Summary
Purpose KRAS is frequently mutated in non-small cell lung cancers (NSCLC), resulting in activation of the MEK/ERK pathway. Because there are currently no drugs that target oncogenic KRAS, MEK inhibitors have been tested clinically as a possible treatment option for patients with NSCLC. However, KRAS-mutant cancers exhibit resistance to MEK inhibitors. Therefore, a combinational strategy is necessary for effective therapy. To address this, we investigated the therapeutic effects of combining selumetinib, a MEK1/2 inhibitor, with BYL719, a PI3Kα inhibitor. Methods We evaluated the effects of selumetinib and BYL719 in vitro and in vivo in NSCLC cell lines. Results The combination of BYL719 and selumetinib resulted in synergistic cytotoxic activity compared with the single agents alone in KRAS-mutant NSCLC cells. At the molecular level, we found that AKT activation strongly influenced the sensitivity of KRAS-mutant NSCLC cells to selumetinib. Selumetinib upregulated phospho-AKT and phosphorylated BAD at ser136, which is responsible for intrinsic drug resistance in KRAS-mutant NSCLC cells. In contrast, inhibition of the PI3K/AKT pathway by BYL719 hindered selumetinib-induced BAD phosphorylation and increased the antitumor efficacy of selumetinib. Furthermore, selumetinib and BYL719 combination therapy showed synergy in the suppression of A549 xenograft tumor growth. On analysis of the pharmacodynamics, selumetinib and BYL719 together resulted in effective inhibition of both p-ERK and p-AKT expression in tumor tissue. Conclusion Taken together, these data suggest that combination treatment with selumetinib and BYL719 is a promising therapeutic approach to overcoming resistance to MEK inhibitors.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
KRAS is a member of the RAS family of oncogenes, a collection of small guanosine triphosphate (GTP)-binding proteins that activate intracellular signaling pathways to regulate cell proliferation, differentiation, and survival [1]. KRAS mutations predominantly arise as single amino acid substitutions at residues G12, G13, or Q61, and confer transforming capacity. Activating KRAS mutations are found in 15–30 % of patients with non-small cell lung cancer (NSCLC) and are associated with poor responses to conventional treatment regimens [2–4]. These mutations lead to impaired GTPase activity and constitutive activation of KRAS effectors, including RAF/MEK/ERK and the phosphoinositide 3-kinase (PI3K)/AKT signaling pathway [1, 4]. However, there are currently no effective therapies for mutant KRAS, since KRAS itself has proven difficult to directly target with small molecules [5, 6].
An alternative approach to targeting mutant KRAS involves using small molecule inhibitors that target KRAS effectors (e.g. RAF/MEK/ERK). As the MEK/ERK pathway is critical for cell growth, survival, and transformation, MEK inhibitors have been actively investigated as a treatment option for various cancers [7, 8]. Selumetinib is an orally active MEK inhibitor that inhibits both basal and induced ERK phosphorylation in numerous types of cancer cells [9]. Although selumetinib has shown activity in vitro and in several tumor xenografts models, a subset of tumors, particularly NSCLC, are resistant to this inhibition [7, 10–12]. Resistance to inhibition of the MEK/ERK pathway may result from mutations in MEK1 or activation of the PI3K pathway [13, 14]. Recently, it has been reported that a high level of AKT activation is associated with resistance to the MEK inhibitor selumetinib in cases of lung cancer, and that dual inhibition of the AKT and EKR pathways increased antitumor activity by selumetinib [15–17]. In addition, several studies have also demonstrated that simultaneous inhibition of MEK and PI3K leads to tumor regression in KRAS-mutant cancer cell models [18–20].
PI3K/AKT signaling pathways are also activated in a variety of cancers including NSCLC, and PI3K is the second best-characterized RAS effector [21, 22]. PI3K converts PIP2 to PIP3, which activates AKT to promote cell growth and proliferation. The PI3Ks are organized into three classes (I-III). Class I PI3Ks are further divided into three class IA isoforms, PI3Kα, PI3Kβ, and PI3Kδ, whereas PI3Kγ constitutes class IB. As PI3Kα is ubiquitously expressed and has been linked to AKT activation, PI3Kα appears to be an ideal target for drug development [22]. In this regard, targeting PI3K represents a promising combination treatment strategy in KRAS-mutant NSCLC.
In this study, we investigated the efficacy of a combination of selumetinib and BYL719, a novel specific PI3Kα inhibitor with pharmacologic and biologic properties [23, 24]. Here, we present evidence that combining these two inhibitors in cases of KRAS-mutant NSCLC results in enhanced antitumor activity in vitro as well as in vivo. These findings support the potential clinical use of this drug combination in patients with KRAS-mutant NSCLC.
Materials and methods
Cell lines and cell cultures
Human NSCLC cell lines A549 and NCI-H2009 were obtained from the American Type Culture Collection (ATCC, Manassas, VA, USA). Cells were cultured in RPMI-1640 containing 10 % FBS at 37 °C in a humidified atmosphere containing 5 % CO2.
Chemical reagents and antibodies
Selumetinib (AZD6244, AstraZeneca) and BYL 719 (Novartis) were dissolved in dimethyl sulfoxide (DMSO) to a 10 mM concentration and stored in small aliquots at −20 °C until further use. Antibodies to p-Akt (Ser473), Akt, p-ERK1/2 (Thr202/Thy204), ERK1/2, p-BIM (Ser69), BIM, p-BAD (Ser136), BAD, PARP, and β-actin were purchased from Cell Signaling Technology. Anti-14-3-3 was purchased from Santa Cruz Biotechnology.
Cell viability assay and combination index analysis
Cells were seeded on a 96-well plate, allowed to adhere overnight, and treated with a dilution series of test compounds for 72 h. Cell viability was determined using a Cell Counting Kit (Dojindo Molecular Technologies) according to the manufacturer’s instructions. Combination index (CI) data were generated using CompuSyn (Combosyn). A CI of 1 indicated an additive drug interaction, whereas a CI of <1 was synergistic and a CI of> 1 was antagonistic.
Cell cycle and apoptosis assay
Cell cycle analysis was performed after 24 h of treatment. Cells were fixed with ice-cold 70 % ethanol, stained with propidium iodide, and analyzed by flow cytometry (BD Biosciences).
Western blot analysis
Cells were lysed in PRO-PREP™ protein extraction solution (iNtRON Biotechnology) supplemented with a protease and phosphatase inhibitor cocktail (Sigma). Equal amounts of protein were then subjected to SDS-PAGE (NuPAGE 4–12 % Bis-Tris Gel; Invitrogen) and transferred to polyvinylidene difluoride (PVDF) membranes. Membranes were then incubated with the aforementioned antibodies and developed by ECL.
Immunoprecipitation
Cells were lysed in radioimmunoprecipitation assay (RIPA) buffer supplemented with a protease and phosphatase inhibitor cocktail (Sigma). Equal amounts of protein were incubated with BAD, 14-3-3, or immunoglobulin G control antibodies overnight at 4 °C to allow the formation of immune complexes. Immune complexes were subsequently precipitated with protein A/G agarose beads (Santa Cruz Biotechnology) and analyzed using Western blot analyses with the aforementioned antibodies.
Xenograft studies
All procedures involving animals were reviewed and approved by the Institutional Animal Care and Use Committee (IACUC) at the Samsung Biomedical Research Institute (SBRI). SBRI is an Association of Assessment and Accreditation of Laboratory Animal Care International (AAALAC International) accredited facility and abides by the Institute of Laboratory Animal Resources (ILAR) guidelines. Six-week-old BALB/c female nude mice were injected subcutaneously with A549 cells (5 × 106). When tumor sizes reached approximately 100 mm3, mice were randomized into four groups of 10–12 mice each. Each group of mice was dosed via daily oral gavage with vehicle, selumetinib (25 mg/kg/d, twice per day), BYL719 (25 mg/kg/d), or a combination of both. The selumetinib vehicle contained 0.5 % hydroxypropyl methylcellulose plus 0.1 % Tween-80, and the BYL719 vehicle contained 0.5 % hydroxypropyl methylcellulose. All mice received both vehicles. Tumor volumes were determined using calipers and were calculated using the following formula: V = (L x W2)/2 (L, Length; W, width). Toxicity was monitored according to weight loss. Three days after treatment was initiated, the tumors were removed for Western blot analysis 3 h after the last dose of medication or vehicle was administered.
Statistical analysis
All numerical data are presented as the mean±SEM. Statistical analyses were carried out using GraphPad Prism (GraphPad software). P-values <0.05 were considered to be statistically significant.
Results
PI3Kα and MEK inhibitors exhibit synergistic effects
To test whether a PI3Kα inhibitor in combination with a MEK inhibitor have a synergistic effect on MEK inhibitor-resistant cells, we first evaluated the sensitivity to MEK inhibitors in KRAS-mutant NSCLC cell lines (A549 and NCI-H2009) by assessing cell viability. Cells were treated with the selumetinib (Fig. 1a) at concentrations ranging from 1 to 10,000 nM for 72 h. Both cell lines had a selumetinib IC50 of ≥ 1 μM (Fig. 1b and c). It was previously reported that 1 μM was close to the average plasma concentration of selumetinib achieved in patients at the maximum tolerated dose for this agent [7]. Thus, we considered these cell lines to be resistant to selumetinib. We next examined the effects of a PI3Kα inhibitor, BYL719, at increasing concentrations (Fig. 1a) from 1 to 10,000 nM. BYL719 reduced cell viability in a manner similar to selumetinib in both cell lines (Fig. 1b and c). The combination of selumetinib and BYL719 significantly reduced cell viability in A549 and NCI-H2009 cells (Fig. 1b and c). To determine whether the antitumor effects obtained with different doses of selumetinib and BYL719 combinations were synergistic, we evaluated the combination index (CI). After treatment with various concentrations (0.125–4 μM) of selumetinib, BYL719, and selumetinib plus BYL719, the CI was measured for each cell line. As shown in Fig. 1d, the combination treatment produced a strong synergistic effect in both cell lines (CI of A549: 0.003–0.321 and CI of H2009: 0.002–0.005).
A combination of selumetinib and BYL719 was more efficacious than selumetinib alone in the treatment of KRAS-mutant lung cancers. a Structure of selumetinib and BYL719. b A549 and c NCI-H2009 cells were treated with various concentrations of selumetinib, BYL719, or selumetinib plus BYL719 for 72 h. Cell viability was measured using CCK-8 assays. Results represent the mean of three independent experiments. Error bars, SEM. d Combination index plots of selumetinib and BYL719 in A549 and NCI-H2009 cells. Most of the data points were presented with CI <1, indicating that the selumetinib-BYL719 combination is synergistic
BYL719 enhances selumetinib-induced apoptosis
To test whether this reduction in cell viability was attributed to induction of apoptosis or growth arrest, we analyzed apoptosis and cell cycle profiles using A549 (Fig. 2a) and H2009 (Fig. 2b) cells. After 24 h of treatment, apoptosis was assessed by the detection sub-G1 peak. We found that cell death was increased in a dose-dependent manner in combination-treated cells. The apoptosis was more significantly increased in H2009 cells. In the cell-cycle profile, G1 phase cells were increased by selumetinib and BYL719 in both cells. However the combination of selumetinib and BYL719 increased the G1 phase population in A549 cells. Thus, the combination treatment induces both cell death and cell-cycle arrest at the G1 phase.
Treatment with selumetinib and BYL719 synergistically induced cell apoptosis in KRAS-mutant cells. a A549 and b H2009 cells were treated with selumetinib, BYL719, or a combination of the two at the indicated concentrations for 24 h. Flow cytometric histograms of cells stained with propidium iodide were analyzed using Modifit software (BD Bioscience). Percentages of cells in apoptotic sub-G1, G1, S, and G2/M phases are presented
BYL719 enhances selumetinib-induced apoptosis through BAD
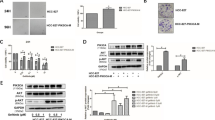
A recent study reported that PI3K/AKT activation mediates resistance to MEK inhibitors [16, 25, 26]. Based on those results, we investigated the mechanism by which selumetinib and BYL719 cooperate to induce apoptosis in KRAS-mutant NSCLC cells. A549 cells were treated with 3 μM selumetinib and levels of p-ERK and p-AKT were measured at 2, 4, 8, and 24 h. As expected, ERK phosphorylation was inhibited by selumetinib, but AKT phosphorylation was induced in a time-dependent (Fig. 3a) and dose-dependent (Fig. 3b) manner. BYL719 efficiently inhibited selumetinib-induced AKT phosphorylation in A549 (Fig. 3b) and H2009 (Fig. 3c). At high concentrations (≥2.5 μM), BYL719 caused a slight reduction of p-ERK in A549 cells after 24 h of treatment. Similar to our results, it has been reported that lapatinib along with BYL719 inhibits ERK phosphorylation [27], and others have shown that PI3K inhibition actually enhances ERK activation in BT474 cells [28].
Pathway modulation in the KRAS-mutant cell line following MEK and PI3K inhibition. a A549 cells were treated with 3 μM selumetinib for 0, 2, 4, 8, or 24 h. Cell lysates were immunoblotted for levels of p-ERK and p-Akt. b A549 and c H2009 Cells were treated with the indicated concentrations of selumetinib or BYL719 for 24 h. Western blot analysis was carried out to determine the levels of p-ERK and p-Akt using specific antibodies. β-actin was used as a loading control
To determine the direct mediators of selumetinib/BYL719-induced apoptosis, we determined protein levels of pro-apoptotic Bcl-2 family members (BIM and BAD). Consistent with prior studies, suppression of p-ERK by selumetinib led to increased levels of BIMEL, and, to a lesser extent, of BIML and BIMS which are well-known targets of MAPK signaling [29–33]. However, selumetinib /BYL719 did not induce obvious changes in BIM expression compared to selumetinib alone in A549 and H2009 cells (Fig. 4). Interestingly, p-BAD (ser136) was significantly induced by selumetinib alone, and we also observed a clear synergistic inhibition of p-BAD with the combination of selumetinib and BYL719 (Fig. 4). BAD can be phosphorylated at ser112 and ser136 by the MEK/ERK and the PI3K/AKT pathways, respectively [25], and this phosphorylation inactivates its pro-apoptotic function [34]. In accordance with reduced BAD phosphorylation, PARP cleavage was increased with combination therapy (Fig. 4).
Phosphorylation of BAD has been reported to promote BAD translocation from the mitochondria into the cytosol, interaction with the scaffold protein 14-3-3, and dissociation from Bcl-XL [35, 36, 34]. Immunoprecipitation of BAD revealed that when p-BAD levels were induced by selumetinib, a proportional increase in the amount of 14-3-3 associated with BAD was observed. However, BYL719 disrupted the association of BAD with 14-3-3 following p-BAD induction by selumetinib (Fig. 5). These results suggest that selumetinib-induced BAD phosphorylation may lead to the loss of pro-apoptotic activity and thereby contribute to the resistance of KRAS-mutant NSCLC cells to MEK inhibitors. Thus, BYL719 in combination with selumetinib effectively promotes apoptosis by blocking the ability of BAD to bind 14-3-3.
BYL719 inhibits selumetinib-induced BAD association with 14-3-3. A549 cells were treated for 24 h with selumetinib, BYL719, or a combination of the two. Immunoprecipitation was performed with BAD, 14-3-3, or immunoglobulin G (IgG) control antibodies. BAD-associated 14-3-3, 14-3-3-associated BAD, total BAD, and total 14-3-3 were analyzed using Western blot. IgG was used as a negative control
A combination of selumetinib and BYL719 leads to enhanced antitumor efficacy in the KRAS-mutant xenograft model
In light of the synergistic effects of the combination therapy observed in vitro, we investigated the efficacy of combining selumetinib and BYL719 in vivo. Mice bearing A549 xenografts were treated with vehicle, selumetinib, BYL719, or a combination of selumetinib and BYL719. As shown in Fig. 6a, selumetinib and BYL719 alone had a modest effect on the inhibition of tumor growth (55 and 65 % growth compared with vehicle, respectively). The combination therapy resulted in a significantly enhanced reduction in tumor volume when compared with selumetinib alone (P = 0.06), BYL719 alone (P = 0.0009), or vehicle (P = 0.00001) at day 28. Furthermore, no significant differences in body weight were found between the four groups during the 28 days of treatment, and no obvious toxicities were observed (data not shown). To investigate the pharmacodynamic effects of combining selumetinib and BYL719 in vivo, A549 xenografts were collected 3 h after the final dose of selumetinib and/or BYL719 was administered on day 3. Tumor lysates were analyzed for p-ERK and p-AKT by immunoblotting. Consistent with the in vitro findings above, combination therapy inhibited selumetinib-induced AKT activation (Fig. 6b). Taken together, these results suggest that the combination of selumetinib and BYL719 has a synergistic therapeutic effect on KRAS-mutant NSCLC.
The combination of selumetinib and BYL719 resulted in enhanced antitumor efficacy in a KRAS-mutant xenograft model. a A549 tumor cells were subcutaneously injected into the flank of Balb/c nude mice. Drug treatments began after the tumor reached a volume of ~100 mm3 (day 0). All mice were treated with vehicle, selumetinib (25 mg/kg/d), BYL719 (25 mg/kg/d), or selumetinib plus BYL719 by oral gavage for 5 days each week for a total of 4 weeks. Error bars, SEM. (n = 10–12) **, P < 0.01 for all groups vs. vehicle; ##, P < 0.01 for selumetinib+BYL719 vs. selumetinib or BYL719 alone. b Xenografts from A were harvested for Western blot analysis on treatment day 3, approximately 3 h after their last treatment. Tumors were subsequently lysed and Western blot analysis was performed for p-Akt, Akt, p-ERK, ERK, and β-actin
Discussion
Advances in the understanding of genetic alterations in NSCLC have given rise to therapies that target specific oncogenic pathways. At present, however, there are no effective therapies for KRAS-driven lung cancers, and mutations in KRAS are associated with poor prognosis and resistance to both adjuvant therapy and targeted EGFR TKIs [37, 38]. Since MEK/ERK and PI3K/AKT are two of the key pathways in the transformational activity of mutant KRAS, the combined inhibition of MEK and PI3K may constitute an anti-KRAS therapeutic strategy.
Selumetinib is a small-molecule inhibitor that is selective for MEK. It has been investigated in clinical trials for use in the treatment of advanced NSCLC, melanoma, and a variety of other cancers [7, 11, 39]. BIM, a member of the intrinsic apoptosis pathway, has been shown to mediate selumetinib-induced apoptosis in patients with lung cancer [29, 30, 33]. Although intrinsic and acquired resistance to this compound occurs, especially in NSCLC, the precise underlying mechanism remains controversial. Several specific genetic mutations have been suggested as predictors of sensitivity to MEK inhibitors, such as BRAF, MEK1, PI3Kα, and PTEN [40, 18, 41, 13]. However, more evidence indicates that feedback activation of compensatory pathways is responsible for resistance to MEK inhibitors, and identifying and targeting those pathways may help overcome resistance and induce synergistic antitumor effects [21, 42, 25, 12].
Previous studies have reported that resistance to selumetinib in lung cancer cells is mediated by AKT activation [17, 26, 14]. It has been shown that dual-agent combination therapy using selumetinib and the AKT inhibitor MK2206 resulted in synergistic effects on cell viability in vitro as well as tumor growth in KRAS-driven NSCLC tumors in vivo [17]. In another report, down-regulation of PIK3CA resensitized cells with co-occurring KRAS and PIK3CA mutations to MEK inhibition [14]. Collectively, these findings demonstrate that PI3K pathway activation is a major mechanism of resistance that impairs the efficacy of MEK inhibitors in KRAS-mutant cancers. Thus, we hypothesized that dual inhibition of MEK and PI3K could synergistically induce antitumor effects in KRAS-mutant NSCLC.
In this study we demonstrated that the combination of the MEK inhibitor selumetinib and the PI3Kα inhibitor BYL719 can induce synergistic inhibition of tumor growth in vitro and in vivo. Previous studies reported that selumetinib -resistant cells expressed higher levels of p-Akt than sensitive cells, and that A549 cells showed persistent activation of AKT and were resistant to selumetinib [15, 16]. In the same manner, due to increased AKT phosphorylation, selumetinib caused only a partial suppression of cell viability in KRAS-mutant A549 cells in this study. In contrast, in the presence of both selumetinib and BYL719, AKT signaling was strongly suppressed and a highly synergistic induction of apoptosis was observed. The PI3K/AKT and MEK/ERK pathways converge on the pro-apoptotic Bcl-2 homology 3 (BH3) family of proteins, which regulate apoptosis [30]. It has been recently reported that induction of p-BAD is required for selumetinib -resistance [25]. Therefore, we examined protein levels of this family and found that the combination of selumetinib and BYL719 led to a complete inhibition of phosphorylation of the serine 136 residue on the pro-apoptotic protein BAD. These findings provide evidence that selumetinib -induced S136 site phosphorylation occurs through the PK3K/AKT pathway. It has previously been shown that BAD is a downstream target that can integrate EGFR/ERK and PI3K/AKT signaling in PTEN-negative/EGFR amplified tumors, and that knocking down BAD significantly attenuates the effects of combined pathway inhibition in breast and colon cancer cells [43, 19]. In addition, phosphorylation of BAD sequesters it in 14-3-3 protein complexes at the plasma membrane, thereby inhibiting its pro-apoptotic action [35, 44, 45]. In this study, the combination of selumetinib and BYL719 induced synergistic inhibition of p-BAD along with increased PARP cleavage, which is consistent with previous reports.
In summary, we have shown that treatment with BYL719, a PI3Kα specific inhibitor which is currently in early phase clinical trials, is able to overcome resistance to MEK inhibition in selumetinib-resistant cancer cell lines both in vitro and in vivo. These results suggest that the PI3K/AKT pathway could be activated in human cancer cells with intrinsic resistance to selective MEK inhibitors, and represent a rationale for the investigation of combined MEK and PI3K inhibitors for treatment of NSCLC.
References
Pylayeva-Gupta Y, Grabocka E, Bar-Sagi D (2011) RAS oncogenes: weaving a tumorigenic web. Nat Rev Cancer 11(11):761–774. doi:10.1038/nrc3106
Roberts PJ, Stinchcombe TE, Der CJ, Socinski MA (2010) Personalized medicine in non-small-cell lung cancer: is KRAS a useful marker in selecting patients for epidermal growth factor receptor-targeted therapy? J Clin Oncol : Off J Am Soc Clin Oncol 28(31):4769–4777. doi:10.1200/JCO.2009.27.4365
Mascaux C, Iannino N, Martin B, Paesmans M, Berghmans T, Dusart M, Haller A, Lothaire P, Meert AP, Noel S, Lafitte JJ, Sculier JP (2005) The role of RAS oncogene in survival of patients with lung cancer: a systematic review of the literature with meta-analysis. Br J Cancer 92(1):131–139. doi:10.1038/sj.bjc.6602258
Karachaliou N, Mayo C, Costa C, Magri I, Gimenez-Capitan A, Molina-Vila MA, Rosell R (2013) KRAS mutations in lung cancer. Clin Lung Cancer 14(3):205–214. doi:10.1016/j.cllc.2012.09.007
Cox AD, Der CJ (2002) Ras family signaling: therapeutic targeting. Cancer Biol Ther 1(6):599–606
Young A, Lyons J, Miller AL, Phan VT, Alarcon IR, McCormick F (2009) Ras signaling and therapies. Adv Cancer Res 102:1–17. doi:10.1016/S0065-230X(09)02001-6
Adjei AA, Cohen RB, Franklin W, Morris C, Wilson D, Molina JR, Hanson LJ, Gore L, Chow L, Leong S, Maloney L, Gordon G, Simmons H, Marlow A, Litwiler K, Brown S, Poch G, Kane K, Haney J, Eckhardt SG (2008) Phase I pharmacokinetic and pharmacodynamic study of the oral, small-molecule mitogen-activated protein kinase kinase 1/2 inhibitor AZD6244 (ARRY-142886) in patients with advanced cancers. J Clin Oncol : Off J Am Soc Clin Oncol 26(13):2139–2146. doi:10.1200/JCO.2007.14.4956
Friday BB, Adjei AA (2008) Advances in targeting the Ras/Raf/MEK/Erk mitogen-activated protein kinase cascade with MEK inhibitors for cancer therapy. Clin Cancer Res : Off J Am Assoc Cancer Res 14(2):342–346. doi:10.1158/1078-0432.CCR-07-4790
Yeh TC, Marsh V, Bernat BA, Ballard J, Colwell H, Evans RJ, Parry J, Smith D, Brandhuber BJ, Gross S, Marlow A, Hurley B, Lyssikatos J, Lee PA, Winkler JD, Koch K, Wallace E (2007) Biological characterization of ARRY-142886 (AZD6244), a potent, highly selective mitogen-activated protein kinase kinase 1/2 inhibitor. Clin Cancer Res : Off J Am Assoc Cancer Res 13(5):1576–1583. doi:10.1158/1078-0432.CCR-06-1150
Davies BR, Logie A, McKay JS, Martin P, Steele S, Jenkins R, Cockerill M, Cartlidge S, Smith PD (2007) AZD6244 (ARRY-142886), a potent inhibitor of mitogen-activated protein kinase/extracellular signal-regulated kinase kinase 1/2 kinases: mechanism of action in vivo, pharmacokinetic/pharmacodynamic relationship, and potential for combination in preclinical models. Mol Cancer Ther 6(8):2209–2219. doi:10.1158/1535-7163.MCT-07-0231
Bennouna J, Lang I, Valladares-Ayerbes M, Boer K, Adenis A, Escudero P, Kim TY, Pover GM, Morris CD, Douillard JY (2011) A Phase II, open-label, randomised study to assess the efficacy and safety of the MEK1/2 inhibitor AZD6244 (ARRY-142886) versus capecitabine monotherapy in patients with colorectal cancer who have failed one or two prior chemotherapeutic regimens. Investig New Drugs 29(5):1021–1028. doi:10.1007/s10637-010-9392-8
Troiani T, Vecchione L, Martinelli E, Capasso A, Costantino S, Ciuffreda LP, Morgillo F, Vitagliano D, D’Aiuto E, De Palma R, Tejpar S, Van Cutsem E, De Lorenzi M, Caraglia M, Berrino L, Ciardiello F (2012) Intrinsic resistance to selumetinib, a selective inhibitor of MEK1/2, by cAMP-dependent protein kinase A activation in human lung and colorectal cancer cells. Br J Cancer 106(10):1648–1659. doi:10.1038/bjc.2012.129
Emery CM, Vijayendran KG, Zipser MC, Sawyer AM, Niu L, Kim JJ, Hatton C, Chopra R, Oberholzer PA, Karpova MB, MacConaill LE, Zhang J, Gray NS, Sellers WR, Dummer R, Garraway LA (2009) MEK1 mutations confer resistance to MEK and B-RAF inhibition. Proc Natl Acad Sci U S A 106(48):20411–20416. doi:10.1073/pnas.0905833106
Wee S, Jagani Z, Xiang KX, Loo A, Dorsch M, Yao YM, Sellers WR, Lengauer C, Stegmeier F (2009) PI3K pathway activation mediates resistance to MEK inhibitors in KRAS mutant cancers. Cancer Res 69(10):4286–4293. doi:10.1158/0008-5472.CAN-08-4765
Meng J, Peng H, Dai B, Guo W, Wang L, Ji L, Minna JD, Chresta CM, Smith PD, Fang B, Roth JA (2009) High level of AKT activity is associated with resistance to MEK inhibitor AZD6244 (ARRY-142886). Cancer Biol Ther 8(21):2073–2080
Yoon YK, Kim HP, Han SW, Oh Do Y, Im SA, Bang YJ, Kim TY (2010) KRAS mutant lung cancer cells are differentially responsive to MEK inhibitor due to AKT or STAT3 activation: implication for combinatorial approach. Mol Carcinog 49(4):353–362. doi:10.1002/mc.20607
Meng J, Dai B, Fang B, Bekele BN, Bornmann WG, Sun D, Peng Z, Herbst RS, Papadimitrakopoulou V, Minna JD, Peyton M, Roth JA (2010) Combination treatment with MEK and AKT inhibitors is more effective than each drug alone in human non-small cell lung cancer in vitro and in vivo. PLoS One 5(11):e14124. doi:10.1371/journal.pone.0014124
Engelman JA, Chen L, Tan X, Crosby K, Guimaraes AR, Upadhyay R, Maira M, McNamara K, Perera SA, Song Y, Chirieac LR, Kaur R, Lightbown A, Simendinger J, Li T, Padera RF, Garcia-Echeverria C, Weissleder R, Mahmood U, Cantley LC, Wong KK (2008) Effective use of PI3K and MEK inhibitors to treat mutant Kras G12D and PIK3CA H1047R murine lung cancers. Nat Med 14(12):1351–1356. doi:10.1038/nm.1890
She QB, Halilovic E, Ye Q, Zhen W, Shirasawa S, Sasazuki T, Solit DB, Rosen N (2010) 4E-BP1 is a key effector of the oncogenic activation of the AKT and ERK signaling pathways that integrates their function in tumors. Cancer Cell 18(1):39–51. doi:10.1016/j.ccr.2010.05.023
Kinross KM, Brown DV, Kleinschmidt M, Jackson S, Christensen J, Cullinane C, Hicks RJ, Johnstone RW, McArthur GA (2011) In vivo activity of combined PI3K/mTOR and MEK inhibition in a Kras(G12D);Pten deletion mouse model of ovarian cancer. Mol Cancer Ther 10(8):1440–1449. doi:10.1158/1535-7163.MCT-11-0240
Heavey S, O’Byrne KJ, Gately K (2014) Strategies for co-targeting the PI3K/AKT/mTOR pathway in NSCLC. Cancer Treat Rev 40(3):445–456. doi:10.1016/j.ctrv.2013.08.006
Castellano E, Downward J (2011) RAS interaction with PI3K: more than just another effector pathway. Genes Cancer 2(3):261–274. doi:10.1177/1947601911408079
Furet P, Guagnano V, Fairhurst RA, Imbach-Weese P, Bruce I, Knapp M, Fritsch C, Blasco F, Blanz J, Aichholz R, Hamon J, Fabbro D, Caravatti G (2013) Discovery of NVP-BYL719 a potent and selective phosphatidylinositol-3 kinase alpha inhibitor selected for clinical evaluation. Bioorg Med Chem Lett 23(13):3741–3748. doi:10.1016/j.bmcl.2013.05.007
Fritsch C, Huang A, Chatenay-Rivauday C, Schnell C, Reddy A, Liu M, Kauffmann A, Guthy D, Erdmann D, De Pover A, Furet P, Gao H, Ferretti S, Wang Y, Trappe J, Brachmann SM, Maira SM, Wilson C, Boehm M, Garcia-Echeverria C, Chene P, Wiesmann M, Cozens R, Lehar J, Schlegel R, Caravatti G, Hofmann F, Sellers WR (2014) Characterization of the novel and specific PI3Kalpha inhibitor NVP-BYL719 and development of the patient stratification strategy for clinical trials. Mol Cancer Ther 13(5):1117–1129. doi:10.1158/1535-7163.MCT-13-0865
Sun C, Hobor S, Bertotti A, Zecchin D, Huang S, Galimi F, Cottino F, Prahallad A, Grernrum W, Tzani A, Schlicker A, Wessels LF, Smit EF, Thunnissen E, Halonen P, Lieftink C, Beijersbergen RL, Di Nicolantonio F, Bardelli A, Trusolino L, Bernards R (2014) Intrinsic resistance to MEK inhibition in KRAS mutant lung and colon cancer through transcriptional induction of ERBB3. Cell Rep 7(1):86–93. doi:10.1016/j.celrep.2014.02.045
Balmanno K, Chell SD, Gillings AS, Hayat S, Cook SJ (2009) Intrinsic resistance to the MEK1/2 inhibitor AZD6244 (ARRY-142886) is associated with weak ERK1/2 signalling and/or strong PI3K signalling in colorectal cancer cell lines. Int J Cancer J Int Cancer 125(10):2332–2341. doi:10.1002/ijc.24604
Brady SW, Zhang J, Seok D, Wang H, Yu D (2014) Enhanced PI3K p110alpha signaling confers acquired lapatinib resistance that can be effectively reversed by a p110alpha-selective PI3K inhibitor. Mol Cancer Ther 13(1):60–70. doi:10.1158/1535-7163.MCT-13-0518
Serra V, Scaltriti M, Prudkin L, Eichhorn PJ, Ibrahim YH, Chandarlapaty S, Markman B, Rodriguez O, Guzman M, Rodriguez S, Gili M, Russillo M, Parra JL, Singh S, Arribas J, Rosen N, Baselga J (2011) PI3K inhibition results in enhanced HER signaling and acquired ERK dependency in HER2-overexpressing breast cancer. Oncogene 30(22):2547–2557. doi:10.1038/onc.2010.626
Faber AC, Li D, Song Y, Liang MC, Yeap BY, Bronson RT, Lifshits E, Chen Z, Maira SM, Garcia-Echeverria C, Wong KK, Engelman JA (2009) Differential induction of apoptosis in HER2 and EGFR addicted cancers following PI3K inhibition. Proc Natl Acad Sci U S A 106(46):19503–19508. doi:10.1073/pnas.0905056106
Cragg MS, Jansen ES, Cook M, Harris C, Strasser A, Scott CL (2008) Treatment of B-RAF mutant human tumor cells with a MEK inhibitor requires Bim and is enhanced by a BH3 mimetic. J Clin Invest 118(11):3651–3659. doi:10.1172/JCI35437
Corcoran RB, Cheng KA, Hata AN, Faber AC, Ebi H, Coffee EM, Greninger P, Brown RD, Godfrey JT, Cohoon TJ, Song Y, Lifshits E, Hung KE, Shioda T, Dias-Santagata D, Singh A, Settleman J, Benes CH, Mino-Kenudson M, Wong KK, Engelman JA (2013) Synthetic lethal interaction of combined BCL-XL and MEK inhibition promotes tumor regressions in KRAS mutant cancer models. Cancer Cell 23(1):121–128. doi:10.1016/j.ccr.2012.11.007
Dai B, Meng J, Peyton M, Girard L, Bornmann WG, Ji L, Minna JD, Fang B, Roth JA (2011) STAT3 mediates resistance to MEK inhibitor through microRNA miR-17. Cancer Res 71(10):3658–3668. doi:10.1158/0008-5472.CAN-10-3647
Meng J, Fang B, Liao Y, Chresta CM, Smith PD, Roth JA (2010) Apoptosis induction by MEK inhibition in human lung cancer cells is mediated by Bim. PLoS One 5(9):e13026. doi:10.1371/journal.pone.0013026
Liu Y, Sun SY, Owonikoko TK, Sica GL, Curran WJ, Khuri FR, Deng X (2012) Rapamycin induces bad phosphorylation in association with its resistance to human lung cancer cells. Mol Cancer Ther 11(1):45–56. doi:10.1158/1535-7163.MCT-11-0578
Datta SR, Katsov A, Hu L, Petros A, Fesik SW, Yaffe MB, Greenberg ME (2000) 14-3-3 proteins and survival kinases cooperate to inactivate BAD by BH3 domain phosphorylation. Mol Cell 6(1):41–51
Masters SC, Yang H, Datta SR, Greenberg ME, Fu H (2001) 14-3-3 inhibits bad-induced cell death through interaction with serine-136. Mol Pharmacol 60(6):1325–1331
Riely GJ, Marks J, Pao W (2009) KRAS mutations in non-small cell lung cancer. Proc Am Thorac Soc 6(2):201–205. doi:10.1513/pats.200809-107LC
Mao C, Qiu LX, Liao RY, Du FB, Ding H, Yang WC, Li J, Chen Q (2010) KRAS mutations and resistance to EGFR-TKIs treatment in patients with non-small cell lung cancer: a meta-analysis of 22 studies. Lung Cancer 69(3):272–278. doi:10.1016/j.lungcan.2009.11.020
Janne PA, Shaw AT, Pereira JR, Jeannin G, Vansteenkiste J, Barrios C, Franke FA, Grinsted L, Zazulina V, Smith P, Smith I, Crino L (2013) Selumetinib plus docetaxel for KRAS-mutant advanced non-small-cell lung cancer: a randomised, multicentre, placebo-controlled, phase 2 study. Lancet Oncol 14(1):38–47. doi:10.1016/S1470-2045(12)70489-8
Pratilas CA, Taylor BS, Ye Q, Viale A, Sander C, Solit DB, Rosen N (2009) (V600E)BRAF is associated with disabled feedback inhibition of RAF-MEK signaling and elevated transcriptional output of the pathway. Proc Natl Acad Sci U S A 106(11):4519–4524. doi:10.1073/pnas.0900780106
Pratilas CA, Hanrahan AJ, Halilovic E, Persaud Y, Soh J, Chitale D, Shigematsu H, Yamamoto H, Sawai A, Janakiraman M, Taylor BS, Pao W, Toyooka S, Ladanyi M, Gazdar A, Rosen N, Solit DB (2008) Genetic predictors of MEK dependence in non-small cell lung cancer. Cancer Res 68(22):9375–9383. doi:10.1158/0008-5472.CAN-08-2223
Acquaviva J, Smith DL, Sang J, Friedland JC, He S, Sequeira M, Zhang C, Wada Y, Proia DA (2012) Targeting KRAS-mutant non-small cell lung cancer with the Hsp90 inhibitor ganetespib. Mol Cancer Ther 11(12):2633–2643. doi:10.1158/1535-7163.MCT-12-0615
She QB, Solit DB, Ye Q, O’Reilly KE, Lobo J, Rosen N (2005) The BAD protein integrates survival signaling by EGFR/MAPK and PI3K/Akt kinase pathways in PTEN-deficient tumor cells. Cancer Cell 8(4):287–297. doi:10.1016/j.ccr.2005.09.006
Scheid MP, Schubert KM, Duronio V (1999) Regulation of bad phosphorylation and association with Bcl-x(L) by the MAPK/Erk kinase. J Biol Chem 274(43):31108–31113
Zha J, Harada H, Yang E, Jockel J, Korsmeyer SJ (1996) Serine phosphorylation of death agonist BAD in response to survival factor results in binding to 14-3-3 not BCL-X(L). Cell 87(4):619–628
Acknowledgments
This study was supported in part by a grant from the Samsung Biomedical Research Institute (GE1-B3-081-1). The authors thank AstraZeneca Pharmaceutics for selumetinib.
Ethical standards
All experiments were performed in accordance with the regulation of the Institutional Animal Care and Use Committee (IACUC) at the Samsung Biomedical Research Institute (SBRI) and with the applicable laws and regulations of Korea.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ku, B.M., Jho, E.H., Bae, YH. et al. BYL719, a selective inhibitor of phosphoinositide 3-Kinase α, enhances the effect of selumetinib (AZD6244, ARRY-142886) in KRAS-mutant non-small cell lung cancer. Invest New Drugs 33, 12–21 (2015). https://doi.org/10.1007/s10637-014-0163-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-014-0163-9