Abstract
Adaptive expertise represents the combination of both efficient problem-solving for clinical encounters with known solutions, as well as the ability to learn and innovate when faced with a novel challenge. Fostering adaptive expertise requires careful approaches to instructional design to emphasize deeper, more effortful learning. These teaching strategies are time-intensive, effortful, and challenging to implement in health professions education curricula. The authors are educators whose missions encompass the medical education continuum, from undergraduate through to organizational learning. Each has grappled with how to promote adaptive expertise development in their context. They describe themes drawn from educational experiences at these various learner levels to illustrate strategies that may be used to cultivate adaptive expertise.
At Vanderbilt University School of Medicine, a restructuring of the medical school curriculum provided multiple opportunities to use specific curricular strategies to foster adaptive expertise development. The advantage for students in terms of future learning had to be rationalized against assessments that are more short-term in nature. In a consortium of emergency medicine residency programs, a diversity of instructional approaches was deployed to foster adaptive expertise within complex clinical learning environments. Here the value of adaptive expertise approaches must be balanced with the efficiency imperative in clinical care. At Mayo Clinic, an existing continuous professional development program was used to orient the entire organization towards an adaptive expertise mindset, with each individual making a contribution to the shift.
The different contexts illustrate both the flexibility of the adaptive expertise conceptualization and the need to customize the educational approach to the developmental stage of the learner. In particular, an important benefit of teaching to adaptive expertise is the opportunity to influence individual professional identity formation to ensure that clinicians of the future value deeper, more effortful learning strategies throughout their careers.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Adaptive expertise is the capacity to apply a wide range of approaches to a problem, not only routinized procedural approaches but also creative innovative ones when the situation calls for it (Kua, 2021; Mylopolous, 2016). Adaptive expertise is especially important as healthcare moves from an acute care model to one where complex chronic conditions predominate (Gonzalo et al., 2017). Recently, the COVID pandemic disrupted routine practices, demanding innovation in almost every theatre of care and serving as a visible demonstration of the value of this skill/approach (Merritt et al., 2022).
However, learning to become an adaptive expert is not easy. The instructional strategies that foster adaptive expertise—e.g. developing deep conceptual understanding, exposure to meaningful variation, an emphasis on productive struggle and discovery, and metacognitive strategizing—are each difficult to incorporate in a standard curriculum and more difficult to assess than a corresponding instructional strategy for routinization (Pusic et al., 2019a). Adaptive expertise also requires a different attitude towards expertise development, one that may not be initially apparent to learners or educators (Mylopoulos and Woods, 2009; Betinol et al., 2022). See Table 1 for definitions of some adaptive expertise terms.
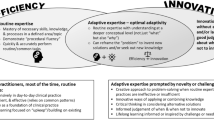
The learning of adaptability. Graphic showing the productive tension underlying adaptive expertise (based on Bransford & Schwartz conceptualization of the Optimal Adaptability Corridor). Activities at an academic healthcare organization, as in the Mayo Clinic example, could fall anywhere in this hypothetical space from investigative research in the top left corner to fully routinized care optimized for efficiency in the bottom right. Learning adaptability requires being placed in situations where both aspects of care are in play and the balance needs to be determined (e.g. the diagonal corridor). In the Vanderbilt University School of Medicine example, clinical case problems are evaluated by students in the simultaneous presence of both a basic science researcher who brings an innovation perspective and a clinician with the experience of real‐world care. In the University of Michigan Emergency Medicine example, an emergency physician is trained in deep conceptual understanding of critical care physiology to ensure that a resource-intensive innovation perspective can complement a routinized efficient one. This benefits the trainee who learns indications for each approach
In systematic reviews, Carbonell (2014; general education) and Kua (2021; HPE) found that the primary literature clearly specifies the core methods for developing adaptive expertise. For example, developing adaptive expertise often requires taking a “desirable difficulties” approach in which more effortful methods (e.g. productive struggle and discovery) are used in preference to labor-efficient ones (e.g. lecture). The former approach promotes a deeper understanding that is better retained over time (Bjork, 2011; Pusic, 2019a). Attention to learners’ mindset (growth vs. fixed), resilience, curiosity, motivation, and conceptual understanding of adaptive expertise can create the conditions where learners are willing to work harder in order to become adaptive experts (Cutrer et al., 2018). These core ideas have been incorporated into over-arching learning frameworks such as the Master Adaptive Learner (Cutrer et al., 2017).
What has yet to emerge, however, is a delineation of how adaptive expertise should be developed in each phase of the medical education training continuum. What describes an adaptive medical student? How do we inculcate conceptual understanding in residents striving for efficiency and routinization of tasks? To what extent should adaptive expertise be the goal of continuing professional development?
Our author team includes experts in the design of curricula that promote adaptive expertise all along the training continuum. Using educational case examples from real-world settings, we describe how instructional strategies must vary based on the level of the learner, our experiences to date, and our lessons learned in promoting adaptive expertise.
Method
We present case examples to illustrate how we promoted adaptive expertise (AE) development in our educational programs. The cases are intentionally chosen to represent the continuum of medical education from undergraduate medical education (medical school) to graduate medical education (residency/specialty training) to a continuing professional development program aimed at an entire healthcare organization. We are leaders and educators in relevant U.S. educational programs. WBC is Associate Dean of Undergraduate Medical Education at Vanderbilt University where he was responsible for implementing an adaptive expertise curriculum for medical students. JB, LH, LR, MG are current or former residency program directors in emergency medicine who each implemented adaptive expertise teaching interventions into their respective residency curricula. HB and EH are professional educators at Mayo Clinic who lead enterprise-wide faculty development programs and education strategic priorities focused on promoting adaptive expertise at the institutional level. MP, a clinician and education researcher, provided content expertise and insights.
We organized this paper based on our expertise with different levels of learners. We first enumerated the key strategies that distinguish learning for adaptive expertise, based on our prior work and key literature. In particular, we agreed that the following four instructional strategies are particularly important for developing adaptive expertise: emphasizing deep conceptual understanding, exposure to meaningful variation, allowing for productive struggle and discovery, and cultivating metacognitive reflection on learning (e.g. Mylopoulos et al., 2016, 2018a, b). Sensitized by this consensus, the three groups then independently wrote descriptions of their interventions and resultant experiences. Using an approach derived from interpretive phenomenological analysis, these case descriptions and the data we collected in our respective programs provide our lived experiences (Neubauer et al., 2019). We then, as a group, compared the sections of the paper written in parallel, discussing how our experiences differed and require approaches customized to the needs of the learner, both within and across learner levels. Through our writing process, we sought to describe how developmental differences might affect how we teach adaptive expertise.
Ultimately, we identified themes that seem to underlie each developmental stage on the continuum, as well as cross-cutting themes (See Fig. 2). In the next sections, we describe each case experience and a theme that characterizes the learning of adaptive expertise at that level. A subsequent section lists cross-cutting themes. We finish by connecting our findings to the relevant research literature.
Case descriptions
Undergraduate medical education – Vanderbilt University School of Medicine
UME Themes – In an undergraduate medical curriculum, structures and learning processes can be engineered to explicitly favor learning of adaptive expertise. However, the labor-intensive learning for adaptive expertise can be seen as a luxury relative to the efficient learning of foundational knowledge that characterizes undergraduate medical education. For example, Preparation for Future Learning and metacognition can be perceived as adding extraneous load during learning.
Vanderbilt University School of Medicine (Vanderbilt) implemented Curriculum 2.0, a responsive, agile, highly-personalized system of lifelong learning designed to prepare medical students to adapt to a rapidly evolving health care system (Cutrer & Brady, 2020). The redesigned curriculum includes a one-year pre-clerkship phase, core clerkships in year two, and an individualized two-year post-clerkship phase. Key components include early clinical exposure, competency-based assessment with portfolio coaching, utilization of a variety of learning modalities, and facilitation of professional identity formation, all utilizing a developmental approach to learner support.
Vanderbilt leaders collaborated in developing the Master Adaptive Learner (MAL) framework with the American Medical Association’s Accelerating Change in Medical Education (ACE) Consortium (Cutrer et al., 2017; Lomis et al., 2021b). The MAL model frames student development as expert learners and guides iterative curricular improvements to Vanderbilt Curriculum 2.0.
Conceptual understanding in an undergraduate medical education program
Leaders reconsidered the approach to pre-clerkship education during the design of Curriculum 2.0. With the goal of improving conceptual understanding, intentional choices were made to de-emphasize (though not eliminate) lectures, structure the typical week around case-based learning, and incorporate team-based learning. Demonstrating the curricular framework proposed by Kulasagarem et al. (2013), implementation addressed program, course, and session level integration of foundational and clinical sciences to foster the meaningful conceptual understanding needed to serve as the basis for development of clinical reasoning. This approach was extended to clerkship and post-clerkship phases.
To foster conceptual understanding in the post-clerkship phase, Integrated Science Courses were created to deepen foundational science knowledge and integrate it with clinical understanding. “The courses contextualize foundational science within disease processes to optimize the transfer of information… and foster the use of prior knowledge to master and create new knowledge and skills, leveraging both horizontal and vertical integration of foundational sciences.” (Dahlman et al., 2018). The strategy moves away from standardized content learning to a standardized process of learning, approaching clinical problems conceptually while remaining grounded within the clinical context. Students are required to complete four of the available 17 Integrated Science Courses during their two-year post-clerkship phase, ensuring broad exposure and learning integration of different foundational sciences.
Productive struggle and discovery in a UME program
Case-based learning promotes adaptive expertise because “learners are presented with a clinical problem and have time to struggle, define and resolve the problem.” (Thistlethwaite et al., 2012). Students explore unknown cases, encountering gaps in their understanding which must be addressed to appropriately diagnose and treat the cases’ patients, returning later in the week to teach each other, addressing these gaps. Students are supported in their struggle and discovery process by a faculty facilitator. These sessions also provide an early opportunity for students to learn how to give and receive feedback via peer assessments (Bird et al., 2017), which creates additional struggle and discovery related to their own learning beliefs and skills.
Meaningful variation in a UME program
Clinical experts typically organize and store clinical information as exemplars or illness scripts (Charlin et al., 2000; Mylopoulos et al., 2018a, b). Meaningful variation can be utilized to allow learners to compare and contrast their nascent exemplars or illness scripts with unique case presentations and progressions (Cutrer et al., 2013; Fleming et al., 2012). At Vanderbilt, students participate in sessions that highlight the strengths and pitfalls of this type of clinical reasoning. They compare and contrast illness scripts to create their differential diagnosis during a patient evaluation and during case-based clerkship conferences. A key element of adaptive expertise is the ability to recognize deviation from the expected clinical progression, allowing the adaptive expert to reframe the situation for learning and innovation. Mylopoulos et al. (2016) describe preparation for future learning as “the capacity to learn new information, to use resources effectively and innovatively, and to invent new strategies for learning and problem-solving in practice.” Working to firmly establish prototypical illness scripts at the UME level is essential before the greater levels of meaningful variation are encountered during graduate medical education training as described in later sections.
Metacognitive and self-regulated learning skills in a UME program
Adaptive expertise is “the product of a learned skill set, characterized by habits of mind that develop over time and with practice” (Mylopoulos & Woods, 2009). Metacognitive and self-regulated learning skills are at the core of this approach. Vanderbilt targets the development of these skills and habits of mind across the curriculum through longitudinal learning communities (Fleming et al., 2013). Serving as the academic component of an advisory Colleges program, the Learning Communities coursework requires students to explore and discuss relevant skills and ideal habits (See Table 2). Throughout the four years, students create written reflections and participate in small group College-based reflection discussions to foster the habit and skills of reflective practice.
Additionally, to foster metacognitive and self-regulated learning skills, students are paired with a longitudinal Portfolio Coach to discuss accrued competency-based assessment evidence in their learning portfolio, explore achievement of performance expectations, and direct future learning. Before coaching meetings, students complete a guided self-assessment in each competency domain, while Portfolio Coaches independently review the student’s portfolio. Students and coaches employ (often implicitly) the Master Adaptive Learners process (Cutrer et al., 2017), identifying areas for growth (Planning), strategies for learning (Learning), comparing internal student and external coach interpretation of data (Assessing), and development of personalized learning goals (Adjusting).
Lessons learned – UME
We found that there are curriculum design trade-offs to be made in promoting AE at the undergraduate medical education level. While our educators have a great deal of control over the curriculum and learning environment, we had to fight the tendency to pack the already congested medical school curriculum ever more tightly. The students felt an imperative toward learning efficiency that works against educational elements intended for long-term benefit such as preparation for future learning and adaptive expertise.
Graduate medical education (GME) – four emergency medicine residency programs
GME Themes: Compared to centralized undergraduate curricula, graduate medical education programs have less control over the workplace-based learning environment. However, many features of that environment align with adaptive expertise teaching strategies: opportunities for meaningful variation abound in daily clinical work, productive struggle and discovery are facilitated under cognitive apprenticeship models, while quality improvement methods invite reflective metacognition.
Teaching residents about the concept of adaptive expertise fosters their investment in effortful learning. Residents must learn to balance expectations for clinical efficiency with time-intensive, effortful learning necessary for deep conceptual understanding. Routinizing work may yield better efficiency metrics, but it is insufficient for unforeseen problems that demand knowledge transfer. To solve such problems, learners must innovate, a skill gleaned through laborious, curiosity-driven inquiry that requires attention separate from clinical work.
We describe strategies used by our emergency medicine residency programs to cultivate adaptive expertise. We represent Johns Hopkins University, New York University, Stanford University, and University of Michigan.
Conceptual understanding in a GME Program
At the University of Michigan, emergency department patients identified as critically ill are moved to the Emergency Critical Care Center (EC3), a designated critical care area where a specific care team with advanced critical care training relies on a deep understanding of pathophysiology and critical care to provide optimal, customized care. (Gunnerson et al., 2019) We incorporated the EC3 into the EM residency curriculum to promote residents’ deep conceptual understanding of the pathophysiology of critical illness and their time-dependent interventions. Unlike time-pressured initial resuscitations, EC3 allows residents to better explore complex conditions—thus helping them develop conceptual understanding and cognitive integrations needed for future learning (Mylopoulos et al., 2018b). We assign EC3 shifts to both junior learners just starting to integrate foundational knowledge with clinical presentations and senior learners focusing on content mastery and subtleties of presentation and management.
Productive struggle and discovery in a GME program
Productive struggle and discovery during autonomous patient care is critical to learning adaptive expertise. (Branzetti et al., 2022) Appropriately challenging clinical responsibilities generate real-life problems which spur intrinsic motivations to learn. Thus, we refined the clinical responsibilities of our residents through a lens of productive struggle and discovery. In each program, this culminated in a senior resident supervisory experience that approached that of the attending. These experiences focus on clinical efficiency, team management, and clinical teaching. At New York University we made a strategic decision to promote this role by physically relocating the attending away from the senior resident workstation to emphasize the resident team leader role. Additionally, we placed more learners under the supervision of senior residents than attending-led teams to intentionally promote a teaching struggle. We also maximized resident autonomy and struggle through a programmatic emphasis on relational autonomy, the support for learners to enact reasonable care plans different from their supervisors (Schumacher et al., 2013). Complementary faculty development emphasized the importance of learner autonomy and the restraint needed to accept safe deviations from faculty practice patterns.
Meaningful variation in a GME program
Trainees whose learning depends on clinical experiences alone may develop superficial and incomplete foundational knowledge, given it is impossible to see the breadth of all clinical presentations during residency. (Regan et al., 2019, Branzetti et al., 2022) We mitigate this challenge using meaningful case variation (Mylopoulos et al., 2018b) during clinical encounters and in complex simulated scenarios. This approach is most effective when multiple concepts are combined in a theoretical case. For example, supervisors change the history or physical using “What if…” questions, such as “What if the patient was a child?” At Johns Hopkins University, we incorporated meaningful variation into our simulation and remediation programs. Residents participate in simulated, consecutive cases of status epilepticus that have distinct etiologies reflected in contrasting histories and examinations. Residents then synthesize commonalities and differences in patient presentations and management during debriefing. We also use meaningful variation to diagnose and remediate struggling learners through divergent presentations and etiologies of seemingly common cases. This helps struggling learners build the cognitive schema critical to conceptual understanding and helps our educators diagnose underlying reasoning issues (Mylopoulos et al., 2018b).
Metacognitive and self-regulated learning skills in a GME program
We found that residents entering training had minimal, if any, preparation in how to plan their learning, set learning goals, or use evidence-based learning strategies (Regan et al., 2019, Branzetti et al., 2022). Intern orientation provided an ideal time to teach metacognition and self-regulated learning. We conducted orientation sessions at Stanford University and Johns Hopkins University focused on planning for learning. Interns listened to a clinical case and were asked to identify their knowledge gaps, prioritize the most relevant gap, and identify learning resources to fill that gap. Learners then discussed their decisions. This activity emphasized agency, curiosity, and goal setting — all areas with which typical learners struggle. (Branzetti et al., 2022) We also taught strategies to plan learning, promote self-directed learning, and establish personal learning goals. All of our programs incorporate coaching strategies to hold learners accountable to goals, acknowledge barriers, and support emotional responses to self-regulated learning. This metacognitive self-assessment promotes continued skill development and adaptive expertise.
Lessons learned – GME
There is an imperative for clinical efficiency in residency that can disfavour adaptive expertise training. Whereas medical students may favour efficiency of learning, residents emphasize efficiency of patient care work. Nevertheless, we found many opportunities to develop adaptive expertise. The clinical learning environment promotes skill development through productive struggle and discovery. Finally, we found ways to promote deep conceptual knowledge through advanced clinical placements and case variations.
Continuing professional development – The Mayo Clinic Education and Technology Forum
CPD Themes: Continuing Professional Development has traditionally provided episodic lecture-based sessions. Alternatively, it can also offer unique opportunities to deliberately design interprofessional communities of inquiry through which adaptive expertise can flourish. CPD participants have deep conceptual knowledge and expertise in their professional domain, which can make them more willing to learn about and through desirable difficulties. Similarly, they are more fully vested in their healthcare system where they can apply and adapt new learning to accelerate organizational efficiencies and innovations.
For 10 years, the Mayo Clinic College of Medicine and Science (Mayo) has held an annual, multi-site, interprofessional faculty development program, the “Education and Technology Forum”, designed to advance knowledge and skills related to pedagogy and technology, support innovation in education, and create a community of practice (Billings et al., 2022; Mayo, 2021). The program evolved from a narrow focus on technology and pedagogy to more general co-creation of knowledge, informing strategic planning, and fostering change in education. It has been attended by over 1700 health professions educators (physicians, allied health professionals, basic scientists, nurses, etc.) and education staff (technologists, instructional designers, administrators, coordinators, faculty developers, and specialists).
Over the past several years, we focused the Education and Technology Forum on the evolving and intersecting roles of the health professions educator, learner, and learning environment. In 2021, we promoted ideation and assumption checking, and collaboratively generated solutions for a defined organization problem space, namely the learning environments of the future (Billings et al., 2022).
We designed the 2022 Education and Technology Forum to advance shared conceptual understanding through productive struggle and discovery, support meaningful variation, engage in metacognitive activities, and apply Master Adaptive Learner and coaching frameworks. (Auerbach et al., 2020; Cutrer et al., 2021) The program was a 3-h synchronous, virtual curriculum coupled with asynchronous pre-and post-event curated resources to promote discovery and self-regulated learning. Establishing social presence was critical to promote curiosity, exploration, and vulnerability in the virtual space (Garrison, 2007). Personalization of learning, clear expectations for engagement, rapid-fire breakouts to engage with other participants, mailed swag boxes, and consistent small group membership contributed to the creation of an environment for cognitive engagement and testing of assumptions (Billings et al., 2022).
Conceptual understanding in a CPD program
Before the event, we provided access to a web-based Education and Technology Forum resource hub, including pre-work, agenda, and information about the interprofessional event planning team. The curated pre-work (e.g., literature, video snippets, podcasts) promoted a deeper conceptual understanding of the Master Adaptive Learner framework and coaching skills. The pre-work primed participants to self-assess performance driven gaps in knowledge, skills, and attitudes, and engage with primary and secondary (deeper dive) resources in order to prepare for in-person learning. To personalize their own learning experience during small group activities and cultivate interprofessional community before the event, we invited participants to choose which 1 of 8 learner/educator persona they best related to. The personas reinforced transferability and internalization of learning. To normalize independent struggle and guided discovery while learning new technological skills, we hosted a live “prep your tech” session prior to the event and built in opportunities for participants to use virtual whiteboards and conferencing technologies throughout the event.
Meaningful variation, productive struggle and discovery, and metacognition in a CPD program
During the live experience, participants learned how to cultivate adaptive expertise in their own learning, teaching, and supervising practices. To promote a shared mental model, we designed the live session to align with the steps of the Master Adaptive Learner framework (Plan, Learn, Assess, and Adjust) (Cutrer et al., 2017). Each segment included a microlecture from an external Master Adaptive Learner expert, local in-practice applications, and a small group activity. The microlectures defined the common language terms, the significance of the framework component, and application as a case scenario (Cutrer et al., 2017; Steenhof, 2020). Following each microlecture, Mayo health professions educators provided examples of authentic local applications of effective learning strategies, coaching connections, and assessment in practice. Using role modeling by peers and sharing of meaningful variations, we aimed to influence and inspire (Auerbach et al., 2020). Small group activities allowed participants to apply developing knowledge and skills, including effective learning strategies and external feedback, while practicing coaching methods such as asking powerful questions and deep listening. Personas and scenarios were leveraged to introduce meaningful variation and reinforce transference of new skills and adaptive expertise. Variation became more complex with each small group activity, promoting a progressive, iterative approach to problem solving and scaffolding of learning through each of the Master Adaptive Learner phases. Trained small group leaders supported participants during periods of struggle and guided discovery, and afforded opportunities for community-driven gap identification (Regan et al., 2019). Metacognitive moments book-ended the synchronous session by inviting participants to reflect on prior approaches and commit to future actions to support Master Adaptive Learner characteristics.
Following the program, we focused on building individuals’ capacity to contribute to organizational change (Jolly, 2014). Cultivating social presence and cognitive flexibility during the event promoted individual learner commitment to self-regulating behaviors (Grotzer et al., 2021). The web-based resource hub evolved to support knowledge retrieval, facilitate sharing with peers, and encourage adaptation to novel solutions. To invest in development of adaptive expertise, we employed tactics, strategies, and priorities which support co-creation of new knowledge and continuous learning as a part of working (Mylopoulos et al., 2016). Participants rated their experiences with the Education and Technology Forum positively. By establishing the community, we contributed to a learning environment where participants could be vulnerable, draw from personal motivators, and embrace a growth mindset (Auerbach et al., 2020; Kegan et al., 2014). The Education and Technology Forum served as an incubator environment to cultivate awareness of possibilities and reinforce shifts in individual and organizational practices (Pusic et al., 2018).
Lessons learned – continuing professional development
Learning organizations like Mayo continually evolve. Organizational commitments to foster an optimal teaching and learning environment have reinforced the general culture of learning and enhanced organization capabilities. (Auerbach et al., 2020; Gephardt 1996; Senge, 1990). We leveraged deliberately designed CPD as an effective means to advance the adaptive expertise of our individual health care workers and foster learning environments where collective learning and shared mental models facilitate individual contributions to the capacity of the organization to also act adaptively, appropriately balancing routinization with innovation. (Garvin, 1993).
Cross-cutting themes –adaptive expertise across the continuum
The discussion, analysis and writing of our case descriptions revealed several themes that interact differentially with learner level when educating for adaptive expertise.
-
This work is time and resource intensive.
-
Education must be sensitive to learner needs and changing environments.
-
Success is dependent on a clear understanding of the value proposition to learners.
-
Extrinsic motivators can work against an adaptive expertise mindset.
Resource allocation
The key instructional strategies used to teach adaptive expertise are costly as measured in the time, money, and the human capital required to redesign and execute necessary curricula. At Vanderbilt, the entire medical school curriculum was reimagined to provide a perspective on adaptive expertise. For the four emergency medicine residency programs who adopted methods of promoting productive struggle and discovery while on clinical shifts, there was a necessary sacrifice of clinical efficiencies like patient throughput. And at Mayo Clinic, the investment to design and deliver an annual faculty development program of the scale described is significant.
Program level adaptivity
Rigid standardized educational structures work against a message of learning for adaptivity. The VUSM curriculum supported learner agency through co-creation of a dynamic curriculum with considerable flexibility of experience. Allowing learners to choose from a diversity of potential learning outcomes reinforced core adaptive learning processes. An emergency medicine residency structure that promotes productive struggle and discovery necessitates flexible program supervision that assures patient safety while meeting the unique needs of each resident. And the continuing professional development event held by Mayo celebrated organizational learning and organizational adaptivity. Each creates space for individual learning for adaptivity by creating a favourable context and environment for it.
Changing perceptions of value
Learning for adaptivity requires instructional strategies that ask for more from each learner, including sacrifices in learning or work efficiency. Not only do trainees have to learn the subject matter, for which they are rewarded in the short term with improved assessment scores, but they also must learn how to learn, which yields a payoff of adaptive expertise that is much further downstream in their careers. Success is predicated on a clear articulation of the benefit of adaptive expertise and the necessary support of learners to achieve that goal. In the Vanderbilt project, an appreciation for deep conceptual understanding is built into the structure of pre-clinical learning. The connections to clinical practice are made clear from the earliest days of medical school and reiterated in the post-clerkship phase by having both a basic-scientist and a clinician together facilitate integrated science courses. For resident trainees, the value of deep conceptual (physiologic) understanding is represented by the sub-specialist critical-care physician working alongside the generalist EM physician, both of whom coach the EM resident in the care of the sickest, most complex patients; they model what can be routinized, what needs clinical innovation, and where the balance lies. In the Mayo faculty development program, value of adaptivity was established by highlighting authentic adaptivity work in the full organization and its support of the approach.
Incentives
Learning for adaptive expertise is generally a long-term process of developing habits of mind that are an investment for the future. Related to value perception, the mal-alignment of incentives, especially short-term ones, was found to be detrimental across all three levels of training. Medical students who are focused on the next knowledge test are likely to use discretionary time on those tests instead of developing a sustainable approach to deeper reflections on the material. Similarly, residents who are rewarded directly or indirectly for the number of patients they see will not take the time to reflect on practice in a way that leads to incremental improvement over a career. In continuing professional development, the incentives that an organization offers sends a message about its values. A key success factor for Mayo was investing over the longer term in a community of interprofessional educators while reinforcing the significance of collaborative struggle, discovery, and reflection in a safe, supportive learning environment.
Discussion
Using educational case descriptions of recent efforts to promote adaptive expertise, we drew lessons that might advantage other programs with this intent. At the undergraduate level, Vanderbilt University School of Medicine shows how a restructuring of the entire program can provide multiple opportunities to foster adaptive expertise development. At the residency level, the participating emergency medicine programs showed useful variability in opportunistically implementing adaptive expertise training. The CPD example shows that an existing event can be designed to orient an entire multi-matrix institution towards an adaptive expertise mindset when the organization embraces, as a cultural goal, an emphasis on the ability to balance routinization with innovation.
An important theme was that the learning strategies that engender adaptive expertise – deep conceptual understanding, productive struggle and discovery, meaningful variation, and meta-cognition – require considerable personal investment by and for the learner. The complexity of training for adaptive expertise is exponentiated when, instead of delivering a standardized curriculum to a standardized notion of the learner, processes for promoting adaptability are layered onto individualized learning plans. However, these strategies enable a higher goal allowing the learner to treat never-standard patients with, for example, chronic diseases in difficult contexts. Each educational program had to make a different value argument for learning in this more difficult manner. Research programs in general education that advocate for depth approaches, whether under the rubric of Preparation for Future Learning or the Bjorks’ “desirable difficulties”, are only now engaging with the question of how to motivate learners to embrace these difficulties (Bjork & Bjork, 2020). Our case descriptions bring this issue into clear relief in medical education.
In a qualitative study of the learner perspective, Betinol et al. (2022) interviewed recent graduates of a physiotherapy training program and found that adaptive expertise may be a “threshold concept”, one that is difficult to grasp initially but once successfully learned opens up new way of thinking within a professional domain. They found that a learner’s evolving definition of expertise shifted from accumulation of knowledge to “advancing understanding and maintaining a creative approach to practice”. The learners seemed to be in a”transitional state”, alternating between routinized and adaptive approaches, instead of integrating them. Their findings suggested that a number of “epistemological obstacles…undermine localized efforts by individual teachers…to support transformation to an adaptive expertise framing”. In an unanticipated finding, the researchers noticed that the participants seemed to be reconceptualizing their notions of adaptive expertise right before the researchers’ eyes, with the interviews “functioning as a form of guided reflection” in these early graduates. Our findings, from the perspective of educators, support this view in that we noted a developmental progression to the ease with which we could speak of adaptive expertise to our learners, with residency seemingly a transitional state (Regan et al., 2019; Branzetti et al., 2022).
Helping learners reconceptualize to an adaptive expertise framing requires educators who have this shared language, an express goal of the more general Master Adaptive Learner framework. MAL is a knowledge translation device that brings together foundational education science theories – centered around adaptive expertise – in an accessible format that can inform both curriculum development and coaching processes (Lomis et al., 2021a; Pusic et al., 2019b). In this regard, the Mayo Clinic CPD example is informative for its institution-wide embrace of the MAL framework as a basis for emphasizing learning adaptive expertise at the organizational level. The structure of the event, with its emphasis on productive struggle with individual complexity in learning, shows the organization walking the walk of taking on desirable difficulties by going beyond routinized care to a more adaptive individualized approach.
Complicating the work will be the difficulty in measuring its direct impact (Stringer et al., 2022; Beniol et al., 2022). To consider the effect of learning for adaptive expertise, one must examine a learner for longer-term, not immediate performance. Each of these instructional methods represent constructivist advances but each necessarily complicates attempts at numerical summary that require accumulation of fungible like-for-like units of analysis. Systematic reviews (e.g. Kua et al., 2021) confirm this difficulty likely stemming from the complexity of the methodological setup required to demonstrate a preparation-for-future learning effect (Kulasegaram et al., 2013; Bransford and Schwartz, 1999). These research methods would be difficult if not impossible to replicate in the real-world contexts we describe here. Instead, detailed case descriptions like the ones we have started at our institutions may be a useful way to find the right level of implementation.
In summary, we have described the use of instructional designs for promoting adaptive expertise in medical education contexts representative of the full developmental continuum. True to the complexity inherent in the ambition, we have found success, difficulty, and a sense of the investment required.
References
Auerbach, L., Santen, S. A., Cutrer, W. B., Daniel, M., Wilson-Delfosse, A. L., & Roberts, N. K. (2020). The educators’ experience: Learning environments that support the master adaptive learner. Medical Teacher, 42(11), 1270–1274.
Betinol, E., Murphy, S., & Regehr, G. (2022). Exploring the development of adaptive expertise through the lens of threshold concepts. Medical Education. https://doi.org/10.1111/medu.14887
Billings, H., Malin, T., Allen, J., Bergene, A., Cornelius, K., Craft, S., Hartzheim, L., Johnson, S. A., Kallay, J., Kreuter, J., & Raths, M. (2022). Reimagining learning spaces of the future: An interprofessional, virtual workshop utilizing rapid idea generation and lean startup methodologies. MedEdPORTAL, 18, 11217.
Bird, E. C., Osheroff, N., Pettepher, C. C., Cutrer, W. B., & Carnahan, R. H. (2017). Using small case-based learning groups as a setting for teaching medical students how to provide and receive peer feedback. Medical Science Educator, 27(4), 759–765.
Bjork, E. L., & Bjork, R. A. (2011). Making things hard on yourself, but in a good way: Creating desirable difficulties to enhance learning. In M. A. Gernsbacher, R. W. Pew, L. M. Hough, & J. R. Pomerantz (Eds.), Psychology and the real world: Essays illustrating fundamental contributions to society (pp. 56–64). Worth Publisher.
Bjork, R. A., & Bjork, E. L. (2020). Desirable difficulties in theory and practice. Journal of Applied Research in Memory and Cognition, 9(4), 475–479.
Bransford, J. D., & Schwartz, D. L. (1999). Rethinking transfer: A simple proposal with multiple implications. Review of Research in Education, 24(1), 61–100.
Branzetti, J., Commissaris, C., Croteau, C., Ehmann, M. R., Gisondi, M. A., Hopson, L. R., Lai, K. Y., & Regan, L. (2022). The best laid plans? A qualitative investigation of how resident physicians plan their learning. Academic Medicine : Journal of the Association of American Medical Colleges, Advance Online Publication. https://doi.org/10.1097/ACM.0000000000004751
Carbonell, K. B., Stalmeijer, R. E., Könings, K. D., Segers, M., & van Merriënboer, J. J. (2014). How experts deal with novel situations: A review of adaptive expertise. Educational Research Review, 12, 14–29.
Charlin, B., Tardif, J., & Boshuizen, H. P. (2000). Scripts and medical diagnostic knowledge: Theory and applications for clinical reasoning instruction and research. Academic Medicine, 75(2), 182–190.
Cutrer, W. B., & Brady, D. (2020). Vanderbilt university school of medicine. Academic Medicine, 95(9S), S474–S477.
Cutrer, W. B., Sullivan, W. M., & Fleming, A. E. (2013). Educational strategies for improving clinical reasoning. Current Problems in Pediatric and Adolescent Health Care, 43(9), 248–257.
Cutrer, W. B., Miller, B., Pusic, M. V., Mejicano, G., Mangrulkar, R. S., Gruppen, L. D., Hawkins, R. E., Skochelak, S. E., & Moore, D. E., Jr. (2017). Fostering the development of master adaptive learners: a conceptual model to guide skill acquisition in medical education. Academic Medicine, 92(1), 70–75.
Cutrer, W. B., Atkinson, H. G., Friedman, E., Deiorio, N., Gruppen, L. D., Dekhtyar, M., & Pusic, M. (2018). Exploring the characteristics and context that allow master adaptive learners to thrive. Medical Teacher, 40(8), 791–796.
Cutrer, W. B., Spickard, W. A., III., Triola, M. M., Allen, B. L., Spell, N., III., Herrine, S. K., Dalrymple, J. L., Gorman, P. N., & Lomis, K. D. (2021). Exploiting the power of information in medical education. Medical Teacher, 43(2), S17–S24.
Dahlman, K. B., Weinger, M. B., Lomis, K. D., Nanney, L., Osheroff, N., Moore, D. E., Estrada, L., & Cutrer, W. B. (2018). Integrating foundational sciences in a clinical context in the post-clerkship curriculum. Medical Science Educator, 28(1), 145–154.
Fleming, A., Cutrer, W., Reimschisel, T., & Gigante, J. (2012). You too can teach clinical reasoning! Pediatrics, 130(5), 795–797.
Fleming, A., Cutrer, W., Moutsios, S., Heavrin, B., Pilla, M., Eichbaum, Q., & Rodgers, S. (2013). Building learning communities: Evolution of the colleges at Vanderbilt University school of medicine. Academic Medicine, 88(9), 1246–1251.
Garrison, D. R. (2007). Online community of inquiry review: Social, cognitive, and teaching presence issues. Journal of Asynchronous Learning Networks, 11(1), 61–72.
Garvin, D. A. (1993). Building a learning organization. Harvard Business Review, 71(4), 78–91. PMID:1012704.
Gephart, M. A., Marsick, V. J., Van Buren, M. E., Spiro, M. S., & Senge, P. (1996). Learning organizations come alive. Training & Development, 50(12), 34–46.
Gonzalo, J. D., Haidet, P., Papp, K. K., Wolpaw, D. R., Moser, E., Wittenstein, R. D., & Wolpaw, T. (2017). Educating for the 21st-century health care system. Academic Medicine, 92(1), 35–39.
Grotzer, T.A., Forshaw, T., & Gonzalez, E. (2021). Developing adaptive expertise for navigating new terrain: An essential element of success in learning and the workplace. The Next Level Lab at the Harvard Graduate School of Education. President and Fellows of Harvard College: Cambridge, MA.
Gunnerson, K. J., Bassin, B. S., Havey, R. A., Haas, N. L., Sozener, C. B., Medlin, R. P., Gegenheimer-Holmes, J. A., Laurinec, S. L., Boyd, C., Cranford, J. A., & Whitmore, S. P. (2019). Association of an emergency department–based intensive care unit with survival and inpatient intensive care unit admissions. JAMA Network Open, 2(7), e197584–e197584.
Jolly, B. (2014). Faculty development for organizational change. In Faculty Development in the Health Professions (pp. 119–137). Springer, Dordrecht.
Kegan, R., Lahey, L., Fleming, A., & Miller, M. (2014). Making business personal. Harvard Business Review, 92(4), 44–52.
Kua, J., Lim, W. S., Teo, W., & Edwards, R. A. (2021). A scoping review of adaptive expertise in education. Medical Teacher, 43(3), 347–355.
Kulasegaram, K. M., Martimianakis, M. A., Mylopoulos, M., Whitehead, C. R., & Woods, N. N. (2013). Cognition before curriculum: Rethinking the integration of basic science and clinical learning. Academic Medicine, 88(10), 1578–1585.
Lomis, K. D., Mejicano, G. C., Caverzagie, K. J., Monrad, S. U., Pusic, M., & Hauer, K. E. (2021a). The critical role of infrastructure and organizational culture in implementing competency-based education and individualized pathways in undergraduate medical education. Medical Teacher, 43(sup2), S7–S16.
Lomis, K. D., Santen, S. A., Dekhtyar, M., Elliott, V. S., Richardson, J., Hammoud, M. M., Hawkins, R., & Skochelak, S. E. (2021b). The accelerating change in medical education consortium: key drivers of transformative change. Academic Medicine, 96(7), 979–988.
Mayo Clinic College of Medicine and Science. (2021, March). Our Voices, Our Ideas: Students at the Education and Technology Forum. Accessed at https://college.mayo.edu/about/news/news-archive/our-voices-our-ideas-students-at-the-education-and-technology-forum
Merritt, C., Santen, S. A., Cico, S. J., Wolff, M., & Pusic, M. (2022). Punctuated equilibrium: COVID and the duty to teach for adaptive expertise. Western Journal of Emergency Medicine, 23(1), 56.
Mylopoulos, M., & Woods, N. N. (2009). Having our cake and eating it too: Seeking the best of both worlds in expertise research. Medical Education, 43(5), 406–413.
Mylopoulos, M., Brydges, R., Woods, N. N., Manzone, J., & Schwartz, D. L. (2016). Preparation for future learning: A missing competency in health professions education? Medical Education, 50(1), 115–123.
Mylopoulos, M., Steenhof, N., Kaushal, A., & Woods, N. N. (2018a). Twelve tips for designing curricula that support the development of adaptive expertise. Medical Teacher, 40(8), 850–854. https://doi.org/10.1080/0142159X.2018.1484082
Mylopoulos, M., Kulasegaram, K., & Woods, N. N. (2018b). Developing the experts we need: Fostering adaptive expertise through education. Journal of Evaluation in Clinical Practice, 24(3), 674–677.
Neubauer, B. E., Witkop, C. T., & Varpaio, L. (2019). How phenomenology can help us learn from the experiences of others. Perspectives on Medical Education, 8(2), 90–97.
Pusic, M. V., Santen, S. A., Dekhtyar, M., Poncelet, A. N., Roberts, N. K., Wilson-Delfosse, A. L., & Cutrer, W. B. (2018). Learning to balance efficiency and innovation for optimal adaptive expertise. Medical Teacher, 40(8), 820–827.
Pusic, M., Cutrer, W., & Santen, S. A. (2019a). How does Master Adaptive Learning advance expertise development? Chapter 2. In W. Cutrer & M. V. Pusic (Eds.), The Master Adaptive Learner (pp. 10–17). NL. Elsevier Publishing Group.
Pusic, M., Boutis, K., Cutrer, W., & Santen, S. A. (2019b). How does master adaptive learning ensure optimal pathways to clinical expertise? Chapter 16. In W. Cutrer & M. V. Pusic (Eds.), The Master Adaptive Learner (pp. 174–192). NL. Elsevier Publishing Group.
Regan, L., Hopson, L. R., Gisondi, M. A., & Branzetti, J. (2019). Learning to learn: A qualitative study to uncover strategies used by master adaptive learners in the planning of learning. Medical Teacher, 41(11), 1252–1262.
Schumacher, D. J., Englander, R., & Carraccio, C. (2013). Developing the master learner: Applying learning theory to the learner, the teacher, and the learning environment. Academic Medicine, 88(11), 1635–1645.
Senge, P. (1990). The Fifth Discipline: The Art and Practice of the Learning Organization. New York.
Steenhof, N. (2020). Adaptive expertise in continuing pharmacy professional development. Pharmacy, 8(1), 21.
Stringer, J. K., Gruppen, L. D., Ryan, M. S., Ginzburg, S. B., Cutrer, W. B., Wolff, M., & Santen, S. A. (2022). Measuring the master adaptive learner: development and internal structure validity evidence for a new instrument. Medical Science Educator, 32(1), 183–193.
ten Cate, O., Snell, L., Mann, K., & Vermunt, J. (2004). Orienting teaching toward the learning process. Academic Medicine : Journal of the Association of American Medical Colleges, 79(3), 219–228. https://doi.org/10.1097/00001888-200403000-00005.
Thistlethwaite, J. E., Davies, D., Ekeocha, S., Kidd, J. M., MacDougall, C., Matthews, P., Purkis, J., & Clay, D. (2012). The effectiveness of case-based learning in health professional education. A BEME systematic review: BEME Guide No 23. Medical teacher, 34(6), e421–e444.
Acknowledgements
HB and EH wish to acknowledge the 2021 and 2022 Mayo Clinic ETF Team, in particular Dr. Amy Seegmiller Renner and Lisa Hartzheim for their development of the personas.
Funding
WBC and MVP wish to acknowledge the grant support of the American Medical Association Reimagining Residency initiative. No funding was received to assist with the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the manuscript conception and design. Material preparation and the first outline of the manuscript was written by MVP and WBC; WBC wrote the first draft of the UME section; LH, LR, MG, JB wrote the first draft of the GME section; HB, EH wrote the first draft of the CPD section; and all authors commented on subsequent versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Research involving human participants
The authors describe their experiences in innovating in their specific education programs where the innovations are considered within the scope of work.
Informed consent
Where we report on research data that was collected, we cite references that report the study details including consent processes and institutional review board approval. No new primary research was carried out for this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pusic, M.V., Hall, E., Billings, H. et al. Educating for adaptive expertise: case examples along the medical education continuum. Adv in Health Sci Educ 27, 1383–1400 (2022). https://doi.org/10.1007/s10459-022-10165-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10459-022-10165-z