Abstract
Although spinal instrumentation technique has undergone revolutionary progress over the past few decades, it may still carry significant surgery-related risks. The purpose of the present study was to assess the radiological accuracy of spinal screw instrumentation using a hybrid operating room (OR) and quantify the related radiation exposure. This retrospective study included 33 cases of complex spine fusion surgeries that were conducted using a hybrid OR with a flat panel detector (FPD) angiography system. Twelve cases (36.4%) were cervical, and 21 (63.6%) were thoracolumbar. The average number of spine fusion levels was 3 and 4.8, respectively, at the cervical and thoracolumbar spine levels. A FPD angiography system was used for intraoperative cone-beam computed tomography (CBCT) to obtain multi-slice spine images. All operations were conducted under optimized radiation shielding. Entrance surface doses (ESDs) and exposure times were recorded in all cases. A total of 313 screws were placed. Satisfactory screw insertion could be achieved in all cases with safe screw placement in 97.4% and acceptable placement in 2.6%. None of the cases showed any significant anatomical violation by the screws. The radiation exposure to the patients was absolutely consistent with the desired ESD value, and that to the surgeons, under the annual dose limit. These results suggest that the hybrid OR with a FPD angiography system is helpful to achieve safe and precise spinal fusion surgery, especially in complex cases.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Spinal instrumentation technique has undergone revolutionary progress over the past few decades. This progress has significantly changed the surgical strategy for spine disease, for not only spinal trauma but also congenital diseases, cancer, infection, and aging degeneration. Hospitalization time has been reduced, patients are mobilized more rapidly, and the overall surgical outcome has improved. On the other hand, spinal instrumentation such as pedicle screws may carry a risk of neural or vascular injury [1, 2, 4, 13]. To avoid such surgery-related complications, intraoperative image guidance using fluoroscopy or CT-based computer navigation was developed. However, technical pitfalls and the means to avoid them need to be carefully considered [31]. More recently, a 3D-CT-based navigation system using intraoperative cone-beam computed tomography (CBCT) with a flat panel detector angiography module, also referred to as hybrid operating room (OR), has been actively developed to achieve more accurate and safe surgery [23]. Meanwhile, the associated radiation exposure to the patients and surgeons remains a major concern. The purpose of the present study was to assess the radiological accuracy of spinal screw instrumentation using a hybrid OR system and quantify the related radiation exposure. The benefits and possible disadvantages of the hybrid OR system for spinal instrumentation surgery are discussed with a literature review.
Methods
Patients
This retrospective study included a total of 33 (23.2%) of 142 spine fusion surgeries in the study period from April 2014 to May 2017. The indication for use of hybrid OR with intraoperative CBCT imaging was carefully determined based on the complexity of the cases. So were indicated, cases of revision, multi-spine fusion, infectious, multi-trauma, and spinal deformity surgeries, while ordinary cases such as short fusion surgeries were usually completed using the conventional C-arm fluoroscopy. The patients included 22 men and 11 women, and their mean age at surgery was 62.8 years (range, 20–86 years). Twelve cases (36.4%) were cervical, and 21 (63.6%) were thoracolumbar. The average number of spine fusion levels was 3 and 4.8, respectively, at the cervical and thoracolumbar spine levels. Patients’ characteristics are summarized in Table 1.
Hybrid OR system
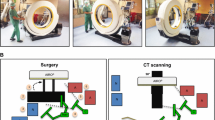
Spinal instrumentation, such as the cervical pedicle screw (CPS), cervical lateral mass screw (CLMS), cervical translaminar screw (CTL), thoracolumbar pedicle screw (TLPS), or lumbar cortical bone trajectory screw (LCBTS), was achieved using a fluoroscopy image guidance system. The initial insertion (screw or Kirschner wire) was conducted with free hands or assistance of a preoperative CT-based navigation module (Stealth Station, Medtronic, Inc., Memphis, TN, USA). A flat panel detector (FPD) angiography system AlluraClarity FD20 (Philips, Amsterdam, The Netherlands) was combined with a carbon-fiber operating table (Maquet, Germany) and used for intraoperative CBCT to obtain multi-slice spine images in the hybrid OR (Fig. 1). The size of the FPD was maximally 19 in, with a pulsed fluoroscopy rate of 7.5 p/s. The digital subtraction angiography frame rate was 30 f/s. Multi-slice spine images were then acquired immediately after the placement of spine instrumentation screws or temporary Kirschner wires to confirm their satisfactory and safe positioning, or the need of repositioning. After the placement of all instrumentation screws, local decompression, bilateral facet release, or interbody fusion was carried out if necessary. The rods, bent earlier according to the preoperative plan, were then applied to the screws and fully tightened. Bone grafting from local bone and beta tricalcium phosphate application were done to ensure adequate fusion.
A flat panel detector angiography system. The flat panel detector is combined with a carbon-fiber operation table and used for intraoperative cone-beam computed tomography (CBCT) in the hybrid OR system. a A flat panel detector angiography system is introduced after covering the operative site with sterile sheets. b, c Multi-slice spine images are obtained in a smooth and quick motion
Measurement of radiation exposure
All operations were conducted under optimized radiation shielding in the hybrid OR system. Entrance surface doses (ESDs) and exposure times were recorded in all cases in milliGray (mGy) and seconds, respectively, by radiological technicians. ESD can be measured at the center of the entrance surface in the X-ray beam field, and it includes backscattered radiation from the patient [20, 45]. In 23 cases, pocket radiation dosimeters (Hitachi, Tokyo, Japan) were placed inside and outside the protective suit of the principal surgeon to evaluate the radiation exposure to the surgeon during the surgery. Exposures are reported in microSievert (μSv).
Postoperative assessment of radiological accuracy of screw placement
The radiological accuracy of spinal instrumentation screws was evaluated based on the postoperative CT scans and defined retrospectively using our proposed grading scale (Table 2). Screw positions were classified into three grades based on the potential risk of neural or vascular injury: grade 0, safe placement; grade 1, minor cortical perforation without any possible clinical risks; and grade 2, major perforation associated with possible risks.
Statistical analysis
All data are expressed as means ± standard deviation. Statistical analysis of correlations between two variables was performed using the Pearson correlation coefficient. JMP version 9.0 software (SAS Institute, Cary, NC) was used for all statistical analyses in the present study. Values of p < 0.05 were considered significant.
Results
A total of 313 screws were placed in 33 cases to stabilize the spine using the hybrid OR system during the study period. The intraoperative fluoroscopic images obtained using a FPD angiography system were of great quality, wide and long enough to cover even cases of long spine fusions (Figs. 2 and 3). The intraoperative axial reconstruction images acquired from the CBCT were comparable in terms of quality to postoperative CT images (Fig. 4). The radiological accuracy of the screws was grade 0 in 97.4% (305 of the 313 screws) (Fig. 5a–c), grade 1 in 2.6% (8 of the 313 screws) (Fig. 4d–f), and grade 2 in 0%. No neural or vascular complications closely associated with screw placement were encountered in the present study. A total of 8 of the 313 screws were found to perforate the bone cortex, classified as grade 1 radiological accuracy. Four cervical LMS or TLS were found to outstrip by less than 2 mm, 1 thoracolumbar PS outstripped by less than 5 mm, and 3 lumbar CBTS were protruding by less than 10 mm. Fortunately, no screw of grade 2 was found in the present study. The radiological accuracy of screw placement is summarized in Table 3.
Radiation exposure
The radiation ESD of cervical spine cases ranged from 6.38 to 30.62 mGy, with an average of 14.11 mGy, and that of the thoracolumbar spine cases ranged from 27.15 to 381.32 mGy, with an average of 113.01 mGy. The average fluoroscopy time per surgery including CBCT was 90.3 s (22.2–277.2 s) for the cervical spine cases and 210.9 s (43.0–508.8 s) for the thoracolumbar spine cases. Radiation exposures outside the surgeon’s protective suit in cervical spine cases ranged from 1.0 to 15.0 μSv, with an average of 4.8 μSv, and from 0 to 3.0 μSv inside the protective suit, with an average of 0.25 μSv. These values in the thoracolumbar spine cases ranged from 7.0 to 146.0 μSv outside the protective suit, with an average of 54.1 μSv, and from 0 to 18.0 μSv, with an average of 5.7 μSv, inside the surgeon’s protective suit. The radiation exposure data for the patients and surgeon are summarized in Table 4. A linear regression and correlation analysis of collected data showed no significant correlation between the number of spine fusion levels and the recorded exposure time, but there was a noteworthy correlation between exposure time and ESD (p = 0.00005; r = 0.64602), as well as between the exposure time and doses recorded outside (p = 0.00003; r = 0.75411) and inside (p = 0.00003; r = 0.75689) the surgeon’s protective suit (Fig. 6).
Discussion
The latest technological advances for safe surgery
This study aimed to evaluate the benefits and possible disadvantages of a hybrid OR system, for spinal instrumentation surgery, in the context of the progressing intraoperative imaging technology. Its first benefit may be the fact that surgeons can avoid the high risk of instrumentation-related neural or vascular injury, using a combination of intraoperative wide fluoroscopy, CBCT, and eventually navigation. Spinal instrumentation surgery has become essential to manage spinal pathologies related to aging degeneration, trauma, inflammation, and infection. However, factors like the individual anatomical variations, surgeon’s experience, or material specifications may expose patients to risks of screw misplacement and their potentially associated complications [1, 2, 4, 13]. To avoid these, various protocols such as rational use, as in the present study, of pulsed fluoroscopy combined with intraoperative CBCT may help accurately reach the initially planned goals while minimizing the risks. Furthermore, the addition of navigation reduces the need of extensive radiation exposure while providing extra precision [5, 44].
The latest technological advances in imaging systems, such as 3D navigation, intraoperative O-arm, or the hybrid OR system presented here, have brought the possibility of instant visualization of anatomical structures and guidance support during surgery [8, 23, 25]. Among these options, some modalities demonstrated better surgical precision than others [35,36,37]. Though, the achieved accuracy taken alone could not suffice to determine the efficiency and must be weighed against the radiation exposure that accompanies it. From recent publications focusing on the surgical safety, it has emerged that spinal navigation was quite helpful for surgeons to place screws accurately, with higher success rates than the free-hand technique or standard fluoroscopy-guided surgery [6, 16, 22, 35]. Intraoperative CBCT offers helpful and reliable instant CT-like images of better clarity than those of conventional fluoroscopy, with reportedly the highest accuracy at all spinal levels, where used [19]. These images, once processed, also deliver high-quality 3D representations that are suitable for navigation during spinal surgery and indirectly help in reducing the overall radiation dose [33, 41].
No doubt remaining about the interest of navigation, two major types of CBCT systems are being actively used now for various spinal surgeries: the hybrid OR in this series and the O-arm system. The accuracy for spinal screw placement in the present study was comparable to that obtained using the O-arm system (Table 5). Satisfactory screw insertion could be achieved in all our cases (100%), with safe screw placement (grade 0) in 97.4% and acceptable ones (grade 1) in 2.6%. None of the present cases showed any significant anatomical violation by the screws exposing the patient to neural, vascular, or any visceral injury. Our hybrid OR system modality of intraoperative wide fluoroscopy and main usage of CBCT images allowed us to confirm the correct position of spinal instrumentation and to reposition any unsatisfactorily inserted screw. In addition to the comparable achievement capabilities to the O-arm, our hybrid OR CBCT can offer a great flexibility and provide wider 3D images than the O-arm system, making it a valuable tool for multilevel spinal fusion surgery.
Intraoperative radiation exposure
While the use of intraoperative CBCT has become popular and no doubt remains about its efficacy, concern about the intraoperative radiation exposure to surgeons and patients remains. A previous comparative clinical study demonstrated that the use of intraoperative CBCT resulted in higher radiation exposure than standard fluoroscopy during standard posterior fusion surgery for idiopathic scoliosis, whereas in vitro studies demonstrated decreased radiation exposure to the operator specifically [24, 36]. The recent developments have led to more complex systems, such as the O-arm that is being actively deployed now, but evaluations regarding its efficacy and safety of use are still needed [23, 28]. An anthropomorphic study put forward that O-arm system may expose patients to significant radiation doses [30]. A comparative phantom study demonstrated higher radiation doses to the surgeon by the O-arm than the C-arm in their 2D fluoroscopy mode [28], partly contrasting with the results found by other authors that suggested less radiation exposure for the surgeon in one series, but similarly, higher radiation exposure to the patient with the O-arm than the C-arm in both reports [39, 40]. Among the clinical series reported so far, Costa et al. demonstrated that the O-arm, as seen for the C-arm system, exposed patients to a higher radiation dose than standard fluoroscopy but concluded that their recorded doses were still acceptable when balancing with the advantages of the O-arm system [3]. Another author concluded to higher radiation doses with O-arm system than those in their free-hand series, without any noticeable benefit in cases of screw placement for moderate idiopathic scoliosis [42]. It is well-understandable that CBCT devices may add radiation to the customary use of fluoroscopic sessions from standard fluoroscopy. The current recommendations for addressing this issue suggest a reduction of the fluoroscopic time, potentiating the use of navigation or preferring low-dose protocols [29]. Our series brings additional data that may help to compare the relative radiation exposure between the common CBCT devices being used currently. The radiation exposures encountered during spinal fusion surgeries with use of O-arm system in clinical series found in the literature are summarized in Table 5. Notwithstanding the fact that there are some differences in operative protocols, number of spine fusion, surgeon’s experience, and method of evaluation among the available data, our imaging modality demonstrated acceptable results, in comparison to the O-arm system in terms of radiation exposure.
The levels of exposure may be affected by several factors, such as the surgeon’s experience and fluoroscopy technician’s aptitude, the extent of spinal fusion, and the intraoperative imaging modalities, which make standardization of these studies and strict comparison difficult [21]. Iprenburg et al., who analyzed their prospective study regarding patient radiation exposure during transforaminal lumbar endoscopic spine surgery, suggested that patients are likely to be exposed to higher doses of radiation during a surgeon’s early experience [10]. Indeed, surgeon’s evaluation capacity and agility are most likely to increase with time, allowing further avoidance of needless acquisitions. Distances to the radiation source and beam path are other essential factors affecting radiation exposure to the surgeon and operating staff. In addition, better devices and optimal system configurations may lead to higher efficiency and a better balance between the benefits and risks. The AlluraClarity FD20 system used in the present study comes with advantages that were described previously, among which is an improved algorithm for image noise reduction that allows higher-quality images for less acquisitions, and optimized functions that lower considerably the amount of radiation per acquisition [7]. The frame rate acquisitions in this study allowed no image deterioration by the system, contributed to containing the overall radiation exposure to both patient and surgeon. The radiation exposure to patients in the present study was absolutely consistent with the desired ESD value of less than 2000 mGy proposed by the Japan Association of Radiological Technologists [12]. Similarly, the radiation exposure to the surgeons stayed under the annual dose limit of 20,000 μSv recommended by the International Commission on Radiological Protection [9]. This leads us to the conclusion that the hybrid OR system used in the present study remains safe for routine spinal instrumentation surgery.
Conclusions
Our hybrid OR system allowed us to achieve precise surgery and was well suited for complex spinal fusion cases. Although concerns remain about the radiation exposure to both patients and surgeons, the data analyzed in the present study suggests that the hybrid OR with a FPD angiographic system is helpful to achieve safe and accurate spinal fusion surgery, especially in complex cases.
References
Abumi K, Shono Y, Ito M, Taneichi H, Kotani Y, Kaneda K (2000) Complications of pedicle screw fixation in reconstructive surgery of the cervical spine. Spine 25:962–969
Carbone JJ, Tortolani PJ, Quartararo LG (2003) Fluoroscopically assisted pedicle screw fixation for thoracic and thoracolumbar injuries: technique and short-term complications. Spine 28:91–97
Costa F, Tosi G, Attuati L, Cardia A, Ortolina A, Grimaldi M, Galbusera F, Fornari M (2016) Radiation exposure in spine surgery using an image-guided system based on intraoperative cone-beam computed tomography: analysis of 107 consecutive cases. J Neurosurg Spine 25:654–659
Esses SI, Sachs BL, Dreyzin V (1993) Complications associated with the technique of pedicle screw fixation: a selected survey of ABS members. Spine 18:2231–2239
Fomekong E, Pierrard J, Raftopoulos C (2017) Comparative cohort study of percutaneous pedicle screw implantation without versus with navigation in patients undergoing surgery for degenerative lumbar disc disease. World Neurosurg 111:e410–e417
Gelalis ID, Paschos NK, Pakos EE, Politis AN, Arnaoutoglou CM, Karageorgos AC, Ploumis A, Xenakis TA (2012) Accuracy of pedicle screw placement: a systematic review of prospective in vivo studies comparing free hand, fluoroscopy guidance and navigation techniques. Eur Spine J 21:247–255
Haas NA, Happel CM, Mauti M, Sahyoun C, Tebart LZ, Kececioglu D, Laser KT (2015) Substantial radiation reduction in pediatric and adult congenital heart disease interventions with a novel X-ray imaging technology. Int J Cardiol Heart Vasc 6:101–109
Houten JK, Nasser R, Baxi N (2012) Clinical assessment of percutaneous lumbar pedicle screw placement using the O-arm multidimensional surgical imaging system. Neurosurgery 70(4):990–995
International Commission Radiological Protection (2008) Recommendations of the International Commission on Radiological Protection ICRP Publication 103. Elsevier Ltd.
Iprenburg M, Wagner R, Godschalx A, Telfeian AE (2016) Patient radiation exposure during transforaminal lumbar endoscopic spine surgery: a prospective study. Neurosurg Focus 40:E7
Ishikawa Y, Kanemura T, Yoshida G, Matsumoto A, Ito Z, Tauchi R, Muramoto A, Ohno S, Nishimura Y (2011) Intraoperative, full rotation, three-dimensional image (O-arm)-based navigation system for cervical pedicle screw insertion. J Neurosurg Spine 15(5):472–478
Japan Association of Radiological Technologists (2017) Available at http://www.jart.jp/index.html
Jutte PC, Castelein RM (2002) Complications of pedicle screws in lumbar and lumbosacral fusions in 105 consecutive primary operations. Eur Spine J 11:594–598
Kleck CJ, Cullilmore I, LaFleur M, Lindley E, Rentschler ME, Burger EL, Cain CMJ, Patel VV (2016) A new 3-dimensional method for measuring precision in surgical navigation and methods to optimize navigation accuracy. Eur Spine J 25:1764–1774
Kobayashi K, Ando K, Ito K, Tsushima M, Morozumi M, Tanaka S, Machino M, Ota K, Ishiguro N, Imagama S (2018) Intraoperative radiation exposure in spinal scoliosis surgery for pediatric patients using the O-arm® imaging system. Eur J Orthop Surg Traumatol. https://doi.org/10.1007/s00590-018-2130-1
Kosmopoulos V, Schizas C (2007) Pedicle screw placement accuracy: a meta-analysis. Spine 32:E111–E120
Kotani T, Akazawa T, Sakuma T, Koyama K, Nemoto T, Nawata K, Yamazaki A, Minami S (2014) Accuracy of pedicle screw placement in scoliosis surgery: a comparison between conventional computed tomography-based and O-arm-based navigation techniques. Asian Spine J 8(3):331–338
Ling JM, Dinesh SK, Pang BC, Chen MW, Lim HL, Louange DT, Yu CS, Wang CME (2014) Routine spinal navigation for thoraco-lumbar pedicle screw insertion using the O-arm three-dimensional imaging system improves placement accuracy. J Clin Neurosci 21:493–498
Mason A, Paulsen R, Babuska JM, Rajpal S, Burneikiene S, Nelson EL, Villavicencio AT (2014) The accuracy of pedicle screw placement using intraoperative image guidance systems. J Neurosurg Spine 20:196–203
McParland BJ (1998) Entrance skin dose estimates derived from dose-area product measurements in interventional radiological procedures. Br J Radiol 71:1288–1295
Mulconrey DS (2016) Fluoroscopic radiation exposure in spinal surgery: in vivo evaluation for operating room personnel. Clin Spine Surg 29:E331–E335
Nakashima H, Sato K, Ando T, Inoh H, Nakamura H (2009) Comparison of the percutaneous screw placement precision of isocentric C-arm 3-dimensional fluoroscopy-navigated pedicle screw implantation and conventional fluoroscopy method with minimally invasive surgery. J Spinal Disord Tech 22:468–472
Nottmeier EW (2012) A review of image-guided spinal surgery. J Neurosurg Sci 56:35–47
O'Donnell C, Maertens A, Bompadre V, Wagner TA, Krengel W 3rd (2014) Comparative radiation exposure using standard fluoroscopy versus cone-beam computed tomography for posterior instrumented fusion in adolescent idiopathic scoliosis. Spine 39:E850–E855
Overley SC, Cho SK, Mehta AI, Arnold PM (2017) Navigation and robotics in spinal surgery: where are we now? Neurosurgery 80:S86–S99
Oertel MF, Hobart J, Stein M, Schreiber V, Scharbrodt W (2011) Clinical and methodological precision of spinal navigation assisted by 3D intraoperative O-arm radiographic imaging. J Neurosurg Spine 14(4):532–536
Patil S, Lindley EM, Burger EL, Yoshihara H, Patel VV (2012) Pedicle screw placement with O-arm and stealth navigation. Orthopedics 35:e61–e65
Park MS, Lee KM, Lee B, Min E, Kim Y, Jeon S, Huh Y, Lee K (2012) Comparison of operator radiation exposure between C-arm and O-arm fluoroscopy for orthopaedic surgery. Radiat Prot Dosim 148:431–438
Pireau N, Cordemans V, Banse X, Irda N, Lichtherte S, Kaminski L (2017) Radiation dose reduction in thoracic and lumbar spine instrumentation using navigation based on an intraoperative cone beam CT imaging system: a prospective randomized clinical trial. Eur Spine J 26:2818–2827
Pitteloud N, Gamulin A, Barea C, Damet J, Racloz G, Sans-Merce M (2017) Radiation exposure using the O-arm® surgical imaging system. Eur Spine J 26(3):651–657
Rahmathulla G, Nottmeier EW, Pirris SM, Deen HG, Pichelmann MA (2014) Intraoperative image-guided spinal navigation: technical pitfalls and their avoidance. Neurosurg Focus 36:E3
Safaee MM, Oh T, Pekmezci M, Clark AJ (2018) Radiation exposure with hybrid image-guidance-based minimally invasive transforaminal lumbar interbody fusion. J Clin Neurosci 48:122–127
Schafer S, Nithiananthan S, Mirota DJ, Uneri A, Stayman JW, Zbijewski W, Schmidgunst C, Kleinszig G, Khanna AJ, Siewerdsen JH (2011) Mobile C-arm cone-beam CT for guidance of spine surgery: image quality, radiation dose, and integration with interventional guidance. Med Phys 38:4563–4574
Shimokawa N, Takami T (2017) Surgical safety of cervical pedicle screw placement with computer navigation system. Neurosurg Rev 40:251–258
Shin MH, Hur JW, Ryu KS, Park CK (2015) Prospective comparison study between the fluoroscopy-guided and navigation coupled with O-arm-guided pedicle screw placement in the thoracic and lumbosacral spines. J Spinal Disord Tech 28(6):E347–E351
Smith HE, Welsch MD, Sasso RC, Vaccaro AR (2008) Comparison of radiation exposure in lumbar pedicle screw placement with fluoroscopy vs computer-assisted image guidance with intraoperative three-dimensional imaging. J Spinal Cord Med 31:532–537
Smith JD, Jack MM, Harn NR, Bertsch JR, Arnold PM (2016) Screw placement accuracy and outcomes following O-arm-navigated atlantoaxial fusion: a feasibility study. Glob Spine J 6:344–349
Silbermann J, Riese F, Allam Y, Reichert T, Koeppert H, Gutberlet M (2011) Computer tomography assessment of pedicle screw placement in lumbar and sacral spine: comparison between free-hand and O-arm based navigation techniques. Eur Spine J 20(6):875–881
Tabaraee E, Gibson AG, Karahalios DG, Potts EA, Mobasser JP, Burch S (2013) Intraoperative cone beam-computed tomography with navigation (O-ARM) versus conventional fluoroscopy (C-ARM): a cadaveric study comparing accuracy, efficiency, and safety for spinal instrumentation. Spine 38:1953–1958
Theologis AA, Burch S, Pekmezci M (2016) Placement of iliosacral screws using 3D image-guided (O-Arm) technology and stealth navigation: comparison with traditional fluoroscopy. Bone Joint J 98-B:696–702
Tjardes T, Shafizadeh S, Rixen D, Paffrath T, Bouillon B, Steinhausen ES, Baethis H (2010) Image-guided spine surgery: state of the art and future directions. Eur Spine J 19:25–45
Urbanski W, Jurasz W, Wolanczyk M, Kulej M, Morasiewicz P, Dragan SL et al (2018) Increased radiation but no benefits in pedicle screw accuracy with navigation versus a freehand technique in scoliosis surgery. Clin Orthop Relat Res. https://doi.org/10.1007/s11999.0000000000000204
Van de Kelft E, Costa F, Van der Planken D, Schils F (2012) A prospective multicenter registry on the accuracy of pedicle screw placement in the thoracic, lumbar, and sacral levels with the use of the O-arm imaging system and StealthStation navigation. Spine (Phila Pa 1976) 37:E1580–E1587
Villard J, Ryang YM, Demetriades AK, Reinke A, Behr M, Preuss A (2014) Radiation exposure to the surgeon and the patient during posterior lumbar spinal instrumentation: a prospective randomized comparison of navigated versus non-navigated freehand techniques. Spine (Phila Pa 1976) 39:1004–1009
Yakoumakis E, Tsalafoutas IA, Nikolaou D, Nazos I, Koulentianos E, Proukakis C (2001) Differences in effective dose estimation from dose-area product and entrance surface dose measurements in intravenous urography. Br J Radiol 74:727–734
Acknowledgements
All of the authors are sincerely grateful to Mr. Koji Yokoyama, Mr. Shohei Sasaki, Mr. Akihiko Kakimi, Mr. Toshiyo Norimasa, and Mr. Yoshinori Takao for their technical contribution to intraoperative image guidance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical approval and informed consent
The authors certify that all applicable institutional and governmental regulations concerning the ethical use of clinical data were adhered to for the present study. This retrospective outcome analysis of spine surgery was approved by the ethics committee of Osaka City University Graduate School of Medicine.
Rights and permissions
About this article
Cite this article
Bohoun, C.A., Naito, K., Yamagata, T. et al. Safety and accuracy of spinal instrumentation surgery in a hybrid operating room with an intraoperative cone-beam computed tomography. Neurosurg Rev 42, 417–426 (2019). https://doi.org/10.1007/s10143-018-0977-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-018-0977-6