Abstract
Chronic kidney disease (CKD) increases myocardial infarct size by an unknown mechanism. Here we examined the hypothesis that impairment of protective PI3K-PDK1-Akt and/or mTORC-Akt signaling upon reperfusion contributes to CKD-induced enlargement of infarct size. CKD was induced in rats by 5/6 nephrectomy (SNx group) 4 weeks before myocardial infarction experiments, and sham-operated rats served as controls (Sham group). Infarct size as a percentage of area at risk after ischemia/reperfusion was significantly larger in the SNx group than in the Sham group (56.3 ± 4.6 vs. 41.4 ± 2.0%). In SNx group, myocardial p-Akt-Thr308 level at baseline was elevated, and reperfusion-induced phosphorylation of p-Akt-Ser473, p-p70s6K and p-GSK-3β was significantly suppressed. Inhibition of Akt-Ser473 phosphorylation upon reperfusion by Ku-0063794 significantly increased infarct size in the Sham group but not in the SNx group. There was no difference between the two groups in activities of mTORC2 and PDK1 and protein level of PTEN. However, the PP2A regulatory subunit B55α, which specifically targets Akt-Thr308, was reduced by 24% in the SNx group. Knockdown of B55α by siRNA increased baseline p-Akt-Thr308 and blunted Akt-Ser473 phosphorylation in response to insulin-like growth factor-1 (IGF-1) in H9c2 cells. A blunted response of Akt-Ser473 to IGF-1 was also observed in HEK293 cells transfected with a p-Thr308-mimetic Akt mutant (T308D). These results indicate that increased Akt-Thr308 phosphorylation by down-regulation of B55α inhibits Akt-Ser473 phosphorylation upon reperfusion in CKD and that the impaired Akt activation by insufficient Ser473 phosphorylation upon reperfusion contributes to infarct size enlargement by CKD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic kidney disease (CKD) is not only a major risk factor of acute myocardial infarction (AMI) but also a factor that significantly reduces the survival rate after AMI [20, 29, 38]. Mechanisms by which CKD worsens the prognosis after AMI appear to be multifactorial, including diminished response to diuretics, reduced tolerability to inhibitors of the renin-angiotensin system and enlargement of infarct size [5, 8, 10, 38]. Earlier animal studies consistently showed that CKD enlarges myocardial infarct size after ischemia/reperfusion [5, 8, 9], and significant impairment of mitochondrial functions by uremia was recently reported [36]. On the other hand, myocardial responses to protection afforded by ischemic or pharmacological preconditioning were reported to be preserved in some, but not all, rat models of CKD [5, 9, 32]. However, the impact of CKD on pro-survival signal pathways in cardiomyocytes at the time of reperfusion has not been fully characterized, and the mechanism of CKD-induced enlargement of infarct size remains unclear.
In the present study, we hypothesized that CKD impairs activation of phosphoinositide 3-kinase (PI3K)-Akt and/or mechanistic target of rapamycin complex 2 (mTORC2)-Akt signaling upon reperfusion, aggravating reperfusion injury. The rationale for this hypothesis is two-fold. First, CKD induces insulin resistance, i.e., disruption of insulin receptor-mediated signaling, which participates in regulation of glucose and fatty acid metabolism and protection from cell death [18, 33]. Second, amino acid metabolism, which is closely related to mechanistic target of rapamycin complex (mTORC) signaling, is significantly modified by CKD [13]. mTORC signals have been shown to play a major role in protection from ischemia/reperfusion and in autophagy that modifies cell tolerance to injury [31, 39]. We tested the hypothesis by using a rat model of CKD and cultured cell lines (H9c2 and HEK293) in vitro, and the results showed that down-regulation of protein phosphatase 2A (PP2A)-B55α by CKD is a novel mechanism that inhibits full activation of Akt-mediated protective signaling upon reperfusion.
Methods
This study was conducted in strict accordance with the Guide for the Care and Use of Laboratory Animals published by National Research Council of the National Academies, USA (2011) and was approved by the Animal Use Committee of Sapporo Medical University.
Preparation of a model of chronic kidney disease (CKD) and its control
CKD was induced in male Sprague–Dawley (SD) rats (10–12 weeks old) by two-step subtotal nephrectomy (5/6 nephrectomy) as in previous studies [5, 8, 9]. In brief, rats were anesthetized with intraperitoneal injection of pentobarbital sodium (80 mg/kg) and the adequacy of anesthesia during the experiments was frequently checked and confirmed by absence of corneal reflex. Additional doses of pentobarbital (0.5 mg each) were administered intravenously if necessary to maintain the adequate level of anesthesia. Under anesthesia, the right kidneys of the rats assigned to the subtotal nephrectomy group (SNx group) were decapsulated and removed. Seven days later, two-thirds of the left kidney was additionally resected. In rats assigned to the Sham group, only decapsulation of the kidneys was performed. Four weeks after the second operation, rats were used for infarct size experiments or immunoblotting experiments.
Infarct size experiments in vivo
Infarct size experiments were performed as previously reported [16, 39]. In brief, rats were anesthetized as described above and ventilated with a Harvard Model 683 respirator (Harvard Apparatus, South Natick, MA, USA). The chest was opened via a left thoracotomy, and a coronary snare was prepared around the left main coronary artery. Saline-filled catheters were inserted into a jugular vein and carotid artery for drug injection and for monitoring of blood pressure, respectively. The catheter placed in the carotid artery was connected to a Nihon-Kohden SCK-590 pressure transducer. An electrocardiogram was obtained using precordial bipolar electrodes. Rectal temperature was adjusted to within 37.5–38.5 °C by using a heating lamp when necessary. After 15 min of stabilization, rats underwent 20 min of left coronary artery occlusion and 2 h of reperfusion.
In a separate series of infarct size experiments, rats in the Sham and SNx groups were divided into a vehicle-treated group and a group treated with Ku-0063794, an inhibitor of both mTORC1 and mTORC2 [39], respectively. Rats underwent 20-min coronary occlusion/2-h reperfusion, and the vehicle or Ku-0063794 (8 mg/kg) was administered intravenously at 5 min before reperfusion. In a separate subgroup of rats in the Sham group, tissues for immunoblotting were sampled from the area at risk at 5 min after reperfusion to confirm the inhibitory effect of Ku-0063794.
After 2 h of reperfusion, rats were heparinized with 200 U of heparin and then euthanized by intravenous injection of a lethal dose of pentobarbital (100 mg). Hearts were excised, mounted onto a Langendorff apparatus and perfused with saline to wash out blood, and then the coronary artery was re-occluded. A saline suspension of fluorescent polymer microspheres (Duke Scientific, Palo Alto, CA, USA) was infused into the aorta to negatively mark the area at risk, and the hearts were frozen at −20 °C. Frozen hearts were sliced into 1.5-mm-thick sections and stained with triphenyltetrazolium chloride. Areas of infarct and those of region at risk were determined by using Image J software (National Institutes of Health). Their volumes were obtained by multiplying each area by 1.5 mm, i.e., the thickness of the heart slice.
Isolated perfused heart preparation for sampling of the myocardium
Preparation of buffer-perfused isolated hearts was performed as previously reported [16, 40]. In brief, rats were anesthetized as described above and ventilated with a Harvard Model 683 respirator. After the adequacy of anesthesia was confirmed by lack of corneal reflex, hearts were quickly excised and perfused in a Langendorff mode at a pressure of 75 mmHg with non-circulating modified Krebs-Henseleit buffer. The buffer was gassed with 95% O2/5% CO2, and the temperature of the perfusate was maintained at 38 °C. A fluid-filled latex balloon was inserted into the left ventricle to monitor hemodynamics and was connected to an SCK-590 transducer. Heart preparations were stabilized for 20 min before entry to the tissue sampling protocol and then received 25 min of global ischemia followed by reperfusion. This duration of ischemia ex vivo was selected since infarct size as a percentage of area at risk (IS/AR) after 20-min regional ischemia in vivo has been shown to be similar to that after 25-min global ischemia in our isolated heart preparation [22, 25]. Myocardial biopsy samples (0.2–0.3 g) were taken from the left ventricle under the baseline condition (just after stabilization) and at 5 min after reperfusion. Tissues were snap-frozen in liquid nitrogen and stored at −80 °C until biochemical analysis.
Immunoblotting and immunoprecipitation
Frozen myocardial samples were homogenized in ice-cold CHAPS buffer containing 20 mmol/l HEPES (pH 7.5), 120 mmol/l NaCl, 1 mmol/l EDTA, 50 mmol/l NaF, 0.3% CHAPS, 0.5 mmol/l Na3VO4, a protease inhibitor cocktail (Complete mini, Roche Molecular Biochemicals, Mannheim, Germany), and a phosphatase inhibitor cocktail (PhosSTOP, Roche Molecular Biochemicals). The homogenate was centrifuged at 13,000g for 15 min to obtain the supernatant. Protein concentration was determined using the Bradford assay.
Equal amounts of proteins were electrophoresed on polyacrylamide gels and then blotted onto PVDF membranes (Millipore, Bedford, MA, USA). After blocking, the blots were incubated with antibodies that recognize the following: phospho-Akt (Ser473, Thr308) and total Akt, phospho-glycogen synthase kinase-3β (p-Ser9-GSK-3β) and total GSK-3β, phospho-p70s6 kinase (p-Thr389-p70s6K) and total p70s6K, phospho-extracellular-signal regulated kinase (p-Thr202/Tyr204-ERK1 and p-Thr185/Tyr187-ERK2) and total ERK, phospho-janus activating kinase-2 (p-JAK2) and total JAK2, phosphatase and tensin homolog (PTEN), phosphoinositide-dependent kinase-1 (PDK1), mTOR, Rictor, Sin1, Deptor, PP2A A subunit, PP2A B subunit (B55α isoform), PP2A C subunit (Cell Signaling Technology, Beverly, MA, USA); PH domain and leucine rich repeat protein phosphatases 1 (PHLPP1) (Bethyl Laboratories, Montgomery, TX, USA); human influenza hemagglutinin (HA) (Millipore, Billerica, MA, USA); and vinculin (Sigma Aldrich, St Louis, MO, USA). Immunoblotted proteins were visualized by using an Immobilon Western detection kit (Millipore, Billerica, MA, USA). Intensities of individual bands were quantified by using Image J software.
Immunoprecipitation was performed as previously reported [39, 40]. The lysates from total homogenates were incubated for 30 min with 40 μl of protein G magnetic beads (New England Biolabs, Ipswich, MA, USA) to remove endogenous IgG. Equal amounts (1000 μg) of the pre-cleaned supernatants were incubated with either 3 μg of rabbit anti-Sin1 antibody or normal rabbit IgG for 1 h at 4 °C. The mixture was then incubated with 40 μl of fresh beads for 1 h. The beads were washed thrice with PBS containing protease inhibitor cocktail and re-suspended in SDS sample loading buffer followed by denaturation. The supernatant was used for immunoblotting.
In vitro kinase assay
In isolated perfused hearts, the ventricular myocardium was sampled at baseline and at 5 min after reperfusion for an in vitro kinase assay. mTORC2 and PDK1 were immunoprecipitated by an anti-Sin1 antibody and anti-PDK1 antibody, respectively, and incubated with 40 μl of fresh beads for 1 h. After the supernatant had been removed, the beads were washed 3 times with 500 μl of CHAPS buffer and then with kinase assay buffer containing 25 mmol/l HEPES (pH 7.4), 100 mmol/l sodium acetate, and 1 mmol/l magnesium chloride. The beads with immunoprecipitated mTORC2 or PDK1 were incubated with 0.5 μg of recombinant Akt (Millipore, Bedford, MA, USA) and 1 mmol/l ATP at 37 °C for 15 min. The reaction was stopped by adding SDS sample buffer and then boiling at 70 °C for 10 min. Immunoblotting for phospho-Ser473 Akt and for phospho-Thr308 Akt was performed by using supernatants from mixtures with mTORC immunoprecipitates and mixtures with PDK1 immunoprecipitates, respectively.
Cell culture and transfection
H9c2 cells and human embryonic kidney cells (HEK-293 cells) were obtained from ATCC (American Type Culture Collection). The cells were cultured in DMEM (4.5 g/l glucose) supplemented with 10% fetal bovine serum and antibiotics as reported previously [26, 27].
To knock down PP2A B55α expression in H9c2 cells, PP2A B55α siRNA (ON-TARGETplus) and non-silencing siRNA were purchased from Dharmacon (Chicago, IL, USA) and were transfected to H9c2 cells using Lipofectamine RNAiMAX (Thermo Scientific, Waltham, MA, USA). The culture medium was exchanged with serum-free DMEM after 12 h of transfection for serum starvation. To examine the effect of knockdown of PP2A B55α expression on cytoprotective signals, cells were treated with 50 nmol/l insulin-like growth factor-1 (IGF-1) or a vehicle for 15 min at 12 h after serum starvation, and whole cell lysates of the cells were prepared using CellLytic-M Mammalian Cell Lysis/Extraction agent (Sigma).
To demonstrate the role of constitutive phosphorylation of Thr308-Akt in regulation of Ser473-Akt response to upstream signals, the HA-AktWT plasmid (WT) (Addgene 9021, Cambridge, MA, USA) or the HA-AktThr308D (T308D) were transfected into HEK293 cells using FuGENE HD (Promega, Madison, WI, USA). A QuikChange Lightening mutagenesis kit (Stratagene) was used for site-directed mutagenesis of Akt, and the primer sets for mutated Akt are as follows: Akt T308D (Forward, 5′-GCCACCATGAAGGACTTTTGCGGCAC-3′; reverse, 5′-GTGCCGCAAAAGTCCTTCATGGTGGC-3′). The culture medium was exchanged with serum-free DMEM after 24 h of transfection, followed by replacement of the culture medium with Tyrode’s formulation after 23 h of serum starvation. One hour after replacement with Tyrode’s solution, the cells were treated with 50 nmol/l of IGF-1 or a vehicle for 15 min, and then lysates of the cells were prepared for immunoblotting.
mRNA quantification
Total RNA was isolated from myocardial tissues by using an RNeasy Fibrous Tissue Mini Kit (Qiagen, Valencia, CA, USA). First-strand cDNA was synthesized using a SuperScript VILO™ cDNA synthesis Kit (Life Technologies). DNA amplification was performed in StepOne™ (Life Technologies) by using Taqman Universal Master Mix (Applied Biosystems, Inc). The following Taqman probes (Applied Biosystems, Inc, Assay ID) were used: for rat PP2A Bα (Rn00696406_m1), PP2A Bβ (Rn00573573_m1), PP2A Bγ (Rn00589064_m1), and PP2A Bδ isoform (Rn00518189_m1). All assays were performed in duplicate and by the standard curve method using serial cDNA dilution.
Statistical analysis
All data are presented as mean ± SEM. Student’s t test was used for detecting statistical significance in group mean data between two treatment groups. The relationship between serum creatinine concentration and infarct size was examined by simple linear regression analysis. Those analyses were performed using JMP (version 11, SAS Institute, Cary, NC). Hemodynamic data were analyzed by two-way repeated measures ANOVA followed by the Student–Newman–Keuls post hoc test in SigmaStat software (Systat Software, San Jose, CA). A difference was considered to be statistically significant if the p value was less than 0.05.
Results
Infarct size experiments
Hemoglobin level was lower (13.2 ± 0.2 vs. 16.1 ± 0.4 g/dl) and serum creatinine level was higher (0.71 ± 0.03 vs. 0.36 ± 0.03 mg/dl) in the SNx group than in the Sham group (Table S1). Heart rates and blood pressure were similar throughout experiments in the Sham and SNx groups (Table S2). There was no significant difference between the two groups in mortality rates after 20-min coronary artery occlusion/2-h reperfusion (14.2% in the Sham group vs. 17.6% in the SNx group).
Infarct size as a percentage of area at risk (IS/AR) was significantly larger in the SNx group than in the Sham group (56.3 ± 4.6 vs. 41.4 ± 2.0%), while area-at-risk sizes were comparable (Fig. 1a, b; Table S3). As shown in Fig. 1c, IS/AR was weakly correlated with serum creatinine level (r = 0.47, p < 0.01).
Infarct size enlargement by CKD is mimicked by inhibition of Akt-Ser473 phosphorylation upon reperfusion. Representative stained heart slices (a) and infarct size expressed as a percentage of area at risk after ischemia/reperfusion (b) in the Sham and SNx groups. N = 12 in Sham and N = 14 in SNx. *p < 0.05 vs. Sham. Infarct size was correlated with serum creatinine levels before ischemia/reperfusion (c). Effects of an mTOR inhibitor, Ku-0063794, on reperfusion-induced phosphorylation of Akt-Ser473 and p70s6K at 5 min after reperfusion (d) and on infarct size at 2 h after reperfusion in the Sham group (e) and in the SNx group (f). N = 5–6 in each group. Myocardial samples for immunoblotting were excised from the area at risk. Ku = Ku-0063794. *p < 0.05 vs. Control
Because phosphorylation of myocardial Akt at Ser473 upon reperfusion was found to be attenuated in the SNx group (data below), we examined whether inhibition of the phosphorylation of Akt at Ser473 modifies infarct size. Administration of Ku-0063794, an mTORC1 and 2 inhibitor [39], 5 min before reperfusion suppressed phosphorylation of Akt-Ser473 and its downstream p70s6K and significantly increased IS/AR in the Sham group (Fig. 1d, e; Tables S4, S5). However, change in IS/AR by Ku-0063794 was not statistically significant in the SNx group (Fig. 1f; Tables S6, S7).
Modification of protective signaling by CKD
An ischemia/reperfusion protocol ex vivo was selected to examine alterations in protective signaling as in our previous studies [16, 40]. Protein levels of JAK2, ERK1/2, Akt, p70s6K, GSK-3β, PDK1, mTORC2 subunits, PHLPP1 and PTEN (Fig. 2a; Fig. S1) and levels of mTOR and Rictor in the Sin1 immunoprecipitates (Fig. S2) were comparable in the SNx and Sham groups.
Reperfusion-induced phosphorylation of Akt-Ser473 and its downstream kinases in the myocardium is attenuated in CKD. Representative blots for signal molecules relevant to Akt-mediated signaling (a) and summarized data for Akt phosphorylation (b) are shown. Vinculin served as a loading control. The level of each phosphorylated kinase is expressed as the ratio to its total kinase level. a.u. = arbitrary unit, Base = baseline, R = 5 min after reperfusion. N = 5–10 in each group. *p < 0.05 vs. Sham
The level of phosphorylation at Thr308 in Akt at baseline was significantly higher in the SNx group than in the Sham group, while Akt-Ser473 phosphorylation levels were similar in the two groups (Fig. 2a, b). However, reperfusion-induced phosphorylation of Akt-Ser473 was suppressed in the SNx group, while Thr308 phosphorylation levels were similar in the two groups. Significant suppression of Akt activity upon reperfusion in the SNx group was indicated also by attenuated phosphorylation of p70s6K and GSK-3β, two kinases downstream of Akt (Fig. 2a, b). Since mTORC2 and PDK1 is a kinase to phosphorylate Akt at Ser473 and Thr308, respectively, we examined whether mTORC2 or PDK1 activity is modulated by CKD. As shown in Fig. 3a, there was no significant difference in baseline mTORC2 activity between the Sham and SNx groups and mTORC2 activity was similarly increased after reperfusion in the two groups. PDK1 activity at baseline and that upon reperfusion were also similar in the Sham and SNx groups, while reperfusion did not significantly change PDK1 activity in both groups (Fig. 3b).
Myocardial mTORC2 and PDK1 activities are not modified by CKD. Representative blots and summarized data for mTORC2 activity (a) and PDK1 activity (b) are shown. Levels of phosphorylation of recombinant Akt at Ser473 and that at Thr308 were measured as indices of mTORC2 and PDK1 activities, respectively. a.u. = arbitrary unit, Base = baseline, R = 5 min after reperfusion. N = 3 in each group. *p < 0.05 vs. Base
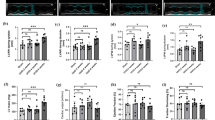
Since PDK1 activities were similar in the SNx and Sham groups, we examined alterations in a phosphatase specifically targeting Akt-Thr308, PP2A which has B55α as its B subunit [19]. There was no significant difference in protein levels of subunits A and C of PP2A between the two groups, but B55α level was significantly lower in the SNx group (Fig. 4a, b). The mRNA levels of B55α, β, γ and δ subunits were comparable in the SNx and Sham groups (Fig. S3).
Down-regulation of PP2A B55α expression by CKD and the effect of suppressed PP2A B55α expression on response of Akt-Ser473 phosphorylation in H9c2 cells. Representative blots for PP2A subunits in the myocardium (a) and summarized data for baseline PP2A (b) are shown. Vinculin served as a loading control. a.u. = arbitrary unit, Base = baseline, R = 5 min after reperfusion. N = 8 in each group. *p < 0.05 vs. Sham. Representative blots for PP2A B55α and Akt (c) and summarized data for Akt phosphorylation (d) in H9c2 cells transfected with control or PP2A B55α siRNA are shown. Data before and after treatment with 50 nmol/l IGF-1 are shown. Phosphorylated Akt levels are expressed as ratios to total Akt levels. N = 6 in each group. *p < 0.05 vs. Control
To confirm that down-regulation of PP2A B55α protein expression is causally related to up-regulated Thr308 phosphorylation in Akt in the cardiomyocyte, we examined the effect of knockdown of PP2A B55α protein expression in H9c2 cells. As shown in Fig. 4c, d, knockdown of PP2A B55α increased Akt-Thr308 phosphorylation without a significant effect on Akt-Ser473 phosphorylation.
Impact of Thr308 phosphorylation on response of Ser473 in Akt
Based on a report that Thr308 phosphorylation in Akt regulates conformation of Akt and its association with the cell membrane [1], we hypothesized that up-regulated phosphorylation of Akt-Thr308 blunts the response of Akt-Ser473 to upstream signals. To examine this hypothesis, we used two cell models of up-regulated Akt-Thr308 phosphorylation: H9c2 cells in which PP2A B55α was knocked down by siRNA and HEK293 cells transfected with a phospho-Thr308-mimetic mutant Akt (T308D). Phosphorylation of Akt-Ser473, GSK-3β and p70s6K by IGF-1 (50 nmol/l) was suppressed in B55α knocked-down H9c2 cells (Fig. 4c, d; Fig. S4). In experiments using HEK293 cells, the efficiency of transfection appeared to be lower in HA-tagged T308D-Akt than in HA-tagged wild-type Akt (Fig. 5a), and thus we compared their degree of phosphorylation in response to IGF-1 as a percentage of the baseline level. Ser473 phosphorylation by IGF-1 was suppressed by 30% in T308D compared with that in HA-tagged wild-type Akt (Fig. 5a, b). Phosphorylation of GSK-3β and p70s6K after IGF-1 treatment was also suppressed in T308D-transfected cells (Fig. 5a), indicating that the increase in Akt activity by IGF-1 was significantly blunted.
IGF-1-induced Akt activation is suppressed in a phospho-Thr308-mimetic Akt mutant. HEK293 cells were transfected with HA-AktWT plasmid (WT) and HA-AktThr308D (T308D). Phosphorylation of Akt-Ser473, GSK-3β and p70s6K after IGF-1 (50 nmol/l) treatment was suppressed in T308D-transfected cells compared with that in WT-transfected cells. a Representative blots. Vinculin served as a loading control. b Group mean data. N = 5 in each group. *p < 0.05 vs. Control. c A scheme of CKD-induced modification of protective signal pathways
Discussion
The mechanism by which CKD increases myocardial vulnerability to ischemia/reperfusion injury has been unclear. Involvement of hypertension per se in the increased myocardial vulnerability was excluded by the findings that blood pressure control by low salt diet or by pharmacological agents failed to reduce infarct size in CKD [8]. A recent study showed increased mitochondrial susceptibility to ischemia/reperfusion injury in CKD [36], but its relation to infarct size or to cytoprotective signals remains unclear. The present study focused on CKD-induced alterations in PI3K-Akt and mTOR-Akt-mediated pathways, two major cell survival signaling pathways [15, 23, 40], at baseline and at 5 min after reperfusion. We selected 5 min after reperfusion as a time point for the analysis for two reasons: opening of the mitochondrial permeability transition pore (mPTP) occurs within 5–10 min after reperfusion [14], and activation of PI3K-Akt-GSK-3β signaling at 5 min after reperfusion is closely associated with elevation of the threshold for mPTP opening and mPTP-mediated cell necrosis [17, 21, 23, 25]. We found that CKD suppressed phosphorylation of Akt at Ser473 and also its downstream targets, GSK-3β and p70s6K, at 5 min after reperfusion (Fig. 2). Selective inhibition of Ser473 phosphorylation in Akt by use of an mTORC inhibitor, Ku-0063794, mimicked the effect of CKD on infarct size in non-CKD rats (Fig. 1d, e). In addition, treatment with Ku-0063794 did not further increase infarct size in CKD rats (Fig. 1f). Taken together, the results indicate that insufficient activation of Akt upon reperfusion contributes to enlargement of infarct size by CKD.
Two phosphorylation sites in Akt for activation, Thr308 and Ser473, are regulated by distinct mechanisms [28]. Akt-Thr308 is phosphorylated by PI3K-PDK1 signaling and dephosphorylated by PP2A, while mTORC2 and PHLPP1 are responsible for phosphorylation and dephosphorylation, respectively, of Akt-Ser473. Although there was no CKD-induced change in protein levels of PDK1, mTORC2 subunits and PHLPP1 (Fig. 2a) or composition of mTORC2 (Fig. S2), Akt-Ser473 phosphorylation upon reperfusion was significantly suppressed in CKD (Fig. 2a, b). On the other hand, CKD did not modify the activity of mTORC2 or activity of PDK1 (Fig. 3). Interestingly, phosphorylation of Akt-Thr308 at baseline was up-regulated in the SNx group (Fig. 2), and phosphorylation of this residue in the activation loop of Akt has been shown to regulate conformational changes of Akt and its association with the membrane [1]. Thus, we hypothesized that up-regulated phosphorylation at Thr308 blunts Ser473 phosphorylation in Akt in response to upstream signaling. This hypothesis was supported by the findings that Ser473 phosphorylation after IGF-1 treatment was suppressed in H9c2 cells in which the level of Akt-Thr308 phosphorylation was elevated by knockdown of PP2A-B55α (Fig. 4c, d) and in HEK293 cells expressing a Thr308 constitutively active mutant (T308D) (Fig. 5a, b). A functional impact of the mutation in Thr308 and that of PP2A-B55α knockdown on Akt activity were confirmed by suppressed phosphorylation of Akt targets, GSK-3β and p70s6K (Fig. 5a, b, Fig. S4).
The molecular mechanism by which increased Thr308 phosphorylation in Akt attenuates the response of Akt-Ser473 to its upstream signaling remains unclear. A plausible explanation is promotion of Akt dissociation from the plasma membrane by Thr308 phosphorylation as reported for non-cardiac cells by Ananthanarayanan et al. [1]. However, recent studies [2, 4, 11] have shown that mTORC2 localizes not only in the plasma membrane but also in the outer membrane of mitochondria and endoplasmic reticulum membranes, and intracellular sites where Akt relevant to cardioprotection is phosphorylated by mTORC2 have not been identified. Nevertheless, the present results of in vitro experiments strongly support the notion that up-regulated phosphorylation of Thr308 in Akt is responsible for blunted Ser473 phosphorylation upon reperfusion in the myocardium of CKD rats.
This study showed for the first time that CKD down-regulates PP2A-B55α protein expression, leading to up-regulated Akt-Thr308 phosphorylation. B55α mRNA level was unchanged in the SNx group (Fig. S3), suggesting that CKD impairs translation or post-translational modification of B55α. In fact, CKD has been reported to enhance or suppress protein ubiquitination depending on types of proteins [6, 30]. However, immunoblotting for ubiquitin in immunoprecipitated B55α did not show change in ubiquitination of B55α by CKD (data not shown). The mechanism by which CKD reduces B55α protein expression may warrant further investigation.
Insufficient erythropoietin (EPO) production in the kidney underlies anemia associated with CKD. Since EPO has been shown to be a cardioprotective molecule, it might be speculated that reduction in circulating EPO level contributes to infarct size enlargement by CKD. However, this possibility was not supported by the results of a study [26] conducted in parallel with the present study. In the second protocol of that study, we determined serum EPO levels in the same rat CKD model and sham-operated rats as those in the present study. There was no significant difference between the serum EPO levels in the SNx and Sham groups (0.9 ± 0.3 vs. 0.5 ± 0.2 mIU/ml), while hemoglobin level was lower in the SNx group (13.8 ± 0.5 vs. 17.1 ± 0.4 g/dl, p < 0.05), indicating insufficient EPO production in response to anemia, a phenotype of renal anemia, in the SNx group [26]. Post hoc calculation of a correlation coefficient between infarct size as a percent of area at risk and serum EPO level in the SNx group (r = 0.437, p = 0.327) argued against role of circulating EPO in infarct size enlargement by CKD.
In the present study, we selected a 5/6-nephrectomized rat as a model of CKD for clarifying the mechanism by which CKD increases myocardial infarct size since this model consistently showed significantly increased vulnerability to ischemia/reperfusion injury in earlier studies [5, 8, 9]. The alterations in PI3K-PDK1-Akt and mTORC2-Akt signaling in CKD rats (Figs. 2, 3, 4) indicate that insufficient activation of Akt at the time of reperfusion underlies the infarct size enlargement by CKD in rats. However, the findings may not be directly extrapolated to other species because of species differences in roles of pro-survival kinases [15, 24, 34]. A study by Skyschally et al. [34] showed that phosphorylation of Akt at Ser473 was not associated with infarct size limitation by ischemic postconditioning in pigs. Unfortunately, to our knowledge, the impact of CKD on myocardial infarct size has not been examined in animal species other than rodents. Nevertheless, the findings in a rat model of CKD support the notion that CKD substantially modifies endogenous cytoprotective signaling in the myocardium.
CKD-induced alterations in renal and cardiovascular functions depend on etiologies and duration of CKD [7, 37]. Thus, although a rat with 5/6 nephrectomy is an established model of CKD [3, 8, 12, 35], impaired Akt-mediated signaling upon reperfusion shown by the present study is unlikely to be the only mechanism of increased myocardial susceptibility to ischemia/reperfusion in CKD. In fact, mitochondrial dysfunction [36] and down-regulated expression of the adiponectin receptor in the myocardium [35] were reported to be associated with increased myocardial injury by CKD. In our study conducted in parallel with this study [26], disturbed malate-aspartate shuttle in the myocardium in CKD was indicated by results of metabolome analysis. Relationships between mitochondrial dysfunction, impaired response of cytoprotective signaling, and duration and severity of renal dysfunction remain to be investigated.
In conclusion, CKD increases Akt-Thr308 phosphorylation via down-regulation of PP2A-B55α protein expression, leading to attenuated response of Akt-Ser473 to upstream signals (Fig. 5c). Impaired activation of Akt upon reperfusion by the CKD-induced modification of Akt response underlies the enlargement of infarct size in CKD.
References
Ananthanarayanan B, Fosbrink M, Rahdar M, Zhang J (2007) Live-cell molecular analysis of Akt activation reveals roles for activation loop phosphorylation. J Biol Chem 282:36634–36641. doi:10.1074/jbc.M706227200
Betz C, Stracka D, Prescianotto-Baschong C, Frieden M, Demaurex N, Hall MN (2013) mTOR complex 2-Akt signaling at mitochondria-associated endoplasmic reticulum membranes (MAM) regulates mitochondrial physiology. Proc Natl Acad Sci USA 10:12526–12534. doi:10.1073/pnas.1302455110
Bongartz LG, Joles JA, Verhaar MC, Cramer MJ, Goldschmeding R, Tilburgs C, Gaillard CA, Doevendans PA, Braam B (2012) Subtotal nephrectomy plus coronary ligation leads to more pronounced damage in both organs than either nephrectomy or coronary ligation. Am J Physiol Heart Circ Physiol 302:H845–H854
Boulbés DR, Shaiken T, dos Sarbassov D (2011) Endoplasmic reticulum is a main localization site of mTORC2. Biochem Biophys Res Commun 413:46–52. doi:10.1016/j.bbrc.2011.08.034
Byrne CJ, McCafferty K, Kieswich J, Harwood S, Andrikopoulos P, Raftery M, Thiemermann C, Yaqoob MM (2012) Ischemic conditioning protects the uremic heart in a rodent model of myocardial infarction. Circulation 125:1256–1265. doi:10.1161/CIRCULATIONAHA.111.055392
Chitalia VC, Shivanna S, Martorell J, Balcells M, Bosch I, Kolandaivelu K, Edelman ER (2013) Uremic serum and solutes increase post-vascular interventional thrombotic risk through altered stability of smooth muscle cell tissue factor. Circulation 127:365–376. doi:10.1161/CIRCULATIONAHA
Clark LE, Khan I (2010) Outcomes in CKD: what we know and what we need to know. Nephron Clin Pract 114:c95–c102. doi:10.1159/000254381
Dikow R, Kihm LP, Zeier M, Kapitza J, Törnig J, Amann K, Tiefenbacher C, Ritz E (2004) Increased infarct size in uremic rats: reduced ischemia tolerance? J Am Soc Nephrol 15:1530–1536. doi:10.1097/01.ASN.0000130154.42061.C6
Dikow R, Wasserhess C, Zimmerer K, Kihm LP, Schaier M, Schwenger V, Hardt S, Tiefenbacher C, Katus H, Zeier M, Gross LM (2009) Effect of insulin and glucose infusion on myocardial infarction size in uraemic rats. Basic Res Cardiol 104:571–579. doi:10.1007/s00395-009-0018-2
Di Lullo L, House A, Gorini A, Santoboni A, Russo D, Ronco C (2015) Chronic kidney disease and cardiovascular complications. Heart Fail Rev 20:259–272. doi:10.1007/s10741-014-9460-9
Ebner M, Sinkovics B, Szczygieł M, Ribeiro DW, Yudushkin I (2017) Localization of mTORC2 activity inside cells. J Cell Biol 216:343–353. doi:10.1083/jcb.201610060
Francis J, Weiss RM, Wei SG, Johnson AK, Felder RB (2001) Progression of heart failure after myocardial infarction in the rat. Am J Physiol Regul Integr Comp Physiol 281:R1734–R1745
Garibotto G, Bonanni A, Verzola D (2012) Effect of kidney failure and hemodialysis on protein and amino acid metabolism. Curr Opin Clin Nutr Metab Care 15:78–84. doi:10.1097/MCO.0b013e32834d9df6
Griffiths EJ, Halestrap AP (1995) Mitochondrial non-specific pores remain closed during cardiac ischaemia, but open upon reperfusion. Biochem J 307:93–98. doi:10.1042/bj3070093
Heusch G (2015) Molecular basis of cardioprotection: signal transduction in ischemic pre-, post-, and remote conditioning. Circ Res 116:674–699. doi:10.1161/CIRCRESAHA.116.305348
Hotta H, Miura T, Miki T, Togashi N, Maeda T, Kim SJ, Tanno M, Yano T, Kuno A, Itoh T, Satoh T, Terashima Y, Ishikawa S, Shimamoto K (2010) Angiotensin II type 1 receptor-mediated upregulation of calcineurin activity underlies impairment of cardioprotective signaling in diabetic hearts. Circ Res 106:129–132. doi:10.1161/CIRCRESAHA.109.205385
Juhaszova M, Zorov DB, Kim SH, Pepe S, Fu Q, Fishbein KW, Ziman BD, Wang S, Ytrehus K, Antos CL, Olson EN, Sollott SJ (2004) Glycogen synthase kinase-3β mediates convergence of protection signaling to inhibit the mitochondrial permeability transition pore. J Clin Invest 113:1535–1549. doi:10.1172/JCI19906
Koppe L, Pelletier CC, Alix PM, Kalbacher E, Fouque D, Soulage CO, Guebre-Egziabher F (2014) Insulin resistance in chronic kidney disease: new lessons from experimental models. Nephrol Dial Transplant 29:1666–1674. doi:10.1093/ndt/gft435
Kuo YC, Huang KY, Yang CH, Yang YS, Lee WY, Chiang CW (2008) Regulation of phosphorylation of Thr-308 of Akt, cell proliferation, and survival by the B55alpha regulatory subunit targeting of the protein phosphatase 2A holoenzyme to Akt. J Biol Chem 283:1882–1892. doi:10.1074/jbc.M709585200
Langston RD, Presley R, Flanders WD, McClellan WM (2003) Renal insufficiency and anemia are independent risk factors for death among patients with acute myocardial infarction. Kidney Int 64:1398–1405. doi:10.1046/j.1523-1755.2003.00200.x
Miki T, Miura T, Hotta H, Tanno M, Yano T, Sato T, Terashima Y, Takada A, Ishikawa S, Shimamoto K (2009) Endoplasmic reticulum stress in diabetic hearts abolishes erythropoietin-induced myocardial protection by impairment of phospho-glycogen synthase kinase-3beta-mediated suppression of mitochondrial permeability transition. Diabetes 58:2863–2872. doi:10.2337/db09-0158
Miki T, Miura T, Yano T, Takahashi A, Sakamoto J, Tanno M, Kobayashi H, Ikeda Y, Nishihara M, Naitoh K, Ohori K, Shimamoto K (2006) Alteration in erythropoietin-induced cardioprotective signaling by postinfarct ventricular remodeling. J Pharmacol Exp Ther 317:68–75. doi:10.1124/jpet.105.095745
Miura T, Tanno M (2012) The mPTP and its regulatory proteins: final common targets of signalling pathways for protection against necrosis. Cardiovasc Res 94:181–189. doi:10.1093/cvr/cvr302
Murphy E, Steenbergen C (2008) Does inhibition of glycogen synthase kinase protect in mice? Circ Res 103:226–228. doi:10.1161/CIRCRESAHA.108.181602
Nishihara M, Miura T, Miki T, Sakamoto J, Tanno M, Kobayashi H, Ikeda Y, Ohori K, Takahashi A, Shimamoto K (2006) Erythropoietin affords additional cardioprotection to preconditioned hearts by enhanced phosphorylation of glycogen synthase kinase-3 beta. Am J Physiol Heart Circ Physiol 291:H748–H755. doi:10.1152/ajpheart.00837.2005
Nishizawa K, Yano T, Tanno M, Miki T, Kuno A, Tobisawa T, Ogasawara M, Muratsubaki S, Ohno K, Ishikawa S, Miura T (2016) Chronic treatment with an erythropoietin receptor ligand prevents chronic kidney disease-induced enlargement of myocardial infarct size. Hypertension 68:697–706. doi:10.1161/HYPERTENSIONAHA.116.07480
Ohori K, Miura T, Tanno M, Miki T, Sato T, Ishikawa S, Horio Y, Shimamoto K (2008) Ser9 phosphorylation of mitochondrial GSK-3beta is a primary mechanism of cardiomyocyte protection by erythropoietin against oxidant-induced apoptosis. Am J Physiol Heart Circ Physiol 295:H2079–H2086. doi:10.1152/ajpheart.00092.2008
Risso G, Blaustein M, Pozzi B, Mammi P, Srebrow A (2015) Akt/PKB: one kinase, many modifications. Biochem J 468:203–214. doi:10.1042/BJ20150041
Rodrigues FB, Bruetto RG, Torres US, Otaviano AP, Zanetta DM, Burdmann EA (2010) Effect of kidney disease on acute coronary syndrome. Clin J Am Soc Nephrol 5:1530–1536. doi:10.2215/CJN.01260210
Ryu ES, Kim MJ, Shin HS, Jang YH, Choi HS, Jo I, Johnson RJ, Kang DH (2013) Uric acid-induced phenotypic transition of renal tubular cells as a novel mechanism of chronic kidney disease. Am J Physiol Renal Physiol 304:F471–F480. doi:10.1152/ajprenal.00560
Sciarretta S, Volpe M, Sadoshima J (2014) Mammalian target of rapamycin signaling in cardiac physiology and disease. Circ Res 114:549–564. doi:10.1161/CIRCRESAHA.114.302022
Semple DJ, Bhandari S, Seymour AM (2012) Uremic cardiomyopathy is characterized by loss of the cardioprotective effects of insulin. Am J Physiol Renal Physiol 303:F1275–F1286. doi:10.1152/ajprenal.00048.2012
Semple D, Smith K, Bhandari S, Seymour AM (2011) Uremic cardiomyopathy and insulin resistance: a critical role for akt? J Am Soc Nephrol 22:207–215. doi:10.1681/ASN.2009090900
Skyschally A, van Caster P, Boengler K, Gres P, Musiolik J, Schilawa D, Schulz R, Heusch G (2009) Ischemic postconditioning in pigs: no causal role for RISK activation. Circ Res 104:15–18. doi:10.1161/CIRCRESAHA.108.186429
Song Y, Yu Q, Zhang J, Huang W, Liu Y, Pei H, Liu J, Sun L, Yang L, Li C, Li Y, Zhang F, Qu Y, Tao L (2014) Increased myocardial ischemia-reperfusion injury in renal failure involves cardiac adiponectin signal deficiency. Am J Physiol Endocrinol Metab 306:E1055–E1064. doi:10.1152/ajpendo.00428.2013
Taylor D, Bhandari S, Seymour AM (2015) Mitochondrial dysfunction in uremic cardiomyopathy. Am J Physiol Renal Physiol 308:F579–F587. doi:10.1152/ajprenal.00442.2014
Virzì GM, Clementi A, Ronco C (2016) Cellular apoptosis in the cardiorenal axis. Heart Fail Rev 21:177–189. doi:10.1007/s10741-016-9534-y
Wright RS, Reeder GS, Herzog CA, Albright RC, Williams BA, Dvorak DL, Miller WL, Murphy JG, Kopecky SL, Jaffe AS (2002) Acute myocardial infarction and renal dysfunction: a high-risk combination. Ann Intern Med 37:563–570. doi:10.7326/0003-4819-137-7-200210010-00
Yano T, Ferlito M, Aponte A, Kuno A, Miura T, Murphy E, Steenbergen C (2014) Pivotal role of mTORC2 and involvement of ribosomal protein S6 in cardioprotective signaling. Circ Res 114:1268–1280. doi:10.1161/CIRCRESAHA.114.303562
Yano T, Miki T, Tanno M, Kuno A, Itoh T, Takada A, Sato T, Kouzu H, Shimamoto K, Miura T (2011) Hypertensive hypertrophied myocardium is vulnerable to infarction and refractory to erythropoietin-induced protection. Hypertension 57:110–115. doi:10.1161/HYPERTENSIONAHA.110.158469
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
The present study was supported by Grant-in-aid for Scientific Research (#2646113 and #16K09505) from the Japan Society for the Promotion of Science, Tokyo, Japan and by Grant for Research and Education 2015 from Sapporo Medical University, Sapporo, Japan.
Conflict of interest
The authors declare that they have no competing interests.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tobisawa, T., Yano, T., Tanno, M. et al. Insufficient activation of Akt upon reperfusion because of its novel modification by reduced PP2A-B55α contributes to enlargement of infarct size by chronic kidney disease. Basic Res Cardiol 112, 31 (2017). https://doi.org/10.1007/s00395-017-0621-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00395-017-0621-6