Abstract
Chronic rhinosinusitis with nasal polyposis (CRSwNP) is a group of multifactorial and heterogeneous disorders with a significant economic strain on society, likely made up of different endotypes, each with a unique pathomechanism. In addition to the traditional clinical measures, there is a recognized need for reliable biomarkers to provide predictive information regarding diagnosis, endotypes, treatment responses, and future risk of recurrence. Fueled by the advances in basic research, various biomarkers have been explored in recent years. Biomarkers of CRSwNP can originate from a variety of sources, including nasal secretions, nasal biopsies, exhaled breath, and peripheral blood. In this review, we aim to summarize the existing and emerging biomarkers available for the evaluation and management of CRSwNP. Currently, eosinophil count in nasal mucosa has proved particularly valuable for endotyping, assessing disease severity, and predicting steroid responsiveness and surgical outcomes. Blood eosinophilia may be used as a surrogate for tissue eosinophilic inflammation, whereas its utility remains limited. Type 2 cytokines, such as IL-4, IL-5, and IL-13, and IgE have been identified as potential therapeutic targets. Moreover, matrix metalloproteinases (MMP)-9 is linked to healing quality after sinus surgery. Nasal nitric oxide (nNO) appears to fill the niche as a noninvasive measure for sinus ostial patency. In addition, recent data have shown some promising biomarkers involved in corticosteroid resistance and olfactory dysfunction. However, rigorous validation using large cohort studies is necessary before these biomarkers can be mainstreamed into clinical practice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic rhinosinusitis with nasal polyposis (CRSwNP) represents a clinical phenotype of chronic rhinosinusitis (CRS) characterized by persistent polypoid inflammation of the sinonasal mucosa [1]. Despite the fact that CRSwNP accounts for only approximately 25–30% of all CRS cases, CRSwNP is considered a more severe condition that seriously affects patient’s quality of life (QOL) and productivity, and is associated with a large economic burden [2]. Unfortunately, significant variations in clinical manifestations, therapeutic responses, and prognosis in patients with CRSwNP make this disease difficult to identify, assess, and manage. This has strengthened the concept that rather than being one single disease entity, CRSwNP appears to be a heterogeneous disease spectrum consisting of several different endotypes that might be discerned by corresponding biomarkers [3]. For these reasons, there is a clear need for reliable biomarkers to provide additional information beyond that supplied by conventional clinical measures.
In recent years, basic research has shed some light on the pathogenesis of CRSwNP and has contributed to the discovery of various biomarkers from airway inflammation and tissue remodeling. Compared with clinical traits, endoscopic examinations, and imaging techniques, biomarkers are more objective, quantitative and reflective of the underlying pathophysiology [4]. Successful identification and clinical translation of CRSwNP biomarkers can aid to classify patients, monitor treatment effects, assess risk of recidivism, and develop novel biological therapies. In this paper, we review the current state of knowledge with respect to biomarkers in the evaluation and management of CRSwNP.
Current sources of CRSwNP biomarkers
In general, CRSwNP biomarkers can be assessed in the nasal secretions, nasal biopsies, exhaled breath via nasal nitric oxide (nNO) evaluation, and peripheral blood. Soluble mediators such as chemokines and cytokines can be obtained from nasal secretions. In addition, it has been shown that cytokines in nasal secretions typically correlate with tissue levels [5]. Nasal biopsies can provide more detailed and accurate information about structural components, cellular patterns and expression of inflammatory mediators. Similarly to the lower airways, many recent studies have evaluated sinonasal diseases by measuring nNO, which is a simple, rapid, well-tolerated, and noninvasive method [6]. In the clinical setting, the identification of biomarkers in peripheral blood is relatively cost-effective and readily available.
Biomarker discovery in CRSwNP is a steadily developing field, and different kinds of biomarkers have been explored in well-defined patient cohorts. At present, most of the literature on CRSwNP biomarkers is concerned with proof-of-concept studies of single markers which have been deduced from related biological processes in other diseases such as asthma and atopic dermatitis, or have been identified from genomic and proteomic data. For instance, Liu et al. [7] discovered 192 upregulated and 156 downregulated disease-related genes in polyp tissue by DNA microarray technology. Using standard proteomic methodology, Upton et al. [8] identified more than 300 differentially expressed proteins in sinonasal mucosa of CRSwNP patients. Theoretically, all biological components participating in pathophysiological processes could be eligible candidate biomarkers. Nevertheless, each candidate is involved in different molecular pathways and may capture only a fraction of the information. Consequently, a multiplex panel of biomarkers will be required to better clarify such complex pathological processes and to improve their predictive power.
Biomarkers for CRSwNP evaluation and management
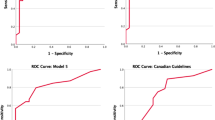
In the context of pathogenic mechanisms, CRSwNP biomarkers appear to fall into several main categories, including eosinophils, type 2 cytokines, immunoglobulins, remodeling factors, and nNO, along with molecules involved in steroid responsiveness and olfactory loss (Fig. 1).
Schematic overview of various biomarkers involved in the pathophysiology of CRSwNP. On exposure to pathogens or allergens, epithelial cells (ECs) can release TSLP, IL-25, and IL-33, which subsequently act on ILC2s to produce IL-5 and IL-13. In addition, TSLP stimulates DCs to induce Th2-cell differentiation with an amplified type 2 cytokine response. Furthermore, IL-5 is responsible for promoting eosinophil recruitment, activation, and survival. IL-4 and IL-13 not only promote basilar secretion of periostin from ECs, but also contribute to local production of antibodies, including several autoantibodies in severe cases. In addition, NO is constantly being released in the nasal airways. Abnormal expression of MUC1 and MUC4 in ECs may cause steroid resistance. MUC1, Mucin 1; MUC4, Mucin 4; nNO, nasal nitric oxide; TSLP, thymic stromal lymphopoietin; DC, dendritic cell; ILC2, type 2 innate lymphoid cell
Tissue and blood eosinophils
Classically, eosinophils are considered key effector cells infiltrating the polyp tissue. However, more than 50% of CRSwNP cases in East Asia present noneosinophilic inflammation [9, 10]. In general, eosinophilic nasal polyps (NPs) are pharmacologically glucocorticoid responsive, but noneosinophilic or neutrophilic CRSwNP is frequently resistant to steroid treatment [11–13]. Moreover, tissue eosinophilia has been recognized as a valuable predictor of augmented disease severity and worse prognosis after endoscopic sinus surgery (ESS) [14, 15]. Hence, several groups have argued endotyping patients into eosinophilic versus noneosinophilic subtypes to establish a personalized treatment plan. Currently, there is no unanimous histopathologic criterion to exactly define tissue eosinophilia. Kountakis et al. [16] proposed a cut-point of >5 eosinophils per high-power field (HPF) based on the degree of activated eosinophils and patients with tissue eosinophilia had more severe disease as measured by computed tomography (CT) and endoscopy scores. In a study by Soler et al. [17], mucosal eosinophilia was defined as >10 eosinophils/HPF, because this was predictive for less QOL improvement after surgery. More recently, Lou et al. [18] enrolled 387 Chinese patients with CRSwNP in a cohort and demonstrated that a tissue eosinophil proportion of >27% or an absolute tissue eosinophil count of >55 eosinophils/HPF predicted the relapse of NPs within 2 years after ESS. Tokunaga et al. [19] used a larger cohort of patients in Japan and found that tissue eosinophilia of more than 70 eosinophils/HPF was strongly associated with recurrence after surgery.
Blood eosinophilia is also correlated with CRS outcomes. Matsuwaki et al. [20] reported that CRS patients with peripheral eosinophil count above 520/μl were more likely to experience relapse within 5 years after ESS. As an alternative, blood eosinophil levels have been investigated as a potential surrogate marker for tissue eosinophilic inflammation in CRS and are easy to obtain in an outpatient setting [14]. In one study [21], a blood eosinophil percentage of ≥6% predicted eosinophilic CRS with a sensitivity of 97.4% and a specificity of 70.7%. In another study [22], a blood eosinophil number of 0.16 × 109/L yielded a sensitivity of 84.9% and a specificity of 84.4% and a blood eosinophil ratio of 2.05% yielded a sensitivity of 89.0% and a specificity of 84.4% for the diagnosis of eosinophilic CRS. Of note, various disorders and causes, including allergies, autoimmune diseases, adverse drug reactions and parasitic infections, can alter circulating eosinophil counts [23]. Accordingly, blood eosinophilia does not necessarily reflect tissue eosinophilia and its utility remains limited.
Type 2 cytokines as promising therapeutic targets
IL-5 is a crucial driver for eosinophil recruitment, activation, and survival [24]. In patients with CRSwNP, it has been confirmed as the main positive determinant of eosinophilic inflammation [25]. IL-5 positive NPs are associated with a higher likelihood of suffering from comorbid asthma and revision surgery [25–27]. Furthermore, a recent cluster analysis generated 10 inflammatory endotypes of CRS based on an array of biomarkers, and IL-5 was a critical parameter to dictate the phenotype with NPs and asthma [28]. Therefore, IL-5 plays an important role in CRSwNP pathogenesis and anti-IL-5 treatment may be a promising therapeutic strategy in these patients. Indeed, two clinical trials have examined the potential of IL-5 antagonism in cases with severe CRSwNP. Reslizumab and mepolizumab, which are both humanized antibodies directed against IL-5, significantly reduced the size of NPs and the number of blood eosinophils [29, 30]. Interestingly, IL-5 levels in nasal secretions were found to predict the response to treatment with reslizumab [29], thus emphasizing the importance of biomarkers for the appropriate patient selection.
IL-4 and IL-13 are also essential cytokines that activate type 2 inflammatory responses. They synergistically promote the synthesis of IgE from B cells and stimulate mucus secretion in epithelial cells (ECs). Despite the lack of association between these two cytokines and conventional measures of disease burden, blocking the IL-4/IL-13 signaling pathway has become a major step forward in the management of CRSwNP [31]. In a recent Phase II clinical trial, dupilumab, a fully human monoclonal antibody to the α subunit shared by IL-4 and IL-13 receptors, significantly improved clinical, endoscopic, radiological, and pharmacodynamic outcomes in patients with nasal polyposis after 16 weeks [32].
In addition, there is growing evidence that newly identified epithelial-derived cytokines, including IL-25, IL-33, and thymic stromal lymphopoietin (TSLP), have the capacity to shape the type 2 inflammatory milieu via effects on dendritic cells (DCs), mast cells, and group 2 innate lymphoid cells (ILC2s), as well as adaptive Th2 cells [33–36]. IL-25, also known as IL-17E, is a member of the IL-17 cytokine family. It has been reported that increased IL-25 expression is associated with poor CT scores and elevated blood eosinophil numbers in CRS patients [37]. In a murine NP model, IL-25 blockade not only reduced the number of polypoid lesions and the thickness of edematous mucosa, but also suppressed infiltration of inflammatory cells and expression of associated chemokines and cytokines, thus indicating the possibility of IL-25 as a novel pharmacologic target for CRSwNP patients [38].
IL-33, which is a nuclear cytokine from the IL-1 family and a ligand for the orphan IL-1 family receptor ST2, plays a pathogenic role in several Th2-related inflammatory diseases [39, 40]. Inhibition of the IL-33/ST2 signaling pathway has been shown to ameliorate eosinophilic airway inflammation and to reduce Th2 cytokine production in a murine model of allergic asthma [41]. In the case of CRS, one study reported that baseline expression levels of IL-33 were markedly increased in treatment-recalcitrant patients with CRSwNP [42]. Another study found that IL-33 concentrations were negatively associated with CT findings in CRS patients [43]. Intriguingly, in a recent study by Kim et al. [44], IL-33 was related to the expression of various Th1/Th17 cytokines and neutrophil recruitment in Asian patients with CRSwNP. Moreover, in a murine model of CRS, IL-33 neutralizing antibody diminished mucosal thickness and subepithelial collagen deposition, and inhibited infiltration of neutrophils. These findings indicate that IL-33 may represent a potential new therapeutic target for noneosinophilic CRSwNP.
TSLP, an IL-7-like cytokine, appears to facilitate Th2-skewed responses and subsequent recruitment of eosinophils in the airways. Enhanced expression and activity of TSLP have been found in polyp tissue [45]. Furthermore, TSLP expression positively correlated with the markers of Th2-biased eosinophilic inflammation in sinonasal mucosa and with symptom and CT scores in eosinophilic CRSwNP [46]. More importantly, in a Phase II double-blind, placebo-controlled trial, AMG 157, a human monoclonal antibody binding to TSLP, has been shown to attenuate allergen-induced early and late asthmatic responses and to reduce sputum and blood eosinophils in patients with allergic asthma [47]. Since TSLP also contributes to type 2 immunity in CRSwNP, neutralizing TSLP may become an effective pharmacologic method in patients with eosinophilic CRSwNP.
B-cell-associated biomarkers
B cells are one of the most important components of adaptive immunity. It is becoming increasingly apparent that B cells may play an essential role in perpetuating inflammatory reactions observed in patients with CRSwNP [48]. The numbers of naïve B cells and activated plasma cells are significantly upregulated within nasal polyp tissue [49]. In addition to their ability to secrete pro-inflammatory mediators and function as antigen-presenting cells for T cells, B cells can produce a variety of antibodies at mucosal sites. It has been well documented that levels of many different isotypes of immunoglobulins are highly elevated in NPs, but not in sera, of patients with CRSwNP, indicating a local immune response rather than a systemic response [49].
Mucosal tissue polyclonal IgE, as a major contributing factor in CRSwNP, has already been studied with some showing promising results [50]. Bachert et al. [51] found that concentrations of total IgE correlated significantly with levels of eosinophil cationic protein (ECP) and IL-5, and thus local eosinophilic inflammation. In a prospective follow-up study performed over 12 years after ESS, Gevaert et al. [26] showed that high local IgE could predict whether a patient was likely to experience a recurrence requiring repeated surgery. Furthermore, in patients with CRSwNP, tissue IgE and specific IgE against S. aureus enterotoxins (SE-IgE) were identified as risk factors for the comorbidity of asthma [25]. Finally, in a recent proof-of-concept clinical trial, omalizumab, a recombinant humanized monoclonal antibody to IgE, demonstrated significantly improvements in clinical parameters, symptoms, and QOL measures in patients with CRSwNP and comorbid asthma, irrespective of their allergic status [52]. Therefore, IgE may be an attractive therapeutic target in a specific subset of patients with CRSwNP.
In addition, the levels of several autoantibodies have been reported to be increased in CRS patients. Tan et al. [53] showed that IgG and IgA autoantibodies against nuclear antigens were highly elevated in polyp tissue, and anti-dsDNA IgG antibody was strongly correlated with a more severe clinical course necessitating a second surgical intervention. In addition, Goncalves et al. [54] detected antineutrophil cytoplasmic antibodies (ANCA) in serum samples in 49 consecutive CRS patients, and concluded that ANCA might be a helpful clue in establishing the early diagnosis of undisclosed vasculitides in a subset of difficult-to-treat CRS patients. Collectively, the presence of several specific autoantibodies insinuates a more aggressive form of CRS and may be used as clinically useful biomarkers.
Markers of tissue remodeling
Besides the persistent airway inflammation, tissue remodeling is another cardinal pathologic feature of CRSwNP. It is a dynamic process of formation and degradation of extracellular matrix (ECM), leading to transient or permanent changes in tissue architecture [55]. In CRSwNP, it is exhibited in both the mucosa and bone, characterized by epithelial damage and erosions, basement membrane thickening, massive stromal edema, pseudocyst formation, and osteitis [56]. Matrix metalloproteinases (MMPs) are key enzymes with proteolytic activities that can degrade various components of ECM and contribute to progressive histologic changes. Among the MMP family, MMP-9 levels have been extensively reported to be increased in NPs [57–60]. However, no significant correlation has been demonstrated between MMP-9 expression and the severity of CRSwNP assessed by CT scans and polyp grades [58, 60]. Furthermore, Watelet et al. [61, 62] have found that MMP-9 concentrations in nasal fluids are linked to MMP-9 expression inside the ECM, and high MMP-9 amounts in the pre- and postoperative period predict unfavorable healing outcome after ESS. In addition, MMP-9 may also serve as an interesting therapeutic target in CRSwNP. Doxycycline possesses an anti-MMP effect, and has been shown to significantly lower MMP-9 levels in secretions, modify polyp size, and ameliorate postoperative healing quality [63, 64].
Periostin is a secreted extracellular protein that has emerged as a marker in pathologic remodeling process. Periostin is produced mainly by ECs in response to IL-4 and IL-13 and has a pivotal role in subepithelial fibrosis [65, 66]. Periostin expression has been confirmed to be increased in patients with CRSwNP, independent of their atopic status or comorbid asthma [65]. Elevated periostin in the sera and nasal fluids may be used to differentiate between patients with CRSwNP and healthy subjects or patients with allergic rhinitis [67]. Moreover, Zhang et al. [68] found that periostin expression was elevated in active CRS, and decreased after effective treatment, suggesting that periostin could represent an indicator of disease activity and responsiveness to therapy. On the other hand, periostin has been perceived as a marker of Th2-type eosinophilic inflammation. Tissue periostin levels were significantly associated with IL-5 expression [65]. In eosinophilic CRSwNP, periosin levels positively correlated with radiographic findings [69].
Nasal nitric oxide
Nitric oxide is a regulatory mediator widespread in the body. In the nasal airways, it is produced constantly from ECs lining the paranasal sinuses, and contributes to local host defense by bacteriostatic and antiviral properties and by stimulation of ciliary motility [6]. Numerous reports have so far supported a role for nNO in CRSwNP assessment and management. A frank decrease in nNO has been observed in patients with nasal polyposis, mainly because of sinus ostial occlusion and failure of gaseous NO in the sinuses to reach the nasal cavities [70, 71]. Testing for nNO might be valuable for the distinction of subjects having NPs from those without NPs. Jeong et al. [72] reported that the cut-point of less than 163 ppb was suggestive of CRSwNP with a sensitivity of 81.3% and a specificity of 93.3%. In symptomatic patients suspected of having CRS, nNO cut-off value of <442 ppb could allow for screening and diagnosis of patients suffering from CRSwNP with a sensitivity of 87% and a specificity of 91% [73].
In addition, in cases of CRSwNP, the initial nNO levels correlated inversely with the extent of sinus disease as documented by CT changes and endoscopic appearances, and might fill the niche for an objective and noninvasive measure of NP severity [70–74]. Following surgical or medical treatment, the levels of nNO were dramatically elevated in parallel with improvements in an array of clinical markers of disease activity [71, 74, 75]. Hence, the change in nNO over time could help to assess the patency of sinus ostium and to determine the effectiveness of therapeutic interventions.
Biomarkers of corticosteroid responsiveness
Glucocorticoids (GCs) remain the mainstay of CRS treatment and are most effective drugs to control NP inflammation and growth. However, the response to GCs is variable and a proportion of patients exhibit steroid insensitivity [76]. Given these observations, biomarkers used for identification of GC-resistance may allow more tailored therapy, while minimizing inappropriate use and undesirable side-effects. As previously discussed, Wen et al. [11] revealed that increased accumulation of neutrophils in NPs was correlated with corticosteroid hyporesponsiveness. In addition, glucocorticoid receptor β (GRβ), an endogenous inhibitor of GC action, appears to be linked to steroid treatment response in CRSwNP [77, 78]. In one study, Hamilos et al. [79] reported an inverse relationship between baseline GRβ expression in NP inflammatory cells and the efficacy of topical fluticasone. In another study, Valera et al. [80] found higher expression of GRβ in poor responders following 2-month treatment with intranasal budesonide.
Recently, studies on the anti-inflammatory effects of GCs demonstrated that the abnormal expression level of mucin 1 (MUC1) and mucin 4 (MUC4) might be functionally involved in steroid resistance. Milara et al. [81] showed that MUC1 expression was significantly downregulated in NP epithelium of CRSwNP patients resistant to systemic corticosteroids. Opposite results were observed for MUC4 expression [82]. Thus, the higher ratio of MUC4/MUC1 in patients with CRSwNP could help to distinguish poor versus favorable responders.
Biomarkers for assessment of olfactory function
Olfaction is an important sensory function and is deeply involved in appetite, motivation, and libido. Olfactory loss represents a frequent complaint for patients with CRS, especially with CRSwNP, and has a significant long-term impact on QOL [2, 83]. It has been reported that eosinophilic CRS can induce more severe smell impairment even in early stages [12]. In a study by Mori et al. [84], serum total IgE ≥ 400 IU/ml was identified as an independent risk factor for olfactory loss in patients with eosinophilic CRS. In addition, treatment with anti-IgE agents could contribute to a significant improvement in subjective olfactory function [52]. More recently, it has been found that increased levels of eosinophils within the olfactory tissue were strongly related to olfactory disturbance in CRSwNP patients, implying that local eosinophils might act as essential effectors in olfactory dysfunction [85]. Schlosser et al. [86] examined correlations between an array of inflammatory mediators in mucus from the olfactory cleft and objective olfactory function assessed using the Sniffin’ Sticks test, and found that IL-5 levels correlated inversely with olfactory scores irrespective of polyp status. In addition, neuron-specific enolase (NSE), as an indicator of neuronal injury, has been reported to be elevated in nasal secretions in CRSwNP patients, and the higher concentrations of NSE were linked to worse olfactory function [87].
Conclusion
The heterogeneous nature of CRSwNP is progressively being recognized and acknowledged, necessitating the discovery, refinement, and utilization of biomarkers to delineate specific endotypes, monitor disease activity, and determine the optimized therapeutic modality. Currently, various potential biomarkers have been explored in nasal secretions, nasal biopsies, exhaled air, and peripheral blood. Tissue eosinophil count represents a valuable marker for endotyping, assessing disease severity, predicting steroid responsiveness and NP recurrence after ESS. Blood eosinophilia is related to tissue levels, whereas its utility remains limited. Type 2 cytokines and IgE have been proposed as essential targets for biological therapies. Furthermore, MMP-9 is correlated with postoperative healing quality. Measuring nNO may serve as a noninvasive tool for assessment of sinus ostial patency. In addition, MUC1 and MUC4 are novel biomarkers involved in steroid resistance. NSE appears to be a useful indicator for olfactory dysfunction. Despite these promising results, very few of biomarkers have emerged with sufficient power and enough evidence to support their feasibility and reproducibility in routine clinical practice. Longitudinal and prospective studies are needed to better characterize the role of biomarkers, individually or in combination, in the evaluation and management of CRSwNP.
References
Fokkens WJ, Lund VJ, Mullol J et al (2012) EPOS 2012: European position paper on rhinosinusitis and nasal polyps 2012. A summary for otorhinolaryngologists. Rhinology 50:1–12
Stevens WW, Schleimer RP, Kern RC (2016) Chronic rhinosinusitis with nasal polyps. J Allergy Clin Immunol Pract 4:565–572
Akdis CA, Bachert C, Cingi C, Dykewicz MS, Hellings PW, Naclerio RM, Schleimer RP, Ledford D (2013) Endotypes and phenotypes of chronic rhinosinusitis: a PRACTALL document of the European Academy of Allergy and Clinical Immunology and the American Academy of Allergy, Asthma & Immunology. J Allergy Clin Immunol 131:1479–1490
Taylor DR (2011) Using biomarkers in the assessment of airways disease. J Allergy Clin Immunol 128:927–934 (quiz 935–936)
Oyer SL, Mulligan JK, Psaltis AJ, Henriquez OA, Schlosser RJ (2013) Cytokine correlation between sinus tissue and nasal secretions among chronic rhinosinusitis and controls. Laryngoscope 123:E72–E78
Phillips PS, Sacks R, Marcells GN, Cohen NA, Harvey RJ (2011) Nasal nitric oxide and sinonasal disease: a systematic review of published evidence. Otolaryngol Head Neck Surg 144:159–169
Liu Z, Kim J, Sypek JP, Wang IM, Horton H, Oppenheim FG, Bochner BS (2004) Gene expression profiles in human nasal polyp tissues studied by means of DNA microarray. J Allergy Clin Immunol 114:783–790
Upton DC, Welham NV, Kuo JS, Walker JW, Pasic TR (2011) Chronic rhinosinusitis with nasal polyps: a proteomic analysis. Ann Otol Rhinol Laryngol 120:780–786
Cao PP, Li HB, Wang BF et al (2009) Distinct immunopathologic characteristics of various types of chronic rhinosinusitis in adult Chinese. J Allergy Clin Immunol 124:478–484, 484.e1–2
Ikeda K, Shiozawa A, Ono N, Kusunoki T, Hirotsu M, Homma H, Saitoh T, Murata J (2013) Subclassification of chronic rhinosinusitis with nasal polyp based on eosinophil and neutrophil. Laryngoscope 123:E1–E9
Wen W, Liu W, Zhang L et al (2012) Increased neutrophilia in nasal polyps reduces the response to oral corticosteroid therapy. J Allergy Clin Immunol 129:1522–1528.e5
Ishitoya J, Sakuma Y, Tsukuda M (2010) Eosinophilic chronic rhinosinusitis in Japan. Allergol Int 59:239–245
Bachert C, Zhang L, Gevaert P (2015) Current and future treatment options for adult chronic rhinosinusitis: focus on nasal polyposis. J Allergy Clin Immunol 136:1431–1440 (quiz 1441)
Snidvongs K, Lam M, Sacks R, Earls P, Kalish L, Phillips PS, Pratt E, Harvey RJ (2012) Structured histopathology profiling of chronic rhinosinusitis in routine practice. Int Forum Allergy Rhinol 2:376–385
Ottaviano G, Cappellesso R, Mylonakis I et al (2015) Endoglin (CD105) expression in sinonasal polyposis. Eur Arch Otorhinolaryngol 272:3367–3373
Kountakis SE, Arango P, Bradley D, Wade ZK, Borish L (2004) Molecular and cellular staging for the severity of chronic rhinosinusitis. Laryngoscope 114:1895–1905
Soler ZM, Sauer D, Mace J, Smith TL (2010) Impact of mucosal eosinophilia and nasal polyposis on quality-of-life outcomes after sinus surgery. Otolaryngol Head Neck Surg 142:64–71
Lou H, Meng Y, Piao Y, Wang C, Zhang L, Bachert C (2015) Predictive significance of tissue eosinophilia for nasal polyp recurrence in the Chinese population. Am J Rhinol Allergy 29:350–356
Tokunaga T, Sakashita M, Haruna T et al (2015) Novel scoring system and algorithm for classifying chronic rhinosinusitis: the JESREC Study. Allergy 70:995–1003
Matsuwaki Y, Ookushi T, Asaka D et al (2008) Chronic rhinosinusitis: risk factors for the recurrence of chronic rhinosinusitis based on 5-year follow-up after endoscopic sinus surgery. Int Arch Allergy Immunol 146(Suppl 1):77–81
Sakuma Y, Ishitoya J, Komatsu M et al (2011) New clinical diagnostic criteria for eosinophilic chronic rhinosinusitis. Auris Nasus Larynx 38:583–588
Zuo K, Guo J, Chen F, Xu R, Xu G, Shi J, Li H (2014) Clinical characteristics and surrogate markers of eosinophilic chronic rhinosinusitis in Southern China. Eur Arch Otorhinolaryngol 271:2461–2468
Roufosse F, Weller PF (2010) Practical approach to the patient with hypereosinophilia. J Allergy Clin Immunol 126:39–44
Gevaert P, Bachert C, Holtappels G et al (2003) Enhanced soluble interleukin-5 receptor alpha expression in nasal polyposis. Allergy 58:371–379
Bachert C, Zhang N, Holtappels G et al (2010) Presence of IL-5 protein and IgE antibodies to staphylococcal enterotoxins in nasal polyps is associated with comorbid asthma. J Allergy Clin Immunol 126:962–968, 968.e1–6
Gevaert P, Calus L, Van Bruaene N, Van Zele T, Bachert C (2015) Allergic sensitization, high local IL-5 and IgE predict surgical outcome 12 years after endoscopic sinus surgery for chronic rhinosinusitis with nasal polyposis. J Allergy Clin Immunol 135:AB238
Van Zele T, Holtappels G, Gevaert P, Bachert C (2014) Differences in initial immunoprofiles between recurrent and nonrecurrent chronic rhinosinusitis with nasal polyps. Am J Rhinol Allergy 28:192–198
Tomassen P, Vandeplas G, Van Zele T et al (2016) Inflammatory endotypes of chronic rhinosinusitis based on cluster analysis of biomarkers. J Allergy Clin Immunol 137:1449–1456.e4
Gevaert P, Lang-Loidolt D, Lackner A et al (2006) Nasal IL-5 levels determine the response to anti-IL-5 treatment in patients with nasal polyps. J Allergy Clin Immunol 118:1133–1141
Gevaert P, Van Bruaene N, Cattaert T et al (2011) Mepolizumab, a humanized anti-IL-5 mAb, as a treatment option for severe nasal polyposis. J Allergy Clin Immunol 128:989–995.e1–e8
Pauwels B, Jonstam K, Bachert C (2015) Emerging biologics for the treatment of chronic rhinosinusitis. Expert Rev Clin Immunol 11:349–361
Bachert C, Mannent L, Naclerio RM et al (2016) Effect of subcutaneous dupilumab on nasal polyp burden in patients with chronic sinusitis and nasal polyposis: a randomized clinical trial. JAMA 315:469–479
Kato A (2015) Immunopathology of chronic rhinosinusitis. Allergol Int 64:121–130
Lam EP, Kariyawasam HH, Rana BM et al (2016) IL-25/IL-33-responsive TH2 cells characterize nasal polyps with a default TH17 signature in nasal mucosa. J Allergy Clin Immunol 137:1514–1524
Mjosberg JM, Trifari S, Crellin NK et al (2011) Human IL-25- and IL-33-responsive type 2 innate lymphoid cells are defined by expression of CRTH2 and CD161. Nat Immunol 12:1055–1062
Shaw JL, Fakhri S, Citardi MJ, Porter PC, Corry DB, Kheradmand F, Liu YJ, Luong A (2013) IL-33-responsive innate lymphoid cells are an important source of IL-13 in chronic rhinosinusitis with nasal polyps. Am J Respir Crit Care Med 188:432–439
Lam M, Hull L, McLachlan R et al (2013) Clinical severity and epithelial endotypes in chronic rhinosinusitis. Int Forum Allergy Rhinol 3:121–128
Shin HW, Kim DK, Park MH et al (2015) IL-25 as a novel therapeutic target in nasal polyps of patients with chronic rhinosinusitis. J Allergy Clin Immunol 135:1476–1485.e7
Cayrol C, Girard JP (2014) IL-33: an alarmin cytokine with crucial roles in innate immunity, inflammation and allergy. Curr Opin Immunol 31:31–37
Cherry WB, Yoon J, Bartemes KR, Iijima K, Kita H (2008) A novel IL-1 family cytokine, IL-33, potently activates human eosinophils. J Allergy Clin Immunol 121:1484–1490
Lee HY, Rhee CK, Kang JY et al (2014) Blockade of IL-33/ST2 ameliorates airway inflammation in a murine model of allergic asthma. Exp Lung Res 40:66–76
Reh DD, Wang Y, Ramanathan M Jr, Lane AP (2010) Treatment-recalcitrant chronic rhinosinusitis with polyps is associated with altered epithelial cell expression of interleukin-33. Am J Rhinol Allergy 24:105–109
Ozturan A, Eyigor H, Eyigor M, Osma U, Yilmaz MD, Selcuk OT, Renda L, Gultekin M (2017) The role of IL-25 and IL-33 in chronic rhinosinusitis with or without nasal polyps. Eur Arch Otorhinolaryngol 274:283–288
Kim DK, Jin HR, Eun KM, Mo JH, Cho SH, Oh S, Cho D, Kim DW (2016) The role of interleukin-33 in chronic rhinosinusitis. Thorax
Nagarkar DR, Poposki JA, Tan BK et al (2013) Thymic stromal lymphopoietin activity is increased in nasal polyps of patients with chronic rhinosinusitis. J Allergy Clin Immunol 132:593–600.e12
Liao B, Cao PP, Zeng M et al (2015) Interaction of thymic stromal lymphopoietin, IL-33, and their receptors in epithelial cells in eosinophilic chronic rhinosinusitis with nasal polyps. Allergy 70:1169–1180
Gauvreau GM, O’Byrne PM, Boulet LP et al (2014) Effects of an anti-TSLP antibody on allergen-induced asthmatic responses. N Engl J Med 370:2102–2110
Stevens WW, Lee RJ, Schleimer RP, Cohen NA (2015) Chronic rhinosinusitis pathogenesis. J Allergy Clin Immunol 136:1442–1453
Hulse KE, Norton JE, Suh L et al (2013) Chronic rhinosinusitis with nasal polyps is characterized by B-cell inflammation and EBV-induced protein 2 expression. J Allergy Clin Immunol 131:1075–1083, 1083.e1–7
De Schryver E, Devuyst L, Derycke L, Dullaers M, Van Zele T, Bachert C, Gevaert P (2015) Local immunoglobulin e in the nasal mucosa: clinical implications. Allergy Asthma Immunol Res 7:321–331
Bachert C, Gevaert P, Holtappels G, Johansson SG, van Cauwenberge P (2001) Total and specific IgE in nasal polyps is related to local eosinophilic inflammation. J Allergy Clin Immunol 107:607–614
Gevaert P, Calus L, Van Zele T et al (2013) Omalizumab is effective in allergic and nonallergic patients with nasal polyps and asthma. J Allergy Clin Immunol 131:110–116.e1
Tan BK, Li QZ, Suh L et al (2011) Evidence for intranasal antinuclear autoantibodies in patients with chronic rhinosinusitis with nasal polyps. J Allergy Clin Immunol 128:1198–1206.e1
Goncalves C, Pinaffi JV, Carvalho JF et al (2007) Antineutrophil cytoplasmic antibodies in chronic rhinosinusitis may be a marker of undisclosed vasculitis. Am J Rhinol 21:691–694
Watelet JB, Dogne JM, Mullier F (2015) Remodeling and repair in rhinosinusitis. Curr Allergy Asthma Rep 15:34
Bassiouni A, Chen PG, Wormald PJ (2013) Mucosal remodeling and reversibility in chronic rhinosinusitis. Curr Opin Allergy Clin Immunol 13:4–12
Li X, Meng J, Qiao X et al (2010) Expression of TGF, matrix metalloproteinases, and tissue inhibitors in Chinese chronic rhinosinusitis. J Allergy Clin Immunol 125:1061–1068
Malinsky RR, Valera FC, Cavallari FE, Kupper DS, Milaneze C, Silva JS, Tamashiro E, Anselmo-Lima WT (2013) Matrix metalloproteinases and their impact on sinusal extension in chronic rhinosinusitis with nasal polyps. Eur Arch Otorhinolaryngol 270:1345–1348
Yeo NK, Eom DW, Oh MY, Lim HW, Song YJ (2013) Expression of matrix metalloproteinase 2 and 9 and tissue inhibitor of metalloproteinase 1 in nonrecurrent vs recurrent nasal polyps. Ann Allergy Asthma Immunol 111:205–210
Wang LF, Chien CY, Chiang FY, Chai CY, Tai CF (2012) Corelationship between matrix metalloproteinase 2 and 9 expression and severity of chronic rhinosinusitis with nasal polyposis. Am J Rhinol Allergy 26:e1–e4
Watelet JB, Claeys C, Van Cauwenberge P, Bachert C (2004) Predictive and monitoring value of matrix metalloproteinase-9 for healing quality after sinus surgery. Wound Repair Regen 12:412–418
Watelet JB, Demetter P, Claeys C, Van Cauwenberge P, Cuvelier C, Bachert C (2005) Neutrophil-derived metalloproteinase-9 predicts healing quality after sinus surgery. Laryngoscope 115:56–61
Van Zele T, Gevaert P, Holtappels G et al (2010) Oral steroids and doxycycline: two different approaches to treat nasal polyps. J Allergy Clin Immunol 125:1069–1076.e4
Huvenne W, Zhang N, Tijsma E et al (2008) Pilot study using doxycycline-releasing stents to ameliorate postoperative healing quality after sinus surgery. Wound Repair Regen 16:757–767
Wang M, Wang X, Zhang N et al (2015) Association of periostin expression with eosinophilic inflammation in nasal polyps. J Allergy Clin Immunol 136:1700–1703.e1–e9
Takayama G, Arima K, Kanaji T et al (2006) Periostin: a novel component of subepithelial fibrosis of bronchial asthma downstream of IL-4 and IL-13 signals. J Allergy Clin Immunol 118:98–104
Ohta N, Ishida A, Kurakami K et al (2014) Expressions and roles of periostin in otolaryngological diseases. Allergol Int 63:171–180
Zhang W, Hubin G, Endam LM, Al-Mot S, Filali-Mouhim A, Desrosiers M (2012) Expression of the extracellular matrix gene periostin is increased in chronic rhinosinusitis and decreases following successful endoscopic sinus surgery. Int Forum Allergy Rhinol 2:471–476
Kim DW, Kulka M, Jo A et al (2016) Cross-talk between human mast cells and epithelial cells by IgE-mediated periostin production in eosinophilic nasal polyps. J Allergy Clin Immunol
Delclaux C, Malinvaud D, Chevalier-Bidaud B, Callens E, Mahut B, Bonfils P (2008) Nitric oxide evaluation in upper and lower respiratory tracts in nasal polyposis. Clin Exp Allergy 38:1140–1147
Colantonio D, Brouillette L, Parikh A, Scadding GK (2002) Paradoxical low nasal nitric oxide in nasal polyposis. Clin Exp Allergy 32:698–701
Jeong JH, Yoo HS, Lee SH, Kim KR, Yoon HJ, Kim SH (2014) Nasal and exhaled nitric oxide in chronic rhinosinusitis with polyps. Am J Rhinol Allergy 28:e11–e16
Bommarito L, Guida G, Heffler E, Badiu I, Nebiolo F, Usai A, De Stefani A, Rolla G (2008) Nasal nitric oxide concentration in suspected chronic rhinosinusitis. Ann Allergy Asthma Immunol 101:358–362
Lee JM, McKnight CL, Aves T, Yip J, Grewal AS, Gupta S (2015) Nasal nitric oxide as a marker of sinus mucosal health in patients with nasal polyposis. Int Forum Allergy Rhinol 5:894–899
Vaidyanathan S, Williamson P, Anderson K, Lipworth B (2010) Effect of systemic steroids on humming nasal nitric oxide in chronic rhinosinusitis with nasal polyposis. Ann Allergy Asthma Immunol 105:412–417
Mullol J, Obando A, Pujols L, Alobid I (2009) Corticosteroid treatment in chronic rhinosinusitis: the possibilities and the limits. Immunol Allergy Clin North Am 29:657–668
Pujols L, Mullol J, Picado C (2010) Importance of glucocorticoid receptors in upper and lower airways. Front Biosci (Landmark Ed) 15:789–800
Grzanka A, Misiolek M, Golusinski W, Jarzab J (2011) Molecular mechanisms of glucocorticoids action: implications for treatment of rhinosinusitis and nasal polyposis. Eur Arch Otorhinolaryngol 268:247–253
Hamilos DL, Leung DY, Muro S, Kahn AM, Hamilos SS, Thawley SE, Hamid QA (2001) GRbeta expression in nasal polyp inflammatory cells and its relationship to the anti-inflammatory effects of intranasal fluticasone. J Allergy Clin Immunol 108:59–68
Valera FC, Queiroz R, Scrideli C, Tone LG, Anselmo-Lima WT (2009) Evaluating budesonide efficacy in nasal polyposis and predicting the resistance to treatment. Clin Exp Allergy 39:81–88
Milara J, Peiro T, Armengot M, Frias S, Morell A, Serrano A, Cortijo J (2015) Mucin 1 downregulation associates with corticosteroid resistance in chronic rhinosinusitis with nasal polyps. J Allergy Clin Immunol 135:470–476
Milara J, Morell A, Ballester B, Armengot M, Morcillo E, Cortijo J (2017) MUC4 impairs the anti-inflammatory effects of corticosteroids in patients with chronic rhinosinusitis with nasal polyps. J Allergy Clin Immunol 139:855–862.e13
Rombaux P, Huart C, Levie P, Cingi C, Hummel T (2016) Olfaction in chronic rhinosinusitis. Curr Allergy Asthma Rep 16:41
Mori E, Matsuwaki Y, Mitsuyama C, Okushi T, Nakajima T, Moriyama H (2013) Risk factors for olfactory dysfunction in chronic rhinosinusitis. Auris Nasus Larynx 40:465–469
Hulse KE, Stevens WW, Tan BK, Schleimer RP (2015) Pathogenesis of nasal polyposis. Clin Exp Allergy 45:328–346
Schlosser RJ, Mulligan JK, Hyer JM, Karnezis TT, Gudis DA, Soler ZM (2016) Mucous cytokine levels in chronic rhinosinusitis-associated olfactory loss. JAMA Otolaryngol Head Neck Surg 142:731–737
Tsybikov NN, Egorova EV, Kuznik BI, Fefelova EV, Magen E (2016) Neuron-specific enolase in nasal secretions as a novel biomarker of olfactory dysfunction in chronic rhinosinusitis. Am J Rhinol Allergy 30:65–69
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Funding
There was no funding for this study.
Rights and permissions
About this article
Cite this article
Yao, Y., Xie, S., Yang, C. et al. Biomarkers in the evaluation and management of chronic rhinosinusitis with nasal polyposis. Eur Arch Otorhinolaryngol 274, 3559–3566 (2017). https://doi.org/10.1007/s00405-017-4547-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-017-4547-2