Abstract
Background
While accumulating research has tested the hypothesis that screen time causes psychiatric symptoms in children, less attention has been paid to the hypothesis that children with psychiatric symptoms change their patterns of screen time and digital media use. We aimed to test whether children with psychiatric symptoms subsequently change their patterns of screen time and digital media use.
Methods
N = 9,066 children primarily aged 9–10 in the Adolescent Brain Cognitive Development Study at baseline and 1-year later. Psychiatric symptoms included internalizing, attention, and externalizing symptoms. Screen time was measured as ordinally defined weekday and weekend time on social and nonsocial [e.g., YouTube] digital media). Models assessed psychiatric symptoms as predictors of screen time, and screen time as predictors of psychiatric symptoms, controlled for baseline measures of each, sex, age, race/ethnicity, and income.
Results
Children with psychiatric symptoms spent more time on non-social media one year later compared with peers. Considering total psychiatric problems, clinical levels of problems predicted higher levels of weekday (OR = 1.22, 95% CI 1.22–1.23) and weekend (OR = 1.10, 95% CI 1.09–1.11) nonsocial screen time. For nearly all analyses of psychiatric symptoms predicting screen time, associations were highest for a non-social screen time outcome rather than a social screen time outcome (Highest OR = 1.65, 95% CI 1.63–1.67, clinical rule breaking predicting weekday nonsocial screen time). Comparable magnitude associations were observed for social and nonsocial media use predicting future psychiatric symptoms, suggesting bidirectionality.
Conclusion
Children with psychiatric symptoms have different subsequent media use patterns, including higher rates of subsequent nonsocial engagement. Ensuring that ongoing data collection and analysis efforts attend to temporality and transitions in the relation between media use and psychiatric symptoms will accelerate progress in the field.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Psychiatric symptoms and disorders often onset in childhood and adolescence [1], are prevalent [2], and are associated with substantial distress, impairment, and additional morbidity and mortality [3]. Broad categories of psychiatric symptoms include internalizing symptoms and disorders such as depressive and anxious symptoms, attention deficits and hyperactivity, as well as externalizing symptoms such as conduct problems and oppositional defiance [4, 5]. In the past decade, there has been considerable evidence that internalizing symptoms among youth are increasing at rates that are historically unprecedented in at least the last four decades [6, 7], while externalizing symptoms are simultaneously declining rapidly [8, 9]. Understanding novel risk factors for these symptoms, or changes in the prevalence or strength of existing risk factors, is key to identifying the causes of symptom distribution changes in a rapidly changing environment for intervention and prevention efforts.
Screen time and social media use have increased during the same time period in which youth internalizing symptoms have increased [10], and are often hypothesized to be a central contributor to increases in these symptoms [11]. Screen time and social media use are posited to influence youth internalizing symptoms through numerous pathways, including increased social isolation, exposure to violent or depressogenic content, envy and comparison, and cyberbullying, as well as other potential pathways [10, 12]. Yet, the evidence for the effects of screen time and social media use on internalizing symptoms remains inconsistent; two recent reviews of reviews of the literature, covering more than 50 studies, concluded that the existing evidence base is relatively weak, with generally small effect sizes and study designs that do not allow for robust causal inference [10, 13, 14]. Other studies, however, have suggested harmful associations between screen time and adolescent psychiatric symptoms [15, 16].
Additional empirical literature has evaluated the role of screen and media use on attention symptoms in children and adolescents [17,18,19]; it has been hypothesized that video games, television, and short-video (e.g. YouTube videos, TikToks) may influence attention symptoms through several pathways, including teaching attentional styles focused on short scan and shift, arousal changes through rapid attention shifts, as well as through displacing activities that would practice longer attention spans [17]. Existing meta-analyses of the relation between patterns of screen use and attention symptoms are also inconclusive, however, with a majority of studies identified as cross-sectional [17,18,19]; several longitudinal studies have found that while various screen time patterns are associated with attention symptoms, there is also evidence for the reverse pathway: that children and adolescents with attention symptoms and disorders prefer activities that do not require long attention spans [20, 21]. Studies covering externalizing symptoms and disorders (oppositional defiant symptoms, conduct problems) with patterns of screen time have largely focused on violent video games, with evidence for significant effects as well as subgroup selection (i.e., children with aggressive traits more likely to select violent video games) [18, 22]. Broader patterns of externalizing symptoms and other forms of screen time including social media use are a significant gap in the literature.
Taken together, a central threat to inference on the relation between psychiatric symptoms and screen time that has been consistently identified in previous reviews as not sufficiently examined is reverse causation; that is, while screen time and social media use are hypothesized to increase psychiatric symptoms and disorders, it remains less adequately investigated whether psychiatric symptoms and disorders may influence patterns of screen time and social media use. Existing evidence supports such pathways, with data demonstrating that adolescents with internalizing psychiatric symptoms report different, and often more distressing, patterns of social media and screen use than those without [23,24,25,26]. Further, evidence supports the hypothesis that children with ADHD symptoms prefer online activities with shorter time windows [27,28,29]. Available evidence, however, is limited, with small sample sizes and non-representative target populations, and limited attention to how these associations unfold over time; the paucity of robust evidence on the pathway from psychiatric symptoms to screen time and social media use is concerning given the growing number of studies that reflexively conclude that correlations reflect the reverse path.
Utilizing comprehensive and population-based longitudinal data from the Adolescent Brain and Cognitive Development (ABCD) study, among the largest and most recent population-based studies of youth in the US, the present study takes on the question of psychiatric symptoms as a potential cause of social media and screen time use. Specifically, we aim to examine whether and how psychiatric symptoms, including internalizing, externalizing, and attention symptoms as well as subscales of specific symptom patterns influence screen use, both social (e.g., social media, texting) and nonsocial (e.g., YouTube, video games), one year later. We also construct comparable models for the association between screen time use and later psychiatric symptoms in order to provide a comprehensive assessment of the relative strengths of the alternative pathways.
Methods
Research was conducted in accordance with ethical standards laid out in the Helsinki Declaration, and was approved by the Institutional Review Board of Columbia University: IRB # IRB-AAAU0102.
Sample
Data are drawn from the Adolescent Brain and Cognitive Development (ABCD) study, a longitudinal multisite study designed to examine the risk for, and development of, mental and physical health outcomes using multiple methods detailed in Barch et al., 2018 [30]. Youth and their parents completed in-person assessments at baseline and one-year later. The data were collected using an epidemiologically-informed approached to approximate the US population by recruiting from a geographically and demographically diverse set of 21 sites [31, 32]. Baseline data was collected between September 2016 and August 2018, examining primarily 9 and 10-year-olds (N = 11,876). A one-year follow up was conducted from 2017–2019, resulting in 10,001 respondents successfully followed up with a non-zero weight. Among these youth, 9,066 had complete information on psychiatric symptoms, screen time, and demographics (described below), suggesting 9.3% of the initial follow-up sample had missingness. This suggests that missingness was not substantial and was left unimputed. ABCD data release 4.0 was used, and a propensity weight was used for all analyses approximating American Community Survey sociodemographic of 9 and 10-year-olds [33].
Measures
Demographics
Parents reported children’s demographic information on a survey, including children’s sex, age, race, and ethnicity, and family income.
Screen time
The Youth Screen Time Survey queried youth about the amount of time they spent using screens for six different activities at baseline and follow up one year later, based on a previously validated measure [34]. Items were rated on a 7-point scale (0 = none; 0.25 = < 30 min; 0.5 = 30 min, 1 = 1 h; 2 = 2 h; 3 = 3 h; 4 = 4 + hours)[35]. Activities were queried separately for typical weekend versus weekday use. We constructed social screen time variables, which summed time spent texting, using social media, and video chatting separately on weekends and weekdays, and nonsocial screen time variables, which summed time spent watching TV shows or movies, watching videos on YouTube, and playing video games, also separately on weekend and weekday. We examined distributions of the screen time measures (see Appendix A), many of which were highly right skewed. Due to the skew of these variables, we trichotomized them across waves 1 and 2 based on percentile rank (i.e., 1–33, 34–66, 67–100). This resulted in the following categorizations: 0 h [reference group], 0.25–0.5 h, and 0.75–12 h as low, medium, and high screen time for weekday and weekend social use, 0–1.5 [ref], 1.75–3.5, and 3.75–12 h for weekday non-social use, and 0–2.5 [ref], 2.75–5, and 5.25–12 for weekend non-social use.
Psychiatric symptoms
Psychiatric symptoms were assessed at each wave with the Child Behavior Checklist (CBCL), a 112-item parent-/guardian-report of children’s psychiatric symptoms and behaviors [36]. Items were rated on a 3-point scale (0 = not true; 2 = very true/often true) and summed into subscales, which were in turn T-scored using age and gender norms. Scales included total problems and the three higher-order subscales of internalizing, externalizing, and attention, as well as the internalizing subscales of withdrawn-depressive and anxious-depressive symptoms, and the externalizing subscales of rule-breaking and aggressive behavior. These subscales have all been tested for validity and reliability [37, 38]. Continuous symptom measures were highly right skewed (see Appendix A), and regression models accommodating continuous right skewed outcome measures did not provide adequate model fit. Thus, we used recommended cut-scores to stratify data into non-significant symptoms, borderline symptoms, and clinical symptoms. Typically, borderline scores ranged from 65 to 69, while clinical scores were 70 + , though with lower thresholds for internalizing, externalizing, and total problems, 60–63 for borderline and 64 + for clinical [39, 40]. In models, trichotomous psychiatric symptom categories were dummy-coded; Non-significant symptoms served as the reference group for all models.
Analysis
Modeling. Our primary analysis examined psychiatric symptoms as independent variables and weekday and weekend social and nonsocial screen time use one year later as dependent variables. We modeled the effects of psychiatric symptoms, with each scale and subscale measured as trichotomized variables (ref = Non-significant symptoms), on screen use, measured as trichotomous variables due to skewness, using cumulative logistic regression in R using the VGAM package [41]. All models controlled for screen use at baseline, thus the models are residualized change models. We also included children’s sex (female [ref] vs male), age (continuous, range: 107 months to 132 months), race and ethnicity (Non-Hispanic White [ref], Non-Hispanic Black, Hispanic/Latino, Non-Hispanic Other), and family income (< 50,000 [ref], 50,000–100,000, > 100,000) at baseline as control variables. Effects can thus be understood as how much greater or smaller the odds of the outcome are given scores at baseline, and beyond the effects of demographic characteristics.
In supplementary analyses, we examined screen use as independent variables and psychiatric problems one year later as dependent variables. These models controlled for the respective baseline measurement of screen time, as well as all demographic variables. Here, baseline screen time and future psychiatric symptoms were structured identically to their counterparts in the primary analysis.
Results
Study sample
See Table 1 for sample characteristics. A little under half of the sample was female, a majority were white, and about one-fifth were Hispanic or Latino. On average, children were just under 10 years old at the baseline visit. About 44% of families had an income greater than $100,000.
Association between psychiatric symptoms and future screen use
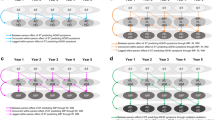
We estimated the association between baseline psychiatric symptoms on social and nonsocial weekend and weekday screen use one year later in a series of residualized change models adjusted for demographic covariates: age, sex, race/ethnicity, and household income at baseline (Fig. 1; odds ratios that comprise Fig. 1 shown in Supplementary Table 1).
Considering total psychiatric problems, clinical levels of problems predicted higher levels of screen time compared to peers one year later, across weekday social (OR = 1.02, 95% CI 1.01–1.02), weekday nonsocial (OR = 1.22, 95% CI 1.22–1.23), weekend social (OR = 1.15, 95% CI 1.14–1.15), and weekend nonsocial (OR = 1.10, 95% CI 1.09–1.10). Generally, across most categories of psychiatric problems, associations were strongest for a form of non-social screen time rather than social screen time. However, it should be noted that the OR of 1.65 for clinical rule breaking predicting high weekday nonsocial screen time constitutes the largest effect in these primary results, suggesting that while patterns were consistent, the magnitude of any effects were generally of small magnitude.
The general pattern that clinical and borderline levels of psychiatric symptoms predicted higher levels of non-social screen time one year later was found for many of the psychiatric symptom categories. Higher levels of non-social screen time, especially among those with clinical symptoms and for weekday nonsocial screen use, were observed for internalizing symptoms (OR = 1.17, 95% CI 1.17–1.18), the internalizing symptom subscales of depressive symptoms (OR = 1.24, 95% CI 1.23–1.25), anxiety/depressive symptoms (OR = 1.04, 95% CI 1.03–1.05) and withdrawn depressive symptoms (OR = 1.39, 95% CI 1.38–1.41), externalizing symptoms (OR = 1.27, 95% CI 1.26–1.27), and the externalizing symptom subscales of aggression (OR = 1.14, 95% CI 1.12–1.15) and rule breaking (OR = 1.65, 95% CI 1.63–1.67).
Additionally, a general pattern emerged of higher levels of some psychiatric symptom categories, especially internalizing symptoms, predicting null or lower levels of social screen time one year later compared with peers who had lower levels of psychiatric symptoms. For example, Fig. 1 shows that children with clinical levels of internalizing problems were less likely to be in a high screen time use category one year later than those with no significant internalizing problems (OR = 0.92, 95% CI 0.92–0.93 for weekday social, OR = 0.98, 95% CI 0.97–0.98 for weekend social), controlling for their baseline screen time use. Additional inverse or null associations were observed for multiple assessments of internalizing subscales and social screen time. Take, for instance, withdrawn depressive symptoms; children with clinical levels of withdrawn depressive symptoms were less likely to be in weekday high (OR = 0.74, 95% CI 0.74–0.75), weekend high (OR = 0.86, 95% CI 0.85–0.86), weekday medium (OR = 0.73, 95% CI 0.73–0.74), or weekend medium (OR = 0.80, 95% CI 0.80–0.81) social screen time categories one year later. However, it is worth noting that these associations, while consistent, are smaller.
Associations between externalizing symptoms and social screen time were more variable, but we found that clinical levels of externalizing and rule breaking predicted high social screen time compared with peers one year later for both weekday (externalizing: OR = 1.15, 95% CI 1.14–1.15; rule breaking: OR = 1.14, 95% CI 1.13–1.15) and weekend screen time (externalizing: OR = 1.27, 95% CI 1.27–1.28; rule breaking: OR = 1.35, 95% CI 1.34–1.36). Inverse or null associations emerged for many externalizing and externalizing subscale problems, particularly with medium screen time use, but nearly all inverse associations were observed for social screen time use; nonsocial screen time use was typically elevated at all levels of externalizing problems.
Association between screen use and future psychiatric symptoms
Supplementary Fig. 1 and Supplementary Table 2 shows the reverse association as Supplementary Table 1; baseline screen use predicting future mental health problems, again adjusting for demographic covariates, and additionally adjusting for baseline mental health problems.
Generally, the reverse associations were similar in direction and strength; higher screen time was associated with elevated levels of psychiatric symptoms the following year across subscales compared to peers with lower screen time, with stronger associations for non-social screen use.
Higher social weekday (OR = 1.11, 95% CI 1.10–1.12) and weekend (OR = 1.12, 95% CI 1.11–1.13), nonsocial weekday (OR = 1.27, 95% CI 1.26–1.28), and nonsocial weekend (OR = 1.47, 95% CI 1.46–1.48) screen time predicted clinical total psychiatric problems compared to peers one year later, controlling for baseline psychiatric problems. Higher levels of non-social screen time, especially among those with clinical symptoms and for weekday screen use, predicted ADHD (OR = 2.17, 95% CI 2.15–2.21), internalizing symptoms (OR = 1.18, 95% CI 1.17–1.19), the internalizing symptom subscales of depressive symptoms (OR = 1.12, 95% CI 1.11–1.13) and withdrawn depressive symptoms (OR = 1.37, 95% CI 1.36–1.39), and externalizing subscales of aggression (OR = 1.15, 95% CI 1.13–1.16) and rule breaking (OR = 1.96, 95% CI 1.93–1.99). Still, many associations were null or inverse, such as those with higher levels of weekday and weekend social screen time being less likely to have clinical levels of withdrawn depressive symptoms (weekday: OR = 0.70, 95% CI 0.69–0.71; weekend: OR = 0.67, 95% CI 0.66–0.68).
Taken together, these analyses indicate that there are observed associations between screen time use and psychiatric symptoms one year later. Coupled with Table 1 indicating associations between psychiatric symptoms and screen time use one year later, together these analyses suggest that associations are bidirectional. Of note, the magnitude of associations in both directions are of similar magnitude.
Discussion
Psychiatric symptoms in early adolescence predict different patterns of subsequent screen time and social media use. We demonstrate in the present paper that, controlling for baseline screen time patterns, internalizing and externalizing symptoms typically predict lower or unchanging social screen use (social media, texting, video chatting), while elevated symptoms across domains typically predict higher nonsocial screen use (e.g., YouTube, videogames), particularly on weekdays, one year later compared to peers without such symptoms. Associations between screen use and future psychiatric symptoms, across domains and subscales, were of comparable magnitude, suggestive of bidirectional and potentially reinforcing relationships. The magnitude of associations between screen time and later psychiatric symptoms was comparable to the magnitude of associations in the opposite direction. Taken together, these results add to the literature on the role of technology in the lives of adolescence, supporting the hypothesis that correlations between screen time and mental health arise, in part, due to the impact of psychiatric symptoms on future screen use. However, magnitudes of association where generally small across all comparisons.
These results should be situated alongside the developing literature on the association between patterns of digital media and screen time on child and adolescent mental health. Much of the existing research is cross-sectional and correlational, thus while the stated hypothesis may be that screen time may affect mental health, the reverse pathway cannot be differentiated. Even in longitudinal data, the lack of robust analytical approaches that attend to pre-existing psychiatric symptoms renders questionable inference. Reviews of existing literature consistently find that the direction and magnitude of associations between various measures of screen time and mental health are highly heterogeneous, with positive, negative, and null findings throughout the literature depending on the measures, age groups, and study design [10, 14]. In addition to study design and measurement heterogeneity, a potential driver of differences in results may be the lack of explicit causal theoretical models and identification strategies [42] that attend to the types of selection effects that we identify here: that people with psychiatric symptoms use screen time and social media differently than those without psychiatric symptoms. Recognizing these selection effects allows for a nuanced understanding of the connection between psychiatric symptoms and screen time seen in our results: a bidirectional, likely mutually reinforcing link.
Further, studies predominantly examine internalizing symptoms, such as depressive and anxious symptoms, while our results suggest that the findings with externalizing symptoms are robust. Externalizing and attention symptoms may be indicative of a greater desire for stimulation, activity, and distraction, thus extended YouTube and videogame play may be especially reinforcing and may explain why youth with these symptoms select into these media use patterns. Further, given the correlational meta-structure of internalizing and externalizing symptoms, additional attention to broader patterns of comorbidity in psychiatric phenomenology is a critical area for ongoing research.
Literature that has examined psychiatric disorders and symptoms as a potential cause of differences in screen time is consistent with the current study. Early reviews and meta-analyses found evidence for selection effects in social media use; for example, an early 2014 meta-analysis reported that individuals with higher levels of loneliness spent more time on Facebook [43], setting the stage for hypotheses that people select into their patterns of screen time based on mood and mental health status. As the literature has progressed throughout the last decade, and as child and adolescent patterns of online time use have grown in frequency, and popular platforms have shifted, so too has the available evidence for a nuanced understanding of the role of media in youth mental health. Available evidence indicates that youths' offline lives often spill into their online lives, with youth who are marginalized and bullied offline often experiencing the most negative interactions with peers online as well [10, 13, 26, 44]. This may underlie our finding that children with psychiatric symptoms, including internalizing, attention, and externalizing symptoms, often report more non-social screen time one year later than children without those symptoms. Children with psychiatric symptoms are often stigmatized and targeted for victimization, and these peer experiences may lead children with symptoms to pursue more solitary activities online. Additional pathways for particular symptoms may also underlie observed associations.
Given that children with psychiatric symptoms typically engage in greater subsequent nonsocial screen time than their peers, it is worth noting that treatment for mental health symptoms through smart phone-based technology is increasingly feasible, low cost and accessible. Treatment engagement among youth with psychiatric symptoms and disorders remains frustratingly low and providers are increasingly overwhelmed with requests, resulting in significant delays in care. However, the evidence base for efficacy of smartphone delivery modalities for treatment is generally weak [45], although evidence for reductions in depressive symptoms is emerging [46]. The accessibility of these treatments, however, should be considered alongside their potential for harm; many of these app-based programs are developed by for-profit enterprises with little adherence to treatment best-practices or training for providers. In particular, disorders and symptoms that require medication management benefit from higher levels of care. For example, one app-based company recently stopped prescribing Adderall, a common medication therapy for attention deficit hyperactivity disorder, after reports revealed excessive prescribing with little oversight or competent provider expertise or evaluation [47]. Nevertheless, more independent research into how to use teletherapy and app-based approaches to reach adolescents who are experiencing psychiatric symptoms is important moving forward given the accessibility through smart phones and potential to increase access to care.
Additionally, the development of research tools and measurements to capture more nuanced ways in which youth use media is increasingly urgent. Considerable research, including ours, uses basic measures of amount of time spent using various forms of media. As has been thoroughly discussed in existing literature synthesizing results of available studies [10, 14], the activities that children and adolescents engage in online are diverse in intention, content and goal, and thus may be diffuse in their effects. Engagement on social media may increase positive emotions related to social connectedness, for example, while simultaneously increasing distress. Studies have found that associations with psychiatric symptoms differ depending on whether adolescents are actively engaging with peers online versus passively scrolling and consuming content [14, 48]. As ubiquitous digital engagement among children is increasingly constant, basic measures of time spent online may become irrelevant. This has been made even more clear during the COVID-19 pandemic, as many children and adolescents ceased in-person learning and social activities during the height of pandemic-related closures.
The present study should be considered with limitations. As noted above, time spent using various forms of screen time are relatively crude metrics for the totality of adolescent engagement with digital media. We were limited by the measures included in the ABCD study, which has notable strengths, but acknowledge that we may be missing associations due to imperfect construct capture. All psychiatric symptoms are reported by parent or guardian. Caregivers may not be aware of all psychiatric symptoms in children, and particularly for symptoms such as attention problems, teacher reports are useful adjuncts. However, given that these participants are children, parent reports are likely most valid for most constructs presented here [49]. Finally, while we were able to adjust for a number of important covariates, the analyses presented here are based on observational data and are thus subject to interpretation with caution as there may be unmeasured confounding. Measures were highly skewed [50], which resulted in the need to trichotomize for model fit, but potentially reduces statistical power to detect relationships; further psychometric work on measuring psychiatric and screen time constructs would be beneficial.
Identifying children with psychiatric symptoms, and aligning them with effective and available providers, remains a critical public health goal. While the digital age has changed the nature of the way children and adolescents interact, it also provides new opportunities for connection and engagement. Providing guidance and platforms for children and adolescents to engage safely with peers online, building support networks for children and adolescents who have marginalized identities and are stigmatized (often due to psychiatric symptoms) may be especially beneficial, as sense of belonging and connection can be especially preventative and ameliorative of mental health problems. Online sources of hateful conduct and bullying should be addressed, as they contribute to mental health problems in children and adolescents. However, this paper demonstrates that correlations between mental health and screen time reflects a potentially causal role for both screen time on mental health and mental health on screen time, and this bidirectional association needs to be teased apart for public health recommendations. Ensuring that ongoing data collection and analysis efforts rigorously attend to temporality and transitions, as well as consideration of alternative causes, will accelerate progress in the field.
Data availability
Data from the ABCD study is available for research through https://abcdstudy.org/scientists/data-sharing/.
Change history
05 June 2024
A Correction to this paper has been published: https://doi.org/10.1007/s00127-024-02699-x
References
Solmi M, Radua J, Olivola M et al (2021) Age at onset of mental disorders worldwide: large-scale meta-analysis of 192 epidemiological studies. Mol Psychiatry 271(27):281–295
Kessler RC, Angermeyer M, Anthony JC et al (2007) Lifetime prevalence and age-of-onset distributions of mentaldisorders in the world health organization’s world mental health survey initiative. World Psychiatry 6:168
Ferrari A (2022) Global, regional, and national burden of 12 mental disorders in 204 countries and territories, 1990–2019: a systematic analysis for the global burden of disease study 2019. Lancet Psychiatry 9:137–150
Keyes KM, Eaton NR, Krueger RF et al (2013) Thought disorder in the meta-structure of psychopathology. Psychol Med 43:1673–1683
Krueger RF (1999) The structure of common mental disorders. Arch Gen Psychiatry 56:921–926
Kreski NT, Chen Q, Olfson M et al (2022) Explaining US adolescent depressive symptom trends through declines in religious beliefs and service attendance. J Relig Health 61:300–326
Platt JM, Bates L, Jager J et al (2021) Is the US gender gap in depression changing over time? Meta Regres Am J Epidemiol 190:1190–1206
Keyes KM, Gary DS, Beardslee J et al (2017) Age, period, and cohort effects in conduct problems among American adolescents from 1991 through 2015. Am J Epidemiol. https://doi.org/10.1111/jcpp.13190
Askari MS, Rutherford CG, Mauro PM et al (2022) Structure and trends of externalizing and internalizing psychiatric symptoms and gender differences among adolescents in the US from 1991 to 2018. Soc Psychiatry Psychiatr Epidemiol 57:737–748
Odgers CL, Jensen MR (2020) Annual Research Review: Adolescent mental health in the digital age: facts, fears, and future directions. J Child Psychol Psychiatry Allied Discip. https://doi.org/10.1111/jcpp.13190
Twenge JM (2020) Why increases in adolescent depression may be linked to the technological environment. Curr Opin Psychol 32:89–94
Riehm KE, Feder KA, Tormohlen KN et al (2019) Associations between time spent using social media and internalizing and externalizing problems among US youth. JAMA Psychiat. https://doi.org/10.1001/jamapsychiatry.2019.2325
Odgers CL, Jensen MR (2022) Adolescent development and growing divides in the digital age. Dialog Clin Neurosci 22(2):143–149
Orben A (2020) Teenagers, screens and social media: a narrative review of reviews and key studies. Soc Psychiatry Psychiatr Epidemiol. https://doi.org/10.1007/s00127-019-01825-4
Santos RMS, Mendes CG, Sen Bressani GY et al (2023) The associations between screen time and mental health in adolescents: a systematic review. BMC Psychol 11:1–21
Nigg CR, Wunsch K, Nigg C et al (2021) Are physical activity, screen time, and mental health related during childhood, preadolescence, and adolescence? 11-year results from the German Motorik-Modul longitudinal study. Am J Epidemiol 190:220–229
Beyens I, Valkenburg PM, Piotrowski JT (2018) Screen media use and ADHD-related behaviors: four decades of research. Proc Natl Acad Sci 115:9875–9881
Ferguson CJ (2015) Do angry birds make for angry children? a meta-analysis of video game influences on children’s and adolescents’ aggression, mental health, prosocial behavior, and academic performance. Perspect Psychol Sci 10:646–666
Nikkelen SWC, Valkenburg PM, Huizinga M et al (2014) Media use and ADHD-related behaviors in children and adolescents: a meta-analysis. Dev Psychol 50:2228–2241
Valkenburg PM, Peter J (2013) The Differential susceptibility to media effects model. J Commun 63:221–243
Valkenburg PM, Peter J (2013) Communication research paradigms five challenges for the future of media-effects research. Int J Commun 7:197–215
Prescott AT, Sargent JD, Hull JG (2018) Metaanalysis of the relationship between violent video game play and physical aggression over time. Proc Natl Acad Sci U S A 115:9882–9888
Andreassen CS, Billieux J, Griffiths MD et al (2016) The relationship between addictive use of social media and video games and symptoms of psychiatric disorders: a large-scale cross-sectional study. Psychol Addict Behav 30:252–262
Morrison CM, Gore H (2010) The relationship between excessive internet use and depression: a questionnaire-based study of 1,319 young people and adults. Psychopathology 43:121–126
Augner C, Hacker GW (2011) Associations between problematic mobile phone use and psychological parameters in young adults. Int J Public Heal 572(57):437–441
Underwood MK, Ehrenreich SE (2017) The power and the pain of adolescents’ digital communication: cyber victimization and the perils of lurking. Am Psychol 72:144–158
Thoma VK, Schulz-Zhecheva Y, Oser C et al (2018) Media use, sleep quality, and adhd symptoms in a community sample and a sample of adhd patients aged 8 to 18 years. J Atten Disord 24:576–589
Lo CB, Waring ME, Pagoto SL et al (2015) A television in the bedroom is associated with higher weekday screen time among youth with attention deficit hyperactivity disorder (ADD/ADHD). Prev Med Reports 2:1–3
Pagani LS, Jalbert M, Derevensky JL (2022) From one year to the next: Video gaming life-style predicts subsequent psychosocial risk in adolescent boys and girls. J Paediatr Child Health. https://doi.org/10.1111/jpc.16032
Barch DM, Albaugh MD, Avenevoli S et al (2018) Demographic, physical and mental health assessments in the adolescent brain and cognitive development study: rationale and description. Dev Cogn Neurosci 32:55–66
Volkow ND, Koob GF, Croyle RT et al (2018) The conception of the ABCD study: from substance use to a broad NIH collaboration. Dev Cogn Neurosci 32:4–7
Compton WM, Dowling GJ, Garavan H (2021) Ensuring the best use of data the adolescent brain cognitive development study HHS public access. Pediatrics 173(9):809–810
Heeringa SG, Berglund PA (2020) A guide for population-based analysis of the adolescent brain cognitive development (abcd) study baseline Data. Bio 32(2):16
Sharif I, Wills TA, Sargent JD (2010) Effect of visual media use on school performance: a prospective study. J Adolesc Health 46:52
Paulich KN, Ross JM, Lessem JM et al (2021) Screen time and early adolescent mental health, academic, and social outcomes in 9-and 10-year old children: utilizing the adolescent brain cognitive developmentSM(ABCD) study. PLoS ONE 16:e0256591
Achenbach TM, Thomas M. 1999. The Child Behavior Checklist and related instruments. use Psychol Test Treat Plan. outcomes Assess., p. 429–66.
Achenbach TM, Dumenci L, Rescorla LA (2003) DSM-oriented and empirically based approaches to constructing scales from the same item pools. J Clin Child Adolesc Psychol 32:328–340
Ebesutani C, Bernstein A, Nakamura BJ et al (2010) Concurrent validity of the child behavior checklist dsm-oriented scales: correspondence with DSM diagnoses and comparison to syndrome scales. J Psychopathol Behav Assess 32:373–384
Achenbach TM (2001) Manual for ASEBA school-age forms & profiles. Univ Vermont, Res Cent Child Youth Fam
Achenbach TM, Edelbrock C (1991) Child behavior checklist. Burlingt 7:371–392
Yee TW (2010) The VGAM package for categorical data analysis. J Stat Softw 32:1–34
Keyes KM, Kreski N (2020) Is There an association between social media use and mental health? the timing of confounding measurement matters. JAMA Psychiat 77:437
Song H, Zmyslinski-Seelig A, Kim J et al (2014) Does facebook make you lonely?: a meta analysis. Comput Human Behav 36:446–452
Kowalski RM, Giumetti GW, Schroeder AN et al (2014) Bullying in the digital age: a critical review and meta-analysis of cyberbullying research among youth. Psychol Bull 140:1073–1137
Grist R, Porter J, Stallard P (2017) Mental health mobile apps for preadolescents and adolescents: a systematic review. J Med Internet Res. https://doi.org/10.2196/jmir.7332
Leech T, Dorstyn D, Taylor A et al (2021) Mental health apps for adolescents and young adults: a systematic review of randomised controlled trials. Child Youth Serv Rev 127:106073
Rolfe Winkler. 2022. Telehealth Startup Cerebral to Stop Prescribing Adderall for New Patients. Wall Str J.
Beyens I, Pouwels JL, van Driel II et al (2020) The effect of social media on well-being differs from adolescent to adolescent. Sci Rep 10:10763
De Los RA, Augenstein TM, Wang M et al (2015) The validity of the multi-informant approach to assessing child and adolescent mental health. Psychol Bull 141:858–900
Altman DG, Royston P (2006) The cost of dichotomising continuous variables. BMJ 332:1080
Funding
This work was funded by NIDA: R01-DA048853 (Keyes) and NIMH: T32-MH013043 (Finsaas).
Author information
Authors and Affiliations
Contributions
KMK was main contributor to manuscript text. MF, NK, and AH all contributed additional text. AH and NK handled analyses and visualizations.
Corresponding author
Ethics declarations
Conflict of interests
The authors have no relevant financial or non-financial interests to disclose.
Electronic supplementary material
Below is the link to the electronic supplementary material.
127_2024_2669_MOESM1_ESM.pdf
Supplementary file1 Baseline screen use predicting future mental health problems Models controlled for mental health problems, sex, age, race, and ethnicity, and family income at baseline (PDF 16 KB)
Appendix
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Keyes, K., Hamilton, A., Finsaas, M. et al. Childhood internalizing, externalizing and attention symptoms predict changes in social and nonsocial screen time. Soc Psychiatry Psychiatr Epidemiol (2024). https://doi.org/10.1007/s00127-024-02669-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00127-024-02669-3