Abstract
Intensive Care Units (ICU) are costly yet critical hospital departments that should be available to care for patients needing highly specialized critical care. Shortage of ICU beds in many regions of the world and the constant fire-fighting to make these beds available through various ICU management policies motivated this study. The paper discusses the application of a generic system dynamics model of emergency patient flow in a typical hospital, populated with empirical evidence found in the medical and hospital administration literature, to explore the dynamics of intended and unintended consequences of such ICU management policies under a natural disaster crisis scenario. ICU management policies that can be implemented by a single hospital on short notice, namely premature transfer from ICU, boarding in ward, and general ward admission control, along with their possible combinations, are modeled and their impact on managerial and health outcome measures are investigated. The main insight out of the study is that the general ward admission control policy outperforms the rest of ICU management policies under such crisis scenarios with regards to reducing total mortality, which is counter intuitive for hospital administrators as this policy is not very effective at alleviating the symptoms of the problem, namely high ED and ICU occupancy rates that are closely monitored by hospital management particularly in times of crisis. A multivariate sensitivity analysis on parameters with diverse range of values in the literature found the superiority of the general ward admission control to hold true in every scenario.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Intensive Care Units (ICU) are costly yet critical hospital departments that should be available to care for patients needing highly specialized critical care. There is a shortage of ICU beds in many countries [1–5] and ICU occupancy rates are increasing [6]. When demand for critical care is high relative to available ICU capacity, ICU becomes a bottleneck to patient flow [5], making critical patients access to ICUs limited [7]. As a result, critically ill patients may be boarded in emergency departments (ED) which causes ED overcrowding [8, 9] and potential closure [10] and puts pressure on ED physicians who have to care for boarded patients in addition to ED patients [11]. Most importantly, boarding critically ill patients in ED puts the patients at risk of higher adverse events and mortality [12, 13], potentially increasing risk of ICU mortality by 1.5 % for each hour of waiting [14]. In addition to disrupting the workings of the ED, shortage of ICU beds could cause elective surgery cancellations [5, 7], affect discharge decisions [15–17], and increase risk of early death [18].
Various ICU management policies have been proposed and implemented over time in hospitals to lower ICU occupancy rates and improve critical care availability. While all are good intentioned and have positive intended consequences in terms of improving patient flow, there is evidence of unintended consequences that could put patient health at risk.
While there is empirical research within the medical and hospital administration literature on the silo effects of individual ICU management policies on particular aspects of care outcomes, there seems to be a research gap in terms of the combined effects of such management policies in a typical hospital. As such, clinicians and hospital administrators may have a difficult time putting all the evidence together to conclude what the best ICU management policies are in times of crisis. The purpose of this research is to address this gap in the literature by quantitatively assessing the combined effects of select ICU management policies in a typical hospital, and identify the best performing policy in managing ICU capacity.
To do so, a system dynamics modeling approach [19] has been applied to the context of emergency patient flow in a typical hospital. The choice of this methodology was based on the fact that by modeling the interactions of various elements of the patient flow at the aggregate level, it enables gaining a strategic perspective on the effects of management policies at the system level. System dynamics not only offers a rigorous approach to focus on the interconnectedness inherent in healthcare settings, but also the models can serve as learning environments for decision makers to understand why a certain structure produces a behaviour and conduct policy analysis to see how varying the conditions can change behavior [20]. The latter was of utmost importance to us in this study, as we intend that our fully documented generic model of a typical hospital can be used to test ICU management policies by decision makers in the field, using either the generic parameter values in this study or institution-specific parameter values applicable to their local circumstances. System dynamics has been applied to modeling patient flow problems extensively. Some examples include Brailsford et al. (2004) [21], Lattimer et al. (2004) [22], Desai et al. (2008) [23], Lane and Husemann (2008) [24], and Rashwan et al. (2015) [25].
The paper is organized as follows. First, the literature on ICU management policies is reviewed. The following section presents the research question and focus of the study. Next, a high-level cause and effect dynamic hypothesis of the effects of ICU management policies on system performance is discussed, followed by a system dynamics simulation model of emergency patient flow at a typical hospital, populated and calibrated with data from the literature. After a description of system-level performance measures, output of a baseline scenario that represents a typical hospital operating under stable conditions is presented. Subsequently, a crisis scenarios of a natural disaster that could put significant pressure on the critical care capacity of the hospital is introduced. Various ICU management policies are tested to assess their effects on alleviating the pressure on the ICU under this crisis scenario. The final sections discuss ICU management insights derived from the simulation, sensitivity of these insights to input parameters, as well as a discussion of study limitations and areas for future exploration.
2 ICU Management policies
Due to the fact that ICU is the best place for critically ill patients [4] to receive early interventions, many policies have been suggested to increase ICU bed availability [5, 7, 26]. Most common policies, starting from the three policies within the scope of this study that a single hospital can implement on short notice without incurring high costs, include:
-
1
Premature Transfer from ICU: Shortening ICU Length of Stay (LOS), estimated to occur for 6 to 42 % of initial discharges from ICU [27, 28], is another intuitive policy for admitting more patients into an ICU [17, 29]. However, it has been shown that transferring patients faster and sicker to the general ward is associated with increased in-hospital, ICU and Post-ICU, mortality [30, 31] as well as increased readmission rates [32, 33]. Early transfer out of ICU is responsible for 22 to 42 % of ICU readmissions [28] and 39 % of discharge mortality [34].
-
2
Boarding in Ward (ICU Admission Control): Under this policy, when ICU is full, critical patients waiting for ICU admission are admitted to the general ward instead [4, 14, 26]. It has been shown that admitted critical patients in ICU have better outcomes compared to those admitted to wards [14]. Parkhe et al. (2002) found that critically ill patients who were detoured to the Ward had an increased relative risk of 30-day mortality of 2.46 versus patients directly admitted to the ICU from ED [35].
-
3
General Ward Admission Control: Dunn (2003) mentioned that in order to decrease hospital overcrowding we may need some priorities in allocation of scarce resources in hospital [36]. Under this policy, ICU patients ready to be transferred to the general ward are given priority over those waiting for a ward bed in ED.
-
4
Expanding ICU Capacity: Adding more beds to ICU is usually seen as an intuitive yet costly policy that is widely discussed in the literature. By investigating five hospitals in UK, Lyons et al. (2000) estimated that to meet demands 95 % of times a two-fold increase in the number of ICU beds is required for a region [3]. Daly et al. (2001) concluded that to avoid post-ICU death caused by inappropriate discharge, a 16 % increase in the number of ICU beds in UK is necessary [34]. Yet, Kim et al. (2014) estimated that adding each bed to ICU costs $0.8 million per year [26]. It has been mentioned that investments in ICU beds also resulted in higher fixed costs, excess capacity, and long-term inefficiencies [37]. Limitations in the number of ICU staff, spaces within hospitals, government regulations and high costs associated with adding more beds to ICUs are mentioned as main reasons that hinder expansion of ICUs [1, 38, 39].
-
5
Expanding General Ward Capacity: Inadequate availability of beds in the general ward is seen as a reason for prolonged ICU stay, which in turn may cause blocked access to ICU beds [40, 41]. As such, expanding general ward capacity is considered as another policy to free blocked ICU beds.
-
6
ICU Direct Discharge Home: Johnson et al. (2013) propose directly discharging ICU patient home from ICU in instances where they have waited for a ward bed for a long time [40].
-
7
Discharge Home without Admitting to ICU: Armony et al. (2014) propose that patients who have waited long enough for admission to ICU in another department may have recovered and no longer need admission to ICU, and as such may be ready to be discharged [42]. This is confirmed by Hodgins’ (2011) observation that 14 % of admitted patients spend all of their hospital stay in ED [43]. Similarly, Dunn (2003) mentions that some admitted patients in the ED admission group recover enough during their waiting times in ED that are discharged directly from the ED without ever being transferred to a hospital bed [36].
-
8
Intermediate Units: To decrease ICU occupancy rates, intermediate units such as a Step Down Unit (SDU) or High Dependency Unit (HDU) can be used. These units provide an intermediate level of care between ICU and the general ward for semi-critical patients who do not need the level of care in ICU but are not ready to be transferred to the general ward either [44, 45].
-
9
Ambulance Diversion: To overcome crowding in ED, ambulances may be diverted to other hospitals. Given that many ICU patients are brought into the hospital by an ambulance [46], this policy also alleviates the pressure on ICUs by reducing the demand for ICU beds. However, Scheulen et al. (2001) states that diverting patients is ineffective in decreasing ED volume [47]. More importantly, Begley et al. (2004) found a higher mortality rate among trauma patients who were admitted during ambulance diversions [48].
-
10
ICU Patient Transfer: In times of inadequate ICU beds, patients may be transferred from a hospital to another hospital in order to be admitted in the latter hospital’s ICU. It has been found that these patients experience worse outcomes than those admitted to the ICU in the same hospital [49, 50].
-
11
Elective Surgical Demand Control: Elective surgery cancellation is another way to make room in ICU, basically by reducing the demand for ICU beds generated from elective surgical cases. Moreover, demand from elective surgeries can be controlled through better scheduling. McManus et al. (2003) investigated the impact of variability in patient flow on access to medical care and found that variability in scheduled surgical cases was higher than variability in unscheduled ICU admissions [51]. By smoothing the number of elective surgeries over the days of the week, Kolker (2009) made an 8.5 % reduction in ICU diversions [52].
3 Research question and focus of the study
The study aims to analyze ICU management policies that a single hospital can implement on short notice in times of crisis to alleviate the pressure on the ICU without incurring additional costs or the need for coordination with other sectors, and most importantly without jeopardizing the rest of its operations (e.g. regarding the care for elective patients). As such, cost-incurring or long term capacity decisions (i.e. expanding ICU capacity, general ward capacity, and intermediate units), policies where patients are transferred to other hospitals and as such cannot be implemented by a single hospital in silo (i.e. ambulance divergence and ICU patient transfer), or else need coordination with the community to care for prematurely discharged patients from hospitals (i.e. ICU Direct Discharge Home and Discharge Home without Admitting to ICU policies) as well as the elective surgical demand control policy which disrupts the operations of the hospital for other patients are not investigated. In short, three policies of Premature Transfer from ICU, Boarding in Ward and General Ward Admission Control, as well as their combinations, are fully analyzed to reveal the best performing policy under the crisis scenario.
4 Cause and effect hypothesis
Figure 1 shows a high level cause and effect dynamic hypothesis of the relationships between the selected ICU management policies and particular performance measures. The diagram is not meant to be a comprehensive demonstration of all causal and feedback relationships. The purpose here is to show main intended consequences (IC) and unintended consequences (UIC) of the selected ICU management policies, namely Premature Transfer from ICU, Boarding in Ward, and General Ward Admission Control, and possible combinations of these.
All the selected policies share the central balancing loop, which shows the intended consequence (IC) of reducing higher than desired ICU bed occupancy through implementing these policies, regardless of the degree to which this intended consequence is realized. To varying degrees, as empirically demonstrated in the literature and summarized under section 2, the policies could also result in UIC of increased ICU readmissions, UIC of increased ICU LOS, UIC of increased mortality, and UIC of occupancy spillover.
The “UIC of Increased ICU Readmission” loop demonstrates how responding to higher than desired ICU occupancy rate by implementing selected ICU management policies, to varying degrees, could result in a higher percentage of patients who would require ICU readmission (i.e. higher ICU readmission ratio) [32, 33], and as a result increase ICU occupancy rate.
The “UIC of Increased ICU LOS” loop depicts how higher ICU readmission rate (as part of the dynamics of “UIC of increased ICU readmission”) could increase average ICU LOS [27, 53, 54], further increasing ICU occupancy rate above the intended level.
The “UIC of Increased Mortality” loops shows how responding to higher than desired ICU occupancy rate by implementing selected ICU management policies, to varying degrees, could result in a higher mortality rate [30, 31, 34, 35], decreasing average ICU LOS, and as a result decreasing average ICU occupancy rate. Such a decrease in ICU occupancy rate is of course not desired, as it is achieved through higher mortality.
Finally, the “UIC of Occupancy Spillover” indicates how responding to higher than desired ICU occupancy rate by implementing selected ICU management policies, to varying degrees, could have spillover effects on occupancy rates of other departments, as patients transferred prematurely out of ICU or otherwise boarded in other departments inevitably increase occupancy rates of those departments.
We quantify these cause and effect relationships in the context of emergency patient flow based on empirical evidence from the literature, so that a whole system analysis of effects of any combination of ICU management policies can be performed to inform best practices in managing precious ICU capacity.
The following section explains the high level structure of a system dynamics model developed for this purpose.
5 Model structure
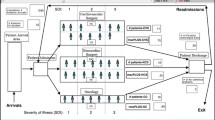
We developed a system dynamics simulation model of emergency patient flow within a typical acute care hospital consisting of an Emergency Department (ED), an Intensive Care Unit (ICU), and a general ward (Ward). A high level schematic picture of the model is presented in Fig. 2. The full model consists of 36 stock and 50 flow variables, as well as 86 auxiliary variables. To ensure replicability of the results and enable various hospitals to run the model with generic parameter values presented in this study, as well as institution-specific parameter values to obtain hospital-specific results (if desired), we have provided model documentation following the guidelines devised by Sterman and Rahmandad [55] in the Appendix: Model Documentation. Our model documentation also includes sources of data for each parameter, where applicable.
The general emergency patient flow of the baseline model is as follows. Patients arrive at the hospital through the ED, and depending on the severity of their condition, are either discharged from the ED (titled “non-admitted patients”), earmarked to be transferred to the ICU (titled “critical patients”) or to the Ward (titled “non-critical admitted patients”). Most admitted patients are discharged home from the ward, though some need to be readmitted to the ICU due to deterioration of their medical condition. Consistent with the literature [8, 10], the baseline model assumes that if ICU is full, patients would remain (board) in ED until there is capacity to admit them to ICU and that regardless of the boarding time in ED, patients would still require their full LOS in ICU. However, non-critical admitted patients boarding in ED and waiting for a ward bed may be discharged home from ED [56].
To keep the model simple, although some emergency patients require surgery and are admitted to ICU or the ward post operation, the model does not explicitly model the operating room (OR). It is assumed that once the patients leave the ED for OR, the few hours spent in OR can be modelled as part of the subsequent ICU or ward LOS, as a bed is usually vacated for these patients as early as the start of the operation.
To evaluate various ICU management policies, the model also allows variations to the generic emergency patient flow described earlier. For instance, the percentage of patients readmitted to ICU is a function of the baseline percentage of ICU readmission and the effect of “premature transfer from ICU” policy on ICU readmission rates. Similarly, ICU mortality rate is a function of baseline ICU mortality rates and the effects of average wait time for admission into ICU on ICU mortality rate. Another example is the average ICU LOS, which depends on the percentage of patients who have been readmitted to ICU and require longer ICU LOS. Overall shape and specific values of these functions are also derived from the literature [14, 32, 33, 56] and documented under the Appendix: Model Documentation section.
6 Performance measures
We analyze the policies with regards to two sets of performance measures. One set of performance measures captures the intended effect of ICU management policies, namely decreasing hospital overcrowding by reducing departmental (ED, ICU, and Ward) occupancy rates. Occupancy rates are closely monitored by hospital management in times of crisis and their reduction is usually interpreted as controlling the crisis. The other set of performance measures deal with the ultimate health outcome measure of mortality, as hospitals’ mission is to save lives, especially in times of crisis. We would like to assess the ICU management policies with regards to alleviating the symptom of the problem (occupancy rates) as well as potential unintended effects on mortality.
There are numerous possible intermediate outcome measures, such as total time spent in ICU, number of blocked beds in one department and wait times associated to get admitted to another department, readmissions to ICU, etc., which are all modeled in detail but are not reported individually in the results section, as their combined effect demonstrates itself on either the occupancy rates or mortality (or both). For instance, longer time spent in ICU (either due to ICU readmissions of health-deteriorated patients prematurely transferred out of ICU or alternatively due to insufficient beds in the ward resulting in bed blockage in ICU) affects both ICU occupancy rate and mortality. Similarly, long wait times in ED for ICU beds affects both ED occupancy and mortality. As such, occupancy rates (as the managerial performance measure representing the alleviation of the symptoms of the problem) and mortality (as the health outcome performance measure representing unintended consequences of ICU management policies) are the two main performance measures reported in this study.
With regards to departmental occupancy rates, two different performance measures should be distinguished here. One is the departmental instantaneous occupancy rate, which measures the occupancy rate at a point in time. The other is the departmental average occupancy rate, which measures the average of the departmental occupancy rate from the beginning of the simulation to a particular point in time. We have reported both these performance measures in this paper, as the instantaneous occupancy rate could best reflect what happens at any point during a crisis and the average occupancy rate could demonstrate a cumulative effect of various policies on departmental occupancy rates over time.
7 Baseline results
The baseline scenario mimics the performance of a typical hospital at equilibrium for 2000 h (nearly 3 months). As documented under the model documentation section, values of medically-driven model parameters for the baseline model, such as average length of stay at each department, percentage of patients leaving one department for another, percentage of patients dying in each department, and percentage of patients readmitted to ICU, are derived from the literature. To best mimic a typical hospital, arrival rate is set close to the average of 89 EDs studied by Schneider et al. (2003) [57]. Ratio of bed capacities in each department to overall hospital beds is set in line with what is observed in the literature [57–60]. To calibrate the model, total number of hospital beds and initial number of patients in each department are set in a way that results in occupancy levels close to what is typically reported in the literature [61–63] (See sources of parameter values under Appendix: Model Documentation).
Table 1 outlines the performance of the baseline scenario against the performance measures. As seen in the table, average ED occupancy of 97.88 %, average ICU occupancy of 87.78 %, and average ward occupancy of 85 % in the baseline model are close to 100 % ED occupancy observed in 6 EDS [61], 90 % ICU occupancy [62], and 85 % ward occupancy [63] respectively. These results ensure some level of face validity where a full validation of the model is not possible due to lack of data from a single source.
8 Crisis scenario
We consider a crisis scenarios to evaluate the effects of different policies on the performance measures. Under this scenario, beginning from the second day of the simulation and for a duration of 2 days, we double the hospital arrival rate. We call this scenario a “natural disaster” scenario, as it could represent a disaster such as a flood or mass accident that brings an influx of patients over a period of time (in this scenario assumed to be 2 days), after which the majority of remaining victims are found deceased on the scene and as such not taken to the hospital. Such a crisis could put a lot of pressure on the critical care capacity of a hospital that is operating under stable conditions before the crisis, and as such provides good grounds for evaluating the effects of various ICU management policies on selected performance measures.
Figure 3 shows the instantaneous departmental occupancy rates under the crisis scenario in the baseline model, which assumed no ICU management policies are implemented. As shown in the figure, the model is at equilibrium before the start of the crisis. Then the instantaneous occupancy rates rise sharply (and in case of ED, are allowed to go well beyond 100 %) during the crisis and stay high shortly after the crisis as well. The model reaches equilibrium again at time 1356 (on day 56.5). It should be noted that the term Dmnl in Fig. 3 and elsewhere in the paper stands for dimensionless.
Figure 4 shows the average departmental occupancy rates under the crisis scenario in the baseline model, in essence smoothing the occupancy rates over time. This performance measure may better reflect the cumulative occupancy rate from the start of the simulation to a particular point in time.
Figure 5 shows the behavior of health outcome measures of hospital-wide hourly mortality rate and accumulated total hospital mortality under the crisis scenario in the baseline model (i.e. assuming no ICU management policies are implemented). As seen in Fig. 5, hospital-wide hourly mortality rate sees a temporary and sharp increase during and shortly after the crisis, but then decreases to near pre-crisis equilibrium values. As a result of the temporary increase in hospital-wide mortality rate, the rate of increase in the accumulated total hospital mortality increases temporarily, but reverts back to the pre-crisis rate of increase shortly after the end of the crisis.
9 ICU Management policies under the crisis scenario
Figures below show the selected performance measures under the crisis scenario given the implementation of each policy (or combination of policies). It is assumed that the hospital, operating under stable equilibrium conditions only starts to implement the policies after the beginning of the crisis (i.e. the second day) and continues to apply the policies to the end of the simulation period.
We first evaluate ICU management policies against their intended effect of reducing average ICU occupancy rate which sees a sudden increase after the crisis. As seen in Fig. 6 below, all policies except the boarding in ward policy actually reduce the average ICU occupancy rate against the baseline scenario of implementing no policies. We rank the policies at time 1356, which is the time the baseline model would have reached equilibrium if no policies were implemented. Most effective policies in reducing average ICU occupancy rate at time 1356 are 1) General Ward Admission Control and Premature Transfer from ICU, 2) All Policies, 3) Premature Transfer from ICU, 4) Boarding in Ward and Premature Transfer from ICU, 5) General Ward Admission Control, 6) Boarding in Ward and General Ward Admission Control, 7) Baseline, and 8) Boarding in Ward policy respectively.
Average ED occupancy rate also skyrockets after the crisis. As seen in Fig. 7 and the zoomed version in Fig. 8 around time 1356, policies most effective at controlling average ED occupancy at time 1356 are 1) All Policies, 1) Boarding in Ward and Premature Transfer from ICU, 2) Boarding in Ward and General Ward Admission Control, 3) Boarding in Ward, 4) General Ward Admission Control and Premature Transfer from ICU, 5) Premature Transfer from ICU, 6) General Ward Admission Control, and 7) Baseline. When we use the same rank number for two policies, it means that the two policies had the exact same performance.
The crisis also affects the average ward occupancy rate. As seen in Fig. 9 and the zoomed Fig. 10, policies most effective at controlling average ward occupancy at time 1356 are 1) General Ward Admission Control, 2) Baseline, 3) General Ward Admission Control and Premature Transfer from ICU, 4) Premature Transfer from ICU, 5) Boarding in Ward and General Ward Admission Control, 6) All Policies, 7) Boarding in Ward, and 8) Boarding in Ward and Premature Transfer from ICU respectively.
As the ultimate measure of health quality, measures of mortality are of utmost importance. In terms of accumulated total hospital mortality, as seen in Fig. 11 and the zoomed Fig. 12, the best performing policies at time 1356 are as follows: 1) General Ward Admission Control, 2) Baseline, 3) Boarding in Ward and General Ward Admission Control, 4) Boarding in Ward, 5) General Ward Admission Control and Premature Transfer from ICU, 6) Premature Transfer from ICU, 7) All Policies, and 8) Boarding in Ward and Premature Transfer from ICU.
As for hospital-wide hourly mortality rate, as seen in Fig. 13 and the zoomed Fig. 14, the best performing policies at time 1356 are as follows: 1) Baseline, 1) General Ward Admission Control, 2) Boarding in Ward and General Ward Admission Control, 2) Boarding in Ward, 3) Premature Transfer from ICU, 4) General Ward Admission Control and Premature Transfer from ICU, 5) Boarding in Ward and Premature Transfer from ICU, and 6) All Policies.
10 Discussion and management insights
Which ICU management policies are the best in terms of alleviating the pressure on hospitals in times of temporary crisis? Table 2 summarizes the performance of the various analyzed policies or combination of policies at time 1356, the point at which the baseline model would have reached equilibrium after the crisis without implementing any ICU management policies.
In terms of the ultimate health outcome measure of accumulated total hospital mortality, which measures the total number of deaths from the beginning of the simulation to the particular point in time (1356 in this case), all ICU management policies except the General Ward Admission Control perform worse than the Baseline policy of doing nothing. So one may argue that by implementing any of the ICU management policies or their combinations except in the case of the General Ward Admission Control, hospitals may be indeed putting patients’ lives at higher risk and do more harm than good. The General Ward Admission Control policy outperforms the Baseline policy of doing nothing, but even this superiority in performance does not appear to be very significant (0.1 lives saved compared to the Baseline policy). As we show later under the sensitivity analysis though, this degree of significance could be higher under different departmental capacity assumptions.
The fact that the General Ward Admission Control policy outperformed the rest of the ICU management policies (by a range of 0.9 to 3.3 lives saved) may be counter intuitive to hospital management used to assess the situation of the crisis based on the managerial outcome measure of departmental occupancy rates. Indeed, one might have hypothesized that the General Ward Admission Control policy even increases ED occupancy over the Baseline as it prioritizes critical patients who have completed their medically-necessary critical care period in ICU in accessing general ward beds over emergency patients in ED who are competing for the same ward beds. The results show that this is not the case and the policy decreases (albeit slightly) the ED occupancy rate over the Baseline, but overall is not that effective in decreasing occupancy rates when compared to the rest of the policies.
The counter intuitive finding that the General Ward Admission Control policy which is among the worst in alleviating the symptoms of the problem (i.e. high ED and ICU occupancy rates) outperforms the rest of the policies has a logical explanation though. Unlike policies involving Premature Transfer of Patients from ICU, this policy does not put the patients’ health at risk by making them receive sub-standard critical care in the general ward when they should have still been occupying an ICU bed. Furthermore, unlike policies involving boarding in ward that make it hard for ED patients to get admitted to ICU, this policy helps empty to a greater extent ICU beds for ED patients, and as such somewhat alleviate the pressure on the ICU by housing critical patients whose critical care period in ICU is completed where they belong (in general ward) and ED patients who need ICU beds in ICU. Putting patients where they medically need to be is the right medical decision and as such should have positive effects on health outcomes.
The main management insight from this research, as such, is that while on the face of it the General Ward Admission Control policy is not an effective policy in times of crisis, as it does not adequately alleviate the symptoms of the problem (high ED and ICU occupancy rates), it is indeed the policy that outperforms the rest of the policies with regards to the ultimate measure of saving patients’ lives.
11 Sensitivity analysis
We populated our model with parameter values found in empirical studies published in the medical as well as hospital administration literature. While for the most part the values of these parameters showed little variation from one study to another (see sources of parameter values under Appendix: Model Documentation), there were three parameter values that showed a wide range of empirical values in the literature, namely: Non-Survivor LOS in Ward, Ward LOS for Non-Critical Admitted Patients, and Ward LOS for Critical Discharged home Patients.
To test the sensitivity of our findings to different values of these parameters, we first conducted a series of single variable sensitivity analyses. We varied Ward LOS for Non-Critical Admitted Patients from 120 h (used in the baseline model) to 144 [64], and 175.2 h [65]. We also varied Non-Survivors LOS in Ward from 297.6 h (used in the baseline model) to 369.6 h [66], 499.2 [67], and 1202.4 [68]. Similarly, we varied Ward LOS for Discharge-from-Ward Critical Patients from 126 h (used in the baseline model) to 93.8 h [69], 513.6 h [67], and 895.2 h [68]. In each of these 11 experiments, the General Ward Admission Control remained as the best performing policy with regards to accumulated total hospital mortality. In all but two experiments, the second best performing policy was the Baseline policy of implementing no particular ICU management policy. In two experiments, one setting the Ward LOS for Non-Critical Admitted Patients to 175.2 h and the other one setting the Ward LOS for Discharge-from-Ward Critical Patients to 895.2 h, the second best performing policy changed from Baseline to “General Ward Admission Control and Premature Transfer from ICU”.
The reason that the second best performing policy changes to “General Ward Admission Control and Premature Transfer from ICU” in these two scenarios is that in both scenarios, the pressure on the ward is increased significantly due to higher ward LOS for a large portion of patients. As such, discharging critical patients more quickly from ICU and prioritizing them over non-critical admitted patients in the ward admission process make more ICU beds available for those who are boarded in ED (and at risk of higher mortality) and helps reduce overall mortality rates.
We also conducted a series of multi-variable sensitivity analyses using the combination of the three values for Ward LOS for Non-Critical Admitted Patients (120, 144, 175.2), four values for Non-Survivors LOS in Ward (297.6, 369.6, 499.2, 1202.4), and four values for Ward LOS for Discharge-from-Ward Critical Patients (126, 93.8, 513.6, 895.2). This resulted in 48 combination of values. We implemented the eight ICU management policies or combination of policies in each of the 48 scenarios (i.e. a total of 384 simulation experiments) and found that in every single scenario, the General Ward Admission Control was the best performing policy with regards to accumulated total hospital mortality. The second best policy in the various scenarios was either the Baseline or the “General Ward Admission Control and Premature Transfer from ICU”.
To assess the sensitivity of the findings to relative departmental capacity assumptions, we conducted another series of multi-variable sensitivity analyses. We evaluated the impact of 15 % change in each departmental capacity. This resulted in 27 combination of values. Like the previous sensitivity analyses, we implemented the eight ICU management policies or combination of policies in each of the 27 scenarios and found that in every single scenario, the General Ward Admission Control outperformed the rest of the policies with regards to accumulated total hospital mortality. We also found that the degree of its significance over the second best performing policy could range from 0.081 to 1.837 lives saved. As the number of beds in the ICU or general ward decreases, the number of lives saved as a result of implementing the General Ward Admission Control policy increases.
12 Areas for future research
The model and insights gained from the analysis presented in this paper are a first step in understanding the performance of various hospital management policies on managerial and health outcome measures. With the ever growing empirical evidence of the effects of various policies on intermediate and ultimate performance measures, it may be possible to add a costing layer to the analysis to evaluate the cost effectiveness of various management policies, especially those that involve significant investments such as capacity expansion policies.
Other crisis scenarios especially those that are of a more permanent nature, such as the ever increasing pressure on hospitals to serve an ageing population in many countries [70–72], could be an interesting line of research for future exploration. These type of crisis scenarios would likely require more fundamental (and potential costly) management policies than the short term policies implementable by a single hospital explored in this study.
13 Conclusions
In light of the fact that there is a shortage of costly ICU beds in many regions of the world necessitating constant fire-fighting to make these beds available through various ICU management policies, we studied the intended and unintended consequences of these policies on managerial and health outcome measures in the context of emergency patient flow. The system dynamics simulation model is based in empirical evidence found in the medical and hospital administration literature. The model is fully documented so that it can be customized with institution-specific parameter values where applicable. Nonetheless, the preliminary insight generated by populating generic models such as ours with “typical” data can firm up guideline thinking, by facilitating the thinking for the relationship between the structure of an organization and its behaviour over time [73].
The main policy implications of the study is that the General Ward Admission Control policy outperforms the rest of the ICU management policies under a defined natural disaster crisis scenario. This policy basically prioritizes critical patients whose medically-necessary episode of critical care in ICU is completed in accessing general ward beds over emergency patients competing for ward beds in ED. This policy saves more lives when compared to implementing no policies (Baseline), Premature Transfer of Patients from ICU, Boarding in Ward, and possible combinations of these policies. The superiority of the General Ward Admission Control policy over other policies may be counter-intuitive to hospital administrators, as this policy is not as effective as other policies in alleviating the symptoms of the problem, which are the high ED and ICU occupancy rates closely monitored by hospital administrators during any bed crisis period. More importantly, our findings show that the other ICU management policies may be doing more harm than good in saving patients’ lives, and as such implementing no ICU management policy could be regarded a relatively good policy compared to all the ICU management policies studies except the General Ward Admission Control policy.
Future research could look into exploring the performance of various policies under different crisis scenarios, and adding a costing layer to the model to assess the cost-effectiveness of these policies.
References
Bing-Hua YU (2014) Delayed admission to intensive care unit for critically surgical patients is associated with increased mortality. Am J Surg 208:268–274
Kelley MA, Angus D, Chalfin DB, Crandall ED, Ingbar D, Johanson W, Medina J, Sessler CN, Vender JS (2004) The critical care crisis in the United States: a report from the profession. Chest 125:1514–1517
Lyons RA, Wareham K, Hutchings HA, Major E, Ferguson B (2000) Population requirement for adult critical care beds: a prospective quantitative and qualitative study. Lancet 355:595–598
Simchen E, Sprung CL, Galai N, Zitser-Gurevich Y, Bar-Lavi Y, Gurman G, Klein M, Lev A, Levi L, Zveibil F, Mandel M, Mnatzaganian G (2004) Survival of critically ill patients hospitalized in and out of intensive care units under paucity of intensive care unit beds. Crit Care Med 32:1654–1661
Hosseinifard S, Abbasi B, Minas J (2014) Intensive care unit discharge policies prior to treatment completion. Oper Res Health Care 3:168–175
Halpern NA, Pastores SM (2010) Critical care medicine in the United States 2000–2005: an analysis of bed numbers, occupancy rates, payer mix, and costs. Crit Care Med 38:65–71
Duke GJ, Buist MD, Pilcher D, Scheinkestel CD, Santamaria JD, Gutteridge GA, Cranswick PJ, Ernest D, French C, Botha JA (2009) Interventions to circumvent intensive care access block: a retrospective 2-year study across metropolitan Melbourne. Med J Aust 190:375–378
Hoot NR, Aronsky D (2008) Systematic review of emergency department crowding: causes, effects, and solutions. Ann Emerg Med 52:126–136
Olshaker JS, Rathlev NK (2006) Emergency department overcrowding and ambulance diversion: the impact and potential solutions of extended boarding of admitted patients in the emergency department. J Emerg Med 30:351–356
Moskop JC, Sklar DP, Geiderman JM, Schears RM, Bookman KJ (2009) Emergency department crowding, part 1—concept, causes, and moral consequences. Ann Emerg Med 53:605–611
Zhou JC, Pan KH, Zhou DY, Zheng SW, Zhu JQ, Xu QP, Wang CL (2012) High hospital occupancy is associated with increased risk for patients boarding in the emergency department. Am J Med 125:416
Young MP, Gooder VJ, McBride K, James B, Fisher ES (2003) Inpatient transfers to the intensive care unit: delays are associated with increased mortality and morbidity. J Gen Intern Med 18:77–83
Chalfin DB, Trzeciak S, Likourezos A, Baumann BM, Dellinger RP (2007) Impact of delayed transfer of critically ill patients from the emergency department to the intensive care unit. Crit Care Med 35:1477–1483
Cardoso LT, Grion CM, Matsuo T, Anami EH, Kauss IA, Seko L, Bonametti AM (2011) Impact of delayed admission to intensive care units on mortality of critically ill patients: a cohort study. Crit Care 15:R28
Profit J, McCormick MC, Escobar GJ, Richardson DK, Zheng Z, Coleman-Phox K, Roberts R, Zupancic JA (2007) Neonatal intensive care unit census influences discharge of moderately preterm infants. Pediatrics 119:314–319
Stelfox HT, Hemmelgarn BR, Bagshaw SM, Gao S, Doig CJ, Nijssen-Jordan C, Manns B (2012) Intensive care unit bed availability and outcomes for hospitalized patients with sudden clinical deterioration. Arch Intern Med 172:467–474
Wagner J, Gabler NB, Ratcliffe SJ, Brown SE, Strom BL, Halpern SD (2013) Outcomes among patients discharged from busy intensive care units. Ann Intern Med 159:447–455
Chrusch CA, Olafson KP, McMillan PM, Roberts DE, Gray PR (2009) High occupancy increases the risk of early death or readmission after transfer from intensive care. Crit Care Med 37:2753–2758
Sterman JD (2000) Business dynamics: systems thinking and modeling for a complex world. Irwin McGrawHill, Boston
Lane DC, Monefeldt C, Rosenhead JV (2000) Looking in the wrong place for health care improvements: a system dynamics study of an accident and emergency department. J Oper Res Soc 51:518–531
Brailsford SC, Lattimer VA, Tamaras P, Turnbull JC (2004) Emergency and on demand health care: modelling a large and complex system. J Oper Res Soc 55:34–42
Lattimer V, Brailsford S, Turnbull J, Tarnaras P, Smith H, George S, Gerard K, Maslin-Prothero S (2004) Reviewing emergency care systems I: insights from system dynamics modelling. Emerg Med J 21:685–691
Desai MS, Penn ML, Brailsford S, Chipulu M (2008) Modelling of Hampshire Adult Services—gearing up for future demands. Health Care Manag Sci 11:167–176
Lane DC, Husemann E (2008) System dynamics mapping of acute patient flows. J Opl Res Soc 59:213–224
Rashwan W, Abo-Hamad W, Arisha A (2015) A system dynamics view of the acute bed blockage problem in the Irish healthcare system. Eur J Oper Res 247:276–293
Kim SH, Chan CW, Olivares M, Escobar G (2015) ICU admission control: an empirical study of capacity allocation and its implication on patient outcomes. Manag Sci 61:19–38
Cooper GS, Sirio CA, Rotondi AJ, Shepardson LB, Rosenthal GE (1999) Are readmissions to the intensive care unit a useful measure of hospital performance? Med Care 37:399–408
Rosenberg AL, Watts C (2000) Patients readmitted to ICUs: a systematic review of risk factors and outcomes. Chest 118:492–502
Anderson D, Price C, Golden B, Jank W, Wasil E (2011) Examining the discharge practices of surgeons at a large medical center. Health Care Manag Sci 14:338–347
Goldfrad C, Rowan K (2000) Consequences of discharges from intensive care at night. Lancet 355:1138–1142
Beck DJ, McQuillan P, Smith GB (2002) Waiting for the break of dawn? The effects of discharge time, discharge TISS scores and discharge facility on hospital mortality after intensive care. Intensive Care Med 28:1287–1293
Utzolino S, Kaffarnik M, Keck T, Berlet M, Hopt UT (2010) Unplanned discharges from a surgical intensive care unit: readmissions and mortality. J Crit Care 25:375–381
Kc DS, Terwiesch C (2012) An econometric analysis of patient flows in the cardiac intensive care unit. Manuf Serv Oper Manag 14:50–65
Daly K, Beale R, Chang RW (2001) Reduction in mortality after inappropriate early discharge from intensive care unit: logistic regression triage model. BMJ 322:1274–1276
Parkhe M, Myles PS, Leach DS, Maclean AV (2002) Outcome of emergency department patients with delayed admission to an intensive care unit. Emerg Med 14:50–57
Dunn R (2003) Reduced access block causes shorter emergency department waiting times: an historical control observational study. Emerg Med 15:232–238
Terwiesch C, Diwas KC, Kahn JM (2011) Working with capacity limitations: operations management in critical care. Crit Care 15:308
Howell MD (2011) Managing ICU throughput and understanding ICU census. Curr Opin Crit Care 17:626–633
Halpern NA, Pastores SM, Oropello JM, Kvetan V (2013) Critical care medicine in the United States: addressing the intensivist shortage and image of the specialty. Crit Care Med 41:2754–2761
Johnson DW, Schmidt UH, Bittner EA, Christensen B, Levi R, Pino RM (2013) Delay of transfer from the intensive care unit: a prospective observational study of incidence, causes and financial impact. Crit Care 17:R128
Levin PD, Worner TM, Sviri S, Goodman SV, Weiss YG, Einav S, Weissman C, Sprung CL (2003) Intensive care outflow limitation: frequency, etiology, and impact. J Crit Care 18:206–211
Armony M, Chan CW, Zhu B (2013) Critical care in hospitals: when to introduce a step down unit? Working Paper, Columbia University
Hodgins MJ, Moore N, Legere L (2011) Who is sleeping in our beds? Factors predicting the ED boarding of admitted patients for more than 2 hours. J Emerg Nurs 37:225–230
Harding AD (2009) What can an intermediate care unit do for you? J Nurs Adm 39:4–7
Stacy KM (2011) Progressive care units: different but the same. Crit Care Nurse 31:77–83
Burt CW, McCaig LF, Valverde RH (2006) Analysis of ambulance transports and diversions among US emergency departments. Ann Emerg Med 47:317–326
Scheulen JJ, Li G, Kelen GD (2001) Impact of ambulance diversion policies in urban, suburban, and rural areas of central Maryland. Acad Emerg Med 8:36–40
Begley CE, Chang Y, Wood RC, Weltge A (2004) Emergency department diversion and trauma mortality: evidence from Houston, Texas. J Trauma 57:1260–1265
Rosenberg AL, Hofer TP, Strachan C, Watts CM, Hayward RA (2003) Accepting critically ill transfer patients: adverse effect on a referral center’s outcome and benchmark measures. Ann Intern Med 138:882–890
Combes A, Luyt CE, Trouillet JL, Chastre J, Gibert C (2005) Adverse effect on a referral intensive care unit’s performance of accepting patients transferred from another intensive care unit. Crit Care Med 33:705–710
McManus ML, Long MC, Cooper A, Mandell J, Berwick DM, Pagano M, Litvak E (2003) Variability in surgical caseload and access to intensive care services. Anesthesiology 98:1491–1496
Kolker A (2009) Process modeling of ICU patient flow: effect of daily load leveling of elective surgeries on ICU diversion. J Med Syst 33:27–40
Kramer AA, Higgins TL, Zimmerman JE (2013) The association between ICU readmission rate and patient outcomes. Crit Care Med 41:24–33
Kramer AA, Higgins TL, Zimmerman JE (2012) Intensive care unit readmissions in U.S. hospitals: patient characteristics, risk factors, and outcomes. Crit Care Med 40:3–10
Rahmandad H, Sterman JD (2012) Reporting guidelines for simulation-based research in social sciences. Syst Dyn Rev 28:396–411
St Noble VJ, Davies G, Bell D (2008) Improving continuity of care in an acute medical unit: initial outcomes. QJM 101:529–533
Schneider SM, Gallery ME, Schafermeyer R, Zwemer FL (2003) Emergency department crowding: a point in time. Ann Emerg Med 42:167–172
Kirchhoff KT, Dahl N (2006) American Association of Critical-Care Nurses’ national survey of facilities and units providing critical care. Am J Crit Care 15:13–27
Multz AS, Chalfin DB, Samson IM, Dantzker DR, Fein AM, Steinberg HN, Niederman MS, Scharf SM (1998) A “closed” medical intensive care unit (MICU) improves resource utilization when compared with an “open” MICU. Am J Respir Crit Care Med 157:1468–1473
Iapichino G, Gattinoni L, Radrizzani D, Simini B, Bertolini G, Ferla L, Mistraletti G, Porta F, Miranda DR (2004) Volume of activity and occupancy rate in intensive care units. Association with mortality. Intensive Care Med 30:290–297
McCarthy ML, Aronsky D, Jones ID, Miner JR, Band RA, Baren JM, Desmond JS, Baumlin KM, Ding R, Shesser R (2008) The emergency department occupancy rate: a simple measure of emergency department crowding? Ann Emerg Med 51:15–24
Pronovost PJ, Needham DM, Waters H, Birkmeyer CM, Calinawan JR, Birkmeyer JD, Dorman T (2004) Intensive care unit physician staffing: financial modelling of the Leapfrog standard. Crit Care Med 32:1247–1253
de Bruin A, Bekker R, van Zanten L, Koole G (2010) Dimensioning hospital wards using the Erlang loss model. Ann Oper Res 178:23–43
Curley C, McEachern JE, Speroff T (1998) A firm trial of interdisciplinary rounds on the inpatient medical wards: an intervention designed using continuous quality improvement. Med Care 36:AS4–AS12
Asplund K, Gustafson Y, Jacobsson C, Bucht G, Wahlin A, Peterson J, Blom JO, Angquist KA (2000) Geriatric-based versus general wards for older acute medical patients: a randomized comparison of outcomes and use of resources. J Am Geriatr Soc 48:1381–1388
Iapichino G, Morabito A, Mistraletti G, Ferla L, Radrizzani D, Reis Miranda D (2003) Determinants of post-intensive care mortality in high-level treated critically ill patients. Intensive Care Med 29:1751–1756
Wallis CB, Davies HT, Shearer AJ (1997) Why do patients die on general wards after discharge from intensive care units? Anaesthesia 52:9–14
Mayr VD, Dünser MW, Greil V, Jochberger S, Luckner G, Ulmer H, Friesenecker BE, Takala J, Hasibeder WR (2006) Causes of death and determinants of outcome in critically ill patients. Crit Care 10:R154
Garland A, Connors AF Jr (2013) Optimal timing of transfer out of the intensive care unit. Am J Crit Care 22:390–397
LaPierre TA, Hughes ME (2009) Population aging in Canada and the United States. In: Poston D (ed) International handbook of population aging. Springer, New York, pp 191–228
George G, Jell C, Todd BS (2006) Effect of population ageing on emergency department speed and efficiency: a historical perspective from a district general hospital in the UK. Emerg Med J 23:379–383
Schulz E, Leidl R, König HH (2004) The impact of ageing on hospital care and long-term care-the example of Germany. Health Policy 67:57–74
Wolstenholme E (1999) A patient flow perspective of UK Health Services: exploring the case for new “intermediate care” initiatives. Syst Dyn Rev 15:253–271
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 1.10 mb)
Rights and permissions
About this article
Cite this article
Mahmoudian-Dehkordi, A., Sadat, S. Sustaining critical care: using evidence-based simulation to evaluate ICU management policies. Health Care Manag Sci 20, 532–547 (2017). https://doi.org/10.1007/s10729-016-9369-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10729-016-9369-z