Abstract
Right ventricular (RV) function is a critical determinant of the prognosis of patients with pulmonary hypertension (PH). Upon establishment of PH, RV dysfunction develops, leading to a gradual worsening of the condition over time, culminating in RV failure and premature mortality. Despite this understanding, the underlying mechanisms of RV failure remain obscure. As a result, there are currently no approved therapies specifically targeting the right ventricle. One contributing factor to the lack of RV-directed therapies is the complexity of the pathogenesis of RV failure as observed in animal models and clinical studies. In recent years, various research groups have begun utilizing multiple models, including both afterload-dependent and afterload-independent models, to investigate specific targets and pharmacological agents in RV failure. In this review, we examine various animal models of RV failure and the recent advancements made utilizing these models to study the mechanisms of RV failure and the potential efficacy of therapeutic interventions, with the ultimate goal of translating these findings into clinical practice to enhance the management of individuals with PH.
Zusammenfassung
Die Rechtsherzfunktion spielt eine entscheidende Rolle für die Symptomatik und Prognose von Patienten mit pulmonaler Hypertonie (PH). Im Laufe der Erkrankung führt eine progrediente Rechtsherzbelastung zu einer allmählichen Verschlechterung der rechtsventrikulären (RV-)Funktion, die im Rechtsherzversagen und im vorzeitigen Tod der Patienten gipfelt. Trotz dieses grundlegenden pathophysiologischen Verständnisses bleiben die ursächlichen Mechanismen des Rechtsherzversagens unklar. Daher gibt es derzeit keine zugelassenen Therapien für eine zielgerichtete Behandlung des rechten Ventrikels. Ein Faktor, der hierzu beiträgt, ist die Komplexität der Pathogenese des Rechtsherzversagens, die in tierexperimentellen und klinischen Studien beobachtet wurde. In den letzten Jahren haben daher verschiedene Forschungsgruppen begonnen, Tiermodelle zu verwenden, darunter sowohl nachlastabhängige als auch nachlastunabhängige Modelle, um spezifische therapeutisch angehbare Ziele und pharmakologische Wirkstoffe bei Rechtsherzversagen zu untersuchen. In der vorliegenden Übersichtsarbeit werden verschiedene Tiermodelle des Rechtsherzversagens und die aktuellen Fortschritte dargestellt, die unter Verwendung dieser Modelle erzielt wurden, um die Mechanismen des Rechtsherzversagens und die potenzielle Wirksamkeit therapeutischer Interventionen zu untersuchen. Das ultimative Ziel dabei ist es, diese Ergebnisse in die klinische Praxis zu übersetzen, um somit das Management und die Therapie von PH-Patienten zu verbessern.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Pulmonary hypertension (PH) is a clinical condition rather than an isolated disease of the cardiopulmonary circuit as its causes and symptoms are manifold. By definition, PH is characterized by an elevation of invasively measured mean pulmonary arterial pressure (mPAP) above 20 mm Hg at rest. Additional hemodynamic parameters, i.e., pulmonary arterial wedge pressure (PAWP) as well as pulmonary vascular resistance (PVR), are used to further discriminate between pre-capillary PH, isolated post-capillary PH, and combined post- and pre-capillary PH. The clinical classification into the five groups of PH is mostly based on clinical conditions of the patients but also on the pathological mechanisms: pulmonary arterial hypertension (group 1), PH associated with left heart disease (group 2), PH associated with lung diseases and/or hypoxia (group 3), PH associated with pulmonary artery (PA) obstructions (group 4), and unclear and/or multifactorial mechanisms (group 5). Here, all the underlying causes leading to the increase in mPAP are taken into account. But regardless of the underlying reason for the elevation in pressure and resistance in the pulmonary circulation, the common life-threatening event is right heart failure. Right heart failure commences at the end of disease progression starting from an initial stage of physiological adaptation due to a continuously increasing blood pressure in the cardiopulmonary system.
In both healthy and diseased conditions, the right ventricle has to overcome the right ventricular (RV) afterload to eject blood into the pulmonary circulation during systole. In PH, this function is compromised leading to increased RV wall tension, which will result in right heart failure if this remains hidden and thus untreated. Therefore, understanding and assessing the afterload faced by the right ventricle to eject blood into the PAs are vital. Afterload in its purest sense is defined as the wall stress that occurs during RV ejection. In 1892, Wood laid out an estimation to describe this wall tension in the heart, which is based on the LaPlace’s law [1, 2]. Here, the right ventricle was considered to be a spherical object, where the wall stress is proportional to the pressure during ejection multiplied by the radius of the wall divided by the wall thickness. This concept is widely accepted, although the sphere assumption of the right ventricle is not fully correct. Nevertheless, because the radius and the wall thickness are relatively constant, the main determinant of the afterload (i.e., wall stress) is the pressure during ejection. While pressure-dictating parameters such as mPAP and PVR can be obtained by right heart catheterization (RHC), several other components of the pulsatile loading are not reflected by this equation. Therefore, newer techniques are used to more accurately define RV function including adaptive mechanisms to increasing afterload as this is the crucial parameter.
In general, RV performance and integrity can be studied by different techniques mainly RHC, echocardiography, and cardiac magnetic resonance imaging (cMRI). Still, there have been limitations to the full investigation of ventricular function especially with regard to disease-driving processes that distinguish the adaptive state of compensation from the maladaptive phenotype characterized by decompensation. On the physiological level, a complex orchestra of contraction versus relaxation as well as ejection versus filling has to be coordinated. So-called pressure-volume (PV) analysis using conductance catheters is now used exactly for this purpose, which is the simultaneous assessment of pressure and volume to generate load-independent measures of systolic and diastolic heart chamber properties [3]. Moreover, it is able to capture the dynamic changes in these relationships throughout the cardiac cycle.
Under healthy conditions, the right heart is “coupled” to the pulmonary circulation as a cardiopulmonary unit, keeping a relative match between contractility and afterload pressure, which is also called “RV-to-PA coupling” (RV–PA coupling; [4, 5]). As PH develops, the pulmonary vascular system turns into a high-pressure, high-resistance, and low-compliance system. All these hemodynamic changes lead to an additional load on the contracting ventricle and can induce changes in the RV–PA coupling. In patients with early-stage PH, RV contractility is enhanced in order to cope with an increased afterload and RV–PA coupling is still preserved (homeometric adaptation; [5]). At later stages of severe PH with RV–PA uncoupling, the right ventricle enlarges and the heart rate increases in order to maintain stroke volume (heterometric adaptation; [5]). In its final stage, this is associated with high metabolic demands and reduced cardiac output ultimately leading to right heart failure-related death. The reader is referred to excellent articles addressing the details of RV function, its assessment, and its clinical relevance [6].
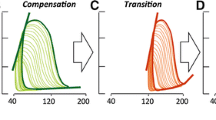
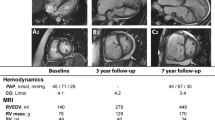
In-depth knowledge about the anatomical structures and dynamics of the right ventricle can now be combined with the understanding of cellular and molecular mechanisms. It is possible to study processes of both disease onset and progression including the (patho-) physiological adaptation and the functional deterioration of the right ventricle. Beside the different underlying causes for the increase in afterload in the PH groups, the function of the right ventricle remains the main determinant of survival [7]. Therefore, PH therapies should focus not only on the alterations in the pulmonary vasculature and RV afterload but also more on the diseased RV. For this purpose, experimental models are needed to mimic the clinical symptoms of PH and to establish new therapeutic treatment modalities. Since the technological advances—i.e., pressure–volume loops, cMRI, PA impedance analysis etc.—have been developed initially for applications in humans, vendors now also offer this equipment for use in animals even on the level of small species such as rodents. In this article, we provide recent insights into these experimental models of RV failure since the right ventricle is the key factor regarding disease symptoms and patient outcome (Fig. 1). Due to the complexity of the topic and the specific focus of this review, we excluded transgenic mouse models and large-animal models.
Animal models to study right ventricular failure in pulmonary hypertension. In pulmonary hypertension, initial physiological adaptive right ventricular remodeling turns into a maladaptive state with decompensation. This all precedes right heart insufficiency and right heart failure-related death. Several experimental models in rodents can mimic the various aspects of these processes to different extents, as highlighted in this scheme. MCT monocrotaline, PAB pulmonary artery banding. (Modified after [42])
Afterload-dependent small-animal models of RV failure
Animal models play a crucial role in studying disease progression and treatment impact on right heart function and afterload. Several afterload-dependent small-animal models of RV failure have been described, including monocrotaline (MCT)-induced PH in rats, as well as hypoxia-induced PH, and Sugen-hypoxia-induced PH in both rats and mice [8].
Monocrotaline model
The MCT model in rats involves a single subcutaneous injection of 60–80 mg/kg MCT, which induces PH with damage to lung endothelial cells and perivascular inflammation within hours to 1 week after administration [9, 10]. However, plexiform lesions comparable to pulmonary arterial hypertension (PAH) are not present [8]. In the second week after MCT injection, PVR rises due to the muscularization of the PAs, and in the third week, substantial PA remodeling results in the commencement of RV hypertrophy [11, 12]. Then, rapid progression of PH leads to maladaptive RV remodeling, RV failure, and finally to premature death. Alternatively, a lower dose of 20–40 mg/kg MCT can be used, which decreases the extent of PA remodeling and induces adaptive RV hypertrophy that spontaneously reverses after 4 weeks [13]. However, it has some disadvantages, including lung parenchyma involvement (i.e., fibrosis and hypoxemia) as well as toxicity of MCT itself [8]. The MCT model is widely available and mimics some (but not all) features of group 1 PH.
Chronic hypoxia model
Many species develop PH in response to chronic hypoxia. In rodents, exposure to 10% oxygen leads to an increase in RV systolic pressure (RVSP), PVR, and subsequently RV hypertrophy [14]. Histologically, media hypertrophy and adventitial fibrosis, muscularization of the PA, and perivascular inflammation are present [15, 16]. Again, plexiform lesions are not observed in this model. Thus, the chronic hypoxic PH model represents group 3 PH rather than PAH. However, the chronic hypoxia model has the advantage of a modest phenotype with adaptive RV remodeling and sustained RV function. It has the disadvantage of no RV failure or evidence of premature mortality due to PH.
Sugen hypoxia model
The Sugen hypoxia (SuHx) model attempts to increase the severity of PH induced by hypoxia with the administration of the VEGF receptor 2 antagonist, Sugen 5416 [17]. In rats, a single subcutaneous injection of 20 mg/kg Sugen followed by 3–4 weeks of 10% oxygen results in severe and progressive pulmonary vascular remodeling including plexiform lesions that are irreversible, even with a return to normoxia (in contrast to hypoxia only; [18, 19]). Both RV maladaptive remodeling and RV failure are evident in SuHx rats within 6 weeks. Premature death is present in a strain-dependent manner in rats [20].
By contrast, administration of three consecutive weekly doses of Sugen is required for the development of PH in mice, and RV dysfunction does not worsen to failure [21]. However, in mice, the PH and RV remodeling are also reversible upon a return to normoxia. Thus, mice do not show increased mortality rates.
One important consideration of all the hitherto described models is the afterload dependence of RV failure. In all three models, the severity of right heart failure is closely linked to the afterload imposed by PH. As a result, drugs that improve hemodynamics by pulmonary arterial vasodilation and/or reverse structural remodeling of the pulmonary vasculature can indirectly improve RV function. Therefore, the direct impact of drugs on RV function can hardly be examined in these models.
In conclusion, animal models are essential for the development of new therapeutic agents for PH. The MCT, chronic hypoxia, and SuHx models are widely used to study the pathogenesis of PH and evaluate novel therapeutic approaches. However, further models are needed to study afterload-independent effects of novel agents.
Small-animal models of RV failure with mechanically fixed afterload
In patients with PH, pressure overload is deemed as the predominant cause for RV hypertrophy and failure, irrespective of its underlying etiology. Nonetheless, other factors, such as neurohormonal activation, inflammation, metabolic alterations, and genetic predispositions, may contribute to the exacerbation of RV hypertrophic responses to pressure overload. Pulmonary artery banding (PAB) is a frequently employed model for investigating the changes independently associated with pressure overload-induced RV failure [22, 23]. The PAB model of RV failure has gained significant attention recently as a vital tool for investigating the mechanisms behind RV remodeling and assessing various treatment options that target the right ventricle [24]. To induce a fixed RV pressure overload, there are two possible methods: applying a metal clip onto the main PA or using a suture to ligate it. Either method is intended to reduce the main pulmonary cross-sectional area to approximately 65–70%. This fundamental characteristic of the PAB model has been utilized in diverse animals, ranging from small rodents such as mice and rats to larger species such as sheep, pigs, and lambs. Among these models, mice and rats are the most commonly used, given their distinct advantages over other animal models.
Animals subjected to PAB exhibit variable severity of RV remodeling, depending on the animal species selected, the genetic background, the sex, the duration of exposure, and the degree of PAB constriction [25,26,27]. In addition to myocardial hypertrophy, the PAB model is also characterized by myocardial fibrosis and inflammation, which eventually results in RV dilation and failure [28, 29]. Although the animal models described above, including MCT, SuHx, and hypoxia, cause structural changes both in the RV and pulmonary vasculature that are similar to those observed in patients with PH, pharmacological studies with these models do not provide any insight into whether the improvements in RV structure and function are caused by RV unloading or are the result of RV-directed effects [30]. In this context, the use of a PAB model presents a noteworthy advantage over the aforementioned models. This is due to the fact that a partial stenosis of the main PA induces a consistent increase in RV afterload, which is unrelated to changes in the pulmonary vasculature. This provides an opportunity to differentiate between afterload-dependent and afterload-independent RV-directed effects. This allows for a comprehensive and precise examination of the mechanisms behind RV hypertrophy and failure, irrespective of alterations in pulmonary hemodynamics and vascular remodeling. This makes the PAB model a valuable tool in the study of RV pathophysiology.
It is crucial to acknowledge that in the PAB model, the extent of long-term RV remodeling and the risk of RV failure are directly correlated with the initial severity of the PAB [27]. It is essential to preserve the uniformity of PAB ligation size to facilitate comparisons of RV remodeling responses across different animal groups. Rodent models of PAB can be particularly useful in assessing the potential cardiotoxic effects of drugs intended for treating various diseases, including PH, before advancing to clinical trials [31]. Moreover, some of the drugs with evidenced benefits for the RV in afterload-dependent models may still have RV-directed adverse effects. For instance, in isolated perfused rat hearts with RV hypertrophy, bosentan reduced RV contractility in dosage-dependent way. However, this effect was not observed in the heart with a healthy right ventricle [32].
Previous research has shown that PAB rats exhibit compensated RV remodeling and do not show signs of RV failure, in contrast to rats exposed to SuHx or MCT. As a result, the authors concluded that the PAB model does not fully replicate the development of RV failure observed in PH patients [33]. However, the phenotypes of RV observed in PAB models are causally linked to the degree of PAB constriction. As the PAB constriction becomes tighter, the RV remodeling becomes decompensated resulting in higher mortality rates [27]. Interestingly, a recent study has demonstrated that rats subjected to PAB surgery develop all of the hemodynamic and histological characteristics of RV failure in the same way as in the MCT and SuHx models [34].
Furthermore, PAB models can be used to identify and discover RV-specific biomarkers; for example, recent RV-specific biomarkers that have been identified in PAH patients, including hepatocyte growth factor and SPARC-like protein 1 [35, 36]. This proved that PAB model can serve as a valuable tool for translational research in RV failure.
The degree of structural and functional remodeling of the RV is dependent on the degree of constriction in the PA. For instance, rats with mild constriction can maintain their cardiac function despite RV hypertrophy [33]. On the other hand, increasing the severity of constriction results in RV functional decline, decreased RV pumping function, RV dilatation, and eventually RV failure [37, 38]. It is noteworthy that despite the severe changes in the RV, many features of RV failure can be reversible upon unloading. For instance, in a modified version of the PAB model that applies absorbable sutures to constrict the PA, there is an initial functional decline followed by functional and structural recovery once the PA band dissolves, and the afterload burden is relieved [39]. This model provides a useful tool for studying the processes involved in RV recovery from chronic pressure overload and subsequent unloading (comparable to patients with chronic thromboembolic PH undergoing surgery).
The PAB model can be a particularly useful tool in mouse models and in some cases in rat models in terms of identifying novel drug targets that are specific to RV failure. Specifically, the mouse PAB model can be employed to investigate the effects of gene-specific loss-of-function or gain-of-function mutations, which can be introduced broadly or selectively to particular cell types of interest in a controllable manner. This approach helps to uncover the spatial and temporal roles of the target gene in relation to RV hypertrophy and failure. Despite the many advantages of this model, one of the major disadvantages is that it immediately results in a fixed increase in resistance following surgery. This reflects, to some extent, an acute pulmonary embolism rather than a progressive gradual increase in resistance as a result of PH and the transition from RV adaptation to decompensation and failure. Since alternative models that more closely reflect the human situation are missing, the PAB model remains the gold standard model when addressing RV-directed treatment effects.
Collectively, the PAB model has the potential to assess a range of physiological changes such as hemodynamic, mechanical, neurohormonal, cellular, and molecular alterations that contribute to the development of RV remodeling. Furthermore, this model can be utilized to assess the efficacy of RV-targeted treatments. A more widespread application of the PAB model may lead to the development of therapies targeting RV failure in PAH and other cardiovascular diseases, ultimately improving the outcome of the disease.
Summary
Animal models are crucial in enhancing our comprehension of the causes, progression, and course of diverse diseases. They also aid in the identification of possible targets for the design and development of therapeutic interventions. An ideal animal model should replicate the disease processes with similar manifestations as observed in humans, while being cost-effective and easy to reproduce. However, emulating the severity, progression, histological findings, and treatment response in experimental models of PH poses significant challenges. The commonly used animal models for PH include MCT-induced PH, chronic hypoxia-induced PH, and SuHx-induced PH. These models have been useful in transferring various treatment strategies from the laboratory to the clinic, such as sildenafil or riociguat [40, 41]. In these models, the function of the RV is heavily reliant on RV afterload. Thus, an enhancement in RV function or a decrease in mortality rates cannot always be directly linked to an improvement in RV function, since PA vasodilation (and reverse remodeling) can also indirectly enhance RV function. As a result, afterload-independent models such as the PAB model are necessary. In this model, RV afterload remains fixed and cannot be modified since it is mechanically increased. Therefore, it is more probable that the improvement in RV function is directly related to the drug being tested. Nonetheless, the translational gap for all PH models is evident, and further animal model refinement is required to improve the efficiency of the bench-to-bedside process. Development and improvements of animal models and phenotyping methods (such as pressure–volume loop assessment in rodents) are ongoing so as to improve our understanding of RV failure and to establish better therapeutic strategies.
Change history
09 May 2023
An Erratum to this paper has been published: https://doi.org/10.1007/s00059-023-05190-6
References
Woods RH (1892) A few applications of a physical theorem to membranes in the human body in a state of tension. J Anat Physiol 26(3):362–370
Mirsky I (1969) Left ventricular stresses in the intact human heart. Biophys J 9(2):189–208
Sanz J, Sanchez-Quintana D, Bossone E et al (2019) Anatomy, function, and dysfunction of the right ventricle: JACC state-of-the-art review. J Am Coll Cardiol 73(12):1463–1482
Todaro MC, Carerj S, Zito C et al (2020) Echocardiographic evaluation of right ventricular-arterial coupling in pulmonary hypertension. Am J Cardiovasc Dis 10(4):272–283
Rako ZA, Kremer N, Yogeswaran A et al (2023) Adaptive versus maladaptive right ventricular remodelling. ESC Heart Fail 10(2):762–775
Tello K, Gall H, Richter M et al (2019) Right ventricular function in pulmonary (arterial) hypertension. Herz 44(6):509–516
Humbert M, Kovacs G, Hoeper MM et al (2022) 2022 ESC/ERS guidelines for the diagnosis and treatment of pulmonary hypertension. Eur Heart J 43(38):3618–3731. https://doi.org/10.1093/eurheartj/ehac237
Dignam JP, Scott TE, Kemp-Harper BK, Hobbs AJ (2022) Animal models of pulmonary hypertension:getting to the heart of the problem. Br J Pharmacol 179(5):811–837
Schultze AE, Wagner JG, White SM, Roth RA (1991) Early indications of monocrotaline pyrrole-induced lung injury in rats. Toxicol Appl Pharmacol 109(1):41–50
Gomez-Arroyo JG, Farkas L, Alhussaini AA et al (2012) The monocrotaline model of pulmonary hypertension in perspective. Am J Physiol Lung Cell Mol Physiol 302(4):L363–369
Rosenberg HC, Rabinovitch M (1988) Endothelial injury and vascular reactivity in monocrotaline pulmonary hypertension. Am J Physiol 255(6):H1484–1491
Urboniene D, Haber I, Fang YH et al (2010) Validation of high-resolution echocardiography and magnetic resonance imaging vs. high-fidelity catheterization in experimental pulmonary hypertension. Am J Physiol Lung Cell Mol Physiol 299(3):L401–412
Ruiter G, de Man FS, Schalij I et al (2013) Reversibility of the monocrotaline pulmonary hypertension rat model. Eur Respir J 42(2):553–556
West J, Hemnes A (2011) Experimental and transgenic models of pulmonary hypertension. Compr Physiol 1(2):769–782
Drexler ES, Bischoff JE, Slifka AJ et al (2008) Stiffening of the extrapulmonary arteries from rats in chronic hypoxic pulmonary hypertension. J Res Natl Inst Stand Technol 113(4):239–249
Meyrick B, Reid L (1980) Hypoxia-induced structural changes in the media and adventitia of the rat hilar pulmonary artery and their regression. Am J Pathol 100(1):151–178
Taraseviciene-Stewart L, Kasahara Y, Alger L et al (2001) Inhibition of the VEGF receptor 2 combined with chronic hypoxia causes cell death-dependent pulmonary endothelial cell proliferation and severe pulmonary hypertension. FASEB J 15(2):427–438
Bogaard HJ, Natarajan R, Mizuno S et al (2010) Adrenergic receptor blockade reverses right heart remodeling and dysfunction in pulmonary hypertensive rats. Am J Respir Crit Care Med 182(5):652–660
de Raaf MA, Schalij I, Gomez-Arroyo J et al (2014) SuHx rat model: partly reversible pulmonary hypertension and progressive intima obstruction. Eur Respir J 44(1):160–168
Suen CM, Chaudhary KR, Deng Y et al (2019) Fischer rats exhibit maladaptive structural and molecular right ventricular remodelling in severe pulmonary hypertension: a genetically prone model for right heart failure. Cardiovasc Res 115(4):788–799
Ciuclan L, Bonneau O, Hussey M et al (2011) A novel murine model of severe pulmonary arterial hypertension. Am J Respir Crit Care Med 184(10):1171–1182
Mamazhakypov A, Weiss A, Zukunft S et al (2020) Effects of macitentan and tadalafil monotherapy or their combination on the right ventricle and plasma metabolites in pulmonary hypertensive rats. Pulm circ 10(4):2045894020947283
Sydykov A, Luitel H, Mamazhakypov A et al (2020) Genetic deficiency and pharmacological stabilization of mast cells ameliorate pressure overload-induced maladaptive right ventricular remodeling in mice. Int J Mol Sci 21(23):9099
Mamazhakypov A, Sommer N, Assmus B et al (2021) Novel therapeutic targets for the treatment of right ventricular remodeling: insights from the pulmonary artery banding model. Int J Environ Res Public Health 18(16):8297
Müller M, Bischof C, Kapries T et al (2022) Right heart failure in mice upon pressure overload is promoted by mitochondrial oxidative stress. JACC Basic Transl Sci 7(7):658–677
Hemnes AR, Maynard KB, Champion HC et al (2012) Testosterone negatively regulates right ventricular load stress responses in mice. Pulm Circ 2(3):352–358
Andersen S, Schultz JG, Holmboe S et al (2018) A pulmonary trunk banding model of pressure overload induced right ventricular hypertrophy and failure. J Vis Exp. https://doi.org/10.3791/58050
Sydykov A, Mamazhakypov A, Petrovic A et al (2018) Inflammatory mediators drive adverse right ventricular remodeling and dysfunction and serve as potential biomarkers. Front Physiol 9:609
Egemnazarov B, Crnkovic S, Nagy BM et al (2018) Right ventricular fibrosis and dysfunction: actual concepts and common misconceptions. Matrix Biol 68–69:507–521
Lahm T, Douglas IS, Archer SL et al (2018) Assessment of right ventricular function in the research setting: knowledge gaps and pathways forward. An official American thoracic society research statement. Am J Respir Crit Care Med 198(4):e15–e43
Axelsen JB, Andersen S, Sun XQ et al (2019) Effects of 6‑mercaptopurine in pressure overload induced right heart failure. PLoS ONE 14(11):e225122
Nagendran J, Sutendra G, Paterson I et al (2013) Endothelin axis is upregulated in human and rat right ventricular hypertrophy. Circ Res 112(2):347–354
Bogaard HJ, Natarajan R, Henderson SC et al (2009) Chronic pulmonary artery pressure elevation is insufficient to explain right heart failure. Circulation 120(20):1951–1960
Akazawa Y, Okumura K, Ishii R et al (1985) Pulmonary artery banding is a relevant model to study the right ventricular remodeling and dysfunction that occurs in pulmonary arterial hypertension. J Appl Physiol 129(2):238–246
Amsallem M, Sweatt AJ, Arthur Ataam J et al (2021) Targeted proteomics of right heart adaptation to pulmonary arterial hypertension. Eur Respir J 57(4):2002428. https://doi.org/10.1183/13993003.02428-2020
Keranov S, Dorr O, Jafari L et al (2020) SPARCL1 as a biomarker of maladaptive right ventricular remodelling in pulmonary hypertension. Biomarkers 25(3):290–295
Piao L, Fang YH, Parikh K et al (2013) Cardiac glutaminolysis: a maladaptive cancer metabolism pathway in the right ventricle in pulmonary hypertension. J Mol Med 91(10):1185–1197
Borgdorff MA, Koop AM, Bloks VW et al (2015) Clinical symptoms of right ventricular failure in experimental chronic pressure load are associated with progressive diastolic dysfunction. J Mol Cell Cardiol 79:244–253
Boehm M, Tian XM et al (2020) Delineating the molecular and histological events that govern right ventricular recovery using a novel mouse model of pulmonary artery de-banding. Cardiovasc Res 116(10):1700–1709
Schermuly RT, Kreisselmeier KP, Ghofrani HA et al (2004) Chronic sildenafil treatment inhibits monocrotaline-induced pulmonary hypertension in rats. Am J Respir Crit Care Med 169(1):39–45
Lang M, Kojonazarov B, Tian X et al (2012) The soluble guanylate cyclase stimulator riociguat ameliorates pulmonary hypertension induced by hypoxia and SU5416 in rats. PLoS One 7(8):e43433
Boucherat O, Agrawal V, Lawrie A, Bonnet S (2022) The latest in animal models of pulmonary hypertension and right ventricular failure. Circ Res 130(9):1466–1486
Funding
Support: This work was supported by the Excellence Cluster Cardio-Pulmonary System (ECCPS) and the Collaborative Research Center (SFB) 1213—Pulmonary Hypertension and Cor Pulmonale, grant number SFB1213/1, projects A08 and B08 (German Research Foundation, Bonn, Germany).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
A. Weiß, A. Mamazhakypov and R.T. Schermuly declare that they have no competing interests. A. Yogeswaran reports personal fees from MSD outside the submitted work.
For this article no studies with human participants or animals were performed by any of the authors. All studies mentioned were in accordance with the ethical standards indicated in each case.
Additional information
The original online version of this article was revised: Due to an editing error, the authors appeared in the wrong order, correct is: Athiththan Yogeswaran, Argen Mamazhakypov, Ralph T. Schermuly, Astrid Weiß
Rights and permissions
About this article
Cite this article
Yogeswaran, A., Mamazhakypov, A., Schermuly, R.T. et al. Right ventricular failure in pulmonary hypertension: recent insights from experimental models. Herz 48, 285–290 (2023). https://doi.org/10.1007/s00059-023-05180-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00059-023-05180-8
Keywords
- Pulmonary arteries
- Heart ventricle
- Right heart
- Right ventricular afterload
- Pulmonary vascular resistance