Abstract
Purpose
Several studies have examined effectiveness of primary fascial defect closure (FDC) versus bridged repair (no-FDC) during laparoscopic ventral hernia mesh repair (LVHMR). The purpose of this study was to systematically review and meta-analyse randomized controlled trials (RCTs) which compared safety and effectiveness of two techniques.
Methods
Systematic literature searches (EMBASE, MEDLINE, PubMed, and CINAHL) were conducted according to the Preferred Reporting Items for Systematic Reviews and Meta-Analysis (PRISMA) guidelines using predefined terms. RCTs comparing FDC and no-FDC in LVHMR were identified and retrieved. Primary outcomes were risk of recurrence and risk of major complications analyzed as a single composite outcome. Secondary outcomes were risks of seroma formation, clinical or radiologically confirmed eventration, incidence of readmission to hospital, postoperative changes in quality of life (QoL), and postoperative pain. Random effects modeling to summarize statistics were performed. The risk of bias was assessed using Cohrane’s Risk of Bias tool 2.
Results
Three RCTs that enrolled total of 259 patients were included. There was clinical heterogeneity present between studies related to patients’ characteristics, hernia characteristics, and operative techniques. There was no difference found in primary outcomes, risks of seroma formation, eventration, and chronic pain. There is conflicting evidence on how both techniques affect postoperative QoL or early postoperative pain.
Conclusions
Both techniques were detected to have equal safety profile and do not differ in risk of recurrence, seroma formation, risks of clinical or radiological eventration. Giving uncertainty and clinical equipoise, another RCT examining FDC vs no-FDC laparoscopic mesh repair separately for primary and secondary hernias using narrow inclusion criteria for hernia size on well-defined population would be ethical and pragmatic.
Prospero registration
CRD42021274581.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Laparoscopic ventral hernia mesh repair (LVHMR) is a well-established technique worldwide to treat both primary and incisional abdominal wall hernias [1]. There are several variations of LVHMR. One of the variations is concerned about approach to the fascial defect. European Hernia Society and Americas Hernia Society guidelines as well as International Endohernia Society guidelines suggest adopting fascial defect closure (FDC) approach [2,3,4]. This recommendation is based on two systematic reviews of observational studies that showed that FDC reduces recurrence and seroma formation rates as compared to no-FDC (also known as bridged repair) technique [5, 6]. However, since publication of these reviews, several new high-quality prospective studies have been reported comparing FDC and no-FDC in LVHMR. The objective of our study was to perform an updated systematic review and comprehensive meta-analysis based on published randomized controlled trials (RCTs) comparing safety profile, risk of recurrence, other important secondary outcome measures such as risk of seroma formation, clinical or radiological eventration, acute and chronic pain and quality of life following FDC or non-FDC repairs.
Methods
Search strategy
The study was prospectively registered with PROSPERO (CRD42021274581) and conducted according to the Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) guidelines [7].
The search terms were devised to cover technical aspects of laparoscopic ventral hernia repair with regards to FDC. This was performed using the following text words (including their synonyms/variants) and Medical Subject Headings (MESH terms): laparoscopy, ventral hernia repair, incisional hernia repair, umbilical hernia repair, primary fascial closure, and no-closure mesh repair. The search terms were combined using the Boolean AND/OR operators.
PubMed, Medline, Embase, and CINAHL were comprehensively searched. ClinicalTrials.gov was also explored for any registered trials. The initial database searches encompassed studies published in English from the inception date of each database to 21st of August 2021. To ensure that all relevant studies were identified, no restrictions were placed on the date of publication or regional state. Two reviewers identified relevant articles comparing FDC and no-FDC in patients undergoing LVHMR. Reference lists of all retrieved articles were manually searched to identify additional studies. Complete search algorithms for each database are available in Appendix 1.
Inclusion criteria
Studies published in English that fulfilled the following criteria were included: (1) studies that compared primary FDC with mesh and bridged mesh repair (no-FDC) in laparoscopic ventral hernia surgery, (2) randomized controlled studies, and (3) full-text manuscripts.
Exclusion criteria
Studies were excluded from analysis: (1) studies in which it was not possible to extract data from the published results, (2) the studies contained re-published data, (3) non-randomized studies, (4) studies published in other language than English, and (5) publications that are editorials, comments, letters, review articles, conference abstracts, retractions, and case reports.
Outcome measures
Primary outcomes for this study were recurrence and major complications. This study combined all complications which could be classified as grade II or above as per Clavien–Dindo classification [8, 9] into a single composite outcome. Cases of death during follow-up period which were not judged to be directly related to primary surgery were taken note of, but not included in the meta-analysis.
Secondary outcomes studied were acute and chronic postoperative pain, seroma formation, clinical or radiologically confirmed eventration (bulging), readmission to hospital, and postoperative changes in quality of life (QoL).
Study selection
Two authors (YT and CSW) implemented the search strategy independently. Both reviewed the abstracts identified by the search to exclude those that did not meet the inclusion criteria. Differences of opinion were resolved by consensus with the senior author (AK).
Data extraction
Data from each study reporting the outcomes of interest were extracted by two independent reviewers (VT, ID). The extracted data included the following: the basic characteristics of the study, including authors, year, and sample size; the basic patient characteristics and comparative outcomes. Disagreement was resolved by discussion to reach a consensus; if an agreement between the two reviewers could not be reached, a third person (AK) was involved.
Risk of bias assessment
All studies were independently assessed by two investigators for quality and validity using the Cochrane Risk of Bias Tool 2 Algorithm with the effect of principal interest being assignment to intervention at baseline [10]. Full-text manuscripts and trial protocols were assessed where available. Disagreements in the quality assessment were resolved by consensus.
Statistical analysis
All statistical analyses were performed using Revman software, version 5.3 (Cochrane Collaboration, The Nordic Cochrane Centre, Copenhagen). Meta-analysis was performed for primary outcomes as well as for two secondary outcomes (seroma formation, clinically or radiologically confirmed eventration). Random-effects models to analyze data were used. Risk difference (RD) was calculated for dichotomous outcomes. A 95% confidence interval (CI) was recorded. Statistical heterogeneity was assessed using the I2 test statistic [11].
Results
Description of study selection
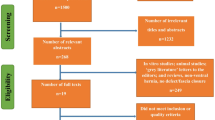
The predefined search strategy captured 315 potentially relevant publications. In total, 56 duplicate studies were removed. After titles and abstracts screening, additional 252 studies were excluded. After full-text screening, additional four studies were excluded. The full texts of the remaining three studies were reviewed and subsequently confirmed to be eligible to be entered into the review and meta-analysis. The PRISMA flow diagram of this process is shown in Fig. 1.
Study characteristics
The 3 RCT studies enrolled 259 participants. All studies included patients who underwent LVHMR repair with FDC or no-FDC. Overall, 129 and 130 patients were allocated and received intervention in the FDC group and no-FDC group, respectively. Short-term outcome data were available for meta-analysis for 251 patients, while long-term (12 months to 24 months) follow-up data were available for lower number of patients.
The main characteristics of studies are provided in Tables 1 and 2.
Risk of bias
Assessment of quality was based on journal articles, published protocols and trial protocols registered in clinicaltrials.gov. Included studies were found to have low risk of bias. The risk of bias summary data is provided in Table 3.
Primary outcomes
Recurrence
Recurrence rates in selected studies ranged from 0 to 23% [1, 12, 13]. The study of Christoffersen et al. which had the highest rate of recurrence found significantly lower number of events in no-closure group [12]. Pooled analysis of included studies based on 244 patients did not demonstrate difference in the risk of recurrence (Risk difference RD – 0.01 [95 Confidence Interval CI – 0.13, 0.10] p = 0.81) (Fig. 2). Heterogeneity was 72% (Table 4).
Major complications
Complications that fell within Clavien–Dindo grade II or above were two cases of surgical site infection requiring antibiotics and one case of re-operation due to severe pain [1, 12, 13]. There were two cases of death reported during follow-up, although these were not directly related to primary surgery [1, 13]. These cases were not accounted for in the meta-analysis. No difference between two techniques was found when RD of major complications as a composite outcome was calculated (RD 0.01 [– 0.02, 0.04], p = 0.58) (Fig. 3; Table 4).
Secondary outcomes
Postoperative pain
Acute pain (day 1–day 30)
Two studies reported on pain in 30-day postoperative period [1, 12]. The study of Christoffersen et al. showed that there was no significant difference between the groups at day 1 for pain on activity assessed by Visual Analogue Scales (VAS) (P = 0⋅906) and Verbal Rating Scale (VRS) (P = 0⋅205) as well as at 30 days (VAS (P = 0⋅986); VRS (P = 0⋅142)) [12]. In addition, there was no difference in need of rescue opioids between the two study groups (p = 0⋅350). In contrast, the study of Ali et al. showed that there was significant difference between groups at day 7 for acute pain by VAS (p < 0⋅001) and at 1 month by VAS (p = 0⋅045) favoring no-FDC in both cases [1] (Table 5).
Chronic pain (6 months–24 months)
Three patients reported moderate or severe chronic pain on the VRS at 2-year follow-up (2 in the no-closure and 1 in the closure group) in the study of Christoffersen et al. [12]. There was no significant difference between groups in chronic pain using VAS score at 6 months (p = 0.052), and no pain was reported at 12 months in either group in the study of Ali et al. [1]. There was no significant difference in the severity of pain in the study of Bernardi et al. in the follow-up time to 2 years after randomization [13] (Table 5).
Quality of life (QoL) and satisfaction rates
Long-term (12–24 months) quality of life outcomes were assessed by two studies. The study of Bernardi et al. examined QoL changes as a primary outcome and had a median follow-up of 24 months (range 9–42). Modified Activity Assessment Scale (mAAS), a validated hernia-specific QoL survey, was used [14,15,16]. The data were available for 107 patients. Both groups experienced an increase in their QoL scores after repair; however, those who underwent FDC had on average a 12-point higher improvement in their QoL scores (41.3 ± 31.5 vs 29.7 ± 28.7, P = 0.047) (Table 5). There was 2.1X reported factor change in the FDC group as compared to 1.7X factor change in the no-FDC group.
The study of Christoffersen et al. used CCS, Carolinas Comfort Scale [17], to assess quality of life at 2-year follow-up [12]. This was available for 73 patients. There was no difference found in the CCS (p = 0.528) between two groups. Neither one of two techniques was associated with better satisfaction score on VRS scale (p = 0⋅955) (Table 5).
Seroma formation
Seroma formation was reported by all three studies with rates ranging from 8 to 45%. There was no significant difference in the risk of seroma formation between groups (RD of – 0.03 [– 0.24, 0.18] p = 0.77). The heterogeneity in the studies was at 80% (Fig. 4; Table 5).
Clinical or radiologically confirmed eventration
The rate of clinical eventration in the study of Bernardi et al. [13] was reported to be 13% (16 cases). The study of Christoffersen et al. reported on radiological signs of eventration and demonstrated the rate of 4.1% [12]. There was no significant difference between two groups when meta-analysis was performed (Fig. 5).
Incidence of readmission to hospital
Two studies reported incidence of re-admission to hospital [12, 13]. While it was confirmed that reason for two readmissions in the study of Christoffersen et al. [12] was pain, there was no explanation provided for seven cases of readmission in the study of Bernardi et al. [13] (Table 5).
Assessment of reporting biases
According to the Cochrane guidelines, we were unable to assess the reporting biases because there were fewer than 10 trials included in the analysis.
Discussion
Our systematic review and meta-analysis is the first study that compared FDC and non-FDC LVHMR using high-quality data. Our study included RCTs only as it is agreed that a meta-analysis of RCTs offers the highest level of evidence and thus allows for the highest grade of recommendation [18]. All included studies were judged to have low risk of bias and methodology design was compliant with Palermo consensus group statement recommendations on measuring and reporting outcomes in studies analyzing abdominal wall repair techniques (Palermo CG statement) [18]. Primary and secondary outcomes in our study were selected based on Palermo CG statement [18].
Our study confirmed that both techniques have equal safety profile, and no difference was detected in risk of recurrence. There was no difference detected in secondary outcomes such as risk of clinical or radiological eventration, risk of seroma formation. Findings of our study are contrary to findings of previous meta-analysis which was based on data of lower quality (observational studies) and showed better outcomes in seroma rates [5, 6]. In addition, the meta-analysis of Tandon et al. reported less adverse hernia outcomes (composite outcome consisting of all terms of recurrence, pseudo-recurrence, mesh eventration, tissue eventration, clinical eventration or bulging) in FDC group.
With regards to postoperative pain, in our review, we found that there is conflicting evidence on whether one technique is superior to another when it comes to severity of early (up to 30 days) postoperative pain. However, all studies in our review confirmed no difference in postoperative pain at a longer follow-up (6 months and onwards).
It is difficult to draw conclusion on whether one technique is superior to another with regards to postoperative QoL. One study included in our review assessed this as a primary outcome and identified better results in FDC group [13], while another study which assessed QoL as a secondary outcome using different scale did not find any difference [12].
Our study has some limitations. The main limitation of the study was clinical heterogeneity related to patients’ characteristics, hernia characteristics, and operative techniques. In the study of Bernardi et al., there were more patients with ASA equal or above III as well as with higher BMI as compared to two other studies [1, 13]. In the study of Bernardi et al. and Ali et al., there were more patients included with secondary hernia while in the study of Christoffersen most of enrolled patients had primary hernia [1, 12, 13]. There was some heterogeneity in measurement of outcomes with regards to timing and methodology. The time point at which incidence of recurrence was recorded as well as diagnostic criteria differed between the studies. While Christoffersen et al. analyzed recurrence 2 years after surgery [12], in the study of Ali et al., this outcome was recorded at 1-year time point [1]. In the study of Christoffersen, screening for recurrence was performed using clinical investigation and if this was inconclusive, computer tomography (CT) with oral contrast was performed during Valsalva maneuver [12]. In the study of Ali, recurrence was detected using CT [16]. In the study of Bernardi et al., recurrence was evaluated at 1–2 years with clinical assessment and CT imaging was utilized selectively [13]. Similarly, the time point of assessment and diagnostic criteria for seroma and eventration differed between the studies [1, 12, 13]. Differences in outcome measurement could have introduced bias to results of meta-analysis. Due to loss to follow-up in all three studies, there was decreased sample size for such outcomes as recurrence and eventration, 244 and 196 participants, respectively, hence decreased power of the result.
Our study has not resolved uncertainty with regards to whether one technique is superior to another in QoL outcomes. This is because there was heterogeneity in the QoL tools used for reporting outcome. Currently, there is no dominant widely accepted QoL tool to measure outcomes in abdominal wall hernia surgery [19].
Giving this uncertainty and clinical equipoise, another RCT examining FDC vs no-FDC laparoscopic mesh repair separately for primary and secondary hernias using well-defined narrow inclusion criteria for hernia size on a large but well-defined population would be ethical and pragmatic.
Availability of data and material
Data available on reasonable request.
References
Ali F, Wallin G, Fathalla B, Sandblom G (2020) Peritoneal bridging versus fascial closure in laparoscopic intraperitoneal onlay ventral hernia mesh repair: a randomized clinical trial. BJS Open 4:587–592
Henriksen NA, Montgomery A, Kaufmann R, Berrevoet F, East B, Fischer J, Hope W, Klassen D, Lorenz R, Renard Y, Garcia Urena MA, Simons MP (2020) Guidelines for treatment of umbilical and epigastric hernias from the European Hernia Society and Americas Hernia Society. Br J Surg 107:171–190
Bittner R, Bain K, Bansal VK, Berrevoet F, Bingener-Casey J, Chen D, Chen J, Chowbey P, Dietz UA, de Beaux A, Ferzli G, Fortelny R, Hoffmann H, Iskander M, Ji Z, Jorgensen LN, Khullar R, Kirchhoff P, Köckerling F, Kukleta J, LeBlanc K, Li J, Lomanto D, Mayer F, Meytes V, Misra M, Morales-Conde S, Niebuhr H, Radvinsky D, Ramshaw B, Ranev D, Reinpold W, Sharma A, Schrittwieser R, Stechemesser B, Sutedja B, Tang J, Warren J, Weyhe D, Wiegering A, Woeste G, Yao Q (2019) Update of Guidelines for laparoscopic treatment of ventral and incisional abdominal wall hernias (International Endohernia Society (IEHS)): Part B. Surg Endosc 33:3511–3549
Bittner R, Bain K, Bansal VK, Berrevoet F, Bingener-Casey J, Chen D, Chen J, Chowbey P, Dietz UA, de Beaux A, Ferzli G, Fortelny R, Hoffmann H, Iskander M, Ji Z, Jorgensen LN, Khullar R, Kirchhoff P, Köckerling F, Kukleta J, LeBlanc K, Li J, Lomanto D, Mayer F, Meytes V, Misra M, Morales-Conde S, Niebuhr H, Radvinsky D, Ramshaw B, Ranev D, Reinpold W, Sharma A, Schrittwieser R, Stechemesser B, Sutedja B, Tang J, Warren J, Weyhe D, Wiegering A, Woeste G, Yao Q (2019) Update of Guidelines for laparoscopic treatment of ventral and incisional abdominal wall hernias (International Endohernia Society (IEHS))-Part A. Surg Endosc 33:3069–3139
Tandon A, Pathak S, Lyons NJ, Nunes QM, Daniels IR, Smart NJ (2016) Meta-analysis of closure of the fascial defect during laparoscopic incisional and ventral hernia repair. Br J Surg 103:1598–1607
He C, Lu J, Ong MW, Lee DJK, Tan KY, Chia CLK (2020) Seroma prevention strategies in laparoscopic ventral hernia repair: a systematic review. Hernia 24:717–731
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, Shekelle P, Stewart LA (2015) Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev 4:1
Dindo D, Demartines N, Clavien PA (2004) Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg 240:205–213
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng HY, Corbett MS, Eldridge SM, Emberson JR, Hernán MA, Hopewell S, Hróbjartsson A, Junqueira DR, Jüni P, Kirkham JJ, Lasserson T, Li T, McAleenan A, Reeves BC, Shepperd S, Shrier I, Stewart LA, Tilling K, White IR, Whiting PF, Higgins JPT (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327:557–560
Christoffersen MW, Westen M, Rosenberg J, Helgstrand F, Bisgaard T (2020) Closure of the fascial defect during laparoscopic umbilical hernia repair: a randomized clinical trial. Br J Surg 107:200–208
Bernardi K, Olavarria OA, Holihan JL, Kao LS, Ko TC, Roth JS, Tsuda S, Vaziri K, Liang MK (2020) Primary fascial closure during laparoscopic ventral hernia repair improves patient quality of life: a multicenter, blinded randomized controlled trial. Ann Surg 271:434–439
Krpata DM, Schmotzer BJ, Flocke S, Jin J, Blatnik JA, Ermlich B, Novitsky YW, Rosen MJ (2012) Design and initial implementation of HerQLes: a hernia-related quality-of-life survey to assess abdominal wall function. J Am Coll Surg 215:635–642
Barber MD, Kenton K, Janz NK, Hsu Y, Dyer KY, Greer WJ, White A, Meikle S, Ye W (2012) Validation of the activities assessment scale in women undergoing pelvic reconstructive surgery. Female Pelvic Med Reconstr Surg 18:205–210
McCarthy M Jr, Jonasson O, Chang CH, Pickard AS, Giobbie-Hurder A, Gibbs J, Edelman P, Fitzgibbons R, Neumayer L (2005) Assessment of patient functional status after surgery. J Am Coll Surg 201:171–178
Heniford BT, Lincourt AE, Walters AL, Colavita PD, Belyansky I, Kercher KW, Sing RF, Augenstein VA (2018) Carolinas comfort scale as a measure of hernia repair quality of life: a reappraisal utilizing 3788 international patients. Ann Surg 267:171–176
Muysoms FE, Deerenberg EB, Peeters E, Agresta F, Berrevoet F, Campanelli G, Ceelen W, Champault GG, Corcione F, Cuccurullo D, DeBeaux AC, Dietz UA, Fitzgibbons RJ Jr, Gillion JF, Hilgers RD, Jeekel J, Kyle-Leinhase I, Köckerling F, Mandala V, Montgomery A, Morales-Conde S, Simmermacher RK, Schumpelick V, Smietański M, Walgenbach M, Miserez M (2013) Recommendations for reporting outcome results in abdominal wall repair: results of a Consensus meeting in Palermo, Italy, 28–30 June 2012. Hernia 17:423–433
Grove TN, Muirhead LJ, Parker SG, Brogden DRL, Mills SC, Kontovounisios C, Windsor ACJ, Warren OJ (2021) Measuring quality of life in patients with abdominal wall hernias: a systematic review of available tools. Hernia 25:491–500
Funding
There was no funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
YT, CSW, ID, VT, AK, and VP have no conflicts of interest or financial ties to disclose. DP received consulting fees from Johnson and Johnson and payment or honoraria for educational events from Johnson and Johnson, Medtronic, Novo Nordisk. These benefits were not related to this manuscript.
Ethical approval
Not applicable.
Human and animal rights
Not applicable.
Informed consent
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tryliskyy, Y., Wong, C.S., Demykhova, I. et al. Fascial defect closure versus bridged repair in laparoscopic ventral hernia mesh repair: a systematic review and meta-analysis of randomized controlled trials. Hernia 26, 1473–1481 (2022). https://doi.org/10.1007/s10029-021-02533-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10029-021-02533-2