Abstract
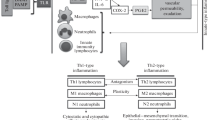
Inflammatory infiltration of tumor stroma is an integral reflection of reactions that develop in response to any damage to tumor cells including immune responses to antigens or necrosis caused by vascular disorders. In this review, we use the term “immune-inflammatory response” (IIR) that allows us to give an integral assessment of the cellular composition of the tumor microenvironment. Two main types of IIRs are discussed: type 1 and 2 T-helper reactions (Th1 and Th2), as well as their inducers: immunosuppressive responses and reactions mediated by Th22 and Th17 lymphocytes and capable of modifying the main types of IIRs. Cellular and molecular manifestations of each IIR type are analyzed and their general characteristics and roles in tissue regeneration and tumor growth are presented. Since inflammatory responses in a tumor can also be initiated by innate immunity mechanisms, special attention is given to inflammation based on them. We emphasize that processes accompanying tissue regeneration are prototypes of processes underlying cancer progression, and these processes have the same cellular and molecular substrates. We focus on evidence that tumor progression is mainly contributed by processes specific for the second phase of “wound healing” that are based on the Th2-type IIR. We emphasize that the effect of various types of immune and stroma cells on tumor progression is determined by the ability of the cells and their cytokines to promote or prevent the development of Th1- or Th2-type of IIR. Finally, we supposed that the nonspecific influence on the tumor caused by the cytokine context of the Th1- or Th2-type microenvironment should play a decisive role for suppression or stimulation of tumor growth and metastasis.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Abbreviations
- CCL:
-
C-C motif ligand
- CTL:
-
cytotoxic lymphocytes
- CXCL:
-
chemokine (C-X-C motif) ligand
- DAMP:
-
damage-associated molecular pattern
- DC:
-
dendritic cells
- EMT:
-
epithelial–mesenchymal transition
- GM-CSF:
-
granulocyte-macrophage colony-stimulating factor 2
- IFN:
-
interferon
- IIR:
-
immune-inflammatory response
- IL:
-
interleukin
- ILC:
-
innate lymphoid cells
- MDSC:
-
myeloid-derived suppressor cells
- NK:
-
natural killers
- NOS:
-
nitric oxide synthase
- PAMP:
-
pathogen-associated molecular pattern
- PGE2:
-
prostaglandin E2
- TAM:
-
tumor associated macrophages
- TCR:
-
T-cell receptor
- TGF-β:
-
transforming growth factor β
- Th:
-
T helper
- TLR:
-
Toll-like receptor
- Treg:
-
regulatory T cell
- VEGF:
-
vascular endothelial growth factor
References
Coussens, L. M., and Werb, Z. (2002) Inflammation and cancer, Nature, 420, 860–867.
Grivennikov, S. I., Greten, F. R., and Karin, M. (2010) Immunity, inflammation, and cancer, Cell, 140, 883–899.
Burgio, E., and Migliore, L. (2015) Towards a systemic paradigm in carcinogenesis: linking epigenetics and genetics, Mol. Biol. Rep., 42, 777–790.
Khansari, N., Shakiba, Y., and Mahmoudi, M. (2009) Chronic inflammation and oxidative stress as a major cause of agerelated diseases and cancer, Recent Pat. Inflamm. Allergy Drug Discov., 3, 73–80.
Khan, S., Jain, M., Mathur, V., and Feroz, S. M. (2016) Chronic inflammation and cancer: paradigm on tumor progression, metastasis and therapeutic intervention, Gulf J. Oncol., 1, 86–93.
Bondar, T., and Medzhitov, R. (2013) The origins of tumorpromoting inflammation, Cancer Cell, 24, 143–144.
Rakoff-Nahoum, S., and Medzhitov, R. (2008) Role of tolllike receptors in tissue repair and tumorigenesis, Biochemistry (Moscow), 73, 555–561.
Dvorak, H. F. (1986) Tumors: wounds that do not heal. Similarities between tumor stroma generation and wound healing, N. Engl. J. Med., 315, 1650–1659.
Eming, S. A., Krieg, T., and Davidson, J. M. (2007) Inflammation in wound repair: molecular and cellular mechanisms, J. Invest. Dermatol., 127, 514–525.
Blanpain, C., and Fuchs, E. (2014) Stem cell plasticity. Plasticity of epithelial stem cells in tissue regeneration, Science, 344, 1242281.
Arnold, K. M., Opdenaker, L. M., Flynn, D., and Sims-Mourtada, J. (2015) Wound healing and cancer stem cells: inflammation as a driver of treatment resistance in breast cancer, Cancer Growth Metast., 8, 1–13.
Arbach, H., Viglasky, V., Lefeu, F., Guinebretiere, J.-M., Ramirez, V., Bride, N., Boualaga, N., Bauchet, T., Peyrat, J.-P., Mathieu, M.-C., Mourah, S., Podgorniak, M.-P., Seignerin, J.-M., Takada, K., and Joab, I. (2006) Epstein–Barr virus (EBV) genome and expression in breast cancer tissue: effect of EBV infection of breast cancer cells on resistance to paclitaxel (Taxol), J. Virol., 80, 845–853.
Li, Y. Y., Ge, Q. X., Cao, J., Zhou, Y. J., Du, Y. L., Shen, B., Wan, Y. J., and Nie, Y. Q. (2016) Association of Fusobacterium nucleatum infection with colorectal cancer in Chinese patients, World J. Gastroenterol., 22, 3227–3233.
Zhang, Q., Jia, Q., Deng, T., Song, B., and Li, L. (2015) Heterogeneous expansion of CD4+ tumorinfiltrating T-lymphocytes in clear cell renal cell carcinomas, Biochem. Biophys. Res. Commun., 458, 70–76.
Dieu-Nosjean, M. C., Goc, J., Giraldo, N. A., Sautes-Fridman, C., and Fridman, W. H. (2014) Tertiary lymphoid structures in cancer and beyond, Trends Immunol., 35, 571–580.
Brucklacher-Waldert, V., Carr, E. J., Linterman, M. A., and Veldhoen, M. (2014) Cellular plasticity of CD4+ T cells in the intestine, Front. Immunol., 5, 488–499.
Caza, T., and Landas, S. (2015) Functional and phenotypic plasticity of CD4+ T cell subsets, Biomed Res. Int., 521957.
Werb, Z., and Lu, P. (2015) The role of stroma in tumor development, Cancer J., 21, 250–253.
Portou, M. J., Baker, D., Abraham, D., and Tsui, J. (2015) The innate immune system, Tolllike receptors and dermal wound healing: a review, Vascul. Pharmacol., 71, 31–36.
Moore, K. W., De Waal Malefyt, R., Coffman, R. L., and O’Garra, A. (2001) Interleukin-10 and the interleukin-10 receptor, Annu. Rev. Immunol., 19, 683–765.
Sionov, R. V., Fridlender, Z. G., and Granot, Z. (2015) The multifaceted roles neutrophils play in the tumor microenvironment, Cancer Microenviron., 8, 125–158.
Artis, D., and Spits, H. (2015) The biology of innate lymphoid cells, Nature, 517, 293–301.
Bernink, J. H., Peters, C. P., Munneke, M., te Velde, A. A., Meijer, S. L., Weijer, K., Hreggvidsdottir, H. S., Heinsbroek, S. E., Legrand, N., Buskens, C. J., Bemelman, W. A., Mjosberg, J. M., and Spits, H. (2013) Human type 1 innate lymphoid cells accumulate in inflamed mucosal tissues, Nat. Immunol., 14, 221–229.
Neill, D. R., Wong, S. H., Bellosi, A., Flynn, R. J., Daly, M., Langford, T. K., Bucks, C., Kane, C. M., Fallon, P. G., Pannell, R., Jolin, H. E., and McKenzie, A. N. (2010) Nuocytes represent a new innate effector leukocyte that mediates type-2 immunity, Nature, 464, 1367–1370.
Buonocore, S., Ahern, P. P., Uhlig, H. H., Ivanov, I. I., Littman, D. R., Maloy, K. J., and Powrie, F. (2010) Innate lymphoid cells drive interleukin-23-dependent innate intestinal pathology, Nature, 464, 1371–1375.
Vremec, D., and Shortman, K. (2015) What’s in a name? Some early and current issues in dendritic cell nomenclature, Front. Immunol., 6, 267.
Nizzoli, G., Krietsch, J., Weick, A., Steinfelder, S., Facciotti, F., Gruarin, P., Bianco, A., Steckel, B., Moro, M., Crosti, M., Romagnani, C., Stolzel, K., Torretta, S., Pignataro, L., Scheibenbogen, C., Neddermann, P., De Francesco, R., Abrignani, S., and Geginat, J. (2013) Human CD1c+ dendritic cells secrete high levels of IL-12 and potently prime cytotoxic T-cell responses, Blood, 122, 932–942.
Hemont, C., Neel, A., Heslan, M., Braudeau, C., and Josien, R. (2013) Human blood mDC subsets exhibit distinct TLR repertoire and responsiveness, J. Leukoc. Biol., 93, 599–609.
Suga, H., Sugaya, M., Fujita, H., Asano, Y., Tada, Y., Kadono, T., and Sato, S. (2014) TLR4, rather than TLR2, regulates wound healing through TGF-β and CCL5 expression, J. Dermatol. Sci., 73, 117–124.
Spits, H., and Di Santo, J. P. (2011) The expanding family of innate lymphoid cells: regulators and effectors of immunity and tissue remodeling, Nat. Immunol., 12, 21–27.
Gonzalez-Reyes, S., Marin, L., Gonzalez, L., Gonzalez, L. O., del Casar, J. M., Lamelas, M. L., Gonzalez-Quintana, J. M., and Vizoso, F. J. (2010) Study of TLR3, TLR4 and TLR9 in breast carcinomas and their association with metastasis, BMC Cancer, 10, 665.
Voelcker, V., Gebhardt, C., Averbeck, M., Saalbach, A., Wolf, V., Weih, F., Sleeman, J., Anderegg, U., and Simon, J. (2008) Hyaluronan fragments induce cytokine and metalloprotease upregulation in human melanoma cells in part by signaling via TLR4, Exp. Dermatol., 17, 100–107.
Liao, S. J., Zhou, Y. H., Yuan, Y., Li D., Wu, F. H., Wang, Q., Zhu, J. H., Yan, B., Wei, J. J., Zhang, G. M., and Feng Z. H. (2012) Triggering of Tolllike receptor 4 on metastatic breast cancer cells promotes ανβ3-mediated adhesion and invasive migration, Breast Cancer Res. Treat., 133, 853–863.
Jing, Y. Y., Han, Z. P., Sun, K., Zhang, S. S., Hou, J., Liu, Y., Li, R., Gao, L., Zhao, X., Zhao, Q. D., Wu, M. C., and Wei, L. X. (2012) Tolllike receptor 4 signaling promotes epithelialmesenchymal transition in human hepatocellular carcinoma induced by lipopolysaccharide, BMC Med., 10, 98.
Liu, C. Y., Xu, J. Y., Shi, X. Y., Huang, W., Ruan, T. Y., Xie, P., and Ding, J. L. (2013) M2-polarized tumorassociated macrophages promoted epithelialmesenchymal transition in pancreatic cancer cells, partially through TLR4/IL-10 signaling pathway, Lab. Invest., 93, 844–854.
Elinav, E., Nowarski, R., Thaiss, C. A., Hu, B., Jin, C., and Flavell, R. A. (2013) Inflammationinduced cancer: crosstalk between tumors, immune cells and microorganisms, Nat. Rev. Cancer, 13, 759–771.
Gajewski, F., Schreiber, H., and Fu, Y.-X. (2013) Innate and adaptive immune cells in the tumor microenvironment, Nat. Immunol., 14, 1014–1022.
Balkwill, F. R., Capasso, M., and Hagemann, T. (2012) The tumor microenvironment at a glance, J. Cell Sci., 125, 5591–5596.
Shields, J. D., Kourtis, I. C., Tomei, A. A., Roberts, J. M., and Swartz, M. A. (2010) Induction of lymphoidlike stroma and immune escape by tumors that express the chemokine CCL21, Science, 328, 749–752.
Eisenring, M., vom Berg, J., Kristiansen, G., Saller, E., and Becher, B. (2010) IL-12 initiates tumor rejection via lymphoid tissueinducer cells bearing the natural cytotoxicity receptor NKp46, Nat. Immunol., 11, 1030–1038.
Braumuller, H., Wieder, T., Brenner, E., Abmann, S., Hahn, M., Alkhaled, M., Schilbach, K., Essmann, F., Kneilling, M., Griessinger, C., Ranta, F., Ullrich, S., Mocikat, R., Braungart, K., Mehra, T., Fehrenbacher, B., Berdel, J., Niessner, H., Meier, F., van den Broek, M., Haring, H. U., Handgretinger, R., Quintanilla-Martinez, L., Fend, F., Pesic, M., Bauer, J., Zender, L., Schaller, M., Schulze-Osthoff, K., and Rocken, M. (2013) T-helper-1-cell cytokines drive cancer into senescence, Nature, 494, 361–365.
Tachibana, T., Onodera, H., Tsuruyama, T., Mori, A., Nagayama, S., Hiai, H., and Imamura, M. (2005) Increased intratumor Valpha24-positive natural killer T cells: a prognostic factor for primary colorectal carcinomas, Clin. Cancer Res., 11, 7322–7327.
Fridman, W. H., Pages, F., Sautes-Fridman, C., and Galon, J. (2012) The immune contexture in human tumors: impact on clinical outcome, Nat. Rev. Cancer, 12, 298–306.
Jia, L, and Wu, C. (2014) The biology and functions of Th22 cells, Adv. Exp. Med. Biol., 841, 209–230.
Fujita, H., Nograles, K. E., Kikuchi, T., Gonzalez, J., Carucci, J. A., and Krueger, J. G. (2009) Human Langerhans cells induce distinct IL-22-producing CD4+ T cells lacking IL-17 production, Proc. Natl. Acad. Sci. USA, 106, 21795–21800.
Simonian, P. L., Wehrmann, F., Roark, C. L., Born, W. K., O’Brien, R. L., and Fontenot, A. P. (2010) γδ T cells protect against lung fibrosis via IL-22, J. Exp. Med., 207, 2239–2253.
Wolk, K., Kunz, S., Asadullah, K., and Sabat, R. (2002) Cutting edge: immune cells as sources and targets of the IL-10 family members? J. Immunol., 168, 5397–5402.
Sabat, R., Witte, E., Witte, K., and Wolk, K. (2013) in IL-17, IL-22 and Their Producing Cells: Role in Inflammation and Autoimmunity, Springer, Basel, pp. 3–131.
Wolk, K., Witte, E., Witte, K., Warszawska, K., and Sabat, R. (2010) Biology of interleukin-22, Semin. Immunopathol., 32, 17–31.
Eyerich, S., Eyerich, K., Pennino, D., Carbone, T., Nasorri, F., Pallotta, S., Cianfarani, F., Odorisio, T., Traidl-Hoffmann, C., Behrendt, H., Durham, S. R., Schmidt-Weber, C. B., and Cavani, A. (2009) Th22 cells represent a distinct human T cell subset involved in epidermal immunity and remodeling, J. Clin. Invest., 119, 3573–3585.
McGee, H. M., Schmidt, B. A., Booth, C. J., Yancopoulos, G. D., Valenzuela, D. M., Murphy, A. J., Stevens, S., Flavell, R. A., and Horsley, V. (2013) IL-22 promotes fibroblastmediated wound repair in the skin, J. Invest. Dermatol., 133, 1321–1329.
Reuss, B., Dono, R., and Unsicker, K. (2003) Functions of fibroblast growth factor (FGF)-2 and FGF-5 in astroglial differentiation and bloodbrain barrier permeability: evidence from mouse mutants, J. Neurosci., 23, 6404–6412.
Varga, J., and Abraham, D. (2007) Systemic sclerosis: a prototypic multisystem fibrotic disorder, J. Clin. Invest., 117, 557–567.
Hwang, J., Son, K. N., Kim, C. W., Ko, J., Na, D. S., Kwon, B. S., Gho, Y. S., and Kim, J. (2005) Human CC chemokine CCL23, a ligand for CCR1, induces endothelial cell migration and promotes angiogenesis, Cytokine, 30, 254–263.
Kirchberger, S., Royston, D. J., Boulard, O., Thornton, E., Franchini, F., Szabady, R. L., Harrison, O., and Powrie, F. (2013) Innate lymphoid cells sustain colon cancer through production of interleukin-22 in a mouse model, J. Exp. Med., 210, 917–931.
Takahashi, H., Numasaki, M., Lotze, M. T., and Sasaki, H. (2005) Interleukin-17 enhances bFGF, HGF-and VEGF-induced growth of vascular endothelial cells, Immunol. Lett., 98, 189–193.
Numasaki, M., Fukushi, J., Ono, M., Narula, S. K., Zavodny, P. J., Kudo, T., Robbins, P. D., Tahara, H., and Lotze, M. T. (2003) Interleukin-17 promotes angiogenesis and tumor growth, Blood, 101, 2620–2627.
Liao, Y., Wang, B., Huang, Z. L., Shi, M., Yu, X. J., Zheng, L., Li, S., and Li, L. (2013) Increased circulating Th17 cells after transarterial chemoembolization correlate with improved survival in stage III hepatocellular carcinoma: a prospective study, PLoS One, 8, e60444.
Zhu, J., and Paul, W. E. (2008) CD4 T cells: fates, functions, and faults, Blood, 112, 1557.
Zhang, Y., Zhang, Y., Gu, W., He, L., and Sun, B. (2014) Th1/Th2 cell’s function in immune system, Adv. Exp. Med. Biol., 841, 45.
Sica, A., and Mantovani, A. (2012) Macrophage plasticity and polarization: in vivo veritas, J. Clin. Invest., 122, 787–795.
Martinez, F. O., and Gordon, S. (2014) The M1 and M2 paradigm of macrophage activation: time for reassessment, F1000Prime Rep., 6, 13.
Scapini, P., Lapinet-Vera, J. A., Gasperini, S., Calzetti, F., Bazzoni, F., and Cassatella, M. A. (2000) The neutrophil as a cellular source of chemokines, Immunol. Rev., 177, 195–203.
Fridlender, Z. G., Sun, J., Kim, S., Kapoor, V., Cheng, G., Ling, L., Worthen, G. S., and Albelda, S. M. (2009) Polarization of tumorassociated neutrophil phenotype by TGF-beta: “N1” versus “N2” TAN, Cancer Cell, 16, 183–194.
Sindrilaru, A., Peters, T., Wieschalka, S., Baican, C., Baican, A., Peter, H., Hainzl, A., Schatz, S., Qi, Y., Schlecht, A., Weiss, J. M., Wlaschek, M., Sunderkotter, C., and Scharffetter-Kochanek, K. (2011) An unrestrained proinflammatory M1 macrophage population induced by iron impairs wound healing in humans and mice, J. Clin. Invest., 121, 985–997.
Barrientos, S., Stojadinovic, O., Golinko, M. S., Brem, H., and Tomic-Canic, M. (2008) Growth factors and cytokines in wound healing, Wound Rep. Regen., 16, 585–601.
Wieder, T., Braumuller, H., Kneilling, M., Pichler, B., and Rocken, M. (2008) T cellmediated help against tumors, Cell Cycle, 7, 2974–2977.
Hensbergen, P. J., Wijnands, P. G. B., Schreurs, M. W., Scheper, R. J., Willemze, R., and Tensen, C. P. (2005) The CXCR3 targeting chemokine CXCL11 has potent antitumor activity in vivo involving attraction of CD8+ T lymphocytes but not inhibition of angiogenesis, J. Immunother., 28, 343–351.
Morishima, N., Owaki, T., Asakawa, M., Kamiya, S., Mizuguchi, J., and Yoshimoto, T. (2005) Augmentation of effector CD8+ T cell generation with enhanced granzyme B expression by IL-27, J. Immunol., 175, 1686–1693.
Shen, M., Hu, P., Donskov, F., Wang, G., Liu, Q., and Du, J. (2014) Tumorassociated neutrophils as a new prognostic factor in cancer: a systematic review and metaanalysis, PLoS One, 9, e98259.
Muranski, P., Boni, A., Antony, P. A., Cassard, L., Irvine, K. R., Kaiser, A., Paulos, C. M., Palmer, D. C., Touloukian, C. E., Ptak, K., Gattinoni, L., Wrzesinski, C., Hinrichs, C. S., Kerstann, K. W., Feigenbaum, L., Chan, C. C., and Restifo, N. P. (2008) Tumorspecific Th17-polarized cells eradicate large established melanoma, Blood, 112, 362–373.
Roberts, S. J., Ng, B. Y., Filler, R. B., Lewis, J., Glusac, E. J., Hayday, A. C., Tigelaar, R. E., and Girardi, M. (2007) Characterizing tumorpromoting T cells in chemically induced cutaneous carcinogenesis, Proc. Natl. Acad. Sci. USA, 104, 6770–6775.
Duffield, J. S., Lupher, M., Thannickal, V. J., and Wynn, T. A. (2013) Host responses in tissue repair and fibrosis, Annu. Rev. Pathol., 8, 241–276.
Kuang, D. M., Zhao, Q., Peng, C., Xu, J., Zhang, J. P., Wu, C., and Zheng, L. (2009) Activated monocytes in peritumoral stroma of hepatocellular carcinoma foster immune privilege and disease progression through PD-L1, J. Exp. Med., 206, 1327–1337.
Eming, S. A., Martin, P., and Tomic-Canic, M. (2014) Wound repair and regeneration: mechanisms, signaling, and translation, Sci. Transl. Med., 6, 265.
Ferrante, C. J., and Leibovich, S. J. (2012) Regulation of macrophage polarization and wound healing, Adv. Wound Care (New Rochelle), 1, 10–16.
Dong, H. P., Elstrand, M. B., Holth, A., Silins, I., Berner, A., Trope, C. G., Davidson, B., and Risberg, B. (2006) NK-and B-cell infiltration correlates with worse outcome in metastatic ovarian carcinoma, Am. J. Clin. Pathol., 125, 451–458.
Olkhanud, P. B., Damdinsuren, B., Bodogai, M., Gress, R. E., Sen, R., Wejksza, K., Malchinkhuu, E., Wersto, R. P., and Biragyn, A. (2011) Tumorevoked regulatory B cells promote breast cancer metastasis by converting resting CD4+ T cells to T-regulatory cells, Cancer Res., 71, 3505–3515.
Barbera-Guillem, E., Nelson M. B., Barr, B., Nyhus, J. K., May, K. F., Jr., Feng, L., and Sampsel, J. W. (2000) B lymphocyte pathology in human colorectal cancer. Experimental and clinical therapeutic effects of partial B cell depletion, Cancer Immunol. Immunother., 48, 541–549.
Nielsen, J. S., Sahota, R. A., Milne, K., Kost, S. E., Nesslinger, N. J., Watson, P. H., and Nelson, B. H. (2012) CD20+ tumorinfiltrating lymphocytes have an atypical CD27– memory phenotype and together with CD8+ T cells promote favorable prognosis in ovarian cancer, Clin. Cancer Res., 18, 3281–3292.
Van Herpen, C. M., Van der Voort, R., Van der Laak, J. A., Klasen, I. S., De Graaf, A. O., Van Kempen, L. C., De Vries, I. J., Boer, T. D., Dolstra, H., and Torensma, R. (2008) Intratumoral rhIL-12 administration in head and neck squamous cell carcinoma patients induces B cell activation, Int. J. Cancer, 123, 2354–2361.
Germain, C., Gnjatic, S., Tamzalit, F., Knockaert, S., Remark, R., Goc, J., Lepelley, A., Becht, E., Katsahian, S., and Bizouard, G. (2014) Presence of B cells in tertiary lymphoid structures is associated with a protective immunity in patients with lung cancer, Am. J. Respir. Crit. Care Med., 189, 832–844.
Germain, C., Gnjatic, S., and Dieu-Nosjean, M.-C. (2015) Tertiary lymphoid structureassociated B cells are key players in antitumor immunity, Front. Immunol., 6, 67.
Murdoch, C., Giannoudis, A., and Lewis, C. E. (2004) Mechanisms regulating the recruitment of macrophages into hypoxic areas of tumors and other ischemic tissues, Blood, 104, 2224–2234.
Mantovani, A., Sica, A., Sozzani, S., Allavena, P., Vecchi, A., and Locati, M. (2004) The chemokine system in diverse forms of macrophage activation and polarization, Trends Immunol., 25, 677–686.
Gregory, A. D., and Houghton, A. M. (2011) Tumorassociated neutrophils: new targets for cancer therapy, Cancer Res., 71, 2411–2416.
Liao, D., Luo, Y., Markowitz, D., Xiang, R., and Reisfeld, R. A. (2009) Cancer associated fibroblasts promote tumor growth and metastasis by modulating the tumor immune microenvironment in a 4T1 murine breast cancer model, PLoS One, 4, e7965.
Atanasov, G., Hau, H. M., Dietel, C., Benzing, C., Krenzien, F., Brandl, A., Wiltberger, G., Matia, I., Prager, I., Schierle, K., Robson, S. C., Reutzel-Selke, A., Pratschke, J., Schmelzle, M., and Jonas, S. (2015) Prognostic significance of macrophage invasion in hilar cholangiocarcinoma, BMC Cancer, 15, 790.
Beyer, M., and Schultze, J. L. (2006) Regulatory T cells in cancer, Blood, 108, 804–811.
Bilate, A. M., and Lafaille, J. J. (2012) Induced CD4+Foxp3+ regulatory T cells in immune tolerance, Annu. Rev. Immunol., 30, 733–758.
Thornton, A. M., and Shevach, E. M. (1998) CD4+CD25+ immunoregulatory T cells suppress polyclonal T cell activation in vitro by inhibiting interleukin 2 production, J. Exp. Med., 188, 287–296.
Crome, S. Q., Clive, B., Wang, A. Y., Kang, C. Y., Chow, V., Yu, J., Lai, A., Ghahary, A., Broady, R., and Levings, M. K. (2010) Inflammatory effects of ex vivo human Th17 cells are suppressed by regulatory T cells, J. Immunol., 185, 3199–3208.
Murphy, T. J., Choileain, N. Ni., Zang, Y., Mannick, J. A., and Lederer, J. A. (2005) CD4+CD25+ regulatory T cells control innate immune reactivity after injury, J. Immunol., 174, 2957–2963.
Mailloux, A. W., and Young, M. R. (2010) Regulatory T-cell trafficking: from thymic development to tumorinduced immune suppression, Crit. Rev. Immunol., 30, 435–447.
Sfondrini, L., Rossini, A., Besusso, D., Merlo, A., Tagliabue, E., Menard, S., and Balsari, A. (2006) Antitumor activity of the TLR-5 ligand flagellin in mouse models of cancer, J. Immunol., 176, 6624–6630.
Huang, Y., Wang, F. M., Wang, T., Wang, Y. J., Zhu, Z. Y., Gao, Y. T., and Du, Z. (2012) Tumorinfiltrating FoxP3+ Tregs and CD8+ T cells affect the prognosis of hepatocellular carcinoma patients, Digestion, 86, 329–337.
Leong, P. P., Mohammad, R., Ibrahim, N., Ithnin, H., Abdullah, M., Davis, W. C., and Seow, H. F. (2006) Phenotyping of lymphocytes expressing regulatory and effector markers in infiltrating ductal carcinoma of the breast, Immunol. Lett., 102, 229–236.
Lin, Y. C., Mahalingam, J., Chiang, J. M., Su, P. J., Chu, Y. Y., Lai, H. Y., Fang, J. H., Huang, C. T., Chiu, C. T., and Lin, C. Y. (2013) Activated but not resting regulatory T cells accumulated in tumor microenvironment and correlated with tumor progression in patients with colorectal cancer, Int. J. Cancer, 132, 1341–1350.
Hoechst, B., Voigtlaender, T., Ormandy, L., Gamrekelashvili, J., Zhao, F., Wedemeyer, H., Lehner, F., Manns, M. P., Greten, T. F., and Korangy, F. (2009) Myeloid derived suppressor cells inhibit natural killer cells in patients with hepatocellular carcinoma via the NKp30 receptor, Hepatology, 50, 799–807.
Motz, G. T., and Coukos, G. (2011) The parallel lives of angiogenesis and immunosuppression: cancer and other tales, Nat. Rev. Immunol., 11, 702–711.
Willenborg, S., Lucas, T., van Loo, G., Knipper, J. A., Krieg, T., Haase, I., Brachvogel, B., Hammerschmidt, M., Nagy, A., Ferrara, N., Pasparakis, M., and Eming, S. A. (2012) CCR2 recruits an inflammatory macrophage subpopulation critical for angiogenesis in tissue repair, Blood, 120, 613–625.
Huang, B., Pan, P. Y., Li, Q., Sato, A. I., Levy, D. E., Bromberg, J., Divino, C. M., and Chen, S. H. (2006) Gr-1+CD115+ immature myeloid suppressor cells mediate the development of tumorinduced T regulatory cells and T-cell energy in tumorbearing host, Cancer Res., 66, 1123–1131.
Yang, L., and Moses, H. L. (2008) Transforming growth factor beta: tumor suppressor or promoter? Are host immune cells the answer? Cancer Res., 68, 9107–9111.
Bronte, V., Serafini, P., Mazzoni, A., Segal, D. M., and Zanovello, P. (2003) L-arginine metabolism in myeloid cells controls T-lymphocyte functions, Trends Immunol., 24, 301–305.
Hurwitz, A. A., and Watkins, S. K. (2012) Immune suppression in the tumor microenvironment: a role for dendritic cellmediated tolerization of T cells, Cancer Immunol. Immunother., 61, 289–93.
Van Beek, J. J., Gorris, M. A., Skold, A. E., Hatipoglu, I., Van Acker, H. H., Smits, E. L., De Vries, I. J., and Bakdash, G. (2016) Human blood myeloid and plasmacytoid dendritic cells cross activate each other and synergize in inducing NK cell cytotoxicity, Oncoimmunology, 5, e1227902.
Miossec, P., and Kolls, J. K. (2012) Targeting IL-17 and TH17 cells in chronic inflammation, Nat. Rev. Drug Discov., 11, 763–776.
Nyirenda, M. H., Sanvito, L., Darlington, P. J., O’Brien, K., Zhang, G. X., Constantinescu, C. S., Bar-Or, A., and Gran, B. (2011) TLR2 stimulation drives human naive and effector regulatory T cells into a Th17-like phenotype with reduced suppressive function, J. Immunol., 187, 2278–2290.
Veldhoen, M., Hocking, R. J., Atkins, C. J., Locksley, R. M., and Stockinger, B. (2006) TGFbeta in the context of an inflammatory cytokine milieu supports de novo differentiation of IL-17-producing T cells, Immunity, 24, 179–189.
Miljkovic, D., Cvetkovic, I., Vuckovic, O., Stosic-Grujicic, S., Mostarica Stojkovic, M., and Trajkovic, V. (2003) The role of interleukin-17 in inducible nitric oxide synthasemediated nitric oxide production in endothelial cells, Cell Mol. Life Sci., 60, 518–525.
Paris, I., Charreau, S., Guignouard, E., Garnier, M., Favot-Laforge, L., Huguier, V., Bernard, F.-X., Morel, F., and Lecron, J.-C. (2012) Critical role of Th17 proinflammatory cytokines to delay skin wound healing, Cytokine, 59, 503.
Bailey, S. R., Nelson, M. H., Himes, R. A., Li, Z., Mehrotra, S., and Paulos, C. M. (2014) Th17 cells in cancer: the ultimate identity crisis, Front. Immunol., 5, 276.
Sallusto, F., and Lanzavecchia, A. (2009) Human Th17 cells in infection and autoimmunity, Microbes Infect., 11, 620–624.
Lv, L., Pan, K., Li, X. D., She, K. L., Zhao, J. J., Wang, W., Chen, J. G., Chen, Y. B., Yun, J. P., and Xia, J. C. (2011) The accumulation and prognosis value of tumor infiltrating IL-17 producing cells in esophageal squamous cell carcinoma, PLoS One, 6, e18219.
Liu, J., Duan, Y., Cheng, X., Chen, X., Xie, W., Long, H., Lin, Z., and Zhu, B. (2011) IL-17 is associated with poor prognosis and promotes angiogenesis via stimulating VEGF production of cancer cells in colorectal carcinoma, Biochem. Biophys. Res. Commun., 407, 348–354.
Wang, L., Yi, T., Kortylewski, M., Pardoll, D. M., Zeng, D., and Yu, H. (2009) IL-17 can promote tumor growth through an IL-6-Stat3 signaling pathway, J. Exp. Med., 206, 1457–1464.
Guery, L., and Hugues, S. (2015) Th17 cell plasticity and functions in cancer immunity, Biomed. Res. Int., 2015, 314620.
Kim, J. S., Sklarz, T., Banks, L. B., Gohil, M., Waickman, A. T., Skuli, N., Krock, B. L., Luo, C. T., Hu, W., Pollizzi, K. N., Li, M. O., Rathmell, J. C., Birnbaum, M. J., Powell, J. D., Jordan, M. S., and Koretzky, G. A. (2013) Natural and inducible TH17 cells are regulated differently by Akt and mTOR pathways, Nat. Immunol., 14, 611–618.
Author information
Authors and Affiliations
Corresponding author
Additional information
To whom correspondence should be addressed.
Original Russian Text © L. A. Tashireva, V. M. Perelmuter, V. N. Manskikh, E. V. Denisov, O. E. Savelieva, E. V. Kaygorodova, M. V. Zavyalova, 2017, published in Biokhimiya, 2017, Vol. 82, No. 5, pp. 732-748.
Rights and permissions
About this article
Cite this article
Tashireva, L.A., Perelmuter, V.M., Manskikh, V.N. et al. Types of immune-inflammatory responses as a reflection of cell–cell interactions under conditions of tissue regeneration and tumor growth. Biochemistry Moscow 82, 542–555 (2017). https://doi.org/10.1134/S0006297917050029
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0006297917050029