Abstract
Objective
This study aims to evaluate the differences between The balloon catheter method and End-hole Catheter Method in measuring hepatic venous pressure gradient (HVPG) among cirrhosis patients.
Methods
From October 2017 to January 2024, patients who underwent HVPG measurements using both methods were consecutively included. HVPGs obtained from both methods were compared with the portal vein pressure gradient (PPG) obtained via transjugular intrahepatic portosystemic shunt (TIPS) using paired comparisons. Additionally, the consistency and predictive ability for bleeding risk of the two methods, as well as the impact of intrahepatic veno-venous shunt (IHVS), were analyzed.
Results
The study enrolled 145 patients, each of whom had HVPG measured by both methods. PPG was measured in 61 patients. There was a statistically significant difference between the PPGs and HVPGs measured by both the balloon catheter method and the end-hole catheter method (P < 0.001), with the HVPG mean values obtained by the end-hole catheter method being closer to the PPGs. In the non-IHVS group, no significant statistical difference was found between the two methods (P = 0.071). In contrast, the IHVS group showed a significant difference (P < 0.001), with a mean difference of 2.98 ± 4.03 mmHg. When IHVS was absent, the measurement results from the end-hole catheter method and the balloon catheter method were found to be highly correlated. The end-hole catheter method has a higher screening capability for patients at risk of bleeding compared to the balloon catheter method (75.90% vs. 72.86%).
Conclusion
HVPG measurements using either the balloon catheter method or end-hole catheter method showed significant difference with the PPG. The end-hole catheter method has a higher screening capability for patients at risk of bleeding, and IHVS could lead to lower HVPG measurements with The balloon catheter method.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Clinically, Portal hypertension (PH) manifests in various severe conditions, including ascites, esophageal-gastric varices, and hepatic encephalopathy, significantly impacting the quality of life and prognosis of affected individuals. Among these, variceal bleeding is a particularly grave complication, with a high mortality rate of 15–20% when it occurs [1]. This life-threatening event underscores the critical need for accurate assessment and monitoring of portal pressure.
HVPG is utilized to assess portal hypertension by measuring the difference between WHVP (Wedged Hepatic Venous Pressure) and FHVP (Free Hepatic Venous Pressure). Due to the high risks of trauma and bleeding associated with direct portal vein puncture and its strong correlation with portal hypertension, HVPG has become the gold standard for assessing portal pressure [2,3,4]. Based on HVPG measurements, clinicians stratify patients with portal hypertension, applying different management strategies for each stage [5]. Thus, HVPG measurements are crucial for managing and planning treatment in patients with cirrhosis. However, the presence of intrahepatic venous shunts (IHVS) can lead to an underestimation of WHVP, consequently affecting the accuracy of HVPG measurements obtained through this method [6,7,8]. Studies indicate that IHVS, seen in about 36.5% to 55.0% of cirrhosis patients, can reduce the HVPG measured by the balloon method by more than 5 mmHg [6,7,8,9], reducing the accuracy in assessing bleeding risks in patients with portal hypertension. The end-hole catheter method, by selectively cannulating and avoiding shunting venous branches, can effectively overcome this issue and accurately assess portal pressure in these patients [10]. Despite its advantages, there has been debate over the reliability and accuracy of the end-hole catheter method. Bosch et al. [11] suggested that the balloon method might offer more accurate readings by occluding a larger liver area. Smith et al. [10] observed minor differences between the methods, with the balloon method yielding slightly higher WHVP values. Zipprich et al. [12] reported lower variability and more stable values in the balloon method in their study of 47 patients. However, these studies did not clarify the specific differences between the balloon and End-hole Catheter Methods when IHVS is present, nor did they determine the impact of IHVS on predicting bleeding risks or detail their correlation with PPG.
This study is aimed at comparing HVPG measurements obtained using both the balloon catheter and end-hole catheter methods in the same patients, with an analysis of their characteristics and consistency being conducted. Additionally, the predictive ability of both methods for assessing bleeding risk in patients with portal hypertension is evaluated. By comparing these measurements with PPG, the accuracy of each method in evaluating the severity of portal hypertension is also analyzed. This comparison is essential for enhancing clinical decision-making and improving the management of patients with cirrhosis and portal hypertension.
Materials and Methods
Study Participants
Between October 2017 and January 2023, our center consecutively included patients diagnosed with cirrhosis either through imaging studies (ultrasound, CT, or MRI) or liver biopsy, who also underwent HVPG measurement via both the balloon catheter and end-hole catheter methods. Cirrhosis imaging characteristics are identified as an uneven liver surface, widened liver fissures, disproportionate liver lobes, reduced liver volume, and splenomegaly [13]. The inclusion criteria: individuals with cirrhotic portal hypertension, a patent right jugular vein, the ability to lie flat during the procedure, and no history of contrast agent allergy. Exclusion criteria: hepatic vein stenosis, coagulopathy, portal vein thrombosis, pregnancy, cardiac or renal failure, and constrictive pericarditis. All patients or their family members provided informed consent prior to the measurement, and the study received ethical committee approval (2019-P2-165–01).
HVPG Measurement
The procedures were performed by the same group of two experienced interventional physicians, each with over five years of experience, guided by the 2018 Chinese standards for measuring hepatic venous pressure gradient [14]. All patients were required to fast for at least 6 h before the procedure.
End-Hole Catheter Method
A 6F vascular sheath was inserted into the right jugular or femoral vein, followed by the introduction of a 5F H1 catheter (Cook Medical, USA) with a guidewire for selective hepatic vein cannulation. The tip of the catheter was positioned 2–4 cm from the inferior vena cava. The pressure transducer (Mindray Bio-Medical Electronics Co., Ltd., China) was calibrated with the ‘zero pressure’ point set at the mid-axillary line level. The blood was cleared by injecting 5 ml of saline, following which the Free Hepatic Venous Pressure (FHVP) was measured using the pressure transducer. The catheter and guidewire were advanced to the hepatic vein's small branches, with slow hand injection of contrast confirming a satisfactory wedged position (no contrast reflux or venous shunt, and visualization of liver parenchyma or small portal veins) (Fig. 1). Following contrast clearance, WHVP was measured. This measurement was repeated at least twice in the right or middle hepatic vein. When the variation in measurements was 1.00 mmHg or less, the average of these readings was recorded as the Wedged Hepatic Venous Pressure (WHVP). If the variation exceeded 1.00 mmHg, a third measurement was conducted, and the average of all three readings was determined as the WHVP. For patients with intrahepatic venous shunts, WHVP was measured using selective cannulation to bypass these shunts.
During contrast injection, the End-hole Catheter Method reveals hepatic parenchymal staining (A) or visualization of portal vein branches (B, marked with red arrows), with no observed reflux or intrahepatic venous shunting. With The balloon catheter method, stagnation of contrast material within the hepatic vein is visible, without any observed reflux or intrahepatic venous shunting (C). Hepatic venography shows shunting between the right hepatic vein and the middle hepatic vein (D)
Balloon Catheter Method
This method followed the same cannulation procedure as the end-hole catheter method. A 5.5 F compliant balloon catheter (Fogarty catheter, Edwards Lifesciences, USA) was inserted along an exchange guidewire. FHVP was measured approximately 2–4 cm from the inferior vena cava. Upon inflating the balloon to occlude the hepatic vein completely (hand injection of contrast showed no reflux or venous shunt, and contrast stagnation within the hepatic vein) (Fig. 1C), WHVP was measured after clearing the contrast. This process was repeated for at least twice, and the average of these measurements was considered as the final WHVP if the variation was less than or equal to 1.00 mmHg; otherwise, a third measurement was taken, and the average of all three readings was determined as the WHVP.
PPG Measurement
A vascular sheath was placed after puncturing the right jugular vein. FHVP was acquired as above. The portal vein branch was punctured via the right or middle hepatic vein with the Rups100 (Cook, America), and an exchange guidewire is inserted. The catheter is inserted along the guidewire to the main portal trunk to measure the portal pressure (PV). PPG is the difference of the PV and PPG.
Statistical Methods
Continuous data were presented as \(\overline{x }\)± s and analyzed using the independent samples t-test or Mann–Whitney U test. Categorical data were represented as cases (percentage, %) and compared with the χ2 test or Fisher's exact test. The paired samples t-test was employed for comparing measurements between the two methods. Pearson's correlation analysis was used to assess correlations, while Bland–Altman’s analysis was adopted to evaluate the consistency of measurements between groups. Statistical analyses were conducted using SPSS 22.0 and R 4.2.1, with a significance level set at P < 0.05.
Results
Patient Characteristics
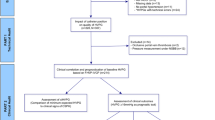
A total of 192 patients were initially screened. Among these, 145 patients qualified for inclusion in the study, as detailed in Table 1. Details of the patient screening process can be found in Fig. 2. Notably, 36 patients (24.83%) were found to have intrahepatic veno-venous shunt (IHVS). In the HVPG measurements conducted using The balloon catheter method, 8 patients had an HVPG between 5.00 and 10.00 mmHg, while the remaining 28 patients had an HVPG greater than 10.00 mmHg.
Measuring outcome of Balloon Catheter Method and End-Hole Catheter Method
The balloon catheter method was applied after occluding the hepatic vein with a balloon, followed by high-pressure injection angiography (flow rate 5 ml/s, pressure 300 psi, iodixanol 15 ml) to examine the collateral circulation. This procedure identified 36 patients with IHVS (Fig. 1D). Despite challenges in bypassing IHVS through selective cannulation, these patients were still assessed using the standard pressure measurement protocol. During this process, 17 patients experienced transient radiating right shoulder pain, which subsided after balloon deflation. There were no other reported complications related to the procedure.
In End-Hole Catheter Method, three patients initially showed extreme pressure values (greater than 73.53 mmHg), likely caused by the catheter tip’s adherence to the vessel wall. These outlier values were excluded, and subsequent remeasurements provided stable HVPG values. For the 36 patients with IHVS, selective cannulation effectively avoided shunting veins, leading to reliable HVPG measurements. No adverse effects related to the procedure were observed in this group.
Comparison of PPG and HVPG
PPG was measured in 61 patients. The differences between PPG and HVPG, as measured by The balloon catheter method and the end-hole catheter method, were 5.07 ± 4.40 mmHg and 3.95 ± 1.89 mmHg, respectively. There was a statistically significant difference between the HVPG measurements obtained by both methods compared to PPG (P < 0.001), with HVPG values from both methods being lower than PPG.
3.4. Comparison of Balloon Catheter Method and End-Hole Catheter Method
HVPG was measured in all 145 patients using both the balloon and end-hole catheter methods. The balloon method yielded an HVPG of 12.62 ± 4.73 mmHg, and the end-hole method yielded 12.80 ± 5.74 mmHg. The statistical analysis indicated no significant difference between these measurements (P = 0.492, 95% CI: -0.34, 0.71). Patients were then further analyzed based on IHVS status. In the non-IHVS group of 109 patients, the HVPG results were 12.31 ± 4.77 mmHg for the balloon method and 11.83 ± 5.27 mmHg for the end-hole method, showing no significant statistical difference (P = 0.070, 95% CI: -1.02, 0.04) (Fig.3). Meanwhile, among the 36 patients with IHVS, a significant difference in measured HVPG was noted between the two groups. The balloon method showed an HVPG of 13.53 ± 4.82 mmHg, while the end-hole method showed 15.75 ± 5.17 mmHg (P = 0.001, 95% CI: 0.10, 3.44), with a mean difference of 2.22 ± 2.62 mmHg (Fig.4).
3.5 Consistency Analysis Between the Two Methods
When IHVS was absent, the measurement results from the end-hole catheter method and The balloon catheter method were found to be highly correlated (r = 0.850; P < 0.001). In 105 cases (96.33%), the differences in measurements fell within the range of M ± 1.96 SD, indicating good overall consistency (Fig.5). This robust consistency in measurement results between the two methods was observed regardless of the presence of clinically significant portal hypertension.
Impact of Two Methods on Bleeding Risk Prediction
Among the enrolled patients, 68 had a history of bleeding. Based on whether the HVPG was greater than 12 mmHg, patients were stratified into high-risk (HVPG > 12 mmHg) and low-risk (HVPG < 12 mmHg) groups for bleeding. Using The balloon catheter method, there were 70 patients in the high-risk group, with 72.86% (51/70) having a history of bleeding; in the low-risk group of 75 patients, 25.33% (19/75) had a history of bleeding, showing a significant difference in bleeding probability between the two groups (P < 0.001). The detection rate of this method for patients with a history of bleeding was 72.86% (51/70). Correlation analysis showed a significant relationship between risk stratification and bleeding history, with a correlation coefficient of 0.475.
Using the end-hole catheter method, there were 83 patients in the high-risk group, with 75.90% (63/83) having a history of bleeding; in the low-risk group of 62 patients, 11.29% (7/62) had a history of bleeding, showing a significant difference in bleeding probability between the two groups (P < 0.001). The detection rate for this method for patients with a history of bleeding was 90% (63/70). Correlation analysis showed a significant relationship between risk stratification and bleeding history, with a correlation coefficient of 0.640.
In patients with HVPG (measured by balloon method) less than 12 mmHg, IHVS was observed in 22 cases. When using the end-hole catheter method to measure HVPG while avoiding IHVS, 12 cases (54.55%) were found to be greater than 12 mmHg, representing a false-negative rate of 8.28%. Among these patients, nine had a history of bleeding. When IHVS was observed during angiography and pressure was measured using the end-hole catheter method for correction, there were 82 patients in the high-risk group, with 73.17% (60/82) having a history of bleeding; in the low-risk group of 63, 15.87% (10/63) had a history of bleeding. Correlation analysis showed a significant relationship between risk stratification and bleeding history, with a correlation coefficient of 0.568.
Discussion
The Hepatic Venous Pressure Gradient (HVPG) reflects pressures within the hepatic sinusoids and portal veins [15], and serves as an alternative “gold standard” to assessing the severity of portal hypertension. It’s crucial in evaluating fibrosis stages, aiding in treatment selection, prognosticating liver transplantation, and predicting risks associated with liver cancer and decompensated cirrhosis [16,17,18,19,20,21,22,23,24,25,26]. HVPG measurements can be acquired through both The balloon catheter method and the end-hole catheter method. However, their accuracy in measuring WHVP or HVPG remains controversial. Our study, which employed both methods to measure HVPG in the same group of patients, found no statistical difference between the two sets of values.
Reducing portal pressure according to HVPG can significantly increase patient survival rates [27], making accurate and reliable pressure measurements vital for clinical practice. Previous studies have extensively examined both methods. During measurement, IHVS was observed in approximately 36.5% to 55.0% of cirrhosis patients [6,7,8,9], which could reduce HVPG measured by the balloon method by more than 5 mmHg, thereby affecting its accuracy. However, these studies were not comparative analyses of the two methods on the same patients; they only demonstrated that IHVS could cause The balloon catheter method to underestimate HVPG. In this study, a paired analysis of HVPG measurements was conducted using both methods on the same patients, and the differences in values obtained were compared. Stratified analysis revealed significant differences in measurements from the same patient with IHVS, with the balloon method generally showing lower pressures. IHVS was more common in patients with HVPG > 5 mmHg, and the probability of IHVS increased with higher HVPG, indicating that the balloon method's accuracy decreases with severe cirrhosis and higher portal pressure. The end-hole catheter method, also known as the non-balloon or catheter method, allows for selective pressure measurement in non-shunting venous branches, overcoming the influence of IHVS and correlating well with portal pressure [28], suggesting a broader application for this method.
HVPG is particularly significant in evaluating the risk of variceal hemorrhage [29]. However, the accuracy of HVPG also impacts the assessment of bleeding risk. In this study, an HVPG greater than 12 mmHg was considered indicative of high bleeding risk. Among high-risk patients assessed using The balloon catheter method, 72.86% had a history of bleeding, while 75.90% of high-risk patients assessed using the end-hole catheter method had a history of bleeding. A comparison of the two methods showed that the end-hole catheter method had a higher capability in identifying patients at risk of bleeding. Additionally, in The balloon catheter method, 12 cases were identified as false negatives due to the presence of IHVS, and combining it with the end-hole catheter method improved the detection rate of patients at risk of bleeding.
WHVP, the hydrostatic pressure after occluding the main trunk of the middle or right hepatic vein, is considered the average WHVP of numerous venous branches. Therefore, theoretically, the WHVP measurements by the balloon and end-hole catheter methods should be consistent, and thus the HVPG would not differ. However, Zipprich et al.[12] found that the end-hole method's measurements were less stable and less reliable. Based on our center's experience, the observed variability in measurements can be attributed primarily to the suboptimal placement of the catheter for wedging. Directly advancing the catheter for wedge pressure measurements often resulted in incomplete occlusion of small veins, leading to notable pressure fluctuations. Guiding the catheter to an optimal wedge position using a guidewire, while simultaneously cannulating a hepatic vein branch close to the mid-axillary line, may overcome the issue of unstable pressure measurements. This technique is one of the standardization requirements in our study.
Inevitably, there were limitations in this study. One limitation of our study is that both methods are influenced by gravity. When cannulating the posterior segment of the right liver, WHVP values are theoretically higher than in the anterior segment, potentially leading to elevated HVPG. Considering that the middle hepatic vein is closer to the mid-axillary line or the 'zero pressure' level, it is recommended as the preferred target vein for hepatic venous pressure measurement. Moreover, the number of patients with shunts in this study was relatively small. Although our stratified research indicated that IHVS affects the accuracy of the balloon method, the overall analysis of both methods did not show a statistical difference.
Conclusion
HVPG measurements using either the balloon catheter method or end-hole catheter method showed significant difference with the PPG. The end-hole catheter method has a higher screening capability for patients at risk of bleeding, and IHVS could lead to lower HVPG measurements with The balloon catheter method.
References
Procopet B, Berzigotti A. Diagnosis of cirrhosis and portal hypertension: imaging, non-invasive markers of fibrosis and liver biopsy. Gastroenterol Rep (Oxf). 2017;5(2):79–89.
Garcia-Tsao G, et al. Portal pressure, presence of gastroesophageal varices and variceal bleeding. Hepatology. 1985;5(3):419–24.
Groszmann RJ, et al. Hemodynamic events in a prospective randomized trial of propranolol versus placebo in the prevention of a first variceal hemorrhage. Gastroenterology. 1990;99(5):1401–7.
[Expert consensus on diagnosis and treatment of esophagogastric variceal bleeding in cirrhotic portal hypertension (2019 edition)]. Zhonghua Wai Ke Za Zhi, 2019. 57(12): p. 885–892.
de Franchis R, et al. Baveno VII - Renewing consensus in portal hypertension. J Hepatol. 2022;76(4):959–74.
Peng, R., et al., 04:21 PM Abstract No. 82 Wedged hepatic venous pressure as a surrogate for direct portal pressure: how accurate is it? Journal of Vascular and Interventional Radiology, 2019.
Wang T, et al. A computational model-based study on the exchangeability of hepatic venous pressure gradients measured in multiple hepatic veins. Med Eng Phys. 2020;84:28–35.
Ma J, et al. Impact of Intrahepatic Venovenous Shunt on Hepatic Venous Pressure Gradient Measurement. J Vasc Interv Radiol. 2020;31(12):2081–8.
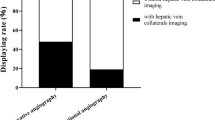
Lv YF, Song QK, Yue ZD, et al. The Impact of Hepatic Venous Collaterals on Hepatic Venous Pressure Gradient in Patients with Cirrhotic Portal Hypertension. Chinese Journal of Interventional Imaging and Therapy. 2023;20(2):86–90.
Smith TP, et al. Hepatic venous pressure measurements: comparison of end-hole and balloon catheter methods. J Vasc Interv Radiol. 2012;23(2):219-26.e6.
Bosch J, et al. The clinical use of HVPG measurements in chronic liver disease. Nat Rev Gastroenterol Hepatol. 2009;6(10):573–82.
Zipprich, A., et al., Comparison of balloon vs. straight catheter for the measurement of portal hypertension. Aliment Pharmacol Ther, 2010. 32(11–12): p. 1351–6.
Feng LM, et al. The evaluation of non-invasive multi-slice spiral computed tomography-based indices for the diagnosis and prognosis prediction of liver cirrhosis. J Dig Dis. 2017;18(8):472–9.
[Consensus on clinical application of hepatic venous pressure gradient in China (2018)]. Zhonghua Gan Zang Bing Za Zhi,. 26(11): p. 801-812.
Procopeţ B, Tantau M, Bureau C. Are there any alternative methods to hepatic venous pressure gradient in portal hypertension assessment? J Gastrointestin Liver Dis. 2013;22(1):73–8.
Lee E, et al. Comparison of hepatic venous pressure gradient and endoscopic grading of esophageal varices. World J Gastroenterol. 2016;22(11):3212–9.
Mandorfer M, et al. Changes in hepatic venous pressure gradient predict hepatic decompensation in patients who achieved sustained virologic response to interferon-free therapy. Hepatology. 2020;71(3):1023–36.
Bosch J, Iwakiri Y. The portal hypertension syndrome: etiology, classification, relevance, and animal models. Hepatol Int. 2018;12(Suppl 1):1–10.
Schwarzer R, et al. Carvedilol for reducing portal pressure in primary prophylaxis of variceal bleeding: a dose-response study. Aliment Pharmacol Ther. 2018;47(8):1162–9.
Vincent JK, et al. Hepatic venous pressure gradient correlates with advanced hepatic fibrosis: a retrospective review. Abdom Radiol (NY). 2017;42(11):2609–14.
Sourianarayanane A, et al. Stage of fibrosis and portal pressure correlation in nonalcoholic steatohepatitis. Eur J Gastroenterol Hepatol. 2017;29(5):516–23.
Ripoll C, et al. Hepatic venous pressure gradient predicts clinical decompensation in patients with compensated cirrhosis. Gastroenterol. 2007;133(2):481–8.
Libânio D, Marinho RT. Impact of hepatitis C oral therapy in portal hypertension. World J Gastroenterol. 2017;23(26):4669–74.
Ripoll C, et al. Hepatic venous pressure gradient predicts development of hepatocellular carcinoma independently of severity of cirrhosis. J Hepatol. 2009;50(5):923–8.
de Franchis R. Expanding consensus in portal hypertension: report of the baveno vi consensus workshop: stratifying risk and individualizing care for portal hypertension. J Hepatol. 2015;63(3):743–52.
Zhang PF, Chen YJ, Cao JL, et al. The value of hepatic venous pressure gradient in preoperative assessment and prognostic prediction of liver transplant recipients. Organ Transplant. 2023;14(1):154–9.
Villanueva C, et al. A randomized trial to assess whether portal pressure guided therapy to prevent variceal rebleeding improves survival in cirrhosis. Hepatology. 2017;65(5):1693–707.
Cheng Y, et al. Agreement between wedged hepatic venous pressure and portal pressure in hepatic sinusoidal obstruction syndrome. J Pers Med. 2022;13(1):4.
Zhang M, Zhuge YZ, Zou XP, et al. The hepatic venous wedge pressure and direct portal vein pressure and their correlation in 22 cases of cirrhosis. Chin J Digest. 2016;36(8):5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical Approval
The study received ethical committee approval (Bioethics Committee of Beijing Friendship Hospital Affiliated to Capital Medical University, No. 2019-P2-165-01).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yu, Ja., Yang, Sw., Wang, Y. et al. The Balloon Catheter Method and the End-hole Catheter Method in the Measurement of Hepatic Venous Pressure Gradient: a Comparative Study. Cardiovasc Intervent Radiol (2024). https://doi.org/10.1007/s00270-024-03814-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00270-024-03814-w