Abstract
Circumventricular organs (CVOs) are specialized brain structures located around the third and fourth ventricles. They differ from the rest of the brain parenchyma in that they are highly vascularised areas that lack a blood–brain barrier. These neurohaemal organs are classified as “sensory”, when they contain neurons that can receive chemical inputs from the bloodstream. This review focuses on the sensory CVOs to describe their unique structure, and their functional roles in the maintenance of body fluid homeostasis and cardiovascular regulation, and in the generation of central acute immune and febrile responses. In doing so, the main neural connections to visceral regulatory centres such as the hypothalamus, the medulla oblongata and the endocrine hypothalamic-pituitary axis, as well as some of the relevant chemical substances involved, are described. The CVOs are vulnerable to circulating pathogens and can be portals for their entry in the brain. This review highlights recent investigations that show that the CVOs and related structures are involved in pathological conditions such as sepsis, stress, trypanosomiasis, autoimmune encephalitis, systemic amyloidosis and prion infections, while detailed information on their role in other neurodegenerative diseases such as Alzheimer’s disease or multiple sclerosis is lacking. It is concluded that studies of the CVOs and related structures may help in the early diagnosis and treatment of such disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Sensory CVOs: cross-talkers between blood, cerebrospinal fluid and brain
It is barely a century since experiments demonstrated for the first time that there was some kind of compartmentalization between the central nervous system (CNS) and the bloodstream, the so-called blood–brain barrier (BBB). Ehrlich [38] and Goldmann [54] became the first to demonstrate that the CNS was the only organ which is not stained by dyes injected intravenously, and that it is stained only after intracerebral injection. The BBB is formed by capillary endothelial cells joined together by tight junctions, their basal membrane, and surrounding pericytes, astrocytic end-feet, and microglial and neuronal processes [1, 102]. This barrier effectively segregates the CNS from the periphery, ensuring that neurotransmitters, neuromodulators, neuropeptides and growth factors do not diffuse out of the CNS into the circulation, and that blood-borne endocrine hormones, pathogens and cytokines, amongst others, are prevented from entering the CNS [102].
Despite this barrier, CNS regulatory centres are able to respond to changes in the level or concentration of circulating molecules, solutes or toxic substances in order to maintain the “milieu intérieur” (homeostasis). Early experiments by Wislocki et al. [155] and by Behnsen [13] demonstrated that minute structures in the CNS were stained with intravenously administered dyes indicating that they lacked a BBB [154]. In 1958, it was found that those neurohaemal structures were located around the ventricles, and were accordingly named circumventricular organs (CVOs; [65]). The CVOs can be traced by intravenous injection with horseradish peroxidase [16] or examined in vivo by fluorescence endoscopy [79]. Later on, CVOs were called the “windows of the brain” [59] because of their distinct neurohaemal morphological features, such as their capillaries being fenestrated and glial cells being more loosely apposed, creating relatively large perivascular spaces. In consequence, large molecules and polar substances can readily pass to and from the blood to the perivascular spaces exposing neurons to peripheral signals [39].
According to recent opinions, there are eight CVOs: three sensory, four secretory and one that is unclassified [25]. The sensory CVOs include the subfornical organ (SFO), the organum vasculosum of the lamina terminalis (OVLT) and the area postrema (AP). The secretory CVOs are the neurohypophysis, the median eminence, the pineal gland and the subcommisural organ. The choroid plexus is occasionally considered as a CVO because of its fenestrated capillaries but it lacks any neural tissue, while the subcommisural organ is often disregarded as a CVO because it does not have fenestrated capillaries [108].
Circumventricular organs (CVOs) have been regarded as likely points of communication between the blood, the cerebrospinal fluid (CSF) and the brain parenchyma [69, 92]. Eight classes of interactions between these three compartments have been proposed considering both signal source and target, and mode of information transfer (hormonal, neural or humoral [69]). Sensory CVOs mainly act as class II and class III CVOs [69]. By definition, class II CVOs contain both neuronal soma and terminals [57] to sample molecules from blood and interstitial fluid. Subsequently, these neurons will transfer information via neural connections (Class III) to distant brain structures that have a BBB.
Functionally, the CVOs help in maintaining homeostasis through regulation of movement of solutes and chemicals from the circulatory system into the brain parenchyma and vice versa, and respond immunologically to inflammatory cells or to infectious agents that circulate in the bloodstream. The sensory CVO neurons in turn innervate major neural effector centres for most autonomic functions, for maintaining body fluid homeostasis, and for initiating immune responses.
The present review focuses on the sensory CVOs with the main aims of (i) describing their unique characteristics as neurohaemal organs, (ii) showing that—as a dynamic system—they are capable of responding to peripheral and local changes and requirements, (iii) describing their ability to regulate a number of mechanisms in physiological and pathological conditions, (iv) pointing out their possible roles as portals of entry and distributors of some infectious agents that can affect animals and humans, and (v) formulating the hypothesis that disruption of these organs might be critical in the initiation, development and progression of some neurological diseases.
Vascular architecture and neuroanatomy
Although with some slight differences depending on the species (reviewed in [91]), the mammalian sensory CVOs receive blood supply through branches of the anterior cerebral (OVLT and SFO) and of the cerebellar (AP) arteries. These arteries branch into extensive networks of primary capillary plexuses arising from intrapial vessels, which can be twisted and looped as secondary capillaries when entering subependymal regions [35, 36]. Those capillary plexuses drain into veins usually located within the CVOs themselves and occasionally in the brain parenchyma, like in the case of the OVLT that drains into the preoptic region [20]. A recent atlas highlights some of the differences in the vascular architecture within the CVOs between humans and non-human species [37].
Capillaries within the CVOs differ in type according to the continuity of the endothelial sheath, the number of intracellular vesicles, the lumen diameter, the endothelial wall thickness and the size of the peri-capillary space [58, 124–126]. Dellmann [31] described three different types of capillaries that can be found in the CVOs. Type I capillaries have a continuous, non-fenestrated endothelium but differ from the typical CNS capillaries in that they have relatively larger perivascular spaces and abundant vesicles within the endothelial cells. Type II capillaries possess the same characteristics as those of the rest of the CNS, while type III capillaries differ fundamentally from those of the brain parenchyma. Type III is the most permeable capillary type as, in addition to the endothelial fenestrations, their endothelial cells have many intracellular vesicles and pits, their walls are thin, their luminal diameter is large, and their perivascular spaces are dilated containing neuroglia elements [31]. In addition, basement membranes surrounding the perivascular sheaths contain neurons, axon terminals, collagenous fibrils, macrophages and fibroblasts, but not astrocytes.
In coronal sections, the lamina terminalis, historically called supraoptic crest, forms a sagittal fold above the optic chiasm as part of the supraoptic recess of the third ventricle [37]. Two of the sensory CVOs are part of this structure: the OVLT and the SFO (Fig. 1).
Neuroanatomical location of the SFO and the OVLT in the sheep brain. a Sagittal section of the diencephalon indicating the locations of the CVOs (arrows) associated with the lamina terminalis (LT) and the three levels of trimming (1, 2 and 3) for their optimal visualisation. b Transversal sections obtained from Sections 1, 2 and 3. Section 1 shows the most anterior part of the OVLT (arrow) ventral to the anterior white commissure (AWC) and dorsal to the optic recess (OR). Note that the third ventricle (III) is not represented in this section. Section 2 shows the most anterior part of the SFO (arrow) between the columns of the fornix (FC) and dorsal to the AWC. Note that the ventral opening of the III is represented in this section. Section 3 shows the posterior part of the SFO (arrow) at the dorsal opening of the III. c The OVLT grossly has a gelatinous appearance and it is found dorsomedial to the optic chiasm (OC). d Grossly, the SFO is translucent in appearance and highly vascularised. In sheep, the SFO is quite prominent and protrudes towards the communication between the III and the lateral ventricles (LV). Bar 0.2 mm. CC corpus callosum, CP choroids plexus, PG pineal gland, T thalamus, OC optic chiasm, MB mammillary body
The OVLT, which is the vascular organ of the lamina terminalis, is a thin structure fixed in the anterioventral border of the optic chiasm that forms the anterior wall of the third ventricle. The vascular architecture of the OVLT is similar to that of the median eminence in the sense that it is formed by two primary capillary networks (a superficial intrapial plexus and a deeper outer plexus) and a secondary capillary plexus [124]. The intrapial plexus connects with the subarachnoidal space at the prechiasmatic cistern, whereas the secondary capillary plexus is limited to a subependymal network of looping capillaries that connects with the third ventricle (Fig. 2a). In humans, such a capillary network forms a ring with the loops oriented towards the centre of the ring [37]. Only the deep plexus has fenestrated capillaries [76] except in the rat, in which endothelial tight junctions are found in all capillaries of the OVLT [108]. Processes of meningeal cells and tanycytes separate the periventricular compartment, which contains the fenestrated secondary vascular plexus and subependymal capillary loops, from the superficial intrapial compartment. These processes may form a perivascular double basal membrane [122].
Drawings of the vasculature, anatomical subdivisions and main efferent connections of the sensory CVOs in a lateral view (a, c, e) and a transversal front view (b, d, f). a The vascular architecture of the OVLT contains rostrally two capillary networks originating from the anterior communicating artery (ACA) and the preoptic artery branches (PO): the superficial intrapial primary plexus (yellow background) and the deep outer primary capillary plexus with capillary loops (orange background). The anterior limit of the OVLT is separated by meninges (thick black line) at its proximity with the prechiasmatic cistern. The deep outer capillary plexus which is continuous with the secondary capillary plexus has fenestrated capillaries. The secondary capillary plexus is located in the periventricular area in contact with the ependyma of the 3rd ventricle (III). The posterior thick wall represents the specialized ependyma of this CVO. Blood drains into branches of the PO vein. b The three main subdivisions of the OVLT are shown in different colours. The anterior vascular inner region is surrounded dorsally by the dorsal cap and by the lateroposterior zone both of which maintain connections mainly with hypothalamic nuclei. c The ventromedial core of the SFO has the most dense fenestrated vascular architecture and contains the specialized ependyma (thick wall). They arise from branches of the preoptic artery and drain into vein branches. d Most efferent hypothalamic connections leave from the outer shell, as shown in the posterior transversal view. e The vasculature of the AP arises from the cerebellar artery (red) and branches into tortuous capillary networks in the periventricular zone, which is in contact with the fourth ventricle (IV). Blood is drained into vein branches (blue) that run ventrally along the ventral zone. f Most efferent connections are originated in intermedio-ventral areas of the AP and terminate in adrenergic cell centres. The ventral junctional zone is in contact with the solitary tract nucleus (STN). Note that afferent nerve input from the vagus and glossopharyngeal nerves terminate in the periventricular medial zone. SON supraoptic nucleus, PVNm magnocellular part of the paraventricular nucleus, PVNp parvacellular part of the paraventricular nucleus, BNST bed nucleus of the stria terminalis, Lat HT lateral hypothalamic nucleus, OR optic recess, OC optic chiasm, PBN parabrachial nuclei, MnPO median preoptic area, LV-III intersection between lateral and III ventricles, NA nucleus ambiguous, VLM ventrolateral medulla
The SFO, previously named ganglion psalterii [134] or intercolumnar tubercle [114], is on the midline rostral wall of the third ventricle in the dorsal region of the lamina terminalis, ventral to the origins of the columns of the fornix and dorsal to the anterior white commissure ([32]; Fig. 1). In humans, it protrudes slightly into the intersection point between the lateral and the third ventricles at the confluence of the foramen of Monro [3, 37, 114]. The most superficial capillaries are seen on an endo-ventricular view [37]. The posterioventral surface of the SFO is in contact with the pial connective tissue of the choroid plexus through a continuous layer of glial processes ([58]; Fig. 2c). In the rat SFO, there is an outer dorsal shell and an inner ventromedial core (Fig. 2c); it is the inner core that contains the dense networks of type III capillaries [31, 126].
The AP is attached to the ventral angle of the floor of the fourth ventricle at its opening to the central canal at the level of the obex. It consists of two lateral masses in humans and most mammals, but a single median mass in rodents and lagomorphs. The dorsolateral part of the AP is attached to the tela choroidea, and in humans is connected with the subarachnoidal medullo-cerebellar cistern. The gross morphology of the AP is different from the adjacent vagal complex nuclei in that it is a highly vascularised structure (Fig. 3a) composed of large and sinusoidal capillaries [97]. Similar to the OVLT, a layer of tanycytes representing the funiculus separans provides a barrier with adjacent structures that contain a BBB, like the solitary tract nucleus (STN [76]). It is uniformly composed of a network of numerous subependymal loops of anastomosed large-calibre type III capillaries. Electron microscopy studies in the 20th century revealed double subendothelial basement membranes between which electron dense particles were trapped [33, 146].
Macro- and microscopical appearance of the ovine AP. The distribution of the rich vasculature is more homogenous throughout this CVO (a). The AP contains high numbers of neuronal somas, as denoted by positive immunolabelling with neuronal nuclei (NeuN) antibodies in the central zone (b). It is very well interconnected with the vagal complex, as shown by strong synaptophysin immunolabelling (c), in comparison to neighbouring structures like the solitary tract nucleus (STN) and the dorsal motor nucleus of the vagus nerve (DMNV). STT solitary tract, XII hypoglossal nucleus. Distinctly from vagal complex structures, the AP shows strong immunoreactivity against paravalbumin (d). Immunolabelling for microglial cells/macrophages with coronin-1 shows differences in numbers of positive microglia resident cells between the AP of a healthy sheep (e) and activated mononuclear cells in a case of a non-purulent encephalitis in sheep (f). b, e: ×10; c, d: ×2; f: ×20
As mentioned earlier, the vascular architecture of the OVLT is similar to that of the median eminence but different from that of the SFO and AP. Recent investigations showed that the fenestrated capillaries of the SFO and AP, but not those of the OVLT, can express type 1 aquaporin water channels [153]. Gross [58] observed that the plasma flow and blood-to-tissue transfer was increased in the capillaries of the SFO and AP compared to adjacent brain structures, and that the blood flow within those CVO capillaries was slower than in those of the rest of the brain. They concluded that this would allow plasma to gain better access to the receptors of those sensory CVOs.
The SFO and AP are located in close proximity to ventricular junctions, and the OVLT to ventricular recesses. At those sites, the ependymal lining contains specialized ependymocytes and tanycytes. Ependymocytes are linked by tight junctions that establish a barrier between the CSF and the brain [37, 91]. In contrast, tanycytes have multiple processes (microvilli or cilia) that contact with the CSF and extend into the body of the CVOs [57]. By linking the CSF and CVO environments, tanycytes could provide a functional role for the CVOs to monitor the composition of the CSF [37, 98]. Goren et al. [56] defined the CVOs as “hypendymal organs” because they possess glial and vascular plexuses, no BBB, and high aquaporin-4 expression. In contrast, the so-called “ependymal organs” of the brain do have a BBB and a thickened and pseudostratified ependyma immuno-negative for aquaporin-4 [56].
Roles of the sensory CVOs in health: regulators of endocrine and integrated autonomic functions through the CNS
Most anatomical studies describing the projections to and from the CVOs have been conducted in rats and using tracing methods further validated by electrophysiological techniques [42]. The OVLT, SFO and AP are integrated in CNS circuits which connect them mainly with the autonomic regulatory centres of the CNS, the hypothalamus and the dorsal vagal complex [25].
Many different anatomical subdivisions have been proposed for the sensory CVOs (as reviewed by McKinley et al. [91] and Dellmann [31]). Drawings in Fig. 2 reproduce those subdivisions as given by McKinley et al. [91] from a functional point of view, but also depict the main neural connections as proposed by several authors [25, 69, 91].
Neural architecture of the sensory CVOs
Three main functional subdivisions of the rat OVLT are proposed: an arching dorsal cap, a ventrorostral inner vascular region, and two ventrolateral areas that converge in the posterior aspect of the organ in close apposition to the ependyma of the third ventricle (Fig. 2b). In humans, the rostral part of the vascular region is devoid of neuronal perikarya and is composed largely of astrocytic processes, basement membranes and perivascular spaces of the intrapial primary plexus. The dorsal cap provides the major source of efferent connections to the supraoptic nucleus [89, 99, 109, 136], to magnocellular neurons of the paraventricular nucleus [60, 136, 145] and to the cerebral cortex [91]. Neural projections leave the lateral-periventricular subdivision to connect with the lateral hypothalamic area, the bed nucleus of the stria terminalis and the parvocellular neurons of the paraventricular nucleus [136, 145]. Terminal fields of those projections are found in limbic structures such as the septal area, hippocampus and cingulate cortex [18], in midbrain areas such as the periaqueductal grey matter, lateral parabrachial nucleus and locus coeruleus [18, 60], and in the medullary raphe nucleus [145]. Moreover, experimental data using viral tracers have revealed polysynaptic efferent pathways originating in the dorsal cap and lateral areas of the OVLT connecting with neurons of the hypothalamic paraventricular nuclei and ending in peripheral organs such as the kidney (for details see [91]). Neurons in the OVLT also send and receive projections from the two other components of the lamina terminalis, the SFO and the median preoptic nucleus in rats [18, 60, 100] and in sheep [101], and may receive neural input from the nucleus of the solitary tract [25]. Minor connections with other hypothalamic nuclei (ventromedial, arcuate, medial preoptic, anterior and posterior nuclei) have also been described [18].
In the rat SFO, there is an outer dorsal shell and an inner ventromedial core (Fig. 2c, d). According to morphological studies, both subdivisions contain numerous neurons, but it is the inner core that contains the largest number of neuronal somas and afferent nerve terminals [31]. The outer shell is the origin of almost all efferent fibre projections towards hypothalamic nuclei ([142]; Fig. 2d). The median preoptic area is one of the major efferent targets of the SFO in rats [84, 94] and sheep [90, 91, 101]. Fibres leaving the SFO travel mainly through its ventral stalk into the adjacent median preoptic area or into the columns of the fornix to project directly or indirectly towards the OVLT, paraventricular and supraoptic nuclei [84, 91, 95, 141], suprachiasmatic nuclei [91, 100] and ventrolateral medulla [74]. Neurons of the outer shell project to the infra-limbic part of the pre-frontal cortex, to the substantia innominata (ventral pallidum), to parts of the zona incerta, and to the lateral hypothalamus [94, 96, 140], whereas those of the ventromedial core project to the bed nucleus of the stria terminalis [140] with efferent terminal fields found in the midbrain raphe [83]. Similar to the OVLT, STN projects laterally to the SFO. The outer shell of the SFO has polysynaptic pathways to sympathetic and parasympathetic nerves that supply peripheral organs and tissues such as the kidney, adrenal gland, heart and gut [91].
Gross [58] proposed that the AP was divided into three main divisions: a dorsal periventricular mantle zone, a half-moon shaped central zone, and a ventrolateral zone containing the ventral junctional zone adjacent to the STN (Fig. 2f). The AP forms the vagal complex together with the STN and the dorsal motor nucleus of the vagus nerve (DMNV; Fig. 3c, d). Fewer neurons, but many glial cells are found in the ventral zone of the AP next to its boundaries with the STN ([106]; Fig 3b, e). Efferent pathways from the central and lateral zones project first to the adjacent solitary tract, and ventrolaterally to the A1 noradrenergic group, and to the nucleus ambiguous (Fig. 2f), where some monosynaptic axons terminate [123]. Alternatively, they relay on the lateral parabrachial nucleus to further terminate in the ventrolateral aspect of the periaqueductal grey matter and in the mesencephalic nucleus of the trigeminal nerve [123], the dorsal tegmental nucleus [148], and unspecified parts of the cerebellar vermis [123]. A similar polysynaptic pathway from the AP to the suprachiasmatic nucleus has been identified [78]. In the rat, according to Cunningham et al. [27], the DMNV receives few if any fibres from the AP. Most afferent projections terminating in the AP originate in the parvocellular group of neurons of the paraventricular nucleus and in neurons of the dorsomedial nucleus of the hypothalamus and perifornical region [123], STN and the lateral parabrachial nucleus. Unlike those CVOs related to the lamina terminalis, the AP receives direct innervation from visceral nerves through sensory components of the vagus and glossopharyngeal nerves, which terminate in the dorsal periventricular mantle ([71, 91]; Fig. 2f), conveying information from the abdomen and thorax [21, 23, 24, 71, 72, 111], and from the kidney [132].
CVOs as neurochemical sensors and transducers
Autoradiographic binding studies, in situ hybridisation and immunohistochemistry have revealed that sensory CVO neurons or fibres contain hormones, neurotransmitters, neuropeptides and enzymes. These neurons act as neurochemical sensors for blood-borne stimuli, through synaptic input (through axonal terminals) or by coupling to receptors.
When extracellular ligands such as hormones or neurotransmitters, which act as the “first messenger”, bind to different receptors, usually transmembrane proteins [91, 111], they in turn activate intracellular protein effector responses named “second messenger”. These second messengers act as transducers leading to increased levels of intracellular calcium. Subsequently, gene expression of transcriptional factors is increased. Table 1 provides a partial overview of some receptors that are discretely localized in the CVOs, as reported by McKinley et al. [91].
Large numbers of investigations on early gene expression have provided the main bulk of knowledge on the functional roles of the sensory CVOs. These studies are based on the examination of the distribution of activated neurons by means of the expression of the gene transcription factor c-Fos in response to blood-borne stimuli. Some examples found in the literature include, (i) increased c-Fos expression in the OVLT and SFO after infusion of hypertonic solutions, after induction of sodium depletion or dehydration, or as a result of increased levels of circulating angiotensin II, suggesting that these CVOs can be responsible for maintaining the water and electrolyte balance, (ii) increased c-Fos expression in the AP after elevated arterial pressure and after infusion of anorectic peptides or emetic stimulation, implying that this CVO influences somewhat the cardiovascular function and appetite, and (iii) increased c-Fos expression in the CVOs after parenteral injections with bacterial endotoxin lipopolysaccharides (LPS) or after interleukin-1 (IL-1) administration, suggesting that CVOs might be responsible for fever and immune responses.
Gross [57] proposed some CVO functions in the maintenance of body fluid balance, blood pressure, temperature, respiration, energy balance, mediation of immune responses, pain modulation, protection against ingested toxic substances, biological rhythms, reproduction, parental behaviour, lactation, growth, sleep, arousal and attention. Our understanding of the prominent role of the CVOs has advanced in these past two decades and extensive reviews on some of the specific functions of the CVOs are available [25, 34, 47, 49, 63, 69, 91, 135]. Herein, we focus on their direct role in the regulation of body fluid homeostasis and cardiovascular function and in the stimulation of autonomic regulatory centres of the CNS.
Physiological role of CVOs in the maintenance of body fluid homeostasis
Body fluid homeostasis is disturbed in the face of water and/or sodium deficiency or excess. The renin–angiotensin system is classically considered as an endocrine mediator in the regulation of the cardiovascular function, with angiotensin II affecting vascular tone, and stimulating water and sodium reabsorption by the kidney when low water and sodium levels are present in blood. In addition, angiotensin (I and II) can act centrally through initial signalling into sensory CVOs influencing (i) drinking behaviour, (ii) neuroendocrine secretion of adrenocorticotropic, oxytocin and vasopressin hormones, and (iii) autonomic control of the cardiovascular function via sympathetic efferences. Conversely, when water and sodium ion levels are high, the opposite orchestration—the pattern of the behavioural, cardiovascular and renal responses—will take place.
Water deprivation, hyponatremia or blood-borne angiotensin I or II activate osmoreceptors in neurons of the OVLT [67, 115, 151] and SFO [7, 62]. Calretinin- or calbindin-expressing neurons in the OVLT and neurons of the SFO are rich in angiotensin II type 1 receptors and angiotensin-converting enzyme [6, 52, 91, 133]. Their c-Fos expressing neurons will in turn, via previously mentioned connections, stimulate salt and water-intake behaviour [46]. Efferent stimulations towards neurons in the A3V3 region, in the supraoptic nucleus and magnocellular neurons of the paraventricular nucleus, which are known to be the source of vasopressin and oxytocin [43–45, 66, 129], will direct such response by releasing those hormones to the posterior lobe of the pituitary gland. In addition, the SFO transduces the signal to parvocellular neurons of the paraventricular nucleus, with the ensuing release of corticotrophin-related hormones from the anterior pituitary gland. Simultaneously, hypothalamic responses will activate sympathetic outflow regulatory autonomic centres located in the medulla oblongata that react to oxytocin, vasopressin or corticotropin-releasing factor. Subsequently, neurons in the intermediolateral column of the spinal cord and sympathetic ganglia are stimulated [22, 84]. Figure 4 shows the presence of oxytocin in axons and in neurons of the CVOs of the lamina terminalis and the hypothalamic nuclei, respectively.
Oxytocin immunoreactivity in the sheep OVLT and SFO and their main connecting nuclei, the paraventricular and supraoptic. a Strong oxytocin-containing fibres can be observed in the anterior part of the OVLT (encircled), which is mainly composed of astrocytes and basement membranes of the primary capillary plexus. OC optic chiasm. In contrast, its dorsal cap (b) shows low numbers of positive neurites (arrows), similar to its neighbouring median preoptic nucleus (MNPO). c The SFO also shows strong immunoreactivity for oxytocin in the area of the superficial capillary plexus in the outer zone and weaker in the ventromedial core (framed). Note the strong immunolabelling in the perifornical area surrounding the branches of the preoptic artery (POA). The fewer oxytocin-containing fibres of the ventromedial core are better appreciated at higher magnification (d). Both the OVLT and the SFO stimulate the synthesis of oxytocin by the magnocellular neurons of the paraventricular nucleus (PVN; e) and by neurons of the supraoptic nucleus (SON; f). FC fornix columns, PFN perifornical nucleus. a: ×2; b: ×20; c: ×10; d, e: x4
Circulating angiotensin II concurrently stimulates the AP directly, which in turn activates the sympathetic regulatory centres such as the STN, and the ventrolateral medulla in order to increase blood pressure or reset the baroreceptor reflex, respectively [91]. Angiotensin II type 1 receptors are uniformly present in the AP [6], which is the only sensory CVO that contains an A2 noradrenergic subpopulation of catecholamine- or serotonin-containing neurons [91] and the highest numbers of neurons exhibiting GABA neurotransmitters (Fig. 3d). This stimulation produces vasoconstriction, thus regulating arterial pressure and cardiovascular function. This effect is balanced by the baroreceptor reflex that vasopressin, atrial natriuretic peptides and endothelin produce by acting on neurons of the AP [15, 19, 61, 70, 144]. The influence of the OVLT on blood pressure is believed to be mediated by its intimate connections with the preoptic area [64, 86]. In addition, Giles et al. [52] suggested that polysynaptic input generated by neurons in the SFO and in the OVLT might influence the sympathetic supply to the kidney and to the adrenal medulla.
The knowledge of these orchestrating events in health can provide the basis for some therapeutical strategies in disease. Alzheimer’s disease (AD) is characterized by dementia in association with deterioration of the cardiovascular system. Pharmacotherapy targeting the renin–angiotensin system, especially that using angiotensin blockers rather than angiotensin-converting enzyme inhibitors is one of the most effective means of reducing hypertension and cardiovascular morbidity [81]. In the following sections, we will discuss the role of CVOs in disease.
Role of sensory CVOs in inflammatory diseases
In health, CVOs are cross-talkers between the immune, the endocrine and the nervous systems in order to maintain homeostasis. If we consider that inflammation alters homeostasis, then we could anticipate that the CVOs might have a role in inflammatory diseases. In this section, we will describe some known roles of the CVOs such as (i) portals of entry for circulating infectious agents, immunogenic peptides or inflammatory cells, (ii) transduction sites for the activation of the regulatory sites to control the immune response and fever, and (iii) contributors to sickness behaviour.
CVOs are portals for infectious agents to entry into the brain
Most infectious agents can reach the CNS via peripheral nerves or via blood, or by a combination of both as has been recently suggested in animal prion diseases (see section below). Similarly, the immune response to peripheral infections can reach the CNS either through visceral sensory afferent fibres, or via the blood through the CVOs or crossing the BBB [17, 29, 30, 152]. A few investigations have explored the involvement of the CVOs in the neuroinvasion process for some infectious diseases.
Human African trypanosomiasis, also known as sleeping sickness, is caused by extracellular Trypanosoma spp. parasites. This disease is characterized by severe disturbances in regulatory functions of the CNS such as disruption of sleep–wake rhythms, hormonal secretion, or body temperature. Recent evidence suggests that the CVOs act as portals of entry for circulating parasites [121] and elicit the central immune response [77]. This response leads to the production of pro-inflammatory cytokines like interleukin-1β (IL-1β), tumour necrosis factor-α (TNF-α), interferon-γ and inducible nitric oxide synthase [77]. Subsequent spread of the inflammatory process to adjacent limbic brain areas causes pathology and clinical symptoms [77].
The CVOs have also been reported to play a role in the recruitment of inflammatory cells into the brain. In experiments in rats with experimental autoimmune encephalomyelitis (EAE), the animal model for multiple sclerosis, immune cells migrate from the blood into the CNS and CSF overcoming the BBB. Schulz et al. [120] examined the role of the CVOs in this model and found that during clinical stages of EAE, there was an increase of CD45+ leukocytes and an up-regulation of the adhesion molecules ICAM-1 and VCAM-1 in the fenestrated capillaries of the CVOs, with presence of cells positive for MHC class I and class II antigens in the perivascular spaces. They found that these inflammatory changes were more severe in the CVOs than in neighbouring brain areas, suggesting that the CVOs could be the sites of entry of inflammatory cells into the CNS. CVOs from rats with systemic immunological disorders such as systemic lupus erythematosus or systemic amyloidosis showed protein deposits in the fenestrated vessels [107, 128].
CVOs role in stress: transduction sites for fever and activation of the hypothalamic-pituitary axis (HPA)
Stress can be defined as an anticipated threat to well-being and a disruption of homeostasis [143]. Despite the CNS being considered an immunologically privileged site, it is well known now that the brain and the CVOs monitor peripheral innate immune responses [48]. Ageing itself is associated with increased pro-inflammatory activity in the brain. In this section, we will describe the mechanisms by which the CNS interconnects with the periphery in order to balance the pro- and anti-inflammatory response.
There are two main pathways by which the immune system communicates with the brain in order to activate the HPA: a neural pathway and a humoral pathway [17, 29, 30, 152]. Briefly, the neural pathway is characterized by immune stimulation of visceral sensory afferent fibres of the sub-diaphragmatic vagus nerve that relay in the STN [30]. The humoral pathway involves the Toll-like receptors on macrophage-like cells residing in the CVOs and the choroid plexus [30, 152]. The parallelism or convergence of both pathways in target brain areas is unclear at present [29]. For example, is fever the result of pyrogenic cytokines in the hypothalamus being stimulated by prostaglandin E2 (PGE2) production in the CVOs (humoral hypothesis)? Or is the liver production of PGE2 mediated by LPS and complement component C5a which stimulates the hypothalamus via the vagus nerve (neural hypothesis)? [137, 138]. As part of the humoral response, endothelial and microglial cells of the CVOs are activated (Fig. 3e, f) and secrete pro-inflammatory cytokines such as IFN-γ, TNF-α and PGE2 [41, 73, 118, 137, 147]. Such cytokines may pass from the CVOs into the brain by diffusion and activate the febril response indirectly by acting on the preoptic area of the hypothalamus, the area that regulates the body temperature [30, 116, 138, 142]. This acute-phase response with IL-1β and TNF-α results in the development of “sickness” behaviour such as decreased appetite, altered sleep/wake cycles and changes in the neuroendocrine system [17, 28, 30].
The activation of the HPA in stress, which is a multi-step process [17], is the most important neuroendocrine disturbance associated with inflammation [80]. Initial circulating cytokines activate prostaglandin production in the CVOs and by catecholaminergic cell groups of the ventrolateral medulla and STN [17]. Subsequently, paraventricular neurons that contain corticotrophin-releasing hormone (CRH) and vasopressin are stimulated. In turn, they activate the release of adrenocorticotropic hormone (ACTH) from the anterior pituitary, and the ACTH stimulates the production of cortisol from the adrenal cortex increasing cortisol levels in plasma. This last effect has a negative feedback towards the stimulation of the HPA [17] in an attempt to protect the organism against the potentially toxic effects of cytokines after they have produced their initial beneficial effects. If this dampening does not take place, animals or humans will die. Sepsis-associated encephalopathy is a neurological syndrome that reflects an uncontrolled systemic inflammatory response to a source of infection [5, 8]. In sepsis, the concomitant expressions of IL-1β and the inducible isoform of nitric oxide have been demonstrated in the CVOs and related structures [75]. These neurotoxic effectors have a detrimental inhibitory effect on the central production and release of hormones, thus impairing the restoration of homeostasis due to stress [5, 17].
The role of CVOs in patients with depression has not been explored in depth. Evidence compiled from different studies suggest that patients with panic disorder show a dysregulation of the HPA [2], comprising a GABAergic dysfunction in the dorsomedial hypothalamus, which is activated by the OVLT when sensing increases in plasma lactate [127]. In depression, chronic inflammation can increase hypothalamic vasopressin production or glucocorticoid receptor resistance, both of which could act as a precedent for increased CRH levels, which intensifies the stress response system [68].
Role of the CVOs in chronic neurodegenerative diseases: terra incognita
In order to understand disease pathogenesis, it is vital to identify the key actors that participate in the initiation, progression and termination of the inflammatory reaction. Recent evidence suggests that the progression of Parkinson’s disease can be due to an uncontrolled excessive inflammation that causes neuronal loss [50]. Cunningham et al. [26] demonstrated that systemic inflammation induced by injection of LPS in rodents with scrapie, an animal prion disease, acutely exacerbates cognitive and motor signs of disease and accelerates its progression. Alzheimer’s disease (AD) and multiple sclerosis (MS) are two of the most prevalent human neurodegenerative disorders in which immunity and inflammation play a pivotal role in pathology [4, 138, 156, 157]. A putative link between the inflammatory processes, the sympathetic noradrenergic pathways and elevated plasma cortisol levels has been proposed in MS [159]. In none of these diseases, the role of the CVOs in their pathogenesis has been investigated.
Prion protein found in prion diseases is associated with chronic inflammation similar to that observed around amyloid plaques of AD [40]. Although disease-associated prion protein (PrPd) deposition is found in the CVOs in preclinical sheep with scrapie [130; Fig. 5], it remains unknown whether neuroinflammation occurs before the deposition of extracellular protein, or as part of the repair process after neurodegeneration. In the following sections, we will discuss the possible role of the CVOs in prion diseases. For that purpose, we will focus mainly in some of the recent findings available from animal models.
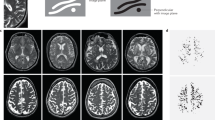
Early deposition of PrPd in the sensory CVOs and related brain structures of scrapie-infected goats. a Sections 1, 2 and 3 show the location of the OVLT and SFO (arrows) at the level of the diencephalon in b, c and d, respectively. e The exact location of the AP at the level of the obex. PrPd accumulations are detected by immunohistochemistry in the CVOs and related structures rather than randomly. The exact location of the CVOs is indicated by black arrows whereas the location of related nuclei is denoted by grey capital letters and arrows. Neuroanatomical sites are in lowercase to assist with the section orientation. STN solitary tract nucleus, DMNV dorsal motor nucleus of the vagus nerve, PVN paraventricular nucleus, Lat HT lateral hypothalamic area, AV3V anterioventral part of the third ventricle, SCN suprachiasmatic nucleus, SON supraoptic nucleus, ARC arcuate nucleus, PFN perifornical nucleus, MnPO median preoptic area, BNST bed nucleus of stria terminalis, lat V lateral ventricle, awc anterior white commisure, oc optic chiasm, fc fornix columns; or optic recess, sa septal area. a–d: ×1; e: x4
Animal prion diseases: neuroinvasion can occur through the CVOs
Some viruses like reoviruses, herpesviruses and the rabies virus can be transported from axon terminals to the neuronal cell body, and vice versa, in a retrograde or anterograde manner, respectively. Recent investigations confirmed that rabies virus can also enter the CNS via blood, although it is unclear if they do so by crossing the BBB or through the CVOs [112]. Similarly, prions can reach the CNS by neural routes [88]. In ovine prion diseases, neuroinvasion can occur by retrograde transport of infectivity along sympathetic and parasympathetic peripheral nerves [90, 131, 149]. However, a bulk of data generated by experimental studies on bovine spongiform encephalopathy (BSE) and scrapie in sheep and on chronic wasting disease in cervids have confirmed that blood is infectious; this notion has been further supported by transmission of the new variant of Creutzfeldt–Jakob disease between humans by blood transfusion (reviewed in [131]). Recent studies in sheep and goats infected with scrapie or BSE have shown that PrPd accumulation in the CVOs is an early and consistent event that is not affected by the route of challenge or the agent strain [55, 131]. This has been interpreted to suggest that blood-borne prions can enter the CNS through the CVOs. PrPd deposition in the CVOs has also been observed in mice infected with several murine strains and in cattle and deer infected with the BSE agent [131].
Role of the CVOs in the spread of prion infectivity to the brain parenchyma
In the case of prion diseases, the CVOs have been shown to accumulate PrPd before adjacent structures of the brain parenchyma [55, 130]. It is likely that once infection is established in the CVOs, it could spread to interconnected neural structures. Thus, for example, PrPd in the hypothalamic paraventricular nucleus and in the bed nucleus of the stria terminalis could result from spread from the SFO and from the OVLT (Fig. 5a–d). The involvement of the DMNV and of the AP is often simultaneous [55, 131], and it is shortly thereafter accompanied by accumulation of PrPd in the STN (Fig. 5e). Interestingly, there is an absence of immunolabelling for some proteins that are specific for the BBB in the STN, supporting previous statements that this nucleus contains a proportion of fenestrated capillaries [58, 87]. All these issues make it difficult to determine if the mechanism of entry of infection at this level of the brain is through the vagus nerve or from the blood, or from both. Figure 6 highlights the initial brain structures that are stimulated by the neural or humoral pathways and their subsequent connections to other neuronal nuclei.
Pathways of neuroinvasion in prion diseases. As illustrated in Dantzer et al. [30], there are two main pathways by which the immune system communicates with the brain in order to activate the hypothalamic-pituitary axis: a neural pathway (a) and a humoral pathway (b). In the neural pathway, peripheral visceral sensory afferent fibres of the vagus nerve stimulate the solitary tract nucleus, which have established connections with other nuclei highlighted in green (a). In the humoral pathway, circulating cytokines directly stimulate the CVOs (b) which have established connections with other nuclei (arrows) as reported in previous investigations [26, 76, 100]. Note that different arrow colours in b have been used to denote the CVO of origin. Investigations in sheep with preclinical scrapie or BSE indicate initial PrPd deposition in the CVOs and in those neuronal nuclei that have been highlighted in purple (b). We believe that the fact that those nuclei are common to those involved in the stimulation of the HPA axis may suggest that abnormalities in this axis might be present early in prion diseases. The non-sensory CVOs like the median eminence (ME), the neurohypophysis (NH), the pineal gland (PG) and the subcommisural organ (SCO) are shown. STN solitary tract nucleus, SPTN spinal trigeminal nucleus, DMNV dorsal motor nucleus of the vagus nerve, NA nucleus ambiguous, VLM ventrolateral medulla, PVN paraventricular nucleus, SCN suprachiasmatic nucleus, SON supraoptic nucleus, CEA central amygadolid nucleus, ARC arcuate nucleus, MePO median preoptic nucleus, BNST bed nucleus of stria terminalis, BNST bed nucleus of the stria terminalis, PBN parabrachial nuclei, PAG periacqueductal grey matter, R raphe nuclei
Could endocrine dysfunction in prion disorders be associated with pathology in the CVOs and related areas?
Several investigations point towards a dysfunction of the HPA and autonomic system in animal prion diseases. In 1964, Beck et al. [12] reported neural cell degeneration of the HPA axis in sheep with scrapie. Scrapie clinical signs include altered drinking and food intake behaviour caused by disturbances at the central level [9, 11, 12, 103–105]. Abnormal hormone plasma concentrations suggest alterations of the somatotropic (metabolic homeostasis and neuroprotection) and corticotropic (stress response) functions in sheep [51, 110, 119, 150] and rodents [158] infected with scrapie.
Endocrinopathies in patients with familial fatal insomnia or Creutzfeldt–Jakob disease include hypersecretion of cortisol, growth hormone and insulin growth factors, hyperinsulinaemia, altered glucose tolerance and/or insulin-resistant, adrenal-dependent obesity, loss of body weight, etc. [10, 85, 113]. While some research indicates that neurodegeneration and clinical signs are the result of the toxic effect of PrPd, other investigations support the notion of an impaired physiological function of the normal cellular prion protein (PrPc). In that respect, experiments with PrPc knockout mice suggested that this protein might play an important role in the modulation of the corticosteroid-dependent negative feedback on the HPA axis [117]. Nevertheless, a full understanding of the nature of clinical disease in prion diseases is still lacking.
Abnormal heart rate variability has been described in sheep with scrapie as an early and clinically-silent abnormality [53], and possibly as a manifestation of the pathology targeting the DMNV. We hypothesize that sites like the CVOs, which accumulate PrPd at early stages, are more vulnerable to pathological changes, which would lead to early clinically-detectable abnormalities. On-going investigations in sheep with preclinical scrapie or BSE show PrPd deposition in brain areas that can be activated by both the neural and the humoral pathways (Figs. 5, 6), and this could lead to an early dysfunction of the HPA axis in these prion diseases. In sheep with clinical scrapie, there is a glial response characterized by diffuse astrocytosis and microglial activation restricted to the preoptic area of the hypothalamus. Brains of these sheep also show an increase in (i) vasopressin-containing fibres crossing the median eminence and terminating in the neurohypophysis, (ii) oxytocin-containing neurons within the suprachiasmatic and arcuate nuclei, and (iii) the number of neurons containing these two hormones in the supraoptic and paraventricular nuclei (S. Sisó and M. C. Garza, unpublished observations).
Opinion and perspectives
Because of its impermeable nature, an intact BBB protects the CNS from toxic agents and pathogens circulating in the blood. Disruption of the BBB is, therefore, a critical event in the initiation and progression of neurological disorders. There are, however, some tiny structures of the brain where the BBB is absent; those are the CVOs which, having fenestrated capillaries, enable their neurons to have a direct contact with blood-borne substances. In some infectious diseases, these organs can provide the route of entry for the pathogens into the brain activating a cytokine-transcription cascade producing prostaglandins (febrile response) that subsequently can disrupt the BBB resulting in widespread CNS pathology. At present, the relative contribution of the immunopathological mechanisms that take place in the CVOs and their cross-talking with the brain parenchyma possessing a BBB is not well defined.
The CVOs are pivotal for most autonomic and endocrine functions. Investigations of the CVO–HPA circuits could contribute to the detection of clinically-silent abnormalities at early stages of disease. Chronic CNS disorders with disruptions in the HPA axis include multiple sclerosis, depression, bipolar disorder, anorexia nervosa, schizophrenia, prion diseases and AD [139]. An improved understanding of the role of the CVOs in disease might allow the development of therapies aimed at blocking the entry of pathogens into the CNS or at modulating the acute immune response at a central level. Moreover, recent research [14] suggests that the CVOs provide a source of stem/progenitor cells that can proliferate and give rise to neurons or glial cells in the adult brain [82, 93]. For all these reasons, opportunities in future could emerge for targeting the CVOs not only to maintain health but also to aid recovery from injury or infection. Finally, CNS disorders are a major focus of the pharmaceutical industry, with drugs able to cross the BBB representing some of its most successful products. An additional way to side step the constraints of such a barrier are to design CNS drugs that may be taken-up by the blood vessels within the CVOs. These therapeutic strategies may benefit from increased knowledge on the properties of these organs.
References
Abbott NJ, Rönnbäck L, Hansson E (2006) Astrocyte-endothelial interactions at the blood–brain barrier. Nat Rev Neurosci 7:41–53
Abelson JL, Khan S, Liberzon I, Young EA (2007) HPA axis activity in patients with panic disorder: review and synthesis of four studies. Depress Anxiety 24:66–76
Akert K, Potter HD, Anderson JW (1961) The subfornical organ in mammals. J Comp Neurol 116:1–14
Akiyama H, Barger S, Barnum S et al (2000) Inflammation and Alzheimer’s disease. Neurobiol Aging 21:383–421
Akrout N, Sharshar T, Annane D (2009) Mechanisms of brain signaling during sepsis. Curr Neuropharmacol 7:296–301
Allen AM, Oldfield BJ, Giles ME (2000) Localization of angiotensin receptors in the nervous sytem. In: Quirion R, Björklund A, Hökfelt T et al (eds) Peptide receptors, Part 1, vol 16. Elsevier Science, Amsterdam., pp 79–124
Anderson JW, Washburn DL, Ferguson AV (2000) Intrinsic osmosensitivity of subfornical organ neurons. Neuroscience 100:539–547
Annane D, Bellissant E, Cavaillon JM (2005) Septic shock. Lancet 365:63–78
Bailey JD, Berardinelli JG, Rocke TE, Bessen RA (2008) Prominent pancreatic endocrinopathy and altered control of food intake disrupt energy homeostasis in prion diseases. J Endocrinol 197:251–263
Barash JA (2008) Do midlife hormonal changes play a role in the onset of sporadic Creutzfeldt–Jakob disease? An epidemiologic perspective. Med Hypotheses 71:611–612
Beck E, Daniel PM (1969) Degenerative diseases of the central nervous system transmissible to experimental animals. Postgrad Med J 45:361–370
Beck E, Daniel PM, Parry HB (1964) Degeneration of the cerebellar and hypothalamoneurohypophysial systems in sheep with scrapie; and its relationship to human system degenerations. Brain 87:153–176
Behnsen G (1927) Über die Farbstoffspeicherung im Zentralnervensystem der weißen Maus in verschiedenen Alterszuständen. Z Zellforsch 4:515–572
Bennett L, Yang M, Enikolopov G, Iacovitti L (2009) Circumventricular organs: a novel site of neural stem cells in the adult brain. Mol Cell Neurosci 41:337–347
Bianchi C, Gutkowska J, Ballak M et al (1986) Radioautographic localization of 125I-atrial natriuretic factor binding sites in the brain. Neuroendocrinology 44:365–372
Broadwell RD, Balin BJ, Salcman M, Kaplan RS (1983) Brain–blood barrier? Yes and no. Proc Natl Acad Sci USA 80:7352–7356
Buller KM (2001) Circumventricular organs: gateways to the brain. Role of circumventricular organs in pro-inflammatory cytokine-induced activation of the hypothalamic-pituitary-adrenal axis. Clin Exp Pharmacol Physiol 28:581–589
Camacho A, Phillips MI (1981) Horseradish peroxidase study in rat of the neural connections of the organum vasculosum of the lamina terminalis. Neurosci Lett 25:201–204
Carpenter DO, Briggs DB, Knox AP, Strominger N (1988) Excitation of the area postrema neurons by transmitters, peptides, and cyclic nucleotides. J Neurophysiol 59:358–369
Ceccatelli S, Fahrenkrug J, Villar MJ, Hokfelt T (1991) Vasoactive intestinal polypeptide/peptide histidine isoleucine immunoreactive neuron systems in the basal hypothalamus of the rat with special reference to the portal vasculature: an immunohistochemical and in situ hybridization study. Neuroscience 43:483–502
Chernicky CL, Barnes KL, Ferrario CM, Conomy JP (1983) Brainstem distribution of neurons with efferent projections in the cervical vagus of the dog. Brain Res Bull 10:345–351
Ciriello J, Gutman MB (1991) Functional identification of central pressor pathways originating in the subfornical organ. Can J Physiol Pharmacol 69:1035–1045
Ciriello J, Hrycyshyn AW, Calaresu FR (1981) Glossopharyngeal and vagal afferent projections to the brain stem of the cat: a horseradish peroxidase study. J Auton Nerv Syst 4:63–79
Contreras RJ, Beckstead RM, Norgren R (1982) The central projections of the trigeminal, facial, glossopharyngeal and vagus nerves: an autoradiographic study in the rat. J Auton Nerv Syst 6:303–322
Cotrell GT, Ferguson AV (2004) Sensory circumventricular organs: central roles in integrated autonomic regulation. Regul Pept 117:11–23
Cunningham C, Campion S, Lunnon K et al (2009) Systemic inflammation induces acute behavioral and cognitive changes and accelerates neurodegenerative disease. Biol Psychiatry 65:304–312
Cunningham ET Jr, Miselis RR, Sawchenko PE (1994) The relationship of efferent projections from the area postrema to vagal motor and brain stem catecholamine-containing cell groups: an axonal transport and immunohistochemical study in the rat. Neuroscience 58:635–648
Dantzer R (2001) Cytokine-induced sickness behavior: where do we stand? Brain Behav Immun 15:7–24
Dantzer R, Konsman JP, Bluthe RM, Kelley KW (2000) Neural and humoral pathways of communication from the immune system to the brain: parallel or convergent? Auton Neurosci 85:60–65
Dantzer R, O’Connor JC, Freund GG, Johnson RW, Kelley KW (2008) From inflammation to sickness and depression: when the immune system subjugates the brain. Nat Rev Neurosci 9:46–56
Dellmann HD (1998) Structure of the subfornical organ: a review. Microsc Res Tech 41:85–97
Dellmann HD, Simpson J (1979) The subfornical organ. Int Rev Cytol 58:333–421
Dempsey EW, Wislocki GB (1955) An electron microscopic study of the blood brain barrier in the rat, employing silver nitrate as a vital stain. J Biophys Biochem Cytol 1:245–256
Denton DA, McKinley MJ, Weisinger RS (1996) Hypothalamic integration of body fluid regulation. PNAS 93:7397–7404
Duvernoy H, Koritke JG (1964) Contribution a l’etude de l’angioarchitectonie des organes circumventricularies. Arch Biol 75:849–904
Duvernoy H, Koritke JG (1969) Concerning the relationships of the circumventricular organs and their vessels with the cavity of he ventricles. In: Sterba G (ed) Zirkumventrikulare Organe und Liquor. VEB Gustav Fischer Verlag, Jena., pp 113–115
Duvernoy HM, Risold P-Y (2007) The circumventricular organs: an atlas of comparative anatomy and vascularization. Brain Res Rev 56:119–147
Ehrlich P (1885) Das Sauerstoff-Bedurfnis des Organismus: eine Farbenanalytische studie. Hirschwald, Berlin
Ehrlich P (1956) Über die methylenblaureaktion der lebenden Nervensubstans. In: Himmelweit F (ed) The Collected Papers of Paul Elrich. Pergamon Press, London, pp 500–508 (reprinted from Deutche Medizinische Wochen Schrift 1886)
Eikelenboom P, Bate C, Van Gool WA et al (2002) Neuroinflammation in Alzheimer’s disease and prion disease. Glia 40:232–239
Elmquist JK, Breder CD, Sherin JE et al (1997) Intravenous lipopolysaccharide induce cyclooxygenase 2-like immunoreactivity in rat brain perivascular microglia and meningeal macrophages. J Comp Neurol 381:119–129
Ferguson AV, Bains JS (1996) Electrophysiology of the circumventricular organs. Front Neuroendocrinol 17:440–475
Ferguson AV, Kasting NW (1986) Electrical stimulation in the subfornical organ increases plasma vasopressin concentrations in the conscious rat. Am J Physiol 251:425–428
Ferguson AV, Kasting NW (1987) Activation of subfornical organ efferents stimulates oxytocin concentrations in the rat. Regul Pept 18:93–100
Ferguson AV, Kasting NW (1988) Angiotensin acts at the subfornical organ to increase plasma oxytocin concentrations in the rat. Regul Pept 23:343–352
Fitts DA, Masson DB (1990) Preoptic angiotensin and salt appetite. Behav Neurosci 104:643–650
Fry M, Ferguson AV (2007) The sensory circumventricular organs: brain targets for circulating signals controlling ingestive behaviour. Physiol Behav 91:413–423
Galea I, Bechmann I, Perry VH (2007) What is immune privilege (not)? Trends Immunol 28:12–18
Ganong WF (2000) Circumventricular organs: definition and role in the regulation of endocrine and autonomic function. Clin Exp Pharmacol Physiol 27:422–427
Gao H-M, Hong J-S (2008) Why neurodegenerative diseases are progressive: uncontrolled inflammation drives disease progression. Trends Immunol 29:357–365
Gayrard V, Picard-Hagen N, Grino M et al (2000) Major hypercorticism is an endocrine feature of ewes with naturally occurring scrapie. Endocrinology 141:988–994
Giles ME, Fernley RT, Nakamura Y et al (1999) Characterization of a specific antibody to the rat angiotensin II AT1 receptor. J Histochem Cytochem 47:507–516
Glover DG, Pollard BJ, González L, Sisó S, Kennedy D, Jeffrey M (2007) A non-invasive screen for infectivity in transmissible spongiform encephalopathies. Gut 56:1329–1330
Goldmann EE (1909) Die äussere and innere Sekretion des gesunden und kranken Organismus im Lichte der “vitalen Färbung”. Beitr Klin Chir 64:192–265
González L, Martin S, Hawkins SA, Goldmann W, Jeffrey M, Sisó S (2010) Pathogenesis of natural goat scrapie: modulation by host PRNP genotype and effect of co-existent conditions. Vet Res 41:48
Goren O, Adorján I, Kálmán M (2006) Heterogenous occurrence of aquaporin-4 in the ependyma and in the circumventricular organs in rat and chicken. Anat Embryol 211:155–172
Gross PM (1987) Circumventricular organs and body fluids, Chaps. 1, 7, 8 in vol I, and Chap. 1 of vol II, and III. CRC Press, Boca Raton
Gross PM (1991) Morphology and physiology of capillary systems in subregions of the subfornical organ and area postrema. Can J Physiol Pharmacol 69:1010–1025
Gross PM, Weindl A (1987) Peering through the windows of the brain. J Cereb Blood Flow Metabol 7:663–672
Gu GB, Simerly RB (1997) Projections of the sexually dimorphic anteroventral periventricular nucleus in the female rat. J Comp Neurol 384:142–164
Guan JL, Wang QP, Shioda S (2000) Observation of the ultrastructure and synaptic relationships of angiotensin II-like immunoreactive neurons in the rat area postrema. Synapse 38:231–237
Gutman MB, Ciriello J, Mogenson GJ (1988) Effects of plasma angiotensin II and hypernatremia on subfornical organ neurons. Am J Physiol 254:R746–R754
Guyenet PG (2006) The sympathetic control of blood pressure. Nat Rev Neurosci 7:335–346
Haywood JR, Fink GD, Buggy J, Boutelle S, Johnson AK, Brody MJ (1983) Prevention of two-kidney, one clip renal hypertension in rat by ablation of AV3V tissue. Am J Physiol 245:683–689
Hofer H (1958) Zur Morphologie der circumventrikulären Organe des Zwischenhirns der Säugetiere. Verhandl Deut Zool Ges 8:202–251
Holmes MC, Catt KJ, Aguilera G (1987) Involvement of vasopressin in the down-regulation of pituitary corticotropin-releasing factor receptors after adrenolectomy. Endocrinology 121:2093–2098
Honda K, Negoro H, Higuchi T, Tadokoro Y (1987) Activation of neurosecretory cells by osmotic stimulation of anteroventral third ventricle. Am J Physiol 252:R1039–R1045
Irwin MR, Miller AH (2007) Depressive disorders and immunity: 20 years of progress and discovery. Brain Behav Immun 21:374–383
Johnston AK, Gross PM (1993) Sensory circumventricular organs and brain homeostatic pathways. FASEB J 7:678–686
Jones CR, Hiley CR, Pelton JT, Mohr M (1989) Autoradiographic visualization of the binding sites for [125I] endothelin in rat and human brain. Neurosci Lett 97:276–279
Kalia M, Mesulam MM (1980) Brain stem projections of sensory and motor components of the vagus complex in the cat: I. The cervical vagus and nodose ganglion. J Comp Neurol 193:435–465
Kalia M, Sullivan JM (1982) Brainstem projections of sensory and motor components of the vagus nerve in the rat. J Comp Neurol 211:248–265
Katsuura G, Gottschall PE, Dahl RR, Arimura A (1988) Adrenocorticotropin release induce by intracerebroventricular injection of recombinant human interleukin-1 in rats: possible involvement of prostaglandin. Endocrinology 122:1773–1779
Kawano H, Masuko S (2001) Tyrosine hydroxylase-immunoreactive projections from the caudal ventrolateral medulla to the subfornical organ in the rat. Brain Res 903:154–161
Konsman JP, Kelley K, Dantzer R (1991) Temporal and spatial relationships between lipopolysaccharide-induced expression of Fos, interleukin-1β and inducible nitric oxide synthase in rat brain. Neuroscience 89:535–548
Krisch B, Leonhardt H, Oksche A (1987) Compartments in the organum vasculosum laminae terminalis of the rat and their delineation against the outer cerebrospinal fluid-containing space. Cell Tissue Res 250:331–347
Kristensson K, Nygård M, Bertini G, Bentivoglio M (2010) African trypanosome infections of the nervous system: parasite entry and effects on sleep and synaptic functions. Prog Neurobiol 91:152–171
Krout KE, Kawano J, Mettenleiter TC, Loewy AD (2001) CNS inputs to the suprachiasmatic nucleus of the rat. Neuroscience 110:73–92
Kubo S, Inui T, Yamazato K (2004) Visualisation of the circumventricular organs by fluorescence endoscopy. J Neurol Neurosurg Psychiatry 75:180
Kushner I (1982) The phenomenon of the acute phase response. Ann NY Acad Sci 389:39–48
Li NC, Lee A, Whitmer RA, Kivipelto M, Lawler E, Kazis LE, Wolozin B (2010) Use of angiotensin receptor blockers and risk of dementia in a predominantly male population: prospective cohort analysis. BMJ 340:b5465. doi:10.1136/bmj.b5465
Lie DC, Song H, Colamarino SA, Ming GL, Gage FH (2004) Neurogenesis in the adult brain: new strategies for central nervous system diseases. Annu Rev Pharmacol Toxicol 44:399–421
Lind RW (1987) Neural connections. In: Gross PM (ed) Circumventricular organs and body fluids, vol I. CRC Press, Boca Raton, pp 27–42
Lind RW, Van Hoesen GW, Johnson AK (1982) An HRP study of the connections of the subfornical organ of the rat. J Comp Neurol 210:265–277
Lugaresi E, Provini F, Montagna P (2004) The neuroanatomy of sleep. Considerations on the role of the thalamus in sleep and a proposal for a caudorostral organization. Eur J Anat 8:85–94
Mangiapane ML, Brody MJ (1987) Vasoconstrictor and vasodilator sites within anteroventral third ventricle region. Am J Physiol 253:R827–R831
Maolood N, Meister B (2009) Protein components of the blood–brain barrier (BBB) in the brainstem area postrema-nucleus tractus solitarius region. J Chem Neuroanat 37:182–195
McBride PA, Schulz-Schaeffer WJ, Donaldson M et al (2001) Early spread of scrapie from the gastrointestinal tract to the central nervous system involves autonomic fibers of the splanchnic and vagus nerves. J Virol 75:9320–9327
McKinley MJ, Bicknell RJ, Hards D et al (1992) Efferent neural pathways of the lamina terminalis subserving osmoregulation. Prog Brain Res 91:395–402
McKinley MJ, Congiu M, Miselis RR, Oldfield BJ, Pennington G (1988) The lamina terminalis and osmotically stimulated vasopressin secretion. In: Yoshida S, Share L (eds) Recent progress in pituitary hormones. Excerpta Medica, Amsterdam, pp 117–124
McKinley MJ, McAllen RM, Davern P et al (2003) The sensory circumventricular organs of the mammalian brain. In: Advances in anatomy embryology and cell biology, vol 172, 1st edn. Springer, Berlin, Heidelberg
Mészáros T, Leranth C, Palkovits M, Hazas J (1969) Secretory and esterase activity of the circumventricular organs with special reference to the infundibular ependyma. In: Sterba G (ed) Zirkumventrikulare Organe und Liquor. VEB Gustav Fischer Verlag, Jena, pp 131–134
Mignone JL, Kukekov V, Chiang AS, Steindler D, Enikolopov G (2004) Neural stem and progenitor cells in nestin-GFP transgenic mice. J Comp Neurol 469:311–324
Miselis RR (1981) The efferent projections of the subfornical organ of the rat: a circumventricular organ within a neural network subserving water balance. Brain Res 230:1–23
Miselis RR, Shapiro RE, Hand PJ (1979) Subfornical organ efferents to neural systems for control of body water. Science 205:1022–1102
Miselis RR, Weiss ML, Shapiro RE (1987) Modulation of the visceral neuraxis. In: Gross PM (ed) Circumventricular organs and body fluids, vol III. CRC Press, Boca Raton, pp 143–162
Morest DK (1960) A study of the structure of the area postrema with Golgi methods. Am J Anat 107:291–303
Mullier A, Bouret SG, Prevot V, Dehouck B (2010) Differential distribution of tight junction proteins suggests a role for tanycytes in blood-hypothalamus barrier regulation in the adult mouse brain. J Comp Neurol 518:943–962
Oldfield BJ, Badoe E, Hards DK, McKinley MJ (1994) Fos production in retrogradely labelled neurons of the lamina terminalis following intravenous infusion of either hypertonic saline or angiotensin II. Neuroscience 60:255–262
Oldfield BJ, Hards DK, McKinley MJ (1991) Projections from the subfornical organ to the supraoptic nucleus in the rat: ultrastructural identification of an interposed synapse in the median preoptic nucleus using a combination of neural tracers. Brain Res 558:13–19
Oldfield BJ, Miselis RR, McKinley MJ (1991) Median preoptic nucleus projections to vasopressin-containing neurons of the supraoptic nucleus in sheep—a light and electron microscope study. Brain Res 542:193–200
Pan W, Kastin AJ (2007) Adipokines and the blood–brain barrier. Peptides 28:1317–1330
Parry HB (1962) Scrapie: a transmissible and hereditary disease of sheep. Heredity 17:75–105
Parry HB, Livett BG (1973) A new hypothalamic pathway to the median eminence containing neurophysin and its hypertrophy in sheep with natural scrapie. Nature 242:63–65
Parry HB, Livett BG (1976) Neurophysin in the brain and pituitary gland of normal and scrapie-affected sheep—I. Its localization in the hypothalamus and neurohypophysis with particular reference to a new hypothalamic neurosecretory pathway to the median eminence. Neuroscience 1:275–299
Pecchi E, Dallaporta M, Charrier C et al (2007) Glial fibrillary acidic protein (GFAP)-positive radial-like cells are present in the vicinity of proliferative progenitors in the nucleus tractus solitarius of adult rat. J Comp Neurol 501:353–368
Peress NS, Perillo E, Fenstermacher JD (1989) Circumventricular organs in chronic serum sickness: a model for cerebral lupus. Biol Psychiatry 26:397–407
Petrov T, Howarth AG, Krukoff TL, Stevenson BR (1994) Distribution of the tight junction-associated protein ZO-1 in circumventricular organs of the CNS. Mol Brain Res 21:235–246
Phillips MI, Camacho A (1987) Neural connections of the organum vasculosum of the lamina terminalis. In: Gross PM (ed) Circumventricular organs and body fluids, vol I. CRC Press, Boca Raton., pp 157–169
Picard-Hagen N, Gayrard V, Alvinerie M et al (2000) Naturally occurring scrapie is associated with a lower CBG binding capacity in ewes. J Endocrinol 165:527–532
Price CJ, Hoyda TD, Ferguson AV (2008) The area postrema: a brain monitor and integrator of systemic autonomic state. Neuroscientist 14:182–194
Preuss MA, Faber ML, Tan GS et al (2009) Intravenous inoculation of a bat-associated rabies virus causes lethal encephalopathy in mice through invasion of the brain via neurosecretory hypothalamic fibers. PLoS Pathog 5(6):e1000485
Provini F, Cortelli P, Montagna P, Gambetti P, Lugaresi E (2008) Fatal insomnia and agrypnia excitata: sleep and the limbic system. Rev Neurol 164:692–700
Putnam TJ (1922) The intercolumnar tubercle: an undescribed area in the anterior wall of the third ventricle. Bull J Hopkins Hosp 33:181
Richard D, Bourque CW (1995) Synaptic control of rat supraoptic neurons during osmotic stimulation of the organum vasculosum lamina terminalis in vitro. J Physiol 489:567–577
Roth J, Harré EM, Rummel C, Gerstberger R, Hübschle T (2004) Signaling the brain in systemic inflammation: role of sensory circumventricular organs. Front Biosci 9:290–300
Sánchez-Álavez M, Criado JR et al (2008) Hypothalamic-pituitary-adrenal axis disregulation in PrPC-null mice. Neuroreport 19:1473–1477
Scammell TE, Elmquist JK, Griffin JD, Saper CB (1996) Ventromedial preoptic prostaglandin E2 activates fever-producing autonomic pathways. J Neurosci 16:6246–6254
Schelcher F, Picard-Hagen N, Laroute V et al (1999) Corticoid concentrations are increased in the plasma and urine of ewes with naturally occurring scrapie. Endocrinology 140:2422–2425
Schulz M, Engelhardt B (2005) The circumventricular organs participate in the immunopathogenesis of experimental autoimmune encephalomyelitis. Cerebrospinal Fluid Res 2:8
Schultzberg M, Ambatsis M, Samuelsson EB, Kristensson K, van Meirvenne N (1988) Spread of Trypanosoma brucei to the nervous sytem: early attack on circumventricular organs and sensory ganglia. J Neurosci Res 21:56–61
Schwendemann G (1973) Zur Ultrastruktur des Organon vasculosum laminae terminalis der ratte mit besonderer Berucksichtigung der Gefaße. In: Advances in anatomy, embryology and cell biology, vol 47. Springer, Berlin Heidelberg. pp 7–72
Shapiro RE, Miselis RR (1985) The central connections of the area postrema of the rat. J Comp Neurol 234:344–364
Shaver SW, Pang JJ, Wainman DS, Wall KM, Gross PM (1992) Morphology and function of capillary networks in subregions of the rat tuber cinereum. Cell Tissue Res 267:437–448
Shaver SW, Pang JJ, Wall KM, Sposito NM, Gross PM (1991) Subregional topography of capillaries in the dorsal vagal complex of rats. I. Morphometric properties. J Comp Neurol 306:73–82
Shaver SW, Sposito NM, Gross PM (1990) Quantitative fine structure of capillaries in subregions of the rat subfornical organ. J Comp Neurol 294:145–152
Shekhar A, Keim SR (1997) The circumventricular organs form a potential neural pathway for lactate sensitivity: implications for panic disorder. J Neurosci 17:9726–9735
Schröder R, Linke RP (1999) Cerebrovascular involvement in systemic AA and AL amyloidosis: a clear haematogenic pattern. Virchows Arch 434:551–560
Simpson JB (1981) The circumventricular organs and the central actions of angiotensin. Neuroendocrinology 32:248–256
Sisó S, Jeffrey M, González L (2009) Neuroinvasion in sheep transmissible spongiform encephalopathies: the role of the haematogenous route. Neuropathol Appl Neurobiol 35:232–246
Sisó S, Jeffrey M, González L (2010) Neuroinvasion in prion diseases: the roles of ascending neural infection and blood dissemination. Interdiscip Perspect Infect Dis 2010:747892. doi:10.1155/2010/747892
Solano-Flores LP, Rosas-Arellano MP, Ciriello J (1997) Fos induction in central structures after afferent renal nerve stimulation. Brain Res 753:102–119
Song K, Allen AM, Paxinos G, Mendelsohn FA (1992) Mapping of angiotensin II receptor subtype heterogeneity in rat brain. J Comp Neurol 316:467–484
Spiegel EA (1918) Das ganglion psalterii. Anat Anz 51:454–462
Summy-Long JY, Kadekaro M (2001) Circumventricular organs: gateways to the brain. role of circumventricular organs (CVO) in neuroendocrine responses: interactions of CVO and the magnocellular neuroendocrine system in different reproductive states. Clin Exp Pharmacol Physiol 28:590–601
Sunn N, McKinley MJ, Oldfield BJ (2001) Identification of efferent neural pathways from the lamina terminalis activated by blood-borne relaxin. J Neuroendocrinol 13:432–437
Steinman L (2004) Elaborate interactions between the immune and nervous systems. Nat Immunol 5:575–581
Steinman L (2008) Nuanced roles of cytokines in three major human brain disorders. J Clin Invest 118:3557–3563
Swaab DF, Ai-Min B, Lucassen PJ (2005) The stress system in the human brain in depression and neurodegeneration. Ageing Res Rev 4:141–194
Swanson LW, Lind RW (1986) Neural projections subserving the initiation of a specific motivated behavior in the rat: new projections from the subfornical organ. Brain Res 379:399–403
Tanaka J, Saito H, Kaba H (1987) Subfornical organ and hypothalamic paraventricular nucleus connections with median preoptic nucleus neurons: an electrophysiological study in the rat. Exp Brain Res 68:579–585
Turrin NP, Rivest S (2004) Unraveling the molecular details involved in the intimate link between the immune and neuroendocrine systems. Exp Biol Med (Maywood) 229:996–1006
Ulrich-Lai YM, Herman JP (2009) Neural regulation of endocrine and autonomic stress responses. Nat Rev 10:397–409
Undesser KP, Hasser E, Haywood JR, Johnson AK, Bishop VS (1985) Interactions of vasopressin with the area postrema in arterial baroreflex function in conscious rabbits. Circ Res 56:410–417
Uschakov A, McAllen RM, Oldfield BJ, McKinley MJ (2001) Efferent projections of subpopulations of neurons in the lamina terminalis. Abstr Soc Neurosci 27:733–738
van Breemen VL, Clemente CD (1955) Silver deposition in the central nervous system and the hematoencephalic barrier studied with the electron microscope. J Biophys Biochem Cytol 1:161–166
Van Dam A-M, Brouns M, Man-A-Hing W, Berkenbosch F (1993) Immunocytochemical detection of prostaglandin E2 in microvasculature of rat brain after administration of bacterial endotoxin. Brain Res 613:331–336
van der Kooy D, Koda LY (1983) Organization of the projections of a circumventricular organ: the area postrema in the rat. J Comp Neurol 219:328–338
van Keulen LJM, Vromans MEW, van Zijderveld FG (2002) Early and late pathogenesis of natural scrapie infection in sheep. APMIS 110:23–32
Viguié C, Chilliard Y, Gayrard V et al (2004) Alterations of somatotropic function in prion disease in sheep. J Endocr 183:427–435
Vivas L, Chiaraviglio E, Carrer HF (1990) Rat organum vasculosum laminae terminalis I vitro-responses to changes in sodium concentration. Brain Res 519:294–300
Watkins AD (1994) Hierarchical cortical control of neuroimmunomodulatory pathways. Neuropathol Appl Neurobiol 20:423–431
Wilson AJ, Carati CJ, Gannon BJ, Haberberger R, Chataway TK (2010) Aquaporin-1 in blood vessels of rat circumventricular organs. Cell Tissue Res 340:159–168
Wislocki GB, Leduc EH (1952) Vital staining of the hematoencephalic barrier by silver nitrate and trypan blue, and cytological comparison of the neurohypophysis, pineal body, area postrema, intercolumnar tubercle and supraoptic crest. J Comp Neurol 96:371–414
Wislocki GB, Putnam TJ (1924) Further observations on the anatomy and physiology of the areae postremae. Anat Rec 27:151–156
Wyss-Coray T (2006) Inflammation in Alzheimer disease: driving force, bystander or beneficial response. Nat Med 12:1005–1015
Wyss-Coray T, Mucke L (2002) Inflammation in neurodegenerative disease: a double-edged sword. Neuron 35:419–432
Ye X, Carp RI, Yu Y, Kozielski R, Kozlowski P (1994) Effect of infection with the 139H scrapie strain on the number, area and/or location of hypothalamic CRF- and VP-immunostained neurons. Acta Neuropathol 88:44–54
Zoukos Y, Leonard JP, Thomaides T, Thompson AJ, Cuzner ML (1992) β-Adrenergic receptor density and function of peripheral blood mononuclear cells are increased in multiple sclerosis: a regulatory role for cortisol and interleukin-1. Ann Neurol 31:657–662
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sisó, S., Jeffrey, M. & González, L. Sensory circumventricular organs in health and disease. Acta Neuropathol 120, 689–705 (2010). https://doi.org/10.1007/s00401-010-0743-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-010-0743-5