Abstract
Hepatic stellate cells (HSCs) are the main extracellular matrix (ECM)-producing cells in liver fibrogenesis. The excessive synthesis of ECM proteins deteriorates hepatic architecture and results in liver fibrosis and cirrhosis. This study investigated the role of bone morphogenetic protein 7 (BMP7) as a member of the transforming growth factor (TGF)-ß superfamily in chronic liver disease. Plasma levels of BMP7 were significantly elevated in patients with chronic liver disease compared with healthy controls. Immunohistochemistry of cirrhotic human liver demonstrated upregulated BMP7 protein expression in hepatocytes as compared with normal human liver. Because gene expression for all putative BMP7 receptors was induced during the culture activation process of primary human HSCs, we studied the effects of BMP7 on hTERT immortalized human HSCs in vitro. BMP7, as expressed and secreted after infection with adenoviruses encoding BMP7 (AdBMP7), increased proliferation of HSCs. The mRNA and protein expression of type I collagen and fibronectin was increased in BMP7-stimulated HSCs. Elevated systemic and hepatic levels of BMP7 in patients with chronic liver disease may contribute to progression of liver fibrogenesis in vivo.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Bone morphogenetic proteins (BMPs) are members of the transforming growth factor (TGF)-ß superfamily of secreted signaling molecules [1]. Dimeric BMPs bind to and bring together 2 distinct kinds of transmembrane serine/threonine kinase receptors, type I and II receptors. Within that receptor complex the constitutively active type II receptor recruits and transphosphorylates type I receptor. BMP7 interacts with several type II chains, including BMP receptor (BMPR)-II, activin receptor (ActR)-II and ActR-IIB, which in turn can activate BMPR-IA, BMPR-IB, and ActR-I [2]. The activated type I receptor transiently associates with and phosphorylates Smad1, Smad5, and Smad8, which then form heteromeric complexes with Smad4. These complexes translocate to the nucleus, where the proteins function as transcriptional activators through their interaction with DNA-binding proteins [1]. There is growing evidence that BMPs initiate other non-Smad intracellular pathways, including mitogen-activated protein kinase family members, as well as the PI3 kinase pathways [3–8].
Although the underlying cause of chronic liver disease can be as a different as chronic virus hepatitis, alcohol abuse, autoimmune disorders or others, the cellular and pathologic mechanisms of liver fibrosis and – as an end stage – cirrhosis are relatively common and uniform. Liver fibrosis is characterized by an accumulation of extracellular matrix (ECM) proteins, including fibronectin and fibrillar types I and III collagens [9]. In cirrhotic liver, accumulation of ECM disrupts the hepatic architecture by formation of fibrous scars and nodules of regenerating hepatocytes [9]. The activation process of hepatic stellate cells (HSCs) is the central event leading to hepatic fibrosis. Upon a fibrogenic stimulus, quiescent HSCs become activated, a process characterized by an increase in proliferation, changes in cellular morphology to a more myofibroblast-like cell type, and an upregulation of ECM proteins [9].
During the activation of HSCs, enhanced cytokine responses occur through increased expression of cell membrane receptors and enhanced signaling. Although the critical role for TGF-ß1 in hepatic fibrogenesis is well established, the potential role of BMPs in chronic liver disease and for the activation process of HSCs is less clear. Interestingly, expression and phosphorylation of Smad1 is increased during the activation of rat HSCs [10]. The aim of our study was to assess the role of BMP7 in chronic liver disease and in human HSCs.
Materials and methods
Patients
The study population consisted of 111 patients with chronic liver disease who were evaluated as inpatients for potential liver transplantation at the Hannover Medical School. Ninety-six healthy volunteers served as controls (Table 1). The study was approved by the local ethical committee, and written informed consent was obtained from each participant. Routine and experimental blood samples were collected in EDTA separator tubes, centrifuged at 2000 ×g at 4°C for 10 minutes, and plasma was stored at −80°C.
Cell culture
Isolation and culture of primary human HSCs, rat HSCs, and rat hepatocytes were described previously [11–14]. Human telomerase reverse transcriptase (hTERT) HSCs immortalized by infection with a VSV-G pseudotyped vector encoding hTERT resemble the activated phenotype of human HSCs [11, 12]. These cells are called hTERT HSCs throughout the paper.
Adenoviruses and adenoviral infections
The adenovirus AdBMP7 was kindly provided by Dr. R. T. Franschesi (University of Michigan, Ann Arbor, MI) [15]. AdEGFP-expressing enhanced green fluorescence protein (EGFP) was used as a control virus in all experiments [16]. Amplification and purification of adenoviruses were performed as described [13]. HSCs were infected as previously described [13, 17]. To ensure a reproducible amount of BMP7 in the supernatant of AdBMP7-infected hTERT HSCs, cells were plated with a constant density (7.7 × 104 cells per milliliter growth medium and per 27 mm2 growth surface area).
RNA isolation and reverse transcriptase polymerase chain reaction
Total RNA from cultured cells was extracted using TRIZOL (Invitrogen, Carlsbad, CA) according to the manufacturer’s protocol. RNA was digested with DNAse I for 10 minutes at 37°C. Semiquantitative reverse transcriptase polymerase chain reaction (RT-PCR) was performed as described previously [11, 13, 18) using published primer sequences and PCR conditions: BMPR-IA [19], BMPR-IB [20], BMPR-II [21], ActR-I, ActR-II, ActR-IIB [22], smooth muscle α-actin (α-SMA) [23], and cellular retinol-binding protein I (CRBP-I) [24]. The cycle number for each amplicon was determined to be in the linear range of amplification. Real-time PCR was performed for 40 cycles of 15 seconds at 95°C and 60 seconds at 60°C using an ABI 7000 sequence detection system. Probes and primers for collagen α1(I), α-SMA, fibronectin 1, BMP7, and 18S were designed by ABI.
ELISA for BMP7 and phospho-p38
For measuring BMP7 homodimers in human plasma samples, a commercially available ELISA was used according to the manufacturer’s protocol (R&D Systems, Minneapolis, MN). To analyze BMP7 concentrations in the supernatant of AdEGFP- and AdBMP7-infected hTERT HSCs, culture medium was collected 24 and 48 hours after adenoviral infection.
For phospho-p38 ELISA, after adenoviral infection, hTERT HSCs were starved in serum-free medium for 24 hours and stimulated with recombinant interleukin (IL)-1ß (2.5 ng/mL; R&D Systems) for 15 minutes or were left untreated. Whole cell extracts were prepared, and ELISA for phospho-p38 (Biosource, Camarillo, CA) was performed in duplicate according to the manufacturer’s protocol. The concentration of phospho-p38 (U/mL) of each sample was normalized to the protein content of whole cell extracts (μg).
Immunohistochemistry
Human liver tissue samples were obtained from patients undergoing liver resection for metastatic liver tumors. Cirrhotic human liver tissue samples were obtained from patients who underwent liver transplantation. Immunohistochemical staining for BMP7 was performed as described [25].
Western blot analysis
For signaling studies, after adenoviral infection of hTERT HSCs, medium was replaced by serum-free medium and cells were incubated for 24 hours. HSCs were subsequently stimulated with recombinant platelet-derived growth factor (PDGF)-BB (20 ng/mL), TGF-ß1 (5 ng/mL), tumor necrosis factor (TNF)-α (30 ng/mL; all from R&D Systems) or were left untreated. For all other studies, hTERT HSCs were cultured after viral infection in regular growth medium containing 10% FCS for additional 24 or 48 hours as indicated. Whole cell extracts were prepared, and Western blotting was performed using 25–100 μg protein per lane as described [12, 18, 26]. Blots were either reprobed using anti-tubulin antibody or whole cell extracts were run in duplicate on the same gel and probed for tubulin. Primary antibodies were anti-phospho-p44/42, anti-phospho-Akt, anti-phospho-Smad1 (Cell Signaling, Beverly, MA), anti–phospho-c-Jun, anti–α-tubulin, anti-PCNA (Santa Cruz Biotechnology, Santa Cruz, CA), anti-fibronectin (BD Biosciences Pharmingen, San Diego, CA), anti-collagen type I (Rockland, Gilbertsville, PA), and anti-smooth muscle α-actin (DAKO, Carpinteria, CA).
Electrophoretic mobility shift assay
After adenoviral infection, hTERT HSCs were starved for 24 hours in serum-free medium, then treated with 5 ng/mL TGF-ß1 (R&D Systems) for 15 or 30 minutes or were left untreated. Nuclear extracts were extracted and electrophoretic mobility shift assay (EMSA) for Smad3/Smad4 was performed as described [18, 27]. For supershift analysis or competition experiments, extracts were incubated with 4 μL of anti-Smad4 antibody (Santa Cruz Biotechnology) or with the nonradiolabeled probe on ice, respectively.
Statistics
Results from the measurements in humans are reported as medians and range because of the skewed distribution of most parameters in patients. Spearman rank correlation was calculated to quantify the degree of linear association between 2 variables. Comparisons between 2 groups were performed by the Mann–Whitney U test; multiple comparisons between subgroups were analyzed by Kruskal–Wallis ANOVA with the closed testing procedure and Mann–Whitney U test used for post hoc analysis [28]. P < .05 was considered statistically significant. All statistics were performed using SPSS statistical package. The results from in vitro experiments were analyzed for statistical significance according to the Mann–Whitney U statistic test.
Results
BMP7 is elevated in patients with chronic liver disease as compared to healthy controls
To investigate the role of BMP7 in liver fibrosis and cirrhosis, plasma levels of BMP7 in patients with chronic liver disease (n = 111; median age, 46 years; range, 18–70) were measured and compared to healthy controls. Because we observed a linear increase of BMP7 with the age in healthy volunteers (correlation coefficient r = 0.453; P < .001), the control population (n = 96; median age, 48 years; range, 20–75) was strictly age matched with the patient group. In healthy controls, BMP7 had a median of 12.6 pg/mL (range, 2.4–168.6), whereas in patients with chronic liver disease, BMP7 was significantly elevated to a median of 16.6 pg/mL (range, 2.4–240.2; P = .004; Fig. 1A). Furthermore, among patients with chronic liver disease, BMP7 was significantly increased in patients with a Child A–C cirrhosis (median, 16.9 pg/mL; range, 4.4–240.2) as compared to patients without cirrhosis (median, 14.7 pg/mL; range, 2.4–30.5; P = .042; Fig. 1B). Highest BMP7 levels were found in Child C cirrhosis (median, 21.5 pg/mL; range, 4.7–64.9; P < .04 to all other classes; Fig. 1C). In addition, BMP7 was significantly higher in patients with Child A (median, 16.6 pg/mL; range, 4.4–240.2; P = .033), Child B (median, 15.7 pg/mL; range, 4.4–64.0; P = .037), or Child C (P = .001) cirrhosis as compared to healthy controls (Fig. 1C).
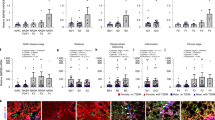
BMP7 plasma levels are enhanced in patients with chronic liver disease. A BMP7 plasma levels are significantly elevated in patients with chronic liver diseases (n = 111, median 16.6 pg/mL; range, 2.4–240.2) when compared with an age-matched healthy control group (n = 96, median 12.6 pg/mL; range, 2.4–168.6; P = .004). B BMP7 plasma levels are significantly higher in patients with Child A–C cirrhosis (n = 93, median 16.9 pg/mL; range, 4.4–240.2) than chronic liver disease patients without cirrhosis (n = 18, median 14.7 pg/mL; range, 2.4–30.5; P = .042). C BMP7 was significantly higher in patients with Child A (n = 35, median 16.6 pg/mL; range, 4.4–240.2, p = 0.033), Child B (n = 44, median 15.7 pg/mL; range, 4.4–64.0; P = .037), or Child C (n = 14, median 21.5 pg/mL; range, 4.7–64.9; P = .001) cirrhosis as compared with healthy controls. BMP7 levels were also significantly higher in Child C cirrhosis as compared to all other classes (P < .04). Comparisons between groups are illustrated with box plot graphics, where the bold line indicates the median per group, the box represents 50% of the values, and horizontal lines show minimum and maximum values of the calculated nonoutlier values; ○ and * indicate outlier values
BMP7 protein expression is upregulated in hepatocytes of cirrhotic human liver
To identify the cellular source of BMP7 in vivo, we investigated the expression of BMP7 in human liver tissues by using immunohistochemistry. A weak staining for BMP7 was detected in hepatocytes of normal human liver (Fig. 2A, B) as compared with negative control staining (Fig. 2E). Much stronger staining intensity was detected in hepatocytes of cirrhotic human liver indicative of increased BMP7 protein expression (Fig. 2C, D, negative control 2F). However, cholangiocytes and HSCs in fibrotic septa did not express BMP7. Consistent with these data, cultured primary rat hepatocytes expressed higher levels of BMP7 mRNA as compared to culture activated rat HSCs (Fig. 2G).
BMP7 expression in human liver tissue. BMP7 protein expression was analyzed by immunohistochemistry in normal human liver (A and B) and in liver tissue from a patient with cryptogenic liver cirrhosis (C and D). Negative control staining for normal human (E) and cirrhotic liver (F). Original magnification ×100 (A and C) or ×400 (B, D–F). G Expression of BMP7 mRNA was assessed in cultured rat hepatocytes, and in activated rat HSCs (culture day 12) using real-time RT-PCR and normalized to 18S RNA
The mRNA expression of putative BMP7 receptors is induced during culture activation of primary human HSCs
To determine whether HSCs might be a target of BMP7, the mRNA expression of putative receptors for BMP7 was assessed in primary quiescent and culture-activated human HSCs by semiquantitative RT-PCR analysis. Quiescent human HSCs after the isolation from normal human liver (day 0) did not express any of the receptors investigated (Fig. 3). Activated HSCs on culture day 2 showed an induction of BMPR-IA, ActR-I and ActR-II mRNA as compared to quiescent human HSCs. BMPR-IA, ActR-I and ActR-II mRNA expression further increased when HSCs were cultured for a period up to 17 days (Fig. 3). BMPR-IB and BMPR-II mRNA was exclusively detectable in activated human HSCs cultured for 17 days (Fig. 3). The induction of ActR-IIB mRNA peaked in HSCs on culture days 2 and 17 (Fig. 3). In addition, we confirmed that in our experiments α-SMA mRNA as a marker of activation gradually increased during culture activation (Fig. 3). CRBP-I served as housekeeping gene; CRBP-I is similarly expressed in quiescent and activated human HSCs [29].
The expression of putative BMP7 receptors is upregulated in culture activated human HSCs. The expression of BMPR-IA, BMPR-IB, BMPR-II, ActR-I, ActR-IIB, ActR-II, α-SMA, and CRBP-I was analyzed by semiquantitative RT-PCR using 1 μg of total RNA. With primers specific for each amplicon, cDNA was analyzed from human HSCs freshly isolated (day 0) or cultured for 2, 7, 12, or 17 days as indicated. CRBP-I was amplified to confirm equal amount of mRNA was present in each sample. Negative controls without cDNA (H20) were performed with each PCR reaction. Lane M contains the molecular weight marker
Adenoviral expression of BMP7 results in increased secretion of BMP7 by human hTERT HSCs
To comprehensively study the effect of BMP7 on human HSCs, we used an adenoviral vector that expresses human BMP7 [15]. We first tested whether this approach results in an increased secretion of BMP7 in hTERT HSCs. Therefore, human hTERT HSCs were infected with AdBMP7 or AdEGFP as control, and secreted BMP7 was measured in cell culture supernatants by ELISA. BMP7 secretion was strongly induced in AdBMP7-infected human hTERT HSCs as compared with control infected hTERT HSCs. The amount of secreted BMP7 was approximately 100 ng/mL 24 hours after infection with AdBMP7, which increased to approximately 400 ng/mL after 48 hours of adenoviral infection (Fig. 4).
BMP7 secretion is increased upon adenoviral expression of BMP7 in hTERT human HSCs. hTERT human HSCs were infected with either control adenovirus AdEGFP or adenovirus encoding BMP7 (AdBMP7) for 12 hours, and then incubated with fresh medium for 24 or 48 hours. Supernatants were collected and BMP7 concentrations were measured by ELISA. Results represent the mean values ± standard error of the mean (SEM) of 4 experiments performed in duplicate
The effect of BMP7 on intracellular signaling pathways in human hTERT HSCs. hTERT HSCs were infected with AdBMP7 or AdEGFP as control. The medium was then replaced by serum-free medium 12 hours after infection, and cells were incubated for 24 hours. Subsequently, serum-starved hTERT HSCs were stimulated with (A and B) PDGF (20 ng/mL], (C) TNF-α (30 ng/mL), and (D) TGF-ß1 (5 ng/mL) for 15 or 30 minutes, or were left untreated. Whole cell lysates were subjected to Western blot analysis for (A) phospho-p44/42 (ERK1/2), (B) phospho-Akt, (C) phospho-c-Jun, and (D) phospho-Smad1. Equal protein loading was monitored by analyzing tubulin expression. All experiments were performed in duplicate; a representative blot is shown. E After adenoviral infection, hTERT HSCs were serum starved for 24 hours, and treated with IL-1ß (2.5 ng/mL) for 15 minutes, or were left untreated. Phospho-p38 was measured in whole cell lysates using a phospho-p38–specific ELISA. The concentration (U/mL) of phospho-p38 was normalized to the total amount of cell lysate protein analyzed. Data represent the mean values ± standard error of the mean (SEM) of 3 independent experiments performed in duplicate. F DNA binding activity of Smad proteins was assessed using EMSA. Following adenoviral infection of hTERT HSCs with AdBMP7 and AdEGFP as control, cells were starved in serum-free medium for 24 hours. hTERT HSCs were stimulated with TGF-ß1 (5 ng/mL) for 15 and 30 minutes, or were left untreated. Nuclear extracts were incubated for 20 minutes with a radiolabeled Smad3/Smad4 probe, followed by 4% nondenaturing gel electrophoresis. The TGF-ß1–induced complex is indicated by an arrow. For supershift analysis, extracts from AdEGFP infected HSCs stimulated with TGF-ß1 for 30 minutes were incubated with anti-Smad4 antibody for 30 minutes on ice before the addition of the radiolabeled probe. A competition with 200-fold excess unlabeled probe using extracts from AdEGFP infected hTERT HSCs stimulated with TGF-ß1 for 30 minutes is shown. A representative experiment is shown, which was performed in duplicate
BMP7 induces phosphorylation of Smad1 in activated human hTERT HSCs
Next we tested whether BMP7 in the supernatant modulates various signaling pathways shown to be important signal transducers during the activation process of HSCs. In activated human hTERT HSCs, BMP7 did not induce phosphorylation of ERK1/2 and Akt, or modulate PDGF-induced phosphorylation of ERK1/2 and Akt as compared to control cells (Fig. 5A, B). Similarly, BMP7 did not change the basal or TNF-α induced phosphorylation of c-Jun in hTERT HSCs (Fig. 5C). However, BMP7 caused efficient phosphorylation of Smad1 in hTERT HSCs, which was not modulated by costimulation with TGF-ß1 (Fig. 5D). Basal and IL-1ß–induced p38 phosphorylation was not modulated in AdBMP7-infected hTERT HSCs compared with control infected hTERT HSCs as assessed by phospho-p38–specific ELISA (Fig. 5E). The Smad3/4 signaling pathway is thought to be the major TGF-ß1–induced signaling pathway for fibrogenesis in HSCs. Upon TGF-ß1 stimulation, a complex was induced in control hTERT HSCs, which was not altered by BMP7 (Fig. 5F). Thus, Smad1 seems to be the preferred signaling pathway for BMP7 in human hTERT HSCs.
The effect of BMP7 on proliferation of activated human hTERT HSCs
After 48 hours of adenoviral infection with AdBMP7, hTERT HSCs showed a higher expression of PCNA protein as marker for proliferation as compared with control infected hTERT HSCs (Fig. 6A, B). However, the proliferation rate was the same in AdEGFP-infected hTERT HSCs as compared with AdBMP7-infected hTERT HSCs 24 hours after adenoviral infection (Fig. 6A, B).
The effect of BMP7 on human hTERT HSC proliferation. hTERT HSCs were either infected with AdBMP7 or AdEGFP as control, and cultured for 24 or 48 hours in the presence of 10% FCS before harvesting. Western blotting for PCNA was performed (A), and the expression of PCNA was normalized to tubulin (B). Data represent the mean values ± standard error of the mean (SEM) of 5 (24 hours) or 6 (48 hours) independent experiments (B)
BMP7 shows fibrogenic effects on activated human hTERT HSCs
The mRNA and protein expression of two ECM proteins accumulating in liver fibrosis, type I collagen and fibronectin, were determined in hTERT HSCs infected with AdEGFP as control or AdBMP7. No difference in steady state mRNA levels of collagen α1(I) was observed 24 hours after infection as assessed by real-time PCR (Fig. 7A). However, culturing hTERT HSCs for 48 hours resulted in a significant increase of endogenous collagen α1(I) mRNA by 1.9-fold in AdBMP7-infected hTERT HSCs as compared with control infected hTERT HSCs (Fig. 7A). Similarly, 48 hours, but not 24 hours, after adenoviral infection, hTERT HSCs infected with AdBMP7 showed an increase in type I collagen synthesis compared to control infected hTERT HSCs as demonstrated by western blotting (Fig. 7B). After normalization to tubulin, BMP7 increased type I collagen synthesis significantly by 3.2-fold (Fig. 7C).
Synthesis of type I collagen and fibronectin is increased by BMP7 in hTERT human HSCs. hTERT HSCs were either infected with AdBMP7 or AdEGFP as control, and cultured for 24 or 48 hours before harvesting. A and D, Total RNA was extracted, (A) collagen α1(I) mRNA and (D) fibronectin mRNA levels were measured by real-time RT-PCR and normalized to 18S RNA. The results are expressed relative to the level of hTERT HSCs infected with AdEGFP. Data represent the mean values ± standard error of the mean (SEM) of 3 experiments measured in duplicate. * P < .05 when compared with AdEGFP-infected hTERT HSCs and cultured for 48 hours. B and E, Whole cell lysates were extracted and subjected to SDS-PAGE followed by immunoblotting for (B) procollagen α1(I) or (E) fibronectin protein expression. Equal protein loading was determined by probing with anti-tubulin antibody. Shown is a typical experiment. C and F, Expression of (C) procollagen α1(I) and (F) fibronectin protein were normalized to tubulin using densitometry. Data represent the mean values ± standard error of the mean (SEM) of 4–5 independent experiments. The results are expressed relative to AdEGFP infected HSCs. * P = .009 when compared with hTERT HSCs infected with AdEGFP and cultured for 48 hours
Levels of fibronectin mRNA were found to be increased in AdBMP7-infected hTERT HSCs as compared with AdEGFP-infected hTERT HSCs as control (Fig. 7D). The increase in transcription rate of fibronectin mRNA was similar to the increase in fibronectin protein expression. BMP7 moderately elevated fibronectin protein expression levels 24 or 48 hours after adenoviral infection, as compared with control hTERT HSCs (Fig. 7E, F).
BMP7 increases smooth muscle α-actin in activated HSCs
We next investigated whether BMP7 affects expression of α-SMA as a marker of activation in HSCs. When activated HSCs were infected with AdBMP7, they showed moderately increased levels of α-SMA mRNA as determined by real-time PCR (Fig. 8A). This corresponded to increased α-SMA protein expression in AdBMP7-infected cells compared with HSCs infected with control AdEGFP as assessed by western blotting (Fig. 8B, C).
Smooth muscle α-actin expression is higher in AdBMP7-infected human hTERT HSCs as compared with control hTERT HSCs. Human hTERT HSCs were infected with adenoviruses encoding BMP7 or EGFP as control and cultured for 24 hours. A α-SMA mRNA levels were assessed using quantitative real-time RT-PCR and normalized to 18S. The results are expressed relative to the level of hTERT HSCs infected with AdEGFP. Data represent the mean values ± standard error of the mean (SEM) of 3 experiments measured in duplicate. B Cell lysates were prepared and immunoblotting using an anti–α-SMA antibody was performed. Additionally, the membrane was immunoblotted using anti-tubulin antibody to ensure equal protein loading. Shown is a representative experiment. C The protein expression level of α-SMA was normalized to tubulin. Data represent the mean values ± standard error of the mean (SEM) of 5 experiments and are expressed relative to AdEGFP-infected hTERT HSCs
Discussion
Our study demonstrates that BMP7 serum levels are elevated in patients with chronic liver disease and highest in Child C cirrhosis. Hepatocytes are the cellular source of BMP7 in human liver, and BMP7 expression is upregulated in cirrhotic human liver in vivo. We further show that gene expression of all receptors necessary for BMP7 signaling are induced during the activation process of primary human HSCs, thereby rendering activated HSCs as potential targets to the ligand BMP7 secreted by hepatocytes. Human hTERT HSCs respond to BMP7 with an increase in proliferation and in synthesis of type I collagen and fibronectin. Thus, our data indicate that BMP7, which is upregulated in patients with liver cirrhosis, might perpetuate the activation process of human HSCs and promote liver fibrogenesis in vivo.
Our principal approach to study the in vitro effect of BMP7 on hTERT HSCs was to use adenoviruses encoding human BMP7. This approach is widely used to explore the biologic effect of ectopically expressed proteins in various cells types [15]. Using a defined number of cells per volume of growth medium and per surface area of the dish, adenovirally infected hTERT HSCs were challenged with reproducible amounts of secreted BMP7. It is difficult to ascertain whether the concentrations of BMP7 used in our in vitro experiments are within the physiologic range because the concentrations in supernatants of AdBMP7-infected hTERT HSCs are much higher as compared with the amount of BMP7 measured in serum of patients with chronic liver disease. However, as demonstrated by immunohistochemistry, hepatocytes of cirrhotic liver produce enhanced levels of BMP7 as compared with normal liver, and therefore the local concentration in damaged liver tissue acting directly on neighboring cells might be considerably higher than in the circulation. Other in vitro studies used BMP7 in concentrations comparable to the concentrations we used [8, 30–32].
Whether BMP7 has fibrogenic effects is controversial. BMP7 has been shown to prevent tubulointerstitial fibrogenesis in different models of renal injury in rats [33–35]. The mechanism of renal protection is related to preservation of renal tubular epithelial integrity and to an anti-inflammatory process by downregulation of intercellular adhesive molecules and thereby reducing the number of infiltrating mononuclear cells, which secondarily prevented renal fibrogenesis [33–35]. Several in vitro studies [8, 32] support the anti-inflammatory role of BMP7. Recently, the function of BMP7 as a differentiation factor was demonstrated in vitro to contribute to regeneration of injured kidney. BMP7 induces mesenchymal-to-epithelial transition (EMT) in adult renal fibroblasts generating functional epithelial cells, and thereby counteracts the TGF-ß1–induced EMT [31, 36]. In renal fibrosis, EMT-induced accumulation of myofibroblasts and the subsequent tubular atrophy are considered key determinants during chronic renal injury [36]. Recently, kielin/chordin-like protein (KCP) has been shown to act as a potent paracrine enhancer of BMP7 signaling by increasing its affinity to the receptor [37]. KCP knockout mice are more susceptible to developing renal fibrosis and show substantial pathology after recovery [37]. Although not directly shown by the authors, the underlying mechanism might be that KCP, as a positive mediator of BMP7 signaling, reverses EMT and impacts the ability of renal epithelial cells to recover from injury [37]. Taken together, the anti-fibrogenic effect observed in vivo in animal models of renal disease seems to be secondary to the anti-inflammatory and cytoprotective effect of BMP7.
In contrast to observations in renal disease, BMP7 serum levels are elevated in patients with chronic liver disease and BMP7 expression increased in hepatocytes of cirrhotic human liver tissue, whereas BMP7 expression decreases in injured kidney [33]. These profound differences in BMP7 regulation following organ injury between liver and kidney and the above mentioned anti-inflammatory and cytoprotective effect of BMP7, might explain the differences we found in our study. BMP7 exerts fibrogenic effects on hTERT human HSCs in culture by increasing fibronectin and type I collagen expression and synthesis. However, the main cellular pathways leading to fibrosis in HSCs were not modulated by BMP7, including TGF-ß1 secretion, DNA binding activity of Smad3/4, which is thought to be the dominant fibrosis mediator of TGF-ß1 in HSCs [18], JNK, or p38 activity [13]. Consistent with our results, BMP7 was shown to induce synthesis of collagens (predominantly type II) in human chondrocytes [38–40], and type I collagen expression in rat osteosarcoma cells [41] and primary rat medial collateral ligament cells [42]. Additionally, numerous studies have shown that rhBMP7 or adenoviral-mediated gene transfer of BMP7 induce bone formation in vitro and in vivo [43].
Taken together, our results indicate that the role of BMP7 is proliferative and fibrogenic on HSCs. Under physiologic conditions, HSCs remain in their quiescent state and do not express receptors for BMP7 signaling. Following activation, HSCs express the mRNA for all putative BMP7 receptors. Elevated systemic and hepatic levels of BMP7 in patients with chronic liver disease may then contribute to progression of liver fibrogenesis.
However, it is currently unknown whether changes observed in vitro occur in vivo after BMP7 administration, and whether BMP7 acts in an autocrine manner on hepatocytes and in a paracrine manner on other resident or infiltrating cells in the liver. Ultimately, these issues deserve further investigation in a liver fibrosis model in vivo. Such studies will be necessary to fully delineate the role of BMP7 in development and progression of chronic liver disease and to elucidate the net effect of BMP7.
References
Shi Y, Massague J (2003) Mechanisms of TGF-beta signaling from cell membrane to the nucleus. Cell 113:685–700
Sebald W, Nickel J, Zhang JL, Mueller TD (2004) Molecular recognition in bone morphogenetic protein (BMP)/receptor interaction. Biol Chem 385:697–710
Zwijsen A, Verschueren K, Huylebroeck D (2003) New intracellular components of bone morphogenetic protein/Smad signaling cascades. FEBS Lett 546:133–139
Miyazono K, Kusanagi K, Inoue H (2001) Divergence and convergence of TGF-beta/BMP signaling. J Cell Physiol 187:265–276
Nohe A, Keating E, Knaus P, Petersen NO (2004) Signal transduction of bone morphogenetic protein receptors. Cell Signal 16:291–299
Hu MC, Wasserman D, Hartwig S, Rosenblum ND (2004) p38MAPK acts in the BMP7-dependent stimulatory pathway during epithelial cell morphogenesis and is regulated by Smad1. J Biol Chem 279:12051–12059
Wang SN, Lapage J, Hirschberg R (2001) Loss of tubular bone morphogenetic protein-7 in diabetic nephropathy. J Am Soc Nephrol 12:2392–2399
Lee MJ, Yang CW, Jin DC, Chang YS, Bang BK, Kim YS (2003) Bone morphogenetic protein-7 inhibits constitutive and interleukin-1 beta-induced monocyte chemoattractant protein-1 expression in human mesangial cells: role for JNK/AP-1 pathway. J Immunol 170:2557–2563
Bataller R, Brenner DA (2005) Liver fibrosis. J Clin Invest 115:209–218
Shen H, Huang G, Hadi M, Choy P, Zhang M, Minuk GY, Chen Y, Gong Y (2003) Transforming growth factor-beta1 downregulation of Smad1 gene expression in rat hepatic stellate cells. Am J Physiol Gastrointest Liver Physiol 285:G539–546
Schnabl B, Choi YH, Olsen JC, Hagedorn CH, Brenner DA (2002) Immortal activated human hepatic stellate cells generated by ectopic telomerase expression. Lab Invest 82:323–333
Schnabl B, Purbeck CA, Choi YH, Hagedorn CH, Brenner DA (2003) Replicative senescence of activated human hepatic stellate cells is accompanied by a pronounced inflammatory but less fibrogenic phenotype. Hepatology 37:653–664
Schnabl B, Bradham CA, Bennett BL, Manning AM, Stefanovic B, Brenner DA (2001) TAK1/JNK and p38 have opposite effects on rat hepatic stellate cells. Hepatology 34:953–963
Schwabe RF, Bradham CA, Uehara T, Hatano E, Bennett BL, Schoonhoven R, Brenner DA (2003) c-Jun-N-terminal kinase drives cyclin D1 expression and proliferation during liver regeneration. Hepatology 37:824–832
Franceschi RT, Wang D, Krebsbach PH, Rutherford RB (2000) Gene therapy for bone formation: in vitro and in vivo osteogenic activity of an adenovirus expressing BMP7. J Cell Biochem 78:476–486
Neumann E, Judex M, Kullmann F, Grifka J, Robbins PD, Pap T, Gay RE, Evans CH, Gay S, Scholmerich J, Muller-Ladner U (2002) Inhibition of cartilage destruction by double gene transfer of IL-1Ra and IL-10 involves the activin pathway. Gene Ther 9:1508–1519
Hellerbrand C, Jobin C, Iimuro Y, Licato L, Sartor RB, Brenner DA (1998) Inhibition of NFkappaB in activated rat hepatic stellate cells by proteasome inhibitors and an IkappaB super-repressor. Hepatology 27:1285–1295
Schnabl B, Kweon YO, Frederick JP, Wang XF, Rippe RA, Brenner DA (2001) The role of Smad3 in mediating mouse hepatic stellate cell activation. Hepatology 34:89–100
Yanagisawa M, Takizawa T, Ochiai W, Uemura A, Nakashima K, Taga T (2001) Fate alteration of neuroepithelial cells from neurogenesis to astrocytogenesis by bone morphogenetic proteins. Neurosci Res 41:391–396
Wordinger RJ, Agarwal R, Talati M, Fuller J, Lambert W, Clark AF (2002) Expression of bone morphogenetic proteins (BMP), BMP receptors, and BMP associated proteins in human trabecular meshwork and optic nerve head cells and tissues. Mol Vis 8:241–250
Kim IY, Lee DH, Lee DK, Kim BC, Kim HT, Leach FS, Linehan WM, Morton RA, Kim SJ (2003) Decreased expression of bone morphogenetic protein (BMP) receptor type II correlates with insensitivity to BMP-6 in human renal cell carcinoma cells. Clin Cancer Res 9:6046–6051
Vanttinen T, Kuulasmaa T, Liu J, Voutilainen R (2002) Expression of activin/inhibin receptor and binding protein genes and regulation of activin/inhibin peptide secretion in human adrenocortical cells. J Clin Endocrinol Metab 87:4257–4263
Fujii S, Maeda H, Wada N, Kano Y, Akamine A (2006) Establishing and characterizing human periodontal ligament fibroblasts immortalized by SV40T-antigen and hTERT gene transfer. Cell Tissue Res 324:117–125
Borghi R, Vene R, Arena G, Schubert D, Albini A, Tosetti F (2003) Transient modulation of cytoplasmic and nuclear retinoid receptors expression in differentiating human teratocarcinoma NT2 cells. J Neurochem 84:94–104
Rothhammer T, Poser I, Soncin F, Bataille F, Moser M, Bosserhoff AK (2005) Bone morphogenic proteins are overexpressed in malignant melanoma and promote cell invasion and migration. Cancer Res 65:448–456
Schnabl B, Hu K, Muhlbauer M, Hellerbrand C, Stefanovic B, Brenner DA, Scholmerich J (2005) Zinc finger protein 267 is up-regulated during the activation process of human hepatic stellate cells and functions as a negative transcriptional regulator of MMP-10. Biochem Biophys Res Commun 335:87–96
Hu K, Fink M, Froh M, Gabele E, Hellerbrand C, Muhlbauer M, Wiest R, Scholmerich J, Schnabl B (2005) Characterization of the human zinc finger protein 267 promoter: Essential role of nuclear factor Y. Biochim Biophys Acta 1729:14–23
Tacke F, Brabant G, Kruck E, Horn R, Schoffski P, Hecker H, Manns MP, Trautwein C (2003) Ghrelin in chronic liver disease. J Hepatol 38:447–454
Lepreux S, Bioulac-Sage P, Gabbiani G, Sapin V, Housset C, Rosenbaum J, Balabaud C, Desmouliere A (2004) Cellular retinol-binding protein-1 expression in normal and fibrotic/cirrhotic human liver: different patterns of expression in hepatic stellate cells and (myo)fibroblast subpopulations. J Hepatol 40:774–780
Dorai H, Vukicevic S, Sampath TK (2000) Bone morphogenetic protein-7 (osteogenic protein-1) inhibits smooth muscle cell proliferation and stimulates the expression of markers that are characteristic of SMC phenotype in vitro. J Cell Physiol 184:37–45
Zeisberg M, Shah AA, Kalluri R (2005) Bone morphogenic protein-7 induces mesenchymal to epithelial transition in adult renal fibroblasts and facilitates regeneration of injured kidney. J Biol Chem 280:8094–8100
Gould SE, Day M, Jones SS, Dorai H (2002) BMP-7 regulates chemokine, cytokine, and hemodynamic gene expression in proximal tubule cells. Kidney Int 61:51–60
Hruska KA, Guo G, Wozniak M, Martin D, Miller S, Liapis H, Loveday K, Klahr S, Sampath TK, Morrissey J (2000) Osteogenic protein-1 prevents renal fibrogenesis associated with ureteral obstruction. Am J Physiol Renal Physiol 279:F130–143
Vukicevic S, Basic V, Rogic D, Basic N, Shih MS, Shepard A, Jin D, Dattatreyamurty B, Jones W, Dorai H, Ryan S, Griffiths D, Maliakal J, Jelic M, Pastorcic M, Stavljenic A, Sampath TK (1998) Osteogenic protein-1 (bone morphogenetic protein-7) reduces severity of injury after ischemic acute renal failure in rat. J Clin Invest 102:202–214
Morrissey J, Hruska K, Guo G, Wang S, Chen Q, Klahr S (2002) Bone morphogenetic protein-7 improves renal fibrosis and accelerates the return of renal function. J Am Soc Nephrol 13:S14–21
Zeisberg M, Hanai J, Sugimoto H, Mammoto T, Charytan D, Strutz F, Kalluri R (2003) BMP-7 counteracts TGF-beta1-induced epithelial-to-mesenchymal transition and reverses chronic renal injury. Nat Med 9:964–968
Lin J, Patel SR, Cheng X, Cho EA, Levitan I, Ullenbruch M, Phan SH, Park JM, Dressler GR (2005) Kielin/chordin-like protein, a novel enhancer of BMP signaling, attenuates renal fibrotic disease. Nat Med 11:387–393
Flechtenmacher J, Huch K, Thonar EJ, Mollenhauer JA, Davies SR, Schmid TM, Puhl W, Sampath TK, Aydelotte MB, Kuettner KE (1996) Recombinant human osteogenic protein 1 is a potent stimulator of the synthesis of cartilage proteoglycans and collagens by human articular chondrocytes. Arthritis Rheum 39:1896–1904
Nishida Y, Knudson CB, Eger W, Kuettner KE, Knudson W (2000) Osteogenic protein 1 stimulates cells-associated matrix assembly by normal human articular chondrocytes: up-regulation of hyaluronan synthase, CD44, and aggrecan. Arthritis Rheum 43:206–214
Soder S, Hakimiyan A, Rueger DC, Kuettner KE, Aigner T, Chubinskaya S (2005) Antisense inhibition of osteogenic protein 1 disturbs human articular cartilage integrity. Arthritis Rheum 52:468–478
Maliakal JC, Asahina I, Hauschka PV, Sampath TK (1994) Osteogenic protein-1 (BMP-7) inhibits cell proliferation and stimulates the expression of markers characteristic of osteoblast phenotype in rat osteosarcoma (17/2.8) cells. Growth Factors 11:227–234
Tsai AD, Yeh LC, Lee JC (2003) Effects of osteogenic protein-1 (OP-1, BMP-7) on gene expression in cultured medial collateral ligament cells. J Cell Biochem 90:777–791
Ebara S, Nakayama K (2002) Mechanism for the action of bone morphogenetic proteins and regulation of their activity. Spine 27:S10–15
Acknowledgments
We thank Dr R. T. Franschesi from University of Michigan, Ann Arbor, for providing AdBMP7. We thank Marina Fink and Dr Kanghong Hu for excellent technical assistance. This study was supported in part by grants from Deutsche Forschungsgemeinschaft Ta 434/1–1 (to F.T.), Schn 620/3–1 and Schn 620/3–2 (to B.S.), and Regensburger Forschungsförderung (to B.S.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tacke, F., Gäbele, E., Bataille, F. et al. Bone Morphogenetic Protein 7 is Elevated in Patients with Chronic Liver Disease and Exerts Fibrogenic Effects on Human Hepatic Stellate Cells. Dig Dis Sci 52, 3404–3415 (2007). https://doi.org/10.1007/s10620-007-9758-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-007-9758-8