Abstract
Purpose
To determine the plasma concentrations of propofol required to achieve different levels of sedation during monitored anesthesia care.
Methods
Sixty ASA 1-11, 18–65 yr-old patients, received a target-controlled continuousiv infusion of propofol. The target plasma concentration of propofol (Cpt) was initially set at 0.4 μ·g·ml−1. Two minutes after calculated equilibrium between plasma and effect-site concentrations, the Cpt of propofol was increased by 0.2 μg·ml−1 steps until the patient showed no reaction to squeezing the trapezius. The level of sedation was assessed immediately before each increase in propofol Cpt using the Observer’s Assessment of Alertness/Sedation (OAA/S) scale.
Results
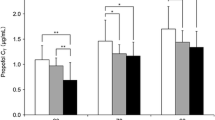
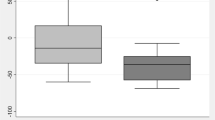
The Cpt of propofol required to induce lethargic response to name was 1.3 μg·ml−1 (5° and 95° percentiles: 1.0 – 1.8 μg·ml−1), to obtain response after loud and repeated calling name was 1.7 μg·ml−1 (1.2 – 2.2 μg·ml−1), to obtain response after prodding or shaking was 2.0 μg·ml−1(1.6 – 2.6 μg·ml−1), to obtain response after squeezing the trapezius was 2.4 μg·ml−1 (1.8 – 3.0 μg·ml−1). Patients showed no response after squeezing the trapezius at 2.8 μg·ml−1 (2.0 – 3.6 μg·ml−1). Correlation between Cpt propofol and sedation scores were r =0.76, P< 0.0001.
Conclusions
Target-controlled infusion of propofol provided easy and safe management of intraoperative sedation, allowing fast and predictable deepening in the level of sedation, while minimizing systemic side effects of intravenous sedation due to the minimal risk of overdosing the drug.
Résumé
Objectif
Déterminer les concentrations plasmatiques de propofol nécessaire pour fournir différents niveaux de sédation monitorés.
Méthode
Soixante patients ASA 1–11 de 18–65 ans ont reçu une perfusion continue de propofoliv à cible contrôlée. La concentration plasmatique ciblée de propofol (Cpc) était d’abord de 0,4 μg·ml−1. Deux minutes après avoir atteint l’équilibre entre la concentration plasmatique et celle du site d’effet, la Cpc de propofol a été augmenté par paliers de 0,2μg·ml−1 jusqu’à ce que le patient ne réagisse plus à une pression sur le trapèze. Le niveau de sédation a été évalué immédiatement avant chaque augmentation de la Cpc de propofol à l’aide de l’échelle de cotation de la vigilance par l’observateur/sédation (CVO/S).
Résultats
La Cpc de propofol nécessaire pour induire une réaction léthargique du patient à l’appel de son nom était de 1,3 μg·ml−1(5° et 95° percentiles: 1,0 – 1,8 μg · ml−1, pour obtenir une réaction après l’appel du nom répété et à voix forte était de 1,7 μg·ml−1 (1,2–2,2 μg·ml−1), pour réagir à une poussée ou une secousse, 2.0 μg·ml−1 (1.6 -2.6μg·ml−1), et pour réagir à une pression sur le trapèze, 2,4μg·ml−1 (1,8 – 3,0μg·ml−1). Les patients n’ont pas réagi à la pression sur le trapèze avec une concentration de 2,8 μg·ml−1 (2,0 – 3,6μg·ml−1). La corrélation entre la Cpc de propofol et les niveaux de sédation a été aussi observée, r = 0,76, P < 0,0001.
Conclusion
La perfusion de propofol à cible contrôlée fournit une ligne de conduite facile et sûre pour la sédation peropératoire, permettant l’approfondissement rapide et prévisible de la sédation tout en réduisant les effets secondaires généraux de la sédation intraveineuse causés par le risque minimal d’une surdose de médicament.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Sá Rêgo MM, Watcha MF, White PF. The changing role of monitored anesthesia care in the ambulatory setting. Anesth Analg 1997; 85: 1020–36.
White PF, Negus JB. Sedative infusions during local and regional anesthesia: a comparison of midazolam and propofol. J Clin Anesth 1991; 3: 32–9.
Veselis RA, Reinsel RA, Feshchenko VA, Wronski M. The comparative amnesic effects of midazolam, propofol, thiopental and fentanyl at equisedative concentrations. Anesthesiology 1997; 87: 749–64.
White M, Kenny GMC. Intravenous propofol anaesthesia using a computerised infusion system. Anaesthesia 1990; 45: 204–9.
Russell D, Wilkes MP, Hunter SC, Glen JB, Button P, Kenny GNC. Manual compared with target-controlled infusion of propofol. Br J Anaesth 1995; 75: 562–6.
Swinhoe CF, Peacock JE, Glen JB, Reilly CS. Evaluation of the predictive performance of ‘Diprifusor’ TCI system. Anaesthesia 1998; 53(Suppll): 61–7.
Fanelli G. Peripheral nerve block with electric neurostimulation. Minerva Anestesiol 1992; 58: 1025–6.
Fanelli G, Casati A, Beccaria, P, et al. A double-blind comparison of ropivacaine, bupivacaine and mepivacaine during sciatic and femoral nerve blockade. Anesth Analg 1998; 87: 597–600.
Gepts E, Camu F, Cockshott ID, Douglas EJ. Disposition of propofol administered as constant rate intravenous infusions in humans. Anesth Analg 1987; 66: 1256–63.
Marsh B, White M, Morton N, Kenny GNC. Pharmacokinetic model driven infusion of propofol in children. Br J Anaesth 1991; 67: 41–8.
Glen JB. The development of ‘Diprifusor’: a TCI system for propofol. Anaesthesia 1998; 58(Suppll): 13–21.
Glass PSA, Jacobs JR, Reves JG. Intravenous anesthetic delivery.In: Miller RD (Ed.). Anesthesia, 3rd ed. New York: Churchill Livingston, 1990: 367–88.
Chernik DA, Gillings D, Laine H, et al. Validity and reliability of the Observer’s Assessment of Alertness/Sedation scale: study with intravenous midazolam. J Clin Psycopharmacol 1990; 10: 244–51.
Oei-Lim VLB, White M, Kalkman CJ, Engbers FHM, Makkes PC, Ooms WG. Pharmacokinetics of propofol during conscious sedation using target-controlled infusion in axious patients undergoing dental treatment. Br J Anaesth 1998; 80: 324–31.
Oei-Lim VLB, Kalkman CJ, Makkes PC, Ooms WG. Patient-controlled versus anesthesiologist-controlled conscious sedation with propofol for dental treatment in anxious patients. Anesth Analg 1998; 86: 967–72.
Coetzee JF, Glen JB, Wium CA, Boshoff L. Pharmacokinetic model selection for target-controlled infusions of propofol. Assessment of three parameter sets. Anesthesiology 1995; 82: 1328–45.
Newson C, Josbi GP, Victory R, White PF. Comparison of propofol administration techniques for sedation during monitored anesthesia care. Anesth Analg 1995; 81: 486–91.
Servin FS. TCI compared with manually controlled infusion of propofol: a multicentre study. Anaesthesia 1998; 58(Suppll): 82–6.
Avramov MN, White PF. Methods for monitoring the level of sedation. Crit Care Clin 1995; 11: 803–26.
Johnson LC, Chernik DA. Sedative-hypnotics and human performance. Psychopharmacology 1982; 76: 101–13.
Struys M, Versichelen L, Roily G. Influence of pre-anaesthetic medication on target propofol concentration using a ‘diprifusor’ TCI system during ambulatory surgery. Anaesthesia 1998; 58(Suppll): 68–71.
Servin FS, Marchand-Maillet F, Desmonts JM. Influence of analgesic supplementation on the target propofol concentrations for anaesthesia with ‘Diprifusor’ TCI. Anaesthesia 1998; 58(Suppll): 72–6.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Casati, A., Fanelli, G., Casaletti, E. et al. Clinical assessment of target-controlled infusion of propofol during monitored anesthesia care. Can J Anesth 46, 235–239 (1999). https://doi.org/10.1007/BF03012602
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/BF03012602