Abstract
Inflammatory reactions play a key role in the cerebral injury after stroke or other ischemic brain diseases. Curcumin, which is extracted from herb turmeric, has been reported to have anti-inflammatory effects. The present study was aimed to investigate the anti-inflammatory effects of curcumin on oxygen-glucose deprivation (OGD) injured brain microvascular endothelial cells (BMECs). Rat BMECs were used and the results showed that OGD induced a significant elevation of the leakage of lactate dehydrogenase and the secretion of the proinflammation cytokine, IL-1β. Activation of p38, JNK MAPKs, and NF-κB in BMECs was also observed after OGD. The treatment of curcumin (20 μM) inhibited the increased production of IL-1β both at the protein and mRNA levels. The increased phosphorylation of p38 and JNK induced by OGD was decreased under the treatment of curcumin, whereas the p38 inhibitor, SB203580, significantly inhibited OGD-induced IL-1β production, but the JNK inhibitor, SP600125, failed to do so. These results suggest that the inhibition of IL-1β by curcumin may dependent on the p38 signaling pathway. The OGD-induced IL-1β production was also inhibited by the NF-κB inhibitor, and curcumin suppressed OGD-induced NF-κB activation. Furthermore, the NF-κB activation was attenuated by the SB203580, indicating that NF-κB activation was dependent on p38 signaling pathway. The present study suggests that curcumin displays an anti-inflammatory effect on OGD-injured BMECs via down-regulating of MAPK and NF-κB signaling pathways and might have therapeutic potential for the ischemic brain diseases.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Brain ischemia due to stroke affects a large population. Ischemic brain injury, as a secondary neuronal degenerative and inflammatory disease, can lead to the breakdown of the blood–brain barrier (BBB) and cause secondary damage to neurons. Brain microvascular endothelial cells (BMECs), as the main constituents of the BBB, play an essential role in maintaining normal blood flow within the brain. BMECs are also involved in the inflammatory reaction and cell apoptosis that may occur secondary to cerebral ischemia [1]. Besides the inflammatory damage to BMECs itself, BMECs also exacerbate the ischemic injury by affecting the survival of peripheral neurons and the activation of microglial cells [2, 3]. Therefore, protecting the BMECs and ameliorating their inflammatory reactions have been suggested to be the promising methods of alleviating brain damage. In recent years, searching for active ingredients which target multiple signaling molecules from natural medicines is considered to be the new trend in pharmaceutical development, as most of the currently available mono-targeted drugs are associated with numerous side effects.
Curcumin (7-bis (4-hydroxy-3-methoxyphenyl)-1,6-heptad iene-3,5-dione) is the major yellow pigment extracted from turmeric, which is isolated from the powdered dry rhizome of the herb Curcuma longa. Accumulating evidences have shown that curcumin possesses a wide range of properties including anti-inflammation, antioxidation, anticancer, antiparasite, and antimalaria [4]. Recent studies have demonstrated the neuroprotective effect of curcumin on cerebral ischemic injury in rodent animals [5–8]. In addition, in vitro studies have shown that curcumin protects cortical neurons exposed to oxygen and glucose deprivation (OGD) in an Akt/nuclear factor-erythroid 2-related factor two dependent pathway [8], protects BMECs against OGD-induced disruption of tight junction and barrier dysfunction via the heme oxygenase-1 pathway [9], and inhibits the adhesion of thrombin-activated platelets to BMECs [10].
However, little information is available regarding the effect of curcumin on inflammatory responses in the OGD challenged BMECs. Therefore, in the present study, we investigated the effects of curcumin on inflammatory molecules and signaling pathways in BMECs challenged by OGD.
Materials and methods
Cell culture and reagent
Rat BMECs were separated from male Sprague Dawley (SD) rats (provided by the Center of Experimental Animals at Tianjin Medical University) weighing 50–60 g as previously described [11] with minor modifications and cultured at 37 °C in a humidified atmosphere of 5 % CO2. The purity of the BMECs was more than 95 % based on factor VIII staining and 3–6 passages were achieved prior to the following experiments. All cell culture supplies, Dulbecco’s modified Eagle’s medium (DMEM) and fetal bovine serum were purchased from Invitrogen (Carlsbad, CA, USA); and all chemicals and reagents were purchased from Sigma-Aldrich (St. Louis, MO, USA), unless stated otherwise. Experiments were performed in accordance with the NIH guidelines and the approval of the ethics committee of Tianjin Medical University was obtained.
OGD and other treatments
Cells were divided into the following groups: control group, control + curcumin group, OGD group, OGD + curcumin group, and OGD + curcumin + inhibitor group. For the control group and control + curcumin group, BMECs were not exposed to OGD. For the OGD group, the original medium was removed, and then the cultures were rinsed with phosphate-buffered saline (PBS, 0.01 M, pH 7.4) twice, and exposed to DMEM (glucose free) and placed into a sealed anaerobic chamber flushed with 5 % CO2 and 95 % N2 (v/v) for the indicated time. Curcumin (at a final concentration of 20 μM), SB203580 (p38 inhibitor, 20 μM), SP600125 (JNK inhibitor, 25 μM), or pyrrolidine dithiocarbamate (PDTC, NF-κB inhibitor, 10 μM) was added at 30 min before OGD exposure, respectively.
Cell injury assay
The cell injury was determined by measuring lactate dehydrogenase (LDH) release in the culture medium using the LDH assay kit (Nanjing Jiancheng Bioengineering Institute, Jiangsu, China) according to the manufacturer’s instructions. In brief, an aliquot of the medium was mixed with nicotinamide adenine dinucleotide and lactate solution, and the LDH release was measured on the microplate reader at 450 nm.
Measurement of IL-1β secretion
The level of IL-1β secretion in culture media was determined by the ELISA kit (R&D System, Minneapolis, MN, USA) following the manufacturer’s instructions. Concentrations were calculated with reference to the standard curve.
Quantitative analysis of the IL-1β mRNA expression
Total RNA was extracted using Trizol reagent (Invitrogen). After reverse transcription, quantitative analysis of the IL-1β mRNA expression was performed with the real-time PCR method. The primers are as follows: for IL-1β, forward: 5′-ATGCCTCGTGCTGTCTGACC-3′, reverse: 5′-CCATCTTTAGGAAGACACGGGTT-3′; and for GAPDH, forward: 5′-ATGTGCCGGACCTTGGAAG-3′, reverse: 5′-CCTCGGGTTAGCTGAGAGATCA-3′. The mRNA level was quantified using the 2−∆∆CT method.
Western blots
BMECs were collected in lysis buffer (20 mM HEPES, pH 7.5, 150 mM NaCl, 1 mM EDTA, 1 mM EGTA, 1 % Triton X-100, 1 mM dithiothreitol (DTT), 1 mM β-glycerol-phosphate, 1 mM Na3VO4, 1 mM phenylsulfonyl fluoride (PMSF), and protease inhibitor cocktail), after centrifugation, total cellular protein in the supernatant was determined using the bicinchoninic acid (BCA) method. Equal amounts of protein (40 μg per lane) were separated on 12 % SDS-PAGE gels and electrically transferred to nitrocellulose membranes. The nitrocellulose membranes were blocked with 5 % nonfat dry milk, and then blots were incubated overnight at 4 °C with primary antibodies (rabbit anti-p-p38, anti-p38, anti-p-JNK, anti-JNK, anti-NF-κB p65, anti-p-IκB, or anti-β-actin antibody, 1:1,000, Cell Signaling Technology, Danvers, MA, USA). Next morning, the membranes were washed in PBS with Tween-20, incubated with horseradish-peroxidase-conjugated goat antirabbit second antibody and washed again. Signals were visualized by enhanced chemiluminescence. The intensity of each band was measured and analyzed with the Quantity One software (Bio-Rad, Hercules, CA, USA).
Statistical analysis
Each experiment was repeated at least three times, data were expressed as mean ± SEM and analyzed using statistical package SPSS13.0. Statistical analyses were carried out by one-way analysis of variance (ANOVA) followed by Tukey’s post hoc test. A value of P < 0.05 was considered statistically significant.
Results
Curcumin attenuated OGD-induced cell injury
To assess cell injury after OGD, the leakage of LDH into the medium was measured. The effect of curcumin on LDH release in the BMECs was more significant in the 20 and 100 μM groups than in the 5 μM group (Fig. 1a). Curcumin at the dose of 20 μM was administrated in the following experiments. In addition, the LDH release was increased time dependently after OGD (P < 0.05 vs. control, Fig. 1b). As shown in Fig. 1c, the activity of LDH was significantly reduced after curcumin treatment (P < 0.05 vs. OGD). These results have shown that curcumin could attenuate the injury of the BMECs induced by OGD.
Effects of OGD and curcumin on cell injury in BMECs. Cell injury was measured by lactate dehydrogenase release assay. Curcumin at indicated concentrations was applied to BMECs 30 min prior to OGD for 6 h (a). Cell injury was determined at different time points after OGD (b), *P < 0.05 vs. control. OGD-induced cell injury was ameliorated by curcumin (c), *P < 0.05 vs. control group, # P < 0.05 vs. OGD group
Curcumin reduced IL-1β level in BMECs
After 6 h exposure to the OGD, the concentration of IL-1β in the culture medium was significantly elevated as compared to the control group (P < 0.05). As shown in Fig. 2a, under the treatment of 20 μM curcumin, OGD-induced IL-1β secretion was remarkably inhibited (P < 0.05 vs. OGD), whereas curcumin did not influence the IL-1β level in normally cultured BMECs (P > 0.05 vs. control); moreover, pretreating with p38 inhibitor SB203580 or the NF-κB inhibitor PDTC inhibited the OGD induced increase in IL-1β level (P < 0.05 vs. OGD), whereas the JNK inhibitor SP600125 failed to do so (P > 0.05 vs. OGD). For IL-1β mRNA expression, a significant decline in IL-1β level was induced by 20 μM curcumin when compared with the OGD group (P < 0.05, Fig. 2b).
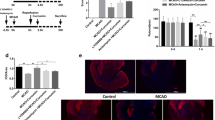
Effects of OGD, curcumin and various signaling pathway inhibitors on secretion of IL-1β in BMECs. IL-1β protein levels in the culture media of BMECs exposed to OGD and not, with or without curcumin, p38 inhibitor (SB203580, 20 μM), JNK inhibitor (SP600125, 25 μM) or NF-κB inhibitor (PDTC, 10 μM) for 6 h were analyzed by ELISA (a). Effects of OGD and curcumin on IL-1β mRNA expression in BMECs were determined by real-time PCR. *P < 0.05 vs. control group, # P < 0.05 vs. OGD group
Curcumin suppressed OGD-induced phosphorylation of p38 and JNK MAP kinases
Protein expressions of key molecules in intracellular MAPK signaling pathways, p-p38 and p-JNK were investigated by Western blots. The results showed that expressions of p-p38 and p-JNK were up-regulated in the OGD group significantly (P < 0.05 vs. control), whereas treatment with curcumin could suppress the expressions of p-p38 and p-JNK significantly when compared with the OGD group (P < 0.05, Fig. 3).
Effects of OGD and curcumin on phosphorylation of p38 and JNK in BMECs. Expressions of p-p38, p38, p-JNK, and JNK were detected by western blots. Immunostaining of p38 and JNK served as respective controls (a). Bar graph represents semi-quantitative densitometry from Western blot analysis (b). *P < 0.05 vs. control group, # P < 0.05 vs. OGD group
Curcumin suppressed OGD-induced NF-κB activation via inhibition of p38 phosphorylation
The activity of the molecules in the NF-κB signaling pathway was determined by measurement of the NF-κB p65 and p-IκB proteins in the cellular extraction of the BMECs. The expressions of NF-κB p65 and p-IκB were increased significantly in the OGD group (P < 0.05 vs. control); treatment with curcumin inhibited the OGD-induced increase of NF-κB p65 and p-IκB significantly (P < 0.05 vs. OGD); furthermore, pretreatment with p38 inhibitor SB203580 attenuated the increase of NF-κB p65 and p-IκB remarkably (P < 0.05 vs. OGD) (Fig. 4).
Effects of OGD, curcumin and p38 inhibitor on phosphorylation of proteins in intracellular NF-κB signaling pathway. Expressions of NF-κB p65 and p-IκB were detected by western blots, and β-actin was used as a control (a). Bar graph represents semi-quantitative densitometry from Western blot analysis (b). *P < 0.05 vs. control group, # P < 0.05 vs. OGD group
Discussion
Previous studies have demonstrated that curcumin has a neuroprotective effect on cerebral ischemic models in vitro and in vivo [5–7, 9]. However, the effects of curcumin on BMECs in terms of inflammation have not yet been described. Curcumin is known to exert its anti-inflammatory activity in various cell lines [12–16]. Consistently, the results of the present study indicate that curcumin may have anti-inflammatory effects on OGD-injured BMECs via inhibition of MAPK, and NF-κB pathways in the setting of stroke and ischemic cerebrovascular diseases.
BMECs, the essential cells that contribute to the function of the BBB, are important responsive and regulatory components of cerebral inflammation induced by OGD and have also been proved to generate inflammatory cytokines, such as TNF-α and IL-1β, which have been demonstrated to mediate ischemic cerebral injury [17, 18]. In the present study, we investigated the effects of curcumin against ischemia-like injury in the BMECs. The results showed that curcumin significantly ameliorated the LDH release after OGD, indicating its protective effects on the ischemia. The effect of curcumin on the secretion of key inflammatory cytokine IL-1β was then investigated, and the results showed that the increased protein and mRNA levels of IL-1β induced by OGD were significantly decreased after the treatment of curcumin.
Accumulated data suggest that MAPKs signaling pathways positively regulate the production of inflammatory molecules [19]. The MAPKs have been shown to be up-regulated after cerebra ischemia [20, 21], and recent studies have revealed that inhibition of p38 and/or JNK MAPK pathways can improve the outcome of ischemic brain injury by improving neural cell survival directly or indirectly, including the inhibition of inflammatory cytokines [22–26]. In this study, increased activation of p38 and JNK was observed in BMECs after OGD, and the curcumin treatment significantly decreased their activation. Meanwhile, p38 MAPK inhibitor was able to decrease IL-1β secretion in BMECs induced by OGD, whereas JNK inhibitor failed to do so. These results indicate that the inhibition of p38 MAPK signaling pathway is one of the mechanisms that underlying curcumin’s inhibitory effect on the inflammatory cytokines.
In resting states, NF-κB, is primarily located in the cytoplasm and bound to inhibitors of κB (IκB), while under simulation, NF-κB translocates to the nucleus and regulates the transcription of genes, including those coding for the inflammatory molecules [27]. Previous reports showed that NF-κB was activated in cerebral ischemia, and curcumin was also able to inhibit inflammatory processes through the NF-κB signaling pathway [28]. The results from the present study showed that NF-κB specific inhibitor PDTC significantly prohibited the OGD-induced IL-1β elevation, which suggests that OGD-induced IL-1β increase may dependent on the NF-κB signaling pathway. Furthermore, NF-κB activation was significantly increased in OGD-induced BMECs as evidenced by increased expression of NF-κB p65 and p-IκB, whereas curcumin treatment inhibited the activation of NF-κB after OGD significantly. These results indicate that the inhibitory effect of curcumin on the OGD-induced IL-1β elevation is also dependent on the NF-κB activation. Moreover, p38 inhibitor attenuated the NF-κB activation after OGD significantly, which suggests that OGD-induced NF-κB activation may dependent on p38 activation and this result is in consistent with previous studies conducted in other cell lines under different stimuli [28–31].
In conclusion, curcumin may protect BMECs injury induced by OGD via anti-inflammation through the inhibition of MAPK and NF-кB signaling pathways. Curcumin may serve as a promising anti-inflammatory agent and therefore be a candidate for the treatment of cerebral ischemic diseases.
References
Danton GH, Dietrich WD (2003) Inflammatory mechanisms after ischemia and stroke. J Neuropathol Exp Neurol 62:127–136
Li W, Li P, Hua Q et al (2009) The impact of paracrine signaling in brain microvascular endothelial cells on the survival of neurons. Brain Res 1:28–38
Wang J, Li PT, Du H et al (2011) Impact of paracrine signals from brain microvascular endothelial cells on microglial proliferation and migration. Brain Res Bull 86:53–59
Gupta SC, Patchva S, Koh W et al (2012) Discovery of curcumin, a component of golden spice, and its miraculous biological activities. Clin Exp Pharmacol Physiol 39:283–299
Wang Q, Sun AY, Simonyi A et al (2005) Neuroprotective mechanisms of curcumin against cerebral ischemia-induced neuronal apoptosis and behavioral deficits. J Neurosci Res 82:138–148
Jiang J, Wang W, Sun YJ et al (2007) Neuroprotective effect of curcumin on focal cerebral ischemic rats by preventing blood–brain barrier damage. Eur J Pharmacol 561:54–62
Zhao J, Yu S, Zheng W et al (2010) Curcumin improves outcomes and attenuates focal cerebral ischemic injury via antiapoptotic mechanisms in rats. Neurochem Res 35:374–379
Wu J, Li Q, Wang X et al (2013) Neuroprotection by curcumin in ischemic brain injury involves the akt/nrf2 pathway. PLoS One 8:e59843
Wang YF, Gu YT, Qin GH et al (2013) Curcumin ameliorates the permeability of the blood–brain barrier during hypoxia by upregulating heme oxygenase-1 expression in brain microvascular endothelial cells. J Mol Neurosci 51:344–351
Zhang L, Zq LIANG (2008) Effect of curcumin on the adhesion of platelets to brain microvascular endothelial cells in vitro. Acta Pharmacol Sin 29:800–807
Perriere N, Demeuse P, Garcia E et al (2005) Puromycin-based purification of rat brain capillary endothelial cell cultures. Effect on the expression of blood–brain barrier-specific properties. J Neurochem 93:279–289
Chen D, Nie M, Fan M-w et al (2008) Anti-inflammatory activity of curcumin in macrophages stimulated by lipopolysaccharides from Porphyromonas gingivalis. Pharmacology 82:264–269
Abe Y, Hashimoto S, HORIE T (1999) Curcumin inhibition of inflammatory cytokine production by human peripheral blood monocytes and alveolar macrophages. Pharmacol Res 39:41–47
Wang S-L, Li Y, Wen Y et al (2009) Curcumin, a potential inhibitor of up-regulation of TNF-alpha and IL-6 induced by palmitate in 3T3-L1 adipocytes through NF-kappaB and JNK pathway. Biomed Environ Sci 22:32–39
Ranjan D, Chen C, Johnston TD et al (2004) Curcumin inhibits mitogen stimulated lymphocyte proliferation, NFkappaB activation, and IL-2 signaling. J Surg Res 121:171–177
Cohen AN, Veena MS, Srivatsan ES et al (2009) Suppression of interleukin 6 and 8 production in head and neck cancer cells with curcumin via inhibition of Ikappa beta kinase. Arch Otolaryngol Head Neck Surg 135:190–197
Stanimirovic D, Satoh K (2000) Inflammatory mediators of cerebral endothelium: a role in ischemic brain inflammation. Brain Pathol 10:113–126
Feuerstein GZ, Wang X, Barone FC (1998) The role of cytokines in the neuropathology of stroke and neurotrauma. NeuroImmunomodulation 5:143–159
Maddahi A, Edvinsson L (2010) Cerebral ischemia induces microvascular pro-inflammatory cytokine expression via the MEK/ERK pathway. J Neuroinflammation 7:14
Irving EA, Barone FC, Reith AD et al (2000) Differential activation of MAPK/ERK and p38/SAPK in neurones and glia following focal cerebral ischaemia in the rat. Mol Brain Res 77:65–75
Hayashi T, K-i Sakai, Sasaki C et al (2000) c-Jun N-terminal kinase (JNK) and JNK interacting protein response in rat brain after transient middle cerebral artery occlusion. Neurosci Lett 284:195–199
Irving EA, Bamford M (2002) Role of mitogen-and stress-activated kinases in ischemic injury. J Cereb Blood Flow Metab 22:631–647
Okami N, Narasimhan P, Yoshioka H et al (2012) Prevention of JNK phosphorylation as a mechanism for rosiglitazone in neuroprotection after transient cerebral ischemia: activation of dual specificity phosphatase. J Cereb Blood Flow Metab 33:106–114
Wallace BK, Jelks KA, O’Donnell ME (2012) Ischemia-induced stimulation of cerebral microvascular endothelial cell Na-K-Cl cotransport involves p38 and JNK MAP kinases. Am J Physiol Cell Physiol 302:C505–C517
Li J, Li Y, Ogle M et al (2010) dl-3-n-Butylphthalide prevents neuronal cell death after focal cerebral ischemia in mice via the JNK pathway. Brain Res 1359:216–226
Benakis C, Bonny C, Hirt L (2010) JNK inhibition and inflammation after cerebral ischemia. Brain Behav Immun 24:800–811
Dogra C, Changotra H, Mohan S et al (2006) Tumor necrosis factor-like weak inducer of apoptosis inhibits skeletal myogenesis through sustained activation of nuclear factor-kappaB and degradation of MyoD protein. J Biol Chem 281:10327–10336
Nonn L, Duong D, Peehl DM (2007) Chemopreventive anti-inflammatory activities of curcumin and other phytochemicals mediated by MAP kinase phosphatase-5 in prostate cells. Carcinogenesis 28:1188–1196
Craig R, Larkin A, Mingo AM et al (2000) p38 MAPK and NF-kappa B collaborate to induce interleukin-6 gene expression and release. Evidence for a cytoprotective autocrine signaling pathway in a cardiac myocyte model system. J Biol Chem 275:23814–23824
Carter AB, Knudtson KL, Monick MM et al (1999) The p38 mitogen-activated protein kinase is required for NF-κB-dependent gene expression. The role of tata-binding protein (TBP). J Biol Chem 274:30858–30863
Berghe WV, Plaisance S, Boone E et al (1998) p38 and extracellular signal-regulated kinase mitogen-activated protein kinase pathways are required for nuclear factor-κB p65 transactivation mediated by tumor necrosis factor. J Biol Chem 273:3285–3290
Acknowledgments
This work was supported by the team of Scientific Research Innovation Foundation of Logistics University of Chinese People’s Armed Police Force (No.: WHTD201308-2). Curcumin attenuates ischemia-like injury induced IL-1β elevation in BMEC via inhibiting MAPK pathways and nuclear factor-κB activation.
Author information
Authors and Affiliations
Corresponding authors
Additional information
Hua-jiang Dong, Chong-zhi Shang and Ding-wei Peng contributed equally to this work (co-first authors).
Li Zhan and Peng Wang are co-corresponding authors.
Rights and permissions
About this article
Cite this article
Dong, Hj., Shang, Cz., Peng, Dw. et al. Curcumin attenuates ischemia-like injury induced IL-1β elevation in brain microvascular endothelial cells via inhibiting MAPK pathways and nuclear factor-κB activation. Neurol Sci 35, 1387–1392 (2014). https://doi.org/10.1007/s10072-014-1718-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-014-1718-4