Abstract
Pre-eclampsia (PE) is thought to be related to placental dysfunction, particularly poor extravillous trophoblast (EVT) invasion and migration abilities. However, the pathogenic mechanism is not fully understood. This article describes the impact of the cyclic adenosine monophosphate(cAMP) signaling pathway on EVT behavior, focusing on EVT proliferation, invasion, and migration. Here, we used the HTR8/SV-neo cell line to study human EVT function in vitro. HTR8/SV-neo cells were treated with different concentrations of forskolin (cAMP pathway-specific agonist) to alter intracellular cAMP levels, and dimethyl sulfoxide (DMSO) was used as the control. First, a cAMP assay was performed to measure the cAMP concentration in HTR8/SV-neo cells treated with different forskolin concentrations, and cell proliferation was assessed by constructing cell growth curves and assessing colony formation. Cell invasion and migration were observed by Transwell experiments, and intracellular epithelial-mesenchymal transition (EMT) marker expression was evaluated by quantitative real-time polymerase chain reaction (qPCR) and Western blotting (WB). According to our research, the intracellular cAMP levels in HTR8/SV-neo cells were increased in a dose-dependent manner, and HTR8/SV-neo cell proliferation, invasion and migration were significantly enhanced. The expression of EMT and angiogenesis markers was upregulated. Additionally, with the increase in intracellular cAMP levels, the phosphorylation of intracellular mitogen-activated protein kinase (MAPK) signaling pathway components was significantly increased. These results suggested that the cAMP signaling pathway promoted the phosphorylation of MAPK signaling components, thus enhancing EVT functions, including proliferation, invasion, and migration, and to a certain extent, providing a novel direction for the treatment of PE patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pre-eclampsia (PE) occurs in pregnant women after 20 weeks of gestation, and it is characterized by symptoms such as high blood pressure and proteinuria. PE is thought to be related to placental dysfunction [1], particularly poor extravillous trophoblast (EVT) invasion and migration in uterine spiral arteries, which leads to defective vascular remodeling and placental hypoperfusion [2].
However, overly invasive EVTs can cause multiple pathologies during pregnancy, including placenta accreta, placental implantation, uterine perforation, hemorrhagic shock and even death [3]. Therefore, it is thought that highly coordinated EVT functions are necessary to maintain a healthy utero-placental status.
EVTs exhibit high degrees of invasion, migration and proliferation during placental implantation, which are similar to the pathological effects observed during cancer invasion [4]. Recent tumor studies have shown that cyclic adenosine monophosphate (cAMP), which is an important mediator of signaling cascades between cells, is closely associated with the development of tumors [5]. The currently recognized cAMP signaling pathway mainly includes cAMP/protein kinase A/cyclic-AMP response binding protein (cAMP/PKA/CREB) and cAMP/exchange protein activated by cAMP/Ras-proximate-1 (cAMP/Epac/Rap1) [5]. Changes in intracellular cAMP levels can cause a variety of physiological and pathological changes, including changes to tissue metabolism, cell proliferation or apoptosis, and tumor cell invasion and migration [6, 7].
Furthermore, previous studies have shown that cAMP signaling pathway may affect the proliferation and migration of various tumor cells by regulating the downstream mitogen-activated protein kinase (MAPK) signaling pathway [5]. The MAPK signaling pathway is also a key pathway that regulates a variety of intracellular processes, and the MAPK pathway includes the extracellular signal-regulated kinase 1/2 (ERK1/2), JUN N-terminal kinases 1/2/3 (JNK1/2/3) and p38-MAPK kinase signaling pathways [8]. However, the cAMP signaling pathway exert different effects on the MAPK signaling pathway depending on the type of cell. In studies on clear cell renal cell carcinoma (ccRCC), activation of the intracellular cAMP signaling pathway was shown to inhibit the phosphorylation of ERK in the MAPK signaling pathway in a c-Raf-dependent manner, thereby attenuating the proliferation of tumor cells [9]. However, in prostate cancer, the overexpression of PKA inhibitor proteins (PKIs) was shown to block the activation of PKA, causing a continuous increase in intracellular cAMP levels through negative feedback; then, these increased cAMP levels activated another signaling pathway, namely, the cAMP/Epac/Rap1 pathway, and induced the phosphorylation of downstream MAPK signaling pathway components, ultimately promoting the proliferation and migration of cells [10].
Forskolin, which is an ancient herbal remedy that is derived from Indian plants [11], is used as a selective agonist of the cAMP signaling pathway to elevate intracellular cAMP levels. Many in vivo and in vitro studies have shown that it inhibits the development of cancer to a certain degree. Forskolin directly binds to the catalytic subunit of adenylate cyclase(AC), inducing conformational changes at the adenosine 5'-triphosphate(ATP) site, thereby converting ATP to cAMP and pyrophosphate [12].
Based on the discovery of the role of the cAMP signaling pathway in tumors, we speculate that the cAMP signaling pathway may also exert a certain effect on trophoblasts. Our study involved the use of forskolin to activate the cAMP signaling pathway and focused on observing changes in EVT proliferation, invasion, and migration. This investigation aimed to elucidate the potential involvement of the cAMP signaling pathway in EVT behavior, particularly its interplay with the MAPK signaling pathway. This is of great importance for understanding embryo implantation, placenta formation and regulation, and the prevention and treatment of pregnancy-related placental disorders.
Materials and Methods
Cell Culture
The human first-trimester placenta trophoblast cell line HTR8/SV-neo (HTR8) was obtained from the Shanghai Institute of Cell Biology, Chinese Academy of Sciences. Cells were cultured in Dulbecco’s modified Eagle medium (DMEM) supplemented with 10% fetal bovine serum (FBS) in a 5% CO2 humidified atmosphere at 37 °C.
cAMP Assay
Prior to the experiment, HTR8 cells were plated in dishes (5 × 105 cells) and incubated for 48 h in DMEM with forskolin (Beyotime, China) at concentrations of 10, 50, or 100 μM. Moreover, cells that were treated with dimethyl sulfoxide (DMSO) solution in medium were used as controls. The experiment was conducted with the cAMP ELISA Kit (Gersion Biotechnology, China). After lysis with radio immunoprecipitation assay (RIPA) buffer on ice, the cell suspensions were centrifuged for 10 min at 600 g to remove insoluble materials. According to the instructions, the cells were seeded in 96-well plates, as well as the standards S0-S5 in the kit and incubated with cAMP-HRP solution for 1 h at 37 °C. The cells were later washed by washing buffer, and incubated again with reaction substrate A and B for 30 min in the dark. Then, add stop solution 50 μl to each well to stop the reaction. The plate was read at OD450 nm. The standard curve of cAMP was drawn according to the formula. Then, the cAMP levels in HTR8 cells were calculated.
Cell Growth Curve
The cells were allowed to grow in 24-well plates (2 × 103 cells) and cultured for 4 days. The cells were dispersed with 0.25% trypsin–EDTA (Gibco, USA) and counted every day. Each cell line experiment was performed in triplicate. The cell growth curve assays were performed according to the methods that we previously described [13].
Colony Formation Assay
After incubation in DMEM containing different concentrations of forskolin for 48 h, the cells were harvested and seeded in 6-well plates (2 × 103 cells). After approximately two weeks, when microscopy revealed that the number of cells in the vast majority of individual clones in the dish was greater than 50, the culture was terminated. The cells were then washed and stained with Giemsa (Sigma-Aldrich, Germany) staining solution for 15 min after fixation with 4% paraformaldehyde (Biosharp, China) for 30 min. After drying, the dishes were imaged with a camera, and the clones were counted with ImageJ. The colony formation assay was performed according to the methods that we previously described [13].
Transwell Assay
A Transwell assay was performed to assess the invasive ability of cells. The membranes of the filters were coated with Matrigel (100 μl per filter; BD Biosciences) in plates with 8-μm pores (BD Biosciences). Cells (2 × 104) treated with different concentrations of forskolin for 48 h and seeded in the upper chambers, while medium supplemented with 10% FBS was seeded in the lower chambers. After 24 h of culture, the cells that invaded to the lower surface of the membrane were fixed with 4% paraformaldehyde and stained with Giemsa. After drying, the cells were examined under a microscope (OLYMPUS, Japan). For each well, 10 fields of view were randomly selected, the number of cells was quantified at a magnification of 20 × . Transwell assays were performed according to the methods that we previously described [14].
Transwell Migration Assay
Cells(2 × 104) were treated with different concentrations of forskolin for 48 h and seeded into the upper chambers (8-μm pores, 24-well plates), and medium supplemented with 10% FBS was added to the lower chambers. After 24 h of culture, the cells that had migrated to the lower surface of the membrane were fixed with 4% paraformaldehyde and stained with Giemsa. The cell numbers were counted as described above.
RNA Isolation and Quantitative Real-Time Polymerase Chain Reaction (qPCR)
Total RNA was extracted using TRIzol reagent (Invitrogen Life Technologies, USA) according to the manufacturer’s instructions. Complementary DNA (cDNA) was synthesized with the Prime Script® RT reagent Kit (Takara, Japan). The primers that were used in this study are listed in Supplementary Table 1. The qPCR thermocycling conditions were as follows: initial denaturation at 95 °C for 30 s and 40 cycles of 95 °C for 5 s and 60 °C for 30 s. The mRNA expression levels of the target genes were quantified using a SYBR® Premix Ex Taq TM II kit (Takara, Japan). Data analyses were performed using the 2(-∆∆Ct) method. Matrix Metalloproteinase 2(MMP2), Platelet Endothelial Cell Adhesion Molecule (PECAM), Neural-cadherin/Cadherin-2 (N-cadherin/CDH2) and Vascular Endothelial-cadherin/Cadherin-5 (VE-cadherin/CDH5) expression was normalized to the expression of GAPDH, which is a housekeeping gene. The samples were run in triplicate. qRT‒PCR was performed according to the methods that we previously described [14].
Western Blotting (WB)
Total proteins were extracted and purified from cells that were treated with different concentrations of forskolin for 48 h. Then, the proteins (30 μg) were separated by sodium dodecyl sulfate–polyacrylamide gel electrophoresis (SDS-PAGE, Beyotime, China) and transferred to polyvinylidene fluoride (PVDF, Beyotime, China) membranes. After blocking with 3% bovine serum albumin (BSA, Beyotime, China) in Tris-buffered saline containing 0.1% Tween-20 (TBST), the membranes were incubated with an anti-N-cadherin antibody (1:1000, CST, USA), anti-MMP-2 antibody (1:1000, Abcam, UK), anti-CDH5 antibody (1:1000, CST, USA), anti-PECAM antibody (1:1000, Solarbio, China), anti-c-Raf antibody(1:1000, CST, USA), anti-phospho-c-Raf antibody (1:1000, CST, USA), anti-MEK1/2 antibody (1:1000, CST, USA), anti-phospho-MEK1/2 antibody (1:1000, CST, USA), anti-ERK1 + ERK2 antibody(1:1000, Abcam, UK), and anti-phospho-p44/42 MAPK (Erk1/2) antibody (1:1000, CST, USA) at 4 °C overnight. Then, the membranes were incubated with HRP-conjugated Affinipure goat anti-mouse/rabbit IgG (1:10000, Proteintech, USA) the next day. Finally, the specific protein bands were visualized with a chemiluminescent substrate kit (Millipore, USA), and images were captured using a Tanon 4600SF instrument (Tanon, China). The densitometric analyses were performed using ImageJ® software (NIH, USA), and all the results are expressed as target protein expression relative to GAPDH total protein expression as needed. An anti-GAPDH antibody (1:20000, Abcam, UK) was used as the control. WB was performed according to the methods that we previously described [14].
Statistical Analysis
All the statistical analyses were performed using the SPSS software package (version 26.0, SPSS, Inc.) and Prism 7.0 software (GraphPad, La Jolla, CA, USA). The data are presented as the means ± standard deviations (SD) of at least three independent experiments. The t test was used to analyze differences in the data between two groups. Differences were considered statistically significant at the level of p < 0.05.
Results
cAMP Levels Were Upregulated by Forskolin in HTR8/SV-Neo Cells
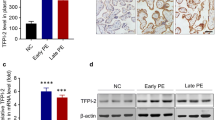
Forskolin was used to activate adenylate cyclase in cells and therefore increase intracellular cAMP concentrations, thus regulating multiple cellular mechanisms, such as gene transcription, ion transport, and protein phosphorylation. We treated HTR8 cells with 0, 10, 50, or 100 µM forskolin for 48 h. As shown in Fig. 1, intracellular cAMP levels in HTR8/SV-neo cells were increased in a dose-dependent manner.
cAMP levels were upregulated by forskolin in HTR8/SV-neo cells (A). HTR8/SV-neo cells were treated with 0, 10, 50, or 100 μM forskolin for 48 h, and a dose-dependent increase in cAMP levels was observed (B). The data are presented as the mean ± SD obtained from at least three independent experiments
The cAMP Signaling Pathway Enhanced HTR8/SV-Neo Cell Proliferation
To determine the effect of the cAMP signaling pathway on the proliferation of EVTs, HTR8/SV-neo cells were incubated with forskolin as described above. Compared with the control group, the proliferation of cells that were treated with 10 μM or 50 μM forskolin for 72 or 96 h was significantly increased, while that of the cells that were treated with 100 μM seemed very similar to that of the control (Fig. 2A, B). In addition, the colony formation assay revealed that 10 µM forskolin, followed by 50 µM forskolin, increased HTR8/SV-neo cell proliferation (Fig. 2C), and the results were analyzed as shown in Fig. 2D. Thus, 10 μM and 50 μM forskolin were used in subsequent experiments.
The cAMP signaling pathway enhances HTR8/SV-neo cell proliferation. When HTR8/SV-neo cells were treated with 0 μM, 10 μM, 50 μM, or 100 μM forskolin, (A, B) growth curve assays and (C, D) colony-forming assays showed that the proliferation of HTR8/SV-neo cells that were treated with 10 μM or 50 μM forskolin was higher than that of the control cells. Error bars represent the mean ± SD of three independent experiments. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001
The cAMP Signaling Pathway Enhanced HTR8/SV-Neo Cell Invasion and Migration
In concordance with cell growth and proliferation, we investigated whether the cAMP signaling pathway promotes or suppresses HTR8 cell invasion and migration. The Transwell assay revealed a significant increase in the invasion of cells that were treated with 10 µM or 50 µM concentrations compared to the control, and the increase was especially notable after treatment with 50 μM (Fig. 3A, B). The Transwell migration assay indicated that HTR8/SV-neo cells with higher cAMP levels exhibited significantly more extensive migration than control cells, as shown in Fig. 3C.
The cAMP signaling pathway enhances HTR8/SV-neo cell invasion and migration. (A, B) In the cells that were treated with 10 μM or 50 μM forskolin, invasion was significantly enhanced compared to the control, and migration was also significantly enhanced (C, D). Error bars represent the mean ± SD of three independent experiments. ***p < 0.001, ****p < 0.0001
The cAMP Signaling Pathway Increased the mRNA and Protein Expression Levels of N-Cadherin, CDH5, MMP2, and PECAM
To investigate the molecular mechanism by which cAMP signaling pathway affected cell proliferation, invasion and migration, we employed qPCR and WB to assess Epithelial-Mesenchymal Transition (EMT). Thus, the mRNA and protein expression levels of EMT markers were measured. As the intracellular cAMP levels increased, the mRNA expression levels of N-cadherin, CDH5, MMP2 and PECAM were significantly increased compared with those in the control group (Fig. 4A). As shown in Fig. 4B, the protein expression of N-cadherin, CDH5 and MMP2 was significantly increased, compared to that in the control group. Overall, the cAMP signaling pathway may induce EMT in HTR8/SV-neo cells, thus promoting the invasion and migration of trophoblasts.
The cAMP signaling pathway regulates the expression of invasion and migration marker proteins. (A) The mRNA expression of N-cadherin, CDH5, MMP2 and PECAM in HTR8/SV-neo cells that were treated with 10 μM or 50 μM forskolin was measured by qPCR. (B) The protein expression of N-cadherin, CDH5, MMP2 and PECAM in HTR8/SV-neo cells that were treated with 10 μM or 50 μM forskolin was measured by WB. (C) The protein levels were quantified by densitometry analysis using ImageJ software. Error bars represent the mean ± SD of three independent experiments. *p < 0.05, **p < 0.01, ***p < 0.001, ****p < 0.0001
The cAMP Signaling Pathway Promoted the Phosphorylation of MAPK/ERK Signaling Pathway Components
It was reported that the cAMP signaling pathway was associated with the MAPK signaling pathway, in trophoblasts; thus, the level of phosphorylated MAPK/ERK signaling components were evaluated in HTR8/SV-neo cells that were treated with different concentrations of forskolin. As the intracellular cAMP levels increased, phosphorylation of MAPK/ERK signaling components, including c-raf259, MEK1/2 and ERK1/2, was significantly increased (Fig. 5A–F).
The cAMP signaling pathway regulates the phosphorylation of MAPK/ERK signaling pathway components. (A-F) Protein levels of total and phosphorylated c-raf259, MEK and ERK were significantly increased in cells that were treated with 10 μM or 50 μM forskolin compared with the control group. (G, H) The ratio of the protein expression p-ERK to ERK was decreased by using U0126, which is an inhibitor of the MAPK/ERK signaling pathway. Error bars represent the mean ± SD of three independent experiments. *p < 0.05, ****p < 0.0001
Prior studies revealed that the cAMP signaling pathway enhanced cell growth, proliferation, invasion and migration, especially in cells that were treated with a concentration of 50 μM. To confirm whether the cAMP signaling pathway regulated trophoblasts via the MAPK/ERK signaling pathway, a specific ERK inhibitor, namely, U0126, was used to block this pathway. Then, we examined the phosphorylation of MAPK/ERK signaling pathway components after treatment with 50 μM forskolin, the MAPK/ERK pathway inhibitor U0126 or a combination. When HTR8/SV-neo cells were treated with U0126 alone, the phosphorylation of the ERK protein in the cells was suppressed. When HTR8/SV-neo cells were treated with 50 μM forskolin alone, the phosphorylation of the ERK protein in the cells was significantly enhanced. However, when the cells were treated again with 50 μM forskolin after treatment with U0126, the phosphorylation of ERK remained low, and ERK activity was even more potently inhibited (Fig. 5G, H).
Discussion
Before an embryo implants into the maternal endometrium, the embryo develops to the blastocyst stage, and the trophectoderm layer differentiates into two subtypes: villous trophoblasts (VTs) and EVTs [15]. In the first trimester, EVTs, together with natural killer cells and macrophages, infiltrate the maternal endometrium and migrate through the myometrium to reach the spiral arteries. This physiological process transforms spiral arteries into wide-diameter, low-resistant vessels, enhancing fetal blood supply and promoting embryo and placental growth [16]. The HTR8/SV-neo cell line is widely used to study the adhesion, migration and invasion of trophoblasts, and this cells line was generated by transfecting human primary trophoblasts with SV40-containing large T antigens [17]. Therefore, the HTR8/SV-neo cell line is an important in vitro model of human EVTs, and it is used to observe changes in the proliferation, invasion and migration of these cells and to explore possible potential mechanisms.
The cAMP signaling pathway is involved in regulating a variety of basic biological processes in the body as well as the occurrence and development of tumor cells. Based on the characteristics of EVTs in the first trimester, which are similar to those of tumor cells, we investigated whether the cAMP signaling pathway is also involved in regulating EVT functions. Forskolin is a specific activator of the cAMP signaling pathway. As expected, we found that intracellular cAMP levels increased in a dose-dependent manner after forskolin treatment. However, due to the poor solubility of forskolin, up to 3% DMSO solution by mass is required to dissolve it, whereas most intact mammalian cell experiments can tolerate only up to 1% DMSO [18]. In this experiment, the cells were treated with different concentrations of forskolin, which was dissolved in DMSO solution as necessary. To exclude the possible effect of DMSO, which is toxic to cells at certain concentrations, on the experimental results, we treated the control group with the highest amount of DMSO that was added to the experimental groups. In addition, the high hydrophobicity of forskolin means that it has a slow rate of dissociation; thus, there is a certain drug-prolonging effect, and the effect can be effectively achieved by applying forskolin to cells for 48 h and 10 min.
As intracellular cAMP levels increased, we found that HTR8/SV-neo cells exhibited significantly enhanced proliferation, invasion, and migration. Interestingly, at a concentration of 100 μM, the cells were no longer clearly able to proliferate. We speculate that intracellular cAMP may improve the proliferation of cells within a certain concentration range. Studies have shown that elevated cAMP levels can promote cell proliferation in some physiological cells or tumors, and some studies have suggested that cAMP may cause cell cycle arrest or even apoptosis [9, 19]. When cAMP levels exceed a certain threshold, cell proliferation can decrease or stop and cells can even be prone to apoptosis, such as in tumors. Since EVTs exhibit high proliferation, aggressiveness, and migration, similar to tumor cells [20], we deeply suspect that high levels of Camp may inhibit cell proliferation and even promote apoptosis. This provides a new idea for our research.
Furthermore, our results suggested that the Camp signaling pathway promoted EMT in HTR8/SV-neo cells, which was associated with an increase in the expression of N-cadherin, CDH5, MMP2, and PECAM. In a variety of epithelial tumor cells, the junctions between cells become loose, adhesion to the basement membrane decreases, and then EMT occurs. Tumor cells exhibit invasion and migration characteristics similar to those of mesenchymal cells, and these characteristics promote the metastasis of tumor cells [21]. Additionally, the morphology of tumor cells changed, the cytoskeleton was remodeled, and the expression of epithelial markers, such as E-cadherin, was downregulated; these markers were replaced with the expression of N-cadherin and wave proteins and so on [22]. MMPs are among the key enzymes in the process of cell invasion and migration [23]. They are able to degrade the extracellular matrix, which is especially important for cell invasion and vascular remodeling [24]. CDH5 and PECAM are important components of vascular endothelial cells [25], and involved in maintaining vascular barrier function [26]. However, the protein expression of PECAM was not observed in HTR8/SV-neo cells. We wondered why and consulted the literature. Interestingly, it was reported that PECAM is expressed on the vascular endothelium in the placenta but not throughout the villous or in EVTs in normal or pathological samples [26]. However, in our study, the mRNA expression of PECAM was increased, and the specific mechanism underlying this phenomenon may be a good topic for future research.
The cAMP/PKA/CREB signaling pathway and MAPK signaling pathway are two classical pathways that regulate cell growth and metabolism, and they have been extensively studied in a variety of tumor cells and trophoblasts [27]. Studies on urothelial bladder carcinoma (UCB) have shown that centrosomal protein (CEP)-72 promotes the invasion and migration of UCB cells by enhancing the binding of CREB in the cAMP signaling pathway to the SERPINE1 promoters of serpin family gene [28]. In esophageal squamous cell carcinoma, lysosomal-associated membrane protein 3(LAMP3) attenuates the phosphorylation of VASP at the Ser239 site through PKA, thereby enhancing the aggressiveness of esophageal squamous cell carcinomas (ESCC) and promoting the metastasis of ESCC [29]. In trophoblasts, the cAMP/PKA/CREB signaling pathway has been found to be involved in the regulation of trophoblast fusion function [30, 31]. In our study, we found that the levels phosphorylated c-Raf259, MEK1/2 and ERK1/2 in the MAPK signaling pathway were significantly increased after the cAMP signaling pathway was activated. This finding led us to wonder whether EVT function was enhanced by increases in the phosphorylation of c-raf, which is a member of the MAPK signaling pathway, at the Ser259 locus. The specific connection between the cAMP signaling pathway and the MAPK signaling pathway still needs further exploration.
Pre-eclampsia is a complication of pregnancy to which substantial attention has been given because of its high morbidity and mortality rates and its association with increased risk of chronic diseases, such as diabetes, hypertension and cardiovascular diseases, in the postpartum period. However, the pathogenesis of PE is poorly understood, and to date, there is no effective treatment other than childbirth [1]. Many studies have shown that after an embryo is implanted into the maternal endometrium, the ability of EVTs to proliferate, invade and migrate gradually increases. In contrast, when PE occurs, the invasion and migration of EVTs appear to be impaired, which leads to insufficient remodeling of the uterine spiral artery, low placental blood perfusion and superficial placental implantation in the uterus [32]. Thus, the proliferation, invasion and migration of EVTs are thought to be essential for pregnancy [33]. In our study, the proliferation, invasion and migration of EVTs were increased, which was accompanied by activation of the cAMP and MAPK signaling pathways. This helps us to better understand EVT function and provides some direction for the treatment of trophoblast-derived diseases of pregnancy. Although extensive research has been conducted on PE, there is no effective treatment for the disease other than termination of pregnancy. At present, some anticoagulant drugs are also used to improve placental blood circulation perfusion, thereby improving the perinatal safety of PE patients. The results of this study suggest that we can also improve placental function with certain drugs, thereby improving perinatal pregnancy outcomes and poor prognosis in PE patients.
However, there are some limitations in our study. Since the experiments were performed in a cell line model, in vivo experiments are required for further validation. In the future, there are still many challenges, such as establishing animal models of PE, observing changes in cell function within placental tissues after treatment with forskolin, and even determining the relationship between the two signaling pathways.
Conclusion
This experimental study explored the effects of the cAMP signaling pathway on the proliferation, invasion, and migration of EVTs and the interplay of this pathway with the MAPK signaling pathway. Forskolin was used as an activator to alter the level of cAMP in cells. The HTR8/SV-neo cell line was selected as the in vitro model. After treatment with forskolin, the level of cAMP in cells was elevated in a dose dependent manner. As the cAMP signaling pathway was activated, the activities of EVTs, including proliferation, invasion and migration, were significantly enhanced. Moreover, the phosphorylation of MAPK signaling pathway components was significantly promoted. In conclusion, the cAMP signaling pathway can improve the behaviors of EVTs through the coordinated regulation of the MAPK signaling pathway. These findings may contribute to a better understanding of EVT function and provide a feasible solution to improve placental cell function, thereby improving perinatal outcomes and the poor prognosis of PE patients.
Data Availability
The data used to support the results of the study are included in the published paper.
The data are clearly presented and can be made publicly available for publication.
Code Availability
Not applicable.
References
Nakashima A, Cheng SB, Ikawa M, et al. Evidence for lysosomal biogenesis proteome defect and impaired autophagy in preeclampsia [J]. Autophagy. 2020;16(10):1771–85.
Zhang H, He Y, Wang JX, et al. miR-30–5p-mediated ferroptosis of trophoblasts is implicated in the pathogenesis of preeclampsia [J]. Redox Biol. 2020;29:101402.
Varberg KM, Iqbal K, Muto M, et al. ASCL2 reciprocally controls key trophoblast lineage decisions during hemochorial placenta development. Proc Natl Acad Sci USA. 2021;118(10):e2016517118.
Tabrizi MEA, Gupta JK, Gross SR. Ezrin and its phosphorylated Thr567 form are key regulators of human extravillous trophoblast motility and invasion. Cells. 2023;12(5):711.
Zhang H, Kong Q, Wang J, et al. Complex roles of cAMP-PKA-CREB signaling in cancer [J]. Exp Hematol Oncol. 2020;9(1):32.
Matsumoto H, Sato Y, Horie A, et al. CD9 suppresses human extravillous trophoblast invasion [J]. Placenta. 2016;47:105–12.
Naviglio S, Caraglia M, Abbruzzese A, et al. Protein kinase A as a biological target in cancer therapy [J]. Expert Opin Ther Targets. 2009;13(1):83–92.
Guo YJ, Pan WW, Liu SB, et al. ERK/MAPK signalling pathway and tumorigenesis [J]. Exp Ther Med. 2020;19(3):1997–2007.
Cao M, Nawalaniec K, Ajay AK, et al. PDE4D targeting enhances anti-tumor effects of sorafenib in clear cell renal cell carcinoma and attenuates MAPK/ERK signaling in a CRAF-dependent manner [J]. Transl Oncol. 2022;19:101377.
Hoy JJ, Salinas Parra N, Park J, et al. Protein kinase A inhibitor proteins (PKIs) divert GPCR-Galphas-cAMP signaling toward EPAC and ERK activation and are involved in tumor growth [J]. FASEB J. 2020;34(10):13900–17.
Sapio L, Gallo M, Illiano M, et al. The Natural cAMP Elevating Compound Forskolin in Cancer Therapy: Is It Time? [J]. J Cell Physiol. 2017;232(5):922–7.
Sengupta S, Mehta G. Natural products as modulators of the cyclic-AMP pathway: evaluation and synthesis of lead compounds [J]. Org Biomol Chem. 2018;16(35):6372–90.
Sun F, Jie Q, Li Q, et al. TUSC3 inhibits cell proliferation and invasion in cervical squamous cell carcinoma via suppression of the AKT signalling pathway [J]. J Cell Mol Med. 2022;26(5):1629–42.
Jie Q, Sun F, Li Q, et al. Downregulated ribosomal protein L39 inhibits trophoblast cell migration and invasion by targeting E-cadherin in the placenta of patients with preeclampsia [J]. FASEB J. 2021;35(4):e21322.
Papuchova H, Kshirsagar S, Xu L, et al. Three types of HLA-G+ extravillous trophoblasts that have distinct immune regulatory properties [J]. Proc Natl Acad Sci U S A. 2020;117(27):15772–7.
Nakashima A, Yamanaka-Tatematsu M, Fujita N, et al. Impaired autophagy by soluble endoglin, under physiological hypoxia in early pregnant period, is involved in poor placentation in preeclampsia [J]. Autophagy. 2013;9(3):303–16.
Baryla M, Kaczynski P, Goryszewska E, et al. Prostaglandin F2alpha stimulates adhesion, migration, invasion and proliferation of the human trophoblast cell line HTR-8/SVneo [J]. Placenta. 2019;77:19–29.
Dessauer CW, Watts VJ, Ostrom RS, et al. International Union of Basic and Clinical Pharmacology. CI. Structures and Small Molecule Modulators of Mammalian Adenylyl Cyclases [J]. Pharmacol Rev. 2017;69(2):93–139.
Smith SA, Newby AC, Bond M. Ending restenosis: inhibition of vascular smooth muscle cell proliferation by cAMP. Cells. 2019;8(11):1447.
Abbas Y, Turco MY, Burton GJ, et al. Investigation of human trophoblast invasion in vitro [J]. Hum Reprod Update. 2020;26(4):501–13.
Mittal V. Epithelial Mesenchymal Transition in Tumor Metastasis [J]. Annu Rev Pathol. 2018;13:395–412.
Wang M, Xu Y, Wang P, et al. Galectin-14 Promotes Trophoblast Migration and Invasion by Upregulating the Expression of MMP-9 and N-Cadherin [J]. Front Cell Dev Biol. 2021;9:645658.
Vissenberg R, Manders VD, Mastenbroek S, et al. Pathophysiological aspects of thyroid hormone disorders/thyroid peroxidase autoantibodies and reproduction [J]. Hum Reprod Update. 2015;21(3):378–87.
Staff AC, Ranheim T, Henriksen T, et al. 8-Iso-prostaglandin f(2alpha) reduces trophoblast invasion and matrix metalloproteinase activity [J]. Hypertension. 2000;35(6):1307–13.
Chen X, Zhang S, Du K, et al. Gastric cancer-secreted exosomal X26nt increases angiogenesis and vascular permeability by targeting VE-cadherin [J]. Cancer Sci. 2021;112(5):1839–52.
Lyall F, Bulmer JN, Duffie E, et al. Human trophoblast invasion and spiral artery transformation: the role of PECAM-1 in normal pregnancy, preeclampsia, and fetal growth restriction [J]. Am J Pathol. 2001;158(5):1713–21.
Delidaki M, Gu M, Hein A, et al. Interplay of cAMP and MAPK pathways in hCG secretion and fusogenic gene expression in a trophoblast cell line [J]. Mol Cell Endocrinol. 2011;332(1–2):213–20.
Li X, Dong P, Wei W, et al. Overexpression of CEP72 Promotes Bladder Urothelial Carcinoma Cell Aggressiveness via Epigenetic CREB-Mediated Induction of SERPINE1 [J]. Am J Pathol. 2019;189(6):1284–97.
Huang F, Ma G, Zhou X, et al. Depletion of LAMP3 enhances PKA-mediated VASP phosphorylation to suppress invasion and metastasis in esophageal squamous cell carcinoma [J]. Cancer Lett. 2020;479:100–11.
Duan FM, Fu LJ, Wang YH, et al. THBS1 regulates trophoblast fusion through a CD36-dependent inhibition of cAMP, and its upregulation participates in preeclampsia [J]. Genes Dis. 2021;8(3):353–63.
Darashchonak N, Koepsell B, Bogdanova N, et al. Adenosine A2B receptors induce proliferation, invasion and activation of cAMP response element binding protein (CREB) in trophoblast cells. BMC Pregnancy Childbirth. 2014;14:2. https://doi.org/10.1186/1471-2393-14-2.
Wang XH, Xu S, Zhou XY, et al. Low chorionic villous succinate accumulation associates with recurrent spontaneous abortion risk [J]. Nat Commun. 2021;12(1):3428.
Moser G, Windsperger K, Pollheimer J, et al. Human trophoblast invasion: new and unexpected routes and functions [J]. Histochem Cell Biol. 2018;150(4):361–70.
Acknowledgements
The authors sincerely thank all the participants in this study.
Funding
This study was financially supported by the Hainan Provincial Natural Science Foundation (No. ZDKJ2021037), the China Postdoctoral Science Foundation (No. 2021M691466) and the National Natural Science Foundation of China (No. 8220061871).
Author information
Authors and Affiliations
Contributions
Yuanhua Huang and Yanlin Ma were responsible for the conception and design of the study and the experiments, while data collection was performed by Jiaoqi Mei and Mengyi Song. Yanhong Yi and ChaoSun designed the experiments and drafted the manuscript. The final version of the manuscript was approved by all the authors.
Corresponding authors
Ethics declarations
Ethics Approval
All the studies were approved by the Medical Ethics Committee of First Affiliated Hospital of Hainan Medical University(2022-KYL-039), and performed in accordance with the Declaration of Helsinki.
Consent for Publication
All the authors have consented to the publication of this article.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Chao Sun and Jiaoqi Mei share first authorship
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sun, C., Mei, J., Yi, H. et al. The Effect of the cAMP Signaling Pathway on HTR8/SV-Neo Cell Line Proliferation, Invasion, and Migration After Treatment with Forskolin. Reprod. Sci. 31, 1268–1277 (2024). https://doi.org/10.1007/s43032-023-01396-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43032-023-01396-5