Abstract
Purpose
To evaluate the effect of K-line on posterior single-door decompression with fusion fixation (PFF) and posterior single-door decompression with non-fusion fixation (PNF) for patients with ossification of posterior longitudinal ligament (OPLL).
Methods
A total of 65 patients with OPLL were analyzed retrospectively. They consisted of 44 patients with positive K-line, designated as the K ( +) group, and 21 patients with negative K-line, designated as K (−). The patients were also divided into a PFF group (38 patients) and a PNF group (27 patients). The Japanese Orthopaedic Association (JOA) score, C2–C7 Cobb angle, improvement rate of JOA score, and complications were calculated and statistically analyzed between the groups.
Results
In the K ( +) group, there were no significant differences in the incidence of C5 nerve root palsy and C2–C7 Cobb angle between the two groups of surgical patients, but there were significant differences in the improvement rate of JOA score and the incidence of axial pain. In the K (−) group, there were no significant differences in the incidence of axial pain, the incidence of C5 nerve root palsy, and preoperative C2–C7 Cobb angle between the two groups, but significant differences were observed in the improvement rate of JOA score and C2–C7 Cobb angle at the last follow-up.
Conclusion
In the K ( +) group, the improvement rate of JOA score was higher and the incidence of axial pain was lesser in the PNF group than in the PFF group. In the K (−) group, the improvement rate of JOA score was higher in the PFF group than in the PNF group, and there was significant loss of C2–C7 Cobb angle in the PNF group.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
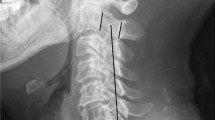
Ossification of posterior longitudinal ligament (OPLL) is a pathological condition characterized by heterotopic ossification of the cervical spinal ligament, which can lead to spinal stenosis and compression of the spinal cord, which in turn result in limb numbness and weakness, walking difficulties, and other clinical manifestations. Cervical OPLL was first reported in 1984 by Tsuyama [1]. Since then, research has increasingly been conducted on the condition. OPLL is a common cause of myelopathy in individuals over 55 years of age [2, 3]. Cervical OPLL is most common in men, the elderly, and Asians, and it commonly occurs in the C4–C5 vertebral region [4]. Its pathogenesis is not clear as many factors are in play. These include genetic factors [5, 6], endocrine factors [7, 8], mechanical stress stimulation, and biomechanical factors [9]. Continued ossification often results in cervical spinal stenosis and progressive compression of the nervous system so that patients with OPLL often require surgical treatment. According to Hirabayashi et al. [10, 11], expansive open-door laminoplasty (ELAP) is a simple and effective surgical method for the treatment of cervical spinal stenosis of various etiologies. The operation entails relieving the compression on the spinal cord and nerves by directly lifting the lamina and increasing the anteroposterior diameter of the spinal canal. Posterior single-door decompression with fusion fixation (PFF) and posterior single-door decompression with non-fusion fixation (PNF) are two common types of ELAP. Fujiyoshi et al. [12] suggested that K-line is a predictor of the clinical efficacy of posterior cervical decompression in patients with OPLL. K-line is a straight line on a standard lateral X-ray film of the cervical spine that joins the midpoints of the spinal canal at C2 and C7. K-line is said to be positive when the OPLL is not beyond the K-line and negative when the K-line is beyond the K-line. How effective are the two types of posterior cervical surgery in patients with OPLL and a positive K-line, designated as the K ( +) group, and in patients with OPLL and a negative K-line, designated as the K (−) group? Which type of surgery is better for each group of patients? In this study, the aims of the retrospective analysis of the medical records of patients with OPLL who underwent PFF and PNF were as follows: 1. To evaluate the impact of K-line on the clinical efficacy of the two types of surgery by comparing them, 2. To analyze the correlation between the change of the sagittal curvature of the cervical spine and clinical efficacy in patients with OPLL, and 3. To find a safer and more effective surgical treatment strategy for patients with OPLL through preoperative K-line evaluation.
Materials and methods
Inclusion and exclusion criteria
The inclusion criteria were as follows: 1. Diagnosis of OPLL and progressive neurological damage requiring surgical intervention; 2. Obvious spinal cord compression on magnetic resonance imaging (MRI); 3. OPLL involving two or more vertebrae; and 4. Patient participation in follow-up assessment and main outcome measures that include improvements in spinal nerve function, sagittal curvature of the cervical spine, and complications.
The exclusion criteria were as follows: 1. Cervical trauma and tumor, 2. Scapulohumeral periarthritis and other factors affecting the evaluation of axial symptoms, 3. Severe internal diseases that make surgery intolerable, and 4. History of cervical surgery.
General information
From September 2011 to September 2017, of the 78 patients eligible to participate in the study, a total of 13 patients (16.67%) were lost to follow-up at 2 years. Based on the inclusion and exclusion criteria listed above, a total of 65 patients were included in this study. The patients included consisted of 42 men and 23 women aged 40–75 with a mean age of 57.03 ± 10.87 years. The disease course was 6–24 months and the mean disease course was 12.68 ± 4.65 months. The percentage of spinal canal occupied by ossified mass was 30–75%, and the mean percentage was 52.28 ± 12.86%. All the patients had sensory and motor disorders. OPLL was confirmed by X-ray, computed tomography (CT), and MRI. The clinical research plan was approved by the medical ethics committee, and all the patients signed the informed consent document.
Patient grouping
In this retrospective study, we analyzed the clinical effect of PFF and PNF on patients with cervical OPLL. All operations were performed by the same group of doctors. The surgeons fully communicated with the patients before surgery, so that all patients could understand the process, advantages and disadvantages of the two surgical procedures. Finally the patients selected the surgical procedures.The 65 patients with cervical OPLL were divided into two groups according to the surgical type. The 38 patients who underwent posterior single-door decompression with fusion fixation were categorized as the PFF group. This group consisted of 24 men and 14 women aged 40–75 with a mean age of 57.710 ± 11.104 years. The disease course in the PFF group was 6–24 months and the mean disease course was 12.526 ± 4.596 months. The mean percentage of spinal canal occupation was 51.316 ± 11.780%. The decompression segment was C3–C6 in 15 patients (39.47%) and C3–C7 in 23 patients (60.53%). The 27 patients who underwent posterior single-door decompression with non-fusion fixation were categorized as the PNF group. This group consisted of 18 men and 9 women aged 43–72 with a mean age of 56.074 ± 10.662 years. The disease course was 7–24 months and the mean disease course was 12.889 ± 4.807 months. The percentage of vertebral canal occupied by ossification mass was 30–75% and the mean percentage was 53.630 ± 14.369%. The decompression segment was C3-C6 in 10 patients (37.04%) and C3–C7 in 17 patients (62.96%).
Operative method
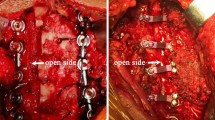
General anesthesia was used in both groups. The patients laid on a disinfected gypsum bed covered with a towel. In the PFF group, a midline incision was made to expose the laminae and articular processes of the decompression segment. A high-speed grinding drill or an ultrasonic bone knife was used to cut grooves along the junction of the lamina and facet articular process on both sides. The inner lamina was retained on the side of the door shaft, and the whole lamina was cut off on the side of the door opening. A lateral mass screw system was placed on each of the 2 sides of the decompression segment. The laminae were slowly lifted in succession to the opposite side, and holes were punched in the spinous processes using towel pliers. The laminae were then pulled through the spinous processes using the ETHIBOND suture. They were then fixed on the titanium bar on the side of the door shaft, and the suture was tightened, knotted, and fixed. The opening angle was 30°–40°, and the opening width was 1.0–1.5 cm. After the slotted bone was reserved, it was implanted onto the side of the door shaft to promote bone healing. During the operation, hemostasis was meticulously performed, and a large amount of normal saline was used for washing. A drainage tube was placed in each of the two sides of the spinous process, and the incision was closed layer by layer. The exposure method in the PNF group was the same as in the PFF group. In both groups, the hormone was administered when the door was opened, and 0.5 g of methylprednisolone was added to 100 mL of normal saline for rapid intravenous drip.
Postoperative management
Antibiotics were administered to all the patients to prevent infection. The drainage tubes were pulled out 24–48 h after the operation depending on the drainage flow, and the patients were encouraged to wear neck brackets and to get out of bed. With their necks protected and supported by a neck bracket, the patients resumed active neck flexion and extension 2 weeks after the operation, and they started exercising the posterior neck muscles.
Follow-up and evaluation index
All the patients were followed up for 24–72 months, and the mean follow-up period was 39.68 ± 14.78 months. All the patients were reexamined at 3 and 6 months after the operation and at the last follow-up appointment. Routine X-ray, CT, or MRI examination was performed. The Japanese Orthopaedic Association (JOA) score (17-point method) [13] was used to evaluate the neurological status of patients before the operation, at 3 months after the operation, and at the last follow-up assessment. The improvement rate of JOA score at the last follow-up was also calculated. The Hirabayashi method was used to calculate the improvement rate of JOA score. The formula is as follows:\(({\text{postoperative JOA score}} - {\text{preoperative JOA score}})/(17 - {\text{preoperative JOA score}}) \times 100\%\) . The percentage of spinal canal occupation by ossification block was determined by selecting the axial CT section of the highest point of ossification block, measuring the thickness of the ossification block and the anteroposterior diameter of the spinal canal, and calculating the percentage (Fig. 1). The C2–C7 Cobb angle was determined using the standard lateral X-ray film of the cervical spine. It is the angle between the extension line of the lower edge of the C2 vertebra and the extension line of the lower edge of the C7 vertebra. The front convex angle is expressed as a positive value and the back convex angle as a negative value (Fig. 1). Two independent clinical research assistants, who were not involved with the study and blinded to all clinical information, performed radiological measurements. Radiological parameters were measured twice at 1-week intervals, and the average values of both observers were used in this study. In the study, we investigated the reliability of the measurement techniques and found good to excellent intra- and inter-observer agreement for each parameter (Kappa > 0.75). The postoperative complications of the two groups were recorded.
A Schematic diagram for the measurement of the sagittal curvature of the cervical spine. On the standard lateral X-ray film of the cervical spine, the line between the midpoints of the spinal canal at C2 and C7 is the K-line, and the angle between the extension line of the lower edge of C2 and the extension line of the lower edge of C7 is the C2–C7 Cobb angle; B Schematic diagram for the measurement of percentage of spinal canal occupation by ossified mass. The thickness of the ossification block (a, green line) and the anteroposterior diameter of the spinal canal (b, yellow line) were measured on the axial CT section of the highest point of the ossification block. The percentage of spinal canal occupation by the ossification block = a/b × 100%
Statistical methods
The SPSS (version 22.0) statistical software (SPSS company, USA) was used for statistical analysis. The chi square test was used for counting data (when the sample size is less than 40, Fisher test is used), and (\(\overline{x} \pm s\)) was used for measuring data. Comparison of basic data, the independent sample t-test was used for inter-group comparison. At each time point before and after the operation, the rank sum test was used for intra-group comparison and inter-group comparison. The test level α value was 0.05 for both sides, and a difference was considered statistically significant if P < 0.05.
Results
There were no significant differences in age, gender, disease course, percentage of vertebral canal occupation by ossification mass, distribution of decompression segments, and follow-up time between the two groups (Table 1). This means that the basic data of the two groups are comparable.
In the K ( +) group, no significant differences were observed in preoperative JOA score and preoperative C2–C7 Cobb angle between the PFF and PNF groups (P > 0.05). At the last follow-up, the mean JOA scores of the PFF and PNF groups were 11.960 ± 2.111 and 13.526 ± 2.366, respectively, and the difference was statistically significant (P < 0.05). The improvement rate of nerve function was 43.646 ± 16.961% in the PFF group and 63.492 ± 21.185% in the PNF group, and the difference was statistically significant (P < 0.05). At the last follow-up, there was no significant difference in the C2–C7 Cobb angle between the two groups (P > 0.05). The incidence of postoperative axial pain was 32% (8/25) in the PFF group and 5.26% (1/19) in the PNF group, and the difference between the two groups was statistically significant (P < 0.05). There was no significant difference in the incidence of C5 nerve root paralysis (P > 0.05) (Table 2).
In the K (−) group, no significant differences were observed in the preoperative JOA score and preoperative C2–C7 Cobb angle between the two groups (P > 0.05). At the last follow-up, the mean JOA scores of the PFF and PNF groups were 11.923 ± 2.326 and 9.625 ± 1.768 respectively, and the difference was statistically significant (P < 0.05) (Figs. 2 and 3). The improvement rate of nerve function was 45.607 ± 19.387% in the PFF group and 20.095 ± 10.770% in the PNF group, and the difference was statistically significant (P < 0.05). At the last follow-up, the mean C2–C7 Cobb angles in the PFF and PNF groups were (3.923 ± 1.847)° and (0.875 ± 1.727)° respectively, and the difference between the two groups was statistical significant (P < 0.05). There were no significant differences in the incidences of postoperative axial pain and C5 nerve root palsy between the two groups (P > 0.05) (Table 2).
A 66-year-old man with ossification of cervical posterior longitudinal ligament and negative K-line. A Standard preoperative lateral X-ray film of the cervical spine showing that the highest point of ossification mass of the posterior longitudinal ligament is beyond the K-line. B Preoperative sagittal CT showing that the range of ossification of the posterior longitudinal ligament is C3–C5. C Preoperative MRI showing obvious compression in front of the cervical spinal cord. D Lateral X-ray performed 6 months after surgery showing that the C3–C6 nail rod fixation had in situ fusion and that the curvature of the cervical spine did not change significantly from its preoperative state. E Lateral X-ray performed 4 years after surgery showing good internal fixation and well-maintained curvature of the cervical spine. F MRI performed 2 years after surgery showing that the anteroposterior diameter of the spinal canal increased significantly and that the spinal cord compression reduced significantly
A 54-year-old woman with ossification of cervical posterior longitudinal ligament and negative K-line. A Standard preoperative lateral X-ray film of the cervical spine showing that the highest point of ossification mass of the posterior longitudinal ligament is beyond the K-line. B Preoperative sagittal CT showing that the range of ossification of the posterior longitudinal ligament is C3–C5. C Preoperative MRI showing obvious compression in front of the cervical spinal cord. D Lateral X-ray performed 6 months after surgery showing that C3–C6 were fixed with an arch titanium plate and that the curvature of the cervical spine was partially lost compared to the preoperative state. E Lateral X-ray performed 3.5 years after surgery showing good internal fixation and partially lost curvature of cervical spine compared to the preoperative state. F MRI performed 3.5 years after surgery showing that the anteroposterior diameter of the spinal canal increased significantly and that the spinal cord compression reduced significantly
Discussion
The choice of OPLL operation
Many study results show that the anterior and posterior approaches to the surgical treatment of cervical OPLL have their respective advantages, disadvantages, and limitations [14,15,16]. OPLL causes anterior compression of the spinal canal; therefore, the anterior approach is preferred. However, the ossification focus is often large spanning multiple segments and causing severe spinal cord compression. It is also often associated with hypertrophy or ossification of the ligamentum flavum and stenosis of the spinal canal, which makes it difficult to avoid the spinal cord in the anterior approach and increases the risk of nerve injury. In addition, the anterior approach is associated with many complications and is a relatively complex procedure; consequently, the posterior approach is more commonly used in the surgical treatment of cervical OPLL [16]. The complications include progression of OPLL, cervical axial pain, C5 paralysis, and postoperative instability [17]. To treat patients with continuous OPLL, direct spinal canal decompression can be performed using the anterior approach, but indirect decompression using the posterior approach is more commonly performed [18]. Posterior spinal cord decompression is widely performed even though the ossified posterior longitudinal ligament cannot be directly removed [19, 20]. Total laminectomy is feasible in the posterior approach and the decompression effect is perfect, but the surgical trauma is significant and spine stability is greatly affected. Single open-door laminoplasty not only achieves the purpose of decompression, but it also preserves spine stability to a certain extent. It has yielded favorable outcomes when used for the treatment of cervical spondylosis and cervical stenosis of various etiologies [21,22,23]. The posterior approach of the operation can increase the sagittal diameter of the spinal canal, which can directly reduce the pressure behind the spinal cord, move the spinal cord backward, and indirectly reduce the pressure in front of the spinal cord. Although the range of posterior movement of the spinal cord is limited, a small range of movement is enough to significantly improve patient symptoms. In this study, the JOA scores of the PFF and PNF patient groups at the last follow-up were better than the preoperative scores, and the difference was statistically significant (P < 0.05). The results in both groups were satisfactory.
The impact of K-line on the clinical effect of the two types of surgical operation
In 2008, Fujiyoshi et al. [12] proposed K-line as a novel clinical evaluation index based on a large number of experiments. K-line as an index can evaluate the alignment of the vertebral body and describe the extent of OPLL. It can also be used to evaluate the rationality of the choice of surgical operation and is characterized by simplicity and high accuracy. In the K ( +) group in this study, there was no significant difference in preoperative JOA scores between the two types of operation. However, the JOA score of the PNF group was better than that of the PFF group. The improvement rate of nerve function in the PNF group was higher than that in the PFF group. The incidence of postoperative axial pain in the PNF group was significantly lower than that in the PFF group. PNF entails non-fusion fixation, and arch titanium plates were used for fixation. The advantages of the plate include the following: (a) from the design point of view, the fork structure at both ends of the arch titanium plate is directly fixed on the lateral mass and the vertebral plate. This forms a strong support, which in combination with screw fixation reduces direct stimulation of the joint capsule and surrounding soft tissue, which is conducive to the recovery of nerve function; (b) it provides true rigid fixation, reduces the incidence of postoperative reclosure, and separates the vertebral canal and extraspinal tissue. This prevents scar tissue retraction into the spinal canal, which can cause new compression. (C) arch titanium plate is used to separately fix each segment of the cervical spine, which makes the lamina and lateral mass of the same segment a unit. This provides strong fixation without affecting the movement function of the cervical spine. After the operation, there is no need to take a long recovery break. Flexion and extension of the cervical spine can be performed early. This reduces the incidence of axial symptoms. Thus, PNF is superior to PFF in patients with OPLL and positive K-line.
Fujiyoshi et al. [12] proposed that K-line can be used to predict the prognosis of patients with OPLL. However, they found that patients with negative K-line had difficulty attaining satisfactory posterior spinal drift and ideal neurological recovery after posterior decompression. The K-line can indicate the cervical spine curvature and the thickness of OPLL. It is a simple way to help clinicians formulate surgical strategies and determine patient prognosis [24]. Some scholars consider the surgical outcomes of laminoplasty in the treatment of patients with OPLL and negative K-line to be poor [14, 25]. Hirai et al. [26] proposed modified K-line similar to the K-line for cervical OPLL and found that posterior fusion surgery was better in patients with minimum interval of the spinal cord < 4 mm. In the K (−) group in this study, there was no significant difference in preoperative JOA scores between the two types of surgery. However, the JOA score of the PFF group was better than that of the PNF group. The improvement rate of nerve function in the PFF group was higher than that in the PNF group. Compared to PNF, PFF is superior as it can maintain cervical spine curvature, prevent the progression of kyphosis caused by the destruction of the posterior structure of cervical vertebrae, and enhance the stability of the decompression segment, which helps to delay the progression of OPLL and prevent the aggravation of spinal cord injury caused by instability of local cervical vertebrae [27, 28]. In the study of 3-dimensional OPLL volume, posterior fusion was shown to have the effect of reducing the growth rate of OPLL compared to operations that allow motion [29, 30]. Therefore, PFF is superior to PNF in the treatment of patients with OPLL and negative K-line.
The correlation between changes of sagittal curvature of cervical spine and postoperative clinical effect
Poor sagittal curvature of cervical spine may be 1 of the risk factors for poor efficacy of PNF in patients with OPLL. Fujiyoshi et al. [12] evaluated and compared the neurological recovery of 8 patients with negative K-line and 19 patients with positive K-line OPLL after ELAP. The results showed that the improvement rate of neurological function in the K ( +) group was 66.0% but only 13.9% in the K (−) group. In the K ( +) group in this study, there was no significant difference in the C2–C7 Cobb angle between the two groups at the last follow-up (P > 0.05). In the K (−) group, there was significant difference in the C2–C7 Cobb angle between the two groups at the last follow-up (P < 0.05). Cervical curvature was well maintained in the PFF group but was partially lost in the PNF group. There is no consensus on whether PFF should be used to correct kyphosis in patients with OPLL. Koda et al. [31] showed that adition of posterior instrumented fusion to laminoplasty can improve the surgical outcome of patients with K-line (−) cervical OPLL compared with laminoplasty alone. Postoperative K-line conversion from (−) to ( +) is an independent factor that is significantly associated with a better surgical outcome. In theory, recovery of the physiological lordosis of the cervical spine can help the spinal cord drift dorsally and lead to greater indirect decompression effect. However, correction of the sagittal curvature of the cervical spine is likely to reduce the height of the intervertebral foramen and cause excessive drifting of the spinal cord, which increases the risk of C5 nerve root palsy [32, 33]. In addition, some patients with multi-level continuous OPLL have poor preoperative cervical movement, and excessive manipulation during operation increases the surgical risk. In this study, the lateral mass screw system was used in the PFF group for in situ fixation and fusion to fully decompress the cervical spinal cord. During the operation, the cervical sagittal kyphosis was deliberately not corrected. The operation also significantly improved the JOA score and the improvement rate of JOA score in the K (-) group and maintained cervical spine curvature.
Conclusion
First, as this is a single-center retrospective study, we did not consider the effect of OPLL on the segment, number of patients, and classification of OPLL. Second, the number of patients is too small, which may lead to selective bias and errors in results. In addition, the follow-up duration in this study is relatively short.
To sum up, K-line evaluation can predict the prognosis of patients with cervical OPLL. PFF and PNF are effective in the treatment of both positive and negative K-line OPLL. However, PNF is recommended for patients with positive K-line because it is more effective. In contrast, PFF is recommended for patients with negative K-line as it is more effective and can maintain good sagittal curvature of the cervical spine, which leads to satisfactory rate of neurological improvement and higher postoperative efficacy. Considering the limitation of small sample size, it is necessary to conduct comprehensive multi-center studies with large sample sizes in the future.
References
Tsuyama N (1984) Ossification of the posterior longitudinal ligament of the spine. Clin Orthop Relat Res 184:71–84
Lau D, Chou D, Mummaneni PV (2015) Two-level corpectomy versus three-level discectomy for cervical spondylotic myelopathy: a comparison of perioperative, radiographic, and clinical outcomes. J Neurosurg Spine 23(3):280–289. https://doi.org/10.3171/2014.12.SPINE14545 (Epub 2015 Jun 19)
Nakashima H, Tetreault L, Nagoshi N et al (2016) Comparison of outcomes of surgical treatment for ossification of the posterior longitudinalligament versus other forms of degenerative cervical myelopathy: results from the prospective, multicenter AOSpine CSM-international study of 479 patients. J Bone Joint Surg Am 98(5):370–378. https://doi.org/10.2106/JBJS.O.00397
Miao J, Sun J, Shi J, Chen Y, Chen D (2018) A novel anterior revision surgery for the treatment of cervical ossification of posterior longitudinal ligament: case report and review of the literature. World Neurosurg 113:212–216. https://doi.org/10.1016/j.wneu.2018.02.076 (Epub 2018 Feb 21)
Yan L, Chang Z, Liu Y, Li YB, He BR, Hao DJ (2013) A single nucleotide polymorphism in the human bone morphogenetic protein-2 gene (109T > G) affects the smad signaling pathway and the predisposition to ossification of the posteriorlongitudinal ligament of the spine. Chin Med J (Engl) 126(6):1112–1118
Jekarl DW, Paek CM, An YJ et al (2013) TGFBR2 gene polymorphism is associated with ossification of the posterior longitudinalligament. J Clin Neurosci 20(3):453–456. https://doi.org/10.1016/j.jocn.2012.05.031 (Epub 2012 Dec 8)
Turner RT, Kalra SP, Wong CP et al (2013) Peripheral leptin regulates bone formation. J Bone Miner Res 28(1):22–34. https://doi.org/10.1002/jbmr.1734
Chen Y, Wang X, Yang H, Miao J, Liu X, Chen D (2014) Upregulated expression of PERK in spinal ligament fibroblasts from the patients with ossificationof the posterior longitudinal ligament. Eur Spine J 23(2):447–454. https://doi.org/10.1007/s00586-013-3053-5 (Epub 2013 Oct 7)
Zhang W, Wei P, Chen Y et al (2014) Down-regulated expression of vimentin induced by mechanical stress in fibroblasts derived from patients with ossification of the posterior longitudinal ligament. Eur Spine J 23(11):2410–2415. https://doi.org/10.1007/s00586-014-3394-8 (Epub 2014 Jun 8)
Hirabayashi K, Watanabe K, Wakano K, Suzuki N, Satomi K, Ishii Y (1983) Expansive open-door laminoplasty for cervical spinal stenotic myelopathy. Spine 8(7):693–699
Hirabayashi K, Satomi K (1988) Operative procedure and results of expansive open-door laminoplasty. Spine 13(7):870–876
Fujiyoshi T, Yamazaki M, Kawabe J et al (2008) A new concept for making decisions regarding the surgical approach for cervical ossification of the posterior longitudinal ligament: the K-line. Spine 33(26):E990–E993. https://doi.org/10.1097/BRS.0b013e318188b300
Fukui M, Chiba K, Kawakami M et al (2007) Japanese orthopaedic association back pain evaluation questionnaire part 2 verification of its reliability : the subcommittee on low back pain and cervical myelopathy evaluation of the clinical outcome committee of the japanese orthopaedic association. J Orthop Sci 12(6):526–532 (Epub 2007 Nov 30)
Kim B, Yoon DH, Shin HC et al (2015) Surgical outcome and prognostic factors of anterior decompression and fusion for cervical compressive myelopathy due to ossification of the posterior longitudinal ligament. Spine J 15(5):875–884. https://doi.org/10.1016/j.spinee.2015.01.028 (Epub 2015 Jan 28)
Lin W, Ha A, Boddapati V, Yuan W, Riew KD (2018) Diagnosing pseudoarthrosis after anterior cervical discectomy and fusion. Neurospine 15(3):194–205. https://doi.org/10.14245/ns.1836192.096 (Epub 2018 Sep 28)
Liu X, Min S, Zhang H, Zhou Z, Wang H, Jin A (2014) Anterior corpectomy versus posterior laminoplasty for multilevel cervical myelopathy: a systematic review and meta-analysis. Eur Spine J 23(2):362–372. https://doi.org/10.1007/s00586-013-3043-7 (Epub 2013 Oct 5)
Qin R, Chen X, Zhou P, Li M, Hao J, Zhang F (2018) Anterior cervical corpectomy and fusion versus posterior laminoplasty for the treatment of oppressive myelopathy owing to cervical ossification of posterior longitudinal ligament: a meta-analysis. Eur Spine J 27(6):1375–1387. https://doi.org/10.1007/s00586-017-5451-6 (Epub 2018 Jan 15)
Geck MJ, Eismont FJ (2002) Surgical options for the treatment of cervical spondylotic myelopathy. Orthop Clin North Am 33(2):329–348
Blizzard DJ, Caputo AM, Sheets CZ et al (2017) Laminoplasty versus laminectomy with fusion for the treatment of spondylotic cervicalmyelopathy: short-term follow-up. Eur Spine J 26(1):85–93. https://doi.org/10.1007/s00586-016-4746-3 (Epub 2016 Aug 23)
Moon BJ, Kim D, Shin DA et al (2019) Patterns of short-term and long-term surgical outcomes and prognostic factors for cervicalossification of the posterior longitudinal ligament between anterior cervical corpectomy and fusion and posterior laminoplasty. Neurosurg Rev 42(4):907–913. https://doi.org/10.1007/s10143-018-01069-x (Epub 2019 Jan 4)
Park JH, Ahn JS, Lee HJ, Shin BK (2016) Comparison between radiological and clinical outcomes of laminoplasties with titaniumminiplates for cervical myelopathy. Clin Orthop Surg 8(4):399–406 (Epub 2016 Nov 4)
Tung KL, Cheung P, Kwok TK, Wong KK, Mak KH, Wong WC (2015) Single-door cervical laminoplasty using titanium miniplates alone. J Orthop Surg 23(2):174–179
Yeh KT, Yu TC, Chen IH et al (2014) Expansive open-door laminoplasty secured with titanium miniplates is a good surgical methodfor multiple-level cervical stenosis. J Orthop Surg Res 9:49. https://doi.org/10.1186/s13018-014-0049-8
Takeuchi K, Yokoyama T, Numasawa T et al (2016) K-line (−) in the neck-flexed position in patients with ossification of the posterior longitudinalligament is a risk factor for poor clinical outcome after cervical laminoplasty. Spine 41(24):1891–1895
Koda M, Mochizuki M, Konishi H et al (2016) Comparison of clinical outcomes between laminoplasty, posterior decompression with instrumented fusion, and anterior decompression with fusion for K-line (–) cervical ossification of the posterior longitudinal ligament. Eur Spine J 25(7):2294–2301. https://doi.org/10.1007/s00586-016-4555-8 (Epub 2016 Apr 13)
Hirai T, Yoshii T, Inose H et al (2019) Is modified K-line a powerful tool of surgical decision making for patientswith cervical spondylotic myelopathy? Clin Spine Surg 32(9):351–356. https://doi.org/10.1097/BSD.0000000000000899
Masaki Y, Yamazaki M, Okawa A et al (2007) An analysis of factors causing poor surgical outcome in patients with cervical myelopathy due to ossification of the posterior longitudinal ligament: anterior decompression with spinal fusionversus laminoplasty. J Spinal Disord Tech 20(1):7–13
Maruo K, Moriyama T, Tachibana T et al (2014) The impact of dynamic factors on surgical outcomes after double-door laminoplasty for ossification of the posterior longitudinal ligament of the cervical spine. J Neurosurg Spine 21(6):938–943. https://doi.org/10.3171/2014.8.SPINE131197 (Epub 2014 Oct 3)
Katsumi K, Izumi T, Ito T, Hirano T, Watanabe K, Ohashi M (2016) Posterior instrumented fusion suppresses the progression of ossification of the posterior longitudinal ligament: a comparison of laminoplasty with and without instrumented fusion by three-dimensional analysis. Eur Spine J 25(5):1634–1640. https://doi.org/10.1007/s00586-015-4328-9 (Epub 2015 Nov 19)
Lee JJ, Shin DA, Yi S et al (2018) Effect of posterior instrumented fusion on three-dimensional volumetric growth of cervicalossification of the posterior longitudinal ligament: a multiple regression analysis. Spine J 18(10):1779–1786. https://doi.org/10.1016/j.spinee.2018.03.002 (Epub 2018 Mar 8)
Koda M, Furuya T, Saito J et al (2018) Postoperative K-line conversion from negative to positive is independentlyassociated with a better surgical outcome after posterior decompression with instrumented fusion for K-line negative cervical ossification of the posteriorligament. Eur Spine J 27(6):1393–1400. https://doi.org/10.1007/s00586-018-5505-4 (Epub 2018 Feb 14)
Takemitsu M, Cheung KM, Wong YW, Cheung WY, Luk KD (2008) C5 nerve root palsy after cervical laminoplasty and posterior fusion with instrumentation. J Spinal Disord Tech 21(4):267–272. https://doi.org/10.1097/BSD.0b013e31812f6f54
Nakashima H, Imagama S, Yukawa Y et al (2012) Multivariate analysis of C-5 palsy incidence after cervical posterior fusion with instrumentation. J Neurosurg Spine 17(2):103–110. https://doi.org/10.3171/2012.4.SPINE11255 (Epub 2012 May 25)
Funding
There is no funding source.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, C., Zhou, H., Yang, S. et al. Effect of K-line on posterior cervical surgery in patients with posterior longitudinal ligament ossification. Eur Spine J 29, 2368–2377 (2020). https://doi.org/10.1007/s00586-020-06507-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06507-3