Abstract
Brazil has a concentrated HIV epidemic among key populations. In 2009, the Ministry of Health conducted a survey in 10 Brazilian cities aiming to estimate HIV prevalence, knowledge, and associated risk behaviors of polysubstance users (PSU). Using Respondent Driven Sampling (RDS), 3449 PSU were recruited, answered an Audio-Computer Self Assisted Interview (ACASI) and were tested for HIV and syphilis. Analyses were weighted by individual’s social network size generated on RDSAT. Pooled HIV prevalence was 5.8% but varied across cities. Most PSU were male, non-white, without income, unemployed, with low levels of education. Overall, 12.0% used injectable drugs, 48.7% had sex with occasional partners and 46.4% engaged in commercial sex. A majority received free condoms (71.4%) but 76.7% exhibited inconsistent condom use. Findings can support policies aiming to improve health care and preventive interventions tailored to this population that remains at high risk of acquiring and transmitting HIV/STI in multiple scenarios.
Resumen
Brasil tiene una epidemia concentrada de VIH en las poblaciones clave. En 2009, el Ministerio de Salud realizó una encuesta en 10 ciudades brasileñas con el objetivo de estimar la prevalencia del VIH y outros indicadores entre los consumidores de múltiples drogas (CMD). Em la muestra Respondent-driven-sampling (RDS), 3,449 CMD contestaron una entrevista auto-asistida con Audio-Computer (A-CASI) y hicieron pruebas del VIH y sífilis. Las estimativas fueron ponderadas – pesos RDS. La prevalência conjunta del VIH (5,8%) varió entre las ciudades. La mayoría eran hombres, no blancos, sin ingresos, desempleados, con bajos niveles de educación. Utilizó fármacos inyectables (12,0%), 48,7% tuvo relaciones sexuales con parejas ocasionales y 46,4% practicó sexo comercial. 71,4% recibió condones gratuitos pero 76,7% con uso inconsistente. Esos hallazgos pueden apoyar políticas destinadas a mejorar la atención y intervenciones preventivas adaptadas a los CMD que continúan en alto riesgo de adquirir y transmitir VIH/ITS en múltiples escenarios.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In 2012 it was estimated that 5.2% (95% CI 3.5–7.0%) of the adult world’s population aged 15–64 had used, at least once in the previous year, cannabis, opioids, cocaine or amphetamine-type stimulants [1]. Illicit drug use is considered a major social and public health problem [2, 3] and it is associated with transmission of blood-borne pathogens, particularly the human immunodeficiency virus (HIV), via shared contaminated syringes and needles (as well as several other materials, containers and liquids, such as vessels from which different users refill their syringes, cotton, filters etc.) and/or unprotected sex.
Among 12.7 million people (0.27%) who use drugs worldwide, it is estimated that an average of 13% are living with HIV and injection drug users have been associated with 30% of new infections outside of Sub-Saharan Africa in recent years [1]. However, non-injecting drugs are also relevant to the dissemination of HIV and other sexually transmitted infections (STI) in different settings, especially through the use of stimulants which may be associated with higher rates of unprotected sex [4], as well as the putative role of shared straws and other paraphernalia used by people who snort powder cocaine in the transmission of both HIV and Hepatitis C virus (HCV) [5].
The number of new HIV infections has been falling globally, whereas in Brazil, where 2% of the world’s and 47% of Latin America’s people living with HIV are located, an increase of 11% in the number of new HIV infections was recorded from 2005 to 2013 [6]. The number of HIV infections among non-injection drug users (non-IDUs) is high in Brazil [7] despite their decrease among IDUs. In both low/middle-income and high income countries, non-IDUs are receiving more attention and have been more frequently targeted by dedicated programs because data and researchers are suggesting that HIV prevalence in this population may be as high as among injection drug users in some contexts [8, 9].
A recent e-report [7] and several papers highlighted that the most frequently used illicit drugs in Brazil are cannabis, cocaine powder, crack-cocaine and related substances [10, 11]. Despite the low rate of drug injection in Brazil compared with rates of injection in USA and European countries [2], the country has reported a high prevalence of HIV among key populations, such as crack-cocaine users whose HIV prevalence was estimated to be eight times higher than that of the general population [7]. Although Brazil has strong HIV prevention and treatment programs, in some way hindered in the last years by the ongoing fiscal crisis [12], drug users have heterogeneous and complex patterns of drug use and may require different targeted interventions, tailored to specific subgroups of different substances, such as ethnic and sexual minorities, women, minors, users of stimulants versus opiates [13].
Thus, behavioral surveillance surveys among drug user populations which are at increased risk of acquisition and/or transmission of STI are fundamental to curb STI spread among these populations, their families, partners and their communities at large. As such, the present paper estimated HIV prevalence, proportions of knowledge on HIV, risky attitudes and practices among polysubstance users (PSU) for each of the 10 Brazilian cities.
Methods
Study Design, Population, and Inclusion Criteria
A cross-sectional survey using Respondent Driven Sampling method (RDS) [14] was conducted with the key objectives of the main study were to assess sexual behaviors, attitudes, practices and HIV and syphilis prevalence among PSU, and to outline data for comparison with past and future surveillance surveys data.
Respondent driven sampling, a chain link sampling method that begins with a convenience sample of members of the target population called ‘seeds’ [14], was used [15] because other sampling methods not designed to assess hard-to-reach populations tend to be affected by three major caveats: (1) the absence of a priori sampling frame that could anchor classic sampling strategies; (b) the invisibility of some subgroups/hidden scenes, such as users of unrecorded alcohol, as previously demonstrated by a former study of our group [16]; (c) and last but not least the strong suspicion the targeted population maintains about interviewers, even those used to work as outreach workers, in case they belong to other communities/areas under the influence of specific criminal factions, which is especially relevant in a context of pervasive violence and mistrust [17].
A sample size was set at 2850 PSU by the Brazilian National Department of Surveillance, Prevention and Control of STIs, HIV/AIDS and Viral Hepatitis (DIAHV), distributed in 10 Brazilian cities, namely: Belo Horizonte, Brasília, Campo Grande, Curitiba, Itajaí, Manaus, Santos, Salvador, Recife, and Rio de Janeiro (Fig. 1).
The targeted population was PSU residing in one of the ten cities and inclusion criteria were as follows: people ≥18 years old in 2009, who had ever reported injecting substances including cocaine, crack, amphetamine, heroin or hallucinogens at least once in the past 6 months, and/or who had reported using any other non-injecting illicit substances for at least 25 times in the 6 months preceding the survey. These criteria were defined after Pan American Health Organization’s (PAHO’s) CODAR (“Consumidores de Drogas con Alto Riesgo or High Risk Drug Users” [Spanish original and respective English versions]) manual and related materials [18].
The study protocol was approved by the Ethical Council of the Sergio Arouca National School of Public Health (CEP/ENSP nº. 90/2008).
Recruitment and Data Collection
At project’s inception, a preliminary formative research was carried out comprising focus group discussion with members of the targeted population and in-depth interviews. Interviewees were probed in terms of their interest in participation, their social connections, and potential study sites, considering accessibility and interviewees’ privacy.
Considering the formative results, study sites in each city was defined and at least three seeds, diverse in age, sex, drug use type, and socioeconomic characteristics, were intentionally selected to start recruitment. Each seed received three coupons to be handled to potential participants who in turn recruited new putative participants.
Once launched the recruitment process, a peer-recruited participant who reached the study site, a public health center located in each city, with a uniquely coded valid coupon connected to the recruiter’s coupon in the coupon manager software and who were not under the acute influence of drugs was screened for eligibility. Coded coupons, coupon manager software, as well as individual characteristics were used to minimize duplications.
After free and informed consenting, eligible participants were invited to answer the main interview based on validated questionnaire delivered as an Audio Computer-Assisted Self Interview (ACASI), which has been used with very high acceptability and good performance among this population in the Brazilian context [19]. The questionnaire included questions on socio-demographic factors, lifetime and current (past 12 months and 30 past days, respectively) drug use and sexual behavior, healthcare services usage, and knowledge of STIs.
After completing research procedures and the main interview, eligible participants received a participation incentive of R$(Brazilian Real) 40.00 (~US$20.00 in 2009) as well as three coupons to invite their peers. Then, a recruitment incentive of R$40.00 was given for each of their three recruitees who reached the study site and participated in the survey.
Field workers were previously trained on RDS, on data collection, and on guiding peers on recruitment strategies. All participants signed a free and informed consent form in order to participate and received pretest and post-test counseling for STI. Blood specimens were drawn for voluntary finger stick rapid tests: rapid plasma reaction (RPR) Bioline Syphilis™ and Rapid Check HIV 1/2 and Bio-Manguinhos HIV 1/2, following the national algorithm established by the Brazilian Ministry of Health [20, 21]. We referred to specialized care those who tested positive for one of the rapid tests.
Measures
Participants’ personal social network size were assessed through the question as follows: “Among the drug users you know by name and have encountered in the last month, how many of them would you invite to participate in this study?”. Recruiter-recruitee relationship was further explored by asking: “What is your relationship with the person who referred you to this study, i.e., with the person who gave you the coupon?”.
The frequency of condom use in the last 12 months before the interview was categorized as ‘Never’, ‘Rarely/Sometimes’—both classified as “Inconsistent use”—and ‘Always’ classified as “Consistent use”. Other variables were: age (taking mean as the cut point), gender, race/skin color, income, a minimum wage in 2009 (taking R$(Brazilian Real) 400 (~USD $210) as cutting point), condom use at first sexual intercourse, self-perceived risk of HIV infection, engaging in commercial sex (sex in exchange of money or drugs), number of commercial sexual partners, marital status, years of education, income, access to condoms, to have received counselling and educational materials on preventing STIs in the last 12 months.
Data Analysis
In this paper, we present descriptive statistics on HIV prevalence, proportions of knowledge on HIV, risky attitudes and practices among PSU for each of the 10 Brazilian cities, with a 95% confidence interval. Pooled and study site estimates were weighted by the inverse of the individual’s probability selection considering the individual’s social network size reported by each respondent (degree) and the measure of “homophily” (degree of similarity between recruiter and recruitee in relation to HIV and syphilis infection).
For adjusting the parameter’s estimation procedure in order to adjust for recruitment biases [14], individual RDS sampling weights were calculated with the RDS Analysis Tool (RDSAT 7.1; available at www.respondentdrivensampling.org). Individuals weights were then exported to Stata 10.0 [22] to proceed the statistical analysis. This analysis included seeds and subsequent recruitees data.
Although adjusted findings do no longer correspond to actual interviewees since they do refer to weighted estimates, we kept the original term “interviewees”/”respondents” for the sake of conciseness and to help the potential readers (most of them not sampling statisticians) to better understand findings.
Results
Study Population and Recruitment Characteristics
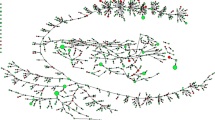
Data collection occurred between March and November 2009 in all study sites. Recruitment duration varied greatly from six weeks in Santos to 28 weeks in Rio de Janeiro, and recruitment waves varied from seven in Santos to 16 in Brasília. At least three seeds were included to start recruitment in each study site. In total, 60 seeds started the recruitment in whole cities, while varied between three seeds in Itajaí and nine seeds in Campo Grande and Salvador. For this survey, a total of 3784 PSU was achieved in the ten cities under study, fluctuating between 679 in Rio de Janeiro and 218 in Campo Grande. 3449 participants were eligible and included in the study and analysis, while pretended sample was 2850 participants (Table 1). After excluding cases with missing information in key variables, the following analysis consider a sample size of 3449 PSU. Patterns of recruitment in each city are presented in Fig. 2.
Sociodemographic and Behavioral Characteristics
A summary of proportions weighted baseline characteristics of PSU in each city is presented in Table 2. The mean age was 30.6 years old (range 18–73), and varied from 18 to 56 years old in Curitiba and from 18 to 73 years old in Brasília (data not presented); and 56.2% were 30 or more years old. Most of the overall sample (73.7%) consisted of males, varying from 53.6% in Manaus to 90.8% in Campo Grande, and 78.0% identified themselves as non-white, ranging from 34.3% in Itajaí to 90.7% in Salvador.
The majority of all participants was non-single or was living with partner (66.8%), ranging from 50.2% in Itajaí to 76.7% in Manaus. More than 1/3 (40.3%) of the participants had a monthly income over R$(Brazilian Real) 400.00 (~US$ 210 in 2009), and 36.3% had no income. In total, unemployment among PSU was quite high (48.9%), varying from 35.7% in Campo Grande to 56.3% in Rio de Janeiro. A low level of education (less than ten years of formal education) was reported by 71.0% of the pooled interviewees, ranging from 54.6% in Manaus to 83.9% in Santos, while 21.4% reported no formal education, 11.3% in Campo Grande and 41.7% in Manaus. Just one quarter of participants (26.6%) stated that their sexual debut took place with condom use, 14.0% in Santos and 33.9% in Manaus.
HIV Prevalence by Study Site, Sex and Injection Status
HIV prevalence varied substantially in the 10 cities. Table 3 presents estimates of HIV prevalence according to sex and injection status bay study site. The weighted pooled estimate was 5.8% (95% CI 5.0–6.6%), and ranged from 1.9% (95% CI 0.3–3.5) in Manaus to 11.2% (95% CI 7.6–14.7) in Itajaí. Weighted pooled estimates of HIV by sex were 7.4% (95% CI 5.7–9.1) for females and 5.2% (95% CI 4.3–6.1) for males. The prevalence of HIV by sex varied greatly from 0.7% (95% CI −0.8 to 2.3) among females in Brasília to 18.9% (95% CI −0.4 to 41.9) among females in Santos, and to 18.8% (95% CI 8.7–28.9) among females in Curitiba. For males, the prevalence of HIV varied from 1.4% (95% CI −0.03 to 3.3) among males in Manaus to 12.2% (95% CI −0.2 to 26.5) among males in Itajaí.
Weighted pooled estimates of HIV according to injection status were 8.2% (95% CI 5.5–10.8) for those who injected drugs in the last 12 months before the interviews and 5.5% (95% CI 4.6–6.3) among those who did not inject drugs in the last 12 months before the interviews. Among injectors in the last 12 months before the interviews, HIV prevalence varied greatly from 1.3% (95% CI −0.0 to 4.8) in Brasília to 19.5% (95% CI −1.1 to 49.8) in Campo Grande (Table 3).
Knowledge, Attitudes, and Practices
The pooled rate of injection drugs in the last 12 months before the interview was 12.0% (95% CI 10.9–13.1), varying from 3.1% (95% CI 1.0–5.2) in Recife to 24.6% (95% CI 20.5–28.8) in Belo Horizonte, while specific injection of powder cocaine was 4.9% (95% CI 4.0–5.7) and varied between 0.4% (95% CI −0.01 to 1.6) in Recife and 10.5% (95% CI 6.7–14.2) in Belo Horizonte (Table 4).
Regarding risky behavioral, most respondents (64.1%) reported having ever used alcohol/drugs and in consequence of it did not use condoms during sexual intercourse. Sex with occasional partner in the last 12 months before the interview was reported by 48.7%, varying from 41.6% in Curitiba to 64.9% in Santos, with 65.0% reporting condom use with occasional partners, 54.5% in Curitiba and 77.1% in Salvador. Ever been engaged in commercial sex (giving or receiving money or drugs for sex) was reported by 46.4% of the participants and varied from 34.8% in Brasília to 58.2% in Recife. The number of partners with whom participants were engaged in commercial sex was reported as ‘one’ by 32.3%, ‘2 to 5’ by 38.1%, and ‘6 or more’ by 29.6% of the whole interviewees. The highest (89.9%) and lowest (13.3%) proportions of engagement in commercial sex with ‘6 or more’ partners were reported in Santos and Manaus, respectively. Engagement in sexual violence (as victim or perpetrator) was reported by 22.7% of hole sample, and was found to be highest (28.8%) in Rio de Janeiro and lowest (14.2%) in Santos.
The frequency of condom use in the last 12 months before the interviews was reported as ‘rarely/sometimes’ by 56.0% and as ‘never’ by 20.7% of participants. Highest and lowest rates of consistent condom use (‘always’) were reported in Itajaí (34.0%) and Rio de Janeiro (18.8%), respectively; with an overall rate of 23.3%, as is presented in Table 4.
Around two-fifths (45.1%) reported receiving educational materials on STI in the last 12 months before the interview, with the highest frequency observed in Itajaí (54.0%) and the lowest in Brasília (37.1%). Nearly half (48.7%) reported receiving counseling on STI in the same period, many in Curitiba (59.6%) and few in Recife (40.5%). Furthermore, participants who received free condoms was 71.4%, with highest rates reported in Salvador (90.3%), followed by Santos (89.6%), and lowest in Rio de Janeiro (60.5%).
Table 4 shows that around half (44.3%) of the interviewees had not been previously tested for HIV in lifetime. Previous HIV testing was lowest (33.1%) in Campo Grande, followed by Manaus (36.1%) and Recife (37.0%), whereas the highest proportion (64.5%) was reported in Santos.
Regarding self-perception of HIV risk acquisition, roughly half of the whole sample (50.8%) considered their risk of becoming infected with HIV as ‘none/low’ (42.3% in Campo Grande and 65.8% in Salvador), while 39.3% did not answer or did not know how to classify their own risk, varying from 24.5% in Salvador to 47.1% in Rio de Janeiro. Only 10.0% ranked themselves as in a ‘high-risk situation’ to acquire HIV infection, the lowest rate (9.7%) in Salvador and the highest rate (16.1%) in Belo Horizonte. Meanwhile, the vast majority (92.0%) perceived syringe and needle sharing as putatively associated with HIV transmission (ranging from 84.0% in Brasília to 98.0% in Santos). PSU who have ever been enrolled in treatment programs were 30.9% (pooled estimated point prevalence), ranging from 13.5% in Manaus to 62.7% in Curitiba.
Discussion
This was the first study conducted among people who misuse substances in Brazil using RDS to amass, integrate and define a pool of data from different study sites. Results indicate a high (5.8%; 95% CI 5.0–6.6) prevalence of HIV infection among our sample of PSU compared to the general Brazilian population (0.6%) [23]. Despite diverse recruitment methodologies, drug using patterns and large differences in socioeconomic characteristics between and within countries, the literature, notwithstanding, highlights key similarities characterizing the drug use phenomenon across countries worldwide. Studies conducted in the Americas, Eastern Europe, and African and Asian countries, found rates of HIV among PSU (of both injectable and non-injectable substances) similar to ours and some of them even higher than our estimates [8, 24–29].
Although differential HIV risk acquisition rates between injecting and non-injectable are not fully understood [30], HIV infection rates as high as 10.9 and 42.0% were reported among injecting drug users in Yerevan, Armenia [24] and Dar es Salaam, Tanzania [31], respectively, countries where rates of injection are low, as have been observed in recent years in Brazil. On the other hand, HIV infection rates ranged from 3.0 to 69.0% in a pool of eight Russian cities [32], where injection rates are very high compared to Brazil.
A high proportion of engagement in occasional sex was found in this study, with 65.0% (95% CI 62.3–67.6) of the interviewees reporting condom use at their last sexual encounter prior to the interview. The proportion is similar to 40.0% found among injecting drug users in Yerevan, Armenia [24] and to 36.2% among frequent drug users in a study summarizing data from Chinese HIV sentinel surveillance sites [33]. In India, a country with high rates of injection and HIV [34], compared to Brazil, in the states of Nagaland and Manipur 60.0 and 72.0% of drug users, respectively, reported to have had unprotected sex with occasional paid/unpaid partners in the last 12 months before the interview [35]. Most (77.0%) interviewees from our sample reported inconsistent condom use, which is the most important risk factor for HIV acquisition and transmission in the Brazilian scenario, even considering the pronounced heterogeneity of general characteristics and the overall low rates of injection in the ten study sites. Despite diverse recruitment methodologies and drug using patterns, similar rates of inconsistent condom use among PSU were reported by all studies conducted in Brazil and several other middle-income countries, such as Colombia, India, and Iran [31, 35–39].
Many participants reported sex with multiple sexual partners. High frequencies of multiple sexual intercourse and engagement in commercial sex have been reported in the most different settings, worldwide, such as in surveys targeting injecting and non-injecting drug users in China [33, 39] and in Lebanon [40].
Findings documenting low condom use and a sizeable proportion of respondents who perceive themselves at none/low risk of HIV infection may increase the risk of acquiring and eventually transmitting HIV, in case self-perception of risks translates into a diminished perception of other people’s risk. Fortunately, as repeatedly shown by the literature, a high proportion of our sample answered correctly that sharing syringes/needles can transmit HIV [41]. Surveys worldwide have reported high rates of drug users with a sound knowledge on HIV transmission ways [27, 42, 43], but it is of great importance to note that a sound knowledge about most risks of acquiring and transmitting HIV may not be comprehensive or coherent [41], and might not be translated into the consistent adoption of safer practices [6].
A small proportion of PSU reported to have been attended treatment programs. Notably, according to UNAIDS only one in six drug users access drug treatment services each year and, on average, each drug user access 90 needles per year, whereas the actual demand was estimated at 200 per year per drug user [6]. The proportion of PSU who have ever been tested for HIV in our study may be defined as a mid-range proportion according to UNAIDS criteria. Although our data are not perfectly comparable to other countries’ published data due to differences in the drug user population’s characteristics (especially the type of substances most frequently consumed), as well as biases associated with each specific method and respective procedures, international surveys have highlighted both similar and different results. For example, higher rates as 75.7 and 97.4% of drug users have been ever documented for HIV in San Francisco [44] and in methadone clinics located in Southern China [45], respectively. On the other hand, much lower rates have been reported in several countries of Sub-Saharan Africa where different cultural characteristics, less than optimal access, as well as long-distances and high transportation costs (especially relevant in cities located far from major urban centers) have compromised testing strategies in real world conditions [46].
Almost half of the sample reported to have received counseling and educational materials on STI, with the majority stating they have received free condoms. In a study conducted in New York City [47], the proportion of people who received counseling was 13.0%, whereas the proportion who received free condoms was 62.9%. The number of commercial sex partners in our sample was similar to that found in Sidney, Australia [48], and it is known that to have unprotected sexual intercourse with many commercial sexual partners could increase the risk of HIV acquisition.
In general, our findings suggest that female (7.4%, 95% CI 5.7–9.1) PSU have higher overall HIV prevalence than their male (5.2%, 95% CI 4.3–6.1) counterparts, instead of local variations. A recent pooled prevalence analysis issued by the UNAIDS estimated as 13% and at 9% the point prevalence of HIV for women and for men drug users worldwide, respectively [6]. Additional literature on HIV differential infection rates between male and female who inject drugs strengthens our findings that female PSU tend to have higher HIV prevalence than males [9], as was observed in this study in Belo Horizonte, Curitiba, Recife and Santos. Yet, HIV prevalence was higher among female drug users than among their male counterparts in Tijuana, Mexico [49]. Notably, we should emphasize that female PSU seem to be at higher risk of HIV infection in the ten study sites through a combination of overlapping risks: high levels of unprotected sexual intercourse, partner/gender based violence, and more frequent unsafe injection habits, as reported in several studies [43, 50–53].
The relatively high HIV prevalence (vis-à-vis much lower infection rates among Brazil´s general population) made evident in this study seem to be secondary to a combination of repeated risky interactions within social networks with high background prevalences [54], as well as in consequence of less than optimal preventive campaigns, which have been fell short of reaching key populations with the necessary broadness and comprehensiveness, as has been suggested by researchers in Mexico [55]. Such specific risk factors tend to be aggravated by structural problems secondary to interpersonal violence, scarcity of health and social facilities, as well as dire poverty with the consequent lack of basic resources, such as free condoms and sterile syringes as well as food insecurity [56].
Study Limitations
Although our findings highlighted some important points regarding HIV infection rates and attitudes, practices and knowledge related to HIV among PSU in ten Brazilian cities, certain limitations should be considered here. Since recruiting chains are driven by the respondents themselves, they are prone to selection bias because recruiters are more likely to recruit peers with characteristics similar to their own, with consequent overrepresentation of such specific segments and specific branches of broader social networks [14]. Cross-sectional studies are also influenced by recall bias, i.e., participants might not remember certain aspects of the past and/or might select some information, which is, consciously or unconsciously, associated with other relevant events, taking place over a whole lifetime. Questions regarding both past 12 months and 30 past days were used to minimize recall bias. Yet, findings may be affected as well by social desirability bias, thus favoring under-report of socially unacceptable behaviors. Last but not least, cross-sectional studies are invariably plagued by the difficulty or impossibility to discern the directionality of observed associations.
Finally, we should mention Brazil is a particularly vast, densely populated and heterogeneous country. In this sense, any study sampling data from 10 municipalities in a universe of over 5500 municipalities spread over a continental-size country should be not viewed as representing the country as such.
Moving from the macro to the micro level, one must keep in mind that pooled estimates of individual networks, tend to mix-up the underlying structure of each local network. Since putative biases are strongly context-dependent, no algorithmic procedure can fix such inaccuracies. Nonetheless, RDS may produce quasi-probabilistic estimates according to its basic assumptions of reaching (after a given number of waves) a situation of actual equilibrium of local networks as the chain-referral process progress over time and across the chain of successive referrals [14]. Importantly, we pooled ten independent networks in order to obtain a large sample as opposed to much smaller [57] single networks, generating a more suitable data for the purpose of surveillance among PSU and multivariable analyses that may be precluded by lack of statistical power. To conclude, other sampling methods not designed to assess hard-to-reach populations might generate biased samples as well, although the magnitude and directionality of these biases are far from straightforward, as demonstrated by cross-comparisons between multimethod studies using RDS and Time-Location Sampling (TLS) [44, 58, 59].
Conclusion
The prevalence of HIV varied across the study site, but remains, notwithstanding, substantially higher than rates observed in the general population. These findings should inform policies and targeted interventions to improve health care and preventive interventions among PSU. The most needed HIV prevention calls for structural interventions that can help to alleviate health inequity and insure the protection (and ideally the promotion of) human rights.
These findings are critical in light of a considerably high level of free condom distribution, as reported by the interviewees of our study. Our results suggest that several obstacles for HIV prevention remain and messages disseminated by mass campaigns are not successfully reaching especially vulnerable groups and/or have not been tailored to them. It is urgent to redesign campaigns strategies, to integrate them with targeted interventions, taking in consideration that sound knowledge of HIV prevention and access to broad campaigns do not necessarily translate into concrete behavioral change and prevention practices. Future studies using RDS must go beyond addressing relationships between HIV infection and risk factors by examining the broader social context where people are inserted and interact with each other.
References
UNODC. World drug report 2014. Trends in Organized Crime. 2014.
Strathdee SA, Stockman JK. Epidemiology of HIV among injecting and non-injecting drug users: current trends and implications for interventions. Curr HIV/AIDS Rep [Internet]. 2010 May [cited 2013 Jun 16];7(2):99–106. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=2856849&tool=pmcentrez&rendertype=abstract.
Mathers BM, Degenhardt L, Phillips B, Wiessing L, Hickman M, Strathdee SA, et al. Global epidemiology of injecting drug use and HIV among people who inject drugs: a systematic review. Lancet [Internet]. 2008 Nov 15 [cited 2013 Jun 17];372(9651):1733–45. http://www.ncbi.nlm.nih.gov/pubmed/18817968.
Shoptaw S, Montgomery B, Williams CT, El-Bassel N, Aramrattana A, Metzger DS, et al. Not just the needle: the state of HIV prevention science among substance users and future directions. J Adquir Immune Defic Syndr. 2013;63(02):174–8.
Vanhommerig JW, Lambers FAE, Schinkel J, Geskus RB, Arends JE, Laar TJW van de, et al. Risk factors for sexual transmission of Hepatitis C virus among Human Immunodeficiency Virus-infectect men who have sex with men: a case-control study. Ofid [Internet]. 2015;1–8. http://ofid.oxfordjournals.org/content/early/2014/06/01/ofid.ofu038.short.
UNAIDS. Global Report: UNAIDS report on the global AIDS epidemic 2013 [Internet]. Geneva; 2013. www.unaids.org/
Brazil. Pesquisa Nacional sobre o uso de crack: quem são os usuários de crack e/ou similares do Brasil? quantos são nas capitais brasileiras? Rio de Janeiro; 2014.
Des Jarlais DC, Arasteh K, McKnight C, Perlman D, Hagan H, Semaan S, et al. Gender and age patterns in HSV-2 and HIV infection among non-injecting drug users in New York City. Sex Transm Dis [Internet]. 2010 Oct [cited 2014 May 16];37(10):637–43. http://www.ncbi.nlm.nih.gov/pubmed/20838366.
Strathdee SA, Sherman SG. The role of sexual transmission of HIV infection among injection and non-injection drug users. J Urban Heal [Internet]. 2003 Dec;80(4 Suppl 3):iii7–14. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3456264&tool=pmcentrez&rendertype=abstract.
Cruz M, Bertoni N, Bastos FI, Burnett C, Gooch J, Fischer B. Comparing key characteristics of young adult crack users in and out-of-treatment in Rio de Janeiro, Brazil. Subst Abuse Treat Prev Policy [Internet]. 2014;9:2. http://apps.webofknowledge.com/full_record.do?product=UA&search_mode=GeneralSearch&qid=10&SID=Y2tYF7FqXM3a3DQf7B3&page=1&doc=4&cacheurlFromRightClick=no.
Santos Cruz M, Andrade T, Bastos FI, Leal E, Bertoni N, Villar LM, et al. Key drug use, health and socio-economic characteristics of young crack users in two Brazilian cities. Int J Drug Policy. 2013;24(5):432–8. doi:10.1016/j.drugpo.2013.03.012.
Krawczyk N, Kerrigan D, Bastos F. The quest to extend health services to vulnerable substance users in Rio de Janeiro, Brazil in the context of an unfolding economic crisis. Int J Heal Serv. 2017;. doi:10.1177/0020731416679351.
Reback CJ, Fletcher JB, Shoptaw S, Grella CE. Methamphetamine and other substance use trends among street-recruited men who have sex with men, from 2008 to 2011. Drug Alcohol Depend. 2013;133(1):262–5.
Heckathorn D. Respondent-driven sampling: a new approach to the study of hidden populations. Soc Probl. 1997;44(2):174–99.
Malekinejad M, Johnston LG, Kendall C, Kerr LRFS, Rifkin MR, Rutherford GW. Using respondent-driven sampling methodology for HIV biological and behavioral surveillance in international settings: a systematic review. AIDS Behav. 2008;12:105–30.
De Boni RB, Bertoni N, Bastos LS, Bastos FI. Unrecorded alcohol in Rio de Janeiro: assessing its misusers through respondent driven sampling. Drug Alcohol Depend. 2014;139:169–73.
Bastos FI. Structural violence in the context of drug policy and initiatives aiming to reduce drug-related harm in contemporary Brazil: a review. Subst Use Misuse [Internet]. 2012;47(13-14):1615–6. http://www.tandfonline.com/doi/full/10.3109/10826084.2012.726546.
Pan American Health Organization. Encuestas de Comportamiento en Consumidores de Drogas con Alto Riesgo (CODAR). Herramientas básicas para vigilancia de segunda generación de la transmisión de VIH y otras ITSS en CODAR. [Spanish] http://www.portalsida.org/repos/Codar_cuadern. Washington, DC; 2004.
Simoes AA, Bastos FI, Moreira RI, Lynch KG, Metzger DS. Acceptability of audio computer-assisted self-interview (ACASI) among substance abusers seeking treatment in Rio de Janeiro, Brazil. Drug Alcohol Depend. 2006;82(1):S103–7.
Brazil. Portaria 34 de julho de 2005. Regulamenta o uso de testes rápidos para disgnóstico da infeção pelo HIV em situações especiais. [Internet]. Brasília: Ministy of Health; 2005. http://bvsms.saude.gov.br/bvs/saudelegis/svs/2005/prt0034_28_07_2005.html.
Brazil. Portaria 3.242 de 30 de dezembro de 2011. Dispõe sobre o Fluxograma Laboratorial da Sífilis e a utilização de testes rápidos para triagem da sífilis em situações especiais e apresenta outras recomendações. [Internet]. Brasília; 2011. http://bvsms.saude.gov.br/bvs/saudelegis/gm/2011/prt3242_30_12_2011.html.
StataCorp. Stata Statistical Software. Release 10. College Station, TX: StataCorp LP; 2007.
Brazil. Boletim Epidemiológico: HIV/AIDS. Brasília; 2013.
Johnston L, Grigoryan S, Papoyan A, Grigoryan T, Balayan T, Zohrabyan L. High HIV and HCV and the unmet needs of people who inject drugs in Yerevan, Armenia. Int J Drug Policy [Internet]. 2014 Feb 15 [cited 2014 May 9];25:10–3. http://www.ncbi.nlm.nih.gov/pubmed/24612640.
Li L, Assanangkornchai S, Duo L, McNeil E, Li J. Cross-border activities and association with current methamphetamine use among Chinese injection drug users (IDUs) in a China–Myanmar border region. Drug Alcohol Depend [Internet]. 2014 May 1 [cited 2014 May 9];138:48–53. http://www.ncbi.nlm.nih.gov/pubmed/24629780.
Sypsa V, Paraskevis D, Malliori M, Nikolopoulos GK, Panopoulos A, Kantzanou M, et al. Homelessness and other risk factors for HIV infection in the current outbreak among injection drug users in Athens, Greece. Am J Public Health [Internet]. 2014 Feb 13 [cited 2014 May 9];10–3. http://www.ncbi.nlm.nih.gov/pubmed/24524508.
Kori N, Roth AM, Lozada R, Vera A, Brouwer KC. Correlates of injecting in an HIV incidence hotspot among substance users in Tijuana, Mexico. Int J Drug Policy [Internet]. Elsevier B.V.; 2014 Dec 17 [cited 2014 May 9]; 25:525–32. http://www.ncbi.nlm.nih.gov/pubmed/24418632.
Wagner KD, Pollini RA, Patterson TL, Lozada R, Ojeda VD, Brouwer KC, et al. Cross-border drug injection relationships among injection drug users in Tijuana. Mexico. Drug Alcohol Depend. 2013;113(2–3):236–41.
Jolley E, Rhodes T, Platt L, Hope V, Latypov A, Donoghoe M, et al. HIV among people who inject drugs in Central and Eastern Europe and Central Asia: a systematic review with implications for policy. BMJ Open [Internet]. 2012 Jan [cited 2013 May 30];2(5):e001465. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3488708&tool=pmcentrez&rendertype=abstract.
Tavitian-Exley I, Vickerman P, Bastos Francisco I, Boily M-C. Influence of different drugs on HIV risk in people who inject: systematic review and meta-analysis. Addiction [Internet]. 2015;110(4):572–84. http://search.ebscohost.com/login.aspx?direct=true&AuthType=ip,shib&db=jlh&AN=2012933270&site=ehost-live&scope=site.
Williams ML, McCurdy SA, Bowen AM, Kilonzo GP, Atkinson JS, Ross MW, et al. HIV seroprevalence in a sample of Tanzanian intravenous drug users. AIDS Educ Prev. 2009;21(5):474–83.
Eritsyan K, Heimer R, Barbour R, Odinokova V, White E, Rusakova MM, et al. Individual-level, network-level and city-level factors associated with HIV prevalence among people who inject drugs in eight Russian cities: a cross-sectional study. BMJ Open [Internet]. 2013 Jan [cited 2013 Nov 6];3:e1–11. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3686233&tool=pmcentrez&rendertype=abstract.
Ge L, Cui Y, Wang L, Li D, Guo W, Ding Z, et al. Study on the characteristics of serology and sexual behavior among drug users at the HIV sentinel surveillance sites in 2012. Zhonghua liu xing bing xue za zhi [Internet]. 2014 Feb;35(2):121–3. http://www.ncbi.nlm.nih.gov/pubmed/24739547.
Sarna A, Saraswati LR, Sebastian M, Sharma V, Madan I, Lewis D, et al. High HIV incidence in a cohort of male injection drug users in Delhi, India. Drug Alcohol Depend [Internet]. 2014;139:106–14. http://dx.doi.org/10.1016/j.drugalcdep.2014.03.021.
Mishra RK, Ganju D, Ramesh S, Lalmuanpuii M, Biangtung L, Humtsoe C, et al. HIV risk behaviors of male injecting drug users and associated non-condom use with regular female sexual partners in north-east India. Harm Reduct J [Internet]. Harm Reduction Journal; 2014 Jan [cited 2014 May 13];11(1):5. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3932044&tool=pmcentrez&rendertype=abstract.
Assari S, Yarmohmmadi Vasel M, Tavakoli M, Sehat M, Jafari F, Narenjiha H, et al. Inconsistent condom use among Iranian male drug injectors. Front Psychiatry [Internet]. 2014 Jan [cited 2014 May 13];4(April):1–6. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3983495&tool=pmcentrez&rendertype=abstract.
Bryant-Genevier MM, Martin CE, Terplan M. Reproductive Health needs among drug treatment clients. Obs Gynecol. 2014;123(Suppl):104S.
Berbesí-Fernadéz D, Montoya-Vélez L, Segura-Cardona Á. Uso del condón y conocimientos sobre prevención del VIH entre los inyectadores de drogas de dos ciudades colombianas. Adicciones. 2013;25(4):321–6.
Li J, Liu H, Li J, Luo J, Des Jarlais D, Koram N. Role of sexual transmission of HIV among young non-injection and injection opiate users: a respondent driven sampling study. Sex Transm Dis. 2011;38(12):1161–6.
Mahfoud Z, Afifi R, Ramia S, El Khoury D, Kassak K, El Barbir F, et al. HIV/AIDS among female sex workers, injecting drug users and men who have sex with men in Lebanon: results of the first biobehavioral surveys. AIDS [Internet]. 2010 Jul;24(Suppl 2):S45–54. http://www.ncbi.nlm.nih.gov/pubmed/20610948.
Bertoni N, Singer M, Silva CM, Clair S, Malta M, Bastos FI. Knowledge of AIDS and HIV transmission among drug users in Rio de Janeiro, Brazil. Harm Reduct J [Internet]. BioMed Central Ltd; 2011 Jan [cited 2013 Mar 2];8(1):5. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3049124&tool=pmcentrez&rendertype=abstract.
Neupane SR, Mishra SR. Knowledge about human immunodeficiency virus infection and sexual behavior among drug users: a cross sectional study in Pokhara submetropolitan city, Nepal. Front psychiatry [Internet]. 2014 Jan; 6:1–7. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=3926783&tool=pmcentrez&rendertype=abstract.
Bryant J, Brener L, Hull P, Treloar C. Needle sharing in regular sexual relationships: an examination of serodiscordance, drug using practices, and the gendered character of injecting. Drug Alcohol Depend [Internet]. 2010 Mar 1 [cited 2014 May 8];107(2-3):182–7. http://www.ncbi.nlm.nih.gov/pubmed/19942380.
Malekinejad M, Mcfarland W, Vaudrey J, Raymond HF. Accessing a diverse sample of injection drug users in San Francisco through respondent-driven sampling. Drug Alcohol Depend [Internet]. 2011;118(2-3):83–91. http://dx.doi.org/10.1016/j.drugalcdep.2011.03.002.
Xia Y-H, Chen W, Tucker JD, Wang C, Ling L. HIV and hepatitis C virus test uptake at methadone clinics in Southern China: opportunities for expanding detection of bloodborne infections. BMC Public Health [Internet]. BMC Public Health; 2013;13(899):e66787. http://ovidsp.ovid.com/ovidweb.cgi?T=JS&PAGE=reference&D=medl&NEWS=N&AN=24079351.
Asher AK, Hahn JA, Couture M, Maher K, Page K. People who inject drugs, HIV risk, and HIV testing uptake in Sub-Saharan Africa. J Assoc Nurses AIDS Care. 2013;24(6):e35–44.
Neaigus A, Reilly KH, Jenness SM, Hagan H, Wendel T, Gelpi-Acosta C. Dual HIV risk: receptive syringe sharing and unprotected sex among HIV-negative injection drug users in New York City. AIDS Behav [Internet]. 2013 May 3 [cited 2013 Jul 1];17(7):2501–9. http://www.ncbi.nlm.nih.gov/pubmed/23640654.
Islam MM, Topp L, Conigrave KM, Haber PS, White A, Day CA. Sexually transmitted infections, sexual risk behaviours and perceived barriers to safe sex among drug users. Aust NZ J Public Health [Internet]. 2013 Aug [cited 2014 May 1];37(4):311–5. http://www.ncbi.nlm.nih.gov/pubmed/23895472.
Robertson AM, Vera AY, Gallardo M, Pollini RA, Patterson TL, Case P, et al. Correlates of seeking injection assistance among injection drug users in Tijuana, Mexico. Am J Addict. 2010;19(4):357–63.
Uribe JI, Amador G, Zacarías X, Villarreal L. Percepciones sobre el uso del condón y la sexualidad entre jóvenes. Rev Latinoam Cienc Soc Ninez y Juv. 2012;10(1):481–94.
El-Bassel N, Terlikbaeva A, Pinkham S. HIV and women who use drugs: double neglect, double risk. Lancet. 2010;376:312–3. doi:10.1016/S0140-6736(10)61026-4.
Marshall BDL, Fairbairn N, Li K, Wood E, Kerr T. Physical violence among a prospective cohort of injection drug users: a gender-focused approach. Drug Alcohol Depend [Internet]. 2008 Oct 1 [cited 2014 May 8];97(3):237–46. http://www.pubmedcentral.nih.gov/articlerender.fcgi?artid=2570226&tool=pmcentrez&rendertype=abstract.
Wechsberg WM, Luseno W, Riehman K, Karg R, Browne F, Parry C. Substance use and sexual risk within the context of gender inequality in South Africa. Subst Use Misuse. 2008;43(8–9):1186–201.
Gwadz M, Cleland C, Kutnick A, Leonard NR, Ritchie AS, Lynch L, et al. Factors associated with recent HIV testing among heterosexuals at high risk for HIV infection in New York City. Front Public Health. 2016;. doi:10.3389/fpubh.2016.00076.
Pavía-Ruz N, Góngora-Biachi R, Vera-Gamboa L, Moguel-Rodríguez W, González-Martinez P. Conocimientos, actitudes y percepción de riesgo en referencia al VIH/SIDA en población rural de Yucatán, México. Rev Biomed. 2012;23(2):53–60.
Colasanti J, Stahl N, Farber EW, Rio C, Armstrong WS. An exploratory study to assess individual and structural level barriers associated with poor retention and re-engagement in care among persons living with HIV/AIDS. JAIDS. 2017;74(S2):S113–20.
Goel S, Salganik MJ. Assessing respondent-driven sampling. PNAS. 2010;107(15):6743–7.
Truong HM, Grasso M, Chen Y, Kellogg TA, Robertson T, Curotto A, et al. Balancing theory and practice in respondent-driven sampling: a case study of innovations developed to overcome recruitment challenges. PLoS ONE. 2013;8(8):e70344.
Kendall C, Kerr L, Gondim R, Macena RM, Pontes MK, Johnston LG, et al. An empirical comparison of respondent-driven sampling, time location sampling, and snowball sampling for behavioral surveillance in men who have sex with men, fortaleza, Brazil. AIDS Behav. 2008;12(17):97–104.
Funding
This study was funded by The Brazilian National Department of Sexually Transmitted Diseases/HIV/AIDS and Viral Hepatitis-Ministry of Health.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study protocol was approved by the Ethical Council of the Sergio Arouca National School of Public Health (CEP/ENSP nº. 90/2008).
Informed Consent
Informed consent was obtained from all participants included in the study.
Additional information
The Brazilian Multicity Study Group on Drug Misuse—Adriana Pinho, Evely Marlene Pereira Koller, Waleska Teixeira Caiaffa, Maria Inês Costa Dourado, Tarcísio Andrade, Jessem Douglas Yamall Orellana, Ana Maria de Brito, Naíde Teodósio Valois Santos, Paulo Cesar Duarte Paes, Sandra Leone, Neide Gravato da Silva, Vicença Paula Soares Querrer, Maria Lúcia Tozetto Vettorazzi, and Simone Tetu Moyses.
Rights and permissions
About this article
Cite this article
Baptista, C.J., Dourado, I., de Andrade, T.M. et al. HIV Prevalence, Knowledge, Attitudes, and Practices Among Polydrug Users in Brazil: A Biological Survey Using Respondent Driven Sampling. AIDS Behav 22, 2089–2103 (2018). https://doi.org/10.1007/s10461-017-1812-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10461-017-1812-8