Abstract
Objectives
The aim of this study was to investigate in vitro the effect of clodronate on interleukin-1ß (IL-1ß)–stimulated human periodontal ligament fibroblasts (HPdLFs) with the focus on inflammatory factors of orthodontic tooth movement with and without compressive force.
Materials and methods
HPdLFs were incubated with 5 μM clodronate and 10 ng/mL IL-1ß. After 48 h, cells were exposed to 3 h of compressive force using a centrifuge. The gene expression of cyclooxygenase-2 (COX-2), interleukin-6 (IL-6), matrix metalloproteinase 8 (MMP-8), and the tissue inhibitor of MMP (TIMP-1) was analyzed using RT-PCR. Prostaglandin E2 (PGE-2), IL-6, and TIMP-1 protein syntheses were quantified via ELISA.
Results
Compressive force and IL-1ß induced an overexpression of COX-2 gene expression (61.8-fold; p < 0.05 compared with control), diminished by clodronate (41.1-fold; p < 0.05 compared with control). Clodronate slowed down the compression and IL-1ß induced IL-6 gene expression (161-fold vs. 85.6-fold; p < 0.05 compared with control). TNF-α was only slightly affected without statistical significance. Clodronate reduced IL-1ß-stimulated MMP-8 expression with and without compressive force. TIMP-1 on gene and protein level was downregulated in all groups. Analyzing the MMP-8/TIMP-1 ratio, the highest ratio was detected in IL-1ß-stimulated HPdLFs with compressive force (21.2-fold; p < 0.05 compared with control). Clodronate diminished IL-1ß-induced upregulation of MMP-8/TIMP-1 ratio with (11.5-fold; p < 0.05 compared with control) and without (12.5-fold; p < 0.05 compared with control) compressive force.
Conclusion
Our study demonstrates a slightly anti-inflammatory effect by clodronate under compressive force in vitro. Additionally, the periodontal remodeling presented by the MMP-8/TIMP-1 ratio seems to be diminished by clodronate.
Clinical relevance
Reduction of pro-inflammatory factors and reduction of periodontal remodeling might explain reduced orthodontic tooth movement under clodronate intake.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
During orthodontic treatment, compressive forces were applied to the tooth and transmitted to the periodontal ligament. The main cell type, human periodontal ligament fibroblasts (HPdLFs), responds with the release of inflammatory cytokines, promoting bone resorption and periodontal remodeling to enable orthodontic tooth movement [1].
Interestingly, the early phase of orthodontic tooth movement consists of an acute inflammatory response [2]. Mechanical force causes capillary vasodilatation, followed by migration of leukocytes and the release of cytokines. One cytokine playing a crucial role in orthodontics is IL-1ß. Blocking IL-1ß by a soluble receptor inhibits orthodontic tooth movement [3]. IL-1ß amplifies the inflammatory response by the release of various pro-inflammatory factors in osteoblasts and HPdLFs. Orthodontic relevant pro-inflammatory factors are prostaglandin E-2 (PGE-2), cytokines like IL-6 and TNF-α, and proteases like the matrix-metalloproteinase 8 (MMP-8). All factors are upregulated in the gingival cervical fluid under compressive force during orthodontic treatment and associated with bone and periodontal turnover [4,5,6].
Bisphosphonates were traditionally used in the therapy of metabolic bone diseases like osteoporosis. With the increasing quantity of adults seeking for orthodontic therapy, patients taking bisphosphonates during orthodontic therapy will increase [7].
The principal therapeutic effect of bisphosphonates results from a suppressed bone resorption by a direct inhibition of osteoclast activity. Due to their mechanism of action, they can be classified in two groups. The non-nitrogen-containing bisphosphonate inhibits bone resorption by synthesizing cytotoxic ATP derivatives, which induce apoptosis of osteoclasts [8]. Clodronate is a first-generation non-nitrogen-containing bisphosphonate, often prescribed and subsequently subject of studies for over 30 years [9]. In addition to the principal inhibitory effect on osteoclasts, various studies demonstrate an interaction of clodronate with other cell types including HPdLFs, endothelial cells, and osteoblasts [10, 11]. Clodronate is often discussed for its anti-inflammatory properties. In connection with this, recent studies examine the use of clodronate in the treatment of destructive inflammatory diseases like periodontitis, osteoarthritis, and acute pancreatitis [12,13,14]. In vitro, clodronate is known to change the expression of various pro-inflammatory molecules like NO [15], MMPs [14], IL-1ß [16], and TNF-α [17].
In vivo studies observed a decelerated orthodontic tooth movement under clodronate intake [18, 19]. Lotwala et al. described a prolonged treatment time and increased numbers of incomplete extraction space closure in patients taking bisphosphonates [20]. Further studies demonstrated reduced osteoclast numbers during orthodontic treatments in rats by clodronate [19]. Searching the causal molecular mechanism, Liu et al. consider the inhibitory effect of clodronate on COX-2-dependent PGE-2 production in periodontal ligament cells [21]. The interaction between compressive force and clodronate regarding their effects on cell metabolism is not clear yet.
The aim of the study was to investigate the anti-inflammatory potential of clodronate on HPdLFs under compressive force. For this, HPdLFs were stimulated by IL-1ß in vitro and exposed to clodronate as well as compressive force.
Materials and methods
Cell culture
Commercially available HPdLFs (Lonza, Basel, Switzerland) were cultured in Dulbecco’s Modified Eagle Medium (DMEM; Invitrogen, Carlsbad, USA) containing 10% fetal calf serum (FCS; Life Technologies GmbH, Darmstadt, Germany), 500 ng/mL beta fibroblast growth factor (bFGF; Life Technologies GmbH, Darmstadt, Germany), and 1% penicillin/streptomycin/neomycin. Cell characterization was provided by the manufacturers and verified via light microscopy and PCR detecting specific markers [22]. HPdLFs were incubated in a cell culture incubator with 5% CO2 and 95% air at 37 °C. When the cells reached confluence, they were detached by using 0.05% trypsin-EDTA solution (PAA, Pasching, Austria).
Bisphosphonates and interleukin-1ß
HPdLFs from passage three to six were used for this study. They were cultured in 6-well plates in the concentration of 100,000 cells/well. After 24 h of cell adhesion, medium was replaced by starvation medium containing 1% FCS. Depending on the group, recombinant human IL-1ß (R&D Systems, Minneapolis, USA) in a concentration of 10 ng/mL was added to the medium. This concentration has also been used in several studies to mimic inflammation in vitro [23,24,25]. The non-nitrogen-containing bisphosphonate clodronate (Bonefos, Bayer AG, Leverkusen, Germany) was added in a concentration of 5 μM. Previous studies showed that a concentration higher than 5 μM starts to affect cell viability significantly and lower concentrations showed absent effect [10, 26,27,28]. The incubation period was 48 h before mechanical compression.
Simulation of compressive force
Compressive force was applied on the 6-well plates by a centrifuge with swing-out rotor (Heraeus Labofuge 400, Heraeus Holding GmbH, Hanau, Germany) for 3 h at 124 g. The centrifugation force of 34.9 g/cm2 was calculated as described in the literature [29, 30].
Isolating RNA and cDNA
The peqGOLD Total RNA KIT (peqLab Biotechnology GmbH, Erlangen, Germany) was used to isolate the messenger RNA (mRNA) of the HPdLFs. The manufacturer’s protocol includes a DNase digestion step. To guarantee the quality, concentration (260) and purity (ratio, 260/280) of the mRNA were measured with the NanoDrop-Spectrophotometer ND-100 (peqLab Biotechnology GmbH, Erlangen, Germany). Reverse transcription of RNA (100 ng) was performed by standard protocol with the iScript cDNA Synthesis Kit (Biorad Laboratories, Hercules, USA) in a total volume of 20 μL and incubation in a thermal cycler (peqSTAR 96 Universal Gradient, peqLab Biotechnology GmbH, Erlangen, Germany).
Real-time PCR
The primers COX-2, IL-6, TNF-α, MMP-8, and TIMP-1 (Eurofins MWG Operon, Ebersberg, Germany) were designed with the NCBI-nucleotide library and Primer3-design. All primers had been matched to the mRNA sequences of the target genes (NCBI Blast software). As housekeeping gene, glyceraldehyde-3-phosphate dehydrogenase (GAPDH) was selected, because of the most stable expression detected by the freeware called GeNorm (Table 1).
Quantitative real-time PCR was performed with the IQ5-I-Cycler and IQ5 Optical System software version 2.0 (Bio-Rad Laboratories, Hercules, USA) according to the manufacturer’s instructions. The initial denaturation was induced at 95 °C for 5 min, followed by 40 cycles at 95 °C for 30 s (denaturation), 56 °C for 30 s (annealing), and 71 °C for 20 s (elongation). Q-PCR amplification was conducted with a reaction mixture containing SYBR Green Supermix (Biorad Laboratories, Hercules, USA), an appropriate amount of paired primers, and 2 μL template cDNA. The background was to determine the threshold at the SYBR green fluorescence curve at the exponential part. This method was applied to calculate the cycle number and CT value for quantitation.
Furthermore, the CT values of GAPDH housekeeping gene and the individual primer efficacy were taken into account. Single product formation was confirmed by melting point analysis. Data were obtained from three individual experiments and normalized to the CT of GAPDH. CDNA from individual cell experiments was analyzed in triplicate PCR. The relative expression levels of each mRNA were evaluated by using a modification of the ΔΔCT method [31].
Enzyme-linked immunosorbent assay
To verify changings on the gene expression levels of COX-2, IL-6, MMP-8, and TIMP-1, an ELISA was added for IL-6, MMP-8, TIMP-1, and the synthesis product of COX-2 and PGE-2. With regard to the time lag between gene and protein synthesis, cell culture supernatants were collected 6 h after the application of compressive force. Protein synthesis level of IL-6, MMP-8, and TIMP-1 was quantified by the DuoSet ELISA Development Kit (R&D Systems, Minneapolis, USA) and protein synthesis of PGE-2 with the Prostaglandin E2 Parameter Assay Kit (R&D Systems, Minneapolis, USA). Optical density was determined using a microplate reader (VersaMax Microplate Reader; Molecular Devices, Sunnyvale, USA) set to 450 nm, and wavelength correction was set to 540 nm. Supernatants of untreated cells were provided as controls. The experiments were performed in triplicate.
Statistical analysis
SPSS 22.0 (IBM-SPSS, Ehningen, Germany) was used for statistical analyses. Normal distributions of the results were verified by Shapiro-Wilk’s test (p > 0.05). To detect the difference between the groups, one-way ANOVA was used with the post hoc Tukey test. A p value ≤ 0.05 was considered statistically significant.
Results
Gene expression of COX-2, IL-6, and TNF-α
Stimulation of HPdLFs with IL-1ß and clodronate led to an increase of COX-2 gene expression about 71-fold compared with the control group. Compressive force induced a 4.4-fold overexpression of COX-2 compared with the control, further enhanced by the stimulation of IL-1ß (61.8-fold compared with the control cells). Combination of compressive force, IL-1ß, and clodronate reduced the overexpression to a 41.1-fold increase (Fig. 1a).
Gene expression of COX-2 (a), IL-6 (b), and TNF-α (c) in HPdLFs exposed to 5 μM clodronate in combination with 10 ng/mL IL-1ß for 48 h and to 3 h of compressive force (compression) as fold of untreated cells (control). Data were obtained from three individual experiments. Asterisks indicate significant difference compared with untreated control cells (*p < 0.05)
IL-1ß increased the IL-6 gene expression (73.6-fold compared with the control cells) in HPdLFs. Compressive force did not affect IL-6 gene expression significantly. When stimulated by IL-1ß, compressive force had an additive effect on IL-6 gene expression in HPdLFs up to a 161-fold increase compared with the control. When combined with clodronate, the IL-1ß-induced IL-6 gene expression increase was abolished (85.6-fold compared with the control cells) (Fig. 1b).
Gene expression of TNF-α was nearly doubled by IL-1ß when compared with the control, whereas the combination of IL-1ß and clodronate led to a smaller increase (1.6-fold compared with the control cells), both results without statistical significance. Compressive force had no statistical significant influence on TNF-α gene expression. Stimulation of HPdLFs with IL-1ß and compressive force slightly enhanced TNF-α gene expression with (1.3-fold compared with the control cells) and without (1.4-fold compared with the control cells) clodronate (Fig. 1c).
Protein synthesis of PGE-2 and IL-6
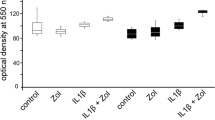
The PGE-2 protein levels in the supernatants substantiate the results at the gene expression level of its synthesizing enzyme COX-2. Neither control HPdLFs nor HPdLFs exposed to compressive force showed any verifiable PGE-2 level (≤ 9.7 pg/mL). IL-1ß-stimulated HPdLFs slightly enhanced PGE-2 protein synthesis to a detectable level with and without clodronate (134.5 pg/mL IL-1ß; 185.1 pg/mL IL-1ß and clodronate). In the presence of compressive force, IL-1ß led to a significant increase of the PGE-2 protein synthesis (1673.5 pg/mL) and combining with clodronate showed a slightly reduced effect (1436.2 pg/mL) compared with the control (Fig. 2a).
Protein synthesis of PGE-2 (a) and IL-6 (b) in HPdLFs exposed to 5 μM clodronate in combination with 10 ng/mL IL-1ß for 48 h and to 3 h of compressive force (compression) as fold of untreated cells (control). Data were obtained from three individual experiments. Asterisks indicate significant difference compared with untreated control cells (*p < 0.05)
The protein synthesis of IL-6 increased significantly in HPdLFs stimulated with IL-1ß (25,705.6 pg/mL) compared with the control (15.5 pg/mL), whereas combining with clodronate had no additional effect (25,971.7 pg/mL). Compressive force had no influence on the protein level of IL-6 (21.7 pg/mL) compared with the control. IL-1ß-induced increase of IL-6 protein synthesis with (27,149.9 pg/mL) and without (27,643.6 pg/mL) clodronate was not affected by compressive force (Fig. 2b).
Gene expression and protein synthesis of MMP-8 and TIMP-1
IL-1ß increased the gene expression of MMP-8 about 8.5-fold compared with the control group; clodronate reduced the IL-1ß-induced gene expression to a 5.4-fold increase. Compressive force led to a 2.6-fold increase and had an additive effect on IL-1ß-induced increase (9.9-fold), whereas clodronate in turn reduced gene expression level of MMP-8 to a 7.6 increase (Fig. 3a). Gene expression of TIMP-1 was reduced in all examined groups. Compressive force led to the lowest significant TIMP-1 expression (0.3-fold) followed by the combinations of IL-1ß with clodronate (0.4-fold) and compressive force with IL-1ß (0.5-fold) (Fig 3b).
Gene expression of MMP-8 (a), TIMP-1 (b), ratio of MMP-8/TIMP-1 (c), and protein synthesis of TIMP-1 (d) in HPdLFs exposed to 5 μM clodronate in combination with 10 ng/mL IL-1ß for 48 h and to 3 h of compressive force (compression) as fold of untreated cells (control). Data were obtained from three individual experiments. Asterisks indicate significant difference compared with untreated control cells (*p < 0.05)
The protein level of MMP-8 in the supernatants of all examined groups was below the measurable quantity (< 62.5 pg/mL; data not shown). Protein synthesis of TIMP-1 confirmed the results at the gene level. TIMP-1 protein level was significantly reduced in all groups compared with the control group (2197 pg/mL). Compressive force decreased protein level (1052.7 pg/mL) as well as stimulation with IL-1ß (1417.7 pg/mL). Clodronate had no further significant influence on TIMP-1 protein level in IL-1ß-stimulated HPdLFs (Fig. 3d).
The highest MMP-8/TIMP-1 gene expression ratios were measured in IL-1ß-stimulated HPdLFs (14.3-fold), particularly in combination with compressive force (21.2-fold). Clodronate diminished IL-1ß-induced upregulation with (11.5-fold) and without (12.5-fold) compressive force (Fig. 3c).
Discussion
The present study investigates the influence of clodronate on compressed HPdLFs with regard to inflammatory cytokines. Clodronate causes an anti-inflammatory effect of stimulated HPdLFs under compressive force particularly with regard to the COX-2 expression and the periodontal remodeling, represented by the MMP-8/TIMP-1 ratio.
COX-2 and PGE-2 are known to play a central role in osteoclastic bone resorption, essential for orthodontic tooth movement [32]. In accordance with this, our study detected an enhanced COX-2 expression in compressed HPdLFs. PGE-2 was under detectable level, but IL-1ß-stimulated HPdLFs with compressive force elevated PGE-2 synthesis up to the highest detected level. Studies with a similar experimental setup confirmed a COX-2-induced PGE-2 expression [22, 33].
Clodronate reduced the compression-induced COX-2 and PGE-2 expressions in IL-1ß-stimulated HPdLFs. Liu et al. also showed that clodronate could reduce the compression-induced production of PGE-2 and RANKL in the periodontal ligament [21]. Inhibition of the COX-2 expression and its derivatives could be the reason for decelerate orthodontic tooth movement. An analogical mechanism is known by NSAIDs, a potent inhibitor of the COX family. This inhibition causes decelerate tooth movement in vivo [34]. Our findings supported by the results of Liu et al. indicate that the inhibitory effect of clodronate on orthodontic tooth movement in vivo may result in part by the inhibition of COX-2-derived PGE-2 by clodronate.
In a previous study, we observed an enhancing effect of the nitrogen-containing bisphosphonate zoledronate on the IL-1ß-induced pro-inflammatory response of HPdLFs. Mechanical strain increased this pro-inflammatory effect additionally [24]. In the presented study, clodronate reduced the compression-induced pro-inflammatory response of HPdLFs to compressive force. Therefore, our results indicate that the pro-inflammatory effect of the nitrogen-containing bisphosphonates cannot be transferred to non-N-containing bisphosphonates such as clodronate. Interestingly, a recent study evidenced a protective role of clodronate toward the inflammatory N-BP side effects via inhibition of selective phosphate transporters in the cellular membrane [35]. However, the extra- and intracellular mechanisms by which clodronate exhibits its anti-inflammatory properties are still unknown. Tsubaki et al. showed an interaction of BP with the Ras/MEK/ERK and the p38MAPK pathways. The same signaling pathways are involved in the mechanotransduction of periodontal tissue remodeling markers during orthodontic tooth movement [36]. For analyzing the extra- and intracellular pathways, further studies have to be conducted to understand the way how the different factors interfere with each other.
Various cell types respond to stress factors like mechanical force by releasing the pro-inflammatory cytokine IL-1ß. IL-1ß, in turn, leads to the expression of further pro-inflammatory cytokines like IL-6 and TNF-α. IL-6 is known as an early biomarker of tooth movement [37]. It was upregulated in our study on gene expression level by compressive force combined with IL-1ß. Clodronate diminished the reaction, suggesting a slightly anti-inflammatory response of compressed HPdLFs with regard to IL-6. Clodronate without compressive force did not alter the IL-6 synthesis. Confirming this, Dehghani et al. detected a significantly reduced secretion of several pro-inflammatory cytokines in microglial cells by clodronate [17]. One of the inhibited pro-inflammatory cytokines of Dehghani et al. was TNF-α. TNF-α is a potent cytokine for osteoclast recruitment, often enhanced by mechanical stress. In accordance with other studies, compressive force did not affect TNF-α in our study [38,39,40]. Different results may take place because of different study designs and a sensitive regulation of TNF-α. With regard to the potential anti-inflammatory role of clodronate, we detected a slightly reductive effect of clodronate on IL-1ß-induced TNF-α expression.
MMP-8 levels increase in periodontal inflammation as well as in orthodontic tooth movement [41]. Llavaneras et al. investigated in vivo the effect of clodronate on bacterial-induced periodontal inflammation in a rat model [14]. They detected a reduction of the pathological elevated levels of MMPs through clodronate, accompanied by reduced tooth mobility and alveolar bone loss. We detected an inhibitory effect of clodronate on the IL-1ß-induced MMP-8 expression in the HPdLFs. Consequently in vivo, MMP-8-mediated collagen degradation may slow down and alveolar bone loss and tooth mobility might be reduced.
Mechanical force enhances MMP-8 expression in vitro and in vivo [41, 42]. Our study complements a synergistically effect of compressive force combined with IL-1ß on the MMP-8 expression, consequently inducing the highest MMP-8/TIMP-1 ratio. The balance of tissue remodeling switched to collagen degradation. Clodronate, particularly combined with compressive force, reduced the synergistically enhanced MMP-8/TIMP-1 ratio. Knowing the limits of an in vitro study and the gap to the complex in vivo situation, the downregulation of tissue remodeling genes by clodronate might be a reason for the decelerated orthodontic tooth movement.
Conclusion
This study provides a contribution to determine the role of clodronate in inflammatory processes. Clodronate demonstrated a slightly anti-inflammatory effect under compressive force with regard to COX-2, PGE-2, and IL-6. In particular, the periodontal remodeling presented by the MMP-8/TIMP-1 ratio was diminished by clodronate. This suggests apart from the direct osteoclastic inhibition an indirect influence of clodronate on the periodontal remodeling by affecting intercellular signaling molecules.
References
Lekic PC, Rajshankar D, Chen H, Tenenbaum H, McCulloch CA (2001) Transplantation of labeled periodontal ligament cells promotes regeneration of alveolar bone. Anat Rec 262:193–202
Saito M, Saito S, Ngan PW, Shanfeld J, Davidovitch Z (1991) Interleukin 1 beta and prostaglandin E are involved in the response of periodontal cells to mechanical stress in vivo and in vitro. Am J Orthod Dentofac Orthop 99:226–240
Jager A, Zhang D, Kawarizadeh A, Tolba R, Braumann B, Lossdorfer S, Gotz W (2005) Soluble cytokine receptor treatment in experimental orthodontic tooth movement in the rat. Eur J Orthod 27:1–11
Nunes L, Quintanilha L, Perinetti G, Capelli JJ (2017) Effect of orthodontic force on expression levels of ten cytokines in gingival crevicular fluid. Arch Oral Biol 76:70–75
Surlin P, Rauten AM, Mogoanta L, Silosi I, Oprea B, Pirici D (2010) Correlations between the gingival crevicular fluid MMP8 levels and gingival overgrowth in patients with fixed orthodontic devices. Romanian J Morphol Embryol 51:515–519
Grieve WG 3rd, Johnson GK, Moore RN, Reinhardt RA, DuBois LM (1994) Prostaglandin E (PGE) and interleukin-1 beta (IL-1 beta) levels in gingival crevicular fluid during human orthodontic tooth movement. Am J Orthod Dentofac Orthop 105:369–374
Scott P, Fleming P, DiBiase A (2007) An update in adult orthodontics. Dent Update 34:427–428, 431-4, 436 passim
Rogers MJ (2003) New insights into the molecular mechanisms of action of bisphosphonates. Curr Pharm Des 9:2643–2658
Schenk R, Merz WA, Muhlbauer R, Russell RG, Fleisch H (1973) Effect of ethane-1-hydroxy-1,1-diphosphonate (EHDP) and dichloromethylene diphosphonate (Cl 2 MDP) on the calcification and resorption of cartilage and bone in the tibial epiphysis and metaphysis of rats. Calcif Tissue Res 11:196–214
Jacobs C, Walter C, Ziebart T, Dirks I, Schramm S, Grimm S, Krieger E, Wehrbein H (2014) Mechanical loading influences the effects of bisphosphonates on human periodontal ligament fibroblasts. Clin Oral Investig 19:699–708
Walter C, Klein MO, Pabst A, Al-Nawas B, Duschner H, Ziebart T (2010) Influence of bisphosphonates on endothelial cells, fibroblasts, and osteogenic cells. Clin Oral Investig 14:35–41
Saviola G, Abdi-Ali L, Campostrini L, Sacco S, Baiardi P, Manfredi M, Mannoni A, Benucci M (2012) Clodronate and hydroxychloroquine in erosive osteoarthritis: a 24-month open randomized pilot study. Mod Rheumatol 22:256–263
Zhang JX, Dang SC, Yin K, Jiang DL (2011) Protective effect of clodronate-containing liposomes on intestinal mucosal injury in rats with severe acute pancreatitis. Hepatobiliary Pancreat Dis Int 10:544–551
Llavaneras A, Ramamurthy NS, Heikkila P, Teronen O, Salo T, Rifkin BR, Ryan ME, Golub LM, Sorsa T (2001) A combination of a chemically modified doxycycline and a bisphosphonate synergistically inhibits endotoxin-induced periodontal breakdown in rats. J Periodontol 72:1069–1077
Dombrecht EJ, Schuerwegh AJ, Bridts CH, Ebo DG, Van Offel JF, Stevens WJ, De Clerck LS (2007) Effect of bisphosphonates on nitric oxide production by inflammatory activated chondrocytes. Clin Exp Rheumatol 25:817–822
Ozdemir SP, Kurtis B, Tuter G, Bozkurt S, Gultekin SE, Senguven B, Watanabe K, Aydin S (2012) Effects of low-dose doxycycline and bisphosphonate clodronate on alveolar bone loss and gingival levels of matrix metalloproteinase-9 and interleukin-1beta in rats with diabetes: a histomorphometric and immunohistochemical study. J Periodontol 83:1172–1182
Dehghani F, Conrad A, Kohl A, Korf HW, Hailer NP (2004) Clodronate inhibits the secretion of proinflammatory cytokines and NO by isolated microglial cells and reduces the number of proliferating glial cells in excitotoxically injured organotypic hippocampal slice cultures. Exp Neurol 189:241–251
Choi J, Baek SH, Lee JI, Chang YI (2010) Effects of clodronate on early alveolar bone remodeling and root resorption related to orthodontic forces: a histomorphometric analysis. Am J Orthod Dentofac Orthop 138:548 e1–548 e8 discussion 548-9
Liu L, Igarashi K, Haruyama N, Saeki S, Shinoda H, Mitani H (2004) Effects of local administration of clodronate on orthodontic tooth movement and root resorption in rats. Eur J Orthod 26:469–473
Lotwala RB, Greenlee GM, Ott SM, Hall SH, Huang GJ (2012) Bisphosphonates as a risk factor for adverse orthodontic outcomes: a retrospective cohort study. Am J Orthod Dentofac Orthop 142:625–634 e3
Liu L, Igarashi K, Kanzaki H, Chiba M, Shinoda H, Mitani H (2006) Clodronate inhibits PGE(2) production in compressed periodontal ligament cells. J Dent Res 85:757–760
Proff P, Reicheneder C, Faltermeier A, Kubein-Meesenburg D, Romer P (2014) Effects of mechanical and bacterial stressors on cytokine and growth-factor expression in periodontal ligament cells. J Orofac Orthop 75:191–202
Nokhbehsaim M, Winter J, Rath B, Jager A, Jepsen S, Deschner J (2011) Effects of enamel matrix derivative on periodontal wound healing in an inflammatory environment in vitro. J Clin Periodontol 38:479–490
Jacobs C, Schramm S, Dirks I, Walter C, Pabst A, Meila D, Jacobs C, Wehrbein H (2018) Mechanical loading increases pro-inflammatory effects of nitrogen-containing bisphosphonate in human periodontal fibroblasts. Clin Oral Investig 22:901–907
Long P, Liu F, Piesco NP, Kapur R, Agarwal S (2002) Signaling by mechanical strain involves transcriptional regulation of proinflammatory genes in human periodontal ligament cells in vitro. Bone 30:547–552
Walter C, Pabst A, Ziebart T, Klein M, Al-Nawas B (2011) Bisphosphonates affect migration ability and cell viability of HUVEC, fibroblasts and osteoblasts in vitro. Oral Dis 17:194–199
Pabst AM, Ziebart T, Koch FP, Taylor KY, Al-Nawas B, Walter C (2012) The influence of bisphosphonates on viability, migration, and apoptosis of human oral keratinocytes--in vitro study. Clin Oral Investig 16:87–93
Grimm S, Walter C, Pabst A, Goldschmitt J, Wehrbein H, Jacobs C (2015) Effect of compressive loading and incubation with clodronate on the RANKL/OPG system of human osteoblasts. J Orofac Orthop 76:531–542
Diercke K, Zingler S, Kohl A, Lux CJ, Erber R (2014) Gene expression profile of compressed primary human cementoblasts before and after IL-1beta stimulation. Clin Oral Investig 18:1925–1939
Redlich M, Roos H, Reichenberg E, Zaks B, Grosskop A, Bar Kana I, Pitaru S, Palmon A (2004) The effect of centrifugal force on mRNA levels of collagenase, collagen type-I, tissue inhibitors of metalloproteinases and beta-actin in cultured human periodontal ligament fibroblasts. J Periodontal Res 39:27–32
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) method. Methods 25:402–408
Meeran NA (2013) Cellular response within the periodontal ligament on application of orthodontic forces. J Indian Soc Periodontol 17:16–20
Mitsui N, Suzuki N, Maeno M, Yanagisawa M, Koyama Y, Otsuka K, Shimizu N (2006) Optimal compressive force induces bone formation via increasing bone morphogenetic proteins production and decreasing their antagonists production by Saos-2 cells. Life Sci 78:2697–2706
Bartzela T, Turp JC, Motschall E, Maltha JC (2009) Medication effects on the rate of orthodontic tooth movement: a systematic literature review. Am J Orthod Dentofac Orthop 135:16–26
Shima K, Nemoto W, Tsuchiya M, Tan-No K, Takano-Yamamoto T, Sugawara S, Endo Y (2016) The bisphosphonates clodronate and etidronate exert analgesic effects by acting on glutamate- and/or ATP-related pain transmission pathways. Biol Pharm Bull 39:770–777
Jiang L, Tang Z (2018) Expression and regulation of the ERK1/2 and p38 MAPK signaling pathways in periodontal tissue remodeling of orthodontic tooth movement. Mol Med Rep 17:1499–1506
Ren Y, Hazemeijer H, de Haan B, Qu N, de Vos P (2007) Cytokine profiles in crevicular fluid during orthodontic tooth movement of short and long durations. J Periodontol 78:453–458
Garlet TP, Coelho U, Silva JS, Garlet GP (2007) Cytokine expression pattern in compression and tension sides of the periodontal ligament during orthodontic tooth movement in humans. Eur J Oral Sci 115:355–362
Alhashimi N, Frithiof L, Brudvik P, Bakhiet M (2001) Orthodontic tooth movement and de novo synthesis of proinflammatory cytokines. Am J Orthod Dentofac Orthop 119:307–312
Taddei SR, Moura AP, Andrade I Jr, Garlet GP, Garlet TP, Teixeira MM, da Silva TA (2012) Experimental model of tooth movement in mice: a standardized protocol for studying bone remodeling under compression and tensile strains. J Biomech 45:2729–2735
Apajalahti S, Sorsa T, Railavo S, Ingman T (2003) The in vivo levels of matrix metalloproteinase-1 and -8 in gingival crevicular fluid during initial orthodontic tooth movement. J Dent Res 82:1018–1022
Jacobs C, Walter C, Ziebart T, Grimm S, Meila D, Krieger E, Wehrbein H (2013) Induction of IL-6 and MMP-8 in human periodontal fibroblasts by static tensile strain. Clin Oral Investig 18:901–908
Funding
The work was supported by the Osteology Foundation (Lucerne, Switzerland).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Grimm, S., Wolff, E., Walter, C. et al. Influence of clodronate and compressive force on IL-1ß-stimulated human periodontal ligament fibroblasts. Clin Oral Invest 24, 343–350 (2020). https://doi.org/10.1007/s00784-019-02930-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-02930-z