Abstract
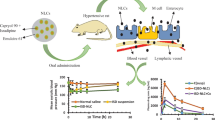
The incidence of pulmonary arterial hypertension (PAH) has significantly increased in the past few decades and therefore requires immediate attention. The applications of drug-loaded nano-systems have shown considerable improvements in controlling PAH compared to plain drugs. The purpose of this current investigation was to prepare and characterize sildenafil-encapsulated polyethylene glycol (PEGylated) liposomes for effective treatment of pulmonary arterial hypertension. Liposomes were prepared using thin film hydration method by varying the concentrations of sildenafil, Phospholipon 90-G, cholesterol, mPEG-DSPE2000 to optimize the formulation. The optimized liposomal formulation had mean hydrodynamic diameter, polydispersity index (PDI), zeta potential (ZP) and %EE of 155.3 ± 3.2 nm, 0.19 ± 0.1, − 42.2 ± 0.3 mV and 75.89 ± 0.5%. Transmission electron microscopy (TEM) revealed that liposomes were spherical and homogenously dispersed. FTIR (Fourier transform infrared spectroscopy) and DSC (Differential scanning calorimetry) confirmed that there was no covalent interaction between the drug and excipients. The release of sildenafil from PEGylated liposomes was found to be sustained compared to free drug. Ex vivo study in the rats showed improved vasorelaxant response for sildenafil loaded liposomes (132. 7 ± 0.7%) compared to pure sildenafil (108.2 ± 0.06%) and marketed Revatio® (113.2 ± 0.8%). In summary, sildenafil loaded PEGylated liposomes produced an impressive vasorelaxant response in rat aortic stip assay and require validation to bring the formulation available for clinical studies in the management of PAH.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Pulmonary arterial hypertension has significantly increased in the past few decades. PAH is an aberrantly progressive disease characterized by complex pulmo-circulatory altered conditions with elevated arterial blood flow and vascular resistance [1, 2]. The prevalence of PAH is estimated to be 15–50 cases per million individuals and is responsible for approximately 15% of deaths every year worldwide [3]. Furthermore, the rare idiopathic PAH has an incidence of seven cases per million [4]. The National Institutes of Health(NIH) Registry offers crucial insights into the evolving epidemiology of PAH as they have provided baseline characteristics and outcome data on > 10,000 patients with pulmonary arterial hypertension [5]. Specific management and prognosis exist for every class of pulmonary hypertension, which requires an appropriate diagnosis. Over the past 30 years, patient’s haemodynamic, clinical and demographic characteristics were the crucial dependent parameters in PAH registries. For incidence, in 1980s NIH registry reported that PAH was typically diagnosed in young adults. However, according to recent registry data, old individuals have also been diagnosed with PAH [6]. These figures are devastating and require exhaustive efforts to control and manage PAH more effectively.
Although the current PAH therapy has shown improvements in controlling PAH, drugs that are used to treat PAH suffer from various limitations, such as lack of specificity to lungs, short half-lives, drug instability and unwanted side effects [7]. Over the past decade, nano-systems loaded with antihypertensive drugs have shown significant progress in managing PAH by overcoming several limitations associated with PAH therapy [7]. Furthermore, these nano-systems have displayed improved results compared to free drugs. For example, fasudil loaded liposomes developed by Nahar et al. showed enhanced site-specific vasodilation compared to free fasudil [8]. In another study by Chen et al., pitavastatin loaded PLGA nanoparticles were found to be more potent than free drugs in attenuating the development of PAH in the rat model [9]. Therefore, nanotherapeutics can prove to be an effective approach to control PAH.
Sildenafil, an USFDA-approved drug is frequently used to control and manage PAH. Sildenafil has been loaded into various nano-systems such as polymeric nanoparticles, solid lipid nanoparticles and liposomes to treat PAH. These nano-systems have been proven to be more effective compared to free sildenafil in managing PAH [7]. Sildenafil citrate gets rapidly absorbed and shows its effect within 30 min to 1 h with a plasma half-life of about 4 h, and it is well tolerated in dosage range studied with no significant effects on heart rate and blood pressure. To the best of our knowledge, PEGylated liposomes loaded with sildenafil have not been explored for the management of PAH. PEGylation of liposomes offers several advantages over bare liposomes, such as longer circulation thus enabling a sustained release of payloads, reduced proteolysis and excretion, improved stability, etc. [10]. Recently, Nahar et al. demonstrated the sustained release of fasudil from PEGylated liposomes with improved anti-PAH activity in contrast to bare drugs [8]. Therefore, PEGylated liposomes encapsulated with sildenafil may prove to be an effective approach in the management of PAH.
In this study, novel PEGylated liposomes loaded with sildenafil were explored for the effective management PAH. This paper reports for the first time, on the delivery of sildenafil using PEGylated liposomes. Sildenafil loaded PEGylated liposomal formulation was optimized for particulate properties and % encapsulation efficiency. Further, the optimized formulation was studied for sustained drug release and ex vivo hypertension assays. The promising results obtained from this study could contribute to solve the current global crisis of pulmonary arterial hypertension.
Materials and methods
Sildenafil citrate was purchased from Cadila Pharmaceutical, Ahmedabad, India. Phospholipon 90-G and MPEG-DSPE2000 were provided as gift samples from Lipoid, Germany. Cholesterol was procured from Sigma-Aldrich, USA. All other ingredients used in the experiment are of analytical grade. Throughout the study, HPLC grade water was used.
Preparation of PEGylated liposome
Sildenafil loaded PEGylated liposomes were prepared using a conventional thin film hydration method [11]. Briefly, the known amount of drug was weighed and mixed with a different molar ratio of lipids (Phospholipon 90-G, Cholesterol, MPEG-DSPE2000). Several formulations were prepared by varying the concentrations of lipids (different molar ratio of Phospholipon 90-G, Cholesterol and MPEG-DSPE2000), while keeping the amount of sildenafil (10 mg) as constant. To prepare an optimized formulation, briefly, a known amount of drug along with 180 mg, 10 mg and 25 mg of Phospholipon 90-G, Cholesterol and MPEG-DSPE2000, respectively, were dissolved in 5 mL of chloroform in a round bottom flask (RBF). The solvent was evaporated in vacuo at 50 °C using a rotary evaporator to form a thin film. The RBF with thin film was placed in a desiccator for 12 h to remove residual traces of chloroform. Thus, resulted dry film was hydrated with 5 mL of phosphate buffer saline pH 7.4 (PBS) along with tween 80 in the rotary evaporator by rotating the flask at 100 rpm at a maintained temperature of 40 °C until the lipid film got completely hydrated to form liposomal dispersion. The liposomal dispersion was then probe sonicated for 10 min (two cycles) at 30% amplitude to reduce the particle size. Liposomes thus formed were stored in the refrigerator for 2 h at 4 °C. The liposomal suspension was further centrifuged at 1000 rpm to remove the un-encapsulated sildenafil. The supernatant was replaced by the addition of the phosphate buffer saline (pH 7.4). Liposomal pellets were separated and washed with PBS and re-suspended into the deionized water containing 50 mg/mL trehalose (cryoprotectant) before lyophilization. Further, the frozen sample of the PEGylated liposomes was lyophilized (“Labconco lyophilizer”) and then the dry sample was collected and stored in vials for further characterization [11, 12].
Determination of particle size, polydispersity index (PDI) and zeta potential (ZP)
The prepared sildenafil loaded PEGylated liposomes were characterized for particle size, PDI and ZP (n = 3) using Malvern Zeta-Sizer, UK. The relative size of liposomes was defined by average particle size, while particle homogeneity was revealed by narrow PDI, which predicts the stability of the formulation and also determines the particle size distribution. Zeta potential is defined as the particle overall charge in a particular medium. Particles with zeta potential above ( +) (−) 30 mV are generally considered to have good stability. In order to determine size, PDI and ZP, the liposomal suspension was diluted (1 in 10 mL) with PBS. All measurements for particle size, PDI and ZP were recorded in triplicate and expressed in mean ± SD.
Encapsulation efficiency (% EE) and loading capacity (LC)
Encapsulation efficiency helps to determine the amount of drug entrapped within liposomes. Briefly, a known amount of the liposomal formulation was placed in an Eppendorf tube and centrifuged using a cooling centrifuge at 14,000 rpm for 15 min at 4 °C. The procedure was repeated multiple times to obtain a clear supernatant. Further, the concentration of unentrapped drug was determined using UV-spectrophotometry(Shimadzu 1800) at a wavelength of 225 nm [13, 14]. The amount of sildenafil entrapped in PEGylated liposomes and loading capacity were determined using the following equations.
Surface morphology
Transmission electron microscopy (TEM, Jeol, JEM-1010, Japan) was used to study the surface morphology of sildenafil loaded PEGylated liposomes. The liposomal formulation was diluted appropriately with PBS, and a drop of it was placed on a copper grid. The excess aqueous solution was removed by blotting with filter paper and allowed to dry. Further, the sample was negatively stained using 2%w/v phosphotungstic acid. After drying, the liposomal sample was viewed at various magnifications [15].
Attenuated total reflection (ATR)-Fourier transform infrared spectroscopy (FTIR)
FTIR spectra of PEGylated liposomes loaded with sildenafil, pure sildenafil, MPEG-DSPE2000, cholesterol and Phospholipon 90-G were obtained to investigate any possible interaction or structural changes that occurred between drug and excipients in the drug-loaded formulation. The study was performed with the help of ATR-FTIR (Bruker EQUINOX 55 FTIR Spectrophotometer) using a detector known as nitrogen cooled MCT (Mercury Cadmium Telluride Detector) at a resolution of 2 cm−1 and diamond as internal reflection element, which was set at 45° of incidence angle. IR spectra of PEGylated liposomes loaded with sildenafil, pure sildenafil, MPEG-DSPE2000, cholesterol and Phospholipon 90-G were obtained and all spectra were scanned between 4000 to 400 cm−1. Peak fitting was done with the help of opus software [16, 17].
Raman spectroscopy analysis
The samples were scanned through Raman spectrophotometric system (Thermo-scientific instrument, DxRxi, equipped with the software “OMINICxi-Analysis”). Raman spectroscopy helps to provide information on rotational, vibrational and various other frequency modes in the system. A laser beam of 532 nm along with a laser power of 5-100mW was used to scan the drug (Sildenafil), Phospholipon 90-G, Cholesterol, MPEG-DSPE2000. The spectra were taken in the range of 125–4000 cm−1 [18].
Differential scanning calorimetry (DSC) analysis
DSC (DSC-204F1Phoenix) was employed to study the thermal behaviors of pure sildenafil, MPEG-DSPE2000, cholesterol, Phospholipon 90-G and lyophilized sildenafil loaded PEGylated liposomes (SPL-3). The samples were placed in a pan separately and sealed with an aluminum lid using a hydraulic press. Further, the sample filled pans were heated to 350 °C at a constant rate (5 °C/min) under constant nitrogen flow (30 mL/min). Indium was placed on another aluminum pan, and was used as a reference. The graph was recorded and plotted with temperature on X-axis against heat flow on Y-axis [19].
Determination of drug release through in vitro study
The in-vitro release of sildenafil was performed using Franz-diffusion cell in PBS 7.4 at 37 °C. Cellulose acetate membrane acting as a semi-permeable membrane was soaked in PBS 7.4 for 24 h prior to use so that it can attach to the donor compartment. Briefly, sildenafil loaded liposomal formulation (containing 5 mg of sildenafil) and free sildenafil 5 mg were added in the donor compartment. The donor compartment was clamped and dipped in the receptor compartment containing 100 mL of PBS 7.4 and maintained at 37 °C. The assembly was placed on a magnetic stirrer for continuous stirring at 500 rpm. At specific time intervals, i.e., in every 1 h, 2 mL of the sample was withdrawn from the receptor compartment and was replaced with an equal volume of PBS 7.4 (2 mL) to maintain a constant buffer solution volume. The withdrawn samples were spectrophotometrically analyzed using UV spectrophotometer at 225 nm and % cumulative drug release (CDR) was determined and against time [20, 21].
Ex vivo study (rat aortic strip assay)
Male adult Wistar rats weighing 220–250 gm were used for the ex vivo antihypertensive study. The experimental procedures were carried out with the prior permission of institutional animal ethics committee (protocol number BV/3535/2017–2018), and entire procedures were implemented in accordance with CPCSEA guidelines.
In the ex vivo study, rat thoracic aortic strip was used to examine the vaso-relaxant property of optimized formulation. Briefly, aortic strips (4 mm) were isolated from anesthetized rats and incubated in Krebs–Henseleit solution at optimal conditions including pH (7.4), temperature and constant oxygenation (O2/CO2, 19:1). The strip was fixed in the bath with the help of sterile stainless-steel pins, which were placed through the lumen of each arterial segment, i.e., one pin was devoted toward force–displacement transducer and other to the bottom of the chamber. The aortic ring was allowed to get stabilized for 2 h at maintained optimal tension of 2 g. Potassium chloride (60 mM) was used to contract aortic rings and achieve submaximal tension. After obtaining a submaximal response, the aortic rings were exposed to cumulative doses (10–6 to 10–2 M) of sildenafil and the % vaso-relaxation was recorded. Further, vasorelaxant responses of Revatio® and SPL-3 were also recorded and compared [22].
Statistical analysis
The vasorelaxant data are presented in mean ± standard deviation (S.D.) from at least three vascular rings from different rats. The response curves were expressed as % relaxation of the KCl precontracted rings and constructed using two-way ANOVA followed by Dunnett test using Graph pad Prism (version 8.0), where applicable. p < 0.05 was considered statistically significant.
Results and discussion
Preparation of PEGylated liposome
Sildenafil loaded PEGylated liposomes were prepared using a simple thin film hydration technique. To optimize the formulation in terms of particle size, PDI, ZP and % EE, several sildenafil loaded PEGylated liposomes formulations (six) were prepared by varying the concentrations of excipients, and were named serially asSPL-1 to SPL-6 (Table 1). A weight ratio of 1:19:2.5 of drug:lipid:mPEG-DSPE2000 displayed satisfactory results with respect to size, PDI, ZP and % EE. The optimized SPL-3 had a mean hydrodynamic size of 155 ± 3.2 nm with a narrow size distribution of 0.186 ± 0.05 and a negative surface charge of −42.2 ± 0.3 (Table 1). The % EE and % LC of SPL-3 were found to be 75.89 ± 0.5% and 3.34 ± 0.8% (Table 1). Since SPL-3 displayed better results in terms of particle size and encapsulation efficiency compared to other liposomal formulations, it was therefore considered as the optimized formulation to perform other studies.
Surface morphology
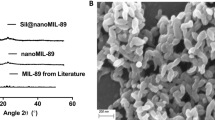
TEM was used to study the surface morphology of optimized formulation, i.e., SPL-3 (Fig. 1). From the images, sildenafil loaded PEGylated liposomes were found to have spherical shape, slightly rough surface and devoid of the crystalline structure of the drug. The image also indicated the presence of multi-lamellar vesicles in homogeneous population, which in turn suggested that encapsulation of sildenafil in PEGylated liposomes did not affect the surface morphology of the vesicles.
ATR-FTIR spectra
FTIR spectra of sildenafil citrate, optimized liposomal formulation SPL-3 and various polymers like cholesterol, Phospholipon 90-G, MPEG-DSPE2000 are shown in Fig. S1a. Pure drug showed a major characteristic peak at 1568.46 cm−1 (C=N stretching), 1456 cm−1, 1167.44 cm−1 (presence of various multiple bonds and aromatic ring), 1079.78 cm−1 (C–N stretching), 932.85 cm−1 (presence of alkenes), 805.43 cm−1 (meta-distribution of aromatic proton), 732.90 cm−1 (C–H stretching), 688.85 cm−1 and at 655.29 cm−1. The physical mixture shows peak at 3744.25 cm−1, 3390.15 cm−1, 2923.97 cm−1, 2853.99 cm−1, 1733.30 cm−1, 1556.28 cm−1, 1455.98 cm−1, 1368.34 cm−1, 1169.34 cm−1, 1050.66 cm−1, 728.98 cm−1. Optimized formulation was also scanned in same region and peak was found close to the peak of pure drug i.e. at 1459.03 cm−1, 1352.00 cm−1, 1243.67 cm−1, 1086.52 cm−1, 946.94 cm−1, 842.67 cm−1, 716.90 cm−1. From the overlay, it has been observed that there was no drug-polymer interaction because FTIR spectra of polymer formulation SPL-3 exhibited all the characteristics peaks as that of a pure drug observed.
Raman spectroscopy
Raman spectroscopy depends on the molecule electric polarizability and provides information of functional group present in the molecule. Pure drug sildenafil showed major characteristic peak at 1560 cm−1 (C=N stretching), 1410 cm−1, 1262 cm−1 (presence of aromatic ring) and 770 cm−1 (C–H stretching) whereas optimized formulation showed characteristics peak at 2870 cm−1, 1665 cm−1, 1480 cm−1 and 760 cm−1. It was observed that the peak of optimized formulation SPL-3 was overlapping with the peak of drug, which indicates the presence of sildenafil in the PEGylated liposome. Results of Raman study are depicted in Fig. S1b.
Differential scanning calorimetry (DSC) analysis
DSC was performed to confirm the encapsulation of sildenafil in PEGylated liposomes. The thermal transition or thermal behaviors of pure sildenafil, DSPE-mPEG2000, phospholipon-90G, cholesterol and optimized sildenafil loaded PEGylatedliposomal formulation (SPL-3) were studied (Fig. 2). Pure sildenafil showed a sharp endothermic peak at 212.06 °C corresponding to its thermal decomposition. Two sharp endothermic peaks were observed for mPEG-DSPE2000and cholesterol at 61.27 °C and 143.24 °C, respectively, whereas, the thermogram for lyophilized SPL-3 did not show any thermal peaks for either sildenafil or other excipients. This disappearance of peak for sildenafil suggested that the drug was encapsulated into the PEGylated liposomes in non-crystalline form.
In vitro drug release
The in vitro release profiles of free sildenafil and optimized sildenafil loaded PEGylated liposomes (SPL-3) in PBS 7.4 are depicted in Fig. 3. The percentage cumulative release for free sildenafil and sildenafil from PEGylated liposomes at 12 h was 90% and 27%, respectively, displaying ~ 60% of the difference in the release pattern. At the end of 24 h, almost 100% of free sildenafil was released, whereas, at the same time period, PEGylated liposomes released 33% of drug, thus, displaying sustained drug-releasing behavior. Through the process of diffusion, drug releases from the liposomes and enters in the systemic circulation. The sustained release can be attributed to the high % EE achieved for sildenafil in the PEGylated liposomes and slow erosion and degradation of mPEG-DSPE2000 and Phospholipon 90-G. From these observations, it was evident that, PEGylated liposomes were able to release the encapsulated sildenafil in a sustained manner, compared to free drug. This slower release of drug from PEGylated liposomes could prove to be beneficial as it can provide sustained anti-hypertensive effects with reduced frequency of administration.
Ex vivo antihypertensive study
Rat aortic strip assay
The cumulative addition of SPL-3 formulation (10–6–10–2 M) produced significant concentration-dependent vasorelaxant responses (p < 0.001) as shown in Table 2 and Fig. 4. The SPL-3 showed maximal relaxant effect of 132.7 ± 0.7% at the concentration of 10–2 nM when compared to sildenafil (108.2 ± 0.06%) and Revatio® (113.2 ± 0.8%), respectively. Medina et al. reported significant relaxation by sildenafil in a forearm vein, radial artery, and human internal mammary artery. However, at the highest concentration, sildenafil was known to have modest relaxant effect only in the coronary artery. Our results also showed that high concentrations of sildenafil cause a significant relaxant effect on rat aortic strip. Increased cGMP levels are assumed to be the reason for sildenafil to produce a vasorelaxant effect within the vessel wall. PDE inhibitors decrease the level of intracellular calcium, activate protein kinases to elicit vasodilation and elevate cGMP. Similarly, the concentration-dependent relaxation in KCl contracted strips by SPL-3 may be due to their potential as PDE inhibition [23].
Conclusions
Sildenafil loaded PEGylated liposomes were prepared using the thin film hydration method. The drug-loaded liposomes showed high encapsulation efficiency and sustained drug release for sildenafil. Ex vivo studies suggested that optimized formulation, SPL-3 was more efficient than free sildenafil and Revatio® in causing vasorelaxation. Therefore, PEGylated liposomes could provide sustained and enhanced delivery of sildenafil with improved bioavailability, better patient compliance, reduced dosage frequency and enhanced efficacy at low doses with minimal side effects. Further studies are required to confirm their efficacy in varied physiological and pathological conditions in rodents and further in clinical volunteers.
References
Galiè N et al (2015) Initial use of ambrisentan plus tadalafil in pulmonary arterial hypertension. N Engl J Med 373(9):834–844
Licarete E, Sesarman A, Banciu M (2015) Exploitation of pleiotropic actions of statins by using tumour-targeted delivery systems. J Microencapsul 32:619–631
Thenappan T et al (2007) A USA-based registry for pulmonary arterial hypertension: 1982–2006. Eur Respir J 30(6):1103–1110
Chin KM et al (2018) psychometric validation of the pulmonary arterial hypertension-symptoms and impact (PAH-SYMPACT) questionnaire: results of the SYMPHONY trial. Chest 154(4):848–861
Lau EM et al (2017) Epidemiology and treatment of pulmonary arterial hypertension. Nat Rev Cardiol 14(10):603
Pramanik N et al (2019) Polyhydroxybutyrate-co-hydroxyvalerate copolymer modified graphite oxide based 3D scaffold for tissue engineering application. Mater Sci Eng C 94:534–546
Segura-Ibarra V et al (2018) Nanotherapeutics for treatment of pulmonary arterial hypertension. Front Physiol 9:890
Nahar K et al (2014) Peptide-coated liposomal fasudil enhances site specific vasodilation in pulmonary arterial hypertension. Mol Pharm 11(12):4374–4384
Chen L et al (2011) Nanoparticle-mediated delivery of pitavastatin into lungs ameliorates the development and induces regression of monocrotaline-induced pulmonary artery hypertension. Hypertension 57(2):343–350
Rafati N, Caldera F, Trotta F, Ghias N (2019) Pyromellitic dianhydride crosslinked cyclodextrin nanosponges for curcumin controlled release; formulation, physicochemical characterization and cytotoxicity investigations. J Microencapsul. https://doi.org/10.1080/02652048.2019.1669728
Shavi GV et al (2016) PEGylated liposomes of anastrozole for long-term treatment of breast cancer: in vitro and in vivo evaluation. J Liposome Res 26(1):28–46
Klibanov AL et al (1990) Amphipathic polyethyleneglycols effectively prolong the circulation time of liposomes. FEBS Lett 268(1):235–237
Musteata FM, Pawliszyn J (2006) Determination of free concentration of paclitaxel in liposome formulations. J Pharm Pharm Sci 9:231–237
Sudhakar B, Krishna MC, Murthy KVR (2016) Factorial design studies of antiretroviral drug-loaded stealth liposomal injectable: PEGylation, lyophilization and pharmacokinetic studies. Appl Nanosci 6(1):43–60
Yang X et al (2009) A novel liposomal formulation of flavopiridol. Int J Pharm 365(1–2):170–174
Dave V et al (2017) Hybrid nanoparticles for the topical delivery of norfloxacin for the effective treatment of bacterial infection produced after burn. J Microencapsul 34(4):351–365
Shah SP, Misra A (2004) Liposomal amikacin dry powder inhaler: effect of fines on in vitro performance. AAPS PharmSciTech 5(4):107–113
Lum W et al (2017) Novel liposome-based surface-enhanced raman spectroscopy (SERS) substrate. J Phys Chem Lett 8(12):2639–2646
Biltonen RL, Lichtenberg D (1993) The use of differential scanning calorimetry as a tool to characterize liposome preparations. Chem Phys Lipid 64(1–3):129–142
Dave V et al (2017) Herbal liposome for the topical delivery of ketoconazole for the effective treatment of seborrheic dermatitis. Appl Nanosci 7(8):973–987
Korsmeyer RW et al (1983) Mechanisms of solute release from porous hydrophilic polymers. Int J Pharm 15(1):25–35
Tripathi N et al (2018) Discovery of novel soluble epoxide hydrolase inhibitors as potent vasodilators. Sci Rep 8(1):1–11
Mojzych M et al (2016) Relaxant effects of selected sildenafil analogues in the rat aorta. J Enzyme Inhib Med Chem 31(3):381–388
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors report no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Paliwal, S., Sharma, J., Dave, V. et al. Novel biocompatible polymer-modified liposome nanoparticles for biomedical applications. Polym. Bull. 81, 535–547 (2024). https://doi.org/10.1007/s00289-023-04731-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00289-023-04731-7