Abstract
Despite the benefit high frequency stimulation (HFS) of the subthalamic nucleus (STN) has on motor symptoms of Parkinson’s Disease (PD), accumulating data also suggest effects of STN-HFS on non-motor behavior. This may be related to the involvement of the STN in the limbic basal ganglia-thalamocortical loops. In the present study we investigated the effect of acute STN-HFS on neurotransmission in associated structures of these pathways, i.e. the nucleus accumbens (NAc) core and shell as well as the ventral tegmental area (VTA) using in vivo microdialysis. Experiments were performed in anaesthetized naïve rats and rats selectively lesioned in the substantia nigra pars compacta (SNc) or VTA. We demonstrate that: 1. STN-HFS leads to an increase in DA in the NAc, 2., these effects are more pronounced in the NAc shell than in the NAc core, 3. STN-HFS leads to a decrease in GABA in the VTA, 4. preceding lesion of the SNc does not seem to affect the effect of STN-HFS on accumbal DA transmission whereas 5. preceding lesion of the VTA seems to prohibit further detection of DA in the NAc. We conclude that STN-HFS significantly affects neurotransmission in the limbic system, which might contribute to explain the non-motor effects of STN-HFS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
High frequency stimulation (HFS) of the subthalamic nucleus (STN) improves motor symptoms in Parkinson’s Disease (PD) (Deuschl et al. 2006; Kumar et al. 1998; Limousin et al. 1998). However, HFS of the STN or closely adjacent structures also affects psychiatric functions: altered mood and depressive symptoms (Bejjani et al. 2002; Czernecki et al. 2005; Doshi et al. 2002; Funkiewiez et al. 2004, 2006; Okun et al. 2003; Thobois et al. 2002; Witt et al. 2006) with suicide (Albanese et al. 2005), transient manic episodes partly with psychotic symptoms (Herzog et al. 2003; Mandat et al. 2006), mirthful laughter, hilarity (Krack et al. 2001), acute reinforcing psychotropic effects (Funkiewiez et al. 2003; Romito et al. 2002) as well as reduction of craving behavior (Witjas et al. 2005) and obsessive compulsive symptoms (Fontaine et al. 2004; Mallet et al. 2002) have been observed in PD patients receiving STN-HFS.
These side effects may be related to the subdivision of the STN in three functionally segregated territories: a motor, an associative and a limbic subregion. Thus, the STN interconnects not only to the motor but also to the limbic basal ganglia-thalamocortical circuitry, involving orbitofrontal and cingulated cortices, nucleus accumbens (NAc), limbic globus pallidus and ventral putamen, substantia nigra (SN), and ventral tegmental area (VTA) (Alexander et al. 1986, 1990; Alexander and Crutcher 1990). Consequently, PET studies in PD-patients demonstrate that STN-HFS increases activity (Ceballos-Baumann et al. 1999; Limousin et al. 1997; Stefurak et al. 2003) (or rather reduces abnormal background noise (Payoux et al. 2004) in the anterior cingulate and prefrontal cortex as well as the temporal and parietal cortex (Hilker et al. 2004). To date, however, little is known about the mechanisms of how STN-HFS modifies non-motor behavior of PD patients. One way of addressing this question is to investigate the neurochemical consequences of STN-HFS in relevant limbic brain structures via in vivo microdialysis in animals.
Previous experimental studies have demonstrated that STN-HFS modulates extracellular levels of GABA and glutamate in the striatum and substantia nigra (Bruet et al. 2003; Windels et al. 2000, 2003) and increases DA-transmission in the dorsolateral striatum of naïve and hemiparkinsonian rats. This effect has been suggested to contribute to the clinical motor improvement and the reduction of DAergic medication in PD patients under chronic STN-HFS (Lee et al. 2006; Meissner et al. 2001, 2003; Paul et al. 2000). With the functional subdivision of the STN and its integration into motor as well as limbic circuitries, it is possible that STN-HFS may also induce neurochemical changes in limbic structures which might attribute to the co-occurrence of psychiatric effects under STN-HFS.
The present study investigates the impact of STN-HFS on the DAergic transmission in the NAc and GABAergic transmission in the VTA using in vivo microdialysis in rats. For further investigation of the pathways involved in mediating the STN-HFS-dependent effects on DA-transmission in the NAc, two separate groups were included, receiving selective 6-hydroxydopamine (6-OHDA)-lesions of either the substantia nigra pars compacta (SNc) or the VTA prior to STN-HFS and microdialysis analysis.
Material and methods
Animals
Principles of laboratory animal care (NIH publication No. 86–23, revised 1985) and of the European Communities Council Directive (86/609/EEC) for care of laboratory animals were followed as well as guidelines of local ethical authorities where applicable. Naive male Wistar rats (Harlan-Winkelmann, Borchen, Germany; n = 78, 280–320 g during the experiment) were housed in a temperature- and humidity-controlled vivarium with a 12-h light/dark cycle. Food and water were available ad libitum. All experiments were performed during day time and in anaesthetized rats only.
Surgery
All surgeries were performed under general anesthesia (for microdialysis sampling: chloral hydrate, 400 mg/kg i.p.; Merck, Darmstadt, Germany, for stereotaxic lesions: pentobarbital, 60 mg/kg, i.p.; Sigma Aldrich, Taufkirchen, Germany (Meissner et al. 2001; Paul et al. 2000). For in vivo microdialysis, microdialysis probes were stereotaxically inserted into the left NAc core (1.6; L: 1.4; V: −7.4), the left NAc shell (A: 1.6; L: 0.7; V: −7.7; CMA 11), or the probe was inserted suchlike that it collected simultaneously from the left NAc core and shell (A: 1.7; L: 1.3; V: −8.2), or the VTA (A: −6.0; L: 0.6; V: −8.3; coordinates with respect to bregma (Paxinos and Watson 1997). Microdialysis probes for separate measures in the NAC core and shell were 0.24 mm in diameter and 1 mm in length (CMA 11, CMA, Solna, Sweden), and for simultaneous collection from the NAc core and shell 0.5 mm in diameter and 2 mm in length (CMA 12). During the same surgical session, a concentric bipolar stimulation electrode (SNEX 100; Rhode Medical Instruments, Woodland Hills, CA, USA) was placed into the left STN in all animals (A: −3.8; L: 2.5; V: 7.6).
Selective 6-OHDA lesions were performed 2 weeks prior to STN-HFS and microdialysis sampling. 7 μg 6-OHDA (Sigma Chemical Co., St. Louis, MO, USA), dissolved in 2 μl saline containing 0.1% ascorbic acid, were applied stereotaxically into the left SNc (A: −5.3; L: 2.3; V: −7.2) or the left VTA (A: −5.3; L: 0.6; V: −7.8) through a 25 gauge stainless steel canula attached to a 20 μl Hamilton microsyringe.
Microdialysis and HFS
Microdialysis procedures were performed as previously described (Meissner et al. 2001; Paul et al. 2000). Briefly, microdialysis probes were perfused with artificial cerebrospinal fluid (125 mM NaCl, 1 mM CaCl2, 1 mM MgCl2 × 6 H2O, 2.5 mM KCl, 5 mM Na2So4, 2.7 mM NaHCO3, 0.5 mM NaH2PO4 × 2 H2O, 2.4 mM NaH2PO4 (pH 7.4) adjusted with H3PO4) with a constant flow rate of 1.1 μl per min. Samples were collected at 20-min intervals in 5 μl of 1 M perchloric acid for immediate analysis of extracellular concentrations of DA, its metabolites 3,4-dihydroxyphenyl-acetic acid (DOPAC) and homovanillic acid (HVA) by HPLC (Synergi 4 μ Hydro-RP 80A, 150 × 2 mm, Phenomenex, Aschaffenburg, Germany) and electrochemical detection (LC-4C, BAS, West Lafayette, USA). GABA was analyzed by HPLC after precolumn derivatization with phthaldialdehyde (Merck) and fluorescence detection. Prior to stimulation, samples were collected until at least four consecutive stable values were measured. Thereafter, one sample was collected during STN stimulation and five thereafter. For STN-HFS the following parameters were applied: alternating pulses (130 Hz for HFS, pulse width 60 μs) with an amplitude of 300 μA in a constant current mode for 20 min using an isolated stimulator (Coulbourn Instruments, Allentown, PA, USA). Frequencies of 130 Hz and a narrow pulse duration of 60 μs were chosen according to the parameters generally applied in rats for inducing net inhibitory effects of the STN (Benazzouz et al. 1995; Meissner et al. 2003; Salin et al. 2002; Windels et al. 2000) and were comparable to the clinical application (Moro et al. 2002). Current intensities of 300 μA were chosen to allow comparability with values that have previously been shown to induce behavioral and biochemical changes (Boulet et al. 2006; Meissner et al. 2001, 2003).
Control animals received no stimulation (insertion of the electrodes and connection to the stimulation device only). Microdialysis experiments were performed in anaesthetized rats only.
Histological verification and immunocytochemistry
After the experiment all animals were transcardially perfused with 0.1 M phosphate buffer saline and 4% paraformaldehyde in deep anesthesia. Free floating 40 μm thick coronal sections of the NAc (+2.9 to +0.5), the STN (−3.4 to −4.3), the SNc (−4.8 to −6.3), and the VTA (−4.52 to −6.3) were prepared. To verify location of electrode, microdialysis probe, and injection canula, every second section of the respective region was mounted and processed for cresyl violet (CV) staining. Only rats with accurate placement of all devices were included into data analysis.
For assessing the extent of the toxic lesions, tyrosine hydroxylase (TH) immunostaining was performed in rats that previously received 6-OHDA application into the SNc or the VTA (plus respective controls). One-in-six series of 40-μm sections (microtome setting) from the rostrocaudal extent of the SNc and the VTA (240 μm apart) were incubated with monoclonal antisera against TH (Sigma Chemical Co., diluted at 1:500). Immunostaining was visualized by avidin-biotin complex and 3,3′-diaminobenzidine as described previously (Winter et al. 2000, 2006). With this, a total of eight nigral and VTA-sections per animal, respectively, were stereologically analyzed for TH-positive cells as described previously (Kempermann et al. 1997; Steiner et al. 2004, 2006). Shortly, the boundaries of the SNc and the VTA were determined with reference to internal anatomic landmarks (Paxinos and Watson 1997; Steiner et al. 2006). The total numbers of positive cells were determined with the optical fractionator method using the semi-automated stereology system StereoInvestigator and as implemented in the software (MicroBrightfield, Magdeburg, Germany). The setup uses a Hitachi HV-C20A video camera attached to a Leica DM-RXE microscope. The coefficient of error (CE, ranging between 0.05 and 0.1) due to estimation was calculated according to Gundersen and Jensen (Gundersen and Jensen 1987). For quantification of TH-labeled cells, numbers were expressed as percentages of contralateral unlesioned side.
Data analysis
Baseline for microdialysis samples was defined as the mean of the last four dialysate samples collected before HFS/sham-HFS. Stability of baseline values was assessed with respect to raw data. All data then were converted to percent of baseline (defined as 100%) in relation to the peak area of the chromatograms (Meissner et al. 2001). Statistical analysis was performed using two-way repeated measures (RM) ANOVA, with stimulation (HFS/control) or lesion (VTA/SNc/control) as the between subjects factor and time bin as the repeated within-subjects factor. If appropriate, this was followed by a Holm Sidak post hoc t-tests corrected for multiple comparisons. A probability level of P < 0.05 was considered significant. Data are shown as mean ± SEM. Baseline values are given as fmol/20 μl dialysate for DA and pmol/20 μl dialysate for DOPAC and HVA.
Results
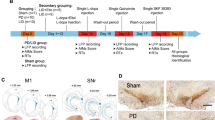
Figure 1a presents a representative photomicrograph of a coronal section taken from a rat implanted with an electrode in the STN. Figure 1b show schematic reconstructions of the stimulating electrodes, placed correctly in the STN of all experimental animals included into the study.
PostMortem Histology. a Photomicrograph of a coronal section stained with cresyl violet and taken from a representative rat showing the tip of the electrode with respect to bregma as assessed by small insertion trauma. b–g Schematic reconstructions of electrodes in the STN of experimental animals of the following experimental paradigm: b Exp. 1: HFS, microdialysis in NAc core, c Exp. 1: HFS, microdialysis in NAc shell, d Exp. 2: HFS, microdialysis in VTA, e Exp. 3: HFS, microdialysis in NAc core/shell, preceding lesion of VTA, f Exp. 3: HFS, microdialysis in NAc core/shell, preceding lesion of SNc, g Exp. 3: HFS, microdialysis in VTA, no preceding lesion
Experiment 1
For investigating the effects of STN-HFS on extracellular DA in the NAc, 41 rats were divided into two subgroups. For the first group (1A; HFS, n = 13; controls, n = 9), microdialysis sampling was performed in the NAc core, for the second group (1B; HFS, n = 12, controls, n = 7) in the NAc shell.
STN-HFS and DAergic transmission in the NAc core
Two-way RM ANOVA revealed a significant difference across stimulation as well as time and a significant interaction between the factors stimulation/sham stimulation and time for DOPAC and HVA, but not for DA (Table in Fig. 2). STN-HFS led to a reversible and non-significant trend towards increasing extracellular levels of DA when compared to baseline and non-stimulated controls (P > 0.05; Fig. 2a). Furthermore, STN-HFS significantly and reversibly increased extracellular levels of DOPAC, and HVA when compared to baseline (DOPAC: t = 0–40 min; HVA: t = 20–60 min P < 0.05) and non-stimulated controls (DOPAC: t = 0–60 min; HVA: t = 20–60 min, P < 0.05; Fig. 2b, c).
Neurotransmission in the NAc under STN-HFS. a–f Extracellular DA (A + D), DOPAC (B + E), and HVA (C + F) in the NAc core (A−C) and NAcs shell (D−E) before, during and after STN-HFS. Baseline concentrations of the NAc core were 21.15 ± 1.05 fmol DA/20 μl, 14.36 ± 0.35 pmol DOPAC/20 μl, and 8.57 ± 0.37 pmol HVA/20 μl. Baseline concentrations of the NAc shell were 37.47 ± 3.17 fmol DA/20 μl, 12.75 ± 1.08 pmol DOPAC/20 μl, and 6.63 ± 0.40 pmol HVA/20 μl. Baseline concentrations of DA, DOPAC, and HVA were significantly higher in the NAc shell than in the NAc core (P < 0.05). Data are expressed as mean ± SEM. §P < 0.05 versus baseline, *P < 0.05 versus non-stimulated controls. The dead space in the microdialysis tubing is responsible for a lag time of 10 min before analysis. Filled rectangular: duration of HFS, filled circle: HFS of the STN, open circle: controls. The table below the figure describes the two-way ANOVA assessing the effect of STN-HFS and time on transmission of DA and its metabolites in the NAc. For further details see text
STN-HFS and DAergic transmission in the NAc shell
Two-way RM ANOVA revealed a significant difference across stimulation as well as time and a significant interaction between the factors stimulation/sham stimulation and time for all parameters investigated, i.e., DA, DOPAC, and HVA (Table in Fig. 2). STN-HFS significantly and reversibly increased extracellular levels of DA, DOPAC, and HVA when compared to baseline (DA: t = 0–60 min; DOPAC: t = 0–80 min; HVA: t = 0–100 min; P < 0.05) and non-stimulated controls (DA: t = 20–60; DOPAC: t = 0–120; HVA: t = 0–120; P < 0.05; Fig. 2d–f). Maximal increases of extracellular concentrations of all parameters were significantly more pronounced in the NAc shell than the NAc core (t-test, P < 0.05).
Experiment 2
In 16 rats (HFS, n = 8; controls, n = 8) the effects of STN-HFS on extracellular contents of GABA in the VTA was investigated.
Two-way RM ANOVA revealed a significant difference across stimulation [F(1, 84) = 52.68; P < 0.001] as well as time [F(6, 84) = 11.4; P < 0.001] and a significant interaction between the factors stimulation/sham stimulation and time [F(6, 84) = 3.4; P = 0.005]. As shown in Fig. 4, STN-HFS significantly decreased extracellular levels of GABA in the VTA when compared to baseline and non-stimulated controls (t: 0–120, P < 0.05; Fig. 3). Notably, baseline values of HFS-stimulated and controls were not stable {ANOVA, HFS: [F(3, 39) = 15.04; P < 0.05]; controls: [F(3, 39) = 11.825; P < 0.05]}. The first stimulation value, however, was significantly different to the mean baseline and the last baseline value indicating that the drop in GABA following HFS did not represent the extension of a trend originating during baseline sampling, but was an independent finding.
Neurotransmission in the ventral tegmental area. Extracellular GABA in the VTA before, during, and after STN-HFS. Baseline concentrations of the VTA were 4.53 ± 0.38 pmol GABA/20 μl. Data are expressed as mean ± SEM. §P < 0.05 versus baseline. *P < 0.05 versus non-stimulated controls. The dead space in the microdialysis tubing is responsible for a lag time of 10 min before analysis. Filled rectangular: duration of HFS, filled circle: HFS of the STN, open circle: controls
Experiment 3
To investigate the involvement of the SNc and the VTA in mediating the potential effects of STN-HFS on DAergic neurotransmission in the NAc, 21 rats were subdivided into three groups depending on pre-treatment 2 weeks prior to microdialysis sampling and HFS: 6-OHDA lesion of the SNc (n = 8) versus 6-OHDA lesion of the VTA (n = 8) versus no lesion (n = 5). Microdialysis sampling was performed simultaneously in the NAc core and shell.
Immunocytochemistry
SNc-lesioning resulted in a 88.66 ± 9.97% reduction of TH positive nigral cells when compared to contralateral (control) side (Fig. 4a–c). VTA-lesioning resulted in a 81.98 ± 8.10% reduction of TH positive VTA cells when compared to contralateral (control) side (Fig. 4b–d). Only animals were included, in which the SNc- or VTA-lesioning resulted in a loss of not more than 15 or 30% of TH expressing neurons in the adjacent VTA or SNc, respectively (Fig. 4b–c).
Histological Verfication of the lesion site. Microphotographs of cresylviolet stainings of the SNc (a + c) and the VTA (b + d). a + b: Exemplary microphotographs of a rat selectively lesioned in the SNc (a) with the VTA left intact (b). c + d exemplary microphotograph of a rat selectively lesioned in the VTA (d) with the SNc left intact (c). Arrows mark boundaries of intact (solid arrow) and lesioned ( open arrow) neuronal regions. Scale bar 100 μm
Microdialysis
Following VTA-lesion, DAergic metabolites remained below detection limit of the HPLC system applied, in all animals investigated and under both, baseline and stimulation conditions. VTA-lesioned animals were consequently not included in further statistical analysis. For the control and SNc-lesioned animals, two-way RM ANOVA solely revealed a significant difference across time for both, DOPAC, and HVA (Table in Fig. 5). In unlesioned animals, STN-HFS significantly and reversibly increased extracellular accumbal levels of DOPAC and HVA when compared to baseline (DOPAC: t = 0–80 min; HVA: t = 20–100 min, Fig. 5a, b), reflecting what we have observed in experiment 1. Also, in SNc-lesioned animals, STN-HFS significantly and reversibly increased extracellular levels of DOPAC and HVA when compared to baseline, though the effects on HVA were less pronounced than in control animals (DOPAC: t = 0–80 min; HVA: t = 20–40, Fig. 5a, b). Notably, however, baseline concentrations of all parameters investigated were significantly lower in SNc-lesioned animals when compared to control animals (P < 0.05, Fig. 5).
Neurotransmission in the NAc of rats prelesioned in either the SNc. Extracellular DOPAC (a) and HVA (b) in the NAc before, during and after STN-HFS of control rats and rats lesioned in the SNc. Baseline concentrations of unlesioned control animals were 21.58 ± 1.82 pmol DOPAC/20 μl and 11.17 ± 0.48 pmol HVA/20 μl. Baseline concentrations of SNc-prelesioned animals were 7.39 ± 1.21 pmol DOPAC/20 μl, pmol and 4.89 ± 0.53 HVA/20 μl. Data are expressed as mean ± SEM. §Significant difference in comparison to baseline (P < 0.05). *Significant difference between lesioned and control HF-stimulated rats (P < 0.05). The dead space in the microdialysis tubing is responsible for a lag time of 10 min before analysis. Filled rectangular duration of STN-HFS, filled circle SNc-lesion, open diamond controls. The table below the figure describes the two-way analysis of variance assessing the effect of substantia nigra pars compacta lesion and time on subthalamic nucleus high frequency dependent transmission of dopamine metabolites in the NAc. For further details see text
Discussion
Main findings of the present study comprise: 1. HFS of the STN increases DA neurotransmission and metabolism in the NAc shell and partly also NAc core. 2. Lesions of the VTA but not of the SNc prevent the modulatory impact of STN-HFS on the DA-system of the NAc. 3. HFS of the STN decreases GABA in the VTA. These data suggest that activation of DAergic neurons in the VTA, possibly via decreased inhibition of GABA, is largely responsible for the STN-HFS-induced increase in DA in the NAc.
The present animal findings indicate that STN-HFS modulates DAergic neurotransmission in limbic areas functionally interconnected with the STN. These data are selective for STN-stimulation at high frequencies as in an additional experiment we could not find any effect on accumbal DAergic neurotransmission following low-frequency stimulation (5 Hz) of the STN (Supplementary Fig. 1). The interconnections of the STN within the limbic basal ganglia-thalamo-cortical circuitry and the similarity between lesion and STN-HFS induced psychiatric effects in both, humans and rats (Absher et al. 2000; Hilker et al. 2004; Mandat et al. 2006; Stefurak et al. 2003; Temel et al. 2006; Trillet et al. 1995; Trost et al. 2006) suggest that the observed effects could be due to a specific action on the STN function. Yet, the present experimental design does not allow to differentiate, whether this effect is mediated by direct modulation of the STN or by current spread to adjacent structures (Ranck Jr. 1975). For instance, the STN is directly adjacent to the lateral hypothalamus (LH), which is highly interconnected with the NAc (DiLeone et al. 2003) and involved in the motivational aspects of behavior. Conceivably, current spread to passing fibers such as the medial forebrain bundle and/or adjacent brain areas such as the LH may potentially contribute to the effects of STN-HFS. In order to distinguish between direct HFS-dependent modulation of the STN activity from unspecific effects to neighboring brain areas and fiber tracts, the comparative investigation of different stimulation parameters (pulse duration, current intensity, and frequency), affecting the extent by which current spreads would be essential. Also an electrochemical method with higher temporary solution, i.e., in vivo cyclic voltammetry (Lee et al. 2006), would allow more detailed temporary information about the coupling of STN-HFS and DA release. The aim of the present study was, however, much more modest, and restricted to test the possibility that HFS of the STN as used in the clinical situation may have effects on neurotransmission in relevant limbic areas, which may contribute to explain the limbic side effects observed in PD patients undergoing STN-HFS. Importantly, current may spread and affect neighboring brain areas and nerve fibers, both, in the animal experimental as well as in the clinical situation (McIntyre et al. 2004a; Stefurak et al. 2003). Conclusive studies on how exactly STN-HFS affects limbic brain function would ultimately require clinical postmortem anatomical reconstruction and computational modeling, which to date are largely missing.
Data from human (Filali et al. 2004; Welter et al. 2004) and animal studies (Benazzouz et al. 2004; Meissner et al. 2005; Salin et al. 2002; Tai et al. 2003) show that selective stimulation of the STN at high frequencies reduces the activity of subthalamic neurons. In line with this hypothesis, similar behavioral effects of STN-HFS, STN lesion and pharmacological inactivation of the STN have been observed in both, PD patients and animal models of parkinsonism (Benazzouz et al. 1996; Darbaky et al. 2003; Deuschl et al. 2006; Levy et al. 2001; Limousin et al. 1995; Wichmann et al. 1994). Electrical stimulation is generally believed to excite nerve fibers rather than to directly act on cell bodies (Holsheimer et al. 2000; Nowak and Bullier 1998a, b). Consequently, the presumed inhibitory effect of STN-HFS might be due to a stimulation of presynaptic GABAergic axon terminals. Provided that inhibition of STN neurons represents the main mechanism, STN-HFS could relieve the projection sites of the STN from their excitatory glutamatergic input and normalize the thalamocortical information flow. Furthermore, modulatory effects of STN-HFS on glutamatergic STN efferens have been suggested to contribute to STN-HFS efficacy (Hashimoto et al. 2003; Maurice et al. 2003; McIntyre et al. 2004b; Stefani et al. 2005; Windels et al. 2000).
The results of the present study concerning involvement of VTA and GABA on STN-HFS-induced modulation of DAergic neurotransmission in the NAc [i.e., (a) toxic prelesion of the VTA antagonizes the effects of STN-HFS on DAergic neurotransmission in the NAc; (b) STN-HFS decreases GABA in the VTA] comply with previously reported clinical and experimental data: Thus, converging data from neuroanatomical studies of animals suggest that the STN is directly and/or indirectly connected to the VTA and NAc (Bonci and Malenka 1999; Hamani et al. 2004; Woods et al. 2002). Furthermore, VTA DA-neurons project to the NAc (Groenewegen et al. 1999) and are under the control of inhibitory GABAergic VTA-interneurons (Ikemoto et al. 1997; Westerink et al. 1996). These GABAergic VTA-interneurons may receive some modulating glutamatergic input from the STN, as has previously been suggested by an in vitro study of glutamate effects on VTA neurons in slices (Bonci and Malenka 1999). Thus, STN-HFS might relieve VTA DAergic neurons from their inhibitory GABAergic tone by modulating the excitatory drive on VTA interneurons, finally resulting in increased levels of DA in the NAc. Further studies allowing a definite coupling of STN-HFS and GABAergic control of DAergic VTA-NAc projection are needed to prove this hypothesis.
The assessment of the presented baseline values of accumbal DA reveals a structure-dependent differentiation of the DAergic load in the NAc core and shell, with basal DA levels being significantly higher in the NAc shell than in the NAc core. Interestingly, the HFS-dependent increases of DA and DA-metabolites were predominantly observed in the NAc shell; in fact, the increase of DA in the NAc core following STN-HFS failed to reach statistical significance. Ascending projections from the mesencephalon (A9 and A10) provide the DAergic innervation of the NAc, with the SNc (A9) projecting mainly to the NAc core and the VTA (A10) to the NAc shell (Groenewegen et al. 1999; Lindvall and Bjorklund 1974). Prelesions of VTA (A10) DAergic neurons lead to larger decreases in DAergic neurotransmission than prelesions of the SNc (A9). Anatomical differences might account for the quantitatively higher basal load and stronger effect of STN-HFS on DAergic transmission in the NAc shell when compared to the NAc core. Alternatively or additionally, different proportions of DA and its receptors in these subregions could be associated with the differential effects of STN-HFS-induced modulation of dopaminergic neurotransmission in the NAc shell versus core (Bassareo et al. 2002; Cadoni and Di 2000; Groenewegen et al. 1999; Ito et al. 2000).
Obviously, and as pointed out by two recent publications, STN-HFS dependent alteration in the DAergic neurotransmission of the NAc may not be the only way by which STN-HFS induces limbic effects: Accordingly, Mallet et al. (2007) found in a recent clinical study PET activation of cortical and thalamic regions under STN-HFS which were paralleled by a hypomanic state in two parkinsonian patients. Furthermore, Baunez et al. (2007) found that STN-HFS had partly similar effects in a visual attention task in both naïve and bilaterally DA-depleted rats, suggesting that some STN-HFS mediated limbic and/or cognitive functions may be independent of an intact DA system.
In conclusion, the present study supplies in vivo evidence in rats for a functional interaction of the STN with the DAergic VTA-NAc projection. Previously, a STN-HFS dependent increase in striatal DA has been suggested to contribute to the acute reversibility of PD symptoms while DAergic medication can be reduced up to 50% under STN-HFS (Lee et al. 2004, 2006; Meissner et al. 2003) Likewise, the present STN-HFS dependent increase in accumbal DA in naïve and SNc-prelesioned rats might present one possible explanation of some of the psychiatric effects of STN-HFS in PD.
References
Absher JR, Vogt BA, Clark DG, Flowers DL, Gorman DG, Keyes JW, Wood FB (2000) Hypersexuality and hemiballism due to subthalamic infarction. Neuropsychiatry Neuropsychol Behav Neurol 13:220–229
Albanese A, Piacentini S, Romito LM, Leone M, Franzini A, Broggi G, Bussone G (2005) Suicide after successful deep brain stimulation for movement disorders. Neurology 65:499–500
Alexander GE, Crutcher MD (1990) Functional architecture of basal ganglia circuits: neural substrates of parallel processing. Trends Neurosci 13:266–271
Alexander GE, Crutcher MD, DeLong MR (1990) Basal ganglia-thalamocortical circuits: parallel substrates for motor, oculomotor, “prefrontal” and “limbic” functions. Prog Brain Res 85:119–146
Alexander GE, DeLong MR, Strick PL (1986) Parallel organization of functionally segregated circuits linking basal ganglia and cortex. Annu Rev Neurosci 9:357–381
Bassareo V, De Luca MA, Di CG (2002) Differential expression of motivational stimulus properties by dopamine in nucleus accumbens shell versus core and prefrontal cortex. J Neurosci 22:4709–4719
Baunez C, Christakou A, Chudasama Y, Forni C, Robbins TW (2007) Bilateral high-frequency stimulation of the subthalamic nucleus on attentional performance: transient deleterious effects and enhanced motivation in both intact and parkinsonian rats. Eur J Neurosci 25:1187–1194
Bejjani BP, Houeto JL, Hariz M, Yelnik J, Mesnage V, Bonnet AM, Pidoux B, Dormont D, Cornu P, Agid Y (2002) Aggressive behavior induced by intraoperative stimulation in the triangle of Sano. Neurology 59:1425–1427
Benazzouz A, Boraud T, Feger J, Burbaud P, Bioulac B, Gross C (1996) Alleviation of experimental hemiparkinsonism by high-frequency stimulation of the subthalamic nucleus in primates: a comparison with L-Dopa treatment. Mov Disord 11:627–632
Benazzouz A, Piallat B, Pollak P, Benabid AL (1995) Responses of substantia nigra pars reticulata and globus pallidus complex to high frequency stimulation of the subthalamic nucleus in rats: electrophysiological data. Neurosci Lett 189:77–80
Benazzouz A, Tai CH, Meissner W, Bioulac B, Bezard E, Gross C (2004) High-frequency stimulation of both zona incerta and subthalamic nucleus induces a similar normalization of basal ganglia metabolic activity in experimental parkinsonism. FASEB J 18:528–530
Bonci A, Malenka RC (1999) Properties and plasticity of excitatory synapses on dopaminergic and GABAergic cells in the ventral tegmental area. J Neurosci 19:3723–3730
Boulet S, Lacombe E, Carcenac C, Feuerstein C, Sgambato-Faure V, Poupard A, Savasta M (2006) Subthalamic stimulation-induced forelimb dyskinesias are linked to an increase in glutamate levels in the substantia nigra pars reticulata. J Neurosci 26:10768–10776
Bruet N, Windels F, Carcenac C, Feuerstein C, Bertrand A, Poupard A, Savasta M (2003) Neurochemical mechanisms induced by high frequency stimulation of the subthalamic nucleus: increase of extracellular striatal glutamate and GABA in normal and hemiparkinsonian rats. J Neuropathol Exp Neurol 62:1228–1240
Cadoni C, Di CG (2000) Differential changes in accumbens shell and core dopamine in behavioral sensitization to nicotine. Eur J Pharmacol 387:R23–R25
Ceballos-Baumann AO, Boecker H, Bartenstein P, von F I, Riescher H, Conrad B, Moringlane JR, Alesch F (1999) A positron emission tomographic study of subthalamic nucleus stimulation in Parkinson disease: enhanced movement-related activity of motor-association cortex and decreased motor cortex resting activity. Arch Neurol 56:997–1003
Czernecki V, Pillon B, Houeto JL, Welter ML, Mesnage V, Agid Y, Dubois B (2005) Does bilateral stimulation of the subthalamic nucleus aggravate apathy in Parkinson’s disease? J Neurol Neurosurg Psychiatry 76:775–779
Darbaky Y, Forni C, Amalric M, Baunez C (2003) High frequency stimulation of the subthalamic nucleus has beneficial antiparkinsonian effects on motor functions in rats, but less efficiency in a choice reaction time task. Eur J Neurosci 18:951–956
Deuschl G, Schade-Brittinger C, Krack P, Volkmann J, Schafer H, Botzel K, Daniels C, Deutschlander A, Dillmann U, Eisner W, Gruber D, Hamel W, Herzog J, Hilker R, Klebe S, Kloss M, Koy J, Krause M, Kupsch A, Lorenz D, Lorenzl S, Mehdorn HM, Moringlane JR, Oertel W, Pinsker MO, Reichmann H, Reuss A, Schneider GH, Schnitzler A, Steude U, Sturm V, Timmermann L, Tronnier V, Trottenberg T, Wojtecki L, Wolf E, Poewe W, Voges J (2006) A randomized trial of deep-brain stimulation for Parkinson’s disease. N Engl J Med 355:896–908
DiLeone RJ, Georgescu D, Nestler EJ (2003) Lateral hypothalamic neuropeptides in reward and drug addiction. Life Sci 73:759–768
Doshi PK, Chhaya N, Bhatt MH (2002) Depression leading to attempted suicide after bilateral subthalamic nucleus stimulation for Parkinson’s disease. Mov Disord 17:1084–1085
Filali M, Hutchison WD, Palter VN, Lozano AM, Dostrovsky JO (2004) Stimulation-induced inhibition of neuronal firing in human subthalamic nucleus. Exp Brain Res 156:274–281
Fontaine D, Mattei V, Borg M, von LD, Magnie MN, Chanalet S, Robert P, Paquis P (2004) Effect of subthalamic nucleus stimulation on obsessive-compulsive disorder in a patient with Parkinson disease. Case report. J Neurosurg 100:1084–1086
Funkiewiez A, Ardouin C, Caputo E, Krack P, Fraix V, Klinger H, Chabardes S, Foote K, Benabid AL, Pollak P (2004) Long term effects of bilateral subthalamic nucleus stimulation on cognitive function, mood, and behaviour in Parkinson’s disease. J Neurol Neurosurg Psychiatry 75:834–839
Funkiewiez A, Ardouin C, Cools R, Krack P, Fraix V, Batir A, Chabardes S, Benabid AL, Robbins TW, Pollak P (2006) Effects of levodopa and subthalamic nucleus stimulation on cognitive and affective functioning in Parkinson’s disease. Mov Disord 21:1656–1662
Funkiewiez A, Ardouin C, Krack P, Fraix V, Van BN, Xie J, Moro E, Benabid AL, Pollak P (2003) Acute psychotropic effects of bilateral subthalamic nucleus stimulation and levodopa in Parkinson’s disease. Mov Disord 18:524–530
Groenewegen HJ, Wright CI, Beijer AV, Voorn P (1999) Convergence and segregation of ventral striatal inputs and outputs. Ann N Y Acad Sci 877:49–63
Gundersen HJ, Jensen EB (1987) The efficiency of systematic sampling in stereology and its prediction. J Microsc 147:229–263
Hamani C, Saint-Cyr JA, Fraser J, Kaplitt M, Lozano AM (2004) The subthalamic nucleus in the context of movement disorders. Brain 127:4–20
Hashimoto T, Elder CM, Okun MS, Patrick SK, Vitek JL (2003) Stimulation of the subthalamic nucleus changes the firing pattern of pallidal neurons. J Neurosci 23:1916–1923
Herzog J, Reiff J, Krack P, Witt K, Schrader B, Muller D, Deuschl G (2003) Manic episode with psychotic symptoms induced by subthalamic nucleus stimulation in a patient with Parkinson’s disease. Mov Disord 18:1382–1384
Hilker R, Voges J, Weisenbach S, Kalbe E, Burghaus L, Ghaemi M, Lehrke R, Koulousakis A, Herholz K, Sturm V, Heiss WD (2004) Subthalamic nucleus stimulation restores glucose metabolism in associative and limbic cortices and in cerebellum: evidence from a FDG-PET study in advanced Parkinson’s disease. J Cereb Blood Flow Metab 24:7–16
Holsheimer J, Demeulemeester H, Nuttin B, de SP (2000) Identification of the target neuronal elements in electrical deep brain stimulation. Eur J Neurosci 12:4573–4577
Ikemoto S, Kohl RR, McBride WJ (1997) GABA(A) receptor blockade in the anterior ventral tegmental area increases extracellular levels of dopamine in the nucleus accumbens of rats. J Neurochem 69:137–143
Ito R, Dalley JW, Howes SR, Robbins TW, Everitt BJ (2000) Dissociation in conditioned dopamine release in the nucleus accumbens core and shell in response to cocaine cues and during cocaine-seeking behavior in rats. J Neurosci 20:7489–7495
Kempermann G, Kuhn HG, Gage FH (1997) More hippocampal neurons in adult mice living in an enriched environment. Nature 386:493–495
Krack P, Kumar R, Ardouin C, Dowsey PL, McVicker JM, Benabid AL, Pollak P (2001) Mirthful laughter induced by subthalamic nucleus stimulation. Mov Disord 16:867–875
Kumar R, Lozano AM, Kim YJ, Hutchison WD, Sime E, Halket E, Lang AE (1998) Double-blind evaluation of subthalamic nucleus deep brain stimulation in advanced Parkinson’s disease. Neurology 51:850–855
Lee KH, Blaha CD, Harris BT, Cooper S, Hitti FL, Leiter JC, Roberts DW, Kim U (2006) Dopamine efflux in the rat striatum evoked by electrical stimulation of the subthalamic nucleus: potential mechanism of action in Parkinson’s disease. Eur J Neurosci 23:1005–1014
Lee KH, Chang SY, Roberts DW, Kim U (2004) Neurotransmitter release from high-frequency stimulation of the subthalamic nucleus. J Neurosurg 101:511–517
Levy R, Lang AE, Dostrovsky JO, Pahapill P, Romas J, Saint-Cyr J, Hutchison WD, Lozano AM (2001) Lidocaine and muscimol microinjections in subthalamic nucleus reverse Parkinsonian symptoms. Brain 124:2105–2118
Limousin P, Greene J, Pollak P, Rothwell J, Benabid AL, Frackowiak R (1997) Changes in cerebral activity pattern due to subthalamic nucleus or internal pallidum stimulation in Parkinson’s disease. Ann Neurol 42:283–291
Limousin P, Krack P, Pollak P, Benazzouz A, Ardouin C, Hoffmann D, Benabid AL (1998) Electrical stimulation of the subthalamic nucleus in advanced Parkinson’s disease. N Engl J Med 339:1105–1111
Limousin P, Pollak P, Benazzouz A, Hoffmann D, Le Bas JF, Broussolle E, Perret JE, Benabid AL (1995) Effect of parkinsonian signs and symptoms of bilateral subthalamic nucleus stimulation. Lancet 345:91–95
Lindvall O, Bjorklund A (1974) The organization of the ascending catecholamine neuron systems in the rat brain as revealed by the glyoxylic acid fluorescence method. Acta Physiol Scand Suppl 412:1–48
Mallet L, Mesnage V, Houeto JL, Pelissolo A, Yelnik J, Behar C, Gargiulo M, Welter ML, Bonnet AM, Pillon B, Cornu P, Dormont D, Pidoux B, Allilaire JF, Agid Y (2002) Compulsions, Parkinson’s disease, and stimulation. Lancet 360:1302–1304
Mallet L, Schupbach M, N’Diaye K, Remy P, Bardinet E, Czernecki V, Welter ML, Pelissolo A, Ruberg M, Agid Y, Yelnik J (2007) Stimulation of subterritories of the subthalamic nucleus reveals its role in the integration of the emotional and motor aspects of behavior. Proc Natl Acad Sci USA 104:10661–10666
Mandat TS, Hurwitz T, Honey CR (2006) Hypomania as an adverse effect of subthalamic nucleus stimulation: report of two cases. Acta Neurochir (Wien) 148:895–897
Maurice N, Thierry AM, Glowinski J, Deniau JM (2003) Spontaneous and evoked activity of substantia nigra pars reticulata neurons during high-frequency stimulation of the subthalamic nucleus. J Neurosci 23:9929–9936
McIntyre CC, Mori S, Sherman DL, Thakor NV, Vitek JL (2004a) Electric field and stimulating influence generated by deep brain stimulation of the subthalamic nucleus. Clin Neurophysiol 115:589–595
McIntyre CC, Savasta M, Walter BL, Vitek JL (2004b) How does deep brain stimulation work? Present understanding and future questions. J Clin Neurophysiol 21:40–50
Meissner W, Harnack D, Reese R, Paul G, Reum T, Ansorge M, Kusserow H, Winter C, Morgenstern R, Kupsch A (2003) High-frequency stimulation of the subthalamic nucleus enhances striatal dopamine release and metabolism in rats. J Neurochem 85:601–609
Meissner W, Leblois A, Hansel D, Bioulac B, Gross CE, Benazzouz A, Boraud T (2005) Subthalamic high frequency stimulation resets subthalamic firing and reduces abnormal oscillations. Brain 128:2372–2382
Meissner W, Reum T, Paul G, Harnack D, Sohr R, Morgenstern R, Kupsch A (2001) Striatal dopaminergic metabolism is increased by deep brain stimulation of the subthalamic nucleus in 6-hydroxydopamine lesioned rats. Neurosci Lett 303:165–168
Moro E, Esselink RJ, Xie J, Hommel M, Benabid AL, Pollak P (2002) The impact on Parkinson’s disease of electrical parameter settings in STN stimulation. Neurology 59:706–713
Nowak LG, Bullier J (1998a) Axons, but not cell bodies, are activated by electrical stimulation in cortical gray matter. I. Evidence from chronaxie measurements. Exp Brain Res 118:477–488
Nowak LG, Bullier J (1998b) Axons, but not cell bodies, are activated by electrical stimulation in cortical gray matter. II. Evidence from selective inactivation of cell bodies and axon initial segments. Exp Brain Res 118:489–500
Okun MS, Green J, Saben R, Gross R, Foote KD, Vitek JL (2003) Mood changes with deep brain stimulation of STN and GPi: results of a pilot study. J Neurol Neurosurg Psychiatry 74:1584–1586
Paul G, Reum T, Meissner W, Marburger A, Sohr R, Morgenstern R, Kupsch A (2000) High frequency stimulation of the subthalamic nucleus influences striatal dopaminergic metabolism in the naive rat. Neuroreport 11:441–444
Paxinos G, Watson C (1997) The rat brain. Ref type: generic. Academic, London
Payoux P, Remy P, Damier P, Miloudi M, Loubinoux I, Pidoux B, Gaura V, Rascol O, Samson Y, Agid Y (2004) Subthalamic nucleus stimulation reduces abnormal motor cortical overactivity in Parkinson disease. Arch Neurol 61:1307–1313
Ranck JB Jr (1975) Which elements are excited in electrical stimulation of mammalian central nervous system: a review. Brain Res 98:417–440
Romito LM, Raja M, Daniele A, Contarino MF, Bentivoglio AR, Barbier A, Scerrati M, Albanese A (2002) Transient mania with hypersexuality after surgery for high frequency stimulation of the subthalamic nucleus in Parkinson’s disease. Mov Disord 17:1371–1374
Salin P, Manrique C, Forni C, Kerkerian-Le GL (2002) High-frequency stimulation of the subthalamic nucleus selectively reverses dopamine denervation-induced cellular defects in the output structures of the basal ganglia in the rat. J Neurosci 22:5137–5148
Stefani A, Fedele E, Galati S, Pepicelli O, Frasca S, Pierantozzi M, Peppe A, Brusa L, Orlacchio A, Hainsworth AH, Gattoni G, Stanzione P, Bernardi G, Raiteri M, Mazzone P (2005) Subthalamic stimulation activates internal pallidus: evidence from cGMP microdialysis in PD patients. Ann Neurol 57:448–452
Stefurak T, Mikulis D, Mayberg H, Lang AE, Hevenor S, Pahapill P, Saint-Cyr J, Lozano A (2003) Deep brain stimulation for Parkinson’s disease dissociates mood and motor circuits: a functional MRI case study. Mov Disord 18:1508–1516
Steiner B, Kronenberg G, Jessberger S, Brandt MD, Reuter K, Kempermann G (2004) Differential regulation of gliogenesis in the context of adult hippocampal neurogenesis in mice. Glia 46:41–52
Steiner B, Winter C, Hosman K, Siebert E, Kempermann G, Petrus DS, Kupsch A (2006) Enriched environment induces cellular plasticity in the adult substantia nigra and improves motor behavior function in the 6-OHDA rat model of Parkinson’s disease. Exp Neurol 199:291–300
Tai CH, Boraud T, Bezard E, Bioulac B, Gross C, Benazzouz A (2003) Electrophysiological and metabolic evidence that high-frequency stimulation of the subthalamic nucleus bridles neuronal activity in the subthalamic nucleus and the substantia nigra reticulata. FASEB J 17:1820–1830
Temel Y, Kessels A, Tan S, Topdag A, Boon P, Visser-Vandewalle V (2006) Behavioural changes after bilateral subthalamic stimulation in advanced Parkinson disease: a systematic review. Parkinsonism Relat Disord 12:265–272
Thobois S, Mertens P, Guenot M, Hermier M, Mollion H, Bouvard M, Chazot G, Broussolle E, Sindou M (2002) Subthalamic nucleus stimulation in Parkinson’s disease: clinical evaluation of 18 patients. J Neurol 249:529–534
Trillet M, Vighetto A, Croisile B, Charles N, Aimard G (1995) Hemiballismus with logorrhea and thymo-affective disinhibition caused by hematoma of the left subthalamic nucleus. Rev Neurol (Paris) 151:416–419
Trost M, Su S, Su P, Yen RF, Tseng HM, Barnes A, Ma Y, Eidelberg D (2006) Network modulation by the subthalamic nucleus in the treatment of Parkinson’s disease. Neuroimage 31:301–307
Welter ML, Houeto JL, Bonnet AM, Bejjani PB, Mesnage V, Dormont D, Navarro S, Cornu P, Agid Y, Pidoux B (2004) Effects of high-frequency stimulation on subthalamic neuronal activity in parkinsonian patients. Arch Neurol 61:89–96
Westerink BH, Kwint HF, deVries JB (1996) The pharmacology of mesolimbic dopamine neurons: a dual-probe microdialysis study in the ventral tegmental area and nucleus accumbens of the rat brain. J Neurosci 16:2605–2611
Wichmann T, Bergman H, DeLong MR (1994) The primate subthalamic nucleus. III. Changes in motor behavior and neuronal activity in the internal pallidum induced by subthalamic inactivation in the MPTP model of parkinsonism. J Neurophysiol 72:521–530
Windels F, Bruet N, Poupard A, Feuerstein C, Bertrand A, Savasta M (2003) Influence of the frequency parameter on extracellular glutamate and gamma-aminobutyric acid in substantia nigra and globus pallidus during electrical stimulation of subthalamic nucleus in rats. J Neurosci Res 72:259–267
Windels F, Bruet N, Poupard A, Urbain N, Chouvet G, Feuerstein C, Savasta M (2000) Effects of high frequency stimulation of subthalamic nucleus on extracellular glutamate and GABA in substantia nigra and globus pallidus in the normal rat. Eur J Neurosci 12:4141–4146
Winter C, Hosmann K, Harnack D, Meissner W, Paul G, Morgenstern R, Kupsch A (2006) Subthalamic nucleus lesioning inhibits expression and phosphorylation of c-Jun in nigral neurons in the rat’s 6-OHDA model of Parkinson’s disease. Synapse 60:69–80
Winter C, Schenkel J, Burger E, Eickmeier C, Zimmermann M, Herdegen T (2000) The immunophilin ligand FK506, but not GPI-1046, protects against neuronal death and inhibits c-Jun expression in the substantia nigra pars compacta following transection of the rat medial forebrain bundle. Neuroscience 95:753–762
Witjas T, Baunez C, Henry JM, Delfini M, Regis J, Cherif AA, Peragut JC, Azulay JP (2005) Addiction in Parkinson’s disease: impact of subthalamic nucleus deep brain stimulation. Mov Disord 20:1052–1055
Witt K, Daniels C, Herzog J, Lorenz D, Volkmann J, Reiff J, Mehdorn M, Deuschl G, Krack P (2006) Differential effects of L-dopa and subthalamic stimulation on depressive symptoms and hedonic tone in Parkinson’s disease. J Neuropsychiatry Clin Neurosci 18:397–401
Woods SP, Fields JA, Troster AI (2002) Neuropsychological sequelae of subthalamic nucleus deep brain stimulation in Parkinson’s disease: a critical review. Neuropsychol Rev 12:111–126
Acknowledgments
We wish to thank C. Koelske and R. Winter for their excellent technical assistance. This study was supported by the grants Ku 830/3-1 and 3-3 (DFG, Germany) and QLK6-CT-1999-02173 (European Community). C. W. is a Rahel-Hirsch Fellow of the Humboldt University, Berlin, Germany.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Winter, C., Lemke, C., Sohr, R. et al. High frequency stimulation of the subthalamic nucleus modulates neurotransmission in limbic brain regions of the rat. Exp Brain Res 185, 497–507 (2008). https://doi.org/10.1007/s00221-007-1171-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00221-007-1171-1