Abstract
Objectives
To evaluate the biaxial flexural strength (BFS), flexural modulus (BFM), and Knoop microhardness (KHN) of incremental and bulk-filled resin-based composites (RBCs) using extended curing exposure times.
Materials and methods
Disc specimens (n = 8; 6-mm diameter) were fabricated using three stacked molds (0.5-mm thick for the top and bottom molds, and a 1-mm-thick center mold for the conventional and 3-mm thick for the bulk-fill RBCs). Conventional (Tetric EvoCeram/TCE and Filtek Z250/FIZ) and bulk-fill RBCs (Tetric EvoCeram Bulk Fill/TBF and Filtek One Bulk Fill Restorative/FOB) were evaluated. The stacked RBC-filled molds were light-cured for (1) the manufacturer-recommended exposure (MRE) duration; (2) 50%, and (3) 100% extension of the MRE. The BFS, BFM, and KHN of the top and bottom discs were measured. BFS and BFM were analyzed by three-way ANOVA (material*curing time*depth) and Tukey’s post hoc (α = 0.05). KHN was analyzed by two-way ANOVA (curing time*depth) and Tukey’s post hoc (α = 0.05).
Results
Extending the exposure duration did not change the BFS and BFM on the top of the RBCs, but the BFS and KHN increased at the bottom of bulk-fill RBCs. For the conventional RBCs, TCE showed the highest increase on BFS at the bottom, going from 53.6 MPa at T1 to 69.9 at T3. Among the bulk-fill RBCs, FOB presented the highest increase on the bottom BFS (T1: 101.0 ± 19.9 MPa, T3: 147.6 ± 12.9 MPa). For all RBCs and exposure times, BFS and KHN were lower at the bottom. Only FIZ and FOB reached a bottom-to-top hardness ratio of 80%, at T3 and T2.
Conclusion
A significant increase on the BFS and KHN on the bottom of bulk-fill RBCs can be observed when the time of exposure to the curing light is double the MRE. However, extended exposure does not eliminate differences on the BFS and KHN between the shallow and deep regions of RBCs. TCE and TBF failed to reach an acceptable B/T hardness ratio at all evaluated exposure times.
Clinical relevance
Mechanical properties of RBCs can be affected by insufficient polymerization, specially at deeper regions of the increment. Therefore, clinicians should consider applying twice the MRE to curing-light to polymerize the maximal increment thickness of bulk-fill RBCs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Commercial resin-based restorative composites (RBCs) must demonstrate an adequate level of photopolymerization at a specific depth and this information is provided in the manufacturer’s instructions for use [1,2,3,4,5]. Studies demonstrate that even when the most superficial regions of an RBC is properly light-cured, the deeper regions may not polymerize adequately [6,7,8,9,10,11]. Quantification of the limitation of light activation at depth within a light-cured RBC is known as its depth of cure (DOC). This concept is defined as the depth at which the resin matrix transitions from a glassy material to a rubbery state [8] and measures the capability of a RBCs to reach an acceptable monomeric conversion at an specific thickness [12], which is related to the attenuation of the light-curing wavelength as it passes through the material [4, 13,14,15].
Analysis of the DOC on light-cured RBCs is important because many factors limit the ability of RBCs to achieve optimal photopolymerization at depth, such as incorrect operator technique [16, 17], inadequate matching of curing light emission spectrum with the needs of photoinitiators within the RBC [11, 17,18,19,20], the RBC shade [9, 10, 17], and general limitations of the material to achieve a satisfactory DOC [9, 11, 12, 20, 21]. Clinically, inadequate polymerization of RBCs has been associated to clinical complications like cytotoxicity [17], marginal leakage [17, 22], discoloration [17], and reduced wear resistance [23], hardness [9, 19, 23], and bond strength [17, 24]. Those potential negative effects may be even more pronounced when the RBCs are light-cured at the maximal increment depth. Hence, to ensure that adequate and sufficient radiant energy is supplied at depths within a RBC increment, some authors suggest extending the manufacturer-recommended exposure (MRE) duration [6, 25,26,27,28] by as long as twice that value [6]. On the other hand, extension of the exposure duration must be performed carefully because it also increases the polymerization shrinkage stress and causes heating of the restorative material as well as of dental and soft oral tissues [15, 16].
The purpose of applying an extended exposure is to compensate for light attenuation in deeper regions [14, 27, 29] by supplying additional photons during the light-curing cycle. The effects of increasing the exposure on the DOC have been evaluated by different methods, such as measuring the degree of conversion of double bonds at different depths [30,31,32,33], removing of the uncured polymer using solvents [6, 21, 32, 34], or manually scraping away uncured material [6, 8, 32,33,34,35]. However, analysis of mechanical properties such as flexural strength [25, 36, 37], flexural modulus [25, 36], and microhardness with greater RBC thickness [11, 17, 29, 36,37,38,39] may also provide important information of a material under specific conditions. Despite the importance of mechanical evaluation of restorative materials, the traditional three-point bending method to evaluate flexural strength of RBCs [35] lacks clinical relevance regarding the influence of light curing, because several overlapping light-curing cycles are required to fabricate the 25-mm length specimens [25, 36].
Therefore, a modified technique for analysis of biaxial flexural strength (BFS) [25, 36, 37, 40, 41] has been recommended as a more clinically relevant method for flexural strength analysis on light-cured RBCs. Also, measuring the microhardness at the top and deeper regions of an RBC increment may allow to determine if the material has reached a bottom-to-top hardness ratio of at least 80% [9, 29, 38, 42], hence resulting in an acceptable DOC. This correlation is of great significance because the physical properties are directly related to the adequacy of the polymerization reaction of the material [9, 18, 25, 36, 38, 43, 44]. In short, a lower degree of monomer conversion at deeper regions causes a reduction in the mechanical properties of RBCs, and the analysis of these effects may provide clinical guidance about the consequences of compensating the light attenuation by extending the light-curing time beyond the MRE [25, 44].
The purpose of this study was to evaluate the effect of extended light exposure durations past those using the MRE on the BFS, biaxial flexural modulus (BFM), and Knoop microhardness (KHN) two conventional (incrementally placed) and two bulk-fill RBCs. The research hypotheses were that extension of the exposure duration past the MRE values would result in (1) a significant increase of BFS and BFM at the bottom 0.5-mm-thick layer of both types of RBCs compared to use of the MRE values, (2) significantly different BFS or BFM values at the bottom and top 0.5-mm-thick layers of the RBC increment, (3) a significant increase of KHN at bottom 0.5-mm-thick layer of all RBCs compared with the MRE, and (4) similar KHN at the top and bottom 0.5-mm-thick portions of the RBCs.
Material and methods
Tested materials
Four commercially available restorative RBCs were evaluated. Two RBCs were indicated for placement using increments of ≤ 2-mm thickness: Filtek Z250 (FIZ/3 M Oral Care, St Paul, MN, USA) and Tetric EvoCeram (TCE/Ivoclar Vivadent AG, Schaan, Liechtenstein). The two other RBCs were high-viscosity, bulk-fill materials intended for single increment thicknesses between 4 and 5 mm: Filtek One Bulk Fill (FOB/3 M Oral Care, St Paul, MN, USA) and Tetric EvoCeram Bulk Fill (TBF/Ivoclar Vivadent AG, Schaan, Liechtenstein). The composition, shades, lot number, and exposure durations used for the tested RBCs are presented in Table 1.
Biaxial flexural strength and flexural modulus
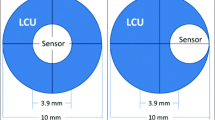
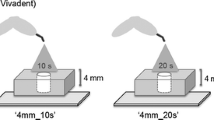
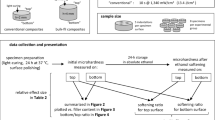
A schematic representation of the specimen fabrication and testing procedures is presented in Fig. 1. A previously reported method for measurement of BFS and BFM was followed [25, 36, 37]. Three cylinder-shaped specimens were fabricated using a set of 3D printed poly-lactic acid molds that were stacked in an aluminum holding jig having two vertical guides to hold the RBC-filled molds. For all evaluated RBCs, the three molds were filled, and light-cured as a single cylinder that could be disassembled into three separate parts. For all RBCs, the top and bottom molds were 0.5-mm thick, and for FIZ and TCE, the middle mold was 1-mm thick (2-mm total RBC cylinder height), while for FOB and TBF, the middle mold was 3-mm thick (4-mm total RBC cylinder height).
Schematic representation of sample preparation and testing. (A) A polyester strip was placed at the flat bottom surface of the holding jig and the first 0.5-mm-thick mold was inserted and filled with the corresponding uncured composite material; (B) a second polyester strip was placed over the filled mold and a new, unfilled mold was placed above the previously filled mold, and the unpolymerized restorative material was inserted. For the conventional resin composite, the second mold had 1-mm thickness, and for the bulk-fill materials, the mold was 3 mm in thickness; (C) a third, 0.5-mm thick, mold was stacked and filled using the same procedure and light-cured for the pre-determined time; (D) the resulting composite disc had a diameter of 6 mm and was 0.5-mm thick. The discs were identified as to the surface that faced the curing light before removal from the molds for testing; (E) the discs were placed in a custom-made jig and subjected to the piston-on-ring biaxial test using a universal testing machine; (F) the fractured specimens were recovered and Knoop microhardness was measured three times (in three different locations) to obtain the mean KHN of the bottom and top samples
The bottom surface of the holding jig presented a flat, unpolished surface where a transparent polyester strip (Mylar, 0.05-mm thick; DuPont, Wilmington, DE, USA) was positioned. The bottom-most, empty mold (with 0.5-mm thick) was placed over the polyester strip. This mold was slightly overfilled with the corresponding RBC and covered with another polyester strip (Fig. 1A), the combination of which were then subjected to vertical pressure applied to displace the uncured material towards the walls of the mold and to extrude excess RBC. The middle mold (1-mm or 3-mm thick) was placed over the second polyester strip of the bottom mold, filled with the RBC (Fig. 1B), and another polyester strip was placed on the top of the middle mold, followed by the same application of vertical pressure [25]. Finally, the top-most mold (third one) was placed over the stacked molds and the same filling procedure (polyester strip placement and vertical pressure) was performed.
The assembly was light-cured using a light-curing unit (LCU) fabricated by the same manufacturer of each RBC (Fig. 1C). Thus, emitting light with an optimized spectrum for the photoinitiator composition of each RBC. The products FIZ and FOB were light-activated using a blue, monowave LCU (Elipar Deep Cure-S, 3 M Oral Care, St Paul, MN, USA; 1200 mW/cm2 radiant exitance), while TCE and TBF were light-activated using a Polywave® LCU (Bluephase Style, Ivoclar Vivadent AG, Schaan, Liechtenstein; 1077 mW/cm2 radiant exitance). The output of the selected LCU was measured using a NIST traceable 6″ integrating sphere (LabSphere, Sutton, NH, USA) connected to a small spectrometer (USB 2000, Ocean Optics, Dunedin, FL, USA) [45]. The emitting end of the LCUs was positioned by gently touching the surface of the strip (at 0-mm distance from the polyester-covered surface of the top-most mold) [36]. The exposure duration used was either the MRE time (T1) or was extended by 50% (T2) or a 100% to double the exposure (T3) (Table 1). After exposure, the resulting “composite disc stacks” were disassembled into three separate discs (Fig. 1D). The top and bottom, 0.5-mm-thick discs were marked to identify the surface facing the curing light and were kept for 24 h in a dark oven (Stabil-Therm, Blue M Electric Company, Blue Island, IL, USA) at 37 °C ± 1 °C and 100% humidity.
The dimensions of top and bottom discs were measured using a digital caliper (MDC-Lite, Mitutoyo Corporation, Kanagawa, Japan). Each disc was individually placed into a custom-made jig and subjected to the piston-on-ring biaxial test (Fig. 1E) [25], using a universal testing machine (Model 5844, Instron Corp., Canton, MA, USA), at a crosshead speed of 1.27 mm/min, until failure [36, 37, 40, 41]. The maximum load at failure was recorded and the BFS and BFM values were calculated using software (SRS Biaxial Testing Software, Instron Corp., Canton, MA, USA) and expressed in MPa, using a previously reported method [36, 37, 40, 41].
Knoop microhardness
The fragments of tested discs were recovered and inspected at 40 × magnification, using the optical microscope assembled into the hardness tester to identify areas that were free of any sign of stress deformation or cracks. Those areas were used to measure the top and bottom microhardness (KNN) of the RBC segments (Fig. 1F). A microhardness tester (Future-Tech FM Corp, Tokyo, Japan) coupled to software (FM-ARS 9000, Future-Tech FM Corp) applied a single static load of 50 g (0.49 N) for 5 s at each disc segment (Fig. 1F) [9]. A total of three microhardness measurements were performed in each sample and averaged to obtain the mean KHN value for the top as well as the bottom of a single disc specimen. The bottom-to-top disc hardness (B/T) ratio of each stack was determined by dividing the hardness of the top of the bottom 0.5-mm-thick disc by the top microhardness of the top 0.5-mm-thick disc [38].
Statistical analyses
The statistical analyses for BFS and BFM were performed separately for the conventional and the bulk-fill RBCs. Data was analyzed for homogeneity and normality (Levene and Shapiro–Wilk test). To attain normality, the data received a logarithmic transformation and were then subjected to three-way ANOVA (factors: material, depth, and exposure duration). Tukey’s post hoc tests were used to detect significant differences between pairwise group comparisons (pre-set α = 0.05). For the KHN data, each material was individually analyzed for homogeneity and normality (Levene and Shapiro–Wilk tests, respectively) and was then subjected to two-way ANOVAs (factors: depth and exposure duration). Tukey post hoc test was used to identify significant differences between pairs of groups (pre-set α = 0.05). The B/T ratio was analyzed for homogeneity and normality (Levene and Shapiro–Wilk tests, respectively) and subjected to two-way ANOVA (factors: material and exposure duration) separately for the conventional and the bulk-fill RBCs followed by Tukey post hoc test for group comparisons (pre-set α = 0.05) and Dunnett post hoc test (pre-set α = 0.05) to compare each group against a reference value established in the literature as an acceptable B/T ratio [9, 21, 38]. All statistical analyses were performed using a personal computer and statistical software (SPSS Statistics for Windows, Version 23, IBM SPSS, Armonk, NY, USA).
Results
Biaxial flexural strength and flexural modulus
Mean BFS and BFM data are presented in Table 2. Statistical analyses for BFS of the conventional RBCs indicated that the material (p < 0.001) and depth (p < 0.001) factors significantly influenced the results. The exposure duration did not produce significant differences (p = 0.3851), nor did the interactions between factors. For the bulk-fill RBCs, material (p < 0.001), depth (p < 0.001), and exposure duration (p < 0.001) significantly influenced the results, as well as the double interaction between depth and exposure duration (p < 0.001).
For all the evaluated RBCs and exposure durations, the BFS of the top 0.5-mm-thick portion was significantly higher than at the bottom 0.5-mm-thick layer. Also, a significant increase on the BFS at the bottom 0.5-mm-thick surface of the bulk-fill RBCs was observed on the T3 exposure, compared to T1. For TBF, the BFS increased from 51.9 ± 6.5 MPa at T1 to 67.1 ± 8.6 MPa at T3. In the case of FOB, T1 produced a BFS of 101.0 ± 19.9 MPa, while T3 resulted on a BFS of 147.6 ± 12.9 MPa. Comparison among RBCs showed that FIZ and FOB presented significantly higher BFS, regardless of the depth and exposure duration than TCE and TBF.
The analyses of BFM data indicated that, for the conventional RBCs, the material (p < 0.001) significantly influenced the test results, but the exposure time (p = 0.3085) and depth (p = 0.1722) did not. For the bulk-fill RBCs, both material (p < 0.001) and depth (p < 0.001), as well as the double interaction between material and depth (p = 0.0055), significantly affected the test results. For TBF, at all the evaluated exposure durations, BFM values at the top 0.5-thick layer were significantly higher than those at the bottom 0.5 mm. Conversely, there were no significant differences in BFM for the other evaluated RBCs (TCE, FIZ, and FOB). Also, increasing the exposure duration did not increase BFM within the top 0.5-mm-thick layer of any of the evaluated RBCs. Comparison among materials did not show significant differences in the BFM of any of the evaluated materials at the top surface. At the bottom 0.5-mm-thick disc, the BFM of FIZ and FOB were significantly higher than those of TCE and TBF respectively.
Knoop microhardness
Surface microhardness results are presented in Table 3. For TCE, factors depth (p ˂ 0.001) and exposure duration (p = 0.001) significantly influenced the results, which is confirmed because for TEC, the lowest KHN was observed at the bottom surface, using the MRE (13.2 ± 1.2). The same tendency was observed for FIZ (depth: p ˂ 0.001; time: p = 0.004), TBF (depth: p ˂ 0.001; time: p = 0.004), and FOB (depth: p ˂ 0.001; time: p ˂ 0.001). TBF showed the highest KHN improvement of all the evaluated RBCs related to extended exposure, both at the top (T1: 37.7 ± 5.9; T2: 46.0 ± 3.8; and T3: 48.4 ± 5.5) and bottom measurements (T1: 9.9 ± 5.8; T2 14.4 ± 3.3; and T3: 18.5 ± 3.1).
For all RBCs, microhardness was always higher at the top 0.5-mm-thick layer than at the bottom (p < 0.05), regardless of the time of exposure. Extending the curing time past MRE values tended to increase microhardness of all RBCs, regardless of the location, except for FIZ at the top (p < 0.05), which showed little change, going from 62.6 ± 6.5 at T1 to 65.3 ± 9.3 and 65.8 ± 7.8 at T2 and T3 respectively. The double interaction between depth and time was not significant for any of the evaluated materials (p > 0.05).
Bottom-to-top hardness ratio
The results of B/T ratio for all materials and exposure durations are presented in Fig. 2. For the conventional RBCs, the factors exposure duration (p = 0.001) and material (p ˂ 0.001) significantly influenced the B/T ratio. The double interaction between exposure duration and material was also significant (p = 0.013). Analysis of this interaction showed that for TEC, there were no significant differences between the evaluated exposure durations, reaching a B/T ration of 43% for T1 and 46% for T2 and T3. However, for FZI, the B/T ratio presented significant differences between the T1 (57%) and T2 (65%) (p = 0.043), T1 and T3 (76%; p ˂ 0.001), and T2 and T3 (p = 0.005), with a tendency to increase with the extension of the exposure duration. The Dunnet post hoc test identified significant differences between the reference value and all the evaluated conditions except for FZI at the T3 exposure duration (p = 0.460).
Mean bottom-to-top microhardness ratios of the evaluated composites using different exposure durations. Statistical analysis was performed separately for conventional and bulk-fill materials (p > 0.05). Similar uppercase letters indicate no significant differences between exposure durations, within the same material. Similar lowercase letters indicate no significant difference between materials, within the same exposure duration. An asterisk (*) indicates significant difference between the acceptable 80% threshold for the bottom-to-top microhardness ratio (represented by the dotted red line) and the evaluated condition. T1, the manufacturer-recommended time; T2, 50%; T3, 100% extension of the exposure duration
For the bulk-fill RBCs, the factors exposure duration (p ˂ 0.001) and material (p ˂ 0.001) influenced the results. Also, the double interaction between exposure duration and material was significant (p = 0.001). Analysis of the interaction showed that for TBF, the B/T ratio differed significantly only between T1 (27%) and T3 (39%; p = 0.004). On the other hand, for FOB, there were significant differences on the B/T ratio between T1 (55%) and T2 (80%; p ˂ 0.001), T1 and T3 (67%; p = 0.004), and T2 and T3 (p = 0.002). Finally, the Dunnet post hoc test identified significant differences between the reference value and all groups, except for FOB at the T2 exposure duration (p = 0.819).
Discussion
The first research hypothesis stating that the BFS and BFM at the bottom layer of the RBCs materials would be increased by the longer exposure durations was partially rejected, because significant increases in BFS were observed only for the bulk-fill RBCs, and there were no changes on the BFM associated with extending light exposure duration. As expected, the extension of the exposure time did not result in a significant change in the BFS and BFM at the top 0.5-mm-thick layer of any of the evaluated RBCs. Also, the BFS at the bottom of TCE and FIZ (the two incremental RBCs) did not significantly increase following extension of the exposure duration past that recommended by the manufacturer. Conversely, the BFS of both bulk-fill RBCs (TBF and FOB) significantly increased when the recommended exposure duration was doubled, although the bottom 0.5-mm-thick BFS was lower than at the top surface disc. Interestingly, extension of the recommended exposure duration did not produce a significant change in the BFM for TCE, FZI, and FOB, regardless of the measurement location.
Coincidentally, the second research hypothesis was accepted because regardless of the exposure duration, the BFS of all RBCs was significantly higher at the top 0.5-mm-thick disc location. Also, for TBF, at all the evaluated exposure durations, BFM was significantly higher at the top than at the bottom. It could be hypothesized that because the DOC is a transition from a glassy to a rubbery state in RBCs [8], a poorly polymerized material could present more “rubber-like” characteristics. Such a circumstance would be reflected as a greater tolerance to bending, which was confirmed by the significantly lower BFM, compared to the adequately polymerized, brittle, top sample from the same material. The effect of the differences between the “rubbery” and the “glassy” RBC may be enhanced in TBF by the increment thickness of 4 mm, compared to the 2-mm increment thickness used for TCE, despite the similar filler and monomer composition of the RBCs.
In general, TCE and TBF showed significantly lower BFS and BFM than FIZ and FOB. The better mechanical properties of FIZ and FOB can be explained by the higher volume content of inorganic fillers [36] and adequate monomeric conversion of the 2- and 4-mm increments, respectively [6, 25]. Previous reports indicate that the presence of pre-polymerized particles as filler, as in the case of TEC and TBF, results in a reduction on the modulus of RBCs [12, 36, 44]. Also, the effect of extension of the exposure duration on BFS at depth for TBF can be explained by a greater activation at depth of camphorquinone (CQ) by the blue light emitted from the multiple peak LCU. Because the violet light has a more limited penetrability through the material [9, 10], the TPO and Ivocerin photoinitiators are not activated at depths greater than 2 mm [10, 20]. Therefore, for a bulk-fill RBC such as TBF, increasing the exposure duration may be beneficial, because the polymerization of the most superficial regions of the increment allows a greater penetrability of blue light, to improve the polymerization of the deeper regions. For FOB, doubling the recommended exposure duration yielded a significantly higher BFS. In this case, the thickness and opacity of the restorative material reduce the passage of light. Thus, extending the exposure duration could tend to compensate for the loss of light in the deeper regions of the RBC.
The third research hypothesis stating that extending the exposure duration would significantly increase the microhardness at the bottom of the RBCs was upheld because for all the evaluated materials, doubling the recommended exposure duration resulted in a significant increase in the bottom KHN values. Also, for TCE and for both bulk-fill RBCs, this effect was also observed at the top 0.5-mm-thick surface. This result is in agreement with previous studies reporting the beneficial effect on the DOC of extending the recommended exposure duration to overcome light attenuation and to improve polymerization [6, 25, 27]. For TBF, the microhardness results are consistent with previous studies reporting lower monomeric conversion [6, 12], reflected as reduced hardness [9, 11, 12, 31] at deeper regions of this RBC. Despite containing CQ/amine as a photoinitiator system, TBF also contains the initiators TPO and Ivocerin that are sensitive to shorter wavelength violet light, resulting in a wide absorption spectrum that matches the emission spectrum of most multi-peak light-curing units. However, because violet light has limited penetration through the RBCs, TBF showed a reduced microhardness in the deepest region compared to the top measurements that fully benefit from optimal activation of all its photoinitiators [9, 10, 15, 21].
Accordingly, the fourth research hypothesis was rejected because, for all the evaluated RBC, the microhardness was significantly higher at the top of the increment than at bottom, regardless of the extension of the exposure to the curing light. Moreover, despite showing an increased KHN at the bottom and a more favorable B/T ratio, when the exposure time was extended, only FIZ at the T3 and FOB at the T2 exposure duration reached a B/T ratio statistically similar to 80%. The microhardness of CQ-based materials (FIZ and FOB) has been documented to be least affected by depth [9], in comparison to TCE and TBF, and these results corroborated with a previous study that reported a decreased BFS and KHN at the deeper regions of light-curable bulk-fill RBCs [37].
The results of this study confirm that there are reduced BFS and microhardness at the bottom of the specimens, which along with the small differences on the BFM among exposure durations and measurement positions could influence the results of laboratory research, such as microtensile bond strength tests [46]. This situation could be produced by a reduction of the mechanical properties at the bottom of the RBC increment, hence increasing the number of cohesive failures on the RBC, instead of properly evaluating the bond strength of the tooth-material interface [46, 47]. Clinically, when polymerization does not occur adequately at the deeper layers of a restoration, the material may lose strength and show reduced hardness [9, 19, 38], wear resistance [17], and bond strength [17], hence becoming susceptible to clinical complications like dissolution [12, 17, 34], increased cytotoxicity [17], discoloration [17], and susceptibility to marginal defects [17]. Insufficient polymerization at depth can be influenced by factors, such as the type of photoinitiator in the material [9, 18], the filler content, type, and refraction index of the particles in the RBC [5, 36], and the wavelength of the curing light [11] that affect the penetration of light through the material.
Also, this study provided valuable information about the DOC of the tested materials, confirming that even using ideal laboratory conditions, conventional or incremental and bulk-fill RBCs may not reach the manufacturer-indicated DOC [6, 9]. Considering that the ideal parameters of accessibility, alignment, and distance of the LCU to the RBC in this research are not achievable in a clinical scenario, the clinician must be cautious and evaluate the need to perform supplementary exposure cycles to achieve adequate polymerization. Also, some materials failed to reach an acceptable B/T hardness ratio threshold, despite being evaluated at a depth shallower than the manufacturer-indicated DOC. Therefore, it may be recommendable to perform the light-curing procedures on smaller increments than the manufacturer recommended. Extension of the exposure duration past that recommended by the manufacturer ensures better mechanical properties, because there is evidence indicating that the degree of conversion of a RBC may influence mechanical properties, such as BFS and KHN [25, 31, 36, 38]. Special attention must be given to opaque or dark shades of materials because the negative effects of insufficient light received by the deeper layer of material can be enhanced. In that regard, this study confirms that increasing the manufacturer-recommended exposure duration improves the polymerization at depth of light-cured materials.
Conclusion
Within the methodological limitations of this in vitro study, the following conclusions may be stated:
-
1.
A significant increase on the BFS on the bottom region of bulk-fill RBCs can be observed when the exposure to the curing light is extended above the MRE. However, increasing the exposure time does not affect the BFM of the evaluated materials.
-
2.
Despite the extension on the exposure duration, the BFS of conventional and bulk-fill RBCs is higher at the regions closer to the curing light than at the deeper parts of the material increment.
-
3.
For conventional and bulk-fill RBCs, the KHN at bottom of the increment increased significantly when the exposure was extended beyond the MRE.
-
4.
There are significant differences on the KHN between the top 0.5-mm-thick disc and the bottom disc of the evaluated RBCs, regardless of the extension of the exposure duration by twice the MRE. Also, for most evaluated conditions, the RBCs failed to reach an acceptable B/T hardness ratio.
References
Rueggeberg FA, Giannini M, Arrais CAG, Price RBT (2017) Light curing in dentistry and clinical implications: a literature review. Braz Oral Res 31:64–91. https://doi.org/10.1590/1807-3107BOR-2017.vol31.0061
Hickey D, Sharif O, Janjua F, Brunton PA (2016) Bulk dentine replacement versus incrementally placed resin composite: a randomised controlled clinical trial. J Dent 46:18–22. https://doi.org/10.1016/j.jdent.2016.01.011
Schneider LFJ, Pfeifer CSC, Consani S et al (2008) Influence of photoinitiator type on the rate of polymerization, degree of conversion, hardness and yellowing of dental resin composites. Dent Mater 24:1169–1177. https://doi.org/10.1016/j.dental.2008.01.007
Leprince JG, Palin WM, Hadis MA et al (2013) Progress in dimethacrylate-based dental composite technology and curing efficiency. Dent Mater 29:139–156. https://doi.org/10.1016/j.dental.2012.11.005
Pfeifer CS (2017) Polymer-based direct filling materials. Dent Clin North Am 61:733–750. https://doi.org/10.1016/j.cden.2017.06.002
Romano B, Soto-Montero J, Rueggeberg F, Giannini M (2020) Effects of extending duration of exposure to curing light and different measurement methods on depth-of- cure analyses of conventional and bulk-fill composites. Eur J Oral Sci 128:336–344. https://doi.org/10.1111/eos.12703
Leprince JG, Palin WM, Vanacker J et al (2014) Physico-mechanical characteristics of commercially available bulk-fill composites. J Dent 42:993–1000. https://doi.org/10.1016/j.jdent.2014.05.009
Leprince JG, Leveque P, Nysten B et al (2012) New insight into the “depth of cure” of dimethacrylate-based dental composites. Dent Mater 28:512–520. https://doi.org/10.1016/j.dental.2011.12.004
Soto-Montero J, Nima G, Rueggeberg F et al (2020) Influence of multiple peak light-emitting-diode curing unit beam homogenization tips on microhardness of resin composites. Oper Dent 45:327–338. https://doi.org/10.2341/19-027-L
Shimokawa C, Sullivan B, Turbino M et al (2017) Influence of emission spectrum and irradiance on light curing of resin-based composites. Oper Dent 42:537–547. https://doi.org/10.2341/16-349-L
AlQahtani MQ, Michaud PL, Sullivan B et al (2015) Effect of high irradiance on depth of cure of a conventional and a bulk fill resin-based composite. Oper Dent 40:662–672. https://doi.org/10.2341/14-244-L
Jang JH, Park SH, Hwang IN (2015) Polymerization shrinkage and depth of cure of bulk-fill resin composites and highly filled flowable resin. Oper Dent 40:172–180. https://doi.org/10.2341/13-307-L
Stansbury JW (2000) Curing dental resins and composites by photopolymerization. J Esthet Dent 12:300–308
Harlow JE, Rueggeberg F, Labrie D et al (2016) Transmission of violet and blue light through conventional ( layered ) and bulk cured resin-based composites. J Dent 53:44–50. https://doi.org/10.1016/j.jdent.2016.06.007
Shimokawa CAK, Lacalle M, Giannini M et al (2018) Effect of light curing units on the polymerization of bulk fill resin-based composites. Dent Mater 34:1211–1221. https://doi.org/10.1016/j.dental.2018.05.002
André CB, Nima G, Sebold M et al (2018) Stability of the light output, oral cavity tip accessibility in posterior region and emission spectrum of light-curing units. Oper Dent 43:398–407. https://doi.org/10.2341/17-033-L
Price RB, Shortall AC, Palin WMW (2014) Contemporary issues in light curing. Oper Dent 39:4–14. https://doi.org/10.2341/13-067-LIT
Uhl A, Mills RW, Jandt KD (2003) Photoinitiator dependent composite depth of cure and Knoop hardness with halogen and LED light curing units. Biomaterials 24:1787–1795. https://doi.org/10.1016/S0142-9612(02)00532-X
Price RBT, Labrie D, Rueggeberg FA et al (2014) Correlation between the beam profile from a curing light and the microhardness of four resins. Dent Mater 30:1345–1357. https://doi.org/10.1016/j.dental.2014.10.001
Sampaio CS, Atria PJ, Rueggeberg FA et al (2017) Effect of blue and violet light on polymerization shrinkage vectors of a CQ/TPO-containing composite. Dent Mater 33:796–804. https://doi.org/10.1016/j.dental.2017.04.010
Reis AF, Vestphal M, Amaral RC, do, et al (2017) Efficiency of polymerization of bulk-fill composite resins: a systematic review. Braz Oral Res 31:37–48. https://doi.org/10.1590/1807-3107bor-2017.vol31.0059
Frassetto A, Breschi L, Turco G et al (2016) Mechanisms of degradation of the hybrid layer in adhesive dentistry and therapeutic agents to improve bond durability - a literature review. Dent Mater 32:e41–e53. https://doi.org/10.1016/j.dental.2015.11.007
Price RBT, Rueggeberg FA, Labrie D, Felix C (2010) Irradiance uniformity and distribution from dental light curing units. J Esthet Restor Dent 22:86–101. https://doi.org/10.1111/j.1708-8240.2010.00318.x
Soto-Montero J, Nima G, Dias CTDS et al (2021) Influence of beam homogenization on bond strength of adhesives to dentin. Dent Mater 37:e47–e58. https://doi.org/10.4103/jcd.jcd_47_19
Rueggeberg FA, Cole MA, Looney SW et al (2009) Comparison of manufacturer-recommended exposure durations with those determined using biaxial flexure strength and scraped composite thickness among a variety of light-curing units: Masters of esthetic dentistry. J Esthet Restor Dent 21:43–61. https://doi.org/10.1111/j.1708-8240.2008.00231.x
Misilli T, Gönülol N (2017) Water sorption and solubility of bulk-fill composites polymerized with a third generation LED LCU. Braz Oral Res 31:e80. https://doi.org/10.1590/1807-3107BOR-2017.vol31.0080
Shimokawa C, Turbino M, Giannini M et al (2020) Effect of curing light and exposure time on the polymerization of bulk-fill resin-based composites in molar teeth. Oper Dent. https://doi.org/10.2341/19-126-l
Shimokawa CAK, Price RB, Soto-Montero J, Giannini M (2021) IAAD working instructions – light curing. J Adhes Dent 23:77–78
Sadeghyar A, Watts DC, Schedle A (2020) Limited reciprocity in curing efficiency of bulk-fill resin-composites. Dent Mater 36:997–1008. https://doi.org/10.1016/j.dental.2020.04.019
Wang R, Liu H, Wang Y (2019) Different depth-related polymerization kinetics of dual-cure, bulk-fill composites. Dent Mater 35:1095–1103. https://doi.org/10.1016/j.dental.2019.05.001
Fronza BM, Rueggeberg FA, Braga RR et al (2015) Monomer conversion, microhardness, internal marginal adaptation, and shrinkage stress of bulk-fill resin composites. Dent Mater 31:1542–1551. https://doi.org/10.1016/j.dental.2015.10.001
Ferracane JL, Hilton TJ, Stansbury JW et al (2017) Academy of Dental Materials guidance—Resin composites: Part II—Technique sensitivity (handling, polymerization, dimensional changes). Dent Mater 33:1171–1191. https://doi.org/10.1016/j.dental.2017.08.188
Dewald JP, Ferracane JL (1987) A comparison of four modes of evaluating depth of cure of light-activated composites. J Dent Res 66:727–730. https://doi.org/10.1177/00220345870660030401
Price RB, Rueggeberg F, Harlow J, Sullivan B (2016) Effect of mold type, diameter, and uncured composite removal method on depth of cure. Clin Oral Investig 20:1699–1707. https://doi.org/10.1007/s00784-016-1733-3
International Standardization Organization (2009) Dentistry — polymer-based restorative materials (ISO 4049:2009). Geneva
Fronza BM, Ayres APA, Pacheco RR et al (2017) Characterization of inorganic filler content, mechanical properties, and light transmission of bulk-fill resin composites. Oper Dent 42:445–455. https://doi.org/10.2341/16-024-L
de Mendonça BC, Soto-Montero J, De CEF et al (2021) Flexural strength and microhardness of bulk-fill restorative materials. J Esthet Restor Dent 33:628–635. https://doi.org/10.1111/jerd.12727
Bouschlicher MR, Rueggeberg F, Wilson BM (2004) Correlation of bottom-to-top surface microhardness and conversion ratios for a variety of resin composite compositions. Oper Dent 29:698–704
Flury S, Peutzfeldt A, Lussi A (2014) Influence of increment thickness on microhardness and dentin bond strength of bulk fill resin composites. Dent Mater 30:1104–1112. https://doi.org/10.1016/j.dental.2014.07.001
Giannini M, Liberti MS, Arrais CAG et al (2012) Influence of filler addition, storage medium and evaluation time on biaxial flexure strength and modulus of adhesive systems. Acta Odontol Scand 70:478–484. https://doi.org/10.3109/00016357.2011.639308
Giannini M, Mettenburg D, Arrais CAG, Rueggeberg FA (2011) The effect of filler addition on biaxial flexure strength and modulus of commercial dentin bonding systems. Quintessence Int (Berl) 42:39–43
Alrahlah A, Silikas N, Watts DC (2014) Post-cure depth of cure of bulk fill dental resin-composites. Dent Mater 30:149–154. https://doi.org/10.1016/j.dental.2013.10.011
Lovell LG, Newman SM, Donaldson MM, Bowman CN (2003) The effect of light intensity on double bond conversion and flexural strength of a model, unfilled dental resin. Dent Mater 19:458–465. https://doi.org/10.1016/S0109-5641(02)00090-8
Beun S, Glorieux T, Devaux J et al (2007) Characterization of nanofilled compared to universal and microfilled composites. Dent Mater 23:51–59. https://doi.org/10.1016/j.dental.2005.12.003
Giannini M, André CB, Gobbo VC, Rueggeberg FA (2019) Accuracy of irradiance and power of light-curing units measured with handheld or laboratory grade radiometers. Braz Dent J 30:397–403
Özer F, Sengun A, Ozturk B et al (2005) Effect of tooth age on microtensile bond strength of two fluoride-releasing bonding agents. J Adhes Dent 7:289–295
Vermelho PM, Reis AF, Ambrosano GMB, Giannini M (2017) Adhesion of multimode adhesives to enamel and dentin after one year of water storage. Clin Oral Investig 21:1707–1715. https://doi.org/10.1007/s00784-016-1966-1
Funding
This project was partially supported by the Coordenação de Aperfeiçoamento de Pessoal de Nível Superior – Brasil (CAPES) – Finance Code 001, by the São Paulo Research Foundation (FAPESP grant #2017/04348–2), and by the University of Costa Rica (grant number OAICE-047–2017).
Author information
Authors and Affiliations
Contributions
B de Mendonça contributed to conceptualization and performed data acquisition and curation. J Soto-Montero was consulted on methodology, performed the statistical analysis, and wrote the original draft. E de Castro provided data acquisition and software management and edited the manuscript. M Kury contributed to data curation and supervision and proofread the manuscript. V Cavalli contributed to project administration, resources, and software and reviewed and edited the manuscript. F Rueggeberg contributed to conceptualization, funding acquisition, investigation, and supervision and proofread the manuscript. M Giannini contributed to conceptualization, methodology, funding acquisition, project administration, and supervision and proofread and edited the original manuscript.
Corresponding author
Ethics declarations
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
de Mendonça, B.C., Soto-Montero, J.R., de Castro, E.F. et al. Effect of extended light activation and increment thickness on physical properties of conventional and bulk-filled resin-based composites. Clin Oral Invest 26, 3141–3150 (2022). https://doi.org/10.1007/s00784-021-04296-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-021-04296-7