Abstract
Background
The hemodynamics of patients with cirrhosis and portal hypertension are complex and variable. We aimed to investigate differences in venous pressures determined by innovative angiography and conventional angiography using balloon occlusion of the hepatic veins in patients with alcoholic cirrhosis and portal hypertension.
Methods
A total of 134 patients with alcoholic cirrhosis who fulfilled the inclusion criteria from June 2017 to June 2020 were included. During transjugular intrahepatic portosystemic shunt, conventional and innovative angiography were performed, and venous pressures were measured. A paired t-test and Pearson’s correlation coefficient were used for analysis.
Results
Conventional and innovative hepatic angiography detected lateral branches of the hepatic vein in 26 (19.4%) and 65 (48.5%) cases, respectively (P < 0.001). Innovative angiography detected a total of 65 patients with lateral shunts, of whom 37 (56.9%) had initial shunts. The average wedged hepatic venous pressure and portal venous pressure of the initial lateral branches were 21.27 ± 6.66 and 35.84 ± 7.86 mmHg, respectively, with correlation and determination coefficients of 0.342 (P < 0.05) and 0.117, respectively. The mean hepatic venous pressure gradient and portal pressure gradient were 9.59 ± 7.64 and 26.86 ± 6.78 mmHg, respectively, with correlation and determination coefficients of 0.292 (P = 0.079) and 0.085, respectively.
Conclusions
Innovative angiography reveals collateral branches of the hepatic veins more effectively than conventional angiography. Hepatic vein collateral branches are the primary factors leading to underestimation of wedged hepatic venous pressures and hepatic venous pressure gradients, with the initial hepatic vein collateral branches resulting in the most severe underestimations.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Background
Hepatitis and alcoholism are common causes of cirrhotic portal hypertension [1, 2]. Hepatocytes are damaged by prolonged heavy drinking, and a series of pathological changes in the liver may occur, resulting in increased portal vein pressure and, eventually, leading to a series of clinical symptoms, such as esophageal gastric varices, gastrointestinal bleeding, and ascites [3, 4]. These symptoms are directly related to a gradual increase in portal vein pressure. The most accurate diagnosis and prognosis prediction for patients should be the direct measurement of portal vein pressure. However, precise measurement of portal vein pressure is complicated, traumatic, and technically demanding; therefore, it is difficult to routinely apply in clinical practice.
In recent years, the measurement of hepatic vein pressure in lieu of portal vein pressure has been used clinically and in research. The hepatic venous pressure gradient (HVPG) can be used as the "gold standard" to indirectly reflect the portal pressure gradient (PPG) [4,5,6,7]. Nevertheless, few studies have been conducted on the correlation between the HVPG and PPG in clinical practice. It has been suggested that there is a certain correlation between wedged hepatic venous pressure (WHVP) and portal venous pressure (PVP) in patients with portal hypertension and alcoholic cirrhosis [8], but these cases are limited. There is a standard for measuring hepatic venous pressure; injection of contrast agent (5 mL) after balloon occlusion of the hepatic vein is an important component of the standardized procedure for observing hepatic vein collateral branches and hepatic vein occlusion. It has been reported that the presence of collateral branches of the hepatic vein affects the accuracy of WHVP, but the detection rate is relatively low [9].
In this study, 134 patients with alcoholic cirrhosis and portal hypertension who fulfilled the inclusion criteria from June 2017 to June 2020 were enrolled for transjugular intrahepatic portosystemic shunt (TIPS) and underwent innovative hepatic venous angiography based on conventional measurement of hepatic venous pressure and angiography. Subsequently, we analyzed the correlation between the hepatic vein anatomy and venous pressure.
Methods
Patients
A total of 134 (males: 119 [88.8%], females: 15 [11.2%]; mean age: 55.02 ± 10.65 [range: 19–75] years) patients with alcoholic cirrhosis who fulfilled the inclusion criteria for portal hypertension underwent TIPS between January 2017 and June 2020. PPG and HVPG were obtained by measuring various pressures during the interventional surgery. There were 88 cases of gastrointestinal hemorrhage in patients with alcoholic cirrhosis and portal hypertension (65.7%), 35 cases of intractable ascites or pleural effusion combined with ascites (26.1%), and 11 cases of gastrointestinal bleeding with intractable ascites (8.2%). According to Child–Pugh classification, there were 36 grade A, 47 grade B, and 51 grade C cases. Fourteen cases of alcoholic cirrhosis with portal hypertension were complicated with liver cancer. The study protocol conforms to the ethical guidelines of the 1975 Declaration of Helsinki (6th revision, 2008) and was approved by the Ethics Committee of Beijing Shijitan Hospital (2018(01)). Informed consent was obtained from each patient included in the study.
Inclusion criteria
The inclusion criteria were as follows: 1) TIPS indications, 2) age 18–75 years, 3) presence of TIPS and undergoing elective surgery, and 4) normal hepatic vein and inferior vena cava.
Exclusion criteria
The exclusion criteria were as follows: 1) portal vein carcinoma thrombus, 2) arterioportal venous fistula, 3) portal vein thrombosis affecting blood flow (generally exceeding 1/3 of the portal vein), 4) use of drugs affecting portal vein pressure within the preceding week, and 5) presence of factors that affect the accuracy of intraoperative pressure measurement, such as biliary-cardiac reflex and incomplete balloon occlusion.
Method of pressure measurement
Preoperative preparation
Various examinations were conducted before the surgery, including routine blood examination, hepatorenal function, ICG-R15 (quantitative determination of liver function, retention rate of indocyanine green in 15 min), blood ammonia, blood type, electrocardiograph, coagulation function, portal vein ultrasound, and abdominal CT and/or magnetic resonance imaging. Coagulation function, platelet count, bilirubin, albumin, and hemoglobin levels should be adjusted according to the interventional surgery. The effects and risks of the surgery were explained to patients and their families, and consent for surgery was obtained. Medications affecting portal vein pressure were discontinued for at least one week preceding surgery.
Pressure measurement
Conventional methods of measuring pressure [10, 11]
Pressure was measured by catheterization of the right internal jugular vein to the right atrium, inferior vena cava, and hepatic vein under routine disinfection and local anesthesia. A Fogarty balloon catheter (Edward Company, USA) was inserted into the hepatic vein using an RUPS-100 outer sheath (COOK Company, USA). The tip of the balloon catheter was placed 3–5 cm from the hepatic vein to the opening of the inferior vena cava. WHVP and FHVP were measured before and after hepatic vein occlusion by expanding the balloon (contrast agent (5 mL) was carefully injected). The pressure was recorded after stabilization; the pressure measurement was repeated three times, and the average value was recorded; the HVPG value was then calculated. The liver parenchyma and portal vein were punctured through the hepatic vein or inferior vena cava. After successful portal vein puncture, a porcine tail catheter was inserted into the splenic or superior mesenteric vein for angiography. Before the shunt, the main portal vein pressure was measured three times; the average value was recorded and the PPG value was then calculated.
Innovative method of angiography
After completion of the standard measurement methods, the hepatic vein was blocked again by inserting a balloon at the same position as was done in the conventional method. The dose of contrast agent was increased (5 mL/s up to a total of 15 mL), and pressure angiography was performed; the pressure was 200–300 psi, and continuous angiography was performed for more than 6 s. Subsequently, subtraction was performed. The WHVP and free hepatic venous pressure (FHVP) were measured again; the pressure was recorded after stabilization, and the measurement was repeated three times; the average value was used to calculate the HVPG value.
Precautions
To observe the occlusion of the balloon catheter after balloon dilatation, if the blockage was incomplete, the position was adjusted and retested; radiography of the balloon catheter was performed. The indwelling catheter in the portal vein was inserted for 24–48 h; the portal vein pressure was measured at least three times per day. The pressures of the inferior vena cava and right atrium were measured three times during extubation, and the average value was recorded.
Statistical analysis
GraphPad Prism 8 (GraphPad, Inc., La Jolla, CA, USA) was used for the statistical analysis. The paired t-test was used to analyze the differences between WHVP and PVP, PPG and HVPG, and FHVP and IVCP. The Pearson correlation test was applied to analyze the correlation and determination coefficients. Blood pressures are expressed as means ± standard deviations. P < 0.05 was considered statistically significant.
Results
Differences between conventional and innovative angiography
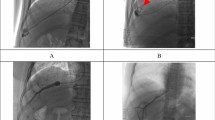
Conventional and innovative hepatic angiography detected hepatic vein collateral branches in 26 (19.4%) and 65 (48.5%) cases, respectively. The difference was statistically significant (P < 0.001) (Fig. 1).
Individual pressure correlations in patients with collateral vessels detected by conventional angiography
Twenty-six patients with collateral branches underwent conventional angiography (Fig. 2A). The average WHVP and PVP were 20.89 ± 6.69 and 34.96 ± 8.08 mmHg (Table 1); the correlation and determination coefficients were 0.303 (P = 0.133) and 0.092, respectively (Fig. 3A). The average HVPG and PPG were 9.86 ± 7.44 and (25.94 ± 7.42) mmHg, respectively (Table 2). The coefficients of correlation and determination were 0.208 (P = 0.309) and 0.043, respectively (Fig. 4A).
Pressure relationships between venous pressure in patients undergoing conventional angiography. A With lateral hepatic vein development and (B) Without lateral hepatic vein development (WHVP, wedged hepatic venous pressure; PVP, portal venous pressure; HVPG, hepatic venous pressure gradient; PPG, portal pressure gradient)
Correlation between WHVP and PVP under different collateral development methods. A patients with collateral vessels detected by conventional angiography, (B) patients with portal vein visualization using innovative angiography, and (C) patients without visualization using innovative angiography (WHVP, wedged hepatic venous pressure; PVP, portal venous pressure; HVPG, hepatic venous pressure gradient; PPG, portal pressure gradient)
Correlation between HVPG and PPG under different collateral development methods. A patients with collateral vessels detected by conventional angiography, (B) patients with portal vein visualization using innovative angiography, and (C) patients without visualization using innovative angiography (WHVP, wedged hepatic venous pressure; PVP, portal venous pressure; HVPG, hepatic venous pressure gradient; PPG, portal pressure gradient)
Initial shunt: the most significant factor causing underestimation of WHVP and HVPG in innovative angiography
Among the 65 patients with lateral branches detected by innovative angiography, 37 cases (56.9%) (Fig. 5A) possessed initial shunts, 22 cases (33.8%) (Fig. 5B) had mid-term shunts, and 6 cases (9.2%) (Fig. 5C) exhibited late shunts (Fig. 6). For the initial shunt, average WHVP and PVP were 21.27 ± 6.66 and 35.84 ± 7.86 mmHg, respectively, with determination coefficients of 0.342 (P = 0.038) and 0.117, respectively (Table 1). The HVPG and PPG were 9.59 ± 7.64 and 26.86 ± 6.78 mmHg, respectively, with correlation and determination coefficients of 0.292 (P = 0.079) and 0.085, respectively (Table 2). For the middle shunts, the mean WHVP and PVP were 28.79 ± 6.94 and 35.64 ± 4.51 mmHg, respectively, with correlation and determination coefficients of 0.208 (P = 0.353) and 0.043, respectively (Table 1). The average HVPG and PPG were 15.62 ± 5.39 and 26.23 ± 5.70 mmHg, respectively, with correlation and determination coefficients of 0.264 (P = 0.236) and 0.069, respectively (Table 2). The mean WHVP and PVP of hepatic collaterals in cases with late shunts were 30.50 ± 8.31 and 34.83 ± 8.11 mmHg, respectively, with correlation and determination coefficients of 0.995 (P < 0.001) and 0.991, respectively (Table 1). The average HVPG and PPG were 17.00 ± 10.02 and 27.33 ± 7.97 mmHg, respectively with correlation and determination coefficients of 0.779 (P = 0.068) and 0.607, respectively (Table 2).
Five different development states under innovative angiography. A Initial hepatic vein collateral formation, (B) Mid-term hepatic vein collateral formation, (C) Late hepatic vein collateral formation, (D) Portal vein imaging, and (E) Absence of hepatic vein collateral branches. *Note: the hepatic vein in innovative angiography: (1) initial shunt: collateral visualization was seen within 2 s after beginning angiography; (2) mid-term shunt: collateral visualization was seen 3–4 s after initiating angiography; (3) late shunt: collateral visualization was seen 5–6 s after beginning angiography; (4) visualization of the portal vein: visualization of the portal vein in the process of angiography; (5) no collateral branches: no collateral visualization in the process of angiography
Venous pressure without collaterals on conventional angiography
There were 108 patients (81.6%) without collateral branches on conventional hepatic venography (Fig. 2B). The average WHVP and PVP were 30.65 ± 8.17 and 33.25 ± 6.60 mmHg, respectively, with correlation and determination coefficients of 0.368 (P < 0.001) and 0.135, respectively. The mean HVPG and PPG were 18.67 ± 9.05 and 24.44 ± 6.79 mmHg, respectively, with correlation and determination coefficients of 0.263 (P = 0.006) and 0.069, respectively.
Innovative angiography for various venous pressure situations without collateral vessels
Sixty-nine patients (51.5%) underwent innovative hepatic venography without detection of collaterals, including 45 patients (65.2%) (Fig. 7A) with portal vein visualization (Fig. 5D) and 24 patients (34.8%) (Fig. 7B) without visualization (Fig. 5E). The mean WHVP and PVP of the 45 patients with portal vein imaging were 31.07 ± 7.53 and 32.39 ± 6.58 mmHg (Table 1), respectively, with correlation and determination coefficients of 0.800 (P < 0.001) and 0.640, respectively (Fig. 3B). The average HVPG and PPG were 20.18 ± 8.31 and 23.99 ± 6.75 mmHg (Table 2), with correlation and determination coefficients of 0.638 (P < 0.001) and 0.407, respectively (Fig. 4B). The mean WHVP and PVP of the 24 patients without portal vein visualization were 35.49 ± 7.78 mmHg and 30.13 ± 6.01 mmHg (Table 1), respectively, with correlation and determination coefficients of 0.570 (P = 0.004) and 0.325, respectively (Fig. 3C). The average HVPG and PPG were 23.50 ± 9.30 and 20.83 ± 6.78 mmHg (Table 2), respectively, with correlation and determination coefficients of 0.334 (P = 0.111) and 0.111, respectively (Fig. 4C).
Pressure relationships in 69 patients without collateral branches on innovative hepatic angiography. A With portal vein imaging and (B) Without portal vein imaging (WHVP, wedged hepatic venous pressure; PVP, portal venous pressure; HVPG, hepatic venous pressure gradient; PPG, portal pressure gradient)
Discussion
Alcoholic cirrhosis is a common cause of portal hypertension. Hemodynamic changes in portal hypertension caused by pathological changes in alcoholic cirrhosis occur mainly in the hepatic sinus, resulting in portal vein resistance and increased blood volume [12, 13]. Normal liver hemodynamics are that the PVP is higher than or equal to the hepatic sinusoidal pressure, WHVP is equal to the hepatic sinusoidal pressure, and the FHVP is higher than the IVCP by 0.5–1.0 mmHg [14,15,16]. PPG is more meaningful and accurate than PVP in predicting the risk of complications associated with portal hypertension [17]. Theoretically, the HVPG can accurately reflect the PPG. It is preferred to represent PPG because it is simple, is associated with minimal trauma, and is easily accepted by patients [4, 18, 19]. There are significant changes in the structure of the liver tissue, hepatic lobules, and microvessels in patients with alcoholic cirrhosis and portal hypertension [2, 20, 21]. In pathological conditions and clinical practice, whether WHVP accurately represents PVP remains controversial in reports [22].
However, it has rarely been reported whether the HVPG represents PPG. The basic principle of measuring WHVP is that after the hepatic vein is completely blocked by a balloon, hepatic vein pressure gradually increases until it achieves the pressure of the hepatic sinuses; this accurately represents the pressure of the hepatic sinuses [22, 23]. However, in the process of measurement, certain objective and subjective factors can impede accurate measurement. For example, in the presence of collateral branches of the hepatic vein, the blood does not achieve the pressure of the hepatic sinusoid, but blood flows from the collateral branches to other hepatic veins or accessory hepatic veins into the inferior vena cava, or may even flow away quickly in the preliminary stage [16, 24]. In addition, among the subjective factors, if balloon sealing is insufficient to enable the pressure of the hepatic sinusoid to be reached and the front end of the balloon catheter is not free in the blood vessel, the accuracy of the measured pressure is directly affected. Based on the principle of measuring WHVP, as long as lateral branches of the hepatic vein exist, it is possible that the WHVP will not truly represent the pressure of the hepatic sinus.
By using innovative hepatic venography in this study, we detected more collateral branches of the hepatic vein (48.5%) than those identified using the conventional method (19.4%). Furthermore, in patients with collateral branches of the hepatic vein, the WHVP was significantly lower than the PVP and HVPG was significantly lower than PPG. Hepatic vein collateral flow is the key factor causing underestimation of WHVP and HVPG. Moreover, our analysis revealed that hepatic vein collateral branches appeared at the three shunt levels, and this underestimation was more obvious the earlier the shunt appeared. In addition to identifying more cases with hepatic vein collaterals, 45 patients (33.6% of total cases) underwent portal vein imaging in the innovative hepatic venography group in this study. The correlation between WHVP and PVP in these patients was good, and the same was true for the HVPG and PPG. This was because the pressure of the hepatic vein increased after it was filled with the contrast agent. When the pressure of the hepatic vein was balanced with that of the hepatic sinus, the contrast agent entered the portal vein through the hepatic sinus countercurrent, which enabled portal vein imaging, indicating that the hepatic sinus pressure was roughly equal to the portal vein pressure. Furthermore, 24 patients (17.9% of the total cases) had no hepatic vein collateral branches. The mean WHVP of these patients (35.49 ± 7.78 mmHg) was higher than the mean PVP (30.13 ± 6.01 mmHg), with correlation and determination coefficients of 0.570 (P = 0.004) and 0.325, respectively. The mean HVPG (23.50 ± 9.30 mmHg) was higher than the PPG (20.83 ± 6.78 mmHg); the correlation and determination coefficients were 0.334 (P = 0.111), and 0.111, respectively. Since the hepatic vein was perfused with contrast medium, the hepatic venous pressure gradually increased, and the contrast medium could not enter the portal vein through the hepatic sinusoids (possibly the blood of the hepatic sinusoids is mainly supplied by the hepatic artery) because of the higher hepatic sinusoidal pressure. The contrast medium was retained in the hepatic vein and could not enter the portal vein or the hepatic venous collateral return. Therefore, the absence of collateral branches of the hepatic vein is an important reason for the overestimation of WHVP and HVPG. Studies [9, 25, 26] have reported that patients with WHVP higher than PVP have adverse hepatic blood flow, umbilical vein opening, portocaval anastomotic branches, and gastro-renal shunts. Among the patients in this study, only two had this condition.
Regarding the measurement of free pressure in the inferior vena cava, hepatic vein, and portal vein, the factors affecting the accuracy of measurement are mainly subjective [19, 25, 27]. For example, preoperative health education should be incorporated so that patients can be fully prepared psychologically. Patients who choose an elective operation should be prepared, and patients with massive ascites should ensure drainage of the ascites appropriately and discontinue drugs that affect venous pressure (non-selective beta-blockers influence PVP [28,29,30], deep sedation using propofol impacts the PPG in patients [31, 32]). During the surgery, the accuracy of the pressure measurement was also affected by the use of local anesthesia and the consistent position of the catheter for multiple pressure measurements. Therefore, it is imperative to pay special attention to patients with the biliary-cardiac reflex and incomplete balloon occlusions. These patients should be excluded if these conditions cannot be corrected.
Conclusions
In conclusion, innovative hepatic vein angiography can identify more cases of hepatic vein collateral branches in alcoholic cirrhosis with portal hypertension than conventional angiography. Hepatic vein collateral branches are the key factors leading to underestimation of WHVP and HVPG, of which the initial hepatic vein collateral branches exhibit the most profound impact, followed by the middle and late hepatic vein collateral branches. Additionally, this innovative method demonstrated good correlation of WHVP with PVP and HVPG with PPG in patients with portal vein visualization. The absence of hepatic vein collaterals is an important factor resulting in the overestimation of the WHVP and HVPG. However, whether additional factors exist requires further investigation. The total amount of contrast agent needed, injection dose (per second), and injection pressure that are most appropriate for innovative angiography also deserve further investigation.
Availability of data and materials
The data that support the findings of this study are available from the corresponding author, upon reasonable request.
Abbreviations
- HVPG:
-
Hepatic venous pressure gradient
- PPG:
-
Portal pressure gradient
- WHVP:
-
Wedged hepatic venous pressure
- PVP:
-
Portal venous pressure
- TIPS:
-
Transjugular intrahepatic portosystemic shunt
- FHVP:
-
Free hepatic venous pressure
- IVCP:
-
Inferior vena cava pressure
References
Garcia-Tsao G, Lim JK. Management and treatment of patients with cirrhosis and portal hypertension: recommendations from the Department of Veterans Affairs Hepatitis C Resource Center Program and the National Hepatitis C Program. Am J Gastroenterol. 2009;104:1802–29.
Chen J, Argemi J, Odena G, et al. Hepatic lipocalin 2 promotes liver fibrosis and portal hypertension. Sci Rep. 2020;10:15558.
Tsochatzis EA, Bosch J, Burroughs AK. Liver cirrhosis. Lancet. 2014;383:1749–61.
Bosch J, Abraldes JG, Berzigotti A, García-Pagan JC. The clinical use of HVPG measurements in chronic liver disease. Nat Rev Gastroenterol Hepatol. 2009;6:573–82.
de Franchis R. Expanding consensus in portal hypertension: report of the Baveno VI consensus workshop: stratifying risk and individualizing care for portal hypertension. J Hepatol. 2015;63:743–52.
Simonetto DA, Liu M, Kamath PS. portal hypertension and related complications: diagnosis and management. Mayo Clin Proc. 2019;94:714–26.
Wang T, Liang F, Zhou Z, Qi X. Global sensitivity analysis of hepatic venous pressure gradient (HVPG) measurement with a stochastic computational model of the hepatic circulation. Comput Biol Med. 2018;97:124–36.
Deplano A, Migaleddu V, Pischedda A, et al. Portohepatic gradient and portal hemodynamics in patients with cirrhosis due to hepatitis C virus infection. Dig Dis Sci. 1999;44:155–62.
Osada Y, Kanazawa H, Narahara Y, Mamiya Y, Nakatsuka K, Sakamoto C. Wedged hepatic venous pressure does not reflect portal pressure in patients with cirrhosis and hepatic veno-venous communications. Dig Dis Sci. 2008;53:7–13.
Consensus on clinical application of hepatic venous pressure gradient in China (2018). Chin J Clin Hepatol. 2018;34(12):2526–2536.
Reiberger T, Schwabl P, Trauner M, Peck-Radosavljevic M, Mandorfer M. Measurement of the hepatic venous pressure gradient and transjugular liver biopsy. J Vis Exp. 2020;(160).
Merkel C, Montagnese S. Hepatic venous pressure gradient measurement in clinical hepatology. Dig Liver Dis. 2011;43:762–7.
Aithal GP, Palaniyappan N, China L, et al. Guidelines on the management of ascites in cirrhosis. Gut. 2021;70:9–29.
Perelló A, Escorsell A, Bru C, et al. Wedged hepatic venous pressure adequately reflects portal pressure in hepatitis C virus-related cirrhosis. Hepatology. 1999;30:1393–7.
Boyer TD. Wedged hepatic vein pressure (WHVP): ready for prime time. Hepatology. 2006;43:405–6.
Rössle M, Blanke P, Fritz B, Schultheiss M, Bettinger D. Free hepatic vein pressure is not useful to calculate the portal pressure gradient in cirrhosis: a morphologic and hemodynamic study. J Vasc Interv Radiol. 2016;27:1130–7.
Turco L, Garcia-Tsao G. Portal hypertension: pathogenesis and diagnosis. Clin Liver Dis. 2019;23:573–87.
Groszmann RJ, Wongcharatrawee S. The hepatic venous pressure gradient: anything worth doing should be done right. Hepatology. 2004;39:280–2.
Qi X, Berzigotti A, Cardenas A, Sarin SK. Emerging non-invasive approaches for diagnosis and monitoring of portal hypertension. Lancet Gastroenterol Hepatol. 2018;3:708–19.
Steib CJ, Schewe J, Gerbes AL. Infection as a trigger for portal hypertension. Dig Dis. 2015;33:570–6.
Shah V, García-Cardeña G, Sessa WC, Groszmann RJ. The hepatic circulation in health and disease: report of a single-topic symposium. Hepatology. 1998;27:279–88.
Ferrusquía-Acosta J, Bassegoda O, Turco L, et al. Agreement between wedged hepatic venous pressure and portal pressure in non-alcoholic steatohepatitis-related cirrhosis. J Hepatol. 2021;74:811–8.
Silva-Junior G, Baiges A, Turon F, et al. The prognostic value of hepatic venous pressure gradient in patients with cirrhosis is highly dependent on the accuracy of the technique. Hepatology. 2015;62:1584–92.
Monroe EJ, Michalsky WS, Koo KSH, et al. Intrahepatic veno-venous collateralization and misrepresentative hepatic venous pressure gradients in children. Pediatr Radiol. 2020;50:1579–86.
Reverter E, Blasi A, Abraldes JG, et al. Impact of deep sedation on the accuracy of hepatic and portal venous pressure measurements in patients with cirrhosis. Liver Int. 2014;34:16–25.
Pomier-Layrargues G, Kusielewicz D, Willems B, et al. Presinusoidal portal hypertension in non-alcoholic cirrhosis. Hepatology. 1985;5:415–8.
Calvaruso V, Craxì A. Hepatic benefits of HCV cure. J Hepatol. 2020;73:1548–56.
Alvarado-Tapias E, Ardevol A, Garcia-Guix M, et al. Short-term hemodynamic effects of β-blockers influence survival of patients with decompensated cirrhosis. J Hepatol. 2020;73:829–41.
Groszmann RJ, Garcia-Tsao G, Bosch J, et al. Beta-blockers to prevent gastroesophageal varices in patients with cirrhosis. N Engl J Med. 2005;353:2254–61.
Villanueva C, Albillos A, Genescà J, et al. β blockers to prevent decompensation of cirrhosis in patients with clinically significant portal hypertension (PREDESCI): a randomised, double-blind, placebo-controlled, multicentre trial. Lancet. 2019;393:1597–608.
Lebrec D, Nouel O, Corbic M, Benhamou JP. Propranolol–a medical treatment for portal hypertension? Lancet. 1980;2:180–2.
Mandell MS, Durham J, Kumpe D, Trotter JF, Everson GT, Niemann CU. The effects of desflurane and propofol on portosystemic pressure in patients with portal hypertension. Anesth Analg. 2003;97:1573–7.
Acknowledgements
The authors would like to express their gratitude to all the medical staff of the Interventional Therapy Department of Beijing Shijitan Hospital affiliated to Capital Medical University for assisting in the collection of clinical data.
Funding
This research was supported by the Special Scientific Research Project for Health Development in The Capital (key scientific project-first publish 2018–1-2081); Scientific Research Program of Beijing Municipal Education Commission (KM201810025093).
Author information
Authors and Affiliations
Contributions
Bowen Liu: Study idea, writing, proofreading and manuscript preparation. Zhendong Yue, Ting Cui, Hongwei Zhao, Lei Wang and Zhenhua Fan: Data access and interpretation. Yifan Wu, Mingming Meng and Ke Zhang: Data analysis. Li Jiang, Huiguo Ding and Yuening Zhang: Image acquisition. Fuquan Liu: Final correction and review. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The research protocol followed every provision of the Declaration of Helsinki and was approved by the Ethics Committee of Beijing Shijitan Hospital (2018(01)). Written informed consent was obtained from all individual participants included in the study.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Liu, B., Yue, Z., Cui, T. et al. Innovative angiography: a new approach to discover more hepatic vein collaterals in patients with cirrhotic portal hypertension. BMC Gastroenterol 23, 144 (2023). https://doi.org/10.1186/s12876-023-02792-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12876-023-02792-6