Abstract
Objective
The aim of this study was to evaluate the correlation between clinical, radiological and histopathological signs of scaphoid non-unions (SNU) with regard to the age of the fracture, primarily because this is relevant for therapy and compensation claims.
Materials and methods
Thirty-eight patients with SNU underwent clinical and radiological examination of the wrist prior to surgery. Preoperative X-rays of the wrist were analysed using the scores of Herbert and Fisher, Filan and Herbert, Trojan and Jahna, Gupta as well as scaphoid non-union advanced collapse. Sclerotic bone of the SNU was resected during surgery. Resected material was evaluated histologically after staining with hematoxylin–eosin and periodic acid-Schiff reaction. Radiological and histological examinations were performed by independent investigators in a blinded fashion.
Results
The preoperative range of motion of the injured compared to the contralateral wrist was significantly reduced for the dorsi- and palmar flexion and for the radial and ulnar deviation; however, this reduction was not time dependent. There was no significant correlation between the radiological results and the age of the SNU, while fibrous tissue or fibrocartilage in the fracture gap was present in all cases. Significantly less fibrous or fibrocartilage bone cysts (p = 0.041) and bone remodelling (p = 0.031) were seen in older SNU (at 45 months). Definitive sclerotic bone covering of the fracture edges was significantly more common in older SNU (p = 0.035).
Conclusion
Radiological and most of the conventional histological findings do not correlate with time after initial injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The scaphoid is the most frequently fractured carpal bone [1, 2]. The specific vascularization pattern of the scaphoid has to be regarded as predisposition to avascular necrosis [3]. There is no doubt that symptomatic non-union of the scaphoid remains a common and disabling problem [4]. The reasons for this high non-union rate are multifactorial and include failure to recognize the original injury, inadequate initial treatment and anatomical and physiological factors beyond the control of the physician [5]. A lot of scaphoid fractures are work-related injuries [6]. The age of the scaphoid non-union (SNU) is a key factor for compensation claims and for therapy. The time course of development of a SNU after an unknown primary injury is an important criterion for establishing causality in compensation claims; something that has only rarely been possible with sufficient certainty. Multiple surgery options exist for the treatment of SNU, which are based on radiological signs. However, these signs are descriptive and only allow few conclusions about the time course of SNU, because the development of the SNU depends on many different factors.
Old SNU with a sclerotic proximal fragment could be treated with a partial mediocarpal arthrodesis [7]. New SNU are treated with resection of the sclerotic bone at the fracture edges, interposition of cancellous bone and compression osteosynthesis with a Herbert screw [4].
Systematic histological investigations of SNU with regard to the age of the non-union and the amount of bone remodelling do not exist. The aim of this study was to evaluate the correlation between clinical, radiological and histopathological signs of SNU with regard to the age of the fracture.
Methods
Patients
All protocols in this retrospective study were approved by the local ethics committee review board. The mean age of the 38 patients (3 women and 35 men) was 26 ± 12 years (12–56 years) at the time of injury. The mean time between injury and surgery for non-union of the scaphoid was 23 ± 28 months (4–144 months).Thirteen right and 25 left wrists were injured. Causes for scaphoid fractures included sports injury in 15 cases, fall on the wrist in 8 cases, traffic accident in 5 cases and other causes in 10 cases. Scaphoid fractures were not diagnosed initially in 12 of 38 cases, but the time of injury was known in all included cases.
Patients with prior surgical treatment of the wrist and associated adjacent injuries were excluded from this study. Thirty-eight patients with SNU underwent clinical and radiological examination of the wrist prior to surgery. Clinical examination included determination of range of motion of the wrist, which was measured with a standard goniometer.
Radiographic examination
Standard radiographs were taken, including a dorso-palmar and lateral view of the wrist. Additional radiographs of the wrist (“Böhler series”) were taken, including a view with the fist closed and maximum ulnar abduction of the wrist (Stecher view), an oblique view with a 45° wedge underneath the thumb (Schreck view or pen holder’s view), a view with the wrist in 30° dorsiflexion (Bridgeman view) and a view where the closed fist lies on a 30° wedge with a low ulnar abduction of the wrist (hyperpronation view).
Radiographs were taken within 2 weeks prior to surgery for all scaphoid non-unions less than 1 year old. In three cases with a SNU older than 3 years, time between radiographs and surgery was up to 3 months. Preoperative radiographs of the wrist were analysed independently according to Herbert and Fisher [4], Trojan and Jahna [8], scaphoid non-union advanced collapse (SNAC) [9] and Gupta [10] without knowing any clinical data of the patients.
The classification of Herbert and Fisher basically divides the scaphoid fractures and non-unions into four types. Type A includes acute stable fractures and type B acute unstable fractures. Type C shows signs of delayed union after six or more weeks. Type D fractures with established non-union must be differentiated from acute fractures, whereas type D1 is defined as fibrous non-union and type D2 as sclerotic non-union [4].
The classification of Trojan and Jahna divides SNU into three stages. Stage I is characterized by a resorption zone, stage II by resorption cysts and stage III sclerosis [8]. The classification of the SNAC wrist is divided into three stages. In stage I the arthritis is limited to the styloid process of the radius. In stage II the arthritis extends to the radioscaphoid joint and in stage III an additional mediocarpal arthritis exists [9].
The classification of Gupta divides SNU into five groups. Group I includes delayed unions with early “vacuolation” or “cystic die-back”. Group II are stable non-unions with fibrous or sclerotic non-union, no loss of volar bone stock, no carpal deformity and no degenerative changes. Group III are unstable non-unions with no degenerative changes, which are subdivided into type A with minimal displacement, volar cortical collapse with flexed scaphoid on tomograms or at surgery, cortical offset > 1 mm but <2 mm, a scapholunate angle < 80°, a capitolunate angle < 30° and no dorsiflexed intercalated segment instability (DISI) deformity. Group III type B is characterized by a marked deformity, a markedly flexed scaphoid, a cortical offset > 2 mm, a scapholunate angle > 80°, a capitolunate angle > 30° and a DISI deformity. Group IV are SNU with degenerative changes in the carpus, which are subdivided into type A with early degenerative changes in the radioscaphoid articulation, type B with moderate radioscaphoid degenerative changes and early midcarpal degeneration and type C with severe degeneration of the wrist joint with carpal collapse. Group V are SNU with proximal pole problems subdivided into type A with a small but viable pole (<20°) and type B with an avascular proximal pole [10].
Histological examination
During surgery sclerotic bone of the SNU was resected, cancellous bone was interpositioned and a compression osteosynthesis was performed using a Herbert screw [4]. Resected material was obtained from both the proximal and distal part of the SNU. Only cases with resected bone underlying the non-union were included in this study. Specimens were immediately fixed in 4% neutral buffered formalin for 24 h, decalcified with diaminoethanetetraacetic acid (EDTA), embedded in paraffin and sectioned with a thickness of 3 μm on a Leica rotation microtome. Subsequently, the tissue sections were stained with hematoxylin-eosin (H&E) and periodic acid-Schiff reaction (PAS). Histopathological examination of the stained tissue sections was performed using an Olympus BHS light microscope in the transmitted and polarized modes at final magnifications of 40×, 100×, 200× and 400×. Histopathological analysis was centred on osteopathological criteria including determination of synovium-like cellular lining, fibrous tissue or fibrocartilage in the fracture space, remodelling and sclerotic changes of the underlying bone, resorptive bone cysts with osteoclastic giant cells, cysts containing fibrous or fibrocartilage tissue as well as osteosclerosis or osteonecrosis of the resident bone [11].
Histopathological assignment to the classifications of Herbert and Fisher [4], Trojan and Jahna [8] was done in a blinded manner without knowing the age of the fracture, the clinical data of the patients or the radiographs. Morphological evidence for delayed fracture union or fibrous non-union of type C/D1 of the classification of Herbert and Fisher [4] was fibrous tissue or fibrocartilage in the fracture space. In addition, evidence of sclerotic bone at the fracture edges with cystic changes was seen in sclerotic non-union of type D2 of the classification of Herbert and Fisher [4]. According to the classification of Trojan and Jahna [8] in the stage of the resorption zone (stage I) a histiocytic and osteoclastic resorption of necrotic bones and detritus would be expected histologically. The stage of resorptive bone cysts (stage II) is characterized by cystic bone lesions rich in osteoclasts similar to the histological changes in secondary aneurysmatic bone cysts. The characteristic morphologic features of the third stage are fragment edges that are covered completely with sclerotic bone.
After completing the blinded radiological and histological analysis, a second radiological analysis was performed with knowledge of the clinical data (e.g. age of the fracture, range of wrist motion), with the same classifications as in the first radiological analysis as well as the classification of Filan and Herbert [12], which consists of clinical and radiological parameters. The fracture non-union is subdivided into five different types. Type 1 is a fibrous non-union without a carpal collapse and degenerative signs. Type 2 is a non-union without dislocation, a minimal pathological mobility and carpal collapse. Type 3 is a fracture non-union with moderate dislocation, pathological mobility, resorptive changes, a DISI deformity, a clinical restricted wrist movement and radiological sign of arthritis. Type 4 is a fracture non-union with dislocation of the fragments, advanced resorptive changes and radiocarpal arthritis, carpal collapse and a clinically restricted wrist movement. Type 5 is a fracture non-union with an additional avascular necrosis of the proximal fragment [12].
Data analysis
Statistical analysis was performed with the Wilcoxon test for nonparametric data, one-way ANOVA with post hoc Bonferroni test at a significance level of p ≤ 0.05.
Results
Statistical analysis of the mean preoperative range of motion revealed a significant reduction of dorsiflexion (injured wrist, 51 ± 14°; contralateral wrist, 63 ± 12°; p < 0.001), palmar flexion (injured wrist, 54 ± 15°; contralateral wrist, 67 ± 14°; p < 0.001), radial deviation (injured wrist, 18 ± 8°; contralateral wrist, 22 ± 6°; p = 0.003), and ulnar deviation (injured wrist, 28 ± 9°; contralateral wrist, 33 ± 9°; p = 0.01) at the injured side. No significant differences were seen for the pronation (injured wrist, 87 ± 7°; contralateral wrist, 88 ± 5°, p = 0.18) and supination (injured wrist, 85 ± 11°; contralateral wrist, 88 ± 5°, p = 0.06). Main results of the radiological and histological analysis are summarized in Tables 1 and 2, respectively. No statistical correlation was found between the blinded radiological results and the age of the SNU (Fig. 1).
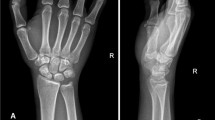
Standard radiographs (a, c) and Böhler series (b, d) of a 4-month-old delayed fracture healing of the scaphoid (a, b same patient as in Figs. 3a, b and 4) and a 25-month-old scaphoid non-union (c, d same patient as in Figs. 2 and 5 b). The big resorption cyst is clearly visible 4 months after scaphoid fracture (a, b). Neither DISI deformity nor SNAC involvement are visible in both cases. No radiological differences between both patients indicate the difference of the age of the fractures
The anatomical structures were clearly discernible in most of the specimens (Fig. 2). There were only a few cases where several criteria could not be assessed (Table 2). The main finding in all cases of SNU was the presence of fibrous tissue or fibrocartilage in the fracture gap (Fig. 3). Coverage of the fibrous tissue with synovium-like cellular lining indicated mechanical instability in 13 cases (34%) (Fig. 4). Such changes were markedly seen between 4 and 36 months. Definitive sclerotic bone covering of the fracture edges according the criteria of stage III of the Trojan and Jahna score was detected in 15 cases (39%). These changes had already appeared after 6 months and did not change with increasing fracture age (mean 37 ± 38 months) but showed a significant difference to non-unions without sclerotic bone covering (4–60 months; mean 15 ± 13 months; p = 0.035). Resorptive bone cysts with osteoclastic giant cells were seen in 13 cases (31%) between 4 and 73 months after scaphoid fracture (Fig. 5). Frequently, cystic bone lesions filled with fibrous tissue or fibrocartilage were seen, which had the same appearance as subchondral bone cysts. Fibrous or fibrocartilage bone cysts were seen in 28 cases (74%) with a mean fracture age of 17 ± 14 months, whereas they were not found in 7 cases (17%) with a mean age of 45 ± 48 months (p = 0.04). Bone remodelling as judged by a high turnover of activated osteoblasts and osteoclasts was seen in 29 cases (76%) with a mean age of 18 ± 16 months, whereas it was not detected in 8 cases (19%) with a mean fracture age of 45 ± 48 months (p = 0.031).
Histological section of a 25-month-old scaphoid non-union (H&E staining) (same patient as in Figs. 1c, d and 5 b). This proximal fragment of the scaphoid is surrounded by hyaline joint cartilage and has a fibrous cystic lesion (asterisk). The cyst lies opposite to the fracture gap (arrows) and is covered by sclerotic bone. (original magnification)
Four-month-old delayed scaphoid fracture healing (a, b same patient as in Figs. 1a, b, and 4) and a 22-month-old scaphoid non-union (c, d) (H&E staining) seen in the transmission mode (a, c) and the polarized mode (b, d). It shows fibrocartilage (asterisk) in the non-union gap as well as adjacent sclerotic bone covering (plus). Original magnification ×40
Histological section of a delayed fracture healing after 4 months (a) and a 25-month-old scaphoid non-union (b same patient as in Figs. 1c, d and 2) with a cyst lined with fibrous and fibrocartilaginous tissue (H&E staining). Figure a shows a typical resorptive bone cyst with necrotic bone fragments (asterisk) within fibrous tissue and the existence of numerous osteoclastic giant cells (arrows). This cyst is surrounded by sclerotic bone. Original magnification ×40
Evident osteosclerosis and osteonecrosis were seen in several cases (Table 2). These features were independent of the age of the scaphoid fracture. Severe degenerative and reparative changes of the local joint cartilage indicative of posttraumatic arthritis were found in 23 cases (61%).
Discussion
Demographic variables
Scaphoid fractures are most common in young, active men aged 15–29 years [13–15]. Scaphoid fractures more often occur in men than in women, which is in accordance to our data. The percentage of male patients ranges between 81 and 97% in the literature [14–17]. In the present series, 13 patients (34%) were younger than 20 years old, 13 patients (34%) were between 20 and 29 years old, 6 patients (16%) were between 30 and 39 years old, 3 patients (7%) were between 40 and 49 years old and 3 patients (7%) were between 50 and 59 years old. Sports injuries and severe physical work are the leading mechanisms of injury, which could explain the age and gender distribution of the affected patients.
Range of motion
SNU has been shown to cause loss of range of wrist motion [18, 19]. This observation could be confirmed significantly in the present study. Prolonged cast immobilization in nonsurgical treatment and altered joint mechanics are potential reasons for the restricted range of motion of the injured wrist.
Radiographic and histological signs
The bony interruption of the proximal carpal row causes flexion of the distal scaphoidal fragment, whereas the proximal fragment is extended dorsally by the pull of the strong scapholunate ligament. This pathological mechanism results in an impingement of the distal scaphoid fragment with the styloid process of the radius, causing posttraumatic arthritis of the styloid process of the radius [20]. Development of posttraumatic arthritis in the radioscaphoid joint is described 5–10 years after injury and increases with time [18, 19]. In another study, posttraumatic arthritis of the styloid process of the radius was seen with mean age for the scaphoid non-union of 17 years [21]; this contrasts with our results. We have seen posttraumatic arthritis of the styloid process of the radius between 6 and 85 months (18%; mean 29 ± 31 months) after scaphoid fracture and a mean age of the patients of 32 ± 12 years old (range 21–52 years) in the unblinded radiological analysis. After additional 5–10 years, arthritis in the mediocarpal joints can be observed [18]. We did not see any mediocarpal arthritis in our cohort, but we had only one case older than 120 months and three cases between 60 and 85 months. Vender et al. studied 64 patients with symptomatic SNU and found, at 4 years, that 75% had developed radioscaphoid arthritis and, at 9 years, that 60% had extended to the midcarpal joint [22]. Mack et al. studied the natural history of 47 symptomatic SNU with follow-up time ranging from 5 to 53 years. They described the radiographic pattern of cyst formation and resorption of scaphoid at an average of 8 years [21]. Again these results differ from our histological data, since we have observed fibrous or fibrocartilage bone cysts in earlier stages of the scaphoid non-unions (Table 2).
The precarious blood supply and the high mobility of the scaphoid increase the risk of non-union, which leads to the hypothesis that it also depends on the time from scaphoid fracture until diagnosis and the primary treatment [23]. We have not found a correlation between the age of the fracture and the development of an osteonecrosis, with a mean fracture age of 18 ± 15 months in comparison to 25 ± 31 months in non-osteonecrosis patients (Table 2). Inoue and Sakuma [19] reported an increased incidence of avascular necrosis of the proximal fragment with time, especially after 20 years. Therefore, it seems that the location or course of the fracture plays a more important role for the early development of an avascular necrosis of the scaphoid.
The classification of Herbert and Fisher defines type D1 as fibrous non-union and type D2 as sclerotic non-union, but no criteria exist for the cystic non-unions. We have found that fibrous or fibrocartilage bone cysts have appeared significantly earlier in SNU with a mean fracture age of 17 months (Table 2). In addition, we have seen significant differences of the unblinded radiological analysis in comparison to the histological analysis of the classification of Herbert and Fisher (p = 0.001; Table 1). This indicates that SNU cannot be subtly classified even when knowing the age of fracture according to Herbert and Fisher.
The primary parameter of the classification of Filan and Herbert [12] is the carpal collapse and the secondary parameter is the clinical rating in our experience. We found some cases with disparate radiological and clinical signs. Resorptive changes do not always coexist with radiocarpal arthritis. In addition, the reduction of range of motion of the wrist did not correlate with the amount of resorptive changes and the severity of radiocarpal arthritis in few cases (n = 16; 38%). One explanation for that could be the different ages of the patients. The classification of the SNAC wrist is a classification for advanced scaphoid non-unions, whereas most of the SNU are detected earlier clinically. In our study we did not find any case with a stage II or III of the classification of the SNAC wrist, even in 4 cases (11%) with an age of fracture of more than 60 months. By contrast, other studies have shown 92% of SNU with an age of 5–9 years having a SNAC stage II or III [24].
The classification of Gupta does not have a single leading symptom. Furthermore, it divides SNU with vacuolation as a sign of resorptive changes in group I and scaphoid non-unions with a cortical offset > 1 mm as a sign of dislocation in group III [10]. The blinded radiological analysis has revealed a mean fracture age of 10 ± 6 months with a range of 6–14 months for group I and a mean fracture age of 14 ± 9 months with a range of 5–28 months for group IIIA. In the present study, we found that the vacuolation does not exist earlier than the cortical offset. Therefore, the group numbers do not appear to follow the clinical sequence and mix different types of staging parameters.
Histological differentiation between stages C and D1 of the Herbert and Fisher classification [4] is impossible. These are differentiated only by the time from the injury. Possible explanations of these findings could be that histological changes like small amounts of unmineralized newly formed bone precede radiological changes. One limitation of that study is that the time of injury was stated by the patients. Therefore, the time of injury is a subjective parameter which relies on accurate reporting by the patient and cannot be verified.
The present study failed to demonstrate any correlation between clinical, radiological and most of the histological results of the fracture. One reason might be the multifactorial aetiology of the observed histological features like resorptive changes and arthritis changes, because reinjury or aseptic osteonecrosis may reproduce these changes at different times. It seems that in earlier stages, up to one and a half year from the injury, the cellular repair of the fibrous tissue and the bone remodelling are higher than in established fracture non-union. A definitive decrease of bone remodelling was seen at a mean age of 45 months after fracture. Sclerotic fragment edges appear with a mean fracture edge of 36 months. Fibrous or fibrocartilage bone cysts of older SNU are possibly not detected as a cause of severe sclerosis. Further immunohistochemical investigations of the cellular repair and bone remodelling at the fracture site as well as investigations with magnetic resonance imaging (MRI) are necessary to understand the mechanism of the non-union and to identify possible time-dependent changes of bone remodelling as well as the blood supply of the fractured scaphoid. At the moment no classification for scaphoid allows a clear distinction of SNU by clinical, radiological and histological parameters with conventional staining.
References
Dunn AW (1972) Fractures and dislocations of the carpus. Surg Clin North Am 52(6):1513–1538
Chen AC, Chao EK, Hung SS, Lee MS, Ueng SW (2005) Percutaneous screw fixation for unstable scaphoid fractures. J Trauma 59(1):184–187
Gelberman RH, Menon J (1980) The vascularity of the scaphoid bone. J Hand Surg Am 5(5):508–513
Herbert TJ, Fisher WE (1984) Management of the fractured scaphoid using a new bone screw. J Bone Jt Surg Br 66(1):114–123
Perlik PC, Guilford WB (1991) Magnetic resonance imaging to assess vascularity of scaphoid nonunions. J Hand Surg Am 16(3):479–484
Gaisne E, Dap F, Bour C, Merle M (1991) Arthrodeses du poignet chez le travailleur manuel. A propos de 36 cas. Rev Chir Orthop Reparatrice Appar Mot 77:537–544
Krimmer H, Sauerbier M, Vispo-Seara JL, Schindler G, Lanz U (1992) Fortgeschrittener karpaler Kollaps (Slac-wrist) bei Skaphoidpseudarthrose. Therapiekonzept: mediokarpale Teilarthrodese. Handchir Mikrochir Plast Chir 24:191–198
Trojan E, Jahna H (1955) Die konservative Behandlung des veralteten Kahnbeinbruches der Hand. Arch Orthop Unfallchir 47(1):99–104
Watson HK, Ryu J (1986) Evolution of arthritis of the wrist. Clin Orthop Relat Res 202:57–67
Gupta A, Risitano G, Crawford RJ, Burke FD (1999) The ununited scaphoid: prognostic factors in delayed and nonunions of the scaphoid. Hand Surg 4(1):11–19
Athanasou NA (2001) Pathological basis of orthopaedic and rheumatic disease. clinical, radiological, and pathological correlation of diseases of bone, joint, and soft tissue. 2. Injury and repair of skeletal tissues. Hodder Arnold, London, pp 21–25
Filan SL, Herbert TJ (1996) Herbert screw fixation of scaphoid fractures. J Bone Jt Surg Br 78(4):519–529
Leslie IJ, Dickson RA (1981) The fractured carpal scaphoid. Natural history and factors influencing outcome. J Bone Jt Surg Br 63(B-2):225–230
Larsen CF, Brondum V, Skov O (1992) Epidemiology of scaphoid fractures in Odense, Denmark. Acta Orthop Scand 63(2):216–218
Düppe H, Johnell O, Lundborg G, Karlsson M, Redlund-Johnell I (1994) Long-term results of fracture of the scaphoid. A follow-up study of more than thirty years. J Bone Jt Surg Am 76(2):249–252
Böhler J, Ender HG (1986) Die Pseudarthrose des Scaphoids. Orthopäde 15(2):109–120
Eitenmüller J, Haas HG, Koob E (1978) Behandlungsergebnisse bei Kahnbeinfrakturen und—pseudarthrosen. Handchirurgie 10(1):9–11
Martini AK (1994) Der Spontanverlauf der Kahnbeinpseudarthrose. Orthopäde 23(3):249–254
Inoue G, Sakuma M (1996) The natural history of scaphoid non-union. Radiographical and clinical analysis in 102 cases. Arch Orthop Trauma Surg 115(1):1–4
Krimmer H, Krapohl B, Sauerbier M, Hahn P (1997) Der posttraumatische karpale Kollaps (SLAC- und SNAC-wrist)-Stadieneinteilung und therapeutische Möglichkeiten. Handchir Mikrochir Plast Chir 29(5):228–233
Mack GR, Bosse MJ, Gelberman RH, Yu E (1984) The natural history of scaphoid non-union. J Bone Jt Surg Am 66(4):504–509
Vender MI, Watson HK, Wiener BD, Black DM (1987) Degenerative change in symptomatic scaphoid nonunion. J Hand Surg Am 12(4):514–519
Beutel FK, Wilhelm K (1999) Abhängigkeit der Nekrose von Verlauf und Lokalisation der Fraktur bei Skaphoidpseudarthrose. Handchir Mikrochir Plast Chir 31(3):207–211
Ruby LK, Stinson J, Belsky MR (1985) The natural history of scaphoid non-union. A review of fifty-five cases. J Bone Jt Surg Am 67(3):428–432
Acknowledgments
The authors wish to thank Ursula Range for her advice with the statistical analysis; Doreen Küchler and Suzanne Manthey for histological preparation; Thomas Albrecht for preparation of the photographs as well as Alexandre Serra for translation support.
Conflict of interest statement
No benefits in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rein, S., Hanisch, U., Rammelt, S. et al. Histopathological, radiological and clinical aspects of the temporal assignment of scaphoid non-union. Arch Orthop Trauma Surg 130, 1243–1250 (2010). https://doi.org/10.1007/s00402-009-1010-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-009-1010-x