrity in lupus nephritis [51]. Studies found that podocyte injury is also associated with T cells-induced intrarenal macrophage infiltration [52]. Additionally, podocytes in lupus nephritis can exert dendritic cell-like function through expression of dendritic cell-specific intercellular adhesion molecule-3-grabbing non-integrin (DC-SIGN), which may be involved in immune and inflammatory responses of renal tissues. Blockage of DC-SIGN can inhibit immune functions of podocytes [53].
UCH-L1
The ubiquitin proteasome system (UPS), one of the major intracellular protein degradation systems, is composed of ubiquitin, ubiquitination enzymes, deubiquitination enzymes (DUBs), and proteasomes. Ubiquitin is a highly conserved 76-amino acid protein, which can be covalently attached to a target protein by ubiquitination enzymes during the ubiquitination process occurring through a three-step sequential action of ubiquitin activating enzyme (E1), ubiquitin carrier protein (E2), and ubiquitin protein ligase (E3). Initially, ubiquitin is activated by E1 through the ATP-dependent manner forming a high energy thioester linkage between the carboxy-terminal glycine residue of ubiquitin and the active cysteine of the E1 enzyme. Subsequently, activated ubiquitin is then transferred to a cysteine residue of an E2 enzyme, and then an E3 enzyme transfers ubiquitin to lysine residues of the targeted protein, forming a polyubiquitin chain (Lys48) that is recognized by the 26S proteasome leading to its degradation [54]. The action of DUBs was opposite to that of the E3 ligases. DUBs cleave the isopeptide bonds between the C-terminal glycine of ubiquitin and lysine residues of targeted proteins to allow for free ubiquitin monomers to be recycled [55].
The ubiquitin carboxyl-terminal hydrolase L1 (UCH-L1) gene, also known as neuronal-specific protein gene product 9.5, is located on chromosome 4 (4p14) and encode a peptide of 223 amino acids [56, 57]. UCH-L1 was firstly discovered as a member of the ubiquitin carboxy-terminal hydrolase family of DUBs catalyzing the hydrolysis of Lys48-linked ubiquitin chains [58]. Moreover, UCH-L1 possesses ATPase-independent dimerization-dependent ubiquitin ligase activity for the Lys63 residue of the ubiquitin molecule, forming undegradable (K63) polyubiquitin chains, which could inhibit proteasomal activity [59]. Additionally, UCH-L1 plays a role in the homeostasis of ubiquitin monomers, where UCH-L1 appears to regulate the degradation of free ubiquitin monomers in cells [58].
Studies have found that UCH-L1 is implicated in the pathogenesis of many diseases. Previously, studies showed that UCH-L1 is exclusively expressed in neurons [58]. Dysfunction of the UPS has been implicated in the pathogenesis of neurodegenerative disorders. Downregulation and extensive oxidative modification of UCH-L1 have been discovered in the brains of patients with Alzheimer’s disease (AD) as well as Parkinson’s disease (PD) [60]. In AD brains, UCH-L1 was negatively related to neurofibrillary tangles whose major component is hyperphosphorylated tau protein, and inhibition of the activity and expression of UCH-L1 decreased microtubule-binding ability and increased the phosphorylation of tau protein, induced the abnormal aggregation and ubiquitination of tau protein [61]. The administration of UCH-L1 was shown to alleviate β-amyloid-induced synaptic dysfunction and memory loss in AD mouse models, demonstrating that UCH-L1 is associated with the proteasomal degradation of PKA-regulatory subunit IIα. The freed catalytic subunit is then activated and can phosphorylate cAMP response element binding protein (CREB) and initiate transcription [62]. In PD, UCH-L1 was found to co-aggregate with α-synuclein, the major component of Lewy bodies. Cartier et al. [63] revealed that suppression of UCH-L1 activity induced its ligase activity increasing α-synuclein levels and resulted in a concomitant accumulation of presynaptic α-synuclein in neurons. These results suggest that the downregulation of UCH-L1 could result in the accumulation of regulators or key materials in neurodegenerative diseases.
Studies also showed that UCH-L1 is associated with the pathogenesis of cancers. Proteomic screens have revealed that UCH-L1 is expressed in many human tumors. It not only functions as a positive regulator in the growth and development of some tumors but also acts as a putative tumor suppressor in certain cancer subtypes (for a recent review, see [64]). Studies indicated that the disruption of UPS function is involved in cancer pathogenesis and progression [65]. The abnormal expression of UCH-L1 may indirectly alter both the poly- and mono-ubiquitination of oncogenes and tumor suppressors, leading to aberrant protein degradation and/or altered protein function and subsequent tumorigenesis [64].
Additionally, studies found that UCH-L1 was abundantly expressed in rat and human β cells, while accumulation of polyubiquinated proteins and UCH-L1 deficiency was found in β cells of humans with type 2 diabetes [66, 67] (Table 3). Increased expression of human- islet amyloid polypeptide (h-IAPP) can lead to the formation of h-IAPP toxic oligomers and accumulation of poly-ubiquitinated proteins associated with decreased UCH-L1 availability. Downregulation of UCH-L1 expression and activity in β cells-induced endoplasmic reticulum stress leading to cell apoptosis [67]. This indicates that defective protein degradation in β cells in type 2 diabetes can be attributed, at least in part, to the misfolded islet amyloid polypeptide, leading to UCH-L1 deficiency. This further decreases free monomeric ubiquitin to initiate the accumulation and aggregation of proteins, causing β cell injury.
UCH-L1 AND PODOCYTES
Recently, much attention has been drawn to the expression and role of UCH-L1 in glomerular diseases. Normal kidney podocytes did not express UCH-L1. In 2008, Liu et al. [68] firstly found that UCH-L1 was obvious in the cytoplasm and processes of podocytes in the specimens of human IgA nephropathy and lupus nephritis via pre-embedding immunoelectron microscopy technique with gold and horseradish peroxidase labeling. Subsequently, Meyer-Schwesinger and colleagues also discovered that a subset of human glomerulopathies involved in podocyte foot process effacement (membranous glomerulonephritis (GN), SLE class V, focal segmental glomerular sclerosis (FSGS)) de novo strongly expressed UCH-L1 in podocyte cell bodies, nuclei, and processes. The expression of UCH-L1 is correlated with internalization of the podocyte-specific proteins nephrin and α-actinin-4 [8]. In contrast, glomerular diseases typically not associated with foot process effacement (SLE class IV, ANCA + necrotizing glomerulonephritis, amyloidosis, IgA nephropathy) expressed low levels of UCH-L1 [8]. Moreover, UCH-L1 expression in podocytes is inversely correlated with podocyte differentiation in cultured human podocytes: higher in undifferentiated cells, lower in differentiated and arborized cells, where expression is accompanied by an increase in podocyte-specific actin-binding protein α-actinin-4, nephrin, and synaptopodin [8]. LDN57444, a specific inhibitor of UCH-L1, led to a time- and concentration-dependent process formation with podocyte-specific protein α-actinin-4 distribution to the cell membrane and processes, suggesting that UCH-L1 plays a role in podocyte differentiation and injury [8]. Additionally, Liu and co-workers reported that UCH-L1 was expressed in podocytes and its expression was remarkably higher in acute proliferative glomerulonephritis (APGN), lupus nephritis, membranous GN, and IgA nephropathy than that in FSGS, minimal change disease (MCD), minor abnormality, and normal kidney tissues. The percentage of PCNA-positive podocytes in lupus nephritis, APGN, and IgA nephropathy was much higher than that in MCD, FSGS, and normal control [7]. These studies showed that the expression of UCH-L1 was contradictory in FSGS and IgA nephropathy, this may be attributed to the small samples or geographical limitations. In any case, UCH-L1 expression in the kidney podocytes of lupus nephritis is significantly higher than normal kidney tissues, and the increased UCH-L1 is apparently responsible for disease aggravation.
Ubiquitin expression was very low in podocytes from normal kidney biopsies; increased expression correlated with UCH-L1 in glomerular diseases [8]. Further studies found that the increased UCH-L1 expression coincided with decreased glomerular mono-ubiquitin content and impaired the UPS in membranous GN. Inhibition of UCH-L1 with LDN57444 reduced UPS impairment and ameliorated proteinuria, whereas inhibition of proteasomal activity enhanced UPS impairment, leading to increased proteinuria [69]. In cultured podocytes, stable overexpression of UCH-L1 resulted in the accumulation of mono-ubiquitin and poly-ubiquitin proteins, while knock-down of UCH-L1 reduced mono-ubiquitin and poly-ubiquitin proteins and notably increased proteasomal activity [69]. These results indicate that UCH-L1 regulates the mono-ubiquitin pool and induces the accumulation and aggregation of poly-ubiquitinated proteins in injured podocytes in membranous GN. Additionally, Lohmann et al. [70] revealed that UCH-L1 enhanced podocyte cytoplasmic p27Kip1 levels by nuclear export and decreased poly-ubiquitination and proteasomal degradation of p27Kip1 to increase the total protein content, leading to podocyte hypertrophy in membranous GN. In lupus nephritis, the increased UCH-L1 expression in podocytes decreases the mono-ubiquitin pool and impairs UPS, causing the accumulation of total protein and resulting in podocyte injury.
To further investigate the regulation mechanism of UCH-L1 in injured podocytes in glomerulonephritis. Zhang et al. [71] firstly found that stimulation of podocytes with the cytokines TNF-α and IL-1β upregulated UCH-L1 expression, while inhibited by the transcription factor nuclear factor-κB (NF-κB) specific inhibitor pyrrolidine dithiocarbamate. The electrophoretic mobility shift assay showed that NF-κB upregulates UCH-L1 via binding the −300- and −109-bp sites of its promoter. Moreover, the expression of NF-κB and UCH-L1 increased and was positively correlated in the renal biopsy from lupus nephritis patients. Activation of NF-κB upregulates UCH-L1 expression following changing of other podocytes molecules like nephrin and snail [71]. This group further revealed that the increases in levels of NF-κB and UCH-L1 were positively correlated with the number of diseased podocytes in human renal biopsies from several cases of immune complex-mediated GN, including lupus nephritis [9]. In contrast, no clear activation of NF-κB and increase of UCH-L1 expression was observed in non-immune complex-mediated GN [9]. In cultured murine podocytes, immune stimulation also led to the upregulation of UCH-L1 through the NF-κB signaling [9]. Collectively, these results indicate that UCH-L1 is upregulated by NF-κB and correlated with podocyte injury in lupus nephritis.
CONCLUSIONS AND PERSPECTIVES
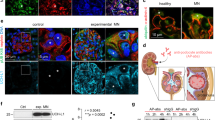
Podocytes, which are terminally differentiated cells, respond to injury with foot-process retraction, hypertrophy, hyperplasia, and loss, which ultimately results in proteinuria in lupus nephritis. The urinary dedifferentiated podocytes were detected and correlated with proteinuria and histological features of lupus nephritis, indicating that it may be a potential non-invasive marker for evaluating the progression of lupus nephritis. UCH-L1, an important DUB, has been found to relate with the progression of neurodegenerative diseases, cancers, and type 2 diabetes. Recently, the role of UCH-L1 in the glomerular diseases has been found. UCH-L1 is not expressed in normal kidney podocytes, but de novo expressed in podocytes of many glomerular diseases including lupus nephritis. The expression is correlated with the number of diseased podocytes, which is responsible for the disease aggravation. So far, no specific marker protein except UCH-L1 has been identified that is absent in healthy but upregulated in diseased podocytes in lupus nephritis. Thus, UCH-L1 could be a marker of histological differentiation between healthy and diseased podocytes or a prediction about prognosis or the degree of podocyte damage [8]. NF-κB, a fundamental intracellular transcription factor, is induced in response to various sources of extracellular stimulation such as proinflammatory cytokine TNF-α (Fig. 1). It is upregulated and correlated with proteinuria and proinflammatory cytokines expression in podocytes of lupus nephritis [72, 73]. Additionally, Brahler and co-workers found that proinflammatory activity of NF-κB in podocytes aggravates proteinuria in experimental GN in mice, suggesting that podocytes may be considered as major regulators of glomerular homeostasis [74]. Thus, UCH-L1, an important downstream target gene of NF-κB, could also provide a specific therapeutic target for lupus nephritis. However, considering the abundantly expression of UCH-L1 in human neurons and β cells, to avoid patients suffering more from AD, PD, or diabetes, the target reduction of UCH-L1 in kidney is of importance in patients with lupus nephritis. Hence, any use of UCH-L1 as a therapeutic in lupus nephritis should be with caution.
NF-κB/UCH-L1 signaling in lupus nephritis. Various stimulations including TNF-α could induce the activation of NF-κB signaling pathway. NF-κB upregulates UCH-L1 expression via binding the −300- and −109-bp sites of its promoter, leading to the injury of podocytes that further contributes to lupus nephritis.
REFERENCES
Lech, M., and H.J. Anders. 2013. The pathogenesis of lupus nephritis. Journal of the American Society of Nephrology 24: 1357–1366.
Maroz, N., and M.S. Segal. 2013. Lupus nephritis and end-stage kidney disease. American Journal of the Medical Sciences 346: 319–323.
Kitamura, N., Y. Matsukawa, M. Takei, and S. Sawada. 2009. Antiproteinuric effect of angiotensin-converting enzyme inhibitors and an angiotensin II receptor blocker in patients with lupus nephritis. Journal of International Medical Research 37: 892–898.
Perysinaki, G.S., D.K. Moysiadis, G. Bertsias, I. Giannopoulou, K. Kyriacou, L. Nakopoulou, D.T. Boumpas, and E. Daphnis. 2011. Podocyte main slit diaphragm proteins, nephrin and podocin, are affected at early stages of lupus nephritis and correlate with disease histology. Lupus 20: 781–791.
Sabino, A.R., P. Teixeira Vde, S.K. Nishida, N. Sass, J.B. Mansur, and G.M. Kirsztajn. 2013. Detection of podocyturia in patients with lupus nephritis. Jornal Brasileiro de Nefrologia 35: 252–258.
Mansur, J.B., A.R. Sabino, S.K. Nishida, and G.M. Kirsztajn. 2016. Is there a role for urinary podocyte excretion assessment in lupus nephritis? Renal Failure 38: 643–647.
Liu, Y., J. Wu, H. Wu, T. Wang, H. Gan, X. Zhang, R. Li, Z. Zhao, Q. Chen, M. Guo, and Z. Zhang. 2009. UCH-L1 expression of podocytes in diseased glomeruli and in vitro. Journal of Pathology 217: 642–653.
Meyer-Schwesinger, C., T.N. Meyer, S. Munster, P. Klug, M. Saleem, U. Helmchen, and R.A. Stahl. 2009. A new role for the neuronal ubiquitin C-terminal hydrolase-L1 (UCH-L1) in podocyte process formation and podocyte injury in human glomerulopathies. Journal of Pathology 217: 452–464.
Zhang, H., X. Mao, Y. Sun, R. Hu, W. Luo, Z. Zhao, Q. Chen, and Z. Zhang. 2015. NF-kappaB upregulates ubiquitin C-terminal hydrolase 1 in diseased podocytes in glomerulonephritis. Molecular Medicine Reports 12: 2893–2901.
Caster, D.J., E.A. Korte, M.L. Merchant, J.B. Klein, D.W. Wilkey, B.H. Rovin, D.J. Birmingham, J.B. Harley, B.L. Cobb, B. Namjou, K.R. McLeish, and D.W. Powell. 2015. Autoantibodies targeting glomerular annexin A2 identify patients with proliferative lupus nephritis. Proteomics Clinical Applications 9: 1012–1020.
Bhinder, S., A. Singh, and V. Majithia. 2010. Membranous (class V) renal disease in systemic lupus erythematosus may be more common than previously reported: results of a 6-year retrospective analysis. American Journal of the Medical Sciences 339: 230–232.
Trivedi, S., M. Zeier, and J. Reiser. 2009. Role of podocytes in lupus nephritis. Nephrology, Dialysis, Transplantation 24: 3607–3612.
Schwartz, N., B. Goilav, and C. Putterman. 2014. The pathogenesis, diagnosis and treatment of lupus nephritis. Current Opinion in Rheumatology 26: 502–509.
Enghard, P., C. Rieder, K. Kopetschke, J.R. Klocke, R. Undeutsch, R. Biesen, D. Dragun, M. Gollasch, U. Schneider, K. Aupperle, J.Y. Humrich, F. Hiepe, M. Backhaus, A.H. Radbruch, G.R. Burmester, and G. Riemekasten. 2014. Urinary CD4 T cells identify SLE patients with proliferative lupus nephritis and can be used to monitor treatment response. Annals of the Rheumatic Diseases 73: 277–283.
Liu, Y., and H.J. Anders. 2014. Lupus nephritis: from pathogenesis to targets for biologic treatment. Nephron. Clinical Practice 128: 224–231.
Okamoto, A., K. Fujio, N.H. Tsuno, K. Takahashi, and K. Yamamoto. 2012. Kidney-infiltrating CD4+ T-cell clones promote nephritis in lupus-prone mice. Kidney International 82: 969–979.
Foster, M.H. 2007. T cells and B cells in lupus nephritis. Seminars in Nephrology 27: 47–58.
Aringer, M., C. Gunther, and M.A. Lee-Kirsch. 2013. Innate immune processes in lupus erythematosus. Clinical Immunology 147: 216–222.
Kiefer, K., M.A. Oropallo, M.P. Cancro, and A. Marshak-Rothstein. 2012. Role of type I interferons in the activation of autoreactive B cells. Immunology and Cell Biology 90: 498–504.
Birmingham, D.J., and L.A. Hebert. 2015. The complement system in lupus nephritis. Seminars in Nephrology 35: 444–454.
Leffler, J., A.A. Bengtsson, and A.M. Blom. 2014. The complement system in systemic lupus erythematosus: an update. Annals of the Rheumatic Diseases 73: 1601–1606.
Kuballa, P., W.M. Nolte, A.B. Castoreno, and R.J. Xavier. 2012. Autophagy and the immune system. Annual Review of Immunology 30: 611–646.
Zhou, X.J., F.J. Cheng, and H. Zhang. 2015. Emerging view of autophagy in systemic lupus erythematosus. International Reviews of Immunology 34: 280–292.
Freedman, B.I., C.D. Langefeld, K.K. Andringa, J.A. Croker, A.H. Williams, N.E. Garner, D.J. Birmingham, L.A. Hebert, P.J. Hicks, M.S. Segal, J.C. Edberg, E.E. Brown, G.S. Alarcon, K.H. Costenbader, M.E. Comeau, L.A. Criswell, J.B. Harley, J.A. James, D.L. Kamen, S.S. Lim, J.T. Merrill, K.L. Sivils, T.B. Niewold, N.M. Patel, M. Petri, R. Ramsey-Goldman, J.D. Reveille, J.E. Salmon, B.P. Tsao, K.L. Gibson, J.R. Byers, A.K. Vinnikova, J.P. Lea, B.A. Julian, and R.P. Kimberly. 2014. End-stage renal disease in African Americans with lupus nephritis is associated with APOL1. Arthritis & Rhematology 66: 390–396.
Zhou, X.J., S.K. Nath, Y.Y. Qi, F.J. Cheng, H.Z. Yang, Y. Zhang, W. Yang, J.Y. Ma, M.H. Zhao, N. Shen, and H. Zhang. 2014. Brief report: identification of MTMR3 as a novel susceptibility gene for lupus nephritis in northern Han Chinese by shared-gene analysis with IgA nephropathy. Arthritis & Rhematology 66: 2842–2848.
Wang, L., and H.K. Law. 2015. The role of autophagy in lupus nephritis. International Journal of Molecular Sciences 16: 25154–25167.
Fenton, K. 2015. The effect of cell death in the initiation of lupus nephritis. Clinical and Experimental Immunology 179: 11–16.
Sun, D., X. Zhao, and L. Meng. 2012. Relationship between urinary podocytes and kidney diseases. Renal Failure 34: 403–407.
Mundel, P., and W. Kriz. 1995. Structure and function of podocytes: an update. Anatomy and Embryology (Berlin) 192: 385–397.
Faul, C., K. Asanuma, E. Yanagida-Asanuma, K. Kim, and P. Mundel. 2007. Actin up: regulation of podocyte structure and function by components of the actin cytoskeleton. Trends in Cell Biology 17: 428–437.
Endlich, N., E. Schordan, C.D. Cohen, M. Kretzler, B. Lewko, T. Welsch, W. Kriz, C.A. Otey, and K. Endlich. 2009. Palladin is a dynamic actin-associated protein in podocytes. Kidney International 75: 214–226.
Peti-Peterdi, J., and A. Sipos. 2010. A high-powered view of the filtration barrier. Journal of the American Society of Nephrology 21: 1835–1841.
Shankland, S.J. 2006. The podocyte’s response to injury: role in proteinuria and glomerulosclerosis. Kidney International 69: 2131–2147.
Weening, J.J., P. Ronco, and G. Remuzzi. 2013. Advances in the pathology of glomerular diseases. Contributions to Nephrology 181: 12–21.
Rezende, G.M., V.S. Viana, D.M. Malheiros, E.F. Borba, N.A. Silva, C. Silva, E.P. Leon, I.L. Noronha, and E. Bonfa. 2014. Podocyte injury in pure membranous and proliferative lupus nephritis: distinct underlying mechanisms of proteinuria? Lupus 23: 255–262.
Bariety, J., P. Bruneval, A. Meyrier, C. Mandet, G. Hill, and C. Jacquot. 2005. Podocyte involvement in human immune crescentic glomerulonephritis. Kidney International 68: 1109–1119.
Mundel, P., H.W. Heid, T.M. Mundel, M. Kruger, J. Reiser, and W. Kriz. 1997. Synaptopodin: an actin-associated protein in telencephalic dendrites and renal podocytes. Journal of Cell Biology 139: 193–204.
Thomas, P.E., B.L. Wharram, M. Goyal, J.E. Wiggins, L.B. Holzman, and R.C. Wiggins. 1994. GLEPP1, a renal glomerular epithelial cell (podocyte) membrane protein-tyrosine phosphatase. Identification, molecular cloning, and characterization in rabbit. Journal of Biological Chemistry 269: 19953–19962.
Takeda, T., T. McQuistan, R.A. Orlando, and M.G. Farquhar. 2001. Loss of glomerular foot processes is associated with uncoupling of podocalyxin from the actin cytoskeleton. Journal of Clinical Investigation 108: 289–301.
Doyonnas, R., D.B. Kershaw, C. Duhme, H. Merkens, S. Chelliah, T. Graf, and K.M. McNagny. 2001. Anuria, omphalocele, and perinatal lethality in mice lacking the CD34-related protein podocalyxin. Journal of Experimental Medicine 194: 13–27.
Palmer, R.E., A. Kotsianti, B. Cadman, T. Boyd, W. Gerald, and D.A. Haber. 2001. WT1 regulates the expression of the major glomerular podocyte membrane protein podocalyxin. Current Biology 11: 1805–1809.
Bollain, Y.G.J.J., M. Gonzalez-Castaneda, F. Torres-Del-Muro, L. Daza-Benitez, P. Zapata-Benavides, C. Rodriguez-Padilla, E. Avalos-Diaz, and R. Herrera-Esparza. 2011. Increased excretion of urinary podocytes in lupus nephritis. Indian Journal of Nephrology 21: 166–171.
Nakamura, T., C. Ushiyama, S. Suzuki, M. Hara, N. Shimada, K. Sekizuka, I. Ebihara, and H. Koide. 2000. Urinary podocytes for the assessment of disease activity in lupus nephritis. American Journal of the Medical Sciences 320: 112–116.
Nakamura, T., C. Ushiyama, N. Shimada, K. Sekizuka, I. Ebihara, M. Hara, and H. Koide. 2001. Effect of cyclophosphamide or azathioprine on urinary podocytes in patients with diffuse proliferative lupus nephritis. Nephron 87: 192–193.
Perez-Hernandez, J., M.D. Olivares, M.J. Forner, F.J. Chaves, R. Cortes, and J. Redon. 2016. Urinary dedifferentiated podocytes as a non-invasive biomarker of lupus nephritis. Nephrology, Dialysis, Transplantation 31: 780–789.
Schiffer, M., L.E. Schiffer, A. Gupta, A.S. Shaw, I.S. Roberts, P. Mundel, and E.P. Bottinger. 2002. Inhibitory smads and tgf-Beta signaling in glomerular cells. Journal of the American Society of Nephrology 13: 2657–2666.
Lasagni, L., L. Ballerini, M.L. Angelotti, E. Parente, C. Sagrinati, B. Mazzinghi, A. Peired, E. Ronconi, F. Becherucci, D. Bani, M. Gacci, M. Carini, E. Lazzeri, and P. Romagnani. 2010. Notch activation differentially regulates renal progenitors proliferation and differentiation toward the podocyte lineage in glomerular disorders. Stem Cells 28: 1674–1685.
Gan, H., S. Feng, H. Wu, Y. Sun, R. Hu, Z. Zhao, and Z. Zhang. 2012. Neonatal Fc receptor stimulation induces ubiquitin c-terminal hydrolase-1 overexpression in podocytes through activation of p38 mitogen-activated protein kinase. Human Pathology 43: 1482–1490.
Pawar, R.D., L. Castrezana-Lopez, R. Allam, O.P. Kulkarni, S. Segerer, E. Radomska, T.N. Meyer, C.M. Schwesinger, N. Akis, H.J. Grone, and H.J. Anders. 2009. Bacterial lipopeptide triggers massive albuminuria in murine lupus nephritis by activating Toll-like receptor 2 at the glomerular filtration barrier. Immunology 128: e206–221.
Kimura, J., O. Ichii, K. Miyazono, T. Nakamura, T. Horino, S. Otsuka-Kanazawa, and Y. Kon. 2014. Overexpression of Toll-like receptor 8 correlates with the progression of podocyte injury in murine autoimmune glomerulonephritis. Scientific Reports 4: 7290.
Ichii, O., S. Otsuka-Kanazawa, T. Horino, J. Kimura, T. Nakamura, M. Matsumoto, M. Toi, and Y. Kon. 2014. Decreased miR-26a expression correlates with the progression of podocyte injury in autoimmune glomerulonephritis. PLoS One 9: e110383.
Ma, R., Jiang, W., Li, Z., Sun, Y., Wei, Z. 2016. Intrarenal macrophage infiltration induced by T cells is associated with podocyte injury in lupus nephritis patients. Lupus
Cai, M., T. Zhou, X. Wang, M. Shang, Y. Zhang, M. Luo, C. Xu, and W. Yuan. 2016. DC-SIGN expression on podocytes and its role in inflammatory immune response of lupus nephritis. Clinical and Experimental Immunology 183: 317–325.
Gong, B., M. Radulovic, M.E. Figueiredo-Pereira, and C. Cardozo. 2016. The ubiquitin-proteasome system: potential therapeutic targets for Alzheimer’s disease and spinal cord injury. Frontiers in Molecular Neuroscience 9: 4.
Zhong, J.L., and C.Z. Huang. 2016. Ubiquitin proteasome system research in gastrointestinal cancer. World Journal of Gastrointestinal Oncology 8: 198–206.
Yu, J., Q. Tao, K.F. Cheung, H. Jin, F.F. Poon, X. Wang, H. Li, Y.Y. Cheng, C. Rocken, M.P. Ebert, A.T. Chan, and J.J. Sung. 2008. Epigenetic identification of ubiquitin carboxyl-terminal hydrolase L1 as a functional tumor suppressor and biomarker for hepatocellular carcinoma and other digestive tumors. Hepatology 48: 508–518.
Day, I.N., and R.J. Thompson. 2010. UCHL1 (PGP 9.5): neuronal biomarker and ubiquitin system protein. Progress in Neurobiology 90: 327–362.
Osaka, H., Y.L. Wang, K. Takada, S. Takizawa, R. Setsuie, H. Li, Y. Sato, K. Nishikawa, Y.J. Sun, M. Sakurai, T. Harada, Y. Hara, I. Kimura, S. Chiba, K. Namikawa, H. Kiyama, M. Noda, S. Aoki, and K. Wada. 2003. Ubiquitin carboxy-terminal hydrolase L1 binds to and stabilizes monoubiquitin in neuron. Human Molecular Genetics 12: 1945–1958.
Liu, Y., L. Fallon, H.A. Lashuel, Z. Liu, and P.T. Lansbury Jr. 2002. The UCH-L1 gene encodes two opposing enzymatic activities that affect alpha-synuclein degradation and Parkinson’s disease susceptibility. Cell 111: 209–218.
Choi, J., A.I. Levey, S.T. Weintraub, H.D. Rees, M. Gearing, L.S. Chin, and L. Li. 2004. Oxidative modifications and down-regulation of ubiquitin carboxyl-terminal hydrolase L1 associated with idiopathic Parkinson’s and Alzheimer’s diseases. Journal of Biological Chemistry 279: 13256–13264.
Xie, M., Y. Han, Q. Yu, X. Wang, S. Wang, and X. Liao. 2015. UCH-L1 inhibition decreases the microtubule-binding function of tau protein. Journal of Alzheimer’s Disease 49: 353–363.
Gong, B., Z. Cao, P. Zheng, O.V. Vitolo, S. Liu, A. Staniszewski, D. Moolman, H. Zhang, M. Shelanski, and O. Arancio. 2006. Ubiquitin hydrolase Uch-L1 rescues beta-amyloid-induced decreases in synaptic function and contextual memory. Cell 126: 775–788.
Cartier, A.E., K. Ubhi, B. Spencer, R.A. Vazquez-Roque, K.A. Kosberg, L. Fourgeaud, P. Kanayson, C. Patrick, E. Rockenstein, G.N. Patrick, and E. Masliah. 2012. Differential effects of UCHL1 modulation on alpha-synuclein in PD-like models of alpha-synucleinopathy. PLoS One 7: e34713.
Hurst-Kennedy, J., Chin, L.S., Li, L. 2012. Ubiquitin C-terminal hydrolase l1 in tumorigenesis. Biochem Res Int 2012: 123706.
Newton, K., and D. Vucic. 2007. Ubiquitin ligases in cancer: ushers for degradation. Cancer Investigation 25: 502–513.
Brackeva, B., V. De Punt, G. Kramer, O. Costa, K. Verhaeghen, G. Stange, J. Sadones, C. Xavier, J.M. Aerts, F.K. Gorus, and G.A. Martens. 2015. Potential of UCHL1 as biomarker for destruction of pancreatic beta cells. Journal of Proteomics 117: 156–167.
Costes, S., C.J. Huang, T. Gurlo, M. Daval, A.V. Matveyenko, R.A. Rizza, A.E. Butler, and P.C. Butler. 2011. Beta-cell dysfunctional ERAD/ubiquitin/proteasome system in type 2 diabetes mediated by islet amyloid polypeptide-induced UCH-L1 deficiency. Diabetes 60: 227–238.
Liu, Y., H. Wu, J. Wu, S. Wang, Z. Zhao, X. Zhang, R. Li, M. Guo, and Z. Zhang. 2008. Detection of UCH-L1 expression by pre-embedding immunoelectron microscopy with colloidal gold labeling in diseased glomeruli. Ultrastructural Pathology 32: 5–9.
Meyer-Schwesinger, C., T.N. Meyer, H. Sievert, E. Hoxha, M. Sachs, E.M. Klupp, S. Munster, S. Balabanov, L. Carrier, U. Helmchen, F. Thaiss, and R.A. Stahl. 2011. Ubiquitin C-terminal hydrolase-l1 activity induces polyubiquitin accumulation in podocytes and increases proteinuria in rat membranous nephropathy. American Journal of Pathology 178: 2044–2057.
Lohmann, F., M. Sachs, T.N. Meyer, H. Sievert, M.T. Lindenmeyer, T. Wiech, C.D. Cohen, S. Balabanov, R.A. Stahl, and C. Meyer-Schwesinger. 2014. UCH-L1 induces podocyte hypertrophy in membranous nephropathy by protein accumulation. Biochimica et Biophysica Acta 1842: 945–958.
Zhang, H., Y. Sun, R. Hu, W. Luo, X. Mao, Z. Zhao, Q. Chen, and Z. Zhang. 2013. The regulation of the UCH-L1 gene by transcription factor NF-kappaB in podocytes. Cellular Signalling 25: 1574–1585.
Rangan, G., Y. Wang, and D. Harris. 2009. NF-kappaB signalling in chronic kidney disease. Frontiers in Bioscience (Landmark Edition) 14: 3496–3522.
Zheng, L., R. Sinniah, and S.I. Hsu. 2006. In situ glomerular expression of activated NF-kappaB in human lupus nephritis and other non-proliferative proteinuric glomerulopathy. Virchows Archiv 448: 172–183.
Brahler, S., C. Ising, H. Hagmann, M. Rasmus, M. Hoehne, C. Kurschat, T. Kisner, H. Goebel, S. Shankland, K. Addicks, F. Thaiss, B. Schermer, M. Pasparakis, T. Benzing, and P.T. Brinkkoetter. 2012. Intrinsic proinflammatory signaling in podocytes contributes to podocyte damage and prolonged proteinuria. American Journal of Physiology. Renal Physiology 303: F1473–1485.
Acknowledgements
This work was supported by the National Natural Science Foundation of China (No. 31300797, 31670996) and Natural Science Basic Research Plan in Shaanxi Province of China (No. 2013JC2-03).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest
The authors declare that they have no potential conflicts of interest.
Rights and permissions
About this article
Cite this article
Cui, Jh., Xie, X. UCH-L1 Expressed by Podocytes: a Potentially Therapeutic Target for Lupus Nephritis?. Inflammation 40, 657–665 (2017). https://doi.org/10.1007/s10753-017-0512-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-017-0512-x