Abstract
Purpose
Time-restricted feeding (TRF) reverses obesity and insulin resistance, yet the central mechanisms underlying its beneficial effects are not fully understood. Recent studies suggest a critical role of hypothalamic galanin and its receptors in the regulation of energy balance. It is yet unclear whether TRF could regulate the expression of galanin and its receptors in the hypothalamus of mice fed a high-fat diet.
Methods
To test this effect, we subjected mice to either ad lib or TRF of a high-fat diet for 8 h per day. After 4 weeks, galanin and many neuropeptides associated with the function of metabolism were examined.
Results
The present findings showed that mice under TRF consume equivalent calories from a high-fat diet as those with ad lib access, yet are protected against obesity and have improved glucose metabolism. Plasma galanin, orexin A, irisin and adropin levels were significantly reversed by TRF regimen. Besides, TRF regimen reversed the progression of metabolic disorders in mice by increasing GLUT4 and PGC-1α expression in skeletal muscles. Moreover, the levels of galanin and GALR1 expression were severely diminished in the hypothalamus of the TRF mice, whereas GALR2 was highly expressed.
Conclusions
TRF diminished galanin and GALR1 expression, and increased GALR2 expression in the hypothalamus of mice fed a high-fat diet. The current studies provide additional evidence that TRF is effective in improving HFD-induced hyperglycemia and insulin resistance in mice, and this effect could be associated with TRF-induced changes of the galanin systems in the hypothalamus.
Level of evidence
No level of evidence, animal studies
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The rapid increase in the prevalence of overweight and obesity is becoming an important health problem. Overweight and obesity may cause several metabolic complications, including type 2 diabetes mellitus, hyperlipidemia, nonalcoholic fatty liver disease, coronary artery disease as well as hypertension. Current strategies for treatment of obesity are not adequately effective and are frequently accompanied by many side effects [13]. Thus, new strategies to treat obesity are urgently needed.
Time-restricted feeding (TRF), a key component of intermittent fasting regimens, has gained considerable attention in recent years [3, 38, 40]. Recent studies from animal models of obesity and diabetes illustrate that TRF appears to be effective against preexisting obesity and insulin resistance [8, 10, 11, 27, 41, 44, 46, 54]. Similar studies in rodents demonstrated that mice under a time-restricted high-fat diet consume equivalent calories as those with ad libitum access which are against obesity, hyperinsulinemia and hepatic steatosis [8, 27, 54]. Furthermore, TRF improved mitochondrial abnormalities, lipid infiltration and insulin resistance in muscle of drosophila and rodent models [49]. A recent study from humans further demonstrated that 5 weeks’ TRF regimen improved insulin sensitivity, β cell responsiveness, blood pressure, oxidative stress, and appetite in men with prediabetes [48]. Besides, a recent study highlighted the effectiveness of time-restricted feeding against different nutritional challenges, including high-fat, high-fructose, and high-fat combined with high-fructose diets, all of which are known to cause metabolic disorders [8]. In addition, studies in rodents found that either food accessibility was limited to the dark or light phase, yet the outcome was very similar [27, 47]. Thus, it is conceivable that the key factor is the time restriction from food itself, rather than its occurrence at a specific circadian time [7]. The preliminary evidence in humans suggests that the benefits of TRF are due mostly or only to weight loss [9, 22]. More recently, early TRF regimen improved insulin sensitivity even without weight loss in men with prediabetes [48]. However, the central mechanisms for TRF against obesity-related diseases are not well understood.
Obesity is often accompanied by oscillations and disruptions of many orexigenic and anorexigenic neuropeptides in the hypothalamus [13, 24, 31, 39, 50]. Of note, the neuropeptide galanin participates in feeding behavior via the modulation of neuroendocrine and monoaminergic systems [13]. Galanin is widely expressed in all brain regions [34], particularly in the hypothalamus, where it has important effects on feeding behavior and energy metabolism. There is a wealth of evidences for the important role of central galanin as a critical element linking energy metabolism and glucose homeostasis [16, 18]. On the one hand, the long-term dysregulation of hypothalamic galanin contributes to the development of obesity [2]. In rats, intracerebroventricular (i.c.v.) injection of exogenous galanin into the paraventricular nucleus significantly enhanced daily caloric intake and weight of fat depots [53]. Furthermore, heterozygous galanin overexpressive mice increased the intake of a fat-rich diet by 55% than wild-type mice [29], while galanin knockout mice decreased the intake of fat-rich diet by 48% than wild-type mice [30]. On the other hand, the fatty diet may affect the central galanin level of the animal. Fed with a high-fat diet, rats showed an increase in galanin level and proliferation of galanin-producing neurons in the hypothalamus [35]. The central galanin may also provide positive feedback to increased food intake and body weight in response to high-fat consumption [13]. This positive feedback is an important cause of obesity [13]. In addition, elevated plasma galanin levels were found in patients with obesity and diabetes [14, 16, 36, 56]. The galanin preproprotein levels were positively correlated with elevated circulating triglyceride levels in rats and humans [17, 42].
Besides the effects of nutritional status on galanin expression [5, 17, 23, 42], the feeding status may modulate central galanin expression [6, 32]. Galanin concentrations were more than doubled in the hypothalamus of 16-h or 72-h fasted mice when compared to the ad lib mice [6, 32]. In addition, galanin neurons located in the hypothalamus were activated by food restriction [32]. Unlike fasting, it is yet unclear whether scheduled feeding could regulate the expression of galanin and its receptors in the hypothalamus of mice fed a high-fat diet. To identify whether galanin and its receptors changed during scheduled feeding and evaluate the central mechanisms of TRF on obesity-related metabolic diseases, we subjected mice to either ad lib or TRF of a high-fat diet for 8 h per day last 4 weeks, and analyzed the levels of galanin and its receptors in the hypothalamus.
Methods and procedures
Reagents
Antibodies against GLUT4 and peroxisome proliferator-activated receptor-γ coactivator-1α (PGC-1α) were from Merck Millipore Inc., Germany. Antibodies against tubulin were from BOSTER Inc., China. RIPA was purchased from Bioteke Corporation (Beijing, China). BCA™ protein assay kit was purchased from Pierce Chemical Company (Pierce, Rockford, USA). Trizol reagent was purchased from Gibco Invitrogen Inc., Invitrogen, USA. Galanin, orexin A, adropin and leptin ELISA assay kits were purchased from CUSABIO, Inc., Wuhan, China. Insulin and irisin ELISA assay kits were purchased from Uscn Life Science, Inc., Wuhan, China.
Animals and feeding schedule
All animal experiments were carried out in accordance with the guidelines of the Animal Care and Use Committee of Yangzhou University. All animals were kept in standard laboratory conditions of temperature 21 ± 2 °C, and relative humidity 50 ± 15%, with water and food available ad libitum. Eight-week-old male C57BL/6 J mice were housed (one mice per cage) under a 12 h light:12 h dark schedule with ad libitum access to normal chow for 2 weeks to adapt to the housing conditions before being randomly assigned to one of the feeding conditions. The mice were fed a high fat diet (20% carbohydrates, 21% protein and 59% fat by energy) for 8 weeks. Then the mice were divided into two groups: fat control group (FC, n = 8) and time-restricted feeding group (TRF, n = 8). The mice in the TRF group were subjected to a time-restricted feeding as previously described [54]. In brief, FC and TRF mice received a high-fat diet with either ad libitum access (FC mice) or during an 8 h window between ZT13 and ZT21 (TRF mice). Access to food was controlled by transferring mice daily between cages with food and water to cages that had only water. Besides, a normal control group (NC, n = 8) was set up. NC mice were fed a normal chow diet with ad libitum access. Animals were maintained on assigned diets and feeding paradigms for 4 weeks. Food intake and body weight were monitored weekly throughout the experiments. At the end of the experiment, all mice were fasted for 12 h and subjected to glucose tolerance test as described below. All animals received human care and all study protocols were approved by the Animal Studies Committee of Yangzhou University.
Metabolic measurements
Animals were fasted for 12 h on paper bedding before the test. Blood glucose levels were measured using One Touch Ultra glucometer prior to injection of glucose (1 g/kg intraperitoneally) and every 30 min after injection.
Collection of blood sample and hypothalamus
After fasting for 12 h, all animals were killed. Then, 1 ml blood, skeletal muscles and hypothalamus were collected quickly. In brief, the blood samples were collected in prechilled EDTA tubes and immediately centrifuged for 5 min at 3500 rpm at 4 °C within 30 min of collection. Plasma was separated into vials and stored at − 80 °C until measurement. The hypothalamus and skeletal muscles were rinsed in precooled phosphate buffer saline and frozen at − 80 °C for further analysis.
Galanin, orexin A, adropin, insulin, irisin and leptin assays
The galanin, orexin A, adropin, insulin, irisin and leptin assays were measured by ELISA under the manufacturer’s instructions. All measurements were performed in duplicate and the mean of two measurements was considered.
Total RNA extraction and RT-qPCR
RNA and cDNA were prepared, and RT-qPCR (reverse transcription-quantitative polymerase chain reaction) was performed as previously described [19, 20]. In brief, RT-qPCR was performed for gene expression levels using real-time fluorescent detection in an Applied Biosystems 7500 real-time PCR instrument (ABI 7500, USA). The oligonucleotide primers are found in Table 1. Amplification condition was: an initial denaturation at 95 °C for 10 min; 95 °C for 15 s, 62 °C for 60 s, 40 cycles. The 2−ΔCT method was used to analyze the PCR data.
Western blot analysis
The total proteins of skeletal muscles were extracted using RIPA agents as described previously and quantified with BCA protein assay kit. Western blot analyses were used to determine the GLUT4 and PGC-1α levels in skeletal muscles. Briefly, 50 µg of samples were separated on a 12% sodium dodecyl sulfate–polyacrylamide gel electrophoresis. The separated proteins were transferred to a polyvinylidene difluoride filter membrane. Membranes were blocked in Tris-buffered saline (pH = 7.5) containing 0.05% Tween-20 (1 × TBST) and 5% skimmed milk for 2 h, then probed overnight at 4 °C with an antibody against tubulin, GLUT4 and PGC-1α respectively. Membranes were washed three times with 1 × TBST for 10 min and incubated for 2 h with horseradish peroxidase-conjugated secondary antibody. Lastly, immunoreactive bands were visualized by chemiluminescence and quantified by densitometry using a Quantity One Analysis Software (Bio-Rad).
Statistical analysis
SPSS 17.0 for Windows was used for statistical analysis. Comparisons between the means of three groups were analyzed by one-way ANOVA with Duncan’s multiple-range tests. Data were presented as mean ± SEM with p < 0.05 as the limit for statistical significance.
Results
TRF regimen ameliorates glucose intolerance and systemic insulin resistance
All mice used in this experiment exhibited similar body weight and food intake at the beginning of the experiment. After fed with a high-fat diet for 6 weeks, the mice started to demonstrate a significant increase in body weight compared with age- and gender-matched mice on a normal diet (Fig. 1A). At the end of time-restricted feeding for 4 weeks, the body weight was decreased in the TRF group compared with the FC group (p > 0.05), while the body weight was significantly increased in the FC group compared with the NC group (p < 0.01) (Fig. 1A). As shown in Fig. 1B, the food intake of mice was not obviously decreased in the TRF group compared with the FC group per week (p > 0.05). These results suggest that mice fed with a high-fat diet ad libitum may develop obesity and metabolic syndrome. Time-limiting access to high-fat diet at night for up to 4 weeks shows some improvement in body weight regulation.
TRF regimen ameliorates glucose intolerance and systemic insulin resistance (n = 8). A During the 4 weeks of TRF regimen, the body weight of mice was measured. The body weight was decreased in the TRF group compared with the FC group (P > 0.05), while the body weight was significantly increased in the FC group compared with the NC group (P < 0.01). B The food intake of mice was not obviously changed in the TRF group compared with the FC group in per week (P > 0.05), while food intake of mice was significantly increased in the FC group compared with the NC group in per week (P < 0.01). C The fasting glucose level was significantly elevated in the FC group compared with the NC group (P < 0.01). After 4 weeks of time-restricted feeding regimen, the mice had a decrease of fasting hyperglycemia (P < 0.01). D The fasting insulin level was significantly elevated in the FC group compared with the NC group (P < 0.01), while the fasting insulin level was not obviously changed in the TRF group compared with the FC group (P > 0.05). E The HOMA-IR was significantly elevated in the FC group compared with the NC group (P < 0.01), while the HOMA-IR was significantly decreased in the FC group compared with the NC group (P < 0.01). F The circulating glucose levels were markedly increased in the fasted state and in response to glucose load in the FC group compared with the NC group (P < 0.01). After 4 weeks of time-restricted feeding regimen, the mice had an improvement in glucose tolerance associated with a decrease in plasma glucose levels in the fasted state and in response to glucose load compared with the FC mice (P < 0.05). G The AUC was significantly elevated in the FC group compared with the NC group (P < 0.01), while the AUC was decreased in the FC group compared with the NC group (P < 0.05). Comparisons between the means of three groups were analyzed by one-way ANOVA with Duncan’s multiple-range tests. All data shown are the means ± SEM. *P < 0.05&**P < 0.01 vs. FC; ##P < 0.01 vs. NC
As shown in Fig. 1C, D, the fasting glucose and insulin levels were significantly elevated in the FC group compared with the NC group (p < 0.01). During the glucose tolerance test, the circulating glucose levels were markedly increased in the fasted state and in response to glucose load in the FC group compared with the NC group (p < 0.01) (Fig. 1F). Besides, the HOMA-IR and areas of glucose tolerance (AUC) were significantly increased in the FC group compared with the NC group (p < 0.01) (Fig. 1E, G).
After 4 weeks of time-restricted feeding regimen, the mice had a decrease of fasting hyperglycemia (p < 0.01) and an improvement in glucose tolerance associated with a decrease in plasma glucose levels in the fasted state and in response to glucose load (p < 0.05) compared with the FC mice (Fig. 1C, F). However, we did not observe significant variation of plasma insulin in response to time-restricted feeding regimen compared with FC mice (p > 0.05) (Fig. 1D), which suggests TRF-induced reduction in glucose stems from effects on insulin sensitivity, rather than on insulin levels. Moreover, the HOMA-IR and areas of glucose tolerance were significantly lower in time-restricted feeding regimen mice than in FC mice (Fig. 1E, G) (p < 0.05). These results suggest that the TRF regimen improves systemic insulin sensitivity and glucose homeostasis.
TRF regimen regulates the levels of plasma orexin A, leptin, irisin and adropin
As shown in Fig. 2A–D, the fasting orexin A, leptin, irisin and adropin levels were significantly elevated in the FC group compared with those in the NC group (p < 0.01). However, after 4 weeks of time-restricted feeding regimen, the mice displayed a significant decrease in the plasma orexin A, irisin and adropin compared with FC mice (p < 0.01), but a significant increase in plasma leptin compared with FC mice (p < 0.01). These results suggest that time-restricted feeding regimen is involved in the regulation of many neuropeptides are induced by nutritional challenge when food is available ad libitum.
The levels of orexin A, leptin, irisin and adropin in TRF mice (n = 8). A Compared with the FC group, TRF mice displayed a marked decrease in level of plasma orexin A (P < 0.01). B Compared with the FC group, and TRF mice displayed a marked decrease in level of plasma irisin (P < 0.01). C Compared with the FC group, TRF mice displayed a marked decrease in level of plasma adropin (P < 0.01). D Compared with the FC group, TRF mice displayed a marked increase in the level of plasma leptin (P < 0.01). Comparisons between the means of three groups were analyzed by one-way ANOVA with Duncan’s multiple-range tests. All data shown are the means ± SEM. **P < 0.01 vs. FC; ##P < 0.01 vs. NC
TRF regimen regulates the expression of GAL and its receptors
As shown in Fig. 3A, the fasting galanin levels were significantly elevated in the FC group compared with those in the NC group (p < 0.01). Furthermore, the galanin mRNA and GALR1 mRNA expression levels were significantly increased in the hypothalamus of the FC group compared with the NC group (p < 0.01), although we did not observe significant variation of GALR2 mRNA expression levels in mice fed with a high-fat diet ad libitum compared with NC mice (p > 0.05) (Fig. 3B–D). After 4 weeks of time-restricted feeding regimen, the mice displayed a significant decrease in the plasma galanin and galanin mRNA and GALR1 mRNA expression of hypothalamus compared with FC mice (p < 0.01) (Fig. 3A–C). However, the GALR2 mRNA expression levels were significantly increased in the hypothalamus of the TRF group compared with those in the FC group (p < 0.01) (Fig. 3D). These results suggested that the TRF regimen regulated galanin and galanin receptor expression.
The levels of plasma GAL and GAL mRNA, GALR1 mRNA, GALR2 mRNA expression in the hypothalamus of TRF mice (n = 6–8). A Compared with the FC group, TRF mice displayed a marked decrease in level of plasma galanin (P < 0.01). B Compared with FC mice, mice under a time-restricted high-fat diet displayed a marked reduction in level of GAL mRNA expression of hypothalamus (P < 0.01). C Compared with FC mice, mice under a time-restricted high-fat diet displayed a marked reduction in the level of GALR1 mRNA expression of the hypothalamus (P < 0.01). D The GALR2 mRNA expression level was significantly increased in the hypothalamus of the TRF group compared with the FC group (P < 0.01). Comparisons between the means of the three groups were analyzed by one-way ANOVA with Duncan’s multiple-range tests. All data shown are the means ± SEM. **P < 0.01 vs. FC; ##P < 0.01 vs. NC
TRF regimen increases the PGC-1α and GLUT4 levels of skeletal muscles
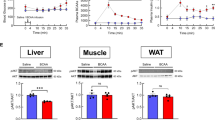
As shown in Fig. 4A, B, the GLUT4 mRNA and PGC-1α mRNA expression levels were significantly decreased in the skeletal muscles of the FC group compared with those in the NC group (p < 0.01). Compared with the FC group mice, mice under a time-restricted high-fat diet displayed a marked elevation in the levels of GLUT4 mRNA and PGC-1α mRNA expression of skeletal muscles (p < 0.01). As shown in Fig. 4C–E, the GLUT4 and PGC-1α contents were significantly decreased in the skeletal muscles of the FC group compared with those in the NC group (p < 0.01). Compared with the FC group mice, mice under a time-restricted high-fat diet displayed a marked increase in the levels of GLUT4 and PGC-1α protein of skeletal muscles (p < 0.01). These results suggested that the TRF regimen improved the PGC-1α and GLUT4 expression in skeletal muscles.
The GLUT4 and PGC-1α expression levels in the skeletal muscles of TRF mice (n = 6). A Compared with FC mice, mice under a time-restricted high-fat diet displayed a marked increase in the level of GLUT4 mRNA expression of skeletal muscles (P < 0.01). B Compared with FC mice, mice under a time-restricted high-fat diet displayed a marked increase in the level of PGC-1α mRNA expression of skeletal muscles (P < 0.01). C The GLUT4 content was significantly decreased in the skeletal muscles of the FC group compared with the NC group (P < 0.01). Compared with the FC mice, mice under a time-restricted high-fat diet displayed a marked increase in the level of GLUT4 in skeletal muscles (P < 0.01). D The PGC-1α content was significantly decreased in the skeletal muscles of the FC group compared with the NC group (P < 0.01). Compared with the FC mice, mice under a time-restricted high-fat diet displayed a marked increase in the level of PGC-1α in skeletal muscles (P < 0.01). E The representative western blot of GLUT4 and PGC-1α. Comparisons between the means of three groups were analyzed by one-way ANOVA with Duncan’s multiple-range tests. All data shown are the means ± SEM. **P < 0.01 vs. FC; ##P < 0.01 vs. NC
Discussion
Lifestyle interventions, including changes in diet, reduced caloric intake and increased exercise, have been the first-line therapy in efforts to combat obesity and its complications. Among these interventions, temporal regulation of feeding offers an innovative strategy to prevent and treat obesity and associated metabolic diseases [38]. Recent studies have shown that preventing obesity with time-restricted feeding (TRF) is an innovative and promising strategy [8, 10, 11, 27, 41, 44, 46, 54]. It emphasizes caloric intake, hence making it an attractive and easily adoptable lifestyle modification. Restricting feeding to 8 h of a rodent’s preferred nocturnal feeding time protects against weight gain and associated metabolic diseases [27]. TRF regimen improved sleep and weight loss as well as deceleration of cardiac aging, even when caloric intake and expenditure were unchanged [25]. The mechanisms by which TRF protects against age- and diet-induced decline in cardiac function may be relative to the circadian clock, TRiC chaperonin and mitochondrial ETC [25]. However, the central mechanisms of TRF against metabolic disorders has not been sufficiently explored.
Previous studies have shown that mice under a time-restricted high-fat diet consume equivalent calories as those with ad libitum access are against preexisting obesity [27, 47, 54]. The preliminary evidence in humans suggests that the benefits of TRF are due mostly or only to weight loss [22]. In agreement with these results, we found that mice fed a high-fat diet ad libitum can develop obesity, while TRF regimen during 4 weeks may maintain weight stability of mice fed with a high-fat diet. These results suggest that time-limiting access to high-fat diet at night for up to 4 weeks is of great help to body weight regulation. In addition, a recent study on humans further demonstrated that the TRF regimen for 5 weeks improved insulin sensitivity, β cell responsiveness, oxidative stress, blood pressure and appetite in men with prediabetes [48]. In this study, our data demonstrated that the TRF regimen reversed high fat diet-induced glucose intolerance and hyperglycemia in diet-induced obese mice. Furthermore, we also detected the role of TRF in glucose metabolism and insulin sensitivity in skeletal muscles. About 85% of insulin-stimulated glucose uptake occurs in skeletal muscles. This process is important for controlling whole-body energy homeostasis [37]. It has been clearly established that glucose transporter 4 (GLUT4) is a particularly important glucose transporter for maintaining glucose transport into skeletal muscles [37]. In addition, PGC-1α is a critical regulator of mitochondrial biogenesis in skeletal muscles to maintain an energy balance [43, 52]. PGC-1α can enhance the expression of GLUT4 to increase glucose uptake in skeletal muscles [4, 45, 51]. Therefore, the levels of PGC-1α and GLUT4 are major indexes that reflect the activity of glucose uptake and insulin sensitivity in skeletal muscles [37, 52]. The results in this study illustrated that the TRF regimen in mice led to elevated mRNA and protein expression of PGC-1α and GLUT4 in skeletal muscle under HFD-fed conditions, suggesting that the effect of TRF on glucose metabolism is stimulation and activation. Our data corroborated previous report that the TRF regimen could induce the expression of many genes associated with the function of glucose transport and metabolism in skeletal muscles [27, 47]. Together with these findings, our data suggest that the TRF regimen ameliorates metabolic dysfunction by activation of PGC-1α/GLUT4 axis-mediated glucose metabolism in skeletal muscles.
The central mechanisms underlying the increase of glucose metabolism in TRF mice remains unclear, but previous studies found that central galanin is a critical element linking energy metabolism and glucose homeostasis [16, 18], and the feeding status could modulate central galanin expression [6, 32]. Therefore, we further analyze the levels of galanin and its receptors in the hypothalamus during scheduled feeding and evaluate the central mechanisms of TRF on obesity-related metabolic diseases. As expected, the levels of plasma galanin were significantly increased along with a trend of the elevation of orexin A, irisin and adropin in mice fed with a high fat diet when compared to the normal control mice. Besides, the levels of galanin mRNA expression were increased in the hypothalamus of mice fed a high fat diet. Our data corroborated previous report that galanin level and proliferation of galanin-producing neurons were increased in the hypothalamus of rats fed a high fat diet [35], suggesting that central galanin provides positive feedback to increase food intake and body weight in response to high-fat consumption [2, 13]. Besides, previous studies showed that central galanin-induced increase in fat intake is mainly mediated by GALR1 [13, 15, 34]. These suggest that the GAL–GALR1 systems help adapt food intake and metabolism to changes in dietary fat. Results in this study illustrated that the TRF regimen diminished plasma galanin as well as hypothalamic galanin and GALR1 expression, but increased GALR2 expression in the hypothalamus of mice fed a high-fat diet. Our observations expand on these studies and document that TRF regimen could reduce fat intake by inhibition of the GAL–GALR1 system and subsequently promote the weight loss in obese mice. In addition, it is plausible that the lower levels of galanin will upregulate the expression of the GALR2 located in the hypothalamus, which may, in turn, stimulate the GALR2-mediated signaling pathways in the hypothalamus, which is known to promote systemic glucose metabolism and energy homeostasis [1, 19, 20, 28]. Activated GALR2 significantly increased GLUT4 expression in skeletal muscles, suggesting that activation of central GALR2 mediates the galanin roles to promote insulin sensitivity in the skeletal muscles [12, 19, 20, 26, 55]. Injection with a GALR2 agonist, M1145, into the lateral hypothalamus of mice might restore the ability of leptin to suppress overeating of high-fat/high-sucrose foods, suggesting that activation of central GALR2 mediates the promoting effect of galanin on leptin sensitivity in the lateral hypothalamus [33]. Therefore, GALR2 improves glycemic control via restoration of insulin sensitivity and leptin sensitivity. Considering the results obtained from our previous studies, we conclude that the metabolic changes of TRF mice may be related to the expression of GALR2 in the hypothalamus. Therefore, the changes of galanin, GALR1 and GALR2 in the hypothalamus are involved in the central mechanism of TRF regulating energy metabolism in mice fed a high-fat diet.
Conclusions
The previous studies confirmed a critical role of hypothalamic galanin and its receptors in the regulation of glucose metabolism and energy balance [1, 21, 28]. The current study addressed the question whether TRF could regulate the expression of galanin and its receptors in the hypothalamus of mice fed a high-fat diet. We demonstrated that TRF diminished galanin and GALR1 expression, and increased GALR2 expression in the hypothalamus of mice fed a high-fat diet. The current studies provide additional evidence that TRF is effective in improving HFD-induced hyperglycemia and insulin resistance in mice, and this effect could be associated with TRF-induced changes of the galanin systems in the hypothalamus. Future pre-clinical studies are necessary to define the relationship between TRF-induced metabolic changes and the galanin system.
What is already known on this subject?
The previous studies confirmed a critical role of hypothalamic galanin and its receptors in the regulation of glucose metabolism and energy balance. Several studies found that time-restricted feeding (TRF) reversed obesity and insulin resistance. However, there were limited studies focused on the central mechanisms of TRF on obesity-related metabolic diseases.
What does this study add?
Our findings revealed that TRF diminished galanin and GALR1 expression, and increased GALR2 expression in the hypothalamus of mice fed a high-fat diet. Our results suggested that the central mechanisms of TRF on obesity-related metabolic diseases could be associated with the changes of the galanin systems in the hypothalamus. TRF regimen may be a nonpharmacological strategy against obesity-related metabolic diseases.
References
Abot A, Lucas A, Bautzova T, Bessac A, Fournel A, Le-Gonidec S, Valet P, Moro C, Cani PD, Knauf C (2018) Galanin enhances systemic glucose metabolism through enteric Nitric Oxide Synthase-expressed neurons. Mol Metab 10:100–108. https://doi.org/10.1016/j.molmet.2018.01.020
Adams AC, Clapham JC, Wynick D, Speakman JR (2008) Feeding behaviour in galanin knockout mice supports a role of galanin in fat intake and preference. J Neuroendocrinol 20:199–206. https://doi.org/10.1111/j.1365-2826.2007.01638.x
Asher G, Sassone-Corsi P (2015) Time for food: the intimate interplay between nutrition, metabolism, and the circadian clock. Cell 161(1):84–92. https://doi.org/10.1016/j.cell.2015.03.015
Benton CR, Holloway GP, Han XX, Yoshida Y, Snook LA, Lally J, Glatz JF, Luiken JJ, Chabowski A, Bonen A (2010) Increased levels of peroxisome proliferator-activated receptor gamma, coactivator 1 alpha (PGC-1alpha) improve lipid utilisation, insulin signalling and glucose transport in skeletal muscle of lean and insulin-resistant obese Zucker rats. Diabetologia 53:2008–2019. https://doi.org/10.1007/s00125-010-1773-1
Beck B, Burlet A, Nicolas JP, Burlet C (1993) Galanin in the hypothalamus of fed and fasted lean and obese Zucker rats. Brain Res 623(1):124–130. https://doi.org/10.1016/0006-8993(93)90019-j
Bocarsly ME, Avena NM (2013) A high-fat diet or galanin in the PVN decreases phosphorylation of CREB in the nucleus accumbens. Neuroscience 248:61–66. https://doi.org/10.1016/j.neuroscience.2013.05.046
Bray MS, Tsai JY, Villegas-Montoya C, Boland BB, Blasier Z, Egbejimi O, Kueht M, Young ME (2010) Time-of-day-dependent dietary fat consumption influences multiple cardiometabolic syndrome parameters in mice. Int J Obes (Lond) 34(11):1589–1598. https://doi.org/10.1038/ijo.2010.63
Chaix A, Zarrinpar A, Miu P, Panda S (2014) Time-restricted feeding is a preventative and therapeutic intervention against diverse nutritional challenges. Cell Metab 20(6):991–1005. https://doi.org/10.1016/j.cmet.2014.11.001
Chaix A, Lin T, Le HD, Chang MW, Panda S (2018) Time-restricted feeding prevents obesity and metabolic syndrome in mice lacking a circadian clock. Cell Metab. https://doi.org/10.1016/j.cmet.2018.08.004
Chung H, Chou W, Sears DD, Patterson RE, Webster NJ, Ellies LG (2016) Time-restricted feeding improves insulin resistance and hepatic steatosis in a mouse model of postmenopausal obesity. Metabolism 65(12):1743–1754. https://doi.org/10.1016/j.metabol.2016.09.006
Duncan MJ, Smith JT, Narbaiza J, Mueez F, Bustle LB, Qureshi S, Fieseler C, Legan SJ (2016) Restricting feeding to the active phase in middle-aged mice attenuates adverse metabolic effects of a high-fat diet. Physiol Behav 167:1–9. https://doi.org/10.1016/j.physbeh.2016.08.027
El-Saka MH, Abo El Gheit RE, El Saadany A, Alghazaly GM, Marea KE, Madi NM (2021) Effect of spexin on renal dysfunction in experimentally obese rats: potential mitigating mechanisms via galanin receptor-2. Arch Physiol Biochem 25:1–10. https://doi.org/10.1080/13813455.2021.1887265
Fang P, Yu M, Guo L et al (2012) Galanin and its receptors: a novel strategy for appetite control and obesity therapy. Peptides 36:331–339. https://doi.org/10.1016/j.peptides.2012.05.016
Fang P, Bo P, Shi M, Yu M, Zhang Z (2013) Circulating galanin levels are increased in patients with gestational diabetes mellitus. Clin Biochem 46(9):831–833. https://doi.org/10.1016/j.clinbiochem.2012.12.013
Fang P, He B, Shi M, Kong G, Dong X, Zhu Y, Bo P, Zhang Z (2015) The regulative effect of galanin family members on link of energy metabolism and reproduction. Peptides 71:240–249. https://doi.org/10.1016/j.peptides.2015.07.007
Fang P, Shi M, Zhu Y, Bo P, Zhang Z (2016) Type 2 diabetes mellitus as a disorder of galanin resistance. Exp Gerontol 73:72–77. https://doi.org/10.1016/j.exger.2015.11.007
Fang P, Yu M, Gu X, Shi M, Zhu Y, Zhang Z, Bo P (2016) Circulating galanin and galanin like peptide concentrations are correlated with increased triglyceride concentration in obese patients. Clin Chim Acta 461:126–129. https://doi.org/10.1016/j.cca.2016.07.019
Fang P, Yu M, He B, Guo L, Huang X, Kong G, Shi M, Zhu Y, Bo P, Zhang Z (2017) Central injection of GALR1 agonist M617 attenuates diabetic rat skeletal muscle insulin resistance through the Akt/AS160/GLUT4 pathway. Mech Ageing Dev 162:122–128. https://doi.org/10.1016/j.mad.2016.03.013
Fang P, He B, Yu M, Shi M, Zhu Y, Zhang Z, Bo P (2018) Central galanin receptor 2 mediates galanin action to promote systemic glucose metabolism of type 2 diabetic rats. Biochem Pharmacol 156:241–247. https://doi.org/10.1016/j.bcp.2018.08.036
Fang P, Zhang L, Yu M, Sheng Z, Shi M, Zhu Y, Zhang Z, Bo P (2018) Activiated galanin receptor 2 attenuates insulin resistance in skeletal muscle of obese mice. Peptides 99:92–98. https://doi.org/10.1016/j.peptides.2017.11.018
Fang P, Yu M, Shi M, Bo P, Zhang Z (2020) Galanin peptide family regulation of glucose metabolism. Front Neuroendocrinol 56:100801. https://doi.org/10.1016/j.yfrne.2019.100801
Gabel K, Hoddy KK, Haggerty N, Song J, Kroeger CM, Trepanowski JF, Panda S, Varady KA (2018) Effects of 8-hour time restricted feeding on body weight and metabolic disease risk factors in obese adults: a pilot study. Nutr Healthy Aging 4:345–353. https://doi.org/10.3233/NHA-170036
Gaysinskaya VA, Karatayev O, Chang GQ, Leibowitz SF (2007) Increased caloric intake after a high-fat preload: relation to circulating triglycerides and orexigenic peptides. Physiol Behav 91:142–153. https://doi.org/10.1016/j.physbeh.2007.02.002
García-Luna C, Soberanes-Chávez P, de Gortari P (2017) Prepuberal light phase feeding induces neuroendocrine alterations in adult rats. J Endocrinol 232(1):15–28. https://doi.org/10.1530/JOE-16-0402
Gill S, Le HD, Melkani GC, Panda S (2015) Time-restricted feeding attenuates age-related cardiac decline in Drosophila. Science 347(6227):1265–1269. https://doi.org/10.1126/science.1256682
Guo L, He B, Fang P, Bo P, Zhang Z (2021) Activation of central galanin receptor 2 mitigated insulin resistance in adipocytes of diabetic rats. J Endocrinol Invest 44(3):515–522. https://doi.org/10.1007/s40618-020-01336-z
Hatori M, Vollmers C, Zarrinpar A, DiTacchio L, Bushong EA, Gill S, Leblanc M, Chaix A, Joens M, Fitzpatrick JA, Ellisman MH, Panda S (2012) Time-restricted feeding without reducing caloric intake prevents metabolic diseases in mice fed a high-fat diet. Cell Metab 15(6):848–860. https://doi.org/10.1016/j.cmet.2012.04.019
Idelevich A, Sato K, Nagano K, Rowe G, Gori F, Baron R (2018) Neuronal hypothalamic regulation of body metabolism and bone density is galanin dependent. J Clin Invest 128:2626–2641. https://doi.org/10.1172/JCI99350
Karatayev O, Baylan J, Leibowitz SF (2009) Increased intake of ethanol and dietary fat in galanin overexpressing mice. Alcohol 43:571–580. https://doi.org/10.1016/j.alcohol.2009.09.025
Karatayev O, Baylan J, Weed V, Chang S, Wynick D, Leibowitz SF (2010) Galanin knockout mice show disturbances in ethanol consumption and expression of hypothalamic peptides that stimulate ethanol intake. Alcohol Clin Exp Res 34:72–80. https://doi.org/10.1111/j.1530-0277.2009.01068.x
Kohsaka A, Laposky AD, Ramsey KM, Estrada C, Joshu C, Kobayashi Y, Turek FW, Bass J (2007) High-fat diet disrupts behavioral and molecular circadian rhythms in mice. Cell Metab 6(5):414–421. https://doi.org/10.1016/j.cmet.2007.09.006
Knight ZA, Tan K, Birsoy K, Schmidt S, Garrison JL, Wysocki RW, Emiliano A, Ekstrand MI, Friedman JM (2012) Molecular profiling of activated neurons by phosphorylated ribosome capture. Cell 151(5):1126–1137. https://doi.org/10.1016/j.cell.2012.10.039
Leidmaa E, Gazea M, Patchev AV, Pissioti A, Christian Gassen N, Kimura M, Liposits Z, Kallo I, Almeida OFX (2020) Blunted leptin sensitivity during hedonic overeating can be reinstated by activating galanin 2 receptors (Gal2R) in the lateral hypothalamus. Acta Physiol (Oxf) 228(2):e13345. https://doi.org/10.1111/apha.13345
Lang R, Gundlach AL, Holmes FE, Hobson SA, Wynick D, Hökfelt T, Kofler B (2015) Physiology, signaling, and pharmacology of galanin peptides and receptors: three decades of emerging diversity. Pharmacol Rev 67:118–175. https://doi.org/10.1124/pr.112.006536
Leibowitz SF, Dourmashkin JT, Chang GQ, Hill JO, Gayles EC, Fried SK, Wang J (2004) Acute high-fat diet paradigms link galanin to triglycerides and their transport and metabolism in muscle. Brain Res 1008(2):168–178. https://doi.org/10.1016/j.brainres.2004.02.030
Legakis I, Mantzouridis T, Mountokalakis T (2005) Positive correlation of galanin with glucose in type 2 diabetes. Diabetes Care 28:759–760. https://doi.org/10.2337/diacare.28.3.759
Leto D, Saltiel AR (2012) Regulation of glucose transport by insulin: traffic control of GLUT4. Nat Rev Mol Cell Biol 13(6):383–396. https://doi.org/10.1038/nrm3351
Longo VD, Panda S (2016) Fasting, circadian rhythms, and time-restricted feeding in healthy lifespan. Cell Metab 23(6):1048–1059. https://doi.org/10.1016/j.cmet.2016.06.001
Méquinion M, Le Thuc O, Zgheib S, Alexandre D, Chartrel N, Rovère C, Hardouin P, Viltart O, Chauveau C (2017) Long-term energy deficit in mice causes long-lasting hypothalamic alterations after recovery. Neuroendocrinology 105(4):372–383. https://doi.org/10.1159/000455048
Melkani GC, Panda S (2017) Time-restricted feeding for prevention and treatment of cardiometabolic disorders. J Physiol 595(12):3691–3700. https://doi.org/10.1113/JP273094
Olsen MK, Choi MH, Kulseng B, Zhao CM, Chen D (2017) Time-restricted feeding on weekdays restricts weight gain: a study using rat models of high-fat diet-induced obesity. Physiol Behav 173:298–304. https://doi.org/10.1016/j.physbeh.2017.02.032
Plaisier CL, Kyttälä M, Weissglas-Volkov D, Sinsheimer JS, Huertas-Vazquez A, Riba L, Ramírez-Jiménez S, de Bruin TW, Tusié-Luna T, Aouizerat BE, Pullinger CR, Malloy MJ, Kane JP, Cruz-Bautista I, Herrera MF, Aguilar-Salinas C, Kuusisto J, Laakso M, Taskinen MR, van der Kallen CJ, Pajukanta P (2009) Galanin preproprotein is associated with elevated plasma triglycerides. Arterioscler Thromb Vasc Biol 29(1):147–152. https://doi.org/10.1161/ATVBAHA.108.178533
Puigserver P, Adelmant G, Wu Z, Fan M, Xu J, O'Malley B, Spiegelman BM (1999) Activation of PPARγ coactivator-1 through transcription factor docking. Science 286(5443):1368–1371. https://doi.org/10.1126/science.286.5443.1368
Rothschild J, Hoddy KK, Jambazian P, Varady KA (2014) Time-restricted feeding and risk of metabolic disease: a review of human and animal studies. Nutr Rev 72(5):308–318. https://doi.org/10.1111/nure.12104
Summermatter S, Shui G, Maag D, Santos G, Wenk MR, Handschin C (2013) PGC-1α improves glucose homeostasis in skeletal muscle in an activity-dependent manner. Diabetes 62(1):85–95. https://doi.org/10.2337/db12-0291
Sundaram S, Yan L (2016) Time-restricted feeding reduces adiposity in mice fed a high-fat diet. Nutr Res 36(6):603–611. https://doi.org/10.1016/j.nutres.2016.02.005
Sherman H, Genzer Y, Cohen R, Chapnik N, Madar Z, Froy O (2012) Timed high-fat diet resets circadian metabolism and prevents obesity. FASEB J 26(8):3493–3502. https://doi.org/10.1096/fj.12-208868
Sutton EF, Beyl R, Early KS, Cefalu WT, Ravussin E, Peterson CM (2018) Early time-restricted feeding improves insulin sensitivity, blood pressure, and oxidative stress even without weight loss in men with prediabetes. Cell Metab 27(6):1212–1221. https://doi.org/10.1016/j.cmet.2018.04.010
Villanueva JE, Livelo C, Trujillo AS, Chandran S, Woodworth B, Andrade L, Le HD, Manor U, Panda S, Melkani GC (2019) Time-restricted feeding restores muscle function in Drosophila models of obesity and circadian-rhythm disruption. Nat Commun 10(1):2700. https://doi.org/10.1038/s41467-019-10563-9
Wang D, Opperhuizen AL, Reznick J, Turner N, Su Y, Cooney GJ, Kalsbeek A (2017) Effects of feeding time on daily rhythms of neuropeptide and clock gene expression in the rat hypothalamus. Brain Res 1671:93–101. https://doi.org/10.1016/j.brainres.2017.07.006
Wright DC (2007) Mechanisms of calcium-induced mitochondrial biogenesis and GLUT4 synthesis. Appl Physiol Nutr Metab 32(5):840–845. https://doi.org/10.1139/H07-062
Wu Z, Puigserver P, Andersson U, Zhang C, Adelmant G, Mootha V, Troy A, Cinti S, Lowell B, Scarpulla RC, Spiegelman BM (1999) Mechanisms controlling mitochondrial biogenesis and respiration through the thermogenic coactivator PGC-1. Cell 98:115–124. https://doi.org/10.1016/S0092-8674(00)80611-X
Yun R, Dourmashkin JT, Hill J, Gayles EC, Fried SK, Leibowitz SF (2005) PVN galanin increases fat storage and promotes obesity by causing muscle to utilize carbohydrate more than fat. Peptides 26:2265–2273. https://doi.org/10.1016/j.peptides.2005.04.005
Zarrinpar A, Chaix A, Yooseph S, Panda S (2014) Diet and feeding pattern affect the diurnal dynamics of the gut microbiome. Cell Metab 20(6):1006–1017. https://doi.org/10.1016/j.cmet.2014.11.008
Zhang Z, Fang P, He B, Guo L, Runesson J, Langel Ü, Shi M, Zhu Y, Bo P (2016) Central administration of Galanin receptor 1 agonist boosted insulin sensitivity in adipose cells of diabetic rats. J Diab Res 2016. https://doi.org/10.1155/2016/9095648
Zhang Z, Fang P, Yu M, Wang Y, Li Y, Shi M, Bo P, Gu X, Zhu Y (2017) Serum galanin concentration is increased in subjects with impaired glucose tolerance. Can J Diabetes 41:563–566. https://doi.org/10.1016/j.jcjd.2017.01.001
Acknowledgements
This work was supported by the Natural Scientific Fund of Jiangsu (No. BK20171319).
Author information
Authors and Affiliations
Contributions
ZZ and JS conceived and designed the experiments. JS, YS and PF performed the experiments. JS and XG analyzed the data. ZZ, PF and XG contributed reagents/materials/analysis tools. ZZ and JS wrote the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declared no conflict of interest.
Ethical approval
This study was approved by Animal Ethics Committee of Yangzhou University.
Informed consent
For this type of study, no informed consent is required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sun, J., She, Y., Fang, P. et al. Time-restricted feeding prevents metabolic diseases through the regulation of galanin/GALR1 expression in the hypothalamus of mice. Eat Weight Disord 27, 1415–1425 (2022). https://doi.org/10.1007/s40519-021-01280-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-021-01280-8