Abstract
The aim of the study was to evaluate facial features and hyoid bone position in children with obstructive sleep apnea syndrome (OSAS) by cephalometric radiography. A prospective cross-sectional study was conducted in a tertiary referral hospital. Twenty-nine children in the 3–6 year age bracket were evaluated: 14 children with OSAS and 15 nasal-breathing children. All children underwent otorhinolaryngologic examination, and those with OSAS also underwent in-laboratory polysomnography for diagnostic confirmation. The children were then submitted to orthodontic evaluation and cephalometry. Lateral cephalometric radiographs from children with OSAS were compared to those of nasal-breathing children. We found no differences between the two groups regarding the linear and angular measurements of the face. However, the children with OSAS presented, already at the preschool age, with an inferiorly positioned hyoid bone, thus increasing the pharyngeal area. In children with OSAS, the hyoid bone appears to be in a significantly inferior position at an early age. Our findings provide evidence that there is a relationship between the position of the hyoid bone and OSAS in children, which could contribute to the persistence of OSAS into adulthood.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The craniofacial development that occurs after birth is complex and is directly related to genetic and environmental factors [1]. Upper airway obstruction, whether it affects the nasal cavities or the pharynx, leads to mouth breathing and, in more pronounced cases, to obstructive sleep apnea syndrome (OSAS). Mouth breathing causes postural changes, such as hypotonic lips, inferior/anterior tongue position, and clockwise rotation of the mandible, to stabilize the airways [2]. The main cause of both mouth breathing and OSAS in children is tonsillar hypertrophy [3, 4], and they are related to neurocognitive and cardiovascular consequences [5–7].
The literature has shown that adult patients with OSAS present craniofacial changes and changes in hyoid bone position [8]. A more inferior hyoid position, greater total anterior face height, and vertical development of the lower third of the anterior face are common in the adult population and have also been reported in school-age children [9, 10]. However, there is still no consensus in the literature as to whether this change in the position of the hyoid bone is a consequence of upper airway obstruction, following the clockwise rotation of the mandible, or whether the change is a possible predictor of or an aggravating factor for the disease. The purpose of the present study was to compare preschool children with OSAS and nasal-breathing children in the same age bracket in terms of facial skeletal changes and changes in the position of the hyoid bone.
Materials and methods
The present study was approved by the Research Ethics Committee of School of Dentistry of Ribeirão Preto—University of São Paulo (Process no. 2000.1.483.58.5). The parents or legal guardians of the participants gave written informed consent.
We selected patients with deciduous dentition who were in the 3–6 year age bracket. We excluded patients who presented with signs of systemic disorders, as well as those who had previously undergone palatal surgery, orthodontic treatment, or speech therapy, together with those having previously undergone ear, nose, and throat (ENT) surgery.
We divided the patients into two groups: OSAS; and age and sex matched nasal breathing (control). The OSAS group patients were selected from among those treated at the Mouth-Breathing Center—School of Medicine of Ribeirão Preto—University of São Paulo and presented symptoms of nocturnal mouth breathing, snoring and apneas, as well as confirmed exams, as detailed below. The nasal-breathing group patients were selected from among those treated at the Pediatric Clinical Dentistry—School of Dentistry of Ribeirão Preto—University of São Paulo, and did not present obstructive respiratory symptoms, agitated sleep or diurnal symptoms suggestive of respiratory sleep disturbance in children.
A questionnaire was administered to the parents or legal guardians to evaluate the intensity and frequency of respiratory symptoms. In addition, all of the children underwent ENT examination. Oroscopy was performed to grade palatine tonsil hypertrophy on the Brodsky scale, and nasal endoscopy was performed to identify associated nasal changes and grade adenoid hypertrophy in relation to the choanae [11]. Children in OSAS group presented in general palatine tonsils grade 3 or 4 and adenoids higher than 70 % of choanal area, whereas all nasal-breathing children presented only grade 1 or 2 for palatine tonsils, and adenoids were at most 50 % of choanal area.
The children selected in OSAS group also underwent full-night polysomnography, in accordance with the 2007 American Academy of Sleep Medicine criteria [12]. Only those with an apnea-hypopnea index >1 and symptoms consistent with OSAS were included in the OSAS group. The children in the control group underwent ENT examination to rule out any suspicion of chronic mouth breathing, in clinical history or examination. However, because of ethical issues, they did not undergo polysomnography.
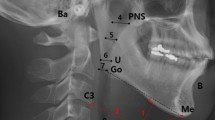
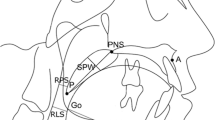
All the children underwent lateral cephalometric radiographs, as described by Ricketts. We obtained the following measurements, as depicted in Fig. 1:
-
N-Me: total anterior face height (i.e., the linear distance between the nasion and the menton)
-
N-ANS: upper anterior face height (i.e., the linear distance between the nasion and the anterior nasal spine [ANS])
-
ANS-Me: lower anterior face height (i.e., the linear distance between the ANS and the menton)
-
S-Gn: total posterior face height (i.e., the linear distance between the sella turcica and the gonion)
-
SNGoGn: angle formed by the base of the skull and the mandibular plane (i.e., the distance between the gonion and the menton), a measurement that characterizes facial morphology
-
HySN: vertical linear distance between the uppermost point of the body of the hyoid bone (point Hy) and the sella turcica
-
HyMP: vertical distance between point Hy and the mandibular plane
-
HyPP: vertical linear distance between the most anterior point of the body of the hyoid bone(point Hy) and the palatal plane (i.e., the distance between the ANS and the posterior nasal spine)
-
H.NP: horizontal linear distance between point H and the posterior wall of the nasopharynx
-
H.C3: linear measurement taken from point H to the most anterior and inferior point of C3
Polysomnography and ENT examination were performed solely to stratify the patients into groups. Therefore, the results of those tests were not submitted to statistical analysis.
We compared the orthodontic changes between the OSAS and the nasal-breathing groups using linear regression models, adjusting the comparisons by sex and age. In addition, we used simple linear regression models to evaluate the association between facial morphology and hyoid bone measurements. For all of the analyses, we obtained the estimated mean difference and their 95 % confidence intervals (95 %CI). The coefficient of determination (R 2) and Pearson’s correlation coefficient were calculated to evaluate the association between measurements. The level of significance was considered at 5 %. All analyses were performed with the program SAS, version 9.2 (SAS institute, Cary, NC, USA, 2008).
Results
A total of 29 non-obese children were selected. Of those, 15 were allocated to the nasal-breathing group (mean age, 5.07 years) and 14 were allocated to the OSAS group (mean age, 5.18 years).
All of the patients in the OSAS group had a history of snoring and apnea, and presented with palatine tonsils grade 3 or 4, and/or with adenoids obstructing more than 70 % of the choanae. Polysomnography revealed that six children had mild OSAS, one had moderate OSAS, and seven had severe OSAS.
The children in the nasal-breathing group had experienced obstructive respiratory symptoms for no more than 15 consecutive days and on no more than 4 occasions during the year. In addition, physical examination revealed the absence of nasal obstruction, as well as non-obstructive adenoids and palatine tonsils.
We found no differences between the two groups regarding both anterior and posterior linear measurements of the face or facial morphology (Table 1). In contrast, we found the hyoid bone to be positioned inferiorly to the palatal (44.5 ± 4.9 for nasal breathing vs. 48.7 ± 4.7 for OSAS, mean difference 4.37, 95 %CI (0.47; 8.26), p value = 0.03, Fig. 2) and mandibular planes (8.1 ± 3.7 for nasal breathing vs. 11.8 ± 4.4 for OSAS, mean difference 4.04, 95 %CI (0.83; 7.26), p value = 0.02, Fig. 3) in the OSAS group (Table 2). We also found a non-significant inferior hyoid bone position related to the skull base in this group (81.4 ± 5.9 for nasal breathing vs. 85.2 ± 5.3 for OSAS, mean difference 3.63, 95 %CI (−0.91;8.18), p value = 0.11, Figs. 3, 4). We found no differences between the two groups in terms of the anteroposterior relation of hyoid bone (Table 2).
We evaluated whether the inferior positioning of the hyoid bone was influenced by facial morphology. We found no association between facial morphology and the vertical distance from point Hy to the mandibular plane (correlation 0.03; R 2 = 0.001 and p value = 0.89) or between facial morphology and the vertical distance from point Hy and the palatal plane (correlation 0.11; R 2 = 0.01 and p value = 0.55), but there was a negative correlation between facial morphology and the distance from the point Hy to skull base (correlation −0.38; R 2 = 0.15 and p value = 0.04).
Discussion
Many studies have evaluated the influence of the breathing pattern on craniofacial development. However, most such studies have involved samples with a broad age bracket and have evaluated mouth-breathing children in general, and not only OSAS children, both of which affect the reliability of the results obtained. There have been few cephalometric studies involving preschool children with confirmed OSAS [10, 13].
According to Segal et al. [7], adult males are more likely to develop OSAS precisely because their greater length of the upper airways unsupported by bone structure, a characteristic that is directly related to an inferiorly positioned hyoid bone. Other articles [14, 15] have related OSAS in adult patients to greater anterior face height (total and lower), clockwise rotation of the mandible, and inferiorly positioned hyoid bone.
On the basis of the abovementioned data and an increased accessibility to the gold standard methods for the diagnosis of OSAS in children, researchers set out to determine when those characteristics begin to emerge. In this context, there have been some studies involving school-age children.
According to Juliano et al. [16], an anterior position of the hyoid bone is noticeable in mouth-breathing children in the 8−14 year age bracket, when compared with controls. However, the respiratory characteristics were not determined by in-laboratory polysomnography.
Pirilä-Parkkinen et al. [17] compared children from 4 to 12 years old with sleep-disordered breathing (as confirmed by overnight polysomnography) and those without and found greater clockwise rotation of the mandible, increased facial height, and inferiorly positioned hyoid bone in the former.
Vieira et al. [10] observed that children with OSAS (as confirmed by polysomnography) in the 7−10 year age bracket presented significant greater total anterior face height, vertical development of the lower anterior face, and anteroinferior position of the hyoid bone when compared to a control group.
The abovementioned characteristics are similar to those observed in adults with OSAS, and led a question to be answered: is the hyoid bone positioned inferiorly because of the respiratory problem—or does this occur at a very early age, contributing to the development of OSAS and its persistence in older children and in adults?
In the present study, we found that the OSAS had little influence on the facial features of preschool children. These results are in agreement with those obtained by Valera et al. [2], who stated that preschool mouth-breathing children (who had not undergone polysomnography) presented significant postural and functional changes, but no differences in terms of their facial features, when compared to a control group. In contrast, Zettergren-Wijk et al. [4] found increased anterior face height in preschool children with OSAS.
In the present study, we found the hyoid bone to be positioned significantly inferior to the palatal and mandibular planes in the children with OSAS, with no direct relationship between this observation and a longer facial pattern. There have been no previous studies relating the position of the hyoid bone and the presence of OSAS in preschool children.
The results presented here suggest that the breathing pattern influences the facial skeletal features of children with OSAS at later ages, but not in preschool children. In contrast, an inferiorly positioned hyoid bone is seen at an early age in children with OSAS, being markedly present in preschool children. This hyoid position could contribute to perpetuation of OSAS after adenotonsillectomy, because these patients present longer upper airways. However, further studies correlating OSAS with hyoid bone characteristics in preschool children are needed to confirm this supposition.
On the basis of the results obtained, we conclude that there are no differences between children with OSAS and nasal-breathing children in the 3−6 year age bracket in terms of the anterior face height, posterior face height, and facial morphology. However, the position of the hyoid bone is markedly inferior in children with OSAS. There was no relationship between the position of the hyoid bone and facial morphology.
References
Shintani T, Asakura K, Kataura A (1996) Adenotonsillar hypertrophy and skeletal morphology of children with obstructive sleep apnea syndrome. Acta Otolaryngol Suppl 523:222–224
Valera FC, Travitzki LV, Mattar SE, Matsumoto MA, Elias AM, Anselmo-Lima WT (2003) Muscular, functional and orthodontic changes in pre school children with enlarged adenoids and tonsils. Int J Pediatr Otorhinolaryngol 67:761–770
Bower C, Buckmiller L (2001) What’s new in pediatric obstructive sleep apnea. Curr Opin Otolaryngol Head Neck Surg 9:352–358
Zettergren-Wijk L, Forsberg CM, Linder-Aronson S (2006) Changes in dentofacial morphology after adeno-/tonsillectomy in young children with obstructive sleep apnoea—a 5-year follow-up study. Eur J Orthod 28:319–326
Marcus CL, Greene MG, Carroll JL (1998) Blood pressure in children with obstructive sleep apnea. Am J Respir Crit Care Med 157:1098–1103
Gozal D, Wang M, Pope DW Jr (2001) Objective sleepiness measures in pediatric obstructive sleep apnea. Pediatrics 108:693–697
Segal Y, Malhotra A, Pillar G (2008) Upper airway length may be associated with the severity of obstructive sleep apnea syndrome. Sleep Breath 12:311–316
Zucconi M, Ferini-Strambi L, Palazzi S, Orena C, Zonta S, Smirne S (1992) Habitual snoring with and without obstructive sleep apnoea: the importance of cephalometric variables. Thorax 47:157–161
Battagel JM, Johal A, Smith AM, Kotecha B (2002) Postural variation in oropharyngeal dimensions in subjects with sleep disordered breathing: a cephalometric study. Eur J Orthod 24:263–276
Vieira BB, Itikawa CE, de Almeida LA et al (2011) Cephalometric evaluation of facial pattern and hyoid bone position in children with obstructive sleep apnea syndrome. Int J Pediatr Otorhinolaryngol 75:383–386
Li KK, Guilleminault C, Riley RW, Powell NB (2002) Obstructive sleep apnea and maxillomandibular advancement: an assessment of airway changes using radiographic and nasopharyngoscopic examinations. J Oral Maxillofac Surg 60:526–530
American Academy of Sleep Medicine (2007) The AASM manual for the scoring of sleep and associated Events: rules, terminology and technical specifications, 1st ed. Westchester, IL
Ozdemir H, Altin R, Söğüt A et al (2004) Craniofacial differences according to AHI scores of children with obstructive sleep apnoea syndrome: cephalometric study in 39 patients. Pediatr Radiol 34:393–399
Gulati A, Chate RA, Howes TQ (2010) Can a single cephalometric measurement predict obstructive sleep apnea severity? J Clin Sleep Med 156:64–68
Peltomäki T (2007) The effect of mode of breathing on craniofacial growth–revisited. Eur J Orthod 29:426–429
Juliano ML, Machado MAC, de Carvalho LBC, do Prado LBF, do Prado GF (2009) Mouth breathing children have cephalometric patterns similar to those of adult patients with obstructive sleep apnea syndrome. Arq Neuropsiquiatr 67:860–865
Pirilä-Parkkinen K, Löppönen H, Nieminen P, Tolonen U, Pirttiniemi P (2010) Cephalometric evaluation of children with nocturnal sleep-disordered breathing. Eur J Orthod 32:662–671
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Vieira, B.B., Itikawa, C.E., de Almeida, L.A. et al. Facial features and hyoid bone position in preschool children with obstructive sleep apnea syndrome. Eur Arch Otorhinolaryngol 271, 1305–1309 (2014). https://doi.org/10.1007/s00405-013-2770-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00405-013-2770-z