Abstract
Magnetic resonance (MR) imaging can be used in the management of pediatric soft-tissue vascular anomalies for diagnosing and assessing extent of lesions and for evaluating response to therapy. MR imaging studies often involve a combination of T1- and T2-weighted images in addition to MR angiography and fat-suppressed post-contrast sequences. The MR imaging features of these vascular anomalies when combined with clinical findings can aid in diagnosis. In cases of complex vascular malformations and syndromes associated with vascular anomalies, MR imaging can be used to evaluate accompanying soft-tissue and bone anomalies. This article reviews the MR imaging protocols and appearances of the most common pediatric soft-tissue vascular anomalies.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Soft-tissue vascular anomalies in children are in many instances diagnosed on the basis of clinical findings. However in select cases imaging might be required for diagnosis or to assess lesion size and extent. This is most common in cases with atypical clinical presentation, those located in the deep soft tissues, or prior to pharmacological therapy, interventional radiologic treatment or surgical excision.
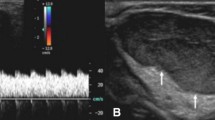
Although this article focuses on MR imaging features of pediatric soft-tissue vascular anomalies, it must be emphasized that ultrasonography (US) plays an important role in the imaging workup of these lesions. US is particularly important in the pediatric age group, especially in younger children, because it can establish diagnosis and can determine anatomical involvement of many lesions in the superficial soft tissues without the need for sedation or general anesthesia, which may be required for MR imaging. Furthermore, even if US is not diagnostic, it can provide useful complementary information, including the presence of intralesional cystic components or calcifications (phleboliths), degree of vascularity, and the location, size and morphology of the lesion, all of which can help in tailoring the MR imaging examination.
This article briefly discusses the MR imaging protocols and features of the most common soft-tissue vascular anomalies seen in children and follows the classification proposed by the International Society for the Study of Vascular Anomalies (ISSVA), recently expanded at the 2014 meeting in Melbourne, Australia [1, 2].
Magnetic resonance imaging technique
It is recommended that the radiologist or a trained technologist review prior imaging studies and briefly examine the patient before acquiring MR images in order to determine the location and extent of the lesion, which can help in determining the best coil and planes for imaging. In general, the goal is to use the smallest coil that covers the entire lesion. Skin markers might also be applied, especially for subtle lesions, in order to ensure that the entire lesion has been imaged. Images are acquired in at least two orthogonal planes.
Multiple MR imaging sequences are routinely used. Spin-echo T1-weighted sequence is well-suited for anatomical detail. Fast spin-echo T2-weighted sequence is useful to demonstrate the lesion and is facilitated by the use of fat-suppression techniques. Fat suppression is especially important if the lesion involves the subcutaneous tissues because it increases the contrast between the lesion and the adjacent fat. Short tau inversion recovery (STIR) sequence can be used as an alternative or to complement the fat-suppressed T2-weighted sequence because of its more homogeneous fat suppression, although STIR has the disadvantage of a lower signal-to-noise ratio and increased image degradation with patient motion [3]. Occasionally a T2-weighted gradient echo sequence facilitates identification of hemosiderin deposits, especially in juxta-articular venous malformations. A gradient echo sequence might also facilitate recognition of high-flow vessels within a vascular anomaly [3, 4].
Sequences are often obtained after the administration of intravenous gadolinium-based contrast material. These include contrast-enhanced MR angiography with dynamic acquisition of images in the arterial and venous phases in order to assess the pattern of perfusion of the lesion. More recent publications favor the use of dynamic time-resolved MR angiography over conventional MR angiography. Dynamic time-resolved MR angiography also acquires 3-D T1-weighted gradient echo images but at a faster rate than conventional contrast-enhanced MR angiography because the former only requires partial filling of the k-space by using a keyhole technique. Dynamic time-resolved MR angiography allows better differentiation of arterial and venous flow, recognition of early venous shunting, and calculation of contrast material arrival time; at the same time it is subject to less degradation by motion [5, 6]. This newer technique has proved useful in outlining the feeding and draining vessels of a vascular anomaly as part of the therapy planning, and for differentiation of high-flow from low-flow vascular malformations [5–8].
Other MR angiographic techniques, such as time-of-flight MR angiography, are less used in the evaluation of soft-tissue vascular anomalies because of their dependence on flow direction and longer acquisition times; additionally, compared to contrast-enhanced MR angiography, time-of-flight MR angiography shows less signal intensity of the vascular structures and has a higher prevalence of flow-related artifacts [9].
The quality of image acquisition in contrast-enhanced MR angiography is highly dependent on adequate timing and patient cooperation — which are often challenging in children. This is because of the rapid diffusion of conventional extracellular contrast agents from the vascular spaces into the interstitium. Intravascular or blood-pool contrast agents have been introduced in clinical practice that might be useful to overcome these challenges in children. The most commonly used of these agents is gadofosveset trisodium (Ablavar®; Lantheus Medical Imaging, North Billerica, MA). Although use of gadofosveset trisodium is still an off-label application in children, it offers the advantages of image acquisition beyond the first arterial bolus passage and acquisition of very-high-spatial-resolution data during the equilibrium phase (blood-pool or steady-state phase) [9]. Similar to extracellular contrast agents, the intravascular contrast agents can be used for the evaluation of anatomical and flow characteristics of vascular anomalies but with the advantages of higher spatial/temporal resolution, better contrast compared to background, and multistation (including whole-body) assessment in children, with extensive lesions [9].
Following MR angiography, a fat suppressed T-1 weighted sequence in one or more planes is commonly obtained. This functions as a delayed contrast enhancement sequence and allows further anatomical delineation.
Vascular tumors
This category is characterized by tumors that demonstrate endothelial cell hyperplasia and includes a broad spectrum of lesions, from benign and common lesions, such as infantile hemangioma, to locally aggressive or borderline vascular lesions, such as kaposiform hemangioendothelioma, and even rare malignant lesions, such as angiosarcoma.
Infantile hemangioma
The MR imaging appearance of infantile hemangioma reflects its evolutionary stage. During the proliferative phase, infantile hemangioma appears as a well-defined, slightly lobulated lesion that is relatively isointense or slightly hyperintense to muscle on T1-weighted images and hyperintense to muscle on T2-weighted images (Fig. 1). The high-flow vascularity results in intra- and peri-lesional signal void foci on spin-echo images [10] (Fig. 1). Perilesional edema is not a characteristic finding of infantile hemangioma [4]. On MR angiography there is early and avid homogeneous enhancement without neovascularity or early venous drainage [8] (Fig. 1). This pattern of enhancement has been found to be useful in the differentiation of infantile hemangioma from other enhancing solid tumors [8]. The diffuse enhancement of hemangiomas remains evident on conventional post-contrast fat-suppressed T1-weighted images [8, 10, 11]. With the progressive involution of infantile hemangioma, the lesion shows less prominent vessels with less degree of enhancement on post-contrast images and increasing fibro-fatty replacement [10–12].
Infantile hemangioma. MR imaging in a 19-month-old girl. a Axial T1-weighted image shows a subcutaneous mass of intermediate signal intensity in the posterior aspect of the left shoulder (arrows). Note the prominent signal void foci, particularly in perilesional distribution, which is caused by high-flow arteries feeding the lesion (arrowhead). b Axial fat-suppressed T2-weighted image shows marked high signal intensity of the lesion (arrows). c Coronal MR angiography image shows early diffuse enhancement of the lesion (arrows)
Congenital hemangioma
The current ISSVA classification includes three types of congenital hemangiomas: rapidly involuting congenital hemangioma (RICH), non-involuting congenital hemangioma (NICH), and partially involuting congenital hemangioma (PICH). These lesions are different from the infantile hemangioma because they are present at birth and exhibit different patterns of evolution. RICH starts involution soon after birth and is completed between 6 months and 14 months of age, much earlier than infantile hemangioma [13]. NICH does not show involution and often shows growth that is commensurate with the child, resembling a vascular malformation. PICH starts involution soon after birth but this involution is slow and only partial, leaving a residual lesion that resembles NICH [13]. Another difference between infantile hemangioma and congenital hemangiomas is the staining for the glucose transporter 1 (GLUT-1) of the endothelial cells; staining is positive in the former but negative in the latter [11–17].
The MR imaging features of congenital hemangiomas have been described in only a few small series of patients, and even fewer cases have been illustrated in the literature [11–18]. The lesions tend to resemble the infantile hemangioma because most congenital hemangiomas are isointense or slightly hyperintense to muscle on T1-weighted images, hyperintense on T2-weighted images and show avid enhancement post contrast administration (Fig. 2). However congenital hemangiomas tend to show with higher frequency heterogeneous signal intensity on T2-weighted images and patchy enhancement post contrast administration, and they sometimes show intralesional fat stranding [12–18].
Congenital hemangioma. MR imaging of a rapidly involuting congenital hemangioma (RICH) in a 6-week-old boy who had been diagnosed with a large upper limb mass on antenatal US. a Coronal short tau inversion recovery (STIR) image shows a left upper arm mass that is hyperintense to muscle and slightly heterogeneous. Prominent vessels are noted within the mass and in the perilesional soft tissues. b Axial gadolinium-enhanced fat-suppressed T1-weighted image shows diffuse enhancement of the lesion with prominent intralesional vessels. In most cases of RICH, including this one, the differentiation from other types of congenital hemangioma and from infantile hemangioma is based on clinical findings rather than MR imaging findings
Kaposiform hemangioendothelioma and tufted angioma
Kaposiform hemangioendothelioma and tufted angioma are tumors that can be locally aggressive and can be associated with the Kasabach–Merritt phenomenon. The Kasabach–Merritt phenomenon is defined by profound thrombocytopenia (<20,000/ml) from intratumoral platelet trapping that can be accompanied by microangiopathic hemolytic anemia and low fibrinogen, with much lower levels than those seen in the coagulopathy that may develop in large vascular malformations or other tumors [19]. The current clinical and histological evidence supports that kaposiform hemangioendothelioma and tufted angioma are closely related. Furthermore, it has been suggested that tufted angioma is a milder and more superficial form of kaposiform hemangioendothelioma [19]. Tufted angioma rarely requires imaging for diagnosis and therefore the imaging features described below refer to the kaposiform hemangioendothelioma.
On MR imaging, kaposiform hemangioendothelioma appears as a soft-tissue mass of heterogeneous signal intensity, isointense or hypointense compared to muscle on T1-weighted images, and hyperintense on T2-weighted images [4, 20]. The lesion tends to be ill-defined and with an infiltrative appearance, commonly associated with stranding of the adjacent subcutaneous fat planes and frequent thickening of the overlying skin [4, 12] (Fig. 3). Intralesional deposition of hemosiderin or other blood products is sometimes evident as well as signal voids from high-flow vessels [4, 20]. On time-resolved MR angiography, kaposiform hemangioendothelioma shows early enhancement, but this is heterogeneous and not as avid as that seen in infantile hemangioma [8]. On conventional post-contrast fat-suppressed T1-weighted images the heterogeneous lesion enhancement remains evident, but there is also enhancement of the adjacent edematous soft tissues [8]. In cases where the kaposiform hemangioendothelioma is adjacent to a bone, its growth can cause lytic bone lesions [4].
Kaposiform hemangioendothelioma. MR imaging of a in a 6-month-old boy with Kasabach–Merritt phenomenon. Coronal STIR image shows a large, irregular, heterogeneous, hyperintense mass involving the right thoracoabdominal wall (arrows). There is dermal thickening and subcutaneous stranding (arrowheads). STIR short tau inversion recovery
Capillary-type intramuscular hemangioma
The capillary-type intramuscular hemangioma is not listed as a specific entity in the ISSVA classification, and, although its histopathology has long been described, its imaging features have only recently been documented [21]. However, it should be mentioned that most cases in the adult and older pediatric radiologic literature called intramuscular hemangioma actually correspond to intramuscular venous malformations. Capillary-type intramuscular hemangioma is a rare high-flow vascular tumor that, as implied by its name, is composed of capillary-like vessels and is confined to the muscle planes [21]. It has been speculated that this atypical hemangioma might correspond to a subgroup of arteriovenous malformations that has been described in the pathology literature as having endothelial microproliferation with immature histology [22]. Capillary-type intramuscular hemangioma can present at any age, even adulthood, and does not show spontaneous involution.
MR imaging features include a well-defined mass, with isointense signal to muscle on T1-weighted images but mixed with peripheral or occasionally intralesional hyperintense areas of adipocytic tissue. On T2-weighted images it is heterogeneously hyperintense to muscle and shows homogeneous enhancement after contrast administration (Fig. 4). Signal void foci from high-flow vessels are always present. The MR imaging characteristics do not allow differentiation from sarcoma, and biopsy is recommended [21]. Occasionally this type of hemangioma does not present as a well-defined focal mass but instead involves almost the entire length of a muscle, and, although it causes expansion, the morphology of the muscle tends to be preserved [23].
Capillary-type intramuscular hemangioma. MR imaging in a 13-year-old boy. a Axial T2-weighted image shows a well-demarcated, slightly heterogeneous, hyperintense lesion within the triceps muscle in the left distal upper arm. b Axial gadolinium-enhanced fat-suppressed T1-weighted image shows diffuse enhancement of the lesion
Vascular malformations
Vascular malformations are developmental vascular anomalies. In contrast to vascular tumors, vascular malformations commonly show normal endothelial turnover and do not tend to spontaneously involute [4]. They can be categorized according to the predominant anomalous vessel found in the lesion and also based on the flow characteristics. High-flow lesions include arteriovenous malformations and arteriovenous fistulas. Low-flow lesions include capillary malformations, venous malformations and lymphatic malformations. However, in some instances lesions contain more than one type of vascular malformation.
Arteriovenous malformation
This type of high-flow soft-tissue lesion is characterized by the presence of a network of primitive vessels that directly connect arteries and veins without interposition of normal arterioles or capillaries. On MR imaging, they typically appear as a group of prominent vascular channels in association with dilated feeding and draining vessels and without a well-defined soft-tissue mass [4, 10, 22]. The high-flow vessels appear as tubular or punctate signal void foci on spin-echo images (Fig. 5) and there might be associated cutaneous thickening and increased fat deposition in the surrounding soft tissues [10]. On occasion they involve adjacent osseous structures, resulting in lytic bone expansion, lace-like appearance of the bone or cortical thinning [10]. MR angiography can demonstrate enhancement of the enlarged vessels within the lesion with characteristic early venous opacification and can depict well the feeding and draining vessels [4, 10] (Fig. 5). The addition of dynamic time-resolved MR angiography has proved to be useful in the differentiation of arteriovenous malformations from low-flow vascular lesions [7, 8].
Arteriovenous malformation. MR imaging in a 7-year-old girl. a Axial T1-weighted image shows a cluster of signal-void foci in the subcutaneous tissues of the volar aspect of the left wrist from high-flow vessels (arrow). There is no discrete mass. b Coronal MR angiography of the left upper extremity shows a conglomerate of vessels in the nidus of the arteriovenous malformation (arrows). There is early opacification of venous structures
It has been recently described that at least 50% of arteriovenous malformations show atypical MR imaging features that can make differentiation from a vascular neoplasm difficult [22]. These atypical features include hyperintense signal on T2-weighted images (Fig. 6), enhancement after gadolinium administration and presence of a discrete soft-tissue mass with small (<2 mm) and filiform intralesional arteries. These lesions frequently involve more than one tissue compartment. Pathology specimens of these arteriovenous malformations with atypical MR imaging features have shown two distinct histological patterns, both of which are different from the histological pattern seen in the typical arteriovenous malformation. The unusual histopathology resembles that seen in the capillary-type intramuscular hemangioma [22].
Arteriovenous malformations with atypical features. MR imaging in a 7-year-old boy. Axial fat-suppressed T2-weighted image shows multiple signal voids of varying size within the expanded quadriceps femoris muscle in keeping with the high-flow vessels of an arteriovenous malformation. However there is increased signal intensity within most of the affected muscle, mimicking the appearance of a mass
Capillary malformation
Most capillary malformations are diagnosed clinically and are therefore not referred to diagnostic imaging. However, MR imaging might be requested in children with capillary malformations as part of the workup of associated anomalies such as hemihypertrophy, Klippel–Trenaunay syndrome, Parkes–Weber syndrome, Sturge–Weber syndrome, CLOVES (congenital lipomatous overgrowth, vascular malformations, epidermal nevi and skeletal anomalies) syndrome or Proteus syndrome [1, 2].
On MR imaging, capillary malformations can appear as focal thickening of the skin, sometimes in association with thickening of the underlying subcutaneous tissues, without other specific features [5, 10, 24].
Venous malformation
Venous malformations can appear as ectatic veins (dysplastic type) or more frequently as spongy localized masses formed by anomalous venous spaces of varying size (cavitary type) [4, 25] (Fig. 7). These localized masses tend to be well-defined and lobulated in shape and might involve multiple tissue planes. They are more frequently hypointense to muscle on T1-weighted images and hyperintense on T2-weighted images [3–6, 10]. A multiloculated appearance representing dilated venous spaces separated by thin interstitial septa is often evident on T2-weighted images [3]. The detection of small intralesional foci that are hypointense on T2-weighted images is a helpful diagnostic clue [4]; these represent fibrous septa, thrombi or less commonly phleboliths (Figs. 8 and 9). The appearances can become atypical in the presence of intralesional fluid-fluid levels, which are attributed to the various rates of intralesional flow resulting in stagnation and layering of blood products [5, 26] (Fig. 9). Following the administration of intravenous contrast agent, the lesions show patchy enhancement that gradually increases over time, which is more apparent on dynamic imaging. The areas with lack of contrast enhancement are commonly attributed to the presence of a lymphatic component as part of mixed venous–lymphatic vascular malformation, but many times these lesions are predominantly venous in nature with areas of thrombosis or very slow flow and fail to enhance with the usual imaging protocols (Fig. 8).
Venous malformation. MR imaging in a 16-year-old girl. Axial STIR image shows a cutaneous/subcutaneous venous malformation in the right gluteal region with two components: a dysplastic component characterized by ectatic superficial veins (arrow), and a cavitary component characterized by a well-defined, hyperintense spongy mass (arrowhead). STIR short tau inversion recovery
Venous malformation. MR imaging in a 5-year-old boy. a Coronal STIR image of the right elbow and proximal forearm shows a well-defined, predominantly hyperintense intramuscular mass that contains multiple hypointense foci caused by thrombi or phleboliths. These are rarely seen in other pediatric soft-tissue masses and therefore their detection is an important clue for the diagnosis of venous malformation. b Coronal gadolinium-enhanced fat-suppressed T1-weighted image shows the frequent patchy enhancement of these lesions. STIR short tau inversion recovery
Venous malformation. MR imaging in a 7-year-old boy. Sagittal STIR image of the right lower thigh shows the presence of a lobulated suprapopliteal mass that involves the subcutaneous tissues and the underlying biceps femoris muscle. The mass is heterogeneous and hyperintense to muscle and contains multiple fluid-fluid levels caused by stagnation and layering of blood products. There are also several intralesional hypointense foci from thrombi and phleboliths, more evident posteriorly. Post-contrast imaging (not shown) revealed the typical patchy enhancement of venous malformations. STIR short tau inversion recovery
Lymphatic malformation
Lymphatic malformations are often classified as macrocystic, microcystic or combined [1–4, 10, 27]. There is no universal agreement in the definition of macrocystic versus microcystic lymphatic malformation. Some authors consider the presence of cysts larger than 1 cm or 1–2 cm as diagnostic of a macrocystic lesion and cysts less than 1 cm or 1–2 cm as diagnostic of a microcystic lesion [28, 29]. Other authors use as a criterion for macrocystic lesions the fact that they can be successfully reduced in size with aspiration or sclerosis, in contrast to the microcystic lesions, which have a more challenging treatment [2]. Any type of lymphatic malformation can be infiltrative, involving more than one anatomical plane, and can be associated with skeletal overgrowth [10, 28]. Other MR imaging features vary depending on the type.
The macrocystic lymphatic malformations have well-defined cystic spaces separated by thin septa. The contents of the cysts often show low signal intensity on T1-weighted images and marked high signal intensity on T2-weighted images [3, 4, 10] (Fig. 10). Fluid-fluid levels within the cystic spaces are not uncommon due to post-traumatic or spontaneous bleeding. Following administration of intravenous contrast agent, there is enhancement of the walls of the cysts and intervening septa but there is no enhancement of the cystic contents, a feature that helps in the differentiation from venous malformations [3, 4, 10] (Fig. 10). However, enhancement of the cystic spaces can be seen in combined lymphatic–venous malformations and after sclerotherapy [4, 10, 28]. The presence of proteinaceous content and blood products might result in changes of the intralesional signal intensity so that the fluid in the cystic spaces appears hyperintense on T1-weighted images and even simulates enhancement on post-contrast fat-suppressed T1-weighted images (Fig. 11).
Macrocystic lymphatic malformation. MR imaging in a 4-week-old girl. a Axial T1-weighted image shows a lobulated, hypointense lesion in the subcutaneous tissues in the anterior aspect of the neck, anterior to the thyroid, left carotid sheath and left sternocleidomastoid muscle. b Axial fat-suppressed T2-weighted image shows that the lesion is hyperintense and multiloculated, with thin septa separating relatively large cystic spaces. c Axial gadolinium-enhanced fat-suppressed T1-weighted image shows lack of enhancement of the contents of the cystic spaces, which helps in the differentiation from venous malformations. The enhancement of macrocystic lymphatic malformations is limited to the periphery and septa
Macrocystic lymphatic malformation. MR imaging in a 20-month-old boy. a Axial T1-weighted image shows a well-defined, lobulated, subcutaneous lesion in the left forearm, which is hyperintense to muscle, although not as hyperintense as the adjacent subcutaneous fat, likely a result of proteinaceous content within the cystic spaces. b Axial gadolinium-enhanced fat-suppressed T1-weighted image shows marked hyperintense signal within the lesion, simulating avid enhancement of a solid lesion. If a lesion is relatively hyperintense on T1-weighted images, it is useful to perform a fat-suppressed T1-weighted sequence prior to the administration of gadolinium contrast agent or to use US to confirm the cystic nature of the lesion
In microcystic lymphatic malformations, the cysts are often too small to be recognized as such on MR imaging. These microcystic lymphatic malformations appear as nonspecific, ill-defined lesions with low signal intensity on T1-weighted images and high signal intensity on T2-weighted images (Fig. 12). Following the administration of intravenous contrast agent, the lesion might not enhance or show just faint enhancement [3, 10] (Fig. 12).
Microcystic lymphatic malformation. MR imaging in a 7-year-old boy. a Axial fat-suppressed T2-weighted image shows a subcutaneous lesion in the medial aspect of the right forearm that is hyperintense to muscle and contains multiple thin hypointense septa resulting in a multilocular appearance, although the locules are very small and irregular in shape, in contrast to the larger well-defined cystic spaces seen in macrocystic lymphatic malformations. b Axial gadolinium-enhanced fat-suppressed T1-weighted image shows absence of enhancement of the lesion. Intralesional hyperintense foci correspond to vessels crossing through the lesion (arrows). The lack of enhancement is helpful in the differentiation from venous malformations
The combined lymphatic malformations, which are more commonly seen below the head and neck, show MR imaging features of both macrocystic and microcystic lesions.
Complex combined vascular malformation
There is a long and heterogeneous list of entities that present with complex combined vascular malformations and syndromes and are associated with vascular malformations. In these conditions, MR imaging is useful not only for the evaluation of the vascular lesions but also in the assessment of abnormalities in the adjacent soft tissues and bones, most commonly overgrowth. In most of these conditions, the vascular malformations are of the low-flow type (capillary, venous, lymphatic or combined), with the exception of Parkes–Weber syndrome, Bannayan–Riley–Ruvalcaba syndrome and CLOVES syndrome, which sometimes present with high-flow vascular malformations [1, 2, 30, 31]. A brief description of the MR imaging findings in some of these entities is found below.
Parkes–Weber syndrome
This is a specific manifestation of capillary–arteriovenous malformation disorders secondary to RASA1 gene mutations [31]. It usually involves an entire extremity, more often a lower limb. The diagnosis is generally based on clinical findings. MR imaging might reveal the bone and soft-tissue hypertrophy in addition to the presence of arteriovenous malformations.
Bannayan–Riley–Ruvalcaba syndrome and PTEN hamartoma tumor syndrome
Bannayan–Riley–Ruvalcaba syndrome along with Cowden syndrome are grouped in the PTEN hamartoma tumor syndromes because of their association with germline mutations in the phosphatase and tensin homolog (PTEN) tumor suppressor. Although the high-flow lesions noted in these conditions are often referred to as arteriovenous malformations, Kurek et al. [32] have suggested that many of these represent a distinct entity that they have labeled as PTEN hamartoma of soft tissue because it appears to represent a disorganized overgrowth of mesenchymal elements. MR imaging might reveal variable-size lesions with an infiltrative appearance involving muscle, fascia and subcutaneous tissue, more frequently in a lower limb. There are enlarged serpiginous vessels and excessive fatty tissue at the site of the anomaly. In some cases, the lesions involve contiguous muscles or are multifocal. The affected muscle shows progressive enlargement and disruption of its architecture on MR imaging [31–33].
CLOVES syndrome
CLOVES is an acronym that stands for congenital lipomatous overgrowth, vascular malformations, epidermal nevi and skeletal anomalies. Many patients who in the past were labeled as having Proteus syndrome are today considered to have CLOVES syndrome, which has been associated with mutations in the PIK3CA gene [31]. MR imaging can demonstrate the characteristic congenital lipomatous mass in the trunk, which is often associated with vascular malformations, including low-flow (lymphatic, venous and capillary) and high-flow (arteriovenous) types [31]. The lymphatic malformations may extend into the retroperitoneum and mediastinum. Venous malformations may present as phlebectasia of central, thoracic and limb veins. Paraspinal and spinal arteriovenous malformations are not uncommon [31].
Klippel–Trénaunay syndrome
This overgrowth syndrome typically affects one of the lower limbs and is characterized by the presence of capillary, lymphatic and venous malformations without high-flow lesions. MR imaging might show soft-tissue overgrowth and its recognition might be facilitated by including both lower extremities during image acquisition (Fig. 13). This overgrowth predominantly affects the fatty tissue, especially in the extrafascial and subcutaneous planes, but it can also affect the intrafascial compartment and the bones [31]. The typical venous malformation in Klippel–Trénaunay syndrome is the presence of the marginal vein of Servelle in the lateral aspect of the thigh and lower leg, which is associated and can communicate with a hypoplastic or interrupted anomalous deep venous system, all of which can be seen on MR imaging [10] (Fig. 13). The lymphatic malformations, which can be macrocystic or microcystic, can extend into the perineum, pelvis and abdomen [31].
Klippel–Trenaunay syndrome. MR imaging in an 11-year-old boy. a Coronal STIR image shows asymmetry of the lower extremities, with overgrowth on the left. There are multiple prominent veins in the subcutaneous soft tissues of the left leg (dysplastic venous malformation) and a more localized spongy venous malformation in the foot (arrow). b Coronal MR angiography shows the lateral marginal vein, also known as the vein of Servelle (arrowheads), coursing along the lateral aspect of the left lower extremity, associated with absence or hypoplasia of segments of the deep venous system. STIR short tau inversion recovery
Fibro-adipose vascular anomaly (FAVA)
FAVA has been recently described as an entity characterized by intramuscular vascular malformation — often affecting the calf (usually the gastrocnemius) or the forearm — that results clinically in significant pain and contracture [34, 35]. The lesion is composed of anomalous veins that are intertwined with fibrofatty tissue. Typically, there is intramuscular or subcutaneous phlebectasia. On MR imaging, FAVA has a significant solid component that demonstrates heterogeneous hyperintense signal on T1-weighted images, as compared to muscle, likely adipose tissue (Fig. 14). On T2-weighted images, FAVA is also heterogeneous and hyperintense compared to muscle but not as hyperintense as the classic venous malformation [34]. There might be disruption of the adjacent fascial planes with transfascial intramuscular and subcutaneous components of the lesion [34]. Following the administration of intravenous contrast agent, FAVA shows moderate to avid homogeneous enhancement as opposed to the patchier enhancement of the classic venous malformation [34, 35].
Fibro-adipose vascular anomaly (FAVA). MR imaging in a 9-year-old girl. a Axial T1-weighted image shows a heterogeneous mass involving the medial gastrocnemius muscle of the right calf. The mass contains a mostly peripheral hyperintense component suggestive of adipose tissue (arrowheads). This fatty component is almost completely encircling an area that is predominantly isointense to muscle (arrow). b Axial fat-suppressed T2-weighted image shows that the peripheral component is of low signal intensity, confirming its fatty nature. The other component is hyperintense to muscle and contains prominent veins (arrow). c Axial gadolinium-enhanced fat-suppressed T1-weighted image shows minimal to no enhancement of the area with adipose tissue, whereas the other component shows moderate enhancement
Conclusion
MR imaging is a useful tool in the evaluation of vascular anomalies, providing valuable information for diagnosis and management. This requires the use of an appropriate technique. The impact of MR imaging and other imaging modalities is amplified when the findings are interpreted in correlation with the clinical assessment. The radiologist must be familiar with the most updated ISSVA classification and use it accordingly to facilitate collaboration and participation in the multidisciplinary team that is often involved in the care of children with vascular anomalies.
References
Dasgupta R, Fishman SJ (2014) ISSVA classification. Semin Pediatr Surg 23:158–161
Wassef M, Blei F, Adams D et al (2015) Vascular anomalies classification: recommendations from the International Society for the Study of Vascular Anomalies. Pediatrics 136:e203–e214
Navarro OM, Laffan E, Ngan BY (2009) Pediatric soft-tissue tumors and pseudotumors: MR imaging features with pathologic correlation. Part 1. Imaging approach, pseudotumors, vascular lesions, and adipocytic tumors. Radiographics 29:887–906
Dubois J, Alison M (2010) Vascular anomalies: what a radiologist needs to know. Pediatr Radiol 40:895–905
Moukaddam H, Pollak J, Haims AH (2009) MRI characteristics and classification of peripheral vascular malformations and tumors. Skeletal Radiol 38:535–547
Flors L, Leiva-Salinas C, Maged IM et al (2011) MR imaging of soft-tissue vascular malformations: diagnosis, classification, and therapy follow-up. Radiographics 31:1321–1340
Ohgiya Y, Hashimoto T, Gokan T et al (2005) Dynamic MRI for distinguishing high- from low-flow peripheral vascular malformations. AJR Am J Roentgenol 185:1131–1137
Kim JS, Chandler A, Borzykowski R et al (2012) Maximizing time-resolved MRA for differentiation of hemangiomas, vascular malformations and vascularized tumors. Pediatr Radiol 42:775–784
Farmakis SG, Khanna G (2014) Extracardiac applications of MR blood pool contrast agent in children. Pediatr Radiol 44:1598–1609
Konez O, Burrows PE (2002) Magnetic resonance of vascular anomalies. Magn Reson Imaging Clin N Am 10:363–388
Restrepo R, Palani R, Cervantes LF et al (2011) Hemangiomas revisited: the useful, the unusual and the new. Part 1: overview and clinical and imaging characteristics. Pediatr Radiol 41:895–904
Lowe LH, Marchant TC, Rivard DC et al (2012) Vascular malformations: classification and terminology the radiologists needs to know. Semin Roentgenol 47:106–117
Nasseri E, Piram M, McCuaig CC et al (2014) Partially involuting congenital hemangiomas: a report of 8 cases and review of the literature. J Am Acad Dermatol 70:75–79
Konez O, Burrows PE, Mulliken JB et al (2003) Angiographic features of rapidly involuting congenital hemangioma (RICH). Pediatr Radiol 33:15–19
Krol A, MacArthur CJ (2005) Congenital hemangiomas. Rapidly involuting and noninvoluting congenital hemangiomas. Arch Facial Plast Surg 7:307–311
Gorincour G, Kokta V, Rypens F et al (2005) Imaging characteristics of two subtypes of congenital hemangiomas: rapidly involuting congenital hemangiomas and non-involuting congenital hemangiomas. Pediatr Radiol 35:1178–1185
Navarro OM (2011) Soft tissue masses in children. Radiol Clin N Am 49:1235–1259
Calvo-Garcia MA, Kline-Fath BM, Adams DM et al (2015) Imaging evaluation of fetal vascular anomalies. Pediatr Radiol 45:1218–1229
Colmenero I, Hoeger PH (2014) Vascular tumours in infants. Part II: vascular tumours of intermediate dignity and malignant tumours. Br J Dermatol 171:474–484
Gruman A, Liang MG, Mulliken JB et al (2005) Kaposiform hemangioendothelioma without Kasabach-Merritt phenomenon. J Am Acad Dermatol 52:616–622
Yilmaz S, Kozakewich HP, Alomari AI et al (2014) Intramuscular capillary-type hemangioma: radiologic–pathologic correlation. Pediatr Radiol 44:558–565
Patel AS, Schulman JM, Ruben BS et al (2015) Atypical MRI features in soft-tissue arteriovenous malformation: a novel imaging appearance with radiologic–pathologic correlation. Pediatr Radiol 45:1515–1521
Merrow AC, Gupta A, Adams DM (2014) Additional imaging features of intramuscular capillary-type hemangioma: the importance of ultrasound. Pediatr Radiol 44:1472–1474
Breugem CC, Maas M, Reekers JA et al (2001) Use of magnetic resonance imaging for the evaluation of vascular malformations of the lower extremity. Plast Reconstr Surg 108:870–877
Hein KD, Mulliken JB, Kozakewich HP et al (2002) Venous malformations of skeletal muscle. Plast Reconstr Surg 110:1625–1635
Koo KSH, Dowd CF, Mathes EF et al (2015) MRI phenotypes of localized intravascular coagulopathy in venous malformations. Pediatr Radiol 45:1690–1695
Elluru RG, Balakrishnan K, Padua HM (2014) Lymphatic malformations: diagnosis and management. Semin Pediatr Surg 23:178–185
Lobo-Mueller E, Amaral JG, Babyn PS et al (2009) Extremity vascular anomalies in children: introduction, classification, and imaging. Semin Musculoskelet Radiol 13:210–235
Ballah D, Cahill AM, Fontalvo L et al (2011) Vascular anomalies: what they are, how to diagnose them, and how to treat them. Curr Probl Diagn Radiol 40:233–247
Lobo-Mueller E, Amaral JG, Babyn PS et al (2009) Complex combined vascular malformations and vascular malformation syndromes affecting the extremities in children. Semin Musculoskelet Radiol 13:255–276
Uller W, Fishman SJ, Alomari AI (2014) Overgrowth syndromes with complex vascular anomalies. Semin Pediatr Surg 23:208–215
Kurek KC, Howard E, Tenant L (2012) PTEN hamartoma of soft tissue: a distinctive lesion in PTEN syndromes. Am J Surg Pathol 36:671–687
Tan WH, Baris HN, Burrows PE et al (2007) The spectrum of vascular anomalies in patients with PTEN mutations: implications for diagnosis and management. J Med Genet 44:594–602
Alomari AI, Spencer SA, Arnold RW et al (2014) Fibro-adipose vascular anomaly: clinical-radiologic-pathologic features of a newly delineated disorder of the extremity. J Pediatr Orthop 34:109–117
Fernandez-Pineda I, Marcilla D, Downey-Carmona FJ et al (2014) Lower extremity fibro-adipose vascular anomaly: a new case of a newly delineated disorder. Ann Vasc Dis 7:316–319
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors have no financial interests, investigational or off-label uses to disclose.
Rights and permissions
About this article
Cite this article
Navarro, O.M. Magnetic resonance imaging of pediatric soft-tissue vascular anomalies. Pediatr Radiol 46, 891–901 (2016). https://doi.org/10.1007/s00247-016-3567-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-016-3567-1