Abstract
Introduction/objectives
Musculoskeletal ultrasound (MSUS) has been extensively studied by rheumatologists in Europe and the Americas, but less is known about MSUS use in Asia. Our hypothesis is that MSUS use is less prevalent in China as compared with its Western counterparts. This study reports the most up-to-date recommendations for MSUS use in rheumatology globally and is also the first study to characterize the current practices, training, and perceptions regarding MSUS of rheumatologists in China.
Method
A 43-question survey was designed and distributed via mobile application to members of the Chinese Rheumatology Association, primarily to investigate the current prevalence and utilization of MSUS in China. Statistical analyses included the use of chi-square tests and independent-samples t tests, with p values less than 0.05 considered statistically significant.
Results
The results showed low rates of MSUS training (129/528, 24%) and current MSUS use (89/524, 17%) in China. However, there was a high level of interest in learning MSUS, especially among younger respondents. Lack of access to training programs and user variability in skill were seen as significant barriers to the uptake of MSUS.
Conclusions
Despite low rates of MSUS training and utilization, the vast majority of respondents believe that MSUS should become a standard clinical tool in rheumatology, and there was great interest in undergoing training. Importantly, lack of access to MSUS training programs and user variability in skill were seen as significant obstacles to the more widespread use of MSUS, which suggests a need for more standardized, high-quality MSUS training in China.
Key Points • A low percentage of Chinese rheumatologists (17%) currently use MSUS. • Chinese rheumatologists expressed a high level of interest in obtaining MSUS training. • The greatest perceived obstacle to more widespread MSUS use is the lack of training programs. |
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The field of rheumatology focuses on the management of autoimmune and musculoskeletal disorders, which collectively represent the second most common cause of disability globally and contribute the second largest burden in terms of years lived with disability [1,2,3]. Furthermore, the prevalence of musculoskeletal disorders has been estimated to have increased by 45% from 1990 to 2010 due to aging populations worldwide and is expected to continue to rise [2].
Musculoskeletal ultrasound (MSUS) was first reported to be clinically used in rheumatology in 1972 [4] and has since been used in the assessment of several rheumatic and musculoskeletal diseases. Improvements in technology, increased access to portable or laptop-sized ultrasound equipment, and improved resolution of images have led to the growing adoption of point-of-care MSUS use among rheumatologists and other musculoskeletal providers in Europe and the Americas. Notably, in the USA, the growth of MSUS use is reflected by a greater than 4-fold increase in number of Medicare-reimbursed MSUS examinations from 56,254 in 2000 to 233,964 in 2009 [5]. The diagnostic advantages of MSUS in providing information on inflammation affecting synovial, tendon, and bony changes in static and dynamic views, along with its benefits of lower cost, lack of radiation, and ability to be performed and clinically interpreted at the bedside or clinic/office, have made MSUS an attractive imaging modality. Well-validated studies have shown the value of MSUS as an effective imaging modality for rheumatologists evaluating musculoskeletal disorders [6,7,8].
There has also been a growing body of literature investigating the uptake of MSUS use in rheumatology [9,10,11,12,13,14,15,16,17,18,19]. Studies have shown MSUS to be useful in guiding diagnostic and therapeutic procedures, leading to improved accuracy of interventions such as joint injection and aspiration [20, 21]. There is also evidence that MSUS is more sensitive than clinical examination on detecting pathology in joints [20, 22] and impacts subsequent patient management [23]. The integration of MSUS into rheumatology has been most extensively studied in European countries such as the UK, Germany, and Italy where organizations like the European League Against Rheumatism (EULAR) and the British Society of Rheumatology offer MSUS training courses. There is also increasing data regarding MSUS use in other Western countries, including the USA and Canada [14,15,16, 24, 25]. Older studies have highlighted barriers to the increased use of MSUS, notably a need for greater access to training opportunities and more uniform training curricula [10, 13, 16, 17, 26].
Several studies have also focused on the development of a more standardized framework for performing and teaching MSUS [24, 27,28,29,30]. MSUS educational curricula, guidelines for MSUS use in rheumatology, and continuing medical education courses have now been developed in both Europe and the Americas through organized efforts from the Pan-American League of Associations for Rheumatology (PANLAR) [30], EULAR and Outcome Measures in Rheumatology (OMERACT) [28, 31], the American College of Rheumatology (ACR) [24, 32, 33], and the Ultrasound School of North American Rheumatologists (USSONAR) [34]. The ACR has issued a position statement on MSUS being a “useful tool used by rheumatologists in the diagnosis, management, and treatment of rheumatic conditions” and provides an individual certification pathway (RhMSUS) for rheumatologists who have received adequate training in MSUS [32, 35].
The diagnoses of rheumatic and musculoskeletal disorders have also been impacted by MSUS. The classification criteria for polymyalgia rheumatica now includes shoulder and hip ultrasonography, increasing the sensitivity and specificity of the diagnostic criteria [21, 36]. Similarly, the classification criteria for gout also includes ultrasound as an imaging modality with utility in identifying urate deposition in joints [37]. For rheumatoid arthritis, ultrasound has been found to be more sensitive for detecting disease activity than clinical examination and ultrasound guidelines for scoring synovitis in rheumatoid arthritis have been developed [38, 39]. EULAR has also published recommendations for the use of imaging in large vessel vasculitis and cites that ultrasound should be the primary imaging choice for evaluation of predominantly cranial symptoms of giant cell arteritis [40]. These recommendations for the use of MSUS in rheumatology practice demonstrate the continued potential for ultrasound technology to directly benefit patient care.
Information regarding MSUS use in other world regions, including Asia, is more limited. Current knowledge regarding MSUS use in Asia comes from studies by Takase et al. [41] and Hama et al. [42] in Japan as well as Kang, Wakefield, and Emery [43] in Korea. These studies showed similar barriers to the greater use of MSUS in routine practice that their Western counterparts initially faced, including lack of access to MSUS training, need for more standardized training, and lack of time to perform studies. However, little is known about MSUS use in other Asian countries, specifically China.
Rheumatology is a relatively new specialty in China with the first rheumatology departments established in the late 1970s. Since then, studies done by the Chinese Rheumatology Association (CRA) have shown the wide prevalence of rheumatic disease in China with as many as 20 million patients living with rheumatic diseases [44]. As the burden of these conditions is increasingly recognized, research on MSUS and its clinical applications in China has been vigorously developed and the presence of MSUS in China has increased. However, due to its late start and weak foundation, MSUS training and promotion of its use lags behind those of other countries and data about the uptake of MSUS in clinical practice by rheumatologists is sparse.
This study aims to determine the current level of MSUS use among rheumatologists in China, knowledge of MSUS, and attitudes towards adoption of MSUS in a country, which encompasses a wide range of socioeconomic and geographic settings with variable access to medical resources and training opportunities. This data will in turn be used to identify current barriers to broader MSUS use in China and potentially inform future strategies to increase MSUS use among rheumatologists.
Materials and methods
Study design
A cross-sectional survey questionnaire was designed and distributed via mobile application during two separate rounds of survey collection with the first round in July 2016 and the second round in November 2016.
This study was exempt from IRB review by the Yale Human Investigation Committee and Peking Union Medical College Hospital IRB prior to study initiation.
Study population
The survey was distributed to 2164 individuals registered with the CRA in China. This sample population included current members of the CRA, which consisted of mostly rheumatologists as well as a minority of providers from other specialties. Inclusion criteria included surveys that were more than 50% complete and surveys that were repeated responses from the first round were excluded.
Statement of human and animal rights
This study did not involve any experiments on human or animal subjects.
Measures
An initial recruitment email was sent to individuals registered with the CRA that invited recipients to participate in the survey study while providing the aim and objectives of the survey, projected survey completion time, statements of voluntary participation and confidentiality of responses, and contact information for the study investigators. An optional section at the end of the survey allowed respondents to provide identifying information if desired for further contact regarding future studies related to MSUS. For anonymization purposes, this information was separated from the rest of the survey responses prior to data review.
The survey comprised of 43 close-ended multiple-choice questions (see Appendix A) that were subdivided into four content areas of practitioner demographics, MSUS training, current MSUS use, and attitudes towards MSUS. As applicable, additional space was provided after appropriate questions for additional comments and/or further clarification of responses. The original survey was written in English and afterwards translated into Chinese by a native Chinese speaker (see Appendix B). It was subsequently piloted by six bilingual study investigators (two native English– and four native Chinese–speaking medical students and physicians) to ensure both comprehensibility and fidelity of content. To facilitate distribution of the survey and aggregation of responses, the survey was adapted to an electronic survey on a mobile application called Fengyun Zhu Shou (风云助手). This electronic data collection platform is designed for and supported by the Chinese Rheumatology Data Center (CRDC), and it was originally used by the CRDC for their national clinical registries and related research projects. The electronic version of the questionnaire was then reviewed and further piloted by approximately 25 rheumatologists at Peking Union Medical College Hospital. Additional feedback regarding the survey questions and ease of use of the mobile platform from pilot testing were incorporated into the final version of the online survey.
Statistical analysis
Statistical analyses were performed using SPSS Statistics Version 24 (IBM Corporation, Armonk, New York, USA) utilizing both descriptive and comparative statistical tests including the Pearson’s chi-square independence test for categorical variables, the z-test for proportions, and the independent-samples t test. Subgroup analyses were also performed by the aforementioned statistical analyses and Fisher’s exact test was utilized for small sample sizes. For all analyses, p values less than 0.05 were considered statistically significant.
Results
Practitioner demographics
Of the total surveyed population, the response rate was 25% (532/2164). Of 532 survey respondents, 70% were female and 70% were ≤ 40 years old (range: 22–63 years) (Table 1). The types of hospitals represented by the surveyed population included public hospitals (88%) and other types of hospitals (12%) such as private, military, pediatric, and traditional Chinese medicine hospitals. The majority of respondents practiced at 3rd tier public hospitals (77%), which are the largest hospitals in China and also provide the most comprehensive health services.
Initial exposure to MSUS
The most common way that respondents first heard about MSUS was during scientific conferences, while the least common was during residency training or medical school. When stratified by academic position, scientific conferences remained the most common method by which respondents first heard about MSUS across all groups. However, the proportion who first heard about MSUS through scientific articles or conferences decreased from 90% of senior level physicians and 84% of attendings to only 73% of residents (p = 0.002). Conversely, the proportion of respondents who first heard about MSUS through medical school or residency increased from only 16% of senior level physicians and 17% of attendings to 30% of residents (p = 0.009).
MSUS training
A majority of individuals had never received any MSUS training (76%) (Fig. 1a). As academic position rank became more senior, a greater proportion of respondents within each group reported they had received MSUS training (20% of residents, 23% of attendings, and 32% of senior level physicians, p = 0.007).
No difference in prevalence of MSUS training (23% of men and 25% of women, p = 0.684) or amount of MSUS training received (p = 0.816) was observed between sexes.
Only 11% of survey respondents reported that their institutions offered MSUS training and, of that proportion, 77% offered MSUS training to rheumatologists. However, MSUS training for rheumatologists has only been available for < 5 years at a majority of institutions that offered it. The most common reported teaching method used in MSUS training was lecture-based teaching.
Current personal use of MSUS
Most respondents reported that they did not personally use MSUS in their practices (83%) (Fig. 1b). Even among participants who had received MSUS training, only 50% reported personally using MSUS in practice.
In stratifying all respondents by academic rank, 12% of residents, 18% of attendings, and 20% of senior level physicians reported personally using MSUS in daily practice, although this difference did not reach a statistically significant level (p = 0.235). When considering only respondents who had received MSUS training, 57% of residents, 55% of attendings, and 44% of senior level positions reported personally using MSUS, although this difference also did not reach a statistically significant level (p = 0.460). No difference was found in terms of percentage of male and female respondents who personally use MSUS in their practices and how long they had been using MSUS.
Current institutional use of MSUS
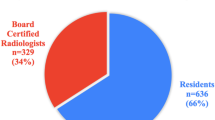
It was found that 62% respondents worked at institutions where MSUS is used by medical providers. However, rheumatologists used MSUS at only 51% of these institutions, while the most common medical providers using MSUS were radiologists at 69%. Only 0–25% of rheumatologists were trained to use MSUS at 75% of institutions where it is used.
MSUS was more widely used by respondents for the purpose of diagnosing inflammatory disease (94%) than for guiding aspiration or injection procedures (68%) or other purposes (8%), including monitoring of disease progression, monitoring for post-treatment effect, and research.
Only 41% reported that MSUS machines were easily accessible for rheumatologists to use at their institutions. All respondents reported having access to at least one other type of musculoskeletal diagnostic imaging tool other than ultrasound, including MRI (96%), CT (93%), X-ray (92%), and bone scan (75%).
Attitudes towards MSUS
General perceptions of MSUS use in rheumatology
Ninety-one percent of respondents believe that MSUS is currently a standard clinical tool in rheumatology and 99% of respondents feel that MSUS should become a standard clinical tool in rheumatology. Ninety-one percent of respondents also felt that either both rheumatologists and radiologists or rheumatologists only should be performing MSUS exams.
A greater proportion of participants who had received MSUS training reported that MSUS is currently a standard clinical tool in rheumatology (95%) as compared with those participants who had not received MSUS training (90%) (p = 0.044). However, regardless of personal history of exposure to MSUS training, an overwhelming majority of respondents from both groups indicated that MSUS should become a standard clinical tool (98% MSUS trained respondents and 99% non-MSUS trained respondents, p = 0.686).
Overall, 81% believed that MSUS is either needed or extremely needed in rheumatology in China.
A majority of respondents (84%) were interested in MSUS training, with the most interest in learning MSUS through hands-on teaching methods (Fig. 2). The younger the age groups were, the more interest there was in learning MSUS with 90% 20–30 year olds, 86% 31–40 year olds, 81% 41–50 year olds, and 67% > 50 year olds interested (p = 0.015).
Perceived benefits of MSUS
The most important benefits of MSUS over other imaging modalities were its greater safety and applicability to a wide range of clinical situations (Fig. 3a). Across all age and academic groups, these two aspects were also felt to be the most important potential benefits of MSUS. However, in the youngest age group and most junior academic position group, the improved diagnostic accuracy of MSUS was found to be the third most important benefit, while it was viewed as the least important benefit in all other groups.
Perceived drawbacks and barriers to the use of MSUS
The most important potential drawback to MSUS was user variability in skill (Fig. 3b). Crucial barriers to the more routine use of MSUS in daily practice were seen to be lack of access to MSUS training and lack of general awareness regarding MSUS (Fig. 3c).
When stratified based on whether respondents had received MSUS training or not, lack of access to training programs and lack of scientific evidence demonstrating benefits of MSUS over other imaging modalities were viewed as more important potential barriers by those who had not received training than those who had. Fifty-seven percent MSUS-trained respondents and 71% non-MSUS-trained respondents viewed lack of access to training programs to be an important barrier (p = 0.012), while 34% MSUS-trained respondents and 49% non-MSUS-trained respondents viewed lack of scientific evidence supporting benefits of MSUS over other imaging modalities to be an important barrier (p = <0.001).
Discussion
Growing evidence of the advantages of MSUS in clinical settings in rheumatology and adoption of its recommended use in rheumatology guidelines in Europe and the Americas have led to increased interest in this imaging modality. While the uptake and use of MSUS has been studied in Europe and the Americas, there are relatively few studies exploring MSUS use in Asia (e.g. Japan and South Korea) and little is known about MSUS in China. This study is the first to provide an in-depth examination of the current training, practices, and perceptions regarding MSUS among rheumatologists in China.
Our survey revealed a low prevalence of MSUS use by rheumatologists with only 17% of participants personally using MSUS in their practices. In comparison, MSUS use in similar European surveys ranges from 33 to 41%, indicating a gap in utilization of MSUS in rheumatology in China [9, 12, 17]. However, other non-European countries have also reported similarly low percentages of surveyed rheumatologists who personally use MSUS [14, 16]. When compared with other countries in Asia, our result is similar to the proportion of surveyed rheumatologists in Japan who personally use MSUS (20%) [42]. However, Kang et al. reported a greater uptake of MSUS use by rheumatologists in Korea, with 61% of their respondents using MSUS [43]. Part of the difference in MSUS utilization may be due to the low proportion of respondents who had received MSUS training (24%), whereas, for example, an aforementioned study by Tamas et al. reported that 54% of respondents had received training in MSUS in Romania [17]. The high level of interest in learning MSUS and the perceived importance of lack of access to MSUS training programs reflect a crucial need for greater access to MSUS training opportunities in China.
Another barrier to the more widespread use of ultrasound by clinicians is a lack of general awareness about MSUS. This is highlighted by the minimal exposure to MSUS that respondents reported during medical school and residency training. Encouragingly, coinciding with the increased interest in MSUS over recent decades, our data did indicate that more junior level physicians had greater exposure to MSUS during medical school and residency as compared with their predecessors. In addition, although the overall percentage of respondents who received MSUS training was lesser among younger practitioners, a greater proportion of younger MSUS-trained practitioners reported using MSUS in their daily practices as compared with older MSUS-trained practitioners. This suggests that the presence of MSUS has been growing in China over recent years, although great potential remains for further incorporation of MSUS into clinical rheumatology practice.
In addition to the need for greater awareness of and access to MSUS training opportunities in China, rheumatology training programs would also benefit significantly from following a standardized curriculum, similar to those proposed by other national organizations [27,28,29,30, 33]. Our study revealed important insights into the major perceived drawbacks of MSUS and only one potential drawback was perceived to be significantly more important than others, which was the user variability in skill associated with ultrasound technology. This limitation of MSUS is similarly reflected in a study by Samuels et al., which showed that the most commonly cited potential downside of MSUS was operator and reader variability as compared with other imaging modalities [14]. As a result, this common concern specifically emphasizes the need for increasing access to more formal and standardized MSUS training programs and longitudinal MSUS mentorship.
In terms of MSUS training, the current most common teaching method is lecture-based training. However, survey respondents actually reported the most interest in learning MSUS through hands-on teaching methods. Lecture-based training may not be the optimal teaching method to provide exposure to the hands-on skills and techniques required to become proficient with using MSUS. The increased promotion of hands-on workshops during which providers can personally practice using MSUS to ensure a higher level of standardization of user skill levels may help to address this issue. Interest in hands-on learning is in keeping with results from other studies, which concluded that personal mentoring is the most preferred educational tool [12, 17]. Furthermore, proposed guidelines for MSUS training curricula have also emphasized practical learning over theoretical learning—for example, EULAR proposed a training program that consists of at least 50% practical skills training instead of being solely theory-based through lectures [28] and PANLAR recommended a training program consisting of 60–70% hands-on sessions [30]. The Belfast MSUS course also utilized a hands-on curriculum that successfully led trainees to achieve basic competency in MSUS [29].
A more systems-level obstacle that may need to be overcome to increase utilization of MSUS by rheumatologists is the organizational structure of how ultrasonography is practiced in China. Many hospitals in China have dedicated ultrasound departments with specialists who perform all ultrasound examinations in place of other clinicians. As MSUS examinations have traditionally been performed by ultrasound specialists and radiologists, it may be difficult to shift the paradigm to training rheumatologists to use MSUS as well. In fact, this survey showed that radiologists are the most commonly reported medical providers using MSUS. In addition, even at the few institutions where MSUS training was offered, it was often not available to rheumatologists or had just recently started being available to rheumatologists within the last 5 years. This indicates that the use of MSUS by rheumatologists is still quite a new practice in China. Overall, based on the low proportions of respondents reporting that their institutions offer MSUS training and the limited ability of rheumatologists to access MSUS machines within their institutions, it is suggested that further improvements could potentially be made to institutional infrastructure to allow practitioners to gain MSUS training more easily and to subsequently practice these skills. A significant proportion of respondents also reported that they did not know whether or not their institutions offered MSUS training or certification. Thus, further analysis can be done to investigate how many institutions do indeed offer MSUS training or certification. This could help illuminate whether the core issue is that practitioners are largely unaware of these training programs or whether institutions have not yet incorporated MSUS training into their educational programs as is standard in several European medical training programs.
Finally, practitioners who were categorized into the youngest age group (20–30 years) and more junior academic positions (residents) were more likely to view the improved diagnostic accuracy of MSUS as an important benefit over other imaging modalities. This likely reflects growth in the body of scientific evidence supporting MSUS as a validated diagnostic imaging modality in rheumatology over the years and increasing acceptance of MSUS use in the evaluation, diagnosis, and treatment of rheumatologic disorders.
Limitations of this study include potential for sampling bias, with those completing the survey possibly having greater interest in or awareness of MSUS than non-respondents. The distribution of the survey through an electronic application could also have possibly limited the participation of older physicians who are less likely to use mobile applications and practitioners in more resource-limited settings, which could have contributed to the survey response rate of 25%. Despite this, we collected over 500 surveys and included practitioners from the vast majority of geographic regions in China, which we feel provides us with reasonable insight into the uptake of MSUS across China. In addition, based on overall demographics of the survey respondents, there may be an overrepresentation of the experiences and opinions of young physicians and female physicians. However, a 2007 survey of rheumatology practitioners by the CRA showed that a majority of the overall workforce was female and 80% were ≤ 45 years old [45]. Thus, our results may reasonably reflect the demographics of rheumatologists in China. There may also be a skew towards the opinions of practitioners in 3rd tier public hospitals. However, given that rheumatology is still a relatively new field in China, the vast majority of rheumatology departments exist in 3rd tier hospitals and are comparatively uncommon in 1st and 2nd tier hospitals.
Conclusions
In this inaugural study of MSUS use among rheumatologists in China, it was found that despite low rates of MSUS training and current MSUS utilization, the vast majority of respondents believe that MSUS is needed in rheumatology practice and should become a standard clinical tool in rheumatology. MSUS was viewed as having several significantly important benefits, including greater safety profile and applicability to a wide range of clinical situations, over other imaging modalities that have been considered the gold standard in rheumatology. Furthermore, the majority of practitioners, especially younger practitioners, would be interested in receiving MSUS training through teaching methods like hands-on workshops. Importantly, lack of access to MSUS training programs and user variability in skill were seen as significant obstacles to the more widespread use of MSUS, which suggests a need for more standardized, high-quality MSUS training in China.
Data availability
The original English language survey and translated Chinese language survey used in the current study are available as supplementary resources.
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Global Burden of Disease Study (2016) DALYs and HALE Collaborators (2017) Global, regional, and national disability-adjusted life-years (DALYs) for 333 diseases and injuries and healthy life expectancy (HALE) for 195 countries and territories, 1990–2016: a systematic analysis for the Global Burden of Disease study 2016. Lancet 390:1260–1344
Storheim K, Zwart JA (2014) Musculoskeletal disorders and the global burden of disease study. Ann Rheum Dis 73:949–950
Vos T, Flaxman AD, Naghavi M, Lozano R, Michaud C, Ezzati M, Shibuya K, Salomon JA, Abdalla S, Aboyans V, Abraham J, Ackerman I, Aggarwal R, Ahn SY, Ali MK, AlMazroa MA, Alvarado M, Anderson HR, Anderson LM, Andrews KG, Atkinson C, Baddour LM, Bahalim AN, Barker-Collo S, Barrero LH, Bartels DH, Basáñez MG, Baxter A, Bell ML, Benjamin EJ, Bennett D, Bernabé E, Bhalla K, Bhandari B, Bikbov B, Abdulhak AB, Birbeck G, Black JA, Blencowe H, Blore JD, Blyth F, Bolliger I, Bonaventure A, Boufous S, Bourne R, Boussinesq M, Braithwaite T, Brayne C, Bridgett L, Brooker S, Brooks P, Brugha TS, Bryan-Hancock C, Bucello C, Buchbinder R, Buckle G, Budke CM, Burch M, Burney P, Burstein R, Calabria B, Campbell B, Canter CE, Carabin H, Carapetis J, Carmona L, Cella C, Charlson F, Chen H, Cheng ATA, Chou D, Chugh SS, Coffeng LE, Colan SD, Colquhoun S, Colson KE, Condon J, Connor MD, Cooper LT, Corriere M, Cortinovis M, de Vaccaro KC, Couser W, Cowie BC, Criqui MH, Cross M, Dabhadkar KC, Dahiya M, Dahodwala N, Damsere-Derry J, Danaei G, Davis A, de Leo D, Degenhardt L, Dellavalle R, Delossantos A, Denenberg J, Derrett S, Des Jarlais DC, Dharmaratne SD, Dherani M, Diaz-Torne C, Dolk H, Dorsey ER, Driscoll T, Duber H, Ebel B, Edmond K, Elbaz A, Ali SE, Erskine H, Erwin PJ, Espindola P, Ewoigbokhan SE, Farzadfar F, Feigin V, Felson DT, Ferrari A, Ferri CP, Fèvre EM, Finucane MM, Flaxman S, Flood L, Foreman K, Forouzanfar MH, Fowkes FGR, Franklin R, Fransen M, Freeman MK, Gabbe BJ, Gabriel SE, Gakidou E, Ganatra HA, Garcia B, Gaspari F, Gillum RF, Gmel G, Gosselin R, Grainger R, Groeger J, Guillemin F, Gunnell D, Gupta R, Haagsma J, Hagan H, Halasa YA, Hall W, Haring D, Haro JM, Harrison JE, Havmoeller R, Hay RJ, Higashi H, Hill C, Hoen B, Hoffman H, Hotez PJ, Hoy D, Huang JJ, Ibeanusi SE, Jacobsen KH, James SL, Jarvis D, Jasrasaria R, Jayaraman S, Johns N, Jonas JB, Karthikeyan G, Kassebaum N, Kawakami N, Keren A, Khoo JP, King CH, Knowlton LM, Kobusingye O, Koranteng A, Krishnamurthi R, Lalloo R, Laslett LL, Lathlean T, Leasher JL, Lee YY, Leigh J, Lim SS, Limb E, Lin JK, Lipnick M, Lipshultz SE, Liu W, Loane M, Ohno SL, Lyons R, Ma J, Mabweijano J, MacIntyre MF, Malekzadeh R, Mallinger L, Manivannan S, Marcenes W, March L, Margolis DJ, Marks GB, Marks R, Matsumori A, Matzopoulos R, Mayosi BM, McAnulty JH, McDermott MM, McGill N, McGrath J, Medina-Mora ME, Meltzer M, Memish ZA, Mensah GA, Merriman TR, Meyer AC, Miglioli V, Miller M, Miller TR, Mitchell PB, Mocumbi AO, Moffitt TE, Mokdad AA, Monasta L, Montico M, Moradi-Lakeh M, Moran A, Morawska L, Mori R, Murdoch ME, Mwaniki MK, Naidoo K, Nair MN, Naldi L, Narayan KMV, Nelson PK, Nelson RG, Nevitt MC, Newton CR, Nolte S, Norman P, Norman R, O'Donnell M, O'Hanlon S, Olives C, Omer SB, Ortblad K, Osborne R, Ozgediz D, Page A, Pahari B, Pandian JD, Rivero AP, Patten SB, Pearce N, Padilla RP, Perez-Ruiz F, Perico N, Pesudovs K, Phillips D, Phillips MR, Pierce K, Pion S, Polanczyk GV, Polinder S, Pope CA III, Popova S, Porrini E, Pourmalek F, Prince M, Pullan RL, Ramaiah KD, Ranganathan D, Razavi H, Regan M, Rehm JT, Rein DB, Remuzzi G, Richardson K, Rivara FP, Roberts T, Robinson C, de Leòn FR, Ronfani L, Room R, Rosenfeld LC, Rushton L, Sacco RL, Saha S, Sampson U, Sanchez-Riera L, Sanman E, Schwebel DC, Scott JG, Segui-Gomez M, Shahraz S, Shepard DS, Shin H, Shivakoti R, Silberberg D, Singh D, Singh GM, Singh JA, Singleton J, Sleet DA, Sliwa K, Smith E, Smith JL, Stapelberg NJC, Steer A, Steiner T, Stolk WA, Stovner LJ, Sudfeld C, Syed S, Tamburlini G, Tavakkoli M, Taylor HR, Taylor JA, Taylor WJ, Thomas B, Thomson WM, Thurston GD, Tleyjeh IM, Tonelli M, Towbin JA, Truelsen T, Tsilimbaris MK, Ubeda C, Undurraga EA, van der Werf MJ, van Os J, Vavilala MS, Venketasubramanian N, Wang M, Wang W, Watt K, Weatherall DJ, Weinstock MA, Weintraub R, Weisskopf MG, Weissman MM, White RA, Whiteford H, Wiersma ST, Wilkinson JD, Williams HC, Williams SRM, Witt E, Wolfe F, Woolf AD, Wulf S, Yeh PH, Zaidi AKM, Zheng ZJ, Zonies D, Lopez AD, Murray CJL (2012) Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990–2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380:2163–2196
McDonald DG, Leopold GR (1972) Ultrasound B-scanning in the differentiation of Baker’s cyst and thrombophlebitis. Br J Radiol 45:729–732
Sharpe RE, Nazarian LN, Parker L, Rao VM, Levin DC (2012) Dramatically increased musculoskeletal ultrasound utilization from 2000 to 2009, especially by podiatrists in private offices. J Am Coll Radiol 9:141–146
Wakefield RJ, Gibbon WW, Emery P (1999) The current status of ultrasonography in rheumatology. Rheumatology 38:195–198
Grassi W (2003) Clinical evaluation versus ultrasonography: who is the winner? J Rheumatol 30:908–909
Estrach C, Thompson RN (2009) Why aren’t we all doing ultrasound? Rheumatology 48:1019–1020
Wakefield RJ, Goh E, Conaghan PG, Karim Z, Emery P (2003) Musculoskeletal ultrasonography in Europe: results of a rheumatologist based survey at a EULAR meeting. Rheumatology 42:1251–1253
Kane D, Balint PV, Sturrock R, Grassi W (2004) Musculoskeletal ultrasound – a state of the art review in rheumatology. Part 1: current controversies and issues in the development of musculoskeletal ultrasound in rheumatology. Rheumatology 43:823–828
Brown AK, Roberts TE, Wakefield RJ, Karim Z, Hensor E, O’Connor PJ et al (2007) The challenges of integrating ultrasonography into routine rheumatology practice: addressing the needs of clinical rheumatologists. Rheumatology 46:821–829
Cunnington J, Platt P, Raftery G, Kane D (2007) Attitudes of United Kingdom rheumatologists to musculoskeletal ultrasound practice and training. Ann Rheum Dis 66:1381–1383
Naredo E, D’Agostino M-A, Conaghan PG, Backhaus MB, Balint P, Bruyn GAW, Filippucci E, Grassi W, Hammer HB, Iagnocco A, Kane D, Koski JM, Szkudlarek M, Terslev L, Wakefield RJ, Ziswiler HR, Schmidt WA (2010) Current state of musculoskeletal ultrasound training and implementation in Europe: results of a survey of experts and scientific societies. Rheumatology 49:2438–2443
Samuels J, Abramson SB, Kaeley GS (2010) The use of musculoskeletal ultrasound by rheumatologists in the United States. Bull NYU Hosp Jt Dis 68:292–298
Torralba KD, Choi KS, Salto LM, Fairchild R, Cannella AC, Kissin EY, Thiele R, Evangelisto A, Nishio MJ, The Ultrasound School of North American Rheumatologists (USSONAR) (2019) Musculoskeletal ultrasound scanning protocol consensus statements on scanning conventions and documentation in the US. Arthritis Care Res. https://doi.org/10.1002/acr.24005
Larché MJ, McDonald-Blumer H, Bruns A, Roth J, Khy V, de Brum-Fernandes AJ, Wakefield RJ, Brown AK, Bykerk V (2011) Utility and feasibility of musculoskeletal ultrasonography (MSK US) in rheumatology practice in Canada: needs assessment. Clin Rheumatol 30:1277–1283
Tămaş MM, Fodor D, Rednic N, Rednic S (2011) Musculoskeletal ultrasonography in Romania – results from a specific questionnaire. Med Ultrason 13:10–14
Duftner C, Schüller-Weidekamm C, Mandl P, Nothnagl T, Schirmer M, Kainberger F, Machold K, Dejaco C (2014) Clinical implementation of musculoskeletal ultrasound in rheumatology in Austria. Rheumatol Int 34:1111–1115
Mandl P, Baranauskaite A, Damjanov N, Hojnik M, Kurucz R, Nagy O, Nemec P, Niedermayer D, Perić P, Petranova T, Pille A, Rednic S, Vlad V, Zlnay M, Balint PV (2016) Musculoskeletal ultrasonography in routine rheumatology practice: data from central and eastern European countries. Rheumatol Int 36:845–854
Kane D, Balint PV, Sturrock R (2003) Ultrasonography is superior to clinical examination in the detection and localization of knee joint effusion in rheumatoid arthritis. J Rheumatol 30:966–971
Schirmer M, Duftner C, Schmidt WA, Dejaco C (2011) Ultrasonography in inflammatory rheumatic disease: an overview. Nat Rev Rheumatol 7:479–488
Karim Z, Wakefield RJ, Conaghan PG, Lawson CA, Goh E, Quinn MA, Astin P, O'Connor P, Gibbon WW, Emery P (2001) The impact of ultrasonography on diagnosis and management of patients with musculoskeletal conditions. Arthritis Rheum 44:2932–2933
Matsos M, Harish S, Zia P, Ho Y, Chow A, Ioannidis G, Khalidi N (2009) Ultrasound of the hands and feet for rheumatological disorders: influence on clinical diagnostic confidence and patient management. Skelet Radiol 38:1049–1054
McAlindon T, Kissin E, Nazarian L, Ranganath V, Prakash S, Taylor M, Bannuru RR, Srinivasan S, Gogia M, McMahon MA, Grossman J, Kafaja S, FitzGerald J (2012) American College of Rheumatology report on reasonable use of musculoskeletal ultrasonography in rheumatology clinical practice. Arthritis Care Res 64:1625–1640
Torralba KD, Cannella AC, Kissin EY, Bolster MB, Salto LM, Higgs J, Samuels J, Nishio MJ, Kaeley GS, Evangelisto A, de Marco P, Kohler MJ (2017) Musculoskeletal ultrasound instruction in adult rheumatology fellowship programs. Arthritis Care Res. https://doi.org/10.1002/acr.23336
Garrood T, Platt P (2010) Access to training in musculoskeletal ultrasound: a survey of UK rheumatology trainees. Rheumatology 49:391
Brown AK, O’Connor PJ, Roberts TE, Wakefield RJ, Karim Z, Emery P (2006) Ultrasonography for rheumatologists: the development of specific competency based educational outcomes. Ann Rheum Dis 65:629–636
Naredo E, Bijlsma JW, Conaghan PG, Acebes C, Balint P, Berner-Hammer H et al (2008) Recommendations for the content and conduct of European League Against Rheumatism (EULAR) musculoskeletal ultrasound courses. Ann Rheum Dis 67:1017–1022
Taggart AJ, Wright SA, Ball E, Kane D, Wright G (2009) The Belfast musculoskeletal ultrasound course. Rheumatology 48:1073–1076
Pineda C, Reginato AM, Flores V, Aliste M, Alva M, Aragón-Laínez RA, González AB, Bouffard JA, Caballero-Uribe CV, Chávez-López M, Chávez-Pérez NN, Collado P, Díaz-Coto JF, Duarte M, Filippucci E, Galarza-Maldonado C, García-Kutzbach A, Javier Godoy F, González-Sevillano E, da Silveira IG, Gutiérrez M, Hernández-Díaz C, Hernández J, Lamuño-Encorrada M, Marcos JC, Marín-Arriaga N, Mendonça JA, Michaud J, Moya C, Muñoz-Louis R, Neubarth F, Quintero M, Reyes B, Ruta S, Rodríguez-Henríquez PJ, Solano C, Ventura-Ríos L, Möller I, Naredo E (2010) Pan-American League of Associations for Rheumatology (PANLAR) recommendations and guidelines for musculoskeletal ultrasound training in the Americas for rheumatologists. J Clin Rheumatol 16:113–118
Iagnocco A, Terslev L, Backhaus M, Balint P, Bruyn GA, Damjanov N et al (2015) Educational recommendations for the conduct, content and format of EULAR musculoskeletal ultrasound Teaching the Teachers Courses. RMD Open 1:e000139. https://doi.org/10.1136/rmdopen-2015-000139
American College of Rheumatology (n.d.) RhMSUS Certification. https://www.rheumatology.org/Learning-Center/RhMSUS-Certification. Accessed 12 February 2020
2018 RhUS Mini-Curriculum Working Group (n.d.) 2019 Rheumatologic ultrasound (RhUS) curriculum supplement to the American College of Rheumatology 2015 core curriculum outline. https://www.rheumatology.org/Portals/0/Files/Rhumatologic-Ultrasound-Curriculum-Supplement.pdf. Accessed 12 February 2020
Ultrasound School of North American Rheumatologists (n.d.) USSONAR Training Program. https://www.ussonar.org/training-program. Accessed 12 February 2020
American College of Rheumatology (2018) Position statement: musculoskeletal ultrasound. https://www.rheumatology.org/Portals/0/Files/Musculoskeletal%20Ultrasound.pdf. Accessed 12 February 2020
Dasgupta B, Cimmino MA, Maradit-Kremers H, Schmidt WA, Schirmer M, Salvarani C, Bachta A, Dejaco C, Duftner C, Jensen HS, Duhaut P, Poór G, Kaposi NP, Mandl P, Balint PV, Schmidt Z, Iagnocco A, Nannini C, Cantini F, Macchioni P, Pipitone N, Amo MD, Espígol-Frigolé G, Cid MC, Martínez-Taboada VM, Nordborg E, Direskeneli H, Aydin SZ, Ahmed K, Hazleman B, Silverman B, Pease C, Wakefield RJ, Luqmani R, Abril A, Michet CJ, Marcus R, Gonter NJ, Maz M, Carter RE, Crowson CS, Matteson EL (2012) 2012 provisional classification criteria for polymyalgia rheumatica: a European League Against Rheumatism/American College of Rheumatology collaborative initiative. Ann Rheum Dis 71:484–492
Neogi T, Jansen TL, Dalbeth N, Fransen J, Schumacher HR, Berendsen D et al (2015) 2015 gout classification criteria: an American College of Rheumatology/European League Against Rheumatism collaborative initiative. Arthritis Rheum 67:2557–2568
Brown AK, Quinn MA, Karim Z, Conaghan PG, Peterfy CG, Hensor E, Wakefield RJ, O'Connor PJ, Emery P (2006) Presence of significant synovitis in rheumatoid arthritis patients with disease-modifying antirheumatic drug-induced clinical remission. Arthritis Rheum 54:3761–3773
D’Agostino M-A, Terslev L, Aegerter P, Backhaus M, Balint P, Bruyn GA, Filippucci E, Grassi W, Iagnocco A, Jousse-Joulin S, Kane D, Naredo E, Schmidt W, Szkudlarek M, Conaghan PG, Wakefield RJ (2017) Scoring ultrasound synovitis in rheumatoid arthritis: a EULAR-OMERACT ultrasound taskforce – part 1: definition and development of a standardised, consensus-based scoring system. RMD Open 3:e000428. https://doi.org/10.1136/rmdopen-2016-000428
Dejaco C, Ramiro S, Duftner C, Besson FL, Bley TA, Blockmans D, Brouwer E, Cimmino MA, Clark E, Dasgupta B, Diamantopoulos AP, Direskeneli H, Iagnocco A, Klink T, Neill L, Ponte C, Salvarani C, Slart RHJA, Whitlock M, Schmidt WA (2018) EULAR recommendations for the use of imaging in large vessel vasculitis in clinical practice. Ann Rheum Dis 77:636–643
Takase K, Ohno S, Ideguchi H, Takeno M, Shirai A, Ishigatsubo Y (2010) Use of musculoskeletal ultrasound in Japan: a survey of practicing rheumatologists. Mod Rheumatol 20:376–380
Hama M, Takase K, Ihata A, Ohno S, Ueda A, Takeno M, Ishigatsubo Y (2012) Challenges to expanding the clinical application of musculoskeletal ultrasonography (MSUS) among rheumatologists: from a second survey in Japan. Mod Rheumatol 22:202–208
Kang T, Wakefield RJ, Emery P (2016) Musculoskeletal ultrasound in rheumatology in Korea: targeted ultrasound initiative survey. Int J Rheum Dis 19:335–342
Li Z, Yang Y (2012) Rheumatology in China: challenges and development. Rheumatology 51:1733–1734
Zhang F (2009) The China rheumatology workforce: a status report. Int J Rheum Dis 12:279–282
Acknowledgments
The authors would like to thank the colleagues who participated in our survey, as well as Chen Yu and Min Hui from Peking Union Medical College for assistance with translations of the original survey responses. The authors would also like to acknowledge the Chinese Rheumatology Association for the organization’s collaboration and assistance with this work.
Code availability
Not applicable.
Funding
This work was supported by the Chinese National High Technology Research and Development Program, Ministry of Science and Technology [grant number 2012AA020830]; the Chinese National Key Technology Research and Development Program, Ministry of Science and Technology [grant number 2008BAI59B02]; the National Key Research and Development Program of China [grant numbers 2017YFC0907601, 2017YFC0907602, 2017YFC0907603, 2017YFC0907604, 2017YFC0907605]; National Natural Science Foundation of China [grant number 81601433]; the National Heart, Lung and Blood Institute of the National Institutes of Health [grant number T35 HL007649 to M.W.]; and the National Institutes of Health/Fogarty International Center [grant number K01 TW009995 to E.H.]. The content is solely the responsibility of the authors and does not necessarily represent the official views of the sponsors.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
None.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wu, M., Peng, L., Donroe, J. et al. Musculoskeletal ultrasound imaging training, use, and knowledge among rheumatologists in China. Clin Rheumatol 40, 321–330 (2021). https://doi.org/10.1007/s10067-020-05175-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-020-05175-4