Abstract
Objectives
Despite a high possibility of technique-related complications, ilio-sacral (IS) screw fixation is the mainstay of operative management in posterior pelvic ring injuries. We aimed to make IS screw trajectory with fully intraosseous path that was optimal and consistent, and confirm the possibility of transiliac–transsacral (TITS) screw fixation in Asian sacrum.
Methods
Eighty-two cadaveric sacra (42 males and 40 females) were enrolled and underwent continuous 1.0-mm slice computed tomography (CT) scans. CT images were imported into Mimics® software to reconstruct three-dimensional model of the pelvis. To simulate IS screws, we inserted 7.0-mm-sized TITS cylinder for first (S1) and second (S2) sacral segment and 7.0-mm oblique cylinder for S1. TITS cylinder could not be inserted into S1 of 14 models (sacral variation models) but could be inserted into the S2 of all models. The actual length of virtual IS screws was measured, and anatomic features of safe zone (SZS2) including the area, horizontal distance (HDS2), and vertical distance (VDS2) were evaluated by the possibility of TITS screw fixation in the S1.
Results
When the oblique cylinder was directed toward the opposite upper corner of S1 at the level of the first foramen, there was no cortical violation regardless of sacral variation. The average length of TITS cylinder was 152.3 mm (range 127.9–178.2 mm) in S1 and 136.0 mm (range 97.8–164.1 mm) in S2, and for oblique cylinder it was 99.2 mm (range 82.4–132.2 mm). The average VDS2, HDS2, and the area of SZS2 were 15.5 mm (range 8.7–24.4 mm), 18.3 mm (range 12.7–26.6 mm), and 221.1 mm2 (range 91.1–386.7 mm2), respectively. The VDS2 and SZS2 of sacral variation were significantly higher than those of normal (both p = 0.001).
Conclusions
Considering the high variability of the S1, it is better to direct the IS screw trajectory toward the opposite upper corner of the S1 at the level of first sacral foramen. If a TITS screw is needed, the transverse fixation for the S2 could be performed alternatively due to its sufficient osseous site even in Asian sacrum.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Ilio-sacral (IS) screw fixation including the transiliac–transsacral (TITS) screw placement is a technically dependent procedure because of complex posterior pelvic structures and high degree of upper sacral variability. Bone overlap, obesity, poor bone quality, and bowel gas can make it difficult to identify well-known landmarks in imaging for safe placement [1,2,3,4,5]. Accurate fluoroscopic imaging of IS screw placement is essential for verifying the distinction of sacral morphology and screw trajectory, and preventing malposition-related complications [6,7,8]. Although there have been many reports on good visualization of safe corridor and radiologic recognition of sacral variations [1, 2, 4, 9], few studies have reported the implication of IS screw placement [5, 10,11,12].
During IS screw placement, three-dimensional (3D) understanding of the safe zone is based on the surgeon’s knowledge of pelvic anatomy. This information is a prerequisite for obtaining optimal intraosseous positions in the first and second sacral segment [13]. Concerning the difference between normal and variant sacra, it is difficult to verify the degree of safe zone obliquity using conventional CT scans [14]. If the CT images were measured using picture archiving and communication system (PACS) software, its true cross-sectional area for safe IS screw placement might be overestimated or distorted because the cutting plane is not perpendicular to the sacral alar axis [4]. Thus, it might be hard to determine the expected IS screw trajectory and the possibility of TITS screw fixation for the first (S1) and second sacral segment (S2) by the usual techniques for preoperative planning. Therefore, the primary purposes of this computational simulation study were to introduce an optimal and consistent IS screw trajectory for S1 and to identify the possibility of TITS screw and its implication in Asian sacrum by simulating a virtual 7.0-mm-sized screw fixation.
Materials and methods
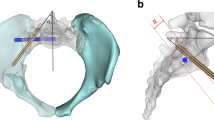
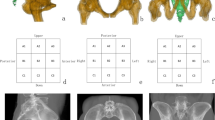
Human body digital data were collected from the Korea Institute of Science and Technology Information after approval. CT data of 105 adult cadavers who underwent continuous 1.0-mm slice CT scans (Pronto, Hitachi, Japan) in supine position were collected. None of the cadavers had pelvic problems based on medical records view. CT data in Digital Imaging and Communications in Medicine (DICOM) format were imported into Mimics® software (Materialise Interactive Medical Image Control System; Materialise, Antwerp, Belgium) to reconstruct 3D models of the pelvis including the sacrum and two iliac bones. Due to poor image quality, 23 cadavers were excluded. The remaining 82 adult cadavers (42 males and 40 females) were enrolled. Their mean age and height at death were 52.1 years (range 21–60 years, SD 9.2) and 161.3 cm (range 146–176 cm, SD 7.1), respectively. After generating the 3D pelvis model, the transparency mode of the model was adjusted to differentiate cancellous bone from sacral foramen and spinal canal. In addition, the safe zones of the first (SZS1) and second sacral segments (SZS2) for TITS screw fixation were verified [5, 10]. The surface area of SZS2, horizontal distance (HDS2), and vertical distance (HDS2) of the second sacral segment were measured using the Mimics® software (Fig. 1a–c).
To simulate the insertion of a conventional 7.0-mm IS screw into the ideal position of S1, a straight cylinder designated the ‘CAD object’ was applied using the Mimics® software. The insertion of oblique cylinder was performed over the midline in the first sacral body (Fig. 1d) [15]. Two 7.0-mm-sized transverse cylinders representing the TITS cylinders were inserted into S1 and S2. They were positioned from the outer cortex of iliac bone to the outer cortex of the opposite iliac bone (Fig. 1e, f) [15,16,17]. To verify the path of cylinders, the pelvic outlet view was adjusted as the cartilage of pubic symphysis overlays with the midline of the sacrum and the inferior border of first sacral foramen unlike prior reports [18, 19] (Fig. 2). The ideal position was defined as containment of a screw within bony confines without violating the first and second sacral foramen, spinal canal, or upper surface of the two iliac bones [5, 10, 14]. After inserting the three cylinders (two TITS cylinders and one oblique cylinder), their positions and entry points were fine-tuned and verified by an experienced surgeon (corresponding author). Due to high variability and complex plane, as well as technical issues, we failed to assess the surface area and anatomic features of SZS1. However, direct comparison between the two safe zones (SZS1 and SZS2) was possible by removing two iliac bones.
All pelvis models were divided into two groups depending on the possibility of TITS cylinder insertion for S1. In the normal group, the transverse insertion of TITS could be possible without any violation. In the sacral variation group, the insertion could not be without any violation [4, 5, 20]. Fourteen models (six female models and eight male models) were identified as sacral variation due to angulated and narrowed SZS1. The entry point and trajectory of cylinders were assessed, and the length of each cylinder was measured to identify the maximum potential length of IS screw. All measurements are presented as mean, range, and standard deviation (SD). Chi-square test and two-sample t test were used to compare means between the pelvic normal group and the variation group. Statistical significance was set at p < 0.05. SPSS statistical software package for Windows version 23.0 (SPSS Inc., Chicago, IL, USA) and R × 64 3.1.1 (R Foundation for Statistical Computing, Vienna, Austria) were used for statistical analyses.
Results
There was no statistically significant difference in sex (p = 0.626) or height (p = 0.419) between the normal and variation group. In the normal group, the average length of the oblique cylinder in S1 was 98.8 mm (range 82.4–132.2 mm, SD 8.7 mm). The average length of the TITS cylinder in S1 was 151.4 mm (range 127.9–178.2 mm, SD 9.6 mm) and 134.2 mm (range 97.8–164.1 mm, SD 10.5 mm) in S2. In the variation group, the average length of the oblique cylinder in S1 was 101.2 mm (range 90.5–110.9 mm, SD 6.1 mm) and the average length of the TITS cylinder in S2 was 144.6 mm (range 128.0–160.3 mm, SD 8.1 mm). The average length of oblique cylinder in the sacral variation group was not significantly different (p = 0.322) from that in the normal group. However, there was a statistically significant difference in the length of TITS cylinder of the second sacral segment between the two groups (p < 0.001).
The average VDS2, HDS2, and the area of SZS2 of all models were 15.5 mm (range 8.7–24.4 mm, SD 3.0 mm), 18.3 mm (range 12.7–26.6 mm, SD 2.9 mm), and 221.1 mm2 (range 91.1–386.7 mm2, SD 68.5 mm2), respectively. The average area of SZS2 was 209.6 mm2 (range 91.1–376.2 mm2, SD 65.4 mm2) in the normal group and 276.9 mm2 (range 145.4–386.7 mm2, SD 56.0 mm2) in the variation group. When the anatomic variable of second segment was compared between two groups, the VDS2 (p < 0.001) and the area of SZS2 (p = 0.001) of variation group were higher than those of the normal group. However, the HDS2 was not significantly different (p = 0.126) between the two groups.
For TITS cylinder insertion of S1, the entry point should be placed just inferior to the iliac cortical density to some extent in the true lateral view to prevent the cortical violation. Concerning the TITS cylinder insertion of S2, the ideal entry was located inferior or slightly anterior, but not posterior, compared to the entry for S1. For safe placement of oblique cylinder in sacral variation model, the height of ideal entry point needed to be always located at the level of first sacral foramen. When the cylinder trajectory was directed toward the opposite upper corner of first sacral body, there was no violation of cortex of sacral ala, first sacral foramen, or iliac cortex regardless of the presence of sacral variation (Fig. 3).
Discussion
Despite concerns of the neurovascular injuries related to IS screw fixation [21,22,23], it has been considered the most important procedure to manage unstable pelvic ring injuries. Most surgeons still perform IS screw fixation as a percutaneous procedure guided by image intensifier depending on their own experiences. We also have performed IS screw fixations for the prior 10 years without significant difference from other surgeons. Thus, the present simulation of the insertion of virtual IS screws examined the possibility of TITS screw fixation in patients of Asian ethnicity with the goal of achieving an optimal and consistent IS screw trajectory. This goal would hopefully prevent malposition-related complications, which would facilitate use of TITS screws in clinical situations [15, 17, 24] regardless of the presence of sacral variation. Our results demonstrated that the optimal and consistent screw trajectory should be obliquely directed toward the opposite upper corner of the first sacral body at the level of first sacral foramen regardless of sacral variation. It could be found that SZS2 was a sufficient osseous site for the fixation of the 7.0-mm TITS screws even in Asians and was larger than SZS1 in those with sacral variation.
A recent study [4] reported radiographic quantification and its implications for IS screw fixation depending on sacral variation. Other authors [9] reported statistically significant differences in the widths of SZS2 between normal and dysmorphic sacra in CT scans. Concerning SZS2, the cross-sectional area was more than twice as large in dysmorphic sacra compared to normal [10]. In our study, however, although SZS2 was also larger in the variation group (p = 0.001), the difference was only 24%. The dichotomy between studies could reflect differences in tools and methods used, including two-dimensional versus three-dimensional reconstructions, and PACS versus Mimics® software. Concerning the possibility of TITS screw fixation in S2, no model had insufficient osseous site for insertion in our study, in contrast to prior findings [4]. Accordingly, the TITS screw could be inserted transversely in the second sacral segment of all models. Considering that Asian people are smaller than Westerners, it has been generally accepted that their area of SZS2 has smaller osseous site for the insertion of 7.0-mm-sized screws based on personnel communications between orthopedic trauma surgeons, even though the supporting evidence is scant [10, 25]. In our study, SZS2 averaged 221.1 mm2 (range 91.1–386.7 mm2), which was larger than expected. Through the postoperative CT scans, we also realized that the TITS screw fixation could be performed without cortical perforation.
The percutaneous IS screw fixation is technically demanding because of the site’s three-dimensional anatomic complexity, being close to neurovascular structures and having frequent upper sacral morphological variations [1, 2, 4, 5, 8, 10, 24, 26, 27]. Although a safe zone and optimal IS screw trajectory were identified using preoperative planning, there is still the possibility of extra-osseous screw placement because of misinterpreted fluoroscopic imaging. For this purpose, we used a 3D rendering program (Mimics®) to allow free 360° rotations with magnification in any plane and to virtually implant IS screw in the optimal position. This computational analysis revealed that the verification for violation of sacral ala could be easily identified by the modified pelvic outlet view during the insertion of oblique cylinder (conventional IS screw), even though it was in sacral variation. Accordingly, this simply modified outlet view of pelvis might be used to check screw trajectory during fluoroscopically guided procedure if possible (Fig. 2) [19]. Concerning the maximal potential length of the optimal IS screw, the average length of the transverse cylinder for S1 was 151.4 mm (screw range 125–180 mm) and the average length for S2 was 134.2 mm (screw range 95–165 mm). Their results differ from prior findings [15]. When it was considered that 7.0-mm-sized screws are not manufactured in lengths sufficient to span between the posterior iliac bones through the upper sacral segments, the available length of 7.0-mm-sized screws should be checked preoperatively.
This computational simulation study has several fundamental limitations. First, because all measurements were from non-fracture sacrum cadavers, the usefulness of our results may be limited in practical situations with rather descriptive characteristics. Second, the number of enrolled pelvises was not enough to generalize the results to all Asian people. Nevertheless, our descriptive findings offer practical information about screw trajectory and the utility of SZS2 and have meaningful implications for conventional IS screw and TITS screw fixation for pelvic ring injuries.
Conclusions
Considering the high variability of S1, safe and consistent IS screw trajectory should be obliquely directed toward the opposite upper corner of first sacral body at the level of first sacral foramen, regardless of the presence of sacral variation. When the TITS screw fixation for S1 could not be fixed due to sacral variation and other conditions, a hybrid fixation construct consisting of oblique screw for S1 and TITS screw for S2 will be useful to achieve sufficient fixation strength, because the osseous site of the second sacral segment is large enough to place a 7.0-mm-sized IS screw.
References
Conflitti JM, Graves ML, Chip Routt ML Jr (2010) Radiographic quantification and analysis of dysmorphic upper sacral osseous anatomy and associated iliosacral screw insertions. J Orthop Trauma 24(10):630–636. doi:10.1097/BOT.0b013e3181dc50cd
Mendel T, Noser H, Kuervers J, Goehre F, Hofmann GO, Radetzki F (2013) The influence of sacral morphology on the existence of secure S1 and S2 transverse bone corridors for iliosacroiliac screw fixation. Injury 44(12):1773–1779. doi:10.1016/j.injury.2013.08.006
Ebraheim NA, Xu R, Biyani A, Nadaud MC (1997) Morphologic considerations of the first sacral pedicle for iliosacral screw placement. Spine 22(8):841–846 (Phila Pa 1976)
Gardner MJ, Morshed S, Nork SE, Ricci WM, Chip Routt ML Jr (2010) Quantification of the upper and second sacral segment safe zones in normal and dysmorphic sacra. J Orthop Trauma 24(10):622–629. doi:10.1097/BOT.0b013e3181cf0404
Routt ML Jr, Simonian PT, Agnew SG, Mann FA (1996) Radiographic recognition of the sacral alar slope for optimal placement of iliosacral screws: a cadaveric and clinical study. J Orthop Trauma 10(3):171–177
Kim JW, Oh CW, Oh JK, Kyung HS, Park KH, Yoon SD, Yoon SH (2016) The incidence of and factors affecting iliosacral screw loosening in pelvic ring injury. Arch Orthop Trauma Surg 136(7):921–927. doi:10.1007/s00402-016-2471-3
Osterhoff G, Ossendorf C, Wanner GA, Simmen HP, Werner CM (2011) Percutaneous iliosacral screw fixation in S1 and S2 for posterior pelvic ring injuries: technique and perioperative complications. Arch Orthop Trauma Surg 131(6):809–813. doi:10.1007/s00402-010-1230-0
Ayoub MA (2012) Type C pelvic ring injuries in polytrauma patients: can percutaneous iliosacral screws reduce morbidity and costs? Eur J Orthop Surg Traumatol 22(2):137–144. doi:10.1007/s00590-011-0811-0
Guy P, Al-Otaibi M, Harvey EJ, Helmy N (2010) The ‘safe zone’ for extra-articular screw placement during intra-pelvic acetabular surgery. J Orthop Trauma 24(5):279–283
Carlson DA, Scheid DK, Maar DC, Baele JR, Kaehr DM (2000) Safe placement of S1 and S2 iliosacral screws: the “vestibule” concept. J Orthop Trauma 14(4):264–269
Wolinsky P, Lee M (2007) The effect of C-arm malrotation on iliosacral screw placement. J Orthop Trauma 21(7):427–434. doi:10.1097/BOT.0b013e318137948d
Ziran BH, Smith WR, Towers J, Morgan SJ (2003) Iliosacral screw fixation of the posterior pelvic ring using local anaesthesia and computerised tomography. J Bone Joint Surg Br 85(3):411–418
van den Bosch EW, van Zwienen CM, van Vugt AB (2002) Fluoroscopic positioning of sacroiliac screws in 88 patients. J Trauma 53(1):44–48
Day CS, Prayson MJ, Shuler TE, Towers J, Gruen GS (2000) Transsacral versus modified pelvic landmarks for percutaneous iliosacral screw placement–a computed tomographic analysis and cadaveric study. Am J Orthop 29(9 Suppl):16–21 (Belle Mead NJ)
Gardner MJ, Routt ML Jr (2011) Transiliac-transsacral screws for posterior pelvic stabilization. J Orthop Trauma 25(6):378–384. doi:10.1097/BOT.0b013e3181e47fad
Heydemann J, Hartline B, Gibson ME, Ambrose CG, Munz JW, Galpin M, Achor TS, Gary JL (2016) Do transsacral-transiliac screws across uninjured sacroiliac joints affect pain and functional outcomes in trauma patients? Clin Orthop Relat Res 474(6):1417–1421. doi:10.1007/s11999-015-4596-z
Vanderschot P, Meuleman C, Lefevre A, Broos P (2001) Trans iliac-sacral-iliac bar stabilisation to treat bilateral lesions of the sacro-iliac joint or sacrum: anatomical considerations and clinical experience. Injury 32(7):587–592
Ozmeric A, Yucens M, Gultac E, Acar HI, Aydogan NH, Gul D, Alemdaroglu KB (2015) Are two different projections of the inlet view necessary for the percutaneous placement of iliosacral screws? Bone Joint J 97-B(5):705–710. doi:10.1302/0301-620X.97B5.34959
Ricci WM, Mamczak C, Tynan M, Streubel P, Gardner M (2010) Pelvic inlet and outlet radiographs redefined. J Bone Joint Surg Am 92(10):1947–1953. doi:10.2106/JBJS.I.01580
Konin GP, Walz DM (2010) Lumbosacral transitional vertebrae: classification, imaging findings, and clinical relevance. AJNR Am J Neuroradiol 31(10):1778–1786. doi:10.3174/ajnr.A2036
Zwingmann J, Hauschild O, Bode G, Sudkamp NP, Schmal H (2013) Malposition and revision rates of different imaging modalities for percutaneous iliosacral screw fixation following pelvic fractures: a systematic review and meta-analysis. Arch Orthop Trauma Surg 133(9):1257–1265. doi:10.1007/s00402-013-1788-4
Zwingmann J, Sudkamp NP, Konig B, Culemann U, Pohlemann T, Aghayev E, Schmal H (2013) Intra- and postoperative complications of navigated and conventional techniques in percutaneous iliosacral screw fixation after pelvic fractures: results from the German Pelvic Trauma Registry. Injury 44(12):1765–1772. doi:10.1016/j.injury.2013.08.008
Routt ML Jr, Simonian PT, Mills WJ (1997) Iliosacral screw fixation: early complications of the percutaneous technique. J Orthop Trauma 11(8):584–589
Mendel T, Noser H, Wohlrab D, Stock K, Radetzki F (2011) The lateral sacral triangle—a decision support for secure transverse sacroiliac screw insertion. Injury 42(10):1164–1170
Fischer S, Vogl TJ, Marzi I, Zangos S, Wichmann JL, Scholtz JE, Mack MG, Schmidt S, Eichler K (2015) Percutaneous cannulated screw fixation of sacral fractures and sacroiliac joint disruptions with CT-controlled guidewires performed by interventionalists: single center experience in treating posterior pelvic instability. Eur J Radiol 84(2):290–294. doi:10.1016/j.ejrad.2014.11.017
Lee JJ, Rosenbaum SL, Martusiewicz A, Holcombe SA, Wang SC, Goulet JA (2015) Transsacral screw safe zone size by sacral segmentation variations. J Orthop Res 33(2):277–282. doi:10.1002/jor.22739
Miller AN, Routt ML Jr (2012) Variations in sacral morphology and implications for iliosacral screw fixation. J Am Acad Orthop Surg 20(1):8–16. doi:10.5435/JAAOS-20-01-008
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article involved human participants. However, because our study design used approved digital data, this study did not need the institutional review board approval.
Rights and permissions
About this article
Cite this article
Chon, CS., Jeong, JH., Kang, B. et al. Computational simulation study on ilio-sacral screw fixations for pelvic ring injuries and implications in Asian sacrum. Eur J Orthop Surg Traumatol 28, 439–444 (2018). https://doi.org/10.1007/s00590-017-2061-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-017-2061-2