Abstract
Pediatric-onset obsessive–compulsive disorder (OCD) is underdiagnosed, and many affected children are untreated. The present study seeks to evaluate the presence and the clinical impact of OCD and obsessive–compulsive symptoms (OCS) in a large sample of school-age children. In Phase I, we performed an initial screening using the Family History Screen (FHS). In Phase II, we identified an “at-risk” sample, as well as a randomly selected group of children. A total of 2,512 children (6–12 years old) were assessed using the FHS, the Development and Well-Being Assessment (DAWBA), the Strengths and Difficulties Questionnaire (SDQ), and the Child Behavior Checklist (CBCL). Data analyses included descriptive and multivariate analytical techniques. 2,512 children (mean age: 8.86 ± 1.84 years; 55.0 % male) were categorized into one of the three diagnostic groups: OCD (n = 77), OCS (n = 488), and unaffected controls (n = 1,947). There were no significant socio-demographic differences (age, gender, socioeconomic status) across groups. The OCS group resembled the OCD on overall impairment, including school problems and delinquent behaviors. However, the OCD group did have significantly higher rates of several comorbid psychiatric disorders, including separation anxiety, generalized anxiety, and major depressive disorder, than OCS or unaffected controls. Moreover, the OCD group also scored higher than the SDQ, as well as on each of CBCL items rated by the parent. Our findings suggest that there is a psychopathological continuum between OCS and OCD in school-aged children. The presence of OCS is associated with functional impairment, which needs further investigation in longitudinal studies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obsessive–compulsive disorder (OCD) is a chronic and disabling psychiatric disorder with a lifetime prevalence of 2–3 % in the general adult population [1, 2]. The onset of the first obsessive–compulsive symptoms (OCS) occurs during childhood in the majority of cases [3–5]. However, data on the prevalence of OCD among children and adolescents are scarce. Available prevalence estimates range from 0.1 % [6] to 3.6 % [7] for pediatric-onset OCD. Pediatric-onset OCD is highly underdiagnosed and 90 % of affected children are left untreated [4, 8].
In line with the obsessive–compulsive spectrum phenomena hypothesis [9], previous studies report that functional impairment [10, 11] and several psychiatric comorbidites are associated not only with OCD, but subclinical OCD and OCS as well [7, 12–14]. Moreover, longitudinal studies suggest that OCS can persist over time [11, 15] and increase the risk of developing OCD [16, 17], supporting a dimensional approach.
However, there is limited evidence on the prevalence and clinical characteristics of OCS in non-clinical populations and most of the studied samples include adolescents [7, 9, 18–21] and young adults [22], but only two focused on school-age children [11, 15]. Furthermore, the literature is not consistent regarding epidemiological and several clinical characteristics. For instance, prevalence rates of OCS in studies range from 2.0 % [12] to 19.0 % [19] in juvenile samples. Additionally, some studies report equal gender ratio distribution [7, 11, 13, 14, 19, 20] while others report higher prevalence of OCS in boys [12, 23]. Studies in children, adolescents and adults indicate that patients with OCS resemble OCD in their presentation and psychiatric comorbidities [7–9, 11–14], but data concerning behavioral problems and the level of clinical impairment for children with OCS/OCD research remain scarce.
Thus, this study aimed to investigate the obsessive–compulsive dimensional approach (OCD, OCS, and unaffected controls) in a community-based sample of 2,512 Brazilian school-age children (6–12 years old) by assessing several socio-demographic and clinical parameters, including psychiatric comorbidities, co-occurring psychiatric symptoms and functional impairment.
Methods
Procedures
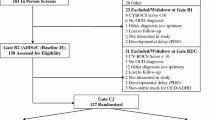
This study examined data from the cross-sectional phase of a large community school-based cohort from the National Institute of Developmental Psychiatry (INPD) in Brazil http://www.inpd.org [24]. A total of 57 public schools from two large Brazilian cities (22 in Porto Alegre and 35 in São Paulo) were included and 12,500 families were approached. This study was approved by the ethics committees from the universities in these two cities. In the initial phase, written consent was obtained from all parents of participants (see Fig. 1).
Flowchart asterisk: refusal or failure to complete interview or consent form (18.8 %), registry by non-biological parent (9.2 %); provided invalid phone contacts/fail contact (5.3 %), other (2.6 %); (double asterisk): school transfer (12.3 %); others (0.61 %); triple asterisk refusal or failure to complete the interviews or consent form (16.2 %); fail contact (8.6 %), other (0.5 %)
Participants
Inclusion Criteria: Children aged 6–12 years old, as of school registration day, who were accompanied by their biological parent. Exclusion criteria: (a) refusal or failure to complete the interviews or consent form; (b) transfer to another school during the project, and/or (c) failure to establish contact. The final sample comprised 2,512 children (no siblings) which are divided into two groups according to an index of individual and familial screened psychopathology by the (Psychiatric) Family History Screen (Milne et al. [32]. As presented in Fig. 1, the community-based sample included 1,554 children judged to be “at-risk” and randomly selected group of 958 children initially judged to be not “at-risk”.
Data collection
In Phase II of the study, extensively trained lay evaluators interviewed the caregivers about the index-children (the child’s biological mother was the informant in 91.5 % of the families). Training procedures for interviewers included instructional sessions comprising major psychiatric syndromes and risk factors, confidentiality, and ethical issues taught by INPD psychiatrists. Each potential interviewer was evaluated through direct observation and a written multiple-choice test. Only interviewers who showed satisfactory performance in the evaluation were recruited.
Clinical assessment and instruments
-
Sociodemographic information age, gender and validated Brazilian socioeconomic classification that categorized families in five (A–E) socioeconomic classes according to educational level and income were obtained [25].
-
Psychiatric diagnoses assessment was conducted with the DAWBA (development and well-being assessment) [26] based on DSM-IV [27]. DAWBA has been used in several countries and is validated in Brazil [28]. Diagnoses were double rated by senior child psychiatrists and a third senior child psychiatrist gave the final diagnosis in case of disagreement.
-
OCS and OCD diagnoses a subject was considered as part of the OCS group if he/she had at least one obsession or compulsion symptom listed in the DAWBA Section F (overall obsessions or compulsions and a list of symptoms including contamination and aggression obsessions; washing, checking, repetition, touching, counting and ordering-symmetry related compulsions) [26]. An OCD diagnosis was determined based on DSM-IV criteria, as follows: obsessions and/or compulsions were time consuming (more than 1 h per day) or caused clinically significant distress or impairment; and could not be attributable to the physiological effects of a substance or another medical condition [27].
-
Behavioral problems assessment was conducted using the child behavior checklist (CBCL) [29]. The CBCL is a dimensional instrument that has been used across the world and was validated in Brazil [30]. It includes total score and sub-scales of anxiety/depression, somatic complaints, social competence problems, rule-breaking, aggressive, internalizing and externalizing behaviors [29, 30].
-
Clinical impairment data on clinical impairment were based on the strengths and difficulties questionnaire (SDQ) [31] that includes 25 items on psychological attributes and an impact supplement assessing chronicity, distress, social impairment, and burden. School problems (failure, refusal or expulsion), delinquent behavior (theft, vandalism), overall functional impairment and referral for mental health services (psychological or psychiatric, inpatient or outpatient) were obtained using the family history screen [32].
Statistical analysis
Our main objective was to compare three groups (OCD, OCS, and unaffected controls) according to several discrete (e.g.: presence of comorbidities or impact factors) and continuous (e.g.: age, dimensional CBCL and SDQ scores) parameters. As the disproportionate number of subjects among groups would greatly affect the variance, the use of conventional modeling procedures was not advisable. Bayesian 95 % credible intervals and nonparametric Tukey 95 % confidence intervals were used [33, 34]. These methods minimize bias due to high variance, enable comparison between groups (statistical similarities or statistical differences), and have been used successfully in previous studies [5]. Finally, to verify categorical sociodemographics variables, we conducted a two-tailed Fisher exact test [35] and Kruskal–Wallis exact test [36].
Results
Composition of OCD, OCS and control groups
This study compared demographic and clinical variables (described above) in the three diagnostic groups of interest (Fig. 1; Table 1). There were 77 (3.1 %) children assigned to the OCD group; 488 (19.4 %) assigned to the OCS group; and 1,947 (77.5 %) assigned to the Control group.
Sociodemographic status
There were no statistically significant differences on the distribution of age (p = 0.34), sex (p = 0.57), or socioeconomic (p = 0.12) status between groups (Table 1). The majority of the children came from middle class families (Class C).
Other psychiatric disorders
The OCD group showed significantly higher prevalence of the following psychiatric disorders: major depressive disorder, mood disorders, separation anxiety disorder, generalized anxiety disorder, attention deficit hyperactivity disorder (ADHD), compared to the OCS and the control groups. The OCD and OCS groups were similar regarding the prevalence of the following comorbidities: social phobia, anxiety disorders (grouped), oppositional defiant disorder, tic disorders and eating disorders. Both the OCD and OCS groups had a higher prevalence of these disorders compared to the unaffected control group. Post-traumatic stress disorder, specific phobia, panic and agoraphobia, and developmental disorders were less prevalent in the whole sample and there was no difference in prevalence among the OCD group, OCS group and unaffected control groups (Table 2).
Behavioral problems and clinical impairment
There was a statistically significant difference between the three groups on CBCL ratings (Table 3). The OCS group showed intermediate scores between OCD (higher behavioral impairment) and unaffected control groups (lower behavioral impairment) on the CBCL scale and its subscales of anxiety/depression, somatic complaints, social problems, rule-breaking, aggressive, internalizing and externalizing behaviors and obsessive–compulsive scale, as well as the SDQ scores. There were no significant differences between OCD and OCS groups in overall functioning impairment, school problems, delinquent behavior, and searching for previous treatment (Table 4).
Discussion
The present study reports from a large epidemiologic sample of school-age children (n = 2,512) in Brazil that were assessed with a comprehensive clinical protocol, including DSM-IV [27] based diagnoses and validated dimensional assessment of patterns of behavior and clinical impact [29, 31, 32]. Additionally, our study report focuses on a younger age cohort and includes a higher number of subjects than most previous reports [10, 11, 15, 21]. Our results demonstrate that children with OCS and OCD have similar levels of impairment. In addition, the prevalence of several comorbid conditions, such as social phobia, anxiety disorders (grouped), oppositional defiant disorder, tic disorders, and eating disorders, was significantly elevated compared to unaffected controls in both the OCD and OCS groups. However, the children with OCD were found to be at greater risk of several comorbid conditions including major depression, several anxiety disorders and ADHD.
The prevalence of OCS (19.4 %) found in similar to previous reports [7, 19, 21, 23]. The prevalence of OCD was 3.1 %, which is high compared to some epidemiological reports in children and adolescents [13, 20] but is in accordance with other studies [7, 21]. This may be attributed to differences in diagnostic instruments utilized in these studies and to the inclusion of a proportion of “at risk” children in our sample (see: Salum et al. [24]).
There were no statistically significant differences between groups regarding gender distribution, which is consistent with some studies [11] but in contrast with others that reported a slightly higher prevalence of obsessive–compulsive phenomena in boys [12, 23]. These inconsistent results may be due to different sample characteristics and instruments used. We used the DAWBA criterion for defining OCS, which does not include questions about “hoarding” dimension. Collecting and hoarding symptoms are reported to be more prevalent in boys in a previous study (Alvarenga et al., submitted). Unexpectedly, OCD and OCS were not associated with increased age compared to controls, which contrasts with the literature [13, 19, 20, 22]. Our OCD group consisted of slightly older male children in comparison to other groups, even though this difference was not statistically significant.
The presence of OCS, even in the absence of full blown OCD, was associated with a higher prevalence of psychiatric comorbidities compared to controls. This finding has previously been reported in several studies [7, 10–12, 14, 20] and deserves clinical attention. Moreover, the profile of comorbidities in OCS resembled that of OCD subjects [37] reaching statistical similarity to the presence of social phobia, anxiety disorders (grouped), oppositional defiant disorder, tic disorders and eating disorders.
Several dimensional ratings of child psychopathology suggested intermediate severity in the OCS group compared to children with OCD and unaffected controls. The patterns in “anxiety/depression,” “somatic complaints,” and “internalizing behaviors” subscales of the CBCL reported in our sample are aligned with previous assessments in clinical OCD [16]. Furthermore, these behavioral patterns are commonly observed in anxiety and mood disorders which were much more prevalent in the OCD and OCS groups compared to controls. The patterns of “rule-breaking,” “aggression,” and “externalizing behaviors” in pediatric OCD have not been as emphasized in the literature [16, 38] although they have been more frequently reported in Tourette syndrome (an OCD spectrum disorder) and tic-related OCD [39]. In our sample, the externalizing and disruptive behaviors may be a directly consequence of the high rate of externalizing comorbidities associated with OCS and OCD groups (as ADHD and disruptive disorders), likewise previously described in the literature [38]. However, the mentioned behaviors may be associated, in part, to the very nature of OCS, which leads to behaviors like confrontation, opposition, and aggression. These combative and deregulated behaviors are often associated with increased family accommodation to symptoms which is associated with OCD poor prognosis [40].
The OCS group showed intermediate scores between OCD (greater impairment) and control groups (lower impairment) concerning reduced social skills, reduced positive behaviors, and increased maladaptive behaviors by SDQ. It is possible that children with OCS already manifest neuropsychological deficits in the social and emotional spheres that have been consistently described in OCD [41].
Regarding functionality, OCD and OCS groups showed a continuous phenotype. It is worth mentioning that previous studies report academic problems and an increased risk of delinquent behaviors in full-blown OCD, but not in OCS [11, 15]. This contradicts our findings that children with OCS also have more behavioral problems and academic and functional impairment compared to the children in the control group. These findings are plausible since executive functioning deficits have been reported in subclinical OCD [42, 43] and also in non-affected first degree relatives of OCD patients [44]. In this sense, more work needs to be done to establish how best to intervene, especially with children who present with sub-threshold OCD and OCD analogs [45].
Finally, we also found more patients in the OCD and OCS groups that had previously sought mental health services (an indirect measure of psychopathology) compared to controls. This is consistent with the literature [11, 46]. However, although a higher number of individuals in the OCD and OCS groups had previously sought mental health services in comparison to controls, only 11.7 % of subjects from the OCD group had sought (or were referred to) mental health services [8, 13]. It is possible that this phenomenon is related to the disease’s clinical features (e.g.: feelings of “shame”, and need for “secrecy”) and a tendency to avoid situations that prompt their obsessive–compulsive thoughts and behaviors [4, 47]. Another explanation for this finding could be the shortage of available mental health services in low and middle income countries, like Brazil [48].
This study must be considered in light of its limitations. Although the categorical diagnoses of OCS and OCD complied with the DSM-IV [27] definitions, they were adapted from the DAWBA [26] items. Moreover, although trained clinicians made the diagnoses, their diagnoses were not independently validated. The absence of multiple informants reduces the confidence of data, especially for OCD due to the need of many patients to be secretive regarding their OCS. Finally, the study included a proportion of “at-risk” children, which limits generalization of our data.
However, these limitations do not preclude the relevance of the main findings of this study; videlicet, OCS group is similar to OCD or holds the middle ground between full-blown OCD and control group in the presence (and type) of comorbidities, specific behavioral and social problems, clinical impact and impaired functioning. Data from this study provide further evidence that there is a psychopathological and clinical continuum between OCS and OCD, which is important not only in enhancing the understanding of the nature of OCD but in developing new diagnostic and treatment guidelines. Prospective longitudinal studies are needed to advance our understanding of the nature and course of this OCS–OCD continuum and when and how best to intervene.
References
Fontenelle LF, Mendlowicz MV, Versiani M (2006) The descriptive epidemiology of obsessive-compulsive disorder. Prog Neuropsychopharmacol Biol Psychiatry 30(3):327–337
Ruscio AM, Stein DJ, Chiu WT, Kessler RC (2010) The epidemiology of obsessive-compulsive disorder in the national comorbidity survey replication. Mol Psychiatry 15(1):53–63
Kessler RC, Berglund P, Demler O, Jin R, Merikangas KR, Walters EE (2005) Lifetime prevalence and age-of-onset distributions of DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 62(6):593–602
Alvarenga PG, Mastrorosa RS, Rosário MC (2012) Obsessive-compulsive disorder in children and adolescents. In: Rey JM (ed) The IACAPAP textbook of child and adolescent mental health, 1st edn. IACAPAP, Paris
De Mathis MA, Diniz JB, Hounie AG, Shavitt RG, Fossaluza V, Ferrão Y, Leckman JF, de Bragança Pereira C, do Rosario MC, Miguel EC (2013) Trajectory in obsessive-compulsive disorder comorbidities. Eur Neuropsychopharmacol 23(7):594–601
Fleitlich-Bilyk B, Goodman R (2004) Prevalence of child and adolescent psychiatric disorders in southeast Brazil. J Am Acad Child Adolesc Psychiatry 43(6):727–734
Zohar AH, Ratzoni G, Pauls DL, Apter A, Bleich A, Kron S, Rappaport M, Weizman A, Cohen DJ (1992) An epidemiological study of obsessive-compulsive disorder and related disorders in Israeli adolescents. J Am Acad Child Adolesc Psychiatry 31(6):1057–1061
American Academy of Child and Adolescent Psychiatry (AACAP) (2012) Practice parameters for the assessment and treatment of children and adolescents with obsessive. J Am Acad Child Adoles Psych 51(1):98–113
Apter A, Pauls DL, Bleich A, Zohar AH, Kron S, Ratzoni G, Dycian A, Kotler M, Weizman (1996) Obsessive-compulsive characteristics: from symptoms to syndrome. J Am Acad Child Adolesc Psychiatry 35(7):907–912
Bruijn C, Beun S, de Graaf R, ten Have M, Denys D (2010) Subthreshold symptoms and obsessive-compulsive disorder: evaluating the diagnostic threshold. Psychol Med 40(6):989–997
Canals J, Hernández-Martínez C, Cosi S, Voltas N (2012) The epidemiology of obsessive-compulsive disorder in Spanish school children. J Anxiety Disord 26(7):746–752
Flament MF, Whitaker A, Rapoport JL, Davies M, Berg CZ, Kalikow K, Sceery W, Shaffer D (1998) Obsessive compulsive disorder in adolescence: an epidemiological study. J Am Acad Child Adolesc Psychiatry 27(6):764–771
Heyman I, Fombonne E, Simmons H, Ford T, Meltzer H, Goodman R (2001) Prevalence of obsessive-compulsive disorder in the British nationwide survey of child mental health. Br J Psychiatry 179:324–329
Shams G, Foroughi E, Esmaili Y, Amini H, Sheehan END, Lecrubier Y (2011) Prevalence rates of obsessive-compulsive symptoms and psychiatric comorbidity among adolescents in Iran. Acta Med Iran 49(10):680–687
Voltas N, Hernández-Martínez C, Arija V, Aparicio E, Canals J (2013) A Prospective Study of Paediatric Obsessive-Compulsive Symptomatology in a Spanish Community Sample. Child Psychiatry Hum Dev 28(3):377
Black DW, Gaffney GR (2008) Subclinical obsessive-compulsive disorder in children and adolescents: additional results from a “high-risk” study. CNS Spectr 13:54–61
Fullana MA, Mataix-Cols D, Caspi A, Harrington H, Grisham JR, Moffitt TE, Poulton R (2009) Obsessions and compulsions in the community: prevalence, interference, help-seeking, developmental stability, and co-occurring psychiatric conditions. Am J Psychiatry 166(3):329–336
Flament M (1990) Epidemiology of obsessive-compulsive disorder in children and adolescents. Encephale 16:311–316
Valleni-Basile LA, Garrison CZ, Jackson KL, Waller JL, McKeown RE, Addy CL et al (1994) Frequency of obsessive-compulsive disorder in a community sample of young adolescents. J Am Acad Child Adolesc Psychiatry 33(6):782–791
Essau CA, Conradt J, Petermann F (2000) Frequency, comorbidity, and psychosocial impairment of anxiety disorders in German adolescents. J Anxiety Disord 14(3):263–279
Vivan AD, Rodrigues L, Wendt G, Bicca MG, Braga DT, Cordioli AV (2013) Obsessive-compulsive symptoms and obsessive-compulsive disorder in adolescents: a population-based study. Rev Bras Psiquiatr 18:111
Fullana MA, Vilagut G, Rojas-Farreras S, Mataix-Cols D, de Graaf R, Demyttenaere K, Haro JM, de Girolamo G, Lépine JP, Matschinger H, Alonso J (2010) Obsessive-compulsive symptom dimensions in the general population: results from an epidemiological study in six European countries. J Affect Disord 124(3):291–299
Mahfouz AA, Al-Gelban KS, Al Amri H, Khan MY, Abdelmoneim I, Daffalla AA, Shaban H, Mohammed AA (2009) Adolescents’ mental health in Abha city, southwestern Saudi Arabia. Int J Psychiatry Med 39(2):169–177
Salum GA, Gadelha A, Pan P, Moriyama TS, Graeff-Martins AS, Tamanaha AC, Alvarenga, PG, Krieger FV, Fleitlich-Bilyk B, Jackowski A, Sato JR, Brietzk, E Polanczyk GV, Brentani E, J, Mari JJ, do Rosário MC, Manfro GG, R. Bressan RA, Mercadante MT, Miguel EC, Rohde LA (2014) High risk cohort study for psychiatric disorders in childhood: rationale, design, methods and preliminary results. Int J Method Psych Res (in press)
Jannuzzi PM, Baeninger R (1996) Qualificação socioeconômica e demográfica das classes da escala Abipeme. Rev Adm São Paulo 31(3):82–90
Goodman R, Ford T, Richards H, Meltzer H, Gatward R (2000) The Development and Well-Being Assessment: description and initial validation of an integrated assessment of child and adolescent psychopathology. J Child Psychol Psychiatry 41:645–657
Association American Psychiatric (ed) (1994) Diagnostic and statistical manual of mental disorders, 4th edn. APA, Washington (DC)
Goodman A, Heiervang E, Fleitlich-Bilyk B, Alyahri A, Patel V, Mullick MS, Slobodskaya H, Dos Santos DN, Goodman R (2012) Cross-national differences in questionnaires do not necessarily reflect comparable differences in disorder prevalence. Soc Psychiatry Psychiatr Epidemiol 47(8):1321–1331
Achenbach TM (1991) Integrative Guide to the 1991 CBCL/4-18, YSR, and TRF Profiles, 1st edn. University of Vermont, Burlington VT
Bordin IA, Rocha MM, Paula CS, Teixeira MC, Achenbach TM, Rescorla LA, Silvares EF (2013) Child Behavior Checklist. Youth Self-Report and Teacher’s Report Form: an overview of the development of the original and Brazilian versions. Cad Saude Publica 29(1):13–28
Goodman R (1997) The Strengths and Difficulties Questionnaire: a research note. J Child Psychol Psychiatry 38(5):581–586
Milne BJ, Caspi A, Crump R, Poulton R, Rutter MR, Sears MR, Moffitt TE (2009) The validity of the family history screen for assessing family history of mental disorders. Am J Med Genetics 150(1):41–49
Bolstad WM (2007) A set of R functions and data sets for the book Introduction to Bayesian statistics, 1st edn. John Wiley & Sons, New York NY
Yandell BS (1997) Practical data analysis for designed experiments, 1st edn. Chapman & Hall, London UK
Agresti A (2002) Categorical data analysis, 2nd edn. Wiley, New York
Siegel C (ed) (1988) Nonparametric statistics for the behavioral sciences, 2nd edn. McGraw–Hill, New York
Geller DA (2006) Obsessive-compulsive and spectrum disorders in children and adolescents. Psychiatr Clin North Am 29(2):353–370
Lebowitz ER, Omer H, Leckman JF (2011) Coercive and disruptive behaviors in pediatric obsessive-compulsive disorder. Depress Anxiety 28(10):899–905
Termine C, Balottin U, Rossi G, Maisano F, Salini S, Di Nardo R, Lanzi G (2006) Psychopathology in children and adolescents with Tourette’s syndrome: a controlled study. Brain Dev 28(2):69–75
McGuire JF, Small BJ, Lewin AB, Murphy TK, De Nadai AS, Phares V, Geffken G, Storch EA (2013) Dysregulation in pediatric obsessive compulsive disorder. Psychiatry Res 209(3):589–595
Grisham JR, Henry JD, Williams AD, Bailey PE (2010) Socioemotional deficits associated with obsessive-compulsive symptomatology. Psychiatry Res 175(3):256–259
Kim MS, Jang KM, Kim BN (2009) The neuropsychological profile of a subclinical obsessive-compulsive sample. J Int Neuropsychol Soc 15(2):286–290
Bédard MJ, Joyal CC, Godbout L, Chantal S (2009) Executive functions and the obsessive-compulsive disorder: on the importance of subclinical symptoms and other concomitant factors. Arch Clin Neuropsychol 24(6):585–598
Rajender G, Bhatia MS, Kanwal K, Malhotra S, Singh TB, Chaudhary D (2011) Acta Psychiatr Scand. Study of neurocognitive endophenotypes in drug-naïve obsessive-compulsive disorder patients, their first-degree relatives and healthy controls 124(2):152–161
Abramowitz JS, Fabricant LE, Taylor S, Deacon BJ, McKay D, Storch EA (2004) The relevance of analogue studies for understanding obsessions and compulsions. Clin Psychol Rev 34(3):206–217
Blom RM, de Bruijn C, de Graaf R, ten Have M, Denys DA (2011) Obsessions in normality and psychopathology. Depress Anxiety 28(10):870–875
Rosário-Campos MC, Alvarenga PG, de Mathis A, Leckman JF (2008) Obsessive-compulsive disorder in childhood. In: Banaschewski T, Rohde LA (eds) Biological Child Psychiatry. Recent Trends and Developments Advances in Biological Psychiatry, Basel, pp 83–95
Moraes EN, Scivoletto S, Fossaluza V, Vieira JE, Miguel EC, Alvarenga PG (2011) Instruction in developmental psychiatry: preliminary findings at the undergraduate level in Brazil. Rev Bras Psiquiatr 33(3):287–291
Acknowledgments
The authors thank Luis Augusto Rohde, Guilherme Polanczyk, Giovanni Salum, Jilian Mulqueen and Monica Rudner for previous contributions and for help in preparing the manuscript.
Conflict of interest
Michael H. Bloch has received support from the National Institutes of Health (salary and research funding), Tourette Syndrome Association (research funding), Patterson Trust Foundation (research funding) and the Rembrandt Foundation (research funding).; James F. Leckman, MD, PhD, has received support from the National Institutes of Health (salary and research funding), Tourette Syndrome Association (research funding), Grifols, LLC (research funding), Klingenstein Third Generation Foundation (medical student fellowship program), John Wiley and Sons (book royalties), McGraw Hill (book royalties), and Oxford University Press (book royalties).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Alvarenga, P.G., do Rosario, M.C., Cesar, R.C. et al. Obsessive–compulsive symptoms are associated with psychiatric comorbidities, behavioral and clinical problems: a population-based study of Brazilian school children. Eur Child Adolesc Psychiatry 25, 175–182 (2016). https://doi.org/10.1007/s00787-015-0723-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-015-0723-3