Abstract
Comparing to primary surgery, revision ACL reconstruction is more technically demanding and has a higher failure rate. Theoretically, rehabilitation can improve knee function after ACL reconstruction surgery. This study aimed to compare knee stability, strength, and function between primary and revision ACL reconstructed knees. 40 primary and 40 revision ACL reconstruction surgeries were included between April 2013 and May 2016. Patients with revision surgery had a higher anteroposterior translation comparing those with primary reconstruction (median laxity, 2.0 mm vs. 3.0 mm, p = 0.0022). No differences were noted in knee extensor at 60°/sec or 180°/sec (p = 0.308, p = 0.931, respectively) or in flexor muscle strength at 60°/sec or 180°/sec between primary and revision ACL reconstruction knees (p = 0.091, p = 0.343, respectively). There were also no significant differences between functional scores including IKDC score and Lysholm score in primary versus revision surgeries at 12th months after index operation (p = 0.154, p = 0.324, respectively). In conclusion, despite having higher anteroposterior instability, patients with revision ACL reconstruction can have non-inferior outcomes in isokinetic knee strength and function compared to those with primary ACL reconstruction after proper rehabilitation.
Similar content being viewed by others
Introduction
Anterior cruciate ligament reconstruction (ACLR) surgery is a common procedure to improve functional stability after an anterior cruciate ligament (ACL) injury. The successful rate of primary ACLR is approximated to be 75% to 97% among patients1,2. This means that almost one-fourth of primary ACLR surgeries bound to fail despite improved surgical methods3. The causes associated with failed ACLR surgery are surgical factors and repetitive injury to the knee4,5. Among these patients, approximately 2.9 to 8.9% underwent the following revision ACLR surgery6,7.
Compared to primary ACLR surgery, revision surgery is more technically demanding. In revision surgery, accessibility to original tunnels is a key factor of success since the removal of hardware is often required and bone grafting is likely to be necessary8. This contributes to an estimated 35% failure rate of revision ACLR surgery, which translated to approximately 54% of patients returning to pre-injury levels9. Therefore, with these technical difficulties, the success rate of revision ACLR surgery is commonly less compared to primary ACLR surgery10.
In addition to regain the joint stability, the goal of ACLR surgery is also to recover the function of the knee joint and muscle strength10. To maximize the outcomes of surgery and enhance the functional recovery, an appropriate rehabilitation program is incorporated into the routine postoperative care. The impaired knee functions associated with ACL injury include instability in dynamic movement and quadriceps weakness. As being critical to dynamic joint stability, the quadriceps muscle weakness eventually leads to decreased knee function, and poor exercise performance, and may contribute early onset of osteoarthritis11,12,13. Thus, the strength of muscle around the knee joint, especially the quadriceps muscle, was the main target of training and keep indicator for monitoring the functional recovery after ACLR surgery13.
Thus, to evaluate the success of primary ACLR surgery, joint stability, muscle strength and knee function were common outcomes reported in previous studies1,10,11. However, there were limited studies which have assessed muscle strength recovery following revision ACLR surgery. Thus, we performed this study to assess the stability and functional recovery after primary and revision ACLR surgery under the scheduled rehabilitation program.
This study aimed to (1) compare recovery of knee extensor muscle (quadriceps) and flexor muscle (hamstring) strength in primary versus revision ACLR surgery, and (2) compare clinical functional and stability outcomes in primary versus revision ACLR surgery.
Results
Demographics
There were 80 male participants included in this study. There were no statistically significant differences in age, height and body weight between primary and revision groups (p = 0.538, p = 0.105, p = 0.969 respectively) (Table 1).
Ligament stability
The AP laxity between groups was statistically different (p = 0.0022) (Fig. 1). The median laxity was 2.0 mm (IQR, 1.0 mm–2.5 mm) in primary group and 3.0 mm (IQR, 2.0 mm–3.25 mm) in revision group. AP laxity between involved and healthy limb was also recorded. For the primary group, the difference was <3 mm in 30 cases, 3–5 mm in 10 cases, and >5 mm in none of the cases. For the revision group. The difference was <3 mm in 7 cases, 3–5 mm in 28 cases, and >5 mm in 5 cases. The degree of side-to-side laxity difference was significantly different between two groups (X2 test, p < 0.0001) (Table 2).
Isokinetic knee strength
Deficits in knee extensor strength were not significantly different between primary and revision ACL reconstruction groups, showing 18.0% (IQR, 13.0–28.0%) and 22.0% (IQR, 14.0–33.0%) respectively, at 60°/sec. The knee extensor also showed 17.0% (IQR, 7.0–24.5%) and 14.5% (IQR, 10.0–21.5%) deficit in primary and revision group, respectively at 180°/sec. Moreover, there were no differences in knee flexor strength between primary and revision ACLR groups, showing 9.5% (IQR, 1.5–14.5%) and 12.5 (IQR, 6.0–21.5%), respectively, at 60°/sec and 4.5% (IQR, −2.0–16.5%) and 11.5% (IQR, −0.5–15.0%), respectively, at 180°/sec (Table 3).
Knee functional score
For primary reconstruction, the median IKDC subject score was 81.05 (IQR, 71.7–89.7) and the median Lysholm score was 95.0 (IQR, 89.0–99.0) at the last follow-up. For the revision reconstruction group, the median IKDC subject score was 80.4 (IQR, 67.85–83.85) and the median Lysholm score was 92.5 (IQR, 88.0–95.0) at the last follow-up. There were no differences in functional scores including IKDC score and Lysholm score for primary reconstruction versus revision surgery (p = 0.154, p = 0.324, respectively) (Table 4).
Discussion
The principal findings of this study are patients with revision ACL reconstructed knees had a higher AP translation and a higher percentage of instability than those with primary ACLR surgery. However, after planned rehabilitation, patients in revision groups can have non-inferior results in the isokinetic knee strength and knee functional outcomes compared to those with primary ACLR surgery.
Revision ACLR surgeries are known to show inferior results compared with those for primary ACLR surgeries with respect to postoperative instability, return to sports, and patients’ satisfaction2,10,14,15,16. However, it is unclear that whether the poor clinical outcomes are from knee joint instability or other factors such as muscle strength. Gifstad et al. found an overall reduction in muscle strength for the injured knee compared with the uninjured knee in the patients with revised ACLR, which correspond to the decreased performance in various knee functional scores10. Meanwhile, several studies showed loss of knee flexion strength only17,18,19,20 or both flexion and extension muscle power in patients with the revision ACLR surgery but not in those with the primary ACLR surgery10. In the current study, though with higher degrees of joint instability, patients in the revision ACLR group still had similar performance in the knee flexion and extension muscle power, and had similar clinical outcomes when compared with those in the primary ACLR group.
The ideal graft for ACLR surgery remains controversial. Nevertheless, the degree of joint instability is reported to be associated with graft laxity, whereas allografts can theoretically trigger immune responses and show relatively slower postoperative reformation21,22. In a study comparing autografts and allografts in ACLR surgery, a significant difference of ≥3 mm was found in ligament laxity measurements in 14.9% of autografts and 31.1% of allografts23. In contrast, there was no difference in laxity between the revision group and primary group when only autologous hamstring tendon was used as the graft material24. Accordingly, in this study, we used double-looped semitendinosus and gracilis autografts for primary ACLR compared to tibialis anterior tendon allografts for revision ACLR. Considering significant laxity as side-to-side difference more than 5 mm in AP laxity25,26, none in primary group and five patients of the revision group (12.5%) showed laxity of ≥5 mm in this study. As such, we found a statistically significant difference in the joint laxity between two groups. To sum up, this difference between the two groups may possibly attribute to the different graft materials used.
Muscle strength is a factor greatly influencing knee function. Therefore, it is important to accurately determine the level of muscular strength during postoperative recovery. The quadriceps muscle plays a key role in maintaining dynamic stability of the knee joint, whereas hamstring muscles act as an agonist to the ACL preventing anterior dislocation of the knee27. Atrophy of these two muscles causes more functional instability and impairment. Although isokinetic equipment is widely used for accurate and objective assessment of muscle strength in the knee joint1,10,11, evidence on revision ACLR surgery using isokinetic equipment to assess muscle strength is lacking. In this study, we used isokinetic equipment to assess the degree of muscle strength recovery in the knee joint between the two groups at the same time point of 1 year postoperatively. The two groups had similar outcomes in isokinetic muscle strengths, which corresponded to similar results in functional scores.
Uribe et al.28 reported that the outcomes of revision ACLR, in that only about half patients returned to their pre-injury activity level which was not as good as primary ACLR, regardless of the type of graft materials. However, we observed similar results in extensor and flexor muscle defect rates between primary and revision ACLR groups. Moreover, there were also no differences in functional knee scores (IKDC and Lysholm score) between the two groups. That is, after planned training and rehabilitation, patients with revision ACR still can have good results in knee strength and functions.
Our study had four limitations. First, there is the small number of revision ACLR cases, and all patients are males. The findings of our study cannot apply to the female patients. Further studies on females are needed. Second, the fixation methods of tendon graft were not identical with and between two groups, which cause inherent bias of this study. Third, the pre-injury status of each patient was hardly recorded, which might make the interpretation of findings difficult, especially muscle strength. However, we presented the data of isokinetic muscle strength deficit by comparing the healthy limb, which could minimize this potential bias. Fourth, we cannot address the impact of potential covariates including commitment meniscus injury and critical physical findings status due to incomplete recording and limited sample size. Further study with a large sample will validate the findings of comparison after adjustment of potential covariates.
In conclusion, patients with revision ACLR surgery had significantly higher AP laxity than those with primary ACLR surgery but can have similar results in knee strength and functions after rehabilitation. More intensive rehabilitation is suggested for patients with revision ACLR surgery.
Methods
Subjects and demographics
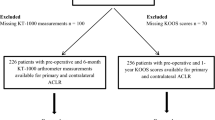
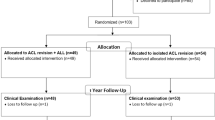
This is a cross-sectional study with 80 male patients with arthroscopic ACL reconstruction surgery (40 primaries and 40 revisions) recruited from Samsung Medical Center between April 2013 and May 2016. Hamstring (semitendinosus-gracilis) tendon autografts were used in the primary ACL reconstruction group, while tibialis anterior tendon allografts were used in revision ACL reconstruction group. The grafts were fixed by a cortical suspensory device (ENDOBUTTON CL, Smith-Nephew, London, UK) for the femoral side and bioabsorbable interference screws with a post-tie for the tibial side. The exclusion criteria were that patient who had more than one revision ACL reconstruction surgery on the same knee, combined/multiple ligamentous injuries or previous surgery on the same lower limb. All participants provided informed consent prior to testing, and the study was approved by the Sungkyunkwan University School of Medicine Clinical Research Ethics Board (SMC 2016-09-074-001). The committee that approved the research, confirm that all research was performed in accordance with relevant guidelines/regulations. Informed consent was obtained from all participants and/or their legal guardians.
Rehabilitation
The same postoperative rehabilitation program was used for primary and revision groups. At the first week right after the operation, the general light intensity of isometric exercises and range of motion (ROM) exercises were performed. The angle of knee flexion increased 15° each week in ROM exercise program. At the fourth week, the knee joint range of motion achieved at 90°, and reached 130° at the sixth week. The patients subjected to partial weight bearing for 4–6 weeks postoperatively and progressively switched to full weight-bearing. By the 6–12 weeks, the patient would achieve combined strength, endurance and balance exercise without pain. At six months, light running was allowed. By nine month after surgery, the patient could receive sports-related training if there were no problems such as effusion, pain, or knee instability.
Assessment
Anteroposterior (AP) knee translation was assessed via the KT-2000 arthrometer (MEDmetric, San Diego, CA, USA) with maximal manual tension and a knee flexion angle of 20° and 30 lb (134 N) anterior force at 12 months after surgery. The measurements were done three times, and a mean value was calculated. These examinations were done by the same personnel who have several years of arthrometry experience to minimize the errors of measurements. Side-to-side AP laxity difference between injured and noninjured knee was also recorded.
At 12 months after index surgery, Isokinetic knee strength with peak extensor and flexor torque (Nm/kg) was evaluated via a CSMI dynamometer (CSMI Medical Solutions, Stoughton, MA, USA) whereby angular velocities of 60°/sec and 180°/sec were measured to determine isokinetic knee strength. After warming up on a cycle ergometer for 5 min, subjects were allowed to practice the test protocol for familiarization. Subsequently, patients allowed to perform the strength test 3 times with a 1 minute washout period between each test session. While doing the sessions, patients were encouraged to perform with the maximum effort by the examiner. Isokinetic concentric measurements of quadriceps and hamstring strength demonstrated excellent reliability29. Both injured and non-injured side were measured for three times, and a mean difference was calculated as
Knee joint functional scores were evaluated at 12 months after index surgery using International Knee Documentation Committee (IKDC)30 and Lysholm knee scales31. The IKDC knee scale quantifies symptoms, sports activities, and function30. The Lysholm knee scale quantifies pain, instability, locking, swelling, stair-climbing, squatting abilities, and need for support31.
Statistical analysis
A priori calculated power >0.80 at an alpha level equal to 0.05 was used to determine that a sample size of 35 for each group was necessary to determine in KT-2000 arthrometry value32. All data statistical analysis was performed using SPSS version 13.0 (SPSS Inc., Chicago, IL, USA). Chi-Squared test and Mann-Whitney U test were used throughout to compare variables between two groups, with p < 0.05 considered statistically significant. All data were reported with median and interquartile range (IQR).
Data availability
The datasets generated during and analysed during the current study are not publicly available due to policy of the Sungkyunkwan University School of Medicine Clinical Research Ethics Board but are available from the corresponding author on reasonable request.
References
Biau, D. J., Tournoux, C., Katsahian, S., Schranz, P. & Nizard, R. ACL reconstruction: a meta-analysis of functional scores. Clin. Orthop. Relat. Res. 458, 180–187 (2007).
Kamath, G. V., Redfern, J. C., Greis, P. E. & Burks, R. T. Revision Anterior Cruciate Ligament Reconstruction. Am J Sports Med 39, 199–217 (2010).
Brown, C. H. & Carson, E. W. Revision Anterior Cruciate Ligament Surgery. Clin Sports Med 18, 109–171 (1999).
Bach, B. R. Revision anterior cruciate ligament surgery. Arthroscopy 19, 14–29 (2003).
Diamantopoulos, A. P., Lorbach, O. & Paessler, H. H. Anterior cruciate ligament revision reconstruction: results in 107 patients. Am J Sports Med 36, 851–860 (2008).
Muneta, T. et al. Revision anterior cruciate ligament reconstruction by double-bundle technique using multi-strand semitendinosus tendon. Arthroscopy 26, 769–781 (2010).
Wolf, R. S. & Lemak, L. J. Revision anterior cruciate ligament reconstruction surgery. Journal of the Southern Orthopaedic Association 11, 25–32 (2002).
Group, M. et al. Descriptive epidemiology of the Multicenter ACL Revision Study (MARS) cohort. Am J Sports Med 38, 1979–1986 (2010).
Busfield, B. T., Safran, M. R. & Cannon, W. D. Extensor Mechanism Disruption After Contralateral Middle Third Patellar Tendon Harvest for Anterior Cruciate Ligament Revision Reconstruction. Arthroscopy 21, 1268 (2005).
Gifstad, T., Drogset, J. O., Viset, A., Grontvedt, T. & Hortemo, G. S. Inferior results after revision ACL reconstructions: a comparison with primary ACL reconstructions. Knee Surg Sports Traumatol Arthrosc 21, 2011–2018 (2013).
Kim, D. K., Hwang, J. H. & Park, W. H. Effects of 4 weeks preoperative exercise on knee extensor strength after anterior cruciate ligament reconstruction. J Phys Ther Sci 27, 2693–2696 (2015).
Muaidi, Q. I., Nicholson, L. L., Refshauge, K. M., Herbert, R. D. & Maher, C. G. Prognosis of conservatively managed anterior cruciate ligament injury: a systematic review. Sports Med 37, 703–716 (2007).
Slemenda, C. et al. Quadriceps weakness and osteoarthritis of the knee. Ann Intern Med 127, 97–104 (1997).
Thomas, N. P., Kankate, R., Wandless, F. & Pandit, H. Revision anterior cruciate ligament reconstruction using a 2-stage technique with bone grafting of the tibial tunnel. Am J Sports Med 33, 1701–1709 (2005).
Wright, R. et al. Revision ACL reconstruction outcomes: MOON cohort. J Knee Surg 24, 289–294 (2011).
Wright, R. W. et al. Outcome of revision anterior cruciate ligament reconstruction: a systematic review. J Bone Joint Surg Am 94, 531–536 (2012).
Aune, A. K., Holm, I., Risberg, M. A., Jensen, H. K. & Steen, H. Four-strand hamstring tendon autograft compared with patellar tendon-bone autograft for anterior cruciate ligament reconstruction. Am J Sports Med 29, 722–728 (2001).
Drogset, J. O. et al. Autologous patellar tendon and quadrupled hamstring grafts in anterior cruciate ligament reconstruction: a prospective randomized multicenter review of different fixation methods. Knee Surg Sports Traumatol Arthrosc 18(8), 1085–1093 (2010).
Matsumoto, A. et al. A comparison of bone-patellar tendon-bone and bone-hamstring tendon-bone autografts for anterior cruciate ligament reconstruction. Am J Sports Med 34(2), 213–219 (2006).
Mohtadi, N. G., Chan, D. S., Dainty, K. N. & Whelan, D. B. Patellar tendon versus hamstring tendon autograft for anterior cruciate ligament rupture in adults. Cochrane Database Syst Rev 9, CD005960, https://doi.org/10.1002/14651858.CD005960.pub2 (2011).
Ahn, J. H. & Choi, H. J. Arthroscopic anterior cruciate ligament reconstruction using bone-patellar tendon-bone autograft. Journal of the Korean Orthopaedic Association 35, 375–380 (2000).
Harner, C. D. et al. Allograft versus autograft anterior cruciate ligament reconstruction: 3- to 5-year outcome. Clin. Orthop. Relat. Res. 324, 134–144 (1996).
Tibor, L. M. et al. Clinical outcomes after anterior cruciate ligament reconstruction: a meta-analysis of autograft versus allograft tissue. Sports Health 2, 56–72 (2010).
Weiler, A., Schmeling, A., Stohr, I., Kaab, M. J. & Wagner, M. Primary versus single-stage revision anterior cruciate ligament reconstruction using autologous hamstring tendon grafts: a prospective matched-group analysis. Am J Sports Med 35, 1643–1652 (2007).
Battaglia, M. J. et al. Results of revision anterior cruciate ligament surgery. Am J Sports Med 35, 2057–2066 (2007).
Denti, M. et al. Revision anterior cruciate ligament reconstruction: causes of failure, surgical technique, and clinical results. Am J Sports Med 36, 1896–1902 (2008).
Keays, S. L., Bullock-Saxton, J. E., Newcombe, P. & Bullock, M. I. The effectiveness of a pre-operative home-based physiotherapy programme for chronic anterior cruciate ligament deficiency. Physiother Res Int 11, 204–218 (2006).
Uribe, J. W., Hechtman, K. S., Zvijac, J. E. & Tjin-A-Tsoi, E. W. Revision anterior cruciate ligament surgery: experience from Miami. Clin. Orthop. Relat. Res. 325, 91–99 (1996).
Myer, G. D. et al. The relationship of hamstrings and quadriceps strength to anterior cruciate ligament injury in female athletes. Clin J Sport Med 19, 3–8 (2009).
Peters, G., Wirth, C. & Kohn, D. Comparison of knee ligament scores and rating systems. Z Orthop und Ihre Grenzgeb 135, 63–69 (1997).
Lysholm, J. & Gillquist, J. Evaluation of knee ligament surgery results with special emphasis on use of a scoring scale. Am J Sports Med 10, 150–154 (1982).
Anderson, A. F., Snyder, R. B. & Lipscomb, A. B. Anterior cruciate ligament reconstruction. A prospective randomized study of three surgical methods. Am J Sports Med 29, 272–9 (2001).
Author information
Authors and Affiliations
Contributions
D.K.K. and W.H.P. designed the study and directed the project. D.K.K. and G.P. performed the test and recorded the data. D.K.K. and L.T.K. analyzed the data and prepared the tables and figures. D.K.K., G.P. and K.B.H.M.K. wrote the paper. D.K.K., G.P. and L.T.K. contributed to interpretation of the results. All authors provided critical feedback and helped shape the research, analysis and manuscript.
Corresponding authors
Ethics declarations
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Kim, D.K., Park, G., Kadir, K.B.H.M.S. et al. Comparison of Knee Stability, Strength Deficits, and Functional Score in Primary and Revision Anterior Cruciate Ligament Reconstructed Knees. Sci Rep 8, 9186 (2018). https://doi.org/10.1038/s41598-018-27595-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-018-27595-8
- Springer Nature Limited
This article is cited by
-
Joint effusion, anteroposterior stability, muscle strength and degree of patellofemoral osteoarthritis significantly impact outcome following revision ACL reconstruction
Journal of Experimental Orthopaedics (2021)
-
Patients older than 50 years had similar results of knee strength and anteroposterior stability after ACL reconstruction compared to younger patients
Knee Surgery, Sports Traumatology, Arthroscopy (2019)