Abstract
Background
The study aimed to analyze the effect of uteroplacental insufficiency (UPI) on leptin expression and lung development of intrauterine growth restriction (IUGR) rats.
Methods
On day 17 of pregnancy, time-dated Sprague-Dawley rats were randomly divided into either an IUGR group or a control group. Uteroplacental insufficiency surgery (IUGR) and sham surgery (control) were conducted. Offspring rats were spontaneously delivered on day 22 of pregnancy. On postnatal days 0 and 7, rats’ pups were selected at random from the control and IUGR groups. Blood was withdrawn from the heart to determine leptin levels. The right lung was obtained for leptin and leptin receptor levels, immunohistochemistry, proliferating cell nuclear antigen (PCNA), western blot, and metabolomic analyses.
Results
UPI-induced IUGR decreased leptin expression and impaired lung development, causing decreased surface area and volume in offspring. This results in lower body weight, decreased serum leptin levels, lung leptin and leptin receptor levels, alveolar space, PCNA, and increased alveolar wall volume fraction in IUGR offspring rats. The IUGR group found significant relationships between serum leptin, radial alveolar count, von Willebrand Factor, and metabolites.
Conclusion
Leptin may contribute to UPI-induced lung development during the postnatal period, suggesting supplementation as a potential treatment.
Impact
-
The neonatal rats with intrauterine growth restriction (IUGR) caused by uteroplacental insufficiency (UPI) showed decreased leptin expression and impaired lung development.
-
UPI-induced IUGR significantly decreased surface area and volume in lung offspring.
-
This is a novel study that investigates leptin expression and lung development in neonatal rats with IUGR caused by UPI.
-
If our findings translate to IUGR infants, leptin may contribute to UPI-induced lung development during the postnatal period, suggesting supplementation as a potential treatment.
Similar content being viewed by others
Introduction
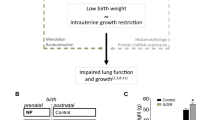
Intrauterine growth restriction (IUGR) has a global frequency of roughly 10% and is linked with a higher likelihood of fetal and neonatal mortality and morbidity.1,2 Current evidence suggests that stressful prenatal settings alter the development of lungs and result in lasting abnormalities in the structure of lungs and decreased respiratory performance during postnatal life.3,4,5 Our and other preclinical investigations have shown that IUGR is related to decreased lung development during the neonate and early childhood.6,7 Human investigation has discovered that IUGR increases the chances of having lower lung function in individuals during their developmental years, adolescence, and later in life.8,9,10,11,12 The condition is marked by reduced placental activity and impaired vital nutrients and oxygen transfer to the developing fetus.2,4,13 Previous studies have demonstrated that an impaired placental function may impede the appropriate growth and development of a fetus, and is closely associated with bronchopulmonary dysplasia.14,15 A fetus’s growth rate below its genetically determined potential size per race and sex is characterized as IUGR.16,17 Research conducted both in vivo and in vitro has demonstrated that adipose tissue is capable of synthesizing various amino acids.18 Within adipose tissue, leptin is mainly synthesized and secreted.19,20 Leptin is a hormone approximately 16-kDa in size and possesses pro-inflammatory properties. As an adipokine, it significantly impacts both innate and adaptive immune responses. Leptin performs essential bodily functions such as cellular homeostasis, metabolism, angiogenesis, and regulating the immune system and inflammatory responses. Additionally, studies have shown that it can cause airway smooth muscle cells to produce higher levels of vascular endothelial growth factors (VEGF), which might be linked to IUGR.21,22,23,24 Pathways related to amino acid metabolism, such as the urea cycle, aspartate metabolism, arginine and proline metabolism, and glycine and serine metabolism, demonstrate a significant association with leptin levels. 25,26,27 Nonetheless, leptin and its receptors are present in fat tissue and various organs, such as the lungs.20,28 Leptin levels increase at late gestation and influence postnatal organ development.29 Administering leptin to pregnant rats increased the lung weight/body weight ratio and promoted alveolar type II cell number and maturation, enhancing surfactant protein expression in rat fetuses.30 In a rat model of fetal growth restriction, Chen et al. discovered that administering maternal leptin treatment improved lung maturation and elevated levels of SP-A expression.31 These lung maturational effects of leptin were also found in the ovine fetus.32 In rats, postnatal leptin deficiency persistently impaired lung development and decreased surface area and lung volume from 2 to 10 weeks of age.33
These findings suggest that leptin is critical for postnatal lung remodeling. However, the lung leptin status during the postnatal period was unknown in intrauterine growth-restricted offspring. We hypothesized that if leptin has a significant impact on lung development, UPI would decrease leptin during the postnatal period, and leptin expression would be correlated with lung development in growth-restricted rat offspring. This study aimed to investigate UPI’s effects on lung leptin expression and lung development in rat offspring.
Materials and Methods
Animal model
The animal study conducted at Taipei Medical University was reviewed and approved by the Laboratory Animal Care Committee. Time-dated pregnant Sprague-Dawley rats were kept in separate cages and given laboratory food and water as per their needs. They were exposed to a 12:12-hour light-dark cycle. On the 17th day of gestation, either bilateral uterine artery ligation was performed to induce uteroplacental insufficiency (IUGR group) or sham surgery was done (control group).7 The dams recovered fast from the uterine artery ligation and sham surgeries and were able to resume feeding the next day. On gestation day 22, all newborn rats were born normally. The day of birth for the rats was designated as postnatal day 0. The newborn pups were gathered and redistributed among the mothers within 12 hours of birth. To ensure all pups had equal access to breast milk, the control and IUGR groups’ litters were culled to nine and four pups, respectively, after the pups were euthanized on postnatal days 0 and 7. The pulmonary tissues employed in these experiments were obtained from a previous study to investigate metabolomics, which detected metabolites, and miobiota investigation, which revealed the radial alveolar count (RAC) and the von Willebrand Factor (vWF) in IUGR rats.34,35
Rat tissue collection and processing
On the postnatal days 0 and 7, rats were randomly selected for examination from each group, irrespective of sex. Animals were euthanized with an overdose of isoflurane inhalation, body weights were recorded and blood from the heart was withdrawn to check serum leptin levels, and lungs were harvested for lung leptin and leptin receptor levels, histological and western blot analysis.
Serum leptin levels
Serum leptin levels were measured using the Bio-Plex 200 analyzer (Bio-Rad Laboratories, Hercules, CA) in accordance with the manufacturer’s instructions. In sample diluent, we diluted the serum 1:4. The samples were measured using a low Photomultiplier Tube setting, as specified in the assay manual. The Bio-Plex filter plates and manual vacuum manifold were used for the tests. The Bio-Plex ManagerTM software was used.
Lung morphometry
The volume fraction was calculated by digitizing pictures and selecting five nonoverlapping fields (four corners and one middle region) from each section. At a final magnification of 200×, the images were printed and analyzed. Each animal was observed in 10 different regions at random. The number of points along the alveolar airways and alveolar walls was counted by superimposing 49-point clear grids onto enlarged printed pictures. The volume fraction was equal to Pi/Pt, where Pi was the number of test points that touched the structure of interest and Pt was the total number of points that hit the reference space.36
Western blot analysis of leptin and leptin receptor
Lung tissues were homogenized in ice-cold buffer containing 50 mM TrisHCl (pH 7.5), 1 mM egtazic acid, 1 mM ethylenediaminetetraacetic acid, and a protease inhibitor cocktail (complete minitablets; Roche, Mannheim, Germany). The samples were sonicated and then centrifuged at 500 g for 20 min at 4 °C to remove cellular debris. Proteins (30 μg) were resolved on 12% sodium dodecyl sulfate–polyaylamide gel electrophoresis gels under reducing conditions. Next, they were electroblotted onto a polyvinylidene difluoride membrane (ImmobilonP, Millipore, Bedford, MA). Following blocking with 5% nonfat dry milk, the membranes were incubated with an anti-leptin antibody (1:500, ab117751, Abcam, Boston, MA), an anti-leptin receptor antibody (1:750, ab5593, Abcam, Boston), and an anti-β-actin antibody (1:1000, C4 sc-47778, Santa uz Biotechnology, Santa uz, CA). They were subsequently incubated with horseradish peroxidase-conjugated goat antirabbit IgG or anti-mouse IgG (Pierce Biotechnology, Rockford, IL). The protein bands were detected using the BioSpectrum AC System (UVP, Upland, CA) and VisionWorks LS Software version 8.6 (UVP, Upland).
Immunohistochemistry of proliferating cell nuclear antigen
Proliferating cell nuclear antigen (PCNA) is expressed in cells from late G1 through S-phase. As a result, antibodies targeted towards this particular protein should be used as a probe for immunocytochemically marking the nuclei of proliferating cells.37 By measuring immunostained pulmonary nuclei, we demonstrated the feasibility and reliability of this approach. Furthermore, after deparaffinization in xylene and rehydration in an alcohol series, the 5-μm lung sections were preincubated for 1 hour at room temperature in 0.1 M PBS containing 10% normal goat serum and 0.3% H2O2 to block endogenous peroxidase activity and nonspecific antibody binding. The sections were then incubated for 20 hours at 4 °C with rabbit monoclonal anti-PCNA antibody (1:100, ab92552 Abcam, Cambridge, MA). The sections were followed for one hour at 37 °C with biotinylated goat anti-rabbit immunoglobulin G (1:200, Vector Laboratories, Burlingame, CA), and then reacted with the reagents from an Avidin–Biotin Complex kit (Vector Laboratories). The brown reaction products were visualized after using a diaminobenzidine substrate kit (Vector Laboratories) according to the manufacturer’s recommendations. The immunostained sections were viewed and photographed using a Nikon Eclipse E600 (Nikon, Tokyo, Japan). PCNA-stained vessel density was calculated in an unbiased manner at 200× magnification, with at least five random lung regions selected per animal, according to the method modified by Agard et al.38. The digital images were quantified using the automatic object counting and measuring process to generate a percentage of positive vessels.
Statistical analysis
Data are expressed in terms of the mean ± SD. Age groups were compared using Student’s t-test. Correlations between the serum leptin, the RAC, and the vWF were analyzed using Pearson’s correlation test. Differences were considered statistically significant at p < 0.05 and a strong positive linear relationship at r’s value near 1.39
Results
UPI decreased body weights at birth and on postnatal days 0 and 7
In summary, four sham-operated delivered 39 control pups and three dams with UPI delivered 26 IUGR rats. The IUGR rats’ mean birth weight (5.89 ± 0.74 g) was significantly lower than the control rats (6.36 ± 0.55 g; p < 0.01). These findings indicate that IUGR has been established. We retrieved 12 and 8 pups from the sham-operated and UPI-induced dams for examination on postnatal day 0. On postnatal day 7, we retrieved eight pups from the sham-operated and eight pups from the UPI-induced dams, respectively. On both postnatal days 0 and 7, the IUGR rats had significantly lower body weights than the control rats (Fig. 1a).
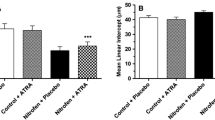
a Body weight and b serum leptin levels (pg/ml) of the control and intrauterine growth restriction (IUGR) groups on postnatal days 0 and 7. Compared with the control rats, the IUGR rats had a significantly lower body weight and serum leptin. Data are expressed in terms of the mean ± standard deviation. Age groups were compared using Student’s t-test (control, n = 12; IUGR, n = 8) (**p < 0.01, ***p < 0.001 vs. control).
UPI decreased serum leptin levels in growth-restricted newborn rats
The lungs of the IUGR rats exhibited significantly lower serum leptin levels on postnatal day 0 (253.65 pg/ml; p < 0.001) and postnatal day 7 (270.36 pg/ml; p < 0.001) than the control rats on postnatal days 0 (429.41 pg/ml) and 7 (445.40 pg/ml) (Fig. 1b).
UPI decreased lung leptin and leptin receptor expression in growth-restricted newborn rats
Representative Western blots and quantitative data determined using densitometry for lung leptin and leptin receptor are presented in Fig. 2a, b. The IUGR rats had significantly lower leptin and leptin receptor levels on postnatal day 0 (p < 0.01) and 7 (p < 0.05) than the control rats, respectively.
a Representative western blots of leptin and (b) leptin-receptor in the lung tissue sample of the control and intrauterine growth restriction (IUGR) groups on postnatal days 0 and 7. Compared with the control rats, the IUGR rats had significantly lower leptin and leptin-receptor. Data are expressed in terms of the mean ± standard deviation. Age groups were compared using Student’s t-test (control, n = 12; IUGR, n = 8) (*p < 0.05, **p < 0.01 vs. control).
UPI altered lung morphometry in growth-restricted newborn rats
Figure 3a presents the representative lung tissue sections stained with hematoxylin and eosin on postnatal days 0 and 7. In both those days, the lungs of rats born to control dams exhibited normal morphology. The lungs of the IUGR rats exhibited a significantly higher volume fraction of alveolar airspace on postnatal day 0 (p < 0.01) and 7 (p < 0.001). The IUGR rats had a significantly lower volume fraction of the alveolar wall on postnatal day 0 (p < 0.05) and 7 (p < 0.001) than the control rats (Fig. 3b).
a Representative lung sections stained with hematoxylin and eosin, b alveolar space volume fraction, and alveolar wall volume fraction in the lung tissue sample of the control and intrauterine growth restriction (IUGR) groups on postnatal days 0 and 7. Compared with the control rats, the IUGR rats had a significantly higher alveolar space volume fraction and lower alveolar wall volume fraction. Data are expressed in terms of the mean ± standard deviation. Age groups were compared using Student’s t-test (control, n = 12; IUGR, n = 8) (*p < 0.05, **p < 0.01, ***p < 0.001 vs. control).
UPI decreased lung PCNA expression in growth-restricted newborn rats
Representative immunohistochemical images of PCNA are presented in Fig. 4a and the results of semiquantitative analysis for vascular density determined by PCNA-positive vessels. The control rats exhibited high and similar PCNA immunoreactivity on postnatal days 0 and 7. The PCNA immunoreactivity and vascular density of the IUGR rats were significantly lower on postnatal days 0 (p < 0.0001) and 7 (p < 0.001) than the control group (Fig. 4b).
a Representative immunohistochemistry for proliferating cell nuclear antigen (PCNA) and b semiquantitative analysis for vascular density determined by PCNA-positive vessels in the lung tissue sample of the control and intrauterine growth restriction (IUGR) groups on postnatal days 0 and 7. Compared with the control rats, the IUGR rats had a significantly lower PCNA-stained vessel. Data are expressed in terms of the mean ± standard deviation. Age groups were compared using Student’s t-test (control, n = 12; IUGR, n = 8) (***p < 0.001, ****p < 0.0001 vs. control).
UPI had high correlations between serum leptin, RAC, vWF, and metabolites
Strong correlations were found between serum leptin and RAC (r = 0.876, p = 4.08 × 10–7), and vWF (r = 0.8911, p = 1.3 × 10–7) on postnatal days 0 (Fig. 5a), serum leptin and RAC (r = 0.617, p = 0.004) and vWF (r = 0.9324, p = 2.1 × 10–9) on postnatal day 7 (Fig. 5b), which metabolite data from IUGR rats’ metabolomics analysis, RAC and vWF data from microbiota research, derived from previous studies [34,35]. Moreover, the correlation coefficient showed high correlations between RAC and metabolites such as LysoPC(20:5(5Z,8Z,11Z,14Z,17Z)/0:0),1-Isopropyl-N-((6-methyl-2-oxo-4-propyl-1,2-dihydropyridin-3-yl)methyl)-6-(2-(4-methylpipe razin-1yl)pyridin-4-yl)-1H-inazole-4-carboxamide,Cytosine,1H-Imidazole-4-carboxamide,3-Aminopyrazin-2-ol, Imexon (p < 0.05), and vWF with metabolites such as LysoPC(20:5(5Z,8Z, 11Z,14Z,17Z)/0:0),1-Isopropyl-N-((6-methyl-2-oxo-4-propyl-1,2-dihydropyridin-3yl)methyl) -6-(2-(4-methylpipe-razin-1yl)pyridin-4-yl)-1H-indazole-4-carboxamid, S-Methylmethanesulf inothioate (p < 0.05), Val-Pro-Asp-Pro-Arg, and viloxazine (p < 0.01) on postnatal day 7.
a Correlations coefficient between serum leptin, radial alveolar count (RAC), and von Willebrand Factor (vWF) in the lung tissue sample of the control and intrauterine growth restriction (IUGR) groups on postnatal days 0 and b 7. Correlations were analyzed using Pearson’s correlation test (control, n = 12; IUGR, n = 8).
Discussion
The present study was designed to unravel the effects of uteroplacental insufficiency-induced IUGR on lung leptin expression and lung morphology using an experimental animal model. We found that experimental IUGR-induced altered lung development during early postnatal development in rats. Our in vivo model demonstrated that UPI during the saccular stage of lung development impaired lung and vascular development, as evidenced by a higher volume fraction of the alveolar airspace and lower volume fraction of the alveolar wall, and decreased vascular density. This is consistent with defective alveolarization in newborn rats exposed to uteroplacental insufficiency during lung development.7,40 These UPI effects were associated with decreased serum leptin and decreased lung leptin and leptin receptor expression, suggesting that the leptin pathway is involved in UPI-induced impaired lung development during the postnatal period.
In this study, IUGR was induced by UPI and all sham-operated and UPI-induced dams were fed standard rat chow through the pregnancy and nourished their offspring during the lactation period. We found that UPI affected body weight in IUGR rats. The IUGR rats exhibited significantly lower body weights at birth (p < 0.01) and on postnatal days 7 (p < 0.001) than control rats. These findings indicate that IUGR has been established.
On postnatal days 0 and 7, these histological abnormalities were the most and least significant, respectively. These findings suggest that developmental exposure to uteroplacental insufficiency has the greatest impact on lung maturation during the immediate postnatal period. Decreased alveolar surface area is associated with reduced lung compliance and increased resistance, while a decreased alveolar wall volume fraction is associated with disturbed pulmonary diffusion capacity.41 However, alveolar and capillary structure estimations are typically associated with measurements of gas diffusion.41 Moreover, PCNA has been investigated as a cell proliferation marker in rat offspring lung tissue. In the presence of peroxidase enzymes that evaluate vascular density, PCNA-stained vessels using 3,3’-diaminobenzidine eate a brown reaction result. Interestingly, the assessment of PCNA revealed that the control rats had high and similar PCNA immunoreactivity, the IUGR rats group had a significant decrease on postnatal days 0 and 7, representing the proliferation in the lung. In support, PCNA promotes the proliferation of cells and growth, also known as a proliferative marker in the lungs.42,43,44 On the other hand, previous studies showed PCNA levels were not changed by the effect of IUGR on apoptosis in neonatal and adult rat lungs,45 and another clinical finding in humans showed that PCNA in IUGR with catchup growth group had a significant increase in primary neonatal myofibroblasts from rat lungs of IUGR, supporting the increase in proliferation, indicated airway resistance, and reduced lung compliance.42 Our results were consistent with the latter concept.
Furthermore, we investigated the correlations between serum leptin, RAC, and vWF on postnatal days 0 and 7. Previous research revealed that various cell types in the healthy lung had high amounts of Ob-Rb,46,47 with particular leptin-binding sites detected in both bronchial and alveolar epithelial cells,48,49,50 airway smooth muscle cells, and (infiltrating) inflammatory cells. Notably, leptin significantly correlates with fibrinogen and von Willebrand factor.51,52 These studies support our findings whereas UPI had high correlations between serum leptin with RAC and vWF on postnatal days 0 and 7. On the other hand, we only investigated the correlation coefficient between RAC, vWF, and metabolites on postnatal day 7, whereas lysophosphatidylcholine (Lyso-PC) showed high correlations with both RAC and vWF. Lyso-PC, a minor fraction, plays a central role in phosphatidylcholine (PC) metabolism and substrate generation. Pulmonary surfactants primarily consist of phospholipids and surfactant proteins, with PC being the most abundant.53,54,55 However, Lyso-PC is potentially toxic, impairing alveolar epithelium barrier functions, causing cell swelling, membrane loss, and protein leak due to its wedge-shaped shape. Earlier research stated lyso-PC, a bioactive proinflammatory lipid, has a substantial impact on inflammatory disorders. LysoPC activates a wide variety of cell types, including endothelial cells, smooth muscle cells, monocytes, maophages, and T-cells. According to a recent study, LysoPC may control second messenger systems by using cloned orphan G-protein-coupled receptors, and directly modulates contractile responses in vascular smooth muscle and prevents relaxations that are dependent on the endothelium.54,56 As a result, based on our research, we speculate that lyso-PC is one of many potential metabolites that can foretell changes in lung development. These findings support the study of altered metabolites in metabolomic analysis and impaired lung development in microbiota investigation in IUGR rats.34,35
The limitation of this study is that it mainly concentrated on the lungs of IUGR and the control group, which only demonstrates the knowledge of itself and does not involve the use of other organs that enable the investigation of certain circumstances in the lungs, and the calculation of correlation between variables was only investigated on postnatal day 7.
In conclusion, leptin may be involved in the mechanism of UPI-induced impaired lung development during the postnatal period and suggests that leptin supplementation may be a promising treatment modality to enhance lung development in IUGR neonates.
Data availability
The datasets generated and analyzed during the current study are available from the corresponding author upon reasonable request.
References
Sun, L. The update of fetal growth restriction associated with biomarkers. Matern. Fetal Med. 4, 210–217 (2022).
Harding, R. et al. The compromised intra-uterine environment: implications for future lung health. Clin. Exp. Pharm. Physiol. 27, 965–974 (2000).
Henriksen, T. & Clausen, T. The fetal origins hypothesis: placental insufficiency and inheritance versus maternal malnutrition in well-nourished populations. Acta Obstet. Gynecol. Scand. 81, 112–114 (2002).
Gagnon, R. Placental Insufficiency and Its Consequences. Eur. J. Obstet. Gynecol. Reprod. Biol. 110, S99–S107 (2003).
Mazarico, E., Molinet-Coll, C., Martinez-Portilla, R. J. & Figueras, F. Heparin therapy in placental insufficiency: systematic review and meta-analysis. Acta Obstet. Gynecol. Scand. 99, 167–174 (2020).
Chen, C. M., Wang, L. F. & Su, B. Effects of maternal undernutrition during late gestation on the lung surfactant system and morphometry in rats. Pediatr. Res. 56, 329–335 (2004).
Huang, L. T., Chou, H. C., Lin, C. M. & Chen, C. M. Uteroplacental insufficiency alters the retinoid pathway and lung development in newborn rats. Pediatr. Neonatol. 57, 508–514 (2016).
Kotecha, S. J. et al. Spirometric lung function in school-age children: effect of intrauterine growth retardation and catch-up growth. Am. J. Respir. Crit. Care Med. 181, 969–974 (2010).
Pike, K., Jane Pillow, J. & Lucas, J. S. Long term respiratory consequences of intrauterine growth restriction. Semin. Fetal Neonatal Med. 17, 92–98 (2012).
Arigliani, M. et al. Lung function between 8 and 15 years of age in very preterm infants with fetal growth restriction. Pediatr. Res. 90, 657–663 (2021).
den Dekker, H. T., Jaddoe, V. W. V., Reiss, I. K., de Jongste, J. C. & Duijts, L. Fetal and infant growth patterns and risk of lower lung function and asthma. The Generation R Study. Am. J. Respir. Crit Care Med 197, 183–192 (2018).
Jordan, B. K. & McEvoy, C. T. Trajectories of lung function in infants and children: setting a course for lifelong lung health. Pediatrics 146, e20200417 (2020).
Wu, G., Bazer, F. W., Wallace, J. M. & Spencer, T. E. Board-invited review: intrauterine growth retardation: implications for the animal sciences. J. Anim. Sci. 84, 2316–2337 (2006).
Pierro, M. et al. Association of the dysfunctional placentation endotype of prematurity with bronchopulmonary dysplasia: a systematic review, meta-analysis and meta-regression. Thorax 77, 268–275 (2022).
Torchin, H. et al. Placental complications and Bronchopulmonary Dysplasia: Epipage-2 Cohort Study. Pediatrics 137, e20152163 (2016).
Sharma, D., Shastri, S. & Sharma, P. Intrauterine growth restriction: antenatal and postnatal aspects. Clin. Med. Insights Pediatr. 10, 67–83 (2016).
Rosenberg, A. The Iugr Newborn. Semin. Perinatol. 32, 219–224 (2008).
Kowalski, T. J., Wu, G. & Watford, M. Rat Adipose tissue amino acid metabolism in vivo as assessed by miodialysis and arteriovenous techniques. Am. J. Physiol. 273, E613–E622 (1997).
Ali Assad, N. & Sood, A. Leptin, Adiponectin and pulmonary diseases. Biochimie 94, 2180–2189 (2012).
Jutant, E. M., Tu, L., Humbert, M., Guignabert, C. & Huertas, A. The thousand faces of leptin in the lung. Chest 159, 239–248 (2021).
Shin, J. H., Kim, J. H., Lee, W. Y. & Shim, J. Y. The expression of Adiponectin receptors and the effects of Adiponectin and Leptin on airway smooth muscle cells. Yonsei Med J. 49, 804–810 (2008).
Otero, M. et al. Leptin: A metabolic hormone that functions like a proinflammatory Adipokine. Drug N. Perspect. 19, 21–26 (2006).
Iikuni, N., Lam, Q. L., Lu, L., Matarese, G. & La Cava, A. Leptin and Inflammation. Curr. Immunol. Rev. 4, 70–79 (2008).
Lanier, V. et al. Leptin-induced Transphosphorylation of vascular endothelial growth factor receptor increases notch and stimulates endothelial cell angiogenic transformation. Int J. Biochem. Cell Biol. 79, 139–150 (2016).
Chao de la Barca, J. M. et al. A metabolomic profiling of intra-uterine growth restriction in placenta and cord blood points to an impairment of lipid and energetic metabolism. Biomedicines 10, 1411 (2022).
Stingl, H., Raffesberg, W., Nowotny, P., Waldhäusl, W. & Roden, M. Reduction of plasma leptin concentrations by arginine but not lipid infusion in humans. Obes. Res. 10, 1111–1119 (2002).
Vernooy, J. H. et al. Leptin as regulator of pulmonary immune responses: involvement in respiratory diseases. Pulm. Pharm. Ther. 26, 464–472 (2013).
Malli, F., Papaioannou, A. I., Gourgoulianis, K. I. & Daniil, Z. The role of Leptin in the respiratory system: an overview. Respir. Res. 11, 152 (2010).
Attig, L., Larcher, T., Gertler, A., Abdennebi-Najar, L. & Djiane, J. Postnatal Leptin is necessary for maturation of numerous organs in newborn rats. Organogenesis 7, 88–94 (2011).
Kirwin, S. M. et al. Leptin enhances lung maturity in the fetal rat. Pediatr. Res. 60, 200–204 (2006).
Chen, H. et al. Leptin promotes fetal lung maturity and upregulates Sp-a Expression in Pulmonary Alveoli Type-Ii epithelial cells involving Ttf-1 activation. PLoS One 8, e69297 (2013).
De Blasio, M. J. et al. Leptin matures aspects of lung structure and function in the Ovine Fetus. Endocrinology 157, 395–404 (2016).
Huang, K. et al. Effects of Leptin deficiency on postnatal lung development in mice. J. Appl. Physiol. 105, 249–259 (2008).
Yuliana, M. E., Huang, Z. H., Chou, H. C. & Chen, C. M. Effects of Uteroplacental insufficiency on growth-restricted rats with altered lung development: a metabolomic analysis. Front. Pediatr. 10, 952313 (2022).
Yang, Y. S. H., Chou, H. C., Liu, Y. R. & Chen, C. M. Uteroplacental insufficiency causes microbiota disruption and lung development impairment in growth-restricted newborn rats. Nutrients 14, 4388 (2022).
Huang, L. T., Chou, H. C., Lin, C. M., Yeh, T. F. & Chen, C. M. Maternal Nicotine exposure exacerbates neonatal hyperoxia-induced lung fibrosis in rats. Neonatology 106, 94–101 (2014).
Thaete, L. G., Ahnen, D. J. & Malkinson, A. M. Proliferating Cell Nuclear Antigen (Pcna/Cyclin) immunocytochemistry as a labeling index in mouse lung tissues. Cell Tissue Res. 256, 167–173 (1989).
Agard, C. et al. Protective role of the antidiabetic drug metformin against chronic experimental pulmonary hypertension. Br. J. Pharm. 158, 1285–1294 (2009).
Obilor, E. I. & Amadi, E.C. Test for significance of Pearson’s correlation coefficient (r). Int. J. Innov. Math. Stat. Energy Policies 6, 11–23 (2018).
Joss-Moore, L. et al. Intrauterine growth restriction transiently delays alveolar formation and disrupts retinoic acid receptor expression in the lung of female rat pups. Pediatr. Res. 73, 612–620 (2013).
Cox, A. M., Gao, Y., Perl, A. T., Tepper, R. S. & Ahlfeld, S. K. Cumulative effects of neonatal hyperoxia on murine alveolar structure and function. Pediatr. Pulmonol. 52, 616–624 (2017).
Nawabi, J. et al. Novel functional role of Gh/Igf-I in neonatal lung myofibroblasts and in rat lung growth after intrauterine growth restriction. Am. J. Physiol. Lung Cell Mol. Physiol. 315, L623–l637 (2018).
Rössig, L. et al. Akt-dependent Phosphorylation of P21(Cip1) regulates pcna binding and proliferation of endothelial cells. Mol. Cell Biol. 21, 5644–5657 (2001).
Muglia, L. J. et al. Proliferation and differentiation defects during lung development in Corticotropin-releasing hormone-deficient mice. Am. J. Respir. Cell Mol. Biol. 20, 181–188 (1999).
Alejandre Alcázar, M. A. et al. Inhibition of Tgf-Β signaling and decreased apoptosis in IUGR-associated lung disease in rats. PLoS One 6, e26371 (2011).
Löllmann, B., Grüninger, S., Stricker-Krongrad, A. & Chiesi, M. Detection and quantification of the leptin receptor splice variants Ob-Ra, B, and, E in different mouse tissues. Biochem. Biophys. Res. Commun. 238, 648–652 (1997).
Tsuchiya, T., Shimizu, H., Horie, T. & Mori, M. Expression of Leptin receptor in lung: leptin as a growth factor. Eur. J. Pharm. 365, 273–279 (1999).
Dal Farra, C., Zsürger, N., Vincent, J. P. & Cupo, A. Binding of a Pure 125i-Monoiodoleptin Analog to mouse tissues: a developmental study. Peptides 21, 577–587 (2000).
Bergen, H. T., Cherlet, T. C., Manuel, P. & Scott, J. E. Identification of Leptin receptors in lung and isolated fetal Type Ii cells. Am. J. Respir. Cell Mol. Biol. 27, 71–77 (2002).
Bellmeyer, A. et al. Leptin resistance protects mice from hyperoxia-induced acute lung injury. Am. J. Respir. Crit. Care Med. 175, 587–594 (2007).
Koh, K. K., Park, S. M. & Quon, M. J. Leptin and cardiovascular disease. Circulation 117, 3238–3249 (2008).
Guagnano, M. T. et al. Leptin Inease is associated with markers of the hemostatic system in obese healthy women. J. Thromb. Haemost. 1, 2330–2334 (2003).
Batenburg, J. J. Surfactant Phospholipids: Synthesis and storage. Am. J. Physiol. 262, L367–L385 (1992).
O’Hare, M. M. et al. Lyso-Phosphatidylcholine and outcome of preterm babies with respiratory distress syndrome treated with surfactant. Early Hum. Dev. 49, 135–141 (1997).
Agassandian, M. & Mallampalli, R. K. Surfactant phospholipid metabolism. Biochim Biophys. Acta 1831, 612–625 (2013).
Matsumoto, T., Kobayashi, T. & Kamata, K. Role of Lysophosphatidylcholine (Lpc) in Atherosclerosis. Curr. Med Chem. 14, 3209–3220 (2007).
Acknowledgements
We thank Zheng-Hao Huang for the technical assistance.
Funding
This work was supported by a grant from the Ministry of Science and Technology of Taiwan (MOST 111-2314-B-038-113-MY2).
Author information
Authors and Affiliations
Contributions
The experiments were conducted at the animal center of Taipei Medical University. C-MC. contributed to the conception and design of this study. M.Y., H.-C.C., E. C.-YS., H.-C.C., L.-T.H. and C.-M.C contributed to the performance of the experiments, analysis and interpretation of the data, and approval of the manuscript. All authors agree to assume responsibility for all aspects of the work to ensure proper investigation and resolution of issues related to the accuracy or integrity of any part of the work. All authors contributed to the article and approved the submitted version.
Corresponding author
Ethics declarations
Competing interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yuliana, M.E., Chou, HC., Su, E.CY. et al. Uteroplacental insufficiency decreases leptin expression and impairs lung development in growth-restricted newborn rats. Pediatr Res 95, 1503–1509 (2024). https://doi.org/10.1038/s41390-023-02946-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-023-02946-y
- Springer Nature America, Inc.