Abstract
Taxanes are an established option in the standard treatment paradigm for patients with metastatic breast cancer (MBC). Neuropathy is a common, dose-limiting side effect of taxane therapy that is often managed by dose reductions and delays. The severity, time to onset, and improvement in neuropathy are important considerations for patient management and vary among currently approved taxanes. The rate of grade ≥3 neuropathy with taxanes has been shown to be dose and schedule dependent; however, time to improvement to grade ≤1 is typically shorter for nab-paclitaxel than for other taxanes in patients with MBC. Many tools for assessing patient-reported neuropathy exist. Because MBC is incurable and patient quality of life must be critically considered when making treatment decisions, there is a need for more prospective trials to assess patient-reported neuropathy. Validated predictors of taxane-related neuropathy may play an important role in treatment decisions in the future. This review will focus on the toxicity profile (i.e., neuropathy) of each of the taxanes used in the treatment of MBC, will provide updates on tools used for the assessment of neuropathy, and will highlight newly discovered predictors of taxane-related neuropathy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Overview of taxane-related neuropathy
The National Comprehensive Cancer Network Guidelines recommend taxanes for the treatment of early-stage and metastatic breast cancer (MBC) [1]. Over the past several decades, the efficacy and safety profiles of taxanes—including paclitaxel (Taxol; Bristol-Myers Squibb), docetaxel (Taxotere; sanofi-aventis), and nab-paclitaxel (Abraxane; Celgene Corporation)—have been well established in MBC [2–4]. Neuropathy, a common side effect of taxane therapy, is a significant challenge for clinicians and patients. Taxane-associated neuropathy can compromise dose delivery and result in dose delays, reductions, or discontinuations that ultimately adversely affect treatment outcomes [5]. Some patients experience painful and persistent taxane-associated neuropathy that affects their activities of daily living and overall quality of life [6].
Taxane-associated peripheral neuropathies generally comprise sensory or motor neuropathy, depending on the type of nerve fibers involved [7]. The mechanism of taxane-induced neuropathy has been reported in numerous reviews [8–10]; thus, this review will not go into great detail regarding this topic. Briefly, neurons rely on transport and communication spanning the distance between the cell body and axons. These processes depend on intact and functional cytoskeletal microtubules. The binding of taxanes to the β-tubulin subunit of microtubules results in stabilization of the microtubule and disruption of microtubule function [11]. It is believed that the inhibition of microtubule function affects the structure and function of neurons, resulting in clinically apparent neuropathy [10]. The degree of neuronal damage depends on several factors, such as agent, cumulative dose, and duration of therapy [6]. Because of their extended axon length, peripheral nerves may be especially sensitive to taxane-induced damage, and the permeability of the blood–nerve barrier also lends itself to greater exposure of the sensory nerves to taxanes [7]. Taxane-related neuropathy may fall into several categories, namely sensory and motor. Sensory neuropathy generally manifests as bilateral sensations in the toes and fingertips, such as numbness, tingling, and pain; allodynia and diminished reflexes can also occur [12]. Motor weakness with taxane therapy generally affects the extremities [12].
Another important consideration in the development of taxane-related neuropathy is the solvent used in formulation, a key difference among the currently available taxanes [2–4]. Paclitaxel is formulated with polyoxyethylated castor oil, or Cremophor® EL (recently renamed Kolliphor® EL), docetaxel is formulated with polysorbate 80 (or TWEEN® 80), and nab-paclitaxel is solvent free, consisting of paclitaxel and human serum albumin at a concentration similar to the concentration of albumin in the blood [2–4]. These differences can result in variations in toxicity profiles because the solvents themselves have been associated with varying biological effects. With respect to neurotoxicity, in preclinical studies, axonal swelling, degeneration, and demyelination have been observed with Cremophor EL [13, 14]. Thus, the damage it induces may be related to the persistent neuropathy caused by Cremophor EL-based paclitaxel. Polysorbate 80 may also contribute to the neuropathy observed with docetaxel by resulting in degeneration of neuronal vesicles [15]. In clinical studies of patients with MBC, severe neuropathy associated with paclitaxel and docetaxel persisted longer after discontinuation of therapy compared with that associated with nab-paclitaxel [16–18]. Severity of taxane-related neuropathy is related to a number of factors, including dosing and administration, which will be discussed later in this review.
Peripheral neuropathy related to chemotherapy can limit treatment for many patients. In a retrospective cohort study of patients receiving docetaxel or paclitaxel for nonmetastatic breast cancer, it was observed that the cumulative dose delivered was significantly lower than the planned cumulative dose in patients who had a dose reduction/discontinuation due to taxane-related chemotherapy (P < .001) [19]. In addition, taxane-related neuropathy is often cumulative and can progress after each treatment cycle [20]. Cumulative and persistent neuropathy in patients is often linked with a decreased ability to receive later lines of therapy. As an example, in a phase III trial of patients with advanced non-small cell lung cancer, those receiving first-line paclitaxel plus carboplatin demonstrated increased rates of peripheral neuropathy from cycle 4 (20 %) to cycle 8 (43 %) [21]; the most common reason for not progressing to second-line therapy was residual grade 2/3 peripheral neuropathy.
Data regarding the long-term effects of taxane-related peripheral neuropathy are varied. One study in patients who were 1–13 years post-taxane therapy demonstrated that paclitaxel- and docetaxel-related peripheral neuropathy completely resolved in only 14 % after treatment discontinuation [22]. However, the symptoms of peripheral neuropathy in these patients were considered to be well tolerated. In a second study of patients who were 6 months to 2 years post-adjuvant taxane therapy, 81 % of patients evaluated still reported symptoms of peripheral neuropathy, with up to 27 % reporting severe symptoms in the hands and feet [23]. Chemotherapy-related peripheral neuropathy may also be predictive of the development of neuropathic pain. A survey of patients who had previously received paclitaxel treatment for breast cancer revealed that 27 % of those who developed paclitaxel-related neuropathy eventually developed neuropathic pain [24]. The study suggested that monitoring patients who develop peripheral neuropathy on taxane treatment is important, even after treatment is discontinued.
The effects of taxane-related neuropathy may differ from other microtubule-inhibiting agents used to treat MBC. To date, no published head-to-head studies of taxanes and single-agent eribulin or ixabepilone exist, but preclinical evidence may provide clues about the neuropathic effects of these agents. In a preclinical study, mice treated with ixabepilone or paclitaxel had significant deficits in nerve conduction parameters as well as degenerative changes in the pathology of dorsal root ganglia and sciatic nerves, whereas mice treated with eribulin mesylate did not experience significant effects on nerve conduction and experienced less frequent morphological effects [25]. These findings led the authors to conclude that, in mice, eribulin mesylate was associated with less neuropathy compared with paclitaxel or ixabepilone. A subsequent preclinical study demonstrated that paclitaxel was associated with additional deleterious effects in mice with preexisting paclitaxel-induced peripheral neuropathy, whereas the neuropathic effect with eribulin in these mice was limited [26].
Neuropathy in clinical trials of taxanes in the treatment of metastatic breast cancer
The development of taxane-related neuropathy has been reported in numerous phase II/III clinical trials (Table 1). A major limitation of many studies is the inconsistent reporting of neuropathy data; most studies report only grade ≥3 neuropathy. Taxane-related neuropathy appears to be related to dose and/or schedule [6, 10, 27–29].
Neuropathy in trials of paclitaxel
In a phase III study of paclitaxel (± trastuzumab) administered weekly versus every 3 weeks (q3w) for the first- or second-line treatment of MBC [Cancer and Leukemia Group B (CALGB) 9840], the weekly schedule produced a significantly higher overall response rate (ORR) versus the q3w schedule (42 vs 29 %; P = .004) and a longer median time to progression (TTP; 9 vs 5 months; P < .0001) and median overall survival (OS; 24 vs 12 months; P = .0092) [29]. The weekly dose was decreased from 100 to 80 mg/m2 because of a 30 % incidence of sensory neuropathy [29]. Both treatment arms had similar incidences of grade 2 neuropathy (21 %), but the weekly schedule of paclitaxel produced twice as much grade 3 sensory neuropathy (24 %) versus the q3w schedule (12 %) (P = .0046 for grade ≥2). In the same study, the weekly arm was associated with a significantly higher rate of grade 2 and 3 motor neuropathy (8 and 9 %, respectively) versus the q3w arm (4 and 5 %, respectively) (P = .013 for grade ≥2). CALGB Protocol 9342 assessed the efficacy and safety of three paclitaxel doses administered q3w: 175, 210, and 250 mg/m2 in patients with MBC who had received ≥1 prior chemotherapy regimen for metastatic disease [30]. No differences were observed in ORR between the arms (21–26 %; P = NS) or in median OS (11–14 months; P = NS), but the 250-mg/m2 dose demonstrated a slightly longer median TTP versus the 210- and 175-mg/m2 doses (4.9 vs 4.1 vs 3.9 months, respectively; P = .045). The incidence of grade 3/4 sensory and motor neuropathy was dose related. The 250-mg/m2 dose produced the highest rate of grade 3/4 sensory and motor neuropathy (33 and 14 %, respectively), followed by the 210-mg/m2 dose (19 and 11 %, respectively) and the 175-mg/m2 dose (7 and 5 %, respectively). Interestingly, the incidences of grade 1/2 sensory neuropathy appeared to be higher in the 175- and 210-mg/m2 arms than in the 250-mg/m2 arm [79 vs 57 vs 35 %, respectively; P = not reported (NR)], as did the incidences of grade 1/2 motor neuropathy (89 vs 83 vs 79 %, respectively; P = NR).
Neuropathy in trials of docetaxel
A phase III study assessed the efficacy and safety of docetaxel 75 mg/m2 q3w versus docetaxel 35 mg/m2 weekly for 3 weeks followed by 1 week of rest (qw 3/4) in patients who had received ≥one prior chemotherapy regimen for metastatic disease [28]. The q3w schedule demonstrated a numerically higher ORR (36 vs 20 %; P = NR), a similar median progression-free survival (PFS) (5.7 vs 5.5 months; P = NS), and OS (18.3 vs 18.6 months; P = NS), but more grade 3/4 neuropathy versus the weekly schedule (10 vs 5 %; P = NR). In a phase II study of patients with MBC who had received ≥one prior chemotherapy regimen for metastatic disease, docetaxel 40 mg/m2 weekly versus docetaxel 100 mg/m2 q3w, respectively, demonstrated similar ORRs (34 vs 33 %; P = NR) and median TTPs (5.7 vs 5.3 months; P = NR) and a longer median OS (29.1 vs 20.1 months; P = NR) [31]. Again, the q3w schedule demonstrated a higher incidence of grade 3/4 neurotoxicity (17 vs 2 %; P = NR), and more patients discontinued treatment in the q3w arm versus the weekly arm because of neurotoxicity (12 vs 2 %; P = NR). In a phase III trial of patients with anthracycline-pretreated MBC, no differences were observed between docetaxel 36 mg/m2 weekly and docetaxel 100 mg/m2 q3w in ORR (25 vs 26 %; P = NR), median PFS (4.5 vs 5.1 months; P = NS), and OS (7.8 vs 9.9 months; P = NS); however, the median time to treatment failure was significantly longer in the q3w arm (3.2 vs 4.0 weeks; P = .015) [32]. Grade 3/4 motor neuropathy was observed in 6.5 % of patients in the q3w arm versus 1.3 % of patients in the weekly arm, and 2.6 % of patients withdrew as a result of motor neuropathy in the q3w arm versus none in the weekly arm.
Neuropathy in trials comparing paclitaxel with docetaxel
In a phase III study of paclitaxel 175 mg/m2 q3w versus docetaxel 100 mg/m2 q3w in patients with MBC that had progressed after an anthracycline-based regimen, docetaxel produced a significantly longer median OS (15.4 vs 12.7 months; P = .03), a significantly longer median TTP (5.7 vs 3.6 months; P < .0001), and a numerically higher ORR (32 vs 25 %; P = NS) versus paclitaxel [33]. Docetaxel versus paclitaxel produced a higher incidence of grade 3/4 neurosensory toxicity (7 vs 4 %; P = .08) and neuromotor toxicity (5 vs 2 %; P = .001) and more all-grade neurosensory toxicity (64 vs 59 %; P = NR) and neuromotor toxicity (28 vs 13 %; P = NR). A greater percentage of patients treated with docetaxel versus paclitaxel discontinued therapy because of neurosensory toxicity (8 vs 4 %) and neuromotor toxicity (5 vs 1 %).
Neuropathy in trials comparing nab-paclitaxel with other taxanes
In the phase III study of nab-paclitaxel 260 mg/m2 versus paclitaxel 175 mg/m2 (both q3w), as ≥first-line therapy for patients with MBC, nab-paclitaxel produced a significantly longer ORR (33 vs 19 %; P = .001) and a significantly longer median TTP (5.3 vs 3.9 months; P = .006) [17]. No grade 4 sensory or motor neuropathy was observed in either arm; however, grade 3 sensory neuropathy was observed in 10 % of patients treated with nab-paclitaxel versus 2 % treated with paclitaxel (P < .001). The higher rate of neuropathy with nab-paclitaxel was not unexpected, because the actual delivered paclitaxel dose was 49 % higher with nab-paclitaxel versus paclitaxel (mean ± SD: 85.13 ± 3.118 vs 57.02 ± 3.008 mg/m2 per week, respectively). The incidence of grade 3 neuropathy observed with nab-paclitaxel 260 mg/m2 q3w was lower than that reported with a similar dose and schedule of paclitaxel in the CALGB 9342 trial. In that trial, 32 % of patients who received paclitaxel 250 mg/m2 q3w experienced grade 3 sensory neuropathy [30].
A randomized phase II study compared the efficacy and safety of various doses of qw 3/4 and q3w nab-paclitaxel versus docetaxel q3w as first-line treatment for MBC [27]. nab-Paclitaxel 150 mg/m2 qw 3/4 resulted in the longest median OS (33.8 months) followed by nab-paclitaxel 300 mg/m2 q3w (27.7 months), docetaxel 100 mg/m2 q3w (26.6 months), and nab-paclitaxel 100 mg/m2 qw 3/4 (22.2 months) [16]. Furthermore, treatment with nab-paclitaxel 100 mg/m2 qw 3/4, 150 mg/m2 qw 3/4, and 300 mg/m2 q3w resulted in a significantly higher investigator-assessed ORR versus docetaxel (63, 74, and 46 % vs 39 %; P < .001 overall); independently assessed ORR was also higher with the nab-paclitaxel 100 mg/m2 qw 3/4, 150 mg/m2 qw 3/4, and 300 mg/m2 q3w arms versus the docetaxel arm (34, 36, and 28 % vs 26 %; P = NS) [27]. Nonsignificant differences in the incidence of neuropathy existed between the various doses/schedules of nab-paclitaxel and docetaxel [16]. No grade 4 neuropathy was reported, but nab-paclitaxel at 300 mg/m2 q3w and 150 mg/m2 qw 3/4 resulted in the highest rates of sensory neuropathy (21 and 22 % of patients, respectively) versus 12 % of patients in the docetaxel arm and 9 % of patients in the nab-paclitaxel 100 mg/m2 qw 3/4 arm (P = NS overall) [16].
Neuropathy in recent trials comparing nab-paclitaxel combinations with other taxane combinations
Rates of neuropathy associated with taxanes or ixabepilone plus bevacizumab for the treatment of MBC from a large cooperative group trial were reported [34]. The phase III CALGB 40502 trial compared the efficacy and safety of nab-paclitaxel 150 mg/m2 qw 3/4 plus bevacizumab 10 mg/kg q2w with either paclitaxel 90 mg/m2 qw 3/4 or ixabepilone 16 mg/m2 qw 3/4, both combined with the same dose/schedule of bevacizumab. A protocol amendment made the use of bevacizumab optional after the withdrawal of Food and Drug Administration approval in March 2011, but 98 % of patients in the study received bevacizumab. The median PFS (primary endpoint) was not statistically significantly different between the nab-paclitaxel (n = 271) and paclitaxel arms (n = 283) (9.2 vs 10.6 months; P = .12) and neither was the median OS (27 vs 26 months; P = .92). Rates of grade 2 neuropathy were similar between the nab-paclitaxel and paclitaxel arms (27 % for both) as were rates of grade 4 neuropathy (1 vs <1 %). However, a higher incidence of grade 3 neuropathy was observed in patients receiving nab-paclitaxel versus those receiving paclitaxel (24 vs 16 %) leading to a significantly higher rate of grade ≥3 neuropathy for nab-paclitaxel versus paclitaxel (25 vs 16 %; P = .012). Complete results from this study are eagerly anticipated. Similarly, in a phase II study of three different doses/schedules of nab-paclitaxel (260 mg/m2 q3w, 260 mg/m2 q2w with filgrastim, or 130 mg/m2 qw) with bevacizumab (10 mg/kg q2w or 15 mg/kg q3w) in patients with MBC, the ORRs (primary endpoint) were 45, 41, and 46 %, respectively, and rates of grade ≥3 neuropathy were 33, 56, and 46 %, respectively [35]. These findings suggest that nab-paclitaxel plus bevacizumab is active in MBC; however, the optimal schedule/dose of nab-paclitaxel requires further evaluation.
Time to onset and improvement of neuropathy
Most phase II/III studies of taxanes in MBC have not reported time to onset or improvement of neuropathy, which are important factors affecting treatment decisions. One major reason for this may be that many patients have a preexisting level of neuropathy at enrollment because of prior chemotherapy treatment; thus, it may be difficult to distinguish preexisting neuropathy from that brought on by therapy. In one study of weekly paclitaxel 80 mg/m2 in patients with MBC who received ≤2 prior chemotherapy regimens for metastatic disease, 69 % of patients developed neuropathy and 9 % of patients developed grade 3 neuropathy (no grade 4) [36]. The median time to onset of grade 2/3 neuropathy in that study was approximately 4.7 months. In another study of paclitaxel 200–250 mg/m2 q3w, symptoms of neuropathy occurred after an average of 1.7 cycles in 84 % of patients [37].
Rapid improvement in neuropathic symptoms may allow patients to resume treatment more quickly and is important to note when considering timing, choice, and dose/schedule of later lines of therapy. Studies of nab-paclitaxel in MBC have reported time to improvement in neuropathy, and it is generally faster than with paclitaxel or docetaxel. In the study by Forsyth et al. of paclitaxel 200–250 mg/m2 q3w in previously treated patients with MBC, follow-up data were obtained in 19 % of patients; peripheral neuropathy had improved or resolved in all of these patients 1–6 months after treatment stopped [37]. In the phase II study by Gradishar et al. of nab-paclitaxel (100 and 150 mg/m2 qw 3/4 and 300 mg/m2 q3w) versus docetaxel 100 mg/m2 q3w for the first-line treatment of MBC, the median time to improvement in grade 3 neuropathy to grade ≤2 was 20–22 days with nab-paclitaxel compared with 41 days with docetaxel [16]. In the phase III study of nab-paclitaxel (260 mg/m2 qw) versus paclitaxel (175 mg/m2 qw) in patients with MBC by Gradishar et al., the median time to improvement in grade 3 neuropathy to grade ≤2 was 22 days for nab-paclitaxel and 79 days for paclitaxel [18]. Because peripheral neuropathy associated with nab-paclitaxel treatment appears to improve more quickly than with treatment with either paclitaxel or docetaxel, patients previously receiving nab-paclitaxel who have seen improvement in their peripheral neuropathy theoretically could progress to later lines of therapy more quickly.
Predictors of taxane-induced neuropathy
Recent studies have identified potential molecular predictors of taxane-induced neuropathy. In the Eastern Cooperative Oncology Group (ECOG) 5103 study of women with early-stage breast cancer treated with weekly paclitaxel (± bevacizumab) in the adjuvant setting, a genome-wide association study showed that single nucleotide polymorphisms (SNPs) in two genes—RWDD3 and TECTA—were significantly associated with time to onset of neuropathy (P < 5 × 10−7) [38], but this association could not be confirmed in a recent study of Scandinavian patients with ovarian cancer [39]. Another genome-wide association study in the CALGB 40101 trial showed a SNP in the gene FGD4 that was associated with the early onset of peripheral neuropathy in patients treated with paclitaxel [40]. In the same study, other SNPs in the EPHA5 and FZD3 genes were also identified as being potential risk factors for the onset and severity of peripheral sensory neuropathy. In another study, patients with ABCB1 variants were potentially more likely to develop paclitaxel-induced peripheral neuropathy than were those with the wild-type allele (P = .09) [41]. An association between a GSTP1 polymorphism and docetaxel-induced peripheral neuropathy has also been identified [42]. Patients with the 105Ile/105Ile GSTP1 genotype had a significantly greater risk of developing more severe docetaxel-induced peripheral neuropathy than did those with other GSTP1 genotypes (P = .03). Finally, in breast cancer patients treated with paclitaxel, CYP2C8*3 status was significantly associated with an increased risk of paclitaxel-induced neuropathy (P = .006); each CYP2C3*8 allele approximately doubled a patient’s risk of developing grade ≥2 neuropathy (P = .004) [43].
Age, race, and comorbid conditions, such as diabetes, may also be associated with an increased risk of developing neuropathy. The results of the ECOG 5103 study showed a significant association between neuropathy and age (12.9 % increase with each 10 years; P = .004) and African-American race (P = 4.5 × 10−11) [38]. In an analysis of the ECOG 1199 study of patients with breast cancer who received adjuvant taxane-containing therapy, hyperglycemia and obesity were associated with an increased risk of neuropathy, and African-American race demonstrated a trend toward an increased risk of neuropathy with weekly paclitaxel [44]. Although age was associated with an increased risk of neuropathy in the ECOG 5103 study [38], this trend was not observed in the ECOG 1199 study [44]. In that study, the development of neuropathy was found not to be predictive of survival outcomes. Furthermore, approximately half of all patients with diabetes are at risk of developing diabetic peripheral neuropathy [45, 46]. It is well known that high blood glucose can damage peripheral nerves; thus, patients with diabetes who are treated with chemotherapy agents associated with peripheral neuropathy, such as taxanes, may be at greater risk for developing chemotherapy-related peripheral neuropathy. While data are limited, some reports have suggested an increased risk of chemotherapy-related peripheral neuropathy or a worsening of preexisting neuropathy in patients with diabetes [47, 48]. With respect to taxane-based therapy, in an exploratory analysis of a phase III trial in patients with advanced non-small cell lung cancer, those with diabetes who were treated with nab-paclitaxel plus carboplatin had a 4 % higher rate of grade ≥3 peripheral neuropathy (7 %) than did the intent-to-treat population (3 %), while patients with diabetes who were treated with paclitaxel plus carboplatin had a 12 % higher rate of grade ≥3 peripheral neuropathy (23 %) compared with the intent-to-treat population (11 %) [49, 50]. While this finding is interesting, because of the exploratory nature of this analysis, no conclusions can be definitively drawn about whether patients with diabetes are at increased risk of developing peripheral neuropathy with nab-paclitaxel or paclitaxel regimens.
Management of neuropathy
Early recognition of the signs and symptoms of taxane-related neuropathy is critical for appropriate management and improved outcomes. Typically, taxane-related neuropathy is managed with dose delays and/or reductions. For example, it is recommended that, for patients experiencing grade 3 neuropathy, the dose of nab-paclitaxel should be held until resolution to grade 1 or 2, followed by a dose reduction for all subsequent doses of nab-paclitaxel [2]. A 20 % dose reduction is recommended for all subsequent courses in patients receiving paclitaxel who develop severe peripheral neuropathy, and discontinuation is recommended in patients receiving docetaxel who develop grade 3/4 neuropathy [3, 4]. Numerous studies of interventions for the management of neuropathy exist; however, for the most part, many of these interventions have not demonstrated a meaningful improvement in neuropathic symptoms, and some agents have even worsened symptoms of chemotherapy-induced neuropathy compared with placebo (Table 2) [51–56]. Several of these interventions have been covered in previous reviews of taxane-related neuropathy [12, 57]. This review will focus only on recent highlights in this area.
Results of the phase III CALGB 170601 study of duloxetine 60 mg daily, in patients who developed chemotherapy-induced neuropathic pain after taxane or oxaliplatin treatment, showed that the drug was significantly more effective than placebo at reducing taxane-related neuropathic pain symptoms (P = .003) [58]. Patients treated with duloxetine also experienced a significant decrease in the amount of pain that interfered with daily functioning compared with placebo (P = .01). Furthermore, 41 % of patients treated with duloxetine reported a decrease in numbness and tingling in the feet compared with only 23 % of patients treated with placebo (P = NR); this trend was not observed for numbness and tingling in the hands (P = NR). Although the safety profile of duloxetine is generally considered to be acceptable, it should not be administered with drugs that inhibit serotonin reuptake, CYP P450 2D6 substrates, warfarin, or nonsteroidal anti-inflammatory drugs.
Another study found that omega-3 fatty acids may offer protection against paclitaxel-induced peripheral neuropathy [59]. In that study, patients with breast cancer received omega-3 fatty acid pearls or placebo during paclitaxel treatment. For 1 month after treatment, the patients were evaluated by using the reduced total neuropathy score; 70 % of the group that received omega-3 fatty acids did not develop peripheral neuropathy (any grade) compared with 41 % of patients in the placebo group (P = .029); no significant difference in the severity of peripheral neuropathy was observed between the 2 groups.
Other agents are in the early stages of assessment for the treatment or prevention of chemotherapy-related peripheral neuropathy. A recent preclinical study demonstrated that coadministration of metformin protected mice against chemotherapy-induced peripheral neuropathy [60]. The study found that cisplatin treatment led to the loss of intraepidermal nerve fibers in the paws and that metformin prevented this phenomenon. A separate preclinical study demonstrated that concurrent administration of interleukin-6 and cisplatin, vincristine, or paclitaxel in rodents prevented electrophysical abnormalities associated with neuropathy as well as pathological changes in peripheral nerves [61]. Treatment with interleukin-6 did not appear to affect the antitumor activity of these agents or affect tumor growth. Whether or not these preclinical findings will translate to humans remains to be seen.
Nonpharmaceutical methods of neuropathy management are also being studied. A case report of a patient with esophageal carcinoma who developed grade 2 peripheral neuropathy with docetaxel plus cisplatin demonstrated that manual therapy (i.e., massage) completely resolved the patient’s neuropathic symptoms [62]. In uncontrolled studies, treatment with a noninvasive electro-analgesia device, referred to as “Scrambler” therapy, demonstrated benefit for painful chemotherapy-induced peripheral neuropathy [63]; however, the results of other studies have been mixed. In a randomized controlled study of patients with neuropathic pain, Scrambler therapy appeared to be more beneficial than guideline-based drug management at relieving chronic neuropathic pain as assessed with a visual analog scale (P < .0001) [64]. However, Scrambler therapy failed to show any significant difference from sham therapy in pain scores in a recent randomized double-blind study of patients with neuropathic pain [65]. Further studies of Scrambler therapy in various solid tumors are ongoing. Several case series, case reports, and other small studies have demonstrated improvement in neuropathic symptoms with acupuncture [66–69]. A phase II randomized trial that will assess the effects of acupuncture in preventing dose reductions due to chemotherapy-induced peripheral neuropathy in patients with breast cancer is currently ongoing (ClinicalTrials.gov identifier NCT01881932).
Neuropathy assessment tools
Many times, neuropathy is underrecognized and underreported by physicians compared with patients [70–72]. Furthermore, neuropathy induced by taxanes is generally quantified in clinical studies by using toxicity grading scales [e.g., National Cancer Institute Common Toxicity Criteria for Adverse Events (NCI CTCAE)], and these scales often have suboptimal reliability, sensitivity, and validity [71, 73, 74]. Therefore, patient-reported neuropathy tools are important for assessing the development and improvement in chemotherapy-induced peripheral neuropathy, and more prospective studies using these types of tools in trials of MBC are critically needed. A major advantage to these patient-reported tools is the ability to capture treatment effects over time, even after treatment has been completed. This is important for patients receiving taxane therapy, because peripheral neuropathy with some taxanes can persist for an extended period of time.
Select patient-reported tools for use in assessing taxane-induced neuropathy are shown in Table 3. Numerous patient-reported tools have been validated [75]; however, the Functional Assessment of Cancer Therapy (FACT)-Taxane tool is the only taxane-specific tool for assessing patient-reported taxane-related symptoms, including neuropathy [76]. FACT-Taxane consists of a 16-item FACT-General (FACT-G) and an 11-item taxane subscale that allow for the evaluation of disease symptoms and taxane-related toxicity [77]. The FACT-Ntx scale is another iteration of the FACT family of tools that specifically measures neurotoxicity produced by chemotherapy [77]. The FACT-Ntx is an 11-item questionnaire that focuses solely on chemotherapy-induced neurotoxicity; it is commonly used in combination with the FACT-G scale as part of the FACT/Gynecologic Oncology Group Neurotoxicity scale. In one study, the addition of paclitaxel to cisplatin plus doxorubicin in patients with advanced endometrial cancer produced more neuropathy and lower FACT-Ntx scores (indicating worse neuropathy) compared with doxorubicin plus cisplatin alone (P < .001), and the differences were still significant after 6 months (P = .014) [78].
The Chemotherapy-Induced Peripheral Neuropathy Assessment Tool (CIPNAT) was recently developed but has not yet been validated in any studies to date [79]. The CIPNAT is a 36-item tool that evaluates the occurrence, severity, distress, and frequency of nine neuropathic symptoms and 14 items that evaluate neuropathic interference with activities. Another tool, the Patient Neurotoxicity Questionnaire (PNQ), contains only two items to assess the incidence and severity of sensory and motor neuropathy [70]. It was prospectively assessed in a phase III study of patients with breast cancer receiving adjuvant therapy with a taxane [70]. The PNQ scores were compared with FACT-Ntx, FACT-G, and NCI CTCAE scores, and the results showed a strong correlation between the PNQ and the FACT-Ntx but only a weak correlation between the PNQ and the FACT-G. The PNQ scores were significantly correlated with the NCI CTCAE sensory neuropathy scores but not with the motor neuropathy scores; the physician-assessed scores were lower than the patient-reported scores in this study. Finally, the Quality of Life Questionnaire (QLQ)–Chemotherapy-Induced Peripheral Neuropathy (CIPN) 20 scale is a 20-item patient-reported tool that supplements the European Organization for Research and Treatment of Cancer QLQ questionnaire [80]. The QLQ-CIPN20 recently demonstrated good validity and reliability scores in a standardization study performed by the Chemotherapy-Induced Peripheral Neuropathy Outcome Measures Study Group, and further studies are planned to evaluate the responsiveness aspects of this tool [73].
Conclusions and future perspectives
Although newer targeted agents are being developed, taxanes remain a standard of care therapy for patients with MBC. Neuropathy is an important, dose-limiting, painful, and often irreversible toxicity associated with taxane therapy. Thus, there exists a need to balance taxane efficacy and toxicity. Fully understanding the differences in the development and improvement in neuropathy between the taxanes is highly important for making treatment decisions and proactively managing patients with MBC on taxane therapy.
References
NCCN practice guidelines in oncology: breast cancer. Ver. 3 (2014)
Abraxane [package insert]. Summit, NJ: Celgene Corporation; December 2014
Taxol [package insert]. Bristol-Myers Squibb Co; April 2011
Taxotere [package insert]. Bridgewater, NJ: sanofi-aventis US LLC; December 2013
Hausheer FH, Schilsky RL, Bain S, Berghorn EJ, Lieberman F (2006) Diagnosis, management, and evaluation of chemotherapy-induced peripheral neuropathy. Semin Oncol 33:15–49
Pachman DR, Barton DL, Watson JC, Loprinzi CL (2011) Chemotherapy-induced peripheral neuropathy: prevention and treatment. Clin Pharmacol Ther 90:377–387
Swain SM, Arezzo JC (2008) Neuropathy associated with microtubule inhibitors: diagnosis, incidence, and management. Clin Adv Hematol Oncol 6:455–467
Argyriou AA, Koltzenburg M, Polychronopoulos P, Papapetropoulos S, Kalofonos HP (2008) Peripheral nerve damage associated with administration of taxanes in patients with cancer. Crit Rev Oncol Hematol 66:218–228
Hagiwara H, Sunada Y (2004) Mechanism of taxane neurotoxicity. Breast Cancer 11:82–85
Lee JJ, Swain SM (2006) Peripheral neuropathy induced by microtubule-stabilizing agents. J Clin Oncol 24:1633–1642
Bettelheim FA, Brown WH, Campbell MK, Farrell SO (2010) Introduction to organic and biochemistry, 7th edn. Cengage Learning, Belmont
Smith EM (2013) Current methods for the assessment and management of taxane-related neuropathy. Clin J Oncol Nurs 17(Suppl):22–34
Authier N, Gillet JP, Fialip J, Eschalier A, Coudore F (2000) Description of a short-term taxol-induced nociceptive neuropathy in rats. Brain Res 887:239–249
Windebank AJ, Blexrud MD, de Groen PC (1994) Potential neurotoxicity of the solvent vehicle for cyclosporine. J Pharmacol Exp Ther 268:1051–1056
ten Tije AJ, Verweij J, Loos WJ, Sparreboom A (2003) Pharmacological effects of formulation vehicles: implications for cancer chemotherapy. Clin Pharmacokinet 42:665–685
Gradishar WJ, Krasnojon D, Cheporov SV, Makhson AN, Manikhas GM, Clawson A, Bhar P, Iglesias J (2012) nab-Paclitaxel versus docetaxel for the first-line treatment of metastatic breast cancer: final overall survival (OS) analysis of a randomized phase 2 trial. Clin Breast Cancer 12:313–321
Gradishar WJ, Tjulandin S, Davidson N, Shaw H, Desai N, Bhar P, Hawkins M, O’Shaughnessy J (2005) Phase III trial of nanoparticle albumin-bound paclitaxel compared with polyethylated castor oil-based paclitaxel in women with breast cancer. J Clin Oncol 23:7794–7803
Cortes J, Saura C (2010) Nanoparticle albumin-bound (nab)-paclitaxel: improving efficacy and tolerability by targeted drug delivery in metastatic breast cancer. EJC Suppl 8:1–10
Speck RM, Sammel MD, Farrar JT, Hennessy S, Mao JJ, Stineman MG, DeMichele A (2013) Impact of chemotherapy-induced peripheral neuropathy on treatment delivery in nonmetastatic breast cancer. J Oncol Pract 9:e234–e240
Rowinsky EK, Chaudhry V, Cornblath DR, Donehower RC (1993) Neurotoxicity of taxol. J Natl Cancer Inst Monogr 15:107–115
Socinski MA, Schell MJ, Peterman A, Bakri K, Yates S, Gitten R, Unger P, Lee J, Lee JH, Tynan M, Moore M, Kies MS (2002) Phase III trial comparing a defined duration of therapy versus continuous therapy followed by second-line therapy in advanced-stage IIIB/IV non-small-cell lung cancer. J Clin Oncol 20:1335–1343
Osmani K, Vignes S, Aissi M, Wade F, Milani P, Levy BI, Kubis N (2012) Taxane-induced peripheral neuropathy has good long-term prognosis: a 1- to 13-year evaluation. J Neurol 259:1936–1943
Hershman DL, Weimer LH, Wang A, Kranwinkel G, Brafman L, Fuentes D, Awad D, Crew KD (2011) Association between patient reported outcomes and quantitative sensory tests for measuring long-term neurotoxicity in breast cancer survivors treated with adjuvant paclitaxel chemotherapy. Breast Cancer Res Treat 125:767–774
Reyes-Gibby CC, Morrow PK, Buzdar A, Shete S (2009) Chemotherapy-induced peripheral neuropathy as a predictor of neuropathic pain in breast cancer patients previously treated with paclitaxel. J Pain 10:1146–1150
Wozniak KM, Nomoto K, Lapidus RG, Wu Y, Carozzi V, Cavaletti G, Hayakawa K, Hosokawa S, Towle MJ, Littlefield BA, Slusher BS (2011) Comparison of neuropathy-inducing effects of eribulin mesylate, paclitaxel, and ixabepilone in mice. Cancer Res 71:3952–3962
Wozniak KM, Wu Y, Farah MH, Littlefield BA, Nomoto K, Slusher BS (2013) Neuropathy-inducing effects of eribulin mesylate versus paclitaxel in mice with preexisting neuropathy. Neurotox Res 24:338–344
Gradishar WJ, Krasnojon D, Cheporov S, Makhson AN, Manikhas GM, Clawson A, Bhar P (2009) Significantly longer progression-free survival with nab-paclitaxel compared with docetaxel as first-line therapy for metastatic breast cancer. J Clin Oncol 27:3611–3619
Rivera E, Mejia JA, Arun BK, Adinin RB, Walters RS, Brewster A, Broglio KR, Yin G, Esmaeli B, Hortobagyi GN, Valero V (2008) Phase 3 study comparing the use of docetaxel on an every-3-week versus weekly schedule in the treatment of metastatic breast cancer. Cancer 112:1455–1461
Seidman AD, Berry D, Cirrincione C, Harris L, Muss H, Marcom PK, Gipson G, Burstein H, Lake D, Shapiro CL, Ungaro P, Norton L, Winer E, Hudis C (2008) Randomized phase III trial of weekly compared with every-3-weeks paclitaxel for metastatic breast cancer, with trastuzumab for all HER-2 overexpressors and random assignment to trastuzumab or not in HER-2 nonoverexpressors: final results of Cancer and Leukemia Group B protocol 9840. J Clin Oncol 26:1642–1649
Winer EP, Berry DA, Woolf S, Duggan D, Kornblith A, Harris LN, Michaelson RA, Kirshner JA, Fleming GF, Perry MC, Graham ML, Sharp SA, Keresztes R, Henderson IC, Hudis C, Muss H, Norton L (2004) Failure of higher-dose paclitaxel to improve outcome in patients with metastatic breast cancer: cancer and leukemia group B trial 9342. J Clin Oncol 22:2061–2068
Tabernero J, Climent MA, Lluch A, Albanell J, Vermorken JB, Barnadas A, Anton A, Laurent C, Mayordomo JI, Estaun N, Losa I, Guillem V, Garcia-Conde J, Tisaire JL, Baselga J (2004) A multicentre, randomised phase II study of weekly or 3-weekly docetaxel in patients with metastatic breast cancer. Ann Oncol 15:1358–1365
Schroder CP, de Munck L, Westermann AM, Smit WM, Creemers GJ, de Graaf H, Stouthard JM, van Deijk G, Erjavec Z, van Bochove A, Vader W, Willemse PH (2011) Weekly docetaxel in metastatic breast cancer patients: no superior benefits compared to three-weekly docetaxel. Eur J Cancer 47:1355–1362
Jones SE, Erban J, Overmoyer B, Budd GT, Hutchins L, Lower E, Laufman L, Sundaram S, Urba WJ, Pritchard KI, Mennel R, Richards D, Olsen S, Meyers ML, Ravdin PM (2005) Randomized phase III study of docetaxel compared with paclitaxel in metastatic breast cancer. J Clin Oncol 23:5542–5551
Rugo HS, Barry WT, Moreno-Aspitia A, Lyss A, Cirrincione C, Toppmeyer D, Mayer E, Naughton M, Layman RM, Carey LA, Somer RA, Perez EA, Hudis C, Winer E (2012) CALGB 40502/NCCTG N063H: randomized phase III trial of weekly paclitaxel (P) compared to weekly nanoparticle albumin bound nab-paclitaxel (NP) or ixabepilone (ix) with or without bevacizumab (B) as first-line therapy for locally recurrent or metastatic breast cancer (MBC). J Clin Oncol 30(Suppl). Abstract no. CRA 1002
Seidman AD, Conlin AK, Bach A, Moynahan ME, Lake D, Forero A, Wright GS, Hackney MH, Clawson A, Norton L, Hudis CA (2013) Randomized phase II trial of weekly vs. every 2 weeks vs. every 3 weeks nanoparticle albumin-bound paclitaxel with bevacizumab as first-line chemotherapy for metastatic breast cancer. Clin Breast Cancer 13(239–246):e1
Perez EA, Vogel CL, Irwin DH, Kirshner JJ, Patel R (2001) Multicenter phase II trial of weekly paclitaxel in women with metastatic breast cancer. J Clin Oncol 19:4216–4223
Forsyth PA, Balmaceda C, Peterson K, Seidman AD, Brasher P, DeAngelis LM (1997) Prospective study of paclitaxel-induced peripheral neuropathy with quantitative sensory testing. J Neurooncol 35:47–53
Schneider BP, Li L, Miller K, Flockhart D, Radovich M, Hancock BA, Kassem N, Foroud T, Koller DL, Badve SS, Li Z, Partirdge AH, O’Neill AM, Sparano JA, Dang CT, Northfelt DW, Smith ML, Railey E, Sldege GW (2011) Genetic associations with taxane-induced neuropathy by a genome-wide association study (GWAS) in E5103. J Clin Oncol 29(Suppl). Abstract no. 1000
Bergmann TK, Vach W, Feddersen S, Eckhoff L, Green H, Herrstedt J, Brosen K (2013) GWAS-based association between RWDD3 and TECTA variants and paclitaxel induced neuropathy could not be confirmed in Scandinavian ovarian cancer patients. Acta Oncol 52:871–873
Baldwin RM, Owzar K, Zembutsu H, Chhibber A, Kubo M, Jiang C, Watson D, Eclov RJ, Mefford J, McLeod HL, Friedman PN, Hudis CA, Winer EP, Jorgenson EM, Witte JS, Shulman LN, Nakamura Y, Ratain MJ, Kroetz DL (2012) A genome-wide association study identifies novel loci for paclitaxel-induced sensory peripheral neuropathy in CALGB 40101. Clin Cancer Res 18:5099–5109
Sissung TM, Mross K, Steinberg SM, Behringer D, Figg WD, Sparreboom A, Mielke S (2006) Association of ABCB1 genotypes with paclitaxel-mediated peripheral neuropathy and neutropenia. Eur J Cancer 42:2893–2896
Mir O, Alexandre J, Tran A, Durand JP, Pons G, Treluyer JM, Goldwasser F (2009) Relationship between GSTP1 Ile(105)Val polymorphism and docetaxel-induced peripheral neuropathy: clinical evidence of a role of oxidative stress in taxane toxicity. Ann Oncol 20:736–740
Hertz DL, Roy S, Motsinger-Reif AA, Drobish A, Clark LS, McLeod HL, Carey LA, Dees EC (2013) CYP2C8*3 increases risk of neuropathy in breast cancer patients treated with paclitaxel. Ann Oncol 24:1472–1478
Schneider BP, Zhao F, Wang M, Stearns V, Martino S, Jones V, Perez EA, Saphner T, Wolff AC, Sledge GW Jr, Wood WC, Davidson NE, Sparano JA (2012) Neuropathy is not associated with clinical outcomes in patients receiving adjuvant taxane-containing therapy for operable breast cancer. J Clin Oncol 30:3051–3057
Dyck PJ, Kratz KM, Karnes JL, Litchy WJ, Klein R, Pach JM, Wilson DM, O’Brien PC, Melton LJ 3rd, Service FJ (1993) The prevalence by staged severity of various types of diabetic neuropathy, retinopathy, and nephropathy in a population-based cohort: The Rochester Diabetic Neuropathy Study. Neurology 43:817–824
Abbott CA, Malik RA, van Ross ER, Kulkarni J, Boulton AJ (2011) Prevalence and characteristics of painful diabetic neuropathy in a large community-based diabetic population in the UK. Diabetes Care 34:2220–2224
Chaudhry V, Chaudhry M, Crawford TO, Simmons-O’Brien E, Griffin JW (2003) Toxic neuropathy in patients with pre-existing neuropathy. Neurology 60:337–340
Quasthoff S, Hartung HP (2002) Chemotherapy-induced peripheral neuropathy. J Neurol 249:9–17
Socinski MA, Bondarenko I, Karaseva NA, Makhson AM, Vynnychenko I, Okamoto I, Hon JK, Hirsh V, Bhar P, Zhang H, Iglesias JL, Renschler MF (2012) Weekly nab-paclitaxel in combination with carboplatin versus solvent-based paclitaxel plus carboplatin as first-line therapy in patients with advanced non-small-cell lung cancer: final results of a phase III trial. J Clin Oncol 30:2055–2062
Hirsh V, Owen SP, Ko A, Renschler MF, Socinski MA (2013) nab-Paclitaxel in combination with carboplatin as first-line therapy in diabetic patients with advanced non-small cell lung cancer (NSCLC). In: 15th World conference on lung cancer, poster P1 10-044
Kautio AL, Haanpaa M, Leminen A, Kalso E, Kautiainen H, Saarto T (2009) Amitriptyline in the prevention of chemotherapy-induced neuropathic symptoms. Anticancer Res 29:2601–2606
Rao RD, Michalak JC, Sloan JA, Loprinzi CL, Soori GS, Nikcevich DA, Warner DO, Novotny P, Kutteh LA, Wong GY, North Central Cancer Treatment Group (2007) Efficacy of gabapentin in the management of chemotherapy-induced peripheral neuropathy: a phase 3 randomized, double-blind, placebo-controlled, crossover trial (N00C3). Cancer 110:2110–2118
Rao RD, Flynn PJ, Sloan JA, Wong GY, Novotny P, Johnson DB, Gross HM, Renno SI, Nashawaty M, Loprinzi CL (2008) Efficacy of lamotrigine in the management of chemotherapy-induced peripheral neuropathy: a phase 3 randomized, double-blind, placebo-controlled trial, N01C3. Cancer 112:2802–2808
Hershman DL, Unger JM, Crew KD, Moinpour C, Minasian LM, Hansen L, Lew D, OKane P, Wade JL, Wong S, Hortobagyi GN, Meyskens FL, Albain KS (2012) SWOG S0715: randomized placebo-controlled trial of acetyl-l-carnitine for the prevention of taxane-induced neuropathy during adjuvant breast cancer therapy. J Clin Oncol 30(Suppl). Abstract no. 9018
Afonseca SO, Cruz FM, Cubero Dde I, Lera AT, Schindler F, Okawara M, Souza LF, Rodrigues NP, Giglio AD (2013) Vitamin E for prevention of oxaliplatin-induced peripheral neuropathy: a pilot randomized clinical trial. Sao Paulo Med J 131:35–38
Loprinzi CL, Qin R, Dakhil SR, Fehrenbacher L, Stella PJ, Atherton PJ, Seisler DK, Qamar R, Lewis GC, Grothey A (2013) Phase III, randomized, placebo (PL)-controlled, double-blind study of intravenous calcium/magnesium (CaMg) to prevent oxaliplatin-induced sensory neuropathy (sNT), N08CB: an alliance for clinical trials in oncology study. J Clin Oncol 31(Suppl). Abstract no. 3501
Scripture CD, Figg WD, Sparreboom A (2006) Peripheral neuropathy induced by paclitaxel: recent insights and future perspectives. Curr Neuropharmacol 4:165–172
Smith EM, Pang H, Cirrincione C, Fleishman S, Paskett ED, Ahles T, Bressler LR, Fadul CE, Knox C, Le-Lindqwister N, Gilman PB, Shapiro CL, Alliance for Clinical Trials in Oncology (2013) Effect of duloxetine on pain, function, and quality of life among patients with chemotherapy-induced painful peripheral neuropathy: a randomized clinical trial. JAMA 309:1359–1367
Ghoreishi Z, Esfahani A, Djazayeri A, Djalali M, Golestan B, Ayromlou H, Hashemzade S, Asghari Jafarabadi M, Montazeri V, Keshavarz SA, Darabi M (2012) Omega-3 fatty acids are protective against paclitaxel-induced peripheral neuropathy: a randomized double-blind placebo controlled trial. BMC Cancer 12:355
Mao-Ying QL, Kavelaars A, Krukowski K, Huo XJ, Zhou W, Price TJ, Cleeland C, Heijnen CJ (2014) The anti-diabetic drug Metformin protects against chemotherapy-induced peripheral neuropathy in a mouse model. PLoS ONE 9:e100701
Callizot N, Andriambeloson E, Glass J, Revel M, Ferro P, Cirillo R, Vitte PA, Dreano M (2008) Interleukin-6 protects against paclitaxel, cisplatin and vincristine-induced neuropathies without impairing chemotherapeutic activity. Cancer Chemother Pharmacol 62:995–1007
Cunningham JE, Kelechi T, Sterba K, Barthelemy N, Falkowski P, Chin SH (2011) Case report of a patient with chemotherapy-induced peripheral neuropathy treated with manual therapy (massage). Support Care Cancer 19:1473–1476
Sabato AF, Marineo G, Gatti A (2005) Scrambler therapy. Minerva Anestesiol 71:479–482
Marineo G, Iorno V, Gandini C, Moschini V, Smith TJ (2012) Scrambler therapy may relieve chronic neuropathic pain more effectively than guideline-based drug management: results of a pilot, randomized, controlled trial. J Pain Symptom Manage 43:87–95
Campbell TC, Nimunkar AJ, Retseck J, Eickhoff JC, Backonja M, Cleary JF, Kwekkeboom KL, Yen TY (2013) A randomized, double-blind study of “Scrambler” therapy versus sham for painful chemotherapy-induced peripheral neuropathy (CIPN). J Clin Oncol 31(Suppl). Abstract no. 9635
Xu WR, Hua BJ, Hou W, Bao YJ (2010) Clinical randomized controlled study on acupuncture for treatment of peripheral neuropathy induced by chemotherapeutic drugs. Zhongguo Zhen Jiu 30:457–460
Bao T, Zhang R, Badros A, Lao L (2011) Acupuncture treatment for bortezomib-induced peripheral neuropathy: a case report. Pain Res Treat 2011:920807
Donald GK, Tobin I, Stringer J (2011) Evaluation of acupuncture in the management of chemotherapy-induced peripheral neuropathy. Acupunct Med 29:230–233
Schroeder S, Meyer-Hamme G, Epplee S (2012) Acupuncture for chemotherapy-induced peripheral neuropathy (CIPN): a pilot study using neurography. Acupunct Med 30:4–7
Shimozuma K, Ohashi Y, Takeuchi A, Aranishi T, Morita S, Kuroi K, Ohsumi S, Makino H, Mukai H, Katsumata N, Sunada Y, Watanabe T, Hausheer FH (2009) Feasibility and validity of the Patient Neurotoxicity Questionnaire during taxane chemotherapy in a phase III randomized trial in patients with breast cancer: N-SAS BC 02. Support Care Cancer 17:1483–1491
Kuroi K, Shimozuma K, Ohashi Y, Hisamatsu K, Masuda N, Takeuchi A, Aranishi T, Morita S, Ohsumi S, Hausheer FH (2009) Prospective assessment of chemotherapy-induced peripheral neuropathy due to weekly paclitaxel in patients with advanced or metastatic breast cancer (CSP-HOR 02 study). Support Care Cancer 17:1071–1080
Kuroi K, Shimozuma K, Ohashi Y, Takeuchi A, Aranishi T, Morita S, Ohsumi S, Watanabe T, Bain S, Hausheer FH (2008) A questionnaire survey of physicians’ perspectives regarding the assessment of chemotherapy-induced peripheral neuropathy in patients with breast cancer. Jpn J Clin Oncol 38:748–754
Cavaletti G, Frigeni B, Lanzani F, Mattavelli L, Susani E, Alberti P, Cortinovis D, Bidoli P (2010) Chemotherapy-induced peripheral neurotoxicity assessment: a critical revision of the currently available tools. Eur J Cancer 46:479–494
Griffith KA, Merkies IS, Hill EE, Cornblath DR (2010) Measures of chemotherapy-induced peripheral neuropathy: a systematic review of psychometric properties. J Peripher Nerv Syst 15:314–325
Kanatas A, Velikova G, Roe B, Horgan K, Ghazali N, Shaw RJ, Rogers SN (2012) Patient-reported outcomes in breast oncology: a review of validated outcome instruments. Tumori 98:678–688
Cella D, Peterman A, Hudgens S, Webster K, Socinski MA (2003) Measuring the side effects of taxane therapy in oncology: the functional assessment of cancer therapy-taxane (FACT-taxane). Cancer 98:822–831
Huang HQ, Brady MF, Cella D, Fleming G (2007) Validation and reduction of FACT/GOG-Ntx subscale for platinum/paclitaxel-induced neurologic symptoms: a gynecologic oncology group study. Int J Gynecol Cancer 17:387–393
Cella D, Huang H, Homesley HD, Montag A, Salani R, De Geest K, Lee R, Spirtos NM (2010) Patient-reported peripheral neuropathy of doxorubicin and cisplatin with and without paclitaxel in the treatment of advanced endometrial cancer: results from GOG 184. Gynecol Oncol 119:538–542
Tofthagen CS, McMillan SC, Kip KE (2011) Development and psychometric evaluation of the chemotherapy-induced peripheral neuropathy assessment tool. Cancer Nurs 34:E10–E20
Postma TJ, Aaronson NK, Heimans JJ, Muller MJ, Hildebrand JG, Delattre JY, Hoang-Xuan K, Lanteri-Minet M, Grant R, Huddart R, Moynihan C, Maher J, Lucey R, EORTC Quality of Life Group (2005) The development of an EORTC quality of life questionnaire to assess chemotherapy-induced peripheral neuropathy: the QLQ-CIPN20. Eur J Cancer 41:1135–1139
Albain KS, Nag SM, Calderillo-Ruiz G, Jordaan JP, Llombart AC, Pluzanska A, Rolski J, Melemed AS, Reyes-Vidal JM, Sekhon JS, Simms L, O’Shaughnessy J (2008) Gemcitabine plus paclitaxel versus paclitaxel monotherapy in patients with metastatic breast cancer and prior anthracycline treatment. J Clin Oncol 26:3950–3957
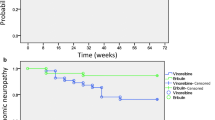
Andersson M, Lidbrink E, Bjerre K, Wist E, Enevoldsen K, Jensen AB, Karlsson P, Tange UB, Sorensen PG, Moller S, Bergh J, Langkjer ST (2011) Phase III randomized study comparing docetaxel plus trastuzumab with vinorelbine plus trastuzumab as first-line therapy of metastatic or locally advanced human epidermal growth factor receptor 2-positive breast cancer: the HERNATA study. J Clin Oncol 29:264–271
Fountzilas G, Dafni U, Dimopoulos MA, Koutras A, Skarlos D, Papakostas P, Gogas H, Bafaloukos D, Kalogera-Fountzila A, Samantas E, Briasoulis E, Pectasides D, Maniadakis N, Matsiakou F, Aravantinos G, Papadimitriou C, Karina M, Christodoulou C, Kosmidis P, Kalofonos HP (2009) A randomized phase III study comparing three anthracycline-free taxane-based regimens, as first line chemotherapy, in metastatic breast cancer: a Hellenic Cooperative Oncology Group study. Breast Cancer Res Treat 115:87–99
Miles DW, Chan A, Dirix LY, Cortes J, Pivot X, Tomczak P, Delozier T, Sohn JH, Provencher L, Puglisi F, Harbeck N, Steger GG, Schneeweiss A, Wardley AM, Chlistalla A, Romieu G (2010) Phase III study of bevacizumab plus docetaxel compared with placebo plus docetaxel for the first-line treatment of human epidermal growth factor receptor 2-negative metastatic breast cancer. J Clin Oncol 28:3239–3247
Miller K, Wang M, Gralow J, Dickler M, Cobleigh M, Perez EA, Shenkier T, Cella D, Davidson NE (2007) Paclitaxel plus bevacizumab versus paclitaxel alone for metastatic breast cancer. N Engl J Med 357:2666–2676
Valero V, Forbes J, Pegram MD, Pienkowski T, Eiermann W, von Minckwitz G, Roche H, Martin M, Crown J, Mackey JR, Fumoleau P, Rolski J, Mrsic-Krmpotic Z, Jagiello-Gruszfeld A, Riva A, Buyse M, Taupin H, Sauter G, Press MF, Slamon DJ (2011) Multicenter phase III randomized trial comparing docetaxel and trastuzumab with docetaxel, carboplatin, and trastuzumab as first-line chemotherapy for patients with HER2-gene-amplified metastatic breast cancer (BCIRG 007 study): two highly active therapeutic regimens. J Clin Oncol 29:149–156
Lavoie Smith EM, Pang H, Cirrincione C, Fleishman SB, Paskett ED, Fadul CE, Knox C, Shapiro CL, Gilman P, Cancer and Leukemia Group B (2012) CALGB 170601: a phase III double blind trial of duloxetine to treat painful chemotherapy-induced peripheral neuropathy (CIPN). J Clin Oncol 30(Suppl). Abstract no. CRA 9013
Kottschade LA, Sloan JA, Mazurczak MA, Johnson DB, Murphy BP, Rowland KM, Smith DA, Berg AR, Stella PJ, Loprinzi CL (2011) The use of vitamin E for the prevention of chemotherapy-induced peripheral neuropathy: results of a randomized phase III clinical trial. Support Care Cancer 19:1769–1777
Grothey A, Nikcevich DA, Sloan JA, Kugler JW, Silberstein PT, Dentchev T, Wender DB, Novotny PJ, Chitaley U, Alberts SR, Loprinzi CL (2011) Intravenous calcium and magnesium for oxaliplatin-induced sensory neurotoxicity in adjuvant colon cancer: NCCTG N04C7. J Clin Oncol 29:421–427
Grothey A, Hart LL, Rowland KM, Ansari RH, Alberts SR, Chowhan NM, Shpilsky A, Hochster HS (2008) Intermittent oxaliplatin (oxali) administration and time-to-treatment-failure (TTF) in metastatic colorectal cancer (mCRC): final results of the phase III CONcePT trial. J Clin Oncol 26(Suppl). Abstract no. 4010
Barton DL, Wos EJ, Qin R, Mattar BI, Green NB, Lanier KS, Bearden JD III, Kugler JW, Hoff KL, Reddy PS, Rowland KM Jr, Riepl M, Christensen B, Loprinzi CL (2011) A double-blind, placebo-controlled trial of a topical treatment for chemotherapy-induced peripheral neuropathy: NCCTG trial N06CA. Support Care Cancer 19:833–841
Calhoun EA, Welshman EE, Chang CH, Lurain JR, Fishman DA, Hunt TL, Cella D (2003) Psychometric evaluation of the Functional Assessment of Cancer Therapy/Gynecologic Oncology Group-Neurotoxicity (Fact/GOG-Ntx) questionnaire for patients receiving systemic chemotherapy. Int J Gynecol Cancer 13:741–748
Acknowledgments
Medical writing assistance was provided by Christopher Carter, PhD, MediTech Media, funded by Celgene Corporation. The authors are fully responsible for the content and editorial decisions for this manuscript.
Conflict of interest
E. R. and M. C. have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution License which permits any use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
About this article
Cite this article
Rivera, E., Cianfrocca, M. Overview of neuropathy associated with taxanes for the treatment of metastatic breast cancer. Cancer Chemother Pharmacol 75, 659–670 (2015). https://doi.org/10.1007/s00280-014-2607-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00280-014-2607-5